Design and Applications of Biodegradable Polyester Tissue Scaffolds Based on Endogenous Monomers Found in Human Metabolism
Abstract
:Introduction
| Material | Modulus (MPa) | Ult. Stress (MPa) | Ult. Strain (%) | Ref. |
|---|---|---|---|---|
| Bovine elastin | 1.1 | 2 | - | 4 |
| Collagen fibers | 100 | - | 50 | 5 |
| Knee articular cartilage | 2.1-11.8 | 6,7 | ||
| Smooth muscle (relaxed) | 0.006 | - | 300 | 5 |
| Smooth muscle (contracted) | 0.01 | - | 300 | 5 |
| Human bladder | 0.25 | 0.27 | 0.69 | 8 |
| Porcine bladder | 0.26 | 0.32 | 1.66 | 8 |
| Porcine aortic heart valve | 6.4 – 44.7 | 1.4–8.3 | 48.7–134.8 | 9 |
| PGAa | 6,900 | 70 | < 3 | 2,82 |
| PLLAb | 1,200–2,700 | 28 - 50 | 6 | 2,82 |
| PDLLAc | 1,900–2,400 | 29 - 35 | 6 | 2,82 |
| PCLd | 0.21–0.34 | 20.7 | 300–500 | 2 |
| PTMCe | 6.3–6.8 | 12 - 24 | 820–831 | 90 |
| PLGAf | 1.4–2.8 | 41.4–55.2 | 3–10 | 2 |
| PLCLg | 0.192–68.573 | 0.57–8.55 | 175–854.4 | 83,84,85 |
| PLTMCh | 4–1,900 | 1 - 53 | 4–830 | 88,89,92 |
| PGSi | 0.282 | > 0.5 | > 267 | 34,93,94 |
| PGSAj | 0.048 - 1.375 | 0.054 - 0.498 | 47.4–170 | 29,95,96 |
| PPSk | 0.37 - 378.0 | 0.57 - 17.64 | 10.90–205.2 | 97,98 |
| APSl | 2.45 - 4.24 | 1.33 - 1.69 | 64–92 | 99 |
| PDCm | 1.60–13.98 | 2.93–11.15 | 117–502 | 101,108 |
| PGlSun | - | - | - | 118 |
| PTKo | 0.1–657.4 | 0.2–30.8 | 22–583 | 135 |
| PPFp | 0.9–4,500 | .05–120 | 5 -20 | 138,139,140,141,142 |
Biological Role of Common Polyester Monomers
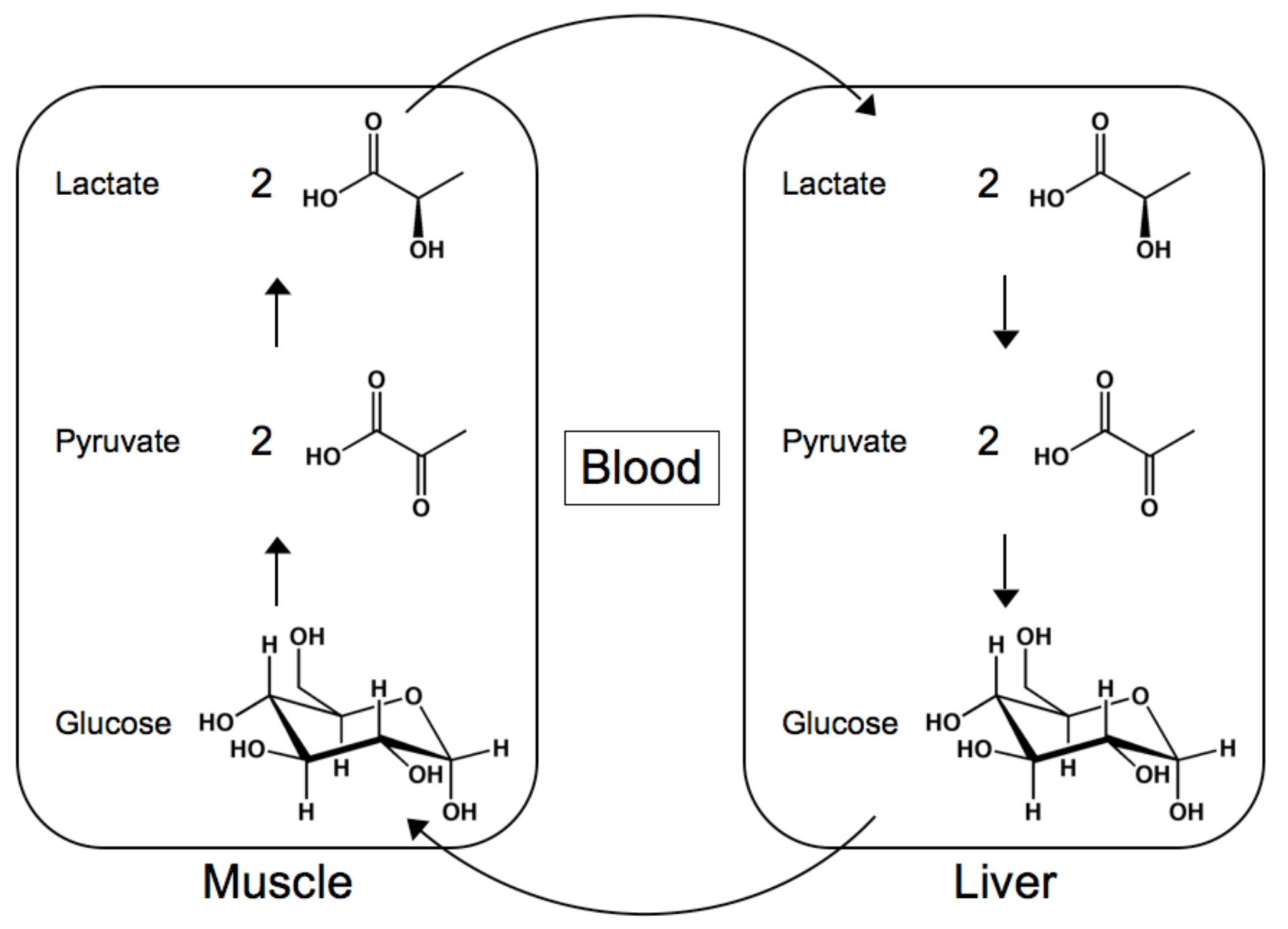
Lactic Acid
Glycerol
Sebacic Acid
Sugar Alcohols
Citric, Succinic, and α-Ketoglutaric Acids
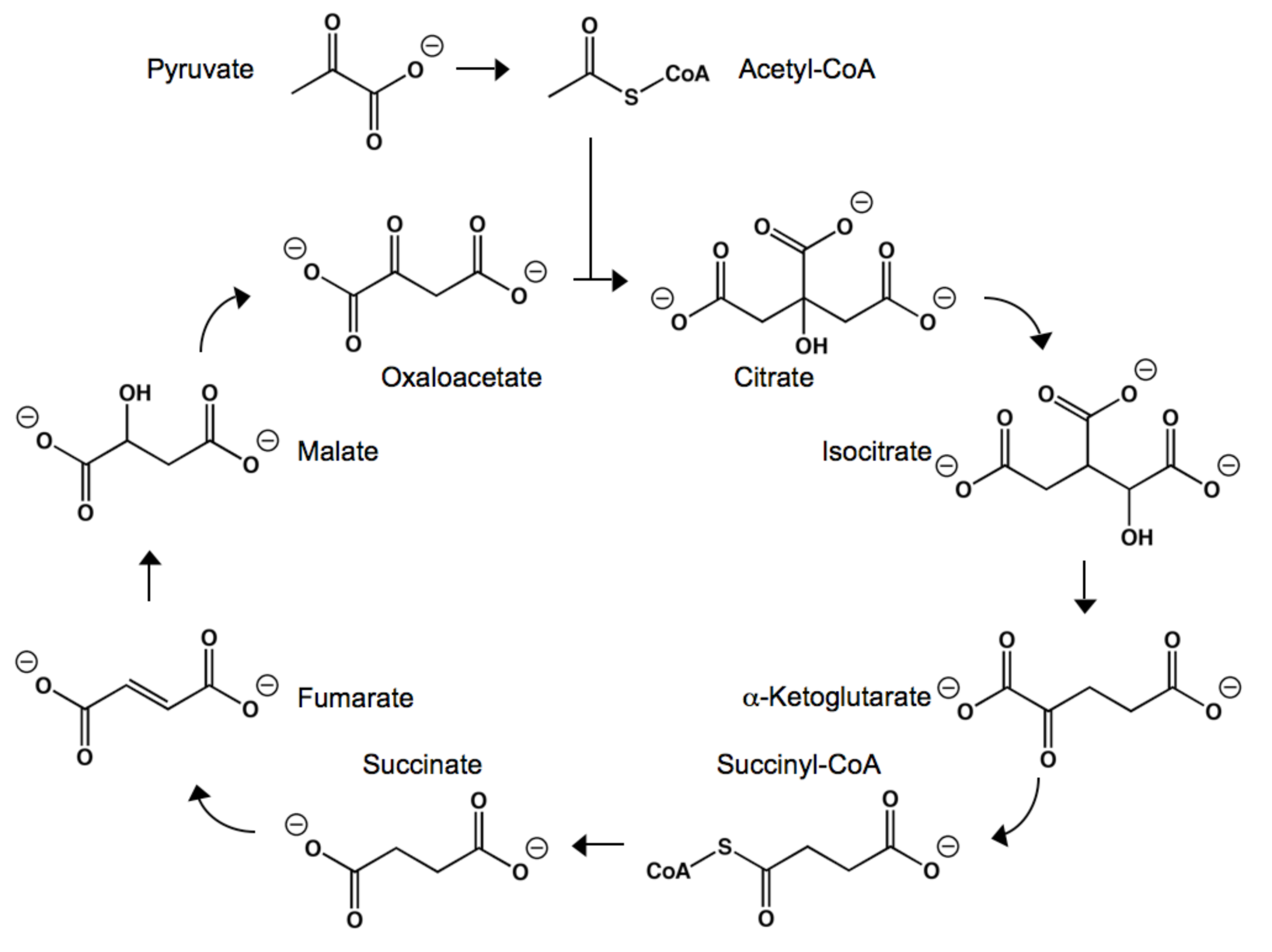
Polyesters as Tissue Scaffolds
Poly(d,l-lactide-co-ε-caprolactone)
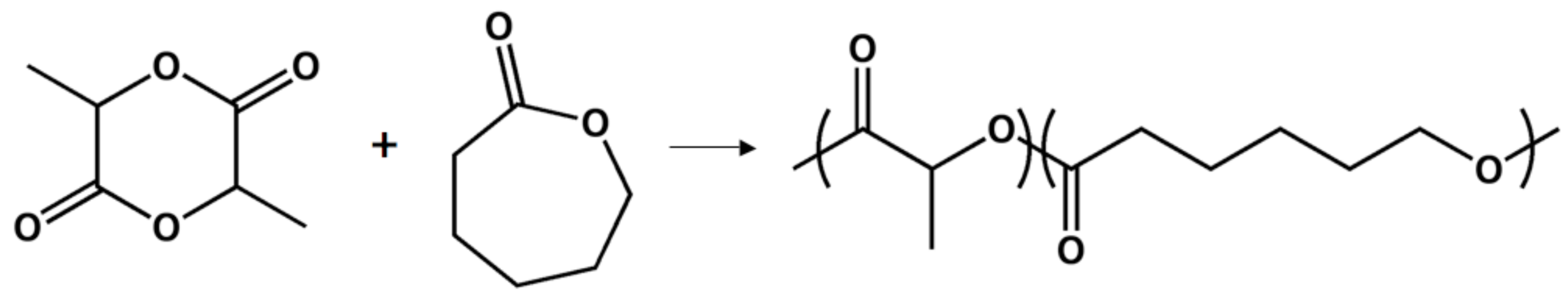
Poly(d,l-lactide-co-trimethylene carbonate)
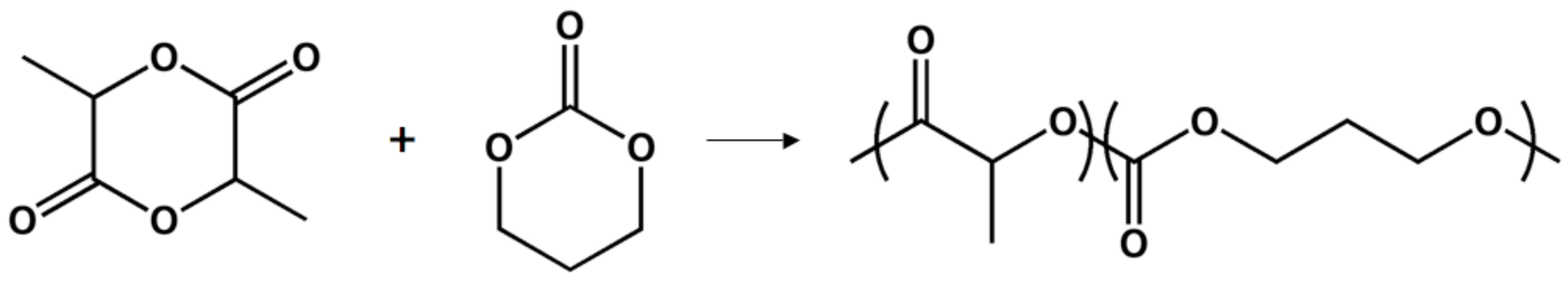
Poly(glycerol sebacate)
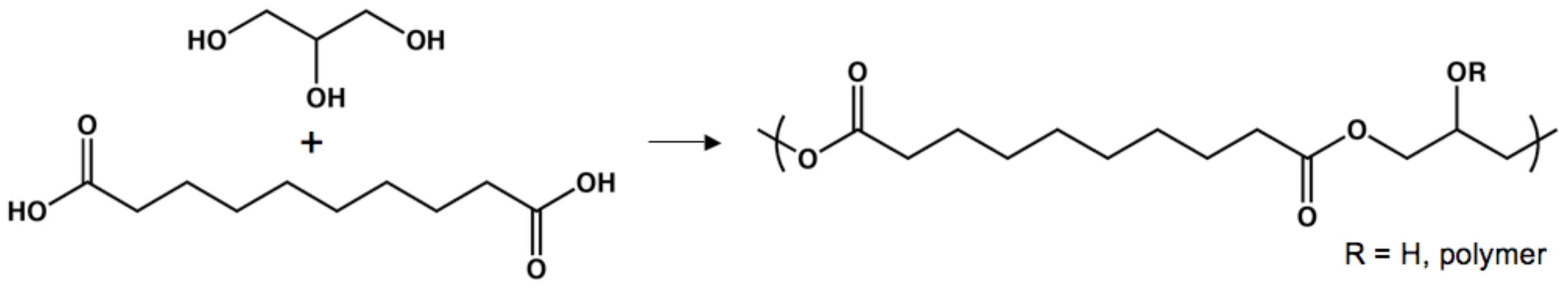
Poly(glycerol sebacate acrylate)
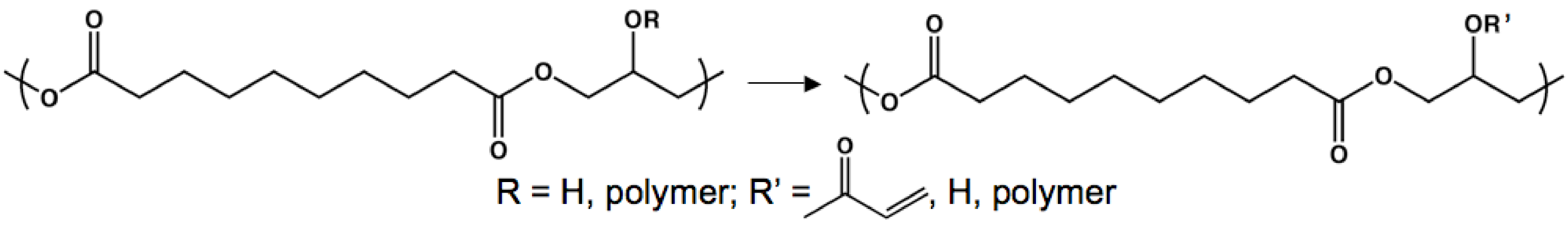
Poly(polyol sebacate)
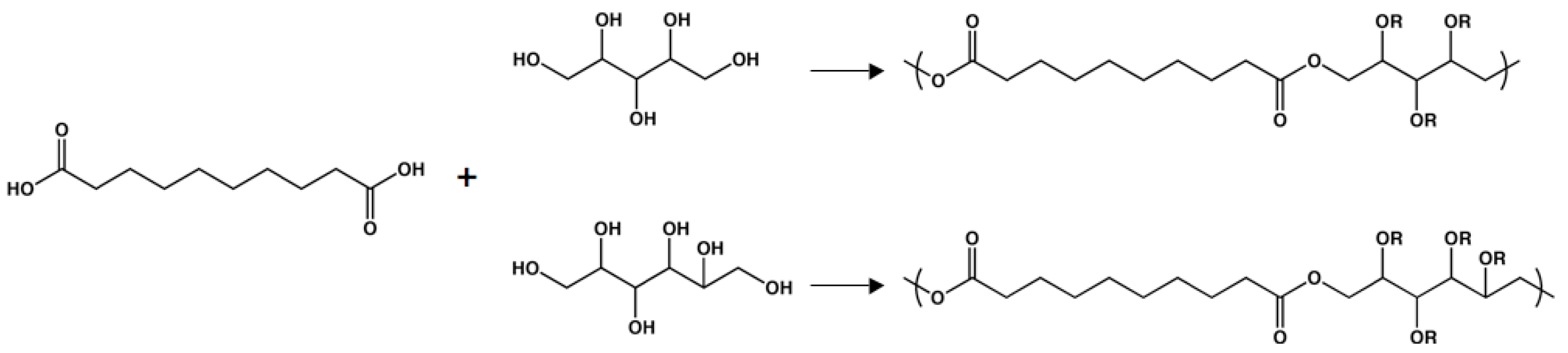
Poly(amino alcohol sebacate)
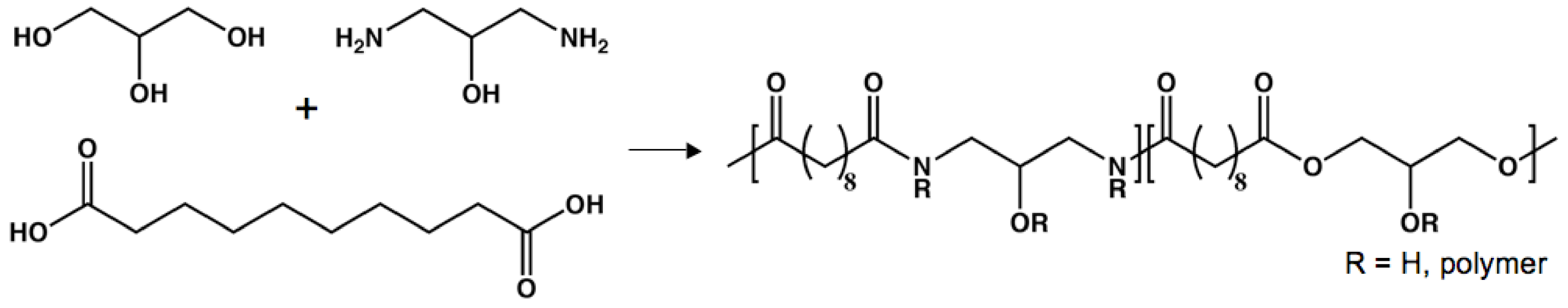
Poly(diol-co-citrate)
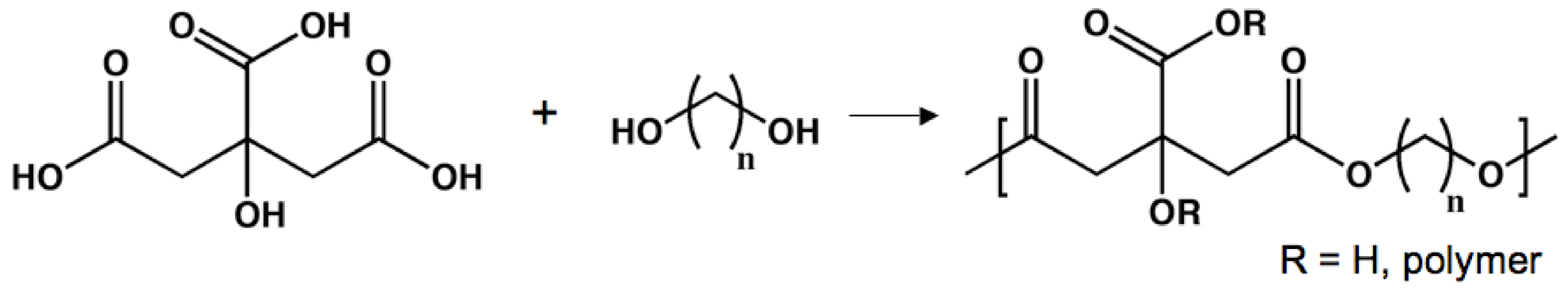
Dendritic Poly(glycerol succinate)

Poly[tetra(ethylene glycol) α-ketoglutarate]
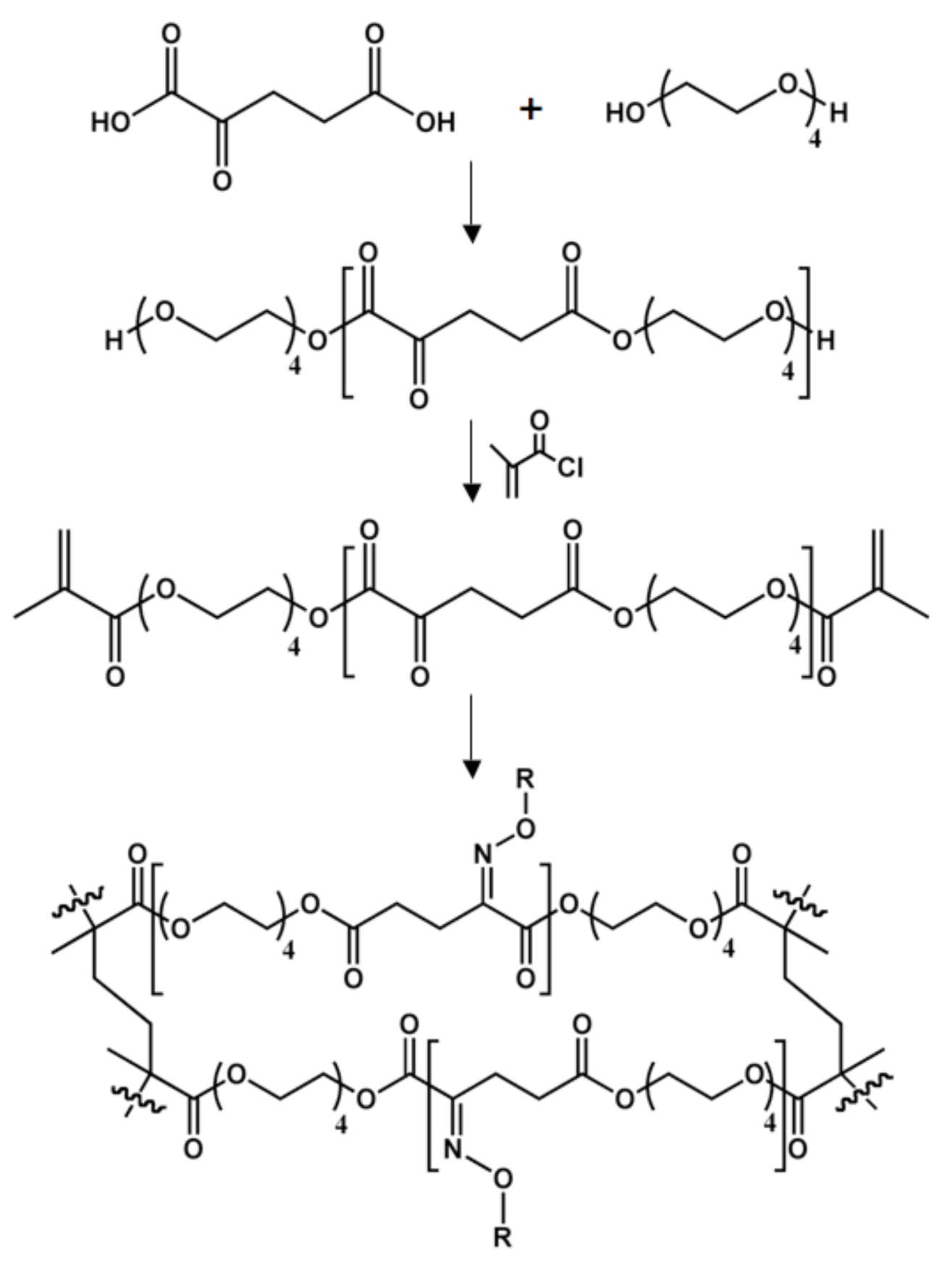
Poly(triol α-ketoglutarate)
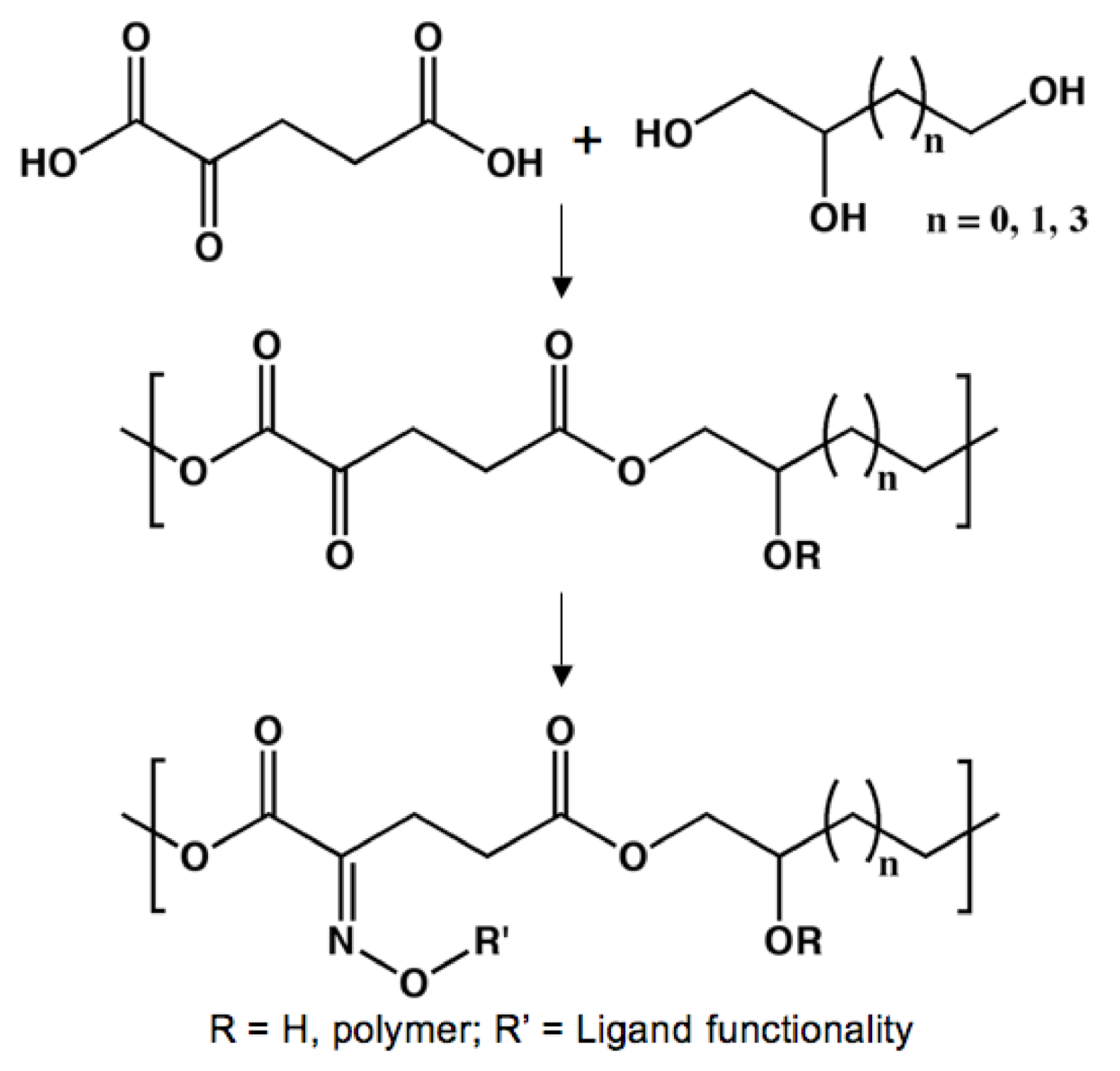
Poly(propylene fumarate)
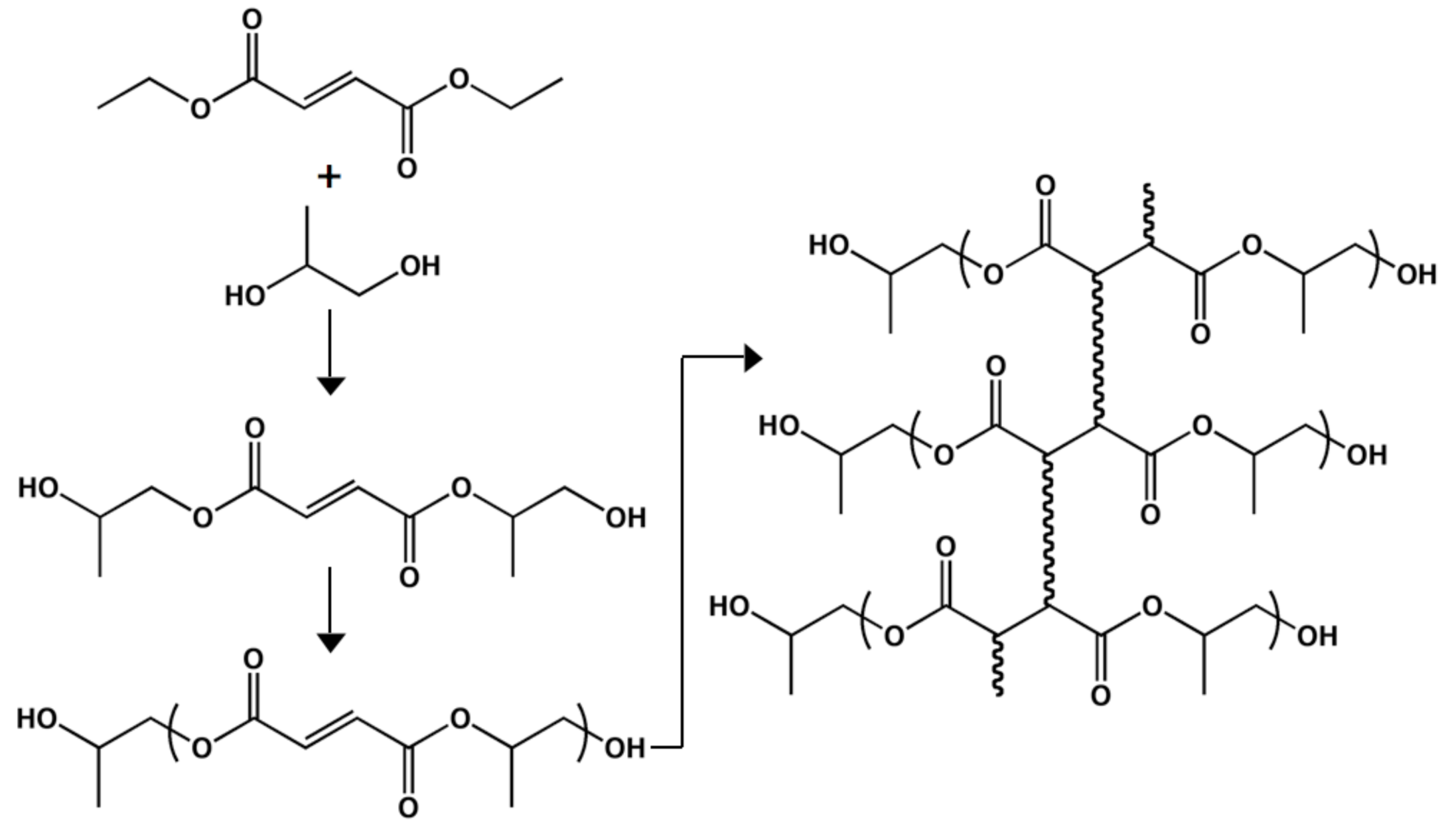
Conclusions
Supplementary Files
Supplementary File 1Acknowledgements
References and Notes
- Langer, R.; Vacanti, J.P. Tissue engineering. Science 1993, 260, 920–926. [Google Scholar] [CrossRef] [PubMed]
- Yang, S.; Leong, K.F.; Du, Z.; Chua, C.K. The design of scaffolds for use in tissue engineering. Part I. Traditional factors. Injury-Int. J. Care Injured 2008, 39, S77–S87. [Google Scholar] [CrossRef] [PubMed]
- Stoop, R. Smart biomaterials for tissue engineering of cartilage. Tissue Eng. 2001, 7, 679–689. [Google Scholar] [CrossRef] [PubMed]
- Gosline, J.; Lillie, M.; Carrington, E.; Guerette, P.; Ortlepp, C.; Savage, K. Elastic proteins: Biological roles and mechanical properties. Phil. Trans. R. Soc. Lond. B 2002, 357, 121–132. [Google Scholar] [CrossRef] [PubMed]
- Chandran, K.B. Cardiovascular Biomechanics; Chandran, K.B., Ed.; New York University Press: New York, NY, USA, 1992. [Google Scholar]
- Shepherd, D.E.T.; Seedhom, B.B. The ‘instantaneous’ compressive modulus of human articular cartilage in joints of the lower limb. Rheumatology 1999, 38, 124–132. [Google Scholar] [CrossRef] [PubMed]
- Thambyah, A.; Nather, A.; Goh, J. Mechanical properties of articular cartilage covered by the meniscus. Osteoarthritis Cartilage 2006, 14, 580–588. [Google Scholar] [CrossRef] [PubMed]
- Dahms, S.E.; Piechota, H.J.; Dahiya, R.; Lue, T.F.; Tanagho, E.A. Composition and biomechanical properties of the bladder acellular matrix graft: Comparative analysis in rat, pig, and human. Br. J. Urol. 1998, 82, 411–419. [Google Scholar] [CrossRef] [PubMed]
- Sung, H.W.; Chang, Y.; Chiu, C.T.; Chen, C.N.; Liang, H.C. Mechanical properties of a porcine aortic valve fixed with a naturally occurring crosslinking agent. Biomaterials 1999, 20, 1759–1772. [Google Scholar] [CrossRef]
- Webb, A.R.; Yang, J.; Ameer, G.A. Biodegradable polyester elastomers in tissue engineering. Expert Opin. Biol. Ther. 2004, 4, 801–812. [Google Scholar] [CrossRef] [PubMed]
- Amsden, B. Curable, biodegradable elastomers: Emerging biomaterials for drug delivery and tissue engineering. Soft Matter 2007, 3, 1335–1348. [Google Scholar] [CrossRef]
- Gupta, B.S.; Kasyanov, V.A. Biomechanics of human common carotid artery and design of novel hybrid textile compliant vascular grafts. J. Biomed. Mater. Res. 1997, 34, 341–349. [Google Scholar] [CrossRef]
- Balguid, A.; Rubbens, M.P.; Mol, A.; Bank, R.A.; Bogers, A.J.J.C.; van Kats, J.P.; de Mol, B.A.J.M.; Baaijens, F.P.T.; Bouten, C.V.C. The role of collagen cross-links in biomechanical behavior of human aortic heart valve leaflets-relevance for tissue engineering. Tissue Eng. 2007, 13, 1501–1511. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.M.; Boughner, D.R. Mechanical properties of human pericardium. Differences in viscoelastic response when compared to canine pericardium. Circ. Res. 1985, 57, 475–481. [Google Scholar] [CrossRef] [PubMed]
- Monson, K.L.; Goldsmith, W.; Barbaro, N.M.; Manley, G.T. Axial mechanical properties of fresh human cerebral blood vessels. J. Biomech. Eng. 2003, 125, 288–294. [Google Scholar] [CrossRef] [PubMed]
- Waldman, S.D.; Spiteri, C.G.; Grynpas, M.D.; Pilliar, R.M.; Kandel, R.A. Long-term intermittent compressive stimulation improves the composition and mechanical properties of tissue-engineered cartilage. Tissue Eng. 2004, 10, 1323–1331. [Google Scholar] [CrossRef] [PubMed]
- Stegemann, J.P.; Nerem, R.M. Phenotype modulation in vascular tissue engineering using biochemical and mechanical stimulation. Ann. Biomed. Eng. 2003, 31, 391–402. [Google Scholar] [CrossRef] [PubMed]
- Niklason, L.E.; Gao, J.; Abbott, W.M.; Hirschi, K.K.; Houser, S.; Marini, R.; Langer, R. Functional arteries grown in vitro. Science 1999, 284, 489–493. [Google Scholar] [CrossRef] [PubMed]
- Seliktar, D.; Nerem, R.M.; Galis, Z.S. Mechanical strain-stimulated remodeling of tissue-engineered blood Bessel constructs. Tissue Eng. 2003, 9, 657–666. [Google Scholar] [CrossRef] [PubMed]
- Kim, B.S.; Mooney, D.J. Scaffolds for engineering smooth muscle under cyclic mechanical strain conditions. J. Biomech. Eng. 2000, 122, 210–215. [Google Scholar] [CrossRef] [PubMed]
- Sipos, L.; Zsuga, M.; Deák, G. Synthesis of poly(l-lactide)-block-polyisobutylene-block-poly(l-lactide), a new biodegradable thermoplastic elastomer. Macromol. Rapid Commun. 1995, 16, 935–940. [Google Scholar] [CrossRef]
- Zhang, Z.; Grijpma, D.W.; Feijen, J. Triblock copolymers based on 1,3-trimethylene carbonate and lactide as biodegradable thermoplastic elastomers. Macromol. Chem. Phys. 2004, 205, 867–875. [Google Scholar] [CrossRef]
- Jeong, S.I.; Kim, B.S.; Kang, S.W.; Kwon, J.H.; Lee, Y.M.; Kim, S.H.; Kim, Y.H. In vivo biocompatibility and degradation behavior of elastic poly(l-lactide-co-ε-caprolactone) scaffolds. Biomaterials 2004, 25, 5939–5946. [Google Scholar] [CrossRef] [PubMed]
- Hiki, S.; Miyamoto, M.; Kimura, Y. Synthesis and characterization of hydroxy-terminated [RS]-poly(3-hydroxybutyrate) and its utilization to block copolymerization with l-lactide to obtain a biodegradable thermoplastic elastomer. Polymer 2000, 41, 7369–7379. [Google Scholar] [CrossRef]
- Odelius, K.; Plikk, P.; Albertsson, A.C. Elastomeric hydrolysable porous scaffolds: Copolymers of aliphatic polyesters and a polyether-ester. Biomacromolecules 2005, 6, 2718–2725. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.H.; Sheares, V.V. Amorphous unsaturated aliphatic polyesters derived from dicarboxylic monomers synthesized by Diels-Alder chemistry. Macromolecules 2007, 40, 4848–4853. [Google Scholar] [CrossRef]
- Amsden, B.G.; Tse, M.Y.; Turner, N.D.; Knight, D.K.; Pang, S.C. In vivo degradation behavior of photo-cross-linked star-poly(ε-caprolactone-co-d,l-lactide) elastomers. Biomacromolecules 2006, 7, 365–372. [Google Scholar] [CrossRef] [PubMed]
- Borgaonkar, P.; Sharma, S.; Chen, M.; Bhowmick, S.; Schmidt, D.F. A flexible approach to the preparation of polymer scaffolds for tissue engineering. Macromol. Biosci. 2007, 7, 201–207. [Google Scholar] [CrossRef] [PubMed]
- Gerecht, S.; Townsend, S.A.; Pressler, H.; Zhu, H.; Nijst, C.L.E.; Bruggeman, J.P.; Nichol, J.W.; Langer, R. A porous photocurable elastomer for cell encapsulation and culture. Biomaterials 2007, 28, 4826–4835. [Google Scholar] [CrossRef] [PubMed]
- Muroya, T.; Yamamoto, K.; Aoyagi, T. Degradation of cross-linked aliphatic polyester composed of poly(ε-caprolactone-co-d,l-lactide) depending on the thermal properties. Polym. Degrad. Stabil. 2009, 94, 285–290. [Google Scholar] [CrossRef]
- Pitt, C.G.; Gratzl, M.M.; Kimmel, G.L.; Surles, J.; Schindler, A. Aliphatic polyesters II. The degradation of poly(d,l-lactide), poly(ε-caprolactone), and their copolymers in vivo. Biomaterials 1981, 2, 215–220. [Google Scholar] [CrossRef]
- Wanamaker, C.L.; Tolman, W.B.; Hillmyer, M.A. Hydrolytic degradation behavior of a renewable thermoplastic elastomer. Biomacromolecules 2009, 10, 443–448. [Google Scholar] [CrossRef] [PubMed]
- Stoery, R.F.; Hickey, T.P. Degradable polyurethane networks based on d,l-lactide, glycolide, ε-caprolactone, and trimethylene carbonate homopolyesters and copolyester triols. Polymer 1994, 35, 830–838. [Google Scholar] [CrossRef]
- Wang, Y.; Kim, Y.M.; Langer, R. In vivo degradation characteristics of poly(glycerol sebacate). J. Biomed. Mater. Res. Part A 2003, 66, 192–197. [Google Scholar] [CrossRef] [PubMed]
- Richter, E.A.; Ruderman, N.B.; Gavras, H.; Belur, E.R.; Galbo, H. Muscle glycogenolysis during exercise: Dual control by epinephrine and contractions. Am. J. Physiol. Endocrinol. Metab. 1982, 242, E25–E32. [Google Scholar] [CrossRef] [PubMed]
- Chasiotis, D.; Sahlin, K.; Hultman, E. Regulation of glycogenolysis in human muscle at rest and during exercise. J. Appl. Physiol. 1982, 53, 708–715. [Google Scholar] [CrossRef] [PubMed]
- Febbraio, M.A.; Lamber, D.L.; Starkie, R.L.; Proietto, J.; Hargreaves, M. Effect of epinephrine on muscle glycogenolysis during exercise in trained men. J. Appl. Physiol. 1998, 84, 465–470. [Google Scholar] [CrossRef] [PubMed]
- Robergs, R.A.; Pearson, D.R.; Costill, D.L.; Fink, W.J.; Pascoe, D.D.; Benedict, M.A.; Lambert, C.P.; Zachweija, J.J. Muscle glycogenolysis during differing intensities of weight-resistance exercise. J. Appl. Physiol. 1991, 70, 1700–1706. [Google Scholar] [CrossRef] [PubMed]
- Gaitanos, G.C.; Williams, C.; Boobis, L.H.; Brooks, S. Human muscle metabolism during intermittent maximal exercise. J. Appl. Physiol. 1993, 75, 712–719. [Google Scholar] [CrossRef] [PubMed]
- Brooks, G.A.; Brauner, K.E.; Cassens, R.G. Glycogen synthesis and metabolism of lactic acid after exercise. Am. J. Physiol. 1973, 224, 1162–1166. [Google Scholar] [CrossRef] [PubMed]
- Brooks, G.A. The lactate shuttle during exercise and recovery. Med. Sci. Sports Exerc. 1986, 18, 360–368. [Google Scholar] [CrossRef] [PubMed]
- Kusaka, M.; Ui, M. Activation of the Cori cycle by epinephrine. Am. J. Physiol. 1977, 232, E145–E155. [Google Scholar] [CrossRef] [PubMed]
- Brooks, G.A. Current concepts in lactate exchange. Med. Sci. Sports Exerc. 1991, 23, 895–906. [Google Scholar] [CrossRef] [PubMed]
- Garcia, C.K.; Goldstein, J.L.; Pathak, R.K.; Anderson, R.G.; Brown, M.S. Molecular characterization of a membrane transporter for lactate, pyruvate, and other monocarboxylates: Implications for the Cori cycle. Cell 1994, 76, 865–873. [Google Scholar] [CrossRef]
- Waterhouse, C.; Keilson, J. Cori cycle activity in man. J. Clin. Invest. 1969, 48, 2359–2366. [Google Scholar] [CrossRef] [PubMed]
- May, G.L.; Wright, L.C.; Homes, K.T.; Williams, P.G.; Smith, I.C.; Wright, P.E.; Fox, R.M.; Mountford, C.E. Assignment of methylene proton resonances in NMR spectra of embryonic and transformed cells to plasma membrane triglyceride. J. Biol. Chem. 1986, 261, 3048–3053. [Google Scholar] [PubMed]
- Mattson, F.H.; Volpenhein, R.A. The digestion and absorption of triglycerides. J. Biol. Chem. 1964, 239, 2772–2777. [Google Scholar] [PubMed]
- Gavino, V.C.; Gavino, G.R. Adipose hormone-sensitive lipase preferentially releases polyunsaturated fatty acids from triglycerides. Lipids 1992, 27, 950–954. [Google Scholar] [CrossRef] [PubMed]
- Mattson, F.H.; Volpenhein, R.A. Rearrangement of glyceride fatty acids during digestions and absorption. J. Biol. Chem. 1962, 237, 53–55. [Google Scholar] [PubMed]
- Hauser, H.; Pascher, I.; Sundell, S. Preferred conformation and dynamics of the glycerol backbone in phospholipids. An NMR and x-ray single-crystal analysis. Biochemistry 1988, 27, 9166–9174. [Google Scholar] [CrossRef] [PubMed]
- Brezesinski, G.; Dietrich, A.; Struth, B.; Böhm, C.; Bouwman, W.G.; Kjaer, K.; Möhwald, H. Influence of ether linkages on the structure of double-chain phospholipid monolayers. Chem. Phys. Lipids 1995, 76, 145–157. [Google Scholar] [CrossRef]
- Brown, M.F.; Seelig, J.; Häberlen, U. Structural dynamics in phospholipid bilayers from deuterium spin-lattice relaxation time measurements. J. Chem. Phys. 1979, 70, 5045–5053. [Google Scholar] [CrossRef]
- Lin, E.C.C. Glycerol utilization and its regulation in mammals. Ann. Rev. Biochem. 1977, 46, 765–795. [Google Scholar] [CrossRef] [PubMed]
- Phillips, J.W.; Jones, M.E.; Berry, M.N. Implications of the simultaneous occurrence of hepatic glycolysis from glucose and gluconeogenesis from glycerol. Eur. J. Biochem. 2002, 269, 792–797. [Google Scholar] [CrossRef] [PubMed]
- Baba, H.; Zhang, X.J.; Wolfe, R.R. Glycerol gluconeogenesis in fasting humans. Nutrition 1995, 11, 149–153. [Google Scholar] [PubMed]
- Rognstad, R. Estimation of gluconeogenesis and glycogenolysis in vivo using tritiated water. Biochem. J. 1991, 279, 911. [Google Scholar] [CrossRef] [PubMed]
- Peroni, O.; Large, V.; Beylot, M. Measuring gluconeogenesis with [2–13C]glycerol and mass isotopomer distribution analysis of glucose. Am. J. Physiol. Endocrinol. Metab. 1995, 269, E516–E523. [Google Scholar] [CrossRef] [PubMed]
- Liu, G.; Hinch, B.; Beavis, A.D. Mechanisms for the transport of α,ω-dicarboxylates through the mitochondrial inner membrane. J. Biol. Chem. 1996, 271, 25338–25344. [Google Scholar] [CrossRef] [PubMed]
- Grego, A.V.; Mingrone, G. Dicarboxylic acids, an alternate fuel substrate in parenteral nutrition: an update. Clin. Nutr. 1995, 14, 143–148. [Google Scholar] [CrossRef]
- Mortensen, P.B.; Gregersen, N. The biological origin of ketotic dicarboxylic aciduria. In vivo and in vitro investigations of the omega-oxidation of C6-C16-monocarboxylic acids in unstarved, starved, and diabetic rats. Biochim. Biophys. Acta 1981, 666, 394–404. [Google Scholar] [CrossRef]
- Mortensen, P.B. C6-C10-dicarboxylic aciduria in starved, fat-fed, and diabetic rats receiving decanoic acid or medium-chain triacylglycerol. An in vivo measure of the rate of β-oxidation of fatty acids. Biochim. Biophys. Acta 1981, 664, 349–355. [Google Scholar] [CrossRef]
- Lynch, H.; Milgrom, P. Xylitol and dental caries: an overview for clinicians. J. Calif. Dent. Assoc. 2003, 31, 205–209. [Google Scholar] [PubMed]
- Birkhed, D. Cariologic aspects of xylitol and its use in chewing gum: a review. Acta Odontol. Scand. 1994, 52, 116–127. [Google Scholar] [CrossRef] [PubMed]
- Birkhed, D.; Kalfas, S.; Svensäter, G.; Edwardsson, S. Microbiological aspects of some caloric sugar substitutes. Int. Dent. J. 1985, 35, 9–17. [Google Scholar] [PubMed]
- Edgar, W.M. Sugar substitutes, chewing gum, and dental caries—A review. Br. Dent. J. 1998, 184, 29–32. [Google Scholar] [CrossRef] [PubMed]
- Hollmann, S.; Touster, O. The l-xylulose-xylitol enzyme and other polyol dehydrogenases of guinea pig liver mithochondria. J. Biol. Chem. 1957, 225, 87–102. [Google Scholar] [PubMed]
- Asakura, T.; Adachi, K.; Minakami, S.; Yoshikawa, H. Non-glycolytic sugar metabolism in human erythrocytes. J. Biochem. 1967, 62, 184–193. [Google Scholar] [CrossRef] [PubMed]
- El-Kabbani, O.; Carbone, V.; Darmanin, C.; Ishikura, S.; Hara, A. Structure of the tetrameric form of human l-xylulose reductase: probing the inhibitor-binding site with molecular modeling and site-directed mutagenesis. Proteins 2005, 60, 424–432. [Google Scholar] [CrossRef] [PubMed]
- Nakagawa, J.; Ishikura, S.; Asami, J.; Isaji, T.; Usami, N.; Hara, A.; Sakurai, T.; Tsuritani, K.; Oda, K.; Takahashi, M.; Yoshimoto, M.; Otsuka, N.; Kitamura, K. Molecular characterization of mammalian dicarbonyl/l-xylulose reductase and its localization in kidney. J. Biol. Chem. 2002, 277, 17883–17891. [Google Scholar] [CrossRef] [PubMed]
- Maret, W.; Auld, D.S. Purification and characterization of human liver sorbitol dehydrogenase. Biochemistry 1988, 27, 1622–1628. [Google Scholar] [CrossRef] [PubMed]
- Darmanin, C.; El-Kabbani, O. Modeling studies of the active site of human sorbitol dehydrogenase: as approach to structure-based inhibitor design of the enzyme. Bioorg. Med. Chem. Lett. 2001, 11, 3133–3136. [Google Scholar] [CrossRef]
- Lee, F.K.; Chung, S.; Cheung, M.C. The human sorbitol dehydrogenase gene: cDNA cloning, sequence determination, and mapping by fluorescence in situ hybridization. Genomics 1994, 21, 354–358. [Google Scholar] [CrossRef] [PubMed]
- Pauly, T.A.; Ekstrom, J.L.; Beebe, D.A.; Chrunyk, B.; Cunningham, D.; Griffor, M.; Kamath, A.; Lee, S.E.; Madura, R.; Mcguire, D.; Subashi, T.; Wasilko, D.; Watts, P.; Mylari, B.L.; Oates, P.J.; Adams, P.D.; Rath, V.L. X-ray crystallographic and kinetic studies of human sorbitol dehydrogenase. Structure 2003, 11, 1071–1085. [Google Scholar] [CrossRef]
- Garrett, R.H.; Grisham, C.M. The tricarboxylic acid cycle. In Biochemistry; Saunders College Publishing: Philadelphia, PA, USA, 1999; pp. 639–672. [Google Scholar]
- Lodish, H.; Baltimore, D.; Berk, A.; Zipursky, S.L.; Matsudaira, P.; Darnell, J. Mitochondria and the metabolism of carbohydrates and lipids. In Molecular Cell Biology; Scientific American Books, Inc.: New York, NY, USA, 1995; pp. 745–752. [Google Scholar]
- Peng, L.; Schousboe, A.; Hertz, L. Utilization of alpha-ketoglutarate as a precursor for transmitter glutamate in cultured cerebellar granule cells. Neurochem. Res. 1991, 16, 29–34. [Google Scholar] [CrossRef] [PubMed]
- Hertz, L.; Dringen, R.; Schousboe, A.; Robinson, S.R. Astrocytes: glutamate producers for neurons. J. Neurosci. Res. 1999, 57, 417–428. [Google Scholar] [CrossRef]
- LaNoue, K.F.; Walajtys, E.I.; Williamson, J.R. Regulation of glutamate metabolism and interactions with the citric acid cycle in rat heart mitochondria. J. Biol. Chem. 1973, 248, 7171–7183. [Google Scholar] [PubMed]
- Krebs, H.A. Equilibria in transamination systems. Biochem. J. 1953, 54, 82–86. [Google Scholar] [CrossRef] [PubMed]
- Shin’oka, T.; Imai, Y.; Ikada, Y. Transplantation of a tissue-engineered pulmonary artery. New Engl. J. Med. 2001, 344, 532–533. [Google Scholar] [CrossRef] [PubMed]
- Matsumura, G.; Hibino, N.; Ikada, Y.; Kurosawa, H.; Shin’oka, T. Successful application of tissue engineered vascular autografts: clinical experience. Biomaterials 2003, 24, 2303–2308. [Google Scholar] [CrossRef]
- Shin’oka, T.; Matsumura, G.; Hibino, N.; Naito, Y.; Watanabe, M.; Konuma, T.; Nagatsu, M.; Sakamoto, T.; Kurosawa, H. Midterm clinical results of tissue-engineered vascular autografts seeded with autologous bone marrow cells. J. Thorac. Cardiovasc. Surgery 2005, 129, 1330–1338. [Google Scholar] [CrossRef] [PubMed]
- Martin, D.P.; Williams, S.F. Medical applications of poly-4-hydroxybutyrate: A strong flexible absorbable biomaterial. Biochem. Eng. J. 2003, 16, 97–105. [Google Scholar] [CrossRef]
- Burks, C.A.; Bundy, K.; Fotuhi, P.; Alt, E. Characterization of 75:25 poly(l-lactide-co-ε-caprolactone) thin films for the endoluminal delivery of adipose-derived stem cells to abdominal aortic aneurysms. Tissue Eng. 2006, 12, 2591–2600. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.H.; Kwon, J.H.; Chung, M.S.; Chung, E.; Jung, Y.; Kim, S.H.; Kim, Y.H. Fabrication of a new tubular fibrous PLCL scaffold for vascular tissue engineering. J. Biomater. Sci. Polm. Ed. 2006, 17, 1359–1374. [Google Scholar] [CrossRef]
- McKay, R. Stem cells – hype and hope. Nature 2000, 406, 361–364. [Google Scholar] [CrossRef] [PubMed]
- Noishiki, Y.; Tomizawa, Y.; Yamane, Y.; Matsumoto, A. Autocrine angiogenic vascular prosthesis with bone marrow transplantation. Nat. Med. 1996, 2, 90–93. [Google Scholar] [CrossRef] [PubMed]
- He, W.; Ma, Z.W.; Yong, T.; Teo, W.E.; Ramakrishna, S. Fabrication of collagen-coated biodegradable polymer nanofiber mesh and its potential for endothelial cells growth. Biomaterials 2005, 26, 7606–7615. [Google Scholar] [CrossRef] [PubMed]
- Pêgo, A.P.; Siebum, B.; Van Luyn, M.J.A.; Gallego, Y.; Van Seijen, X.J.; Poot, A.A.; Grijpma, D.W.; Feijen, J. Preparation of degradable porous structures based on 1,3-trimethylene carbonate and d,l-lactide (co)polymers for heart tissue engineering. Tissue Eng. 2003, 9, 981–994. [Google Scholar] [CrossRef] [PubMed]
- Pêgo, A.P.; Poot, A.A.; Grijpma, D.W.; Feijen, J. Biodegradable elastomeric scaffolds for soft tissue engineering. J. Controll. Release 2003, 87, 69–79. [Google Scholar] [CrossRef]
- Pêgo, A.P.; Poot, A.A.; Grijpma, D.W.; Feijen, J. Copolymers of trimethylene carbonate and ε-caprolactone for porous nerve guides: synthesis and properties. J. Biomater. Sci. Polym. Ed. 2001, 12, 35–53. [Google Scholar] [CrossRef] [PubMed]
- Pêgo, A.P.; Van Luyn, M.J.A.; Brouwer, L.A.; van Wachem, P.B.; Poot, A.A.; Grijpma, D.W.; Feijen, J. In vivo behavior of poly(1,3-trimethylene carbonate) and copolymers of 1,3-trimethylene carbonate with d,l-lactide or ε-caprolcatone: degradation and tissue response. J. Biomed. Mater. Res. A 2003, 67, 1044–1054. [Google Scholar] [CrossRef] [PubMed]
- Pêgo, A.P.; Poot, A.A.; Grijpma, D.W.; Feijen, J. In vitro degradation of trimethylene carbonate based (co)polymer. Macrmol. Biosci. 2002, 2, 411–419. [Google Scholar] [CrossRef]
- Wang, Y.; Ameer, G.A.; Sheppard, B.J.; Langer, R. A tough biodegradable elastomer. Nat. Biotech. 2002, 20, 602–606. [Google Scholar] [CrossRef] [PubMed]
- Engelmayr, G.C.; Cheng, M.; Bettinger, C.J.; Borenstein, J.T.; Langer, R.; Freed, L.E. Accordion-like honeycombs for tissue engineering of cardiac anisotropy. Nat. Mater. 2008, 7, 1003–1010. [Google Scholar] [CrossRef] [PubMed]
- Nijst, C.L.E.; Bruggeman, J.P.; Karp, J.M.; Ferreira, L.; Zumbuehl, A.; Bettinger, C.J.; Langer, R. Synthesis and characterization of photocurable elastomers from poly(glycerol-co-sebacate). Biomacromolecules 2007, 8, 3067–3073. [Google Scholar] [CrossRef] [PubMed]
- Mahdavi, A.; Ferreira, L.; Sundback, C.; Nichol, J.W.; Chan, E.P.; Carter, D.J.D.; Bettinger, C.J.; Patanavanich, S.; Chignozha, L.; Ben-Joseph, E.; Galakatos, A.; Pryor, H.; Pomerantseva, I.; Masiakos, P.T.; Faquin, W.; Zumbuehl, A.; Hong, S.; Borenstein, J.; Vacanti, J.; Langer, R.; Karp, J.M. A biodegradable and biocompatible gecko-inspired tissue adhesive. Proc. Natl. Acad. Sci. USA 2008, 105, 2307–2312. [Google Scholar] [CrossRef] [PubMed]
- Bruggeman, J.P.; Bettinger, C.J.; Nijst, C.L.E.; Kohane, D.S.; Langer, R. Biodegradable xylitol-based polymers. Adv. Mater. 2008, 20, 1922–1927. [Google Scholar] [CrossRef]
- Bruggeman, J.P.; de Bruin, B.J.; Bettinger, C.J.; Langer, R. Biodegradable poly(polyol sebacate) polymers. Biomaterials 2008, 29, 4726–4735. [Google Scholar] [CrossRef] [PubMed]
- Bettinger, C.J.; Bruggeman, J.P.; Borenstein, J.T.; Langer, R. Amino alcohol-based degradable poly(ester amide) elastomers. Biomaterials 2008, 29, 2315–2325. [Google Scholar] [CrossRef] [PubMed]
- Roy, D.R.; Parthasarathi, R.; Maiti, B.; Subramanian, V.; Chattaraj, P.K. Electrophilicity as a possible descriptor for toxicity prediction. Bioorg. Med. Chem. 2005, 13, 3405–3412. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.; Webb, A.R.; Ameer, G.A. Novel citric acid-based biodegradable elastomers for tissue engineering. Adv. Mater. 2004, 16, 511–516. [Google Scholar] [CrossRef]
- Yang, J.; Webb, A.R.; Pickerill, S.J.; Hageman, G.; Ameer, G.A. Synthesis and evaluation of poly(diol citrate) biodegradable elastomers. Biomaterials 2006, 27, 1889–1898. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.; Motlagh, D.; Webb, A.R.; Ameer, G.A. Novel biphasic elastomeric scaffold for small-diameter blood vessel tissue engineering. Tissue Eng. 2005, 11, 1876–1886. [Google Scholar] [CrossRef] [PubMed]
- Roeder, R.; Wolfe, J.; Lianakis, N.; Hinson, T.; Geddes, L.A.; Obermiller, J. Compliance, elastic modulus, and burst pressure of small-intestine submucosa (SIS), small-diameter vascular grafts. J. Biomed. Mater. Res. 1999, 47, 65–70. [Google Scholar] [CrossRef]
- Ma, P.X.; Zhang, R. Microtubular architecture of biodegradable polymer scaffolds. J. Biomed. Mater. Res. 2001, 56, 469–477. [Google Scholar] [CrossRef]
- Yang, J.; Motlagh, D.; Allen, J.B.; Webb, W.R.; Kibbe, M.R.; Aalami, O.; Kapadia, M.; Carroll, T.J.; Ameer, G.A. Modulating expanded polytetrafluoroethylene vascular graft host response via citric acid-based biodegradable elastomers. Adv. Mater. 2006, 18, 1493–1498. [Google Scholar] [CrossRef]
- Xue, L.; Greisler, H.P. Biomaterials in the development and future of vascular grafts. J. Vasc. Surg. 2003, 37, 472–480. [Google Scholar] [CrossRef] [PubMed]
- Eagleton, M.J.; Ouriel, K.; Shortell, C.; Green, R.M. Femoral-infrapopliteal bypass with prosthetic grafts. Surgery 1999, 126, 759–765. [Google Scholar] [CrossRef]
- Noh, I.; Goodman, S.L.; Hubbell, J.A. Chemical modification and photograft polymerization upon expanded poly(tetrafluoroethylene). J. Biomater. Sci. Polym. Ed. 1998, 9, 407–426. [Google Scholar] [CrossRef] [PubMed]
- Herring, M.B.; Dilley, R.; Jersild, R.A.; Boxer, L.; Gardner, A.; Glover, J. Seeding arterial prostheses with vascular endothelium: the nature of the lining. Ann. Surg. 1979, 190, 84–90. [Google Scholar] [CrossRef] [PubMed]
- Motlagh, D.; Allen, J.; Hoshi, R.; Yang, J.; Lui, K.; Ameer, G. Hemocompatibility evaluation of poly(diol citrate) in vitro for vascular tissue engineering. J. Biomed. Mater. Res. A 2007, 82, 907–916. [Google Scholar] [CrossRef] [PubMed]
- Heijnen, H.F.; Schiel, A.E.; Fijnheer, R.; Geuze, H.J.; Sixma, J.J. Activated platelets release two types of membrane vesicles: microvesicles by surface shedding and exosomes derived from exocytosis of multivesicular bodies and α-granules. Blood 1999, 94, 3791–3799. [Google Scholar] [PubMed]
- Gorbet, M.B.; Sefton, M.V. Biomaterial-associated thrombosis: roles of coagulation factors, complement, platelets and leukocytes. Biomaterials 2004, 25, 5681–5703. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.H.; Brennan, F.R.; Jacobs, J.J.; Urban, R.M.; Ragasa, D.R.; Glant, T.T. Human monocyte/macrophage response to cobalt-chromium corrosion products and titanium particles in patients with total joint replacements. J. Orthop. Res. 1997, 15, 40–49. [Google Scholar] [CrossRef] [PubMed]
- Heil, T.L.; Volkmann, K.R.; Wataha, J.C.; Lockwood, P.E. Human peripheral blood monocytes versus THP-1 monocytes for in vitro biocompatibility testing of dental material components. J. Oral Rehabil. 2002, 29, 401–407. [Google Scholar] [CrossRef] [PubMed]
- Ifkovits, J.L.; Burdick, J.A. Review: Photopolymerizable and degradable biomaterials for tissue engineering applications. Tissue Eng. 2007, 13, 2369–2385. [Google Scholar] [CrossRef] [PubMed]
- Grinstaff, M.W. Biodendrimers: New polymeric biomaterials for tissue engineering. Chem. Eur. J. 2002, 8, 2839–2846. [Google Scholar] [CrossRef]
- Sntjens, S.H.M.; Nettles, D.L.; Carnahan, M.A.; Setton, L.A.; Grinstaff, M.W. Biodendrimer-based hydrogel scaffolds for cartilage tissue repair. Biomacromolecules 2006, 7, 310–316. [Google Scholar] [CrossRef] [PubMed]
- Velazquez, A.J.; Carnahan, M.A.; Kristinsson, J.; Stinnett, S.; Grinstaff, M.W.; Kim, T. New dendritic adhesives for sutureless ophthalmic surgical procedures: In vitro studies of corneal laceration repair. Arch. Ophthalmol. 2004, 122, 867–870. [Google Scholar] [CrossRef] [PubMed]
- Bain, W.E.; Maurice, D.M. Physiological variations in intraocular pressure. Trans. Ophthalmol. Soc. UK 1959, 79, 249–260. [Google Scholar] [PubMed]
- Luman, N.R.; Kim, T.; Grinstaff, M.W. Dendritic polymers composed of glycerol and succinic acid: Synthetic methodologies and medical applications. Pure Appl. Chem. 2004, 76, 1375–1385. [Google Scholar] [CrossRef]
- Barrett, D.G.; Yousaf, M.N. A tunable, chemoselective, and moldable biodegradable polyester for cell scaffolds. ChemBioChem 2008, 9, 62–66. [Google Scholar] [CrossRef] [PubMed]
- Azim, H.; Dekhterman, A.; Jiang, Z.; Gross, R.A. Candida Antarctica lipase B-catalyzed synthesis of poly(butylene succinate): shorter chain building block also work. Biomacromolecules 2006, 7, 3093–3097. [Google Scholar] [CrossRef] [PubMed]
- Chan, E.W.L.; Yousaf, M.N. Immobilization of ligands with precise control of density to electroactive surfaces. J. Am. Chem. Soc. 2006, 128, 15542–15546. [Google Scholar] [CrossRef] [PubMed]
- Chan, E.W.L.; Yousaf, M.N. Site-selective immobilization of ligands with control of density on electroactive microelectrode arrays. ChemPhysChem 2007, 8, 1469–1472. [Google Scholar] [CrossRef] [PubMed]
- Chan, E.W.L.; Yousaf, M.N. A photo-electroactive surface strategy for immobilizing ligands in patterns and gradients for studies of cell polarization. Mol. Biosyst. 2008, 4, 746–753. [Google Scholar] [CrossRef] [PubMed]
- Chan, E.W.L.; Park, S.; Yousaf, M.N. An electroactive catalytic dynamic substrate that immobilizes and releases patterned ligands, proteins, and cells. Angew. Chem. Int. Ed. 2008, 47, 6267–6271. [Google Scholar] [CrossRef] [PubMed]
- Park, S.; Yousaf, M.N. An interfacial oxime reaction to immobilize ligands and cells in patterns and gradients to photo-active surfaces. Langmuir 2008, 24, 6201–6207. [Google Scholar] [CrossRef] [PubMed]
- Barrett, D.G.; Yousaf, M.N. Preparation of a class of versatile, chemoselective, and amorphous polyketoesters. Biomacromolecules 2008, 9, 2029–2035. [Google Scholar] [CrossRef] [PubMed]
- Prime, K.L.; Whitesides, G.M. Self-assembled organic monolayers: model systems for studying adsorption of proteins at surfaces. Science 1991, 252, 1164–1167. [Google Scholar] [CrossRef] [PubMed]
- Prime, K.L.; Whitesides, G.M. Adsorption of proteins onto surfaces containing end-attached oligo(ethylene oxide): A model system using self-assembled monolayers. J. Am. Chem. Soc. 1993, 115, 10714–10721. [Google Scholar] [CrossRef]
- Pierschbacher, M.D.; Ruoslahti, E. Cell attachment activity of fibronectin can be duplicated by small synthetic fragments of the molecule. Nature 1984, 309, 30–33. [Google Scholar] [CrossRef] [PubMed]
- Ruoslahti, E. RGD and other recognition sequences for integrins. Ann. Rev. Cell Dev. Biol. 1996, 12, 697–715. [Google Scholar] [CrossRef] [PubMed]
- Barrett, D.G.; Yousaf, M.N. Poly(triol α-ketoglutarate) as biodegradable, chemoselective, and mechanically tunable elastomers. Macromolecules 2008, 41, 6347–6352. [Google Scholar] [CrossRef]
- Barrett, D.G.; Lamb, B.M.; Yousaf, M.N. Microfluidic etching and oxime-based tailoring of biodegradable polyketoesters. Langmuir 2008, 24, 9861–9867. [Google Scholar] [CrossRef] [PubMed]
- Peter, S.J.; Yaszemski, M.J.; Suggs, L.J.; Payne, R.G.; Langer, R.; Hayes, W.C.; Unroe, M.R.; Alemany, L.B.; Engel, P.S.; Mikos, A.G. Characterization of partially saturated poly(propylene fumarate) for orthopedic application. J. Biomater. Polym. Sci. Ed. 1997, 8, 893–904. [Google Scholar] [CrossRef]
- Fisher, J.P.; Holland, T.A.; Dean, D.; Engel, P.S.; Mikos, A.G. Synthesis and properties of photocross-linked poly(propylene fumarate) scaffolds. J. Biomater. Sci. Polym. Ed. 2001, 12, 673–687. [Google Scholar] [CrossRef] [PubMed]
- Timmer, M.D.; Ambrose, C.G.; Mikos, A.G. Evaluation of thermal- and photo-crosslinked biodegradable poly(propylene fumarate)-based networks. J. Biomed. Mater. Res. Part A 2003, 66, 811–818. [Google Scholar] [CrossRef] [PubMed]
- Fisher, J.P.; Timmer, M.D.; Holland, T.A.; Dean, D.; Engel, P.S.; Mikos, A.G. Photoinitiated cross-linking of the biodegradable polyester poly(propylene fumarate). Part I. Determination of network structure. Biomacromolecules 2003, 4, 1327–1334. [Google Scholar] [CrossRef] [PubMed]
- Fisher, J.P.; Holland, T.A.; Dean, D.; Engel, P.S.; Mikos, A.G. Photoinitiated cross-linking of the biodegradable polyester poly(propylene fumarate). Part II. In vitro degradation. Biomacromolecules 2003, 4, 1335–1342. [Google Scholar] [CrossRef] [PubMed]
- Fisher, J.P.; Vehof, J.W.M.; Dean, D.; van der Waerden, J.P.C.M.; Holland, T.A.; Mikos, A.G.; Jansen, J.A. Soft and hard tissue response to photocrosslinked poly(propylene fumarate) scaffolds in a rabbit model. J. Biomed. Mater. Res. 2002, 59, 547–556. [Google Scholar] [CrossRef] [PubMed]
- Solheim, E.; Sudmann, B.; Bang, G.; Sudmann, E. Biocompatibility and effects on osteogenesis of poly(orthoester) compared to poly(d,l-lactic acid). J. Biomed. Mater. Res. 2000, 49, 257–263. [Google Scholar] [CrossRef]
- van der Elst, M.; Klein, C.P.A.T.; de Blieck-Hogervorst, J.M.; Patka, P.; Haarman, H.J.T.M. Bone tissue response to biodegradable polymers used for intra medullary facture fixation: A long-term in vivo study in sheep femora. Biomaterials 1999, 20, 121–128. [Google Scholar] [CrossRef]
- Ibim, S.M.; Uhrich, K.E.; Bronson, R.; El-Amin, S.F.; Langer, R.S.; Laurencin, C.T. Poly(anhydride-co-imides): In vivo biocompatibility in a rat model. Biomaterials 1998, 19, 941–951. [Google Scholar] [CrossRef]
- Jansen, J.A.; de Ruijter, J.E.; Janssen, P.T.M.; Paquay, Y.G.C.J. Histological evaluation of a biodegradable polyactive/hydroxyapatite membrane. Biomaterials 1995, 16, 819–827. [Google Scholar] [CrossRef]
Sample Availability: Not available. |
© 2009 by the authors; licensee Molecular Diversity Preservation International, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Barrett, D.G.; Yousaf, M.N. Design and Applications of Biodegradable Polyester Tissue Scaffolds Based on Endogenous Monomers Found in Human Metabolism. Molecules 2009, 14, 4022-4050. https://doi.org/10.3390/molecules14104022
Barrett DG, Yousaf MN. Design and Applications of Biodegradable Polyester Tissue Scaffolds Based on Endogenous Monomers Found in Human Metabolism. Molecules. 2009; 14(10):4022-4050. https://doi.org/10.3390/molecules14104022
Chicago/Turabian StyleBarrett, Devin G., and Muhammad N. Yousaf. 2009. "Design and Applications of Biodegradable Polyester Tissue Scaffolds Based on Endogenous Monomers Found in Human Metabolism" Molecules 14, no. 10: 4022-4050. https://doi.org/10.3390/molecules14104022
APA StyleBarrett, D. G., & Yousaf, M. N. (2009). Design and Applications of Biodegradable Polyester Tissue Scaffolds Based on Endogenous Monomers Found in Human Metabolism. Molecules, 14(10), 4022-4050. https://doi.org/10.3390/molecules14104022





