A Nursing Process for Shared Decision-Making for Patients with Severe Mental Illness Receiving Treatment Involving Long-Term Coercive Measures: A Modified Grounded Theory Approach
Abstract
1. Introduction
2. Materials and Methods
2.1. Research Design
2.2. Participants
2.3. Data Collection
2.4. Data Analysis
2.5. Ethical Considerations
3. Results
3.1. Participants’ Demographic Information
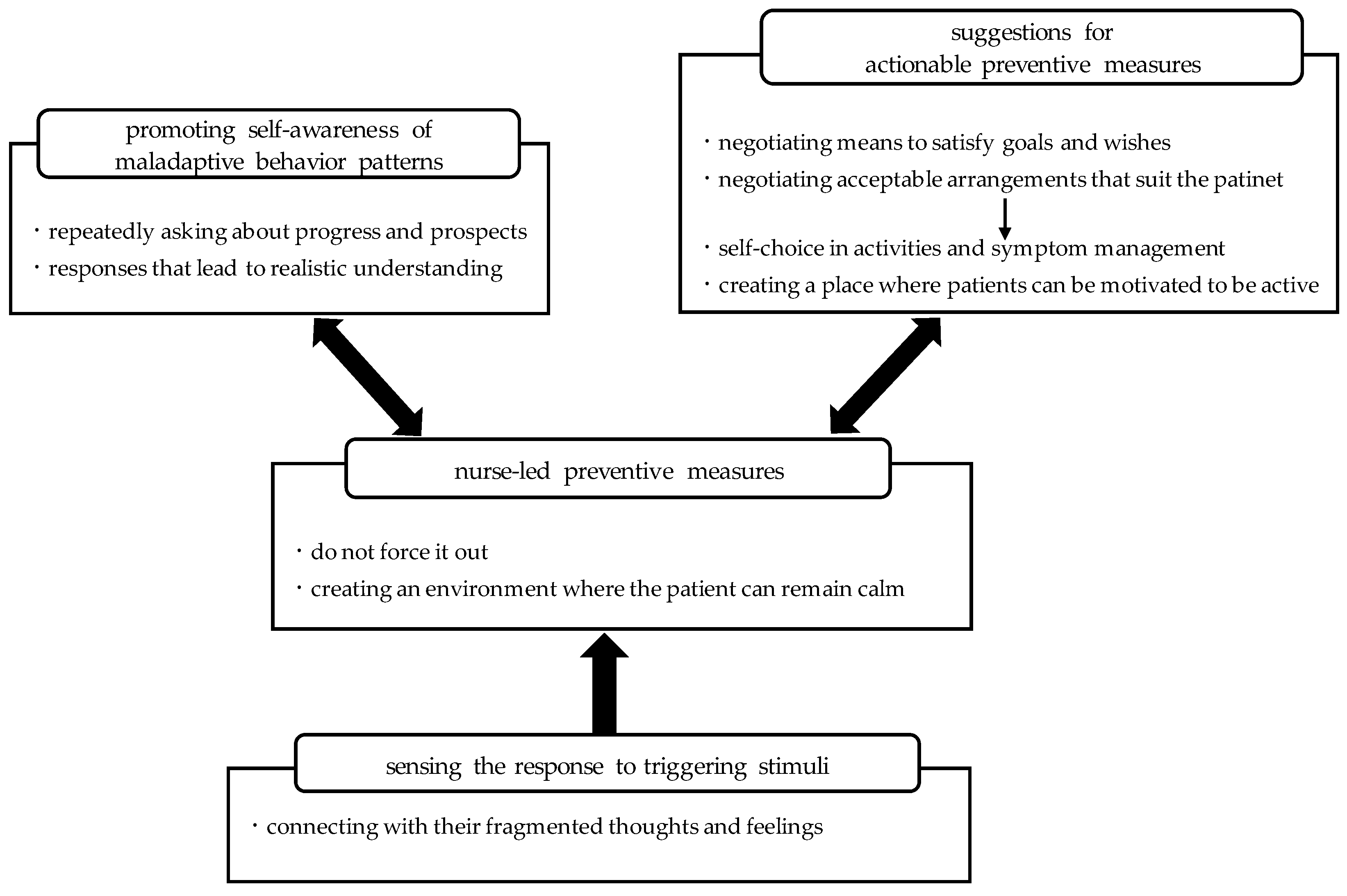
3.2. Storyline
3.3. Categories and Concepts
3.3.1. Category: Sensing the Response to Triggering Stimuli
Concept: Connecting with Their Fragmented Thoughts and Feelings
When I ask patients, “Why do you think you’re feeling well now?” they say they don’t know. This shows that patients have a hard time expressing their feelings in their own words. When a nurse says, “How about this?” or “This is what it is, so this is what it is”, the patient’s answers often seem like those of parrots. Nevertheless, the patient can answer.(J)
3.3.2. Category: Nurse-Led Preventive Measures
Concept: Do Not Force It Out
Patients sometimes simply do not accept it. Even when I approach patients under the assumption that they appear to be calm, there are times when they are still not receptive to conversation. At such times, I do not try to forcefully draw out the patient’s thoughts and feelings or deepen the discussion; instead, I resume the conversation in a calm manner.(K)
Concept: Creating an Environment Where the Patient Can Remain Calm
The patient is quite vocal and restless before meal times. He suddenly starts saying “Food, food” and then says “I’m going home”. We are particular about meal times. Another time, I was calmly soaking up the sun and feeling relaxed, but then I suddenly became restless when I heard other patients and staff talking about food. Therefore, I avoided open observation during meal times and instead conducted open observation from 2 to 4 p.m.(I)
When the patient is in the room, he talks about “someone coming in”, states that “the ceiling is falling down”, and becomes increasingly anxious. We wanted patients to feel at ease when they were in the room, so we decided to reverse the head and foot ends of the bed. By changing the position of the bed, ceiling vents and lighting may appear different when the patient looks up. Also, you may feel safer if you can’t see the entrance, if your head is facing the door. The patient’s line of sight is positioned so that the patient can see the balcony through the acrylic panel. Maybe the patient is not paying attention to the door. The patient likes where he is now.(M)
3.3.3. Category: Promoting Self-Awareness of Maladaptive Behavior Patterns
Concept: Repeatedly Asking about Progress and Prospects
If a patient continues to behave in a particular way, such as getting angry at the nurse, acting violently in the room, or refusing to take his or her medication, I tell them that no matter how long they stall, they will not be discharged from the hospital because treatment will not progress. I am referring to things like not taking specific medicines properly, getting angry, or acting harshly toward medical professionals.(L)
Concept: Responses That Lead to Realistic Understanding
Patients come to the nurse center to talk and make requests. One patient had the delusion that his clothes stank. The patient told the nurse, “My clothes stink again, so I want you to change them”, and “My body stinks, so I want you to look at my butt”. The nurse looked at the patient’s body and said, “You’re perfectly fine”, and the patient calmed down. The nurse looked over toward the patient and told him, “It’s okay”.(O)
3.3.4. Category: Suggestions for Actionable Preventive Measures
Concept: Negotiating Means to Satisfy Goals and Wishes
The requests are always the same, such as wanting clothes or a watch. Once, we gave a patient a watch, but he broke it. For financial reasons, I can’t give out a watch every time. We thought about what we could do to placate the patient, so we asked him to make his own clock. The patient was satisfied and stopped banging on the wall. Together, nurses and patients consider how patients can meet their own needs.(Q)
Concept: Negotiating Acceptable Arrangements That Suit the Patient
There were times when I couldn’t get the patients to take a bath for about a month. If the patient was in a bad mood, he would get angry even if I asked him if he would like to take a bath. The patient was reluctant to take a bath or change his clothes. The patient did not feel that delusions were involved. I didn’t feel like there was any reason for his reluctance. I get the impression that it doesn’t matter if you don’t enter. I suggested some minimum goals to him, such as, “Let’s change our clothes at least once a week”.(J)
Concept: Creating a Place Where Patients Can Be Motivated to Be Active
The patient often reads newspapers and watches baseball games on TV. When a patient does something that they normally do when they are feeling well, I say to them, “You’re reading the newspaper properly today”. Other activities include attending occupational therapy and riding a stationary bike. When I see someone riding an exercise bike, I say to them, “I see you’re riding your bike today”. I think a good indicator of how a patient is doing is seeing that they are motivated to ride the bike.(M)
Concept: Self-Choice in Activities and Symptom Management
Patients can tap on the nursing center window and say, “I need some help”. However, patients may not give us time to prepare for the situation. The patient sends out an “SOS”, and I ask, “So what do we do? Sometimes the patient says, “But I don’t want to drink”, and sometimes they say, “Okay, I’ll drink”. How the patient behaves is left up to them. Of course I won’t force it. However, if a patient is feeling unwell for a long time or is in a state of agitation, we may recommend coercive measures.(B)
Patients can walk around the hospital with the assistance of a nurse. I asked a patient, “What do you want to do?” and the patient said that he wanted to sit in a chair. Patients are often relaxing in a chair in front of the TV, and we can confirm that their stated intentions were genuine. Additionally, even when I am observing patients in open conditions, they may want to go back to their rooms, so I respect their wishes and allow them to be where they want to be.(I)
4. Discussion
5. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Elwyn, G.; Frosch, D.; Thomson, R.; Joseph-Williams, N.; Lloyd, A.; Kinnersley, P.; Cording, E.; Tomson, D.; Dodd, C.; Rollnick, S.; et al. Shared Decision Making: A Model for Clinical Practice. J. Gen. Intern. Med. 2012, 27, 1361–1367. [Google Scholar] [CrossRef] [PubMed]
- Charles, C.; Gafni, A.; Whelan, T. Shared Decision-Making in the Medical Encounter: What Does It Mean? (Or It Takes at Least Two to Tango). Soc. Sci. Med. 1997, 44, 681–692. [Google Scholar] [CrossRef] [PubMed]
- Gurtner, C.; Schols, J.M.G.A.; Lohrmann, C.; Halfens, R.J.G.; Hahn, S. Conceptual Understanding and Applicability of Shared Decision-Making in Psychiatric Care: An Integrative Review. J. Psychiatr. Ment. Health Nurs. 2021, 28, 531–548. [Google Scholar] [CrossRef] [PubMed]
- Aoki, Y. Shared Decision Making for Adults with Severe Mental Illness: A Concept Analysis. Jpn. J. Nurs. Sci. 2020, 17, e12365. [Google Scholar] [CrossRef] [PubMed]
- Ministry of Health. Labour and Welfare Act on Mental Health and Welfare for Persons with Mental Disorders or Disabilities. Available online: https://www.japaneselawtranslation.go.jp/en/laws/view/4235 (accessed on 27 April 2024).
- Noda, T.; Sugiyama, N.; Sato, M.; Ito, H.; Sailas, E.; Putkonen, H.; Kontio, R.; Joffe, G. Influence of Patient Characteristics on Duration of Seclusion/Restrain in Acute Psychiatric Settings in Japan. Psychiatry Clin. Neurosci. 2013, 67, 405–411. [Google Scholar] [CrossRef] [PubMed]
- Fukasawa, M.; Miyake, M.; Suzuki, Y.; Fukuda, Y.; Yamanouchi, Y. Relationship between the Use of Seclusion and Mechanical Restraint and the Nurse-Bed Ratio in Psychiatric Wards in Japan. Int. J. Law Psychiatry 2018, 60, 57–63. [Google Scholar] [CrossRef] [PubMed]
- Mgutshini, T. Risk Factors for Psychiatric Re-Hospitalization: An Exploration. Int. J. Ment. Health Nurs. 2010, 19, 257–267. [Google Scholar] [CrossRef] [PubMed]
- Frueh, B.C.; Knapp, R.G.; Cusack, K.J.; Grubaugh, A.L.; Sauvageot, J.A.; Cousins, V.C.; Yim, E.; Robins, C.S.; Monnier, J.; Hiers, T.G. Special Section on Seclusion and Restraint: Patients’ Reports of Traumatic or Harmful Experiences within the Psychiatric Setting. Psychiatr. Serv. 2005, 56, 1123–1133. [Google Scholar] [CrossRef] [PubMed]
- Walji, I.; Egan, V.; Fonseca, A.; Huxley, A. The Relationship between Violence, Level of Functioning, and Treatment Outcome in Psychiatric Inpatients. J. Forensic Pract. 2014, 16, 295–303. [Google Scholar] [CrossRef]
- Mötteli, S.; Hotzy, F.; Lamster, F.; Horisberger, R.; Theodoridou, A.; Vetter, S.; Seifritz, E.; Jäger, M. Optimistic Recovery Expectations Are Associated with Critical Attitudes toward Coercion among Mental Health Professionals. Int. J. Ment. Health 2020, 49, 157–169. [Google Scholar] [CrossRef]
- Nagayama, Y.; Hasegawa, M. Nursing Care Process for Releasing Psychiatric Inpatients from Long-Term Seclusion in Japan: Modified Grounded Theory Approach. Nurs. Health Sci. 2014, 16, 284–290. [Google Scholar] [CrossRef] [PubMed]
- Wesseldijk-Elferink, I.J.M.; Hendriks, A.W.; van den Heuvel, S.C.G.H. Shared Decision Making in a Semi-Secluded Chronic Psychiatric Ward: The Reflective Lifeworld Experiences of Patients with Schizophrenia or Schizoaffective Disorders and Nursing Staff. Arch. Psychiatr. Nurs. 2021, 35, 519–525. [Google Scholar] [CrossRef] [PubMed]
- Nagayama, Y.; Tanaka, K.; Oe, M. Strengths Model-Based Nursing Interventions for Inpatients in Psychiatric Inpatient Settings Using a Seclusion Room: A Case Series Study. Nurs. Rep. 2023, 13, 644–658. [Google Scholar] [CrossRef] [PubMed]
- Fitzgerald, S.; Chan, F.; Deiches, J.; Umucu, E.; Hsu, S.-T.; Lee, H.-L.; Bezyak, J.; Iwanaga, K. Assessing Self-Determined Work Motivation in People with Severe Mental Illness: A Factor-Analytic Approach. Aust. J. Rehabil. Couns. 2015, 21, 123–136. [Google Scholar] [CrossRef]
- Kinoshita, Y. Teihon M-GTA Jissenn No Rironka Wo Mezasu Situtekikenkyuuhouhouronn. Modified Grounded Theory Approach, Qualitative Methodology to Aim for Theorization of Practice; Igakushoin: Tokyo, Japan, 2020. [Google Scholar]
- Glaser, B.; Strauss, A. The Discovery of Grounded Theory: Strategies for Qualitative Research; Aldine: Chicago, IL, USA, 1967. [Google Scholar]
- The Japanese Society of M-GTA. The Japanese Society of M-GTA Q&A. Available online: https://m-gta.jp/en/qa.html (accessed on 28 March 2024).
- Voogt, L.A.; Goossens, P.J.J.; Nugter, A.; van Achterberg, T. The Patient’s Perspective on “Providing Structure” in Psychiatric Inpatient Care: An Interview Study. Perspect. Psychiatr. Care 2015, 51, 136–147. [Google Scholar] [CrossRef] [PubMed]
- Taua, C.; Farrow, T. Negotiating Complexities: An Ethnographic Study of Intellectual Disability and Mental Health Nursing in New Zealand. Int. J. Ment. Health Nurs. 2009, 18, 274–284. [Google Scholar] [CrossRef] [PubMed]
- Mahone, I.H.; Farrell, S.; Hinton, I.; Johnson, R.; Moody, D.; Rifkin, K.; Moore, K.; Becker, M.; Barker, M.R. Shared Decision Making in Mental Health Treatment: Qualitative Findings from Stakeholder Focus Groups. Arch. Psychiatr. Nurs. 2011, 25, e27–e36. [Google Scholar] [CrossRef] [PubMed]
- Lenk-Adusoo, M.; Hürden, L.; Tohvre, R.; Tretjakov, I.; Evert, L.; Haring, L. Healthcare Professionals’ and Patients’ Attitudes toward the Causes and Management of Aggression in Estonian Psychiatric Clinics: A Quantitative Cross-Sectional Comparative Study. J. Ment. Health 2022, 31, 699–708. [Google Scholar] [CrossRef] [PubMed]
- Olsson, H.; Schön, U.-K. Reducing Violence in Forensic Care—How Does It Resemble the Domains of a Recovery-Oriented Care? J. Ment. Health 2016, 25, 506–511. [Google Scholar] [CrossRef]
- Ljungberg, A.; Denhov, A.; Topor, A. Non-Helpful Relationships with Professionals—A Literature Review of the Perspective of Persons with Severe Mental Illness. J. Ment. Health 2016, 25, 267–277. [Google Scholar] [CrossRef]
- Fervaha, G.; Foussias, G.; Agid, O.; Remington, G. Motivational Deficits in Early Schizophrenia: Prevalent, Persistent, and Key Determinants of Functional Outcome. Schizophr. Res. 2015, 166, 9–16. [Google Scholar] [CrossRef] [PubMed]
- Schauer, C.; Everett, A.; del Vecchio, P.; Anderson, L. Promoting the Value and Practice of Shared Decision-Making in Mental Health Care. Psychiatr. Rehabil. J. 2007, 31, 54–61. [Google Scholar] [CrossRef] [PubMed]
- Mahone, I.; Maphis, C.; Snow, D. Effective Strategies for Nurses Empowering Clients with Schizophrenia: Medication Use as a Tool in Recovery. Issues Ment. Health Nurs. 2016, 37, 372–379. [Google Scholar] [CrossRef] [PubMed]
| Participant ID | Years of Nursing Experience | Years of Psychiatric Nursing Experience | Diagnosis of Patients as Described by Participants | Reasons for Coersive Measures | Types of Coersive Measures |
|---|---|---|---|---|---|
| A | 7 | 4 | Schizophrenia, intellectual developmental disorder | Self-harm | Seclusion, physical restraint |
| B | 8 | 8 | Schizophrenia | Agitation, restlessness, self-harm, harm to others | Seclusion, physical restraint |
| C | 10 | 10 | Schizophrenia, intellectual developmental disorder | Agitation, restlessness, harm to others, nuisance | Seclusion |
| D | 7 | 2 | Schizophrenia | Agitation, restlessness, self-harm, harm to others | Seclusion, physical restraint |
| E | 20 | 14 | Schizophrenia | Harm to others | Seclusion |
| F | 28 | 28 | Schizophrenia, intellectual developmental disorder | Harm to others, polydipsia | Seclusion |
| G | 25 | 15 | Schizophrenia, intellectual developmental disorder | Agitation, restlessness, harm to others | Seclusion |
| H | 19 | 19 | Schizophrenia, intellectual developmental disorder | Self-harm, harm to others | Seclusion, physical restraint |
| I | 10 | 3 | Schizophrenia | Agitation, restlessness | Seclusion |
| J | 23 | 20 | Schizophrenia | Self-harm, harm to others | Seclusion, physical restraint |
| K | 15 | 10 | Schizophrenia | Self-harm | Seclusion, physical restraint |
| L | 10 | 6 | Schizophrenia | Self-harm | Seclusion, physical restraint |
| M | 24 | 11 | Schizophrenia | Self-harm | Seclusion, physical restraint |
| N | 26 | 19 | Schizophrenia, intellectual developmental disorder | Harm to others, nuisance | Seclusion |
| O | 10 | 6 | Schizophrenia | Harm to others, nuisance | Seclusion |
| P | 11 | 11 | Schizophrenia | Harm to others | Seclusion |
| Q | 13 | 7 | Schizophrenia | Harm to others | Seclusion |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nagayama, Y. A Nursing Process for Shared Decision-Making for Patients with Severe Mental Illness Receiving Treatment Involving Long-Term Coercive Measures: A Modified Grounded Theory Approach. Healthcare 2024, 12, 967. https://doi.org/10.3390/healthcare12100967
Nagayama Y. A Nursing Process for Shared Decision-Making for Patients with Severe Mental Illness Receiving Treatment Involving Long-Term Coercive Measures: A Modified Grounded Theory Approach. Healthcare. 2024; 12(10):967. https://doi.org/10.3390/healthcare12100967
Chicago/Turabian StyleNagayama, Yutaka. 2024. "A Nursing Process for Shared Decision-Making for Patients with Severe Mental Illness Receiving Treatment Involving Long-Term Coercive Measures: A Modified Grounded Theory Approach" Healthcare 12, no. 10: 967. https://doi.org/10.3390/healthcare12100967
APA StyleNagayama, Y. (2024). A Nursing Process for Shared Decision-Making for Patients with Severe Mental Illness Receiving Treatment Involving Long-Term Coercive Measures: A Modified Grounded Theory Approach. Healthcare, 12(10), 967. https://doi.org/10.3390/healthcare12100967






