Diagnostic and Therapeutic Potential of Circulating-Free DNA and Cell-Free RNA in Cancer Management
Abstract
:1. Introduction
- ⯀
- Circulating tumor DNA
- ⯀
- Cell-Free fetal DNA
- ⯀
- Cell-Free mitochondrial DNA
2. Secretion
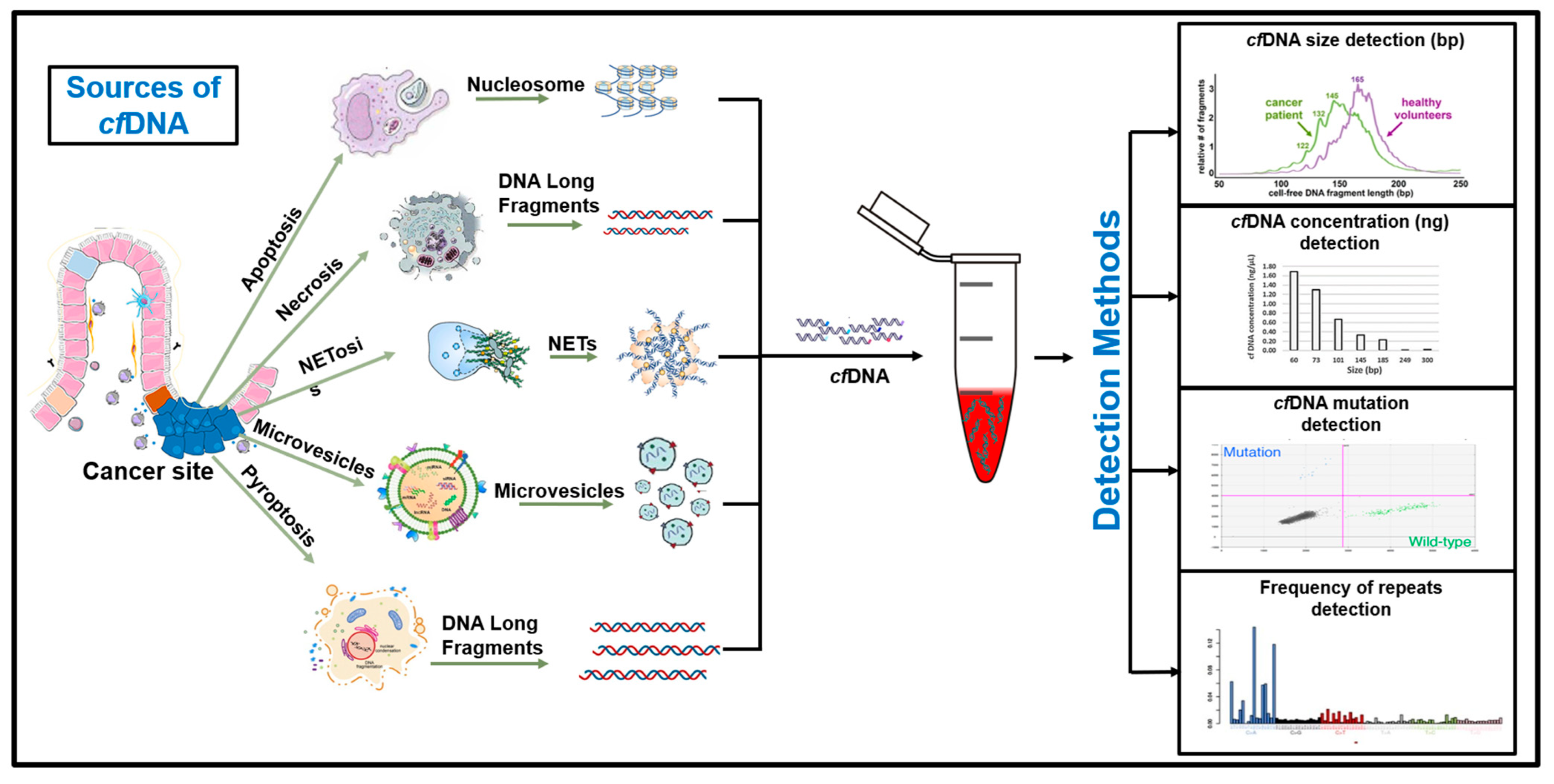
2.1. Secretion of cfDNA
2.2. Secretion of cfRNA
- ⯀
- Passive leakage from the tumor or apoptotic or necrotic cells;
- ⯀
- Active secretion through microvesicles;
- ⯀
- Secretion through nucleoproteins or protein-RNA complex.
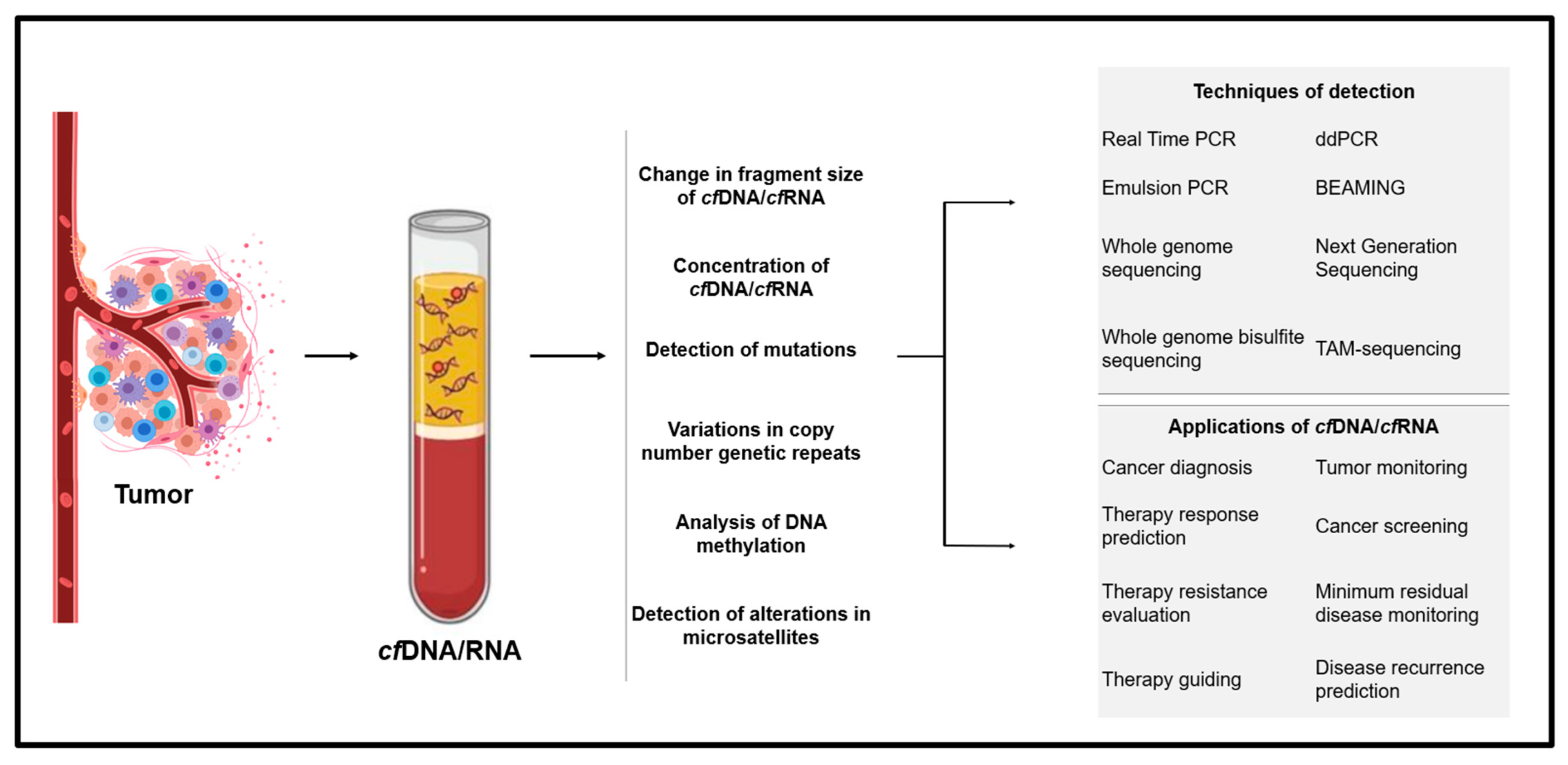
3. Discerning cfDNA and cfDRNA Molecular Alterations in Clinical Management
4. Applications of cfDNA and cfRNA
4.1. Role of cfDNA and cfRNA in Cancer Diagnosis
4.1.1. Role of cfDNA
4.1.2. Role of cfRNA
| Sr number | Technique Name | Description | Sensitivity (Lower Limit of Detection) | Specificity | Limitations | Cancer Type |
|---|---|---|---|---|---|---|
| 1 | Quantitative polymerase chain reaction | Amplifies the genes in real-time | 0.01–0.1% | 90% for breast cancer [70] | Needs standard, prone to errors, primer design depends on results | Non-small cell lung cancer, breast cancer |
| 2 | Droplet digital polymerase chain reaction | Water–oil emulsion droplet technology-based PCR | 0.01–0.1% | 100% [71] | Lower quantification, loss of linearity at a high concentration | Lung adenocarcinomas, squamous cell carcinoma, neck cancer, breast cancer, gastric cancer, and others |
| 3 | Beads, emulsion, amplification, and magnetics | Combination of emulsion PCR and flow cytometry ultrasensitive technique | <0.1% | ---- | Single mutation per test; lacks standard data | Blood cancer, colorectal cancer |
| 4 | Cancer personalized profiling by deep sequencing | NGS-based method for ctDNA detection | 0.01%–2.0% | 96% [72] | For selected alterations across targeted regions | Cervical squamous cancer, bladder cancer, esophageal, lung cancer |
| 5 | Whole-genome sequencing | Analysis of the whole genome | 2 × 10−3 [73], up to 10−5 shown by different studies [74]. | 98.4% for somatic SNV and indels [75] | Expensive, comparatively low sensitivity and specificity, large amounts of data | Gastric cancer, pancreatic cancer, breast cancer |
| 6 | TAm-Sequencing | Identify low-frequency mutations in ctDNA | 2% | 97% for ovarian cancer [76] | Less comprehensive | Breast cancer, hepatocellular carcinoma |
| 7 | Whole exome sequencing | A sequencing-based technique to study protein-coding regions in the genome | Generally 5% [77], some studies show 50% [78] | 99.9% [79] | Rare variants affect the sensitivity, restricted only to exon regions | Metastatic melanoma, multiple myeloma |
| 8 | Whole-genome bisulfite sequencing | NGS-based technique to find out the methylation status of cytosine | --- | 99% [80] | It is difficult to differentiate between substitutions and epiallele changes; single reference genomes are not enough to discriminate the changes. It is expensive and generates a large amount of data [81] | Breast cancer, prostate cancer |
4.1.3. Challenges in cfDNA and cfRNA Diagnoses
4.2. cfDNA and cfRNA Roles as Prognostic Markers
4.2.1. cfDNA
4.2.2. cfRNA
4.3. Role of cfDNA and cfRNA in Measuring Residual Disease
4.3.1. ctDNA
4.3.2. cfRNA
| Cancer Types | Clinical Management | Conclusion | References |
|---|---|---|---|
| Breast Cancer | Assessment of early ctDNA dynamics in 149 patients | Assessment of early dynamic changes in ctDNA can predict the efficacy of targeted therapy | [106] |
| Prediction of recurrence of cancer | Predicted metastatic relapse with high accuracy | [103] | |
| Detection of PIK3CA mutations | CtDNA can be used for the detection of PIK3CA mutations | [107] | |
| Lung cancer | Cancer diagnosis and therapeutics | EGFR L858R and T790M mutations can be detected in ctDNA using NGS and ddPCR | [108] |
| Detection of cancer at IA, IB, and IIA stages | Found an association among tumor stage, subtype, and cfDNA concentration, and demonstrated the utility and feasibility of targeted sequencing for ctDNA monitoring | [109] | |
| Monitoring treatment response and drug resistance | Proved the decrease of mutant copies after treatment and monitored the emergence of secondary mutations | [110] | |
| Detection of copy number variations in tumor cells | Copy number changed in BAX, P53, CASP3, SOX2, GRB2, SOS1, MAPK1, and a few other genes of cancer patients | [111,112] | |
| Diagnostic marker | The presence of ctDNA in cancer patients was found to be eight times higher than in healthy persons | [113] | |
| Colon cancer | Adjuvant therapy | Provided evidence of the potential use of ctDNA with adjuvant novel drugs for cancer patients | [114] |
| Colorectal cancer | Marker for cancer recurrence | Postoperative ctDNA positivity may be associated with the recurrence of cancer | [115] |
| Predicting response to neoadjuvant chemoradiotherapy | Combination of MRI and ctDNA potentially improves the predictive performance of cancer | [116] | |
| Novel biomarker Optimizing chemotherapy | Described that ctDNA can potentially be utilized for diagnosis and personalized medicine for colorectal cancer | [117] | |
| Melanoma | Monitoring of relapse in stage III | ctDNA identified the highest risk stage III melanoma patients and helped in adjuvant therapy decisions | [118] |
| Detection of ctDNA levels in patients treated with anti-PD1 therapy | The evaluation of ctDNA during anti-PD1 antibody therapy provided reliable information | [119] | |
| Leiomyosarcoma | Detection of genetic variants using Guardant360 | The identification of molecular alterations can help develop therapy, targeting TP53, cell cycle, and kinase signaling pathways | [120] |
5. Clinical Trials
5.1. ctDNA
5.1.1. TARGET Study
5.1.2. MONALEESA Study
5.1.3. I-PREDICT Study
5.2. cfRNA
5.2.1. ICE-PAC
5.2.2. NCT02853097
6. Food and Drug Administration Approved ctDNA and cfRNA Tests
7. Other Techniques for Cancer Detection
8. Discussion
9. Future Directions and Limitations
10. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Hassan, S.; Ali, M.N.; Ghafoor, B. Evolutionary perspective of drug eluting stents: From thick polymer to polymer free approach. J. Cardiothorac. Surg. 2022, 17, 65. [Google Scholar] [CrossRef] [PubMed]
- Mandel, P.; Metais, P. Nuclear Acids In Human Blood Plasma. Comptes Rendus Seances Soc. Biol. Fil. 1948, 142, 241–243. [Google Scholar]
- Bendich, A.; Wilczok, T.; Borenfreund, E. Circulating dna as a possible factor in oncogenesis. Science 1965, 148, 374–376. [Google Scholar] [CrossRef] [PubMed]
- Tan, E.M.; Schur, P.H.; Carr, R.I.; Kunkel, H.G. Deoxybonucleic acid (DNA) and antibodies to DNA in the serum of patients with systemic lupus erythematosus. J. Clin. Investig. 1966, 45, 1732–1740. [Google Scholar] [CrossRef] [PubMed]
- Leon, S.A.; Shapiro, B.; Sklaroff, D.M.; Yaros, M.J. Free DNA in the serum of cancer patients and the effect of therapy. Cancer Res. 1977, 37, 646–650. [Google Scholar] [PubMed]
- Pös, O.; Biró, O.; Szemes, T.; Nagy, B. Circulating cell-free nucleic acids: Characteristics and applications. Eur. J. Hum. Genet. 2018, 26, 937–945. [Google Scholar] [CrossRef] [Green Version]
- Tosevska, A.; Morselli, M.; Basak, S.K.; Avila, L.; Mehta, P.; Wang, M.B.; Srivatsan, E.S.; Pellegrini, M. Cell-Free RNA as a Novel Biomarker for Response to Therapy in Head & Neck Cancer. Front. Oncol. 2022, 12, 869108. [Google Scholar] [CrossRef]
- Raez, L.E.; Danenberg, K.; Sumarriva, D.; Usher, J.; Sands, J.; Castrellon, A.; Ferraro, P.; Milillo, A.; Huang, E.; Soon-Shiong, P.; et al. Using cfRNA as a tool to evaluate clinical treatment outcomes in patients with metastatic lung cancers and other tumors. Cancer Drug Resist. 2021, 4, 1061–1071. [Google Scholar] [CrossRef]
- Andree, K.C.; van Dalum, G.; Terstappen, L.W. Challenges in circulating tumor cell detection by the CellSearch system. Mol. Oncol. 2016, 10, 395–407. [Google Scholar] [CrossRef] [Green Version]
- Samsuwan, J.; Somboonchokepisal, T.; Akaraputtiporn, T.; Srimuang, T.; Phuengsukdaeng, P.; Suwannarat, A.; Mutirangura, A.; Kitkumthorn, N. A method for extracting DNA from hard tissues for use in forensic identification. Biomed. Rep. 2018, 9, 433–438. [Google Scholar] [CrossRef]
- Lee, K.J.; Mann, E.; da Silva, L.M.; Scalici, J.; Gassman, N.R. DNA damage measurements within tissue samples with Repair Assisted Damage Detection (RADD). Curr. Res. Biotechnol. 2019, 1, 78–86. [Google Scholar] [CrossRef] [PubMed]
- Seton-Rogers, S. Closing in on cfDNA-based detection and diagnosis. Nat. Rev. Cancer 2020, 20, 481. [Google Scholar] [CrossRef] [PubMed]
- Rafi, I.; Chitty, L. Cell-free fetal DNA and non-invasive prenatal diagnosis. Br. J. Gen. Pract. J. R. Coll. Gen. Pract. 2009, 59, e146–e148. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Berezin, A.J.T.B. The cell-free mitochondrial DNA: A novel biomarker of cardiovascular risk. Transl. Biomed. 2016, 7, 68–71. [Google Scholar] [CrossRef]
- Al Amir Dache, Z.; Otandault, A.; Tanos, R.; Pastor, B.; Meddeb, R.; Sanchez, C.; Arena, G.; Lasorsa, L.; Bennett, A.; Grange, T.; et al. Blood contains circulating cell-free respiratory competent mitochondria. FASEB J. 2020, 34, 3616–3630. [Google Scholar] [CrossRef] [Green Version]
- Pessoa, L.S.; Heringer, M.; Ferrer, V.P. ctDNA as a cancer biomarker: A broad overview. Crit. Rev. Oncol. Hematol. 2020, 155, 103109. [Google Scholar] [CrossRef]
- An, Q.; Hu, Y.; Li, Q.; Chen, X.; Huang, J.; Pellegrini, M.; Zhou, X.J.; Rettig, M.; Fan, G. The size of cell-free mitochondrial DNA in blood is inversely correlated with tumor burden in cancer patients. Precis. Clin. Med. 2019, 2, 131–139. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Underhill, H.R.; Kitzman, J.O.; Hellwig, S.; Welker, N.C.; Daza, R.; Baker, D.N.; Gligorich, K.M.; Rostomily, R.C.; Bronner, M.P.; Shendure, J. Fragment length of circulating tumor DNA. PLoS Genet. 2016, 12, e1006162. [Google Scholar] [CrossRef]
- Fan, H.C.; Blumenfeld, Y.J.; Chitkara, U.; Hudgins, L.; Quake, S.R. Analysis of the size distributions of fetal and maternal cell-free DNA by paired-end sequencing. Clin. Chem. 2010, 56, 1279–1286. [Google Scholar] [CrossRef] [Green Version]
- Wyllie, A.; Morris, R.; Smith, A.; Dunlop, D. Chromatin cleavage in apoptosis: Association with condensed chromatin morphology and dependence on macromolecular synthesis. J. Pathol. 1984, 142, 67–77. [Google Scholar] [CrossRef]
- Stroun, M.; Lyautey, J.; Lederrey, C.; Olson-Sand, A.; Anker, P. About the possible origin and mechanism of circulating DNA apoptosis and active DNA release. Clin. Chim. Acta 2001, 313, 139–142. [Google Scholar] [CrossRef]
- Aucamp, J.; Bronkhorst, A.J.; Badenhorst, C.P.S.; Pretorius, P.J. The diverse origins of circulating cell-free DNA in the human body: A critical re-evaluation of the literature. Biol. Rev. 2018, 93, 1649–1683. [Google Scholar] [CrossRef] [PubMed]
- Heitzer, E.; Auinger, L.; Speicher, M.R. Cell-Free DNA and Apoptosis: How Dead Cells Inform About the Living. Trends Mol. Med. 2020, 26, 519–528. [Google Scholar] [CrossRef]
- Jackson Chornenki, N.L.; Coke, R.; Kwong, A.C.; Dwivedi, D.J.; Xu, M.K.; McDonald, E.; Marshall, J.C.; Fox-Robichaud, A.E.; Charbonney, E.; Liaw, P.C. Comparison of the source and prognostic utility of cfDNA in trauma and sepsis. Intensive Care Med. Exp. 2019, 7, 29. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Goggs, R.; Jeffery, U.; LeVine, D.N.; Li, R.H.L. Neutrophil-Extracellular Traps, Cell-Free DNA, and Immunothrombosis in Companion Animals: A Review. Vet. Pathol. 2020, 57, 6–23. [Google Scholar] [CrossRef] [PubMed]
- Li, R.H.L.; Tablin, F. A Comparative Review of Neutrophil Extracellular Traps in Sepsis. Front. Vet. Sci. 2018, 5, 291. [Google Scholar] [CrossRef] [Green Version]
- Elzanowska, J.; Semira, C.; Costa-Silva, B. DNA in extracellular vesicles: Biological and clinical aspects. Mol. Oncol. 2021, 15, 1701–1714. [Google Scholar] [CrossRef]
- Salehi, B.; Mishra, A.P.; Nigam, M.; Kobarfard, F.; Javed, Z.; Rajabi, S.; Khan, K.; Ashfaq, H.A.; Ahmad, T.; Pezzani, R. Multivesicular liposome (Depofoam) in human diseases. Iran. J. Pharm. Res. IJPR 2020, 19, 9. [Google Scholar]
- Balaj, L.; Lessard, R.; Dai, L.; Cho, Y.J.; Pomeroy, S.L.; Breakefield, X.O.; Skog, J. Tumour microvesicles contain retrotransposon elements and amplified oncogene sequences. Nat. Commun. 2011, 2, 180. [Google Scholar] [CrossRef]
- Thakur, B.K.; Zhang, H.; Becker, A.; Matei, I.; Huang, Y.; Costa-Silva, B.; Zheng, Y.; Hoshino, A.; Brazier, H.; Xiang, J.; et al. Double-stranded DNA in exosomes: A novel biomarker in cancer detection. Cell Res. 2014, 24, 766–769. [Google Scholar] [CrossRef] [Green Version]
- Abe, J.-I.; Morrell, C. Pyroptosis as a Regulated Form of Necrosis: PI+/Annexin V-/High Caspase 1/Low Caspase 9 Activity in Cells = Pyroptosis? Circul. Res. 2016, 118, 1457–1460. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hou, J.; Zhao, R.; Xia, W.; Chang, C.W.; You, Y.; Hsu, J.M.; Nie, L.; Chen, Y.; Wang, Y.C.; Liu, C.; et al. PD-L1-mediated gasdermin C expression switches apoptosis to pyroptosis in cancer cells and facilitates tumour necrosis. Nat. Cell Biol. 2020, 22, 1264–1275. [Google Scholar] [CrossRef] [PubMed]
- Fang, Y.; Tian, S.; Pan, Y.; Li, W.; Wang, Q.; Tang, Y.; Yu, T.; Wu, X.; Shi, Y.; Ma, P.; et al. Pyroptosis: A new frontier in cancer. Biomed. Pharmacother. 2020, 121, 109595. [Google Scholar] [CrossRef] [PubMed]
- Alqurashi, H.; Ortega Asencio, I.; Lambert, D.W. The Emerging Potential of Extracellular Vesicles in Cell-Free Tissue Engineering and Regenerative Medicine. Tissue Eng. Part B Rev. 2021, 27, 530–538. [Google Scholar] [CrossRef]
- Guo, Y.; Wang, H.; Huang, L.; Ou, L.; Zhu, J.; Liu, S.; Xu, X. Small extracellular vesicles-based cell-free strategies for therapy. MedComm 2021, 2, 17–26. [Google Scholar] [CrossRef]
- Chiu, B.C.H.; Chen, C.; You, Q.; Chiu, R.; Venkataraman, G.; Zeng, C.; Zhang, Z.; Cui, X.; Smith, S.M.; He, C.; et al. Alterations of 5-hydroxymethylation in circulating cell-free DNA reflect molecular distinctions of subtypes of non-Hodgkin lymphoma. NPJ Genom. Med. 2021, 6, 11. [Google Scholar] [CrossRef]
- Schwaederle, M.; Chattopadhyay, R.; Kato, S.; Fanta, P.T.; Banks, K.C.; Choi, I.S.; Piccioni, D.E.; Ikeda, S.; Talasaz, A.; Lanman, R.B.; et al. Genomic Alterations in Circulating Tumor DNA from Diverse Cancer Patients Identified by Next-Generation Sequencing. Cancer Res. 2017, 77, 5419–5427. [Google Scholar] [CrossRef] [Green Version]
- Khan, K.; Safi, S.; Abbas, A.; Badshah, Y.; Dilshad, E.; Rafiq, M.; Zahra, K.; Shabbir, M. Unravelling Structure, Localization, and Genetic Crosstalk of KLF3 in Human Breast Cancer. Biomed. Res. Int. 2020, 2020, 1354381. [Google Scholar] [CrossRef]
- Zahra, K.; Shabbir, M.; Badshah, Y.; Trembley, J.H.; Badar, Z.; Khan, K.; Afsar, T.; Almajwal, A.; Alruwaili, N.W.; Razak, S. Determining KLF14 tertiary structure and diagnostic significance in brain cancer progression. Sci. Rep. 2022, 12, 8039. [Google Scholar] [CrossRef]
- Raez, L.; Danenberg, K.; Huang, E.; Usher, J.; Danenberg, P.; Sumarriva, D. P14. 04 cfRNA from Liquid Biopsies Is More Abundant Than cfDNA, Informs Treatment Outcome and Is Concordant with Tissue. J. Thorac. Oncol. 2021, 16, S330. [Google Scholar] [CrossRef]
- Marisa, L.; de Reyniès, A.; Duval, A.; Selves, J.; Gaub, M.P.; Vescovo, L.; Etienne-Grimaldi, M.-C.; Schiappa, R.; Guenot, D.; Ayadi, M.; et al. Gene expression classification of colon cancer into molecular subtypes: Characterization, validation, and prognostic value. PLoS Med. 2013, 10, e1001453. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vasioukhin, V.; Anker, P.; Maurice, P.; Lyautey, J.; Lederrey, C.; Stroun, M. Point mutations of the N-ras gene in the blood plasma DNA of patients with myelodysplastic syndrome or acute myelogenous leukaemia. Br. J. Haematol. 1994, 86, 774–779. [Google Scholar] [CrossRef] [PubMed]
- Sorenson, G.D.; Pribish, D.M.; Valone, F.H.; Memoli, V.A.; Bzik, D.J.; Yao, S.-L. Soluble normal and mutated DNA sequences from single-copy genes in human blood. Cancer Epidemiol. Prev. Biomark. 1994, 3, 67–71. [Google Scholar]
- Panagopoulou, M.; Karaglani, M.; Balgkouranidou, I.; Biziota, E.; Koukaki, T.; Karamitrousis, E.; Nena, E.; Tsamardinos, I.; Kolios, G.; Lianidou, E.; et al. Circulating cell-free DNA in breast cancer: Size profiling, levels, and methylation patterns lead to prognostic and predictive classifiers. Oncogene 2019, 38, 3387–3401. [Google Scholar] [CrossRef]
- Panagopoulou, M.; Esteller, M.; Chatzaki, E. Circulating Cell-Free DNA in Breast Cancer: Searching for Hidden Information towards Precision Medicine. Cancers 2021, 13, 728. [Google Scholar] [CrossRef]
- Rossi, G.; Mu, Z.; Rademaker, A.W.; Austin, L.K.; Strickland, K.S.; Costa, R.L.B.; Nagy, R.J.; Zagonel, V.; Taxter, T.J.; Behdad, A.; et al. Cell-Free DNA and Circulating Tumor Cells: Comprehensive Liquid Biopsy Analysis in Advanced Breast Cancer. Clin. Cancer. Res. 2018, 24, 560. [Google Scholar] [CrossRef] [Green Version]
- Ring, A.; Campo, D.; Porras, T.B.; Kaur, P.; Forte, V.A.; Tripathy, D.; Lu, J.; Kang, I.; Press, M.F.; Jeong, Y.J.; et al. Circulating Tumor Cell Transcriptomics as Biopsy Surrogates in Metastatic Breast Cancer. Ann. Surg. Oncol. 2022, 29, 2882–2894. [Google Scholar] [CrossRef]
- Klein, E.A.; Richards, D.; Cohn, A.; Tummala, M.; Lapham, R.; Cosgrove, D.; Chung, G.; Clement, J.; Gao, J.; Hunkapiller, N.; et al. Clinical validation of a targeted methylation-based multi-cancer early detection test using an independent validation set. Ann. Oncol. 2021, 32, 1167–1177. [Google Scholar] [CrossRef]
- Braicu, E.I.; du Bois, A.; Sehouli, J.; Beck, J.; Prader, S.; Kulbe, H.; Eiben, B.; Harter, P.; Traut, A.; Pietzner, K.; et al. Cell-Free-DNA-Based Copy Number Index Score in Epithelial Ovarian Cancer—Impact for Diagnosis and Treatment Monitoring. Cancers 2022, 14, 168. [Google Scholar] [CrossRef]
- Hannan, N.J.; Cohen, P.A.; Beard, S.; Bilic, S.; Zhang, B.; Tong, S.; Whitehead, C.; Hui, L. Transcriptomic analysis of patient plasma reveals circulating miR200c as a potential biomarker for high-grade serous ovarian cancer. Gynecol. Oncol. Rep. 2022, 39, 100894. [Google Scholar] [CrossRef]
- Hulstaert, E.; Levanon, K.; Morlion, A.; Van Aelst, S.; Christidis, A.-A.; Zamar, R.; Anckaert, J.; Verniers, K.; Bahar-Shany, K.; Sapoznik, S.; et al. RNA biomarkers from proximal liquid biopsy for diagnosis of ovarian cancer. Neoplasia 2022, 24, 155–164. [Google Scholar] [CrossRef] [PubMed]
- Powles, T.; Assaf, Z.J.; Davarpanah, N.; Banchereau, R.; Szabados, B.E.; Yuen, K.C.; Grivas, P.; Hussain, M.; Oudard, S.; Gschwend, J.E.; et al. ctDNA guiding adjuvant immunotherapy in urothelial carcinoma. Nature 2021, 595, 432–437. [Google Scholar] [CrossRef] [PubMed]
- Garcia, J.; Gauthier, A.; Lescuyer, G.; Barthelemy, D.; Geiguer, F.; Balandier, J.; Edelstein, D.L.; Jones, F.S.; Holtrup, F.; Duruisseau, M. Routine Molecular Screening of Patients with Advanced Non-SmallCell Lung Cancer in Circulating Cell-Free DNA at Diagnosis and During Progression Using OncoBEAM TM EGFR V2 and NGS Technologies. Mol. Diagn. Ther. 2021, 25, 239–250. [Google Scholar] [CrossRef] [PubMed]
- Pellini, B.; Chaudhuri, A.A. Circulating tumor DNA minimal residual disease detection of non–small-cell lung cancer treated with curative intent. J. Clin. Oncol. 2022, 40, 567–575. [Google Scholar] [CrossRef]
- Bunduc, S.; Gede, N.; Váncsa, S.; Lillik, V.; Kiss, S.; Dembrovszky, F.; Eross, B.; Szakács, Z.; Gheorghe, C.; Mikó, A. Prognostic role of cell-free DNA biomarkers in pancreatic adenocarcinoma: A systematic review and meta–analysis. Crit. Rev. Oncol. 2022, 169, 103548. [Google Scholar] [CrossRef]
- Kim, H.; Heo, C.M.; Oh, J.; Chung, H.H.; Lee, E.M.; Park, J.; Lee, S.-H.; Lee, K.H.; Lee, K.T.; Lee, J.K. Clinical significance of circulating tumor cells after chemotherapy in unresectable pancreatic ductal adenocarcinoma. Transl. Oncol. 2022, 16, 101321. [Google Scholar] [CrossRef]
- Bustamante, P.; Tsering, T.; Coblentz, J.; Mastromonaco, C.; Abdouh, M.; Fonseca, C.; Proença, R.P.; Blanchard, N.; Dugé, C.L.; Andujar, R.A.S. Circulating tumor DNA tracking through driver mutations as a liquid biopsy-based biomarker for uveal melanoma. J. Exp. Clin. Cancer Res. 2021, 40, 196. [Google Scholar] [CrossRef]
- Bobillo, S.; Crespo, M.; Escudero, L.; Mayor, R.; Raheja, P.; Carpio, C.; Rubio-Perez, C.; Tazón-Vega, B.; Palacio, C.; Carabia, J. Cell free circulating tumor DNA in cerebrospinal fluid detects and monitors central nervous system involvement of B-cell lymphomas. Haematologica 2021, 106, 513. [Google Scholar] [CrossRef] [Green Version]
- Salvianti, F.; Gelmini, S.; Mancini, I.; Pazzagli, M.; Pillozzi, S.; Giommoni, E.; Brugia, M.; Di Costanzo, F.; Galardi, F.; De Luca, F. Circulating tumour cells and cell-free DNA as a prognostic factor in metastatic colorectal cancer: The OMITERC prospective study. Br. J. Cancer 2021, 125, 94–100. [Google Scholar] [CrossRef]
- Ye, P.; Cai, P.; Xie, J.; Wei, Y. The diagnostic accuracy of digital PCR, ARMS and NGS for detecting KRAS mutation in cell-free DNA of patients with colorectal cancer: A systematic review and meta-analysis. PLoS ONE 2021, 16, e0248775. [Google Scholar] [CrossRef]
- Morris, V.K.; Strickler, J.H. Use of Circulating Cell-Free DNA to Guide Precision Medicine in Patients with Colorectal Cancer. Annu. Rev. Med. 2021, 72, 399–413. [Google Scholar] [CrossRef] [PubMed]
- Rizzo, A.; Ricci, A.D.; Tavolari, S.; Brandi, G. Circulating Tumor DNA in Biliary Tract Cancer: Current Evidence and Future Perspectives. Cancer Genom. Proteom. 2020, 17, 441–452. [Google Scholar] [CrossRef] [PubMed]
- Fernando, M.R.; Norton, S.E.; Luna, K.K.; Lechner, J.M.; Qin, J. Stabilization of cell-free RNA in blood samples using a new collection device. Clin. Biochem. 2012, 45, 1497–1502. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lo, K.-W.; Lo, Y.M.D.; Leung, S.-F.; Tsang, Y.-S.; Chan, L.Y.S.; Johnson, P.J.; Hjelm, N.M.; Lee, J.C.K.; Huang, D.P. Analysis of Cell-free Epstein-Barr Virus-associated RNA in the Plasma of Patients with Nasopharyngeal Carcinoma. Clin. Chem. 1999, 45, 1292–1294. [Google Scholar] [CrossRef] [PubMed]
- Larson, M.H.; Pan, W.; Kim, H.J.; Mauntz, R.E.; Stuart, S.M.; Pimentel, M.; Zhou, Y.; Knudsgaard, P.; Demas, V.; Aravanis, A.M.; et al. A comprehensive characterization of the cell-free transcriptome reveals tissue- and subtype-specific biomarkers for cancer detection. Nat. Commun. 2021, 12, 2357. [Google Scholar] [CrossRef]
- Roskams-Hieter, B.; Kim, H.J.; Anur, P.; Wagner, J.T.; Callahan, R.; Spiliotopoulos, E.; Kirschbaum, C.W.; Civitci, F.; Spellman, P.T.; Thompson, R.F.; et al. Plasma cell-free RNA profiling distinguishes cancers from pre-malignant conditions in solid and hematologic malignancies. NPJ Precis. Oncol. 2022, 6, 28. [Google Scholar] [CrossRef]
- Schwarzenbach, H. Clinical relevance of circulating, cell-free and exosomal microRNAs in plasma and serum of breast cancer patients. Oncol. Res. Treat. 2017, 40, 423–429. [Google Scholar] [CrossRef]
- Molnár, B.; Galamb, O.; Kalmár, A.; Barták, B.K.; Nagy, Z.B.; Tóth, K.; Tulassay, Z.; Igaz, P.; Dank, M. Circulating cell-free nucleic acids as biomarkers in colorectal cancer screening and diagnosis-an update. Expert Rev. Mol. Diagn. 2019, 19, 477–498. [Google Scholar] [CrossRef]
- Hasegawa, N.; Kohsaka, S.; Kurokawa, K.; Shinno, Y.; Nakamura, I.T.; Ueno, T.; Kojima, S.; Kawazu, M.; Suehara, Y.; Ishijima, M. Highly sensitive fusion detection using plasma cell-free RNA in non-small-cell lung cancers. Cancer Sci. 2021, 112, 4393. [Google Scholar] [CrossRef]
- Savino, M.; Parrella, P.; Copetti, M.; Barbano, R.; Murgo, R.; Fazio, V.M.; Valori, V.M.; Carella, M.; Garrubba, M.; Santini, S.A. Comparison between real-time quantitative PCR detection of HER2 mRNA copy number in peripheral blood and ELISA of serum HER2 protein for determining HER2 status in breast cancer patients. Cell. Oncol. Off. J. Int. Soc. Cell. Oncol. 2009, 31, 203–211. [Google Scholar] [CrossRef]
- Zhang, R.; Chen, B.; Tong, X.; Wang, Y.; Wang, C.; Jin, J.; Tian, P.; Li, W. Diagnostic accuracy of droplet digital PCR for detection of EGFR T790M mutation in circulating tumor DNA. Cancer Manag. Res. 2018, 10, 1209–1218. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Newman, A.M.; Bratman, S.V.; To, J.; Wynne, J.F.; Eclov, N.C.; Modlin, L.A.; Liu, C.L.; Neal, J.W.; Wakelee, H.A.; Merritt, R.E.; et al. An ultrasensitive method for quantitating circulating tumor DNA with broad patient coverage. Nat. Med. 2014, 20, 548–554. [Google Scholar] [CrossRef] [PubMed]
- Chaudhuri, A.A.; Chabon, J.J.; Lovejoy, A.F.; Newman, A.M.; Stehr, H.; Azad, T.D.; Khodadoust, M.S.; Esfahani, M.S.; Liu, C.L.; Zhou, L.; et al. Early Detection of Molecular Residual Disease in Localized Lung Cancer by Circulating Tumor DNA Profiling. Cancer Discov. 2017, 7, 1394–1403. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zviran, A.; Schulman, R.C.; Shah, M.; Hill, S.T.K.; Deochand, S.; Khamnei, C.C.; Maloney, D.; Patel, K.; Liao, W.; Widman, A.J.; et al. Genome-wide cell-free DNA mutational integration enables ultra-sensitive cancer monitoring. Nat. Med. 2020, 26, 1114–1124. [Google Scholar] [CrossRef]
- Roepman, P.; de Bruijn, E.; van Lieshout, S.; Schoenmaker, L.; Boelens, M.C.; Dubbink, H.J.; Geurts-Giele, W.R.; Groenendijk, F.H.; Huibers, M.M.; Kranendonk, M.E.; et al. Clinical validation of Whole Genome Sequencing for routine cancer diagnostics. J. Mol. Diagn. 2020, 23, 816–833. [Google Scholar] [CrossRef]
- Forshew, T.; Murtaza, M.; Parkinson, C.; Gale, D.; Tsui, D.W.; Kaper, F.; Dawson, S.-J.; Piskorz, A.M.; Jimenez-Linan, M.; Bentley, D. Noninvasive identification and monitoring of cancer mutations by targeted deep sequencing of plasma DNA. Sci. Transl. Med. 2012, 4, 136ra68. [Google Scholar] [CrossRef]
- Bohers, E.; Viailly, P.-J.; Jardin, F. cfDNA Sequencing: Technological Approaches and Bioinformatic Issues. Pharmaceuticals 2021, 14, 596. [Google Scholar] [CrossRef]
- Bos, M.K.; Angus, L.; Nasserinejad, K.; Jager, A.; Jansen, M.P.H.M.; Martens, J.W.M.; Sleijfer, S. Whole exome sequencing of cell-free DNA—A systematic review and Bayesian individual patient data meta-analysis. Cancer Treat. Rev. 2020, 83, 101951. [Google Scholar] [CrossRef] [Green Version]
- Rennert, H.; Eng, K.; Zhang, T.; Tan, A.; Xiang, J.; Romanel, A.; Kim, R.; Tam, W.; Liu, Y.-C.; Bhinder, B.; et al. Development and validation of a whole-exome sequencing test for simultaneous detection of point mutations, indels and copy-number alterations for precision cancer care. NPJ Genom. Med. 2016, 1, 16019. [Google Scholar] [CrossRef]
- Oxnard, G.R.; Klein, E.A.; Seiden, M.; Hubbell, E.; Venn, O.; Jamshidi, A.; Zhang, N.; Beausang, J.F.; Gross, S.; Kurtzman, K.N.; et al. Simultaneous multi-cancer detection and tissue of origin (TOO) localization using targeted bisulfite sequencing of plasma cell-free DNA (cfDNA). J. Glob. Oncol. 2019, 5, 44. [Google Scholar] [CrossRef]
- Paun, O.; Verhoeven, K.J.F.; Richards, C.L. Opportunities and limitations of reduced representation bisulfite sequencing in plant ecological epigenomics. New Phytol. 2019, 221, 738–742. [Google Scholar] [CrossRef] [Green Version]
- Aravanis, A.M.; Lee, M.; Klausner, R.D. Next-Generation Sequencing of Circulating Tumor DNA for Early Cancer Detection. Cell 2017, 168, 571–574. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Phallen, J.; Sausen, M.; Adleff, V.; Leal, A.; Hruban, C.; White, J.; Anagnostou, V.; Fiksel, J.; Cristiano, S.; Papp, E.; et al. Direct detection of early-stage cancers using circulating tumor DNA. Sci. Transl. Med. 2017, 9, eaan2415. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Xu, X.; Yu, Y.; Shen, M.; Liu, M.; Wu, S.; Liang, L.; Huang, F.; Zhang, C.; Guo, W.; Liu, T. Role of circulating free DNA in evaluating clinical tumor burden and predicting survival in Chinese metastatic colorectal cancer patients. BMC Cancer 2020, 20, 1006. [Google Scholar] [CrossRef] [PubMed]
- Valpione, S.; Gremel, G.; Mundra, P.; Middlehurst, P.; Galvani, E.; Girotti, M.R.; Lee, R.J.; Garner, G.; Dhomen, N.; Lorigan, P.C.; et al. Plasma total cell-free DNA (cfDNA) is a surrogate biomarker for tumour burden and a prognostic biomarker for survival in metastatic melanoma patients. Eur. J. Cancer 2018, 88, 1–9. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nygaard, A.D.; Holdgaard, P.C.; Spindler, K.L.G.; Pallisgaard, N.; Jakobsen, A. The correlation between cell-free DNA and tumour burden was estimated by PET/CT in patients with advanced NSCLC. Br. J. Cancer 2014, 110, 363–368. [Google Scholar] [CrossRef] [Green Version]
- Liu, J.; Chen, X.; Wang, J.; Zhou, S.; Wang, C.L.; Ye, M.Z.; Wang, X.Y.; Song, Y.; Wang, Y.Q.; Zhang, L.T.; et al. Biological background of the genomic variations of cf-DNA in healthy individuals. Ann. Oncol. 2019, 30, 464–470. [Google Scholar] [CrossRef] [Green Version]
- Razavi, P.; Li, B.T.; Brown, D.N.; Jung, B.; Hubbell, E.; Shen, R.; Abida, W.; Juluru, K.; De Bruijn, I.; Hou, C.; et al. High-intensity sequencing reveals the sources of plasma circulating cell-free DNA variants. Nat. Med. 2019, 25, 1928–1937. [Google Scholar] [CrossRef]
- Fernandez-Garcia, D.; Hills, A.; Page, K.; Hastings, R.K.; Toghill, B.; Goddard, K.S.; Ion, C.; Ogle, O.; Boydell, A.R.; Gleason, K.; et al. Plasma cell-free DNA (cfDNA) as a predictive and prognostic marker in patients with metastatic breast cancer. Breast Cancer Res. 2019, 21, 149. [Google Scholar] [CrossRef]
- Liu, H.; Gao, Y.; Vafaei, S.; Gu, X.; Zhong, X. The Prognostic Value of Plasma Cell-Free DNA Concentration in the Prostate Cancer: A Systematic Review and Meta-Analysis. Front. Oncol. 2021, 11, 599602. [Google Scholar] [CrossRef]
- Basnet, S.; Zhang, Z.-Y.; Liao, W.-Q.; Li, S.-H.; Li, P.-S.; Ge, H.-Y. The Prognostic Value of Circulating Cell-Free DNA in Colorectal Cancer: A Meta-Analysis. J. Cancer 2016, 7, 1105–1113. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- No, J.H.; Kim, K.; Park, K.H.; Kim, Y.-B. Cell-free DNA Level as a Prognostic Biomarker for Epithelial Ovarian Cancer. Anticancer Res. 2012, 32, 3467. [Google Scholar] [PubMed]
- Bortolin, M.T.; Tedeschi, R.; Bidoli, E.; Furlan, C.; Basaglia, G.; Minatel, E.; Gobitti, C.; Franchin, G.; Trovò, M.; De Paoli, P. Cell-free DNA as a prognostic marker in stage I non-small-cell lung cancer patients undergoing stereotactic body radiotherapy. Biomarkers 2015, 20, 422–428. [Google Scholar] [CrossRef] [PubMed]
- Ibarra, A.; Zhuang, J.; Zhao, Y.; Salathia, N.; Huang, V.; Acosta, A.; Aballi, J.; Toden, S.; Karns, A.; Purnajo, I.; et al. Non-invasive characterization of human bone marrow stimulation and reconstitution by cell-free messenger RNA sequencing. Nat. Commun. 2020, 11, 400. [Google Scholar] [CrossRef] [Green Version]
- Guan, S.; Lu, Y. Dissecting organ-specific transcriptomes through RNA-sequencing. Plant Methods 2013, 9, 42. [Google Scholar] [CrossRef] [Green Version]
- Camunas-Soler, J.; Gee, E.P.S.; Reddy, M.; Mi, J.D.; Thao, M.; Brundage, T.; Siddiqui, F.; Hezelgrave, N.L.; Shennan, A.H.; Namsaraev, E.; et al. Predictive RNA profiles for early and very early spontaneous preterm birth. Am. J. Obstet. Gynecol. 2022, 227, 72.e1–72.e16. [Google Scholar] [CrossRef]
- Pucciarelli, S.; Rampazzo, E.; Briarava, M.; Maretto, I.; Agostini, M.; Digito, M.; Keppel, S.; Friso, M.L.; Lonardi, S.; De Paoli, A.; et al. Telomere-Specific Reverse Transcriptase (hTERT) and Cell-free RNA in Plasma as Predictors of Pathologic Tumor Response in Rectal Cancer Patients Receiving Neoadjuvant Chemoradiotherapy. Ann. Surg. Oncol. 2012, 19, 3089–3096. [Google Scholar] [CrossRef]
- Zaporozhchenko, I.A.; Ponomaryova, A.A.; Rykova, E.Y.; Laktionov, P.P. The potential of circulating cell-free RNA as a cancer biomarker: Challenges and opportunities. Expert Rev. Mol. Diagn. 2018, 18, 133–145. [Google Scholar] [CrossRef]
- Wang, W.; Lou, W.; Ding, B.; Yang, B.; Lu, H.; Kong, Q.; Fan, W. A novel mRNA-miRNA-lncRNA competing endogenous RNA triple sub-network associated with prognosis of pancreatic cancer. Aging 2019, 11, 2610. [Google Scholar] [CrossRef]
- López-Urrutia, E.; Bustamante Montes, L.P.; Ladrón de Guevara Cervantes, D.; Pérez-Plasencia, C.; Campos-Parra, A.D. Crosstalk between long non-coding RNAs, micro-RNAs and mRNAs: Deciphering molecular mechanisms of master regulators in cancer. Front. Oncol. 2019, 9, 669. [Google Scholar] [CrossRef]
- Abbosh, C.; Birkbak, N.J.; Wilson, G.A.; Jamal-Hanjani, M.; Constantin, T.; Salari, R.; Le Quesne, J.; Moore, D.A.; Veeriah, S.; Rosenthal, R.; et al. Phylogenetic ctDNA analysis depicts early-stage lung cancer evolution. Nature 2017, 545, 446–451. [Google Scholar] [CrossRef] [PubMed]
- Leal, A.; van Grieken, N.C.T.; Palsgrove, D.N.; Phallen, J.; Medina, J.E.; Hruban, C.; Broeckaert, M.A.M.; Anagnostou, V.; Adleff, V.; Bruhm, D.C.; et al. White blood cell and cell-free DNA analyses for detection of residual disease in gastric cancer. Nat. Commun. 2020, 11, 525. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Garcia-Murillas, I.; Schiavon, G.; Weigelt, B.; Ng, C.; Hrebien, S.; Cutts, R.J.; Cheang, M.; Osin, P.; Nerurkar, A.; Kozarewa, I.; et al. Mutation tracking in circulating tumor DNA predicts relapse in early breast cancer. Sci. Transl. Med. 2015, 7, 302ra133. [Google Scholar] [CrossRef]
- Del Giudice, I.; Raponi, S.; Della Starza, I.; De Propris, M.S.; Cavalli, M.; De Novi, L.A.; Cappelli, L.V.; Ilari, C.; Cafforio, L.; Guarini, A.; et al. Minimal Residual Disease in Chronic Lymphocytic Leukemia: A New Goal? Front. Oncol. 2019, 9, 689. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rossi, G.; Minervini, M.M.; Carella, A.M.; de Waure, C.; di Nardo, F.; Melillo, L.; D’Arena, G.; Zini, G.; Cascavilla, N. Comparison between multiparameter flow cytometry and WT1-RNA quantification in monitoring minimal residual disease in acute myeloid leukemia without specific molecular targets. Leuk. Res. 2012, 36, 401–406. [Google Scholar] [CrossRef] [PubMed]
- Pascual, J.; Cutts, R.J.; Kingston, B.; Hrebien, S.; Kilburn, L.S.; Kernaghan, S.; Moretti, L.; Wilkinson, K.; Wardley, A.M.; Macpherson, I.R.; et al. Assessment of early ctDNA dynamics to predict efficacy of targeted therapies in metastatic breast cancer: Results from plasmaMATCH trial. Cancer Res. 2021, 81, PS5-02. [Google Scholar] [CrossRef]
- Higgins, M.J.; Jelovac, D.; Barnathan, E.; Blair, B.; Slater, S.; Powers, P.; Zorzi, J.; Jeter, S.C.; Oliver, G.R.; Fetting, J.; et al. Detection of tumor PIK3CA status in metastatic breast cancer using peripheral blood. Clin. Cancer. Res. 2012, 18, 3462–3469. [Google Scholar] [CrossRef] [Green Version]
- Li, Y.; Lv, J.; Wan, S.; Xin, J.; Xie, T.; Li, T.; Zhu, W.; Zhang, G.; Wang, Y.; Tang, Y.; et al. High Sensitive and Non-invasive ctDNAs Sequencing Facilitate Clinical Diagnosis And Clinical Guidance of Non-small Cell Lung Cancer Patient: A Time Course Study. Front. Oncol. 2018, 8, 491. [Google Scholar] [CrossRef]
- Chen, K.Z.; Lou, F.; Yang, F.; Zhang, J.B.; Ye, H.; Chen, W.; Guan, T.; Zhao, M.Y.; Su, X.X.; Shi, R.; et al. Circulating Tumor DNA Detection in Early-Stage Non-Small Cell Lung Cancer Patients by Targeted Sequencing. Sci. Rep. 2016, 6, 31985. [Google Scholar] [CrossRef] [Green Version]
- Lee, J.Y.; Qing, X.; Xiumin, W.; Yali, B.; Chi, S.; Bak, S.H.; Lee, H.Y.; Sun, J.M.; Lee, S.H.; Ahn, J.S.; et al. Longitudinal monitoring of EGFR mutations in plasma predicts outcomes of NSCLC patients treated with EGFR TKIs: Korean Lung Cancer Consortium (KLCC-12-02). Oncotarget 2016, 7, 6984–6993. [Google Scholar] [CrossRef] [Green Version]
- Kutilin, D.S.; Airapetova, T.G.; Anistratov, P.A.; Pyltsin, S.P.; Leiman, I.A.; Karnaukhov, N.S.; Kit, O.I. Copy Number Variation in Tumor Cells and Extracellular DNA in Patients with Lung Adenocarcinoma. Bull. Exp. Biol. Med. 2019, 167, 771–778. [Google Scholar] [CrossRef] [PubMed]
- Peng, H.; Lu, L.; Zhou, Z.; Liu, J.; Zhang, D.; Nan, K.; Zhao, X.; Li, F.; Tian, L.; Dong, H.; et al. CNV Detection from Circulating Tumor DNA in Late Stage Non-Small Cell Lung Cancer Patients. Genes 2019, 10, 926. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sozzi, G.; Conte, D.; Leon, M.; Cirincione, R.; Roz, L.; Ratcliffe, C.; Roz, E.; Cirenei, N.; Bellomi, M.; Pelosi, G. Quantification of free circulating DNA as a diagnostic marker in lung cancer. J. Clin. Oncol. 2003, 21, 3902–3908. [Google Scholar] [CrossRef] [PubMed]
- Naidoo, M.; Gibbs, P.; Tie, J. ctDNA and Adjuvant Therapy for Colorectal Cancer: Time to Re-Invent Our Treatment Paradigm. Cancers 2021, 13, 346. [Google Scholar] [CrossRef]
- Chen, G.; Peng, J.; Xiao, Q.; Wu, H.-X.; Wu, X.; Wang, F.; Li, L.; Ding, P.; Zhao, Q.; Li, Y.; et al. Postoperative circulating tumor DNA as markers of recurrence risk in stages II to III colorectal cancer. J. Hematol. Oncol. 2021, 14, 80. [Google Scholar] [CrossRef]
- Wang, Y.; Yang, L.; Bao, H.; Fan, X.; Xia, F.; Wan, J.; Shen, L.; Guan, Y.; Bao, H.; Wu, X. Utility of ctDNA in predicting response to neoadjuvant chemoradiotherapy and prognosis assessment in locally advanced rectal cancer: A prospective cohort study. PLoS Med. 2021, 18, e1003741. [Google Scholar] [CrossRef]
- Osumi, H.; Shinozaki, E.; Yamaguchi, K. Circulating tumor DNA as a novel biomarker optimizing chemotherapy for colorectal cancer. Cancers 2020, 12, 1566. [Google Scholar] [CrossRef]
- Tan, L.; Sandhu, S.; Lee, R.J.; Li, J.; Callahan, J.; Ftouni, S.; Dhomen, N.; Middlehurst, P.; Wallace, A.; Raleigh, J.; et al. Prediction and monitoring of relapse in stage III melanoma using circulating tumor DNA. Ann. Oncol. 2019, 30, 804–814. [Google Scholar] [CrossRef]
- Seremet, T.; Jansen, Y.; Planken, S.; Njimi, H.; Delaunoy, M.; El Housni, H.; Awada, G.; Schwarze, J.K.; Keyaerts, M.; Everaert, H.; et al. Undetectable circulating tumor DNA (ctDNA) levels correlate with favorable outcome in metastatic melanoma patients treated with anti-PD1 therapy. J. Transl. Med. 2019, 17, 303. [Google Scholar] [CrossRef] [Green Version]
- Arshad, J.; Barreto-Coelho, P.; Jonczak, E.; Espejo, A.; D’Amato, G.; Trent, J.C. Identification of Genetic Alterations by Circulating Tumor DNA in Leiomyosarcoma: A Molecular Analysis of 73 Patients. J. Immunother. Precis. Oncol. 2020, 3, 64–68. [Google Scholar] [CrossRef]
- Krebs, M.; Dive, C.; Dean, E.J.; Rothwell, D.G.; Brognard, J.; Wallace, A.; Miller, C.; Cook, N.; Rafii, S.; Ayub, M.; et al. TARGET trial: Molecular profiling of circulating tumour DNA to stratify patients to early phase clinical trials. J. Clin. Oncol. 2016, 34, TPS11614. [Google Scholar] [CrossRef]
- Yardley, D.A. MONALEESA clinical program: A review of ribociclib use in different clinical settings. Future Oncol. 2019, 15, 2673–2686. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sicklick, J.K.; Kato, S.; Okamura, R.; Schwaederle, M.; Hahn, M.E.; Williams, C.B.; De, P.; Krie, A.; Piccioni, D.E.; Miller, V.A.; et al. Molecular profiling of cancer patients enables personalized combination therapy: The I-PREDICT study. Nat. Med. 2019, 25, 744–750. [Google Scholar] [CrossRef] [PubMed]
- Kwan, E.M.; Spain, L.; Anton, A.; Gan, C.L.; Garrett, L.; Chang, D.; Liow, E.; Bennett, C.; Zheng, T.; Yu, J.; et al. Avelumab Combined with Stereotactic Ablative Body Radiotherapy in Metastatic Castration-resistant Prostate Cancer: The Phase 2 ICE-PAC Clinical Trial. Eur. Urol. 2022, 81, 253–262. [Google Scholar] [CrossRef]
- Grussie, E.; Danenberg, G.; Kollengode, K.A.; Danenberg, K.; Rabizadeh, S.; Huang, E.; Usher, J.L.; Danenberg, P.V.; Pinski, J.K. Gene expression differences in cell-free RNA between prostate cancer patients and healthy individuals. J. Clin. Oncol. 2018, 36, e17077. [Google Scholar] [CrossRef]
- Huang, C.-Y.A.; Warren, S.; Reeves, J.; Wurden, M.; Riordan, T.; Boykin, R.; Liu, M.; Henderson, D.; Hanson, D.; Gerlach, J. Profiling plasma cell-free RNA (cfRNA) with the NanoString low input nCounter assay. In Proceedings of the AACR Annual Meeting, Atlanta, GA, USA, 29 March–3 April 2019; Volume 79, p. 406. [Google Scholar]
- Durand, X.; Moutereau, S.; Xylinas, E.; de la Taille, A. Progensa™ PCA3 test for prostate cancer. Expert Rev. Mol. Diagn. 2011, 11, 137–144. [Google Scholar] [CrossRef]
- Sasamori, H.; Uno, K.; Wu, J. Usefulness of both PET/CT with F18-FDG and whole-body diffusion-weighted imaging in cancer screening: A preliminary report. Ann. Nucl. Med. 2019, 33, 78–85. [Google Scholar] [CrossRef]
- Lennon, A.M.; Buchanan, A.H.; Kinde, I.; Warren, A.; Honushefsky, A.; Cohain, A.T.; Ledbetter, D.H.; Sanfilippo, F.; Sheridan, K.; Rosica, D.; et al. Feasibility of blood testing combined with PET-CT to screen for cancer and guide intervention. Science 2020, 369, eabb9601. [Google Scholar] [CrossRef]
- Kwee, S.; Song, M.-A.; Cheng, I.; Loo, L.; Tiirikainen, M. Measurement of Circulating Cell-Free DNA in Relation to 18F-Fluorocholine PET/CT Imaging in Chemotherapy-Treated Advanced Prostate Cancer. Clin. Transl. Sci. 2012, 5, 65–70. [Google Scholar] [CrossRef] [Green Version]
- Woff, E.; Kehagias, P.; Vandeputte, C.; Ameye, L.; Guiot, T.; Paesmans, M.; Hendlisz, A.; Flamen, P. Combining 18F-FDG PET/CT—Based Metabolically Active Tumor Volume and Circulating Cell-Free DNA Significantly Improves Outcome Prediction in Chemorefractory Metastatic Colorectal Cancer. J. Nucl. Med. 2019, 60, 1366–1372. [Google Scholar] [CrossRef] [Green Version]
- Sun, K.; Wang, J.; Wang, H.; Sun, H. GeneCT: A generalizable cancerous status and tissue origin classifier for pan-cancer biopsies. Bioinformatics 2018, 34, 4129–4130. [Google Scholar] [CrossRef] [PubMed]

| Sr number | Properties | Circulating Tumor DNA | Cell-Free Fetal DNA | Cell-Free Mitochondrial DNA |
|---|---|---|---|---|
| 1 | Strands | Single or double | Single or double | Double |
| 2 | Origin | Tumor cells | Trophoblastic cells [13] | Mitochondria or unknown [17] |
| 3 | Size | Less than 100 bp [18] | 200 bp with dominate peaks at 162 bp [19] | Shorter fragment = less than 1 kb; larger fragments = 21 kb [14] |
| 4 | Applications | Early cancer detection, mutation analysis, cancer prediction, noninvasive cancer detection | Prenatal testing, genetic disease detection in the fetus | Forensic sciences, detection of the geographical distribution of genes, gene flow identification, human remain recognition, cancer detection |
| 5 | Advantages | Sensitive than other cancer detection techniques, can detect mutations better than biopsy, detect heterogeneous tumor cells, predict cancer reoccurrence | Increased chances to detect chromosomal disorders, noninvasive, no side effects | Lacks genetic ambiguities, higher copy number, a diagnostic and prognostic marker for multiple diseases |
| 6 | Disadvantages | Cannot be detected by FISH or ICC techniques, expensive, lack standardization | Increased chances of false positives or false negatives | No heterogenicity, lower discrimination power |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hassan, S.; Shehzad, A.; Khan, S.A.; Miran, W.; Khan, S.; Lee, Y.-S. Diagnostic and Therapeutic Potential of Circulating-Free DNA and Cell-Free RNA in Cancer Management. Biomedicines 2022, 10, 2047. https://doi.org/10.3390/biomedicines10082047
Hassan S, Shehzad A, Khan SA, Miran W, Khan S, Lee Y-S. Diagnostic and Therapeutic Potential of Circulating-Free DNA and Cell-Free RNA in Cancer Management. Biomedicines. 2022; 10(8):2047. https://doi.org/10.3390/biomedicines10082047
Chicago/Turabian StyleHassan, Sadia, Adeeb Shehzad, Shahid Ali Khan, Waheed Miran, Salman Khan, and Young-Sup Lee. 2022. "Diagnostic and Therapeutic Potential of Circulating-Free DNA and Cell-Free RNA in Cancer Management" Biomedicines 10, no. 8: 2047. https://doi.org/10.3390/biomedicines10082047
APA StyleHassan, S., Shehzad, A., Khan, S. A., Miran, W., Khan, S., & Lee, Y.-S. (2022). Diagnostic and Therapeutic Potential of Circulating-Free DNA and Cell-Free RNA in Cancer Management. Biomedicines, 10(8), 2047. https://doi.org/10.3390/biomedicines10082047







