Combination of R-R Interval and Crest Time in Assessing Complexity Using Multiscale Cross-Approximate Entropy in Normal and Diabetic Subjects
Abstract
1. Introduction
2. Methods
2.1. Study Population
2.2. Study Protocol
2.3. Data Acquisitionand Analysis
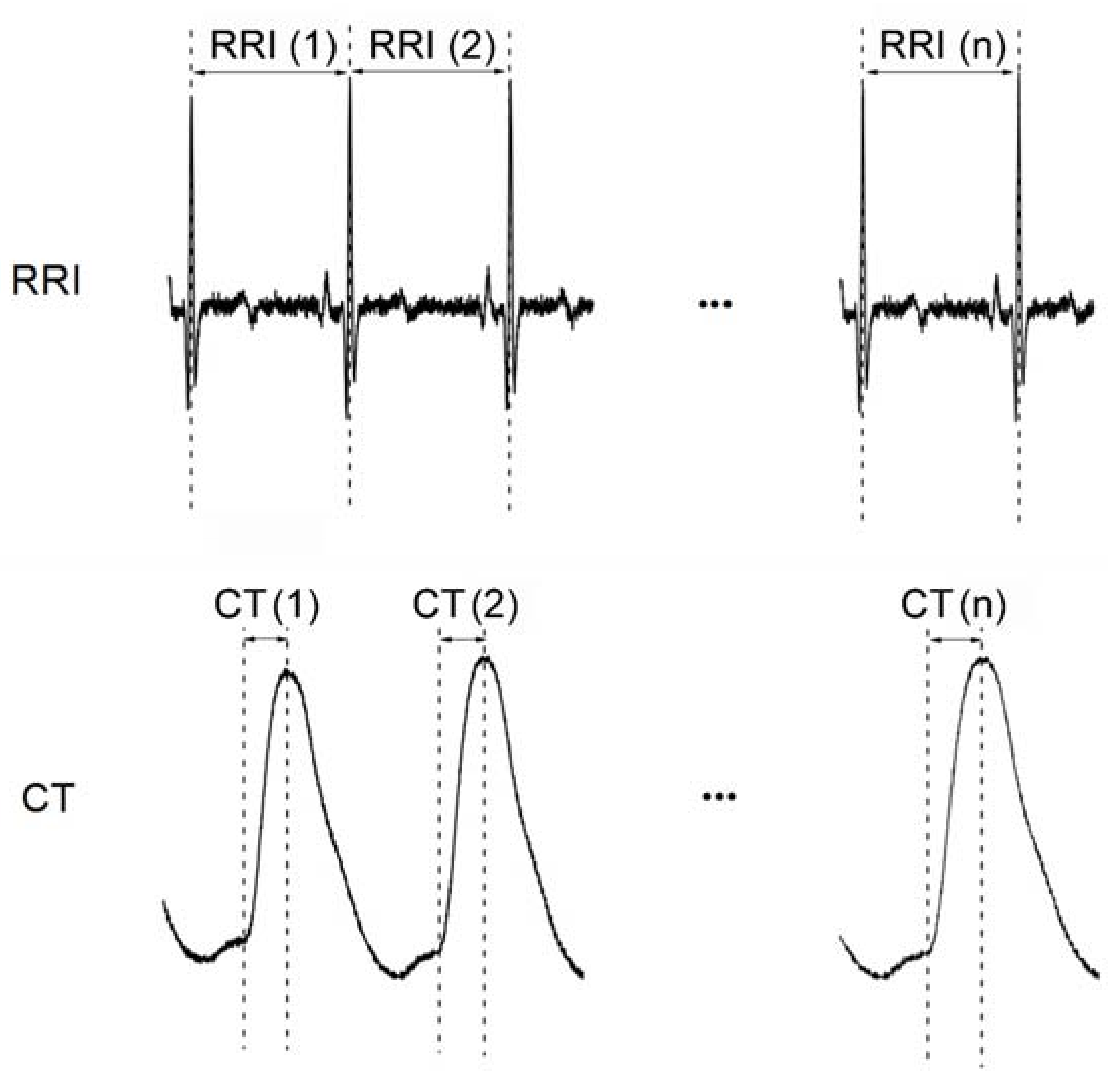
2.3.1. Definition of Two Synchronized Physiological Signals: R-R Interval (RRI) and Crest Time (CT)
2.3.2. MSE and MCAE Analyses
2.4. Statistical Analysis
3. Results
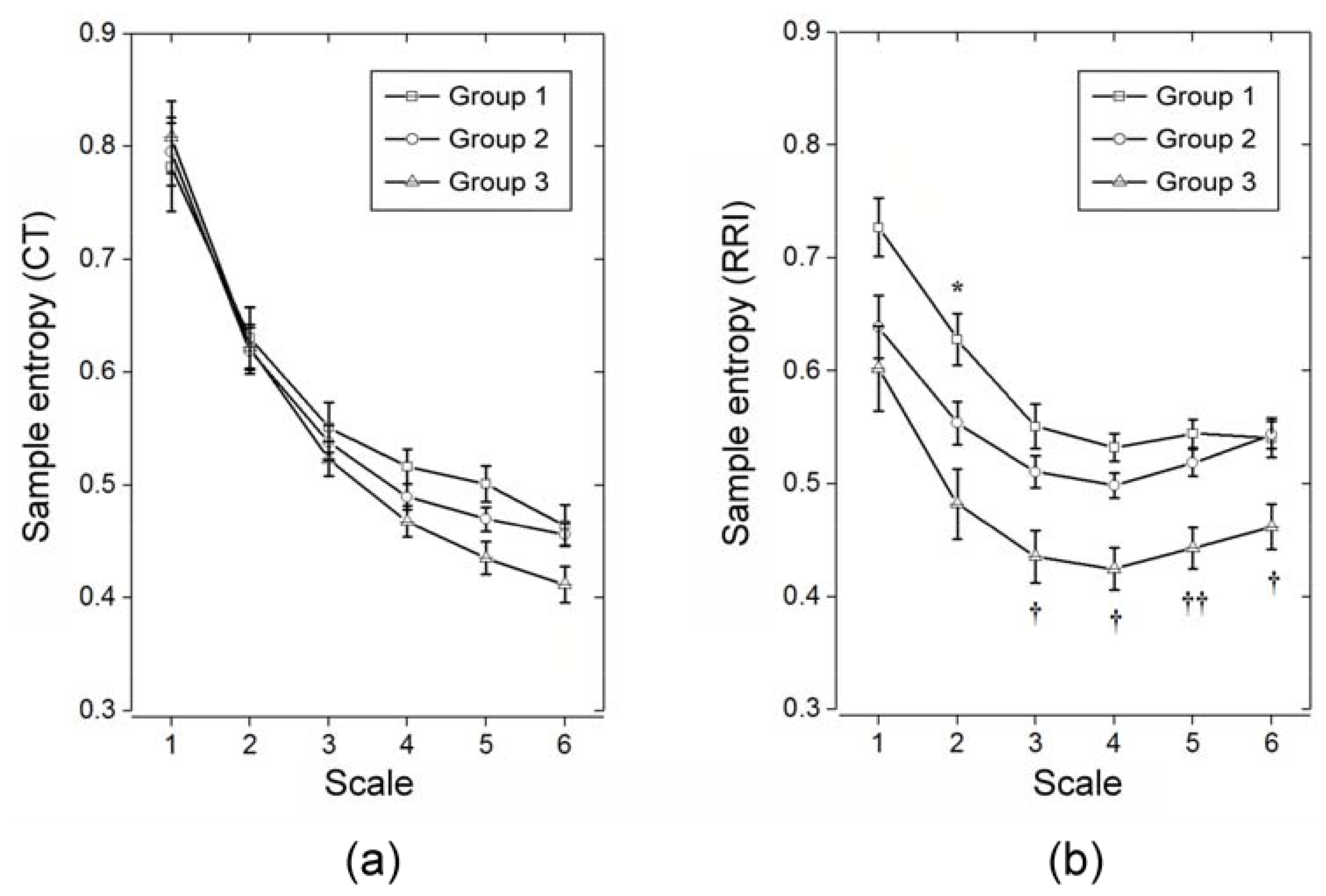
3.1. MSE Analysis on Single Waveform Contour Cardiovascular System-Related Parameters (RRI and CT)
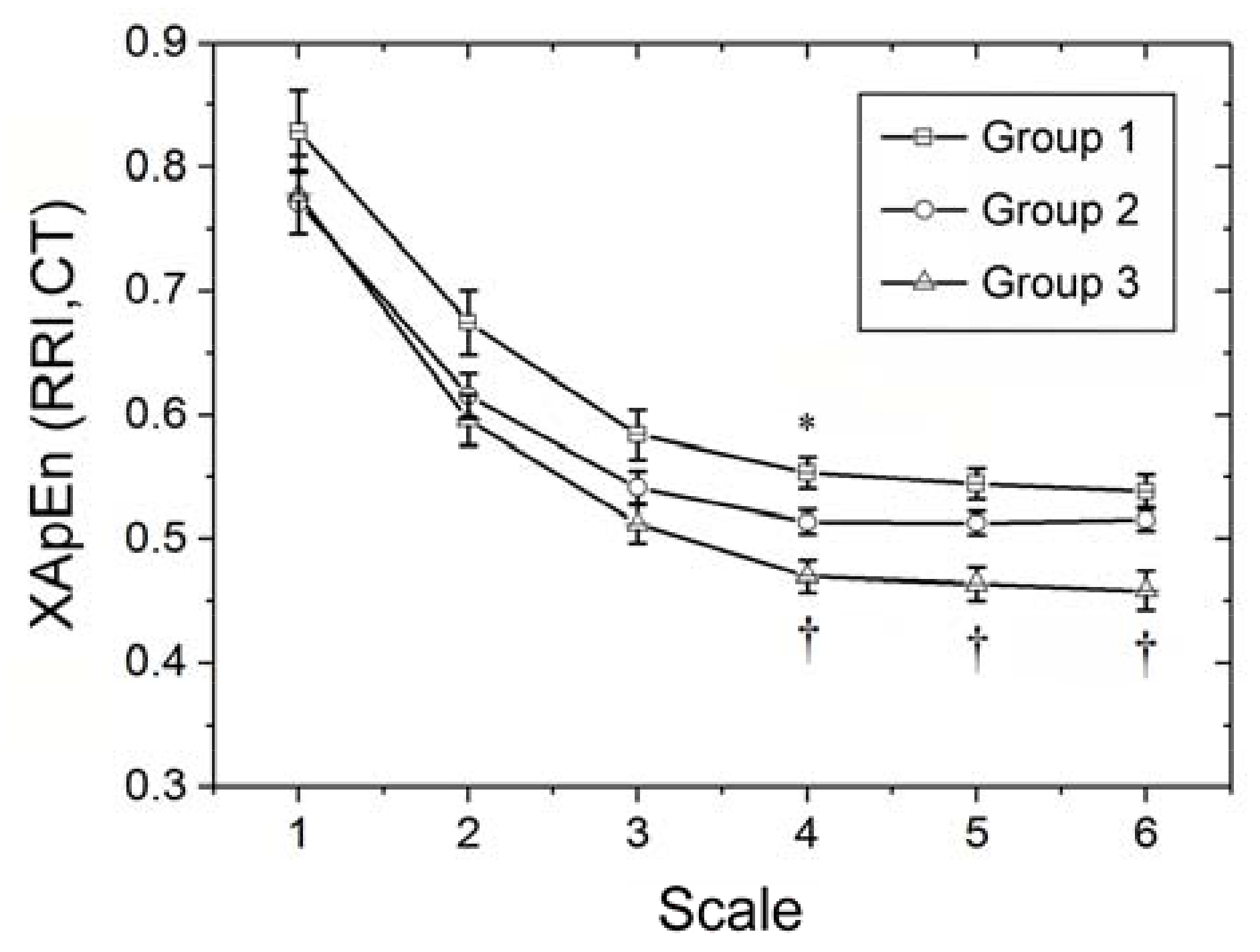
3.2. MultiscaleCross-Approximate Entropy Analysis of Synchronized RRI and CT Time Series
3.3. Correlations of Different Multiscale Entropy Indices with Demographic, Anthropometric, Hemodynamic, and Serum Biochemical Parameters in the Testing Subjects
3.4. Multivariate Analysis for MEILS(CT), MEILS(RRI), and MCEILS(RRI,CT)
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Lennon, R.P.; Claussen, K.A.; Kuersteiner, K.A. State of the Heart: An Overview of the Disease Burden of Cardiovascular Disease from an Epidemiologic Perspective. Prim. Care 2018, 45, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Wu, H.T.; Lin, B.Y.; Yang, C.C.; Ou, Y.N.; Sun, C.K. Assessment of Vascular Health With Photoplethysmographic Waveforms From the Fingertip. IEEE J. Biomed. Health Inform. 2017, 21, 382–386. [Google Scholar] [CrossRef] [PubMed]
- Freis, E.D.; Heath, W.C.; Luchsinger, P.C.; Snell, R.E. Changes in the carotid pulse which occur with age and hypertension. Am. Heart J. 1966, 71, 757–765. [Google Scholar] [CrossRef]
- Endresen, J.; Gamble, A.; Hill, D.W. A comparison of two methods for the computer analysis of arterial blood pressure waveforms. Eur. J. Intensive Care Med. 1975, 1, 125–128. [Google Scholar] [CrossRef] [PubMed]
- Kelly, R.; Hayward, C.; Avolio, A.; O’Rourke, M. Noninvasive determination of age-related changes in the human arterial pulse. Circulation 1989, 80, 1652–1659. [Google Scholar] [CrossRef] [PubMed]
- Su, F.; Li, Z.; Sun, X.; Han, N.; Wang, L.; Luo, X. The pulse wave analysis of normal pregnancy: Investigating the gestational effects on photoplethysmographic signals. Biomed. Mater. Eng. 2014, 24, 209–219. [Google Scholar] [PubMed]
- Wu, H.T.; Lee, K.W.; Pan, W.Y.; Liu, A.B.; Sun, C.K. Difference in bilateral digital volume pulse as a novel non-invasive approach to assessing arteriosclerosis in aged and diabetic subjects: A preliminary study. Diabetes Vasc. Dis. Res. 2017, 14, 254–257. [Google Scholar] [CrossRef] [PubMed]
- Elgendi, M. On the analysis of fingertip photoplethysmogram signals. Curr. Cardiol. Rev. 2012, 8, 14–25. [Google Scholar] [CrossRef] [PubMed]
- Tomiyama, H.; Yamashina, A. Non-invasive vascular function tests: Their pathophysiological background and clinical application. Circ. J. 2010, 74, 24–33. [Google Scholar] [CrossRef] [PubMed]
- Hsu, P.C.; Wu, H.T.; Sun, C.K. Assessment of Subtle Changes in Diabetes-Associated Arteriosclerosis using Photoplethysmographic Pulse Wave from Index Finger. J. Med.Syst. 2018, 42, 43. [Google Scholar] [CrossRef] [PubMed]
- Pomeranz, B.; Macaulay, R.J.; Caudill, M.A.; Kutz, I.; Adam, D.; Gordon, D.; Kilborn, K.M.; Barger, A.C.; Shannon, D.C.; Cohen, R.J.; et al. Assessment of autonomic function in humans by heart rate spectral analysis. Am. J. Physiol. 1985, 248, H151–H153. [Google Scholar] [CrossRef] [PubMed]
- Huynh, L.N.; Truong, Q.D.K. FIDELITY: Fuzzy inferential diagnostic engine for on-Line support to physicians. In 4th International Conference on Biomedical Engineering in Vietnam, IFMBE Proceedings; Vo, V.T., Nguyen, B.T., Truong, Q.D.K., Tran, H.L.P., Eds.; Springer: Berlin/Heidelberg, Germany, 2013; pp. 410–423. [Google Scholar]
- Villecco, F.; Pellegrino, A. Evaluation of uncertainties in the design process of complex mechanical systems. Entropy 2017, 19, 475. [Google Scholar] [CrossRef]
- Alty, S.R.; Angarita-Jaimes, N.; Millasseau, S.C.; Chowienczyk, P.J. Predicting arterial stiffness from the digital volume pulse waveform. IEEE Trans. Biomed. Eng. 2007, 54, 2268–2275. [Google Scholar] [CrossRef] [PubMed]
- Costa, M.; Goldberger, A.L.; Peng, C.K. Multiscale entropy to distinguish physiologic and synthetic RR time series. Comput. Cardiol. 2002, 29, 137–140. [Google Scholar] [PubMed]
- Gao, Y.; Villecco, F.; Li, M.; Song, W. Multi-scale permutation entropy based on improved LMD and HMM for rolling bearing diagnosis. Entropy 2017, 19, 176. [Google Scholar] [CrossRef]
- Villecco, F.; Pellegrino, A. Entropic measure of epistemic uncertainties in multibody system models by axiomatic design. Entropy 2017, 19, 291. [Google Scholar] [CrossRef]
- Liu, A.B.; Wu, H.T.; Liu, C.W.; Liu, C.C.; Tang, C.J.; Tsai, I.T.; Sun, C.K. Application of multiscale entropy in arterial waveform contour analysis in healthy and diabetic subjects. Med. Biol. Eng. Comput. 2015, 53, 89–98. [Google Scholar] [CrossRef] [PubMed]
- Wu, H.T.; Hsu, P.C.; Lin, C.F.; Wang, H.J.; Sun, C.K.; Liu, A.B.; Lo, M.T.; Tang, C.J. Multiscale entropy analysis of pulse wave velocity for assessing atherosclerosis in the aged and diabetic. IEEE Trans. Biomed. Eng. 2011, 58, 2978–2981. [Google Scholar] [PubMed]
- Lin, G.M.; Haryadi, B.; Yang, C.M.; Chu, S.C.; Yang, C.C.; Wu, H.T. Discrepancies between conventional multiscale entropy and modified short-time multiscale entropy of photoplethysmographic pulse signals in middle- and old-aged individuals with or without diabetes. Entropy 2017, 19, 132. [Google Scholar] [CrossRef]
- Wu, H.T.; Lee, C.Y.; Liu, C.C.; Liu, A.B. Multiscale cross-approximate entropy analysis as a measurement of complexity between ECG R-R interval and PPG pulse amplitude series among the normal and diabetic subjects. Comput. Math. Methods Med. 2013, 2013, 231762. [Google Scholar] [CrossRef] [PubMed]
- Wu, H.T.; Liu, C.C.; Lo, M.T.; Hsu, P.C.; Liu, A.B.; Chang, K.Y.; Tang, C.J. Multiscale cross-approximate entropy analysis as a measure of complexity among the aged and diabetic. Comput. Math. Methods Med. 2013, 2013, 324325. [Google Scholar] [CrossRef] [PubMed]
- Wu, H.T.; Yang, C.C.; Lin, G.M.; Haryadi, B.; Chu, S.C.; Yang, C.M.; Sun, C.K. Multiscale cross-approximate entropy analysis of bilateral fingertips photoplethysmographic pulse amplitudes among middle-to-old aged individuals with or without type 2 diabetes. Entropy 2017, 19, 145. [Google Scholar] [CrossRef]
- American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care 2014, 37 (Suppl. 1), S81–S90. [Google Scholar]
- Lin, S.L.; Tung, P.C.; Huang, N.E. Data analysis using a combination of independent component analysis and empirical mode decomposition. Phys. Rev. E Stat. Nonlinear Biol. Soft Matter Phys. 2009, 79, 066705. [Google Scholar] [CrossRef] [PubMed]
- Wu, Z.; Huang, N.E.; Long, S.R.; Peng, C.K. On the trend, detrending, and variability of nonlinear and nonstationary time series. Proc. Natl. Acad. Sci. USA 2007, 104, 14889–14894. [Google Scholar] [CrossRef] [PubMed]
- Wu, H.T.; Lee, C.H.; Liu, A.B.; Chung, W.S.; Tang, C.J.; Sun, C.K.; Yip, H.K. Arterial stiffness using radial arterial waveforms measured at the wrist as an indicator of diabetic control in the elderly. IEEE Trans. Biomed. Eng. 2011, 58, 243–252. [Google Scholar] [PubMed]
- Costa, M.; Goldberger, A.L.; Peng, C.K. Multiscale entropy analysis of biological signals. Phys. Rev. E Stat. Nonlinear Biol. Soft Matter Phys. 2005, 71, 021906. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Yu, S.; Chen, H.; Lu, C.; Zhang, K.; Li, F. Cardiovascular autonomic function analysis using approximate entropy from 24-h heart rate variability and its frequency components in patients with type 2 diabetes. J. Diabetes Investig. 2015, 6, 227–235. [Google Scholar] [CrossRef] [PubMed]
- Pincus, S.; Singer, B.H. Higher-order dangers and precisely constructed taxa in models of randomness. Proc. Natl. Acad. Sci. USA 2014, 111, 5485–5490. [Google Scholar] [CrossRef] [PubMed]
- Pan, W.Y.; Su, M.C.; Wu, H.T.; Su, T.J.; Lin, M.C.; Sun, C.K. Multiscale entropic assessment of autonomic dysfunction in patients with obstructive sleep apnea and therapeutic impact of continuous positive airway pressure treatment. Sleep Med. 2016, 20, 12–17. [Google Scholar] [CrossRef] [PubMed]
- Studinger, P.; Goldstein, R.; Taylor, J.A. Age- and fitness-related alterations in vascular sympathetic control. J. Physiol. 2009, 587, 2049–2057. [Google Scholar] [CrossRef] [PubMed]
- Corman, B.; Duriez, M.; Poitevin, P.; Heudes, D.; Bruneval, P.; Tedgui, A.; Levy, B.I. Aminoguanidine prevents age-related arterial stiffening and cardiac hypertrophy. Proc. Natl. Acad. Sci. USA 1998, 95, 1301–1306. [Google Scholar] [CrossRef] [PubMed]
- McEniery, C.M.; O’Shaughnessy, K.M.; Harnett, P.; Arshad, A.; Wallace, S.; Maki-Petaja, K.; McDonnell, B.; Ashby, M.J.; Brown, J.; Cockcroft, J.R.; et al. Variation in the human matrix metalloproteinase-9 gene is associated with arterial stiffness in healthy individuals. Arterioscler. Thromb. Vasc. Biol. 2006, 26, 1799–1805. [Google Scholar] [CrossRef] [PubMed]
- O’Rourke, M.F.; Hashimoto, J. Mechanical factors in arterial aging: A clinical perspective. J. Am. Coll. Cardiol. 2007, 50, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Jamwal, S.; Sharma, S. Vascular endothelium dysfunction: A conservative target in metabolic disorders. Inflamm. Res. 2018, 67, 391–405. [Google Scholar] [CrossRef] [PubMed]
- Loader, J.; Montero, D.; Lorenzen, C.; Watts, R.; Meziat, C.; Reboul, C.; Stewart, S.; Walther, G. Acute Hyperglycemia Impairs Vascular Function in Healthy and Cardiometabolic Diseased Subjects: Systematic Review and Meta-Analysis. Arterioscler. Thromb. Vasc. Biol. 2015, 35, 2060–2072. [Google Scholar] [CrossRef] [PubMed]
- Huang, R.; Abdelmoneim, S.S.; Nhola, L.F.; Basu, R.; Basu, A.; Mulvagh, S.L. Relationship between glycosylated hemoglobin A1c and coronary flow reserve in patients with Type 2 diabetes mellitus. Expert Rev. Cardiovasc. Ther. 2015, 13, 445–453. [Google Scholar] [CrossRef] [PubMed]
- Richman, J.S.; Moorman, J.R. Physiological time-series analysis using approximate entropy and sample entropy. Am. J. Physiol. Heart Circ. Physiol. 2000, 278, H2039–H2049. [Google Scholar] [CrossRef] [PubMed]
| Parameters | Group 1 (n = 22) | Group 2 (n = 34) | Group 3 (n = 34) |
|---|---|---|---|
| Male/Female | 13/9 | 10/24 | 22/12 |
| Age (years) | 28.68 ± 6.34 | 56.21 ± 10.72 ** | 60.71 ± 8.46 |
| Body weight (kg) | 68.27 ± 15.89 | 61.73 ± 10.55 | 73.88 ± 14.86 †† |
| WC(cm) | 82.30 ± 13.53 | 80.79 ± 9.43 | 95.00 ± 11.56 †† |
| BMI (kg/m2) | 23.60 ± 4.48 | 23.72 ± 3.54 | 27.92 ± 4.70 †† |
| SBP (mmHg) | 117.46 ± 10.94 | 118.97 ± 16.60 | 127.38 ± 17.14 †† |
| DBP (mmHg) | 73.91 ± 7.02 | 72.97 ± 9.03 | 76.06 ± 10.16 |
| PP (mmHg) | 43.55 ± 7.65 | 46.00 ± 11.12 | 51.32 ± 13.84 |
| HDL (mg/dL) | 46.46 ± 15.34 | 55.27 ± 19.34 | 40.21 ± 13.13 †† |
| LDL (mg/dL) | 124.86 ± 41.11 | 157.88 ± 43.48 * | 148.62 ± 47.39 |
| Cholesterol (mg/dL) | 174.64 ± 56.33 | 165.44 ± 94.19 | 154.94 ± 53.51 |
| Triglyceride (mg/dL) | 79.64 ± 36.31 | 102.03 ± 30.99 * | 117.59 ± 45.06 † |
| HbA1c(%) | 5.51 ± 0.34 | 5.87 ± 0.40 ** | 8.14 ± 1.27 †† |
| PWVfinger(m/sec) | 4.48 ± 0.87 | 4.88 ± 0.49 | 5.93 ± 0.58 † |
| Parameters | Group 1 (n = 22) | Group 2 (n = 34) | Group 3 (n = 34) |
|---|---|---|---|
| MEISS(CT) | 0.65 ± 0.13 | 0.65 ± 0.12 | 0.65 ± 0.13 |
| MEILS(CT) | 0.49 ± 0.07 | 0.47 ± 0.06 | 0.44 ± 0.08 |
| MEISS(RRI) | 0.64 ± 0.08 | 0.58 ± 0.11 * | 0.51 ± 0.17 |
| MEILS(RRI) | 0.54 ± 0.06 | 0.52 ± 0.07 | 0.44 ± 0.11 †† |
| MCEISS(RRI,CT) | 0.70 ± 0.11 | 0.64 ± 0.10 | 0.63 ± 0.12 |
| MCEILS(RRI,CT) | 0.55 ± 0.06 | 0.51 ± 0.06 | 0.46 ± 0.08 † |
| MEISS(CT) | MEILS(CT) | MEISS(RRI) | MEILS(RRI) | MCEISS | MCEILS | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| p | r | p | r | p | r | p | r | p | r | p | r | |
| Age (years) | 0.736 | 0.046 | 0.649 | −0.062 | 0.102 | −0.221 | 0.385 | −0.118 | 0.408 | −0.113 | 0.125 | −0.207 |
| BH (cm) | 0.254 | −0.155 | 0.265 | −0.151 | 0.819 | −0.031 | 0.227 | −0.164 | 0.537 | 0.084 | 0.491 | −0.094 |
| BW (kg) | 0.081 | −0.236 | 0.996 | 0.001 | 0.152 | −0.194 | 0.327 | −0.134 | 0.921 | −0.014 | 0.771 | −0.040 |
| WC (cm) | 0.064 | −0.250 | 0.974 | −0.005 | 0.180 | −0.182 | 0.301 | −0.141 | 0.584 | −0.075 | 0.506 | −0.091 |
| BMI (kg/m2) | 0.161 | −0.190 | 0.362 | 0.124 | 0.074 | −0.241 | 0.705 | −0.052 | 0.449 | −0.103 | 0.874 | 0.022 |
| SBP (mmHg) | 0.209 | 0.171 | 0.259 | 0.153 | 0.398 | 0.115 | 0.332 | 0.132 | 0.113 | 0.214 | 0.107 | 0.218 |
| DBP (mmHg) | 0.742 | 0.045 | 0.183 | 0.181 | 0.740 | 0.045 | 0.877 | −0.021 | 0.533 | 0.085 | 0.525 | 0.087 |
| PP (mmHg) | 0.115 | 0.213 | 0.584 | 0.075 | 0.334 | 0.131 | 0.117 | 0.212 | 0.070 | 0.244 | 0.065 | 0.248 |
| HDL (mg/dL) | 0.802 | 0.034 | 0.254 | −0.153 | 0.819 | −0.031 | 0.915 | −0.015 | 0.418 | −0.110 | 0.254 | −0.155 |
| LDL (mg/dL) | 0.515 | 0.089 | 0.590 | −0.074 | 0.051 | −0.263 | 0.239 | −0.160 | 0.927 | −0.012 | 0.259 | −0.153 |
| Cholesterol (mg/dL) | 0.403 | −0.114 | 0.740 | −0.045 | 0.067 | −0.247 | 0.003* | −0.394 | 0.058 | −0.255 | 0.020 | −0.311 |
| Triglyceride (mg/dL) | 0.958 | −0.007 | 0.857 | 0.025 | 0.681 | −0.056 | 0.365 | −0.123 | 0.910 | 0.016 | 0.451 | −0.103 |
| HbA1c (%) | 0.332 | 0.132 | 0.947 | 0.009 | 0.226 | −0.164 | 0.911 | 0.015 | 0.958 | 0.007 | 0.641 | 0.064 |
| FBS (mg/dL) | 0.626 | 0.066 | 0.606 | 0.070 | 0.683 | 0.056 | 0.315 | −0.137 | 0.759 | −0.042 | 0.451 | −0.103 |
| MEISS(CT) | MEILS(CT) | MEISS(RRI) | MEILS(RRI) | MCEISS | MCEILS | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| p | r | p | r | p | r | p | r | p | r | p | r | |
| Age (years) | 0.409 | 0.102 | 0.778 | −0.035 | 0.395 | −0.105 | 0.029 | −0.264 | 0.725 | 0.043 | 0.272 | −0.135 |
| BH (cm) | 0.079 | −0.214 | 0.248 | −0.142 | 0.656 | −0.055 | 0.793 | −0.032 | 0.070 | −0.221 | 0.222 | −0.150 |
| BW (kg) | 0.044 | −0.245 | 0.040 | −0.250 | 0.086 | −0.210 | 0.057 | −0.232 | 0.032 | −0.260 | 0.017 * | −0.288 |
| WC (cm) | 0.031 | −0.262 | 0.009 * | −0.314 | 0.063 | −0.227 | 0.014 * | −0.298 | 0.042 | −0.248 | 0.004 * | −0.343 |
| BMI (kg/m2) | 0.190 | −0.161 | 0.105 | −0.198 | 0.067 | −0.223 | 0.043 | −0.246 | 0.139 | −0.181 | 0.047 | −0.242 |
| SBP (mmHg) | 0.136 | 0.183 | 0.580 | 0.068 | 0.729 | 0.043 | 0.416 | −0.100 | 0.165 | 0.170 | 0.875 | 0.019 |
| DBP (mmHg) | 0.757 | −0.038 | 0.924 | 0.012 | 0.213 | −0.153 | 0.116 | −0.192 | 0.540 | −0.076 | 0.697 | −0.048 |
| PP (mmHg) | 0.022 | 0.276 | 0.498 | 0.084 | 0.156 | 0.174 | 0.936 | 0.010 | 0.017 * | 0.288 | 0.611 | 0.063 |
| HDL (mg/dL) | 0.923 | 0.012 | 0.267 | 0.136 | 0.400 | 0.104 | 0.067 | 0.224 | 0.636 | 0.058 | 0.077 | 0.216 |
| LDL (mg/dL) | 0.555 | 0.073 | 0.833 | 0.026 | 0.187 | −0.162 | 0.829 | −0.027 | 0.869 | 0.020 | 0.482 | 0.087 |
| Cholesterol (mg/dL) | 0.464 | −0.090 | 0.905 | 0.015 | 0.179 | −0.165 | 0.087 | −0.209 | 0.263 | −0.138 | 0.259 | −0.142 |
| Triglyceride (mg/dL) | 0.671 | 0.052 | 0.434 | 0.096 | 0.762 | 0.037 | 0.760 | 0.038 | 0.531 | 0.077 | 0.383 | 0.107 |
| HbA1c (%) | 0.808 | 0.030 | 0.102 | −0.200 | 0.225 | −0.149 | 0.015 * | -0.294 | 0.875 | 0.020 | 0.077 | −0.216 |
| FBS (mg/dL) | 0.778 | 0.035 | 0.092 | −0.206 | 0.148 | −0.177 | 0.005 * | -0.335 | 0.955 | 0.007 | 0.043 | −0.246 |
| MEISS(CT) | MEILS(CT) | MEISS(RRI) | MEILS(RRI) | MCEISS | MCEILS | ||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| p | r | p | r | p | r | p | r | p | r | r | |
| Age (years) | 0.779 | 0.030 | 0.097 | −0.176 | 0.003 * | −0.310 | 0.001 * | −0.332 | 0.135 | −0.159 | −0.334 |
| BH (cm) | 0.037 | −0.221 | 0.272 | −0.117 | 0.838 | 0.022 | 0.743 | 0.035 | 0.696 | −0.042 | −0.013 |
| BW (kg) | 0.006* | −0.286 | 0.053 | −0.204 | 0.040 | −0.217 | 0.046 | −0.211 | 0.089 | −0.180 | −0.237 |
| WC (cm) | 0.008 * | −0.280 | 0.012 * | −0.263 | 0.007 * | −0.284 | 0.004 * | −0.300 | 0.038 | −0.219 | −0.327 |
| BMI (kg/m2) | 0.065 | −0.195 | 0.137 | −0.158 | 0.008 * | −0.276 | 0.010 * | −0.269 | 0.073 | −0.190 | −0.261 |
| SBP (mmHg) | 0.343 | 0.101 | 0.894 | 0.014 | 0.744 | −0.035 | 0.309 | −0.108 | 0.368 | 0.096 | −0.016 |
| DBP (mmHg) | 0.728 | −0.037 | 0.907 | 0.013 | 0.143 | −0.156 | 0.078 | −0.187 | 0.538 | −0.066 | −0.073 |
| PP (mmHg) | 0.119 | 0.165 | 0.927 | 0.010 | 0.504 | 0.071 | 0.966 | −0.005 | 0.089 | 0.180 | 0.034 |
| HDL (mg/dL) | 0.653 | 0.048 | 0.247 | 0.123 | 0.340 | 0.102 | 0.044 | 0.213 | 0.963 | 0.005 | 0.172 |
| LDL (mg/dL) | 0.555 | 0.063 | 0.449 | −0.081 | 0.043 | −0.213 | 0.229 | −0.128 | 0.895 | −0.014 | −0.074 |
| Cholesterol (mg/dL) | 0.495 | −0.073 | 0.897 | −0.014 | 0.316 | −0.107 | 0.114 | −0.168 | 0.241 | −0.125 | −0.139 |
| Triglyceride (mg/dL) | 0.815 | 0.025 | 0.983 | −0.002 | 0.467 | −0.078 | 0.333 | −0.103 | 0.885 | 0.015 | −0.053 |
| HbA1c (%) | 0.842 | 0.021 | 0.013 * | −0.261 | 0.013 * | −0.261 | 0.001 ** | −0.354 | 0.430 | −0.084 | −0.306 |
| FBS (mg/dL) | 0.846 | 0.021 | 0.023 | −0.239 | 0.012 * | −0.263 | <0.001 ** | −0.384 | 0.391 | −0.091 | −0.322 |
| MEILS(CT) | MEILS(RRI) | MCEILS(RRI,CT) | |||||||
|---|---|---|---|---|---|---|---|---|---|
| B-Coef | SE | p | B-Coef | SE | p | B-Coef | SE | p | |
| Variable | |||||||||
| Age (year) | 0.000 | 0.001 | 0.569 | −0.001 | 0.001 | 0.040 | −0.001 | 0.001 | 0.022 |
| HbA1c(%) | −0.012 | 0.006 | 0.041 | −0.018 | 0.007 | 0.012 | −0.012 | 0.006 | 0.041 |
| B0 | 0.563 | 0.039 | <0.001 | 0.686 | 0.046 | <0.001 | 0.644 | 0.036 | <0.001 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Xiao, M.-X.; Wei, H.-C.; Xu, Y.-J.; Wu, H.-T.; Sun, C.-K. Combination of R-R Interval and Crest Time in Assessing Complexity Using Multiscale Cross-Approximate Entropy in Normal and Diabetic Subjects. Entropy 2018, 20, 497. https://doi.org/10.3390/e20070497
Xiao M-X, Wei H-C, Xu Y-J, Wu H-T, Sun C-K. Combination of R-R Interval and Crest Time in Assessing Complexity Using Multiscale Cross-Approximate Entropy in Normal and Diabetic Subjects. Entropy. 2018; 20(7):497. https://doi.org/10.3390/e20070497
Chicago/Turabian StyleXiao, Ming-Xia, Hai-Cheng Wei, Ya-Jie Xu, Hsien-Tsai Wu, and Cheuk-Kwan Sun. 2018. "Combination of R-R Interval and Crest Time in Assessing Complexity Using Multiscale Cross-Approximate Entropy in Normal and Diabetic Subjects" Entropy 20, no. 7: 497. https://doi.org/10.3390/e20070497
APA StyleXiao, M.-X., Wei, H.-C., Xu, Y.-J., Wu, H.-T., & Sun, C.-K. (2018). Combination of R-R Interval and Crest Time in Assessing Complexity Using Multiscale Cross-Approximate Entropy in Normal and Diabetic Subjects. Entropy, 20(7), 497. https://doi.org/10.3390/e20070497







