Quality of Life in Amyotrophic Lateral Sclerosis Patients and Care Burden of Caregivers in Sardinia during COVID-19 Pandemic
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Setting
2.2. Study Design
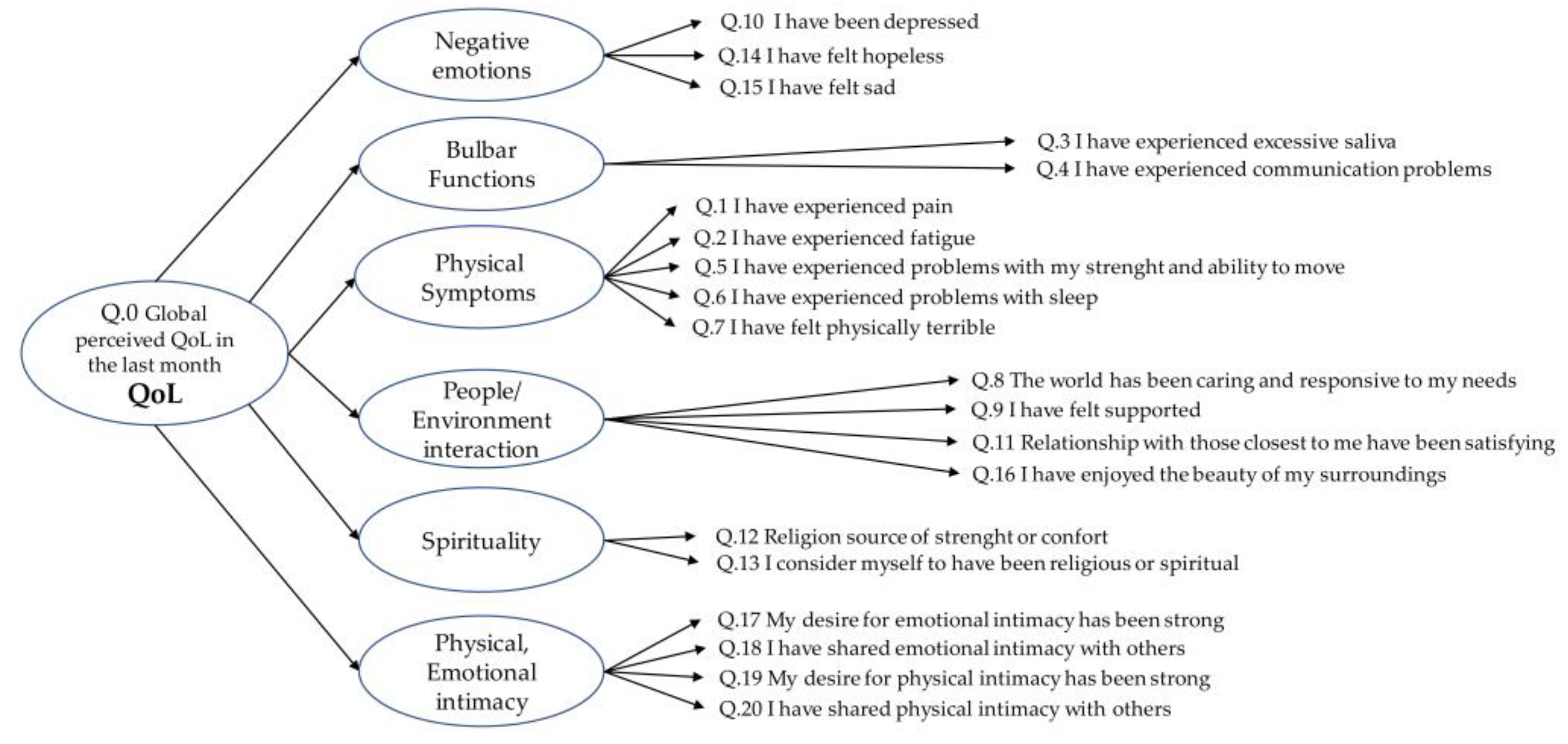
2.3. Questionnaire Design
2.4. Statistical Analysis
3. Results
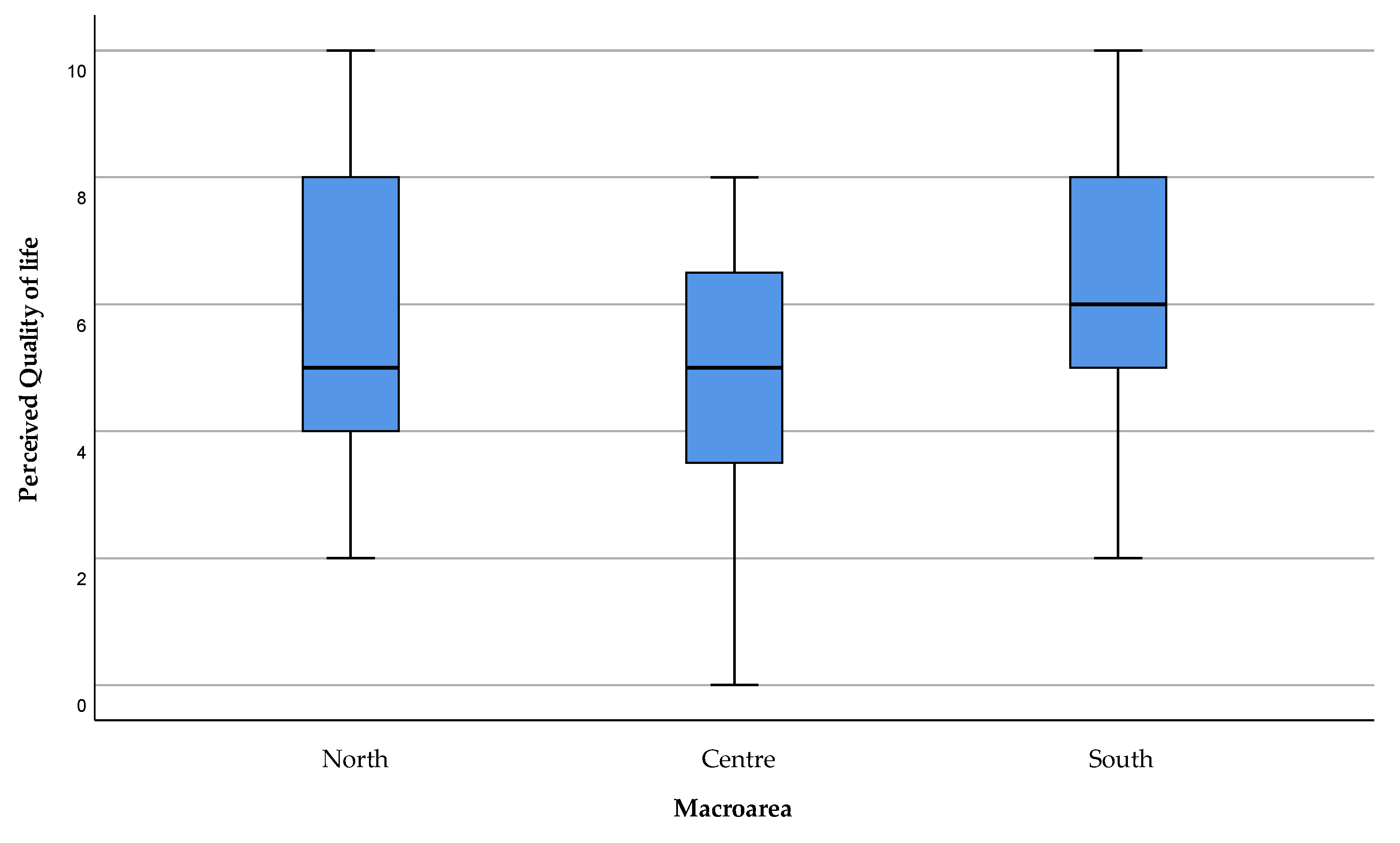
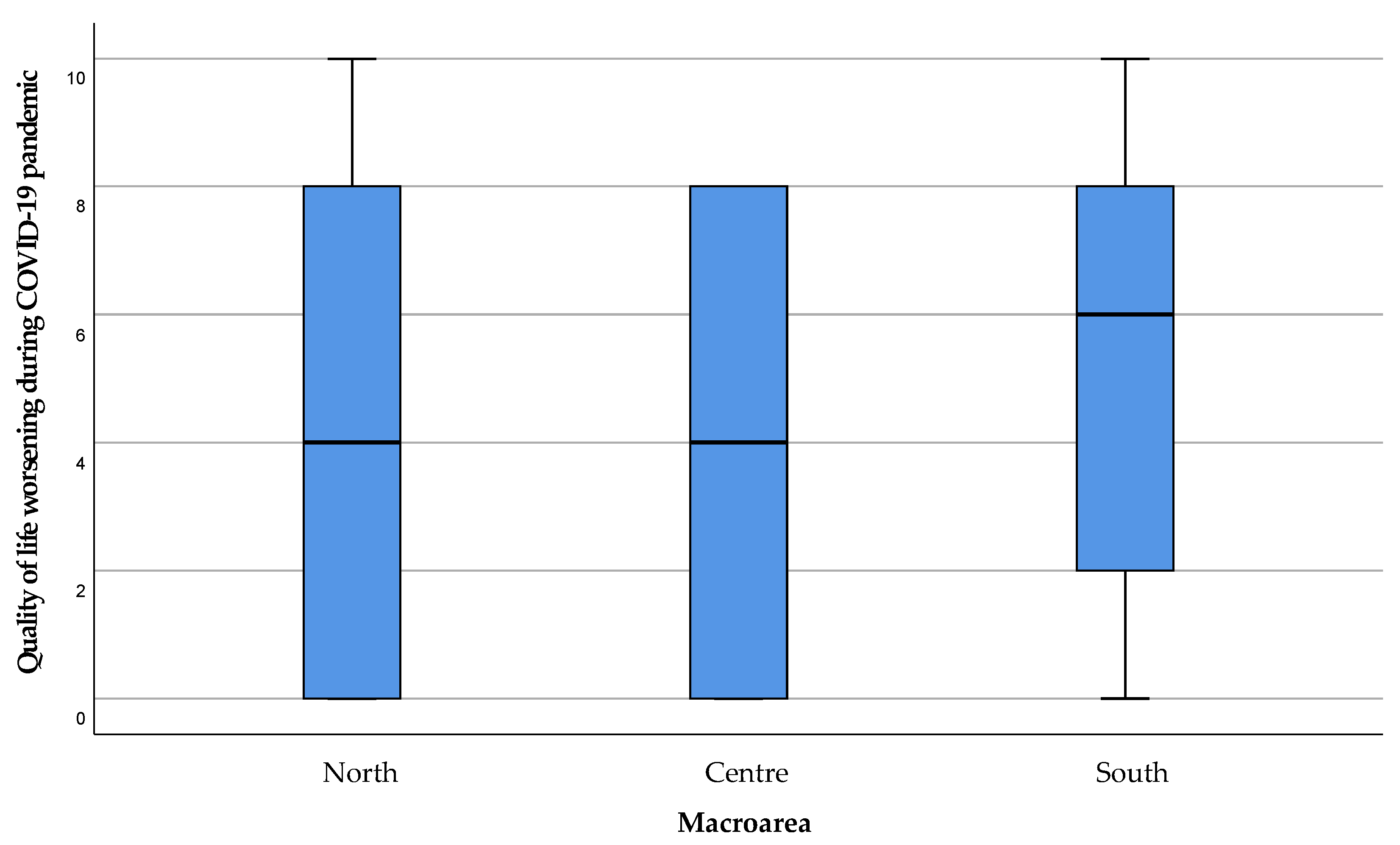
3.1. Quality of Life of the ALS Patient in Sardinia—Modified ALSSQOL-SF
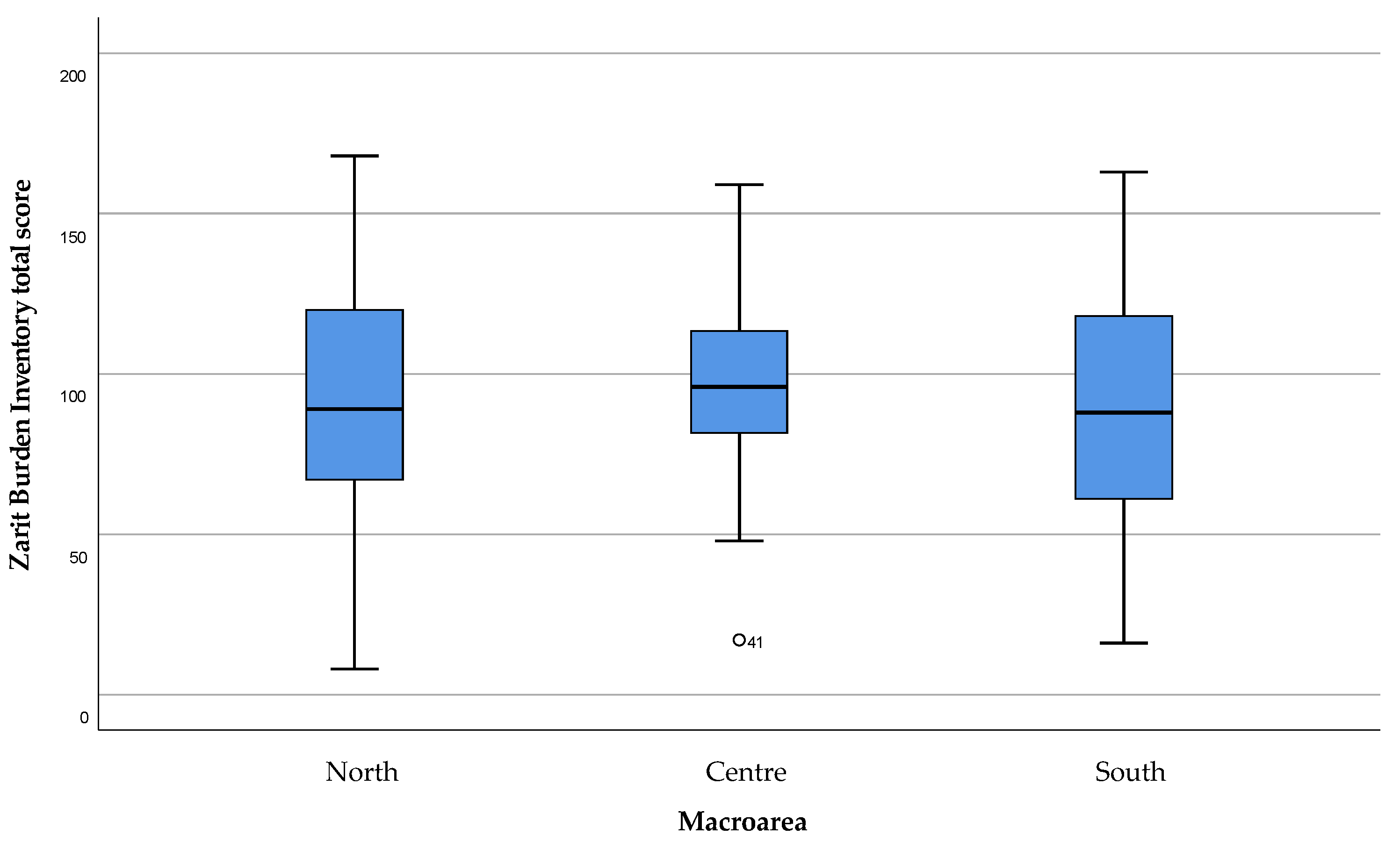
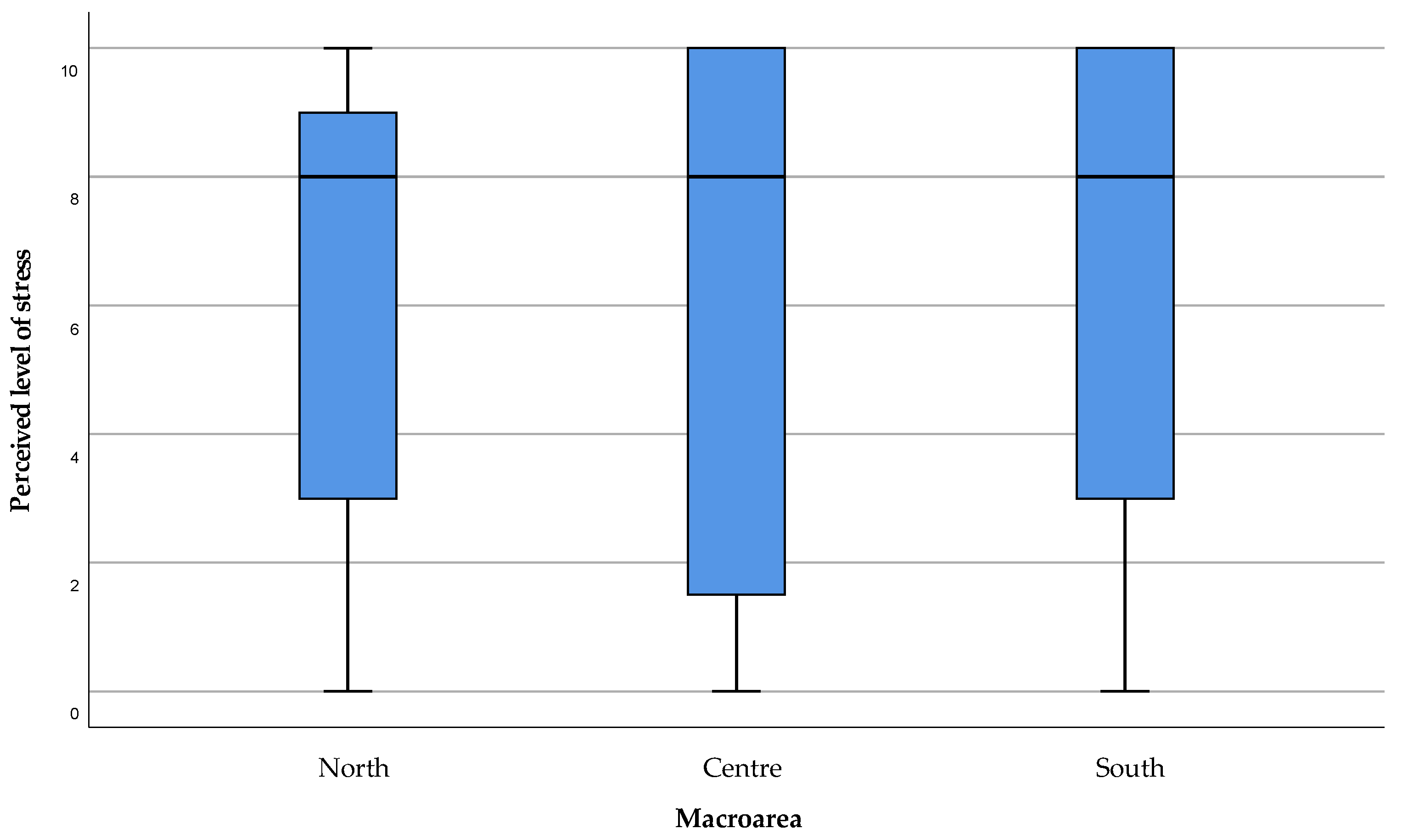
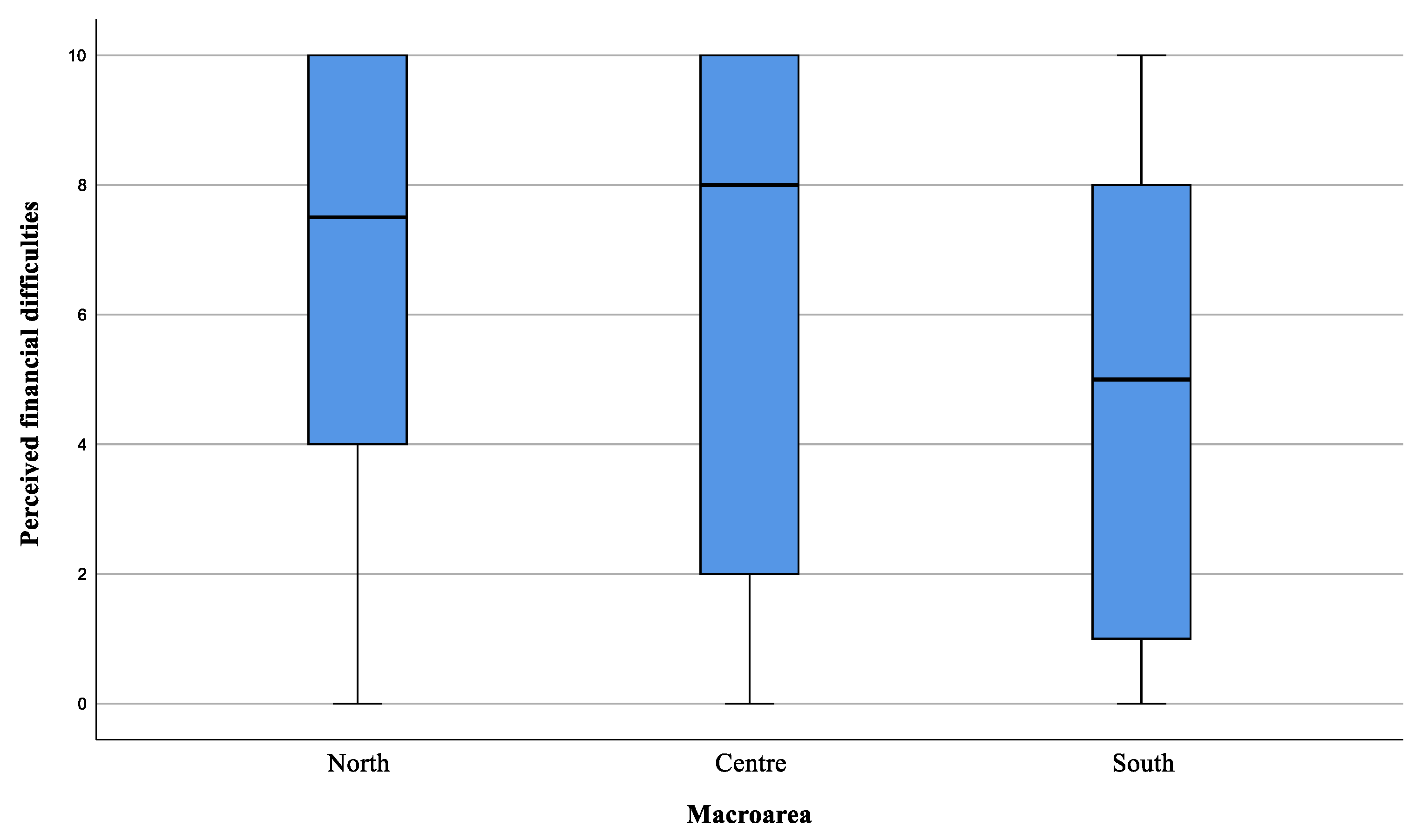
3.2. Caregivers’ Burden—Modified Zarit Burden Interview
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Hardiman, O.; Al-Chalabi, A.; Chio, A.; Corr, E.M.; Logroscino, G.; Robberecht, W.; Shaw, P.J.; Simmons, Z.; van den Berg, L.H. Amyotrophic lateral sclerosis. Nat. Rev. Dis. Primers 2017, 3, 17071. [Google Scholar] [CrossRef]
- Brown, R.H.; Al-Chalabi, A. Amyotrophic Lateral Sclerosis. N. Engl. J. Med. 2017, 377, 162–172. [Google Scholar] [CrossRef] [PubMed]
- van Es, M.A.; Hardiman, O.; Chio, A.; Al-Chalabi, A.; Pasterkamp, R.J.; Veldink, J.H.; van den Berg, L.H. Amyotrophic lateral sclerosis. Lancet 2017, 390, 2084–2098. [Google Scholar] [CrossRef] [PubMed]
- Masrori, P.; Van Damme, P. Amyotrophic lateral sclerosis: A clinical review. Eur. J. Neurol. 2020, 27, 1918–1929. [Google Scholar] [CrossRef]
- Srinivasan, E.; Rajasekaran, R. A Systematic and Comprehensive Review on Disease-Causing Genes in Amyotrophic Lateral Sclerosis. J. Mol. Neurosci. 2020, 70, 1742–1770. [Google Scholar] [CrossRef] [PubMed]
- Logroscino, G.; Piccininni, M. Amyotrophic Lateral Sclerosis Descriptive Epidemiology: The Origin of Geographic Difference. Neuroepidemiology 2019, 52, 93–103. [Google Scholar] [CrossRef]
- Logroscino, G.; Traynor, B.J.; Hardiman, O.; Chiò, A.; Mitchell, D.; Swingler, R.J.; Millul, A.; Benn, E.; Beghi, E.; Eurals, F. Incidence of amyotrophic lateral sclerosis in Europe. J. Neurol. Neurosurg. Psychiatry 2009, 81, 385–390. [Google Scholar] [CrossRef]
- GBD 2016 Motor Neuron Disease Collaborators. Global, regional, and national burden of motor neuron diseases 1990–2016: A systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol. 2018, 17, 1083–1097. [Google Scholar] [CrossRef]
- Chiò, A.; Logroscino, G.; Hardiman, O.; Swingler, R.; Mitchell, D.; Beghi, E.; Traynor, B.G.; On Behalf of the Eurals Consortium. Prognostic factors in ALS: A critical review. Amyotroph. Lateral Scler. 2009, 10, 310–323. [Google Scholar] [CrossRef]
- Couratier, P.; Corcia, P.; Lautrette, G.; Nicol, M.; Preux, P.-M.; Marin, B. Epidemiology of amyotrophic lateral sclerosis: A review of literature. Rev. Neurol. 2015, 172, 37–45. [Google Scholar] [CrossRef]
- Chiò, A.; Logroscino, G.; Traynor, B.J.; Collins, J.; Simeone, J.C.; Goldstein, L.A.; White, L.A. Global epidemiology of amyotrophic lateral sclerosis: A systematic review of the published literature. Neuroepidemiology. 2013, 41, 118–130. [Google Scholar] [CrossRef] [PubMed]
- Worms, P.M. The epidemiology of motor neuron diseases: A review of recent studies. J. Neurol. Sci. 2001, 191, 3–9. [Google Scholar] [CrossRef] [PubMed]
- ALS Association Websaite. About ALS. Available online: https://www.als.org/understanding-als/who-gets-als (accessed on 6 May 2021).
- The Whoqol Group The World Health Organization quality of life assessment (WHOQOL): Development and general psychometric properties. Soc. Sci. Med. 1998, 46, 1569–1585. [CrossRef] [PubMed]
- Aoun, S.M.; Connors, S.L.; Priddis, L.; Breen, L.J.; Colyer, S. Motor Neurone Disease family carers’ experiences of caring, palliative care and bereavement: An exploratory qualitative study. Palliat. Med. 2012, 26, 842–850. [Google Scholar] [CrossRef] [PubMed]
- Galvin, M.; Corr, B.; Madden, C.; Mays, I.; McQuillan, R.; Timonen, V.; Staines, A.; Hardiman, O. Caregiving in ALS—A mixed methods approach to the study of Burden. BMC Palliat. Care 2016, 15, 81. [Google Scholar] [CrossRef] [PubMed]
- Sherman, D.W. A Review of the Complex Role of Family Caregivers as Health Team Members and Second-Order Patients. Healthcare 2019, 7, 63. [Google Scholar] [CrossRef] [PubMed]
- O’Brien, M.R.; Whitehead, B.; Jack, B.A.; Mitchell, J.D. From symptom onset to a diagnosis of amyotrophic lateral sclerosis/motor neuron disease (ALS/MND): Experiences of people with ALS/MND and family carers—A qualitative study. Amyotroph. Lateral Scler. 2011, 12, 97–104. [Google Scholar] [CrossRef] [PubMed]
- O’connor, E.J.; McCabe, M.P. Predictors of quality of life in carers for people with a progressive neurological illness: A longitudinal study. Qual. Life Res. 2011, 20, 703–711. [Google Scholar] [CrossRef]
- Trail, M.; Nelson, N.D.; Van, J.N.; Appel, S.H.; Lai, E.C. A study comparing patients with amyotrophic lateral sclerosis and their caregivers on measures of quality of life, depression, and their attitudes toward treatment options. J. Neurol. Sci. 2003, 209, 79–85. [Google Scholar] [CrossRef]
- Goldstein, L.H.; Atkins, L.; Landau, S.; Brown, R.; Leigh, P.N. Predictors of psychological distress in carers of people with amyotrophic lateral sclerosis: A longitudinal study. Psychol. Med. 2006, 36, 865–875. [Google Scholar] [CrossRef]
- De Wit, J.; Bakker, L.A.; Van Groenestijn, A.C.; van den Berg, L.H.; Schröder, C.D.; Visser-Meily, J.M.; Beelen, A. Caregiver burden in amyotrophic lateral sclerosis: A systematic review. Palliat. Med. 2018, 32, 231–245. [Google Scholar] [CrossRef]
- Boerner, K.; Mock, S.E. Impact of patient suffering on caregiver well-being: The case of amyotrophic lateral sclerosis patients and their caregivers. Psychol. Health Med. 2012, 17, 457–466. [Google Scholar] [CrossRef]
- Ray, R.A.; Street, A.F. Caregiver bodywork: Family members’ experiences of caring for a person with motor neurone disease. J. Adv. Nurs. 2006, 56, 35–43. [Google Scholar] [CrossRef] [PubMed]
- Chio, A.; Gauthier, A.; Vignola, A.; Calvo, A.; Ghiglione, P.; Cavallo, E.; Terreni, A.A.; Mutani, R. Caregiver time use in ALS. Neurology 2006, 67, 902–904. [Google Scholar] [CrossRef] [PubMed]
- Regione Autonoma della Sardegna. Allegato alla Delib.G.R. n. 63/12 del 11.12.2020. Interventi di Sostegno alla Domiciliarità per le Persone con Disabilità Gravissime. Available online: https://delibere.regione.sardegna.it/protected/53510/0/def/ref/DBR53467/ (accessed on 11 December 2020).
- Felgoise, S.H.; Walsh, S.M.; Stephens, H.E.; Brothers, A.; Simmons, Z. The ALS Specific Quality of Life-Revised (ALSSQOL-R) User’s Guide. Available online: https://www.pennstatehealth.org/sites/default/files/Neurology/ALSSQOL-%20Manual.pdf (accessed on 1 February 2021).
- Simmons, Z.; Felgoise, S.H.; Rodriguez, J.L.; Walsh, S.M.; Bremer, B.A.; Stephens, H.E. Validation of a shorter ALS-specific quality of life instrument: The ALSSQOL-R. Neurology 2010, 74 (Suppl. 2), A177–A178. [Google Scholar]
- Simmons, Z.; Felgoise, S.H.; Bremer, B.A.; Walsh, S.M.; Hufford, D.J.; Bromberg, M.B.; David, W.; Forshew, D.A.; Heiman-Patterson, T.D.; Lai, E.C.; et al. The ALSSQOL: Balancing physical and nonphysical factors in assessing quality of life in ALS. Neurology 2006, 67, 1659–1664. [Google Scholar] [CrossRef]
- Felgoise, S.H.; Feinberg, R.; Stephens, H.E.; Barkhaus, P.; Boylan, K.; Caress, J.; Clawson, L.L.; Elman, L.; Goutman, S.A.; McCluskey, L.; et al. Amyotrophic lateral sclerosis-specific quality of life-short form (ALSSQOL-SF): A brief, reliable, and valid version of the ALSSQOL-R. Muscle Nerve 2018, 58, 646–654. [Google Scholar] [CrossRef]
- Ware, J.E.; Sherbourne, C.D. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med. Care 1992, 30, 473–483. [Google Scholar] [CrossRef]
- Cohen, S.R.; Mount, B.M.; Strobel, M.G.; Bui, F. The McGill Quality of Life Questionnaire: A measure of quality of life appropriate for people with advanced disease. A preliminary study of validity and acceptability. Palliat. Med. 1995, 9, 207–219. [Google Scholar] [CrossRef]
- Bergner, M.; Bobbitt, R.A.; Carter, W.B.; Gilson, B.S. The Sickness Impact Profile: Development and Final Revision of a Health Status Measure. Med. Care 1981, 19, 787–805. [Google Scholar] [CrossRef]
- Jenkinson, R.F.C. Evidence for the validity and reliability of the ALS assessment questionnaire: The ALSAQ-40. Amyotroph. Lateral Scler. 2000, 1, 33–40. [Google Scholar] [CrossRef]
- Kiebert, G.M.; Green, C.; Murphy, C.; Mitchell, J.; O’Brien, M.; Burrell, A.; Leigh, P. Patients’ health-related quality of life and utilities associated with different stages of amyotrophic lateral sclerosis. J. Neurol. Sci. 2001, 191, 87–93. [Google Scholar] [CrossRef] [PubMed]
- Simmons, Z.; Bremer, B.A.; Robbins, R.A.; Walsh, S.M.; Fischer, S. Quality of life in ALS depends on factors other than strength and physical function. Neurology 2000, 55, 388–392. [Google Scholar] [CrossRef]
- Robbins, R.; Simmons, Z.; Bremer, B.; Walsh, S.; Fischer, S. Quality of life in ALS is maintained as physical function declines. Neurology 2001, 56, 442–444. [Google Scholar] [CrossRef] [PubMed]
- Kuzma-Kozakiewicz, M.; Andersen, P.M.; Ciecwierska, K.; Vázquez, C.; Helczyk, O.; Loose, M.; Uttner, I.; Ludolph, A.C.; Lulé, D. An observational study on quality of life and preferences to sustain life in locked-in state. Neurology 2019, 93, e938–e945. [Google Scholar] [CrossRef] [PubMed]
- “Simmons, Z. Patient-Perceived Outcomes and Quality of Life in ALS. Neurotherapeutics 2015, 12, 394–402. [Google Scholar] [CrossRef] [PubMed]
- Peseschkian, T.; Cordts, I.; Günther, R.; Stolte, B.; Zeller, D.; Schröter, C.; Weyen, U.; Regensburger, M.; Wolf, J.; Schneider, I.; et al. A Nation-Wide, Multi-Center Study on the Quality of Life of ALS Patients in Germany. Brain Sci. 2021, 11, 372. [Google Scholar] [CrossRef]
- Hébert, R.; Bravo, G.; Préville, M. Reliability, Validity and Reference Values of the Zarit Burden Interview for Assessing Informal Caregivers of Community-Dwelling Older Persons with Dementia. Can. J. Aging/Rev. Can. Vieil. 2000, 19, 494–507. [Google Scholar] [CrossRef]
- Chattat, R.; Cortesi, V.; Izzicupo, F.; Del Re, M.L.; Sgarbi, C.; Fabbo, A.; Bergonzini, E. The Italian version of the Zarit Burden Interview: A validation study. Int. Psychogeriatr. 2011, 23, 797–805. [Google Scholar] [CrossRef]
- Oh, J.; Kim, J.A. Factor analysis of the Zarit Burden Interview in family caregivers of patients with amyotrophic lateral sclerosis. Amyotroph. Lateral Scler. Front. Degener. 2018, 19, 50–56. [Google Scholar] [CrossRef]
- Rabkin, J.G.; Albert, S.M.; Del Bene, M.L.; O’Sullivan, I.; Tider, T.; Rowland, L.P.; Mitsumoto, H. Prevalence of depressive disorders and change over time in late-stage ALS. Neurology 2005, 65, 62–67. [Google Scholar] [CrossRef] [PubMed]
- McElhiney, M.C.; Rabkin, J.G.; Gordon, P.H.; Goetz, R.; Mitsumoto, H. Prevalence of fatigue and depression in ALS patients and change over time. J. Neurol. Neurosurg. Psychiatry 2009, 80, 1146–1149. [Google Scholar] [CrossRef] [PubMed]
- Cupp, J.; Simmons, Z.; Berg, A.; Felgoise, S.H.; Walsh, S.M.; Stephens, H.E. Psychological health in patients with ALS is maintained as physical function declines. Amyotroph. Lateral Scler. 2011, 12, 290–296. [Google Scholar] [CrossRef] [PubMed]
- Körner, S.; Kollewe, K.; Abdulla, S.; Zapf, A.; Dengler, R.; Petri, S. Interaction of physical function, quality of life and depression in Amyotrophic lateral sclerosis: Characterization of a large patient cohort. BMC Neurol. 2015, 15, 84. [Google Scholar] [CrossRef] [PubMed]
- van Groenestijn, A.C.; Reenen, E.T.K.-V.; Visser-Meily, J.M.A.; Berg, L.H.V.D.; Schröder, C.D. Associations between psychological factors and health-related quality of life and global quality of life in patients with ALS: A systematic review. Health Qual. Life Outcomes 2016, 14, 107. [Google Scholar] [CrossRef]
- Galvin, M.; Gavin, T.; Mays, I.; Heverin, M.; Hardiman, O. Individual quality of life in spousal ALS patient-caregiver dyads. Health Qual. Life Outcomes 2020, 18, 371. [Google Scholar] [CrossRef]
- Soofi, A.Y.; Bello-Haas, V.D.; Kho, M.E.; Letts, L. The impact of rehabilitative interventions on quality of life: A qualitative evidence synthesis of personal experiences of individuals with amyotrophic lateral sclerosis. Qual. Life Res. 2017, 27, 845–856. [Google Scholar] [CrossRef]
- Lou, J.-S.; Reeves, A.; Benice, T.; Sexton, G. Fatigue and depression are associated with poor quality of life in ALS. Neurology 2003, 60, 122–123. [Google Scholar] [CrossRef] [PubMed]
- Prell, T.; Steinbach, R.; Witte, O.W.; Grosskreutz, J. Poor emotional well-being is associated with rapid progression in amyotrophic lateral sclerosis. Eneurologicalsci 2019, 16, 100198. [Google Scholar] [CrossRef]
- Edge, R.; The TONiC Study Group; Mills, R.; Tennant, A.; Diggle, P.J.; Young, C.A. Do pain, anxiety and depression influence quality of life for people with amyotrophic lateral sclerosis/motor neuron disease? A national study reconciling previous conflicting literature. J. Neurol. 2020, 267, 607–615. [Google Scholar] [CrossRef]
- Duffy, E.I.; Garry, J.; Talbot, L.; Pasternak, D.; Flinn, A.; Minardi, C.; Dookram, M.; Grant, K.; Fitzgerald, D.; Rubano, J.; et al. A pilot study assessing the spiritual, emotional, physical/environmental, and physiological needs of mechanically ventilated surgical intensive care unit patients via eye tracking devices, head nodding, and communication boards. Trauma Surg. Acute Care Open 2018, 3, e000180. [Google Scholar] [CrossRef] [PubMed]
- Pizzimenti, A.; Aragona, M.; Onesti, E.; Inghilleri, M. Depression, pain and quality of life in patients with amyotrophic lateral sclerosis: A cross-sectional study. Funct. Neurol. 2013, 28, 115–119. [Google Scholar] [CrossRef]
- Mitsumoto, H.; Rabkin, J.G. Palliative Care for Patients With Amyotrophic Lateral Sclerosis. JAMA 2007, 298, 207–216. [Google Scholar] [CrossRef] [PubMed]
- Lillo, P.; Mioshi, E.; Zoing, M.C.; Kiernan, M.C.; Hodges, J.R. How common are behavioural changes in amyotrophic lateral sclerosis? Amyotroph. Lateral. Scler. 2016, 17, 202–207. [Google Scholar] [CrossRef]
- D’alvano, G.; Buonanno, D.; Passaniti, C.; De Stefano, M.; Lavorgna, L.; Tedeschi, G.; Siciliano, M.; Trojsi, F. Support Needs and Interventions for Family Caregivers of Patients with Amyotrophic Lateral Sclerosis (ALS): A Narrative Review with Report of Telemedicine Experiences at the Time of COVID-19 Pandemic. Brain Sci. 2021, 12, 49. [Google Scholar] [CrossRef] [PubMed]
- Tülek, Z.; Özakgül, A.; Alankaya, N.; Dik, A.; Kaya, A.; Ünalan, P.C.; Özaydin, A.N.; Idrisoğlu, H.A. Care burden and related factors among informal caregivers of patients with amyotrophic lateral sclerosis. Amyotroph. Lateral Scler. Front. Degener. 2023, 24, 125–132. [Google Scholar] [CrossRef]
- Gugliotta, C.; Gentili, D.; Marras, S.; Dettori, M.; Muglia, P.P.; Desole, M.G.; Acciaro, M.; Bellu, S.; Azara, A.; Castiglia, P. SARS-CoV-2 Epidemics in Retirement and Nursing Homes in Italy: A New Preparedness Assessment Model after the First Epidemic Wave. Int. J. Environ. Res. Public Health 2021, 18, 5712. [Google Scholar] [CrossRef]
- Pagnini, F.; Rossi, G.; Lunetta, C.; Banfi, P.; Corbo, M. Clinical psychology and amyotrophic lateral sclerosis. Front. Psychol. 2010, 1, 33. [Google Scholar] [CrossRef]
- Matuz, T.; Birbaumer, N.; Hautzinger, M.; Kübler, A. Coping with amyotrophic lateral sclerosis: An integrative view. J. Neurol. Neurosurg. Psychiatry 2010, 81, 893–898. [Google Scholar] [CrossRef]
- Tramonti, F.; Bongioanni, P.; Fanciullacci, C.; Rossi, B. Balancing between autonomy and support: Coping strategies by patients with amyotrophic lateral sclerosis. J. Neurol. Sci. 2012, 320, 106–109. [Google Scholar] [CrossRef] [PubMed]
- Pagnini, F.; Simmons, Z. Amyotrophic Lateral Sclerosis: Understanding and Optimizing Quality of Life and Psychological Well-Being; Oxford University Press: Oxford, UK, 2018; Volume 1. [Google Scholar]
- Galvin, M.; Carney, S.; Corr, B.; Mays, I.; Pender, N.; Hardiman, O. Needs of informal caregivers across the caregiving course in amyotrophic lateral sclerosis: A qualitative analysis. BMJ Open 2018, 8, e018721. [Google Scholar] [CrossRef] [PubMed]
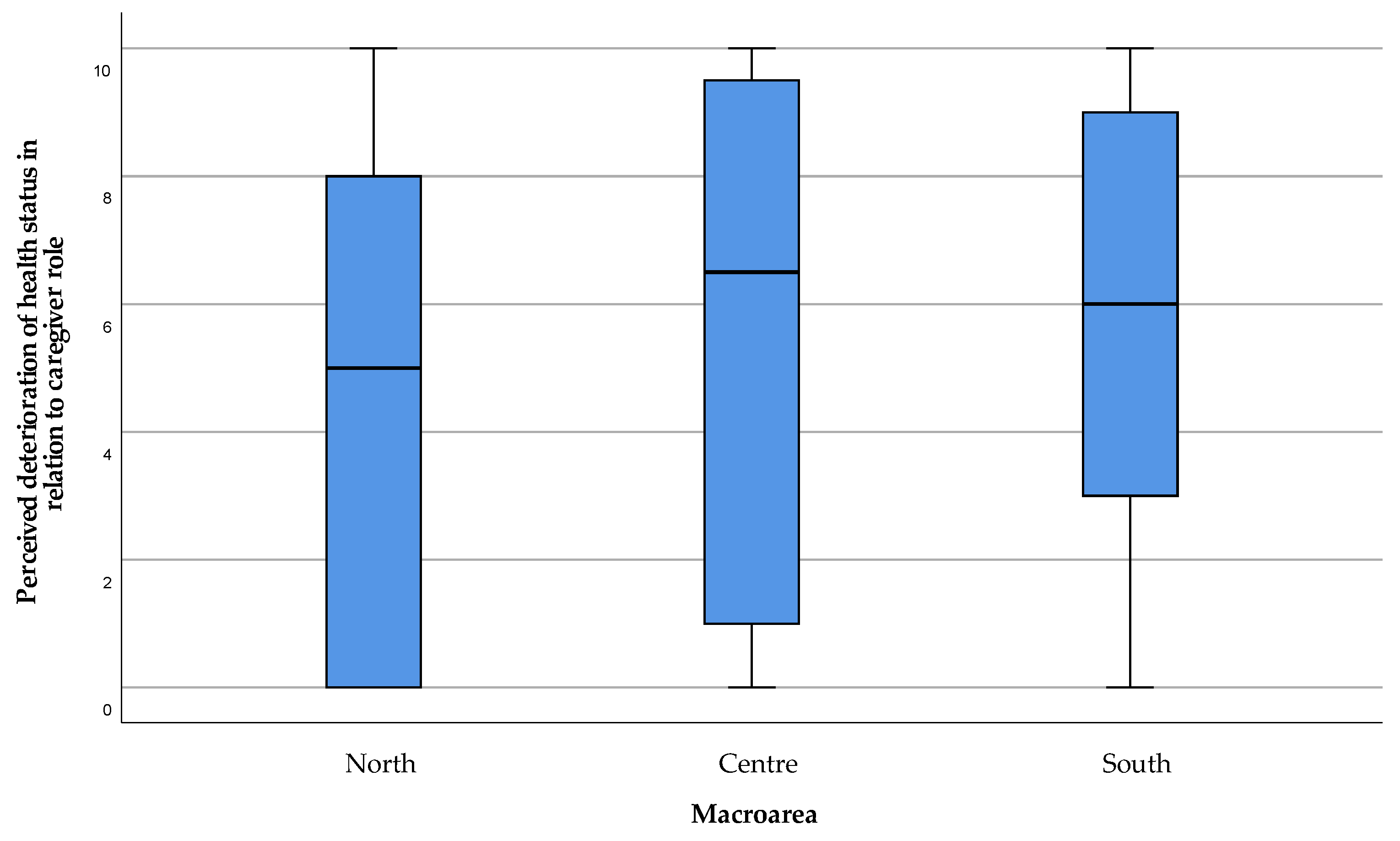

| ALS Patients | North n, % | Center n, % | South n, % | Total n, % | |
|---|---|---|---|---|---|
| Sex | F | 12 (44.4) | 2 (11.8) | 8 (36.4) | 22 (33.3) |
| M | 15 (55.6) | 15 (88.2) | 14 (63.6) | 44 (66.7) | |
| Age range (years) | <40 | 1 (3.7) | 0 (0) | 0 (0) | 1 (1.5) |
| 41–50 | 1 (3.7) | 0 (0) | 3 (13.6) | 4 (6.1) | |
| 51–60 | 7 (25.9) | 6 (35.3) | 7 (31.9) | 20 (30.3) | |
| 61–70 | 9 (33.4) | 7 (41.2) | 5 (22.7) | 21 (31.8) | |
| 71–80 | 5 (18.5) | 3 (17.6) | 5 (22.7) | 13 (19.7) | |
| >80 | 4 (14.8) | 1 (5.9) | 2 (9.1) | 7 (10.6) | |
| CLIS/FTD | No | 21 (77.8) | 12 (70.6) | 15 (68.2) | 48 (72.7) |
| Yes | 6 (22.2) | 5 (29.4) | 7 (31.8) | 18 (27.3) | |
| Tracheostomy | No | 12 (44.4) | 3 (17.6) | 8 (36.4) | 23 (34.8) |
| Yes | 15 (55.6) | 14 (82.4) | 14 (63.6) | 43 (65.2) | |
| Gastrostomy | No | 9 (33.3) | 3 (17.6) | 5 (22.7) | 17 (25.8) |
| Yes | 18 (66.7) | 14 (82.4) | 17 (77.3) | 49 (74.2) |
| Items ALSSQOL-SF 1 | Median | Percentile 25 | Percentile 75 | Mode |
|---|---|---|---|---|
| Global quality of life, 30 days before | 5 | 4 | 8 | 5 |
| 4 | 0 | 6 | 0 |
| 8 | 5 | 9 | 8 |
| 5 | 0 | 8 | 0 |
| 3 | 0 | 7 | 0 |
| 9 | 8 | 10 | 10 |
| 4 | 1 | 8 | 0 |
| 5 | 4 | 8 | 4 |
| 6 | 4 | 9 | 10 |
| 9 | 6 | 10 | 10 |
| 4 | 1 | 8 | 0 |
| 9 | 7 | 10 | 10 |
| 7 | 2 | 10 | 10 |
| 7 | 4 | 9 | 10 |
| 5 | 1 | 8 | 0 |
| 5 | 3 | 7 | 0 a |
| 9 | 7 | 10 | 10 |
| 7 | 3 | 10 | 10 |
| 5 | 3 | 8 | 3 a |
| 7 | 4 | 9 | 10 |
| 8 | 4 | 10 | 10 |
| 5 | 3 | 9 | 10 |
| 8 | 5 | 10 | 10 |
| COVID-19 emergency period | ||||
| 5 | 0 | 8 | 0 |
| 4 | 0 | 7 | 0 |
| 7 | 2 | 8 | 7 |
| 3 | 0 | 8 | 0 |
| 5 | 2 | 8 | 0 |
| 6 | 1 | 8 | 0 |
| 1 | 0 | 5 | 0 |
| 2 | 0 | 5 | 0 |
| Ordinal Regression Number of obs = 47 | |||||
|---|---|---|---|---|---|
| LR chi2(8) = 32.62 | |||||
| Prob > chi2 = 0.0001 | |||||
| Loglikelihood = −83. | Pseudo R2 = 0.1641 | ||||
| QOL GL | Odds Ratio | z | p > |z| | (95% Conf. Interval) | |
| Age | 0.9394915 | −0.23 | 0.815 | 0.5562592 | 1.58675 |
| Sex | 1.559553 | 0.73 | 0.468 | 0.4698767 | 5.176261 |
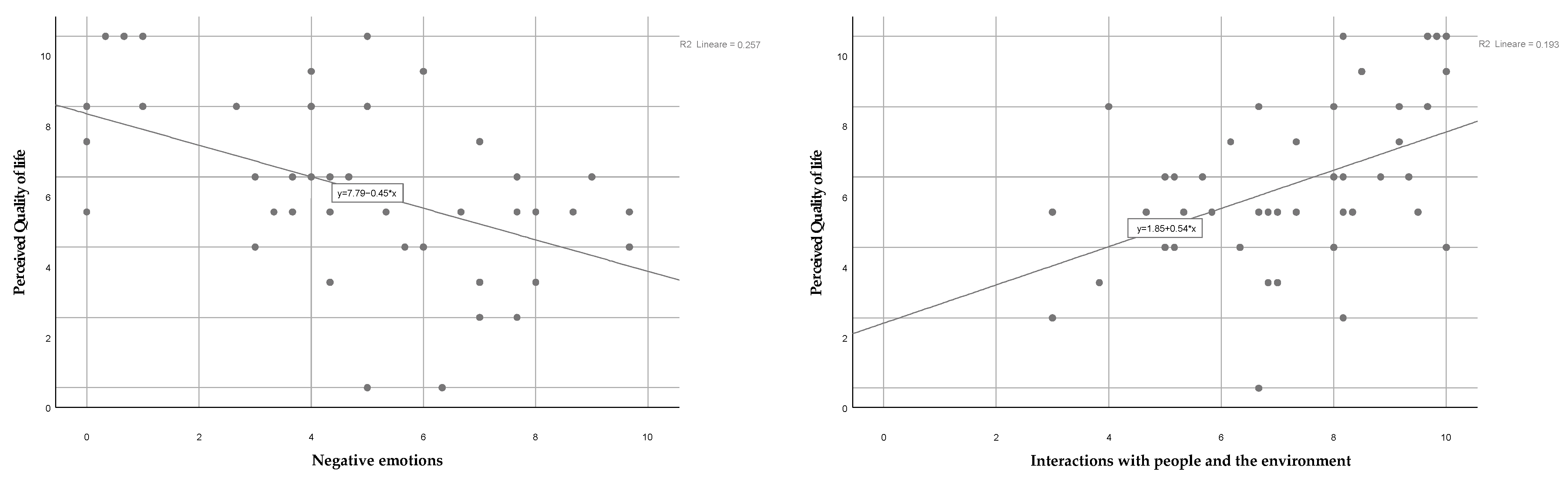
| Negative emotions | 0.7020899 | −2.77 | 0.006 | 0.5464532 | 0.9020537 |
| People/environment interactions | 1.217894 | 1.05 | 0.295 | 0.8423722 | 1.76082 |
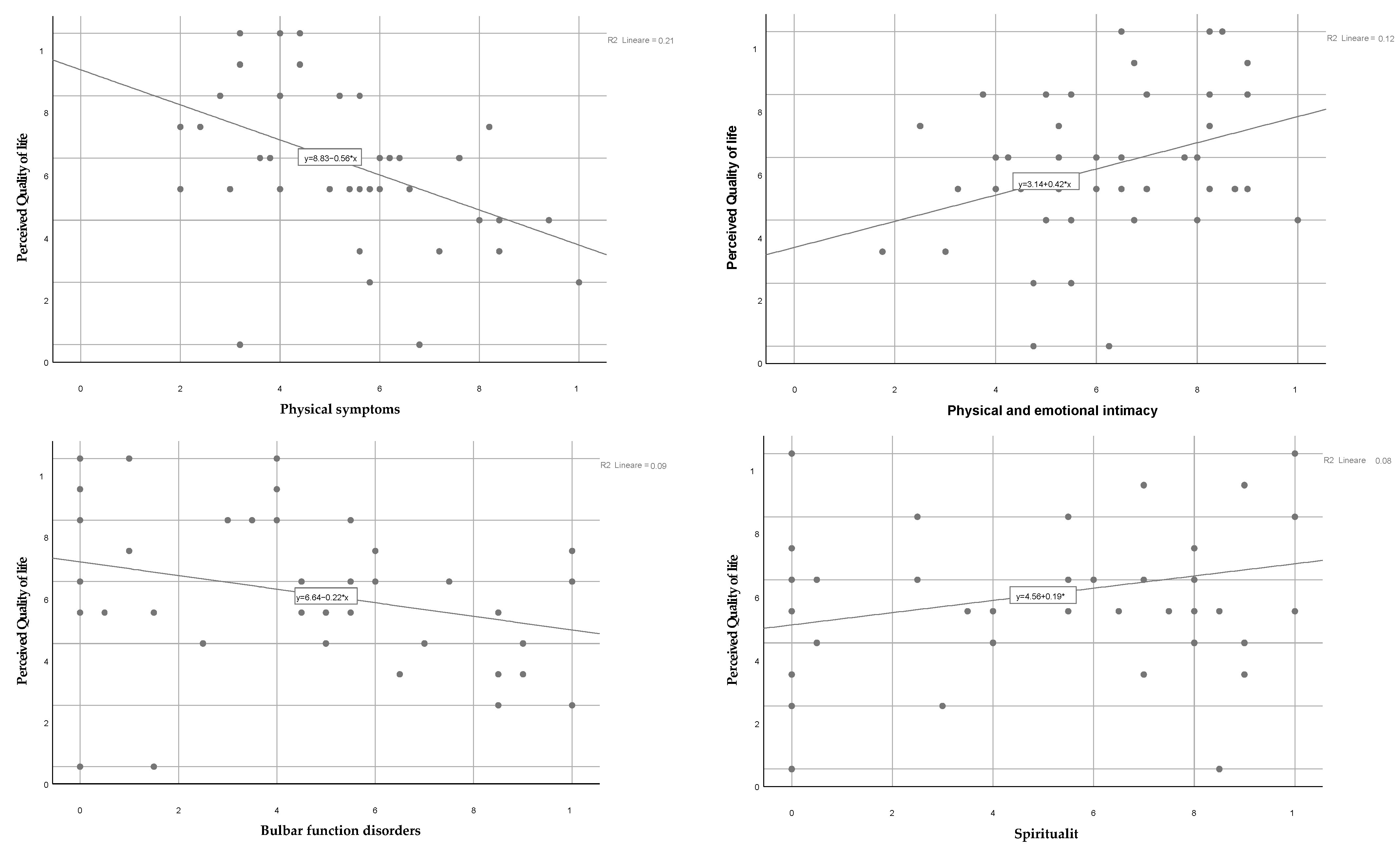
| Physical/emotional intimacy | 1.559291 | 2.56 | 0.010 | 1.110363 | 2.189726 |
| Spirituality | 0.9818377 | −0.19 | 0.846 | 0.8162948 | 1.180952 |
| Physical Symptoms | 0.705342 | −1.79 | 0.074 | 0.4811217 | 1.034057 |
| Bulbar function | 1.009111 | 0.08 | 0.934 | 0.8154303 | 1.248796 |
| Caregivers | North | Center | South | Total | |
|---|---|---|---|---|---|
| Age (mean, SD) | 56 ± 13 | 55 ± 14 | 60 ± 13 | 57 ± 13 | |
| Sex | F | 22 | 17 | 18 | 57 |
| M | 8 | 3 | 8 | 19 | |
| Time interval Starting Assistance-Diagnosis (days) | Median | −31 | 0 | 0 | 0 |
| IQR | −304–61 | 0–199 | −123–31 | −151–92 | |
| Weekly Assistance (hours) | Mode | >50 | >50 | >50 | >50 |
| Items Zarit Burden Interview (ZBI) 1 | Median | Percentile 25 | Percentile 75 | Mode |
|---|---|---|---|---|
| 1 | 0 | 5 | 0 |
| 8 | 4 | 10 | 10 |
| 8 | 3 | 10 | 10 |
| 0 | 0 | 0 | 0 |
| 0 | 0 | 3 | 0 |
| 0 | 0 | 2 | 0 |
| 10 | 7 | 10 | 10 |
| 10 | 8 | 10 | 10 |
| 0 | 0 | 4 | 0 |
| 6 | 1 | 9 | 0 a |
| 5 | 1 | 9 | 0 |
| 7 | 2 | 10 | 10 |
| 0 | 0 | 0 | 0 |
| 8 | 2 | 10 | 10 |
| 6 | 2 | 10 | 10 |
| 2 | 0 | 8 | 0 |
| 5 | 0 | 9 | 0 |
| 0 | 0 | 1 | 0 |
| 2 | 0 | 7 | 0 |
| 4 | 0 | 7 | 0 |
| 3 | 0 | 6 | 0 |
| 5 | 1 | 9 | 0 a |
| COVID-19 emergency period | ||||
| 5 | 0 | 10 | 0 |
| 3 | 0 | 9 | 0 |
| 6 | 2 | 9 | 10 |
| 0 | 0 | 5 | 0 |
| 6 | 1 | 9 | 0 a |
| 0 | 0 | 6 | 0 |
| 4 | 0 | 8 | 0 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gentili, D.; Deiana, G.; Chessa, V.; Calabretta, A.; Marras, E.; Solinas, C.; Gugliotta, C.; Azara, A. Quality of Life in Amyotrophic Lateral Sclerosis Patients and Care Burden of Caregivers in Sardinia during COVID-19 Pandemic. Healthcare 2023, 11, 1641. https://doi.org/10.3390/healthcare11111641
Gentili D, Deiana G, Chessa V, Calabretta A, Marras E, Solinas C, Gugliotta C, Azara A. Quality of Life in Amyotrophic Lateral Sclerosis Patients and Care Burden of Caregivers in Sardinia during COVID-19 Pandemic. Healthcare. 2023; 11(11):1641. https://doi.org/10.3390/healthcare11111641
Chicago/Turabian StyleGentili, Davide, Giovanna Deiana, Vanna Chessa, Annalisa Calabretta, Elisabetta Marras, Costanzo Solinas, Carmelo Gugliotta, and Antonio Azara. 2023. "Quality of Life in Amyotrophic Lateral Sclerosis Patients and Care Burden of Caregivers in Sardinia during COVID-19 Pandemic" Healthcare 11, no. 11: 1641. https://doi.org/10.3390/healthcare11111641
APA StyleGentili, D., Deiana, G., Chessa, V., Calabretta, A., Marras, E., Solinas, C., Gugliotta, C., & Azara, A. (2023). Quality of Life in Amyotrophic Lateral Sclerosis Patients and Care Burden of Caregivers in Sardinia during COVID-19 Pandemic. Healthcare, 11(11), 1641. https://doi.org/10.3390/healthcare11111641







