Enhancement of Epimedium Fried with Suet Oil Based on in Vivo Formation of Self-Assembled Flavonoid Compound Nanomicelles
Abstract
:1. Introduction
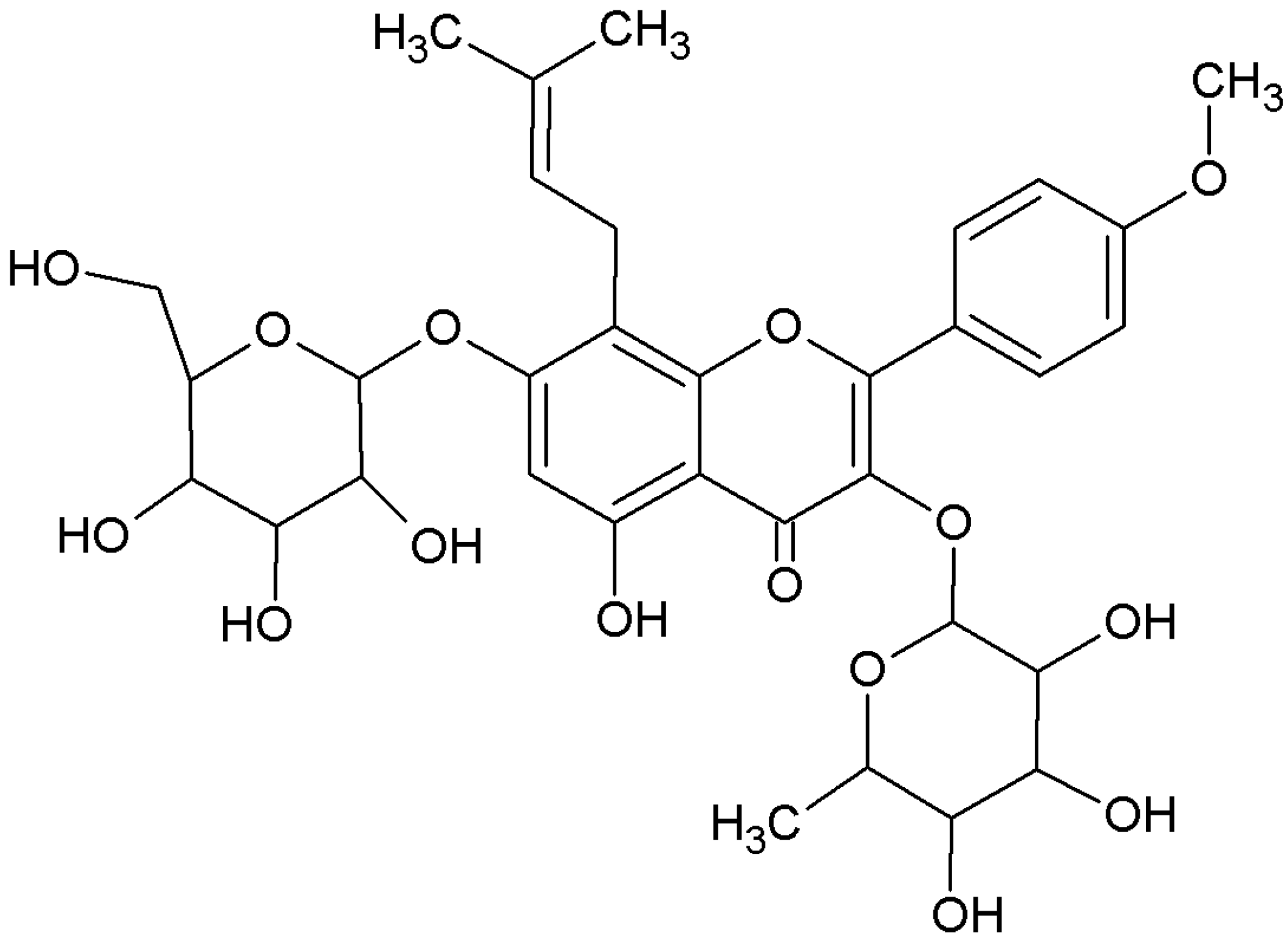
2. Results and Discussion
2.1. Characterization of the Self-Assembled Nanomicelles
2.1.1. Size, Size Distribution and Drug Encapsulation Efficiency
| Samples (20 μM) | Average particle size (nm) | Polydispersity | EE (%) |
|---|---|---|---|
| icariin + DOCi | 553.2 ± 4.06 | 0.851 ± 0.010 | 43.1 ± 1.76 |
| icariin + DOC + suet oili | 164.8 ± 0.98 *** | 0.123 ± 0.003 *** | 89.7 ± 2.23 *** |
2.1.2. Surface Morphology

2.2. Vectorial Transport of icariin + DOC and icariin + DOC + suet oil in Caco-2 Cell Monolayers

| Samples(20 μM) | PAB (cm/s) | PBA (cm/s) | Efflux ratio | ||||
|---|---|---|---|---|---|---|---|
| Mean 10−6 | S.D.10−7 | Mean 10−6 | S.D.10−7 | PBA/PAB | |||
| icariin + DOC | 0.62 ± 0.06 | 0.061 | 3.00 ± 0.27 | 0.265 | 4.84 | ||
| icariin + DOC + suet oil | 1.26 ± 0.03 ** | 0.035 | 5.91 ± 0.38 * | 0.345 | 4.69 | ||
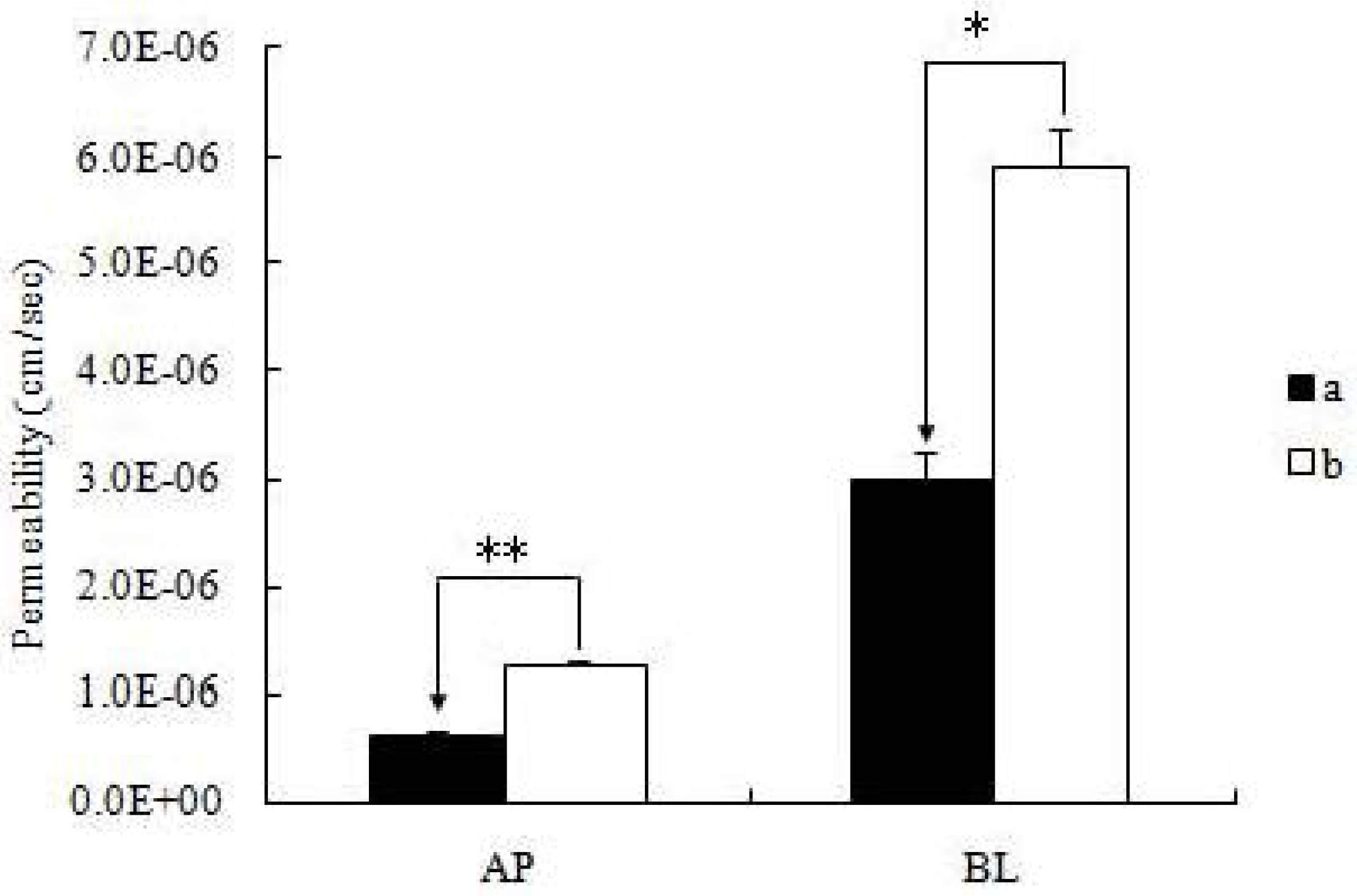
2.3. Cellular Accumulation of Icariin + DOC and Icariin + DOC + Suet Oil
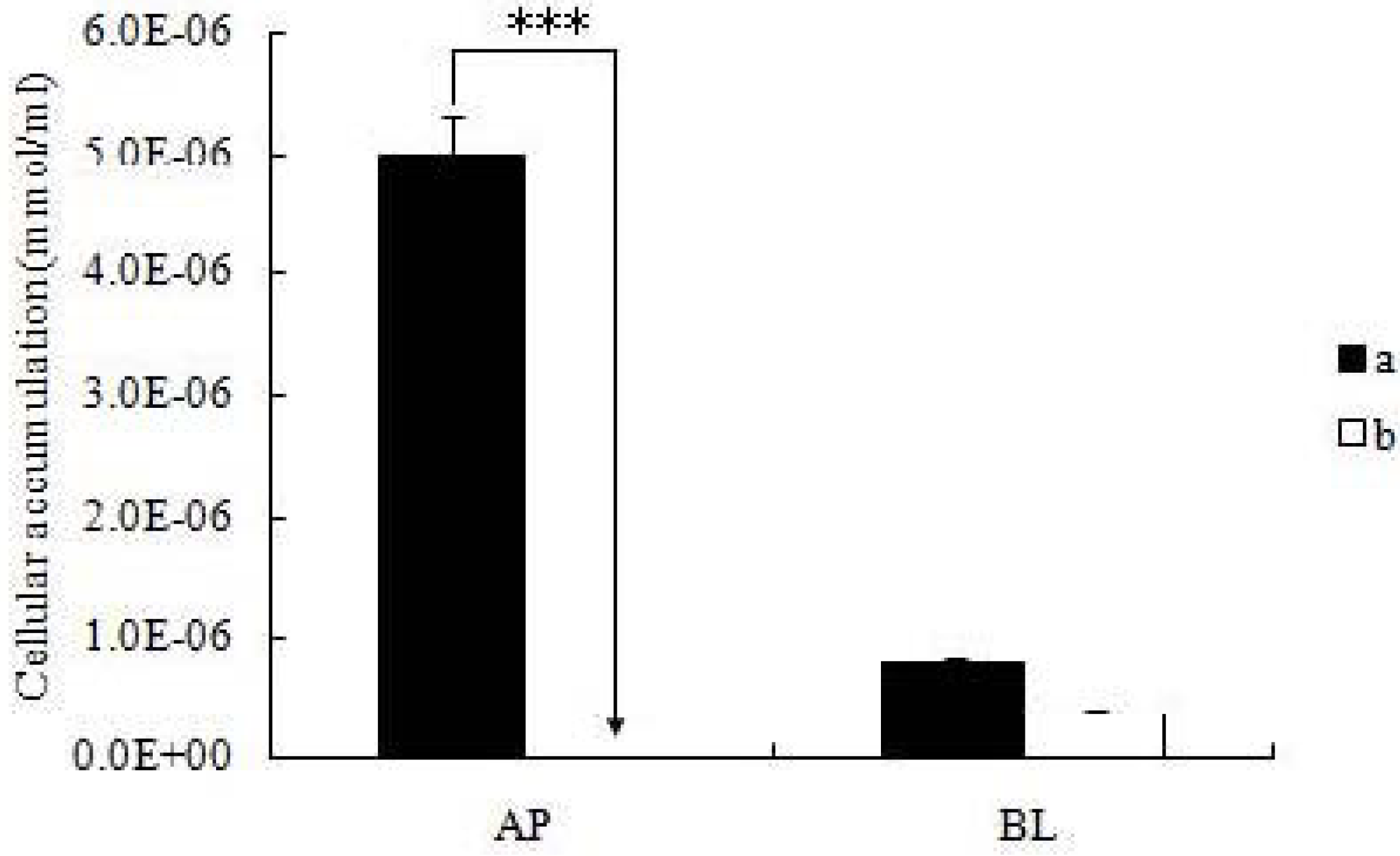
2.4. Absorption of Icariin + DOC and Icariin + DOC + Suet oil in Rat Intestine
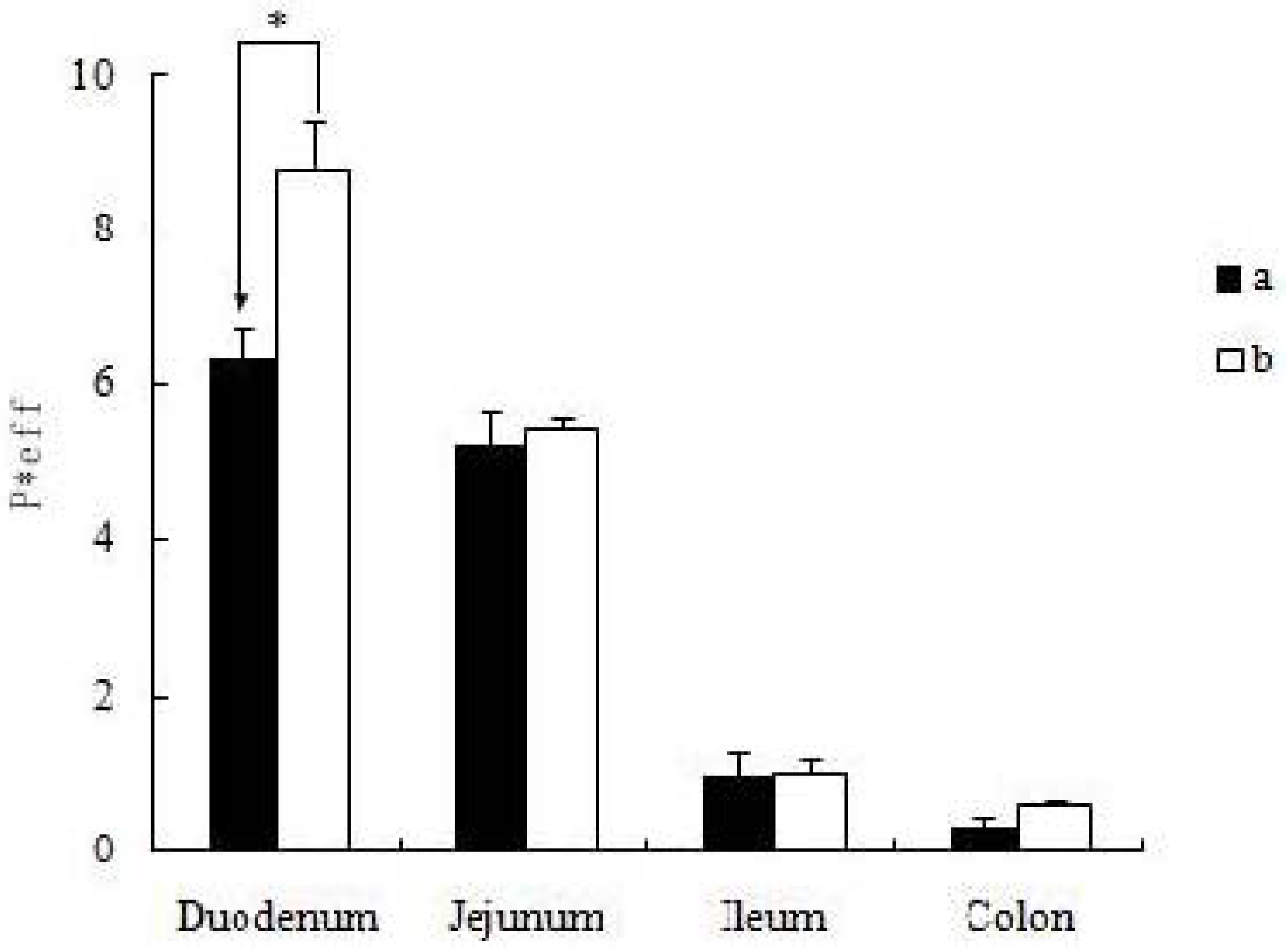
3. Experimental
3.1. Materials
3.2. Preparation of the Self-Assembled Nanomicelles
3.2.1. The Preparation of the icariin Self-Assembled Nanomicelles with Suet Oil
3.2.2. The Preparation of the Icariin Self-assembled Nanomicelles without Suet Oil
3.3. Characterization of the Self-Assembled Nanomicelles
3.3.1. Particle Size, Size Distribution and Surface Morphology
3.3.2. The Encapsulation Efficiency of Self-Assembled Nanomicelles
3.4. Cell Experiments
3.4.1. Cell Culture
3.4.2. Transport Experiments in the Caco-2 Cell Culture Model
3.4.3. Electrical Resistance
3.4.4. Cellular Accumulation Studies in the Cell Monolayers
3.5. Animals Experiments
3.5.1. Animals
3.5.2. Animal Surgery
3.5.3. Four Site Single-pass Rat Intestinal Perfusion Experiments
3.6. Analytical Methods
3.7. Data Analysis


3.8. Statistical Analysis
4. Conclusions
Acknowledgments
References
- Chen, Y.; Wang, J.Y.; Jia, X.B.; Tan, X.B.; Hu, M. Role of Intestinal Hydrolase in the Absorption of Prenylated Flavonoids Present in Yinyanghuo. Molecules 2011, 16, 1336–1348. [Google Scholar] [CrossRef]
- Wei, Y.J.; Li, P.; Fan, H.W.; Sun, E.; Wang, C.M.; Shu, L.; Liu, W.; Xue, X.L.; Qian, Q.; Jia, X.B. Metabolite Profiling of Four Major Flavonoids of Herba Epimdii in Zebrafish. Molecules 2012, 17, 420–432. [Google Scholar] [CrossRef]
- Fan, J.J.; Cao, L.G.; Wu, T.; Wang, D.X.; Jin, D.; Jiang, S.; Zhang, Z.Y.; Bi, L.; Pei, G.X. The Dose-Effect of Icariin on the Proliferation and Osteogenic Differentiation of Human Bone Mesenchymal Stem Cells. Molecules 2011, 16, 10123–10133. [Google Scholar] [CrossRef]
- Huang, X.; Zhu, D.Y.; Lou, Y.J. A novel anticancer agent, Icaritin, Induced cell growth inhibition, G1 arrest and mitochondrial transmembrane potential drop in human prostate carcinoma PC-3 cells. Eur. J. Pharmacol. 2007, 564, 26–36. [Google Scholar] [CrossRef]
- Ning, H.; Xin, Z.C.; Lin, GT.; Banie, L.; Lue, T.F.; Lin, C.S. Effects of icariin on phosphodiesterase-5 activity in vitro and cyclic guanosine monophosphate level in cavernous smooth muscle cells. Urology 2006, 68, 1350–1354. [Google Scholar] [CrossRef]
- Editorial Committee of Pharmacopoeia of Ministry of Health PR China, The Pharmacopeoia of People’s Republic of China; China Chemical Industry Press: Beijing, China, 2010; pp. 306–308.
- Chen, Y.; Zhao, Y.H.; Jia, X.B.; Hu, M. Intestinal Absorption Mechanisms of Prenylated Flavonoids Present in the Heat-Processed Epimedium koreanum Nakai (Yin Yanghuo). Pharm. Res. 2008, 25, 2190–2199. [Google Scholar] [CrossRef]
- Jin, Y.G.; Tong, L.; Ai, P.; Li, M.; Hou, X.P. Self-assembled drug delivery systems: 1. Properties and in vitro/in vivo behavior of acyelovir self-assembled nanoparticles(SAN). Int. J. Pharm. 2006, 309, 199–207. [Google Scholar] [CrossRef]
- Lin, J.B.; Dou, J.; Xu, J.L.; Haji, A.A. Chemical Composition, Antimicrobial and Antitumor Activities of the Essential Oils and Crude Extracts of Euphorbia macrorrhiza. Molecules 2012, 17, 5030–5039. [Google Scholar] [CrossRef]
- Chen, J.; Lin, H.; Hu, M. Metabolism of flavonoids via enteric recycling: Role of intestinal disposition. J. Pharmacol. Exp. Ther. 2003, 304, 1228–1235. [Google Scholar]
- Hu, M.; Chen, J.; Lin, H. Metabolism of flavonoids via enteric recycling: mechanistic studies of disposition of apigenin in the Caco-2 cell culture model. J. Pharmacol. Exp. Ther. 2003, 307, 314–321. [Google Scholar] [CrossRef]
- Hu, M.; Chen, J.; Zhu, Y.; Dantzig, A.H.; Stratford, R.E., Jr.; Kuhfeld, M.T. Mechanism and kinetics of transcellular transport of a new beta-lactam antibiotic loracarbef across an intestinal epithelial membrane model system (Caco-2). Pharm. Res. 1994, 11, 1405–1413. [Google Scholar] [CrossRef]
- Karamustafa, F. Transport of alendronate through human intestinal cell line, Caco-2. In Proceedings of the 33rd Annual Meeting & Exposition of the Controlled Release Society, Vienna, Austria, 22–26 July 2006; pp. 22–26.
- Roger, E.; Lagarce, F.; Garcion, E.; Benoit, J.P. Lipid nanocarriers improve paclitaxel transport throughout human intestinal epithelial cells by using vesicle-mediated transcytosis. J. Control. Release 2009, 140, 174–181. [Google Scholar] [CrossRef]
- Lev, B.; Valery, A. Effects of polyether-modified poly (acrylic acid) Microgels on doxorubicin transport in human intestinal epithelial Caco-2 cell. J. Control. Release 2003, 88, 11–22. [Google Scholar] [CrossRef]
- Lo, Y.L. Relationships between the hydrophilic–lipophilic balance values of pharmaceutical excipients and their multidrug resistance modulating effect in Caco-2 cells and rat intestines. J. Control. Release 2003, 90, 37–48. [Google Scholar] [CrossRef]
- Abuasal, B.; Sylvester, P.W.; Kaddoumi, A. Intestinal Absorption of -Tocotrienol Is Mediated by Niemann-Pick C1-Like 1: In Situ Rat Intestinal Perfusion Studies. Drug Metab. Dispos. 2010, 38, 939–945. [Google Scholar] [CrossRef]
- van Hasselt, P.M.; Janssens, G.E.P.J.; Rijcken, C.J.F.; van Nostrum, C.F. Influence of bile on the oral bioavailability of vitamin K-loaded polymeric micelles. J. Control. Release 2008, 132, 29–31. [Google Scholar] [CrossRef]
- Jiang, L.X.; Wang, K.; Deng, M.L.; Wang, Y.L.; Huang, J.B. Bile salt-induced vesicle-to-micelle transition in catanionic surfactant systems: Steric and electrostatic interactions. Langmuir 2008, 24, 4600–4606. [Google Scholar]
- Sample Availability: Samples of the compounds icariin and sodium deoxycholate are available from the authors.
© 2012 by the authors; licensee MDPI, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Cui, L.; Sun, E.; Zhang, Z.-H.; Tan, X.-B.; Wei, Y.-J.; Jin, X.; Jia, X.-B. Enhancement of Epimedium Fried with Suet Oil Based on in Vivo Formation of Self-Assembled Flavonoid Compound Nanomicelles. Molecules 2012, 17, 12984-12996. https://doi.org/10.3390/molecules171112984
Cui L, Sun E, Zhang Z-H, Tan X-B, Wei Y-J, Jin X, Jia X-B. Enhancement of Epimedium Fried with Suet Oil Based on in Vivo Formation of Self-Assembled Flavonoid Compound Nanomicelles. Molecules. 2012; 17(11):12984-12996. https://doi.org/10.3390/molecules171112984
Chicago/Turabian StyleCui, Li, E Sun, Zhen-Hai Zhang, Xiao-Bin Tan, Ying-Jie Wei, Xin Jin, and Xiao-Bin Jia. 2012. "Enhancement of Epimedium Fried with Suet Oil Based on in Vivo Formation of Self-Assembled Flavonoid Compound Nanomicelles" Molecules 17, no. 11: 12984-12996. https://doi.org/10.3390/molecules171112984
APA StyleCui, L., Sun, E., Zhang, Z.-H., Tan, X.-B., Wei, Y.-J., Jin, X., & Jia, X.-B. (2012). Enhancement of Epimedium Fried with Suet Oil Based on in Vivo Formation of Self-Assembled Flavonoid Compound Nanomicelles. Molecules, 17(11), 12984-12996. https://doi.org/10.3390/molecules171112984





