Platelet Membrane Proteins as Pain Biomarkers in Patients with Severe Dementia
Abstract
1. Introduction
2. Materials and Methods
2.1. Platelets Membrane Proteins Evaluation by Flow Cytometry
2.2. Statistical Analysis
2.3. Inclusion Criteria
3. Results
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Raja, S.N.; Carr, D.B.; Cohen, M.; Finnerup, N.B.; Flor, H.; Gibson, S.; Keefe, F.J.; Mogil, J.S.; Ringkamp, M.; Sluka, K.A.; et al. The revised International Association for the Study of Pain definition of pain: Concepts, challenges, and compromises. Pain 2020, 161, 1976–1982. [Google Scholar] [CrossRef]
- Garcia-Larrea, L.; Peyron, R. Pain matrices and neuropathic pain matrices: A review. Pain 2013, 154 (Suppl. 1), S29–S43. [Google Scholar] [CrossRef] [PubMed]
- Orr, P.M.; Shank, B.C.; Black, A.C. The Role of Pain Classification Systems in Pain Management. Crit. Care Nurs. Clin. N. Am. 2017, 29, 407–418. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. WHO’s Pain Relief Ladder; WHO: Geneva, Switzerland, 2009.
- Ribeiro, H.; Moutinho, R.; Dourado, M. Particularidades da Avaliação e Tratamento da dor no Idoso: Contributo Para a Validação da Pain Quality Assessment Scale© e Abordagem Terapêutica na População Idosa; Universidade de Coimbra: Coimbra, Portugal, 2017. [Google Scholar]
- World Health Organization. Normative Guidelines on Pain Management; WHO: Geneva, Switzerland, 2007.
- Ali, A.; Arif, A.W.; Bhan, C.; Kumar, D.; Malik, M.B.; Sayyed, Z.; Akhtar, K.H.; Ahmad, M.Q. Managing Chronic Pain in the Elderly: An Overview of the Recent Therapeutic Advancements. Cureus 2018, 10, e3293. [Google Scholar] [CrossRef]
- Marchi, A.; Vellucci, R.; Mameli, S.; Piredda, A.R.; Finco, G. Pain Biomarkers. Clin. Drug Investig. 2009, 29 (Suppl. 1), 41–46. [Google Scholar] [CrossRef]
- Chen, Y.; Zhong, H.; Zhao, Y.; Luo, X.; Gao, W. Role of platelet biomarkers in inflammatory response. Biomark. Res. 2020, 8, 28. [Google Scholar] [CrossRef] [PubMed]
- Kopeikina, E.; Ponomarev, E.D. The Role of Platelets in the Stimulation of Neuronal Synaptic Plasticity, Electric Activity, and Oxidative Phosphorylation: Possibilities for New Therapy of Neurodegenerative Diseases. Front. Cell. Neurosci. 2021, 15, 269. [Google Scholar] [CrossRef] [PubMed]
- Ribatti, D.; Crivellato, E. Giulio Bizzozero and the discovery of platelets. Leuk. Res. 2007, 31, 1339–1341. [Google Scholar] [CrossRef]
- Akingbade, O.E.; Gibson, C.; Kalaria, R.N.; Mukaetova-Ladinska, E.B. Platelets: Peripheral Biomarkers of Dementia? J. Alzheimer's Dis. 2018, 63, 1235–1259. [Google Scholar] [CrossRef]
- Arman, M.; Payne, H.; Ponomaryov, T.; Brill, A. Role of Platelets in Inflammation. InTech 2015. [Google Scholar] [CrossRef]
- Ringkamp, M.; Schmelz, M.; Kress, M.; Allwang, M.; Ogilvie, A.; Reeh, P. Activated human platelets in plasma excite nociceptors in rat skin, in vitro. Neurosci. Lett. 1994, 170, 103–106. [Google Scholar] [CrossRef] [PubMed]
- Osman, Y.; Vatte, C.B. Study of platelet activation markers and plasma cytokines in sickle cell disease patients during vaso-occlusive pain crises. J. Hematop. 2018, 11, 37–44. [Google Scholar] [CrossRef]
- Niculescu, A.B.; Le-Niculescu, H.; Levey, D.F.; Roseberry, K.; Soe, K.C.; Rogers, J.; Khan, F.; Jones, T.; Judd, S.; McCormick, M.A.; et al. Towards precision medicine for pain: Diagnostic biomarkers and repurposed drugs. Mol. Psychiatry 2019, 24, 501–522. [Google Scholar] [CrossRef]
- Salem, H.H. Leg Pain and Platelet Aggregates in Thrombocythemic Myeloproliferative Disease. JAMA 1980, 244, 1122. [Google Scholar] [CrossRef] [PubMed]
- Kwon, Y.-J.; Koh, I.; Chung, K.; Lee, Y.-J.; Kim, H.-S. Association between platelet count and osteoarthritis in women older than 50 years. Ther. Adv. Musculoskelet. Dis. 2020, 12. [Google Scholar] [CrossRef] [PubMed]
- Barkai, O.; Puig, S.; Lev, S.; Title, B.; Katz, B.; Eli-Berchoer, L.; Gutstein, H.B.; Binshtok, A.M. Platelet-derived growth factor activates nociceptive neurons by inhibiting M-current and contributes to inflammatory pain. Pain 2019, 160, 1281–1296. [Google Scholar] [CrossRef]
- Weth, D.; Benetti, C.; Rauch, C.; Gstraunthaler, G.; Schmidt, H.; Geisslinger, G.; Sabbadini, R.; Proia, R.; Kress, M. Activated platelets release sphingosine 1-phosphate and induce hypersensitivity to noxious heat stimuli in vivo. Front. Neurosci. 2015, 9, 140. [Google Scholar] [CrossRef]
- Jankovic, S.; Aleksic, Z.; Klokkevold, P.; Lekovic, V.; Dimitrijevic, B.; Kenney, E.B.; Camargo, P. Use of platelet-rich fibrin membrane following treatment of gingival recession: A randomized clinical trial. Int. J. Periodontics Restor. Dent. 2012, 32, e41-50. [Google Scholar]
- Chignon-Sicard, B.; Georgiou, C.A.; Fontas, E.; David, S.; Dumas, P.; Ihrai, T.; Lebreton, E. Efficacy of Leukocyte- and Platelet-Rich Fibrin in Wound Healing. Plast. Reconstr. Surg. 2012, 130, 819e–829e. [Google Scholar] [CrossRef]
- Kumar, N.; Prasad, K.; Ramanujam, L.; Ranganath, K.; Dexith, J.; Chauhan, A. Evaluation of Treatment Outcome After Impacted Mandibular Third Molar Surgery With the Use of Autologous Platelet-Rich Fibrin: A Randomized Controlled Clinical Study. J. Oral Maxillofac. Surg. 2015, 73, 1042–1049. [Google Scholar] [CrossRef]
- Ozgul, O.; Senses, F.; Er, N.; Tekin, U.; Tuz, H.H.; Alkan, A.; Kocyigit, I.D.; Atil, F. Efficacy of platelet rich fibrin in the reduction of the pain and swelling after impacted third molar surgery: Randomized multicenter split-mouth clinical trial. Head Face Med. 2015, 11, 37. [Google Scholar] [CrossRef] [PubMed]
- Ludwig, N.; Hilger, A.; Zarbock, A.; Rossaint, J. Platelets at the Crossroads of Pro-Inflammatory and Resolution Pathways during Inflammation. Cells 2022, 11, 1957. [Google Scholar] [CrossRef] [PubMed]
- Gianazza, E.; Brioschi, M.; Baetta, R.; Mallia, A.; Banfi, C.; Tremoli, E. Platelets in Healthy and Disease States: From Biomarkers Discovery to Drug Targets Identification by Proteomics. Int. J. Mol. Sci. 2020, 21, 4541. [Google Scholar] [CrossRef] [PubMed]
- Warden, V.; Hurley, A.C.; Volicer, L. Development and Psychometric Evaluation of the Pain Assessment in Advanced Dementia (PAINAD) Scale. J. Am. Med. Dir. Assoc. 2003, 4, 9–15. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez, C.S. Pain measurement in the elderly: A review. Pain Manag. Nurs. 2001, 2, 38–46. [Google Scholar] [CrossRef] [PubMed]
- Michels, W.M.; Grootendorst, D.C.; Verduijn, M.; Elliott, E.G.; Dekker, F.W.; Krediet, R.T. Performance of the Cockcroft-Gault, MDRD, and New CKD-EPI Formulas in Relation to GFR, Age, and Body Size. Clin. J. Am. Soc. Nephrol. 2010, 5, 1003–1009. [Google Scholar] [CrossRef]
- Mor, V.; Ms, L.L.; Morris, J.N.; Wiemann, M. The Karnofsky performance status scale: An examination of its reliability and validity in a research setting. Cancer 1984, 53, 2002–2007. [Google Scholar] [CrossRef]
- Soysal, P.; Isik, A.T.; Arik, F.; Kalan, U.; Eyvaz, A.; Veronese, N. Validity of the Mini-Nutritional Assessment Scale for Evaluating Frailty Status in Older Adults. J. Am. Med. Dir. Assoc. 2019, 20, 183–187. [Google Scholar] [CrossRef]
- Saboor, M.; Ayub, Q.; Ilyas, S. Moinuddin Platelet receptors; an instrumental of platelet physiology. Pak. J. Med. Sci. 2013, 29, 891–896. [Google Scholar] [CrossRef]
- Silverstein, R.L.; Febbraio, M. CD36, a Scavenger Receptor Involved in Immunity, Metabolism, Angiogenesis, and Behavior. Sci. Signal. 2009, 2, re3. [Google Scholar] [CrossRef]
- Yang, Z.; Dong, P.; Fu, X.; Li, Q.; Ma, S.; Wu, D.; Kang, N.; Liu, X.; Yan, L.; Xiao, R. CD49f Acts as an Inflammation Sensor to Regulate Differentiation, Adhesion, and Migration of Human Mesenchymal Stem Cells. Stem Cells 2015, 33, 2798–2810. [Google Scholar] [CrossRef]
- Barbar, L.; Jain, T.; Zimmer, M.; Kruglikov, I.; Sadick, J.S.; Wang, M.; Kalpana, K.; Rose, I.V.; Burstein, S.R.; Rusielewicz, T.; et al. CD49f Is a Novel Marker of Functional and Reactive Human iPSC-Derived Astrocytes. Neuron 2020, 107, 436–453.e12. [Google Scholar] [CrossRef] [PubMed]
- Antibody Engineering & Therapeutics, Human P Selectin CD62P. Available online: https://www.creative-biolabs.com/magic-antibody-discovery-human-p-selectin-cd62p-42-771-membrane-protein-partial-higg1-fc-tag-4597.htm?gclid=CjwKCAiA9qKbBhAzEiwAS4yeDb2xogl7NOfoyX_wAeIwqYZ7Uvy2cbPeaGyuErgcsu-zrgV7CMsuIRoC2boQAvD_BwE (accessed on 10 October 2022).
- Weinstock, C.; Anliker, M.; Von Zabern, I. CD59: A long-known complement inhibitor has advanced to a blood group system. Immunohematology 2015, 31, 145–151. [Google Scholar] [CrossRef]
- Dostert, C.; Grusdat, M.; Letellier, E.; Brenner, D. The TNF Family of Ligands and Receptors: Communication Modules in the Immune System and Beyond. Physiol. Rev. 2019, 99, 115–160. [Google Scholar] [CrossRef]
- Steel, H.C.; Venter, W.D.F.; Theron, A.J.; Anderson, R.; Feldman, C.; Arulappan, N.; Rossouw, T.M. Differential Responsiveness of the Platelet Biomarkers, Systemic CD40 Ligand, CD62P, and Platelet-Derived Growth Factor-BB, to Virally-Suppressive Antiretroviral Therapy. Front. Immunol. 2021, 11, 594110. [Google Scholar] [CrossRef]
- Ramos-Cejudo, J.; Johnson, A.D.; Beiser, A.; Seshadri, S.; Salinas, J.; Berger, J.S.; Fillmore, N.R.; Do, N.; Zheng, C.; Kovbasyuk, Z.; et al. Platelet Function Is Associated With Dementia Risk in the Framingham Heart Study. J. Am. Heart Assoc. 2022, 11, e023918. [Google Scholar] [CrossRef]
- Sevush, S.; Jy, W.; Horstman, L.L.; Mao, W.-W.; Kolodny, L.; Ahn, Y.S. Platelet Activation in Alzheimer Disease. Arch. Neurol. 1998, 55, 530–536. [Google Scholar] [CrossRef]
- Green, S.A.; Smith, M.; Hasley, R.B.; Stephany, D.; Harned, A.; Nagashima, K.; Abdullah, S.; Pittaluga, S.; Imamichi, T.; Qin, J.; et al. Activated platelet–T-cell conjugates in peripheral blood of patients with HIV infection. Aids 2015, 29, 1297–1308. [Google Scholar] [CrossRef]
- Valkonen, S.; Mallas, B.; Impola, U.; Valkeajärvi, A.; Eronen, J.; Javela, K.; Siljander, P.R.-M.; Laitinen, S. Assessment of Time-Dependent Platelet Activation Using Extracellular Vesicles, CD62P Exposure, and Soluble Glycoprotein V Content of Platelet Concentrates with Two Different Platelet Additive Solutions. Transfus. Med. Hemotherapy 2019, 46, 267–275. [Google Scholar] [CrossRef]
- Reches, A.; Eldor, A.; Vogel, Z.; Salomon, Y. Do human platelets have opiate receptors? Nature 1980, 288, 382–383. [Google Scholar] [CrossRef]
- Gruba, S.M.; Francis, D.H.; Meyer, A.F.; Spanolios, E.; He, J.; Meyer, B.M.; Kim, D.; Xiong-Hang, K.; Haynes, C.L. Characterization of the Presence and Function of Platelet Opioid Receptors. ACS Meas. Sci. Au 2021, 2, 4–13. [Google Scholar] [CrossRef]
- Farag, M.; Srinivasan, M.; A Gorog, D. 28 Impact of Opiate Analgesia on Platelet Reactivity in Patients Presenting for Primary Percutaneous Coronary Intervention. Heart 2016, 102 (Suppl. 6), A19. [Google Scholar] [CrossRef]
- Schedel, A.; Thornton, S.; Klüter, H.; Bugert, P. The Effect of Psychoactive Drugs on in vitro Platelet Function. Transfus. Med. Hemotherapy 2010, 37, 9. [Google Scholar] [CrossRef]
- Bekő, K.; Koványi, B.; Gölöncsér, F.; Horváth, G.; Denes, A.; Környei, Z.; Botz, B.; Helyes, Z.; Müller, C.E.; Sperlágh, B. Contribution of platelet P2Y12 receptors to chronic Complete Freund’s adjuvant-induced inflammatory pain. J. Thromb. Haemost. 2017, 15, 1223–1235. [Google Scholar] [CrossRef]
- Altintoprak, F.; Arslan, Y.; Yalkin, O.; Uzunoglu, Y.; Ozkan, O.V. Mean platelet volume as a potential prognostic marker in patients with acute mesenteric ischemia–retrospective study. World J. Emerg. Surg. 2013, 8, 49. [Google Scholar] [CrossRef] [PubMed]
- Levi, M.; Toh, C.H.; Thachil, J.; Watson, H.G. Guidelines for the diagnosis and management of disseminated intravascular coagulation. Br. J. Haematol. 2009, 145, 24–33. [Google Scholar] [CrossRef] [PubMed]
- Avcioğlu, S.N.; Altinkaya, S.; Küçük, M.; Demircan-Sezer, S.; Yüksel, H. Can Platelet Indices Be New Biomarkers for Severe Endometriosis? ISRN Obstet. Gynecol. 2014, 2014, 1–6. [Google Scholar] [CrossRef] [PubMed]
| Total of Patients: 53 | Patients with Pain and Dementia (n = 38) | Patients with Pain and without Dementia (n = 6) | Patients without Pain and without Dementia (Controls) (n = 9) | |
|---|---|---|---|---|
| Gender | Male | 29% (n = 11) | 50% (n = 3) | 0 |
| Female | 71% (n = 27) | 50% (n = 3) | 100% | |
| Average age (years) | 84.1 | 62.5 | 44.7 | |
| PAINAD | <5 | 15.8% (n = 6) | NA | NA * |
| 5–7 | 73.7% (n = 28) | NA | NA | |
| 8–10 | 10.5% (n = 4) | NA | NA | |
| Average numeric pain scale | NA | 4.3 | 0 | |
| Type of Pain | Nociceptive | 39.5% (n = 15) | 50% (n = 3) | NA |
| Neuropathic | 2.6% (n = 1) | 16.7% (n = 1) | NA | |
| Mixed | 57.9% (n = 22) | 33.3% (n = 2) | NA | |
| Type of Dementia | Vascular | 36.8% (n = 14) | NA | NA |
| Alzheimer | 36.8% (n = 14) | NA | NA | |
| Mixed | 7.9% (n = 3) | NA | NA | |
| Other | 18.4% (n = 7) | NA | NA | |
| Under opioid treatment | 39.5% (n = 15) | 66.7% (n = 4) | NA | |
| Patients without Pain and without Dementia Controls (n = 9) | Patients with Pain (n = 44) | ||
|---|---|---|---|
| M ± SD | M ± SD | p | |
| CD36 (%) | 98.04 ±1.97 | 91.54 ± 12.30 | 0.004 ** |
| CD36 (MIF) | 6475.64 ± 2081.58 | 5506.31 ± 2168.98 | 0.228 |
| CD49f (%) | 99.16 ± 0.35 | 95.31 ± 10.79 | 0.037 * |
| CD49f (MIF) | 5385.83 ± 855.09 | 4540.24 ± 969.50 | 0.021 * |
| CD61 (%) | 99.37 ± 0.18 | 95.28 ± 10.76 | 0.026 * |
| CD61 (MIF) | 16561.81 ± 1404.83 | 13571.25 ± 4064.78 | 0.009 ** |
| CD62P (%) | 8.47 ± 4.87 | 22.62 ± 23.65 | 0.002 ** |
| CD62P (MIF) | 760.75 ± 114.10 | 1357.76 ± 2606.10 | 0.499 |
| CD59 (%) | 4.76 ± 3.03 | 3.45 ± 5.67 | 0.507 |
| MIF CD59 (MIF) | 1556.62 ± 509.90 | 1771.15 ± 858.56 | 0.478 |
| CD40 (%) | 0.15 ± 0.09 | 0.09 ± 0.17 | 0.289 |
| CD40 (MIF) | 1476.08 ± 352.14 | 1456.12 ± 501.07 | 0.911 |
| Female (n = 39) | Male (n = 14) | ||
|---|---|---|---|
| M ± SD | M ± SD | p | |
| % CD36 | 92.89 ± 10.89 | 92.58 ± 13.25 | 0.899 |
| MIF CD36 | 5392.26 ± 2050.79 | 6662.28 ± 2330.91 | 0.090 |
| % CD49f | 96.35 ± 8.80 | 95.18 ± 12.86 | 0.445 |
| MIF CD49f | 4617.57 ± 978.43 | 4986.02 ± 1057.26 | 0.291 |
| % CD61 | 96.38 ± 8.80 | 95.13 ± 12.83 | 0.272 |
| MIF CD61 | 14465.44 ± 3481.59 | 13172.91 ± 4992.24 | 0.525 |
| % CD62P | 13.76 ± 17.43 | 39.24 ± 24.50 | 0.006 *** |
| MIF CD62P | 829.68 ± 261.73 | 2549.57 ± 4691.50 | 0.251 |
| % CD59 | 3.74 ± 5.35 | 3.59 ± 5.20 | 0.839 |
| MIF CD59 | 1643.84 ± 790.28 | 2000.70 ± 815.41 | 0.130 |
| % CD40 | 0.09 ± 0.10 | 0.14 ± 0.28 | 0.939 |
| MIF CD40 | 1471.59 ± 505.76 | 1423.23 ± 362.89 | 0.899 |
| No Opioids (n = 25) | Opioids (n = 19) | ||
|---|---|---|---|
| M ± SD | M ± SD | p | |
| % pos CD36 | 95.58± 8.38 | 88.52± 14.02 | 0.026 * |
| MIF CD36 | 6007.26 ± 2091.56 | 5211.73 ± 2246.28 | 0.228 |
| % pos CD49f | 98.82 ± 2.39 | 91.78 ± 14.55 | 0.070 |
| MIF CD49f | 4995.90± 850.84 | 4254.22± 1065.23 | 0.012 * |
| % pos CD61 | 98.87 ± 2.40 | 91.73 ± 14.51 | 0.077 |
| MIF CD61 | 15128.72± 3014.28 | 12643.79± 4616.87 | 0.029 * |
| % pos CD62P | 21.08 ± 22.70 | 17.93 ± 21.35 | 0.290 |
| MIF CD62P | 1483.69 ± 2983.98 | 863.37 ± 388.08 | 0.242 |
| % pos CD59 | 2.94 ± 3.33 | 4.90 ± 7.28 | 0.597 |
| MIF CD59 | 1975.92± 886.94 | 1345.35± 444.10 | 0.008 ** |
| % pos CD40 | 0.07 ± 0.08 | 0.15 ± 0.23 | 0.742 |
| MIF CD40 | 1485.36 ± 467.55 | 1420.60 ± 490.21 | 0.458 |
| Nociceptive (n = 18) | Mixed (n = 26) | ||
|---|---|---|---|
| M ± SD | M ± SD | p | |
| % pos CD36 | 91.17 ± 11.90 | 92.52 ± 10.84 | 0.762 |
| MIF CD36 | 4751.72 ± 1640.23 | 5952.76 ± 2468.46 | 0.118 |
| % pos CD49f | 94.47 ± 12.16 | 97.46 ± 5.19 | 0.789 |
| MIF CD49f | 4206.69 ± 995.35 | 4859.81 ± 890.59 | 0.056 |
| % pos CD61 | 94.37 ± 12.13 | 97.45 ± 5.15 | 0.762 |
| MIF CD61 | 12507.53 ± 5215.25 | 14025.16 ± 3190.66 | 0.682 |
| % pos CD62P | 13.89 ± 14.69 | 31.73 ± 28.35 | 0.117 |
| MIF CD62P | 723.55 ± 184.49 | 1953.63 ± 3679.90 | 0.002 ** |
| % pos CD59 | 4.49 ± 6.59 | 3.05 ± 5.46 | 0.789 |
| MIF CD59 | 1570.69 ± 826.36 | 1963.51 ± 937.17 | 0.274 |
| % pos CD40 | 0.16 ± 0.25 | 0.04 ± 0.02 | 0.145 |
| MIF CD40 | 1530.59 ± 601.99 | 1466.89 ± 448.98 | 0.986 |
| Mild Pain (PAINAD < 5) | Moderate or Severe Pain (PAINAD 5-10) | ||
|---|---|---|---|
| M | M | p | |
| % pos CD36 | 90.34 ± 18.24 | 92.88 ± 9.64 | 0.563 |
| MIF CD36 | 5635.97 ± 2538.02 | 5424.41 ± 2158.15 | 0.859 |
| % pos CD49f | 99.19 ± 0.66 | 95.94 ± 9.29 | 0.625 |
| MIF CD49f | 4310.17 ± 1200.38 | 4549.61 ± 949.86 | 0.723 |
| % pos CD61 | 99.16 ± 0.66 | 95.90 ± 9.27 | 0.625 |
| MIF CD61 | 10900.50 ± 4611.48 | 13915.31 ± 3929.31 | 0.059 |
| % pos CD62P | 16.62 ± 21.39 | 23.77 ± 24.53 | 0.690 |
| MIF CD62P | 3966.84 ± 7066.90 | 918.62 ± 383.06 | 0.533 |
| % pos CD59 | 1.25 ± 1.49 | 3.90 ± 6.08 | 0.282 |
| MIF CD59 | 1699.58 ± 1043.69 | 1793.88 ± 856.69 | 0.533 |
| % pos CD40 | 0.02 ± 0.02 | 0.10 ± 0.18 | 0.047 * |
| MIF CD40 | 1202.00 ± 232.79 | 1509.31 ± 524.97 | 0.207 |
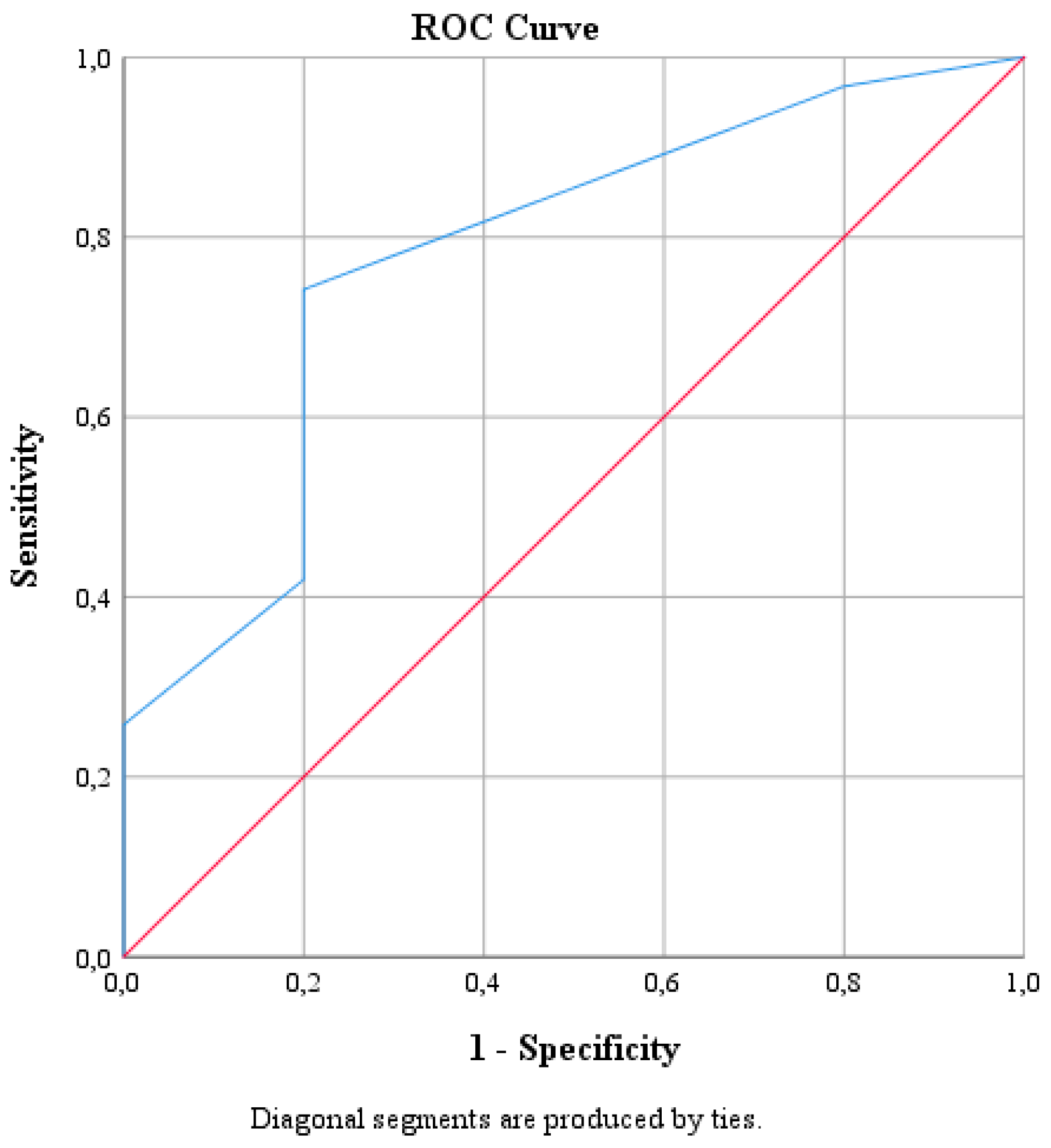
| Area | SE a | Asymptotic p b | Asymptotic 95% Confidence Interval | |
|---|---|---|---|---|
| Lower Bound | Upper Bound | |||
| 0.777 | 0.114 | 0.049 | 0.555 | 1.000 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ribeiro, H.; Alves, R.; Jorge, J.; Gonçalves, A.C.; Sarmento-Ribeiro, A.B.; Teixeira-Veríssimo, M.; Dourado, M.; Andrade, J.P. Platelet Membrane Proteins as Pain Biomarkers in Patients with Severe Dementia. Biomedicines 2023, 11, 380. https://doi.org/10.3390/biomedicines11020380
Ribeiro H, Alves R, Jorge J, Gonçalves AC, Sarmento-Ribeiro AB, Teixeira-Veríssimo M, Dourado M, Andrade JP. Platelet Membrane Proteins as Pain Biomarkers in Patients with Severe Dementia. Biomedicines. 2023; 11(2):380. https://doi.org/10.3390/biomedicines11020380
Chicago/Turabian StyleRibeiro, Hugo, Raquel Alves, Joana Jorge, Ana Cristina Gonçalves, Ana Bela Sarmento-Ribeiro, Manuel Teixeira-Veríssimo, Marília Dourado, and José Paulo Andrade. 2023. "Platelet Membrane Proteins as Pain Biomarkers in Patients with Severe Dementia" Biomedicines 11, no. 2: 380. https://doi.org/10.3390/biomedicines11020380
APA StyleRibeiro, H., Alves, R., Jorge, J., Gonçalves, A. C., Sarmento-Ribeiro, A. B., Teixeira-Veríssimo, M., Dourado, M., & Andrade, J. P. (2023). Platelet Membrane Proteins as Pain Biomarkers in Patients with Severe Dementia. Biomedicines, 11(2), 380. https://doi.org/10.3390/biomedicines11020380








