Knowledge and Expectations on Antibiotic Use among Older Adults in Malaysia: A Cross-Sectional Survey
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Population
2.2. Questionnaire Instrument
2.3. Data Collection
2.4. Data Analysis
3. Results
3.1. Prior Experience and Practices in Antibiotic Use
3.2. Knowledge about Antibiotic Use and Resistance
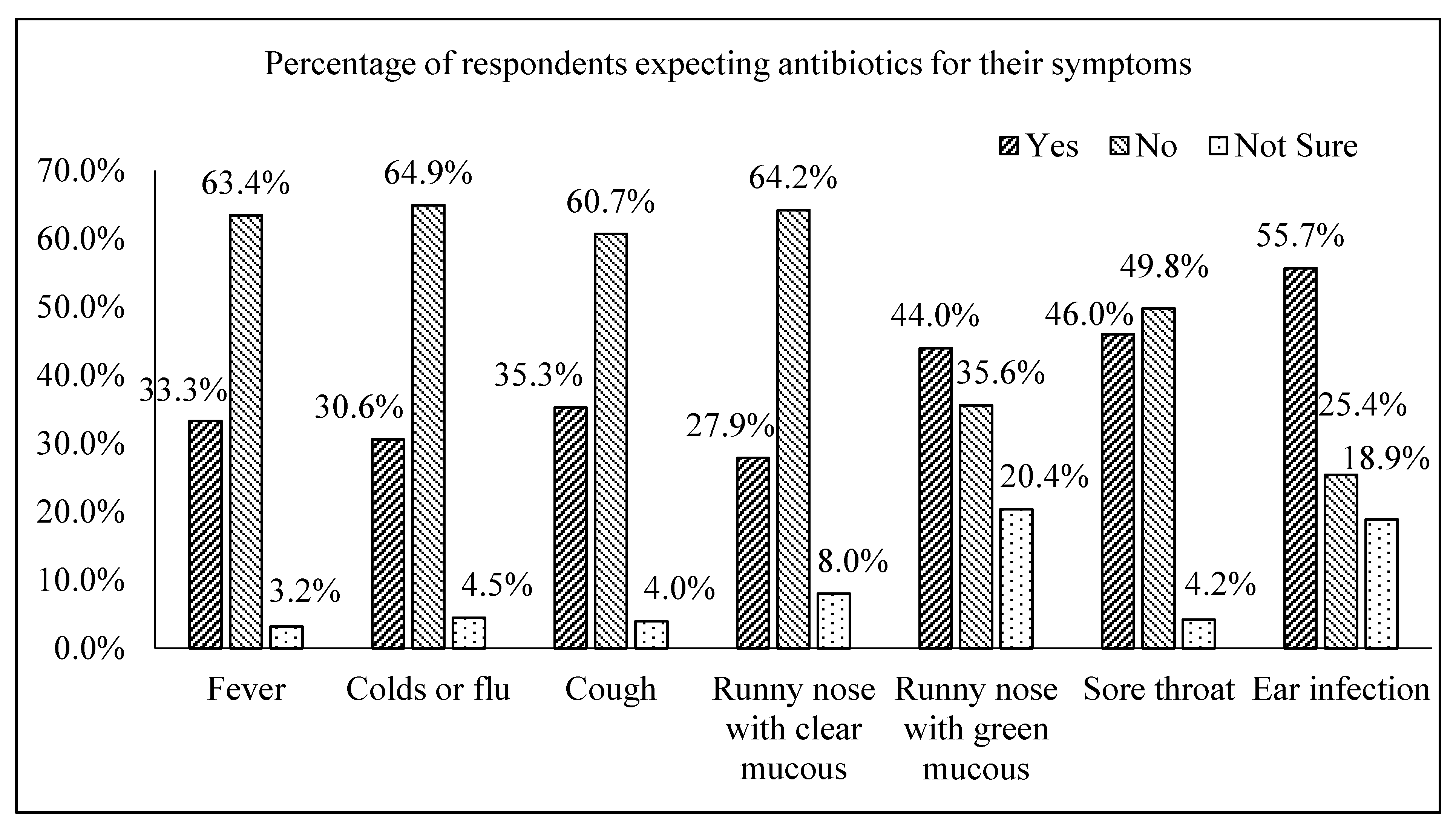
3.3. Expectations for Antibiotic Treatment
3.4. Association between Knowledge, Expectations and Practice
3.5. Factors Associated with Knowledge of Antibiotics
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- World Health Organization. Global Action Plan on Antimicrobial Resistance; WHO Press: Geneva, Switzerland, 2015; pp. 1–28. [Google Scholar]
- Davies, J.; Davies, D. Origins and Evolution of Antibiotic Resistance. Microbiol. Mol. Biol. Rev. 2010, 74, 417–433. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Silver, L.L. Challenges of antibacterial discovery. Clin. Microbiol. Rev. 2011, 24, 71–109. [Google Scholar] [CrossRef] [PubMed]
- Roberts, R.R.; Hota, B.; Ahmad, I.; Scott, R.D., II; Foster, S.D.; Abbasi, F.; Schabowski, S.; Kampe, L.M.; Ciavarella, G.G.; Supino, M.; et al. Hospital and Societal Costs of Antimicrobial-Resistant Infections in a Chicago Teaching Hospital: Implications for Antibiotic Stewardship. Clin. Infect. Dis. 2009, 49, 1175–1184. [Google Scholar] [CrossRef] [PubMed]
- Ministry of Health Malaysia. Malaysian Action Plan on Antimicrobial Resistance (MyAP-AMR) 2017–2021; Minist Heal Malaysia: Putrajaya, Malaysia, 2017; pp. 1–51. [Google Scholar]
- Ventola, C.L. The antibiotic resistance crisis: Part 1: Causes and threats. Pharm. Ther. 2015, 40, 277–283. [Google Scholar]
- Williamson, D.A.; Roos, R.; Verrall, A.; Smith, A.; Thomas, M.G. Trends, demographics and disparities in outpatient antibiotic consumption in New Zealand: A national study. J. Antimicrob. Chemother. 2016, 71, 3593–3598. [Google Scholar] [CrossRef]
- Fleming-dutra, K.E.; Hersh, A.L.; Shapiro, D.J.; Bartoces, M.; Enns, E.A.; File, T.M., Jr.; Finkelstein, J.A.; Gerber, J.S.; Hyun, D.Y.; Linder, J.A.; et al. Prevalence of Inappropriate Antibiotic Prescriptions Among US Ambulatory Care Visits, 2010–2011. JAMA 2016, 315, 1864–1873. [Google Scholar] [CrossRef]
- Palacios-Ceña, D.; Hernández-Barrera, V.; Jiménez-Trujillo, I.; Serrano-Urrea, R.; Fernández-de-las-Peñas, C.; Carrasco-Garrido, P. Time trends in antibiotic consumption in the elderly: Ten-year follow-up of the Spanish National Health Survey and the European Health Interview Survey for Spain (2003–2014). PLoS ONE 2017, 12, e0185869. [Google Scholar] [CrossRef]
- Giarratano, A.; El Green, S.; Nicolau, D.P. Review of antimicrobial use and considerations in the elderly population. Clin. Interv. Aging 2018, 13, 657–667. [Google Scholar] [CrossRef]
- Beckett, C.L.; Harbarth, S.; Huttner, B. Special considerations of antibiotic prescription in the geriatric population. Clin. Microbiol. Infect. 2015, 21, 3–9. [Google Scholar] [CrossRef] [Green Version]
- Lim, C.J.; Stuart, R.L.; Kong, D.C. Antibiotic use in residential aged care facilities. AFP 2015, 44, 192–196. [Google Scholar]
- Morrill, H.J.; Caffrey, A.R.; Jump, R.L.P.; Dosa, D.; LaPlante, K.L. Antimicrobial Stewardship in Long-Term Care Facilities: A Call to Action. J. Am. Med. Dir. Assoc. 2016, 17, 183.e1–183.e16. [Google Scholar] [CrossRef] [PubMed]
- Thompson, N.D.; Laplace, L.; Epstein, L.; Dumyati, G.; Concannon, C.; Quinlan, G.; Quinlan, G.; Witten, T.; Warnke, L.; Lynfield, R.; et al. Prevalence of Antimicrobial Use and Opportunities to Improve Prescribing Practices in U.S. Nursing Homes. J. Am. Med. Dir. Assoc. 2016, 17, 1151–1153. [Google Scholar] [CrossRef] [PubMed]
- Henig, O.; Kaye, K.S. Bacterial Pneumonia in Older Adults. Infect. Dis. Clin. N. Am. 2017, 31, 689–713. [Google Scholar] [CrossRef] [PubMed]
- Han, X.; Zhou, F.; Li, H.; Xing, X.; Chen, L.; Wang, Y.; Zhang, C.; Liu, X.; Suo, L.; Wang, J.; et al. Effects of age, comorbidity and adherence to current antimicrobial guidelines on mortality in hospitalized elderly patients with community-acquired pneumonia. BMC Infect. Dis. 2018, 18, 192. [Google Scholar] [CrossRef] [PubMed]
- Kothe, H.; Bauer, T.; Marre, R.; Suttorp, N.; Welte, T.; Dalhoff, K.; The Competence Network for Community-Acquired Pneumonia Study Group. Outcome of community-acquired pneumonia: Influence of age, residence status and antimicrobial treatment. Eur. Respir. J. 2008, 32, 139–146. [Google Scholar] [CrossRef] [PubMed]
- Geboers, B.; de Winter, A.F.; Spoorenberg, S.L.W.; Wynia, K.; Reijneveld, S.A. The association between health literacy and self-management abilities in adults aged 75 and older, and its moderators. Qual. Life Res. 2016, 25, 2869–2877. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cramm, J.M.; Twisk, J.; Nieboer, A.P. Self-management abilities and frailty are important for healthy aging among community-dwelling older people; A cross-sectional study. BMC Geriatr. 2014, 14, 28. [Google Scholar] [CrossRef]
- Gualano, M.R.; Gili, R.; Scaioli, G.; Bert, F.; Siliquini, R. General population’s knowledge and attitudes about antibiotics: A systematic review and meta-analysis. Pharmacoepidemiol. Drug Saf. 2015, 24, 2–10. [Google Scholar] [CrossRef]
- Kurniawan, K.; Posangi, J.; Rampengan, N. Association between public knowledge regarding antibiotics and self-medication with antibiotics in Teling Atas Community Health Center, East Indonesia. Med. J. Indones. 2017, 26, 62–69. [Google Scholar] [CrossRef]
- Sirijoti, K.; Hongsranagon, P.; Havanond, P.; Pannoi, W. Assessment of Knowledge Attitudes and Practices Regarding Antibiotic Use in Trang Province, Thailand. J. Health Res. 2014, 28, 299–307. [Google Scholar]
- Jafari, F.; Khatony, A.; Rahmani, E. Prevalence of Self-Medication among the Elderly in Kermanshah-Iran. Glob. J. Health Sci. 2015, 7, 360–365. [Google Scholar] [CrossRef] [PubMed]
- Mahmood, A.; Naqvi, R.; Grewal, A.; Diachun, L.; Gutmanis, I. Antibiotic resistance knowledge in the elderly. UWO Med. J. 2009, 78, 69–72. [Google Scholar]
- McNulty, C.A.M.; Boyle, P.; Nichols, T.; Clappison, P.; Davey, P. Don’t wear me out—The public’s knowledge of and attitudes to antibiotic use. J. Antimicrob. Chemother. 2007, 59, 727–738. [Google Scholar] [CrossRef]
- Kim, S.S.; Moon, S.; Kim, E.J. Public Knowledge and Attitudes Regarding Antibiotic Use in South Korea. J. Korean Acad. Nurs. 2011, 41, 742–749. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kistler, C.E.; Beeber, A.; Becker-Dreps, S.; Ward, K.; Meade, M.; Ross, B.; Sloane, P.D. Nursing Home Nurses’ and Community-Dwelling Older Adults’ Reported Knowledge, Attitudes, and Behavior toward Antibiotic Use. BMC Nurs. 2017, 16, 12. [Google Scholar] [CrossRef]
- Koo, H.S.; Omar, M.S. Knowledge and Attitude towards Antibiotic Use and Awareness on Antibiotic Resistance among Older People in Malaysia. Proc. Pak. Acad. Sci. Part B 2018, 55, 1–9. [Google Scholar]
- Hoffman, D.; Botha, J.; Kleinschmidt, I. An assessment of factors influencing the prescribing of antibiotics in Acute Respiratory Illness: A questionnaire study. S. Afr. Fam. Pract. 2003, 45, 20–24. [Google Scholar]
- Gaarslev, C.; Yee, M.; Chan, G.; Fletcher-Lartey, S.; Khan, R. A mixed methods study to understand patient expectations for antibiotics for an upper respiratory tract infection. Antimicrob. Resist. Infect. Control 2016, 5, 39. [Google Scholar] [CrossRef]
- Davis, M.; Liu, T.-L.; Taylor, Y.; Davidson, L.; Schmid, M.; Yates, T.; Scotton, J.; Spencer, M.D. Exploring Patient Awareness and Perceptions of the Appropriate Use of Antibiotics: A Mixed-Methods Study. Antibiotics 2017, 6, 23. [Google Scholar] [CrossRef]
- Liu, C.; Liu, C.; Wang, D.; Zhang, X. Intrinsic and external determinants of antibiotic prescribing: A multi-level path analysis of primary care prescriptions in Hubei, China. Antimicrob. Resist. Infect. Control 2019, 8, 132. [Google Scholar] [CrossRef]
- Sirota, M.; Round, T.; Samaranayaka, S.; Olga, K. Expectations for antibiotics increase their prescribing: Causal evidence about localized impact. Health Psychol. 2017, 36, 402–409. [Google Scholar] [CrossRef] [PubMed]
- Krejcie, R.V.; Morgan, D.W. Determining sample size for research activities. Educ. Psychol. Meas. 1970, 30, 607–610. [Google Scholar] [CrossRef]
- Oh, A.L.; Hassali, M.; Al-Haddad, M.; Syed Azhar, S.; Shafie, A.; Awaisu, A. Public knowledge and attitudes towards antibiotic usage: A cross-sectional study among the general public in the state of Penang, Malaysia. J. Infect. Dev. Ctries. 2011, 5, 338–347. [Google Scholar]
- Kuzujanakis, M.; Kleinman, K.; Rifas-Shiman, S.; Finkelstein, J.A. Correlates of parental antibiotic knowledge, demand, and reported use. Ambul. Pediatr. 2003, 3, 203–210. [Google Scholar] [CrossRef]
- Lim, K.K.; Teh, C.C. A cross sectional study of public knowledge and attitude towards antibiotics in Putrajaya, Malaysia. South. Med. Rev. 2012, 5, 26–33. [Google Scholar] [PubMed]
- WHO. Antibiotic Resistance: Multi-Country Public Awareness Survey; WHO Press: Geneva, Switzerland, 2015; pp. 1–51. Available online: http://apps.who.int/iris/bitstream/10665/194460/1/9789241509817_eng.pdf?ua=1 (accessed on 10 August 2018).
- Hassali, M.A.; Arief, M.; Saleem, F.; Khan, M.U.; Ahmad, A.; Mariam, W.; Bheemavarapu, H.; Hyed, I.A. Assessment of attitudes and practices of young Malaysian adults about antibiotics use: A cross-sectional study. Pharm. Pract. 2017, 15, 1–7. [Google Scholar] [CrossRef]
- Qamar, M.; Abdullah, N.S.; Khan, J.; Mahmud, A.; Ahmad, A. Knowledge and Attitude Towards Antibiotic Usage Among General Public in Shah Alam, Malaysia. UK J. Pharm. Biosci. 2014, 2, 60–66. [Google Scholar] [CrossRef]
- Choo, S.J.; Chang, C.T.; Lee, J.C.Y.; Munisamy, V.; Tan, C.K.; Raj, J.D.; Mat Taib, R.I.; Thong, K.S.; Shafie, A.A. A cross-sectional study on public belief, knowledge and practice towards antibiotic use in the state of perak, malaysia. J. Infect. Dev. Ctries. 2018, 12, 960–969. [Google Scholar] [CrossRef]
- Yusef, D.; Babaa, A.I.; Bashaireh, A.Z.; Al-Bawayeh, H.H.; Al-Rijjal, K.; Nedal, M.; Kailani, S. Knowledge, practices & attitude toward antibiotics use and bacterial resistance in Jordan: A cross-sectional study. Infect. Dis. Health 2018, 23, 33–40. [Google Scholar]
- Abujheisha, K.Y.; Al-Shdefat, R.; Ahmed, N.; Fouda, M.I. Public Knowledge and Behaviours Regarding Antibiotics Use: A Survey among the General Public. Int. J. Med. Res. Health Sci. 2017, 6, 82–88. [Google Scholar]
- Fatokun, O. Exploring antibiotic use and practices in a Malaysian community. Int. J. Clin. Pharm. 2014, 36, 564–569. [Google Scholar] [CrossRef] [PubMed]
- Mouhieddine, T.H.; Olleik, Z.; Itani, M.M.; Kawtharani, S.; Nassar, H.; Hassoun, R.; Houmani, Z.; El Zein, Z.; Fakih, R.; Mortada, I.K.; et al. Assessing the Lebanese population for their knowledge, attitudes and practices of antibiotic usage. J. Infect. Public Health 2015, 8, 20–31. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zajmi, D.; Berisha, M.; Begolli, I.; Hoxha, R.; Mehmeti, R.; Mulliqi-Osmani, G.; Kurti, A.; Loku, A.; Raka, L. Public knowledge, attitudes and practices regarding antibiotic use in Kosovo. Pharm. Pract. 2017, 15, 827. [Google Scholar] [CrossRef] [PubMed]
- Pavydė, E.; Veikutis, V.; Mačiulienė, A.; Mačiulis, V.; Petrikonis, K.; Stankevičius, E. Public knowledge, beliefs and behavior on antibiotic use and self-medication in Lithuania. Int. J. Environ. Res. Public Health 2015, 12, 7002–7016. [Google Scholar] [CrossRef] [PubMed]
- Awad, A.I.; Aboud, E.A. Knowledge, attitude and practice towards antibiotic use among the public in Kuwait. PLoS ONE 2015, 10, e0117910. [Google Scholar] [CrossRef] [PubMed]
- Mohamed Saleem, T.S.; Chandrakanth, P.; Reddy, M.M.; Gopinath, C.; Rao, M.M. Assessment of Public Knowledge and Attitude Regarding Antibiotic Use in a Tertiary Care Hospital. Asian J. Pharm. Clin. Res. 2016, 9, 118–122. [Google Scholar]
- Lescure, D.; Paget, J.; Schellevis, F.; van Dijk, L. Determinants of Self-Medication with Antibiotics in European and Anglo-Saxon Countries: A Systematic Review of the Literature. Front. Public Health 2018, 6, 370. [Google Scholar] [CrossRef]
- You, J.H.S.; Yau, B.; Choi, K.C.; Chau, C.T.S.; Huang, Q.R.; Lee, S.S. Public Knowledge, Attitudes and Behavior on Antibiotic Use: A Telephone Survey in Hong Kong. Infection 2008, 36, 153–157. [Google Scholar] [CrossRef]
- Freidoony, L.; Kim, C.B.; Haghani, H.; Park, M.B.; Chang, S.J.; Kim, S.H.; Koh, S.B. From visiting a physician to expecting antibiotics: Korean perspectives and practices toward respiratory tract infections. J. Korean Med. Sci. 2017, 32, 278–286. [Google Scholar] [CrossRef]
- Jose, J.; Jimmy, B.; Mohammed Saif AlSabahi, A.G.; Al Sabei, G.A. A study assessing public knowledge, belief and behavior of antibiotic use in an Omani population. Oman Med. J. 2013, 28, 324–330. [Google Scholar] [CrossRef]
- Kardas, P.; Devine, S.; Golembesky, A.; Roberts, C. A systematic review and meta-analysis of misuse of antibiotic therapies in the community. Int. J. Antimicrob. Agents 2005, 26, 106–113. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.; Chen, Y.M.; Hwang, K.L.; Lin, S.J.; Yang, C.C.; Tsay, R.W.; Liu, C.E.; Young, T.G. Behavior, attitudes and knowledge about antibiotic usage among residents of Changhua, Taiwan. J. Microbiol. Immunol. Infect. 2005, 38, 53–59. [Google Scholar] [PubMed]
- Farida, I.; Alyaa Madihah, A.T.; Noraida, M.S. Knowledge, Attitudes and Practices about Antibiotic Use Among the General Public in Malaysia. Southeast Asian J. Trop. Med. Public Health 2014, 45, 1474–1482. [Google Scholar]
- André, M.; Vernby, Å.; Berg, J.; Lundborg, C.S. A survey of public knowledge and awareness related to antibiotic use and resistance in Sweden. J. Antimicrob. Chemother. 2010, 65, 1292–1296. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Alzoubi, K.; Al-Azzam, S.; Alhusban, A.; Mukattash, T.; Al-Zubaidy, S.; Alomari, N.; Khader, Y. An audit on the knowledge, beliefs and attitudes about the uses and side-effects of antibiotics among outpatients attending 2 teaching hospitals in Jordan. East. Mediterr. Health J. 2013, 19, 478–484. [Google Scholar] [CrossRef] [PubMed]
- Brookes-Howell, L.; Elwyn, G.; Hood, K.; Wood, F.; Cooper, L.; Goossens, H.; Leven, M.; Butler, C.C. “The body gets used to them”: Patients’ interpretations of antibiotic resistance and the implications for containment strategies. J. Gen. Intern. Med. 2012, 27, 766–772. [Google Scholar] [CrossRef] [PubMed]
- Bacon-Shone, J. General Public’s Knowledge, Attitude and Practice Survey on Antimicrobial Resistance 2016/17; Research Report; The University of Hong Kong. Social Sciences Research Centre: Hong Kong, China, 2018. Unpublished. Available online: https://www.chp.gov.hk/files/pdf/kap_on_amr_main_report.pdf (accessed on 16 August 2018).
- Hawkings, N.J.; Wood, F.; Butler, C.C. Public attitudes towards bacterial resistance: A qualitative study. J. Antimicrob. Chemother. 2007, 59, 1155–1160. [Google Scholar] [CrossRef]
- Mazińska, B.; Struzycka, I.; Hryniewicz, W. Surveys of public knowledge and attitudes with regard to antibiotics in Poland: Did the European Antibiotic Awareness Day campaigns change attitudes? PLoS ONE 2017, 12, e0172146. [Google Scholar] [CrossRef]
- Kecceci, A.; Bulduk, S. Health Education for the Elderly; Atwood, G.S., Ed.; InTech: Rijeka, Croatia, 2012; ISBN 978-953-51-0080-5. Available online: http//www.intechopen.com/books/geriatrics/healtheducation-for-elderly-people (accessed on 28 August 2019).
- Manafo, E.; Wong, S. Health Literacy Programs for Older Adults: A Systematic Literature Review. Health Educ. Res. 2012, 27, 947–960. [Google Scholar] [CrossRef]
- Smith, C.A.; Chang, E.; Gallego, G.; Khan, A.; Armour, M.; Balneaves, L.G. An Education Intervention to Improve Decision Making and Health Literacy among Older Australians: A Randomised Controlled Trial. BMC Geriatr. 2019, 19, 129. [Google Scholar] [CrossRef]
| Respondents’ Characteristics | n (%) |
|---|---|
| Age (mean ± SD) | 67.72 ± 5.77 |
| Gender | |
| Male | 201 (50.0%) |
| Female | 201 (50.0%) |
| Ethnicity | |
| Malay | 233 (58.0%) |
| Chinese | 111 (27.6%) |
| Indian | 55 (13.7%) |
| Others | 3 (0.7%) |
| Educational level | |
| No formal education | 4 (1.0%) |
| Primary education | 50 (12.4%) |
| Secondary education | 228 (56.7%) |
| Pre-university education | 44 (10.9%) |
| Tertiary education | 76 (18.9%) |
| Main occupation | |
| Unemployed | 19 (4.7%) |
| Employed for wages | 10 (2.5%) |
| Self-employed | 23 (5.7%) |
| Housewife/Househusband | 87 (21.6%) |
| Retiree | 263 (65.4%) |
| Occupation related to healthcare | |
| Yes | 9 (2.2%) |
| No | 393 (97.8%) |
| Monthly income | |
| None | 224 (55.7%) |
| <RM 1000 | 21 (5.2%) |
| RM 1000–RM 3999 | 115 (28.6%) |
| RM 4000–RM 6999 | 31 (7.7%) |
| RM 7000–RM 10,000 | 3 (0.7%) |
| ≥RM 10,000 | 8 (2.0%) |
| n (%) | |
|---|---|
| Last take antibiotics (n = 402) | |
| In the last month | 56 (13.9%) |
| In the last 6 months | 75 (18.7%) |
| In the last year | 41 (10.2%) |
| More than a year ago | 85 (21.1%) |
| Never | 12 (3.0%) |
| Cannot remember | 133 (33.1%) |
| Source of antibiotics (n = 257) | |
| Prescribed after consultation with physician | 249 (96.9%) |
| Prescribed after consultation with dentist | 4 (1.6%) |
| Retail pharmacy/community pharmacy | 3 (1.2%) |
| Leftover antibiotics (own/someone’s else) | 1 (0.3%) |
| Reason(s) to take antibiotics (n = 257) | |
| Fever | 56 (19.4%) |
| Pain/inflammation | 41 (14.2%) |
| Respiratory tract infection | 102 (35.4%) |
| Urinary tract infection | 16 (5.6%) |
| Skin problems/wounds/cuts | 21 (7.3%) |
| Dental problem | 4 (1.4%) |
| Diarrhoea/vomiting | 3 (1.0%) |
| Others | 27 (9.4%) |
| Do not know | 6 (2.1%) |
| Cannot remember | 12 (4.2%) |
| Get advice on how to take antibiotics (n = 257) | |
| Yes | 246 (95.7%) |
| No | 11 (4.3%) |
| Source(s) of advice (n = 257) | |
| Physician | 229 (74.6%) |
| Dentist | 3 (0.9%) |
| Pharmacist | 46 (15.0%) |
| Nurse | 7 (2.3%) |
| Friends/family/neighbours | 15 (4.9%) |
| Patient information leaflet | 5 (1.6%) |
| Mass media | 2 (0.7%) |
| Inappropriate practice | |
| Obtained antibiotics without a prescription (n = 402) | |
| Yes | 14 (3.5%) |
| No | 388 (96.5%) |
| Used own/others’ leftover antibiotics without advice from healthcare profession (n = 402) | |
| Yes | 14 (3.5%) |
| No | 388 (96.5%) |
| Not completed antibiotic course (n = 402) | |
| Yes | 69 (17.2%) |
| No | 333 (82.8%) |
| Shared own leftover antibiotics to friends or family or neighbours (n = 402) | |
| Yes | 10 (2.5%) |
| No | 392 (97.5%) |
| Engaged in at least one inappropriate practice (n = 402) | |
| Yes | 83 (20.65%) |
| No | 319 (79.35%) |
| Respondents’ Answer, n (%) | |||||
|---|---|---|---|---|---|
| Correct | Incorrect | Not Sure | |||
| Knowledge about antibiotic use | |||||
| 1. | Antibiotics are medicines that can kill bacteria. | True | 283 (70.4%) | 25 (6.2%) | 94 (23.4%) |
| 2. | Antibiotics can be used to treat viral infections. | False | 76 (18.9%) | 215 (53.5%) | 111 (27.6%) |
| 3. | Antibiotics work on most colds and coughs. | False | 146 (36.3%) | 216 (53.7%) | 40 (10.0%) |
| 4. | Antibiotics can kill bacteria that normally live on the skin and gut (digestion tract). | True | 220 (54.7%) | 60 (14.9%) | 122 (30.3%) |
| 5. | Bacteria that normally live on the skin and in the gut are good for your health. | True | 229 (56.9%) | 97 (24.1%) | 76 (18.9%) |
| 6. | Antibiotics are the same as medications used to relieve pain and fever such as aspirin and paracetamol (Panadol). | False | 179 (44.5%) | 194 (48.3%) | 29 (7.2%) |
| 7. | Penicillin is an antibiotic. | True | 129 (32.1%) | 122 (30.3) | 151 (37.6%) |
| 8. | Antibiotics may cause allergy reactions. | True | 265 (65.9%) | 79 (19.7%) | 58 (14.4%) |
| 9. | All antibiotics do not cause side effects. | False | 223 (55.5%) | 114 (28.3%) | 65 (16.2%) |
| 10. | It is okay to stop taking antibiotic when symptoms are improving. | False | 320 (79.6%) | 72 (17.9%) | 10 (2.5%) |
| 11. | Taking less antibiotics than prescribed is healthier than taking the full course prescribed. | False | 333 (82.8%) | 54 (13.4%) | 15 (3.7%) |
| 12. | Overuse of antibiotics can cause the antibiotics to lose effectiveness in long term. | True | 261 (64.9%) | 71 (17.7%) | 70 (17.4%) |
| Knowledge about antibiotic resistance | |||||
| 1. | Antibiotic resistance occurs when your body becomes resistant to antibiotics and they no longer work as well. | False | 60 (14.9%) | 273 (67.9%) | 69 (17.2%) |
| 2. | Many infections are becoming increasingly resistant to treatment by antibiotics. | True | 246 (61.2%) | 68 (16.9%) | 88 (21.9%) |
| 3. | If bacteria are resistant to antibiotics, it can be very difficult or impossible to treat the infections they cause. | True | 288 (71.6%) | 43 (10.7%) | 71 (17.7%) |
| 4. | Antibiotic resistance is an issue that could affect me or my family. | True | 195 (48.5%) | 124 (30.8%) | 83 (20.6%) |
| 5. | Antibiotic resistance is an issue in other countries but not here. | False | 240 (59.7%) | 40 (10.0%) | 122 (30.3%) |
| 6. | Antibiotic resistance is only a problem for people who take antibiotics regularly. | False | 72 (17.9%) | 251 (62.4%) | 79 (19.7%) |
| 7. | Bacteria which are resistant to antibiotics can be spread from person to person. | True | 167 (41.5%) | 143 (35.6%) | 92 (22.9%) |
| 8. | Antibiotic-resistant infections could make medical procedures like surgery, organ transplants and cancer treatment much more dangerous. | True | 180 (44.8%) | 56 (13.9%) | 166 (41.3%) |
| n (%) | Mean Knowledge Score (±SD) | p-value | ||
|---|---|---|---|---|
| If I expect an antibiotic, I am less satisfied with the physician visit if I do not receive one. | Agree | 50 (12.44%) | 11.2 ± 3.245 | 0.030 * |
| Disagree/ neutral | 352 (87.56%) | 10.05 ± 3.522 | ||
| I would rather take an antibiotic that may not be needed than wait to see if I will get better without it. | Agree | 48 (11.94%) | 9.38 ± 3.751 | 0.086 |
| Disagree/ neutral | 354 (88.06%) | 10.30 ± 3.462 | ||
| If a physician does not prescribe an antibiotic when I think one is needed, I will visit another physician. | Agree | 75 (18.66%) | 10.95 ± 3.238 | 0.0928 |
| Disagree/ neutral | 327 (81.34%) | 10.02 ± 3.546 | ||
| I expect the physician to discuss with me regarding the need of an antibiotic for my symptoms, rather than just giving me a prescription. | Agree | 335(83.40%) | 8.95 ± 4.307 | 0.053 |
| Disagree/ neutral | 67 (16.60%) | 10.33 ± 3.381 |
| Expectations to be Prescribed Antibiotic for Their Cold, Flu or Cough, n (%) | χ2, p-value | |||
|---|---|---|---|---|
| Yes | No | |||
| Antibiotics can be used to treat viral infections. | Answered correctly | 6 (8.1%) | 68 (91.9%) | χ2 = 15.576, p < 0.001* |
| Answered incorrectly/ not sure | 100 (30.5%) | 228 (69.5%) | ||
| Antibiotics work on most colds and coughs. | Answered correctly | 8 (5.4%) | 139 (94.6%) | χ2 = 52.267, p < 0.001* |
| Answered incorrectly/ not sure | 98 (38.4%) | 157 (61.6%) | ||
| Inappropriate Practice of Not Completing Antibiotics Prescribed, n (%) | χ2, p-value | |||
|---|---|---|---|---|
| Yes | No | |||
| It is okay to stop taking antibiotics when symptoms are improving. | Answered correctly | 26 (8.1%) | 294 (91.9%) | χ2 = 90.153, p < 0.001* |
| Answered incorrectly/ not sure | 43 (52.4%) | 39 (47.6%) | ||
| Taking less antibiotics than prescribed is healthier than taking the full course prescribed. | Answered correctly | 40 (12.0%) | 293 (88.0%) | χ2 = 36.221, p < 0.001* |
| Answered incorrectly/ not sure | 29 (42.0%) | 40 (58.0%) | ||
| Factors | n (%) | χ2, p-value | |
|---|---|---|---|
| Adequate Knowledge (≥10) | Inadequate Knowledge (<10) | ||
| Age | |||
| 60–69 years old | 163 (61.7%) | 101 (38.3%) | χ2 = 9.979, p = 0.007* |
| 70–79 years old | 68 (58.6%) | 48 (41.4%) | |
| ≥80 | 6 (27.3%) | 16 (72.7%) | |
| Gender | |||
| Male | 124 (61.7%) | 77 (38.3%) | χ2 = 1.244, p =0.265 |
| Female | 113 (56.2%) | 88 (43.8%) | |
| Ethnicity | |||
| Malay | 140 (60.1%) | 93 (39.9%) | χ2 = 2.289, p = 0.318 |
| Chinese | 68 (61.3%) | 43 (38.7%) | |
| Indian and others | 29 (50.0%) | 29 (50.0%) | |
| Educational level | |||
| No formal education and primary education | 23 (42.6%) | 31 (57.4%) | χ2 = 16.07, p < 0.001* |
| Secondary education | 127 (55.7%) | 101 (44.3%) | |
| Pre-university and tertiary education | 87 (72.5%) | 33 (27.5%) | |
| Last receipt of antibiotics within the past 6 months | |||
| Yes | 73 (55.7%) | 58 (44.3%) | χ2 = 0.838, p = 0.360 |
| No | 164 (60.5%) | 107 (39.5%) | |
| Last receipt of antibiotics within the past 1 year | |||
| Yes | 103 (59.9%) | 69 (40.1%) | χ2 = 0.107, p = 0.743 |
| No | 134 (58.3%) | 96 (41.7%) | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kong, L.S.; Islahudin, F.; Muthupalaniappen, L.; Chong, W.W. Knowledge and Expectations on Antibiotic Use among Older Adults in Malaysia: A Cross-Sectional Survey. Geriatrics 2019, 4, 61. https://doi.org/10.3390/geriatrics4040061
Kong LS, Islahudin F, Muthupalaniappen L, Chong WW. Knowledge and Expectations on Antibiotic Use among Older Adults in Malaysia: A Cross-Sectional Survey. Geriatrics. 2019; 4(4):61. https://doi.org/10.3390/geriatrics4040061
Chicago/Turabian StyleKong, Lai San, Farida Islahudin, Leelavathi Muthupalaniappen, and Wei Wen Chong. 2019. "Knowledge and Expectations on Antibiotic Use among Older Adults in Malaysia: A Cross-Sectional Survey" Geriatrics 4, no. 4: 61. https://doi.org/10.3390/geriatrics4040061





