Virtual Leadership and Nurses’ Psychological Stress during COVID-19 in the Tertiary Hospitals of Pakistan: The Role of Emotional Intelligence
Abstract
:1. Introduction
2. Literature Review
2.1. Virtual Leadership
2.2. Emotional Intelligence
2.3. Work Stress
2.4. Burnout
2.5. Job Performance
2.6. Theory of Emotional Intelligence (EI)
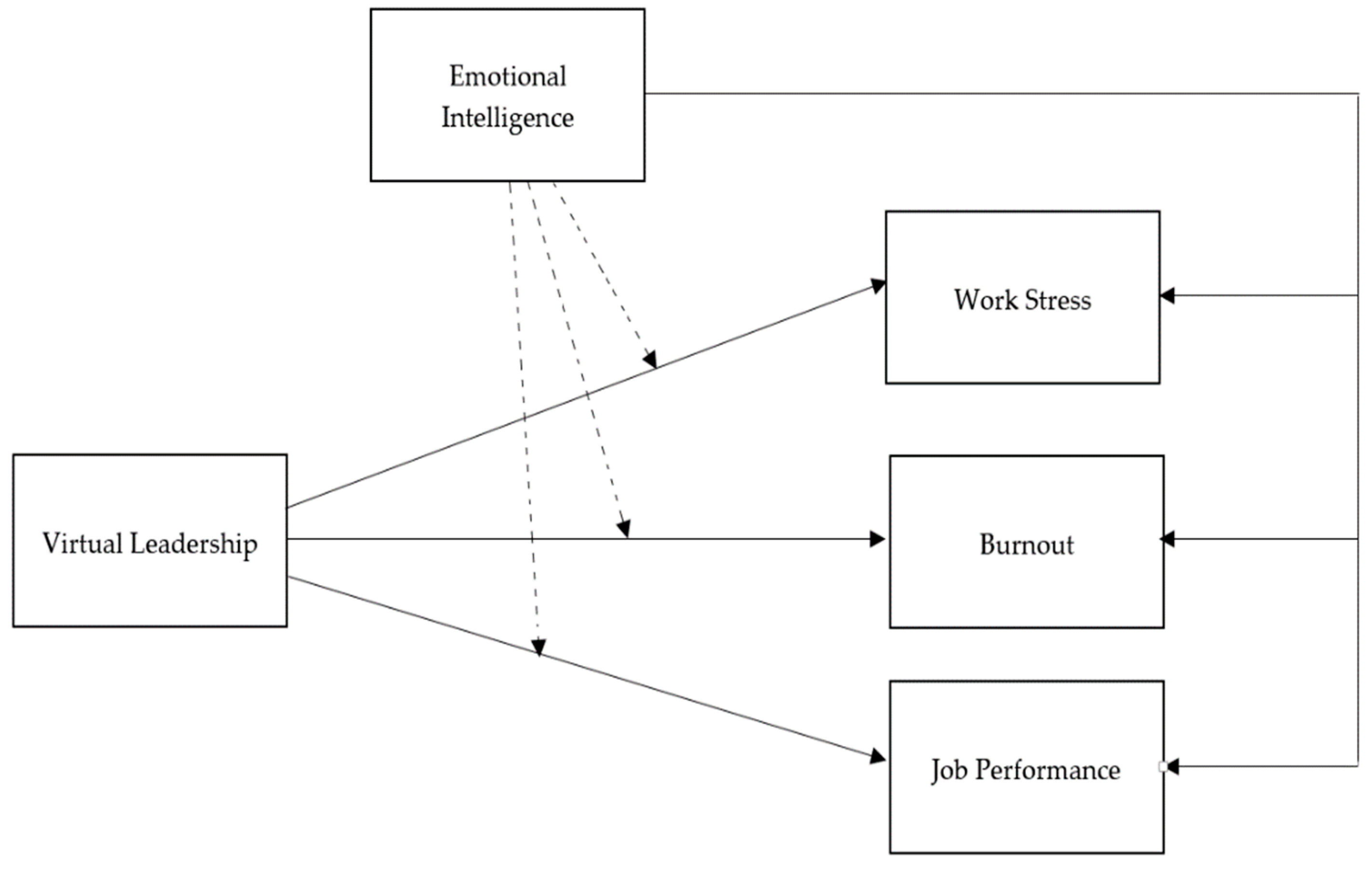
3. Hypothesis Development
3.1. Virtual Leadership, Work Stress, Burnout, and Job Performance
3.2. EI, Work Stress, Work Burnout, and Job Performance
3.3. Moderating Role of Emotional Intelligence
4. Research Methodology
4.1. Research Approach
4.2. Questionnaire Development
4.3. Respondent Summary
4.4. Demographics
4.5. Measurements
4.5.1. Emotional Intelligence
4.5.2. Virtual Leadership
4.5.3. Work Stress
4.5.4. Burnout
4.5.5. Job Performance
5. Results
5.1. Testing Measurement Model
5.2. Assessing Overall Model Fit
6. Discussion
6.1. Conclusions
6.2. Contributions, Limitations, and Future Research
6.2.1. Theoretical Contribution
6.2.2. Practical Implications
6.2.3. Limitations and Future Research
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- World Health Organization. State of the World’s Nursing 2020: Investing in Education, Jobs and Leadership. Licence: CC BY-NC-SA 3.0 IG. 2020. Available online: https://www.google.com/url?sa=t&rct=j&q=&esrc=s&source=web&cd=&ved=2ahUKEwj5-dTn_uvrAhWKHhQKHYqADqQQFjAAegQIBRAB&url=https%3A%2F%2Fapps.who.int%2Firis%2Frest%2Fbitstreams%2F1274201%2Fretrieve&usg=AOvVaw2-6lnNgyzI3LAiwo2glzb5 (accessed on 31 March 2020).
- Laeeque, S.H.; Bilal, A.; Babar, S.; Khan, Z.; Ul Rahman, S. How patient-perpetrated workplace violence leads to turnover intention among nurses: The mediating mechanism of occupational stress and burnout. J. Aggress. Maltreat. Trauma 2018, 27, 96–118. [Google Scholar] [CrossRef]
- Gonçalves, J.V.; Castro, L.; Rêgo, G.; Nunes, R. Burnout determinants among nurses working in palliative care during the coronavirus disease 2019 pandemic. Int. J. Environ. Res. Public Health 2021, 18, 3358. [Google Scholar] [CrossRef]
- Deng, J.; Guo, Y.; Ma, T.; Yang, T.; Tian, X. How job stress influences job performance among Chinese healthcare workers: A cross-sectional study. Environ. Health Prev. Med. 2019, 24, 2. [Google Scholar] [CrossRef] [PubMed]
- Khattak, S.R.; Saeed, I.; Rehman, S.U.; Fayaz, M. Impact of fear of COVID-19 pandemic on the mental health of nurses in Pakistan. J. Loss Trauma 2021, 26, 421–435. [Google Scholar] [CrossRef]
- Parr, J. Pneumonia in China: Lack of information raises concerns among Hong Kong health workers. BMJ 2020, 368, m56. [Google Scholar] [CrossRef]
- Lee, E.; Jang, I. Nurses’ fatigue, job stress, organizational culture, and turnover intention: A culture–work–health model. West. J. Nurs. Res. 2020, 42, 108–116. [Google Scholar] [CrossRef]
- Wang, Z.; Zaman, S.; Rasool, S.F.; uz Zaman, Q.; Amin, A. Exploring the relationships between a toxic workplace environment, workplace stress, and project success with the moderating effect of organizational support: Empirical evidence from Pakistan. Risk Manag. Healthc. Policy 2020, 13, 1055. [Google Scholar] [CrossRef]
- Barello, S.; Palamenghi, L.; Graffigna, G. Burnout and somatic symptoms among frontline healthcare professionals at the peak of the Italian COVID-19 pandemic. Psychiatry Res. 2020, 290, 113129. [Google Scholar] [CrossRef]
- Falatah, R. The impact of the coronavirus disease (COVID-19) pandemic on nurses’ turnover intention: An integrative review. Nurs. Rep. 2021, 11, 787–810. [Google Scholar] [CrossRef] [PubMed]
- Chow, S.K.; Francis, B.; Ng, Y.H.; Naim, N.; Beh, H.C.; Ariffin, M.A.A.; Yusuf, M.H.M.; Lee, J.W.; Sulaiman, A.H. Religious Coping, Depression and Anxiety among Healthcare Workers during the COVID-19 Pandemic: A Malaysian Perspective. Healthcare 2021, 9, 79. [Google Scholar] [CrossRef]
- Saltman, D.C. Is COVID-19 an Opportunity to Improve Virtual Leadership? Aust. J. Gen. Pract. 2020, 49 (Suppl. S12). [Google Scholar] [CrossRef]
- Fernandez, C.S.; Green, M.A.; Noble, C.C.; Brandert, K.; Donnald, K.; Walker, M.R.; Henry, E.; Rosenberg, A.; Dave, G.; Corbie-Smith, G. Training “pivots” from the pandemic: Lessons learned transitioning from in-person to virtual synchronous training in the clinical scholars leadership program. J. Healthc. Leadersh. 2021, 13, 63–75. [Google Scholar] [CrossRef]
- Laukka, E.; Hammarén, M.; Pölkki, T.; Kanste, O. Hospital nurse leaders’ experiences with digital technologies: A qualitative descriptive study. J. Adv. Nurs. 2023, 79, 297–308. [Google Scholar] [CrossRef] [PubMed]
- Sandberg, D.S.; Pennington, C.M.; Lindquist, M.A. Virtual Leadership: CEOs and C-Level Executives of Healthcare Organizations in the United States Reimagined New Roles as Virtual Leaders. J. Leadersh. Stud. 2022, 16, 61–69. [Google Scholar] [CrossRef]
- Blake, N.; Leach, L.S.; Robbins, W.; Pike, N.; Needleman, J. Healthy work environments and staff nurse retention: The relationship between communication, collaboration, and leadership in the pediatric intensive care unit. Nurs. Adm. Q. 2013, 37, 356–370. [Google Scholar] [CrossRef]
- Grunes, P.; Gudmundsson, A.; Irmer, B. To what extent is the Mayer and Salovey (1997) model of emotional intelligence a useful predictor of leadership style and perceived leadership outcomes in Australian educational institutions? Educ. Manag. Adm. Leadersh. 2014, 42, 112–135. [Google Scholar] [CrossRef]
- Mayer, J.D.; Salovey, P. What is emotional intelligence. Emot. Dev. Emot. Intell. Educ. Implic. 1997, 3, 31. [Google Scholar]
- Hurley, J.; Hutchinson, M.; Kozlowski, D.; Gadd, M.; van Vorst, S. Emotional intelligence as a mechanism to build resilience and non-technical skills in undergraduate nurses undertaking clinical placement. Int. J. Ment. Health Nurs. 2020, 29, 47–55. [Google Scholar] [CrossRef] [PubMed]
- Dugué, M.; Sirost, O.; Dosseville, F. A literature review of emotional intelligence and nursing education. Nurse Educ. Pract. 2021, 54, 103124. [Google Scholar] [CrossRef]
- Sharma, J.; Dhar, R.L.; Tyagi, A. Stress as a mediator between work–family conflict and psychological health among the nursing staff: Moderating role of emotional intelligence. Appl. Nurs. Res. 2016, 30, 268–275. [Google Scholar] [CrossRef]
- Forrest, C.B.; Xu, H.; Thomas, L.E.; Webb, L.E.; Cohen, L.W.; Carey, T.S.; Chuang, C.H.; Daraiseh, N.M.; Kaushal, R.; McClay, J.C.; et al. Impact of the early phase of the COVID-19 pandemic on US healthcare workers: Results from the HERO Registry. J. Gen. Intern. Med. 2021, 36, 1319–1326. [Google Scholar] [CrossRef] [PubMed]
- Zaman, S.; Wang, Z.; Rasool, S.F.; uz Zaman, Q.; Raza, H. Impact of critical success factors and supportive leadership on sustainable success of renewable energy projects: Empirical evidence from Pakistan. Energy Policy 2022, 162, 112793. [Google Scholar] [CrossRef]
- Putriastuti, B.C.K.; Stasi, A. How to lead the millennials: A review of 5 major leadership theory groups. J. Leadersh. Organ. 2019, 1, 96–111. [Google Scholar] [CrossRef]
- Kandil, M.A.; Moustafa, M.A.E. The Effect of Virtual Leadership Practices on Work Engagement during COVID-19. Delta Univ. Sci. J. 2021, 4, 44–53. [Google Scholar] [CrossRef]
- Kiljunen, M.; Laukka, E.; Koskela, T.K.; Kanste, O.I. Remote leadership in health care: A scoping review. Leadersh. Health Serv. 2022, 35, 98–115. [Google Scholar] [CrossRef]
- Gemeda, H.K.; Lee, J. Leadership styles, work engagement and outcomes among information and communications technology professionals: A cross-national study. Heliyon 2020, 6, e03699. [Google Scholar] [CrossRef]
- Pourbarkhordari, A.; Zhou, E.H.I.; Pourkarimi, J. How individual-focused transformational leadership enhances its influence on job performance through employee work engagement. Int. J. Bus. Manag. 2016, 11, 249. [Google Scholar] [CrossRef]
- Cowan, L.D. E-Leadership: Leading in a virtual environment-Guiding principles for nurse leaders. Nurs. Econ. 2014, 32, 312. [Google Scholar] [PubMed]
- Salovey, P.; Mayer, J.D. Emotional intelligence. Imagin. Cogn. Personal. 1990, 9, 185–211. [Google Scholar] [CrossRef]
- Goleman, D. Working with Emotional Intelligence; Bantam Books: New York, NY, USA, 1998; p. 103. [Google Scholar]
- Talman, K.; Hupli, M.; Rankin, R.; Engblom, J.; Haavisto, E. Emotional intelligence of nursing applicants and factors related to it: A cross-sectional study. Nurse Educ. Today 2020, 85, 104271. [Google Scholar] [CrossRef]
- Codier, E.; Muneno, L.; Franey, K.; Matsuura, F. Is emotional intelligence an important concept for nursing practice? J. Psychiatr. Ment. Health Nurs. 2010, 17, 940–948. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Aungsuroch, Y.; Gunawan, J.; Zeng, D. Job stress, psychological capital, perceived social support, and occupational burnout among hospital nurses. J. Nurs. Scholarsh. 2021, 53, 511–518. [Google Scholar] [CrossRef]
- Labrague, L.J.; McEnroe-Petitte, D.M.; Gloe, D.; Thomas, L.; Papathanasiou, I.V.; Tsaras, K. A literature review on stress and coping strategies in nursing students. J. Ment. Health 2017, 26, 471–480. [Google Scholar] [CrossRef] [PubMed]
- Chang, E.M.; Bidewell, J.W.; Huntington, A.D.; Daly, J.; Johnson, A.; Wilson, H.; Lambert, V.A.; Lambert, C.E. A survey of role stress, coping and health in Australian and New Zealand hospital nurses. Int. J. Nurs. Stud. 2007, 44, 1354–1362. [Google Scholar] [CrossRef] [PubMed]
- Alexandrova-Karamanova, A.; Todorova, I.; Montgomery, A.; Panagopoulou, E.; Costa, P.; Baban, A.; Davas, A.; Milosevic, M.; Mijakoski, D. Burnout and health behaviours in health professionals from seven European countries. Int. Arch. Occup. Environ. Health 2016, 89, 1059–1075. [Google Scholar] [CrossRef]
- Samma, M.; Zhao, Y.; Rasool, S.F.; Han, X.; Ali, S. Exploring the Relationship between Innovative Work Behavior, Job Anxiety, Workplace Ostracism, and Workplace Incivility: Empirical Evidence from Small and Medium Sized Enterprises (SMEs). Healthcare 2020, 8, 508. [Google Scholar] [CrossRef]
- Alam, F.; Yang, Q.; Bhutto, M.Y.; Akhtar, N. The Influence of E-Learning and Emotional Intelligence on Psychological Intentions: Study of Stranded Pakistani Students. Front. Psychol. 2021, 12, 715700. [Google Scholar] [CrossRef]
- Li, X.; Fang, X.; Wang, L.; Geng, X.; Chang, H. Relationship between emotional intelligence and job well-being in Chinese Registered Nurses: Mediating effect of communication satisfaction. Nurs. Open 2021, 8, 1778–1787. [Google Scholar] [CrossRef]
- Mansel, B.; Einion, A. ‘It’s the relationship you develop with ‘them’: Emotional intelligence in nurse leadership. A qualitative study. Br. J. Nurs. 2019, 28, 1400–1408. [Google Scholar] [CrossRef]
- Chen, S.C.; Chen, C.F. Antecedents and consequences of nurses’ burnout. Manag. Decis. 2018, 56, 777–792. [Google Scholar] [CrossRef]
- Ayalew, M.; Ayenew, Z. Do Paradoxical Virtual Leadership and Emotional Intelligence have Relationships? In Particular from Technology Dependence, Geographical Dispersion, and Human Capital Tensions. Int. J. Organ. Leadersh. 2022, 11, 1–25. [Google Scholar] [CrossRef]
- Foster, K.; Fethney, J.; Kozlowski, D.; Fois, R.; Reza, F.; McCloughen, A. Emotional intelligence and perceived stress of Australian pre-registration healthcare students: A multi-disciplinary cross-sectional study. Nurse Educ. Today 2018, 66, 51–56. [Google Scholar] [CrossRef]
- Bermejo-Martins, E.; Luis, E.O.; Fernández-Berrocal, P.; Martínez, M.; Sarrionandia, A. The role of emotional intelligence and self-care in the stress perception during COVID-19 outbreak: An intercultural moderated mediation analysis. Pers. Individ. Differ. 2021, 177, 110679. [Google Scholar] [CrossRef]
- Zhou, X.; Rasool, S.F.; Yang, J.; Asghar, M.Z. Exploring the relationship between despotic leadership and job satisfaction: The role of self efficacy and leader–member exchange. Int. J. Environ. Res. Public Health 2021, 18, 5307. [Google Scholar] [CrossRef]
- Mysirlaki, S.; Paraskeva, F. Emotional intelligence and transformational leadership in virtual teams: Lessons from MMOGs. Leadersh. Organ. Dev. J. 2020, 41, 551–566. [Google Scholar] [CrossRef]
- Cortellazzo, L.; Bruni, E.; Zampieri, R. The role of leadership in a digitalized world: A review. Front. Psychol. 2019, 10, 1938. [Google Scholar] [CrossRef] [PubMed]
- Van Wart, M.; Roman, A.; Wang, X.; Liu, C. Operationalizing the definition of e-leadership: Identifying the elements of e-leadership. Int. Rev. Adm. Sci. 2019, 85, 80–97. [Google Scholar] [CrossRef]
- Khan, R.; Bukhari, A.; Channar, Z.A. Effects of leadership style on health care organizational performance: A survey of selected tertiary care hospital in Karachi, Pakistan. Int. J. Econ. Manag. Sci. 2016, 5, 2. [Google Scholar] [CrossRef]
- Elyousfi, F.; Anand, A.; Dalmasso, A. Impact of e-leadership and team dynamics on virtual team performance in a public organization. Int. J. Public Sect. Manag. 2021, 34, 508–528. [Google Scholar] [CrossRef]
- Sharpp, T.J.; Lovelace, K.; Cowan, L.D.; Baker, D. Perspectives of nurse managers on information communication technology and e-Leadership. J. Nurs. Manag. 2019, 27, 1554–1562. [Google Scholar] [CrossRef]
- Ingram, A.; Peake, W.O.; Stewart, W.; Watson, W. Emotional intelligence and venture performance. J. Small Bus. Manag. 2019, 57, 780–800. [Google Scholar] [CrossRef]
- Chong, S.C.; Falahat, M.; Lee, Y.S. Emotional Intelligence and Job Performance of Academicians in Malaysia. Int. J. High. Educ. 2020, 9, 69–80. [Google Scholar] [CrossRef]
- Dewaele, J.M.; Lorette, P.; Petrides, K.V. The Effects of Linguistic Proficiency, Trait Emotional Intelligence and Cultural Background on Emotion Recognition by English L1 users. In Emotion in Discourse; Alba Juez, L., Mackenzie, L., Eds.; Benjamins: Amsterdam, The Netherland, 2019; pp. 285–305. [Google Scholar]
- Nespereira-Campuzano, T.; Vázquez-Campo, M. Emotional intelligence and stress management in Nursing professionals in a hospital emergency department. Enferm. Clín. 2017, 27, 172–178. [Google Scholar] [CrossRef]
- Bar-On, R. The impact of emotional intelligence on subjective well-being: Research article: General. Perspect. Educ. 2005, 23, 41–62. Available online: https://hdl.handle.net/10520/EJC87316 (accessed on 10 May 2023).
- Rasool, S.F.; Maqbool, R.; Samma, M.; Zhao, Y.; Anjum, A. Positioning depression as a critical factor in creating a toxic workplace environment for diminishing worker productivity. Sustainability 2019, 11, 2589. [Google Scholar] [CrossRef]
- Sadovyy, M.; Sánchez-Gómez, M.; Bresó, E. COVID-19: How the stress generated by the pandemic may affect work performance through the moderating role of emotional intelligence. Personal. Individ. Differ. 2021, 180, 110986. [Google Scholar] [CrossRef]
- Bar-On, R.; Handley, R.; Fund, S. The impact of emotional intelligence on performance. In Linking Emotional Intelligence and Performance at Work: Current Research Evidence with Individuals and Group; Druskat, V.U., Sala, F., Mount, G., Eds.; Lawrence Erlbaum Associates, Inc.: Mahwah, NJ, USA, 2006; pp. 3–19. [Google Scholar]
- Wang, L.; Tao, H.; Bowers, B.J.; Brown, R.; Zhang, Y. When nurse emotional intelligence matters: How transformational leadership influences intent to stay. J. Nurs. Manag. 2018, 26, 358–365. [Google Scholar] [CrossRef]
- Osborne, S.; Hammoud, M.S. Effective employee engagement in the workplace. Int. J. Appl. Manag. Technol. 2017, 16, 4. [Google Scholar] [CrossRef]
- Chung, E.; Noor, N.M.; Mathew, V.N. Are you ready? An assessment of online learning readiness among university students. Int. J. Acad. Res. Progress. Educ. Dev. 2020, 9, 301–317. [Google Scholar]
- Shahzad, A.; Hassan, R.; Aremu, A.Y.; Hussain, A.; Lodhi, R.N. Effects of COVID-19 in E-learning on higher education institution students: The group comparison between male and female. Qual. Quant. 2021, 55, 805–826. [Google Scholar] [CrossRef]
- University of Toledo. Emotional Intelligence Proves Significant to Remote Leadership in a Crisis. 2021. Available online: https://www.labmanager.com/news/emotional-intelligence-proves-significant-to-remote-leadership-in-a-crisis-27105 (accessed on 23 November 2021).
- Nie, A.; Su, X.; Zhang, S.; Guan, W.; Li, J. Psychological impact of COVID-19 outbreak on frontline nurses: A cross-sectional survey study. J. Clin. Nurs. 2020, 29, 4217–4226. [Google Scholar] [CrossRef]
- Westland, J.C. Lower bounds on sample size in structural equation modeling. Electron. Commer. Res. Appl. 2010, 9, 476–487. [Google Scholar] [CrossRef]
- Schutte, N.S.; Malouff, J.M.; Thorsteinsson, E.B.; Bhullar, N.; Rooke, S.E. A meta-analytic investigation of the relationship between emotional intelligence and health. Pers. Individ. Differ. 2007, 42, 921–933. [Google Scholar] [CrossRef]
- Lovelace, K. A Case Study of E-Leadership Constructs: An Assessment of Leadership in a Healthcare Organization; University of San Francisco: San Francisco, CA, USA, 2015. [Google Scholar]
- He, R. E-Leadership Strategy in Virtual Organizations and Virtual Teams. Master’s Thesis, Helsinki University of Technology, Espoo, Finland, 2008. [Google Scholar]
- Lazarus, R.S.; Folkman, S. Stress, Appraisal, and Coping; Springer Publishing Company: New York, NY, USA, 1984. [Google Scholar]
- Schaufeli, W.B.; Salanova, M.; González-Romá, V.; Bakker, A.B. The measurement of engagement and burnout: A two sample confirmatory factor analytic approach. J. Happiness Stud. 2002, 3, 71–92. [Google Scholar] [CrossRef]
- Singh, J.; Verbeke, W.; Rhoads, G.K. Do organizational practices matter in role stress processes? A study of direct and moderating effects for marketing-oriented boundary spanners. J. Mark. 1996, 60, 69–86. [Google Scholar] [CrossRef]
- Lowry, P.B.; Gaskin, J. Partial least squares (PLS) structural equation modeling (SEM) for building and testing behavioural causal theory: When to choose it and how to use it. IEEE Trans. Prof. Commun. 2014, 57, 123–146. [Google Scholar] [CrossRef]
- Chin, W.W.; Peterson, R.A.; Brown, S.P. Structural equation modeling in marketing: Some practical reminders. J. Mark. Theory Pract. 2008, 16, 287–298. [Google Scholar] [CrossRef]
- Hair, J.F.; Ringle, C.M.; Sarstedt, M. Partial least squares structural equation modeling: Rigorous applications, better results and higher acceptance. Long Range Plan. 2013, 46, 1–12. [Google Scholar] [CrossRef]
- Chin, W.W.; Thatcher, J.B.; Wright, R.T. Assessing common method bias: Problems with the ULMC technique. MIS Q. 2012, 36, 1003–1019. [Google Scholar] [CrossRef]
- Hu, L.-t.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct. Equ. Model. 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Fornell, C.; Larcker, D.F. Structural equation models with unobservable variables and measurement error: Algebra and statistics. J. Mark. Res. 1981, 18, 382–388. [Google Scholar] [CrossRef]
- Henseler, J.; Ringle, C.M.; Sarstedt, M. A new criterion for assessing discriminant validity in variance-based structural equation modeling. J. Acad. Mark. Sci. 2015, 43, 115–135. [Google Scholar] [CrossRef]
- Kline, R.B. Principles and Practice of Structural Equation Modeling; Guilford Publications: New York, NY, USA, 2015. [Google Scholar]
- Hair, J.F.; Anderson, R.E.; Tatham, R.L.; William, C. Black. In Multivariate Data Analysis; Prentice Hall: Hoboken, NJ, USA, 1998. [Google Scholar]
- Cohen, J. Statistical Power Analysis for the Behavioural Sciences; Academic Press: Cambridge, MA, USA, 2013. [Google Scholar]
- Chin, W.W.; Marcolin, B.L.; Newsted, P.R. A partial least squares latent variable modeling approach for measuring interaction effects: Results from a Monte Carlo simulation study and an electronic-mail emotion/adoption study. Inf. Syst. Res. 2003, 14, 189–217. [Google Scholar] [CrossRef]
- Rad, A.M.M.; Yarmohammadian, M.H. A study of relationship between managers’ leadership style and employees’ job satisfaction. Leadersh. Health Serv. 2006, 19, 11–28. [Google Scholar] [CrossRef]
- Iqbal, J.; Qureshi, N.; Ashraf, M.A.; Rasool, S.F.; Asghar, M.Z. The effect of emotional intelligence and academic social networking sites on academic performance during the COVID-19 pandemic. Psychol. Res. Behav. Manag. 2021, 14, 905. [Google Scholar] [CrossRef] [PubMed]
- Ahuja, J.; Puppala, H.; Sergio, R.P.; Hoffman, E.P. E-Leadership Is Un (usual): Multi-Criteria Analysis of Critical Success Factors for the Transition from Leadership to E-Leadership. Sustainability 2023, 15, 6506. [Google Scholar] [CrossRef]
- Soto-Rubio, A.; Giménez-Espert, M.D.C.; Prado-Gascó, V. Effect of emotional intelligence and psychosocial risks on burnout, job satisfaction, and ‘nurses’ health during the COVID-19 pandemic. Int. J. Environ. Res. Public Health 2020, 17, 7998. [Google Scholar] [CrossRef]
- Sun, H.; Wang, S.; Wang, W.; Han, G.; Liu, Z.; Wu, Q.; Pang, X. Correlation between emotional intelligence and negative emotions of front-line nurses during the COVID-19 epidemic: A cross-sectional study. J. Clin. Nurs. 2021, 30, 385–396. [Google Scholar] [CrossRef]
- Kumar, N.; Jin, Y. Impact of nurses’ emotional labour on job stress and emotional exhaustion amid COVID-19: The role of instrumental support and coaching leadership as moderators. J. Nurs. Manag. 2022, 30, 2620–2632. [Google Scholar] [CrossRef]

| Characteristics | Categories | n = 274 | Percentage (%) |
|---|---|---|---|
| Gender | Male | 35 | 13 |
| Female | 239 | 87 | |
| Academic Qualification | College-level | 91 | 33.2 |
| Undergraduate | 126 | 46 | |
| Graduate | 57 | 20.8 | |
| Organizational Position | Supervisor/Senior Nurse | 46 | 16.8 |
| Clinical Nurse | 228 | 83.2 | |
| Job Experience | Less than 3 years | 79 | 28.8 |
| 4–6 years | 97 | 35.4 | |
| 7–9 years | 66 | 24.1 | |
| Above 10 years | 32 | 11.7 |
| Constructs | Items | Loading | Alpha | AVE | CR |
|---|---|---|---|---|---|
| Emotional intelligence | EI1 | 0.741 | 0.758 | 0.576 | 0.831 |
| EI2 | 0.752 | ||||
| EI3 | 0.749 | ||||
| EI4 | 0.763 | ||||
| EI5 | 0.795 | ||||
| EI6 | 0.771 | ||||
| EI7 | 0.739 | ||||
| EI8 | 0.761 | ||||
| Virtual leadership | VL1 | 0.757 | 0.752 | 0.609 | 0.827 |
| VL2 | 0.804 | ||||
| VL3 | 0.826 | ||||
| VL4 | 0.813 | ||||
| VL5 | 0.796 | ||||
| VL6 | 0.733 | ||||
| VL7 | 0.729 | ||||
| Work stress | WS1 | 0.791 | 0.793 | 0.653 | 0.892 |
| WS2 | 0.853 | ||||
| WS3 | 0.855 | ||||
| WS4 | 0.842 | ||||
| WS5 | 0.698 | ||||
| Burnout | BO1 | 0.829 | 0.791 | 0.654 | 0.873 |
| BO2 | 0.830 | ||||
| BO3 | 0.816 | ||||
| BO4 | 0.754 | ||||
| BO5 | 0.813 | ||||
| Job performance | JP1 | 0.681 | 0.749 | 0.600 | 0.839 |
| JP2 | 0.824 | ||||
| JP3 | 0.816 | ||||
| JP4 | 0.831 | ||||
| JP5 | 0.736 | ||||
| JP6 | 0.751 |
| Variables | Mean | SD | 1 | 2 | 3 | 4 | 5 | |
|---|---|---|---|---|---|---|---|---|
| 1 | Job Performance | 3.47 | 0.43 | 1 | ||||
| 2 | Burnout | 3.01 | 0.49 | −0.23 | 1 | |||
| 3 | Work Stress | 3.16 | 0.37 | −0.21 | 0.28 | 1 | ||
| 4 | EI | 4.22 | 0.31 | 0.36 | −0.43 | −0.38 | 1 | |
| 5 | VL | 4.17 | 0.79 | −0.39 | 0.38 ** | 0.29 | −0.23 * | 1 |
| Hypothesis | Beta | T-Value | p-Value | F Square | Decision |
|---|---|---|---|---|---|
| VL -> Work stress | 0.36 | 2.513 ** | 0.00 | 0.071 | Approved |
| VL -> Burnout | 0.31 | 3.151 ** | 0.01 | 0.131 | Approved |
| VL -> Job performance | −0.29 | 2.895 ** | 0.01 | 0.114 | Approved |
| EI -> Work stress | −0.33 | 4.293 ** | 0.01 | 0.174 | Approved |
| EI -> Burn out | −0.38 | 3.125 ** | 0.01 | 0.125 | Approved |
| EI -> Job performance | 0.41 | 4.591 ** | 0.05 | 0.197 | Approved |
| VL * EI -> Work stress | −0.21 | 2.324 ** | 0.01 | 0.052 | Approved |
| VL * EI -> Burn out | −0.23 | 2.697 ** | 0.05 | 0.089 | Approved |
| VL * EI -> Job performance | 0.26 | 3.926 ** | 0.05 | 0.153 | Approved |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alam, F.; Yang, Q.; Rūtelionė, A.; Bhutto, M.Y. Virtual Leadership and Nurses’ Psychological Stress during COVID-19 in the Tertiary Hospitals of Pakistan: The Role of Emotional Intelligence. Healthcare 2023, 11, 1537. https://doi.org/10.3390/healthcare11111537
Alam F, Yang Q, Rūtelionė A, Bhutto MY. Virtual Leadership and Nurses’ Psychological Stress during COVID-19 in the Tertiary Hospitals of Pakistan: The Role of Emotional Intelligence. Healthcare. 2023; 11(11):1537. https://doi.org/10.3390/healthcare11111537
Chicago/Turabian StyleAlam, Fahad, Qing Yang, Aušra Rūtelionė, and Muhammad Yaseen Bhutto. 2023. "Virtual Leadership and Nurses’ Psychological Stress during COVID-19 in the Tertiary Hospitals of Pakistan: The Role of Emotional Intelligence" Healthcare 11, no. 11: 1537. https://doi.org/10.3390/healthcare11111537
APA StyleAlam, F., Yang, Q., Rūtelionė, A., & Bhutto, M. Y. (2023). Virtual Leadership and Nurses’ Psychological Stress during COVID-19 in the Tertiary Hospitals of Pakistan: The Role of Emotional Intelligence. Healthcare, 11(11), 1537. https://doi.org/10.3390/healthcare11111537






