Epigenetic Studies for Evaluation of NPS Toxicity: Focus on Synthetic Cannabinoids and Cathinones
Abstract
1. Introduction
Search Strategy
2. Epigenetic Changes
2.1. Histones Modification
2.2. DNA Methylation
2.3. Non-Coding RNA
3. Addiction and Epigenetic Mechanisms Related to Drugs of Abuse
4. Overview of Epigenetic Factors and Their Clinical-Toxicological Use
Epigenetic Inheritance
5. New Perspectives in the Forensic Field
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
Abbreviations
| NPS | Novel Psychoactive Substance |
| DMEs | Drug-metabolizing enzymes |
| ncRNA | Non-coding RNA |
| CpG | Cytosine–phosphate–guanine |
| miRNA | Micro-RNA |
| ROS | Reactive Oxygen Species |
| HAT | Acetyltransferases catalyse acetylation |
| HDAC | Acetyltransferases catalyse deacetylases |
| HMT | Methyltransferases catalyze methylation |
| HDM | Methyltransferases catalyze demethylation |
| 5-mc | 5-methylCytosine |
| lncRNA | Long non-coding RNA |
| sncRNA | Small non-coding RNA |
| pi-RNA | P-element induced Wimpy testis (PIWI)-interacting RNA |
| sRNA | Short interfering RNA |
| circRNA | Circular RNA |
| NAc | Nucleus accumbens |
| MDMA | 3,4-methylenedioxymethamphetamine |
| Δ9-THC | Δ9-tetrahydrocannabinol |
| CBD | Cannabidiol |
References
- Roman-Urrestarazu, A.; Robertson, R.; Yang, J. European Monitoring Centre for Drugs and Drug Addiction, European drug report 2018: Trends and developments. Bmj 2018, 362. [Google Scholar]
- Luethi, D.; Liechti, M.E. Designer drugs: Mechanism of action and adverse effects. Arch. Toxicol. 2020, 94, 1085–1133. [Google Scholar] [CrossRef]
- EMCDDA European Monitoring Centre for Drugs and Drug Addiction. European Drug Report 2020: Trends and Devel-Opments; Publications Office of the European Union: Lisbon, Portugal, 2020. [Google Scholar]
- United Nations Office on Drugs and Labor. World Drug Report 2020; United Nations: Vienna, Austria, 2021. [Google Scholar]
- Simmler, L.D.; Rickli, A.; Schramm, Y.; Hoener, M.C.; Liechti, M.E. Pharmacological profiles of aminoindanes, piperazines, and pipradrol derivatives. Biochem. Pharmacol. 2014, 88, 237–244. [Google Scholar] [CrossRef]
- Simmler, L.; Buser, T.; Donzelli, M.; Schramm, Y.; Dieu, L.-H.; Huwyler, J.; Chaboz, S.; Hoener, M.; Liechti, M. Pharmacological characterization of designer cathinones in vitro Br. J. Pharmacol. 2013, 168, 458–470. [Google Scholar] [CrossRef]
- Bilel, S.; Neto, J.A.; Arfè, R.; Tirri, M.; Gaudio, R.M.; Fantinati, A.; Bernardi, T.; Boccuto, F.; Marchetti, B.; Corli, G.; et al. In vitro and in vivo pharmaco-dynamic study of the novel fentanyl derivatives: Acrylfentanyl, Ocfentanyl and Furanylfentanyl. Neuropharmacology 2022, 209, 109020. [Google Scholar] [CrossRef]
- EMCDDA European Monitoring Centre for Drugs and Drug Addiction. European Drug Report 2021: Trends and Devel-Opments; Publications Office of the European Union: Lisbon, Portugal, 2021. [Google Scholar]
- ESPAD Report 2019. Available online: http://espad.org/sites/espad.org/files/2020.3878_EN_04.pdf (accessed on 15 November 2021).
- Patrick, M.E.; O’Malley, P.; Kloska, D.D.; Schulenberg, J.; Johnston, L.; Miech, R.; Bachman, J.G. Novel psychoactive substance use by US adolescents: Characteristics associated with use of synthetic cannabinoids and synthetic cathinones. Drug Alcohol Rev. 2015, 35, 586–590. [Google Scholar] [CrossRef]
- Hill, S.L.; Dunn, M.; Cano, C.; Harnor, S.J.; Hardcastle, I.R.; Grundlingh, J.; Dargan, P.I.; Wood, D.M.; Tucker, S.; Bartram, T.; et al. Human Toxicity Caused by Indole and Indazole Carboxylate Synthetic Cannabinoid Receptor Agonists: From Horizon Scanning to Notification. Clin. Chem. 2018, 64, 346–354. [Google Scholar] [CrossRef]
- Klavž, J.; Gorenjak, M.; Marinšek, M. Suicide attempt with a mix of synthetic cannabinoids and synthetic cathinones: Case report of non-fatal intoxication with AB-CHMINACA, AB-FUBINACA, alpha-PHP, alpha-PVP and 4-CMC. Forensic Sci. Int. 2016, 265, 121–124. [Google Scholar] [CrossRef]
- Fujita, Y.; Mita, T.; Usui, K.; Kamijo, Y.; Kikuchi, S.; Onodera, M.; Fujino, Y.; Inoue, Y. Toxicokinetics of the Synthetic Cathinone α-Pyrrolidinohexanophenone. J. Anal. Toxicol. 2018, 42, e1–e5. [Google Scholar] [CrossRef]
- Dragogna, F.; Oldani, L.; Buoli, M.; Altamura, A.C. A case of severe psychosis induced by novel recreational drugs. F1000Research 2014, 3, 21. [Google Scholar] [CrossRef]
- Angerer, V.; Jacobi, S.; Franz, F.; Auwärter, V.; Pietsch, J. Three fatalities associated with the synthetic cannabinoids 5F-ADB, 5F-PB-22, and AB-CHMINACA. Forensic Sci. Int. 2017, 281, e9–e15. [Google Scholar] [CrossRef]
- Schep, L.J.; Slaughter, R.; Hudson, S.; Place, R.; Watts, M. Delayed seizure-like activity following analytically confirmed use of previously unreported synthetic cannabinoid analogues. Hum. Exp. Toxicol. 2015, 34, 557–560. [Google Scholar] [CrossRef]
- Levine, M.; Levitan, R.; Skolnik, A. Compartment Syndrome After “Bath Salts” Use: A Case Series. Ann. Emerg. Med. 2013, 61, 480–483. [Google Scholar] [CrossRef]
- Adamowicz, P.; Hydzik, P. Fetal death associated with the use of 3,4-MDPHP and α-PHP. Clin. Toxicol. 2019, 57, 112–116. [Google Scholar] [CrossRef]
- Nicholson, P.J.; Quinn, M.J.; Dodd, J.D. Headshop heartache: Acute mephedrone ‘meow’ myocarditis. Heart 2010, 96, 2051–2052. [Google Scholar] [CrossRef]
- James, D.; Adams, R.D.; Spears, R.; Cooper, G.; Lupton, D.J.; Thompson, J.P.; Thomas, S.H.L. Clinical characteristics of mephedrone toxicity reported to the U.K. National Poisons Information Service. Emerg. Med. J. 2011, 28, 686–689. [Google Scholar] [CrossRef]
- Castaneto, M.S.; Gorelick, D.A.; Desrosiers, N.A.; Hartman, R.L.; Pirard, S.; Huestis, M.A. Synthetic cannabinoids: Epidemiology, pharmacodynamics, and clinical implications. Drug Alcohol Depend. 2014, 144, 12–41. [Google Scholar] [CrossRef] [PubMed]
- O’Sullivan, S.E. Endocannabinoids and the Cardiovascular System in Health and Disease. Handb. Exp. Pharmacol. 2015, 231, 393–422. [Google Scholar] [CrossRef] [PubMed]
- Kumar, P.; Zaleta, S.; Miller, S. Chest pain, troponin rise, and ST-elevation in an adolescent boy following the use of the synthetic cannabis product K2. Ann. Pediatr. Cardiol. 2016, 9, 79–81. [Google Scholar] [CrossRef]
- Pacher, P. Cannabinoid CB 1 Receptor Antagonists for Atherosclerosis and Cardiometabolic Disorders. Arter. Thromb. Vasc. Biol. 2009, 29, 7–9. [Google Scholar] [CrossRef]
- Le Boisselier, R.; Alexandre, J.; Lelong-Boulouard, V.; Debruyne, D. Focus on cannabinoids and synthetic cannabinoids. Clin. Pharmacol. Ther. 2017, 101, 220–229. [Google Scholar] [CrossRef] [PubMed]
- Pacher, P.; Steffens, S.; Haskó, G.; Schindler, T.H.; Kunos, G. Cardiovascular effects of marijuana and synthetic cannabinoids: The good, the bad, and the ugly. Nat. Rev. Cardiol. 2018, 15, 151–166. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention (CDC). Acute kidney injury associated with synthetic cannabinoid use—Multiple states, 2012. MMWR Morb. Mortal. Wkly. Rep. 2013, 62, 93–98. [Google Scholar]
- Camuto, C.; Guglielmelli, A.; De-Giorgio, F.; de la Torre, X.; Mazzarino, M.; Marti, M.; Botrè, F. In vitro metabolic profile of mexedrone, a mephedrone analog, studied by high- and low-resolution mass spectrometry. Drug Test. Anal. 2022, 14, 269–276. [Google Scholar] [CrossRef] [PubMed]
- Bilel, S.; Tirri, M.; Arfè, R.; Sturaro, C.; Fantinati, A.; Cristofori, V.; Bernardi, T.; Boccuto, F.; Cavallo, M.; Cavalli, A.; et al. In Vitro and In Vivo Pharmaco-Toxicological Characterization of 1-Cyclohexyl-x-methoxybenzene Derivatives in Mice: Comparison with Tramadol and PCP. Int. J. Mol. Sci. 2021, 22, 7659. [Google Scholar] [CrossRef]
- Arfè, R.; Bilel, S.; Tirri, M.; Frisoni, P.; Serpelloni, G.; Neri, M.; Boccuto, F.; Bernardi, T.; Foti, F.; De-Giorgio, F.; et al. Comparison of N-methyl-2-pyrrolidone (NMP) and the “date rape” drug GHB: Behavioral toxicology in the mouse model. Psychopharmacology 2021, 238, 2275–2295. [Google Scholar] [CrossRef]
- Foti, F.; Bilel, S.; Tirri, M.; Arfè, R.; Boccuto, F.; Bernardi, T.; Serpelloni, G.; De-Giorgio, F.; Marti, M. Low-normal doses of methiopropamine induce aggressive behaviour in mice. Psychopharmacology 2021, 238, 1847–1856. [Google Scholar] [CrossRef]
- Martinotti, G.; Negri, A.; Schiavone, S.; Montemitro, C.; Vannini, C.; Baroni, G.; Pettorruso, M.; de Giorgio, F.; Giorgetti, R.; Verrastro, V.; et al. Club Drugs: Psychotropic Effects and Psychopathological Characteristics of a Sample of Inpatients. Front. Psychiatry 2020, 11, 879. [Google Scholar] [CrossRef]
- Camuto, C.; Pellegrini, S.; De-Giorgio, F.; de la Torre, X.; Marti, M.; Mazzarino, M.; Botrè, F. Urinary excretion profile of methiopropamine in mice following intraperitoneal administration: A liquid chromatography–tandem mass spectrometry investigation. Drug Test. Anal. 2021, 13, 91–100. [Google Scholar] [CrossRef]
- Miuli, A.; Pettorruso, M.; Romanelli, E.; Stigliano, G.; Di Giuda, D.; De-Giorgio, F.; Martinotti, G.; Di Giannantonio, M. Does DRD2 Taq1A Mediate Aripiprazole-Induced Gambling Disorder? A Pharmacogenetic Hypothesis. Front. Psychiatry 2020, 11, 275. [Google Scholar] [CrossRef]
- Bilel, S.; Azevedo, N.; Arfè, R.; Tirri, M.; Gregori, A.; Serpelloni, G.; De-Giorgio, F.; Frisoni, P.; Neri, M.; Calò, G.; et al. In vitro and in vivo pharmacological characterization of the synthetic opioid MT-45. Neuropharmacology 2020, 171, 108110. [Google Scholar] [CrossRef] [PubMed]
- Ossato, A.; Bilel, S.; Gregori, A.; Talarico, A.; Trapella, C.; Gaudio, R.M.; De Giorgio, F.; Tagliaro, F.; Neri, M.; Fattore, L.; et al. Neurological, sensorimotor and cardiorespiratory alterations induced by methoxetamine, ketamine and phencyclidine in mice. Neuropharmacology 2018, 141, 167–180. [Google Scholar] [CrossRef]
- Ossato, A.; Uccelli, L.; Bilel, S.; Canazza, I.; Di Domenico, G.; Pasquali, M.; Pupillo, G.; De Luca, M.A.; Boschi, A.; Vincenzi, F.; et al. Psychostimulant Effect of the Synthetic Cannabinoid JWH-018 and AKB48: Behavioral, Neurochemical, and Dopamine Transporter Scan Imaging Studies in Mice. Front. Psychiatry 2017, 8, 130. [Google Scholar] [CrossRef] [PubMed]
- Fantinati, A.; Ossato, A.; Bianco, S.; Canazza, I.; de Giorgio, F.; Trapella, C.; Marti, M. 1-cyclohexyl-x-methoxybenzene derivatives, novel psychoactive substances seized on the internet market. Synthesis and in vivo pharmacological studies in mice. Hum. Psychopharmacol. Clin. Exp. 2017, 32, e2560. [Google Scholar] [CrossRef]
- Lenzi, M.; Cocchi, V.; Gasperini, S.; Arfè, R.; Marti, M.; Hrelia, P. Evaluation of Cytotoxic and Mutagenic Effects of the Synthetic Cathinones Mexedrone, α-PVP and α-PHP. Int. J. Mol. Sci. 2021, 22, 6320. [Google Scholar] [CrossRef] [PubMed]
- Lenzi, M.; Cocchi, V.; Cavazza, L.; Bilel, S.; Hrelia, P.; Marti, M. Genotoxic Properties of Synthetic Cannabinoids on TK6 Human Cells by Flow Cytometry. Int. J. Mol. Sci. 2020, 21, 1150. [Google Scholar] [CrossRef] [PubMed]
- Santos-Toscano, R.; Guirguis, A.; Davidson, C. How preclinical studies have influenced novel psychoactive substance legislation in the UK and Europe. Br. J. Clin. Pharmacol. 2020, 86, 452–481. [Google Scholar] [CrossRef]
- Luethi, D.; Hoener, M.C.; Liechti, M.E. Effects of the new psychoactive substances diclofensine, diphenidine, and methoxphenidine on monoaminergic systems. Eur. J. Pharmacol. 2018, 819, 242–247. [Google Scholar] [CrossRef]
- Belin-Rauscent, A.; Belin, D. Animal Models of Drug Addiction. In Addictions: From Pathophysiology to Treatment; IntechOpen: London, UK, 2012; pp. 3–20. [Google Scholar] [CrossRef]
- Marusich, J.A.; Grant, K.R.; Blough, B.E.; Wiley, J. Effects of synthetic cathinones contained in “bath salts” on motor behavior and a functional observational battery in mice. NeuroToxicology 2012, 33, 1305–1313. [Google Scholar] [CrossRef]
- Fantegrossi, W.E.; Gannon, B.M.; Zimmerman, S.M.; Rice, K.C. In vivo Effects of Abused ‘Bath Salt’ Constituent 3,4-methylenedioxypyrovalerone (MDPV) in Mice: Drug Discrimination, Thermoregulation, and Locomotor Activity. Neuropsychopharmacology 2013, 38, 563–573. [Google Scholar] [CrossRef]
- Bilel, S.; Tirri, M.; Arfè, R.; Stopponi, S.; Soverchia, L.; Ciccocioppo, R.; Frisoni, P.; Strano-Rossi, S.; Miliano, C.; De-Giorgio, F.; et al. Pharmacological and Behavioral Effects of the Synthetic Cannabinoid AKB48 in Rats. Front. Neurosci. 2019, 13, 1163. [Google Scholar] [CrossRef]
- Bilel, S.; Tirri, M.; Arfè, R.; Ossato, A.; Trapella, C.; Serpelloni, G.; Neri, M.; Fattore, L.; Marti, M. Novel halogenated synthetic cannabinoids impair sensorimotor functions in mice. NeuroToxicology 2020, 76, 17–32. [Google Scholar] [CrossRef] [PubMed]
- Simola, N.; Costa, G.; De Luca, M.A.; Piras, G.; Marongiu, J.; Fattore, L. Neuronal and peripheral damages induced by synthetic psychoactive substances: An update of recent findings from human and animal studies. Neural Regen. Res. 2020, 15, 802–816. [Google Scholar] [CrossRef] [PubMed]
- Sumnall, H.R.; Evans-Brown, M.; McVeigh, J. Social, policy, and public health perspectives on new psychoactive substances. Drug Test. Anal. 2011, 3, 515–523. [Google Scholar] [CrossRef] [PubMed]
- Westbrook, K.; Stearns, V. Pharmacogenomics of breast cancer therapy: An update. Pharmacol. Ther. 2013, 139, 1–11. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Miranda Furtado, C.L.; Dos Santos Luciano, M.C.; da Silva Santos, R.; Furtado, G.P.; Moraes, M.O.; Pessoa, C. Epidrugs: Targeting epigenetic marks in cancer treatment. Epigenetics 2019, 14, 1164–1176. [Google Scholar] [CrossRef] [PubMed]
- López-Camarillo, C.; Gallardo-Rincón, D.; Álvarez-Sánchez, M.E.; Marchat, L.A. Pharmaco-epigenomics: On the Road of Translation Medicine. Adv. Exp. Med. Biol. 2019, 1168, 31–42. [Google Scholar] [CrossRef]
- Ravaei, A.; Rubini, M. Rescuing effect of folates on methotrexate cytotoxicity in human trophoblast cells. Clin. Exp. Rheumatol. 2021. [Google Scholar] [CrossRef]
- Moore, D.S. Behavioral epigenetics. WIREs Syst. Biol. Med. 2017, 9, e1333. [Google Scholar] [CrossRef]
- Kyzar, E.J.; Bohnsack, J.P.; Pandey, S.C. Current and Future Perspectives of Noncoding RNAs in Brain Function and Neuropsychiatric Disease. Biol. Psychiatry 2022, 91, 183–193. [Google Scholar] [CrossRef] [PubMed]
- Kanherkar, R.R.; Bhatia-Dey, N.; Csoka, A.B. Epigenetics across the human lifespan. Front. Cell Dev. Biol. 2014, 2, 49. [Google Scholar] [CrossRef]
- Kim, J.K.; Samaranayake, M.; Pradhan, S. Epigenetic mechanisms in mammals. Exp. 2009, 66, 596–612. [Google Scholar] [CrossRef] [PubMed]
- Rask-Andersen, M.; Martinsson, D.; Ahsan, M.; Enroth, S.; Ek, W.E.; Gyllensten, U.; Johansson, A. Epigenome-wide association study reveals differential DNA methylation in individuals with a history of myocardial infarction. Hum. Mol. Genet. 2016, 25, 4739–4748. [Google Scholar] [CrossRef]
- Devaux, Y.; Vausort, M.; Goretti, E.; Nazarov, P.; Azuaje, F.; Gilson, G.; Corsten, M.F.; Schroen, B.; Lair, M.-L.; Heymans, S.; et al. Use of Circulating MicroRNAs to Diagnose Acute Myocardial Infarction. Clin. Chem. 2012, 58, 559–567. [Google Scholar] [CrossRef] [PubMed]
- Dimmeler, S.; Zeiher, A.M. Circulating microRNAs: Novel biomarkers for cardiovascular diseases? Eur. Heart J. 2010, 31, 2705–2707. [Google Scholar] [CrossRef] [PubMed]
- D’Alessandra, Y.; Devanna, P.; Limana, F.; Straino, S.; Di Carlo, A.; Brambilla, P.G.; Rubino, M.; Carena, M.C.; Spazzafumo, L.; De Simone, M.; et al. Circulating microRNAs are new and sensitive biomarkers of myocardial infarction. Eur. Heart J. 2010, 31, 2765–2773. [Google Scholar] [CrossRef]
- Lopomo, A.; Coppedè, F. Pharmacoepigenetics and pharmacoepigenomics of gastrointestinal cancers. Expert Rev. Gastroenterol. Hepatol. 2018, 12, 49–62. [Google Scholar] [CrossRef]
- Smits, K.M.; Cleven, A.H.; Weijenberg, M.P.; Hughes, L.A.; Herman, J.G.; de Bruïne, A.P.; van Engeland, M. Pharmacoepigenomics in colorectal cancer: A step forward in predicting prognosis and treatment response. Pharmacogenomics 2008, 9, 1903–1916. [Google Scholar] [CrossRef]
- Tirri, M.; Frisoni, P.; Bilel, S.; Arfè, R.; Trapella, C.; Fantinati, A.; Corli, G.; Marchetti, B.; De-Giorgio, F.; Camuto, C.; et al. Worsening of the Toxic Effects of (±) Cis-4,4′-DMAR Following Its Co-Administration with (±) Trans-4,4′-DMAR: Neuro-Behavioural, Physiological, Immunohistochemical and Metabolic Studies in Mice. Int. J. Mol. Sci. 2021, 22, 8771. [Google Scholar] [CrossRef]
- Schiavone, S.; Neri, M.; Maffione, A.B.; Frisoni, P.; Morgese, M.G.; Trabace, L.; Turillazzi, E. Increased iNOS and Nitrosative Stress in Dopaminergic Neurons of MDMA-Exposed Rats. Int. J. Mol. Sci. 2019, 20, 1242. [Google Scholar] [CrossRef]
- Rudin, D.; Liechti, M.E.; Luethi, D. Molecular and clinical aspects of potential neurotoxicity induced by new psychoactive stimulants and psychedelics. Exp. Neurol. 2021, 343, 113778. [Google Scholar] [CrossRef] [PubMed]
- Carvalho, M.; Carmo, H.; Costa, V.M.; Capela, J.P.; Pontes, H.; Remião, F.; Carvalho, F.; Bastos, M.D.L. Toxicity of amphetamines: An update. Arch. Toxicol. 2012, 86, 1167–1231. [Google Scholar] [CrossRef]
- Wu, C.-T.; Morris, J.R. Genes, Genetics, and Epigenetics: A Correspondence. Science 2001, 293, 1103–1105. [Google Scholar] [CrossRef]
- Dupont, C.; Armant, D.R.; Brenner, C.A. Epigenetics: Definition, Mechanisms and Clinical Perspective. Semin. Reprod. Med. 2009, 27, 351–357. [Google Scholar] [CrossRef] [PubMed]
- Holliday, R. Epigenetics: A Historical Overview. Epigenetics 2006, 1, 76–80. [Google Scholar] [CrossRef] [PubMed]
- Ashe, A.; Colot, V.; Oldroyd, B.P. How does epigenetics influence the course of evolution? Philos. Trans. R. Soc. B Biol. Sci. 2021, 376, 20200111. [Google Scholar] [CrossRef] [PubMed]
- Alberts, B.; Johnson, A.; Lewis, J.; Raff, M.; Roberts, K.; Walter, P. Chromosomal DNA and Its Packaging in the Chromatin Fiber. In Molecular Biology of the Cell, 4th ed.; Garland Science: New York, NY, USA, 2002. [Google Scholar]
- Walker, D.M.; Cates, H.M.; Heller, E.A.; Nestler, E.J. Regulation of chromatin states by drugs of abuse. Curr. Opin. Neurobiol. 2015, 30, 112–121. [Google Scholar] [CrossRef] [PubMed]
- Romani, M. Epigenetica, 1st ed.; Zanichelli Publisher: Bologna, Italy, 2021. [Google Scholar]
- Solovei, I.; Thanisch, K.; Feodorova, Y. How to rule the nucleus: Divide et impera. Curr. Opin. Cell Biol. 2016, 40, 47–59. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Ali, M.; Zhou, Q. Establishment and evolution of heterochromatin. Ann. N. Y. Acad. Sci. 2020, 1476, 59–77. [Google Scholar] [CrossRef] [PubMed]
- Felsenfeld, G.; Groudine, M. Controlling the double helix. Nature 2003, 421, 448–453. [Google Scholar] [CrossRef] [PubMed]
- Bannister, A.J.; Kouzarides, T. Regulation of chromatin by histone modifications. Cell Res. 2011, 21, 381–395. [Google Scholar] [CrossRef] [PubMed]
- Hyun, K.; Jeon, J.; Park, K.; Kim, J. Writing, erasing and reading histone lysine methylations. Exp. Mol. Med. 2017, 49, e324. [Google Scholar] [CrossRef] [PubMed]
- Maze, I.; Noh, K.-M.; Soshnev, A.; Allis, C.D. Every amino acid matters: Essential contributions of histone variants to mammalian development and disease. Nat. Rev. Genet. 2014, 15, 259–271. [Google Scholar] [CrossRef]
- Tiwari, S. Recent Advancement in Methodology for Understanding Epigenetic Modifications. J. Clin. Epigenetics 2017, 3, 21. [Google Scholar] [CrossRef]
- Li, E.; Zhang, Y. DNA Methylation in Mammals. Cold Spring Harb. Perspect. Biol. 2014, 6, a019133. [Google Scholar] [CrossRef]
- Martín-Subero, J.I. How epigenomics brings phenotype into being. Pediatr. Endocrinol. Rev. 2011, 9 (Suppl. 1), 506–510. [Google Scholar]
- Umer, M.; Herceg, Z. Deciphering the Epigenetic Code: An Overview of DNA Methylation Analysis Methods. Antioxid. Redox Signal. 2013, 18, 1972–1986. [Google Scholar] [CrossRef]
- Bird, A. DNA methylation patterns and epigenetic memory. An excellent review of mammalian DNA methylation. Genes Dev. 2002, 16, 6–21. [Google Scholar] [CrossRef]
- Jones, P.A.; Baylin, S.B. The fundamental role of epigenetic events in cancer. Nat. Rev. Genet. 2002, 3, 415–428. [Google Scholar] [CrossRef]
- Wyatt, G.R. Recognition and estimation of 5-methylcytosine in nucleic acids. Biochem. J. 1951, 48, 581–584. [Google Scholar] [CrossRef]
- Takai, D.; Jones, P.A. Comprehensive analysis of CpG islands in human chromosomes 21 and 22. Proc. Natl. Acad. Sci. USA 2002, 99, 3740–3745. [Google Scholar] [CrossRef] [PubMed]
- Chen, K.; Zhao, B.S.; He, C. Nucleic Acid Modifications in Regulation of Gene Expression. Cell Chem. Biol. 2016, 23, 74–85. [Google Scholar] [CrossRef] [PubMed]
- Li, E.; Beard, C.; Jaenisch, R. Role for DNA methylation in genomic imprinting. Nature 1993, 366, 362–365. [Google Scholar] [CrossRef]
- Curradi, M.; Izzo, A.; Badaracco, G.; Landsberger, N. Molecular Mechanisms of Gene Silencing Mediated by DNA Methylation. Mol. Cell. Biol. 2002, 22, 3157–3173. [Google Scholar] [CrossRef] [PubMed]
- Miller, J.L.; Grant, P.A. The Role of DNA Methylation and Histone Modifications in Transcriptional Regulation in Humans. In Epigenetics: Development and Disease; Kundu, T.K., Ed.; Springer: Dordrecht, The Netherlands, 2013; pp. 289–317. [Google Scholar] [CrossRef]
- Eharrison, A.; Eparle-Mcdermott, A. DNA Methylation: A Timeline of Methods and Applications. Front. Genet. 2011, 2, 74. [Google Scholar] [CrossRef]
- Tang, J.; Fang, F.; Miller, D.F.; Pilrose, J.M.; Matei, D.; Huang, T.H.-M.; Nephew, K.P. Global DNA Methylation Profiling Technologies and the Ovarian. Cancer Epigenetics 2015, 1238, 653–675. [Google Scholar] [CrossRef]
- Bibikova, M.; Fan, J. Genome-wide DNA methylation profiling. WIREs Syst. Biol. Med. 2010, 2, 210–223. [Google Scholar] [CrossRef]
- Mattick, J.S.; Makunin, I.V. Non-coding RNA. Hum. Mol. Genet. 2006, 15, R17–R29. [Google Scholar] [CrossRef]
- Mattick, J.S. RNA regulation: A new genetics? Nat. Rev. Genet. 2004, 5, 316–323. [Google Scholar] [CrossRef]
- Mattick, J.; Makunin, I.V. Small regulatory RNAs in mammals. Hum. Mol. Genet. 2005, 14, R121–R132. [Google Scholar] [CrossRef]
- Wei, M.-M.; Zhou, G.-B. Long Non-coding RNAs and Their Roles in Non-small-cell Lung Cancer. Genom. Proteom. Bioinform. 2016, 14, 280–288. [Google Scholar] [CrossRef] [PubMed]
- Awan, H.M.; Shah, A.; Rashid, F.; Shan, G. Primate-specific Long Non-coding RNAs and MicroRNAs. Genom. Proteom. Bioinform. 2017, 15, 187–195. [Google Scholar] [CrossRef]
- Lee, J.T.; Bartolomei, M.S. X-Inactivation, Imprinting, and Long Noncoding RNAs in Health and Disease. Cell 2013, 152, 1308–1323. [Google Scholar] [CrossRef] [PubMed]
- Kanduri, C. Long noncoding RNAs: Lessons from genomic imprinting. Biochim. Biophys. Acta (BBA) Bioenerg. Mech. 2016, 1859, 102–111. [Google Scholar] [CrossRef]
- Autuoro, J.M.; Pirnie, S.P.; Carmichael, G.G. Long Noncoding RNAs in Imprinting and X Chromosome Inactivation. Biomolecules 2014, 4, 76–100. [Google Scholar] [CrossRef] [PubMed]
- Mao, Y.S.; Sunwoo, H.; Zhang, B.; Spector, D.L. Direct visualization of the co-transcriptional assembly of a nuclear body by noncoding RNAs. Nat. Cell Biol. 2011, 13, 95–101. [Google Scholar] [CrossRef] [PubMed]
- Wei, J.-W.; Huang, K.; Yang, C.; Kang, C.-S. Non-coding RNAs as regulators in epigenetics (Review). Oncol. Rep. 2017, 37, 3–9. [Google Scholar] [CrossRef]
- Choudhuri, S. Small noncoding RNAs: Biogenesis, function, and emerging significance in toxicology. J. Biochem. Mol. Toxicol. 2010, 24, 195–216. [Google Scholar] [CrossRef]
- Shi, Y.; Jia, X.; Xu, J. The new function of circRNA: Translation. Clin. Transl. Oncol. 2020, 22, 2162–2169. [Google Scholar] [CrossRef]
- Saliminejad, K.; Khorram Khorshid, H.R.; Soleymani Fard, S.; Ghaffari, S.H. An overview of microRNAs: Biology, functions, therapeutics, and analysis methods. J. Cell. Physiol. 2019, 234, 5451–5465. [Google Scholar] [CrossRef]
- Hyman, S.E.; Malenka, R.C.; Nestler, E.J. Neural mechanisms of addiction: The Role of Reward-Related Learning and Memory. Annu. Rev. Neurosci. 2006, 29, 565–598. [Google Scholar] [CrossRef] [PubMed]
- Vassoler, F.; Sadri-Vakili, G. Mechanisms of transgenerational inheritance of addictive-like behaviors. Neuroscience 2014, 264, 198–206. [Google Scholar] [CrossRef] [PubMed]
- Gould, T.J. Addiction and cognition. Addict. Sci. Clin. Pract. 2010, 5, 4–14. [Google Scholar] [PubMed]
- Feltenstein, M.W.; See, R.E. The neurocircuitry of addiction: An overview. Br. J. Pharmacol. 2008, 154, 261–274. [Google Scholar] [CrossRef] [PubMed]
- Kalivas, P.W.; Volkow, N.D. The Neural Basis of Addiction: A Pathology of Motivation and Choice. Am. J. Psychiatry 2005, 162, 1403–1413. [Google Scholar] [CrossRef] [PubMed]
- Jayanthi, S.; McCoy, M.T.; Chen, B.; Britt, J.P.; Kourrich, S.; Yau, H.-J.; Ladenheim, B.; Krasnova, I.N.; Bonci, A.; Cadet, J.L. Methamphetamine Downregulates Striatal Glutamate Receptors via Diverse Epigenetic Mechanisms. Biol. Psychiatry 2014, 76, 47–56. [Google Scholar] [CrossRef]
- Heinbockel, T.; Csoka, A.B. Epigenetic Effects of Drugs of Abuse. Int. J. Environ. Res. Public Health 2018, 15, 2098. [Google Scholar] [CrossRef]
- Schratt, G. microRNAs at the synapse. Nat. Rev. Neurosci. 2009, 10, 842–849. [Google Scholar] [CrossRef]
- Dreyer, J.-L. New insights into the roles of microRNAs in drug addiction and neuroplasticity. Genome Med. 2010, 2, 92. [Google Scholar] [CrossRef]
- Levine, A.A.; Guan, Z.; Barco, A.; Xu, S.; Kandel, E.R.; Schwartz, J.H. CREB-binding protein controls response to cocaine by acetylating histones at the fosB promoter in the mouse striatum. Proc. Natl. Acad. Sci. USA 2005, 102, 19186–19191. [Google Scholar] [CrossRef]
- Kumar, A.; Choi, K.-H.; Renthal, W.; Tsankova, N.M.; Theobald, D.E.; Truong, H.-T.; Russo, S.; LaPlant, Q.; Sasaki, T.S.; Whistler, K.N.; et al. Chromatin Remodeling Is a Key Mechanism Underlying Cocaine-Induced Plasticity in Striatum. Neuron 2005, 48, 303–314. [Google Scholar] [CrossRef] [PubMed]
- Cheng, M.-C.; Hsu, S.-H.; Chen, C.-H. Chronic methamphetamine treatment reduces the expression of synaptic plasticity genes and changes their DNA methylation status in the mouse brain. Brain Res. 2015, 1629, 126–134. [Google Scholar] [CrossRef] [PubMed]
- Shen, H.-Y.; Kalda, A.; Yu, L.; Ferrara, J.; Zhu, J.; Chen, J.-F. Additive effects of histone deacetylase inhibitors and amphetamine on histone H4 acetylation, cAMP responsive element binding protein phosphorylation and Delta FosB expression in the striatum and locomotor sensitization in mice. Neuroscience 2008, 157, 644–655. [Google Scholar] [CrossRef]
- Vasudevan, S.; Tong, Y.; Steitz, J.A. Switching from Repression to Activation: MicroRNAs Can Up-Regulate Translation. Science 2007, 318, 1931–1934. [Google Scholar] [CrossRef]
- Rajasethupathy, P.; Fiumara, F.; Sheridan, R.; Betel, D.; Puthanveettil, S.V.; Russo, J.J.; Sander, C.; Tuschl, T.; Kandel, E. Characterization of Small RNAs in Aplysia Reveals a Role for miR-124 in Constraining Synaptic Plasticity through CREB. Neuron 2009, 63, 803–817. [Google Scholar] [CrossRef]
- Tsankova, N.; Renthal, W.; Kumar, A.; Nestler, E.J. Epigenetic regulation in psychiatric disorders. Nat. Rev. Neurosci. 2007, 8, 355–367. [Google Scholar] [CrossRef]
- Robison, A.J.; Nestler, E.J. Transcriptional and epigenetic mechanisms of addiction. Nat. Rev. Neurosci. 2011, 12, 623–637. [Google Scholar] [CrossRef] [PubMed]
- LaPlant, Q.; Vialou, V.; Iii, H.E.C.; Dumitriu, D.; Feng, J.; Warren, B.L.; Maze, I.; Dietz, D.; Watts, E.L.; Iñiguez, S.; et al. Dnmt3a regulates emotional behavior and spine plasticity in the nucleus accumbens. Nat. Neurosci. 2010, 13, 1137–1143. [Google Scholar] [CrossRef]
- Kalda, A.; Zharkovsky, A. Epigenetic Mechanisms of Psychostimulant-Induced Addiction. Int. Rev. Neurobiol. 2015, 120, 85–105. [Google Scholar] [CrossRef]
- Yang, X.; Bam, M.; Nagarkatti, P.S.; Nagarkatti, M. RNA-seq Analysis of δ9-Tetrahydrocannabinol-treated T Cells Reveals Altered Gene Expression Profiles That Regulate Immune Response and Cell Proliferation. J. Biol. Chem. 2016, 291, 15460–15472. [Google Scholar] [CrossRef]
- Feng, J.; Shao, N.-Y.; Szulwach, K.E.; Vialou, V.; Huynh, J.; Zhong, C.; Le, T.; Ferguson, D.; Cahill, M.; Li, Y.; et al. Role of Tet1 and 5-hydroxymethylcytosine in cocaine action. Nat. Neurosci. 2015, 18, 536–544. [Google Scholar] [CrossRef] [PubMed]
- Parsons, L.H.; Hurd, Y.L. Endocannabinoid signalling in reward and addiction. Nat. Rev. Neurosci. 2015, 16, 579–594. [Google Scholar] [CrossRef]
- Mechoulam, R.; Parker, L.A. The Endocannabinoid System and the Brain. Annu. Rev. Psychol. 2013, 64, 21–47. [Google Scholar] [CrossRef]
- Meyer, H.C.; Lee, F.S.; Gee, D.G. The Role of the Endocannabinoid System and Genetic Variation in Adolescent Brain Development. Neuropsychopharmacology 2018, 43, 21–33. [Google Scholar] [CrossRef] [PubMed]
- Fergusson, D.M.; Boden, J.M.; Horwood, L.J. Cannabis use and other illicit drug use: Testing the cannabis gateway hypothesis. Addiction 2006, 101, 556–569. [Google Scholar] [CrossRef] [PubMed]
- Orihuel, J.; Gómez-Rubio, L.; Valverde, C.; Capellán, R.; Roura-Martínez, D.; Ucha, M.; Ambrosio, E.; Higuera-Matas, A. Cocaine-induced Fos expression in the rat brain: Modulation by prior Δ9-tetrahydrocannabinol exposure during adolescence and sex-specific effects. Brain Res. 2021, 1764, 147480. [Google Scholar] [CrossRef]
- Tomas-Roig, J.; Benito, E.; Agis-Balboa, R.C.; Piscitelli, F.; Hoyer-Fender, S.; Di Marzo, V.; Havemann-Reinecke, U. Chronic exposure to cannabinoids during adolescence causes long-lasting behavioral deficits in adult mice. Addict. Biol. 2017, 22, 1778–1789. [Google Scholar] [CrossRef]
- Gobira, P.H.; Roncalho, A.L.; Silva, N.R.; Silote, G.P.; Sales, A.J.; Joca, S.R. Adolescent cannabinoid exposure modulates the vulnerability to cocaine-induced conditioned place preference and DNMT3a expression in the prefrontal cortex in Swiss mice. Psychopharmacology 2021, 238, 3107–3118. [Google Scholar] [CrossRef]
- Scherma, M.; Qvist, J.S.; Asok, A.; Huang, S.-S.C.; Masia, P.; Deidda, M.; Wei, Y.B.; Soni, R.K.; Fratta, W.; Fadda, P.; et al. Cannabinoid exposure in rat adolescence reprograms the initial behavioral, molecular, and epigenetic response to cocaine. Proc. Natl. Acad. Sci. USA 2020, 117, 9991–10002. [Google Scholar] [CrossRef]
- Tomasiewicz, H.C.; Jacobs, M.M.; Wilkinson, M.B.; Wilson, S.P.; Nestler, E.J.; Hurd, Y.L. Proenkephalin Mediates the Enduring Effects of Adolescent Cannabis Exposure Associated with Adult Opiate Vulnerability. Biol. Psychiatry 2012, 72, 803–810. [Google Scholar] [CrossRef]
- Gowen, A.M.; Odegaard, K.E.; Hernandez, J.; Chand, S.; Koul, S.; Pendyala, G.; Yelamanchili, S.V. Role of microRNAs in the pathophysiology of addiction. Wiley Interdiscip. Rev. RNA 2021, 12, e1637. [Google Scholar] [CrossRef] [PubMed]
- Anier, K.; Malinovskaja, K.; Aonurm-Helm, A.; Zharkovsky, A.; Kalda, A. DNA Methylation Regulates Cocaine-Induced Behavioral Sensitization in Mice. Neuropsychopharmacology 2010, 35, 2450–2461. [Google Scholar] [CrossRef] [PubMed]
- Carouge, D.; Host, L.; Aunis, D.; Zwiller, J.; Anglard, P. CDKL5 is a brain MeCP2 target gene regulated by DNA methylation. Neurobiol. Dis. 2010, 38, 414–424. [Google Scholar] [CrossRef] [PubMed]
- Renthal, W.; Maze, I.; Krishnan, V.; Covington, H.E.; Xiao, G.; Kumar, A.; Russo, S.; Graham, A.; Tsankova, N.; Kippin, T.E.; et al. Histone Deacetylase 5 Epigenetically Controls Behavioral Adaptations to Chronic Emotional Stimuli. Neuron 2007, 56, 517–529. [Google Scholar] [CrossRef]
- Renthal, W.; Kumar, A.; Xiao, G.; Wilkinson, M.; Covington, H.E.; Maze, I.; Sikder, D.; Robison, A.; LaPlant, Q.; Dietz, D.; et al. Genome-wide Analysis of Chromatin Regulation by Cocaine Reveals a Role for Sirtuins. Neuron 2009, 62, 335–348. [Google Scholar] [CrossRef]
- Koczor, C.A.; Ludlow, I.; Hight, R.S.; Jiao, Z.; Fields, E.; Ludaway, T.; Russ, R.; Torres, R.A.; Lewis, W. Ecstasy (MDMA) Alters Cardiac Gene Expression and DNA Methylation: Implications for Circadian Rhythm Dysfunction in the Heart. Toxicol. Sci. 2015, 148, 183–191. [Google Scholar] [CrossRef]
- Tian, W.; Zhao, M.; Li, M.; Song, T.; Zhang, M.; Quan, L.; Li, S.; Sun, Z. Reversal of Cocaine-Conditioned Place Preference through Methyl Supplementation in Mice: Altering Global DNA Methylation in the Prefrontal Cortex. PLoS ONE 2012, 7, e33435. [Google Scholar] [CrossRef]
- Anier, K.; Zharkovsky, A.; Kalda, A. S-adenosylmethionine modifies cocaine-induced DNA methylation and increases locomotor sensitization in mice. Int. J. Neuropsychopharmacol. 2013, 16, 2053–2066. [Google Scholar] [CrossRef]
- Zhang, H.; Darwanto, A.; Linkhart, T.A.; Sowers, L.C.; Zhang, L. Maternal Cocaine Administration Causes an Epigenetic Modification of Protein Kinase Cϵ Gene Expression in Fetal Rat Heart. Mol. Pharmacol. 2007, 71, 1319–1328. [Google Scholar] [CrossRef]
- Prini, P.; Penna, F.; Sciuccati, E.; Alberio, T.; Rubino, T. Chronic Δ9-THC Exposure Differently Affects Histone Modifications in the Adolescent and Adult Rat Brain. Int. J. Mol. Sci. 2017, 18, 2094. [Google Scholar] [CrossRef]
- Murphy, S.K.; Itchon-Ramos, N.; Visco, Z.; Huang, Z.; Grenier, C.; Schrott, R.; Acharya, K.; Boudreau, M.-H.; Price, T.; Raburn, D.J.; et al. Cannabinoid exposure and altered DNA methylation in rat and human sperm. Epigenetics 2018, 13, 1208–1221. [Google Scholar] [CrossRef]
- Di Giacomo, D.; De Domenico, E.; Sette, C.; Geremia, R.; Grimaldi, P. Type 2 cannabinoid receptor contributes to the physiological regulation of spermatogenesis. FASEB J. 2016, 30, 1453–1463. [Google Scholar] [CrossRef] [PubMed]
- DiNieri, J.A.; Wang, X.; Szutorisz, H.; Spano, S.M.; Kaur, J.; Casaccia, P.; Dow-Edwards, D.; Hurd, Y.L. Maternal Cannabis Use Alters Ventral Striatal Dopamine D2 Gene Regulation in the Offspring. Biol. Psychiatry 2011, 70, 763–769. [Google Scholar] [CrossRef] [PubMed]
- Watson, C.T.; Szutorisz, H.; Garg, P.; Martin, Q.; Landry, J.A.; Sharp, A.J.; Hurd, Y.L. Genome-Wide DNA Methylation Profiling Reveals Epigenetic Changes in the Rat Nucleus Accumbens Associated With Cross-Generational Effects of Adolescent THC Exposure. Neuropsychopharmacology 2015, 40, 2993–3005. [Google Scholar] [CrossRef]
- Prini, P.; Rusconi, F.; Zamberletti, E.; Gabaglio, M.; Penna, F.; Fasano, M.; Battaglioli, E.; Parolaro, D.; Rubino, T. Adolescent THC exposure in female rats leads to cognitive deficits through a mechanism involving chromatin modifications in the prefrontal cortex. J. Psychiatry Neurosci. 2018, 43, 87–101. [Google Scholar] [CrossRef] [PubMed]
- Hollins, S.; Zavitsanou, K.; Walker, F.R.; Cairns, M.J. Alteration of imprinted Dlk1-Dio3 miRNA cluster expression in the entorhinal cortex induced by maternal immune activation and adolescent cannabinoid exposure. Transl. Psychiatry 2014, 4, e452. [Google Scholar] [CrossRef] [PubMed]
- Levine, M.E.; Lu, A.T.; Quach, A.; Chen, B.H.; Assimes, T.L.; Bandinelli, S.; Hou, L.; Baccarelli, A.A.; Stewart, J.D.; Li, Y.; et al. An epigenetic biomarker of aging for lifespan and healthspan. Aging 2018, 10, 573–591. [Google Scholar] [CrossRef]
- Vidaki, A.; Ballard, D.; Aliferi, A.; Miller, T.; Barron, L.P.; Court, D.S. DNA methylation-based forensic age prediction using artificial neural networks and next generation sequencing. Forensic Sci. Int. Genet. 2017, 28, 225–236. [Google Scholar] [CrossRef]
- Field, A.E.; Robertson, N.; Wang, T.; Havas, A.; Ideker, T.; Adams, P.D. DNA Methylation Clocks in Aging: Categories, Causes, and Consequences. Mol. Cell 2018, 71, 882–895. [Google Scholar] [CrossRef] [PubMed]
- Bocklandt, S.; Lin, W.; Sehl, M.E.; Sánchez, F.J.; Sinsheimer, J.S.; Horvath, S.; Vilain, E. Epigenetic Predictor of Age. PLoS ONE 2011, 6, e14821. [Google Scholar] [CrossRef]
- Ashapkin, V.V.; Kutueva, L.I.; Vanyushin, B.F. Epigenetic Clock: Just a Convenient Marker or an Active Driver of Aging? Adv. Exp. Med. Biol. 2019, 1178, 175–206. [Google Scholar] [CrossRef] [PubMed]
- Slieker, R.; Van Iterson, M.; Luijk, R.; Beekman, M.; Zhernakova, D.V.; Moed, M.H.; Mei, H.; Van Galen, M.; Deelen, P.; Bonder, M.J.; et al. Age-related accrual of methylomic variability is linked to fundamental ageing mechanisms. Genome Biol. 2016, 17, 191. [Google Scholar] [CrossRef] [PubMed]
- Bell, C.G.; Lowe, R.; Adams, P.D.; Baccarelli, A.A.; Beck, S.; Bell, J.T.; Christensen, B.C.; Gladyshev, V.N.; Heijmans, B.T.; Horvath, S.; et al. DNA methylation aging clocks: Challenges and recommendations. Genome Biol. 2019, 20, 249. [Google Scholar] [CrossRef]
- Horvath, S.; Raj, K. DNA methylation-based biomarkers and the epigenetic clock theory of ageing. Nat. Rev. Genet. 2018, 19, 371–384. [Google Scholar] [CrossRef] [PubMed]
- Horvath, S.; Pirazzini, C.; Bacalini, M.G.; Gentilini, D.; Di Blasio, A.M.; Delledonne, M.; Mari, D.; Arosio, B.; Monti, D.; Passarino, G.; et al. Decreased epigenetic age of PBMCs from Italian semi-supercentenarians and their offspring. Aging 2015, 7, 1159–1170. [Google Scholar] [CrossRef] [PubMed]
- Reveron, M.E.; Monks, T.J.; Duvauchelle, C.L. Age-dependent (+)MDMA-mediated Neurotoxicity in Mice. Neurotoxicology 2005, 26, 1031–1040. [Google Scholar] [CrossRef]
- Frau, L.; Costa, G.; Porceddu, P.F.; Khairnar, A.; Castelli, M.P.; Ennas, M.G.; Madeddu, C.; Wardas, J.; Morelli, M. Influence of caffeine on 3,4-methylenedioxymethamphetamine-induced dopaminergic neuron degeneration and neuroinflammation is age-dependent. J. Neurochem. 2016, 136, 148–162. [Google Scholar] [CrossRef]
- Feio-Azevedo, R.; Costa, V.M.; Barbosa, D.J.; Teixeira-Gomes, A.; Pita, I.; Gomes, S.; Pereira, F.C.; Duarte-Araújo, M.; Duarte, J.A.; Marques, F.; et al. Aged rats are more vulnerable than adolescents to “ecstasy”-induced toxicity. Arch. Toxicol. 2018, 92, 2275–2295. [Google Scholar] [CrossRef]
- Yusipov, I.; Bacalini, M.G.; Kalyakulina, A.; Krivonosov, M.; Pirazzini, C.; Gensous, N.; Ravaioli, F.; Milazzo, M.; Giuliani, C.; Vedunova, M.; et al. Age-related DNA methylation changes are sex-specific: A comprehensive assessment. Aging 2020, 12, 24057–24080. [Google Scholar] [CrossRef] [PubMed]
- Masser, D.R.; Hadad, N.; Porter, H.L.; Mangold, C.A.; Unnikrishnan, A.; Ford, M.M.; Giles, C.B.; Georgescu, C.; Dozmorov, M.G.; Wren, J.D.; et al. Sexually divergent DNA methylation patterns with hippocampal aging. Aging Cell 2017, 16, 1342–1352. [Google Scholar] [CrossRef] [PubMed]
- Life Expectancy at Birth (Years). Available online: https://www.who.int/data/gho/data/indicators/indicator-details/GHO/life-expectancy-at-birth-(years) (accessed on 5 November 2021).
- Slieker, R.C.; Relton, C.L.; Gaunt, T.R.; Slagboom, P.E.; Heijmans, B.T. Age-related DNA methylation changes are tissue-specific with ELOVL2 promoter methylation as exception. Epigenetics Chromatin 2018, 11, 25. [Google Scholar] [CrossRef] [PubMed]
- Whitley, H.; Lindsey, W. Sex-based differences in drug activity. Am. Fam. Physician 2009, 80, 1254–1258. [Google Scholar]
- Chu, T. Gender Differences in Pharmacokinetics. US Pharm. 2014, 39, 40–43. Available online: www.uspharmacist.com/article/gender-differences-in-pharmacokinetics (accessed on 2 December 2021).
- Lynch, T.; Price, A. The effect of cytochrome P450 metabolism on drug response, interactions, and adverse effects. Am. Fam. Physician. 2007, 76, 391–396. [Google Scholar] [PubMed]
- Patton, A.L.; Seely, K.A.; Yarbrough, A.L.; Fantegrossi, W.; James, L.P.; McCain, K.R.; Fujiwara, R.; Prather, P.L.; Moran, J.H.; Radominska-Pandya, A. Altered metabolism of synthetic cannabinoid JWH-018 by human cytochrome P450 2C9 and variants. Biochem. Biophys. Res. Commun. 2018, 498, 597–602. [Google Scholar] [CrossRef] [PubMed]
- Fantegrossi, W.E.; Moran, J.H.; Radominska-Pandya, A.; Prather, P.L. Distinct pharmacology and metabolism of K2 synthetic cannabinoids compared to Delta(9)-THC: Mechanism underlying greater toxicity? Life Sci. 2014, 97, 45–54. [Google Scholar] [CrossRef]
- Pedersen, A.J.; Petersen, T.H.; Linnet, K. In Vitro Metabolism and Pharmacokinetic Studies on Methylone. Drug Metab. Dispos. 2013, 41, 1247–1255. [Google Scholar] [CrossRef]
- Harris, R.Z.; Benet, L.Z.; Schwartz, J.B. Gender Effects in Pharmacokinetics and Pharmacodynamics. Drugs 1995, 50, 222–239. [Google Scholar] [CrossRef]
- McClenahan, S.J.; Hambuchen, M.D.; Simecka, C.M.; Gunnell, M.G.; Berquist, M.D.; Owens, S.M. Cardiovascular effects of 3,4-methylenedioxypyrovalerone (MDPV) in male and female Sprague-Dawley rats. Drug Alcohol Depend. 2019, 195, 140–147. [Google Scholar] [CrossRef] [PubMed]
- Fattore, L.; Marti, M.; Mostallino, R.; Castelli, M.P. Sex and Gender Differences in the Effects of Novel Psychoactive Substances. Brain Sci. 2020, 10, 606. [Google Scholar] [CrossRef]
- Bae, S.; Gilbert, R.D.; Ducsay, C.A.; Zhang, L. Prenatal cocaine exposure increases heart susceptibility to ischaemia–reperfusion injury in adult male but not female rats. J. Physiol. 2005, 565, 149–158. [Google Scholar] [CrossRef] [PubMed]
- De Giovanni, N.; Marchetti, D. Cocaine and its metabolites in the placenta: A systematic review of the literature. Reprod. Toxicol. 2012, 33, 1–14. [Google Scholar] [CrossRef]
- Bae, S.; Zhang, L. Prenatal cocaine exposure increases apoptosis of neonatal rat heart and heart susceptibility to ischemia-reperfusion injury in 1-month-old rat. J. Cereb. Blood Flow Metab. 2005, 144, 900–907. [Google Scholar] [CrossRef] [PubMed]
- Meyer, K.D.; Zhang, H.; Zhang, L. Prenatal cocaine exposure abolished ischemic preconditioning-induced protection in adult male rat hearts: Role of PKCε. Am. J. Physiol. Circ. Physiol. 2009, 296, H1566–H1576. [Google Scholar] [CrossRef]
- Novikova, S.I.; He, F.; Bai, J.; Lidow, M.S. Neuropathology of the cerebral cortex observed in a range of animal models of prenatal cocaine exposure may reflect alterations in genes involved in the Wnt and cadherin systems. Synapse 2005, 56, 105–116. [Google Scholar] [CrossRef] [PubMed]
- Thompson, R.; DeJong, K.; Lo, J. Marijuana Use in Pregnancy: A Review. Obstet. Gynecol. Surv. 2019, 74, 415–428. [Google Scholar] [CrossRef] [PubMed]
- Sadeu, J.C.; Hughes, C.L.; Agarwal, S.; Foster, W.G. Alcohol, drugs, caffeine, tobacco, and environmental contaminant exposure: Reproductive health consequences and clinical implications. Crit. Rev. Toxicol. 2010, 40, 633–652. [Google Scholar] [CrossRef]
- Pintori, N.; Castelli, M.P.; Miliano, C.; Simola, N.; Fadda, P.; Fattore, L.; Scherma, M.; Ennas, M.G.; Mostallino, R.; Flore, G.; et al. Repeated exposure to JWH-018 induces adaptive changes in the mesolimbic and mesocortical dopaminergic pathways, glial cells alterations, and behavioural correlates. J. Cereb. Blood Flow Metab. 2021, 178, 3476–3497. [Google Scholar] [CrossRef] [PubMed]
- Skinner, M.K. Environmental epigenetic transgenerational inheritance and somatic epigenetic mitotic stability. Epigenetics 2011, 6, 838–842. [Google Scholar] [CrossRef]
- Skinner, M.K. What is an epigenetic transgenerational phenotype? F3 or F2. Reprod. Toxicol. 2008, 25, 2–6. [Google Scholar] [CrossRef] [PubMed]
- Nilsson, E.E.; Sadler-Riggleman, I.; Skinner, M.K. Environmentally induced epigenetic transgenerational inheritance of disease. Environ. Epigenetics 2018, 4, dvy016. [Google Scholar] [CrossRef] [PubMed]
- Cloutier, M.; Harris, C.; Gayen, S.; Maclary, E.; Kalantry, S. Experimental Analysis of Imprinted Mouse X-Chromosome Inactivation. Methods Mol. Biol. 2018, 1861, 177–203. [Google Scholar] [CrossRef]
- Escher, J.; Robotti, S. Pregnancy drugs, fetal germline epigenome, and risks for next-generation pathology: A call to action. Environ. Mol. Mutagen. 2019, 60, 445–454. [Google Scholar] [CrossRef]
- Wanner, N.M.; Colwell, M.; Drown, C.; Faulk, C. Developmental cannabidiol exposure increases anxiety and modifies genome-wide brain DNA methylation in adult female mice. Clin. Epigenetics 2021, 13, 4. [Google Scholar] [CrossRef]
- Silva, L.; Zhao, N.; Popp, S.; Dow-Edwards, D. Prenatal tetrahydrocannabinol (THC) alters cognitive function and amphetamine response from weaning to adulthood in the rat. Neurotoxicology Teratol. 2012, 34, 63–71. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.N.; Feng, J. Drug Addiction and DNA Modifications. In Neuroepigenomics in Aging and Disease; Delgado-Morales, R., Ed.; Springer International Publishing: Cham, Switzerland, 2017; pp. 105–126. [Google Scholar]
- Alexandre, J.; Carmo, H.; Carvalho, F.; Silva, J.P. Synthetic cannabinoids and their impact on neurodevelopmental processes. Addict. Biol. 2020, 25, e12824. [Google Scholar] [CrossRef] [PubMed]
- Scheyer, A.F.; Melis, M.; Trezza, V.; Manzoni, O.J. Consequences of Perinatal Cannabis Exposure. Trends Neurosci. 2019, 42, 871–884. [Google Scholar] [CrossRef] [PubMed]
- Alexandre, J.; Malheiro, R.; Da Silva, D.D.; Carmo, H.; Carvalho, F.; Silva, J.P. The Synthetic Cannabinoids THJ-2201 and 5F-PB22 Enhance In Vitro CB1 Receptor-Mediated Neuronal Differentiation at Biologically Relevant Concentrations. Int. J. Mol. Sci. 2020, 21, 6277. [Google Scholar] [CrossRef] [PubMed]
- De-Giorgio, F.; Bilel, S.; Ossato, A.; Tirri, M.; Arfè, R.; Foti, F.; Serpelloni, G.; Frisoni, P.; Neri, M.; Marti, M. Acute and repeated administration of MDPV increases aggressive behavior in mice: Forensic implications. Int. J. Legal. Med. 2019, 133, 1797–1808. [Google Scholar] [CrossRef]
- Peacock, A.; Bruno, R.; Gisev, N.; Degenhardt, L.; Hall, W.; Sedefov, R.; White, J.; Thomas, K.V.; Farrell, M.; Griffiths, P. New psychoactive substances: Challenges for drug surveillance, control, and public health responses. Lancet 2019, 394, 1668–1684. [Google Scholar] [CrossRef]
- Foti, F.; Marti, M.; Ossato, A.; Bilel, S.; Sangiorgi, E.; Botrè, F.; Cerbelli, B.; Baldi, A.; De-Giorgio, F. Phenotypic effects of chronic and acute use of methiopropamine in a mouse model. Int. J. Legal Med. 2019, 133, 811–820. [Google Scholar] [CrossRef] [PubMed]
- Grafinger, K.E.; Liechti, M.E.; Liakoni, E. Clinical value of analytical testing in patients presenting with new psychoactive substances intoxication. Br. J. Clin. Pharmacol. 2020, 86, 429–436. [Google Scholar] [CrossRef] [PubMed]
- De-Giorgio, F.; Bilel, S.; Tirri, M.; Arfè, R.; Trapella, C.; Camuto, C.; Foti, F.; Frisoni, P.; Neri, M.; Botrè, F.; et al. Methiopropamine and its acute behavioral effects in mice: Is there a gray zone in new psychoactive substances users? Int. J. Legal Med. 2020, 134, 1695–1711. [Google Scholar] [CrossRef]
- De-Giorgio, F.; Bergamin, E.; Bilel, S.; Tirri, M.; Arfè, R.; Marchetti, B.; Corli, G.; Serpelloni, G.; Marti, M. Ethanol enhanced MDPV- and cocaine-induced aggressive behavior in mice: Forensic implications. Drug Alcohol Depend. 2021, 229, 109125. [Google Scholar] [CrossRef]
- Vidaki, A.; Kayser, M. From forensic epigenetics to forensic epigenomics: Broadening DNA investigative intelligence. Genome Biol. 2017, 18, 238. [Google Scholar] [CrossRef] [PubMed]
- Sabeeha; Hasnain, S.E. Forensic Epigenetic Analysis: The Path Ahead. Med. Princ. Pract. 2019, 28, 301–308. [Google Scholar] [CrossRef]
- Lee, H.Y.; Jung, S.-E.; Lee, E.H.; Yang, W.I.; Shin, K.-J. DNA methylation profiling for a confirmatory test for blood, saliva, semen, vaginal fluid and menstrual blood. Forensic Sci. Int. Genet. 2016, 24, 75–82. [Google Scholar] [CrossRef] [PubMed]
- Tachibana, M. Epigenetic regulation of mammalian sex determination. J. Med. Investig. 2015, 62, 19–23. [Google Scholar] [CrossRef][Green Version]
- Horvath, S. DNA methylation age of human tissues and cell types. Genome Biol. 2013, 14, R115, Erratum in Genome Biol. 2015, 16, 96. [Google Scholar] [CrossRef]
- Fraga, M.F.; Ballestar, E.; Paz, M.F.; Ropero, S.; Setien, F.; Ballestar, M.L.; Heine-Suñer, D.; Cigudosa, J.C.; Urioste, M.; Benitez, J.; et al. From The Cover: Epigenetic differences arise during the lifetime of monozygotic twins. Proc. Natl. Acad. Sci. USA 2005, 102, 10604–10609. [Google Scholar] [CrossRef]
- Liu, C.; Marioni, R.E.; Hedman, Å.K.; Pfeiffer, L.; Tsai, P.-C.; Reynolds, L.M.; Just, A.C.; Duan, Q.; Boer, C.G.; Tanaka, T.; et al. A DNA methylation biomarker of alcohol consumption. Mol. Psychiatry 2018, 23, 422–433. [Google Scholar] [CrossRef] [PubMed]
- Lee, K.W.; Pausova, Z. Cigarette smoking and DNA methylation. Front. Genet. 2013, 4, 132. [Google Scholar] [CrossRef] [PubMed]
- Harris, C. Animal Models in Epigenetic Research: Institutional Animal Care and Use Committee Considerations across the Lifespan. ILAR J. 2012, 53, 370–376. [Google Scholar] [CrossRef] [PubMed]
- Phillips, N.L.H.; Roth, T.L. Animal Models and Their Contribution to Our Understanding of the Relationship Between Environments, Epigenetic Modifications, and Behavior. Genes 2019, 10, 47. [Google Scholar] [CrossRef]
| Epigenetic Mechanisms | Epigenetic Modification | Effects on Gene Expression |
|---|---|---|
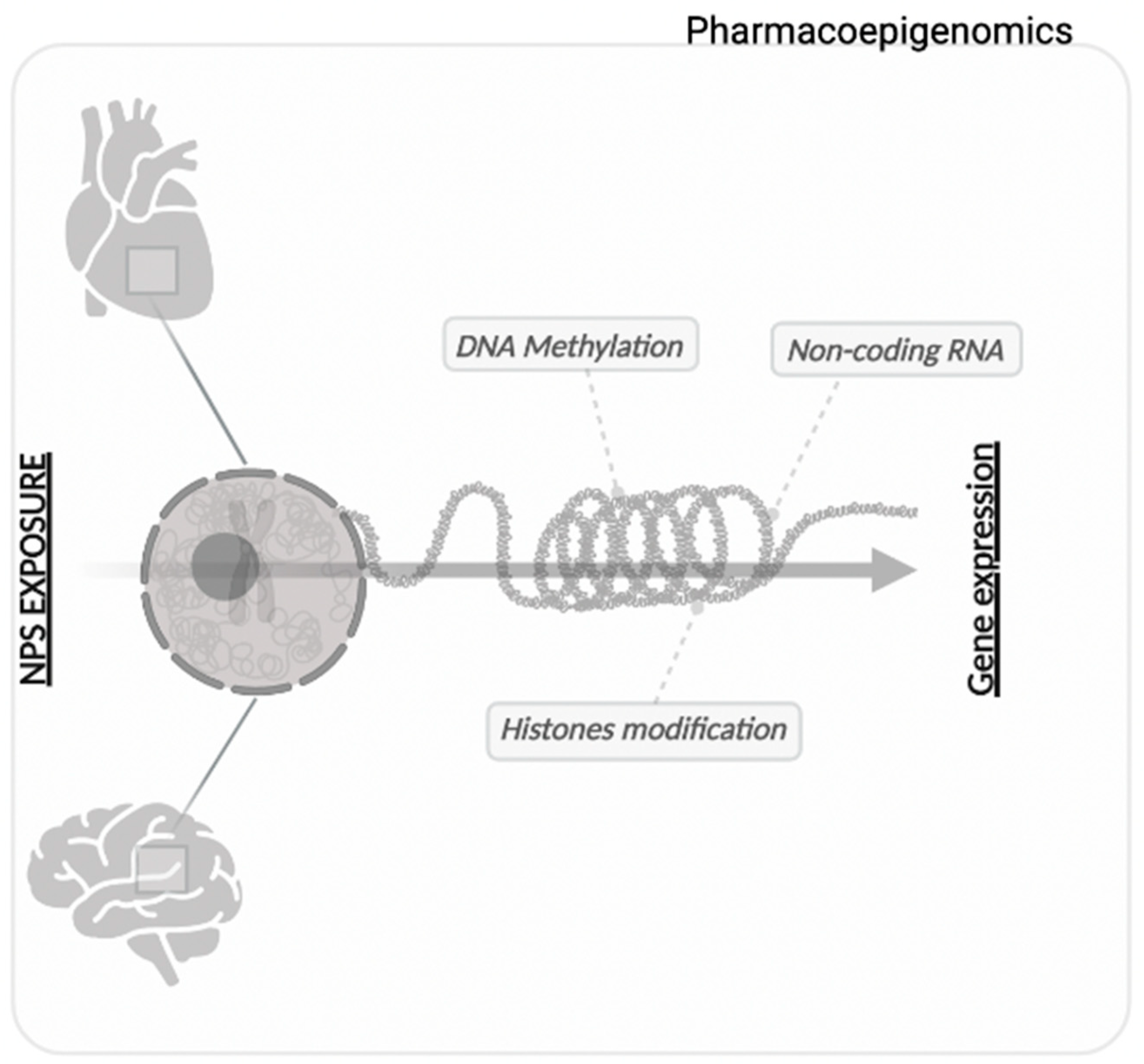
| Histone modification | Addition of an acetyl group (Ac) to the amine group of the lysine residues of histones H2B, H3 and H4; addition of one or more methyl groups (Me) on lysine or arginine residues preferentially found on histone tails. | Activation or repression of gene transcription. |
| DNA methylation | Addition of a methyl (Me) group that occurs preferentially in C- and G-rich genomic region CpG islands. | Gene repression. |
| Non-coding RNA | Different RNAs—not translated into proteins—that influence gene expression at the transcriptional and translational level. | Regulation of gene expression (miRNAs binds mRNAs in the 3’UTR region, which promotes their degradation or prevents their translation in protein). |
| Substance | Target | Epigenetic Modification | Effect | Animal Information | Tissue/Cell Type | DNA Methylation Method | References | ||
|---|---|---|---|---|---|---|---|---|---|
| Genotype | Gender | Age | |||||||
| Methamphetamine | GluA1 | Hypoacetylation H4 | Downregulation | Sprague–Dawley rats | Male | Adult | Striatum | Immunoblot/ChIP/Antibody | [114] |
| GluA2 | |||||||||
| Cocaine | fosB | Increased CBP acetylation H4 | Upregulation | C57BL/6J | Crossed C57BL6J mutant males with BALBc females to generate the F1 hybrids | Adult | Striatum | ChIP/qPCR/Immunoblotting | [118] |
| BALBc mice | |||||||||
| Cocaine | BDNF | Increased | Upregulation | Sprague–Dawley rats | Male | Adult 10–14 weeks old | Striatum | ChIP/qPCR/RT-PCR/immunohistochemistry | [119] |
| Cdk5 | Acetylation H4 | Bl6/C57 mice | |||||||
| Methamphetamine | 5 of IEGs | Increased DNA methylation | Downregulation | CD-1 mice | Male | Adult | PFC | RT2 Profiler PCR/qPCR/Pyrosequencing | [120] |
| Grm1 | Hippocampus | ||||||||
| Methamphetamine | FosB | Increased acetylation H4 | Upregulation | C57BL/6 mice | Male | Adult | Striatum | ChIP/Western Blot | [121] |
| Increase CREB phosphorylation | |||||||||
| Cocaine | N/A | DNMT3A | Downregulation | C57BL/6J mice and Long Evans rats | Male | Adult | NAc | ChIP promoter analysis/Global DNA methylation analysis | [126] |
| Increased DNA methylation | |||||||||
| Cocaine | 55 genes | TET1 | Downregulation Alternative splicing | C57BL/6J mice | Male | Adult 8–10 weeks old | NAc | qPCR/western blotting/immunohistochemistry/stereotaxic viral manipulations/ChIP-seq/RNA-seq | [129] |
| Increased DNA methylation | |||||||||
| Cocaine | PP1c | Increased DNA methylation DNMT3A and DNMT3B | Downregulation and Upregulation of FosB | Mice C57BL/6 | Male | Adult | NAc | qPCR/ChIP/MeDIP/western Blotting | [140] |
| Cocaine | Cdkl5 | Increased DNA methylation (MeCP2) | Downregulation | Wistar rats | Male | Adult 8–9 weeks old | NAc | RT-PCR—qPCR/Bisulfite sequencing/Chromatin immunoprecipitation/Immunohistochemistry | [141] |
| Cocaine | cFos, FosB, BDNF e Cdk5 | Increased Acetylation H3 and H4 | Upregulation | Sprague–Dawley rats | Male | Adult | Striatum | ChIP | [119] |
| Cocaine | ΔΦοσ | Increased Acetylation H3 and H4 | Upregulation: sirt1 sirt2 | C57BL/6 mice | Male | 10–12 weeks | NAc | ChIP/Array | [143] |
| CREB | |||||||||
| Cocaine | 172 genes | Decrease Histone Deacetylation HDAC5 | Upregulation | Mice C57BL/6 | N/A | Not adult | NAc | Western Blotting/Immunohistochemistry/ChIP/qPCR/RT-PCR/Microarrays | [142] |
| Cocaine | N/A | DNMT3B | Upregulation | C57/BL6 mice | Male | Adult | PFC | Global DNA methylation analysis, qPCR, Western blotting | [145] |
| Decrease DNA methylation | |||||||||
| Cocaine | 57 genes | DNMT3A Increased DNA methylation | Up-/downregulation | C57BL/6 mice | Male | Adult aged 5–6 months | NAc | MicroArray Illumina/qPCR/MeDIP | [146] |
| Cocaine | PKCε | Increased DNA methylation | Downregulation | Sprague–Dawley rats | Pregnant | Fetal (21 days) | Heart | Quantitative Methylation-Specific PCR/ChIP | [147] |
| Substance | Target | Epigenetic Modification | Effect | Animal Information | Tissue/Cell Type | DNA Methylation Method | References | ||
|---|---|---|---|---|---|---|---|---|---|
| Genotype | Gender | Age | |||||||
| Δ⁹--THC | Appbp2 CD27 | LncRNA | Downregulation of miR-17/92 cluster and miR-374b/421 cluster Up-regulation of miR-146 | C57BL/6J mice | Female | 6–7 weeks old | Lymph node cells CD4+ | RNA-seq | [128] |
| WIN55212.2 | Rgs7 | Hypermethylation | Downregulation | C57Bl6/J mice | Male | Adolescent aged 4 weeks | Hippocampal CA regions | qPCR/RT--PCR | [135] |
| Δ⁹--THC | Penk | Decrease H3K9 Methylation | Upregulation | Long Evans rats | Male | Adolescents 21-day-old | NAc | ChIP | [138] |
| Δ⁹--THC | N/A | H3K9me2 H3K9me3 H3K9ac H3K14ac | Both | Sprague–Dawley rats | Female | Adolescent (35–45 postnatal day) and adult (75–85 postnatal day) | Hippo NAc Amy | Western Blot | [148] |
| Δ⁹--THC | 177 genes | DNA Methylation | Both | Sprague–Dawley rats | Male | Nine-week-old, sexually mature | Semen | Bisulfite Sequencing/Pyrosequencing | [149] |
| JWH133 | CB2 | Upregulation of H3K4me3 Downregulating H3K9me2 | Upregulation Prdm9 c-Kit Stra8 | Swiss CD-1 mice | Male | Seven-day-old | SPG cells (Spermatogonia) | qPCR/RT--PCR/ChIP/Western Blot | [150] |
| Δ⁹--THC | Drd2 | Increased 2meH3K9 | Decrease 3meH3K4 | Long Evans rat | Male and female | Adult | NAc | In Situ Hybridization Histochemistr/ChIP/ | [151] |
| and mRNA level | |||||||||
| Δ⁹--THC | 1027 | DNA Methylation | Alterated | Long Evan rats | Male and female | Adolescent | NAc | Enhanced Reduced Representation Bisulfite Sequencing | [152] |
| genes | |||||||||
| Δ⁹--THC | Genes associated with plasticity | Increase Suv39H1 and H3K9me3 | Downregulation | Sprague-Dawley rats | Female | Adolescent and adult | PFC | RT2 Profile PCR Array/ChIP | [153] |
| HU-210 | Dlk1-Dio3-imprinted domain | Differential miRNA expression | Both | Wistar rats | Female Male | Pregnant Offspring | Left and right hemispheres of the entorhinal cortex (EC) | qPCR/RT--PCR | [154] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mazdai, L.; Fabbri, M.; Tirri, M.; Corli, G.; Arfè, R.; Marchetti, B.; Bilel, S.; Bergamin, E.; Gaudio, R.M.; Rubini, M.; et al. Epigenetic Studies for Evaluation of NPS Toxicity: Focus on Synthetic Cannabinoids and Cathinones. Biomedicines 2022, 10, 1398. https://doi.org/10.3390/biomedicines10061398
Mazdai L, Fabbri M, Tirri M, Corli G, Arfè R, Marchetti B, Bilel S, Bergamin E, Gaudio RM, Rubini M, et al. Epigenetic Studies for Evaluation of NPS Toxicity: Focus on Synthetic Cannabinoids and Cathinones. Biomedicines. 2022; 10(6):1398. https://doi.org/10.3390/biomedicines10061398
Chicago/Turabian StyleMazdai, Leila, Matteo Fabbri, Micaela Tirri, Giorgia Corli, Raffaella Arfè, Beatrice Marchetti, Sabrine Bilel, Eva Bergamin, Rosa Maria Gaudio, Michele Rubini, and et al. 2022. "Epigenetic Studies for Evaluation of NPS Toxicity: Focus on Synthetic Cannabinoids and Cathinones" Biomedicines 10, no. 6: 1398. https://doi.org/10.3390/biomedicines10061398
APA StyleMazdai, L., Fabbri, M., Tirri, M., Corli, G., Arfè, R., Marchetti, B., Bilel, S., Bergamin, E., Gaudio, R. M., Rubini, M., De-Giorgio, F., & Marti, M. (2022). Epigenetic Studies for Evaluation of NPS Toxicity: Focus on Synthetic Cannabinoids and Cathinones. Biomedicines, 10(6), 1398. https://doi.org/10.3390/biomedicines10061398









