The Impact of Smoking on Microbiota: A Narrative Review
Abstract
1. Introduction
2. Materials and Methods
3. Results
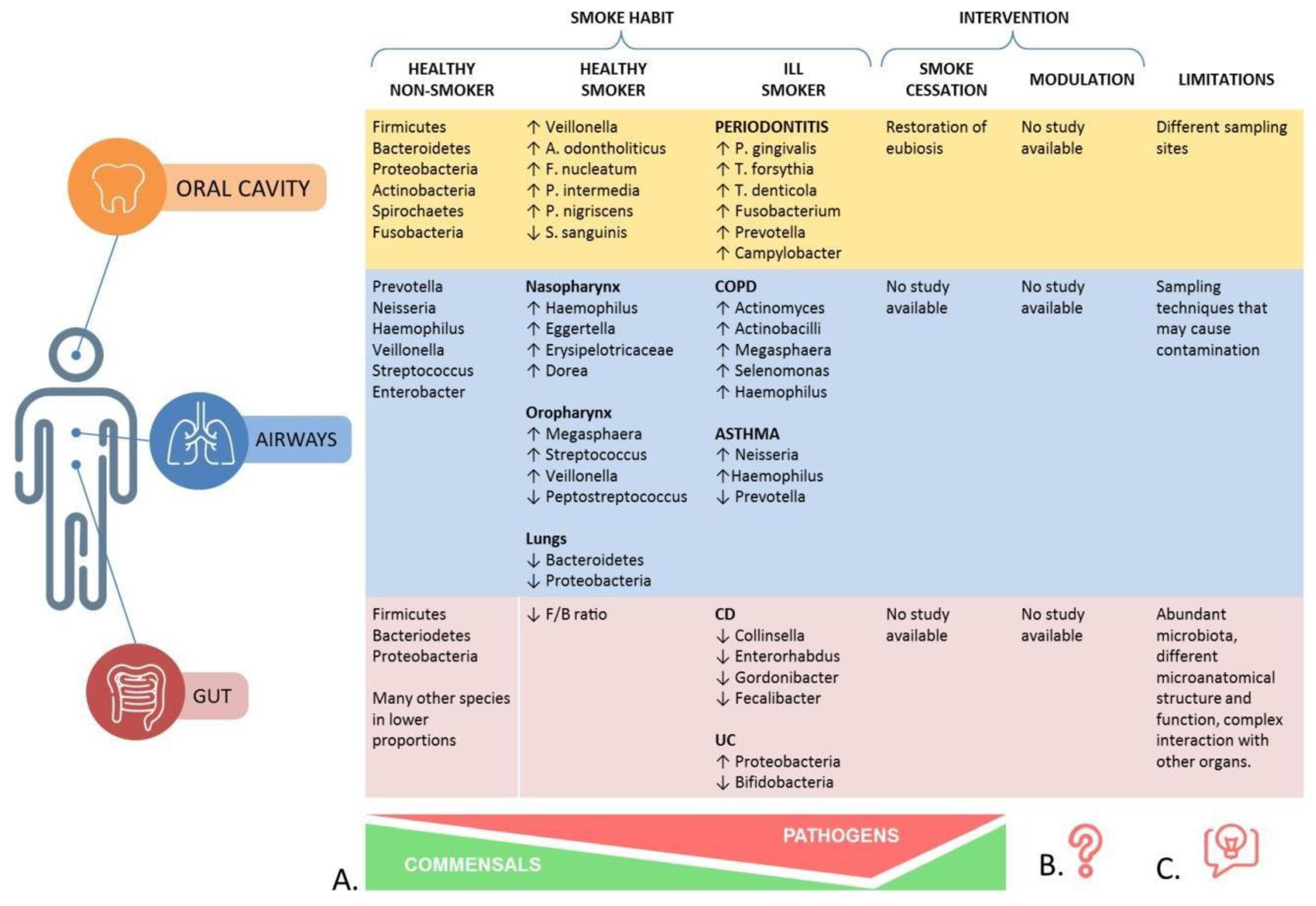
3.1. Section I—Oral Cavity
3.2. Section II—Airways
3.3. Section III—Gut
3.4. Section IV—Other Organs
4. Analysis and Limitations of Results
5. Discussion
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Dai, X.; Gil, G.F.; Reitsma, M.B.; Ahmad, N.S.; Anderson, J.A.; Bisignano, C.; Carr, S.; Feldman, R.; Hay, S.I.; He, J.; et al. Health effects associated with smoking: A Burden of Proof study. Nat. Med. 2022, 28, 2045–2055. [Google Scholar] [CrossRef] [PubMed]
- Gui, X.; Yang, Z.; Li, M.D. Effect of Cigarette Smoke on Gut Microbiota: State of Knowledge. Front. Physiol. 2021, 12, 673341. [Google Scholar] [CrossRef] [PubMed]
- GBD 2019 Tobacco Collaborators. Spatial, temporal, and demographic patterns in prevalence of smoking tobacco use and attributable disease burden in 204 countries and territories, 1990–2019: A systematic analysis from the Global Burden of Disease Study 2019. Lancet 2021, 397, 2337–2360. [Google Scholar] [CrossRef] [PubMed]
- Piccioni, A.; Rosa, F.; Manca, F.; Pignataro, G.; Zanza, C.; Savioli, G.; Covino, M.; Ojetti, V.; Gasbarrini, A.; Franceschi, F.; et al. Gut Microbiota and Clostridium difficile: What We Know and the New Frontiers. Int. J. Mol. Sci. 2022, 23, 13323. [Google Scholar] [CrossRef]
- Piccioni, A.; Saviano, A.; Cicchinelli, S.; Franza, L.; Rosa, F.; Zanza, C.; Santoro, M.C.; Candelli, M.; Covino, M.; Nannini, G.; et al. Microbiota and Myopericarditis: The New Frontier in the Cardiological Field to Prevent or Treat Inflammatory Cardiomyopathies in COVID-19 Outbreak. Biomedicines 2021, 9, 1234. [Google Scholar] [CrossRef]
- Piccioni, A.; Cicchinelli, S.; Valletta, F.; De Luca, G.; Longhitano, Y.; Candelli, M.; Ojetti, V.; Sardeo, F.; Navarra, S.; Covino, M.; et al. Gut Microbiota and Autoimmune Diseases: A Charming Real World Together with Probiotics. Curr. Med. Chem. 2022, 29, 3147–3159. [Google Scholar] [CrossRef]
- Mundula, T.; Russo, E.; Curini, L.; Giudici, F.; Piccioni, A.; Franceschi, F.; Amedei, A. Chronic Systemic Low-Grade Inflammation and Modern Lifestyle: The Dark Role of Gut Microbiota on Related Diseases with a Focus on COVID-19 Pandemic. Curr. Med. Chem. 2022, 29, 5370–5396. [Google Scholar] [CrossRef]
- Huang, C.; Shi, G. Smoking and microbiome in oral, airway, gut and some systemic diseases. J. Transl. Med. 2019, 17, 225. [Google Scholar] [CrossRef]
- Dewhirst, F.E.; Chen, T.; Izard, J.; Paster, B.J.; Tanner, A.C.R.; Yu, W.-H.; Lakshmanan, A.; Wade, W.G. The human oral microbiome. J. Bacteriol. 2010, 192, 5002–5017. [Google Scholar] [CrossRef]
- Human Oral Microbiome Database (HOMD). Available online: https://www.homd.org/ (accessed on 30 December 2022).
- Haffajee, A.D.; Socransky, S.S. Relationship of cigarette smoking to the subgingival microbiota. J. Clin. Periodontol. 2001, 28, 377–388. [Google Scholar] [CrossRef]
- Castillo, A.C.; Mira, A.; Pico, A.; Nibali, L.; Henderson, B.; Donos, N.; Tomã¡s, I. Subgingival microbiota in health compared to periodontitis and the influence of smoking. Front. Microbiol. 2015, 6, 119. [Google Scholar] [CrossRef] [PubMed]
- Yu, G.; Phillips, S.; Gail, M.H.; Goedert, J.J.; Humphrys, M.S.; Ravel, J.; Ren, Y.; Caporaso, N.E. The effect of cigarette smoking on the oral and nasal microbiota. Microbiome 2017, 5, 3. [Google Scholar] [CrossRef] [PubMed]
- Bašić, K.; Peroš, K.; Bošnjak, Z.; Šutej, I. Subgingival Microbiota Profile in Association with Cigarette Smoking in Young Adults: A Cross-Sectional Study. Dent. J. 2021, 9, 150. [Google Scholar] [CrossRef] [PubMed]
- Jia, Y.-J.; Liao, Y.; He, Y.-Q.; Zheng, M.-Q.; Tong, X.-T.; Xue, W.-Q.; Zhang, J.-B.; Yuan, L.-L.; Zhang, W.-L.; Jia, W.-H. Association Between Oral Microbiota and Cigarette Smoking in the Chinese Population. Front Cell Infect. Microbiol. 2021, 11, 658203. [Google Scholar] [CrossRef]
- Mason, M.R.; Preshaw, P.M.; Nagaraja, H.N.; Dabdoub, S.M.; Rahman, A.; Kumar, P.S. The subgingival microbiome of clinically healthy current and never smokers. ISME J. 2015, 9, 268–272. [Google Scholar] [CrossRef] [PubMed]
- Tadjoedin, F.M.; Masulili, S.L.C.; Rizal, M.I.; Kusdhany, L.S.; Turana, Y.; Ismail, R.I.; Bachtiar, B.M. The Red and Orange Complex Subgingival Microbiome of Cognitive Impairment and Cognitively Normal Elderly with Periodontitis. Geriatrics 2022, 7, 12. [Google Scholar] [CrossRef] [PubMed]
- Al Bataineh, M.T.; Dash, N.R.; Elkhazendar, M.; Alnusairat, D.M.H.; Darwish, I.M.I.; Al-Hajjaj, M.S.; Hamid, Q. Revealing oral microbiota composition and functionality associated with heavy cigarette smoking. J. Transl. Med. 2020, 18, 421. [Google Scholar] [CrossRef]
- Wang, X.; Luo, N.; Mi, Q.; Kong, W.; Zhang, W.; Li, X.; Gao, Q. Influence of cigarette smoking on oral microbiota in patients with recurrent aphthous stomatitis. J. Investig. Med. 2022, 70, 805–813. [Google Scholar] [CrossRef]
- Wu, Z.; Han, Y.; Caporaso, J.G.; Bokulich, N.; Mohamadkhani, A.; Moayyedkazemi, A.; Hua, X.; Kamangar, F.; Wan, Y.; Suman, S.; et al. Cigarette Smoking and Opium Use in Relation to the Oral Microbiota in Iran. Microbiol. Spectr. 2021, 9, e0013821. [Google Scholar] [CrossRef]
- Yang, Y.; Cai, Q.; Zheng, W.; Steinwandel, M.; Blot, W.J.; Shu, X.-O.; Long, J. Oral microbiome and obesity in a large study of low-income and African-American populations. J. Oral. Microbiol. 2019, 11, 1650597. [Google Scholar] [CrossRef]
- Fluhr, L.; Mor, U.; Kolodziejczyk, A.A.; Dori-Bachash, M.; Leshem, A.; Itav, S.; Cohen, Y.; Suez, J.; Zmora, N.; Moresi, C.; et al. Publisher Correction: Gut microbiota modulates weight gain in mice after discontinued smoke exposure. Nature 2022, 603, E35. [Google Scholar] [CrossRef] [PubMed]
- McLean, C.; Jun, S.; Kozyrskyj, A. Impact of maternal smoking on the infant gut microbiota and its association with child overweight: A scoping review. World J. Pediatr. 2019, 15, 341–349. [Google Scholar] [CrossRef] [PubMed]
- Al-Marzooq, F.; Al Kawas, S.; Rahman, B.; Shearston, J.A.; Saad, H.; Benzina, D.; Weitzman, M. Supragingival microbiome alternations as a consequence of smoking different tobacco types and its relation to dental caries. Sci. Rep. 2022, 12, 2861. [Google Scholar] [CrossRef] [PubMed]
- Wu, J.; Li, M.; Huang, R. The effect of smoking on caries-related microorganisms. Tob. Induc. Dis. 2019, 17, 32. [Google Scholar] [CrossRef]
- Bunaes, D.F.; Mustafa, M.; Mohamed, H.G.; Lie, S.A.; Leknes, K.N. The effect of smoking on inflammatory and bone remodeling markers in gingival crevicular fluid and subgingival microbiota following periodontal therapy. J. Periodontal. Res. 2017, 52, 713–724. [Google Scholar] [CrossRef]
- Grant, M.; Kilsgård, O.; Åkerman, S.; Klinge, B.; Demmer, R.T.; Malmström, J.; Jönsson, D. The Human Salivary Antimicrobial Peptide Profile according to the Oral Microbiota in Health, Periodontitis and Smoking. J. Innate Immun. 2019, 11, 432–444. [Google Scholar] [CrossRef]
- Mager, D.L.; Haffajee, A.D.; Socransky, S.S. Effects of periodontitis and smoking on the microbiota of oral mucous membranes and saliva in systemically healthy subjects. J. Clin. Periodontol. 2003, 30, 1031–1037. [Google Scholar] [CrossRef]
- Quaranta, A.; Assenza, B.; D’Isidoro, O.; Profili, F.; Polimeni, A.; Vozza, I. The impact of smoking and previous periodontal disease on peri-implant microbiota and health: A retrospective study up to 7-year follow-up. Ann. Stomatol. (Roma) 2015, 6, 21–28. [Google Scholar] [CrossRef]
- Stewart, C.J.; Auchtung, T.; Ajami, N.J.; Velasquez, K.; Smith, D.P.; Ii, R.D.L.G.; Salas, R.; Petrosino, J.F. Effects of tobacco smoke and electronic cigarette vapor exposure on the oral and gut microbiota in humans: A pilot study. PeerJ 2018, 6, e4693. [Google Scholar] [CrossRef]
- Tishchenko, O.V.; Kryvenko, L.S.; Gargina, V.V. Influence of smoking heating up tobacco products and e-cigarettes on the microbiota of dental plaque. Pol. Merkur Lekarski 2022, 50, 16–20. [Google Scholar]
- Morris, A.; Beck, J.M.; Schloss, P.D.; Campbell, T.B.; Crothers, K.; Curtis, J.L.; Flores, S.C.; Fontenot, A.P.; Ghedin, E.; Huang, L.; et al. Comparison of the respiratory microbiome in healthy nonsmokers and smokers. Am. J. Respir. Crit. Care Med. 2013, 187, 1067–1075. [Google Scholar] [CrossRef] [PubMed]
- Turek, E.M.; Cox, M.J.; Hunter, M.; Hui, J.; James, P.; Willis-Owen, S.A.G.; Cuthbertson, L.; James, A.; Musk, A.W.; Moffatt, M.F.; et al. Airway microbial communities, smoking and asthma in a general population sample. EBioMedicine 2021, 71, 103538. [Google Scholar] [CrossRef] [PubMed]
- Zhou, Y.; Jackson, D.; Bacharier, L.B.; Mauger, D.; Boushey, H.; Castro, M.; Durack, J.; Huang, Y.; Robert, F.L., Jr.; Storch, G.A.; et al. The upper-airway microbiota and loss of asthma control among asthmatic children. Nat. Commun. 2019, 10, 5714. [Google Scholar] [CrossRef] [PubMed]
- Lim, M.Y.; Yoon, H.S.; Rho, M.; Sung, J.; Song, Y.-M.; Lee, K.; Ko, G. Analysis of the association between host genetics, smoking, and sputum microbiota in healthy humans. Sci. Rep. 2016, 6, 23745. [Google Scholar] [CrossRef] [PubMed]
- Xu, X.; He, J.; Xue, J.; Wang, Y.; Li, K.; Zhang, K.; Guo, Q.; Liu, X.; Zhou, Y.; Cheng, L.; et al. Oral cavity contains distinct niches with dynamic microbial communities. Environ. Microbiol. 2015, 17, 699–710. [Google Scholar] [CrossRef] [PubMed]
- Brindisi, G.; Marazzato, M.; Brunetti, F.; De Castro, G.; Loffredo, L.; Carnevale, R.; Cinicola, B.; Palamara, A.T.; Conte, M.P.; Zicari, A.M. Allergic rhinitis, microbiota and passive smoke in children: A pilot study. Pediatr. Allergy Immunol. 2022, 33, 22–26. [Google Scholar] [CrossRef] [PubMed]
- Charlson, E.S.; Chen, J.; Custers-Allen, R.; Bittinger, K.; Li, H.; Sinha, R.; Hwang, J.; Bushman, F.D.; Collman, R.G. Disordered microbial communities in the upper respiratory tract of cigarette smokers. PLoS ONE 2010, 5, e15216. [Google Scholar] [CrossRef]
- Pulvirenti, G.; Parisi, G.F.; Giallongo, A.; Papale, M.; Manti, S.; Savasta, S.; Licari, A.; Marseglia, G.L.; Leonardi, S. Lower Airway Microbiota. Front. Pediatr. 2019, 7, 393. [Google Scholar] [CrossRef]
- Elgamal, Z.; Singh, P.; Geraghty, P. The Upper Airway Microbiota, Environmental Exposures, Inflammation, and Disease. Medicina 2021, 57, 823. [Google Scholar] [CrossRef]
- Hasegawa, K.; Camargo, C.A. Airway microbiota and acute respiratory infection in children. Expert Rev. Clin. Immunol. 2015, 11, 789–792. [Google Scholar] [CrossRef]
- Goto, T. Airway Microbiota as a Modulator of Lung Cancer. Int. J. Mol. Sci. 2020, 21, 3044. [Google Scholar] [CrossRef] [PubMed]
- Willers, M.; Viemann, D. Role of the gut microbiota in airway immunity and host defense against respiratory infections. Biol. Chem. 2021, 402, 1481–1491. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, D.M.; Dhotre, D.P.; Kumbhare, S.V.; Gaike, A.H.; Brashier, B.B.; Shouche, Y.S.; Juvekar, S.K.; Salvi, S.S. Disruptions in oral and nasal microbiota in biomass and tobacco smoke associated chronic obstructive pulmonary disease. Arch. Microbiol. 2021, 203, 2087–2099. [Google Scholar] [CrossRef] [PubMed]
- Hilty, M.; Burke, C.; Pedro, H.; Cardenas, P.; Bush, A.; Bossley, C.; Davies, J.; Ervine, A.; Poulter, L.; Pachter, L.; et al. Disordered microbial communities in asthmatic airways. PLoS ONE 2010, 5, e8578. [Google Scholar] [CrossRef] [PubMed]
- Marathe, S.J.; Snider, M.A.; Flores-Torres, A.S.; Dubin, P.J.; Samarasinghe, A.E. Human matters in asthma: Considering the microbiome in pulmonary health. Front. Pharmacol. 2022, 13, 1020133. [Google Scholar] [CrossRef]
- Hilty, M.; Wüthrich, T.M.; Godel, A.; Adelfio, R.; Aebi, S.; Burgener, S.S.; Illgen-Wilcke, B.; Benarafa, C. Chronic cigarette smoke exposure and pneumococcal infection induce oropharyngeal microbiota dysbiosis and contribute to long-lasting lung damage in mice. Microb. Genom. 2020, 6, 485. [Google Scholar] [CrossRef]
- Shen, P.; Whelan, F.J.; Schenck, L.P.; McGrath, J.J.C.; Vanderstocken, G.; Bowdish, D.M.E.; Surette, M.G.; Stämpfli, M.R. Streptococcus pneumoniae Colonization Is Required To Alter the Nasal Microbiota in Cigarette Smoke-Exposed Mice. Infect. Immun. 2017, 85, e00434-17. [Google Scholar] [CrossRef]
- Panzer, A.R.; Lynch, S.V.; Langelier, C.; Christie, J.D.; McCauley, K.; Nelson, M.; Cheung, C.K.; Benowitz, N.L.; Cohen, M.J.; Calfee, C.S. Lung Microbiota Is Related to Smoking Status and to Development of Acute Respiratory Distress Syndrome in Critically Ill Trauma Patients. Am. J. Respir. Crit. Care Med. 2018, 197, 621–631. [Google Scholar] [CrossRef]
- Qu, Z.; Zhang, L.; Hou, R.; Ma, X.; Yu, J.; Zhang, W.; Zhuang, C. Exposure to a mixture of cigarette smoke carcinogens disturbs gut microbiota and influences metabolic homeostasis in A/J mice. Chem. Biol. Interact. 2021, 344, 109496. [Google Scholar] [CrossRef]
- Bhattacharya, S.S.; Yadav, B.; Rosen, L.; Nagpal, R.; Yadav, H.; Yadav, J.S. Crosstalk between gut microbiota and lung inflammation in murine toxicity models of respiratory exposure or co-exposure to carbon nanotube particles and cigarette smoke extract. Toxicol. Appl. Pharmacol. 2022, 447, 1. [Google Scholar] [CrossRef]
- Li, X.; Cheng, W.; Shang, H.; Wei, H.; Deng, C. The Interplay between Androgen and Gut Microbiota: Is There a Microbiota-Gut-Testis Axis. Reprod Sci. 2022, 29, 1674–1684. [Google Scholar] [CrossRef] [PubMed]
- Xie, T.; Wang, Y.; Zou, Z.; He, J.; Yu, Y.; Liu, Y.; Bai, J. Environmental Tobacco Smoke Exposure and Breastfeeding Duration Influence the Composition and Dynamics of Gut Microbiota in Young Children Aged 0–2 Years. Biol. Res. Nurs. 2021, 23, 382–393. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Zhou, J.; Wang, L. Role and Mechanism of Gut Microbiota in Human Disease. Front. Cell Infect. Microbiol. 2021, 11, 625913. [Google Scholar] [CrossRef]
- Yan, S.; Ma, Z.; Jiao, M.; Wang, Y.; Li, A.; Ding, S. Effects of Smoking on Inflammatory Markers in a Healthy Population as Analyzed via the Gut Microbiota. Front. Cell Infect. Microbiol. 2021, 11, 633242. [Google Scholar] [CrossRef]
- Lee, S.H.; Yun, Y.; Kim, S.J.; Lee, E.-J.; Chang, Y.; Ryu, S.; Shin, H.; Kim, H.-L.; Kim, H.-N.; Lee, J.H. Association between Cigarette Smoking Status and Composition of Gut Microbiota: Population-Based Cross-Sectional Study. J. Clin. Med. 2018, 7, 282. [Google Scholar] [CrossRef] [PubMed]
- Shanahan, E.R.; Shah, A.; Koloski, N.; Walker, M.M.; Talley, N.J.; Morrison, M.; Holtmann, G.J. Influence of cigarette smoking on the human duodenal mucosa-associated microbiota. Microbiome 2018, 6, 150. [Google Scholar] [CrossRef]
- Li, Z.; Liu, Y.; Dou, L.; Zhang, Y.; He, S.; Zhao, D.; Zhang, W.; Wang, G. The effects of smoking and drinking on the oral and esophageal microbiota of healthy people. Ann. Transl. Med. 2021, 9, 1244. [Google Scholar] [CrossRef]
- Sublette, M.; Cross, T.-W.; Korcarz, C.; Hansen, K.; Murga-Garrido, S.; Hazen, S.; Wang, Z.; Oguss, M.; Rey, F.; Stein, J. Effects of Smoking and Smoking Cessation on the Intestinal Microbiota. J. Clin. Med. 2020, 9, 963. [Google Scholar] [CrossRef]
- Antinozzi, M.; Giffi, M.; Sini, N.; Gallè, F.; Valeriani, F.; De Vito, C.; Liguori, G.; Spica, V.R.; Cattaruzza, M.S. Cigarette Smoking and Human Gut Microbiota in Healthy Adults: A Systematic Review. Biomedicines 2022, 10, 510. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention (US); National Center for Chronic Disease Prevention and Health Promotion (US); Office on Smoking and Health (US). How Tobacco Smoke Causes Disease: The Biology and Behavioral Basis for Smoking-Attributable Disease: A Report of the Surgeon General; Centers for Disease Control and Prevention: Atlanta, GA, USA, 2010. [Google Scholar]
- Bai, X.; Wei, H.; Liu, W.; Coker, O.O.; Gou, H.; Liu, C.; Zhao, L.; Li, C.; Zhou, Y.; Wang, G.; et al. Cigarette smoke promotes colorectal cancer through modulation of gut microbiota and related metabolites. Gut 2022, 71, 2439–2450. [Google Scholar] [CrossRef]
- Hu, X.; Fan, Y.; Li, H.; Zhou, R.; Zhao, X.; Sun, Y.; Zhang, S. Impacts of Cigarette Smoking Status on Metabolomic and Gut Microbiota Profile in Male Patients With Coronary Artery Disease: A Multi-Omics Study. Front. Cardiovasc. Med. 2021, 8, 766739. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Yang, C.; Lei, Z.; Rong, H.; Yu, S.; Wu, H.; Yang, L.; Lei, Y.; Liu, W.; Nie, Y.; et al. Cigarette smoking exposure breaks the homeostasis of cholesterol and bile acid metabolism and induces gut microbiota dysbiosis in mice with different diets. Toxicology 2021, 450, 152678. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Ye, P.; Fang, L.; Ge, S.; Huang, F.; Polverini, P.J.; Heng, W.; Zheng, L.; Hu, Q.; Yan, F.; et al. Active Smoking Induces Aberrations in Digestive Tract Microbiota of Rats. Front. Cell Infect. Microbiol. 2021, 11, 737204. [Google Scholar] [CrossRef] [PubMed]
- Fluhr, L.; Mor, U.; Kolodziejczyk, A.A.; Dori-Bachash, M.; Leshem, A.; Itav, S.; Cohen, Y.; Suez, J.; Zmora, N.; Moresi, C.; et al. Gut microbiota modulates weight gain in mice after discontinued smoke exposure. Nature 2021, 600, 713–719. [Google Scholar] [CrossRef] [PubMed]
- Biedermann, L.; Zeitz, J.; Mwinyi, J.; Sutter-Minder, E.; Rehman, A.; Ott, S.J.; Steurer-Stey, C.; Frei, A.; Frei, P.; Scharl, M.; et al. Smoking cessation induces profound changes in the composition of the intestinal microbiota in humans. PLoS ONE 2013, 8, e59260. [Google Scholar] [CrossRef]
- Biedermann, L.; Brülisauer, K.; Zeitz, J.; Frei, P.; Scharl, M.; Vavricka, S.R.; Fried, M.; Loessner, M.J.; Rogler, G.; Schuppler, M. Smoking cessation alters intestinal microbiota: Insights from quantitative investigations on human fecal samples using FISH. Inflamm. Bowel. Dis. 2014, 20, 1496–1501. [Google Scholar] [CrossRef]
- Brotman, R.M.; He, X.; Gajer, P.; Fadrosh, D.; Sharma, E.; Mongodin, E.F.; Ravel, J.; Glover, E.D.; Rath, J.M. Association between cigarette smoking and the vaginal microbiota: A pilot study. BMC Infect. Dis. 2014, 14, 471. [Google Scholar] [CrossRef]
- Scheperjans, F.; Pekkonen, E.; Kaakkola, S.; Auvinen, P. Linking Smoking, Coffee, Urate, and Parkinson’s Disease—A Role for Gut Microbiota? J. Park. Dis. 2015, 5, 255–262. [Google Scholar] [CrossRef]
- Zhang, F.; Ma, C.; Zhang, B.; Bi, L. Dynamic changes in gut microbiota under the influence of smoking and TNF-α-blocker in patients with ankylosing spondylitis. Clin. Rheumatol. 2020, 39, 2653–2661. [Google Scholar] [CrossRef]
- Caliri, A.W.; Tommasi, S.; Besaratinia, A. Relationships among smoking, oxidative stress, inflammation, macromolecular damage, and cancer. Mutat. Res. Rev. Mutat. Res. 2021, 787, 108365. [Google Scholar] [CrossRef]
- Bizzarro, S.; Loos, B.G.; Laine, M.L.; Crielaard, W.; Zaura, E. Subgingival microbiome in smokers and non-smokers in periodontitis: An exploratory study using traditional targeted techniques and a next-generation sequencing. J. Clin. Periodontol. 2013, 40, 483–492. [Google Scholar] [CrossRef] [PubMed]
- Malhotra, J.; Malvezzi, M.; Negri, E.; La Vecchia, C.; Boffetta, P. Risk factors for lung cancer worldwide. Eur. Respir. J. 2016, 48, 889–902. [Google Scholar] [CrossRef] [PubMed]
- Toskala, E.; Kennedy, D.W. Asthma risk factors. Int. Forum Allergy Rhinol. 2015, 5 (Suppl. 1), S11–S16. [Google Scholar] [CrossRef] [PubMed]
- Maule, G.; Arosio, D.; Cereseto, A. Gene Therapy for Cystic Fibrosis: Progress and Challenges of Genome Editing. Int. J. Mol. Sci. 2020, 21, 3903. [Google Scholar] [CrossRef]
- Ananthakrishnan, A. Epidemiology and risk factors for IBD. Nat. Rev. Gastroenterol. Hepatol. 2015, 12, 205–217. [Google Scholar] [CrossRef]
- Adams, A.; Kalla, R.; Satsangi, J. Editorial: The influence of genetic factors in mediating the effects of tobacco smoke in IBD. Aliment. Pharmacol. Ther. 2018, 47, 306–307. [Google Scholar] [CrossRef]
- Short, M.W.; Burgers, K.G.; Fry, V.T. Esophageal Cancer. Am. Fam. Physician. 2017, 95, 22–28. [Google Scholar]
- Verhaar, B.J.H.; Prodan, A.; Nieuwdorp, M.; Muller, M. Gut Microbiota in Hypertension and Atherosclerosis: A Review. Nutrients 2020, 12, 2982. [Google Scholar] [CrossRef]
- Zhong, L.; Qin, L.; Ding, X.; Ma, L.; Wang, Y.; Liu, M.; Chen, H.; Yan, H.; Song, L. The regulatory effect of fermented black barley on the gut microbiota and metabolic dysbiosis in mice exposed to cigarette smoke. Food Res. Int. 2022, 157, 111465. [Google Scholar] [CrossRef]
- Dang, A.T.; Marsland, B.J. Microbes, metabolites, and the gut-lung axis. Mucosal. Immunol. 2019, 12, 843–850. [Google Scholar] [CrossRef]
- Margolis, K.G.; Cryan, J.F.; Mayer, E.A. The Microbiota-Gut-Brain Axis: From Motility to Mood. Gastroenterology 2021, 160, 1486–1501. [Google Scholar] [CrossRef] [PubMed]
- Schepis, T.; De Lucia, S.S.; Nista, E.C.; Manilla, V.; Pignataro, G.; Ojetti, V.; Piccioni, A.; Gasbarrini, A.; Franceschi, F.; Candelli, M. Microbiota in Pancreatic Diseases: A Review of the Literature. J. Clin. Med. 2021, 10, 5920. [Google Scholar] [CrossRef] [PubMed]
- Zanza, C.; Romenskaya, T.; Thangathurai, D.; Ojetti, V.; Saviano, A.; Abenavoli, L.; Robba, C.; Cammarota, G.; Franceschi, F.; Piccioni, A.; et al. Microbiome in Critical Care: An Unconventional and Unknown Ally. Curr. Med. Chem. 2022, 29, 3179–3188. [Google Scholar] [CrossRef] [PubMed]

| Inclusion Criteria | Exclusion Criteria |
|---|---|
| Type of article: in order of importance, we have considered clinical trials, observational studies, systematic reviews, narrative reviews. | Topic: articles regarding only the topic “microbiota” or only the topic “smoking”; articles treating other topics. |
| Language: only articles written in English. | |
| Year of publication: articles written in the last 25 years. |
| Group | Total Articles | References |
|---|---|---|
| Oral cavity | 24 | [8,9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31] |
| Airways | 21 | [32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52] |
| Gut | 16 | [53,54,55,56,57,58,59,60,61,62,63,64,65,66,67,68] |
| Other Organs | 3 | [69,70,71] |
| Total | 64 |
| Features of the Study | Conclusions | References |
|---|---|---|
| 82 patients, 22 non-smoking healthy controls, 28 non-smoking periodontal patients, and 32 smoking periodontal patients | Patients with periodontal disease have greater bacterial diversity, and non-smokers have a more diverse microbial community | Camelo-Castillo, A.J. et al., 2015 [12] |
| 32 smoking and 32 non-smoking | Smoking affects the composition of the subgingival microbiota | Bašić, K. et al., 2021 [14] |
| 316 healthy subjects | Smoking alters the composition of the microbiota of the oral cavity | Jia, Y. J. et al., 2021 [15] |
| 558 participants divided into non-smokers, cigarette smokers, opium smokers, or both | Cigarette and opium smoking is associated with lower alpha diversity and a different composition of the oral microbiota | Wu, Z. et al., 2021 [20] |
| Saliva samples donated by 41 people | Evidence of a different composition of the oral microbiota between healthy patients and those with periodontal disease, which in turn diversified, whether smokers or non-smokers | Grant, M. et al., 2019 [27] |
| 30 individuals, 10 tobacco smokers, 10 electronic cigarette users, and 10 controls. | Diverse composition in tobacco smokers, no significant differences between alpha or beta diversity, or in relative taxonomic abundances between e-cigarette users and controls | Stewart, C. J. et al., 2018 [30] |
| Features of the Study | Conclusions | References |
|---|---|---|
| 29 smokers and 33 healthy adults | In smokers, the airway microbiota was significantly more diverse | Charlson, E. S. et al., 2010 [38] |
| 11 patients with COPD associated with tobacco smoke, 10 with COPD associated with biomass smoke, 10 healthy individuals | Evidence of microbial community dysbiosis among different groups | Agarwal, D. M. et al., 2021 [44] |
| 74 patients admitted after severe blunt trauma | Smokers had a significant increase in potential pathogens | Panzer, A. R. et al., 2018 [49] |
| Features of the Study | Conclusions | References |
|---|---|---|
| 33 smokers and 121 non-smokers | Smoking significantly affected the gut microbiota | Yan, S. et al., 2021 [55] |
| 758 men, divided into never smokers, former smokers, and current smokers | Different composition of gut microbiota between smokers and non-smokers; no difference between smokers and ex-smokers | Lee, S. H. et al., 2018 [56] |
| 102 patients undergoing endoscopy | Both smokers and ex-smokers show reduced bacterial diversity in the small intestinal mucosa of the upper intestine compared with those who have never smoked | Shanahan, E. R. et al., 2018 [57] |
| 76 healthy participants | Finding of taxonomic and microbial diversity in the oral and esophageal cavity among non-drinkers and non-smokers compared with drinkers and smokers | Li, Z. et al., 2021 [58] |
| 36 patients who were trying to quit smoking | Minor changes were found once smoking was stopped | Sublette, M. G. et al., 2020 [59] |
| Systematic Review | In most works, a decrease in both bacterial species and variability indices was found in fecal samples from smokers | Antinozzi, M. et al., 2022 [60] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cicchinelli, S.; Rosa, F.; Manca, F.; Zanza, C.; Ojetti, V.; Covino, M.; Candelli, M.; Gasbarrini, A.; Franceschi, F.; Piccioni, A. The Impact of Smoking on Microbiota: A Narrative Review. Biomedicines 2023, 11, 1144. https://doi.org/10.3390/biomedicines11041144
Cicchinelli S, Rosa F, Manca F, Zanza C, Ojetti V, Covino M, Candelli M, Gasbarrini A, Franceschi F, Piccioni A. The Impact of Smoking on Microbiota: A Narrative Review. Biomedicines. 2023; 11(4):1144. https://doi.org/10.3390/biomedicines11041144
Chicago/Turabian StyleCicchinelli, Sara, Federico Rosa, Federica Manca, Christian Zanza, Veronica Ojetti, Marcello Covino, Marcello Candelli, Antonio Gasbarrini, Francesco Franceschi, and Andrea Piccioni. 2023. "The Impact of Smoking on Microbiota: A Narrative Review" Biomedicines 11, no. 4: 1144. https://doi.org/10.3390/biomedicines11041144
APA StyleCicchinelli, S., Rosa, F., Manca, F., Zanza, C., Ojetti, V., Covino, M., Candelli, M., Gasbarrini, A., Franceschi, F., & Piccioni, A. (2023). The Impact of Smoking on Microbiota: A Narrative Review. Biomedicines, 11(4), 1144. https://doi.org/10.3390/biomedicines11041144












