Healthcare Engagement as a Potential Source of Psychological Distress among People without Religious Beliefs: A Systematic Review
Abstract
:1. Introduction
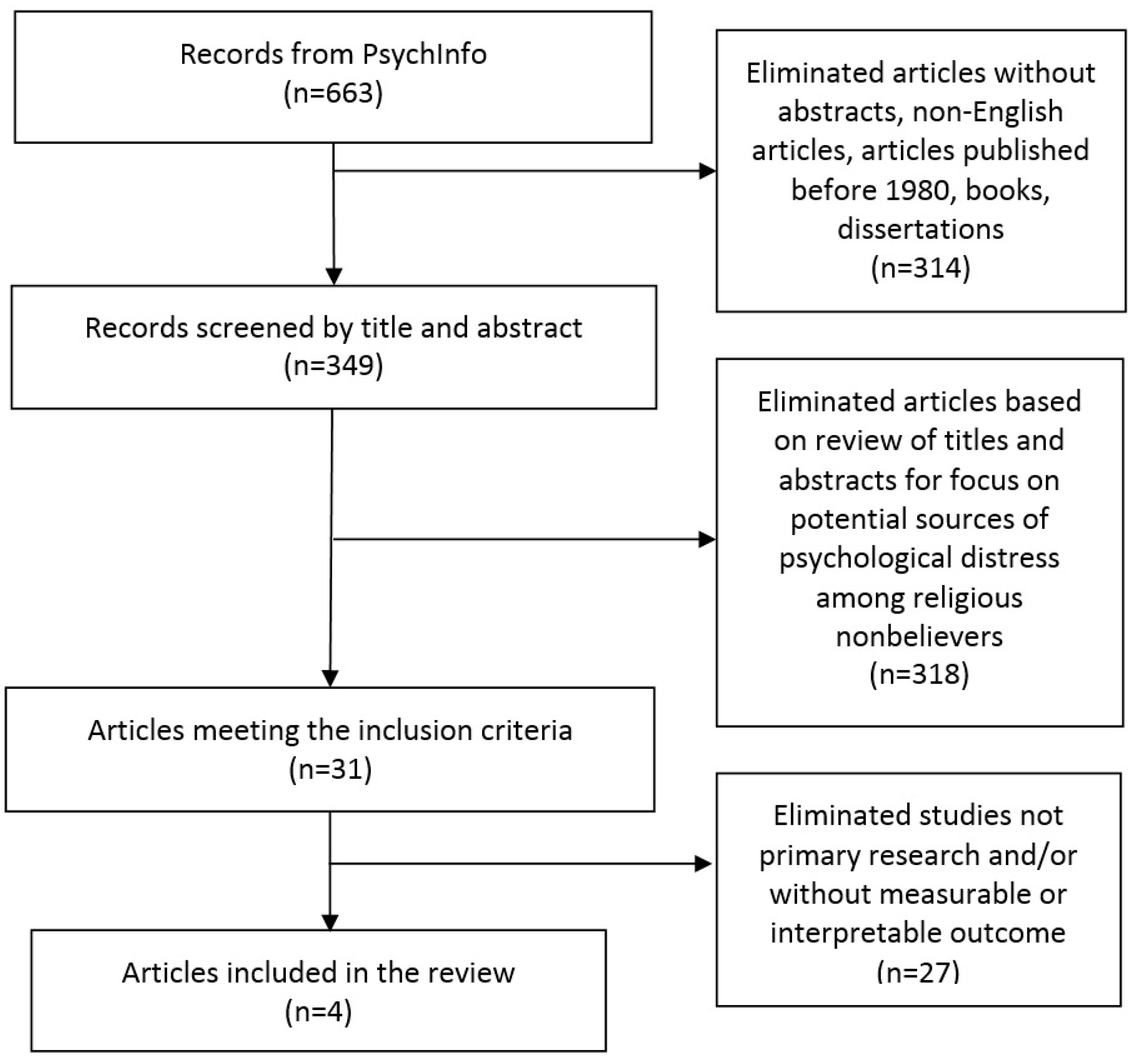
2. Methods
3. Results
3.1. Definitions and Measurements of Lack of Religious Belief
3.2. Healthcare Decision-Making as a Potential Source of Psychological Distress
4. Discussion
5. Conclusions
Author Contributions
Conflicts of Interest
References
- Koenig, H.G. (Ed.) Handbook of Religion and Mental Health; Academic Press: Waltham, MA, USA, 1998. [Google Scholar]
- Pargament, K.I. The Psychology of Religion and Coping: Theory, Research, Practice; The Guilford Press: New York, NY, USA, 2001. [Google Scholar]
- Koenig, H.G.; King, D.; Carson, V. Handbook of Religion and Health, 2nd ed.; Oxford University Press: Oxford, UK, 2012. [Google Scholar]
- Pargament, K.; Exline, J.J.; Jones, J.; Mahoney, A.; Shafranske, E. APA Handbooks in Psychology: APA Handbook of Psychology, Religion, and Spirituality; Pargament, K., Shafranske, E., Eds.; American Psychological Association: Washington, DC, USA, 2013. [Google Scholar]
- Weber, S.R.; Pargament, K.I.; Kunik, M.E.; Lomax, J.W.; Stanley, M.A. Psychological Distress Among Religious Nonbelievers: A Systematic Review. J. Relig. Health 2012, 51, 72–86. [Google Scholar] [CrossRef] [PubMed]
- Frye, C.A.; Weisberg, R.B. Increasing the incidence of routine pelvic examinations: Behavioral medicine’s contribution. Women Health 1994, 21, 33–35. [Google Scholar] [CrossRef] [PubMed]
- Jhalani, J.; Goyal, T.; Clemow, L.; Schwartz, J.E.; Pickering, T.G.; Gerin, W. Anxiety and outcome expectations predict the white-coat effect. Blood Press. Monit. 2005, 10, 317–319. [Google Scholar] [CrossRef] [PubMed]
- Ye, J.; Shim, R. Perceptions of health care communication: Examining the role of patients’ psychological distress. J. Natl. Med. Assoc. 2010, 102, 1237–1242. [Google Scholar] [PubMed]
- Pew Research Center. Religious Landscape Study. Available online: http://www.pewforum.org/religious-landscape-study/ (accessed on 6 March 2017).
- Tonigan, J.S.; Miller, W.R.; Schermer, C. Atheists, agnostics and Alcoholics Anonymous. J. Stud. Alcohol 2002, 63, 534–541. [Google Scholar] [CrossRef] [PubMed]
- Smith, A.F.; Simmonds, J.G. Help-seeking and paranormal beliefs in adherents of mainstream religion, alternative religion, and no religion. Counse. Psychol. Q. 2006, 19, 331–341. [Google Scholar] [CrossRef]
- Baker, P.; Cruickshank, J. I am happy in my faith: The influence of religious affiliation, saliency, and practice on depressive symptoms and treatment preference. Ment. Health Relig. Cult. 2010, 12, 339–357. [Google Scholar] [CrossRef]
- Smith-Stoner, M. End-of-life preferences for atheists. J. Palliat. Med. 2007, 10, 923–928. [Google Scholar] [CrossRef] [PubMed]
| Author | Nonbelief Defined | Measurement Tools | Study Design | Results |
|---|---|---|---|---|
| Tonigan 2002 [10] | Self-identified religious affiliation: atheist, agnostic, unsure | Religious Behavior and Background (RBB) questionnaire Alcoholics Anonymous Involvement (AAI) self-report tool Form 90 interview for client drinking | USA Project MATCH outpatient and aftercare samples, N = 1526 | AA: benefits and likelihood of participation God belief is unimportant in deriving AA-related benefit, but atheist and agnostic clients are less likely to initiate and sustain AA attendance. Unsure patients had the highest rates of drinking and the least improvement after treatment. |
| Smith 2006 [11] | “No religion” group: agnostic, atheist, no religion, humanist, or rationalist | Demographic/help-seeking questionnaire Paranormal Beliefs scale | Australian online study, N = 414 | Relationship between help-seeking and adherence to mainstream religion, alternative religion, and no religion “No religion” group less likely to choose “priest/rabbi/minister/coven/etc.” for counseling support compared with mainstream and alternative groups. No religion group chose “friend or relative” to greater extent than either group. |
| Baker 2010 [12] | Self-reported religious affiliation: atheist, agnostic | 63 item questionnaire: Demographics Depression-Happiness Scale (DHS) Salience Scale Measurement of frequency of religious practices Scale analyzing beliefs about treatments for depression | British study, November 2007–February 2008, N = 471 (130 atheists, 104 agnostics) | Differences in perceived efficacy of depression treatment form Social, cognitive/self-help, or professional/medical treatments: no significant difference between all groups Religious treatments: believers rated more highly than nonbelievers. |
| Smith-Stoner 2007 [13] | Atheist: members of two atheist organizations | Online and paper surveys | USA pilot study, members of two atheist organizations, 3 months in 2005, N = 88 (all atheists) | Atheist preferences for end-of-life care Include pain and symptom management, clear decision making, preparation for death, completion, and affirmation of the whole person (including respect for nonbelief), contributing to others (organ donation), and support of physician-assisted suicide. Atheists expressed concern that healthcare workers may attempt to proselytize them prior to death. |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Weber, S.R.; Lomax, J.W., II; Pargament, K.I. Healthcare Engagement as a Potential Source of Psychological Distress among People without Religious Beliefs: A Systematic Review. Healthcare 2017, 5, 19. https://doi.org/10.3390/healthcare5020019
Weber SR, Lomax JW II, Pargament KI. Healthcare Engagement as a Potential Source of Psychological Distress among People without Religious Beliefs: A Systematic Review. Healthcare. 2017; 5(2):19. https://doi.org/10.3390/healthcare5020019
Chicago/Turabian StyleWeber, Samuel R., James W. Lomax, II, and Kenneth I. Pargament. 2017. "Healthcare Engagement as a Potential Source of Psychological Distress among People without Religious Beliefs: A Systematic Review" Healthcare 5, no. 2: 19. https://doi.org/10.3390/healthcare5020019
APA StyleWeber, S. R., Lomax, J. W., II, & Pargament, K. I. (2017). Healthcare Engagement as a Potential Source of Psychological Distress among People without Religious Beliefs: A Systematic Review. Healthcare, 5(2), 19. https://doi.org/10.3390/healthcare5020019







