The Digital Divide in the Era of COVID-19: An Investigation into an Important Obstacle to the Access to the mHealth by the Citizen
Abstract
1. Introduction
1.1. Work, School, Social Communication
1.2. Connection to Health Services
1.3. New Services for Epidemiological Monitoring
1.4. Access to Resources
1.5. Social Factors
1.6. Cultural Factors
1.7. Disabilities
2. Purpose of the Study
- (1)
- The impact of bandwidth limitations [13]
- (2)
- The attitude, knowledge and practice towards COVID-19 [14].
- (3)
- Learning methods [15].
- (4)
- The racial and ethnic differences in the comparisons of posts shared on COVID-19 [16].
- (5)
- The racial and ethnic differences in the areas of remote assistance during the COVID-19 pandemic [17].
- focused on a specific aspect (bandwidth problems, training, remote assistance, information sharing on COVID-19);
- does not seem to have concretely addressed the limits of administration bias through multimedia technologies which hinder the type of population affected by DD.
- (1)
- Propose a survey tool that addresses in an articulated way the problems that seem to be at the basis of the digital divide.
- (2)
- Propose a tool that minimizes the bias problems that may arise with purely electronic administrations (also used for social distancing)
- (3)
- Test this instrument referred to in the previous points (a, b) on a sample of subjects and also evaluate its robustness.
- (4)
- Analyze the overall results with particular reference to familiarity in the use of tools/Apps that are key elements of mHealth in the pandemic period.
- (5)
- Highlight the ability to categorize this familiarity into two important sub-samples represented by young and elderly people.
3. Materials and Methods
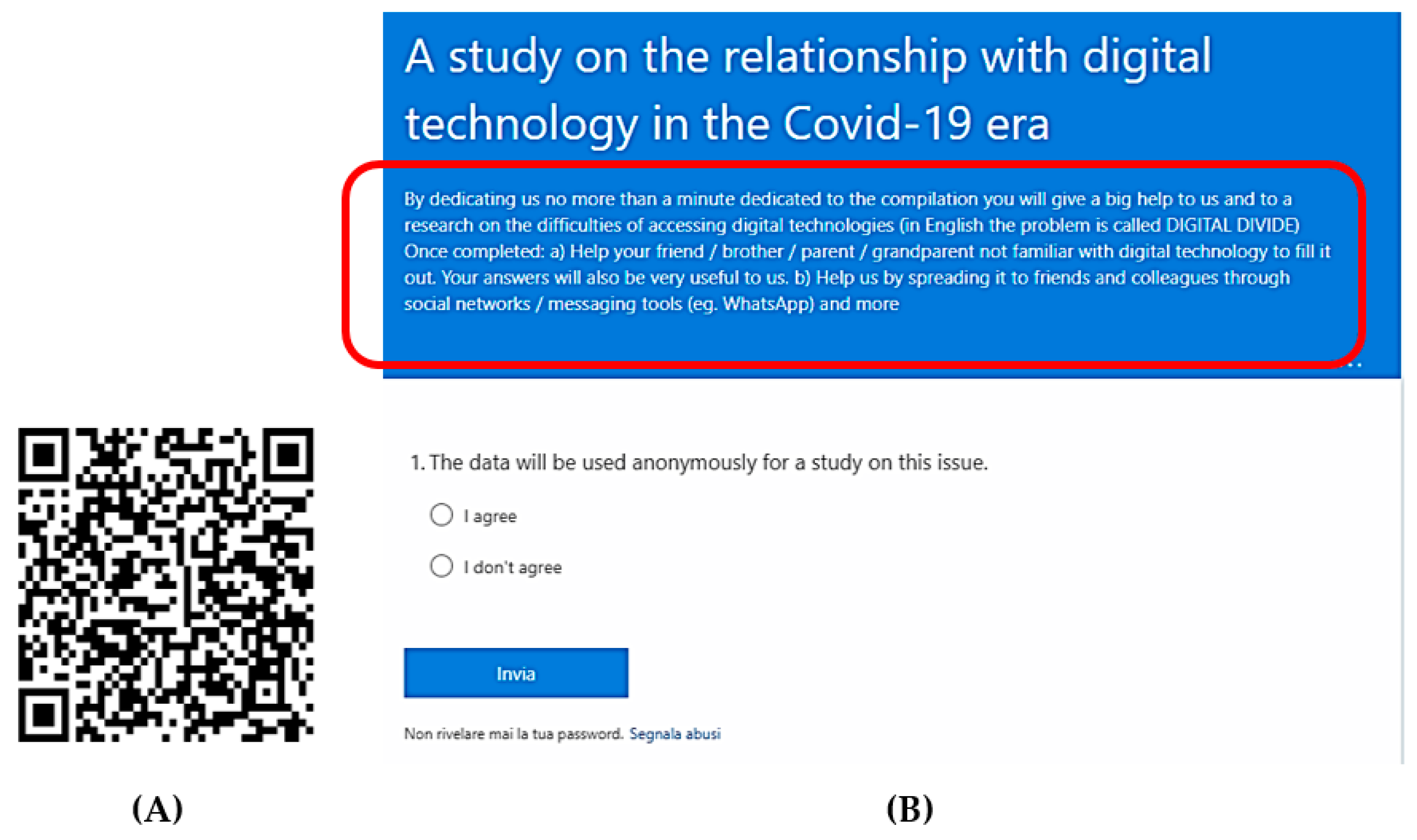
- The first solution is based on an electronic survey (eS) highlighting in the introduction to the receivers to spread it peer to peer within the domain of their acquaintances (family and friends) and supporting them in case of difficulties with the interaction with digital technology.
- The second solution is based on a telephone administration using the fixed network, obtaining fixed numbers from public registers randomly and requesting the same content.
3.1. Electronic Submission (ES)
3.2. Phone Submission (PS) Using a Wire Call
3.3. Methodological Flow
- (1)
- Verification of data normality.
- (2)
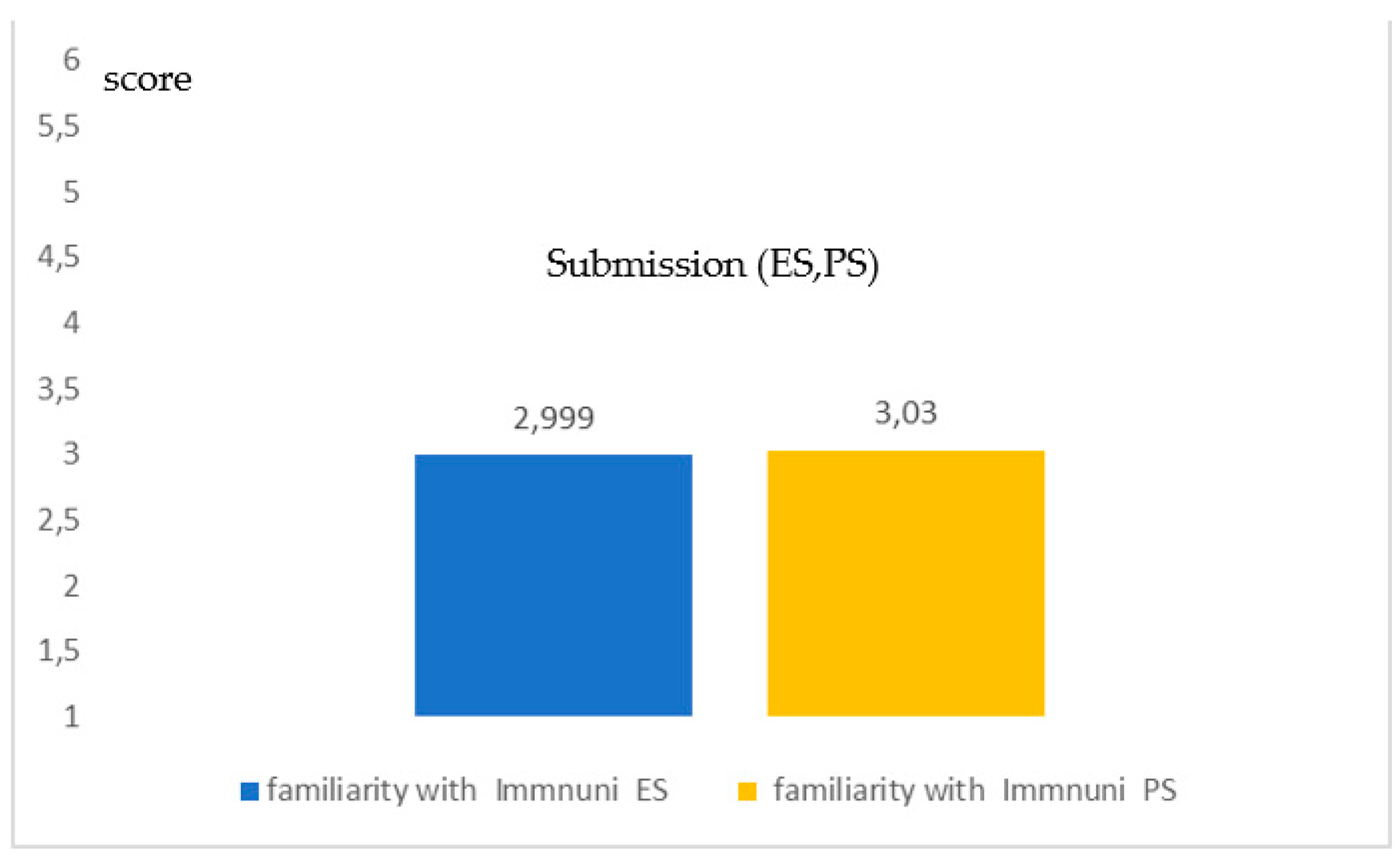
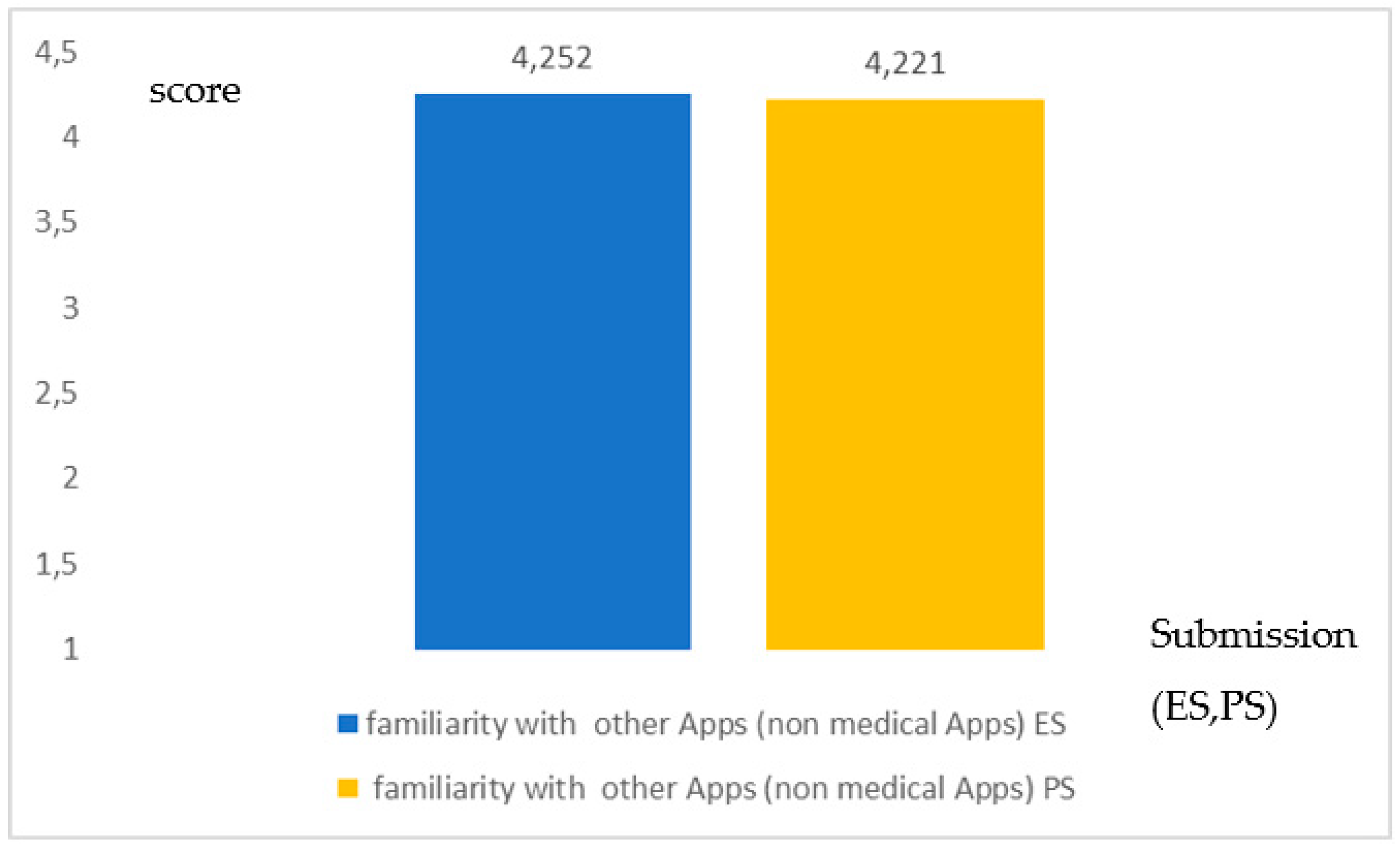
- Application of the T-student for the assessment of the coherence (not difference) with a p value higher than 0.1, when comparing ES and PS.
4. Results and Discussion
4.1. General Outcome
- A little familiarity and trust, all Italian, towards Immuni, an App for digital contact tracing, a problem that the stakeholder will then have to face.
- A low familiarity with mHealth Apps and this, in a pandemic time, where portable health could make a difference [4], is certainly another point that needs to be explored.
- A familiarity just above the threshold with regard to digital health processes in which we interact through digital health, which today have become essential for obtaining for example electronic prescriptions, for accessing blood tests and now also for vaccination.
4.2. In-Depth Study in Two Sub-Samples: Young People and the Elderly against the Digital Divide
- The first sample related to young people (aged 15–25 years): 413 subjects (201 males and 212 females), mean age 20.5 years, standard deviation 2.2; in what follows we refer to this sample as the young.
- The second sample related to elderly people (aged between 65 and 75 years): 382 subjects (199 females and 183 males), mean age 70.2 years, standard deviation 2.1; in what follows we refer to this sample with the term the elderly.
4.3. Intergroup Comparison
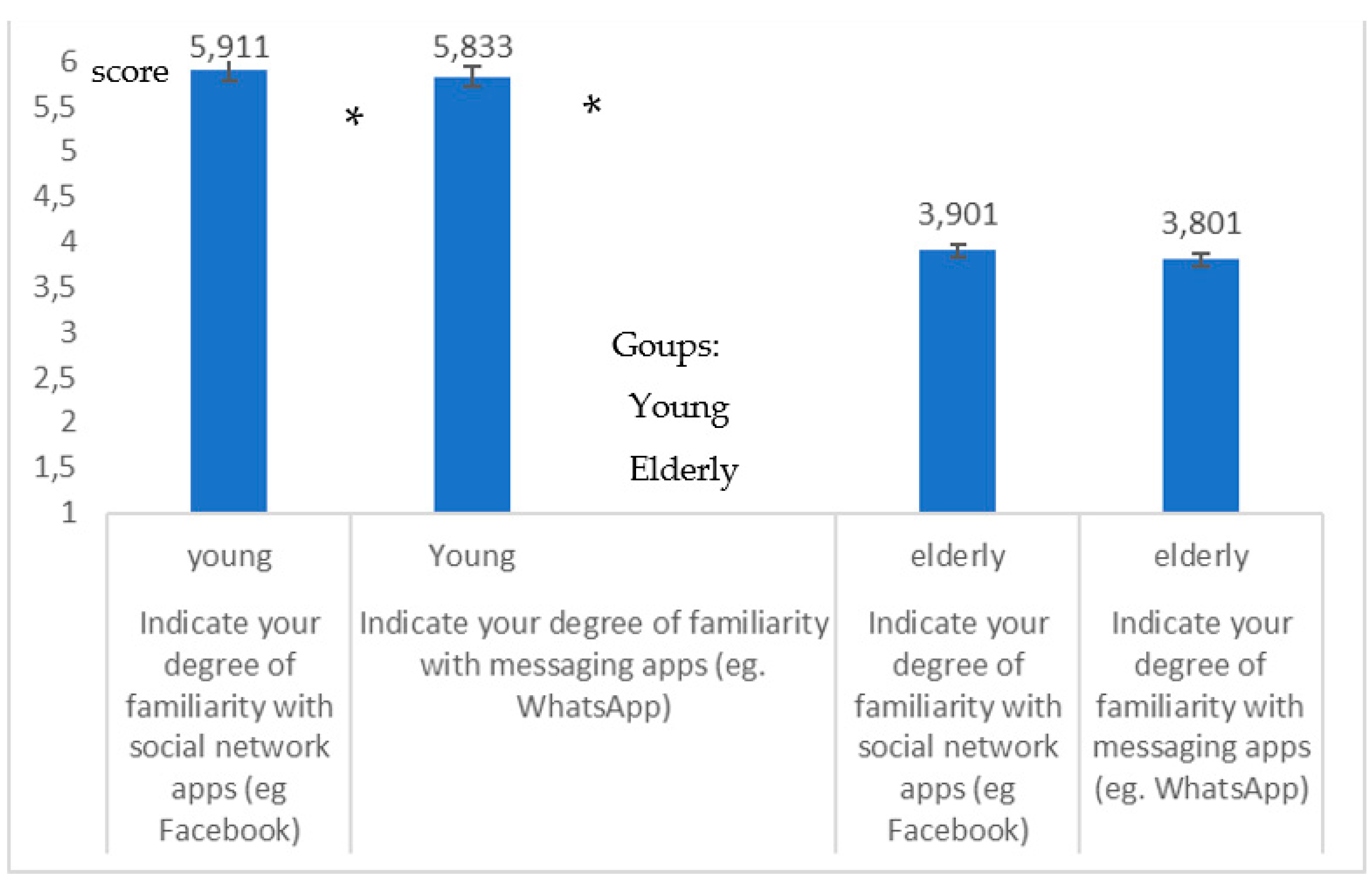
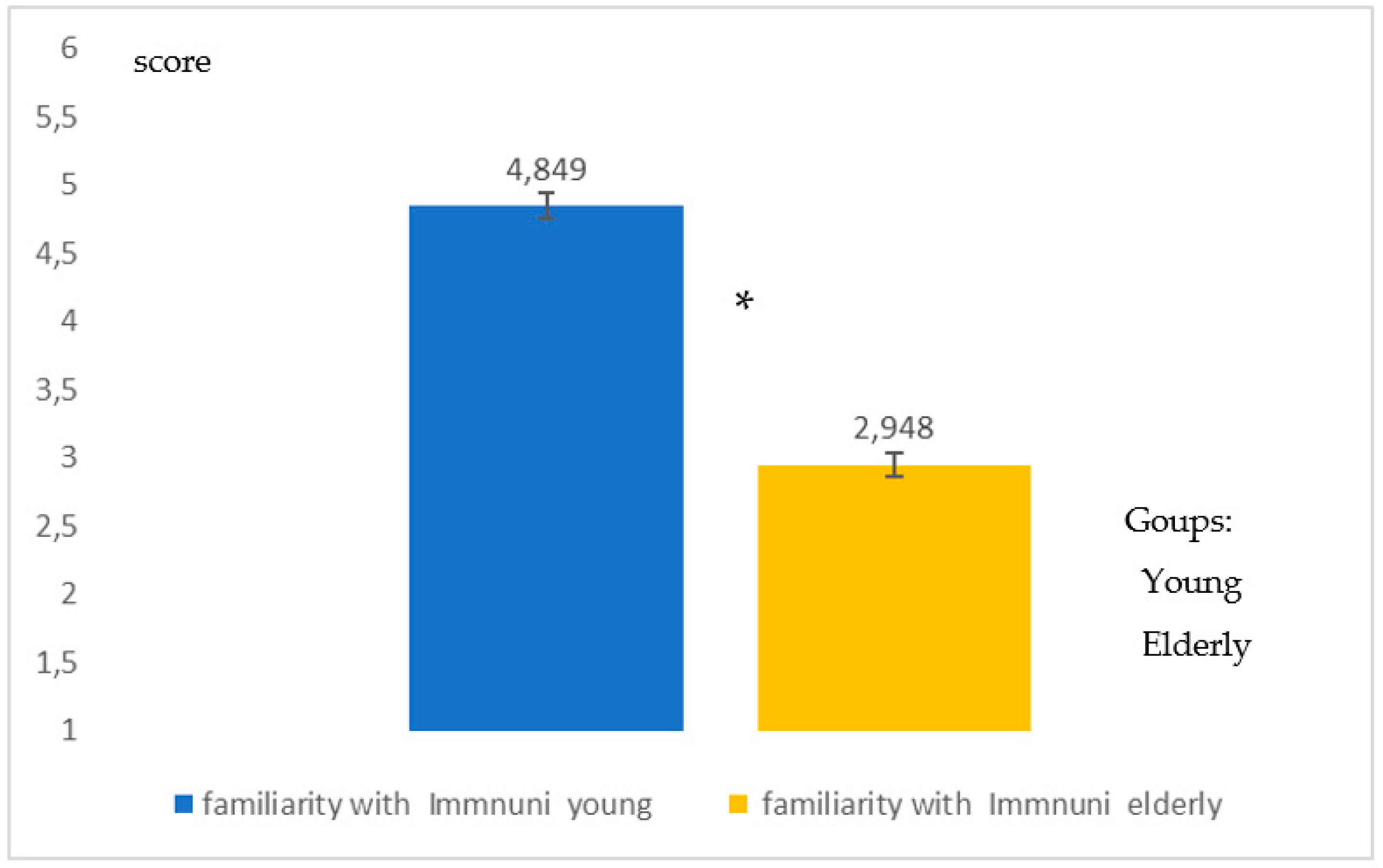
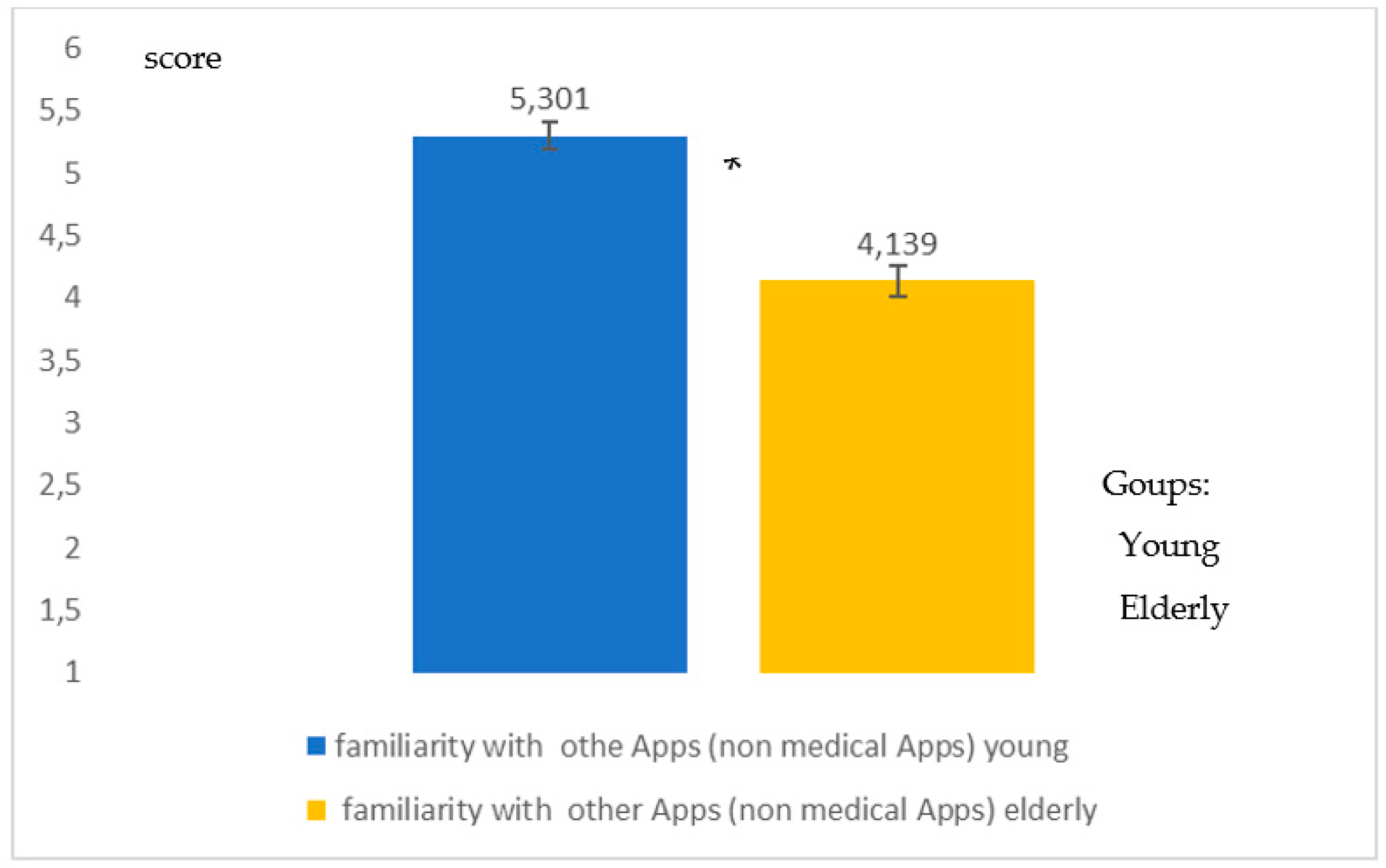
- An evident lower degree of familiarity on the part of the elderly with regard to mobile technology, mHealth, apps for DCT (Immuni) and digital processes.
- A great familiarity of young people with regard to mobile technology and in particular the social and messaging apps
- Young people are less familiar with the App Immuni than with social and messaging apps.
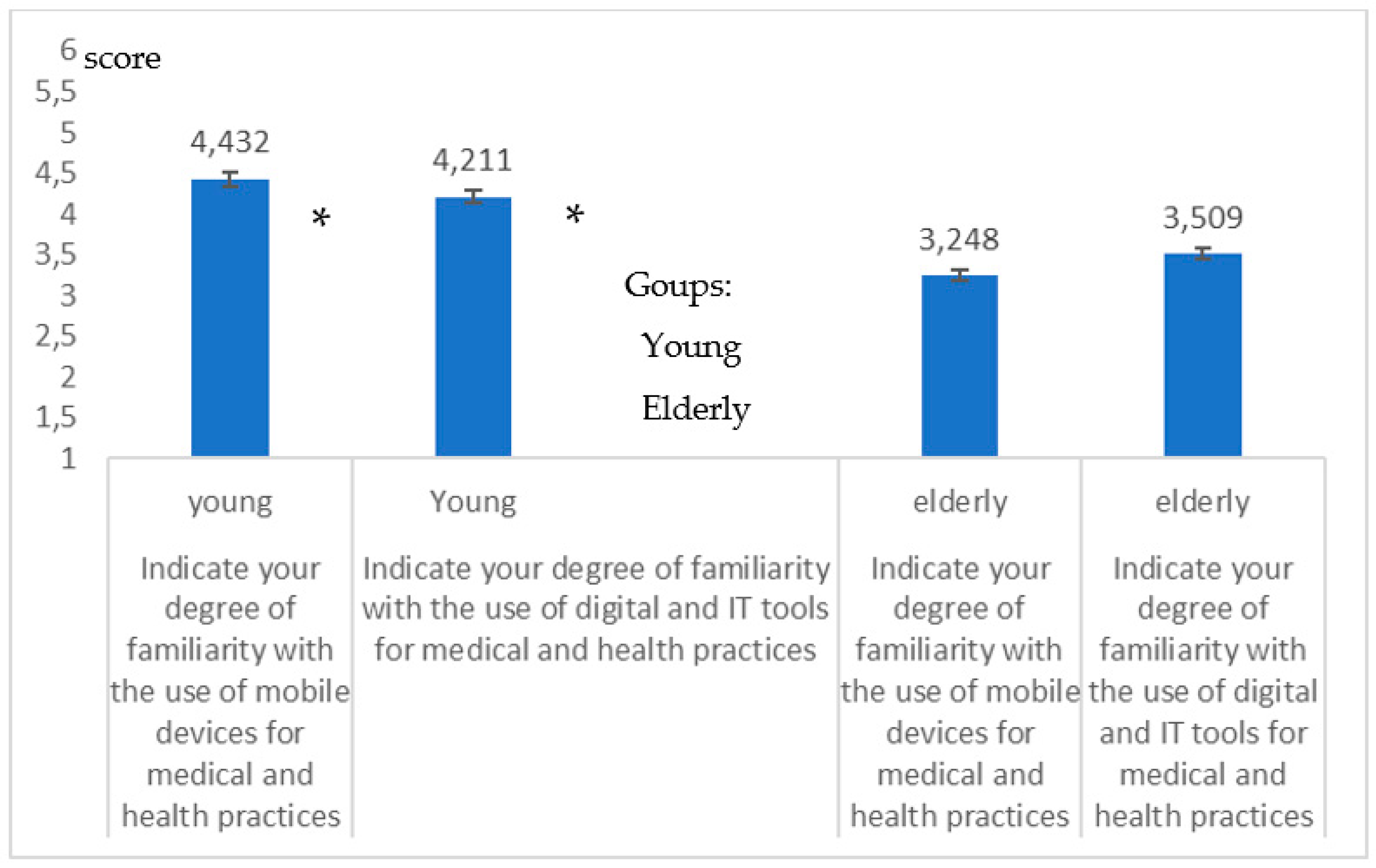
- The gap in the score between young and old falls when considering mHealth and digital health. This presumably, is explained by a greater need on the part of the elderly to be connected to health processes whose digitization pushes them towards a forced familiarization. The last aspect shown in the table relating to digital health (in which the difference in score between young and elderly is only 0.7 of average) seems to highlight this: the elderly must connect with the health system for medical prescriptions, to obtain the results of the analyses, and now also to be vaccinated against SARS-CoV-2. However, this also highlights a loss of resources and opportunities, in fact young people, if they were adequately familiar with these technologies could for the elderly, also represent valid support here.
5. Conclusions
5.1. Why the Need of a Study on the Digital Divide
5.2. What Has Been Proposed in the Study to Investigate the Digital Divide
5.3. What Are the Highlights from the Study?
- An unexpected low familiarity with mHealth Apps, and this worries us as this medical technology could make a difference [4]. This is certainly another point that needs to be explored.
- A familiarity just above the threshold with regard to digital health processes
- An evident lower degree of familiarity on the part of the elderly with regard to mobile technology, mHealth, Apps for DCT (Immuni) and digital processes.
- A great familiarity of young people with regard to mobile technology and in particular social and messaging apps, however not so great in the case of the App Immuni.
- The gap in the score between young and elderly falls when considering mHealth and digital health. This is particularly evident for Digital Health (in which the difference in score between the young and old is only 0.7 on average). This probably depends on the fact that the elderly, due to their having greater health problems, are more forced to interact with the medical digital processes for receiving analyses, online reservations, medical prescriptions and now also vaccines.
- Minimize the digital divide in general from a general point of view and, in particular, where major criticalities have been highlighted, such as in mHealth.
- Minimize the digital divide on some categories, such as in this case the category of the elderly by acting in an incisive way on the range of wider problems.
5.4. What Are the Added Values of the Study?
5.5. What the Study Supports and the Further Initiatives
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Bashshur, R.; Doarn, C.R.; Frenk, J.M.; Kvedar, J.C.; Woolliscroft, J.O. Telemedicine and the COVID-19 Pandemic, Lessons for the Future. Telemed. e-Health 2020, 26, 571–573. [Google Scholar] [CrossRef]
- Giansanti, D.; Aprile, I. Letter to the Editor: Is the COVID-19 Pandemic an Opportunity to Enlarge the Telemedicine Boundaries? Telemed. e-Health 2020, 26, 1123–1125. [Google Scholar] [CrossRef]
- Giansanti, D. The Italian Fight against the COVID-19 Pandemic in the Second Phase: The Renewed Opportunity of Telemedicine. Telemed. e-Health 2020, 26, 1328–1331. [Google Scholar] [CrossRef]
- Giansanti, D. The Role of the mHealth in the Fight against the Covid-19: Successes and Failures. Healthcare 2021, 9, 58. [Google Scholar] [CrossRef]
- Gabbiadini, A.; Baldissarri, C.; Durante, F.; Valtorta, R.R.; De Rosa, M.; Gallucci, M. Together Apart: The Mitigating Role of Digital Communication Technologies on Negative Affect During the COVID-19 Outbreak in Italy. Front. Psychol. 2020, 11, 554678. [Google Scholar] [CrossRef] [PubMed]
- Shah, S.G.S.; Nogueras, D.; Van Woerden, H.C.; Kiparoglou, V. The COVID-19 Pandemic—A pandemic of lockdown loneliness and the role of digital technology: A viewpoint (Preprint). J. Med. Internet Res. 2020, 22, e22287. [Google Scholar] [CrossRef]
- Braithwaite, I.; Callender, T.; Bullock, M.; Aldridge, R.W. Automated and partly automated contact tracing: A systematic review to inform the control of COVID-19. Lancet Digit. Heal. 2020, 2, e607–e621. [Google Scholar] [CrossRef]
- Kondylakis, H.; Katehakis, D.G.; Kouroubali, A.; Logothetidis, F.; Triantafyllidis, A.; Kalamaras, I.; Votis, K.; Tzovaras, D. COVID-19 Mobile Apps: A Systematic Review of the Literature. J. Med. Internet Res. 2020, 22, e23170. [Google Scholar] [CrossRef] [PubMed]
- Lai, J.; Widmar, N.O. Revisiting the Digital Divide in the COVID-19 Era. Appl. Econ. Perspect. Policy 2020, 43, 458–464. [Google Scholar] [CrossRef] [PubMed]
- Van Deursen, A.J.; van Dijk, J.A. The first-level digital divide shifts from inequalities in physical access to inequalities in ma-terial access. New Media Soc. 2019, 21, 354–375. [Google Scholar] [CrossRef] [PubMed]
- Shek, D.T.L. COVID-19 and Quality of Life: Twelve Reflections. Appl. Res. Qual. Life 2021, 16, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Bakhtiar, M.; Elbuluk, N.; Lipoff, J.B. The digital divide: How COVID-19’s telemedicine expansion could exacerbate disparities. J. Am. Acad. Dermatol. 2020, 83, e345–e346. [Google Scholar] [CrossRef]
- Reddick, C.G.; Enriquez, R.; Harris, R.J.; Sharma, B. Determinants of broadband access and affordability: An analysis of a commu-nity survey on the digital divide. Cities 2020, 106, 102904. [Google Scholar] [CrossRef] [PubMed]
- Fatmi, Z.; Mahmood, S.; Hameed, W.; Qazi, I.; Siddiqui, M.; Dhanwani, A.; Siddiqi, S. Knowledge, attitudes and practices towards COVID-19 among Pakistani residents: Information access and low literacy vulnerabilities. East Mediterr. Health J. 2020, 26, 1446–1455. [Google Scholar] [CrossRef]
- Bonal, X.; González, S. The impact of lockdown on the learning gap: Family and school divisions in times of crisis. Int. Rev. Educ. 2020, 66, 635–655. [Google Scholar] [CrossRef]
- Campos-Castillo, C.; Laestadius, L.I. Racial and Ethnic Digital Divides in Posting COVID-19 Content on Social Media among US Adults: Secondary Survey Analysis. J. Med. Internet Res. 2020, 22, e20472. [Google Scholar] [CrossRef] [PubMed]
- Campos-Castillo, C.; Anthony, D. Racial and ethnic differences in self-reported telehealth use during the COVID-19 pandemic: A secondary analysis of a US survey of internet users from late March. J. Am. Med. Inform. Assoc. 2021, 28, 119–125. [Google Scholar] [CrossRef]
- Begay, M.; Kakol, M.; Sood, A.; Upson, D. Strengthening Digital Health Technology Capacity in Navajo Communities to Help Counter the COVID-19 Pandemic. Ann. Am. Thorac. Soc. 2021. [Google Scholar] [CrossRef] [PubMed]
- Nachega, J.B.; Atteh, R.; Ihekweazu, C.; Sam-Agudu, N.A.; Adejumo, P.; Nsanzimana, S.; Rwagasore, E.; Condo, J.; Paleker, M.; Mahomed, H.; et al. Contact Tracing and the COVID-19 Response in Africa: Best Practices, Key Challenges, and Lessons Learned from Nigeria, Rwanda, South Africa, and Uganda. Am. J. Trop. Med. Hyg. 2021. [Google Scholar] [CrossRef] [PubMed]
- Braune, K.; Boss, K.; Schmidt-Herzel, J.; Gajewska, K.A.; Thieffry, A.; Schulze, L.; Posern, B.; Raile, K. Shaping Workflows in Digital and Remote Diabetes Care During the COVID-19 Pandemic: A Service Design Approach. (Preprint). JMIR mHealth uHealth 2020. [Google Scholar] [CrossRef] [PubMed]
- Rosman, L.; Armbruster, T.; Kyazimzade, S.; Tugaoen, Z.; Mazzella, A.J.; Deyo, Z.; Walker, J.; Machineni, S.; Gehi, A. Effect of a virtual self-management intervention for atrial fibrillation during the outbreak of COVID-19. Pacing Clin. Electrophysiol. 2021, 44, 451–461. [Google Scholar] [CrossRef]
- Khanna, R.; Forbes, M. Telepsychiatry as a public health imperative: Slowing COVID-19. Aust. N. Z. J. Psychiatry 2020, 54, 758. [Google Scholar] [CrossRef]
- Bäuerle, A.; Graf, J.; Jansen, C.; Dörrie, N.; Junne, F.; Teufel, M.; Skoda, E.-M. An e-mental health intervention to support burdened people in times of the COVID-19 pandemic: CoPE It. J. Public Heal. 2020, 42, 647–648. [Google Scholar] [CrossRef]
- Zhou, X.; Snoswell, C.L.; Harding, L.E.; Bambling, M.; Edirippulige, S.; Bai, X.; Smith, A.C. The role of telehealth in reducing the mental health burden from COVID-19. Telemed. e-Health 2020, 26, 377–379. [Google Scholar] [CrossRef] [PubMed]
- Saleem, S.M.; Pasquale, L.R.; Sidoti, P.A.; Tsai, J.C. Virtual Ophthalmology: Telemedicine in a COVID-19 Era. Am. J. Ophthalmol. 2020, 216, 237–242. [Google Scholar] [CrossRef] [PubMed]
- Gupta, M.; Shoja, A.; Mikalef, P. Toward the understanding of national culture in the success of non-pharmaceutical technological interventions in mitigating COVID-19 pandemic. Ann. Oper. Res. 2021, 3, 1–18. [Google Scholar] [CrossRef]
- Chen, J.; Hoops, S.; Marathe, A.; Mortveit, H.; Lewis, B.; Venkatramanan, S.; Haddadan, A.; Bhattacharya, P.; Adiga, A.; Vullikanti, A.; et al. Prioritizing allocation of COVID-19 vaccines based on social contacts increases vaccination effectiveness. medRxiv 2021. [Google Scholar] [CrossRef]
- Available online: https://www.immuni.italia.it/ (accessed on 25 March 2021).
- Giansanti, D.; Maccioni, G. Health in the palm of your hand—part 2: Design and application of an educational module for young people on the risks from smartphone abuse and the opportunities of telemedicine and e-Health. mHealth 2021. Available online: https://mhealth.amegroups.com/article/view/61063/44616 (accessed on 16 March 2021).
- Giansanti, D.; Maccioni, G. Health in the palm of your hand—Part 1: The risks from smartphone abuse and the role of telemed-icine and e-Health. mHealth. 2021. Available online: https://mhealth.amegroups.com/article/view/63693/47633 (accessed on 16 March 2021).
- Toh, S.H.; Coenen, P.; Howie, E.K.; Straker, L.M. The associations of mobile touch screen device use with musculoskeletal symptoms and exposures: A systematic review. PLoS ONE 2017, 12, e0181220. [Google Scholar] [CrossRef]
- Neupane, S.; Ali, U.T.I.; Mathew, A. Text-Neck syndrome- systemic review. Imp. J. Interdiscip. Res. 2017, 3, 141–148. [Google Scholar]
- De Pasquale, C.; Sciacca, F.; Hichy, Z. Smartphone addiction and dissociative experience: An investigation in Italian adolescent aged between 14 and 19 years. Int. J. Psychol. Behav. Anal. 2015, 1, 109. [Google Scholar] [CrossRef]


| Submission | Number Invited | Participants | Males/Females | Min Age/Max Age | Mean Age | Notes |
|---|---|---|---|---|---|---|
| Electronic submission Using the smartphone | 4555 | 4512 | 2311/2201 | 12/85 | 49.3 | No anomalies |
| Phone (Wire call) | 1337 | 1312 | 642/670 | 12/84 | 48.9 | No anomalies |
| Social Media | Messaging | Immuni | Non-Medical Apps | mHealth | Digital Health | |
|---|---|---|---|---|---|---|
| Young | 5.9 | 5.8 | 4.8 | 5.3 | 4.4 | 4.2 |
| Elderly | 3.9 | 3.8 | 2,9 | 4.1 | 3.2 | 3.5 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Giansanti, D.; Veltro, G. The Digital Divide in the Era of COVID-19: An Investigation into an Important Obstacle to the Access to the mHealth by the Citizen. Healthcare 2021, 9, 371. https://doi.org/10.3390/healthcare9040371
Giansanti D, Veltro G. The Digital Divide in the Era of COVID-19: An Investigation into an Important Obstacle to the Access to the mHealth by the Citizen. Healthcare. 2021; 9(4):371. https://doi.org/10.3390/healthcare9040371
Chicago/Turabian StyleGiansanti, Daniele, and Giulia Veltro. 2021. "The Digital Divide in the Era of COVID-19: An Investigation into an Important Obstacle to the Access to the mHealth by the Citizen" Healthcare 9, no. 4: 371. https://doi.org/10.3390/healthcare9040371
APA StyleGiansanti, D., & Veltro, G. (2021). The Digital Divide in the Era of COVID-19: An Investigation into an Important Obstacle to the Access to the mHealth by the Citizen. Healthcare, 9(4), 371. https://doi.org/10.3390/healthcare9040371






