Prevalence of Common Diabetes Mellitus Misinformation Exposure, Cognitive Attitude, and Intention to Share Information Among Patients in a Primary Care Unit
Abstract
1. Introduction
2. Materials and Methods
2.1. Ethics Approval
2.2. Study Design
2.3. Participants and Data Collection
2.3.1. Phase I
2.3.2. Phase II
2.4. Statistical Analysis
3. Results
3.1. Baseline Characteristics
3.2. Prevalence of Exposure and Intention to Share Misinformation on T2DM
3.3. Sources of Misinformation
3.4. Cognitive Attitudes Towards Misinformation
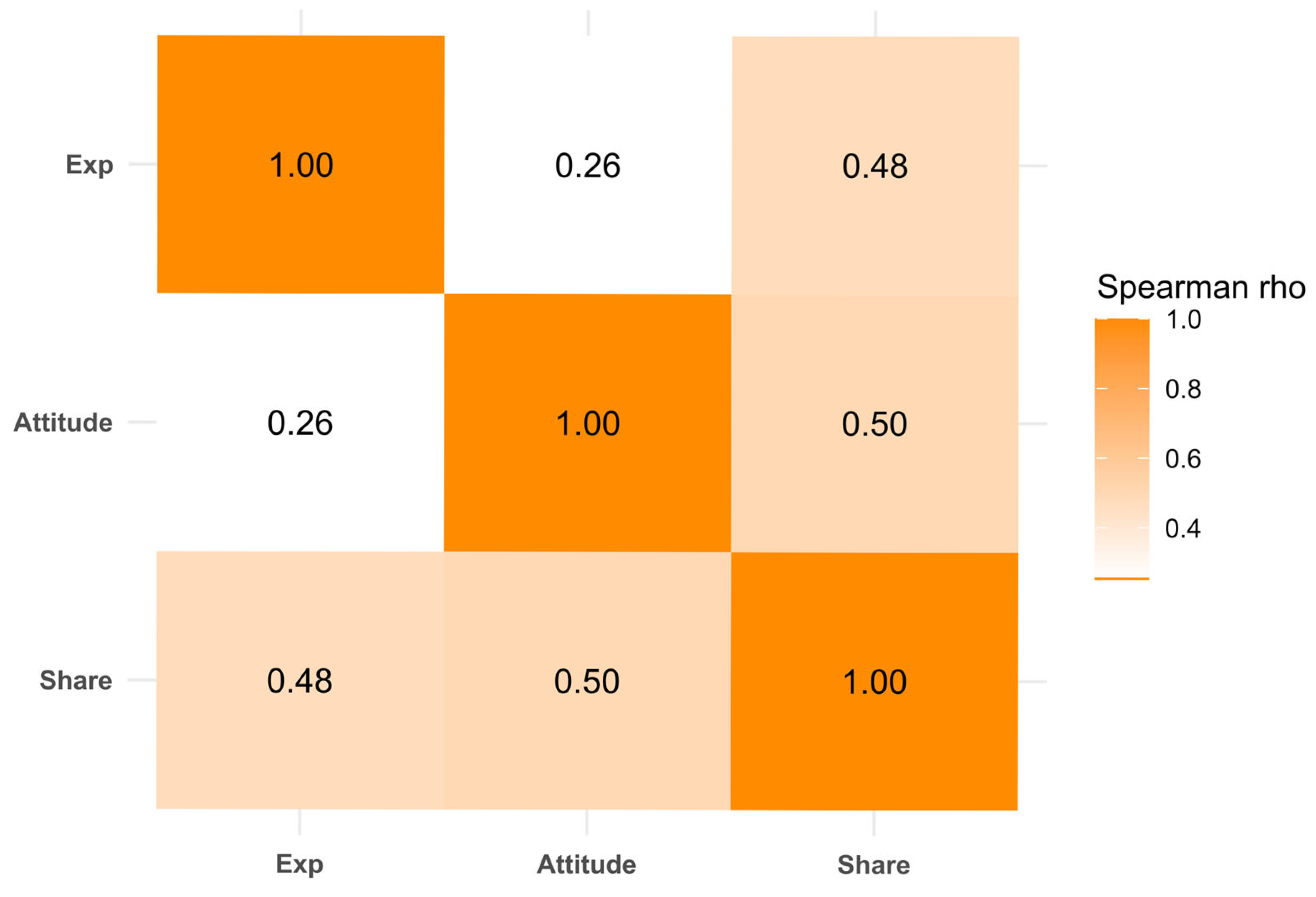
3.5. Correlation Between Exposure, Attitude, and Intention to Share
3.6. Statistical Analysis of Factors Influencing Misinformation Among Patients with T2DM
4. Discussion
4.1. Strengths and Limitations
4.2. Future Research Suggestions
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| CI | Confidence interval |
| T2DM | Type 2 diabetes mellitus |
References
- Gregg, E.W.; Buckley, J.; Ali, M.K.; Davies, J.; Flood, D.; Mehta, R.; Griffiths, B.; Lim, L.L.; Manne-Goehler, J.; Pearson-Stuttard, J.; et al. Improving health outcomes of people with diabetes: Target setting for the WHO Global Diabetes Compact. Lancet 2023, 401, 1302–1312. [Google Scholar] [CrossRef] [PubMed]
- Riegel, B.; Moser, D.K.; Buck, H.G.; Dickson, V.V.; Dunbar, S.B.; Lee, C.S.; Lennie, T.A.; Lindenfeld, J.; Mitchell, J.E.; Treat-Jacobson, D.J.; et al. Self-care for the prevention and management of cardiovascular disease and stroke: A scientific statement for healthcare professionals from the American Heart Association. J. Am. Heart Assoc. 2017, 6, e006997. [Google Scholar] [CrossRef] [PubMed]
- Thorne, S.E.; Paterson, B.L. Health care professional support for self-care management in chronic illness: Insights from diabetes research. Patient Educ. Couns. 2001, 42, 81–90. [Google Scholar] [CrossRef] [PubMed]
- Kalra, S.; Punyani, H. Handling hearsay in diabetes care. J. Pak. Med. Assoc. 2020, 70, 186–187. [Google Scholar] [PubMed]
- Patil, R.; Nasrin A, N.; Datta, S.S.; Boratne, A.V.; Lokeshmaran. Popular misconceptions regarding the diabetes management: Where should we focus our attention? J. Clin. Diagn. Res. 2013, 7, 287–291. [Google Scholar] [CrossRef] [PubMed]
- Kalra, S.; Balachandran, K. De-hearsay (diabetes e-hearsay). J. Pak. Med. Assoc. 2017, 67, 1293–1295. [Google Scholar] [PubMed]
- Dorner, T.E.; Lackinger, C.; Schindler, K.; Stein, K.V.; Rieder, A.; Ludvik, B. Health information regarding diabetes mellitus reduces misconceptions and underestimation of consequences in the general population. Public Health Nutr. 2013, 16, 2032–2039. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Mann, D.M.; Ponieman, D.; Leventhal, H.; Halm, E.A. Misconceptions about diabetes and its management among low-income minorities with diabetes. Diabetes Care 2009, 32, 591–593. [Google Scholar] [CrossRef] [PubMed]
- Almasri, H.; Popp, R.A. Misconceptions and beliefs related to diabetes care and their effect on A1c values in people with type 2 diabetes. Clin. Diabetes 2024, 42, 488–496. [Google Scholar] [CrossRef] [PubMed]
- Sakboonyarat, B.; Pima, W.; Chokbumrungsuk, C.; Pimpak, T.; Khunsri, S.; Ukritchon, S.; Imjaijitt, W.; Mungthin, M.; Kaewput, W.; Bhopdhornangkul, B.; et al. National trends in the prevalence of glycemic control among patients with type 2 diabetes receiving continuous care in Thailand from 2011 to 2018. Sci. Rep. 2021, 11, 14260. [Google Scholar] [CrossRef] [PubMed]
- Hurst, C.P.; Rakkapao, N.; Hay, K. Impact of diabetes self-management, diabetes management self-efficacy and diabetes knowledge on glycemic control in people with type 2 diabetes: A Multi-center Study in Thailand. PLoS ONE 2020, 15, e0244692. [Google Scholar] [CrossRef] [PubMed]
- Reutrakul, S.; Deerochanawong, C. Diabetes in Thailand: Status and policy. Curr. Diabetes Rep. 2016, 16, 28. [Google Scholar] [CrossRef] [PubMed]
- Dutta, D.; Arora, V.; Dhingra, A.; Das, A.K.; Fariduddin, M.; Shaikh, K.; Priya, G.; Shah, P.; Rehim, A.A.; John, M.; et al. Quinary prevention in diabetes care: Need for multidisciplinary approach. Clin. Epidemiol. Glob. Health 2021, 11, 100757. [Google Scholar] [CrossRef]
- Jain, V. 3D model of attitude. Int. J. Adv. Res. Manag. Soc. Sci. 2014, 3, 1–12. [Google Scholar]
- Alajmi, B.M. The intention to share: Psychological investigation of knowledge sharing behaviour in online communities. J. Inf. Knowl. Manag. 2012, 11, 1250022. [Google Scholar] [CrossRef]
- Razmerita, L.; Kirchner, K.; Nielsen, P. What factors influence knowledge sharing in organizations? A social dilemma perspective of social media communication. J. Knowl. Manag. 2016, 20, 1225–1246. [Google Scholar] [CrossRef]
- Chen, C.C.; Chen, C.L.; Ko, Y. The misconceptions and determinants of diabetes knowledge in patients with diabetes in Taiwan. J. Diabetes Res. 2020, 2020, 2953521. [Google Scholar] [CrossRef] [PubMed]
- Sabra, A.; Taha, A.; Al-Zubier, A.; Al-Kurashi, N. Misconceptions about diabetes mellitus among adult male attendees of primary health care centres in Eastern Saudi Arabia. S. Afr. Fam. Pract. 2010, 52, 344–349. [Google Scholar] [CrossRef]
- Nisar, N.; Khan, I.A.; Qadri, M.H.; Sher, S.A. Myths about diabetes mellitus among non-diabetic individuals attending primary health care centers of Karachi subrubs. J. Coll. Physicians Surg. Pak. 2007, 17, 398–401. [Google Scholar] [PubMed]
- Jun, S.Y.; Ju, T.W.; Park, H.K.; Lee, J.C.; Kim, T.M. Information distortion in word-of-mouth retransmission: The effects of retransmitter intention and source expertise. Asian Bus. Manag. 2023, 22, 1848–1876. [Google Scholar] [CrossRef] [PubMed]
- Sweeney, J.C.; Webb, D.; Mazzarol, T.; Soutar, G.N. Self-determination theory and word of mouth about energy-saving behaviors: An online experiment. Psychol. Mark. 2014, 31, 698–716. [Google Scholar] [CrossRef]
- Fritschi, C.; Quinn, L. Fatigue in patients with diabetes: A review. J. Psychosom. Res. 2010, 69, 33–41. [Google Scholar] [CrossRef] [PubMed]
- Polonsky, W.H.; Davis, C.L.; Jacobson, A.M.; Anderson, B.J. Hyperglycaemia, hypoglycaemia, and blood glucose control in diabetes: Symptom perceptions and treatment strategies. Diabet. Med. 1992, 9, 120–125. [Google Scholar] [CrossRef] [PubMed]
- Ranasinghe, P.; Pigera, A.S.; Ishara, M.H.; Jayasekara, L.M.; Jayawardena, R.; Katulanda, P. Knowledge and perceptions about diet and physical activity among Sri Lankan adults with diabetes mellitus: A qualitative study. BMC Public Health 2015, 15, 1160. [Google Scholar] [CrossRef] [PubMed]
- Mogre, V.; Johnson, N.A.; Tzelepis, F.; Paul, C. Barriers to diabetic self-care: A qualitative study of patients’ and healthcare providers’ perspectives. J. Clin. Nurs. 2019, 28, 2296–2308. [Google Scholar] [CrossRef]
- Li, L.; Zhu, L.; Zhou, X.; Zeng, G.; Huang, H.; Gan, Y.; Lu, Z.; Wang, X.; Chen, Z.; Sun, K.; et al. Patients’ trust and associated factors among primary care institutions in China: A cross-sectional study. BMC Prim. Care 2022, 23, 109. [Google Scholar] [CrossRef] [PubMed]
- Bandura, A.; Walters, R.H. Social Learning Theory; Prentice Hall: Englewood Cliffs, NJ, USA, 1977; Volume 1. [Google Scholar]
- Zhou, C.; Zhao, Q.; Lu, W. Impact of repeated exposures on information spreading in social networks. PLoS ONE 2015, 10, e0140556. [Google Scholar] [CrossRef] [PubMed]
- Ashforth, B.E.; Mael, F. Social identity theory and the organization. Acad. Manag. Rev. 1989, 14, 20–39. [Google Scholar] [CrossRef]
- Nalavadey, S.; Baliga, S.S. Misconceptions about diabetes mellitus among diabetes patients: A cross-sectional study. Indian J. Health Sci. Biomed. Res. (KLEU) 2022, 15, 230–234. [Google Scholar] [CrossRef]
- Bravo, T.R.P.; Schiessl, G.W.; Ferreira, I.A.M.; Nogueira, T.A.; Calil-Elias, S. Diabetes and Instagram: Analysis of information in Brazilian publications. J. Consum. Health Internet 2024, 28, 25–39. [Google Scholar] [CrossRef]
- Lee, M.; Shim, J. Effects of diabetes knowledge and attitudes toward Internet health information on e-health literacy in middle-aged patients with diabetes. Healthcare 2025, 13, 512. [Google Scholar] [CrossRef] [PubMed]
- Kong, W.; Song, S.; Zhao, Y.C.; Zhu, Q.; Sha, L. TikTok as a health information source: Assessment of the quality of information in diabetes-related videos. J. Med. Internet Res. 2021, 23, e30409. [Google Scholar] [CrossRef] [PubMed]
- Farukuoye, M.; Oyinlade, M. The influence of social media in fuelling health-related disinformation, misinformation, false information and infodemics. J. Health Inf. Librariansh. 2024, 7, 31–42. Available online: https://johil.org/index.php/johil/article/view/70 (accessed on 2 July 2025).
- Festinger, L. A Theory of Cognitive Dissonance; Stanford University Press: Redwood City, CA, USA, 1957. [Google Scholar] [CrossRef]
- Yahya, A.H.; Sukmayadi, V. A review of cognitive dissonance theory and its relevance to current social issues. Mimb. J. Sos. Dan Pembang. 2020, 36, 480–488. [Google Scholar] [CrossRef]




| Group | Misinformation Question |
|---|---|
| Side effects of medication (Group 1) | 1. Long-term use of diabetes medication leads to kidney impairment. |
| 2. Long-term use of insulin injections leads to kidney impairment. | |
| 3. Using multiple types of diabetes medication together accelerates kidney impairment. | |
| 4. If a doctor starts diabetes treatment with insulin injections, patients must keep injecting for life. | |
| Alternative treatment (Group 2) | 5. Using herbs to treat diabetes might make the disease go away completely. |
| 6. Using sugar substitutes can lower blood sugar levels. | |
| 7. Patients with diabetes mellitus can take supplements instead of controlling their diet. | |
| Imbalanced lifestyle (Group 3) | 8. Patients with diabetes mellitus do not need to limit their food intake if the food is not sweet. |
| 9. Patients with diabetes mellitus who inject insulin are not able to exercise. | |
| 10. Patients with diabetes mellitus who have experienced hypoglycemia during exercise may not be able to exercise again. | |
| 11. Patients with diabetes mellitus cannot eat fruits that are sweet in taste at all. | |
| Symptom perception (Group 4) | 12. When patients with diabetes mellitus experience fatigue, it is necessary to drink sugary beverages to alleviate the symptoms quickly. |
| 13. Patients with diabetes mellitus without any symptoms are those who control their blood sugar levels well. |
| Sociodemographic Characteristics | Patients (n = 107) |
|---|---|
| Age (years), mean (SD) | 64.5 (9.8) |
| Sex, n (%) | |
| Male | 43 (40.2) |
| Female | 64 (59.8) |
| Religion, n (%) | |
| Buddhism | 101 (94.4) |
| Islam | 6 (5.6) |
| Education level, n (%) | |
| No formal education | 2 (1.9) |
| Primary education | 49 (45.8) |
| Secondary education | 18 (16.8) |
| Vocational education/professional bachelor’s degree | 13 (12.1) |
| Bachelor’s degree | 19 (17.8) |
| Above a bachelor’s degree | 6 (5.6) |
| Average monthly income (THB), n (%) | |
| ≤10,000 | 63 (58.9) |
| 10,001–20,000 | 22 (20.6) |
| >20,000 | 22 (20.6) |
| Time since diagnosis (years), median (IQR) | 7 (3.5–10) |
| Dyslipidemia, n (%) | 100 (93.5) |
| Hypertension, n (%) | 72 (67.3) |
| Another comorbidity, n (%) | 6 (5.6) |
| Current diabetes treatment, n (%) | |
| Insulin therapy | 11 (10.3) |
| Oral anti-diabetic drug | 90 (84.1) |
| Lifestyle modifications (no medication) | 6 (5.6) |
| Current diabetic retinopathy | 3 (2.8) |
| Source | Times of Exposure, n (%) * |
|---|---|
| Non-person | |
| Television and radio | 78 (7.12) |
| Online media (Internet, YouTube, Facebook, Twitter) | 128 (11.69) |
| Person | |
| Patients with diabetes mellitus | 244 (22.28) |
| Patients without diabetes mellitus | 506 (46.21) |
| Healthcare providers | 139 (12.69) |
| Factors | Cognitive Attitude | Intention to Share | |||||
|---|---|---|---|---|---|---|---|
| Sociodemographic Characteristics | Patients (n = 107) | Score | SD | p-Value | Score | SD | p-Value |
| Age, years | 0.55 | 0.58 | |||||
| ≥65 | 49 | 3.152 | 0.967 | 0.350 | 0.477 | ||
| <65 | 58 | 3.199 | 0.913 | 0.365 | 0.481 | ||
| Sex | 0.03 * | 0.01 * | |||||
| Male | 43 | 3.077 | 0.944 | 0.315 | 0.464 | ||
| Female | 64 | 3.245 | 0.929 | 0.431 | 0.495 | ||
| Religion | 0.30 | 0.74 | |||||
| Buddhism | 101 | 3.187 | 0.936 | 0.357 | 0.479 | ||
| Islam | 6 | 3.013 | 0.967 | 0.372 | 0.493 | ||
| Educational level | <0.001 * | <0.001 * | |||||
| No formal education | 2 | 3.308 | 0.928 | 0.615 | 0.487 | ||
| Primary education | 49 | 3.306 | 0.911 | 0.394 | 0.489 | ||
| Above primary education | 56 | 3.060 | 0.949 | 0.317 | 0.465 | ||
| Average monthly income, THB | 0.02 * | <0.001 * | |||||
| ≤10,000 | 63 | 3.250 | 0.920 | 0.410 | 0.492 | ||
| >10,000 | 44 | 3.073 | 0.955 | 0.283 | 0.451 | ||
| Time since diagnosis, years | 0.82 | 0.61 | |||||
| <10 | 62 | 3.170 | 0.948 | 0.352 | 0.478 | ||
| ≥10 | 45 | 3.188 | 0.926 | 0.366 | 0.482 | ||
| Dyslipidemia | 0.34 | 0.32 | |||||
| No | 7 | 3.319 | 0.863 | 0.407 | 0.491 | ||
| Yes | 100 | 3.168 | 0.943 | 0.355 | 0.478 | ||
| Hypertension | 0.16 | 0.12 | |||||
| No | 35 | 3.099 | 0.924 | 0.330 | 0.470 | ||
| Yes | 72 | 3.216 | 0.943 | 0.372 | 0.483 | ||
| Another comorbidity | 0.57 | 0.03 * | |||||
| No | 101 | 3.172 | 0.942 | 0.365 | 0.481 | ||
| Yes | 6 | 3.269 | 0.872 | 0.244 | 0.429 | ||
| Current diabetes treatment | 0.08 | 0.15 | |||||
| Insulin therapy | 11 | 3.469 | 1.070 | 0.378 | 0.485 | ||
| Oral anti-diabetic drug | 90 | 3.138 | 0.923 | 0.362 | 0.481 | ||
| Lifestyle modification (no medication) | 6 | 3.231 | 0.799 | 0.256 | 0.439 | ||
| Diabetic complications | 0.50 | 0.09 | |||||
| Current diabetic retinopathy | 3 | 3.173 | 0.942 | 0.487 | 0.506 | ||
| No diabetic complications | 104 | 3.333 | 0.795 | 0.354 | 0.478 | ||
| Cognitive Attitude | Intention to Share | ||||
|---|---|---|---|---|---|
| Factor | Beta (95% CI) | p-Value | Factor | Beta (95% CI) | p-Value |
| Educational level: Primary | −1.72 (8.42, 4.99) | 0.61 | Monthly income (THB) ≤10,000 vs. >10,000 | 0.67 (−0.22, 1.56) | 0.14 |
| Educational level: Above primary | −4.84 (−11.51, 1.83) | 0.15 | Comorbidity #: present vs. absent | −2.04 (−3.88, −0.20) | 0.03 * |
| Source from the healthcare provider’s score | 0.97 (0.43, 1.51) | <0.001 * | Current treatment: oral anti-diabetic drugs | 2.01 (0.50, 3.52) | 0.01 * |
| Source from the diabetes patient score | 0.48 (0.09, 0.87) | 0.02 * | Current treatment: insulin therapy | −0.28 (−2.56, 1.99) | 0.80 |
| Model; Adjusted R-squared: 0.20, Residual standard error: 4.64 | Source from healthcare provider score | 0.40 (0.11, 0.68) | 0.01 * | ||
| Attitude score | 0.24 (0.15, 0.33) | <0.001 * | |||
| Exposure score | 0.46 (0.29, 0.63) | <0.001 * | |||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pratueangpong, T.; Buathong, N.; Sornsenee, P. Prevalence of Common Diabetes Mellitus Misinformation Exposure, Cognitive Attitude, and Intention to Share Information Among Patients in a Primary Care Unit. Healthcare 2025, 13, 1762. https://doi.org/10.3390/healthcare13141762
Pratueangpong T, Buathong N, Sornsenee P. Prevalence of Common Diabetes Mellitus Misinformation Exposure, Cognitive Attitude, and Intention to Share Information Among Patients in a Primary Care Unit. Healthcare. 2025; 13(14):1762. https://doi.org/10.3390/healthcare13141762
Chicago/Turabian StylePratueangpong, Thanapol, Napakkawat Buathong, and Phoomjai Sornsenee. 2025. "Prevalence of Common Diabetes Mellitus Misinformation Exposure, Cognitive Attitude, and Intention to Share Information Among Patients in a Primary Care Unit" Healthcare 13, no. 14: 1762. https://doi.org/10.3390/healthcare13141762
APA StylePratueangpong, T., Buathong, N., & Sornsenee, P. (2025). Prevalence of Common Diabetes Mellitus Misinformation Exposure, Cognitive Attitude, and Intention to Share Information Among Patients in a Primary Care Unit. Healthcare, 13(14), 1762. https://doi.org/10.3390/healthcare13141762






