Sustaining Behavior Changes Following a Venous Leg Ulcer Client Education Program
Abstract
:1. Introduction
1.1. Venous Leg Ulcers: A Common and Costly Wound
1.2. A Chronic Condition, a Complex Treatment
2. Methods
2.1. Design
2.2. The Leg Ulcer Prevention Program (LUPP)
| Session | Topic | Self-Management Recommendations |
|---|---|---|
| Introduction | Overview of program Compression for healing and recurrence prevention | Ownership of wound and self-management plan |
| Leg Ulcer Treatment | Compression therapy most clinically effective treatment Promotion of four layer bandaging | Commence compression therapy for treatment Plan for compression following healing |
| Activity and Exercise | Walking, leg exercises and elevation Use of activity diary | Be active Regular walking (30 min/day) Heel raises and squats (5 sets × 5 repetitions × 3 times/day) Occasional leg elevation (30 min × 3 times/day) |
| Skin Care | Cleansing Moisturizing Inspection | Daily use of pH neutral cleanser Daily use of pH neutral moisturizer Regular inspection Early reporting of skin integrity concerns |
| Nutrition and Hydration | Appropriate diet Adequate hydration Tips for healthy eating Nutrition when wounded | Intake guided by Australian Guidelines Minimum of 1 Litre “good” fluid Ensure adequate protein, consider supplementation |
| Compression stockings for recurrence prevention | Promotion of compression stockings Use of applicators Application and removal technique Stocking care | Wear compression stockings every day Use applicators to assist application and removal Replace stocking every 3 months |
2.3. Data Collection
2.4. Data Analysis
3. Results and Discussion
3.1. Sample
| Demographic/Health Characteristics | Total Sample (n = 49) |
|---|---|
| Gender (% female) | 75.5 |
| Age (Years; Ave. ± SD) | 76.10 ± 11.91 |
| Nutritional Risk (Ave. ± SD) | 12.78 ± 2.02 |
| AACCI (Ave. ± SD) ^ | 4.78 ± 2.62 |
| Diabetes Mellitus (% yes) | 14.3 |
| Wound Characteristics | Total Sample (n = 49) |
|---|---|
| Duration in weeks (Ave. ± SD) * | 26.63 ± 20.66 |
| Size (cm2; Ave. ± SD) ^ | 8.32 ± 12.28 |
| Infected during episode (% yes) | 59.2 |
3.2. Design Sustainability of Health Behavior Changes Overtime of Participants Who Did LUPP
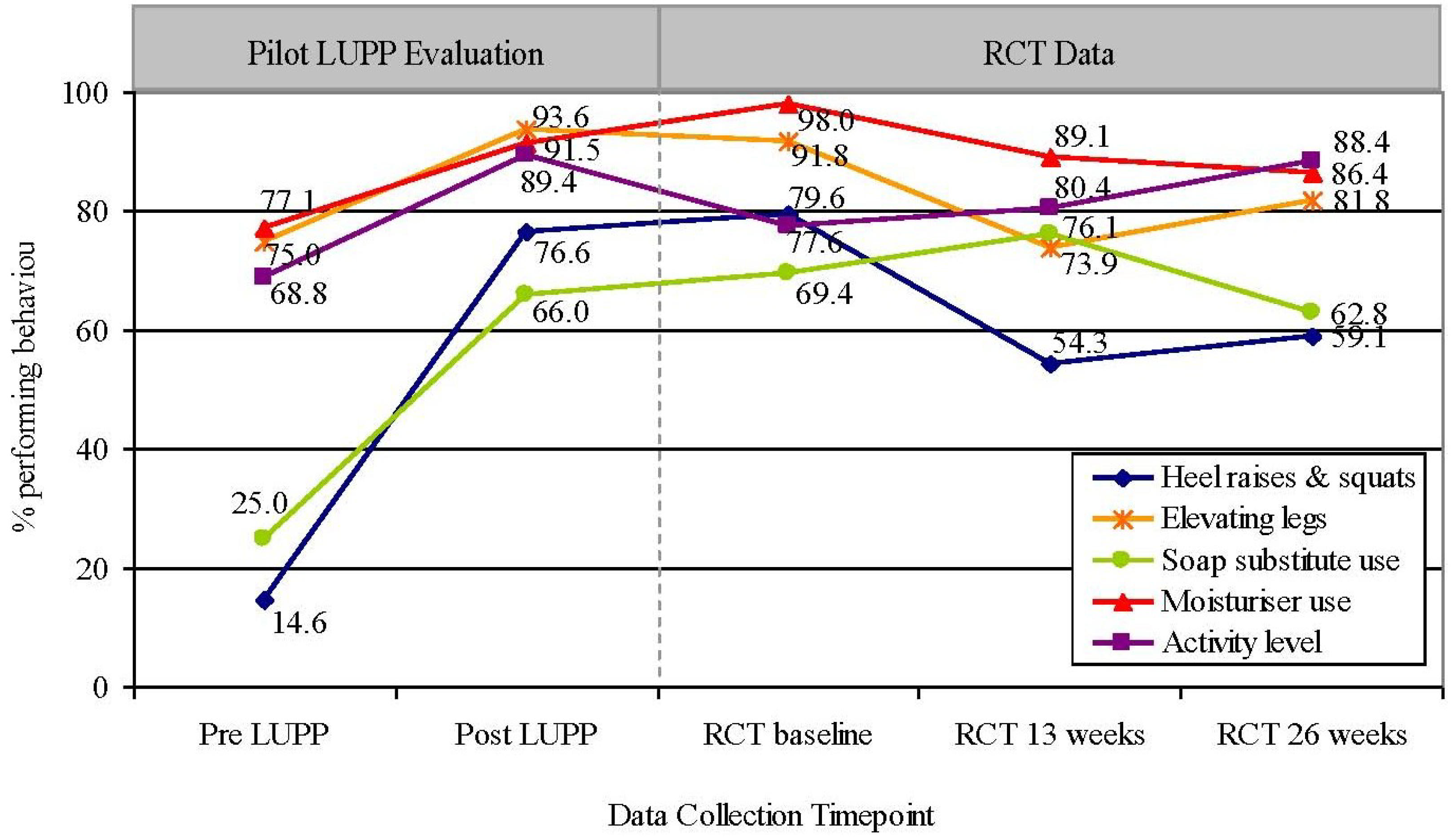
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Briggs, M.; Closs, S.J. The prevalence of leg ulceration: A review of the literature. Eur. Wound Manag. Assoc. J. 2003, 3, 14–20. [Google Scholar]
- Graham, I.D.; Harrison, M.B.; Nelson, E.A.; Lorimer, K.; Fisher, A. Prevalence of lower-limb ulceration: A systematic review of prevalence studies. Adv. Skin Wound Care 2003, 16, 305–316. [Google Scholar] [CrossRef] [PubMed]
- Chase, S.; Melloni, M.; Savage, A. A forever healing: The lived experience of venous ulcer disease. J. Vasc. Nurs. 1997, 15, 73–78. [Google Scholar] [PubMed]
- Chase, S.; Whittemore, R.; Crosby, N.; Freney, D.; Howes, P.; Phillips, T. Living with chronic venous leg ulcers: A descriptive study of patients’ experiences. J. Community Health Nurs. 2000, 17, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Douglas, V. Living with a chronic leg ulcer: An insight into patients’ experiences and feelings. J. Wound Care 2001, 10, 355–360. [Google Scholar] [CrossRef] [PubMed]
- Franks, P.J.; Moffat, C.J. Who suffers most from leg ulceration? J. Wound Care 1998, 7, 383–385. [Google Scholar]
- Husband, L. Venous ulceration: The pattern of pain and the paradox. Clin. Eff. Nurs. 2001, 5, 35–40. [Google Scholar] [CrossRef]
- Hyde, C.; Ward, B.; Horsfall, J.; Winder, G. Older women’s experience of living with chronic leg ulceration. Int. J. Nurs. Pract. 1999, 5, 189–198. [Google Scholar] [CrossRef] [PubMed]
- Krasner, D. Painful venous ulcers: Themes and stories about living with pain and suffering. J. Wound Ostomy Cont. Nurs. 1997, 25, 158–168. [Google Scholar]
- Neil, J.A.; Munjas, B.A. Living with a chronic wound: The voice of sufferers. Ostomy Wound Manag. 2000, 46, 28–38. [Google Scholar]
- Rich, A.; McLachlan, L. How living with a leg ulcer affects peoples’ daily life: A nurse-led study. J. Wound Care 2003, 12, 51–54. [Google Scholar]
- Angel, D.; Sieunarine, K.; Abbas, M.; Mwipatayi, B. The difficult leg ulcer: A case review illustrating the problems and difficulties associated with treatment. Prim. Intent. 2005, 13, 7–16. [Google Scholar]
- Australian Institute of Health and Welfare. Chronic Diseases. Secondary Chronic Diseases. Available online: http://www.aihw.gov.au/chronic-diseases/ (accessed on 10 October 2013).
- Australian Wound Management Association Inc.; New Zealand Wound Care Society Inc. Australian and New Zealand Clinical Practice Guidelines for Prevention and Management of Venous Leg Ulcers; Cambridge Publishing: Perth, Australia, 2011. [Google Scholar]
- Kapp, S.; Sayers, V. Preventing venous leg ulcer recurrence: A review. Wound Pract. Res. 2008, 16, 38–47. [Google Scholar]
- Moffatt, C.; Kommala, D.; Dourdin, N.; Choe, Y. Venous leg ulcers: Patient concordance with compression therapy and its impact on healing and prevention of recurrence. Int. Wound J. 2009, 6, 386–393. [Google Scholar] [CrossRef] [PubMed]
- Van Hecke, A.; Grypdonck, M.; Defloor, T. Interventions to enhance patient compliance with leg ulcer treatment: A review of the literature. J. Clin. Nurs. 2008, 17, 29–39. [Google Scholar]
- Lindsay, E. The Lindsay LEG CLUB model: A model for evidence-based leg ulcer management. Br. J. Community Nurs. 2004, 9, S15–S20. [Google Scholar] [CrossRef]
- Heinen, M.; Borm, G.; van der Vleuten, C.; Evers, A.; Oostendorp, R.; van Achterberg, T. The Lively Legs self-management program increased physical activity and reduced wound days in leg ulcer patients: Results from a randomized controlled trial. Int. J. Nurs. Stud. 2012, 49, 151–161. [Google Scholar] [CrossRef] [PubMed]
- Heinen, M.M.; Bartholomew, L.K.; Wensing, M.; van de Kerkhof, P.; van Achterberg, T. Supporting adherence and healthy lifestyles in leg ulcer patients: Systematic development of the Lively Legs program for dermatology outpatient clinics. Patient Educ. Couns. 2006, 61, 279–291. [Google Scholar] [CrossRef] [PubMed]
- Kapp, S.; Miller, C.; Sayers, V.; Donohue, L. The Leg Ulcer Prevention Program: Effectiveness of a multimedia client education package for people with venous leg ulcers. Wound Pract. Res. 2010, 18, 80–90. [Google Scholar]
- Freeman, E.; Gibbins, A.; Walker, M.; Hapeshi, J. “Look after your legs”: Patients’ experience of an assessment clinic. Wound Care 2007, 12, S19–S25. [Google Scholar]
- Van Hecke, A.; Grypdonck, M.; Beele, H.; Vanderwee, K.; Defloor, T. Adherence to leg ulcer lifestyle advice: Qualitative and quantitative outomes associated with a nurse-led intervention. J. Clin. Nurs. 2011, 20, 429–443. [Google Scholar]
- Kapp, S.; Miller, C.; Donohue, L. The Leg Ulcer Prevention Program: Nurse perspectives of a multimedia client education program for people with venous leg ulcers. Wound Pract. Res. 2010, 18, 91–99. [Google Scholar]
- Blissmer, B.; Prochaska, J.O.; Velicer, W.F.; Redding, C.A.; Rossi, J.S.; Greene, G.W.; Paiva, A.; Robbins, M. Common factors precidting long term changes in multiple health behaviors. J. Health Psychol. 2010, 15, 205–214. [Google Scholar] [CrossRef] [PubMed]
- Bayliss, E.A.; Steiner, J.F.; Fernald, D.H.; Crane, L.A.; Main, D.S. Descriptions of barriers to self-care by persons with comorbid chronic diseases. Ann. Fam. Med. 2003, 1, 15–21. [Google Scholar] [CrossRef] [PubMed]
- Fortin, M.; Soubhi, H.; Hudon, C.; Bayliss, E.A.; van den Akker, M. Multimorbidity’s many challenges. Br. Med. J. 2007, 334, 1016–1017. [Google Scholar] [CrossRef]
- Morris, R.L.; Sanders, C.; Kennedy, A.P.; Rogers, A. Shifting priorities in multimorbidity: A longitudinal qualitative study of patient’s prioritization of multiple conditions. Chronic Illn. 2011, 7, 147–161. [Google Scholar] [CrossRef] [PubMed]
- Australian Bureau of Statistics. Disability, Ageing and Carers, Australia: Summary of Findings, 2012. Available online: http://www.abs.gov.au/ausstats/abs@.nsf/Lookup/D9BD84DBA2528FC9CA257C21000E4FC5?opendocument (accessed on 19 February 2014).
- Currie, C.E.; Amos, A.; Hunt, S. The dynamics and processes of behavioral change in five classes of health-related behavior—Findings from qualitative research. Health Educ. Res. 1991, 6, 443–453. [Google Scholar] [CrossRef]
- Toobert, D.J.; Strychker, L.A.; Barrera, M.; Glasgow, R.E. Seven-year follow-up of a multiple-health-behavior diabetes intervention. Am. J. Health Behav. 2010, 34, 680–694. [Google Scholar] [PubMed]
- Ebbeskog, B.; Ekman, S.L. Elderly persons’ experiences of living with venous leg ulcer: Living in a dialectical relationship between freedom and imprisonment. Scand. J. Caring Sci. 2001, 15, 235–243. [Google Scholar] [CrossRef]
- Walshe, C. Living with a venous leg ulcer: A descriptive study of patients’ experiences. J. Adv. Nurs. 1995, 22, 1092–1100. [Google Scholar] [CrossRef] [PubMed]
- Everson, E.S.; Taylor, A.H.; Ussher, M. Determinants of physical activity promotion by smoking cessation advisors as an aid for quitting: Support for the transtheorectical model. Patient Educ. Couns. 2010, 78, 53–56. [Google Scholar] [CrossRef] [PubMed]
- Everson-Hock, E.S.; Taylor, A.H.; Ussher, M. Readiness to use physical activity as a smoking cessation aid: A multiple behavior change application of the transtheorectical model among quitters attending stop smoking clinics. Patient Educ. Couns. 2010, 79, 156–159. [Google Scholar]
- Everson-Hock, E.S.; Taylor, A.H.; Ussher, M.; Faulkner, G. A qualitative perspective on multiple health behavior change: Views of smoking cessation advisors who promote physical activity. J. Smok. Cessat. 2010, 5, 7–14. [Google Scholar]
- Johnson, S.S.; Paiva, A.L.; Cummins, C.O.; Johnson, J.L.; Dyment, S.J.; Wright, J.A.; Prochaska, J.O.; Prochaska, J.M.; Sherman, K. Transtheorectical model-based multiple behavior intervention for weight management: Effectiveness on a population basis. Prev. Med. 2008, 46, 238–246. [Google Scholar] [CrossRef] [PubMed]
- Prochaska, J.O.; Velicer, W.F. The transtheorectical model of health behavior change. Am. J. Health Behav. 1997, 12, 38–48. [Google Scholar]
- Barlow, J.; Wright, C.; Sheasby, J.; Turner, A.; Hainsworth, J. Self-management approaches for people with chronic conditions: A review. Patient Educ. Couns. 2002, 48, 177–187. [Google Scholar] [CrossRef] [PubMed]
- Berzins, K.; Reilly, S.; Abell, J.; Hughes, J.; Challis, D. UK self-care support initiatives for older patients with long-term conditions: A review. Chronic Illn. 2009, 5, 56–72. [Google Scholar] [CrossRef] [PubMed]
- Prochaska, J.J.; Prochaska, J.O. A review of multiple health behavior change interventions for primary prevention. Am. J. Lifestyle Med. 2011, 5, 208–221. [Google Scholar] [CrossRef]
- Fjeldsoe, B.; Neuhaus, M.; Winkler, E.; Eakin, E. Systematic review of maintenance of behavior change following physical activity and dietary interventions. Health Psychol. 2011, 30, 99–109. [Google Scholar] [CrossRef] [PubMed]
- Green, L.W. Evaluation and measurement: Some dilemmas for health education. Am. J. Public Health 1977, 67, 155–161. [Google Scholar]
- Park, M.J.; Green, J.; Ishikawa, H.; Kiuchi, T. Hidden decay of impact after education for self-management of chronic illnesses: Hypotheses. Chronic Illn. 2012, 9, 73–80. [Google Scholar] [CrossRef] [PubMed]
- Ory, M.G.; Smith, M.L.; Mier, N.; Wernicke, M.M. The science of sustaining health behavior change: The health maintenance consortium. Am. J. Health Behav. 2010, 34, 647–659. [Google Scholar] [CrossRef] [PubMed]
- Wing, R.R. Cross-cutting themes in maintenance of behavior change. Health Psychol. 2000, 19, 84–88. [Google Scholar] [CrossRef]
- Sniehotta, F.F.; Schwarzer, R.; Scholz, U.; Schüz, B. Action planning and coping planning for long-term lifestyle change: Theory and assessment. Eur. J. Soc. Psychol. 2005, 35, 565–576. [Google Scholar] [CrossRef]
- Kapp, S.; Miller, C.; Donohue, L. The clinical effectiveness of two compression stocking treatments on venous leg ulcer recurrence: A randomised controlled trial. J. Low. Extrem. Wounds 2013. [Google Scholar] [CrossRef]
- IBM SPSS Statistics for Windows, 19.0.0 version; IBM Corp.: Armonk, NY, USA, 2010.
- Charlson, M.E.; Pompei, P.; Ales, K.; MacKenzie, C.R. A new method of classifying prognostic comorbidity in longitudinal studies: Development and validation. J. Chronic Dis. 1987, 40, 373–383. [Google Scholar] [CrossRef] [PubMed]
- Fry, J.P.; Neff, R.A. Periodic prompts and reminders in health promotion and health behavior interventions: Systematic review. J. Med. Internet Res. 2009, 11, 1–15. [Google Scholar] [CrossRef]
- Rollnick, S.; Butler, C.C.; McCambridge, J.; Kinnersley, P.; Elwyn, G.; Resnicow, K. Consultations about changing behavior. Br. Med. J. 2005, 331, 961–963. [Google Scholar] [CrossRef]
- Newsom, R.S.; Lion, R.; Crawford, R.J.; Curtis, V.; Elmadfa, I.; Feunekes, G.I.J.; Hicks, C.; van Liere, M.; Lowe, C.F.; Meijer, G.W.; et al. Behavior change for better health: Nutrition, hyigene and sustainability. BMC Public Health 2013, 13, S1–S13. [Google Scholar] [CrossRef]
- Fuller, B.G.; Stewart Williams, J.A.; Byles, J.E. Active living—The perception of older people with chronic conditions. Chronic Illn. 2010, 6, 294–305. [Google Scholar] [PubMed]
- Rosland, A.; Heisler, M.; Choi, H.; Silveira, M.J.; Piette, J.D. Family influences on self-management among functionlly independent adults with diabetes or heart failure: Do family members hinder as much as they help. Chronic Illn. 2010, 6, 22–33. [Google Scholar] [CrossRef] [PubMed]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Miller, C.; Kapp, S.; Donohue, L. Sustaining Behavior Changes Following a Venous Leg Ulcer Client Education Program. Healthcare 2014, 2, 324-337. https://doi.org/10.3390/healthcare2030324
Miller C, Kapp S, Donohue L. Sustaining Behavior Changes Following a Venous Leg Ulcer Client Education Program. Healthcare. 2014; 2(3):324-337. https://doi.org/10.3390/healthcare2030324
Chicago/Turabian StyleMiller, Charne, Suzanne Kapp, and Lisa Donohue. 2014. "Sustaining Behavior Changes Following a Venous Leg Ulcer Client Education Program" Healthcare 2, no. 3: 324-337. https://doi.org/10.3390/healthcare2030324
APA StyleMiller, C., Kapp, S., & Donohue, L. (2014). Sustaining Behavior Changes Following a Venous Leg Ulcer Client Education Program. Healthcare, 2(3), 324-337. https://doi.org/10.3390/healthcare2030324




