Complex Regional Pain Syndrome: Current Practice Management and Referral Trends in a Closed Healthcare System
Abstract
:1. Introduction
2. Materials and Methods
3. Results
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Goh, E.L.; Chidambaram, S.; Ma, D. Complex regional pain syndrome: A recent update. Burn. Trauma 2017, 5. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Guthmiller, K.B.; Varacallo, M. Complex Regional Pain Syndrome (CRPS), Reflex Sympathetic Dystrophy (RSD). In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2020. [Google Scholar]
- Birklein, F.; Dimova, V. Complex regional pain syndrome–Up-to-date. Pain Rep. 2017, 2. [Google Scholar] [CrossRef] [PubMed]
- Norli, E.S.; Brinkmann, G.H.; Kvien, T.K.; Bjørneboe, O.; Haugen, A.J.; Nygaard, H.; Mjaavatten, M.D. Standards for the diagnosis and management of complex regional pain syndrome: Results of a European Pain Federation task force. Eur. J. Pain 2019, 23, 641–651. [Google Scholar] [CrossRef] [Green Version]
- Turner-Stokes, L.; Goebel, A. Complex regional pain syndrome in adults: Concise guidance. Clin. Med. 2011, 11, 596–600. [Google Scholar] [CrossRef] [PubMed]
- Hogan, C.J.; Hurwitz, S.R. Treatment of complex regional pain syndrome of the lower extremity. J. Am. Acad. Orthop. Surg. 2002, 10, 281–289. [Google Scholar] [CrossRef] [PubMed]
- Aim, F.; Klouche, S.; Bauer, T.; Hardy, P. Efficacy of vitamin C in preventing complex regional pain syndrome after wrist fracture: A systematic review and meta-analysis. Orthop. Traumatol. Surg. Res. 2017, 103, 465–470. [Google Scholar] [CrossRef] [PubMed]
- Shibuya, N.; Humphers, J.; Agarwal, M.; Jupiter, D. Efficacy and Safety of High-dose Vitamin C on Complex Regional Pain Syndrome in Extremity Trauma and Surgery Systematic Review and Meta-Analysis. J. Foot Ankle Surg. 2013, 52, 62–66. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- De Mos, M.; Huygen, F.J.P.M.; Van Der Hoeven-Borgman, M.; Dieleman, J.P.; Stricker, B.H.C.; Sturkenboom, M.C.J.M. Referral and treatment patterns for complex regional pain syndrome in the Netherlands. Acta Anaesthesiol. Scand. 2009, 53, 816–825. [Google Scholar] [CrossRef] [PubMed]
- Grieve, S.; Llewellyn, A.; Jones, L.; Manns, S.; Glanville, V.; McCabe, C.S. Complex regional pain syndrome: An international survey of clinical practice. Eur J. Pain 2019, 23, 1890–1903. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bharwani, K.D.; Dirckx, M.; Huygen, F.J. Complex regional pain syndrome: Diagnosis and treatment. BJA Educ. 2017, 17, 262–268. [Google Scholar] [CrossRef] [Green Version]
- Iolascon, G.; de Sire, A.; Moretti, A.; Gimigliano, F. Complex regional pain syndrome (CRPS) type I: Historical perspective and critical issues. Clin. Cases Miner. Bone Metab. 2015, 12 (Suppl. 1), 4–10. [Google Scholar] [CrossRef]
- Harden, R.N.; Bruehl, S.; Perez, R.S.; Birklein, F.; Marinus, J.; Maihofner, C.; Mogilevski, M. Validation of proposed diagnostic criteria (the “Budapest Criteria”) for Complex Regional Pain Syndrome. Pain 2010, 150, 268–274. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Perez, R.S.; Zollinger, P.E.; Dijkstra, P.U.; Thomassen-Hilgersom, I.L.; Zuurmond, W.W.; Rosenbrand, K.C.; Geertzen, J.H. Evidence based guidelines for complex regional pain syndrome Type 1. BMC Neurol. 2010, 10, 1–14. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Misidou, C.; Papagoras, C. Complex Regional Pain Syndrome: An Update. Mediterr. J. Rheumatol. 2019, 30, 16–25. [Google Scholar] [CrossRef] [PubMed]
- Lo, J.; Cavazos, J.; Christopher, B. Management of Complex Regional Pain Syndrome. In Baylor University Medical Center Proceedings; Taylor & Francis: Abingdon, UK, 2017; Volume 30, pp. 286–288. [Google Scholar]
- Gallo, A.C.; Codispoti, V.T. Complex regional pain syndrome type II associated with lumbosacral plexopathy: A case report. Pain Med. 2010, 11, 1834–1836. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Verdolin, M.H.; Stedje-Larsen, E.T.; Hickey, A.H. Ten consecutive cases of complex regional pain syndrome of less than 12 months duration in active duty United States military personnel treated with spinal cord stimulation. Anesth. Analg. 2007, 104, 1557–1560. [Google Scholar] [CrossRef] [PubMed]
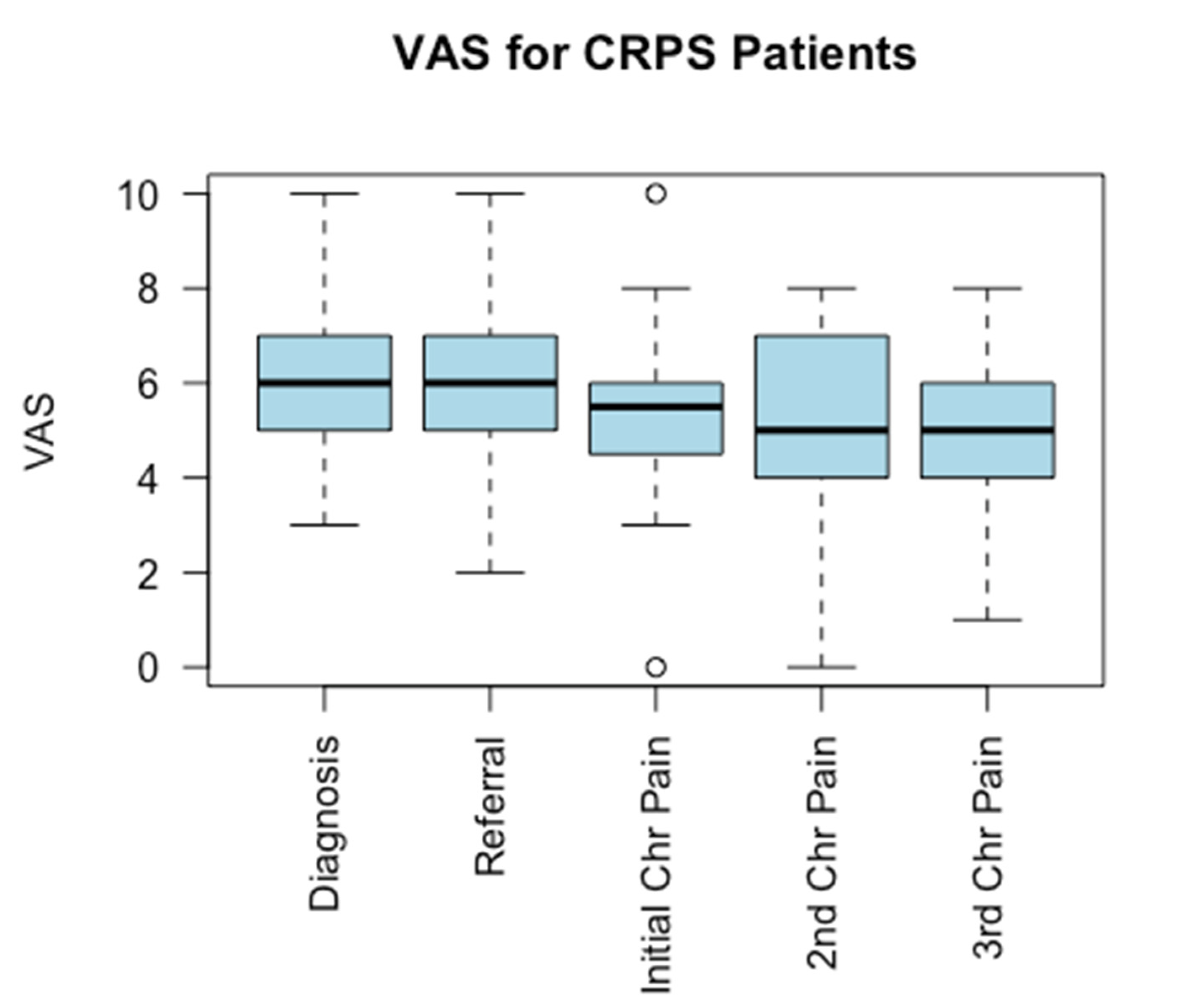
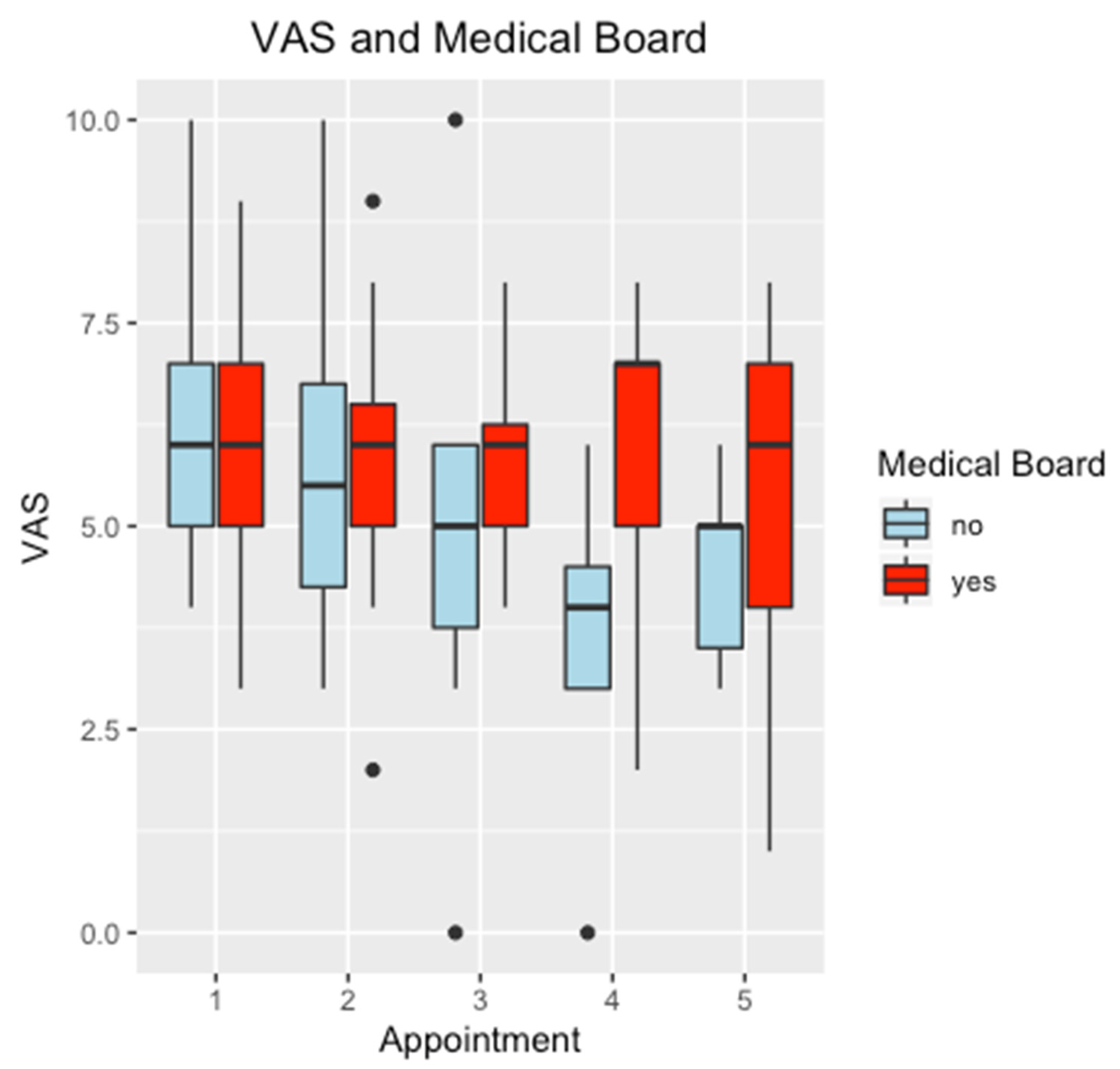
| Case | Injury |
|---|---|
| 1 | Shoulder AC Joint Arthritis |
| 2 | Partial Rotator Cuff Tear |
| 3 | Thumb Ulnar Collateral Ligament Tear |
| 4 | Forearm Crush and Compartment Syndrome |
| 5 | Fifth Metacarpal Fracture |
| 6 | Elbow Lateral Epicondylitis |
| 7 | Distal Humerus Fracture |
| 8 | Distal Radius Fracture |
| 9 | Scaphoid Fracture and Perilunate Dislocation |
| 10 | Cubital Tunnel Syndrome Surgery for Shrapnel to Shoulder |
| 11 | Second Phalanx Fracture |
| 12 | Bilateral Thoracoscopic Sympathectomy |
| 13 | Traumatic Brachial Plexus Injury and T7 Compression Fracture |
| 14 | Bilateral Plantar Fasciitis |
| 15 | Atraumatic Anterior Tibia Pain |
| 16 | Patellofemoral Chondromalacia |
| 17 | Stepped on a Sea Urchin |
| 18 | Atraumatic Right Ankle Pain |
| 19 | Lateral Ankle Sprain |
| 20 | L5 Corpectomy and PSF L4-S1 |
| 21 | Exertional Compartment Syndrome |
| 22 | Cavus Foot Reconstruction |
| 23 | Lapidus Procedure for Hallux Valgus and Hypermobility |
| 24 | Foot Pain after Ruck March |
| 25 | Retrocalcaneal Exostectomy and Debridement of Achilles Tendon |
| 26 | Base of the Fifth Metatarsal Avulsion |
| Patient | Time from Diagnosis to Referral | Time from Injury to Diagnosis | Time from Injury to Referral |
|---|---|---|---|
| 1 | 0 | 686 | 686 |
| 2 | 98 | 148 | 50 |
| 3 | 355 | 419 | 64 |
| 4 | 6 | 60 | 54 |
| 5 | 0 | 613 | 613 |
| 6 | 0 | 1888 | 1888 |
| 7 | 14 | 144 | 158 |
| 8 | 0 | 130 | 130 |
| 9 | 0 | 60 | 60 |
| 10 | 0 | 375 | 375 |
| 11 | 6 | 61 | 67 |
| 12 | 105 | 19 | 124 |
| 13 | 0 | 57 | 57 |
| 14 | 32 | 38,649 | 38,617 |
| 15 | 50 | 40,552 | 40,502 |
| 16 | 0 | 39,011 | 39,011 |
| 17 | 23 | 78 | 55 |
| 18 | 442 | 38,712 | 39,154 |
| 19 | 0 | 580 | 580 |
| 20 | 109 | 159 | 50 |
| 21 | 0 | 56 | 56 |
| 22 | 15 | 45 | 30 |
| 23 | 0 | 97 | 97 |
| 24 | 6 | 73 | 67 |
| 25 | 54 | 180 | 126 |
| 26 | 104 | 359 | 255 |
| Remained on Active Duty (Mean ± std Deviation) | Medical Release (Mean ± std Deviation) | p Value | |
|---|---|---|---|
| Diagnosis to referral (days) | 32 ± 94 | 69 ± 113 | 0.312 |
| Injury to diagnosis (days) | 135 ± 504 | 256 ± 495 | 0.519 |
| Injury to referral (days) | 135 ± 505 | 255 ± 496 | 0.521 |
| All (N = 26) | Remained on Active Duty (N = 10) | Medical Release (N = 16) | p Value | |
|---|---|---|---|---|
| Physical therapy | 26/26 | 10 | 16 | 1 |
| Gabapentin | 21/26 | 8 | 13 | 0.657 |
| Chronic narcotics | 12/26 | 2 | 10 | 0.042 |
| Acetaminophen | 11/26 | 4 | 7 | 0.589 |
| NSAIDs | 11/26 | 4 | 7 | 0.589 |
| Topical lidocaine | 11/26 | 4 | 7 | 0.589 |
| Stellate ganglion or sympathetic block | 10/26 | 4 | 6 | 0.609 |
| Amitripyline | 9/26 | 3 | 6 | 0.517 |
| Acupuncture | 8/26 | 1 | 7 | 0.081 |
| Peripheral nerve block | 4/26 | 1 | 3 | 0.496 |
| Spinal cord stimulator | 4/26 | 1 | 3 | 0.496 |
| Duloxetine | 3/26 | 0 | 3 | 0.215 |
| Vitamin C | 1/26 | 1 | 0 | 0.385 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zale, C.; Hansen, J.; Ryan, P. Complex Regional Pain Syndrome: Current Practice Management and Referral Trends in a Closed Healthcare System. Osteology 2021, 1, 39-47. https://doi.org/10.3390/osteology1010004
Zale C, Hansen J, Ryan P. Complex Regional Pain Syndrome: Current Practice Management and Referral Trends in a Closed Healthcare System. Osteology. 2021; 1(1):39-47. https://doi.org/10.3390/osteology1010004
Chicago/Turabian StyleZale, Connor, Joshua Hansen, and Paul Ryan. 2021. "Complex Regional Pain Syndrome: Current Practice Management and Referral Trends in a Closed Healthcare System" Osteology 1, no. 1: 39-47. https://doi.org/10.3390/osteology1010004
APA StyleZale, C., Hansen, J., & Ryan, P. (2021). Complex Regional Pain Syndrome: Current Practice Management and Referral Trends in a Closed Healthcare System. Osteology, 1(1), 39-47. https://doi.org/10.3390/osteology1010004





