Baseline Body Mass Predicts Average Depressive Symptoms over the Next Two Decades for White but Not Black Older Adults
Abstract
1. Introduction
2. Methods
2.1. Setting and Design
2.2. Ethics
2.3. Participants and Sampling
2.4. Process
2.5. Measures
2.6. Statistical Analysis
3. Results
3.1. Univariate Analysis
3.2. Bivariate Analysis
3.3. Multivariable Analysis
4. Discussion
4.1. Previous Research
4.2. “Jolly Fat” Hypothesis
4.3. Culture and Social Norms
4.4. Cultural Moderation Hypothesis
4.5. Blacks’ Resilience
4.6. Differential Effects
4.7. Black–White Mental Health Paradox
4.8. Inflammation
4.9. Implications
4.10. Limitations
4.11. Future Research
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Office of Disease Prevention and Health Promotion (ODPHP). Healthy People 2020 Leading Health Indicators: Nutrition, Physical Activity, and Obesity. May 2014. Available online: https://www.healthypeople.gov/sites/default/files/HP2020_LHI_Nut_PhysActiv_0.pdf (accessed on 10 January 2019).
- Greenberg, J.A. Obesity and early mortality in the United States. Obesity 2013, 21, 405–412. [Google Scholar] [CrossRef] [PubMed]
- Cuijpers, P.; Smit, F. Excess mortality in depression: A meta-analysis of community studies. J. Affect. Disord. 2002, 72, 227–236. [Google Scholar] [CrossRef]
- Kodjebacheva, G.; Kruger, D.J.; Rybarczyk, G.; Cupal, S. Racial/ethnic and gender differences in the association between depressive symptoms and higher body mass index. J. Public Health 2015, 37, 419–426. [Google Scholar] [CrossRef] [PubMed]
- Kelley, E.A.; Bowie, J.V.; Griffith, D.M.; Bruce, M.; Hill, S.; Thorpe, R.J., Jr. Geography, Race/Ethnicity, and Obesity Among Men in the United States. Am. J. Men Health. 2016, 10, 228–236. [Google Scholar] [CrossRef] [PubMed]
- Murphy, C.C.; Martin, C.F.; Sandler, R.S. Racial differences in obesity measures and risk of colorectal adenomas in a large screening population. Nutr. Cancer. 2015, 67, 98–104. [Google Scholar] [CrossRef] [PubMed]
- Assari, S.; Caldwell, C.H. Gender and Ethnic Differences in the Association Between Obesity and Depression Among Black Adolescents. J. Racial Ethn. Health Disparities 2015, 2, 481–493. [Google Scholar] [CrossRef]
- Assari, S.; Lankarani, M.M. Mediating Effect of Perceived Overweight on the Association between Actual Obesity and Intention for Weight Control; Role of Race, Ethnicity, and Gender. Int. J. Prev. Med. 2015, 6, 102. [Google Scholar] [CrossRef]
- Lincoln, K.D.; Abdou, C.M.; Lloyd, D. Race and socioeconomic differences in obesity and depression among Black and non-Hispanic White Americans. J. Health Care Poor Underserve 2014, 25, 257–275. [Google Scholar] [CrossRef]
- Assari, S. Psychosocial Correlates of Body Mass Index in the United States: Intersection of Race, Gender and Age. Iran. J. Psychiatry Behav. Sci. 2016, 10, e3458. [Google Scholar] [CrossRef]
- Assari, S.; Nikahd, A.; Malekahmadi, M.R.; Lankarani, M.M.; Zamanian, H. Race by gender group differences in the protective effects of socioeconomic factors against sustained health problems across five domains. J. Racial Ethn. Health Disparities 2017, 4, 884–894. [Google Scholar] [CrossRef]
- Assari, S. Combined Racial and Gender Differences in the Long-Term Predictive Role of Education on Depressive Symptoms and Chronic Medical Conditions. J. Racial Ethn. Health Disparities 2017, 4, 385–396. [Google Scholar] [CrossRef] [PubMed]
- Assari, S.; Caldwell, C.H. High Risk of Depression in High-Income African American Boys. J. Racial Ethn. Health Disparities 2018, 5, 808–819. [Google Scholar] [CrossRef] [PubMed]
- Case, S.M.; Stewart, J.C. Race/ethnicity moderates the relationship between depressive symptom severity and C-reactive protein: 2005–2010 NHANES Data. Brain Behav. Immun. 2014, 41, 101–108. [Google Scholar] [CrossRef] [PubMed]
- Vrany, E.A.; Berntson, J.M.; Khambaty, T.; Stewart, J.C. Depressive symptom clusters and insulin resistance: Race/ethnicity as a moderator in 2005–2010 NHANES Data. Ann. Behav. Med. 2016, 50, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Assari, S. Association Between Self-Esteem and Depressive Symptoms Is Stronger Among Black than White Older Adults. J. Racial Ethn. Health Disparities 2017, 4, 687–695. [Google Scholar] [CrossRef] [PubMed]
- Assari, S.; Lankarani, M.M. Reciprocal Associations between Depressive Symptoms and Mastery among Older Adults; Black-White Differences. Front. Aging Neurosci. 2017, 8, 279. [Google Scholar] [CrossRef] [PubMed]
- Assari, S.; Caldwell, C.H. The Link between Mastery and Depression among Black Adolescents; Ethnic and Gender Differences. Behav. Sci. 2017, 7, 32. [Google Scholar] [CrossRef]
- Assari, S.; Lankarani, M.M. Depressive Symptoms Are Associated with More Hopelessness among White than Black Older Adults. Front. Public Health. 2016, 4, 82. [Google Scholar] [CrossRef]
- Lankarani, M.M.; Assari, S. Positive and Negative Affect More Concurrent among Blacks than Whites. Behav. Sci. 2017, 7, 48. [Google Scholar] [CrossRef]
- Assari, S.; Burgard, S.A.; Zivin, K. Long term reciprocal associations between depression and chronic medical conditions; longitudinal support for Black-White health paradox. J. Racial Ethn. Health Disparities 2015, 2, 589–597. [Google Scholar] [CrossRef]
- Assari, S.; Moazen-Zadeh, E.; Lankarani, M.M.; Micol-Foster, V. Race, depressive symptoms, and all-cause mortality in the United States. Front. Public Health. 2016, 4, 40. [Google Scholar] [CrossRef] [PubMed]
- Assari, S.; Lankarani, M.M. Chronic medical conditions and negative affect; racial variation in reciprocal associations over time. Front. Psychiatry 2016, 7, 140. [Google Scholar] [CrossRef] [PubMed]
- Assari, S. Hostility, anger, and cardiovascular mortality among Blacks and Whites. Res. Cardiovasc. Med. 2017, 6, 2. [Google Scholar] [CrossRef]
- Assari, S. High Income Protects Whites but Not African Americans against Risk of Depression. Healthcare 2018, 6, 37. [Google Scholar] [CrossRef] [PubMed]
- Assari, S. Self-rated Health and Mortality due to Kidney Diseases: Racial Differences in the United States. Adv. Biomed. Res. 2018, 7, 4. [Google Scholar] [CrossRef]
- Assari, S. General self-efficacy and mortality in the USA; racial differences. J. Racial Ethn. Health Disparities 2017, 4, 746–757. [Google Scholar] [CrossRef] [PubMed]
- Assari, S. Race, sense of control over life, and short-term risk of mortality among older adults in the United States. Arch. Med. Sci. 2017, 13, 1233–1240. [Google Scholar] [CrossRef]
- Assari, S.; Lankarani, M.M.; Burgard, S.A. Black White difference in long term predictive power of self-rated health on all-cause mortality in United States. Ann Epidemiol. 2016, 26, 106–114. [Google Scholar] [CrossRef]
- Hawkins, M.A.W.; Miller, D.K.; Stewart, J.C. A 9-year, bidirectional prospective analysis of depressive symptoms and adiposity: The African American Health Study. Obesity 2015, 23, 192–199. [Google Scholar] [CrossRef]
- Blazer, D.G.; Moody-Ayers, S.; Craft-Morgan, J.; Burchett, B. Depression in diabetes and obesity: Racial/ethnic/gender issues in older adults. J. Psych. Res. 2002, 53, 913–916. [Google Scholar] [CrossRef]
- Carter, J.D.; Assari, S. Sustained Obesity and Depressive Symptoms over 6 Years: Race by Gender Differences in the Health and Retirement Study. Front. Aging Neurosci. 2017, 8, 312. [Google Scholar] [CrossRef] [PubMed]
- Assari, S.; Rothberg, A.E.; Evans, S.J.; Reger, H.B.; Burant, C.F. Depressive Symptoms and Well-being of Individuals with Obesity; Race by Gender Differences. Int. J. Endocrinol. Metab. 2017. [Google Scholar] [CrossRef]
- Curhan, K.B.; Sims, T.; Markus, H.R.; Kitayama, S.; Karasawa, M.; Kawakami, N.; Love, G.D.; Coe, C.L.; Miyamoto, Y.; Ryff, C.D. Just how bad negative affect is for your health depends on culture. Psychol. Sci. 2014, 25, 2277–2280. [Google Scholar] [CrossRef] [PubMed]
- Kitayama, S.; Park, J.; Boylan, J.M.; Miyamoto, Y.; Levine, C.S.; Markus, H.R.; Karasawa, M.; Coe, C.L.; Kawakami, N.; Love, G.D.; et al. Expression of anger and ill health in two cultures: An examination of inflammation and cardiovascular risk. Psychol. Sci. 2015, 26, 211–220. [Google Scholar] [CrossRef] [PubMed]
- Miyamoto, Y.; Boylan, J.M.; Coe, C.L.; Curhan, K.B.; Levine, C.S.; Markus, H.R.; Park, J.; Kitayama, S.; Kawakami, N.; Karasawa, M.; et al. Negative emotions predict elevated interleukin-6 in the United States but not in Japan. Brain Behav. Immun. 2013, 34, 79–85. [Google Scholar] [CrossRef] [PubMed]
- Park, J.; Kitayama, S.; Markus, H.R.; Coe, C.L.; Miyamoto, Y.; Karasawa, M.; Curhan, B.; Love, G.D.; Kawakami, N.; Boylan, J.M.; et al. Social status and anger expression: The cultural moderation hypothesis. Emotion 2013, 13, 1122–1131. [Google Scholar] [CrossRef] [PubMed]
- Assari, S. Additive Effects of Anxiety and Depression on Body Mass Index among Blacks: Role of Ethnicity and Gender. Int. Cardiovasc. Res. J. 2014, 8, 44–51. [Google Scholar]
- Assari, S. Association between obesity and depression among American Blacks: Role of ethnicity and gender. J. Racial Ethn. Health Disparities 2014, 1, 36–44. [Google Scholar] [CrossRef]
- Keyes, C.L. The Black-White paradox in health: Flourishing in the face of social inequality and discrimination. J. Pers. 2009, 77, 1677–1706. [Google Scholar] [CrossRef]
- Assari, S.; Sonnega, A.; Pepin, R.; Leggett, A. Residual effects of restless sleep over depressive symptoms on chronic medical conditions: Race by gender differences. J. Racial Ethn. Health Disparities 2017, 4, 59–69. [Google Scholar] [CrossRef]
- Assari, S.; Burgard, S. Black-White differences in the effect of baseline depressive symptoms on deaths due to renal diseases: 25 year follow up of a nationally representative community sample. J. Renal Inj. Prev. 2015, 4, 127–134. [Google Scholar]
- Assari, S.; Moghani Lankarani, M. Secular and Religious Social Support Better Protect Blacks than Whites against Depressive Symptoms. Behav. Sci. 2018, 8, 46. [Google Scholar] [CrossRef] [PubMed]
- Anda, R.; Williamson, D.; Jones, D.; Macera, C.; Eaker, E.; Glassman, A.; Marks, J. Depressed affect, hopelessness, and the risk of ischemic heart disease in a cohort of US adults. Epidemiology 1993, 285–294. [Google Scholar] [CrossRef]
- Stewart, J.C. One Effect Size Does Not Fit All—Is the Depression-Inflammation Link Missing in Racial/Ethnic Minority Individuals? JAMA Psychiatry 2016, 73, 301–302. [Google Scholar] [CrossRef] [PubMed]
- Johnson, E.H. The role of the experience and expression of anger and anxiety in elevated blood pressure among black and white adolescents. J. Natl. Med. Assoc. 1989, 81, 573–584. [Google Scholar] [PubMed]
- Morris, A.; Zhao, L.; Ahmed, Y.; Stoyanova, N.; Hooper, W.C.; Gibbons, G.; Vaccarino, V. Association between depression and inflammation—Differences by race and sex: The META-Health study. Psych. Med. 2011, 73, 462. [Google Scholar] [CrossRef]
- Gold, R.; Michael, Y.L.; Whitlock, E.P.; Hubbell, F.A.; Mason, E.D.; Rodriguez, B.L.; Safford, M.M.; Sarto, G.E. Race/ethnicity, socioeconomic status, and lifetime morbidity burden in the women’s health initiative: A cross-sectional analysis. J. Women Health 2006, 15, 1161–1173. [Google Scholar] [CrossRef]
- Franks, P.; Muennig, P.; Lubetkin, E.; Jia, H. The burden of disease associated with being African-American in the United States and the contribution of socio-economic status. Soc. Sci Med. 2006, 62, 2469–2478. [Google Scholar] [CrossRef]
- Williams, D.R.; Mohammed, S.A.; Leavell, J.; Collins, C. Race, socioeconomic status, and health: complexities, ongoing challenges, and research opportunities. Annals New York Acad. Sci. 2010, 1186, 69–101. [Google Scholar] [CrossRef]
- Teti, M.; Martin, A.E.; Ranade, R.; Massie, J.; Malebranche, D.J.; Tschann, J.M.; Bowleg, L. “I’m a keep rising. I’m a keep going forward, regardless”: Exploring Black men’s resilience amid sociostructural challenges and stressors. Qual. Health Res. 2012, 22, 524–533. [Google Scholar] [CrossRef]
- Ward, E.C.; Mengesha, M.M.; Issa, F. Older African American women’s lived experiences with depression and coping behaviours. J. Psychiatr. Ment. Health Nurs. 2014, 21, 46–59. [Google Scholar] [CrossRef] [PubMed]
- Assari, S. Unequal gain of equal resources across racial groups. Int. J. Health Policy Manag. 2018, 7, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Assari, S.; Lankarani, M.M. Association between stressful life events and depression; intersection of race and gender. J. Racial Ethn. Health Disparities 2016, 3, 349–356. [Google Scholar] [CrossRef] [PubMed]
- Assari, S. Black-White Differences in Social, Psychological, and Medical Correlates of Depression in the United States. Int. J. Epid. Res. 2018, 5, 40–42. [Google Scholar] [CrossRef]
- Pope, M.; Corona, R.; Belgrave, F.Z. Nobody’s perfect: A qualitative examination of African American maternal caregivers’ and their adolescent girls’ perceptions of body image. Body Image 2014, 11, 307–317. [Google Scholar] [CrossRef] [PubMed]
- Jackson, K.L.; Janssen, I.; Appelhans, B.M.; Kazlauskaite, R.; Karavolos, K.; Dugan, S.A.; Avery, E.A.; Shipp-Johnson, K.J.; Powell, L.H.; Kravitz, H.M. Body image satisfaction and depression in midlife women: The Study of Women’s Health Across the Nation (SWAN). Arch. Women Ment. Health. 2014, 17, 177–187. [Google Scholar] [CrossRef]
- Ehlinger, P.P.; Blashill, A.J. Self-perceived vs. actual physical attractiveness: Associations with depression as a function of sexual orientation. J. Affect. Disord. 2016, 189, 70–76. [Google Scholar] [CrossRef]
- Webb, H.J.; Zimmer-Gembeck, M.J.; Donovan, C.L. The appearance culture between friends and adolescent appearance-based rejection sensitivity. J. Adolesc. 2014, 37, 347–358. [Google Scholar] [CrossRef]
- Webb, J.B.; Butler-Ajibade, P.; Robinson, S.A. Considering an affect regulation framework for examining the association between body dissatisfaction and positive body image in Black older adolescent females: Does body mass index matter? Body Image 2014, 11, 426–437. [Google Scholar] [CrossRef]
- Altintas, A.; Asci, F.H.; Kin-Isler, A.; Guven-Karahan, B.; Kelecek, S.; Ozkan, A.; Yilmaz, A.; Kara, F.M. The role of physical activity, body mass index and maturity status in body-related perceptions and self-esteem of adolescents. Ann. Hum. Biol. 2014, 41, 395–402. [Google Scholar] [CrossRef]
- Coy, A.E.; Green, J.D.; Price, M.E. Why is low waist-to-chest ratio attractive in males? The mediating roles of perceived dominance, fitness, and protection ability. Body Image 2014, 11, 282–289. [Google Scholar] [CrossRef] [PubMed]
- Das, B.M.; Evans, E.M. Understanding weight management perceptions in first-year college students using the health belief model. J. Am. Coll. Health. 2014, 62, 488–497. [Google Scholar] [CrossRef] [PubMed]
- Laus, M.F.; Costa, T.M.; Almeida, S.S. Gender differences in body image and preferences for an ideal silhouette among Brazilian undergraduates. Eat. Behav. 2015, 19, 159–162. [Google Scholar] [CrossRef] [PubMed]
- Stephen, I.D.; Perera, A.T. Judging the differences between women’s attractiveness and health: Is there really a difference between judgments made by men and women? Body Image 2014, 11, 183–186. [Google Scholar] [CrossRef] [PubMed]
- Chithambo, T.P.; Huey, S.J. Black/white differences in perceived weight and attractiveness among overweight women. J. Obes. 2013, 2013, 320326. [Google Scholar] [CrossRef]
- Fletcher, J.M. The interplay between gender, race and weight status: Self perceptions and social consequences. Econ. Hum Biol. 2014, 14, 79–91. [Google Scholar] [CrossRef]
- Gitau, T.M.; Micklesfield, L.K.; Pettifor, J.M.; Norris, S.A. Eating attitudes, body image satisfaction and self-esteem of South African Black and White male adolescents and their perception of female body silhouettes. J. Child Adolesc. Ment. Health 2014, 26, 193–205. [Google Scholar] [CrossRef]
- Mikolajczyk, R.T.; Iannotti, R.J.; Farhat, T.; Thomas, V. Ethnic differences in perceptions of body satisfaction and body appearance among U.S. schoolchildren: A cross-sectional study. BMC Public Health 2012, 12, 425. [Google Scholar] [CrossRef]
- Richmond, T.K.; Austin, S.B.; Walls, C.E.; Subramanian, S.V. The association of body mass index and externally perceived attractiveness across race/ethnicity, gender, and time. J. Adolesc Health 2012, 50, 74–79.e2. [Google Scholar] [CrossRef]
- Sabik, N.J. Ageism and body esteem: Associations with psychological well-being among late middle-aged African American and European American women. J. Gerontol. 2015, 70, 191–201. [Google Scholar] [CrossRef]
- Thomas, S.; Ness, R.B.; Thurston, R.C.; Matthews, K.; Chang, C.C.; Hess, R. Racial differences in perception of healthy body weight in midlife women: Results from the Do Stage Transitions Result in Detectable Effects study. Menopause 2013, 20, 269–273. [Google Scholar] [CrossRef] [PubMed]
- Blostein, F.; Assari, S.; Caldwell, C.H. Gender and Ethnic Differences in the Association Between Body Image Dissatisfaction and Binge Eating Disorder among Blacks. J. Racial Ethn. Health Disparities 2017, 4, 529–538. [Google Scholar] [CrossRef] [PubMed]
- Baruth, M.; Sharpe, P.A.; Magwood, G.; Wilcox, S.; Schlaff, R.A. Body Size Perceptions among Overweight and Obese African American Women. Ethn. Dis. 2015, 25, 391–398. [Google Scholar] [CrossRef] [PubMed]
- Gustat, J.; Carton, T.W.; Shahien, A.A.; Andersen, L. Body Image Satisfaction Among Blacks. Health Educ. Behav. 2016, 44, 131–140. [Google Scholar] [CrossRef] [PubMed]
- Lynch, E.B.; Kane, J. Body size perception among African American women. J. Nutr. Educ. Behav. 2014, 46, 412–417. [Google Scholar] [CrossRef] [PubMed]
- Nichols, S.D.; Dookeran, S.S.; Ragbir, K.K.; Dalrymple, N. Body image perception and the risk of unhealthy behaviours among university students. West Indian Med. J. 2009, 58, 465–471. [Google Scholar] [PubMed]
- Capodilupo, C.M.; Kim, S. Gender and race matter: The importance of considering intersections in Black women’s body image. J. Couns. Psychol. 2014, 61, 37–49. [Google Scholar] [CrossRef] [PubMed]
- O’Neal, C.W.; Arnold, A.L.; Lucier-Greer, M.; Wickrama, K.A.; Bryant, C.M. Economic pressure and health and weight management behaviors in African American couples: A family stress perspective. J. Health Psychol. 2015, 20, 625–637. [Google Scholar] [CrossRef]
- Capodilupo, C.M. One size does not fit all: Using variables other than the thin ideal to understand Black women’s body image. Cult. Divers. Ethn. Minor. Psychol. 2015, 21, 268–278. [Google Scholar] [CrossRef]
- Argyrides, M.; Kkeli, N. Predictive factors of disordered eating and body image satisfaction in Cyprus. Int. J. Eat. Disord. 2015, 48, 431–435. [Google Scholar] [CrossRef]
- Okosun, I.S.; Choi, S.; Matamoros, T.; Dever, G.E. Obesity is associated with reduced self-rated general health status: Evidence from a representative sample of white, black, and Hispanic Americans. Prev. Med. 2001, 32, 429–436. [Google Scholar] [CrossRef] [PubMed]
- Romo-Perez, V.; Souto, D.; Mota, J. Walking, body mass index, and self-rated health in a representative sample of Spanish adults. Cadernos de Saúde Pública 2016, 32, e00166414. [Google Scholar] [CrossRef] [PubMed]
- Jokela, M.; Berg, V.; Silventoinen, K.; Batty, G.D.; Singh-Manoux, A.; Kaprio, J.; Smith, G.D.; Kivimäki, M. Body Mass Index and Depressive Symptoms: Testing for Adverse and Protective Associations in Two Twin Cohort Studies. Twin Res. Hum. Genet. 2016, 19, 306–311. [Google Scholar] [CrossRef] [PubMed]
- Stunkard, A.J.; Faith, M.S.; Allison, K.C. Depression and obesity. Biol. Psychiatry 2003, 54, 330–337. [Google Scholar] [CrossRef]
- Remigio-Baker, R.A.; Allison, M.A.; Schreiner, P.J.; Carnethon, M.R.; Nettleton, J.A.; Mujahid, M.S.; Jensky, N. Sex and race/ethnic disparities in the cross-sectional association between depressive symptoms and muscle mass: the Multi-ethnic Study of Atherosclerosis. BMC Psychiatry 2015, 15, 221. [Google Scholar] [CrossRef] [PubMed]
- Heeringa, S.G.; Connor, J.H. Technical Description of the Health and Retirement Survey Sample Design. 1995. Available online: http://www.hrsonline.isr.umich.edu/sitedocs/userg/HRSSAMP.pdf (accessed on 10 January 2019).
- Sonnega, A.; Faul, J.D.; Ofstedal, M.B.; Langa, K.M.; Phillips, J.W.; Weir, D.R. Cohort Profile: The Health and Retirement Study (HRS). Int. J. Epidemiol. 2014, 43, 576–585. [Google Scholar] [CrossRef]
- Spencer, E.A.; Appleby, P.N.; Davey, G.K.; Key, T.J. Validity of self-reported height and weight in 4808 EPIC-Oxford participants. Public Health Nutr. 2002, 5, 561–565. [Google Scholar] [CrossRef]
- Kuczmarski, M.F.; Kuczmarski, R.J.; Najjar, M. Effects of age on validity of self-reported height, weight, and body mass index: Findings from the Third National Health and Nutrition Examination Survey, 1988–1994. J. Am. Diet. Assoc. 2001, 101, 28–34. [Google Scholar] [CrossRef]
- Radloff, L.S. The CES-D scale: A self-report depression scale for research in the general population. Appl. Psychol. Meas. 1977, 1, 385–401. [Google Scholar] [CrossRef]
- Alessi, P. Professional iOS Database Applications, and Programming, 2nd ed.; Taylor and Francis Group: New York, NY, USA, 2002. [Google Scholar]
- Arbuckle, J.L. Amos™ 18 User’s Guide; Amos Development Corporation: Crawfordville, FL, USA, 2009. [Google Scholar]
- Kline, R.B. Principles and Practice of Structural Equation Modeling; Guilford Press: New York, NY, USA, 2011. [Google Scholar]
- Hu, L.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct. Equ. Model. 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Lei, M.; Lomax, R.G. The effect of varying degrees of nonnormality in structural equation modeling. Struct. Equ. Model. 2005, 12, 1–27. [Google Scholar] [CrossRef]
- Tabachnick, B.G.; Fidell, L.S. Using Multivariate Statistics, 3rd ed.; Harper Collins: New York, NY, USA, 1996. [Google Scholar]
- Assari, S. The link between mental health and obesity: Role of individual and contextual factors. Int. J. Prev. Med. 2014, 5, 247–249. [Google Scholar]
- Assari, S.; Caldwell, C.H.; Zimmerman, M.A. Depressive Symptoms During Adolescence Predict Adulthood Obesity Among Black Females. J. Racial Ethn. Health Disparities 2018, 5, 774–781. [Google Scholar] [CrossRef] [PubMed]
- Watkins, D.C.; Assari, S.; Johnson-Lawrence, V. Race and Ethnic Group Differences in Comorbid Major Depressive Disorder, Generalized Anxiety Disorder, and Chronic Medical Conditions. J. Racial Ethn. Health Disparities 2015, 2, 385–394. [Google Scholar] [CrossRef] [PubMed]
- Remigio-Baker, R.A.; Allison, M.A.; Schreiner, P.J.; Szklo, M.; Crum, R.M.; Leoutsakos, J.M.; Roux, A.V.D. Difference by sex but not by race/ethnicity in the visceral adipose tissue-depressive symptoms association: the Multi-Ethnic Study of Atherosclerosis. Psychoneuroendocrinology 2014, 47, 78–87. [Google Scholar] [CrossRef]
- Hicken, M.T.; Lee, H.; Mezuk, B.; Kershaw, K.N.; Rafferty, J.; Jackson, J.S. Racial and ethnic differences in the association between obesity and depression in women. J. Women Health 2013, 22, 445–542. [Google Scholar] [CrossRef]
- Kim, E.; Song, J.H.; Hwang, J.Y.; Ahn, K.; Kim, J.; Koh, Y.H.; Park, M.H.; Jo, S.A. Obesity and depressive symptoms in elderly Koreans: Evidence for the “Jolly Fat” hypothesis from the Ansan Geriatric (AGE) Study. Arch. Gerontol Geriatr. 2010, 51, 231–234. [Google Scholar] [CrossRef] [PubMed]
- Yu, N.W.; Chen, C.Y.; Liu, C.Y.; Chau, Y.L.; Chang, C.M. Association of body mass index and depressive symptoms in a Chinese community population: Results from the Health Promotion Knowledge, Attitudes, and Performance Survey in Taiwan. Chang Gung Med. J. 2011, 34, 620–627. [Google Scholar]
- Li, Z.B.; Ho, S.Y.; Chan, W.M.; Ho, K.S.; Li, M.P.; Leung, G.M.; Lam, T.H. Obesity and depressive symptoms in Chinese elderly. Int. J. Geriatr. Psychiatry 2004, 19, 68–74. [Google Scholar] [CrossRef] [PubMed]
- Dong, Q.; Liu, J.J.; Zheng, R.Z.; Dong, Y.H.; Feng, X.M.; Li, J.; Huang, F. Obesity and depressive symptoms in the elderly: A survey in the rural area of Chizhou, Anhui province. Int. J. Geriatr. Psychiatry. 2013, 28, 227–232. [Google Scholar] [CrossRef] [PubMed]
- Han, C.; Jo, S.A.; Seo, J.A.; Kim, B.G.; Kim, N.H.; Jo, I.; Park, M.H.; Park, K.W. Adiposity parameters and cognitive function in the elderly: Application of “Jolly Fat” hypothesis to cognition. Arch. Gerontol. Geriatr. 2009, 49, e133–e138. [Google Scholar] [CrossRef] [PubMed]
- Jasienska, G.; Ziomkiewicz, A.; Górkiewicz, M.; Pająk, A. Body mass, depressive symptoms and menopausal status: An examination of the “Jolly Fat” hypothesis. Women Health Issues 2005, 15, 145–151. [Google Scholar] [CrossRef] [PubMed]
- Palinkas, L.A.; Wingard, D.L.; Barrett-Connor, E. Depressive symptoms in overweight and obese older adults: A test of the “jolly fat” hypothesis. J. Psychosom. Res. 1996, 40, 59–66. [Google Scholar] [CrossRef]
- Nisbett, R.E.; Peng, K.; Choi, I.; Norenzayan, A. Culture and systems of thought: Holistic versus analytic cognition. Psychol. Rev. 2001, 108, 291–310. [Google Scholar] [CrossRef] [PubMed]
- Assari, S.; Lankarani, M.M. The Association Between Obesity and Weight Loss Intention Weaker Among Blacks and Men than Whites and Women. J. Racial Ethn. Health Disparities 2015, 2, 414–420. [Google Scholar] [CrossRef]
- Weinsier, R.L.; Hunter, G.R.; Gower, B.A.; Schutz, Y.; Darnell, B.E.; Zuckerman, P.A. Body fat distribution in white and black women: Different patterns of intraabdominal and subcutaneous abdominal adipose tissue utilization with weight loss. Am. J. Clin. Nutr. 2001, 74, 631–636. [Google Scholar] [CrossRef] [PubMed]
- Godino, J.G.; Lepore, S.J.; Rassnick, S. Relation of misperception of healthy weight to obesity in urban black men. Obesity 2010, 18, 1318–1322. [Google Scholar] [CrossRef] [PubMed]
- Gilliard, T.S.; Lackland, D.T.; Mountford, W.K.; Egan, B.M. Concordance between self-reported heights and weights and current and ideal body images in young adult African American men and women. Ethn. Dis. 2007, 17, 617–623. [Google Scholar] [PubMed]
- Caprio, S.; Daniels, S.R.; Drewnowski, A.; Kaufman, F.R.; Palinkas, L.A.; Rosenbloom, A.L.; Schwimmer, J.B.; Kirkman, M.S. Influence of race, ethnicity, and culture on childhood obesity: Implications for prevention and treatment. Obesity 2008, 16, 2566–2577. [Google Scholar] [CrossRef]
- Latner, J.D.; Stunkard, A.J.; Wilson, G.T. Stigmatized students: Age, sex, and ethnicity effects in the stigmatization of obesity. Obes. Res. 2005, 13, 1226–1231. [Google Scholar] [CrossRef]
- Kemper, K.A.; Sargent, R.G.; Drane, J.W.; Valois, R.F.; Hussey, J.R. Black and white females’ perceptions of ideal body size and social norms. Obes. Res. 1994, 2, 117–126. [Google Scholar] [PubMed]
- Adams, V.H., 3rd.; Jackson, J.S. The contribution of hope to the quality of life among aging African Americans: 1980–1992. Int. J. Aging Hum. Dev. 2000, 50, 279–295. [Google Scholar] [CrossRef]
- Kumanyika, S.; Wilson, J.F.; Guilford-Davenport, M. Weight-related attitudes and behaviors of black women. J. Am. Diet. Assoc. 1993, 93, 416–422. [Google Scholar] [CrossRef]
- Jackson, J.S.; Knight, K.M.; Rafferty, J.A. Race and unhealthy behaviors: Chronic stress, the HPA axis, and physical and mental health disparities over the life course. Am. J. Public Health 2010, 100, 933–939. [Google Scholar] [CrossRef]
- Mezuk, B.; Abdou, C.M.; Hudson, D.; Kershaw, K.N.; Rafferty, J.A.; Lee, H.; Jackson, J.S. “White Box” Epidemiology and the Social Neuroscience of Health Behaviors: The Environmental Affordances Model. Soc. Ment. Health 2013, 3, 79–95. [Google Scholar] [CrossRef]
- Assari, S.; Moghani Lankarani, M. Depressive Symptoms and Self-Esteem in White and Black Older Adults in the United States. Brain Sci. 2018, 8, 105. [Google Scholar] [CrossRef] [PubMed]
- Brody, G.H.; Yu, T.; Chen, Y.F.; Kogan, S.M.; Evans, G.W.; Beach, S.R.; Windle, M.; Simons, R.L.; Gerrard, M.; Gibbons, F.X.; et al. Cumulative socioeconomic status risk, allostatic load, and adjustment: A prospective latent profile analysis with contextual and genetic protective factors. Dev. Psychol. 2013, 49, 913–927. [Google Scholar] [CrossRef] [PubMed]
- Kirby, J.B.; Kaneda, T. “Double jeopardy” measure suggests blacks and hispanics face more severe disparities than previously indicated. Health Aff. 2013, 32, 1766–1772. [Google Scholar] [CrossRef]
- Gibbons, F.X.; O’Hara, R.E.; Stock, M.L.; Gerrard, M.; Weng, C.Y.; Wills, T.A. The erosive effects of racism: Reduced self-control mediates the relation between perceived racial discrimination and substance use in African American adolescents. J. Pers. Soc. Psychol. 2012, 102, 1089–1104. [Google Scholar] [CrossRef]
- Chae, D.H.; Lincoln, K.D.; Jackson, J.S. Discrimination, attribution, and racial group identification: Implications for psychological distress among Black Americans in the National Survey of American Life (2001–2003). Am. J. Orthopsychiatry 2011, 81, 498–506. [Google Scholar] [CrossRef]
- Williams, D.R. Race, socioeconomic status, and health. The added effects of racism and discrimination. Ann. N. Y. Acad. Sci. 1999, 896, 173–188. [Google Scholar] [CrossRef] [PubMed]
- Zemore, S.E.; Karriker-Jaffe, K.J.; Keithly, S.; Mulia, N. Racial prejudice and unfair treatment: Interactive effects with poverty and foreign nativity on problem drinking. J. Stud. Alcohol. Drugs 2011, 72, 361–370. [Google Scholar] [CrossRef] [PubMed]
- Pais, J. Cumulative structural disadvantage and racial health disparities: The pathways of childhood socioeconomic influence. Demography 2014, 51, 1729–1753. [Google Scholar] [CrossRef] [PubMed]
- Umberson, D.; Williams, K.; Thomas, P.A.; Liu, H.; Thomeer, M.B. Race, gender, and chains of disadvantage: Childhood adversity, social relationships, and health. J. Health Soc. Behav. 2014, 55, 20–38. [Google Scholar] [CrossRef] [PubMed]
- Assari, S.; Farokhnia, M.; Mistry, R. Education Attainment and Alcohol Binge Drinking: Diminished Returns of Hispanics in Los Angeles. Behav. Sci. 2019, 9, 9. [Google Scholar] [CrossRef] [PubMed]
- Assari, S. Health Disparities due to Diminished Return among Black Americans: Public Policy Solutions. Soc. Issues Policy Rev. 2018, 12, 112–145. [Google Scholar] [CrossRef]
- Brown, C.S.; Baker, T.A.; Mingo, C.A.; Harden, J.T.; Whitfield, K.; Aiken-Morgan, A.T.; Phillips, K.L.; Washington, T. A review of our roots: Blacks in gerontology. Gerontologist 2014, 54, 108–116. [Google Scholar] [CrossRef]
- Jackson, J. Racial and Ethnic Minority Group Dispari-Ties and the Affordances Model; The Gerontological Society of America: Boston, MA, USA, 2011. [Google Scholar]
- Assari, S. Race and Ethnicity, Religion Involvement, Church-based Social Support and Subjective Health in United States: A Case of Moderated Mediation. Int. J. Prev. Med. 2013, 4, 208–217. [Google Scholar]
- Lincoln, K.D.; Chatters, L.M.; Taylor, R.J. Psychologi cal distress among Black and White Americans: Differential effects of social support, negative interaction and personal control. J. Health Soc. Behav. 2003, 44, 390–407. [Google Scholar] [CrossRef]
- Krause, N. Church-based social support and health in old age: Exploring variations by race. J. Gerontol. 2002, 57, S332–S347. [Google Scholar] [CrossRef]
- K Keyes, C.L. Promoting and protecting mental health as flourishing: A complementary strategy for improving national mental health. Am. Psychol. 2007, 62, 95–108. [Google Scholar] [CrossRef] [PubMed]
- Henderson, D.X.; Bond, G.D.; Alderson, C.J.; Walker, W.R. This Too Shall Pass: Evidence of Coping and Fading Emotion in African Americans’ Memories of Violent and Nonviolent Death. Omega 2015, 71, 291–311. [Google Scholar] [CrossRef] [PubMed]
- Sandu, R.E.; Buga, A.M.; Uzoni, A.; Petcu, E.B.; Popa-Wagner, A. Neuroinflammation and comorbidities are frequently ignored factors in CNS pathology. Neural Regen. Res. 2015, 10, 1349–1355. [Google Scholar] [CrossRef] [PubMed]
- Slevin, M.; Matou, S.; Zeinolabediny, Y.; Corpas, R.; Weston, R.; Liu, D.; Boras, E.; Di Napoli, M.; Petcu, E.; Sarroca, S.; et al. Monomeric C-reactive protein—A key molecule driving development of Alzheimer’s disease associated with brain ischaemia? Sci. Rep. 2015, 5, 13281. [Google Scholar] [CrossRef] [PubMed]
- Popa-Wagner, A.; Buga, A.M.; Tica, A.A.; Albu, C.V. Perfusion deficits, inflammation and aging precipitate depressive behaviour. Biogerontology 2014, 15, 439–448. [Google Scholar] [CrossRef]
- Kiecolt-Glaser, J.K.; Derry, H.M.; Fagundes, C.P. Inflammation: Depression fans the flames and feasts on the heat. Am. J. Psychiatry 2015, 172, 1075–1091. [Google Scholar] [CrossRef] [PubMed]
- Rethorst, C.D.; Bernstein, I.; Trivedi, M.H. Inflammation, obesity, and metabolic syndrome in depression: Analysis of the 2009-2010 National Health and Nutrition Examination Survey (NHANES). J. Clin. Psychiatry 2014, 75, e1428–e1432. [Google Scholar] [CrossRef]
- Berk, M.; Williams, L.J.; Jacka, F.N.; O’Neil, A.; Pasco, J.A.; Moylan, S.; Allen, N.B.; Stuart, A.L.; Hayley, A.C.; Byrne, M.L.; Maes, M. So depression is an inflammatory disease, but where does the inflammation come from? BMC Med. 2013, 11, 200. [Google Scholar] [CrossRef]
- Becker, K.J. Inflammation and the Silent Sequelae of Stroke. Neurotherapeutics 2016, 13, 801–810. [Google Scholar] [CrossRef]
- Moazen-Zadeh, E.; Assari, S. Depressive Symptoms Predict Major Depressive Disorder after 15 Years among Whites but Not Blacks. Front. Public Health 2016, 4, 13. [Google Scholar] [CrossRef]
- Assari, S. Bidirectional associations between chronic medical conditions, disability, and depressive symptoms over 25 years: Black-White differences. Int. J. Epidemiol. Res. 2016, 3, 302–317. [Google Scholar]
- Assari, S.; Caldwell, C.H.; Zimmerman, M.A. Low parental support in late adolescence predicts obesity in young adulthood; Gender differences in a 12-year cohort of African Americans. J. Diabetes Metab. Disord. 2015, 14, 47. [Google Scholar] [CrossRef] [PubMed]
- Krishna, A.; Razak, F.; Lebel, A.; Smith, G.D.; Subramanian, S.V. Trends in group inequalities and interindividual inequalities in BMI in the United States, 1993–2012. Am. J. Clin. Nutr. 2015, 101, 598–605. [Google Scholar] [CrossRef] [PubMed]
- Leon, B.; Miller, B.V., 3rd.; Zalos, G.; Courville, A.B.; Sumner, A.E.; Powell-Wiley, T.M.; Walter, M.F.; Waclawiw, M.A.; Cannon, R.O. Weight Loss Programs May Have Beneficial or Adverse Effects on Fat Mass and Insulin Sensitivity in Overweight and Obese Black Women. J. Racial Ethn. Health Disparities 2014, 1, 140–147. [Google Scholar] [CrossRef] [PubMed]
- Capers, C.F.; Baughman, K.; Logue, E. Behaviors and characteristics of African American and European American females that impact weight management. J. Nurs. Scholarsh. 2011, 43, 133–144. [Google Scholar] [CrossRef]

| All | Whites | Blacks | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Gender * | n | % | n | % | n | % | |||
| Male | 6431 | 42.33 | 5614 | 43.20 | 817 | 37.14 | |||
| Female | 8763 | 57.67 | 7380 | 56.80 | 1383 | 62.86 | |||
| Veterans * | |||||||||
| No | 4348 | 68.33 | 3775 | 67.09 | 573 | 77.85 | |||
| Yes | 2015 | 31.67 | 1852 | 32.91 | 163 | 22.15 | |||
| Married * | |||||||||
| No | 1555 | 20.05 | 1086 | 16.50 | 469 | 40.05 | |||
| Yes | 6199 | 79.95 | 5497 | 83.50 | 702 | 59.95 | |||
| n | Mean | SD | n | Mean | SD | n | Mean | SD | |
| Age (Years) | 7754 | 55.01 | 4.94 | 6583 | 55.01 | 4.97 | 1171 | 55.00 | 4.75 |
| ADL (Count) * | 9728 | 0.09 | 0.43 | 8338 | 0.08 | 0.40 | 1390 | 0.16 | 0.58 |
| CES-D (Count)1 * | 9271 | 1.19 | 1.85 | 7952 | 1.11 | 1.79 | 1319 | 1.69 | 2.11 |
| BMI (kg/m2) 1 * | 7754 | 27.14 | 5.04 | 6583 | 26.81 | 4.78 | 1171 | 29.01 | 6.00 |
| Average CES-D (Count) During 24 Years * | 11,684 | 1.25 | 1.39 | 10,381 | 1.20 | 1.35 | 1303 | 1.67 | 1.57 |
| Average BMI (kg/m2) During 24 Years* | 12,226 | 27.41 | 4.99 | 10,825 | 27.22 | 4.88 | 1401 | 28.85 | 5.61 |
| Characteristics | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 |
|---|---|---|---|---|---|---|---|---|---|---|
| All | ||||||||||
| (1) Race | 1 | 0.043 ** | −0.001 | −0.074 ** | −0.211 ** | 0.063 ** | 0.109 ** | 0.156 ** | 0.107 ** | 0.104 ** |
| (2) Gender | 1 | −0.250 ** | 0.616 ** | −0.136 ** | 0.049 ** | 0.132 ** | −0.026 * | −0.094 ** | 0.012 | |
| (3) Age | 1 | −0.119 ** | −0.025 * | 0.003 | −0.047 ** | −0.005 | 0.019 | −0.055 ** | ||
| (4) Veterans | 1 | 0.026 * | −0.005 | 0.014 | −0.064 ** | −0.118 ** | −0.003 | |||
| (5) Marital Status | 1 | −0.075 ** | −0.156 ** | −0.035 ** | −0.063 ** | 0.002 | ||||
| (6) ADL (count) | 1 | 0.296 ** | 0.128 ** | 0.095 ** | 0.012 | |||||
| (7) CES-D 1 (count) | 1 | 0.100 ** | 0.216 ** | 0.029 * | ||||||
| (8) BMI 1 (kg/m2) | 1 | 0.062 ** | 0.131 ** | |||||||
| (9) Average CES-D During 24 Years | 1 | 0.093 ** | ||||||||
| (10) Average BMI During 24 Years (kg/m2) | 1 | |||||||||
| Whites | ||||||||||
| (2) Gender | 1 | −0.256 ** | 0.639 ** | −0.114 ** | 0.033 ** | 0.125 ** | −0.078 ** | −0.096 ** | 0.052 ** | |
| (3) Age | 1 | −0.130 ** | −0.022 | 0.003 | −0.051 ** | 0.010 | 0.017 | −0.077 ** | ||
| (4) Veterans | 1 | 0.012 | −0.006 | 0.027 | −0.069 ** | −0.105 ** | 0.026* | |||
| (5) Marital Status | 1 | −0.052 ** | −0.140 ** | −0.001 | −0.047 ** | 0.000 | ||||
| (6) ADL (count) | 1 | 0.274 ** | 0.109 ** | 0.087 ** | 0.015 | |||||
| (7) CES-D 1 (count) | 1 | 0.086 ** | 0.204 ** | 0.026 * | ||||||
| (8) BMI 1 (kg/m2) | 1 | 0.059 ** | 0.151 ** | |||||||
| (9) Average CES-D During 24 Years | 1 | 0.090 ** | ||||||||
| (10) Average BMI During 24 Years (kg/m2) | 1 | |||||||||
| Blacks | ||||||||||
| (2) Gender | 1 | −0.216 ** | 0.451 ** | −0.192 ** | 0.106 ** | 0.140 ** | 0.163 ** | −0.082 ** | −0.260 ** | |
| (3) Age | 1 | −0.051 | −0.048 | −0.001 | −0.033 | −0.074 * | 0.041 | 0.087 * | ||
| (4) Veterans | 1 | 0.081 * | 0.023 | −0.030 | 0.040 | −0.163 ** | −0.154 ** | |||
| (5) Marital Status | 1 | −0.100 ** | −0.124 ** | -0.003 | −0.079 * | 0.057 | ||||
| (6) ADL (count) | 1 | 0.357 ** | 0.159 ** | 0.110 ** | −0.025 | |||||
| (7) CES-D 1 (count) | 1 | 0.073 * | 0.233 ** | −0.013 | ||||||
| (8) BMI 1 (kg/m2) | 1 | −0.023 | −0.039 | |||||||
| (9) Average CES-D During 24 Years | 1 | 0.034 | ||||||||
| (10) Average BMI During 24 Years (kg/m2) | 1 |
| Pooled Sample | Whites | Blacks | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
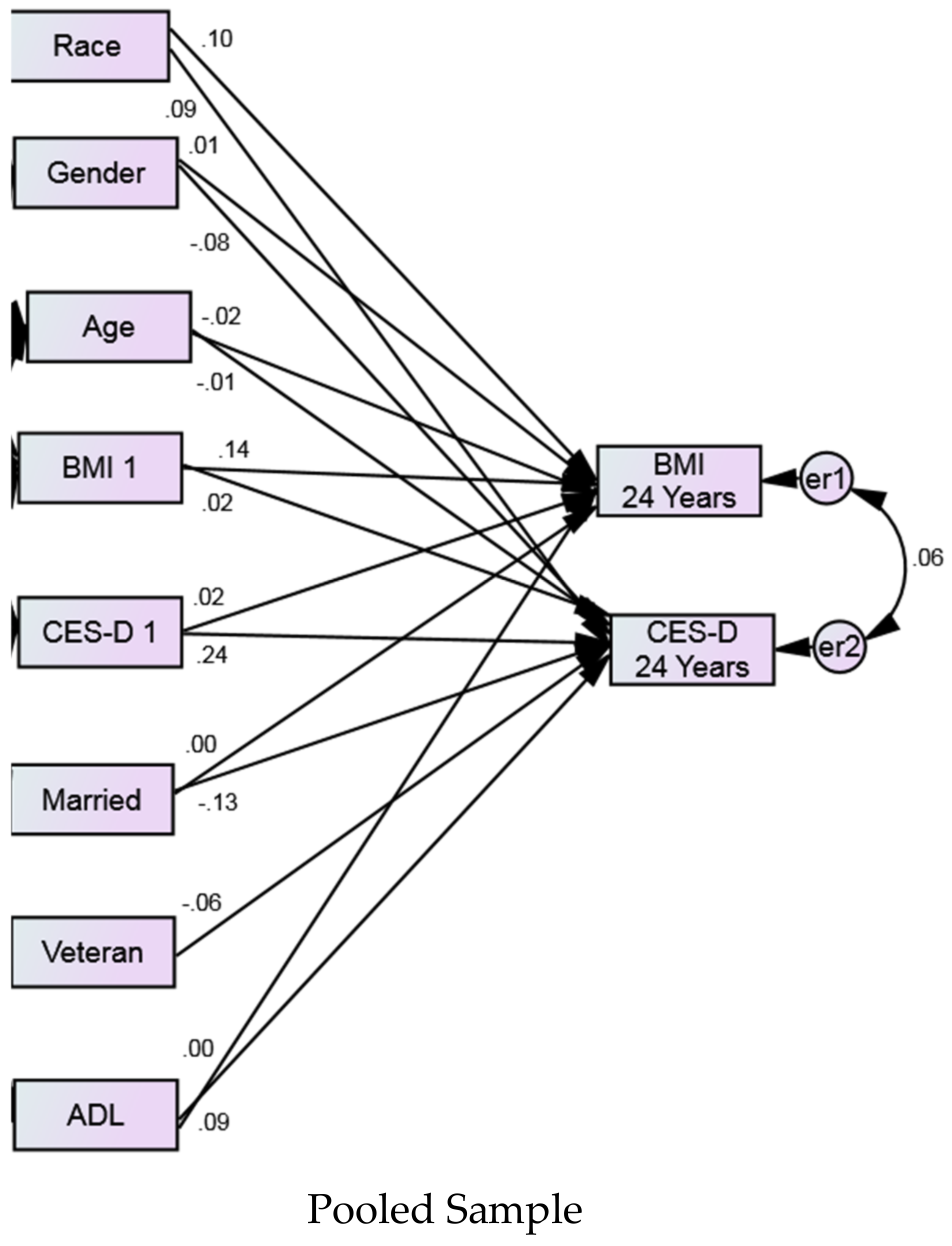
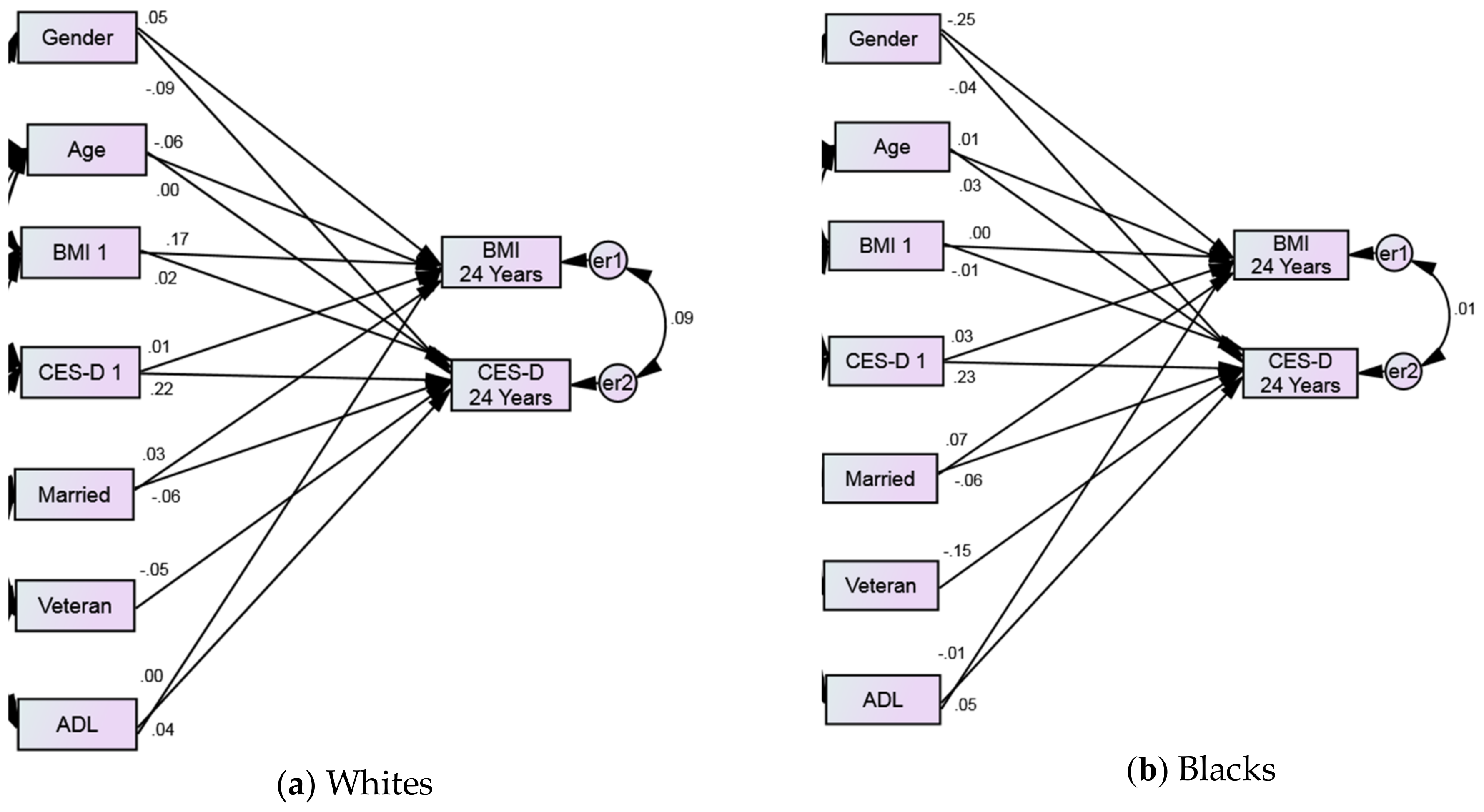
| Cross Lagged Paths | B | SE | p | B | SE | p | B | SE | p | ||
| BMI 1 | → | CES-D 24 Years | 0.02 | 0.00 | 0.017 | 0.03 | 0.00 | 0.050 | −0.01 | 0.01 | 0.809 |
| CES-D 1 | → | BMI 24 Years | 0.02 | 0.03 | 0.055 | 0.01 | 0.04 | 0.459 | 0.03 | 0.10 | 0.391 |
| Autoregressive Paths | |||||||||||
| BMI 1 | → | BMI 24 Years | 0.14 | 0.01 | <0.001 | 0.17 | 0.01 | <0.001 | 0.00 | 0.03 | 0.906 |
| CES-D 1 | → | CES-D 24 Years | 0.24 | 0.01 | <0.001 | 0.22 | 0.01 | <0.001 | 0.23 | 0.03 | <0.001 |
| Covariates on BMI | |||||||||||
| Race (Blacks) | → | BMI 24 Years | 0.10 | 0.14 | <0.001 | - | - | - | - | - | - |
| Gender (Women) | → | BMI 24 Years | 0.01 | 0.10 | 0.236 | 0.05 | 0.10 | <0.001 | −0.25 | 0.33 | <0.001 |
| Age | → | BMI 24 Years | −0.02 | 0.01 | 0.132 | −0.06 | 0.01 | <0.001 | 0.01 | 0.04 | 0.686 |
| Marital Status (Married) | → | BMI 24 Years | 0.00 | 0.16 | 0.741 | 0.03 | 0.17 | 0.034 | 0.08 | 0.40 | 0.033 |
| ADL 1 | → | BMI 24 Years | 0.00 | 0.07 | 1.000 | 0.04 | 0.04 | 0.002 | 0.05 | 0.10 | 0.158 |
| Covariates on CES-D | |||||||||||
| Race (Blacks) | → | CES-D 24 Years | 0.09 | 0.04 | <0.001 | - | - | - | - | - | - |
| Gender (Women) | → | CES-D 24 Years | −0.08 | 0.04 | <0.001 | −0.09 | 0.04 | <0.001 | −0.04 | 0.12 | 0.317 |
| Age | → | CES-D 24 Years | −0.01 | 0.00 | 0.372 | 0.00 | 0.00 | 0.945 | 0.03 | 0.01 | 0.487 |
| Marital Status (Married) | → | CES-D 24 Years | −0.13 | 0.05 | <0.001 | −0.06 | 0.05 | <0.001 | −0.06 | 0.12 | 0.089 |
| Veteran | → | CES-D 24 Years | −0.06 | 0.05 | <0.001 | −0.05 | 0.05 | 0.002 | −0.15 | 0.16 | <0.001 |
| ADL 1 | → | CES-D 24 Years | 0.09 | 0.02 | <0.001 | 0.00 | 0.15 | 0.831 | −0.01 | 0.34 | 0.743 |
© 2019 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Assari, S. Baseline Body Mass Predicts Average Depressive Symptoms over the Next Two Decades for White but Not Black Older Adults. Geriatrics 2019, 4, 14. https://doi.org/10.3390/geriatrics4010014
Assari S. Baseline Body Mass Predicts Average Depressive Symptoms over the Next Two Decades for White but Not Black Older Adults. Geriatrics. 2019; 4(1):14. https://doi.org/10.3390/geriatrics4010014
Chicago/Turabian StyleAssari, Shervin. 2019. "Baseline Body Mass Predicts Average Depressive Symptoms over the Next Two Decades for White but Not Black Older Adults" Geriatrics 4, no. 1: 14. https://doi.org/10.3390/geriatrics4010014
APA StyleAssari, S. (2019). Baseline Body Mass Predicts Average Depressive Symptoms over the Next Two Decades for White but Not Black Older Adults. Geriatrics, 4(1), 14. https://doi.org/10.3390/geriatrics4010014





