Abstract
Bodybuilders routinely engage in many dietary and other practices purported to be harmful to kidney health. The development of acute kidney injury, focal segmental glomerular sclerosis (FSGS) and nephrocalcinosis may be particular risks. There is little evidence that high-protein diets and moderate creatine supplementation pose risks to individuals with normal kidney function though long-term high protein intake in those with underlying impairment of kidney function is inadvisable. The links between anabolic androgenic steroid use and FSGS are stronger, and there are undoubted dangers of nephrocalcinosis in those taking high doses of vitamins A, D and E. Dehydrating practices, including diuretic misuse, and NSAID use also carry potential risks. It is difficult to predict the effects of multiple practices carried out in concert. Investigations into subclinical kidney damage associated with these practices have rarely been undertaken. Future research is warranted to identify the clinical and subclinical harm associated with individual practices and combinations to enable appropriate and timely advice.
1. Introduction
Bodybuilding, or “the use of progressive resistance exercise to develop muscle building by hypertrophy”, has become increasingly popular both recreationally and competitively [1]. Unlike other sports, bodybuilding success is judged on appearances of muscular definition and symmetry rather than athletic ability [2]. Resistance training, including non-competitive-style training, is recommended for both athletes and the general population to improve physical performance, appearance, strength, rehabilitation, health, and aid in weight management [3,4]. Competitive bodybuilding pushes the limits of resistance training adaptations and requires dedication to rigorous training and strict dietary regimes [1,5]. Over 95% of bodybuilders use dietary supplements [6], with the two most common being creatine monohydrate and protein [5,6]. Non-nutritional, performance-enhancing drugs, such as veterinary-grade vitamin supplementation, often in alarming quantities, and/or anabolic–androgenic steroids (AAS) are also used [6,7,8]. Most of the extreme nutritional, drug and training strategies used in bodybuilding are derived from non-evidence-based sources [1,2,5], giving rise to increasing concerns about their potential adverse health impact [9]. Adverse renal effects include increased risks of acute kidney injury (AKI) and a number of conditions that may lead to chronic kidney disease (CKD) [8,10,11]. In this review, we will explore links between dietary and non-nutritional supplementation strategies observed in bodybuilders and their impact on kidney function, injury and disease.
2. Materials and Methods
Google Scholar, PubMed and ScienceDirect were accessed to conduct an online literature search. Although this review is narrative in design, the search strategy and parameters closely followed the PRISMA statement guidelines [12], to promote and focus the findings to a high quality, ensuring scientific and accurate discussion of areas of importance. As such, the key search terms and phrases used were formed from a combination of the following: ‘bodybuilding’, ‘nutrition’, ‘protein’, ‘creatine’, ‘supplements’, ‘anabolic-androgenic steroids’, ‘kidney function’, ‘acute kidney injury’ and ‘chronic kidney injury’. The search method is outlined in Figure 1, where firstly duplicates were removed, and then the title and abstracts were screened for relevance and significance. Additionally, papers were excluded if access to full texts was denied, published by a non-peer-reviewed journal, and if published prior to 2000, to ensure that only the most relevant and up-to-date literature and results are included. To further ensure that the papers reviewed were significant, the compiled full texts were only included if the inclusion criteria were met, namely, concerning a bodybuilding population, measurements of renal function and subsequent assessment of renal dysfunction or injury if applicable. The search resulted in 13 significant full-text articles discussed throughout this review. The reference lists of these key articles were scanned, and additional articles of interest not found by the electronic database search were included or discussed throughout the review.
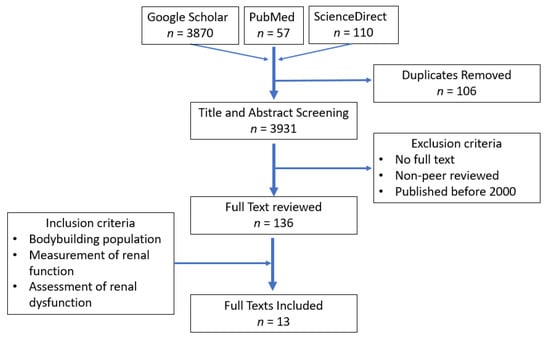
Figure 1.
Flow diagram describing the search methodology used to obtain the research studies for this review.
3. Results
Thirteen studies published since 2000 described kidney disease in 75 bodybuilders (Table 1; the full details of the renal conditions and dietary and supplementary practices can be seen in Supplementary Tables S1 and S2). Most studies (eight) were case reports and the remainder case series. A range of kidney conditions were involved. There were 25 cases of acute kidney injury (AKI)/acute tubular necrosis (ATN), 20 had focal segmental glomerular sclerosis (FSGS) and 10 nephrocalcinosis. Other conditions reported were acute interstitial nephritis (AIN) (5 cases), nephrosclerosis (5 cases), chronic interstitial nephritis (3 cases) and an assortment of other glomerulonephritides (7 cases). Each condition was usually associated with multiple bodybuilding practices, nutritional and non-nutritional, which will be outlined in the following sections.

Table 1.
Overview of Kidney disease and dietary and supplement history in 13 studies of Bodybuilders.
4. Discussion
4.1. Measurement of Kidney Function
Estimation of kidney function in clinical practice is based largely on measurements of serum creatinine. Creatinine is the end-product of creatine and creatine phosphate metabolism. Creatine is generated predominantly in the kidney and liver from glycine, arginine and methionine, and transported to other tissues, particularly skeletal and heart muscles, where it undergoes phosphorylation by creatine kinase to creatine phosphate [13]. Creatine phosphate provides a readily available source of energy, particularly during the early phases of intense muscular contraction. Creatinine is produced by non-enzymatic anhydration of creatine within muscle [14]. Skeletal muscle has the highest concentration of creatine and creatine phosphate (~95%) and is thus the primary source of creatinine generation [14,15], although high-protein diets—particularly those containing cooked meats—are another source of creatinine. The kidney is the main route for creatinine elimination, though there may also be low-level gastrointestinal removal. Creatinine is freely filtered by the glomerulus but also undergoes tubular secretion, the rates of which can be unpredictable and influenced by many drugs, including cimetidine and trimethoprim [14,15]. Figure 2 illustrates the main determinants of serum creatinine.
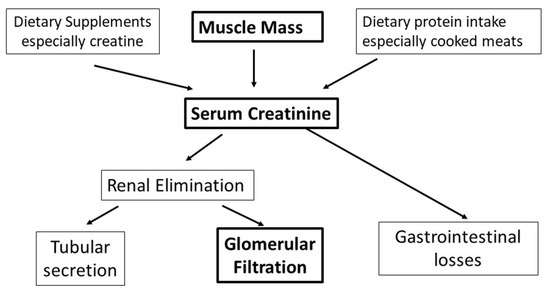
Figure 2.
Determinants of serum creatinine.
Hence serum creatinine values, though key measures of kidney function, must be interpreted with reference to muscle mass. Measurement of creatinine clearance is a more reliable indicator of the glomerular filtration rate (GFR), though it overestimates the gold standard inulin clearance by around 10% [14]. It also involves lengthy, timed urine collections, the impracticability of which in routine practice has favoured the use of estimates of GFR (eGFR) based on empirical modifications of serum creatinine. The simplest equation also involves functions of age, sex and ethnicity to help correct for creatinine generation [16].
Utilising cystatin C could prove to be a more reliable and accurate measure of kidney function. It has fewer non-GFR determinants, and, in particular, is related to neither muscle mass nor diet, as is serum creatinine [17]. However, it has been reported to be increased in the presence of anabolic androgen steroid (AAA) use [18]. Hence, both serum creatinine and cystatin C present issues in the quest for accurate assessment of kidney function in the bodybuilding population. It has been recommended, though, that for individuals with extremes of muscle mass or diet, cystatin C should be measured and eGFR reported as eGFRcr-cys, or that GFR should be measured directly using a clearance procedure [19]. Likewise, for the assessment of albuminuria in patients with extremes of muscle mass or diet, measurement of the albumin:creatinine ratio should be supplemented by the albumin excretion rate measured from a timed urine collection [19]. Few studies of kidney health in bodybuilders have met these criteria. Other promising biomarkers of kidney health may allow detection of early damage (such as plasma NGAL and urinary KIM-1 for risk of developing AKI), localisation of injury and prediction of disease progression [20]. Their use in bodybuilding studies is rare.
4.2. Protein Supplementation
UK government guidelines recommend protein intakes of 0.75–0.8 g/kg/day [21]. This is increased up to 1.4–2.0 g/kg/day for athletes [22]. This is safe, aids training adaptations and optimises building and maintenance of muscle mass [22]. Protein is essential for muscle anabolism. Higher intakes can be beneficial for strength and power athletes, including bodybuilders [23]. Use of high-protein diets is widespread in bodybuilders presenting with kidney dysfunction [7,24,25,26,27,28] (Table 1). Hartung reported a protein intake of 2 g/kg/day in a bodybuilder presenting with end-stage kidney disease due to FSGS [27]. Herlitz found that 8 of 10 bodybuilders consumed high-protein diets (2.8–5.1 g/kg/day) [28], and nine had FSGS. Almukhtar found that four bodybuilders with AKI had a total protein intake of 3.2–4.2 g/kg/day [25]. The protein intake of 22 bodybuilders with a range of kidney conditions (Table 1) was reported as an incredible 20–30 g/kg/day [26]. All these intakes are equal to or greater than the highest intake recommended for sports participation. In none of these studies was high protein intake thought to be the dominant contributor to kidney dysfunction. In most cases multiple other behaviours were also implicated.
Other studies have found no detrimental effects of isolated high-protein diets, albeit consumed for relatively brief periods [29,30]. In five healthy resistance-trained men, taking 2.5 ± 1.0 to 3.5 ± 1.4 g/kg/day for 2 years, there was no significant effect on kidney function [29]. Similarly, in a randomised crossover study in 14 resistance-trained men consuming 2.51–3.32 g/kg/day for one year, no harmful renal effects were observed [30]. In both studies the only parameters reported relating to kidney function were serum creatinine, blood urea nitrogen and eGFR.
There is evidence that high-protein diets can cause issues for those with pre-existing kidney insufficiency [31]. Dietary protein is a key physiological modulator of renal function. High-protein diets can cause glomerular hyperfiltration and increase the intraglomerular pressure, potentially leading to structural damage [32]. Acute haemodynamic effects of high protein intake can be seen in the short term in healthy individuals [33]. In longer-term epidemiological studies, higher levels of protein intake are associated with a more rapid decline in kidney function [34]. A strong case has been made for lower protein intakes in patients with CKD [35].
Bodybuilders generally employ different nutritional strategies [36] during specific phases of training, such as bulking (calorie excess to increase muscle mass) or cutting (pre-competition calorie reduction to reduce body fat and increase muscle definition) [1,37]. Although carbohydrates are the main macronutrient manipulated in the week(s) prior to competition, high protein consumption is maintained [36]. Bodybuilders observed by Gentil [37] increased their daily protein intake from 2.5 g/kg/day during bulking to ~3.0 g/kg/day when cutting. In contrast, Maestu found that baseline protein intake was slightly reduced from 2.68 g/kg/day to 2.48 g/kg/day 3 days prior to competition [38]. Similarly, Lenzi found that 4.16 ± 1.28 g/kg/day of protein was ingested when bulking, reducing to 3.56 ± 1.43 g/kg/day during cutting [1]. None of the studies detailing the protein intake of bodybuilders in relation to kidney dysfunction [7,24,25,26,27,28] stated the training phase of the individuals involved. Multiple assessments of intake during different training phases will be necessary to establish the precise levels of intake and define any risks involved.
Overall, there is little direct evidence that high-protein diets contribute to an increased risk of kidney dysfunction in healthy bodybuilders. In the cases of FSGS reported, concomitant use of other potentially culprit practices were the norm. Risks are likely higher in those with pre-existing kidney impairment. However, the evidence base is poor, and further research necessary.
4.3. Creatine Supplementation
Dietary sources of creatine include fish, meat and dairy products, which contribute to an intake of 1–2 g/day. Creatine can also be synthesized endogenously in the kidney and liver [13]. Creatine supplementation has become increasingly popular in athletes of all levels, due to its perceived performance-enhancing properties, such as increasing lean muscle mass and strength, improved post-exercise recovery and injury prevention [39]. It is one of the most commonly used non-hormonal supplements in bodybuilders [40]. Typically, four equal doses (4 × 5 g) are ingested daily (~0.3 g/kg/day or 20 g/day) for 5–7 days to load muscles with creatine. Following this, 3–5 g/day is used as maintenance. This dosing strategy has been shown to augment resistance-training gains [39]. Seven studies have identified creatine use in bodybuilders with renal dysfunction, although only five outlined specific dosing strategies (Table 1). Maintenance doses consumed were variable with respect to those recommended [25,41,42,43]. In an extreme case it was reported that the individual consumed 210 g/day, which is 22 times greater than the recommended maintenance dose [26]. Again, creatine supplementation was rarely used in isolation. Only one study [41] specifically stated denial of use of AAS, NSAIDS and diuretics, while two studies did not mention any other bodybuilding practices, such as nutritional intake or use of other agents [42,43]. The kidney conditions most frequently associated with creatine supplementation in bodybuilders are acute interstitial nephritis (AIN) and acute tubular necrosis (ATN), which have occurred in individuals consuming relatively low doses [42,43]. It is possible that other agents were also being consumed—though none were reported—or that excipients in the creatine preparations were the real culprits. In keeping with these possibilities, prolonged use of high maintenance doses of 9.7 ± 5.7 g/day for up to four years has been shown to have no apparent detrimental effects [44]. Similarly, creatine supplementation together with a high protein intake (1.2–3.1 g/kg/day) and resistance training had no apparent effect on creatinine clearance and albuminuria [45].
Within tissues or solutions, creatine is gradually and irreversibly converted to creatinine, which is filtered by the kidneys and excreted via urine [46]. However, creatine can also be converted into sarcosine, resulting in the production of methylamine, and via subsequent deamination, the formation of formaldehyde, which is potentially cytotoxic [47]. Creatine supplementation (21 g/day for 14 days) significantly increased the serum levels of methylamine [46] and formaldehyde [48], although both remained within the upper limits of normal [49]. Furthermore, Candow and colleagues examined the effect of a relative low dose of creatine (0.1 g/kg) taken on resistance-training days (3 times/week for 10 weeks) versus the placebo, in older healthy men [50]. There were no significant changes over time, and no group differences, in urinary formaldehyde excretion.
Creatine homeostasis is dependent on dietary creatine intake in conjunction with endogenous creatine production to offset creatine degradation (1.6–1.7% of the total creatine pool is degraded daily). The capacity of renal arginine:glycine amidinotransferase (AGAT), a key enzyme involved in creatine synthesis, is progressively decreased with progression of CKD and is virtually absent in dialysis patients [51]. Furthermore, plant-based foods are increasingly recommended for individuals with kidney dysfunction since they contain smaller amounts of saturated fatty acids, protein and absorbable phosphorus. They also generate less acid and are richer in fibre than meat. It has been suggested that loss of endogenous synthesis capabilities and reduced consumption of creatine rich foods can result in creatine deficiency. Creatine deficiency is associated with clinical manifestations similar to sarcopenia, with fatigue, impaired quality of life and impaired cognition [51]. Future research should examine the impact of creatine-rich foods or creatine supplementation on individuals with CKD. Overall, evidence that creatine supplementation increases the risk of developing kidney damage in bodybuilders is inconclusive. Further research is necessary to ascertain whether creatine supplementation is a true cause for concern.
4.4. Anabolic Androgenic Steroids
Anabolic androgenic steroids (AAS) are used by professional athletes such as bodybuilders and powerlifters to enhance performance, increase muscle mass and decrease body fat [9]. Their use has become increasingly common in bodybuilding and amongst non-competitive athletes seeking an increased muscular appearance [10,26,52]. Illicit use by recreational sportspeople has overtaken that for athletic use (overall prevalence reported as, respectively, 18.4% and 13.4%) [53]. However, ascertaining the true prevalence is challenging since these agents are often taken secretly and research using anonymised questionnaires can only provide a very approximate insight [9,28,52]. There has been an alarming increase in AAS popularity worldwide. The global lifetime prevalence in 2014 was reported as 3.3%, though there were wide regional variations, the highest being in the Middle east (21.7%) followed by South America, (4.8%) and Europe (3.8%) [53]. Use of AAS has been deemed to pose a significant public health issue [9,54]. All major sports organisations have banned their use [9,26].
A recent study assessed the use of performance-enhancing drugs, mainly AAS, in bodybuilders. Current users had a higher prevalence of AKI than previous users and non-users, suggesting that individuals using these agents may be at an increased risk of kidney failure [10]. However, though use of AAS has been associated with a range of kidney conditions, including AKI, AIN, FSGS and nephrosclerosis, in all cases other bodybuilding practices were also being followed (Table). Of the 13 articles relating to bodybuilding (Table 1), three did not specify whether AAS were used [42,43,55] and in only two was their use denied [41,56]. The remaining eight confirmed a positive history of AAS use, although only four detailed specific quantities, type and duration of usage (Table 1). The training phase may also affect the AAS strategy employed [37].
An Endocrine Society scientific statement has warned that the use of AAS as performance-enhancing agents can lead to the development of significant complications, including FSGS, though cardiovascular risks outweigh those to the kidney [40,52]. FSGS may require a longer exposure to manifest [26], though subclinical kidney injury may occur earlier [18].
AAS have the potential to affect multiple pathways linked to kidney injury though evidence is largely limited to data from animal studies [40,57]. Androgens stimulate the renin–angiotensin–aldosterone system (RAAS), resulting in increased blood pressure and increased water retention via tubular reabsorption of salt and water [58]. Increased production of endothelin can result in both afferent and efferent vasoconstriction and increased mitogenic activity [57,59]. Increased RAAS activity and endothelin can also increase oxidative stress via NADPH oxidase [57]. Androgens can also promote apoptosis within the renal tubular cells by activating the caspase-dependent apoptotic pathway, contributing to the development of kidney fibrosis [60]. Testosterone has also been implicated in the production of pro-inflammatory cytokines, such as interleukin-1b, tumour necrosis factor α and interleukin-6, which can accelerate the progression of CKD [61,62].
The threat posed by AAS use to kidney health, as outlined in Figure 3, is better substantiated than protein and creatine supplementation, though again complicated by co-existent potentially harmful practices.
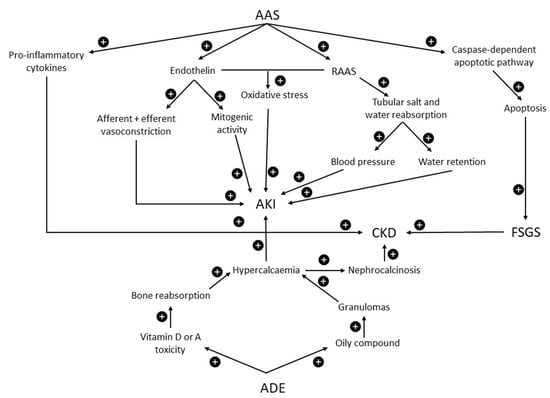
Figure 3.
Possible mechanisms and pathophysiology of kidney injury due to exposure to AAS and intramuscular vitamins A, D and E. ADE = intramuscular vitamins A, D and E. AAS = anabolic androgenic steroids. RAAS = renin–angiotensin–aldosterone system. FSGS = focal segmental glomerulosclerosis. CKD = chronic kidney disease. AKI = acute kidney injury. + = increased effect.
4.5. Vitamins
Vitamins are essential micronutrients with variable quantities required throughout a lifetime to support numerous physiological functions necessary for maintaining health. Vitamins, such as A and D, in large quantities can accumulate within the body, potentially resulting in hypervitaminosis [63]. Bodybuilders are known to inject high doses of vitamins A, D and E contained within an oily substance known as compound ‘ADE’, the consumption of which is damaging to human health and kidney function [54,64]. The first reported use of compound ‘ADE’ in humans was in Brazil in the late 1980s, though this practice may well have been in use sometime earlier [64]. Compound ‘ADE’ was originally used by veterinary professionals to treat cattle and horses experiencing vitamin deficiency and infections, in quantities not exceeding 5 mL per 120-day fattening period for cattle. Bodybuilders often exceed this [11]. The main reason that compound ‘ADE’ is used by bodybuilders is not for the vitamins per se but the oily carrier, which when injected into muscle produces a foreign body reaction and a local false hypertrophy [55], increasing the volume of the muscle through local fluid retention rather than muscle anabolism [64].
Of the six studies that report kidney conditions in relation to vitamin usage, four specifically outline the quantity, dosage and duration of use (Table 1). The quantities of ‘ADE’ that the bodybuilder used were far greater than those recommended for cattle. The resulting kidney pathologies ranged from the more common hypercalcaemia and secondary AKI, which after discontinuation of vitamin supplementation resulted in near complete renal recovery [7,56,64,65], to the development of nephrocalcinosis and CKD [7,55,64]. Abundant deposits of calcium phosphate can occur within the tubulointerstitium, often associated with irreversible interstitial fibrosis and tubular atrophy [11,64].
The development of vitamin D toxicity resulting in hypercalcaemia necessitates significantly increased intakes of 20,000–30,000 IU per day [66,67]. The bodybuilder’s vitamin D intake reported by Rocha (Table 1) was higher, at ~40,000 IU/day, resulting in a 25(OH)D level of 150 ng/mL, somewhat less than previously reported levels associated with vitamin D toxicity of ≥200 mng/mL [66,67]. Hence, it was proposed that vitamin A intoxication was the factor posing the greater influence on the hypercalcaemia and AKI presented by this particular patient [56]. Vitamin A intoxication is rare but known to cause hypercalcaemia by increasing osteoclast-mediated bone resorption [68,69]. However, in the case described by Ronsoni (suS2), the vitamin A levels were elevated but still within the upper limit of normal [65]. So, the vitamins within compound ‘ADE’ may not be the only factors responsible for hypercalcaemia. The use of cosmetic injections consisting of silicone, paraffin and polymethyl methacrylate have been associated with the development of hypercalcaemia [11,55,70]. These agents support the formation of granulomas that increase the 1-α-hydroxylase activity, thus promoting formation of 1,25-OH-D. The reduction in calcium levels in response to glucocorticoids provides some evidence to support this mechanism [68]. Nevertheless, there is strong evidence that use of compound ADE can cause hypercalcaemia, AKI and nephrocalcinosis, as displayed in Figure 3.
4.6. Non-Steroidal Anti-Inflammatory Drugs (NSAID)
NSAIDs are easily accessible, and their use is highly prevalent, accounting for around 5% of prescribed treatments worldwide [71]. NSAIDS are popular in sports medicine [71,72], with a self-reported prevalence of up to 50% among athletes [73]. They can counteract muscle inflammation, pain and soreness during, and in response to, exercise [74,75], and thus improve performance by increasing pain tolerances and delaying fatigue [75,76]. However, using high-dose NSAIDs has been shown to compromise training adaptations, reducing increments in muscle strength and hypertrophic gains from resistance exercise [72,77], thus potentially reducing performance. Regular high-dose NSAID administration significantly increases risks, in particular predisposing to the development of AKI and accelerating the progression of CKD [78]. In only three studies [28,41,56] (Table S2) was the use of NSAID specifically denied. The remaining studies did not report this practice (Table 1). Use of NSAIDS is likely to be an underappreciated factor in reports of kidney damage in bodybuilders.
4.7. Dehydration and Diuretics
The final days before bodybuilding competitions has been coined ‘peak week’ [36], during which the majority of competitors were found to implement strategies to maximise their physical appearance for aesthetic purposes [79,80]. These strategies often include altered exercise regimes; macronutrient, water and electrolyte intakes to enhance muscle glycogen content; minimising subcutaneous water; minimising abdominal bloating; and optimising muscle definition [36]. While natural methods can be used to achieve these objectives, bodybuilders often self-prescribe potentially harmful dosages of drugs, such as diuretics and insulin [36], which have resulted in dangerous outcomes, such as hypokalaemic paralysis [81]. Many bodybuilders acknowledge that these strategies pose increased health risks, but the measures are perceived as necessary and temporary [36]. The majority of strategies involve dehydration and sodium depletion in the final days before competition [79,80,82], which have been linked to increased risk of kidney dysfunction [83,84]. Only three of the studies (Table S2) specifically established a negative history of diuretic use [28,41,56]. Such practices may well pose a risk to kidney function, particularly in hot climates [25].
4.8. Other Supplements/Stimulants and Exertional Rhabdomyolysis
There are many other dietary supplements (DS) easily available to the general population [85] that were not found/highlighted within the scope of the literature search of this review, although they should not be dismissed. One DS of interest used by bodybuilders is “Hydroxycut”, a weight-loss and muscle-building product, comprising of Garcinia cambogia, Cissus quadrangularis, caffeine, Ma Huang (ephedra) and green tea in various quantities over the years of its production [86]. Caffeine is also considered the most popular pre-workout stimulant for bodybuilders, whereby improvements in strength performance requires large supplementation of ~5–6 mg/kg [2,87,88] at the upper range of the safe caffeine dosage of ~6 mg/kg [89]. Chappell et al. (2018) found that bodybuilders consume large amounts of energy and hot drinks, resulting in several bodybuilders exceeding the recommended safe dosage of caffeine [90]. Both consuming “Hydroxycut” [91,92] and caffeine [93,94,95] have been linked to the development of rhabdomyolysis. Therefore, bodybuilders practicing strenuous exercise while also taking these supplements/stimulants could be at increased risk of exertional rhabdomyolysis [96,97]. This is significant, as exertional rhabdomyolysis may also lead to the development of acute renal failure and multiple other organ dysfunctions [98,99]. Exertional rhabdomyolysis is a pathophysiological condition where musculoskeletal cell damage occurs due to intense or excessive exercise indicated by increased creatine kinase or myoglobin levels entering the blood via damaged cell membranes [100]. Myoglobin is said to be the main culprit of renal injury due to rhabdomyolysis, as it is excreted by the kidneys causing urine to be stained red or brown [101]. Although the exact mechanism of the myoglobins’ role in renal dysfunction and subsequent injury is uncertain, some evidence suggests that vasoconstriction of intrarenal blood vessels, direct oxidant and ischemic tubule injury and obstruction of tubular tissues may all be impacted, leading to acidic urine, renal obstruction and eventually acute renal failure if left untreated [101,102]. The three main signs and symptoms of exertional rhabdomyolysis are muscle aches, weakness and dark urine, and can often be overlooked as exercise-induced delayed-onset muscle soreness (DOMS) [99,102]. Bodybuilders should be informed of the risk of rhabdomyolysis and its repercussions on renal function if left untreated.
4.9. Practical Applications
The findings of this review bring certain bodybuilding practices to attention that should be monitored by athletes and coaches, as well as identified by medical professionals. Athletes with knowledge should make coaches aware of pre-existing renal deficiencies to advise their recommendations of nutritional and non-nutritional strategies. Increasing the occurrence of baseline and regular testing could provide more accurate measures of initial kidney function of athletes and can be used to identify previous unknown underlying conditions or significant changes during differing training phases, which could increase the risk of renal decline. The common and consistent concurrent use of multiple practises outlined in this review, including banned substances such as AAS, and the potentially underappreciated negative effect on renal function highlight the need to increase the athlete’s and coach’s knowledge for the promotion of optimal athlete health. This is also true for medical professionals, plus an understanding that athletes may omit positive usage of certain substances due to the preconceived condemnation from medical staff. The option of natural bodybuilding, consisting of excluding the use of AAS and other banned performance-enhancing drugs, could be a safer option, as no cases of AKI, CKD or ESKD were found to be published for this population.
5. Conclusions
Bodybuilders routinely engage in many nutritional and non-nutritional practices potentially harmful to the kidney (Figure 2). There is stronger evidence of damage caused by anabolic androgenic steroids and, particularly, high doses of vitamins A, D and E, than there is for high protein intake and creatine supplementation. Dehydrating practices including diuretic abuse and use of NSAIDs carry potential risks. Combinations of these practices are commonplace and may vary according to the training phase. Further research is required to identify the clinical and subclinical harm associated with individual practices and combinations, to enable the provision of appropriate advice.
Supplementary Materials
The following supporting information can be downloaded at: https://www.mdpi.com/article/10.3390/ijerph19074288/s1, Table S1: Overview of symptoms, renal measures, biopsy results, treatment, and subsequent renal diagnoses of bodybuilders presenting with AKI, CKD, and ESRD in 13 studies. Table S2: Overview of nutritional, pharmacological, and supplementary habits of bodybuilders presenting with AKI, CKD, and ESRD in 13 studies.
Author Contributions
Conceptualization, V.T., J.B., L.B., K.F. and J.H.; writing—original draft preparation V.T.; writing—review editing V.T., J.B., L.B., K.F., J.H. and S.C.F. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Lenzi, J.L.; Teixeira, E.L.; de Jesus, G.; Schoenfeld, B.J.; de Salles Painelli, V. Dietary Strategies of Modern Bodybuilders During Different Phases of the Competitive Cycle. J. Strength Cond. Res. 2021, 35, 2546–2551. [Google Scholar] [CrossRef] [PubMed]
- Iraki, J.; Fitschen, P.; Espinar, S.; Helms, E. Nutrition recommendations for bodybuilders in the off-season: A narrative review. Sports 2019, 7, 154. [Google Scholar] [CrossRef] [PubMed]
- Edholm, P.; Strandberg, E.; Kadi, F. Lower limb explosive strength capacity in elderly women: Effects of resistance training and healthy diet. J. Appl. Physiol. 2017, 123, 190–196. [Google Scholar] [CrossRef] [PubMed]
- Villareal, D.T.; Aguirre, L.; Gurney, A.B.; Waters, D.L.; Sinacore, D.R.; Colombo, E.; Armamento-Villareal, R.; Qualls, C. Aerobic or Resistance Exercise, or Both, in Dieting Obese Older Adults. N. Engl. J. Med. 2017, 376, 1943–1955. [Google Scholar] [CrossRef]
- Spendlove, J.; Mitchell, L.; Gifford, J.; Hackett, D.; Slater, G.; Cobley, S.; O’Connor, H. Dietary Intake of Competitive Bodybuilders. Sports Med. 2015, 45, 1041–1063. [Google Scholar] [CrossRef]
- Hackett, D.A. Training, Supplementation, and Pharmacological Practices of Competitive Male Bodybuilders Across Training Phases. J. Strength Cond. Res. 2021, 36, 936–970. [Google Scholar] [CrossRef]
- Ali, A.A.; Almukhtar, S.E.; Sharif, D.A.; Saleem ZS, M.; Muhealdeen, D.N.; Hughson, M.D. Effects of body-building supplements on the kidney: A population-based incidence study of biopsy pathology and clinical characteristics among middle eastern men. BMC Nephrol. 2020, 21, 1–10. [Google Scholar] [CrossRef]
- Gawad, M.A.; Kalawy, H.A. Gym nephropathy ‘bodybuilding versus kidney damaging’. J. Egypt. Soc. Nephrol. Transplant. 2019, 19, 124–128. [Google Scholar] [CrossRef]
- Bhasin, S.; Hatfield, D.L.; Hoffman, J.R.; Kraemer, W.J.; Labotz, M.; Phillips, S.M.; Ratamess, N.A. Anabolic-Androgenic Steroid Use in Sports, Health, and Society. Med. Sci. Sports Exerc. 2021, 53, 1778–1794. [Google Scholar] [CrossRef]
- Ostovar, A.; Haerinejad, M.; Farzaneh, M.R.; Keshavarz, M. Adverse effects of performance-enhancing drugs on the kidney in the male bodybuilders. Sci. Sports 2017, 32, 91–98. [Google Scholar] [CrossRef]
- Filho, S.L.A.P.; Gomes, P.E.A.D.C.; Forte, G.A.; Lima, L.L.L.; Júnior, G.B.D.S.; Meneses, G.; Martins, A.M.C.; Daher, E.D.F. Kidney disease associated with androgenic—Anabolic steroids and vitamin supplements abuse: Be aware! Nefrología 2020, 40, 26–31. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; PRISMA Group. Preferred reporting items for systematic re-views and meta-analyses: The PRISMA statement. Ann. Intern. Med. 2009, 151, 264–269. [Google Scholar] [CrossRef] [PubMed]
- Andres, S.; Ziegenhagen, R.; Trefflich, I.; Pevny, S.; Schultrich, K.; Braun, H.; Schänzer, W.; Hirsch-Ernst, K.I.; Schäfer, B.; Lampen, A. Creatine and creatine forms intended for sports nutrition. Mol. Nutr. Food Res. 2017, 61, 1600772. [Google Scholar] [CrossRef] [PubMed]
- Kashani, K.; Rosner, M.H.; Ostermann, M. Creatinine: From physiology to clinical application. Eur. J. Intern. Med. 2020, 72, 9–14. [Google Scholar] [CrossRef] [PubMed]
- Delanaye, P.; Cavalier, E.; Pottel, H. Serum Creatinine: Not So Simple! Nephron 2017, 136, 302–308. [Google Scholar] [CrossRef]
- Levey, A.S.; AInker, L. Assessment of Glomerular Filtration Rate in Health and Disease: A State of the Art Review. Clin. Pharmacol. Ther. 2017, 102, 405–419. [Google Scholar] [CrossRef]
- Ferguson, T.W.; Komenda, P.; Tangri, N. Cystatin C as a biomarker for estimating glomerular filtration rate. Curr. Opin. Nephrol. Hypertens. 2015, 24, 295–300. [Google Scholar] [CrossRef]
- Daher, E.D.F.; Fernandes, P.H.P.D.; Meneses, G.C.; Bezerra, G.F.; Ferreira, L.D.S.L.; Viana, G.D.A.; Martins, A.M.C.; Silva, G.B.D., Jr. Novel Kidney Injury Biomarkers Among Anabolic Androgenic Steroids Users—Evidence of Subclinical Kidney Disease. Asian J. Sports Med. 2018, 9, 1–4. [Google Scholar] [CrossRef]
- Levey, A.S.; Becker, C.; Inker, L.A. Glomerular filtration rate and albuminuria for detection and staging of acute and chronic kidney disease in adults: A systematic review. JAMA 2015, 313, 837–846. [Google Scholar] [CrossRef]
- Zhang, W.R.; Parikh, C.R. Biomarkers of Acute and Chronic Kidney Disease. Annu. Rev. Physiol. 2019, 81, 309–333. [Google Scholar] [CrossRef]
- Bennett, E.; Peters, S.A.E.; Woodward, M. Sex differences in macronutrient intake and adherence to dietary recommendations: Findings from the UK Biobank. BMJ Open 2018, 8, e020017. [Google Scholar] [CrossRef] [PubMed]
- Jäger, R.; Kerksick, C.M.; Campbell, B.I.; Cribb, P.J.; Wells, S.D.; Skwiat, T.M.; Purpura, M.; Ziegenfuss, T.N.; Ferrando, A.A.; Arent, S.M.; et al. International Society of Sports Nutrition Position Stand: Protein and exercise. J. Int. Soc. Sports Nutr. 2017, 14, 20. [Google Scholar] [CrossRef] [PubMed]
- Vitale, K.; Getzin, A. Nutrition and Supplement Update for the Endurance Athlete: Review and Recommendations. Nutrients 2019, 11, 1289. [Google Scholar] [CrossRef] [PubMed]
- Akl, A.; Aldabbagh, Y. Does gymnasium harbor an endemic cause of end stage kidney disease? a case report & review of literature. Urol. Nephrol. Open Access J. 2019, 7, 55–57. [Google Scholar] [CrossRef]
- Almukhtar, S.E.; Abbas, A.A.; Muhealdeen, D.N.; Hughson, M.D. Acute kidney injury associated with androgenic steroids and nutritional supplements in bodybuilders. Clin. Kidney J. 2015, 8, 415–419. [Google Scholar] [CrossRef] [PubMed]
- El-Reshaid, W.; El-Reshaid, K.; Al-Bader, S.; Ramadan, A.; Madda, J. Complementary bodybuilding: A potential risk for permanent kidney disease. Saudi J. Kidney Dis. Transplant. 2018, 29, 326–331. [Google Scholar] [CrossRef]
- Hartung, R.; Gerth, J.; Fünfstück, R.; Gröne, H.J.; Stein, G. End-stage renal disease in a bodybuilder: A multifactorial process or simply doping? Nephrol. Dial. Transplant. 2001, 16, 163–165. [Google Scholar] [CrossRef]
- Herlitz, L.C.; Markowitz, G.S.; Farris, A.B.; Schwimmer, J.A.; Stokes, M.B.; Kunis, C.; Colvin, R.B.; D’Agati, V.D. Development of Focal Segmental Glomerulosclerosis after Anabolic Steroid Abuse. J. Am. Soc. Nephrol. 2010, 21, 163–172. [Google Scholar] [CrossRef]
- Antonio, J.; Ellerbroek, A. Case reports on well-trained bodybuilders: Two years on a high protein diet. J. Exerc. Physiol. Online 2018, 21, 14–24. [Google Scholar]
- Antonio, J.; Ellerbroek, A.; Silver, T.; Vargas, L.; Tamayo, A.; Buehn, R.; Peacock, C.A. A High Protein Diet Has No Harmful Effects: A One-Year Crossover Study in Resistance-Trained Males. J. Nutr. Metab. 2016, 2016, 9104792. [Google Scholar] [CrossRef]
- Knight, E.L.; Stampfer, M.J.; Hankinson, S.E.; Spiegelman, D.; Curhan, G.C. The impact of protein intake on renal function decline in women with normal renal function or mild renal insufficiency. Ann. Intern. Med. 2003, 138, 460–467. [Google Scholar] [CrossRef] [PubMed]
- Ko, G.J.; Obi, Y.; Tortorici, A.R.; Kalantar-Zadeh, K. Dietary protein intake and chronic kidney disease. Curr. Opin. Clin. Nutr. Metab. Care 2017, 20, 77–85. [Google Scholar] [CrossRef] [PubMed]
- Frank, H.; Graf, J.; Amann-Gassner, U.; Bratke, R.; Daniel, H.; Heemann, U.; Hauner, H. Effect of short-term high-protein compared with normal-protein diets on renal hemodynamics and associated variables in healthy young men. Am. J. Clin. Nutr. 2009, 90, 1509–1516. [Google Scholar] [CrossRef] [PubMed]
- Jhee, J.H.; Kee, Y.K.; Park, S.; Kim, H.; Park, J.T.; Han, S.H.; Kang, S.-W.; Yoo, T.-H. High-protein diet with renal hyperfiltration is associated with rapid decline rate of renal function: A community-based prospective cohort study. Nephrol. Dial. Transplant. 2019, 35, 98–106. [Google Scholar] [CrossRef] [PubMed]
- Fouque, D.; Aparicio, M. Eleven reasons to control the protein intake of patients with chronic kidney disease. Nat. Clin. Pract. Nephrol. 2007, 3, 383–392. [Google Scholar] [CrossRef]
- Escalante, G.; Stevenson, S.W.; Barakat, C.; Aragon, A.A.; Schoenfeld, B.J. Peak week recommendations for bodybuilders: An evidence based approach. BMC Sports Sci. Med. Rehabil. 2021, 13, 68. [Google Scholar] [CrossRef]
- Gentil, P.; de Lira, C.A.B.; Paoli, A.; Dos Santos, J.A.B.; da Silva, R.D.T.; Junior, J.R.P.; Magosso, R.F. Nutrition, pharmacological and training strategies adopted by six bodybuilders: Case report and critical review. Eur. J. Transl. Myol. 2017, 27, 51–66. [Google Scholar] [CrossRef]
- Mäestu, J.; Eliakim, A.; Jürimäe, J.; Valter, I.; Jürimäe, T. Anabolic and Catabolic Hormones and Energy Balance of the Male Bodybuilders During the Preparation for the Competition. J. Strength Cond. Res. 2010, 24, 1074–1081. [Google Scholar] [CrossRef]
- Kreider, R.B.; Kalman, D.S.; Antonio, J.; Ziegenfuss, T.N.; Wildman, R.; Collins, R.; Candow, D.G.; Kleiner, S.M.; Almada, A.L.; Lopez, H.L. International Society of Sports Nutrition position stand: Safety and efficacy of creatine supplementation in exercise, sport, and medicine. J. Int. Soc. Sports Nutr. 2017, 14, 1–18. [Google Scholar] [CrossRef]
- Davani-Davari, D.; Karimzadeh, I.; Ezzatzadegan-Jahromi, S.; Sagheb, M.M. Potential Adverse Effects of Creatine Supplement on the Kidney in Athletes and Bodybuilders. Iran. J. Kidney Dis. 2018, 12, 253–260. [Google Scholar]
- Thorsteinsdottir, B.; Grande, J.P.; Garovic, V.D. Acute Renal Failure in a Young Weight Lifter Taking Multiple Food Supplements, Including Creatine Monohydrate. J. Ren. Nutr. 2006, 16, 341–345. [Google Scholar] [CrossRef] [PubMed]
- Taner, B.; Aysim, O.; Abdulkadir, U. The effects of the recommended dose of creatine monohydrate on kidney function. NDT Plus 2010, 4, 23–24. [Google Scholar] [CrossRef] [PubMed]
- Ardalan, M.; Samadifar, Z.; Vahedi, A. Creatine monohydrate supplement induced interstitial nephritis. J. Nephropathol. 2012, 1, 117–120. [Google Scholar] [CrossRef] [PubMed]
- Schilling, B.K.; Stone, M.H.; Utter, A.; Kearney, J.T.; Johnson, M.; Coglianese, R.; Stone, M.E. Creatine supple-mentation and health variables: A retrospective study. Med. Sci. Sports Exerc. 2001, 33, 183–188. [Google Scholar] [CrossRef]
- Lugaresi, R.; Leme, M.; Painelli, V.D.S.; Murai, I.H.; Roschel, H.; Sapienza, M.T.; Gualano, B. Does long-term creatine supplementation impair kidney function in resistance-trained individuals consuming a high-protein diet? J. Int. Soc. Sports Nutr. 2013, 10, 26. [Google Scholar] [CrossRef]
- Sale, C.; Harris, R.C.; Florance, J.; Kumps, A.; Sanvura, R.; Poortmans, J.R. Urinary creatine and methylamine excretion following 4 × 5 g day−1 or 20 × 1 g day−1 of creatine monohydrate for 5 days. J. Sports Sci. 2009, 27, 759–766. [Google Scholar] [CrossRef]
- Wyss, M.; Kaddurah-Daouk, R. Creatine and Creatinine Metabolism. Physiol. Rev. 2000, 80, 1107–1213. [Google Scholar] [CrossRef]
- Poortmans, J.R.; Kumps, A.; Duez, P.; Fofonka, A.; Carpentier, A.; Francaux, M. Effect of Oral Creatine Supplementation on Urinary Methylamine, Formaldehyde, and Formate. Med. Sci. Sports Exerc. 2005, 37, 1717–1720. [Google Scholar] [CrossRef]
- Mitchell, S.C.; Zhang, A.Q. Methylamine in human urine. Clin. Chim. Acta 2001, 312, 107–114. [Google Scholar] [CrossRef]
- Candow, D.G.; Little, J.P.; Chilibeck, P.D.; Abeysekara, S.; Zello, G.A.; Kazachkov, M.; Cornish, S.M.; Yu, P.H. Low-Dose Creatine Combined with Protein during Resistance Training in Older Men. Med. Sci. Sports Exerc. 2008, 40, 1645–1652. [Google Scholar] [CrossRef]
- Post, A.; Tsikas, D.; Bakker, S.J. Creatine is a Conditionally Essential Nutrient in Chronic Kidney Disease: A Hypothesis and Narrative Literature Review. Nutrients 2019, 11, 1044. [Google Scholar] [CrossRef] [PubMed]
- Pope, H.G.; Wood, R.I.; Rogol, A.; Nyberg, F.; Bowers, L.; Bhasin, S. Adverse Health Consequences of Performance-Enhancing Drugs: An Endocrine Society Scientific Statement. Endocr. Rev. 2014, 35, 341–375. [Google Scholar] [CrossRef] [PubMed]
- Sagoe, D.; Molde, H.; Andreassen, C.S.; Torsheim, T.; Pallesen, S. The global epidemiology of anabolic-androgenic steroid use: A meta-analysis and meta-regression analysis. Ann. Epidemiol. 2014, 24, 383–398. [Google Scholar] [CrossRef] [PubMed]
- Daher, E.F.; Júnior, G.B.S.; Queiroz, A.L.; Ramos, L.M.A.; Santos, S.Q.; Barreto, D.M.S.; Guimarães, A.A.C.; Barbosa, C.A.; Franco, L.M.; Patrocínio, R.M.S.V. Acute kidney injury due to anabolic steroid and vitamin supplement abuse: Report of two cases and a literature review. Int. Urol. Nephrol. 2009, 41, 717–723. [Google Scholar] [CrossRef]
- Libório, A.B.; Nasserala, J.C.; Gondim, A.S.; Daher, E. The Case|Renal failure in a bodybuilder athlete. Kidney Int. 2014, 85, 1247–1248. [Google Scholar] [CrossRef][Green Version]
- Rocha, P.N.; Santos, C.S.; Avila, M.O.; Neves, C.L.; Bahiense-Oliveira, M. Hypercalcemia and acute kidney in-jury caused by abuse of a parenteral veterinary compound containing vitamins A, D, and E. Braz. J. Nephrol. 2011, 33, 467–471. [Google Scholar] [CrossRef]
- Dousdampanis, P.; Trigka, K.; Fourtounas, C.; Bargman, J.M. Role of Testosterone in the Pathogenesis, Progression, Prognosis and Comorbidity of Men With Chronic Kidney Disease. Ther. Apher. Dial. 2013, 18, 220–230. [Google Scholar] [CrossRef]
- Quan, A.; Chakravarty, S.; Chen, J.-K.; Loleh, S.; Saini, N.; Harris, R.C.; Capdevila, J.; Quigley, R. Androgens augment proximal tubule transport. Am. J. Physiol. Physiol. 2004, 287, F452–F459. [Google Scholar] [CrossRef]
- Kalk, P.; Thöne-Reineke, C.; Schwarz, A.; Godes, M.; Bauer, C.; Pfab, T.; Hocher, B. Renal phenotype of Et-1 transgenic mice is modulated by androgens. Eur. J. Med. Res. 2009, 14, 55–58. [Google Scholar] [CrossRef]
- Verzola, D.; Villaggio, B.; Procopio, V.; Gandolfo, M.T.; Gianiorio, F.; Famà, A.; Tosetti, F.; Traverso, P.; Deferrari, G.; Garibotto, G. Androgen-mediated apoptosis of kidney tubule cells: Role of c-Jun amino terminal kinase. Biochem. Biophys. Res. Commun. 2009, 387, 531–536. [Google Scholar] [CrossRef]
- Doublier, S.; Lupia, E.; Catanuto, P.; Periera-Simon, S.; Xia, X.; Korach, K.; Berho, M.; Elliot, S.J.; Karl, M. Testosterone and 17 b-estradiol have opposite effects on podocyte apoptosis that precedes glomerulosclerosis in female estrogen receptor knockout mice. Kidney Int. 2011, 79, 404–413. [Google Scholar] [CrossRef] [PubMed]
- Metcalfe, P.D.; Leslie, J.A.; Campbell, M.T.; Meldrum, D.R.; Hile, K.L.; Meldrum, K.K. Testosterone exacerbates obstructive renal injury by stimulating TNF-α production and increasing proapoptotic and profibrotic signaling. Am. J. Physiol. Metab. 2008, 294, E435–E443. [Google Scholar] [CrossRef] [PubMed]
- Godswill, A.G.; Somtochukwu, I.V.; O Ikechukwu, A.; Kate, E.C. Health Benefits of Micronutrients (Vitamins and Minerals) and their Associated Deficiency Diseases: A Systematic Review. Int. J. Food Sci. 2020, 3, 1–32. [Google Scholar] [CrossRef]
- Daher, E.D.F.; Martiniano, L.V.M.; Lima, L.L.L.; Filho, N.C.V.L.; Souza, L.E.D.O.; Fernandes, P.H.P.D.; da Silva, G.B., Jr. Acute kidney injury due to excessive and prolonged intramuscular injection of veterinary supplements containing vitamins A, D and E: A series of 16 cases. Nefrología 2017, 37, 61–67. [Google Scholar] [CrossRef]
- Ronsoni, M.F.; Santos, H.D.C.D.; Colombo, B.D.S.; Corrêa, C.G.; Moritz, A.P.G.; Coral, M.H.C.; Van De Sande-Lee, S.; Hohl, A. Hypercalcemia and acute renal insufficiency following use of a veterinary supplement. J. Bras. De Nefrol. 2017, 39, 467–469. [Google Scholar] [CrossRef] [PubMed]
- Heaney, R.P. Vitamin D in Health and Disease. Clin. J. Am. Soc. Nephrol. 2008, 3, 1535–1541. [Google Scholar] [CrossRef] [PubMed]
- Heaney, R.P. Vitamin D: Criteria for safety and efficacy. Nutr. Rev. 2008, 66, S178–S181. [Google Scholar] [CrossRef] [PubMed]
- Bhalla, K.; Ennis, D.M.; Ennis, E.D. Hypercalcemia caused by iatrogenic hypervitaminosis A. J. Am. Diet. Assoc. 2005, 105, 119–121. [Google Scholar] [CrossRef]
- Levi, M.; Ellis, M.A.; Berl, T. Control of renal hemodynamics and glomerular filtration rate in chronic hypercalcemia: Role of prostaglandins, renin-angiotensin system, and calcium. J. Clin. Investig. 1983, 71, 1624–1632. [Google Scholar] [CrossRef]
- Tachamo, N.; Donato, A.; Timilsina, B.; Nazir, S.; Lohani, S.; Dhital, R.; Basnet, S. Hypercalcemia associated with cosmetic injections: A systematic review. Eur. J. Endocrinol. 2018, 178, 425–430. [Google Scholar] [CrossRef]
- Bindu, S.; Mazumder, S.; Bandyopadhyay, U. Non-steroidal anti-inflammatory drugs (NSAIDs) and organ damage: A current perspective. Biochem. Pharmacol. 2020, 180, 114147. [Google Scholar] [CrossRef] [PubMed]
- Cardinale, D.A.; Lilja, M.; Mandić, M.; Gustafsson, T.; Larsen, F.J.; Lundberg, T.R. Resistance Training with Co-ingestion of Anti-inflammatory Drugs Attenuates Mitochondrial Function. Front. Physiol. 2017, 8, 1074. [Google Scholar] [CrossRef] [PubMed]
- Omeragic, E.; Marjanovic, A.; Djedjibegovic, J.; Turalic, A.; Dedić, M.; Niksic, H.; Lugusic, A.; Sober, M. Prevalence of use of permitted pharmacological substances for recovery among athletes. Pharmacia 2021, 68, 35–42. [Google Scholar] [CrossRef]
- Gorski, T.; Cadore, E.L.; Pinto, S.S.; da Silva, E.M.; Correa, C.S.; Beltrami, F.G.; Kruel, L.F.M. Use of NSAIDs in triathletes: Prevalence, level of awareness and reasons for use. Br. J. Sports Med. 2011, 45, 85–90. [Google Scholar] [CrossRef]
- Steckling, F.M.; Lima, F.D.; Farinha, J.B.; Rosa, P.C.; Royes, L.F.F.; Cuevas, M.J.; Bresciani, G.; Soares, F.A.; González-Gallego, J.; Barcelos, R.P. Diclofenac attenuates inflammation through TLR4 pathway and improves exercise performance after exhaustive swimming. Scand. J. Med. Sci. Sports 2019, 30, 264–271. [Google Scholar] [CrossRef] [PubMed]
- Lundberg, T.R.; Howatson, G. Analgesic and anti-inflammatory drugs in sports: Implications for exercise performance and training adaptations. Scand. J. Med. Sci. Sports 2018, 28, 2252–2262. [Google Scholar] [CrossRef]
- Lilja, M.; Mandić, M.; Apró, W.; Melin, M.; Olsson, K.; Rosenborg, S.; Gustafsson, T.; Lundberg, T.R. High doses of anti-inflammatory drugs compromise muscle strength and hypertrophic adaptations to resistance training in young adults. Acta Physiol. 2018, 222, e12948. [Google Scholar] [CrossRef]
- Nderitu, P.; Doos, L.; Jones, P.W.; Davies, S.J.; Kadam, U.T. Non-steroidal anti-inflammatory drugs and chronic kidney disease progression: A systematic review. Fam. Pract. 2013, 30, 247–255. [Google Scholar] [CrossRef]
- Chappell, A.J.; Simper, T.N. Nutritional Peak Week and Competition Day Strategies of Competitive Natural Bodybuilders. Sports 2018, 6, 126. [Google Scholar] [CrossRef]
- Mitchell, L.; Hackett, D.; Gifford, J.; Estermann, F.; O’Connor, H. Do Bodybuilders Use Evidence-Based Nutrition Strategies to Manipulate Physique? Sports 2017, 5, 76. [Google Scholar] [CrossRef]
- Mayr, F.B.; Domanovits, H.; Laggner, A.N. Hypokalemic paralysis in a professional bodybuilder. Am. J. Emerg. Med. 2012, 30, 1324–1325. [Google Scholar] [CrossRef] [PubMed]
- Probert, A.; Palmer, F.; Leberman, S. The Fine Line: An insight into ‘risky’ practices of male and female competitive bodybuilders. Ann. Leis. Res. 2007, 10, 272–290. [Google Scholar] [CrossRef]
- Kasper, A.M.; Crighton, B.; Langan-Evans, C.; Riley, P.; Sharma, A.; Close, G.L.; Morton, J.P. Case Study: Extreme Weight Making Causes Relative Energy Deficiency, Dehydration, and Acute Kidney Injury in a Male Mixed Martial Arts Athlete. Int. J. Sport Nutr. Exerc. Metab. 2019, 29, 331–338. [Google Scholar] [CrossRef] [PubMed]
- Wu, X.; Zhang, W.; Ren, H.; Chen, X.; Xie, J.; Chen, N. Diuretics associated acute kidney injury: Clinical and pathological analysis. Ren. Fail. 2014, 36, 1051–1055. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Alvarez, A.; Egan, B.; De Klein, S.; Dima, L.; Maggi, F.M.; Isoniemi, M.; Ribas-Barba, L.; Raats, M.; Meissner, E.M.; Badea, M.; et al. Usage of Plant Food Supplements across Six European Countries: Findings from the PlantLIBRA Consumer Survey. PLoS ONE 2014, 9, e92265. [Google Scholar] [CrossRef] [PubMed]
- García-Cortés, M.; Robles-Díaz, M.; Ortega-Alonso, A.; Medina-Caliz, I.; Andrade, R.J. Hepatotoxicity by Dietary Supplements: A Tabular Listing and Clinical Characteristics. Int. J. Mol. Sci. 2016, 17, 537. [Google Scholar] [CrossRef]
- Helms, E.R.; Aragon, A.A.; Fitschen, P.J. Evidence-based recommendations for natural bodybuilding contest preparation: Nutrition and supplementation. J. Int. Soc. Sport. Nutr. 2014, 11, 20. [Google Scholar] [CrossRef]
- Hackett, D.A.; Johnson, N.A.; Chow, C.-M. Training Practices and Ergogenic Aids Used by Male Bodybuilders. J. Strength Cond. Res. 2013, 27, 1609–1617. [Google Scholar] [CrossRef]
- Nawrot, P.; Jordan, S.; Eastwood, J.; Rotstein, J.; Hugenholtz, A.; Feeley, M. Effects of caffeine on human health. Food Addit. Contam. 2003, 20, 1–30. [Google Scholar] [CrossRef]
- Chappell, A.J.; Simper, T.; Barker, M.E. Nutritional strategies of high level natural bodybuilders during competition preparation. J. Int. Soc. Sports Nutr. 2018, 15, 1–12. [Google Scholar] [CrossRef]
- Dehoney, S.; Wellein, M. Rhabdomyolysis associated with the nutritional supplement Hydroxycut. Am. J. Health Pharm. 2009, 66, 142–148. [Google Scholar] [CrossRef] [PubMed]
- Carol, M.L. Hydroxycut Weight Loss Dietary Supplements: A Contributing Factor in the Development of Exertional Rhabdomyolysis in Three U.S. Army Soldiers. Mil. Med. 2013, 178, e1039–e1042. [Google Scholar] [CrossRef] [PubMed]
- Campana, C.; Griffin, P.L.; Simon, E.L. Caffeine overdose resulting in severe rhabdomyolysis and acute renal failure. Am. J. Emerg. Med. 2014, 32, 111.e3–111.e4. [Google Scholar] [CrossRef] [PubMed]
- Golcuk, Y.; Ozsarac, M.; Golcuk, B.; Gunay, E. Caffeine-induced rhabdomyolysis. Am. J. Emerg. Med. 2014, 32, 100. [Google Scholar] [CrossRef]
- Chiang, W.-F.; Liao, M.-T.; Cheng, C.-J.; Lin, S.-H. Rhabdomyolysis induced by excessive coffee drinking. Hum. Exp. Toxicol. 2013, 33, 878–881. [Google Scholar] [CrossRef]
- Dong Jun, S.U.N.G.; Eun-Ju, C.H.O.I.; Sojung, K.I.M.; Jooyoung, K.I.M. Rhabdomyolysis from resistance exercise and caffeine intake. Iran. J. Public Health 2018, 47, 138. [Google Scholar]
- Gagliano, M.; Corona, D.; Giuffrida, G.; Giaquinta, A.; Tallarita, T.; Zerbo, D.; Sorbello, M.; Paratore, A.; Virgilio, C.; Cappellani, A.; et al. Low-intensity body building exercise induced rhabdomyolysis: A case report. Cases J. 2009, 2, 1–2. [Google Scholar] [CrossRef]
- Patel, D.R.; Gyamfi, R.; Torres, A. Exertional Rhabdomyolysis and Acute Kidney Injury. Physician Sportsmed. 2009, 37, 71–79. [Google Scholar] [CrossRef]
- Kim, J.; Lee, J.; Kim, S.; Ryu, H.Y.; Cha, K.S.; Sung, D.J. Exercise-induced rhabdomyolysis mechanisms and prevention: A literature review. J. Sport Health Sci. 2016, 5, 324–333. [Google Scholar] [CrossRef]
- Clarkson, P.M.; Hubal, M.J. Exercise-Induced Muscle Damage in Humans. Am. J. Phys. Med. Rehabil. 2002, 81, S52–S69. [Google Scholar] [CrossRef]
- Grimmer, N.M.; Gimbar, R.P.; Bursua, A.; Patel, M. Rhabdomyolysis secondary to clenbuterol use and exercise. J. Emerg. Med. 2016, 50, e71–e74. [Google Scholar] [CrossRef] [PubMed]
- Bosch, X.; Poch, E.; Grau, J.M. Rhabdomyolysis and acute kidney injury. N. Engl. J. Med. 2009, 361, 62–72. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).