Eosinophilic Myocarditis: From Bench to Bedside
Abstract
1. Introduction
2. Epidemiology
3. Etiology
4. Pathophysiology
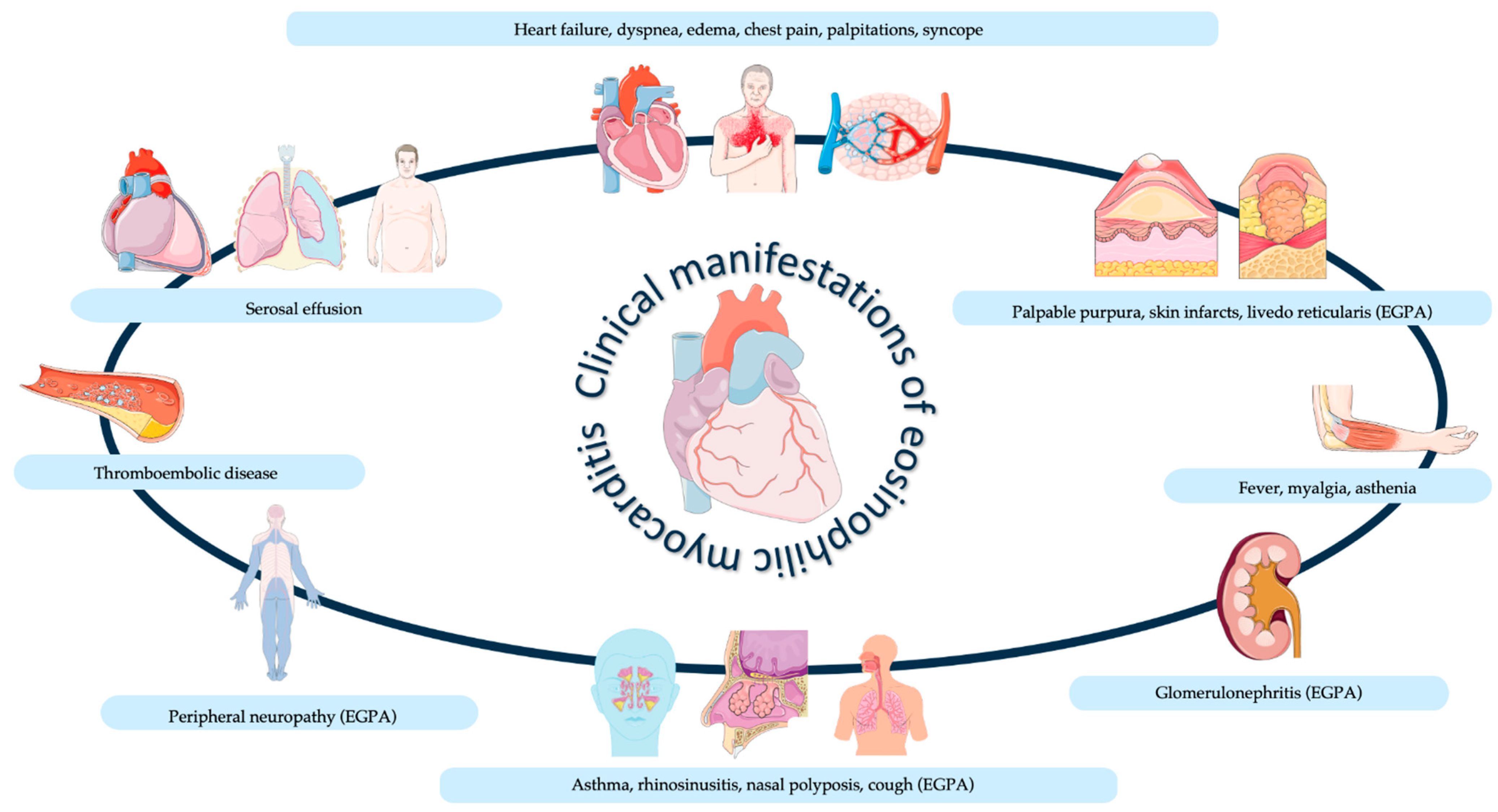
5. Clinical Manifestations
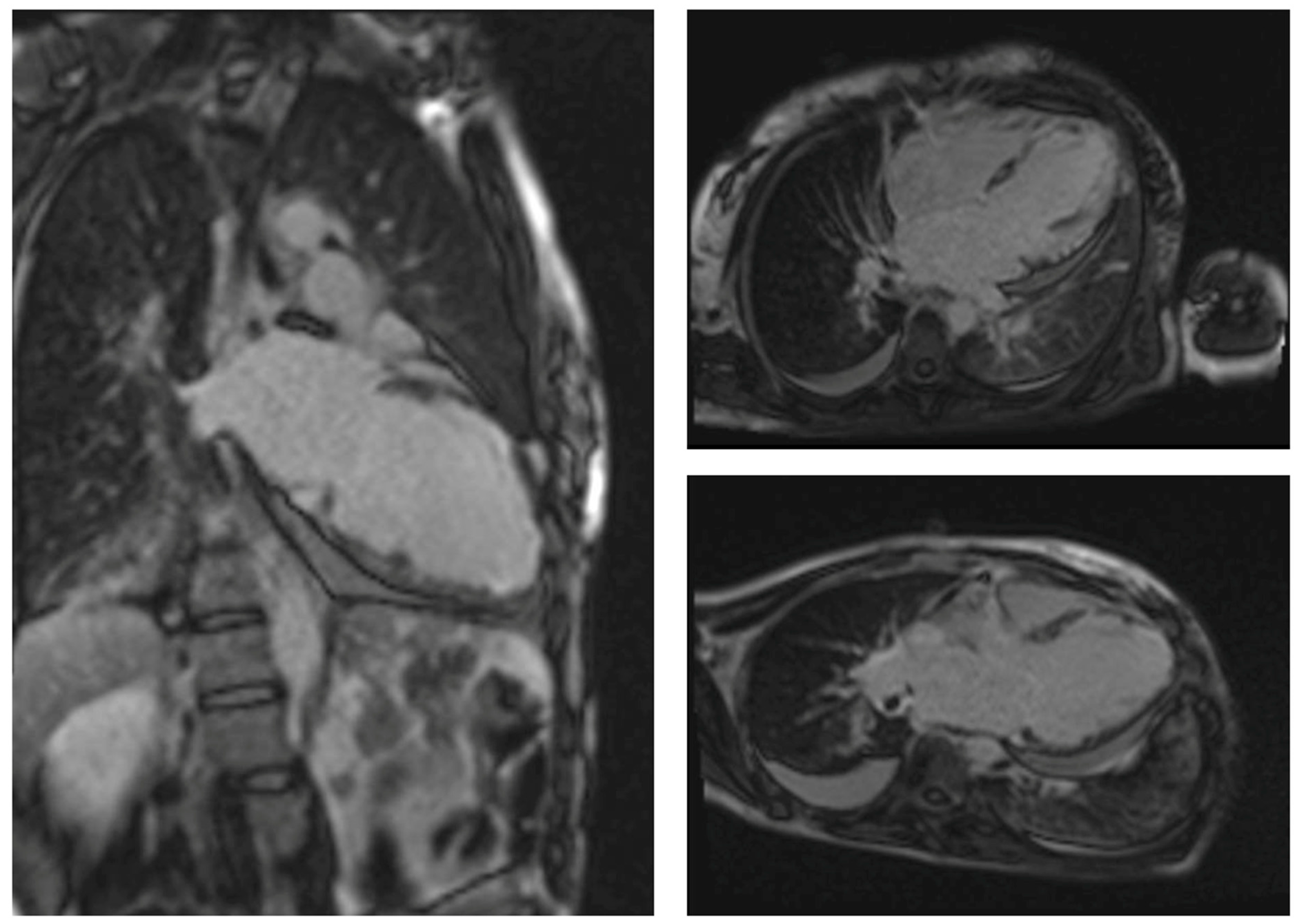
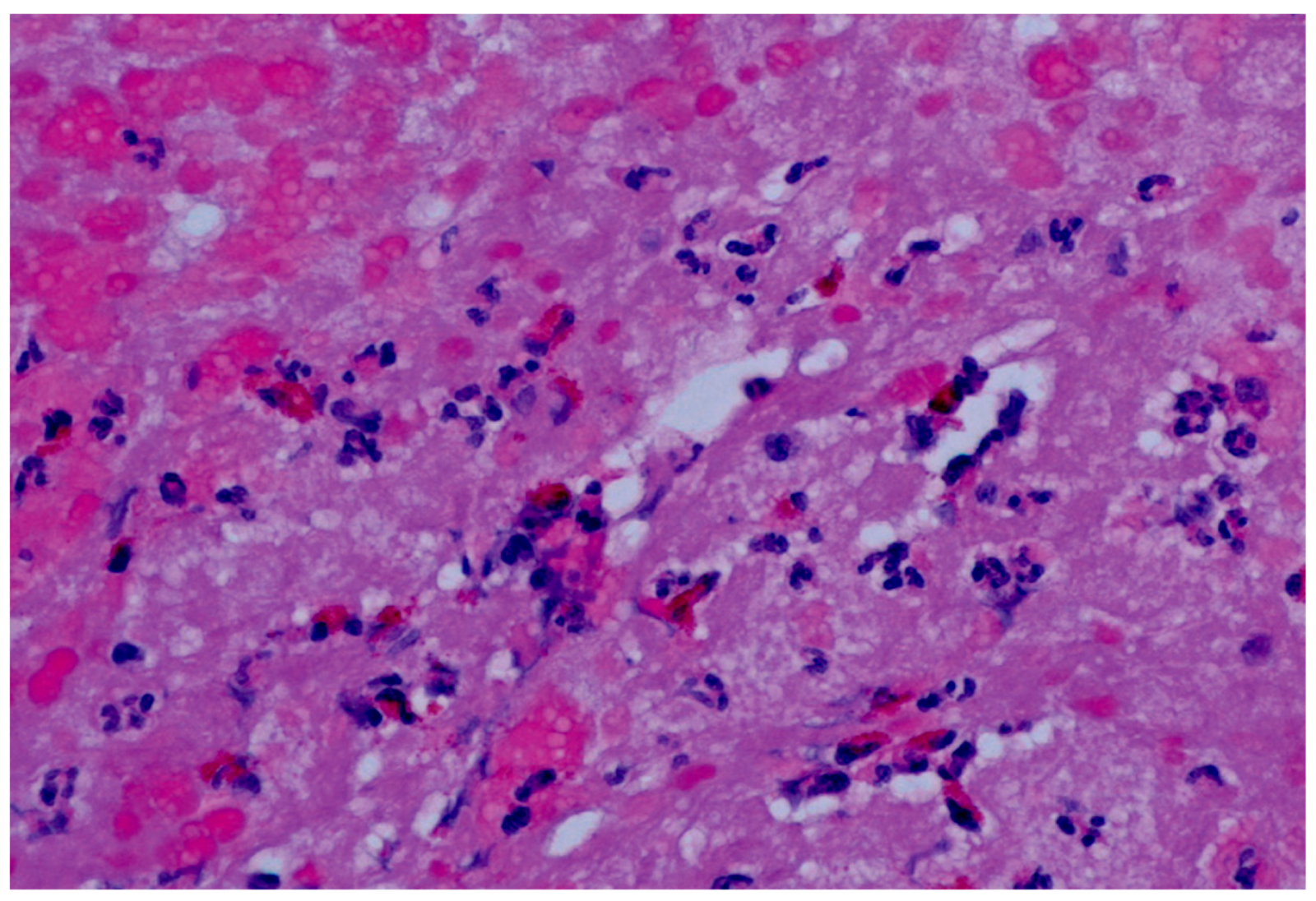
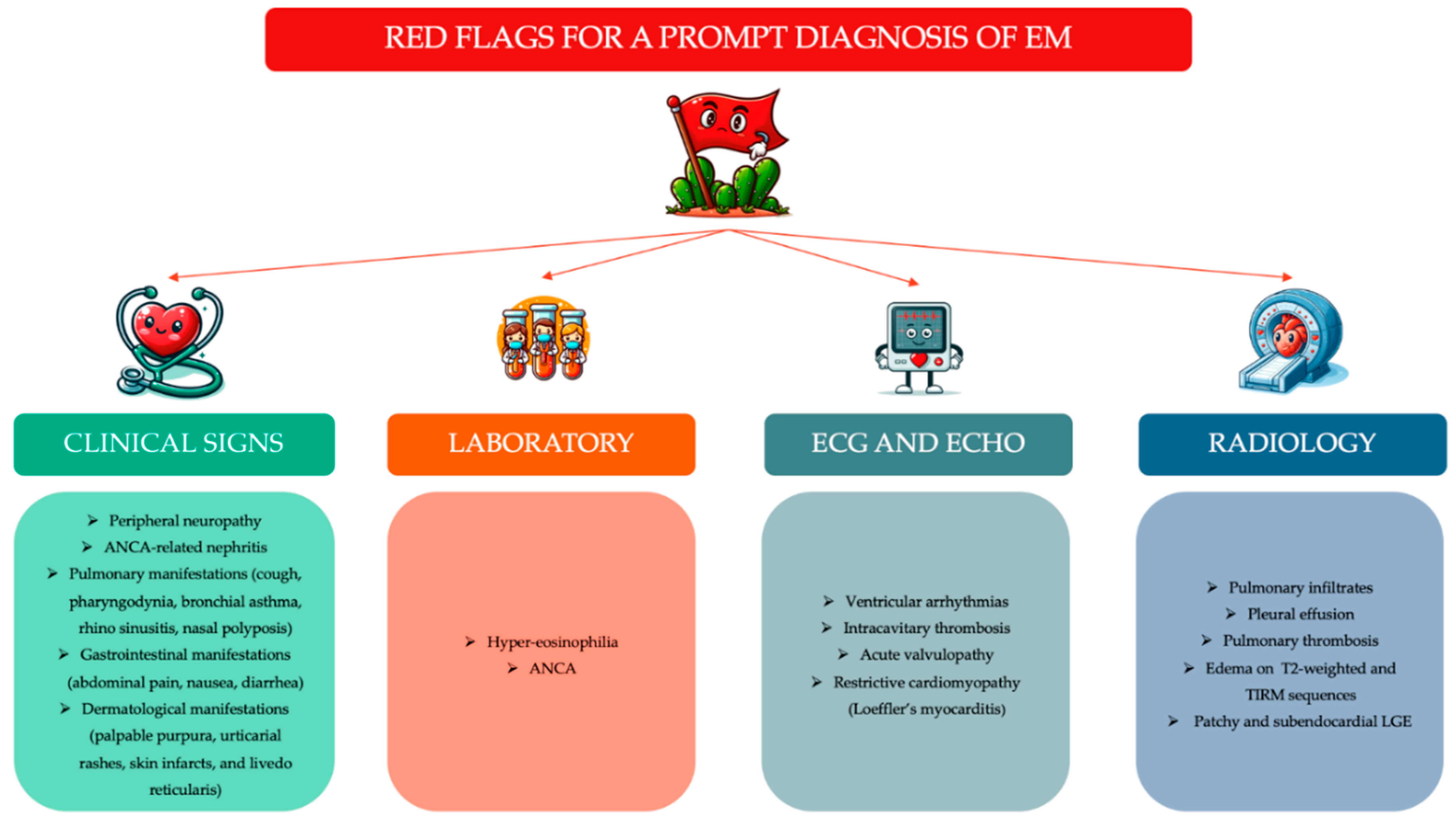
6. Diagnosis
7. Therapy
8. Prognosis
9. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
References
- Piccirillo, F.; Watanabe, M.; Di Sciascio, G. Diagnosis, Treatment and Predictors of Prognosis of Myocarditis. A Narrative Review. Cardiovasc. Pathol. 2021, 54, 107362. [Google Scholar] [CrossRef]
- Watanabe, M.; Panetta, G.L.; Piccirillo, F.; Spoto, S.; Myers, J.; Serino, F.M.; Costantino, S.; Di Sciascio, G. Acute Epstein-Barr Related Myocarditis: An Unusual but Life-Threatening Disease in an Immunocompetent Patient. J. Cardiol. Cases 2020, 21, 137–140. [Google Scholar] [CrossRef]
- Brambatti, M.; Matassini, M.V.; Adler, E.D.; Klingel, K.; Camici, P.G.; Ammirati, E. Eosinophilic Myocarditis. J. Am. Coll. Cardiol. 2017, 70, 2363–2375. [Google Scholar] [CrossRef]
- Caforio, A.L.P.; Pankuweit, S.; Arbustini, E.; Basso, C.; Gimeno-Blanes, J.; Felix, S.B.; Fu, M.; Heliö, T.; Heymans, S.; Jahns, R.; et al. Current State of Knowledge on Aetiology, Diagnosis, Management, and Therapy of Myocarditis: A Position Statement of the European Society of Cardiology Working Group on Myocardial and Pericardial Diseases. Eur. Heart J. 2013, 34, 2636–2648, 2648a–2648d. [Google Scholar] [CrossRef] [PubMed]
- Ginsberg, F.; Parrillo, J.E. Eosinophilic Myocarditis. Heart Fail. Clin. 2005, 1, 419–429. [Google Scholar] [CrossRef] [PubMed]
- Al Ali, A.M.; Straatman, L.P.; Allard, M.F.; Ignaszewski, A.P. Eosinophilic Myocarditis: Case Series and Review of Literature. Can. J. Cardiol. 2006, 22, 1233–1237. [Google Scholar] [CrossRef] [PubMed]
- Takkenberg, J.J.M.; Czer, L.S.C.; Fishbein, M.C.; Luthringer, D.J.; Quartel, A.W.; Mirocha, J.; Queral, C.A.; Blanche, C.; Trento, A. Eosinophilic Myocarditis in Patients Awaiting Heart Transplantation. Crit. Care Med. 2004, 32, 714–721. [Google Scholar] [CrossRef] [PubMed]
- de Alava, E.; Panizo-Santos, A.; Fernández-González, A.L.; Pardo-Mindán, F.J. Eosinophilic Myocarditis in Patients Waiting for Heart Transplantation. Cardiovasc. Pathol. 1995, 4, 43–46. [Google Scholar] [CrossRef] [PubMed]
- Baandrup, U. Eosinophilic Myocarditis. Herz 2012, 37, 849–853. [Google Scholar] [CrossRef]
- Piccirillo, F.; Nusca, A.; Di Sciascio, G. Incidence, Diagnosis, and Prognosis of Myocarditis: Does Gender Matter? Pol. Arch. Intern. Med. 2022, 132, 16246. [Google Scholar] [CrossRef]
- Gotlib, J. World Health Organization-defined Eosinophilic Disorders: 2015 Update on Diagnosis, Risk Stratification, and Management. Am. J. Hematol. 2015, 90, 1077–1089. [Google Scholar] [CrossRef] [PubMed]
- Barin, J.G.; Baldeviano, G.C.; Talor, M.V.; Wu, L.; Ong, S.; Fairweather, D.; Bedja, D.; Stickel, N.R.; Fontes, J.A.; Cardamone, A.B.; et al. Fatal Eosinophilic Myocarditis Develops in the Absence of IFN-γ and IL-17A. J. Immunol. 2013, 191, 4038–4047. [Google Scholar] [CrossRef] [PubMed]
- Yoshida, T.; Fukuda, T.; Hatano, M.; Koseki, H.; Okabe, S.; Ishibashi, K.; Kojima, S.; Arima, M.; Komuro, I.; Ishii, G.; et al. The Role of Bcl6 in Mature Cardiac Myocytes. Cardiovasc. Res. 1999, 42, 670–679. [Google Scholar] [CrossRef] [PubMed]
- Vaglio, A.; Martorana, D.; Maggiore, U.; Grasselli, C.; Zanetti, A.; Pesci, A.; Garini, G.; Manganelli, P.; Bottero, P.; Tumiati, B.; et al. HLA-DRB4 as a Genetic Risk Factor for Churg-Strauss Syndrome. Arthritis Rheum. 2007, 56, 3159–3166. [Google Scholar] [CrossRef]
- Wieczorek, S.; Hellmich, B.; Gross, W.L.; Epplen, J.T. Associations of Churg-Strauss Syndrome with the HLA-DRB1 Locus, and Relationship to the Genetics of Antineutrophil Cytoplasmic Antibody-Associated Vasculitides: Comment on the Article by Vaglio et al. Arthritis Rheum. 2008, 58, 329–330. [Google Scholar] [CrossRef]
- Zhong, Z.; Yang, Z.; Peng, Y.; Wang, L.; Yuan, X. Diagnosis and Treatment of Eosinophilic Myocarditis. J. Transl. Autoimmun. 2021, 4, 100118. [Google Scholar] [CrossRef]
- Russo, M.; Ismibayli, Z.; Antonaci, S.; Piccinni, G.C. Eosinophilic Myocarditis: From Etiology to Diagnostics and Therapy. Minerva Cardiol. Angiol. 2023. online ahead of print. [Google Scholar] [CrossRef]
- Sheikh, H.; Siddiqui, M.; Uddin, S.M.M.; Haq, A.; Yaqoob, U. The Clinicopathological Profile of Eosinophilic Myocarditis. Cureus 2018, 10, e3677. [Google Scholar] [CrossRef]
- Kuchynka, P.; Palecek, T.; Masek, M.; Cerny, V.; Lambert, L.; Vitkova, I.; Linhart, A. Current Diagnostic and Therapeutic Aspects of Eosinophilic Myocarditis. BioMed Res. Int. 2016, 2016, 2829583. [Google Scholar] [CrossRef]
- Lee, C.C.; Luthringer, D.J.; Czer, L.S.C. Dobutamine-Induced Fever and Isolated Eosinophilic Myocarditis in a 66-Year-Old Male Awaiting Heart Transplantation: A Case Report. Transplant. Proc. 2014, 46, 2464–2466. [Google Scholar] [CrossRef] [PubMed]
- Raje, V.P.; Lewis, N.P.; Katlaps, G.J.; Quader, M.A.; Shah, K.B.; Mankad, A.K. Dobutamine Induced Eosinophilic Myocarditis and Right Heart Failure Requiring Emergent Biventricular Assist Device Implantation. ASAIO J. 2015, 61, 213–215. [Google Scholar] [CrossRef]
- Yoshizawa, S.; Sugiyama Kato, T.; Mancini, D.; Marboe, C.C. Characteristics of Patients with Advanced Heart Failure Having Eosinophilic Infiltration of the Myocardium in the Recent Era. Int. Heart J. 2013, 54, 146–148. [Google Scholar] [CrossRef]
- Takeda, M.; Ishio, N.; Shoji, T.; Mori, N.; Matsumoto, M.; Shikama, N. Eosinophilic Myocarditis Following Coronavirus Disease 2019 (COVID-19) Vaccination. Circ. J. 2022, 86, 1020. [Google Scholar] [CrossRef]
- Kimura, M.; Hashimoto, T.; Noda, E.; Ishikawa, Y.; Ishikita, A.; Fujino, T.; Matsushima, S.; Ide, T.; Kinugawa, S.; Nagaoka, K.; et al. Fulminant Necrotizing Eosinophilic Myocarditis after COVID-19 Vaccination Survived with Mechanical Circulatory Support. ESC Heart Fail. 2022, 9, 2732–2737. [Google Scholar] [CrossRef]
- Ohtani, K.; Takahama, S.; Kato, S.; Higo, T. Acute Necrotizing Eosinophilic Myocarditis after COVID-19 Vaccination. Eur. Heart J. 2022, 43, 2640. [Google Scholar] [CrossRef] [PubMed]
- Barton, M.; Finkelstein, Y.; Opavsky, M.A.; Ito, S.; Ho, T.; Ford-Jones, L.E.; Taylor, G.; Benson, L.; Gold, R. Eosinophilic Myocarditis Temporally Associated with Conjugate Meningococcal C and Hepatitis B Vaccines in Children. Pediatr. Infect. Dis. J. 2008, 27, 831–835. [Google Scholar] [CrossRef] [PubMed]
- Emmi, G.; Bettiol, A.; Gelain, E.; Bajema, I.M.; Berti, A.; Burns, S.; Cid, M.C.; Cohen Tervaert, J.W.; Cottin, V.; Durante, E.; et al. Evidence-Based Guideline for the Diagnosis and Management of Eosinophilic Granulomatosis with Polyangiitis. Nat. Rev. Rheumatol. 2023, 19, 378–393. [Google Scholar] [CrossRef] [PubMed]
- White, J.; Dubey, S. Eosinophilic Granulomatosis with Polyangiitis: A Review. Autoimmun. Rev. 2023, 22, 103219. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Vives, E.; Rodriguez-Palomares, J.F.; Harty, L.; Solans-Laque, R.; Jayne, D. Heart Disease in Eosinophilic Granulomatosis with Polyangiitis (EGPA) Patients: A Screening Approach Proposal. Rheumatology 2021, 60, 4538–4547. [Google Scholar] [CrossRef]
- Comarmond, C.; Pagnoux, C.; Khellaf, M.; Cordier, J.-F.; Hamidou, M.; Viallard, J.-F.; Maurier, F.; Jouneau, S.; Bienvenu, B.; Puéchal, X.; et al. Eosinophilic Granulomatosis with Polyangiitis (Churg-Strauss): Clinical Characteristics and Long-Term Followup of the 383 Patients Enrolled in the French Vasculitis Study Group Cohort. Arthritis Rheum. 2013, 65, 270–281. [Google Scholar] [CrossRef] [PubMed]
- Smedema, J.P.; Winckels, S.K.G.; Snoep, G.; Vainer, J.; Bekkers, S.C.A.M.; Crijns, H.J.G.M. Tropical Endomyocardial Fibrosis (Davies’ Disease): Case Report Demonstrating the Role of Magnetic Resonance Imaging. Int. J. Cardiovasc. Imaging 2004, 20, 517–522. [Google Scholar] [CrossRef]
- Bukhman, G.; Ziegler, J.; Parry, E. Endomyocardial Fibrosis: Still a Mystery after 60 Years. PLoS Negl. Trop. Dis. 2008, 2, e97. [Google Scholar] [CrossRef]
- Cottin, V. Eosinophilic Lung Diseases. Immunol. Allergy Clin. N. Am. 2023, 43, 289–322. [Google Scholar] [CrossRef] [PubMed]
- Shibazaki, S.; Eguchi, S.; Endo, T.; Wakabayashi, T.; Araki, M.; Gu, Y.; Imai, T.; Asano, K.; Taniuchi, N. Eosinophilic Myocarditis Due to Toxocariasis: Not a Rare Cause. Case Rep. Cardiol. 2016, 2016, 2586292. [Google Scholar] [CrossRef] [PubMed]
- Craver, R.; Huber, S.; Sandomirsky, M.; McKenna, D.; Schieffelin, J.; Finger, L. Fatal Eosinophilic Myocarditis in a Healthy 17-Year-Old Male with Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2c). Fetal Pediatr. Pathol. 2020, 39, 263–268. [Google Scholar] [CrossRef] [PubMed]
- Thawabi, M.; Habib, M.; Shaaban, H.; Shamoon, F. Acute Eosinophilic Myocarditis and Hyper IgE in HIV Infection: A Case Report. N. Am. J. Med. Sci. 2014, 6, 338–341. [Google Scholar] [CrossRef] [PubMed]
- Cohen, A.J.; Steigbigel, R.T. Eosinophilia in Patients Infected with Human Immunodeficiency Virus. J. Infect. Dis. 1996, 174, 615–618. [Google Scholar] [CrossRef] [PubMed]
- Paganelli, R.; Scala, E.; Mazzone, A.M.; Rosso, R.; Mattiacci, G.; Dell’Anna, L.; Mezzaroma, I.; Aiuti, F. Th2-Type Cytokines, Hypereosinophilia, and Interleukin-5 in HIV Disease. Allergy 1997, 52, 110–111. [Google Scholar] [CrossRef]
- Rezaizadeh, H.; Sanchez-Ross, M.; Kaluski, E.; Klapholz, M.; Haider, B.; Gerula, C. Acute Eosinophilic Myocarditis: Diagnosis and Treatment. Acute Card. Care 2010, 12, 31–36. [Google Scholar] [CrossRef]
- Pearce, C.B.; McMeekin, J.D.; Moyana, T.N.; Sibley, J. A Case of Peripartum Eosinophilic Myocarditis. Can. J. Cardiol. 1999, 15, 465–468. [Google Scholar]
- Borczuk, A.C.; van Hoeven, K.H.; Factor, S.M. Review and Hypothesis: The Eosinophil and Peripartum Heart Disease (Myocarditis and Coronary Artery Dissection)–Coincidence or Pathogenetic Significance? Cardiovasc. Res. 1997, 33, 527–532. [Google Scholar] [CrossRef]
- Pollack, A.; Kontorovich, A.R.; Fuster, V.; Dec, G.W. Viral Myocarditis–Diagnosis, Treatment Options, and Current Controversies. Nat. Rev. Cardiol. 2015, 12, 670–680. [Google Scholar] [CrossRef]
- Kindermann, I.; Barth, C.; Mahfoud, F.; Ukena, C.; Lenski, M.; Yilmaz, A.; Klingel, K.; Kandolf, R.; Sechtem, U.; Cooper, L.T.; et al. Update on Myocarditis. J. Am. Coll. Cardiol. 2012, 59, 779–792. [Google Scholar] [CrossRef]
- Fozing, T.; Zouri, N.; Tost, A.; Breit, R.; Seeck, G.; Koch, C.; Oezbek, C. Management of a Patient with Eosinophilic Myocarditis and Normal Peripheral Eosinophil Count: Case Report and Literature Review. Circ. Heart Fail. 2014, 7, 692–694. [Google Scholar] [CrossRef]
- Cheung, C.C.; Constantine, M.; Ahmadi, A.; Shiau, C.; Chen, L.Y.C. Eosinophilic Myocarditis. Am. J. Med. Sci. 2017, 354, 486–492. [Google Scholar] [CrossRef]
- Young, J.D.; Peterson, C.G.; Venge, P.; Cohn, Z.A. Mechanism of Membrane Damage Mediated by Human Eosinophil Cationic Protein. Nature 1986, 321, 613–616. [Google Scholar] [CrossRef] [PubMed]
- Tai, P.C.; Hayes, D.J.; Clark, J.B.; Spry, C.J. Toxic Effects of Human Eosinophil Products on Isolated Rat Heart Cells in Vitro. Biochem. J. 1982, 204, 75–80. [Google Scholar] [CrossRef] [PubMed]
- Amini, R.; Nielsen, C. Eosinophilic Myocarditis Mimicking Acute Coronary Syndrome Secondary to Idiopathic Hypereosinophilic Syndrome: A Case Report. J. Med. Case Rep. 2010, 4, 40. [Google Scholar] [CrossRef] [PubMed]
- Cugno, M.; Marzano, A.V.; Lorini, M.; Carbonelli, V.; Tedeschi, A. Enhanced Tissue Factor Expression by Blood Eosinophils from Patients with Hypereosinophilia: A Possible Link with Thrombosis. PLoS ONE 2014, 9, e111862. [Google Scholar] [CrossRef] [PubMed]
- Aoki, A.; Hirahara, K.; Kiuchi, M.; Nakayama, T. Eosinophils: Cells Known for over 140 Years with Broad and New Functions. Allergol. Int. 2021, 70, 3–8. [Google Scholar] [CrossRef] [PubMed]
- Maisch, B.; Pankuweit, S. Standard and Etiology-Directed Evidence-Based Therapies in Myocarditis: State of the Art and Future Perspectives. Heart Fail. Rev. 2013, 18, 761–795. [Google Scholar] [CrossRef]
- Diny, N.L.; Hou, X.; Barin, J.G.; Chen, G.; Talor, M.V.; Schaub, J.; Russell, S.D.; Klingel, K.; Rose, N.R.; Čiháková, D. Macrophages and Cardiac Fibroblasts Are the Main Producers of Eotaxins and Regulate Eosinophil Trafficking to the Heart. Eur. J. Immunol. 2016, 46, 2749–2760. [Google Scholar] [CrossRef] [PubMed]
- Yamamoto, H.; Hashimoto, K.; Ikeda, Y.; Isogai, J.; Hashimoto, T. The Diagnostic Challenge of Eosinophilic Granulomatosis with Polyangiitis Presenting as Acute Eosinophilic Myocarditis: Case Report and Literature Review. Front. Cardiovasc. Med. 2022, 9, 913724. [Google Scholar] [CrossRef] [PubMed]
- Noth, I.; Strek, M.E.; Leff, A.R. Churg-Strauss Syndrome. Lancet 2003, 361, 587–594. [Google Scholar] [CrossRef] [PubMed]
- Boussir, H.; Ghalem, A.; Ismaili, N.; El Ouafi, N. Eosinophilic Myocarditis and Hypereosinophilic Syndrome. J. Saudi Heart Assoc. 2017, 29, 211–213. [Google Scholar] [CrossRef] [PubMed]
- Requena, G.; van den Bosch, J.; Akuthota, P.; Kovalszki, A.; Steinfeld, J.; Kwon, N.; Van Dyke, M.K. Clinical Profile and Treatment in Hypereosinophilic Syndrome Variants: A Pragmatic Review. J. Allergy Clin. Immunol. Pract. 2022, 10, 2125–2134. [Google Scholar] [CrossRef] [PubMed]
- Morimoto, S.; Kubo, N.; Hiramitsu, S.; Uemura, A.; Ohtsuki, M.; Kato, S.; Kato, Y.; Sugiura, A.; Miyagishima, K.; Mori, N.; et al. Changes in the Peripheral Eosinophil Count in Patients with Acute Eosinophilic Myocarditis. Heart Vessels 2003, 18, 193–196. [Google Scholar] [CrossRef]
- Valent, P.; Klion, A.D.; Roufosse, F.; Simon, D.; Metzgeroth, G.; Leiferman, K.M.; Schwaab, J.; Butterfield, J.H.; Sperr, W.R.; Sotlar, K.; et al. Proposed Refined Diagnostic Criteria and Classification of Eosinophil Disorders and Related Syndromes. Allergy 2023, 78, 47–59. [Google Scholar] [CrossRef]
- Pakbaz, M.; Pakbaz, M. Cardiac Involvement in Eosinophilic Granulomatosis with Polyangiitis: A Meta-Analysis of 62 Case Reports. J. Tehran Heart Cent. 2020, 15, 18–26. [Google Scholar] [CrossRef]
- Ukena, C.; Mahfoud, F.; Kindermann, I.; Kandolf, R.; Kindermann, M.; Böhm, M. Prognostic Electrocardiographic Parameters in Patients with Suspected Myocarditis. Eur. J. Heart Fail. 2011, 13, 398–405. [Google Scholar] [CrossRef]
- deMello, D.E.; Liapis, H.; Jureidini, S.; Nouri, S.; Kephart, G.M.; Gleich, G.J. Cardiac Localization of Eosinophil-Granule Major Basic Protein in Acute Necrotizing Myocarditis. N. Engl. J. Med. 1990, 323, 1542–1545. [Google Scholar] [CrossRef]
- Ramirez, G.A.; Yacoub, M.-R.; Ripa, M.; Mannina, D.; Cariddi, A.; Saporiti, N.; Ciceri, F.; Castagna, A.; Colombo, G.; Dagna, L. Eosinophils from Physiology to Disease: A Comprehensive Review. BioMed Res. Int. 2018, 2018, 9095275. [Google Scholar] [CrossRef]
- Szczerba, E.; Kowalik, R.; Gorska, K.; Mierzejewski, M.; Slowikowska, A.; Bednarczyk, T.; Marchel, M.; Krenke, R.; Opolski, G. Severe Mitral Stenosis Secondary to Eosinophilic Granulomatosis Resolving after Pharmacological Treatment. Echocardiography 2018, 35, 2099–2103. [Google Scholar] [CrossRef]
- Al-Kaisey, A.M.; Meher-Homji, Z.; Hayward, P.; Jones, E. Mitral and Tricuspid Valve Repair in Hypereosinophilic Syndrome. BMJ Case Rep. 2019, 12, e228951. [Google Scholar] [CrossRef]
- Friedrich, M.G.; Sechtem, U.; Schulz-Menger, J.; Holmvang, G.; Alakija, P.; Cooper, L.T.; White, J.A.; Abdel-Aty, H.; Gutberlet, M.; Prasad, S.; et al. Cardiovascular Magnetic Resonance in Myocarditis: A JACC White Paper. J. Am. Coll. Cardiol. 2009, 53, 1475–1487. [Google Scholar] [CrossRef]
- Guillevin, L.; Cohen, P.; Gayraud, M.; Lhote, F.; Jarrousse, B.; Casassus, P. Churg-Strauss Syndrome. Clinical Study and Long-Term Follow-up of 96 Patients. Medicine 1999, 78, 26–37. [Google Scholar] [CrossRef]
- Marmursztejn, J.; Guillevin, L.; Trebossen, R.; Cohen, P.; Guilpain, P.; Pagnoux, C.; Mouthon, L.; Legmann, P.; Vignaux, O.; Duboc, D. Churg-Strauss Syndrome Cardiac Involvement Evaluated by Cardiac Magnetic Resonance Imaging and Positron-Emission Tomography: A Prospective Study on 20 Patients. Rheumatology 2013, 52, 642–650. [Google Scholar] [CrossRef]
- Mavrogeni, S.; Dimitroulas, T.; Kitas, G.D. Multimodality Imaging and the Emerging Role of Cardiac Magnetic Resonance in Autoimmune Myocarditis. Autoimmun. Rev. 2012, 12, 305–312. [Google Scholar] [CrossRef]
- Markousis-Mavrogenis, G.; Sfikakis, P.P.; Koutsogeorgopoulou, L.; Dimitroulas, T.; Katsifis, G.; Giannakopoulou, A.; Voulgari, P.; Kolovou, G.; Kitas, G.D.; Mavrogeni, S.I. Cardiovascular Magnetic Resonance Reveals Cardiac Pathophysiology in Autoimmune Rheumatic Diseases. Mediterr. J. Rheumatol. 2021, 32, 15–20. [Google Scholar] [CrossRef]
- Greulich, S.; Mayr, A.; Kitterer, D.; Latus, J.; Henes, J.; Steubing, H.; Kaesemann, P.; Patrascu, A.; Greiser, A.; Groeninger, S.; et al. T1 and T2 Mapping for Evaluation of Myocardial Involvement in Patients with ANCA-Associated Vasculitides. J. Cardiovasc. Magn. Reson. 2017, 19, 6. [Google Scholar] [CrossRef]
- Lagan, J.; Naish, J.H.; Fortune, C.; Bradley, J.; Clark, D.; Niven, R.; Chaudhuri, N.; Schelbert, E.B.; Schmitt, M.; Miller, C.A. Myocardial Involvement in Eosinophilic Granulomatosis with Polyangiitis Evaluated with Cardiopulmonary Magnetic Resonance. Int. J. Cardiovasc. Imaging 2021, 37, 1371–1381. [Google Scholar] [CrossRef]
- Liu, X.; Zhou, Y.; Li, J.; Guo, T.; Lv, Z.; Zhang, D.; Feng, X.; Zhang, J.; Fang, L.; Tian, X.; et al. Cardiac Involvement in Eosinophilic Granulomatosis with Polyangiitis: Acute Eosinophilic Myocarditis and Chronic Inflammatory Cardiomyopathy. Rheumatology 2024, keae085, online ahead of print. [Google Scholar] [CrossRef]
- Fijolek, J.; Wiatr, E.; Gawryluk, D.; Nowicka, U.; Martusewicz-Boros, M.M.; Kober, J.; Piotrowska-Kownacka, D.; Roszkowski-Sliz, K. The Significance of Cardiac Magnetic Resonance Imaging in Detection and Monitoring of the Treatment Efficacy of Heart Involvement in Eosinophilic Granulomatosis with Polyangiitis Patients. Sarcoidosis Vasc. Diffus. Lung Dis. 2016, 33, 51–58. [Google Scholar]
- Aretz, H.T.; Billingham, M.E.; Edwards, W.D.; Factor, S.M.; Fallon, J.T.; Fenoglio, J.J.; Olsen, E.G.; Schoen, F.J. Myocarditis. A Histopathologic Definition and Classification. Am. J. Cardiovasc. Pathol. 1987, 1, 3–14. [Google Scholar]
- Cooper, L.T.; Baughman, K.L.; Feldman, A.M.; Frustaci, A.; Jessup, M.; Kuhl, U.; Levine, G.N.; Narula, J.; Starling, R.C.; Towbin, J.; et al. The Role of Endomyocardial Biopsy in the Management of Cardiovascular Disease: A Scientific Statement from the American Heart Association, the American College of Cardiology, and the European Society of Cardiology. Endorsed by the Heart Failure Society of America and the Heart Failure Association of the European Society of Cardiology. J. Am. Coll. Cardiol. 2007, 50, 1914–1931. [Google Scholar] [CrossRef]
- Sharma, A.N.; Stultz, J.R.; Bellamkonda, N.; Amsterdam, E.A. Fulminant Myocarditis: Epidemiology, Pathogenesis, Diagnosis, and Management. Am. J. Cardiol. 2019, 124, 1954–1960. [Google Scholar] [CrossRef]
- Ammirati, E.; Cipriani, M.; Lilliu, M.; Sormani, P.; Varrenti, M.; Raineri, C.; Petrella, D.; Garascia, A.; Pedrotti, P.; Roghi, A.; et al. Survival and Left Ventricular Function Changes in Fulminant Versus Nonfulminant Acute Myocarditis. Circulation 2017, 136, 529–545. [Google Scholar] [CrossRef]
- Legrand, F.; Klion, A.D. Biologic Therapies Targeting Eosinophils: Current Status and Future Prospects. J. Allergy Clin. Immunol. Pract. 2015, 3, 167–174. [Google Scholar] [CrossRef]
- Hayashi, S.; Isobe, M.; Okubo, Y.; Suzuki, J.; Yazaki, Y.; Sekiguchi, M. Improvement of Eosinophilic Heart Disease after Steroid Therapy: Successful Demonstration by Endomyocardial Biopsied Specimens. Heart Vessels 1999, 14, 104–108. [Google Scholar] [CrossRef]
- Ogbogu, P.U.; Bochner, B.S.; Butterfield, J.H.; Gleich, G.J.; Huss-Marp, J.; Kahn, J.E.; Leiferman, K.M.; Nutman, T.B.; Pfab, F.; Ring, J.; et al. Hypereosinophilic Syndrome: A Multicenter, Retrospective Analysis of Clinical Characteristics and Response to Therapy. J. Allergy Clin. Immunol. 2009, 124, 1319–1325.e3. [Google Scholar] [CrossRef]
- Kimura, Y.; Sasaki, K.; Inoko, M. Successful Early Steroid and Anticoagulant Treatment for Loeffler’s Endocarditis Related to Eosinophilic Granulomatosis with Polyangiitis. J. Cardiol. Cases 2017, 16, 109–112. [Google Scholar] [CrossRef] [PubMed]
- Kaneda, T.; Iwai, S.; Suematsu, T.; Yamamoto, R.; Takata, M.; Higashikata, T.; Ino, H.; Tsujibata, A. Acute Necrotizing Eosinophilic Myocarditis Complicated by Complete Atrioventricular Block Promptly Responded to Glucocorticoid Therapy. J. Cardiol. Cases 2017, 16, 5–8. [Google Scholar] [CrossRef]
- Miszalski-Jamka, T.; Szczeklik, W.; Sokołowska, B.; Karwat, K.; Miszalski-Jamka, K.; Jaźwiec, P.; Małek, Ł.A.; Al-Khalidi, H.; Schulz-Menger, J.; Mavrogeni, S.; et al. Noncorticosteroid Immunosuppression Limits Myocardial Damage and Contractile Dysfunction in Eosinophilic Granulomatosis with Polyangiitis (Churg-Strauss Syndrome). J. Am. Coll. Cardiol. 2015, 65, 103–105. [Google Scholar] [CrossRef]
- Song, T.; Jones, D.M.; Homsi, Y. Therapeutic Effect of Anti-IL-5 on Eosinophilic Myocarditis with Large Pericardial Effusion. BMJ Case Rep. 2017, 2017, bcr2016218992. [Google Scholar] [CrossRef]
- Cottu, A.; Groh, M.; Desaintjean, C.; Marchand-Adam, S.; Guillevin, L.; Puechal, X.; Beaumesnil, S.; Lazaro, E.; Samson, M.; Taille, C.; et al. Benralizumab for Eosinophilic Granulomatosis with Polyangiitis. Ann. Rheum. Dis. 2023, 82, 1580–1586. [Google Scholar] [CrossRef]
- FitzGerald, J.M.; Bleecker, E.R.; Nair, P.; Korn, S.; Ohta, K.; Lommatzsch, M.; Ferguson, G.T.; Busse, W.W.; Barker, P.; Sproule, S.; et al. Benralizumab, an Anti-Interleukin-5 Receptor α Monoclonal Antibody, as Add-on Treatment for Patients with Severe, Uncontrolled, Eosinophilic Asthma (CALIMA): A Randomised, Double-Blind, Placebo-Controlled Phase 3 Trial. Lancet 2016, 388, 2128–2141. [Google Scholar] [CrossRef]
- Yilmaz, A.; Kindermann, I.; Kindermann, M.; Mahfoud, F.; Ukena, C.; Athanasiadis, A.; Hill, S.; Mahrholdt, H.; Voehringer, M.; Schieber, M.; et al. Comparative Evaluation of Left and Right Ventricular Endomyocardial Biopsy: Differences in Complication Rate and Diagnostic Performance. Circulation 2010, 122, 900–909. [Google Scholar] [CrossRef]
- Hang, W.; Chen, C.; Seubert, J.M.; Wang, D.W. Fulminant Myocarditis: A Comprehensive Review from Etiology to Treatments and Outcomes. Signal Transduct. Target. Ther. 2020, 5, 287. [Google Scholar] [CrossRef]

| Etiology | Associated Clinical Condition |
|---|---|
| Hypersensitivity [17,18,19,20,21,22,23,24,25,26] |
|
| Vasculitis [27,28,29] |
|
| Hyper-eosinophilic syndrome (HES) [5,18,31,32,33] |
|
| Infections [3,5,34,35,36,37,38] |
|
| Cancer [39] |
|
| Other causes [40,41] |
|
| Idiopathic [3] |
|
| Context | Drugs |
| Systolic dysfunction [4] |
|
| Pulse Therapy [3,16] |
|
| Maintenance Therapy [3,16] |
|
| Fulminant EM [76,77] |
|
| EGPA-related EM [16,78] |
|
| Infections [15,16] |
|
| Hyper-eosinophilic Syndrome (HES) [3,16] |
|
| Hypersensitivity or Allergy [16] |
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Piccirillo, F.; Mastroberardino, S.; Nafisio, V.; Fiorentino, M.; Segreti, A.; Nusca, A.; Ussia, G.P.; Grigioni, F. Eosinophilic Myocarditis: From Bench to Bedside. Biomedicines 2024, 12, 656. https://doi.org/10.3390/biomedicines12030656
Piccirillo F, Mastroberardino S, Nafisio V, Fiorentino M, Segreti A, Nusca A, Ussia GP, Grigioni F. Eosinophilic Myocarditis: From Bench to Bedside. Biomedicines. 2024; 12(3):656. https://doi.org/10.3390/biomedicines12030656
Chicago/Turabian StylePiccirillo, Francesco, Sara Mastroberardino, Vincenzo Nafisio, Matteo Fiorentino, Andrea Segreti, Annunziata Nusca, Gian Paolo Ussia, and Francesco Grigioni. 2024. "Eosinophilic Myocarditis: From Bench to Bedside" Biomedicines 12, no. 3: 656. https://doi.org/10.3390/biomedicines12030656
APA StylePiccirillo, F., Mastroberardino, S., Nafisio, V., Fiorentino, M., Segreti, A., Nusca, A., Ussia, G. P., & Grigioni, F. (2024). Eosinophilic Myocarditis: From Bench to Bedside. Biomedicines, 12(3), 656. https://doi.org/10.3390/biomedicines12030656








