1. Introduction
During the COVID-19 pandemic, healthcare workers (HCWs) have been over-represented globally in the number of infections [
1]. As of 19 August 2020, there were 2497 HCWs diagnosed with COVID-19 infection in Victoria. In the second wave, 69% or more were likely to have been workplace acquired, with a number still under investigation [
2].
SARS-CoV-2 is highly transmissible [
3], and there is growing evidence for its airborne transmission [
3,
4]. Filtering facepiece respirators, including disposable P2/N95 respirators (masks), is used to reduce the wearer’s respiratory exposure to airborne pathogens. The use of P2/N95 respirators are required with airborne infectious diseases or when an aerosol-generating procedure (AGP) is undertaken in a patient with a droplet-spread disease [
5,
6]. For a P2/N95 respirator to provide its designed protection, an adequate face seal must be achieved and maintained for the entire period of time that the worker may be exposed.
Australian Standard 1715:2009 states that a suitable fit test should be conducted on all users of respiratory protection equipment with a close-fitting facepiece such as a P2/N95 respirator [
7].
Despite the Australian Standards recommendation, fit testing is not mandated in the state of Victoria. Other states in Australia, for example, South Australia, require fit testing of P2/N95 respirators for high-risk workers or those working in high-risk areas as well as those performing or assisting with AGPs [
8]. Whilst the Department of Health and Ageing in Australia has previously acknowledged fit testing as the gold standard for the use of P2/N95 respirators, it does acknowledge that fit testing of all HCWs who need to use a P2/N95 respirator will be difficult to accomplish due to limited supplies and range of types/sizes available [
9].
The Department of Health and Human Services in Victoria (DHHS) is the regulatory body for public health in the state. The DHHS guidelines require only a fit check (or user seal check) to be performed each time a P2/N95 respirator is worn (donned) [
10].
The fit check describes the procedure that the wearer performs to determine an adequate facial seal. The fit check can either be a positive pressure or a negative pressure check. In contrast, the fit test is a standardised technique to assess the seal of a P2/N95 respirator to the wearer. This is performed by a trained fit tester. The fit test can be qualitative or quantitative. In general, passing a fit test results in a higher level of protection when compared with no fit testing for P2/N95 respirators [
11].
A quantitative fit test (QNFT) objectively reports a numerical value known as a fit factor. This is derived from measurements of the particle concentration in ambient air relative to the concentration inside the respirator when worn. A value of 100 or greater is the criterion for achieving a pass for a disposable P2/N95 respirator [
12].
There is a broad range of reported fit test failure rates for the first choice of P2/N95 respirator, from 5 to 82% [
13,
14,
15]. Evidence suggests that fit checking alone is limited in predicting respirator fit [
16,
17,
18]. Factors identified that might alter fit test outcomes include ethnicity, facial characteristics, occupation, and training in fit checking [
19,
20]. A number of studies have included interviews or surveys of participants to assess these factors [
19,
21].
There are no previous studies that examine the real-world selection, application, and seal of these P2/N95 respirators during the current pandemic, hence the reason for executing our study.
The objectives of this study were to:
Evaluate the DHHS guideline fit check with a quantitative fit test for the range of currently available P2/N95 respirators.
Determine the pass/fail rates with quantitative fit testing for the first choice of respirator (first-up failure rates).
Evaluate attitudes, experience, and training related to P2/N95 respirators, the fit check, fit testing, and identify factors related to successful P2/N95 respirator facial seal.
2. Materials and Methods
This observational study of perioperative HCWs comprised of three components:
An online (entry) survey;
Fit testing of a P2/N95 self-selected respirator after a self-assessed fit check;
A subsequent online (exit) survey.
The study was conducted from 29 May 2020 to 5 June 2020 at the Royal Victorian Eye and Ear Hospital, a tertiary referral centre in Melbourne, Australia. Ethics approval was obtained as Quality Assurance Research from RVEEH # Reference No. 20/1465HQ.
2.1. Participants
Inclusion criteria: participants were recruited from the theatre complex and Emergency department, including surgical, anaesthetic, and emergency nursing and medical personnel. Staff were selected from rosters using an online generator (
https://www.randomizer.org/ accessed on 23 May 2021).
Exclusion criteria: personnel who refused consent, failed a COVID-19 screening tool (hospital screening tool to assess risk of COVID-19), were furloughed, or unavailable for fit testing.
2.2. Study Protocol
Survey questions (See
Appendix A and
Appendix B) were co-developed from topics generated by a group of anaesthetists interested in perioperative safety, prepared by an engaged survey writer after brief analysis, then tested on perioperative staff. A consensus meeting of 9 anaesthetists selected the final questions. Surveys were collated using QualtricsTM Experience Management (XM) software platform (Qualtrics, Provo, UT, USA). Surveys included demographics, education and training, respirator usage, as well as opinions and satisfaction.
In total, 50 participants were allocated based on time slots created for the fit testing sessions over 2 days. These allocations were divided equally between medical and nursing staff. Within the medical group, this was further subdivided into 4 equal groups representing ophthalmology, ENT, anaesthesia, and emergency departments. A total of 58 people completed the fit testing, which was 8 more than originally planned due to additional slots being available on the fit testing days.
Informed written consent was obtained from participants.
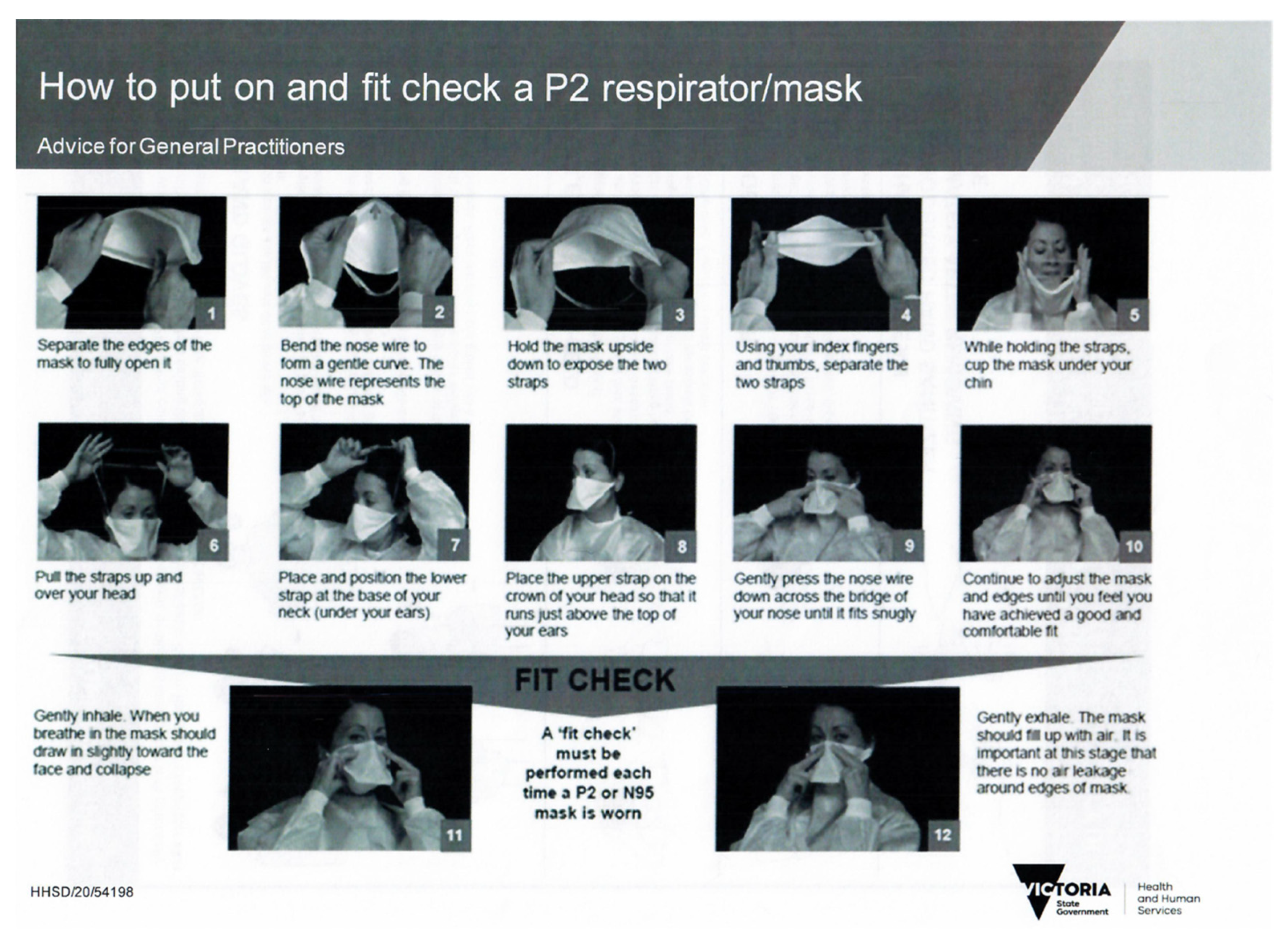
Participants read definitions of fit check, fit test, and were shown a visual guide for DHHS fit check (See
Appendix C and
Appendix D). Participants chose P2/N95 respirators from 7 possible types. (see
Appendix E). A sample of each mask, together with the model name, was placed on a table for the participants to see prior to selection.
Participants donned the P2/N95 respirator, performed a fit-check, and then reported a pass or fail. The participant then underwent fit testing utilising dynamic manoeuvres according to Occupational Safety and Health Administration (OSHA) protocol [
13]. This was performed by a professional fit tester (organised through Kinnect, with the fit tester having completed a Respirator Fit Test course) using a PortaCountTM Model 8048 machine (TSI Inc., Shoreview, MN, USA). Failure to obtain a pass led to a series of adjustments (pinching nose bridge clip, adjusting straps, reseating mask to cover chin), as instructed by the fit tester, and then re-tested. Failing this, the process was repeated for up to a maximum of three respirators.
2.3. Data Collection
Demographics were recorded prior to fit testing, including weight and height. The fit check outcome, the fit test results, and the associated numerical fit factors were recorded.
2.4. Outcomes
The first choice respirator fit test result, of pass or fail, was the primary outcome. The fit check validity in predicting the first fit test result was reported in a 2 × 2 contingency table. Other outcomes included: number of adjustments needed for a fit test pass, and sub-analysis of respirators. Survey data were recorded and summarised.
2.5. Study Size and Bias
Participants were enrolled to fill 2 days of fit testing in order to minimise the impact on the limited stocks of respirators. Any HCW on leave of absence was excluded. A total of 67 people were screened and sent an anonymous online survey, with 58 participants fit tested. The discrepancy between the entry survey sample size of 67 and the fit tested sample size of 58 was due to non-attendance. Sample size could not be determined as there was no accepted fit test pass or fail rate in the literature.
2.6. Statistical Analysis
Demographic and survey data were reported as simple descriptive statistics. Group comparisons were performed using chi-square tests for equal proportion (or Fisher’s exact tests where numbers were small), Student t-tests for normally distributed data and Wilcoxon rank-sum tests otherwise, with results reported as percentages (n), mean (standard deviation) or median (interquartile range), respectively. Agreement between fit check and fit testing results was assessed with marginal homogeneity between paired proportions determined using McNemar’s test. To test for normality of data, histograms were generated for each variable and this distribution visually assessed for symmetry. All analysis was performed using SAS® version 9.4 (SAS Institute Inc., Cary, NC, USA), and a two-sided p-value of 0.05 was used to indicate statistical significance.
3. Results
Demographic data were compiled into a baseline characteristics table (see
Table 1).
After the first respirator fit check, 71% (41/58) of participants reported a pass.
The first selected P2/N95 respirator failure rate for the OSHA protocol quantitative fit test was 69% (40/58 failed and 18/58 passed). The first-up testing results are reported as a contingency table (see
Table 2 and
Table 3). The test characteristics are reported in
Table 3.
There was an improvement in fit factor and pass rate with manoeuvres implemented by a fit tester for the first respirator selected (median number of manoeuvres = 2, interquartile range 0–3). This led to a 76% pass rate for the first respirator.
Of the 14 participants (24%) who failed to achieve a pass with the first respirator, a second P2/N95 respirator led to 51 participants achieving a pass (88% after two respirators). A third respirator passed a further six people (98% overall pass rate). Only one person (2%) did not achieve a fit test pass with three respirators.
Of the seven types of respirator available, the duckbill varieties were the most common respirator chosen (see
Table 4). Fit test success rates differed significantly between the seven different respirators (
p = 0.03) with chi-squared analysis. The 3M
TM 1860 was the respirator type that most often achieved a successful fit (67% (10/15)) while the Halyard small duckbill was the least likely successful fit (8% (1/13))
Response rates for the entry and exit surveys were 80.6% (54/67) and 75.8% (44/58), respectively, and are summarised in
Table 5.
Fit testing was considered absolutely essential or very important by 65.4% (34/52) of respondents, which increased to 95.5% (42/44) on the exit survey. Only 7.5% (4/53) of respondents had a previous fit test prior to this study. Notably, 71.8% (35/49) of respondents had encountered patients with tuberculosis at work, yet only 37% (13/35) had previous fit check training prior to COVID-19. The participant perception of being able to achieve a fit or seal on the face with a P2/N95 respirator improved from 39.2% (20/51) before fit testing to 81.8% (36/44) after fit testing.
4. Discussion
This study found the fit check, as described by the DHHS, was poorly predictive of respirator seal when assessed by a quantitative fit test (PPV 34.1%, 95% CI 25.0–40.5). This is similar to previous studies [
16,
17,
18]. A failed fit check, however, was more likely to be associated with a failed fit test (NPV 76.5%, 95% CI 54.5–91.7), which is marginally higher than previously reported [
17].
The fit test failure rate (69% (40/58)) for the initial respirator selected is significant, and within the broad range reported in the literature [
13,
14,
15]. This result has clinical relevance as it closely resembles the current workplace use of P2/N95 respirators by HCWs. The participant self-selected a respirator from all available types and sizes, and performed a fit check without any additional instruction beyond the DHHS visual aid.
The demographics indicated the cohort were experienced in healthcare, including infectious diseases, yet had relatively low amounts of training and education related to respirators and fit checking. For many decades, Victorian HCWs have cared for patients with airborne infectious diseases, including tuberculosis, without fit testing. This has exposed the knowledge gap in the safe clinical use of these respirators despite their availability. The potential risk of workplace acquired infections is of serious concern, including during the current COVID-19 pandemic.
Perceptions of PPE safety and confidence in the ability to obtain a seal were higher after the fit test, in keeping with a recent international survey [
22]. The heterogeneous study cohort would likely be relevant to perioperative Victorian, and Australian, HCWs.
A study by Or et al. supports the role of ongoing education in fit checking [
20]. Conversely, Wilkinson in 2010 reported that prior training did not translate to a higher fit test pass rate; however, a fit tester was utilised for respirator selection [
19]. In our study, the fit test process improved fit test pass rates. This was in part due to stepwise respirator selection, but also included manoeuvres with a trained fit tester. Further repeat studies with education as a part of fit testing integrated with a Respiratory Protection Program (RPP) are needed to assess retention rates of education over time.
The P2/N95 respirators used for our study were typical of those used at multiple institutions throughout Victoria during that phase of the pandemic. No single P2/N95 respirator provided a universal seal. Nonetheless, each respirator achieved a seal on at least one participant. A broad selection of respirator types and sizes must therefore be available to HCWs. The duckbill respirator was the most popular choice; however, it also had the highest failure rate. Sub-analysis of respirators was not adequately powered for determining respirator design as a factor, and further empirical studies are needed to make correct inferences. Anthropometrics and comparison with respirator design to population data and respiratory panels would also be required [
23,
24,
25].
In the wider HCW population without a regular fit testing program, there would be an unidentified proportion of HCWs who would not have an adequate seal for respiratory protection. Fit testing further identified the one person that failed all fit tests with three respirators despite instruction from a fit tester. Alternative respiratory protection equipment or alternative duties need to be offered to those that fail fit testing, as part of a Respiratory Protection Program (RPP).
It is also notable that alternative forms of respiratory protection have also been successfully fit tested to levels comparable to P2/N95 and P3/N99 standards. The study by Germonpre et al. [
26] uses a modified commercial snorkel mask as effective respiratory protection. Even though the rapid development of this pandemic has led to different approaches to mask selection between countries, the key message is that fit testing plays a crucial role in determining the efficacy of respiratory protection.
Limitations
Having no applicable respirator fit failure rate from the scientific literature prevented any sample size calculation to look for a comparative effect.
This study was conducted during the COVID-19 pandemic and imposed limitations on the ability to fit test a larger number of participants. These limitations, however, are applicable to the current pandemic conditions more broadly.
We made a wide range of respirators available to reflect the choices within our institution, although understanding it would reduce the sample sizes for each respirator and the interpretation of the results. Prior exposure to a particular type of respirator may have influenced the selection made.
The DHHS fit check as described at the time of the study did not include a mirror nor a trained spotter. Seven participants had facial hair despite receiving prior instructions to remove it for the study day. They were included for pragmatic reasons to reflect real-world behaviours, where we find clinicians donning their respirators even with 2-day-old facial hair growth.
5. Conclusions
The current DHHS fit check alone is not a valid surrogate to fit testing for respirator seal. Quantitative fit testing is required to identify the correct size and type of respirator for each user, and provides an educational opportunity for the user to improve respirator seal. This cohort was experienced in healthcare but had minimal respirator related training prior to COVID-19, and fit testing has improved their confidence in achieving a seal with P2/N95 respirators. Hospitals and policymakers will benefit from integrating education and fit testing into a comprehensive RPP.
Author Contributions
Conceptualisation: J.K.C. and M.A.; methodology: J.K.C., K.H.Y. and M.A.; software: J.K.C. and M.A.; validation: J.K.C., S.M., Z.K.-C. and M.A.; formal analysis: J.K.C., S.M., Z.K.-C. and M.A.; investigation: J.K.C., K.H.Y. and M.A.; resources: J.K.C., K.H.Y. and M.A.; data curation: J.K.C. and M.A.; Writing—Original draft preparation: J.K.C.; Writing—Review and editing: J.K.C., K.H.Y., S.M., Z.K.-C. and M.A.; visualisation: K.H.Y.; supervision: J.K.C. and M.A.; project administration: J.K.C., K.H.Y., S.M., Z.K.-C. and M.A. All authors have read and agreed to the published version of the manuscript.
Funding
This research received internal funding from the Royal Victorian Eye and Ear Hospital.
Institutional Review Board Statement
The study was conducted according to the guidelines of the Declaration of Helsinki, and approved by the Ethics Committee of Royal Victorian Eye and Ear Hospital (Reference No. 20/1465HQ on 13/5/20).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Acknowledgments
The authors would like to acknowledge: the Royal Victorian Eye and Ear Hospital for pledging support and funding; Kinnect and the fit tester–Nick Tartaglia for conducting the fit testing on-site; Michael Bailey for statistical data analysis; Rachel MacCulloch for her input into the surveys; John Paul So and Thanh Tran as research nurses for enrolment, recruitment, and data collection; Michael Kluger for his editing and referencing with the manuscript; Michael Kluger, Alan Tse, Gavin Doolan, Rob Wengritzky, and Isaac Cheung for being part of the survey consensus panel.
Conflicts of Interest
The authors declare no conflict of interest.
Appendix A. RVEEH Entry Survey
Appendix B. RVEEH Exit Survey
Appendix C. DHHS Fit Check P2 Respirator Mask
Appendix D. Fit Check and Fit Test Information Sheet
Appendix E. Mask Information Sheet
References
- Nguyen, L.H.; Drew, D.A.; Graham, M.S.; Joshi, A.D.; Guo, C.-G.; Ma, W.; Mehta, R.S.; Warner, E.T.; Sikavi, D.R.; Lo, C.-H.; et al. Risk of COVID-19 among front-line health-care workers and the general community: A prospective cohort study. Lancet Public Health 2020, 5, E475–E483. [Google Scholar] [CrossRef]
- State of Victoria, Australia, Department of Health and Human Services, 25 August 2020. Protecting Our Healthcare Workers. 2001628_v9. Available online: https://www.dhhs.vic.gov.au/help-and-support-healthcare-workers-coronavirus-covid-19 (accessed on 27 August 2020).
- Sanche, S.; Lin, Y.T.; Xu, C.; Romero-Severson, E.; Hengartner, N.; Ke, R. High Contagiousness and Rapid Spread of Severe Acute Respiratory Syndrome Coronavirus 2. Emerg. Infect. Dis. 2020, 26, 1470–1477. [Google Scholar] [CrossRef] [PubMed]
- MacIntyre, C.R.; Ananda-Rajah, M.; Nicholls, M.; Quigley, A. Current guidelines for respiratory protection of Australian health care workers against COVID-19 are not adequate and national reporting of health worker infections is required. Med. J. Aust. 2020. [Google Scholar] [CrossRef] [PubMed]
- Van Doremalen, N.; Bushmaker, T.; Morris, D.H.; Holbrook, M.G.; Gamble, A.; Williamson, B.N.; Tamin, A.; Harcourt, J.L.; Thornburg, N.J.; Gerber, S.I.; et al. Aerosol and Surface Stability of SARS-CoV-2 as Compared with SARS-CoV-1. N. Engl. J. Med. 2020, 382, 1564–1567. [Google Scholar] [CrossRef] [PubMed]
- National Health and Medical Research Council. Australian Guidelines for the Prevention and Control of Infection in Healthcare, Canberra; National Health and Medical Research Council: Canberra, Australia, 2019. [Google Scholar]
- Standards Australia, AS 1715:2009. Selection Use and Maintenance of Respiratory Protective Equipment, (Sydney, NSW: Standards Australia, 2009) in SAI Global. Available online: https://infostore.saiglobal.com/en-au/standards/as-nzs-1715-2009-117496_saig_as_as_275145/ (accessed on 2 April 2020).
- Health Service IC, Branch CDC. Respiratory Protection against Airborne Infectious Diseases Clinical Guideline Version No.: 1.4. Available online: https://www.sahealth.sa.gov.au/wps/wcm/connect/0aca9a80423727cc9e0efeef0dac2aff/Clinical_Directive_Respiratory_Protection_+Against_Airborne_Infectious_Diseases_v1.4_22.06.2020.pdf?MOD=AJPERES&CACHEID=ROOTWORKSPACE-0aca9a80423727cc9e0efeef0dac2aff-nbGoB6p (accessed on 2 September 2020).
- Australia, Department of Health and Ageing, 19 June 2020. Guidance on the Use of Personal Protective Equipment (PPE) in Hospitals during the COVID-19 Outbreak. Available online: https://www.health.gov.au/sites/default/files/documents/2020/07/guidance-on-the-use-of-personal-protective-equipment-ppe-in-hospitals-during-the-covid-19-outbreak.pdf (accessed on 21 August 2020).
- State of Victoria, Australia, Department of Health and Human Services, 21 June 2020. Coronavirus Disease 2019 (COVID-19) Infection Prevention and Control Guideline 2 Version 2. Available online: https://www.dhhs.vic.gov.au/health-services-and-professionals-coronavirus-covid-19 (accessed on 10 July 2020).
- Lawrence, R.B.; Duling, M.G.; Calvert, C.A.; Coffey, C.C. Comparison of performance of three different types of respiratory protection devices. J. Occup. Environ. Hyg. 2006, 3, 465–474. [Google Scholar] [CrossRef] [PubMed]
- Occupational Safety and Health Administration (1970). Occupational Safety and Health Standards: Occupational Health and Environmental Control (Standard No. 1910.134: Fit Testing Procedures (Mandatory) Appendix A Part, I. OSHA-Accepted Fit Test Protocol. Available online: https://www.osha.gov/laws-regs/regulations/standardnumber/1910/1910.134AppA (accessed on 25 March 2020).
- McMahon, E.; Wada, K.; Dufresne, A. Implementing fit testing for N95 filtering facepiece respirators: Practical information from a large cohort of hospital workers. Am. J. Infect. Control. 2008, 36, 298–300. [Google Scholar] [CrossRef] [PubMed]
- Winter, S.; Thomas, J.H.; Stephens, D.P.; Davis, J.S. Particulate face masks for protection against airborne pathogens—One size does not fit all: An observational study. Crit. Care Resusc. J. Australas. Acad. Crit. Care Med. 2010, 12, 24–27. [Google Scholar]
- Manganyi, J.; Wilson, K.S.; Rees, D. Quantitative respirator fit, face sizes, and determinants of fit in South African diagnostic laboratory respirator users. Ann. Work. Expo. Heal. 2017, 61, 1154–1162. [Google Scholar] [CrossRef] [PubMed]
- Derrick, J.; Chan, Y.; Gomersall, C.; Lui, S. Predictive value of the user seal check in determining half-face respirator fit. J. Hosp. Infect. 2005, 59, 152–155. [Google Scholar] [CrossRef] [PubMed]
- Lam, S.C.; Lui, A.K.F.; Lee, L.Y.; Lee, J.K.; Wong, K.; Lee, C.N. Evaluation of the user seal check on gross leakage detection of 3 different designs of N95 filtering facepiece respirators. Am. J. Infect. Control. 2016, 44, 579–586. [Google Scholar] [CrossRef] [PubMed]
- Danyluk, Q.; Hon, C.-Y.; Neudorf, M.; Yassi, A.; Bryce, E.; Janssen, B.; Astrakianakis, G. Health care workers and respiratory protection: Is the user seal check a surrogate for respirator fit-testing? J. Occup. Environ. Hyg. 2011, 8, 267–270. [Google Scholar] [CrossRef] [PubMed]
- Wilkinson, I.J.; Pisaniello, D.; Ahmad, J.; Edwards, S. Evaluation of a large-scale quantitative respirator-fit testing program for healthcare workers: Survey results. Infect. Control. Hosp. Epidemiol. 2010, 31, 918–925. [Google Scholar] [CrossRef] [PubMed]
- Or, P.; Chung, J.; Wong, T. Does training in performing a fit check enhance N95 respirator efficacy? Work. Health Saf. 2012, 60, 511–515. [Google Scholar] [CrossRef]
- Chughtai, A.A.; Seale, H.; Rawlinson, W.D.; Kunasekaran, M.; MacIntyre, C.R. Selection and Use of Respiratory Protection by Healthcare Workers to Protect from Infectious Diseases in Hospital Settings. Ann. Work. Expo. Health 2020, 64, 368–377. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tabah, A.; Ramanan, M.; Laupland, K.B.; Buetti, N.; Cortegiani, A.; Mellinghoff, J.; Morris, A.C.; Camporota, L.; Zappella, N.; Elhadi, M.; et al. Personal protective equipment and intensive care unit healthcare worker safety in the COVID-19 era (PPE-SAFE): An international survey. J. Crit. Care 2020, 59, 70–75. [Google Scholar] [CrossRef] [PubMed]
- Zhuang, Z.; Coffey, C.C.; Ann, R.B. The effect of subject characteristics and respirator features on respirator fit. J. Occup. Environ. Hyg. 2005, 2, 641–649. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Shen, H.; Wu, G. Racial Differences in Respirator Fit Testing: A Pilot Study of Whether American Fit Panels are Representative of Chinese Faces. Ann. Occup. Hyg. 2007, 51, 415–421. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Spies, A.; Wilson, K.S.; Ferrie, R. Respirator fit of a medium mask on a group of South Africans: A cross-sectional study. Environ. Health 2011, 10, 17. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Germonpre, P.; Van Rompaey, D.; Balestra, C. Evaluation of Protection Level, Respiratory Safety, and Practical Aspects of Commercially Available Snorkel Masks as Personal Protection Devices Against Aerosolized Contaminants and SARS-CoV2. Int. J. Environ. Res. Public Health 2020, 17, 4347. [Google Scholar] [CrossRef] [PubMed]
Table 1.
Baseline characteristics.
Table 1.
Baseline characteristics.
| Variable | Values |
|---|
| Age in years mean (std) | 45.7 (11.9) |
| Height mean cm mean (std) | 170 (10.6) |
| Weight mean kg mean (std) | 76.6 (18.9) |
| BMI derived mean (std) | 26.3 (5.3) |
| Gender (n = 59) n (%) | 36 (61.0) |
| Female | 36 (61.0) |
| Male | 23 (39.0) |
| Facial hair (n = 59) n (%) | 7 (11.9) |
| Ethnicity (n = 51) n (%) | |
| Asian | 15 (29.4) |
| Oceanian | 14 (27.5) |
| Southeast Asian | 14 (27.5) |
| European | 11 (21.6) |
| African | 2 (4.0) |
| Years in healthcare mean (std) | 21.6 (2.8) |
| First infectious diseases (first ID) work exposure | |
| Years since first ID median no. years median (IQR) | 13.5 (11–25) |
| Role of healthcare worker (HCW) (n = 59) n (%) | |
| Nurse | 28 (47.5) |
| Doctor | 31 (52.5) |
| Head/neck/face variant (n = 54) n (%) | |
| Nil previous head, neck or face change/anomaly | 52 (96.3) |
| Previous surgery | 0 (0) |
| Congenital anomaly | 1 (1.8) |
| Dental implants | 1 (1.8) |
| Weight change >10 kg past 3 years (n = 54) n (%) | |
| ‘No’ weight change | 46 (85.2) |
| ‘Yes’ to weight change | 8 (14.8) |
Table 2.
Fit check vs. formal fit test contingency table (n = 58).
Table 2.
Fit check vs. formal fit test contingency table (n = 58).
| Fit Check vs. Fit Test | Fit Test Seal | Fit Test Leak | Total |
|---|
| Fit Check Seal | 14 | 27 | 41 |
| Fit Check Leak | 4 | 13 | 17 |
| Total | 18 | 40 | 58 |
Table 3.
Fit check pass rate for initial mask application.
Table 3.
Fit check pass rate for initial mask application.
| Sensitivity | 77.8% (CI 23.2–92.2) |
| Specificity | 32.5% (CI 23.2–39.0) |
| Positive predictive value | 34.1% (CI 25.0–40.5) |
| Negative predictive value | 76.5% (CI 54.5–91.7) |
Table 4.
P2/N95 respirators by type used in first formal fit test.
Table 4.
P2/N95 respirators by type used in first formal fit test.
|
Respirator Type | Pass Fit Test 1
n (%) | Pass Fit Test 1
n (%) | Mask 1 Selection
n (%) | Fit Factor
Median [IQR] |
|---|
| 1860 | 7/18 (38.9) | 2/40 (5.0) | 9/58 (15.6) | 148 (50–200) |
| 1860s | 1/18 (5.6) | 3/40 (7.5) | 4/58 (6.9) | 69.5 (10–86) |
| 8210 | 1/18 (5.6) | 3/40 (7.5) | 4/58 (6.9) | 89 (46–200) |
| 8110s | 3/18 (16.7) | 3/40 (7.5) | 6/58 (10.3) | 61.5 (50–80) |
| Halyard (Regular) | 1/18 (5.6) | 10/40 (25.0) | 11/58 (19) | 17 (7–36) |
| Halyard (Small) | 3/18 (16.7) | 9/40 (22.5) | 12/58 (20.7) | 29 (18–124) |
| Proshield | 2/18 (11.1) | 10/40 (25.0) | 12/58 (20.7) | 21 (10–50) |
Table 5.
Survey Results by Category.
Table 5.
Survey Results by Category.
|
Category |
Entry Survey Response | Result
n |
Exit Survey Response | Result
n (%) |
|---|
Experience
and Exposure | Respondents who had cared for patients with confirmed or suspected tuberculosis (TB) during their career | 35/49 (71.4) | | |
| | No previous fit test experience | 49/53 (92.5) | | |
Respirator
Usage | Respondents who had rarely or never worn a P2/N95 respirator during routine work prior to COVID-19 pandemic | 48/53 (90.6) | | |
| Training | Respondents who reported minimal or no training, or not enough training, for fit check of P2/N95 respirators prior to COVID-19 pandemic | 43/52 (82.7) | | |
| Importance | Respondents who rated fit testing as absolutely essential or very important prior to being surveyed. | 34/52 (65.4) | Respondents who rated fit testing as absolutely essential or very important on exit survey | 42/44 (95.5) |
| Opinions | Respondents who felt completely safe or somewhat safe with the PPE in the hospital prior to COVID-19 pandemic | 12/53 (22.6) | Respondents who felt completely safe or somewhat safe with the PPE in the hospital on exit survey | 29/44 (65.9) |
| User Seal | Respondents who received fit check training of P2/N95 respirators during COVID-19 pandemic | 39/44 (88.6) | Respondents who believed they could achieve a user seal with an available P2/N95 respirator after fit testing | 36/44 (81.8) |
| Respondents who believed they could achieve a user seal with an available P2/N95 respirator prior to fit testing | 20/51 (39.2) |
| Satisfaction | Respondents who were satisfied with the fit testing that was conducted on the study day | 44/44 (100) | | |
| Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).