Abstract
Interstitial cystitis/bladder pain syndrome (IC/BPS) is a chronic condition characterized by pelvic pain coupled with urinary frequency and urgency. The underlying cause of IC/BPS is unknown; there is no cure. Dietary components exacerbate symptoms. The Anti-Inflammatory Diet for Interstitial Cystitis (AID-IC) employs a randomized, crossover design to evaluate the effect of a plant-based, low saturated fat diet on the quality of life of women with IC/BPS. Insights on the implementation of the protocol and reflections on the facilitators and barriers experienced during the pilot study follow. The logistics of the protocol proved time-consuming; however, the barriers were surmountable. Quantitative and qualitative findings suggest that the AID-IC therapeutic diet may have lessened symptoms and improved the quality of life for many of the women in the study.
1. Introduction
Interstitial cystitis/bladder pain syndrome (IC/BPS) is a chronic condition affecting more than 8 million women around the world [1,2]. Prevalence estimates vary greatly, ranging from 4.5 to 440 per 100,000 [3,4,5]. IC/BPS is characterized by pelvic pain, pressure, or discomfort coupled with daytime urinary frequency (10+) or urgency associated with pain, pressure, discomfort, and fear of wetting [6].
The underlying cause is unknown; there is no cure [6]. Presentation includes both periods of severe pain and lower urinary tract symptoms (flares) and periods of remission. Flares are described as mild to severe intensity. Patients report flare frequencies of daily to less than one per year [6,7] and durations of minutes to years [1,6,8]. When symptoms are severe, individuals may need to stay home from work or school, restrict socialization, and limit sexual encounters [8]. Women with IC/BPS also experience increased frequency of psycho-social trauma and suicidal tendencies [7]. Treatment may include a combination of medications, neurostimulation, physical therapy, and dietary modifications [8].
Chronic inflammation is a hallmark characteristic of IC/BPS [9,10]. Studies indicate that IC/BPS patients present with elevated blood and urine levels of proinflammatory cytokines. Jiang et al. examined serum samples from 30 IC/BPS patients and 26 controls and found significantly higher levels of C-reactive protein (CRP), interleukin (IL)-1B, IL-6, IL-8, and tumor necrosis factor-alpha (TNF-a) among those with IC/BPS [10]. Increased serum CRP levels in patients diagnosed with IC/BPS, compared with controls, were also reported by Chung and colleagues [11]. In a more recent study by Jiang et al., urine inflammatory markers were investigated for their IC/BPS diagnostic potential. This group reported significantly elevated urine levels of multiple cytokines in 127 IC/BPS patients versus 28 controls. Further, cytokine levels were significantly correlated with clinical characteristics, including self-reported symptom and pain scores [12].
For decades, individuals with IC/BPS have reported that the consumption of certain foods and beverages increases symptomology [13,14,15,16]. Clinical experience prompted the collection of commonly bothersome foods via a series of self-report surveys [13,14,15,16,17,18]. In 2014, Shorter et al. published a validated survey yielding a list of foods and beverages that the vast majority (90%) of women with IC/BPS appear to find bothersome [18]. Items include coffee and tea (caffeinated and decaffeinated), soda, alcohol, citrus juices and fruits, cranberry juice, tomatoes and tomato products, hot peppers, spicy foods, and foods and beverages containing artificial sweeteners [18]. There are also individual variations in the food/beverage sensitivities [18]. Given these findings, dietary modifications were included in clinical guidelines for six medical societies across the globe [6,19,20,21,22,23].
The pathophysiology underlying the association between symptoms and dietary components is not well understood in IC/BPS. One theory is that damage to the bladder urothelial barrier allows urinary solutes to invade the urothelium and produce noxious stimuli that provoke IC/BPS symptoms [24]. Others hypothesize that consumption of foods that irritate the gastrointestinal tract may stimulate nerves between the GI tract and the bladder; thereby, “neural cross-talk” produces bladder discomfort [25]. Nazif et al. purport that peripheral or central neural upregulation underlies the pathology of IC/BPS; specifically, the release of neurogenic inflammation from sensory nerves may be a catalyst for the pain and urinary symptoms of this condition [26]. Elliott et al. discovered that artificial sweeteners activate T1R2/3 sweet taste receptors expressed in the bladder (human and rat), causing bladder smooth muscle contractions [27]. This may explain the sensitivity to artificial sweeteners reported by those with IC/BPS.
The potential role of diet as a contributing factor to diseases associated with chronic systemic inflammation has been suggested [28,29,30]. Shivappa et al. created the Dietary Inflammatory Index (DII), which rates the influence of foods, dietary components, or nutrients based on their anti-inflammatory property. The degree of inflammation was ranked by the magnitude of the effect of an item on six inflammatory biomarkers (IL-1β, IL-4, IL-6, IL-10, TNF-α, and C-reactive protein) [29]. Forty-five items were assigned DII scores on a scale of −1 to +1 (−1 = strongly anti-inflammatory, 0 = no effect, and +1 = strongly proinflammatory) [29]. A meta-analysis concluded that a high DII score is likely associated with the harmful inflammatory effects related to a variety of health outcomes [31]. The developers of the D-II refined the tool by including an energy adjustment calculation in the algorithm; the E-DII is the preferred tool for assessing the influence of dietary choices on chronic systemic inflammation [32].
Eating patterns that are high in saturated fat, cholesterol, protein, sugar, and salt coupled with regular consumption of ultra-processed foods are associated with a higher prevalence of chronic diseases with inflammatory components [28]. Studies suggest that dietary intake of saturated fat provokes inflammation by activating the Toll-like receptor (TLR)-4 cell-signaling pathways [33,34]. In a molecular dynamics study, it was found that the saturated fat palmitic acid (found in palm oil) produced TLR-4-induced changes to metabolism on a cellular level, as well as alterations in gene expression, lipid metabolic pathways, and membrane lipid composition. The authors purport this contributes to the inflammation related to high consumption of dietary saturated fats [35]. Oberbach et al. reported that saturated fatty acids produced considerable changes in bladder smooth muscle cells. Specifically, bladder inflammation and vascular changes in association with endothelial dysfunction were observed [36]. The authors suggested that these changes may be responsible for clinical symptoms of IC/BPS. Other researchers noted a relationship between the ratio of saturated to polyunsaturated intake and lower urinary tract symptoms [30,37]. Of note, Maserejian et al. reported that modifying the dietary intake of the ratio of saturated fat to polyunsaturated fat may help control urinary urgency and frequency in women [37]. A potential link between diets high in saturated fat and IC/BPS symptomology emerges [30,33,34,35,36].
The goal of the AID-IC pilot study was to investigate the efficacy of an anti-inflammatory diet as a complementary treatment for pharmacological therapies to manage symptom severity and, thereby, contribute to improved quality of life. To date, no studies have been conducted investigating the feasibility of diminishing IC/BPS symptom severity by influencing inflammatory activity; specifically, controlling lipid intake and increasing antioxidant intake. An overview of the design and findings of a pilot study conducted with women with IC/BPS is detailed below. Facilitators and barriers that emerged during the pilot are discussed and revisions to the study protocol are offered.
2. Materials and Methods
The AID-IC pilot study employed a mixed-methods, crossover design to evaluate the effect of a plant-based, low saturated fat diet on IC/BPS symptom mitigation. It was implemented across 11 months, January through November 2021. The AID-IC study employed an adapted version of the randomized, cross-over Anti-inflammatory Diet In Rheumatoid Arthritis (ADIRA) protocol, which investigated if an anti-inflammatory diet diminished rheumatoid arthritis symptoms and improved quality of life [38].
2.1. Development of AID-IC Therapeutic and Control Diets
2.1.1. AID-IC Therapeutic Diet
The AID-IC therapeutic diet incorporated specific foods found to be beneficial in controlling inflammation, while eliminating foods thought to increase inflammation. The E-DII was used to identify items with anti-inflammatory properties, such as foods rich in provitamin A carotenoids, vitamins C, D, and E, and certain spices (garlic, ginger, oregano, rosemary, and thyme) [29,32]. Foods and beverages identified by Shorter et al. as commonly bothersome foods for those with IC/BPS were restricted; for example, citrus foods, tomatoes and tomato products, and alcohol [18].
A typical plate included two ounces of protein, half a plate of vegetables, and a quarter plate of whole grains. Snacks consisted of fresh fruits. The only fat used in the prepared meals was olive oil. About 28% of kilocalories came from animal foods and none of the prepared meals included red meat. The AID-IC diet included cruciferous vegetables, low-fat dairy products, whole grains, nuts and berries, oily fish (3–4 times per week), and meatless entrees (1–2 times per week). Each entree provided about 500 kilocalories and one third of the RDAs for micronutrients. To confirm nutritional composition, meals were entered into a nutrition analysis software (EshaTrak, Salem, OR, USA) and modifications were made, as needed.
The research team contracted with a commercial service for meal production and delivery (MealPro, Sacramento, CA, USA). The prepared meals were provided for lunch and dinner on the five weekdays (one-week cycle menu). The portion sizes were pre-established and the meals pre-cooked. Each meal was plated in a vacuum-sealed, microwave/oven-safe container. The packaging allowed for meals to be stacked for cold storage. Two weeks of meals were delivered in thermal boxes on dry ice.
2.1.2. Control Diet
The control diet was the standard nutrition counseling protocol for those with IC/BPS, specifically the restriction of both individual and commonly bothersome IC/BPS. Registered dietitian nutritionists (RDNs) employed the evidence-based nutrition care process, which includes crafting a nutrition intervention based on the findings of a nutrition assessment. During the assessment, among other things, kilocalories required to meet nutritional needs and maintain current weight were calculated. Nutritional needs related to other health conditions were combined with IC/BPS recommendations. Due to budgetary limitations of the pilot study, participants were responsible for providing their own meals during the control diet phase of the study.
2.2. Recruitment and Screening
Enrollment was conducted from January to February 2021. A convenience sample of women (18 years or older) with physician-diagnosed IC/BPS was referred by the Idaho Urologic Institute (IUI, Meridian, ID, USA), a specialty medical practice. Given that food sensitivities affect nearly all women with IC/BPS (compared to less than half of men with the condition) the protocol only included women. In addition, women were excluded if IC/BPS symptoms currently demanded active medical attention. Other exclusion criteria included being intolerant, allergic, or unwilling to consume the food items in the AID-IC protocol, life-threatening diseases, pregnancy, or lactation (see Table 1).

Table 1.
Inclusion and exclusion criteria for AID-IC pilot study.
2.3. Intervention
Participants were assigned study IDs, which were sequentially entered into an online randomizer (gigacalculator.com, accessed on 15 February 2021). Group 1 received the AID-IC diet for 10 weeks, while Group 2 was assigned to the control diet. After a two-week washout period, Group 1 received the control diet and Group 2 the AID-IC diet. All of the participants were instructed to go back to their usual diet during the two-week washout period.
Participants were assigned to one of three RDNs, and they met with the dietitian four times during the study. At the first visit, the RDNs reviewed the study details, obtained written consent, and performed a basic medical history. In addition, during visits one and three, the dietitians reviewed study protocols (therapeutic or control diet), advised participants to restrict trigger foods, computed kilocalories needed to maintain body weight, and provided nutrition counseling. Participants were provided printed and video versions of educational materials for the control or test diet (meal plans, recipes, and other information in plain language). At all visits, the RDNs walked participants through the dietary recall and disease activity surveys.
Adherence was monitored via periodic correspondence, either in person or telephonically, with the RDN. Participants were encouraged to report any side effects to both the RDN and their IUI health care provider. Table 2 provides an overview of enrollment and data collection tasks stratified by study time points per SPIRIT requirements.

Table 2.
Enrollment and data collection stratified by study time points (SPIRIT requirements).
2.4. Data Collection
2.4.1. Health and Dietary Information
A basic health history was collected by the RDNs, including comorbid conditions, prescription and over-the-counter medications, supplements, IC/BPS trigger foods, height, weight, and activity level. Body mass index (BMI) was calculated. This data was entered into an online survey created in Qualtrics XM (Provo, UT, USA). Using the Mifflin-St Jeor equation, daily kilocalorie needs were calculated for each individual. In addition, dietary intake data for 24-h recalls (one weekday and one weekend day) were collected using the Automated Self-Administered 24-h (ASA24) Dietary Assessment Tool, version 2018, developed by the National Cancer Institute, Bethesda, MD, USA (https://epi.grants.cancer.gov/asa24/respondent/citations.html, accessed on 13 November 2020).
2.4.2. Disease Activity
Three validated tools were employed to collect participant data on the degree of pain, urinary symptoms, sexual dysfunction, and quality of life—the 9-item Genitourinary Pain Index (GUPI, degree of pain and urinary symptoms), 19-item Female Sexual Functioning Inventory (FSFI, pain and frequency during and after intercourse), and 6-item RAND Interstitial Cystitis Epidemiology (RICE) Bladder Symptom Impact Scale (quality of life) [39,40,41]. The primary outcome data (beneficial changes in quality of life) were collected via the three surveys. The surveys were built on the Qualtrics XM platform and administered by the RDNs.
Blood samples were collected to evaluate inflammatory markers—one of the secondary outcomes of the study—four times, both pre/post-therapeutic diet and pre/post-control diet. Tests for three biomarkers were run, including tumor necrosis factor (TNF)-α, interleukin (IL)-1, and C-reactive protein. Given the location of the study, a contract phlebotomist was hired to draw and pack the samples, which were then transported by a courier service to a reference lab for development.
2.4.3. Palatability and Acceptability of AID-IC Therapeutic Diet
A 14-question survey, employing a 5-point Likert rating scale, was developed to assess the palatability and ease of adoption of the AID-IC therapeutic diet. A link to the survey was sent out through secure email five weeks into the first 10-week study period to all of the participants consuming the study diet. The participants were given one week to complete the survey. Reminder emails were sent as needed. The survey was adapted from a palatability and feasibility questionnaire used to assess a Paleolithic diet among a group of Australian women [42]. The individual palatability of each of the 10 AID-IC therapeutic meals was rated from very unpleasant to very tasty. One question rated the overall satiety that the diet provided, ranging from very full and satisfied to very hungry and dissatisfied. Two questions focused on adaptation of the study diet; responses ranged from very easy to very difficult. There was one question rating the ease in coping with social situations while eating the study diet, ranging from very easy to very hard. The survey was also built in Qualtrics.
2.4.4. Participant Experience
Upon completion of the nutrition intervention, online focus groups were conducted to collect qualitative data on the participant experience. The 1 1/2-h focus group was conducted via Zoom and facilitated by one of the RDNs. A moderator’s guide was developed with questions on five topics: (1) meals (delivered and self-prepared) and adherence, (2) IC/BPS symptoms (flares, pain, urgency/frequency, and need for medical appointments), (3) quality of life (intimacy, activities of daily living, and activity level), (4) things learned (triggers, general eating patterns, and other), and (5) recommendations and miscellaneous comments. A USD 50 Amazon gift card was offered as an incentive. Transcripts were downloaded and personal identifying information removed.
2.5. Data Analysis
SPSS v. 27 (IBM, Chicago, IL, USA) was employed to conduct statistical analysis. Given the small sample size, normality was analyzed using the Shapiro–Wilk test. Descriptive statistics were calculated. T-tests were employed to calculate significant differences in dietary intakes pre/post-control diet and pre/post-test. ANOVAs were used to evaluate significant relationships between changes in disease activity (symptomatology, pain, and quality of life) and pre/post-therapeutic diet and pre/post-control diet. Rows containing missing data were excluded from the analysis. E-DII scores (using 28/45 items) for each participant’s pre/post-intervention were calculated using the protocol detailed by the authors of the tool [29,32]. Focus group findings were narratively compiled.
3. Results
3.1. Participant Flow and Demographics
Across two months, 37 women were recruited; 35.48% were excluded because of dietary restrictions (gluten-free, does not eat carbohydrates, or only eats organic foods), demands of the study protocol (in-person blood draws and distance to the facility), and recently learning of pregnancy. Of the remaining 26 women, 8 did not respond to appointment scheduling requests or did not show for initial screening appointments. The remaining 18 participants were randomized; six of them dropped out during the screening process (demands of protocol, out of town travel, or desire to lose weight).
Twelve women took part in the pilot study; 10 completed the intervention (83.33%). One reported that adherence to the therapeutic diet protocol was challenging (first 10 weeks); the other found the prepared meals unpalatable (second 10 weeks). None of the participants reported adverse reactions (see Figure 1).
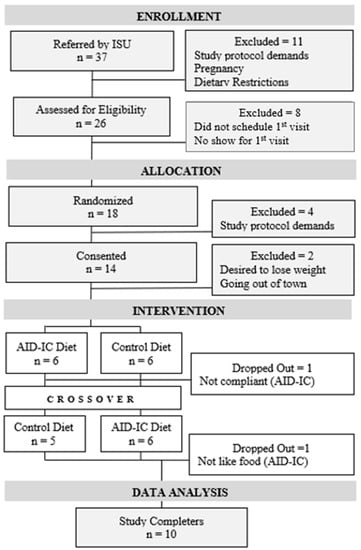
Figure 1.
Participant flow chart (CONSORT).
All of the participants identified as White/Non-Hispanic; they were primarily over 45 years, with incomes above USD 50,000 (8/10, 80%). Most of the women were overweight/obese (8/10, 80%). Comorbid pain conditions (chronic headache, fibromyalgia, and vulvodynia) were reported by 70% of the cohort. The most common IC/BPS trigger foods were tomatoes/tomato products—60% reported these items as bothersome. Half of the participants also identified alcohol and spicy foods as bothersome, and 30% citrus food and coffee (see Table 3).

Table 3.
Participant demographics, comorbid conditions, and trigger foods.
3.2. Nutrient Composition Therapeutic vs. Control Diets
Table 4 provides descriptive statistics for the E-DII scores and therapeutic/control diets. The dataset met the test of normality, Shapiro–Wilk test < 0.01. Comparison of means of the nutrient composition of the control vs. therapeutic diets yielded only one significant change in intake. Vitamin C intake significantly decreased while participants were on the test diet (p = 0.02). No significant associations emerged for intakes pre-/post-control diet.

Table 4.
Descriptive statistics and results of paired t-tests of dietary nutrient composition.
Testing effect of timepoint (control vs. therapeutic diet) was conducted on ASA24 dietary intake data. When participants were on the therapeutic diet, intakes of solid fats (p ≤ 0.01), saturated fat (p = 0.02), and refined grains (p ≤ 0.01) significantly decreased, and seafood (p ≤ 0.01) and vitamin B12 (p = 0.03) significantly increased. There were no significant differences for intakes of other macro- and micro-nutrients. Findings were confirmed with the Tukey’s test. Calculations for individual participant found significant differences in nutrient intakes on therapeutic vs. control diets for three women. The off-study diets of the other participants were, thus, not significantly different from the therapeutic diet.
The E-DII scores ranged from −4.33 to 3.43 anti-inflammatory to proinflammatory, respectively. The mean E-DII score for participants on the AID-IC therapeutic diet was −1.50 (anti-inflammatory) and, for the control diet, was −0.98, which is also anti-inflammatory. The mean E-DII scores for the pre/post-test diets were significantly different (p = 0.05); however, no significant difference emerged between the pre/post-control diets. A simple linear regression was calculated to predict if the E-DII score was associated with the therapeutic diet (test vs. control diet). No significant association emerged.
Mean ratings were calculated for the responses to the acceptable and palatability survey. One participant selected the same rating for all of the questions. These outlier scores were not included in the analysis. The mean rating for one meal was tasty to very tasty (1.80 ± 0.93); of note, it was a meatless entrée. Seven meals were rated okay to tasty (mean ranges: 2.33 ± 1.23 to 2.8 ± 1.23). The two salmon meals ranked okay to a little unpleasant (3.00 ± 1.25, 3.20 ± 1.23). Means for the four acceptance factors were computed; they were satiety (1.78 ± 0.83, very full and satisfied), difficulty eating this way (2.11 ± 0.78, easy), difficulty adapting to eating plan (2.67 ± 0.87, easy to neutral), and difficulty eating this way coping with social situations (2.89 ± 0.78, easy to neutral).
3.3. Impact of Diet on Disease Activity
Both mean RICE and GUPI scores for those in the treatment group were lower than for those in the control group (11.33 vs. 12.56 and 5.00 vs. 4.50, respectively). The inverse was true for the FSFI scores; the treatment group scores were higher than those in the control group (5.0 vs. 4.5, respectively). A series of one-way between-subjects ANOVAs were conducted to compare the effect of the test and control diets on disease activity (scores of the three surveys administered pre/post-intervention vs. pre/post-control diet). The FSFI dataset met the test of normality, Shapiro–Wilk test (<0.03). Though not significant for the RICE and GUPI datasets, the Shapiro–Wilk statistic was below 1.96, which is sufficient to establish normality. Significant changes were found for three of the five factors evaluated in the RICE Bladder Symptom index. Interest in life (p < 0.01), social life (p = 0.04), and ability to fulfill home responsibilities (p = 0.01) significantly improved; the overall RICE score was also significant (p = 0.05). Differences in energy level and mood were not significant. Genitourinary Pain Index scores were significantly less for pain in the pubic or bladder area (p = 0.01), pain/burning during voiding (p = 0.01), and discomfort during/after intercourse (p = 0.01); however, the total GUPI subscores and overall score was not significant. Significant improvements for the Sexual Functioning Inventory scores included sexual desire/interest (p = 0.01), confidence that will become aroused (p = 0.01), and ability to maintain lubrication (p = 0.04). Table 5 provides descriptive statistics and results of paired T-tests for the totaled survey scores.

Table 5.
Descriptive statistics and results of paired T-tests of disease activity measures.
Four viable blood samples were analyzed for significant changes in three inflammatory biomarkers—TNF-alpha, IL-B, and C-reactive protein. ANOVAs failed to calculate because of the small dataset. Improper handling by the courier service resulted in tainted samples and insufficient data for the biomarkers. This incident was reported to the Institutional Review Board.
3.4. Patient Experience
A total of 10 out of the 12 women participated in the focus groups. The AID-IC therapeutic diet lessened IC/BPS symptoms and improved quality of life for 70% of the focus group participants. Newly diagnosed women appeared to find the intervention more beneficial. Participants also noted that the AID-IC diet served as an elimination diet; when they returned to preintervention eating patterns, they were able to identify individual trigger foods. Some participants said that, postintervention, they continued to follow the AID-IC diet, using the patient education materials as a guide.
Participants found the meals very ample. Some consumed leftover portions of the delivered meals on the weekends. Others shared that, due to the satiety of the meals, they did not desire between-meal snacks. Concerns included the mushiness of the vegetables and lack of variety (consumption of the same menu items every week for 10 weeks).
4. Discussion
Despite dietary modifications being considered standard care for this population [6,19,20,21,22,23], there are only three published clinical trials that have investigated the efficacy of dietary changes for helping to manage IC/BPS symptoms [43,44,45]. A pilot study (n = 25) conducted by Hanley et al. included dietary modification as part of a multimodal intervention (behavioral, pharmacologic, and endoscopic) [43]. In addition to fluid restrictions, participants restricted acidic foods and those high in arylalkylamines. The researchers, however, reported no discrete findings on the influence of the dietary modifications [43]. A double-blind, placebo-controlled trial (n = 30) evaluated the influence of caffeine on the exacerbation of IC/BPS symptomology. The intervention group consumed a caffeine pill (equivalent to one cup of coffee), the control group a placebo. No significant difference in pain or voiding volume was found between the two groups [44]. Oh-oka reported on the findings of a small (n = 30), 1-year clinical trial employing an intensive systematic dietary manipulation (restriction of commonly bothersome foods for individuals with IC/BPS). Statistically significant improvements (p < 0.05) were reported for all evaluated factors after three months and throughout the final nine months of the trial [45]. None of the above studies have been replicated.
The lack of clinical trials evaluating dietary adaptations for those with IC/BPS was a facilitator. Many participants expressed their appreciation to the researchers for conducting the study. The ADIRA model [38] of providing home-delivered meals also encouraged adherence; focus group participants spoke positively about the nominal meal preparation and ease of reheating the meals.
Both the testing effect of timepoint and DII score analyses demonstrate that the therapeutic diet achieved the goal of controlling for lipid intake and promoting the intake of anti-inflammatory nutrients and dietary components. Of note, the E-DII score range (4.33 to 3.43) was within the expected range for a dataset of 29 items; per Hébert et al., for 25–30 items, the expected range is from −5.5 to +5.5 [32]. More than 300 studies have been published verifying a relationship, albeit not causal, between the E-DII score and chronic systemic inflammation.
The disease activity scores for the RICE and GUPI (both subscales and overall) were indicative of lesser IC/BPS symptomatology for those on the therapeutic diet compared with the control diet. Scores for the FSFI, however, revealed an inverse relationship between the anti-inflammatory diet and sexual functioning scores. This may reflect the lack of power in the sample size and/or the influence of symptoms to confounders, e.g., stress and comorbid conditions.
The small sample size of this pilot study introduced the risk of a type II error. A power calculation can help address this weakness. Given the study design (two independent groups, binomial endpoint, alpha = 0.05), for an incidence of 50%, 116 participants are required. Recruitment from a single site also weakens the generalizability of the findings. The participant pool lacked racial/ethnic and socioeconomic diversity. Lebowitz et al. note that multi-site trials are more apt to yield heterogeneous participant samples. In addition, these authors emphasize the need for large, multi-site trials when evaluating optimal treatments among individuals with chronic conditions [46].
Based on the findings of this pilot study, the AID-IC protocol offers a feasible approach for assessing the impact of an anti-inflammatory diet among community-dwelling individuals with IC/BPS. Significant beneficial changes were found on the three disease activity surveys. Qualitative findings from focus group participants support these quantitative findings.
Strengths and Limitations
The utilization of RDNs was advantageous because of their training in both clinical care and program management. Furthermore, the strategy of having each RDN follow the same participants throughout the trial helped to establish a rapport, which has been found to be a benefit for urogynecological trials. Analysis of interviews with women considering enrolling in a study of uterine prolapse treatment (n = 8), for example, emphasized the importance of establishing rapport and building a positive relationship with the trial participants [47].
COVID-19 requirements during the study period included the option for telenutrition or in-person visits. Virtual visits were not a barrier to establishing rapport with the participants; others reported similar experiences with conducting clinical trials during COVID-19 restrictions [48]. The initial time allotted of one hour per data collection visit, however, was insufficient. Given the scope of the data collection efforts, most visits required 1 1/2-h per participant.
The prepared meals added an element of scientific control to the community-dwelling setting of this study; however, delivery issues emerged during the study. The first delivery date coincided with a winter snowstorm. Shipments were delayed due to weather; some meals arrived thawed and replacement meals had to be sent out. In addition, during the 10-week phases, many of the participants traveled. This required co-ordinating partial or full deliveries to alternative locations. These expenses had not been calculated into the study budget.
Menu procedural issues also emerged. The one-week cycle menu did not optimally mirror the dietary diversity that participants consumed before the trial. The Clemson University Cooperative Extension Service advocates for at least a 2-week cycle menu for community-dwelling individuals [49]. Other resources recommend at least a 4-week cycle menu to offer a varied diet desired by most individuals [50]. Moreover, of note, the frozen vegetables were described by focus group participants as “too mushy.” In a review article on frozen vegetable production, van der Sman provides eight recommendations, such as employing a “high temperature short time” blanching procedure to help prevent degradation of cell walls and maintain the texture of the vegetables [51]. The two salmon meals received the lowest taste ratings, perhaps because, in the state of Idaho (United States), freshly caught salmon is very accessible. The flash-frozen meal may have not been the same quality that participants typically consume.
The AID-IC protocol employed a two-week washout period compared with the three months used in the ADIRA study. Other dietary interventions have found promising outcomes with shorter washout periods. A clinical trial evaluating the efficacy of the elimination diet for women with migraines and irritable bowel syndrome found that a three-week washout period was adequate to produce measurable outcomes [52]. A longer washout period may have produced more significant differences between the therapeutic and control diet phases for the study outcome variables.
5. Conclusions
The AID-IC protocol offers a feasible model for evaluating dietary modifications for IC/BPS patients. Analysis of disease activity surveys and focus group findings demonstrate that the protocol lessened IC/BPS symptoms and improved the quality of life for many of the women in this study. A larger and more diverse sample is required to mitigate the risk of type II error and increase the generalizability of the findings. Improvements in menu design and meal production are also needed to optimize the impact of an anti-inflammatory diet.
Author Contributions
Conceptualization, B.G.; Methodology, B.G., C.B. and R.H.; Investigation, B.G., C.B., R.R., A.J., L.R. and R.H.; Writing—Original Draft Preparation, B.G.; Writing—Review and Editing, B.G., C.B., R.R., A.J., L.R. and R.H.; Supervision, B.G.; Project Administration, B.G. and C.B.; Funding Acquisition, B.G. All authors have read and agreed to the published version of the manuscript.
Funding
This project is supported by an award from the National Institute of General Medical Sciences, National Institutes of Health under grant number U54 GM104944.
Institutional Review Board Statement
The study was conducted according to the guidelines of the Declaration of Helsinki and approved by the Institutional Review Board of Idaho State University (IRB-FY2020-156, 13 March 2020).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Acknowledgments
The authors thank the staff at Connecting Health Innovations, especially Longgang Zhao, for help with the E-DII calculations.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Berry, S.H.; Elliott, M.N.; Suttorp, M.; Bogart, L.M.; Stoto, M.A.; Eggers, P.; Nyberg, L.; Clemens, J.Q. Prevalence of symptoms of bladder pain syndrome/interstitial cystitis among adult females in the United States. J. Urol. 2011, 186, 540–544. [Google Scholar] [CrossRef] [PubMed]
- Rahnama’I, M.S.; Javan, A.; Vyas, N.; Lovasz, S.; Singh, N.; Cervigni, M.; Pandey, S.; Wyndaele, J.J.; Taneja, R. Bladder pain syndrome and interstitial cystitis beyond horizon: Reports from the Global Interstitial Cystitis/Bladder Pain Society (GIBS) meeting 2019. Anesthesiol. Pain Med. 2020, 10, e101848. [Google Scholar] [CrossRef] [PubMed]
- Ito, T.; Miki, M.; Yamada, T. Interstitial cystitis in Japan. Br. J. Urol. 2001, 86, 634–637. [Google Scholar] [CrossRef] [PubMed]
- Bade, J.J.; Rijcken, B.; Mensink, H.J. Interstitial cystitis in The Netherlands: Prevalence, diagnostic criteria and therapeutic preferences. J. Urol. 1995, 154, 2035–2037. [Google Scholar] [CrossRef]
- Suskind, A.M.; Berry, S.H.; Ewing, B.A.; Elliott, M.N.; Suttorp, M.J.; Clemens, J.Q. The prevalence and overlap of interstitial cystitis/bladder pain syndrome and chronic prostatitis/chronic pelvic pain syndrome in men: Results of the RAND Interstitial Cystitis Epidemiology male study. J. Urol. 2013, 189, 141–145. [Google Scholar] [CrossRef]
- Hanno, P.M.; Burks, D.A.; Clemens, J.Q.; Dmochowski, R.R.; Erickson, D.; Fitzgerald, M.P.; Forrest, J.B.; Gordon, B.; Gray, M.; Mayer, R.D.; et al. AUA guideline for the diagnosis and treatment of interstitial cystitis/bladder pain syndrome. J. Urol. 2011, 185, 2162–2170. [Google Scholar] [CrossRef]
- McKernan, L.C.; Walsh, C.G.; Reynolds, W.S.; Crofford, L.J.; Dmochowski, R.R.; Williams, D.A. Psychosocial comorbidities in interstitial cystitis/bladder pain syndrome (IC/BPS): A systematic review. Neurourol. Urodyn. 2018, 37, 926–941. [Google Scholar] [CrossRef]
- Sutcliffe, S.; Bradley, C.S.; Clemens, J.Q.; James, A.S. Urologic chronic pelvic pain syndrome flares and their impact: Qualitative analysis in the MAPP Network. Int. Urogynecol. J. 2015, 26, 1047–1060. [Google Scholar] [CrossRef]
- Akiyama, Y. Biomarkers in interstitial cystitis/bladder pain syndrome with and without Hunner lesion: A review and future perspectives. Diagnostics 2021, 11, 2238. [Google Scholar] [CrossRef]
- Jiang, Y.H.; Peng, C.H.; Liu, H.T.; Kuo, H.C. Increased pro-inflammatory cytokines, C-reactive protein and nerve growth factor expressions in serum of patients with interstitial cystitis/bladder pain syndrome. PLoS ONE 2013, 8, e76779. [Google Scholar] [CrossRef]
- Chung, S.D.; Liu, H.T.; Lin, H.; Kuo, H.C. Elevation of serum c-reactive protein in patients with OAB and IC/BPS implies chronic inflammation in the urinary bladder. Neurourol. Urodyn. 2011, 30, 417–420. [Google Scholar] [CrossRef] [PubMed]
- Jiang, Y.H.; Jhang, J.F.; Hsu, Y.H.; Ho, H.C.; Wu, Y.H.; Kuo, H.C. Urine cytokines as biomarkers for diagnosing interstitial cystitis/bladder pain syndrome and mapping its clinical characteristics. Am. J. Physiol. Physiol. 2020, 318, F1391–F1399. [Google Scholar] [CrossRef] [PubMed]
- Koziol, J.A.; Clark, D.C.; Gittes, R.F.; Tan, E. The natural history of interstitial cystitis: A survey of 374 patients. J. Urol. 1993, 149, 465–469. [Google Scholar] [CrossRef]
- Interstitial Cystitis Association. Available online: www.ichelp.org/icdietsurvey (accessed on 31 December 2014).
- Warren, J.W.; Brown, J.; Tracy, J.K.; Langenberg, P.; Wesselmann, U.; Greenberg, P. Evidence based criteria for the pain of interstitial cystitis/painful bladder syndrome in women. Urology 2008, 71, 444–448. [Google Scholar] [CrossRef]
- Bassaly, R.; Downes, K.; Hart, S. Dietary consumption triggers in interstitial cystitis/bladder pain syndrome patients. Female Pelvic Med. Reconstr. Surg. 2011, 17, 36–39. [Google Scholar] [CrossRef]
- O’Hare, P.G., 3rd; Hoffmann, A.R.; Allen, P.; Gordon, B.; Salin, L.; Whitmore, K. Interstitial cystitis patients’ use and rating of complementary and alternative medicine therapies. Int. Urogynecol. J. 2013, 24, 977–982. [Google Scholar] [CrossRef]
- Shorter, B.; Ackerman, M.; Varvara, M.; Moldwin, R.M. Statistical validation of the Shorter-Moldwin Food Sensitivity Questionnaire for patients with interstitial cystitis/bladder pain syndrome. J. Urol. 2014, 191, 1793–1801. [Google Scholar] [CrossRef]
- ACOG Committee on Practice Bulletins—Gynecology. ACOG Practice Bulletin No. 51. Chronic pelvic pain. Obstet. Gynecol. 2004, 103, 589–605. [Google Scholar] [CrossRef]
- Haefner, H.K.; Collins, M.E.; Davis, G.D.; Edwards, L.; Foster, D.C.; Hartmann ED, H.; Kaufman, R.H.; Lynch, P.J.; Margesson, L.J.; Moyal-Barracco, M.; et al. The vulvodynia guideline. J. Low. Genit. Tract Dis. 2005, 9, 40–51. [Google Scholar] [CrossRef]
- Hanno, P.M.; Erickson, D.; Moldwin, R.; Faraday, M.M. Diagnosis and treatment of interstitial cystitis/bladder pain syndrome: AUA guideline amendment. J. Urol. 2015, 193, 1545–1553. [Google Scholar] [CrossRef]
- Homma, Y.; Ueda, T.; Tomoe, H.; Interstitial cystitis guideline committee. Japanese Urological Association. Clinical guidelines for interstitial cystitis and hypersensitive bladder syndrome. Int. J. Urol. 2009, 16, 597–615. [Google Scholar] [CrossRef] [PubMed]
- Estaban, M.; Adot, J.M.; Arlandis, S.; Working Group for Recommendations of the Diagnosis and Management of Bladder Pain Syndrome. Recommendations for the diagnosis and management of bladder pain syndrome: Spanish urological association consensus document. Actas Urol. Esp. 2013, 39, 365–472. [Google Scholar] [CrossRef]
- Parsons, C.L. The role of the urinary epithelium in the pathogenesis of interstitial cystitis/prostatitis/urethritis. Urology 2007, 69, 9–16. [Google Scholar] [CrossRef]
- Tillisch, K. The effects of gut microbiota on CNS function in humans. Gut Microbes 2014, 5, 404–410. [Google Scholar] [CrossRef] [PubMed]
- Nazif, O.; Teichman, J.M.; Gebhart, G.F. Neural upregulation in interstitial cystitis. Urology 2007, 69, 24–33. [Google Scholar] [CrossRef] [PubMed]
- Elliott, R.A.; Kapoor, S.; Tincello, D.G. Expression and distribution of the sweet taste receptor isoforms T1R2 and T1R3 in human and rat bladders. J. Urol. 2011, 186, 2455–2462. [Google Scholar] [CrossRef]
- Manzel, A.; Muller, D.N.; Hafler, D.A.; Erdman, S.E.; Linker, R.A.; Kleinewietfeld, M. Role of “Western diet” in inflammatory autoimmune diseases. Curr. Allergy Asthma Rep. 2014, 14, 404. [Google Scholar] [CrossRef]
- Shivappa, N.; Steck, S.; Hurley, T.; Hussey, J.; Hébert, J. Designing and developing a literature-derived, population-based dietary inflammatory index. Public Health Nutr. 2014, 17, 1689–1696. [Google Scholar] [CrossRef]
- Tamma, S.M.; Shorter, B.; Toh, K.-L.; Moldwin, R.; Gordon, B. Influence of polyunsaturated fatty acids on urologic inflammation. Int. Urol. Nephrol. 2015, 47, 1753–1761. [Google Scholar] [CrossRef]
- Liu, F.H.; Liu, C.; Gong, T.T.; Gao, S.; Sun, H.; Jiang, Y.T.; Zhang, J.Y.; Zhang, M.; Gao, C.; Li, X.Y.; et al. Dietary Inflammatory Index and Health Outcomes: An Umbrella Review of Systematic Review and Meta-Analyses of Observational Studies. Front. Nutr. 2021, 8, 647122. [Google Scholar] [CrossRef]
- Hébert, J.R.; Shivappa, N.; Wirth, M.D.; Hussey, J.R.; Hurley, T.G. Perspective: The Dietary Inflammatory Index (DII)-Lessons Learned, Improvements Made, and Future Directions. Adv. Nutr. 2019, 10, 185–195. [Google Scholar] [CrossRef] [PubMed]
- Xu, X.; Qi, M.-Y.; Liu, S.; Song, X.-T.; Zhang, J.-N.; Zhai, Y.-F.; Lu, M.-H.; Han, H.-B.; Lian, Z.-X.; Yao, Y.-C. TLR4 overexpression enhances saturated fatty acid-induced inflammatory cytokine gene expression in sheep. Eur. J. Inflamm. 2018, 16, 1–7. [Google Scholar] [CrossRef]
- Milanski, M.; Degasperi, G.; Coopoe, A. Saturated fatty acids produce an inflammatory response predominantly through the activation of TLR4 signaling in hypothalamus: Implications for the pathogenesis of obesity. J. Neurosci. 2009, 29, 359–370. [Google Scholar] [CrossRef]
- Lancaster, G.I.; Langley, K.G.; Berglund, N.A.; Kammoun, H.L.; Reibe, S.; Estevez, E.; Weir, J.; Mellett, N.A.; Pernes, G.; Conway, J.R.W.; et al. Evidence that TLR4 Is not a receptor for saturated fatty acids but mediates lipid-induced inflammation by reprogramming macrophage metabolism. Cell Metab. 2018, 27, 1096–1110.e5. [Google Scholar] [CrossRef]
- Oberbach, A.; Schlichting, N.; Heinrich, M.; Till, H.; Stolzenburg, J.-U.; Neuhaus, J. Free fatty acid palmitate impairs vitality and function of cultured human bladder smooth muscle cells. PLoS ONE 2012, 7, e41026. [Google Scholar] [CrossRef]
- Maserejian, N.N.; Giovannucci, E.L.; McVary, K.T.; McGrother, C.; McKinlay, J.B. Dietary macronutrient and energy intake and urinary incontinence in women. Am. J. Epidemiol. 2010, 171, 1116–1125. [Google Scholar] [CrossRef]
- Winkvist, A.; Bärebring, L.; Gjertsson, I.; Ellegård, L.; Lindqvist, H.M. A randomized controlled cross-over trial investigating the effect of anti-inflammatory diet on disease activity and quality of life in rheumatoid arthritis: The Anti-inflammatory Diet In Rheumatoid Arthritis (ADIRA) study protocol. Nutr. J. 2018, 17, 44. [Google Scholar] [CrossRef] [PubMed]
- Clemens, J.Q.; Calhoun, E.A.; Litwin, M.S.; McNaughton-Collins, M.; Kusek, J.W.; Crowley, E.M.; Landis, J.R.; Urologic Pelvic Pain Collaborative Research Network. Validation of a modified National Institutes of Health chronic prostatitis symptom index to assess genitourinary pain in both men and women. Urology 2009, 74, 983–987. [Google Scholar] [CrossRef]
- Rosen, R.; Brown, C.; Heiman, J.; Leiblum, S.; Meston, C.; Shabsigh, R.; Ferguson, D.; D’Agostino, R., Jr. The Female Sexual Function Index (FSFI): A multidimensional self-report instrument for the assessment of female sexual function. J. Sex Marital Ther. 2000, 26, 191–208. [Google Scholar] [CrossRef]
- Bogart, L.M.; Suttopr, M.J.; Elliott, M.N.; Clemens, J.Q.; Berry, S.H. Validation of a quality-of-life scale for women with bladder pain syndrome/interstitial cystitis. Qual. Life Res. 2012, 21, 1665–1670. [Google Scholar] [CrossRef] [PubMed]
- Genoni, A.; Lo, J.; Lyons-Wall, P.; Devine, A. Compliance, palatability and feasibility of paleolithic and Australian guide to healthy eating diets in healthy women: A 4-week dietary intervention. Nutrients 2016, 8, 481. [Google Scholar] [CrossRef] [PubMed]
- Hanley, R.S.; Stoffel, J.T.; Zagha, R.M.; Mourtzinos, A.; Bresette, J.F. Multimodal therapy for painful bladder syndrome/interstitial cystitis: Pilot study combining behavioral, pharmacologic, and endoscopic therapies. Int. Braz. J. Urol. 2009, 35, 467–474. [Google Scholar] [CrossRef] [PubMed]
- Herati, A.; Shorter, B.; Sadek, M.; Levey, H.; Okhunov, Z.; Moldwin, R. The effects of caffeine on the symptoms of interstitial cystitis/painful bladder syndrome: A randomized, placebo-controlled double blind study. J. Urol. 2011, 185, e325. [Google Scholar] [CrossRef]
- Oh-oka, H. Clinical efficacy of 1-year intensive systematic dietary manipulation as complementary and alternative medicine therapies on female patients with interstitial cystitis/bladder pain syndrome. Urology 2017, 106, 50–54. [Google Scholar] [CrossRef]
- Lebowitz, B.D.; Vitiello, B.; Norquist, G.S. Approaches to multisite clinical trials: The National Institute of Mental Health perspective. Schizophr. Bull. 2003, 29, 7–13. [Google Scholar] [CrossRef]
- Constable, L.; Pirie, D.; Gillies, K.; McCann, S.; Breeman, S.; Glazener, C. The importance of rapport and relationship building when recruiting to clinical trials: A qualitative investigation of trial recruitment consultations in a surgical RCT. Trials 2015, 16, O37. [Google Scholar] [CrossRef]
- Robison, L.; Cho, Y.; Viecelli, A.K.; Johnson, D.W.; Hawley, C.M.; Valks, A.; Paul-Brent, P.A.; Stastny, R.; Varghese, J.; Kiriwandeniya, C.; et al. Australasian Kidney Trials Network. Conducting clinical trials during the COVID-19 pandemic—A collaborative trial network response. Trials 2021, 22, 278. [Google Scholar] [CrossRef] [PubMed]
- Clemson University. Available online: https://hgic.clemson.edu/factsheet/planning-meals-for-a-family (accessed on 1 October 2021).
- Armstrong, S.; Arsenault, M.; Betwick, S. Menu Planning in Long Term Care and Canada’s Food Guide; Dietitians of Canada: Toronto, ON, Canada, 2019; p. 37. [Google Scholar]
- van der Sman, R.G.M. Impact of Processing Factors on Quality of Frozen Vegetables and Fruits. Food Eng. Rev. 2020, 12, 399–420. [Google Scholar] [CrossRef]
- Aydinlar, E.I.; Dikmen, P.Y.; Tiftikci, A.; Saruc, M.; Aksu, M.; Gunsoy, H.G.; Tozun, N. IgG-based elimination diet in migraine plus irritable bowel syndrome. Headache 2013, 53, 514–525. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).