Marrubiin
Abstract
:1. Introduction
2. Occurrence
3. Physical and Spectroscopic Data [31]
4. Biosynthesis
| Physical properties | Value | NMR data [37] |
|---|---|---|
| Molecular weight | 332.43 |  * Overlapped signals |
| Molecular formula | C20 H28 O4 | |
| CAS Registry Number | 465-92-9 | |
| Molar volume | 288 ± 3.0 cm3/mol(20 °C; 760 Torr) | |
| Density | 1.152±0.06 g/cm3(20 °C; 760 Torr) | |
| Melting Point | ~155–160 °C | |
| Freely Rotatable Bonds | 4 | |
| H Acceptors | 4 | |
| H Donors | 1 | |
| H Donor/ Acceptor sum | 5 | |
| LogP | 3.796±0.414 (at 25 °C) | |
| [α]D: | +45.68° (acetone, 24 °C), +35.8 (CHCl3, 24 °C) |
5. Chemical Aspects
5.1. Synthesis
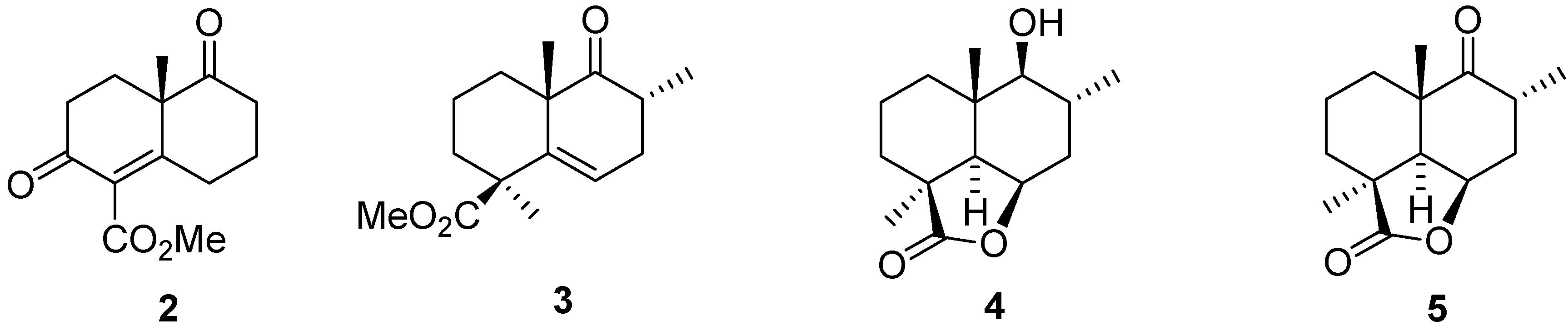
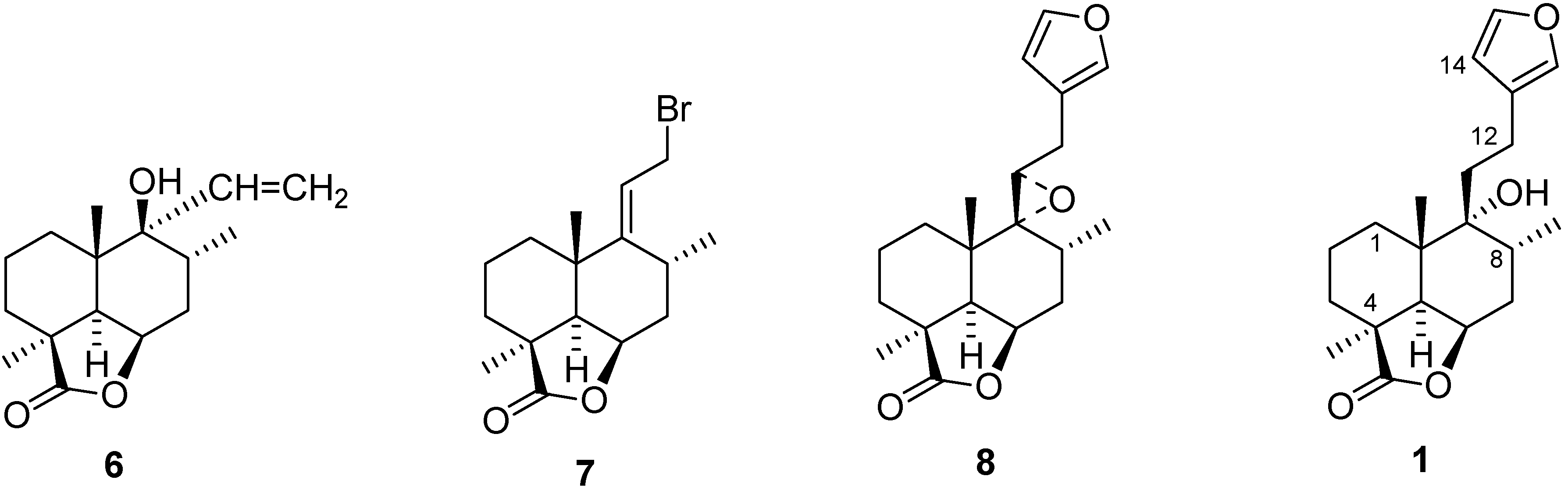
5.2. Structure Modification
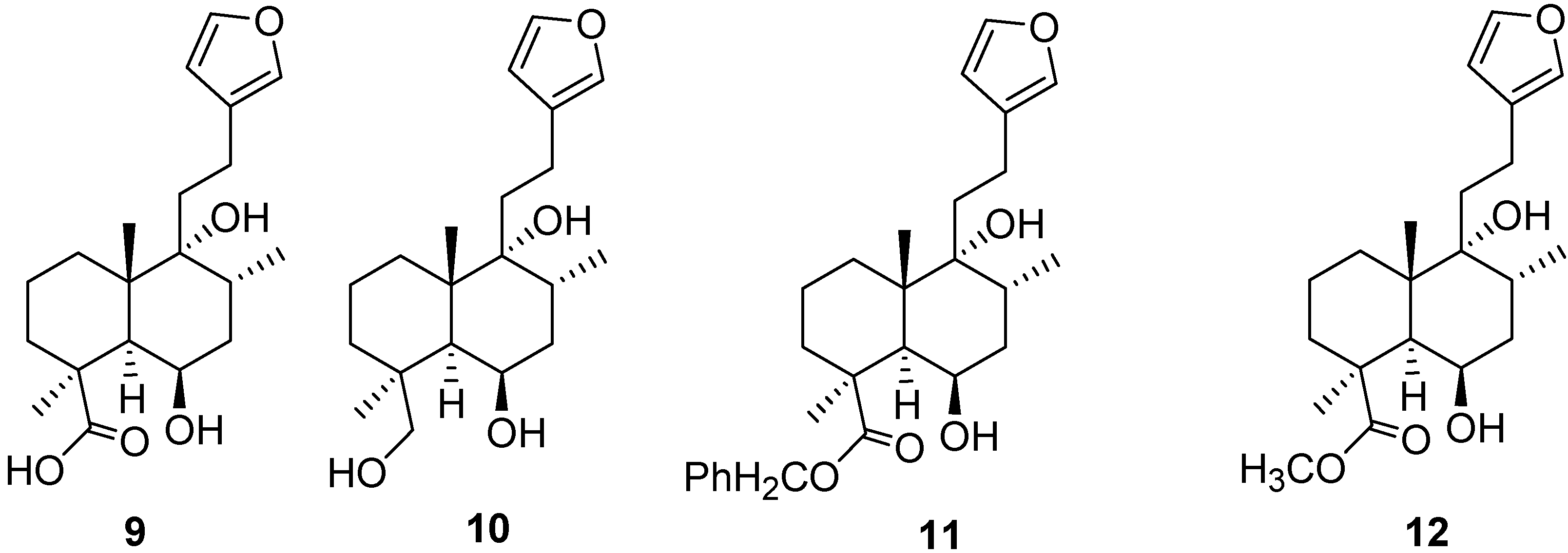
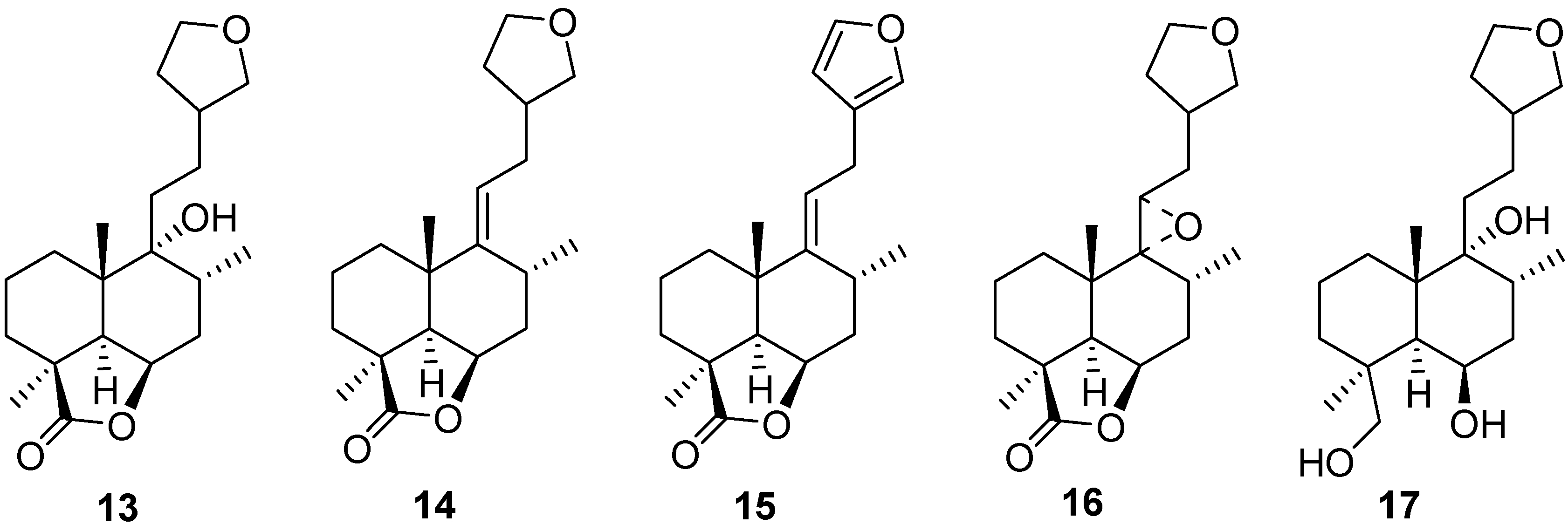
6. Pharmacological Aspects of Marrubiin
6.1. Toxicity Studies
6.2. Antinociceptive Activity
6.3. Cardioprotective Activity
6.4. Gastroprotective (Anti Ulcer) Activity
6.5. Anti-Diabetic Activity
6.6. Antispasmodic and Ca2+ Antagonist Potential
6.7. Antioedematogenic Activity
6.8. Analgesic Activity
6.9. Anticoagulant and Antiplatelet Activities
6.10. Vasorelaxant Potential
7. Conclusions
Acknowledgments
Conflicts of Interest
References
- Abbondanza, A.A.; Breccia, A. Crespi. Biosynthesis of labeled molecules: mechanism of biosynthetic reactions of precursors of furanicterpenes and phytosterol. Prepn. Bio-Med. Appl. Labeled Mol. Proc. Symp. Venice 1964, 67, 95–101. [Google Scholar]
- Marrelli, M.; Conforti, F.; Rigano, D.; Formisano, C.; Bruno, M.; Senatore, F.; Menichini, F. Cytotoxic properties of Marrubium globosum ssp. libanoticum and its bioactive components. Nat. Prod. Comm. 2013, 8, 567–569. [Google Scholar]
- Mnonopi, N.; Levendal, R.A.; Davies-Coleman, R.T.; Frost, C.L. The cardioprotective effects of marrubiin, a diterpenoid found in Leonotis leonurus extracts. J. Ethnopharmacol. 2011, 138, 67–75. [Google Scholar] [CrossRef]
- Laonigro, G.; Lanzetta, R.; Parrilli, M.; Adinolfi, M.; Mangoni, L. The configuration of the diterpene spiro ethers from Marrubium vulgare and from Leonotis leonurus. Gazz. Chim. Ital. 1979, 109, 145–150. [Google Scholar]
- Hussain, J.; Ullah, R.; Khan, A.; Mabood, F.; Shah, M.R.; Al-Harrasi, A.; Gilani, A.H. Antispasmodic and Ca++ antagonist potential of marrubiin, a labdane type diterpene from Phlomis bracteosa. J. Pharmacy Res. 2011, 4, 178–180. [Google Scholar]
- Zaabat, N.; Hay, A.E.; Michalet, S.; Darbour, N.; Bayet, C.; Skandrani, I.; Chekir-Ghedira, L.; Akkal, S.; Dijoux-Franca, M.G. Antioxidant and antigenotoxic properties of compounds isolated from Marrubium deserti de Noe. J. Food Chem. Toxicol. 2011, 49, 3328–3335. [Google Scholar] [CrossRef]
- Paula de Olivera, A.; Santin, J.R.; Lemos, M.; Klein, L.C.J.; Couto, A.G.; Bittencourt, C.M.S.; Cechinel, F.; Valdir, F.A. Gastroprotective activity of methanol extract and marrubiin obtained from leaves of Marrubium vulgare L. (Lamiaceae). J. Pharm. Pharmacol. 2011, 63, 1230–1237. [Google Scholar] [CrossRef]
- Piccoli, P.N.; Bottini, R. Accumulation of the labdane diterpene marrubiin in glandular trichome cells along the ontogeny of Marrubium vulgare plants. Plant Growth Regul. 2008, 56, 71–76. [Google Scholar] [CrossRef]
- Hellen, K.; Stulzer, H.K.; Tagliari, M.P.; Zampirolo, J.A.; Cechinel-Filho, V.; Schlemper, V. Antioedematogenic effect of marrubiin obtained from Marrubium vulgare. J. Ethnopharmacol. 2006, 108, 379–384. [Google Scholar] [CrossRef]
- Meyre-Silva, C.; Yunes, R.A.; Schlemper, V.; Campos-Buzzi, F.; Cechinel-Filho, V. Analgesic potential of marrubiin derivatives, a bioactive diterpene present in Marrubium vulgare (Lamiaceae). Farmaco 2005, 60, 321–326. [Google Scholar] [CrossRef]
- El Bardai, S.; Morel, N.; Wibo, M.; Fabre, N.; Llabres, G.; Lyoussi, B.; Quetin-Leclercq, J. The vasorelaxant activity of marrubenol and marrubiin from Marrubium vulgare. Planta Med. 2003, 69, 75–77. [Google Scholar] [CrossRef]
- De Jesus, R.A.P.; Cechinel-Filho, V.; Oliveira, A.E.; Schlemper, V. Analysis of the antinociceptive properties of marrubiin isolated from Marrubium vulgare. Phytomedicine 2000, 7, 111–115. [Google Scholar] [CrossRef]
- Knoess, W.; Zapp, J. Accumulation of furan labdane diterpenes in Marrubium vulgare and Leonurus cardiaca. Planta Med. 1998, 64, 357–361. [Google Scholar] [CrossRef]
- Rodrigues, C.A.; Savi, A.O.S.; Schlemper, V.; Reynaud, F.; Cechinel-Filho, V. An improved extraction of marrubiin from Marrubium vulgare. Chromatographia 1998, 47, 449–450. [Google Scholar] [CrossRef]
- De Souza, M.M.; De Jesus, R.A.P.; Cechinel-Filho, V.; Schlemper, V. Analgesic profile of hydroalcoholic extract obtained from Marrubium vulgare. Phytomedicine 1998, 5, 103–107. [Google Scholar] [CrossRef]
- Taboada, J.; Camino, M.; Gil, N.M.; Campos, E.; Guerrero, C. Antifeedant activity of marrubiin and reduced marrubiin. Rev. Lat. Am. Quim. 1995, 23, 120–125. [Google Scholar]
- Knoess, W. Furaniclabdane diterpenes in differentiated and undifferentiated cultures of Marrubium vulgare and Leonurus cardiac. Plant Physiol. Biochem. 1994, 32, 785–789. [Google Scholar]
- Mohamed, A.M.A. Constituents of the aerial parts of Marrubium vulgare L. J. Pharm. Sci. 1993, 9, 92–98. [Google Scholar]
- Rey, J.P.; Levesque, J.; Pousset, J.L. Extraction and high-performance liquid chromatographic methods for the γ-lactones parthenolide (Chrysanthemum parthenium Bernh.), marrubiin (Marrubium vulgare L.) and artemisinin (Artemisia annua L.). J. Chromatogr. A 1992, 605, 124–128. [Google Scholar] [CrossRef]
- Savona, G.; Piozzi, F.; Aranguez, L.M.; Rodriguez, B. Diterpenes from Marrubium sericeum, Marrubium supinum and Marrubium alysson. Phytomedicine 1979, 18, 859–860. [Google Scholar]
- Argyropoulou, C.; Karioti, A.; Skaltsa, H. Labdane Diterpenes from Marrubium thessalum. Phytochemistry 2009, 70, 635–640. [Google Scholar] [CrossRef]
- Argyropoulou, C.; Karioti, A.; Skaltsa, H. Minor labdane diterpenes from Marrubium thessalum. Chem. Biodivers. 2011, 8, 1880–1890. [Google Scholar] [CrossRef]
- Karioti, A.; Skopeliti, M.; Tsitsilonis, O.; Heilmann, J.; Skaltsa, H. Cytotoxicity and immunomodulating characteristics of labdane diterpenes from Marrubium cylleneum and Marrubium velutinum. Phytochemistry 2007, 68, 1587–1594. [Google Scholar] [CrossRef]
- Mnonopi, N.; Levendal, R.A.; Mzilikezi, N.; Frost, C.L. Marrubiin, a constituent of Leonotus leonurus, alleviates diabetic symptoms. Phytomedicine 2012, 19, 488–493. [Google Scholar] [CrossRef]
- Meyre-Silva, C.; Cechinel-Filho, V. A review of the chemical and pharmacological aspects of the genus Marrubium. Curr. Pharm. Design 2010, 16, 3503–3518. [Google Scholar] [CrossRef]
- Karioti, A.; Heilmann, J.; Skaltsa, H. Labdane diterpenes from Marrubium velutinum and Marrubium cylleneum. Phytochemistry. 2005, 66, 1060–1066. [Google Scholar] [CrossRef]
- Citoglu, G.S.; Aksit, F. Occurrence of marrubiin and ladanein in Marrubium trachyticumboiss. Biochem. Syst. Ecol. 2002, 30, 885–886. [Google Scholar] [CrossRef]
- Takeda, Y.; Yanagihara, K.; Masuda, T.; Otsuka, H.; Honda, G.; Takaishi, Y.; Sezik, E.; Yesilada, E. Labdane diterpenoids from Marrubium globosum ssp. Globosum. Chem. Pharmaceut. Bull. 2000, 48, 1234–1235. [Google Scholar] [CrossRef]
- Sagitdinova, G.V.; Makhmudov, M.K.; Tashkhozhaev, B.; Mal'tsev, I.I. Labdanoids of Marrubium anisodon. Khim.Prir.Soedin. 1996, 1, 54–58. [Google Scholar]
- Uzma, R.M.; Rashad, M.; Abdul, M.; Bakhat, A.; Muhammad, S.; Rasool, B.T. Spiraeamide, New sphingolipid from Spiraea brahuica. J. Asian. Nat. Prod. Res. 2012, 14, 601–606. [Google Scholar] [CrossRef]
- The data collected without correction from SciFinder. Available online: https://scifinder.cas.org (accessed on 17 May 2012).
- Lichtenthaler, H.K.; Rohmer, M.; Schwender, J. Two independent biochemical pathways for isopentenyl diphosphate and isoprenoid biosynthesis in higher plants. Physiol. Plant. 1997, 101, 643–652. [Google Scholar] [CrossRef]
- Rohmer, M. The discovery of a mevalonate-independent pathway for isoprenoid biosynthesis in bacteria, algae and higher plants. Nat. Prod. Rep. 1999, 16, 565–574. [Google Scholar] [CrossRef]
- Knoss, W.; Reuter, B.; Zapp, J. Biosynthesis of the labdane diterpene marrubiin in Marrubium vulgare via a non-mevalonate pathway. Biochem. J. 1997, 326, 449–454. [Google Scholar]
- Paseshnichenko, V.A. A new alternative non-mevalonate pathway for isoprenoid biosynthesis ineubacteria and plants. Biochemistry (Mosc.) 1998, 63, 139–148. [Google Scholar]
- Cunningham, F.X.; Lafond, T.P.; Gantt, E. Evidence of a role for LytB in the non-mevalonate pathway of isoprenoid biosynthesis. J. Bacteriol. 2000, 118, 5841–5848. [Google Scholar] [CrossRef]
- Hussein, A.A.; Meyer, M.J.J.; Rodriguez, B. Complete 1H and 13C NMR assignments of three labdane diterpenoids isolated from Leonotis ocymifolia and six other related compounds. Magn. Reson. Chem. 2003, 41, 147–151. [Google Scholar] [CrossRef]
- Bergeron, C.; Charbonneau, J.; Desriches, B.; Gosselin, A. Influence of supplemental lighting and irrigation on mineral composition growth and premarrubin content of horehound, Marrubium vulgare L. J. Herbs, Spices Med. Plants 1995, 3, 3–15. [Google Scholar] [CrossRef]
- Hon, P.M.; Wang, E.S.; Lam, S.K.M.; Choy, Y.M.; Lee, C.M.; Wong, H.N.C. Preleoheterin and leoheterin, two labdane diterpenes from Leonurus heterophyllus. Phytochemistry 1993, 33, 639–641. [Google Scholar] [CrossRef]
- Rustaiyan, A.; Mosslemin, K.M.H.; Zdero, C. Furanolabdanes and related compounds from Ballota aucheri. Phytochemistry 1992, 31, 344–346. [Google Scholar] [CrossRef]
- Henderson, M.S.; McCrindle, R. Premarrubiin. A diterpenoid from Marrubium vulgare. J. Chem. Soc. C 1969, 15, 2014–2015. [Google Scholar] [CrossRef]
- Tasdemir, D.; Wright, A.D.; Sticher, O.; Çalıs, I.; Linden, A. Detailed 1H- and 13C-NMR investigations of some diterpenes isolated from Leonurus persicus. J. Nat. Prod. 1995, 58, 1543–1554. [Google Scholar] [CrossRef]
- Tasdemir, D.; Sticher, O.; Çalıs, I.; Linden, A. Further Labdane diterpenoids isolated from Leonurus persicus. J. Nat. Prod. 1997, 60, 874–879. [Google Scholar] [CrossRef]
- Govindasamy, L.; Rajakannan, V.; Velmurugan, D.; Banumathi, S.; Vasanth, S. Structural studies on three plant diterpenoids from Leonotis nepetaefolia. Cryst. Res. Tech. 2002, 37, 896–909. [Google Scholar] [CrossRef]
- He, F.; Lindqvist, C.; Harding, W.W. Leonurenones A–C: Labdane diterpenes from Leonotis leonurus. Phytochemistry 2012, 83, 168–172. [Google Scholar] [CrossRef]
- Wu, H.; Li, J.; Fronczek, F.R.; Ferreira, D.; Burandt, C.L.; Setola, V.; Roth, B.L.; Zjawiony, J.K.L. Diterpenoids from Leonotis leonurus. Phytochemistry 2013, 91, 229–235. [Google Scholar] [CrossRef]
- Naidoo, D.; Maharaj, V.; Crouch, N.R.; Ngwane, A. New labdane-type diterpenoids from Leonotis leonurus support circumscription of Lamiaceae. Biochem. Syst. Ecol. 2011, 39, 216–219. [Google Scholar] [CrossRef]
- Ruzicka, L. The isoprene rule and the biogenesis of terpenic compounds. Experientia 1953, 9, 357–367. [Google Scholar] [CrossRef]
- Busby, M.C.; Day, V.W.; Day, R.O.; Wheeler, D.M.S.; Wheeler, M.M.; Day, C.S. The stereochemistry and conformation of marrubiin: An X-Ray Study. Proc. R. Ir. Acad. 1983, 83B, 21–31. [Google Scholar]
- Marrubiin-Compound Summary (CID 73401). Available online: http://pubchem.ncbi.nlm.nih.gov/summary/summary.cgi?cid=73401 (accessed on 17 May 2012).
- Krejci, I.; Zadina, R. Die Gallentreiben de wirkung von marrubiin und marrabinsäure. Planta Med. 1959, 7, 1–7. [Google Scholar] [CrossRef]
- Ojewole, J.A.O. Hypotensive effect of Leonotis leonurus. Amer. J. Hypertens. 2003, 16, 213–225. [Google Scholar]
- Khan, A.; Ullah, R.; Mustafa, M.R.; Hussain, J.; Murugan, D.D.; Hadi, A.H.B.A. Vasodilator effect of phlomis bracteosa constituents is mediated through dual endothelium-dependent and endothelium-independent pathways. Clin. Exp. Hypertension 2012, 34, 132–139. [Google Scholar] [CrossRef]
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Popoola, O.K.; Elbagory, A.M.; Ameer, F.; Hussein, A.A. Marrubiin. Molecules 2013, 18, 9049-9060. https://doi.org/10.3390/molecules18089049
Popoola OK, Elbagory AM, Ameer F, Hussein AA. Marrubiin. Molecules. 2013; 18(8):9049-9060. https://doi.org/10.3390/molecules18089049
Chicago/Turabian StylePopoola, Olugbenga K., Abdulrahman M. Elbagory, Farouk Ameer, and Ahmed A. Hussein. 2013. "Marrubiin" Molecules 18, no. 8: 9049-9060. https://doi.org/10.3390/molecules18089049
APA StylePopoola, O. K., Elbagory, A. M., Ameer, F., & Hussein, A. A. (2013). Marrubiin. Molecules, 18(8), 9049-9060. https://doi.org/10.3390/molecules18089049






