Home Hospitalization for Acute Decompensated Heart Failure: Opportunities and Strategies for Improved Health Outcomes
Abstract
:1. Introduction
2. Home Hospitalization–Definition
- It provides care that substitutes entirely for an inpatient acute hospital admission;
- It provides an intensity of care, including medical and nursing care, similar to that provided in the hospital;
- It provides care that cannot be provided by usual community-based home-care services [17].
3. Home Hospitalization—Feasibility and Effectiveness
4. Home Hospitalization and Heart Failure
5. Patients’ Selection
6. Limitations
7. Looking Forward
- Resolve challenges with the supply chain going into the home (it is currently tuned for a “post-acute” versus “acute care” reality).
- Lack of a readily accessible reimbursement schema/coding system that aligns the clinical, financial and satisfaction benefits of the model with the current payment system. Current health care financing does envision a “bundled” care plan but not a comprehensive, single episode of care based in a patient’s home.
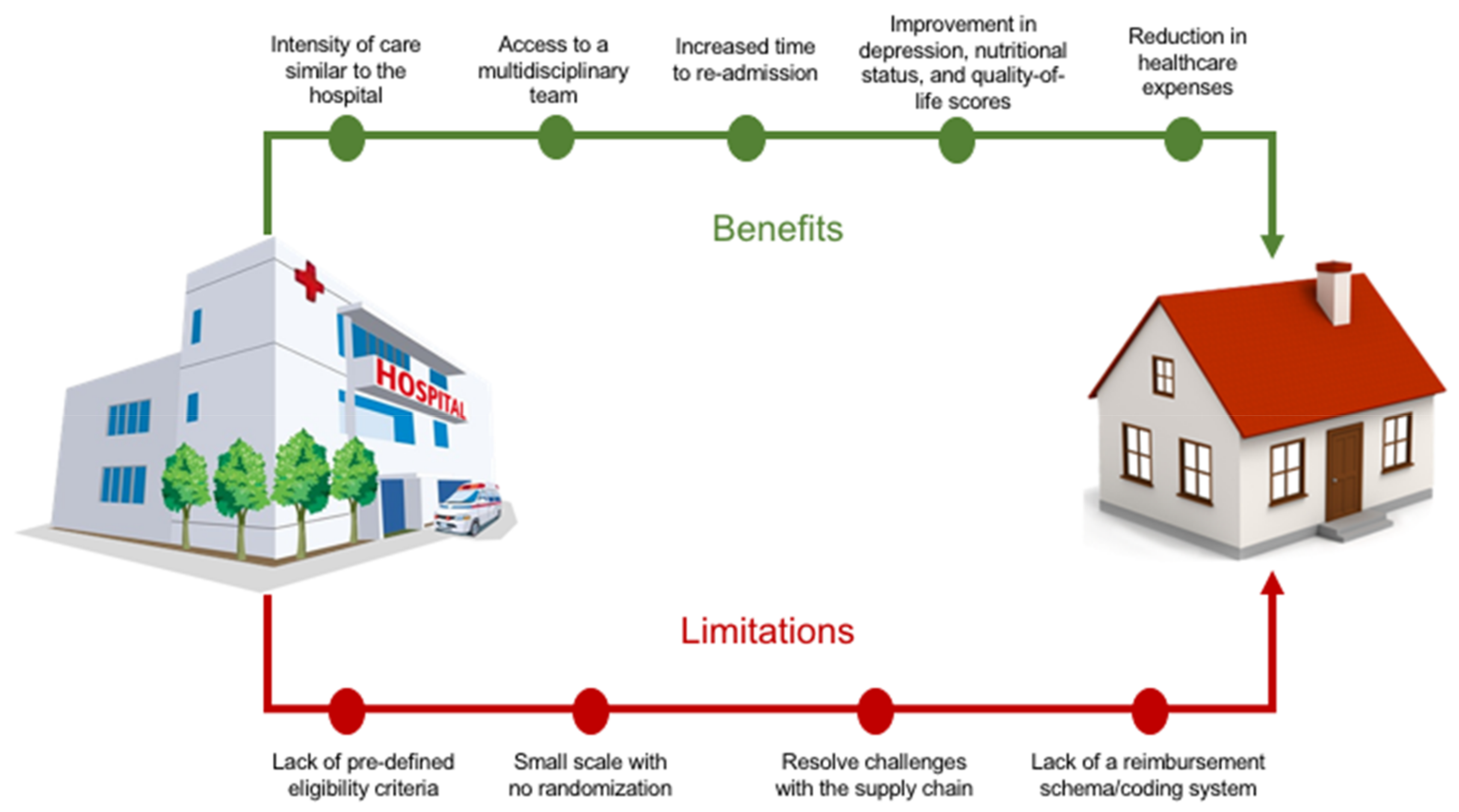
- The critical need to integrate the restorative phase of care with the acute phase using a single care team. A common failure mode is the step off in coordination and understanding of the patients (and family’s) needs to truly recover and prevent future acute exacerbations. There are currently significant limitations in care management and transition plans difficult to overcome in current models (Figure 1).
8. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Yancy, C.W.; Jessup, M.; Bozkurt, B.; Butler, J.; Casey, D.E.; Drazner, M.H.; Fonarow, G.C.; Geraci, S.A.; Horwich, T.; Januzzi, J.L.; et al. 2013 ACCF/AHA guideline for the management of heart failure: A Report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J. Am. Coll. Cardiol. 2013, 62, e147–e239. [Google Scholar] [CrossRef] [PubMed]
- Nieminen, M.S.; Harjola, V.P. Definition and epidemiology of acute heart failure syndromes. Am. J. Cardiol. 2005, 96, 5–10. [Google Scholar] [CrossRef] [PubMed]
- Mozaffarian, D.; Benjamin, E.J.; Go, A.S.; Arnett, D.K.; Blaha, M.J.; Cushman, M.; Das, S.R.; de Ferranti, S.; Després, J.-P.; Fullerton, H.J.; et al. Heart disease and stroke statistics—2016 update: A Report from the American Heart Association. Circulation 2016, 133, e38–e360. [Google Scholar] [CrossRef] [PubMed]
- Abete, P.; Testa, G.; Della-Morte, D.; Gargiulo, G.; Galizia, G.; de Santis, D.; Magliocca, A.; Basile, C.; Cacciatore, F. Treatment for chronic heart failure in the elderly: Current practice and problems. Heart Fail. Rev. 2013, 18, 529–551. [Google Scholar] [CrossRef] [PubMed]
- Cook, C.; Cole, G.; Asaria, P.; Jabbour, R.; Francis, D.P. The annual global economic burden of heart failure. Int. J. Cardiol. 2014, 171, 368–376. [Google Scholar] [CrossRef] [PubMed]
- Neumann, T.; Biermann, J.; Erbel, R.; Neumann, A.; Wasem, J.; Ertl, G.; Dietz, R. Heart failure: The commonest reason for hospital admission in Germany: Medical and economic perspectives. Dtsch. Arzteblatt Int. 2009, 106, 269–275. [Google Scholar]
- Benjamin, E.J.; Blaha, M.J.; Chiuve, S.E.; Cushman, M.; Das, S.R.; Deo, R.; de Ferranti, S.D.; Floyd, J.; Fornage, M.; Gillespie, C.; et al. Heart disease and stroke statistics—2017 update: A report from the American heart association. Circulation 2017, 135, e146–e603. [Google Scholar] [CrossRef] [PubMed]
- Heidenreich, P.A.; Albert, N.M.; Allen, L.A.; Bluemke, D.A.; Butler, J.; Fonarow, G.C.; Ikonomidis, J.S.; Khavjou, O.; Konstam, M.A.; Maddox, T.M.; et al. Forecasting the impact of heart failure in the united states: A policy statement from the American heart association. Circ. Heart Fail. 2013, 6, 606–619. [Google Scholar] [CrossRef] [PubMed]
- Krumholz, H.M.; Merrill, A.R.; Schone, E.M.; Schreiner, G.C.; Chen, J.; Bradley, E.H.; Wang, Y.; Wang, Y.; Lin, Z.; Straube, B.M.; et al. Patterns of hospital performance in acute myocardial infarction and heart failure 30-day mortality and readmission. Circ. Cardiovasc. Qual. Outcomes 2009, 2, 407–413. [Google Scholar] [CrossRef] [PubMed]
- Joynt, K.E.; Jha, A.K. Who has higher readmission rates for heart failure, and why? Implications for Efforts to Improve Care Using Financial Incentives. Circ. Cardiovasc. Qual. Outcomes 2011, 4, 53–59. [Google Scholar] [CrossRef] [PubMed]
- Chun, S.; Tu, J.V.; Wijeysundera, H.C.; Austin, P.C.; Wang, X.; Levy, D.; Lee, D.S. Lifetime analysis of hospitalizations and survival of patients newly admitted with heart failure. Circ. Heart Fail. 2012, 5, 414–421. [Google Scholar] [CrossRef] [PubMed]
- Bodenheimer, T.; Wagner, E.H.; Grumbach, K. Improving primary care for patients with chronic illness: The chronic care model, part 2. JAMA 2002, 288, 1909–1914. [Google Scholar] [CrossRef] [PubMed]
- Brennan, T.A.; Leape, L.L.; Laird, N.M.; Hebert, L.; Localio, A.R.; Lawthers, A.G.; Newhouse, J.P.; Weiler, P.C.; Hiatt, H.H. Incidence of adverse events and negligence in hospitalized patients: Results of the Harvard medical practice study I. 1991. Qual. Saf. Health Care 2004, 13, 145–151. [Google Scholar] [CrossRef] [PubMed]
- Rothschild, J.M.; Bates, D.W.; Leape, L.L. Preventable medical injuries in older patients. Arch. Intern. Med. 2000, 160, 2717–2728. [Google Scholar] [CrossRef] [PubMed]
- Leff, B. Acute? Care at home. The health and cost effects of substituting home care for inpatient acute care: A review of the evidence. J. Am. Geriatr. Soc. 2001, 49, 1123–1125. [Google Scholar] [CrossRef] [PubMed]
- Macdonald, M.T.; Lang, A.; Storch, J.; Stevenson, L.; Barber, T.; Iaboni, K.; Donaldson, S. Examining markers of safety in homecare using the international classification for patient safety. BMC Health Serv. Res. 2013, 13, 191. [Google Scholar] [CrossRef] [PubMed]
- Leff, B.; Montalto, M. Home hospital-toward a tighter definition. J. Am. Geriatr. Soc. 2004, 52, 2141. [Google Scholar] [CrossRef] [PubMed]
- Summerfelt, W.T.; Sulo, S.; Robinson, A.; Chess, D.; Catanzano, K. Scalable hospital at home with virtual physician visits: Pilot study. Am. J. Manag. Care 2015, 21, 675–684. [Google Scholar] [PubMed]
- Leff, B.; Burton, L.; Mader, S.L.; Naughton, B.; Burl, J.; Inouye, S.K.; Greenough, W.B., 3rd; Guido, S.; Langston, C.; Frick, K.D.; et al. Hospital at home: Feasibility and outcomes of a program to provide hospital-level care at home for acutely ill older patients. Ann. Intern. Med. 2005, 143, 798–808. [Google Scholar] [CrossRef] [PubMed]
- Bashi, N.; Karunanithi, M.; Fatehi, F.; Ding, H.; Walters, D. Remote monitoring of patients with heart failure: An overview of systematic reviews. J. Med. Intern. Res. 2017, 19. [Google Scholar] [CrossRef] [PubMed]
- Boriani, G.; Da Costa, A.; Quesada, A.; Ricci, R.P.; Favale, S.; Boscolo, G.; Clementy, N.; Amori, V.; di Mangoni, S.; Stefano, L.; et al. Effects of remote monitoring on clinical outcomes and use of healthcare resources in heart failure patients with biventricular defibrillators: Results of the more-care multicentre randomized controlled trial. Eur. J. Heart Fail. 2017, 19, 416–425. [Google Scholar] [CrossRef] [PubMed]
- Morgan, J.M.; Kitt, S.; Gill, J.; McComb, J.M.; Ng, G.A.; Raftery, J.; Roderick, P.; Seed, A.; Williams, S.G.; Witte, K.K.; et al. Remote management of heart failure using implantable electronic devices. Eur. Heart J. 2017, 38, 2352–2360. [Google Scholar] [CrossRef] [PubMed]
- Shepperd, S.; Doll, H.; Angus, R.M.; Clarke, M.J.; Iliffe, S.; Kalra, L.; Ricauda, N.A.; Wilson, A.D. Admission avoidance hospital at home. Cochrane Database Syst. Rev. 2008. [Google Scholar] [CrossRef]
- Shepperd, S.; Doll, H.; Broad, J.; Gladman, J.; Iliffe, S.; Langhorne, P.; Richards, S.; Martin, F.; Harris, R. Early discharge hospital at home. Cochrane Database Syst. Rev. 2009. [Google Scholar] [CrossRef]
- Jeppesen, E.; Brurberg, K.G.; Vist, G.E.; Wedzicha, J.A.; Wright, J.J.; Greenstone, M.; Walters, J.A. Hospital at home for acute exacerbations of chronic obstructive pulmonary disease. Cochrane Database Syst. Rev. 2012. [Google Scholar] [CrossRef] [PubMed]
- Leff, B.; Burton, L.; Mader, S.L.; Naughton, B.; Burl, J.; Greenough, W.B., 3rd; Guido, S.; Steinwachs, D. Comparison of functional outcomes associated with hospital at home care and traditional acute hospital care. J. Am. Geriatr. Soc. 2009, 57, 273–278. [Google Scholar] [CrossRef] [PubMed]
- Leff, B.; Burton, L.; Mader, S.L.; Naughton, B.; Burl, J.; Koehn, D.; Clark, R.; Greenough, W.B., 3rd; Guido, S.; Steinwachs, D.; et al. Comparison of stress experienced by family members of patients treated in hospital at home with that of those receiving traditional acute hospital care. J. Am. Geriatr. Soc. 2008, 56, 117–123. [Google Scholar] [CrossRef] [PubMed]
- Montalto, M. The 500-bed hospital that isn’t there: The Victorian department of health review of the hospital in the home program. Med. J. Aust. 2010, 193, 598–601. [Google Scholar] [PubMed]
- Ponikowski, P.; Voors, A.A.; Anker, S.D.; Bueno, H.; Cleland, J.G.; Coats, A.J.; Falk, V.; Gonzalez-Juanatey, J.R.; Harjola, V.P.; Jankowska, E.A.; et al. 2016 ESC guidelines for the diagnosis and treatment of acute and chronic heart failure: The task force for the diagnosis and treatment of acute and chronic heart failure of the european society of cardiology (ESC). Developed with the special contribution of the heart failure association (HFA) of the esc. Eur. J. Heart Fail. 2016, 18, 891–975. [Google Scholar] [PubMed]
- Hernandez, A.F.; Greiner, M.A.; Fonarow, G.C.; Hammill, B.G.; Heidenreich, P.A.; Yancy, C.W.; Peterson, E.D.; Curtis, L.H. Relationship between early physician follow-up and 30-day readmission among medicare beneficiaries hospitalized for heart failure. JAMA 2010, 303, 1716–1722. [Google Scholar] [CrossRef] [PubMed]
- McAlister, F.A.; Lawson, F.M.; Teo, K.K.; Armstrong, P.W. A systematic review of randomized trials of disease management programs in heart failure. Am. J. Med. 2001, 110, 378–384. [Google Scholar] [CrossRef]
- Albert, N.M.; Barnason, S.; Deswal, A.; Hernandez, A.; Kociol, R.; Lee, E.; Paul, S.; Ryan, C.J.; White-Williams, C. Transitions of care in heart failure: A scientific statement from the American heart association. Circ. Heart Fail. 2015, 8, 384–409. [Google Scholar] [CrossRef] [PubMed]
- Patel, H.; Shafazand, M.; Ekman, I.; Hojgard, S.; Swedberg, K.; Schaufelberger, M. Home care as an option in worsening chronic heart failure—A pilot study to evaluate feasibility, quality adjusted life years and cost-effectiveness. Eur. J. Heart Fail. 2008, 10, 675–681. [Google Scholar] [CrossRef] [PubMed]
- Tibaldi, V.; Isaia, G.; Scarafiotti, C.; Gariglio, F.; Zanocchi, M.; Bo, M.; Bergerone, S.; Ricauda, N.A. Hospital at home for elderly patients with acute decompensation of chronic heart failure: A prospective randomized controlled trial. Arch. Intern. Med. 2009, 169, 1569–1575. [Google Scholar] [CrossRef] [PubMed]
- Mendoza, H.; Martin, M.J.; Garcia, A.; Aros, F.; Aizpuru, F.; Regalado De Los Cobos, J.; Bello, M.C.; Lopetegui, P.; Cia, J.M. ‘Hospital at home’ care model as an effective alternative in the management of decompensated chronic heart failure. Eur. J. Heart Fail. 2009, 11, 1208–1213. [Google Scholar] [CrossRef] [PubMed]
- Qaddoura, A.; Yazdan-Ashoori, P.; Kabali, C.; Thabane, L.; Haynes, R.B.; Connolly, S.J.; Van Spall, H.G. Efficacy of hospital at home in patients with heart failure: A systematic review and meta-analysis. PLoS ONE 2015, 10, e0129282. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.S.; Austin, P.C.; Rouleau, J.L.; Liu, P.P.; Naimark, D.; Tu, J.V. Predicting mortality among patients hospitalized for heart failure: Derivation and validation of a clinical model. JAMA 2003, 290, 2581–2587. [Google Scholar] [CrossRef] [PubMed]
- Felker, G.M.; Leimberger, J.D.; Califf, R.M.; Cuffe, M.S.; Massie, B.M.; Adams, K.F., Jr.; Gheorghiade, M.; O’Connor, C.M. Risk stratification after hospitalization for decompensated heart failure. J. Card. Fail. 2004, 10, 460–466. [Google Scholar] [CrossRef] [PubMed]
- Fonarow, G.C.; Adams, K.F., Jr.; Abraham, W.T.; Yancy, C.W.; Boscardin, W.J. Risk stratification for in-hospital mortality in acutely decompensated heart failure: Classification and regression tree analysis. JAMA 2005, 293, 572–580. [Google Scholar] [CrossRef] [PubMed]
- O’Connor, C.M.; Hasselblad, V.; Mehta, R.H.; Tasissa, G.; Califf, R.M.; Fiuzat, M.; Rogers, J.G.; Leier, C.V.; Stevenson, L.W. Triage after hospitalization with advanced heart failure: The escape (evaluation study of congestive heart failure and pulmonary artery catheterization effectiveness) risk model and discharge score. J. Am. Coll. Cardiol. 2010, 55, 872–878. [Google Scholar] [CrossRef] [PubMed]
- Stewart, S.; Carrington, M.J.; Marwick, T.; Davidson, P.M.; Macdonald, P.; Horowitz, J.; Krum, H.; Newton, P.J.; Reid, C.; Scuffham, P.A. The which? Trial: Rationale and design of a pragmatic randomized, multicentre comparison of home- vs. Clinic-based management of chronic heart failure patients. Eur. J. Heart Fail. 2011, 13, 909–916. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.S.; Stitt, A.; Austin, P.C.; Stukel, T.A.; Schull, M.J.; Chong, A.; Newton, G.E.; Lee, J.S.; Tu, J.V. Prediction of heart failure mortality in emergent care: A cohort study. Ann. Intern. Med. 2012, 156, 767–775. [Google Scholar] [CrossRef] [PubMed]
- Landro, L. What the Hospitals of the Future Look Like. Available online: https://www.wsj.com/articles/what-the-hospitals-of-the-future-look-like-1519614660 (accessed on 25 February 2018).
| Author | Study | Study Population | Finding |
|---|---|---|---|
| Patel H. et al. [33] | Home care as an option in worsening chronic heart failure—a pilot study to evaluate feasibility, quality adjusted life years and cost-effectiveness. | 31 patients seeking medical attention at hospital for worsening CHF were randomized to home care or conventional care. | Reduction in cost of care for selected patients with CHF eligible for hospital care might be achieved by early discharge from hospital followed by home visits. |
| Tibaldi V. et al. [34] | Hospital at home for elderly patients with acute decompensation of chronic heart failure: a prospective randomized controlled trial. | 101 patients randomly assigned to the general medical ward (n = 53) or to the Geriatric Home Hospitalization Service (n = 48). | (a) Substitutive hospital-at-home care is a viable alternative to traditional hospital inpatient care for elderly patients with acutely decompensated CHF. (b) No difference in mortality at 6 months and number of subsequent hospital admissions was observed. (c) Geriatric Home Hospitalization Service patients experienced improvements in depression, nutritional status, quality-of-life scores and had a longer time to first additional admission. |
| Mendoza H. et al. [35] | 'Hospital at home’ care model as an effective alternative in the management of decompensated chronic heart failure. | Eighty patients over the age of 65 years who presented at the emergency department with decompensated HF randomly assigned to inpatient hospital care or Hospital at Home. | Hospital at home care allows an important reduction in the costs during the index episode compared with hospital care, whilst maintaining similar outcomes with respect to cardiovascular mortality and morbidity and quality of life at 1 year follow-up. |
| Meta-Analysis | |||
| Qaddoura A. et al. [36] | Efficacy of Hospital at Home in Patients with Heart Failure: A Systematic Review and Meta-Analysis. | Meta-analyzed results from 3 RCTs (n = 203) and narratively synthesized results from 3 observational studies (n = 329). | Hospital at Home appears to increase time to readmission, reduce index costs and improve health-related quality of life among patients requiring hospital-level care for HF. |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Voudris, K.V.; Silver, M.A. Home Hospitalization for Acute Decompensated Heart Failure: Opportunities and Strategies for Improved Health Outcomes. Healthcare 2018, 6, 31. https://doi.org/10.3390/healthcare6020031
Voudris KV, Silver MA. Home Hospitalization for Acute Decompensated Heart Failure: Opportunities and Strategies for Improved Health Outcomes. Healthcare. 2018; 6(2):31. https://doi.org/10.3390/healthcare6020031
Chicago/Turabian StyleVoudris, Konstantinos V., and Marc A. Silver. 2018. "Home Hospitalization for Acute Decompensated Heart Failure: Opportunities and Strategies for Improved Health Outcomes" Healthcare 6, no. 2: 31. https://doi.org/10.3390/healthcare6020031
APA StyleVoudris, K. V., & Silver, M. A. (2018). Home Hospitalization for Acute Decompensated Heart Failure: Opportunities and Strategies for Improved Health Outcomes. Healthcare, 6(2), 31. https://doi.org/10.3390/healthcare6020031





