The Management of Myocardial Injury Related to SARS-CoV-2 Pneumonia
Abstract
:1. Introduction
2. Definition of MI Related to SARS-CoV-2 Pneumonia
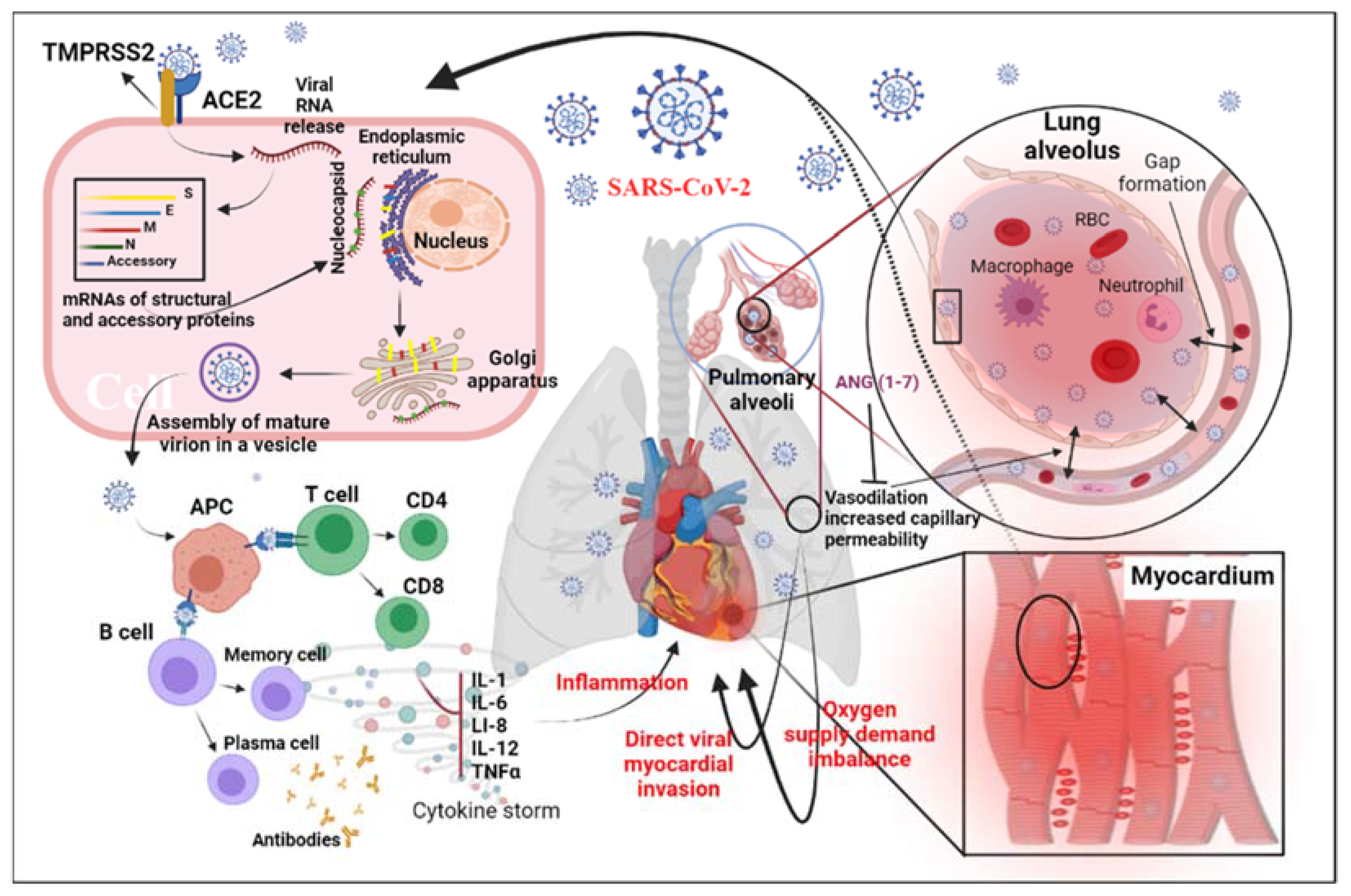
3. Mechanism of MI Related to SARS-CoV-2 Pneumonia
4. Management and Treatment of MI Related to SARS-CoV-2 Pneumonia
| Author | Setting | Study Design | Sample Size, N | Female, n (%) | Age (Years) * | HTN, n (%) | DM, n (%) | CKD, n (%) | Previous Myocardial Injuries, n (%) | Medications (Doses) | Coronary Intervention (PCI/CABG/DES) (%) |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Secco et al. [56] | Italy | Prospective case series | 31 | 7 (22.6) | 72.3 ± 9 | 22 (71%) | 12 (38.7) | - | 11 (35.4) | Aspirin (500 mg), ticagrelor (180 mg), intravenous heparin (70 UI/kg) | 28/31 (93.3) |
| Erol et al. [68] | Turkey | Multicenter retrospective | 991 | 236 (23.8) | 60 ± 13 | 499 (50.4) | 335 (33.8) | - | 283 (28.7) | Fibrinolytic therapy | 682/991 (68.8) |
| Choudry et al. [59] | UK | Single-center prospective | 39 | 6 (15.4) | 61.7 ± 11.0 | 28 (71.8) | 24 (61.6) | - | 9 (23.1) | Heparin (5000/1000 IU) | 38/39 (97.4) |
| Stefanini et al. [69] | Italy | Single-center retrospective l | 28 | 8 (28.6) | 68 ± 11 | 20 (71.4) | 9 (32.1) | 8 (28.6) | 3 (10.7) | - | 17/28 (61) |
| Ayad et al. [70] | Egypt | Single-center retrospective | 270 | 50 (18.5) | 57.1 ± 12.6 | 10 (3.7) | - | - | 5 (1.8) | Ticagrelor (180 mg), clopidogrel (75 mg) | 270/270 (100) |
| Gluckman et al. [71] | USA | Retrospective multicenter cross-sectional study from 6 states | 1915 | 633 (33%) | 67 ± 13 | 1573 (82.1) | 225 (11.7) | - | 395 (20.6) | - | 1915/1915 (100) |
| Reinstadler et al. [72] | Austria | Multicenter retrospective | 163 | 44 (27%) | 61 | (103, 63) | 32 (20) | - | 21 (13) | - | 163/163 (100) |
| Bangalore et al. [60] | USA | Prospective case series | 18 | 3 (17) | 63 | 11/17 (65) | 6/17 (35%) | 1/17 (6%) | 3/17 (17%) | Fibrinolytic agent | 5/9 (56) |
| Hamadeh et al. [61] | Lithuania, Italy, Spain, and Iraq | Multicenter retrospective | 78 | 30 (38.5) | 65 | 57 (73) | 41 (53) | 69 (88.4) | 9 (11) | Fibrinolytic agents (alteplase and tenecteplase) | 28/78 (35.9) |
| Alaarag et al. [73] | Egypt | Single-center retrospective | 26 | 8 (30.8) | 57.7 ± 8.75 | 11 (42.3) | 10 (38.5) | - | 4 (15.4) | Ticagrelor 90 mg, clopidogrel 75 mg, aspirin 75–100 mg, heparin (70 IU/kg) | 26/26 (100) |
| Scholz et al. [74] | Germany | Multicenter prospective | 387 | 147 (28) | 64.5 ± 0.7 | 229 (59%) | 79 (20%) | 26 (7%) | 47 (12%) | - | 352/387 (91.0%) |
| Popovic et al. [75] | France | Single-center prospective | 11 | 4 (36.4) | 63.6 ± 17.4 | 5 (45.5) | 2 (18.2) | - | - | Aspirin (250–500 mg) heparin (70 UI/kg IV bolus), and a P2Y12 inhibitor (clopidogrel 75 mg) | 11/11 (100) |
5. The Impact of the Pandemic on the Reporting and Management of Cardiac Events
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef]
- W.H.O. Emergency Committee. WHO. Statement on the Second Meeting of the International Health Regulations (2005) Emergency Committee Regarding the Outbreak of Novel Coronavirus (2019-nCoV). Available online: https://www.who.int/news-room/detail/30-01-2020-statement-on-the-second-meeting-of-the-international-health-regulations-(2005)-emergency-committee-regarding-the-outbreak-of-novel-coronavirus-(2019-ncov) (accessed on 30 January 2020).
- de Almeida-Pititto, B.; Dualib, P.M.; Zajdenverg, L.; Dantas, J.R.; De Souza, F.D.; Rodacki, M.; Bertoluci, M.C. Severity and mortality of COVID 19 in patients with diabetes, hypertension and cardiovascular disease: A meta-analysis. Diabetol. Metab. Syndr. 2020, 12, 75. [Google Scholar] [CrossRef] [PubMed]
- Jain, U. Effect of COVID-19 on the Organs. Cureus 2020, 12, e9540. [Google Scholar] [CrossRef] [PubMed]
- Brosnahan, S.B.; Jonkman, A.H.; Kugler, M.C.; Munger, J.S.; Kaufman, D.A. COVID-19 and respiratory system disorders: Current knowledge, future clinical and translational research questions. Arterioscler. Thromb. Vasc. Biol. 2020, 40, 2586–2597. [Google Scholar] [CrossRef] [PubMed]
- Bitar, A.N.; Sulaiman, S.A.S.; Ali, I.A.H.; Khan, I.; Khan, A.H. Osteoporosis among patients with chronic obstructive pulmonary disease: Systematic review and meta-analysis of prevalence, severity, and therapeutic outcomes. J. Pharm. Bioallied Sci. 2019, 11, 310. [Google Scholar] [PubMed]
- Bitar, A.N.; Ghoto, M.A.; Dayo, A.; Arain, M.I.; Parveen, R. Pathophysiological correlation between diabetes mellitus type-II & chronic obstructive pulmonary diseases. J. Liaquat Univ. Med. Health Sci. 2017, 16, 41–48. [Google Scholar]
- Bitar, A.N.; Sulaiman, S.A.S.; Ali, I.A.B.H.; Khan, A.H. Prevalence, risk assessment, and predictors of osteoporosis among chronic obstructive pulmonary disease patients. J. Adv. Pharm. Technol. Res. 2021, 12, 395. [Google Scholar] [CrossRef]
- Zhong, Z.; Li, H.; Zhu, J.; Ji, P.; Li, B.; Pang, J.; Zhang, J.; Liang, X. Clinical characteristics of 2,459 severe or critically ill COVID-19 patients: A meta-analysis. Medicine 2021, 100, e23781. [Google Scholar] [CrossRef]
- Wang, D.; Hu, B.; Hu, C.; Zhu, F.; Liu, X.; Zhang, J.; Wang, B.; Xiang, H.; Cheng, Z.; Xiong, Y. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus–infected pneumonia in Wuhan, China. Jama 2020, 323, 1061–1069. [Google Scholar] [CrossRef]
- Chan, J.F.-W.; Yuan, S.; Kok, K.-H.; To, K.K.-W.; Chu, H.; Yang, J.; Xing, F.; Liu, J.; Yip, C.C.-Y.; Poon, R.W.-S. A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-to-person transmission: A study of a family cluster. Lancet 2020, 395, 514–523. [Google Scholar] [CrossRef]
- Zhang, R.; Liu, H.; Li, F.; Zhang, B.; Liu, Q.; Li, X.; Luo, L. Transmission and epidemiological characteristics of Novel Coronavirus (2019-nCoV)-Infected Pneumonia (NCIP): Preliminary evidence obtained in comparison with 2003-SARS. MedRxiv 2020. [Google Scholar] [CrossRef] [Green Version]
- Huang, Z.; Huang, P.; Du, B.; Kong, L.; Zhang, W.; Zhang, Y.; Dong, J. Prevalence and clinical outcomes of cardiac injury in patients with COVID-19: A systematic review and meta-analysis. Nutr. Metab. Cardiovasc. Dis. 2021, 31, 2–13. [Google Scholar] [CrossRef] [PubMed]
- Mohammed, M.; Muhammad, S.; Mohammed, F.Z.; Mustapha, S.; Sha’aban, A.; Sani, N.Y.; Ahmad, M.H.; Bala, A.A.; Ungogo, M.A.; Alotaibi, N.M. Risk factors associated with mortality among patients with novel coronavirus disease (COVID-19) in Africa. J. Racial Ethn. Health Disparities 2021, 8, 1267–1272. [Google Scholar] [CrossRef] [PubMed]
- Albitar, O.; Ballouze, R.; Ooi, J.P.; Ghadzi, S.M.S. Risk factors for mortality among COVID-19 patients. Diabetes Res. Clin. Pract. 2020, 166, 108293. [Google Scholar] [CrossRef] [PubMed]
- Thygesen, K.; Alpert, J.S.; Jaffe, A.S.; Chaitman, B.R.; Bax, J.J.; Morrow, D.A.; White, H.D. Executive Group on behalf of the Joint European Society of Cardiology (ESC); American College of Cardiology (ACC); American Heart Association (AHA); World Heart Federation (WHF); Task Force for the Universal Definition of Myocardial Infarction. Fourth universal definition of myocardial infarction (2018). Circulation 2018, 138, e618–e651. [Google Scholar]
- Hendren, N.S.; de Lemos, J.A.; Ayers, C.; Das, S.R.; Rao, A.; Carter, S.; Rosenblatt, A.; Walchok, J.; Omar, W.; Khera, R. Association of body mass index and age with morbidity and mortality in patients hospitalized with COVID-19: Results from the American Heart Association COVID-19 Cardiovascular Disease Registry. Circulation 2021, 143, 135–144. [Google Scholar] [CrossRef]
- Driggin, E.; Maddox, T.M.; Ferdinand, K.C.; Kirkpatrick, J.N.; Ky, B.; Morris, A.A.; Mullen, J.B.; Parikh, S.A.; Philbin, D.M., Jr.; Vaduganathan, M. ACC health policy statement on cardiovascular disease considerations for COVID-19 vaccine prioritization: A report of the American College of Cardiology Solution Set Oversight Committee. J. Am. Coll. Cardiol. 2021, 77, 1938–1948. [Google Scholar] [CrossRef]
- Harrison, S.L.; Buckley, B.J.; Rivera-Caravaca, J.M.; Zhang, J.; Lip, G.Y. Cardiovascular risk factors, cardiovascular disease, and COVID-19: An umbrella review of systematic reviews. Eur. Heart J. Qual. Care Clin. Outcomes 2021, 7, 330–339. [Google Scholar] [CrossRef]
- Ferrante, G.; Fazzari, F.; Cozzi, O.; Maurina, M.; Bragato, R.; D’Orazio, F.; Torrisi, C.; Lanza, E.; Indolfi, E.; Donghi, V. Risk factors for myocardial injury and death in patients with COVID-19: Insights from a cohort study with chest computed tomography. Cardiovasc. Res. 2020, 116, 2239–2246. [Google Scholar] [CrossRef]
- Aghagoli, G.; Marin, B.G.; Soliman, L.B.; Sellke, F.W. Cardiac involvement in COVID-19 patients: Risk factors, predictors, and complications: A review. J. Card. Surg. 2020, 35, 1302–1305. [Google Scholar] [CrossRef]
- Yang, C.; Liu, F.; Liu, W.; Cao, G.; Liu, J.; Huang, S.; Zhu, M.; Tu, C.; Wang, J.; Xiong, B. Myocardial injury and risk factors for mortality in patients with COVID-19 pneumonia. Int. J. Cardiol. 2021, 326, 230–236. [Google Scholar] [CrossRef] [PubMed]
- Zhou, F.; Yu, T.; Du, R.; Fan, G.; Liu, Y.; Liu, Z.; Xiang, J.; Wang, Y.; Song, B.; Gu, X. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study. Lancet 2020, 395, 1054–1062. [Google Scholar] [CrossRef]
- Chen, T.; Wu, D.; Chen, H.; Yan, W.; Yang, D.; Chen, G.; Ma, K.; Xu, D.; Yu, H.; Wang, H. Clinical characteristics of 113 deceased patients with coronavirus disease 2019: Retrospective study. BMJ 2020, 368, m1091. [Google Scholar] [CrossRef] [PubMed]
- Hui, H.; Zhang, Y.; Yang, X.; Wang, X.; He, B.; Li, L.; Li, H.; Tian, J.; Chen, Y. Clinical and radiographic features of cardiac injury in patients with 2019 novel coronavirus pneumonia. MedRxiv 2020. [Google Scholar] [CrossRef]
- Yang, X.; Yu, Y.; Xu, J.; Shu, H.; Liu, H.; Wu, Y.; Zhang, L.; Yu, Z.; Fang, M.; Yu, T. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: A single-centered, retrospective, observational study. Lancet Respir. Med. 2020, 8, 475–481. [Google Scholar] [CrossRef]
- Cummings, M.J.; Baldwin, M.R.; Abrams, D.; Jacobson, S.D.; Meyer, B.J.; Balough, E.M.; Aaron, J.G.; Claassen, J.; Rabbani, L.E.; Hastie, J. Epidemiology, clinical course, and outcomes of critically ill adults with COVID-19 in New York City: A prospective cohort study. Lancet 2020, 395, 1763–1770. [Google Scholar] [CrossRef]
- Harmouch, F.; Shah, K.; Hippen, J.T.; Kumar, A.; Goel, H. Is it all in the heart? Myocardial injury as major predictor of mortality among hospitalized COVID-19 patients. J. Med. Virol. 2021, 93, 973–982. [Google Scholar] [CrossRef]
- Xu, Z.; Shi, L.; Wang, Y.; Zhang, J.; Huang, L.; Zhang, C.; Liu, S.; Zhao, P.; Liu, H.; Zhu, L. Pathological findings of COVID-19 associated with acute respiratory distress syndrome. Lancet Respir. Med. 2020, 8, 420–422. [Google Scholar] [CrossRef]
- Peng, W.; Wu, H.; Tan, Y.; Li, M.; Yang, D.; Li, S. Mechanisms and treatments of myocardial injury in patients with corona virus disease 2019. Life Sci. 2020, 262, 118496. [Google Scholar] [CrossRef]
- Reynolds, H.R.; Adhikari, S.; Pulgarin, C.; Troxel, A.B.; Iturrate, E.; Johnson, S.B.; Hausvater, A.; Newman, J.D.; Berger, J.S.; Bangalore, S. Renin–angiotensin–aldosterone system inhibitors and risk of Covid-19. N. Engl. J. Med. 2020, 382, 2441–2448. [Google Scholar] [CrossRef]
- Gheblawi, M.; Wang, K.; Viveiros, A.; Nguyen, Q.; Zhong, J.-C.; Turner, A.J.; Raizada, M.K.; Grant, M.B.; Oudit, G.Y. Angiotensin-converting enzyme 2: SARS-CoV-2 receptor and regulator of the renin-angiotensin system: Celebrating the 20th anniversary of the discovery of ACE2. Circ. Res. 2020, 126, 1456–1474. [Google Scholar] [CrossRef] [PubMed]
- Li, W.; Moore, M.J.; Vasilieva, N.; Sui, J.; Wong, S.K.; Berne, M.A.; Somasundaran, M.; Sullivan, J.L.; Luzuriaga, K.; Greenough, T.C. Angiotensin-converting enzyme 2 is a functional receptor for the SARS coronavirus. Nature 2003, 426, 450–454. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chaudhary, M. COVID-19 susceptibility: Potential of ACE2 polymorphisms. Egypt. J. Med. Hum. Genet. 2020, 21, 54. [Google Scholar] [CrossRef]
- Oudit, G.; Kassiri, Z.; Jiang, C.; Liu, P.; Poutanen, S.; Penninger, J.; Butany, J. SARS-coronavirus modulation of myocardial ACE2 expression and inflammation in patients with SARS. Eur. J. Clin. Investig. 2009, 39, 618–625. [Google Scholar] [CrossRef] [PubMed]
- Wan, Y.; Shang, J.; Graham, R.; Baric, R.S.; Li, F. Receptor recognition by the novel coronavirus from Wuhan: An analysis based on decade-long structural studies of SARS coronavirus. J. Virol. 2020, 94, e00127-20. [Google Scholar] [CrossRef]
- Zhou, P.; Yang, X.-L.; Wang, X.-G.; Hu, B.; Zhang, L.; Zhang, W.; Si, H.-R.; Zhu, Y.; Li, B.; Huang, C.-L. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 2020, 579, 270–273. [Google Scholar] [CrossRef] [PubMed]
- Chen, N.; Zhou, M.; Dong, X.; Qu, J.; Gong, F.; Han, Y.; Qiu, Y.; Wang, J.; Liu, Y.; Wei, Y. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: A descriptive study. Lancet 2020, 395, 507–513. [Google Scholar] [CrossRef]
- Conti, P.; Ronconi, G.; Caraffa, A.; Gallenga, C.; Ross, R.; Frydas, I.; Kritas, S. Induction of pro-inflammatory cytokines (IL-1 and IL-6) and lung inflammation by Coronavirus-19 (COVI-19 or SARS-CoV-2): Anti-inflammatory strategies. J. Biol. Regul. Homeost. Agents 2020, 34, 327–331. [Google Scholar]
- Channappanavar, R.; Perlman, S. Pathogenic human coronavirus infections: Causes and consequences of cytokine storm and immunopathology. Semin. Immunopathol. 2017, 39, 529–539. [Google Scholar] [CrossRef]
- Wong, C.; Lam, C.; Wu, A.; Ip, W.; Lee, N.; Chan, I.; Lit, L.; Hui, D.; Chan, M.; Chung, S. Plasma inflammatory cytokines and chemokines in severe acute respiratory syndrome. Clin. Exp. Immunol. 2004, 136, 95–103. [Google Scholar] [CrossRef]
- Mann, D.L. Inflammatory mediators and the failing heart: Past, present, and the foreseeable future. Circ. Res. 2002, 91, 988–998. [Google Scholar] [CrossRef] [PubMed]
- Li, S.S.; Cheng, C.; Fu, C.; Chan, Y.; Lee, M.; Chan, J.W.; Yiu, S. Left ventricular performance in patients with severe acute respiratory syndrome: A 30-day echocardiographic follow-up study. Circulation 2003, 108, 1798–1803. [Google Scholar] [CrossRef] [PubMed]
- Musher, D.M.; Abers, M.S.; Corrales-Medina, V.F. Acute infection and myocardial infarction. New Engl. J. Med. 2019, 380, 171–176. [Google Scholar] [CrossRef] [PubMed]
- Marfella, R.; Paolisso, P.; Sardu, C.; Palomba, L.; D’Onofrio, N.; Cesaro, A.; Barbieri, M.; Rizzo, M.R.; Sasso, F.C.; Scisciola, L. SARS-COV-2 colonizes coronary thrombus and impairs heart microcirculation bed in asymptomatic SARS-CoV-2 positive subjects with acute myocardial infarction. Crit. Care 2021, 25, 217. [Google Scholar] [CrossRef] [PubMed]
- Thygesen, K.; Alpert, J.S.; Jaffe, A.S.; Chaitman, B.R.; Bax, J.J.; Morrow, D.A.; White, H.D.; Mickley, H.; Crea, F.; Van de Werf, F. Fourth universal definition of myocardial infarction (2018). Eur. Heart J. 2019, 40, 237–269. [Google Scholar] [CrossRef] [PubMed]
- Metzler, B.; Siostrzonek, P.; Binder, R.K.; Bauer, A.; Reinstadler, S.J. Decline of acute coronary syndrome admissions in Austria since the outbreak of COVID-19: The pandemic response causes cardiac collateral damage. Eur. Heart J. 2020, 41, 1852–1853. [Google Scholar] [CrossRef]
- Huet, F.; Prieur, C.; Schurtz, G.; Gerbaud, É.; Manzo-Silberman, S.; Vanzetto, G.; Elbaz, M.; Tea, V.; Mercier, G.; Lattuca, B. One train may hide another: Acute cardiovascular diseases could be neglected because of the COVID-19 pandemic. Arch. Cardiovasc. Dis. 2020, 113, 303–307. [Google Scholar] [CrossRef]
- Li, B.; Yang, J.; Zhao, F.; Zhi, L.; Wang, X.; Liu, L.; Bi, Z.; Zhao, Y. Prevalence and impact of cardiovascular metabolic diseases on COVID-19 in China. Clin. Res. Cardiol. 2020, 109, 531–538. [Google Scholar] [CrossRef]
- Maestrini, V.; Birtolo, L.I.; Francone, M.; Galardo, G.; Galea, N.; Severino, P.; Alessandri, F.; Colaiacomo, M.C.; Cundari, G.; Chimenti, C. Cardiac involvement in consecutive unselected hospitalized COVID-19 population: In-hospital evaluation and one-year follow-up. Int. J. Cardiol. 2021, 339, 235–242. [Google Scholar] [CrossRef]
- Gragnano, F.; Cesaro, A.; Pelliccia, F.; Calabrò, P. Multimodality evaluation of cardiac injury in COVID-19: Getting to the heart of the matter. Int. J. Cardiol. 2021, 339, 243–245. [Google Scholar] [CrossRef]
- Cameli, M.; Pastore, M.C.; Mandoli, G.E.; D’ascenzi, F.; Focardi, M.; Biagioni, G.; Cameli, P.; Patti, G.; Franchi, F.; Mondillo, S. COVID-19 and Acute Coronary Syndromes: Current Data and Future Implications. Front. Cardiovasc. Med. 2020, 7, 593496. [Google Scholar] [CrossRef] [PubMed]
- Zeng, J.; Huang, J.; Pan, L. How to balance acute myocardial infarction and COVID-19: The protocols from Sichuan Provincial People’s Hospital. Intensive Care Med. 2020, 46, 1111–1113. [Google Scholar] [CrossRef] [PubMed]
- Welt, F.G.; Shah, P.B.; Aronow, H.D.; Bortnick, A.E.; Henry, T.D.; Sherwood, M.W.; Young, M.N.; Davidson, L.J.; Kadavath, S.; Mahmud, E. Catheterization laboratory considerations during the coronavirus (COVID-19) pandemic: From the ACC’s Interventional Council and SCAI. J. Am. Coll. Cardiol. 2020, 75, 2372–2375. [Google Scholar] [CrossRef] [PubMed]
- Akkaif, M.A.; Sha’aban, A.; Cesaro, A.; Jaber, A.A.S.; Vergara, A.; Yunusa, I.; Jatau, A.I.; Mohammed, M.; Govindasamy, G.S.; Al-Mansoub, M.A. The impact of SARS-CoV-2 treatment on the cardiovascular system: An updated review. Inflammopharmacology 2022, 30, 1143–1151. [Google Scholar] [CrossRef]
- Secco, G.G.; Tarantini, G.; Mazzarotto, P.; Garbo, R.; Parisi, R.; Maggio, S.; Vercellino, M.; Pistis, G.; Audo, A.; Kozel, D. Invasive strategy for COVID patients presenting with acute coronary syndrome: The first multicenter Italian experience. Catheter. Cardiovasc. Interv. 2021, 97, 195–198. [Google Scholar] [CrossRef]
- Akkaif, M.A.; Daud, N.A.A.; Sha’aban, A.; Ng, M.L.; Abdul Kader, M.A.S.; Noor, D.A.M.; Ibrahim, B. The Role of Genetic Polymorphism and Other Factors on Clopidogrel Resistance (CR) in an Asian Population with Coronary Heart Disease (CHD). Molecules 2021, 26, 1987. [Google Scholar] [CrossRef]
- Akkaif, M.A.; Sha’aban, A.; Daud, N.A.A.; Yunusa, I.; Ng, M.L.; Kader, M.A.S.A.; Noor, D.A.M.; Ibrahim, B. Coronary Heart Disease (CHD) in Elderly Patients: Which Drug to Choose, Ticagrelor and Clopidogrel? A Systematic Review and Meta-Analysis of Randomized Controlled Trials. J. Cardiovasc. Dev. Dis. 2021, 8, 123. [Google Scholar] [CrossRef]
- Choudry, F.A.; Hamshere, S.M.; Rathod, K.S.; Akhtar, M.M.; Archbold, R.A.; Guttmann, O.P.; Woldman, S.; Jain, A.K.; Knight, C.J.; Baumbach, A. High thrombus burden in patients with COVID-19 presenting with ST-segment elevation myocardial infarction. J. Am. Coll. Cardiol. 2020, 76, 1168–1176. [Google Scholar] [CrossRef]
- Bangalore, S.; Sharma, A.; Slotwiner, A.; Yatskar, L.; Harari, R.; Shah, B.; Ibrahim, H.; Friedman, G.H.; Thompson, C.; Alviar, C.L. ST-segment elevation in patients with Covid-19—a case series. New Engl. J. Med. 2020, 382, 2478–2480. [Google Scholar] [CrossRef]
- Hamadeh, A.; Aldujeli, A.; Briedis, K.; Tecson, K.M.; Sanz-Sánchez, J.; Al-Obeidi, A.; Diez, J.L.; Žaliūnas, R.; Stoler, R.C.; McCullough, P.A. Characteristics and outcomes in patients presenting with COVID-19 and ST-segment elevation myocardial infarction. Am. J. Cardiol. 2020, 131, 1–6. [Google Scholar] [CrossRef]
- Akşit, E.; Kırılmaz, B.; Gazi, E.; Aydın, F. Ticagrelor can be an important agent in the treatment of severe COVID-19 patients with myocardial infarction. Balk. Med. J. 2020, 37, 233. [Google Scholar] [CrossRef] [PubMed]
- Akkaif, M.A.; Ng, M.L.; Kader, M.A.S.A.; Daud, N.A.A.; Sha’aban, A.; Ibrahim, B. A review of the effects of ticagrelor on adenosine concentration and its clinical significance. Pharmacol. Rep. 2021, 73, 1551–1564. [Google Scholar] [CrossRef] [PubMed]
- Akkaif, M.A.; Sha’aban, A.; Daud, N.A.A.; Ng, M.L.; Ibrahim, B. Investigate the Strategy of Using Pharmacogenetics and Pharmacometabonomics to the Personalization of Ticagrelor Antiplatelet Therapy. Syst. Rev. Pharm. 2020, 11, 1100–1107. [Google Scholar]
- Schaefer, I.-M.; Padera, R.F.; Solomon, I.H.; Kanjilal, S.; Hammer, M.M.; Hornick, J.L.; Sholl, L.M. In situ detection of SARS-CoV-2 in lungs and airways of patients with COVID-19. Mod. Pathol. 2020, 33, 2104–2114. [Google Scholar] [CrossRef]
- Thallapureddy, K.; Thallapureddy, K.; Zerda, E.; Suresh, N.; Kamat, D.; Rajasekaran, K.; Moreira, A. Long-Term Complications of COVID-19 Infection in Adolescents and Children. Curr. Pediatr. Rep. 2022, 10, 11–17. [Google Scholar] [CrossRef] [PubMed]
- Kawakami, R.; Sakamoto, A.; Kawai, K.; Gianatti, A.; Pellegrini, D.; Nasr, A.; Kutys, B.; Guo, L.; Cornelissen, A.; Mori, M. Pathological evidence for SARS-CoV-2 as a cause of myocarditis: JACC review topic of the week. J. Am. Coll. Cardiol. 2021, 77, 314–325. [Google Scholar] [CrossRef]
- Erol, M.K.; Kayıkçıoğlu, M.; Kılıçkap, M.; Güler, A.; Yıldırım, A.; Kahraman, F.; Can, V.; Inci, S.; Baysal, S.S.; Er, O. Treatment delays and in-hospital outcomes in acute myocardial infarction during the COVID-19 pandemic: A nationwide study. Anatol. J. Cardiol. 2020, 24, 334–342. [Google Scholar]
- Stefanini, G.G.; Montorfano, M.; Trabattoni, D.; Andreini, D.; Ferrante, G.; Ancona, M.; Metra, M.; Curello, S.; Maffeo, D.; Pero, G. ST-elevation myocardial infarction in patients with COVID-19: Clinical and angiographic outcomes. Circulation 2020, 141, 2113–2116. [Google Scholar] [CrossRef]
- Ayad, S.; Shenouda, R.; Henein, M. The Impact of COVID-19 on In-Hospital Outcomes of ST-Segment Elevation Myocardial Infarction Patients. J. Clin. Med. 2021, 10, 278. [Google Scholar] [CrossRef]
- Gluckman, T.J.; Wilson, M.A.; Chiu, S.-T.; Penny, B.W.; Chepuri, V.B.; Waggoner, J.W.; Spinelli, K.J. Case rates, treatment approaches, and outcomes in acute myocardial infarction during the coronavirus disease 2019 pandemic. JAMA Cardiol. 2020, 5, 1419–1424. [Google Scholar] [CrossRef]
- Reinstadler, S.J.; Reindl, M.; Lechner, I.; Holzknecht, M.; Tiller, C.; Roithinger, F.X.; Frick, M.; Hoppe, U.C.; Jirak, P.; Berger, R. Effect of the COVID-19 pandemic on treatment delays in patients with ST-segment elevation myocardial infarction. J. Clin. Med. 2020, 9, 2183. [Google Scholar] [CrossRef] [PubMed]
- Alaarag, A.; Hassan, T.; Samir, S.; Naseem, M. Clinical and angiographic characteristics of patients with STEMI and confirmed diagnosis of COVID-19: An experience of Tanta University Hospital. Egypt. Heart J. 2020, 72, 68. [Google Scholar] [CrossRef]
- Scholz, K.H.; Lengenfelder, B.; Thilo, C.; Jeron, A.; Stefanow, S.; Janssens, U.; Bauersachs, J.; Schulze, P.C.; Winter, K.D.; Schröder, J. Impact of COVID-19 outbreak on regional STEMI care in Germany. Clin. Res. Cardiol. 2020, 109, 1511–1521. [Google Scholar] [CrossRef] [PubMed]
- Popovic, B.; Varlot, J.; Metzdorf, P.A.; Jeulin, H.; Goehringer, F.; Camenzind, E. Changes in characteristics and management among patients with ST-elevation myocardial infarction due to COVID-19 infection. Catheter. Cardiovasc. Interv. 2021, 97, E319–E326. [Google Scholar] [CrossRef]
- Baldi, E.; Sechi, G.M.; Mare, C.; Canevari, F.; Brancaglione, A.; Primi, R.; Klersy, C.; Palo, A.; Contri, E.; Ronchi, V. Out-of-hospital cardiac arrest during the Covid-19 outbreak in Italy. N. Engl. J. Med. 2020, 383, 496–498. [Google Scholar] [CrossRef]
- Bitar, A.N.; Zawiah, M.; Al-Ashwal, F.Y.; Kubas, M.; Saeed, R.M.; Abduljabbar, R.; Jaber, A.A.S.; Sulaiman, S.A.S.; Khan, A.H. Misinformation, perceptions towards COVID-19 and willingness to be vaccinated: A population-based survey in Yemen. PLoS ONE 2021, 16, e0248325. [Google Scholar] [CrossRef] [PubMed]
- Al-Ashwal, F.Y.; Kubas, M.; Zawiah, M.; Bitar, A.N.; Saeed, R.M.; Sulaiman, S.A.S.; Khan, A.H.; Ghadzi, S.M.S. Healthcare workers’ knowledge, preparedness, counselling practices, and perceived barriers to confront COVID-19: A cross-sectional study from a war-torn country, Yemen. PLoS ONE 2020, 15, e0243962. [Google Scholar] [CrossRef]
- Kayikcioglu, M.; Tuncel, O.K.; Tokgozoglu, L. Impact of the COVID-19 pandemic in patients with a previous history of premature myocardial infarction. Am. J. Prev. Cardiol. 2020, 4, 100128. [Google Scholar] [CrossRef]
- Khera, A.; Baum, S.J.; Gluckman, T.J.; Gulati, M.; Martin, S.S.; Michos, E.D.; Navar, A.M.; Taub, P.R.; Toth, P.P.; Virani, S.S. Continuity of care and outpatient management for patients with and at high risk for cardiovascular disease during the COVID-19 pandemic: A scientific statement from the American Society for Preventive Cardiology. Am. J. Prev. Cardiol. 2020, 1, 100009. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Akkaif, M.A.; Bitar, A.N.; Al-Kaif, L.A.I.K.; Daud, N.A.A.; Sha’aban, A.; Noor, D.A.M.; Abd Aziz, F.; Cesaro, A.; SK Abdul Kader, M.A.; Abdul Wahab, M.J.; et al. The Management of Myocardial Injury Related to SARS-CoV-2 Pneumonia. J. Cardiovasc. Dev. Dis. 2022, 9, 307. https://doi.org/10.3390/jcdd9090307
Akkaif MA, Bitar AN, Al-Kaif LAIK, Daud NAA, Sha’aban A, Noor DAM, Abd Aziz F, Cesaro A, SK Abdul Kader MA, Abdul Wahab MJ, et al. The Management of Myocardial Injury Related to SARS-CoV-2 Pneumonia. Journal of Cardiovascular Development and Disease. 2022; 9(9):307. https://doi.org/10.3390/jcdd9090307
Chicago/Turabian StyleAkkaif, Mohammed Ahmed, Ahmad Naoras Bitar, Laith A. I. K. Al-Kaif, Nur Aizati Athirah Daud, Abubakar Sha’aban, Dzul Azri Mohamed Noor, Fatimatuzzahra’ Abd Aziz, Arturo Cesaro, Muhamad Ali SK Abdul Kader, Mohamed Jahangir Abdul Wahab, and et al. 2022. "The Management of Myocardial Injury Related to SARS-CoV-2 Pneumonia" Journal of Cardiovascular Development and Disease 9, no. 9: 307. https://doi.org/10.3390/jcdd9090307
APA StyleAkkaif, M. A., Bitar, A. N., Al-Kaif, L. A. I. K., Daud, N. A. A., Sha’aban, A., Noor, D. A. M., Abd Aziz, F., Cesaro, A., SK Abdul Kader, M. A., Abdul Wahab, M. J., Khaw, C. S., & Ibrahim, B. (2022). The Management of Myocardial Injury Related to SARS-CoV-2 Pneumonia. Journal of Cardiovascular Development and Disease, 9(9), 307. https://doi.org/10.3390/jcdd9090307









