Abstract
Thrombophilia, also called hypercoagulability or prothrombotic condition, usually reflects a certain imbalance that occurs either in the coagulation cascade or in the anticoagulation/fibrinolytic system. A similar imbalance may be induced by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Thrombotic complications are associated with multiorgan failure and increased mortality. In this context, activation of coagulation and thrombocytopenia appeared as prognostic markers in COVID-19. Our work provides a structured and updated analysis of inherited thrombophilia and its involvement in COVID-19, emphasizing the importance of diagnosing and initiating thromboprophylaxis. Since the state of hypercoagulation is directly correlated with COVID-19, we consider that studies on the genetic profiles of proteins involved in thrombophilia in patients who have had COVID-19 and thrombotic events are of great importance, both in treating and in preventing deaths due to COVID-19.
1. Introduction
Thrombophilia is a coagulation abnormality that increases the risk of thrombosis (the formation of thrombi in the blood vessels); it is also called hypercoagulability or prothrombotic condition. It usually reflects a certain imbalance occurring either in the coagulation cascade or in the anticoagulation/fibrinolytic system [1]. Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), among other viral infections, may induce a similar imbalance. Thrombophilia can be inherited or acquired. The former is due to deficiencies of natural anticoagulants (antithrombin, protein C and protein S), increased homocysteine values, and changes in fibrinogen and coagulation factors. One important thing to note is that hereditary thrombophilia increases the risk of miscarriage. Acquired thrombophilia occurs as a result of secondary diseases, such as autoimmune disorders (antiphospholipid syndrome), trauma, or malignancy [1,2,3,4].
Thrombophilia aside, there are numerous (extrinsic) factors that increase the risk of thromboembolic disorders: obesity, surgery, smoking, pregnancy, the use of contraceptives, hormone replacement therapy, malignancy and antiphospholipid antibodies (lupus anticoagulant, anticardiolipin antibody, and anti-β2-glycoprotein-1 antibody) [5,6,7,8,9,10].
In-depth knowledge of all risk factors and understanding of their roles in the pathophysiology of venous thrombosis is of great importance, especially in the current pandemic context.
COVID-19 was initially described as an acute respiratory syndrome; later, other important features became apparent, in particular cytokine storms and systemic thromboembolism [11,12]. Since the beginning of the pandemic, significant efforts have been made worldwide to control and treat this disease. In the fight against the virus, the body over activates the immune system and causes a storm of cytokines [11]. The main components of a cytokine storm are the critical immune elements of the pro-inflammatory milieu.
Numerous studies have reported thrombosis as one of the most serious complications that can occur in patients with COVID-19 [13,14,15]. Thrombotic complications, such as deep-vein thrombosis, pulmonary embolism and stroke, are associated with multiorgan failure and increased mortality. In this context, activation of coagulation and thrombocytopenia have appeared as prognostic markers in COVID-19. Severe thrombotic manifestations of COVID-19 are thought to be due to the ability of severe acute respiratory syndrome coronavirus 2 to invade endothelial cells through the angiotensin-converting enzyme 2 (ACE-2). The cells, tissues and organs most affected are those with high expression of ACE-2, the entry receptor for severe acute respiratory syndrome coronavirus 2. Comorbidities that increase the risk of severe COVID-19 infection, including old age, obesity, diabetes, high blood pressure, respiratory disease, a compromised immune system, and coronary heart disease, or heart failure are associated with endothelial dysfunctional [16].
As potential therapies for the prevention of thrombosis associated with COVID-19, antithrombotic drugs, including heparin, factor XII inhibitors, and fibrinolytic drugs, have been administered [17]. One guide to thromboprophylaxis in COVID-19 recommends routine doses of thromboprophylaxis in the absence of contraindications in the hospital, increased intensity thromboprophylaxis in the intensive care unit, and consideration of anticoagulant thromboprophylaxis in patients with increased risk of venous thromboembolism post-hospital [18].
Improving diagnostic and treatment strategies can reduce thrombotic complications and ultimately improve the prognosis of patients with COVID-19.
We aimed to review available data on severe acute respiratory syndrome coronavirus 2 infections and inherited thrombophilia and to identify and highlight points relevant to therapeutic options in order to reduce mortality.
2. Blood Clotting Process
In essence, the phenomenon of blood clotting is the transformation of fibrinogen into insoluble fibrin [19,20] (Figure 1).
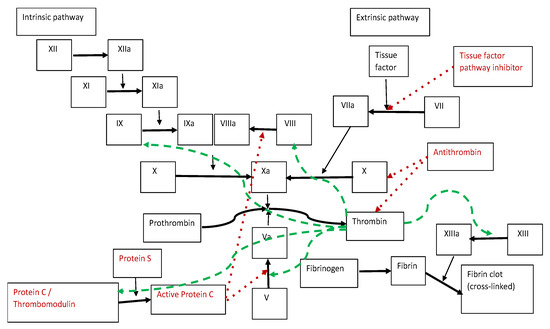
Figure 1.
Schematic representation of the coagulation process: coagulation factors (in black) and natural anticoagulants (in red); red dotted line—inhibitory effect; green dashed line—stimulatory effect; thick line—chemical transformation; thin line—catalytic effect.
Classically, it is considered that the activation of the coagulation cascade can be initiated via two pathways: extrinsic and intrinsic. The extrinsic pathway is initiated by a tissue trauma that leads to damage to the vascular wall. The intrinsic pathway is initiated by exposure of the blood to a negatively charged surface or to collagen in the traumatized vascular wall [21,22]. Both pathways lead to the activation of factor X (following the cleavage of a link between arginine and isoleucine) and converge in a common end pathway [23].
3. Overview of COVID-19
Coronaviruses are single-stranded RNA viruses that have been known for over 50 years. They cause severe acute respiratory syndrome, which in many cases leads to death. The virus that causes COVID-19 is thought to have originated in bats and then spread to humans [24].
Coronavirus disease 2019, also known as COVID-19, is a real challenge for specialists. COVID-19 infection has affected the lives of people around the world in terms of both physical and mental health as well as financial implications. It is characterized by a high mortality rate worldwide [25]. Over this period, considerable efforts have been made to quickly diagnose the disease and prevent and treat it. COVID-19 is known to bind to the angiotensin-converting enzyme 2 receptor and enter cells through the mechanism of endocytosis. Real-time PCR (RT-PCR) is considered the gold standard for diagnosis. Measurement of plasma D-dimer levels has been put forward as a prognostic marker.
Since December 2019, it has been reported that COVID-19 has caused the majority of cases of pneumonia [26]. The average incubation period of the virus was reported to be 5.2 days. The most common initial symptoms are fever, cough and fatigue [27,28]. It is known that the main target of COVID-19 infection is the lung. Although the main target of infection is the lung, the wide distribution of ACE-2 receptors in other organs may lead to cardiovascular, gastrointestinal, kidney, liver, central nervous system and ocular damage. Numerous complications associated with COVID-19 presented in the literature are summarized in Table 1.

Table 1.
Complications associated with COVID-19.
The course of COVID-19 disease in children is generally asymptomatic or mild compared to that seen in adults, for reasons that have not yet been clearly elucidated [61]. Most children have a low prevalence of symptoms [62]. The most common symptoms in children are fever, conjunctivitis, rash, and vomiting [63,64,65,66,67].
Although mortality is low in children with COVID-19, comorbidities are associated with a more severe course of infection [66,68,69,70].
It is obvious that COVID-19 infection causes severe coagulation disorders and that these play a crucial role in the outcomes of patients. Regarding COVID-19, the pathological changes of the disease and its pathogenesis in humans have not been clearly explained to date. Dissemination of information is key, including timely publication of statistics data, early diagnosis, reporting, and isolation and treatment. What is certain is that the lungs are the major organ involved.
4. Inherited Thrombophilia
Hereditary thrombophilia occurs when an inherited factor requires interaction with components that are inherited or acquired prior to a clinical disorder [71].
The most common causes of hereditary thrombophilia are: antithrombin deficiency, protein C deficiency, protein S deficiency, disturbances in fibrinogen levels, elevated homocysteine levels, factor II mutation (F2 c.*97G > A; previous nomenclature G20210A) and factor V Leiden mutation (HGVS nomenclature: F5 c.1601G > A) [71].
4.1. Antithrombin Deficiency
Antithrombin (AT) is a thrombin inhibitor and belongs to the serpin family (serine protease inhibitors); these are plasma proteins that inhibit serine proteases to prevent their uncontrolled activity. AT binds to the catalytic site of thrombin and is cleaved, and the resulting fragments remain firmly attached, block the active site and no longer allow fibrinogen to bind. AT activity is potentiated by heparin [72]. The electrostatic interaction between the electronegative heparin groups and the electropositive AT groups (protonated lysine residues) causes a conformational change of the AT, resulting in an increase in its antithrombin activity by about 1000 times. AT also inactivates other serine proteases involved in coagulation, such as factors Xa, XIa, XIIa and kallikrein [72].
AT deficiency is classified into:
- -
- Type I deficiency: reduced synthesis of the molecule (both antigenic and functional activity of AT in the blood are reduced);
- -
- Type II deficiency: molecular defect (AT immunological activity is normal but functional activity is reduced);
- -
- Type III: affected interaction between AT and heparin [71].
In elderly patients with antithrombin deficiency, the risk of thrombosis is increased and long-term administration of anticoagulants becomes unavoidable. Additionally, the incidence of venous thromboembolism is increased in pregnant women with AT deficiency [71]. Patients with type II AT deficiency have a higher risk of developing venous thromboembolism compared to those with type I AT deficiency [71].
4.2. Protein C Deficiency
Protein C is a protease produced by the liver that contains γ-carboxy-glutamate residues, formed with the participation of vitamin K. It is activated by thrombin. Attached to endothelial thrombomodulin, thrombin modifies its substrate specificity and activates protein C by proteolysis. Activated protein C, in the presence of a cofactor (protein S), degrades factors Va and VIIIa into inactive peptides, leading to coagulation limitation [72].
Hereditary deficiency is caused by a mutation in the PROC gene located on chromosome 2q14.3. Heterozygous and acquired deficiencies are more common than homozygous deficiencies [73]. An inherited or acquired risk factor for thrombophilia is protein C deficiency. People with inherited protein C deficiency have about a 2- to 11- fold increased risk of venous thromboembolism developing [72].
4.3. Protein S Deficiency
Protein S is a glycoprotein synthesized in the liver and is an important cofactor for protein C activation. Protein S is involved in the coagulation process, having anticoagulant properties both dependent on and independent of active protein C [73]. Approximately 40% of S protein circulates freely in the plasma and 60% with the plasma C4b binding protein (C4b-BP) [73].
Protein S deficiency is a rare genetic disorder of blood coagulation that is caused by a variation in the PROS1 gene. This variation is inherited in an autosomal dominant manner. A recent study published by Juhl et al. reported an association between two novel variants of the S protein gene and protein S deficiency [74].
The following types of S protein deficiency are known:
- -
- Type I: characterized by decreased activated protein C cofactor activity, low values of total S protein and free S protein;
- -
- Type II: characterized by decreased activated protein C cofactor activity, normal values of total S protein and free S protein;
- -
- Type III: characterized by decreased activated protein C cofactor activity, normal values of total S protein and low values of free S protein [73].
Patients with hereditary protein S deficiency have a high risk of venous thromboembolism recurrence. A retrospective study has shown that annual incidences of a first recurrence after the first episode of venous thromboembolism were 8.4% in protein S deficient patients [75].
4.4. Disturbances in Fibrinogen Levels
Fibrinogen is a glycoprotein with an elongated molecular shape, one of the least soluble in the protein system of the blood and is essential for the formation of fibrin clots. An increased risk of bleeding is associated with acquired and congenital fibrinogen disorders that can lead to a decreased concentration or altered fibrinogen function [76].
Thrombosis as a consequence of fibrinogen malfunction has been explained by two possible mechanisms: one involves abnormal thrombin binding to abnormal fibrin, leading to increased thrombin levels, and the second refers to the function of abnormal fibrin stimulation in fibrinolysis mediated by plasminogen activators [77]. Some patients with disturbed fibrinogen levels may experience thrombophilia and sometimes both bleeding and thromboembolism [76].
4.5. Elevated Homocysteine Levels
Homocysteine (Hcy) is a non-protein amino acid involved in the metabolism of methionine [78], produced by S-adenosylmethionine (SAM) and S-adenosylhomocysteine (SAH). Homocysteine metabolism involves several enzymes, namely: methionine synthase (MS), methylenetetrahydrofolate reductase (MTHFR), cystathionine β-synthase (CBS), methionine synthase reductase (MSR) and betaine-homocysteine S-methyltransferase (BHMT). Homocysteine can be converted to methionine by remethylation by MTHFR and MS requiring methylcobalamin (vitamin B12). The MTHFR mutation results in reduced enzymatic activity and, consequently, accumulation of homocysteine. Hcy can form cystathionine by condensation with serine, via trans-sulfuration, a CBS-catalyzed reaction dependent on vitamin B6 [79,80,81,82].
At the plasma level, four forms of homocysteine can be found, namely: free Hcy, protein-bound Hcy (S-linked and N-bound), oxidized forms of Hcy, and Hcy-thiolactone. Hyperhomocysteinemia (HHcy) is defined as a plasma level greater than 15 μmol/L [83]. HHcy may be due to genetic defects in the enzymes involved in the metabolism of homocysteine and associated vitamin deficiencies. Elevated homocysteine levels were observed in B12 deficiencies even when folate levels were normal. Only concomitant supplementation of B vitamins (Vitamin B6, Vitamin B12) and folic acid has been reported to be effective in reducing Hcy levels. To date, a large number of studies indicate that Hcy is an independent risk factor for cardiovascular disease and that there is a higher correlation between homocysteine and atherosclerosis levels than between cholesterol and atherosclerosis levels [78,83]. Hcy is thought to be associated with vascular dysfunction through the following mechanisms: generation of reactive species (ROS), triggering/maintaining the inflammatory response; initiation of thrombotic phenomena [80,84]. Endothelial dysfunction is one of the major events in the pathogenic mechanism of cardiovascular disease. In the evolution of this disease, inflammation is the trigger for the process [85,86,87]. Reactive species are among the compounds present at the site of the inflammation and play multiple roles, including as markers of the intensity of the lesion phenomenon, and molecules involved in defense and/or cell signaling. The literature indicates a link between homocysteine and reactive species. Hcy is a risk factor for thrombophilia and is associated with both venous thrombosis and arterial thrombosis [84]. A study by Ridker et al., over a period of 10 years, showed that the combination of hyperhomocysteinemia and Leiden factor V further increases the risk of venous thromboembolism [88].
4.6. Factor II Mutation
Prothrombin or coagulation factor II is the precursor of thrombin and is a major coagulation factor. It is synthesized in the liver and involves the participation of vitamin K. Factor II deficiency can be congenital or acquired.
A specific change in the genetic code causes the body to produce too much of the prothrombin protein. The most common point mutation of thrombosis is a factor II mutation known as prothrombin G20210A [89]. The F2 C.*97G > A (previous nomenclature G20210A) variant with autosomal dominant transmission is the second most common hereditary thrombophilia. Assuming that mutations in factor V Leiden and factor II are two genetic risk factors frequently involved in venous thromboembolism, Emmerich et al. [90] studied the risk of its occurrence in patients with both mutations. Their results showed that the frequency of Leiden factor V was lower in patients with pulmonary embolism than in patients with deep-vein thrombosis without pulmonary embolism, and the G20210A mutation was similar in both groups of patients [90].
4.7. Factor V Leiden
Factor V is a protein in the blood that is involved in the clotting cascade. The proteins involved in the coagulation cascade are activated when it is necessary to stop a hemorrhage. Anticoagulant proteins can deactivate factor V, stopping the formation of thrombi when coagulation is not required.
The point mutation in the factor V gene that leads to the replacement of arginine at position 506 with glutamine is responsible for the resistance to activated protein C. Factor V Leiden is an abnormal protein determined by a single-nucleotide polymorphism (1691G > A) in factor V, and is not susceptible to cleavage at position 506 by activated protein C [91]. Most people with factor V Leiden do not develop thrombophilia, but some may develop thrombosis that leads to long-term health problems and can be life-threatening. Persons with homozygous F2 c.*97G > A or double heterozygous carriers of factor V Leiden and F2 c.*97G > A do not have a risk of developing recurrent venous thromboembolism. Women may have an increased tendency to develop thrombophilia during pregnancy.
The most common inherited form of thrombophilia is related to factor V Leiden, and the second most common genetic form of thrombophilia is related to prothrombin and occurs in approximately 1.7–3% of the general European and American population [92].
5. A Closer Look at the Correlation with COVID-19
Many physicians treating COVID-19 patients have wondered whether patients with a hereditary thrombophilia develop COVID-19-associated coagulation disorders more frequently, whether these patients have a worse prognosis, and whether there are specific therapeutic options.
An important factor in patients diagnosed with COVID-19 is impaired coagulation function. A study of 49 patients with COVID-19 showed that AT levels were lower in non-survivors than in survivors. The authors reported that AT is strongly associated with mortality in COVID-19 and that this may be the link between obesity and a poorer prognosis in patients with COVID-19 [93]. Gardner et al. [94] tested AT levels in 19 patients with COVID-19 and reported an antithrombin deficiency in approximately 26% of them. In order to prevent death in patients with COVID-19, antithrombin deficiency should be considered.
Symptomatic subjects with hereditary protein S deficiency typically present with deep-vein thrombosis or pulmonary embolism [95]. In patients with COVID-19, free S protein may be reduced due to complications, leading to an increased risk of thromboembolism.
A study of the coagulation function of patients with SARS-CoV-2 reported elevated levels of D-dimer and fibrinogen. The results of the study showed significant hypercoagulability in patients with severe COVID-19 [96].
Similar results regarding hemostasis disorders in patients with COVID-19 were also reported by Hardy et al. [97], who investigated the following parameters: prothrombin time, heparin anti-Xa activity, fibrinogen, factor VIII activity, D-dimers, antithrombin and plasminogen activator inhibitor-I (PAI-1). In addition to hypercoagulability, the authors reported a low fibrinolytic capacity [97].
To date, there are very few studies on the link between inherited thrombophilia and COVID-19.
Studies showing the relationship between hereditary thrombophilia and COVID-19 are summarized in Table 2.

Table 2.
Studies on hereditary thrombophilia in the era of COVID-19.
One study has been published investigating the possible correlation of thrombotic events with hereditary thrombophilia factors in patients who died of COVID-19 [104]. The authors evaluated the mutations in FV 506R/Q, MTHFR 223A/V, F2 20210G/A and PAI-1 4G/5G. The results obtained by them show that the highest percentage was detected in pulmonary artery thrombosis, followed by pulmonary embolism. Additionally, the incidence of MTHFR 223A/V heterozygous and PAI-1 4G/5G heterozygous genotypes was higher in patients with COVID-19 and thrombotic events, and that of FV 506R/Q and F2 20210G/A heterozygotes was lower. The authors state that studies are being performed on a larger number of patients in order to establish the relationship between hereditary thrombophilia factors and thrombosis associated with COVID-19 [104]. The MTHFR gene encodes 5,10-methylenetetrahydrofolate reductase, which is involved in homocysteine metabolism. The severity of COVID-19 could be associated with HHcy and possibly with depleted folic acid in infected cells [105,106,107]. HHcy was correlated with an increase in the incidence and severity of COVID-19 [108]. The results of the study conducted by Cappadona et al. [107] showed that evidence for an association with severe COVID-19 was found for five loci: two folate metabolic genes (MTHFR and MTR), two hemostasis inhibitor genes (PROC and ADAMTS13), and a thrombospondin gene (THBS2). HHcy is also a cause of hereditary thrombophilia.
A study conducted by de la Morena-Barrio et al. [99] on the involvement of hereditary thrombophilia in COVID-19 revealed that most patients with severe thrombophilia did not have thrombotic events during SARS-CoV-2 infection. The authors considered that the reason why the hypercoagulability condition did not lead to the development of new thrombotic episodes was related to the fact that these patients were already being treated with anticoagulant drugs before COVID-19 or at the beginning of the disease. In this context, long-term anticoagulation treatment at admission appears to protect patients with COVID-19 from the development of thrombosis [99].
On the other hand, SARS-CoV-2 infection is associated with an increased prevalence of acquired thrombophilia. Ferrari et al. reported on 89 consecutive patients hospitalized for COVID-19 infection and observed a 20% prevalence of S protein deficiency and a higher prevalence (72%) of antiphospholipid antibodies, mainly lupus anticoagulants. They concluded that acquired thrombophilia does not directly correlate with the occurrence of thrombotic events and is probably an integral part of the inflammation storm [98]. Another small study (19 subjects), focused on coagulation tests, showed increased levels of D-dimers, fibrinogen degradation products, fibrinogen and FVIII, and mildly lower activities of natural anticoagulant activities; ten patients tested positive for antiphospholipid antibodies, four of whom developed cerebral thrombotic events. These data suggest a triggering role for the simultaneous elevation of FVIII activity and the presence of antiphospholipid antibodies leading to thrombotic events [109].
Acute cerebrovascular disease has been reported in patients with severe COVID-19 and vascular risk factors [110]. The results of the study, conducted by Topcouglu et al., [111] showed that major thrombophilia did not exist in any of the studied stroke patients with COVID-19.
Since the state of hypercoagulation is directly correlated with COVID-19, we consider that studies on the genetic profiles of proteins involved in thrombophilia in patients who have had COVID-19 and thrombotic events are of great importance, both in treating and in preventing deaths due to COVID-19.
6. Conclusions
Given the evolution of patients infected with COVID-19 (some are asymptomatic, while others have severe symptoms and a rapid deterioration of their condition), there are still many unanswered questions about the mechanisms of action and consequences of the virus. Our work provides a structured and updated analysis of inherited thrombophilia and its involvement in COVID-19. No significant trends of predisposition to hereditary thrombophilia were apparent in COVID-19-positive patients who died of thrombotic complications. It was quite unexpected that patients who died, due to thrombotic complications, had no predisposition to congenital thrombophilia. We can conclude that hereditary thrombophilia can aggravate COVID-19 disease and is a marker of poor prognosis in the disease. Thus, we consider studies of the genetic profiles of proteins involved in thrombophilia in patients with COVID-19 and thrombotic events to be of great importance in both the treatment and prevention of deaths caused by COVID-19.
Author Contributions
Conceptualization, N.F., O.V.B. and M.C.; methodology, P.D.S.; formal analysis, E.C.; investigation, I.B.-B.; resources, B.V.; data curation, M.C.B.; writing—original draft preparation, G.B., C.C.B., B.V., E.C. and I.B.-B.; writing—review and editing, N.F., M.C.B. and O.V.B.; visualization, G.B., C.C.B. and E.C.; supervision, O.V.B., E.C., C.C.B. and N.F.; project administration, M.C. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
Not applicable.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Montagnana, M.; Lippi, G.; Danese, E. An Overview of Thrombophilia and Associated Laboratory Testing. Hemostasis and Thrombosis. In Methods in Molecular Biology; Favaloro, E., Lippi, G., Eds.; Humana Press: New York, NY, USA, 2017. [Google Scholar] [CrossRef]
- Tripodi, A.; Mannucci, P.M. Laboratory investigation of thrombophilia. Clin. Chem. 2001, 47, 1597–1606. [Google Scholar] [CrossRef] [PubMed]
- Siriez, R.; Dogné, J.M.; Gosselin, R.; Laloy, J.; Mullier, F.; Douxfils, J. Comprehensive review of the impact of direct oral anticoagulants on thrombophilia diagnostic tests: Practical recommendations for the laboratory. Int. J. Lab. Hematol. 2021, 43, 7–20. [Google Scholar] [CrossRef] [PubMed]
- Khider, L.; Gendron, N.; Mauge, L. Inherited thrombophilia in the era of direct oral anticoagulants. Int. J. Mol. Sci. 2022, 23, 1821. [Google Scholar] [CrossRef] [PubMed]
- Badulescu, O.V.; Filip, N.; Sirbu, P.D.; Bararu-Bojan, I.; Vladeanu, M.; Bojan, A.; Ciocoiu, M. Current practices in haemophilic patients undergoing orthopedic surgery—A systematic review. Exp. Ther. Med. 2020, 20, 207. [Google Scholar] [CrossRef]
- Badulescu, O.V.; Sirbu, P.D.; Ungureanu, C.; Pȋnzariu, A.; Cojocaru, E.; Filip, N.; Bararu-Bojan, I.; Vladeanu, M.; Ciocoiu, M. Orthopedic surgery in hemophilic patients with musculoskeletal disorders: A systematic review. Exp. Ther. Med. 2021, 22, 995. [Google Scholar] [CrossRef]
- Badulescu, O.V.; Ciocoiu, M.; Filip, N.; Veringa, V. Tranexamic acid-major antifibrinolytic agent used to achieve hemostasis in hemophilic patients with anti-factor VIII antibodies who must undergo total joint replacement. Rev. Chim. Buchar. 2019, 70, 638–641. [Google Scholar] [CrossRef]
- Goldhaber, S.Z. Risk factors for venous thromboembolism. J. Am. Coll. Cardiol. 2010, 29, 1–7. [Google Scholar] [CrossRef]
- Engbers, M.J.; Van Hylckama Vlieg, A.; Rosendaal, F.R. Venous thrombosis in the elderly: Incidence, risk factors and risk groups. J. Thromb. Haemost. 2010, 8, 2105–2112. [Google Scholar] [CrossRef]
- Cushman, M. Epidemiology and risk factors for venous thrombosis. Semin. Hematol. 2007, 44, 62–69. [Google Scholar] [CrossRef]
- Song, P.; Li, W.; Xie, J.; Hou, Y.; You, C. Cytokine storm induced by SARS-CoV-2. Clin. Chim. Acta 2020, 509, 280–287. [Google Scholar] [CrossRef]
- Merrill, J.T.; Erkan, D.; Winakur, J.; James, J.A. Emerging evidence of a COVID-19 thrombotic syndrome has treatment implications. Nat. Rev. Rheumatol. 2020, 16, 581–589. [Google Scholar] [CrossRef] [PubMed]
- Klok, F.A.; Kruip, M.J.H.A.; Van der Meer, N.J.M.; Arbous, M.S.; Gommers, D.A.M.P.J.; Kant, K.M.; Kaptein, F.H.J.; van Passen, J.; Stals, M.A.M.; Huisman, M.V.; et al. Incidence of thrombotic complications in critically ill ICU patients with COVID-19. Thromb. Res. 2020, 191, 145–147. [Google Scholar] [CrossRef] [PubMed]
- Gąsecka, A.; Borovac, J.A.; Guerreiro, R.A.; Giustozzi, M.; Parker, W.; Caldeira, D.; Chiva-Blanch, G. Thrombotic complications in patients with COVID-19: Pathophysiological mechanisms, diagnosis, and treatment. Cardiovasc. Drugs Ther. 2021, 35, 215–229. [Google Scholar] [CrossRef] [PubMed]
- Avila, J.; Long, B.; Holladay, D.; Gottlieb, M. Thrombotic complications of COVID-19. Am. J. Emerg. Med. 2021, 39, 213–218. [Google Scholar] [CrossRef] [PubMed]
- Losso, J.N. The potential of dietary bioactive compounds against SARS-CoV-2 and COVID-19-induced endothelial dysfunction. Molecules 2022, 27, 1623. [Google Scholar] [CrossRef]
- McFadyen, J.D.; Stevens, H.; Peter, K. The emerging threat of (micro) thrombosis in COVID-19 and its therapeutic implications. Circ. Res. 2020, 127, 571–587. [Google Scholar] [CrossRef]
- Barnes, G.D.; Burnett, A.; Allen, A.; Blumenstein, M.; Clark, N.P.; Cuker, A.; Dager, W.E.; Deitelzweig, S.B.; Ellsworth, S.; Garcia, D.; et al. Thromboembolism and anticoagulant therapy during the COVID-19 pandemic: Interim clinical guidance from the anticoagulation forum. J. Thromb. Thrombolysis. 2020, 50, 72–81. [Google Scholar] [CrossRef]
- Hill, J.; Oderberg, D.S.; Gibbins, J.M.; Bojak, I. Mistake-making: A theoretical framework for generating research questions in biology, with illustrative application to blood clotting. Q. Rev. Biol. 2022, 97, 1–13. [Google Scholar] [CrossRef]
- Litvinov, R.I.; Pieters, M.; De Lange-Loots, Z.; Weisel, J.W. Fibrinogen and Fibrin. In Macromolecular Protein Complexes III: Structure and Function; Harris, J.R., Marles-Wright, J., Eds.; Springer: Cham, Switzerland, 2021; Volume 94, pp. 471–501. [Google Scholar] [CrossRef]
- Kumar, R. Physiology, coagulation cascade: Inherited disorders, and the molecular phenomenon of alterations in hemostasis. J. Clin. Haematol. 2021, 2, 62–64. [Google Scholar]
- Gailani, D.; Renné, T. Intrinsic pathway of coagulation and arterial thrombosis. Arter. Thromb Vasc. Biol. 2007, 27, 2507–2513. [Google Scholar] [CrossRef]
- Chaudhry, R.; Usama, S.M.; Babiker, H.M. Physiology, Coagulation Pathways; StatPearls Publishing: Treasure Island, FL, USA, 2021. [Google Scholar]
- Hamed, M.A. An overview on COVID-19: Reality and expectation. Bull. Natl. Res. Cent. 2020, 44, 86. [Google Scholar] [CrossRef]
- Yang, L.; Liu, S.; Liu, J.; Zhang, Z.; Wan, X.; Huang, B.; Chen, Y.; Zhang, Y. COVID-19: Immunopathogenesis and immunotherapeutics. Signal Transduct. Target Ther. 2020, 5, 128. [Google Scholar] [CrossRef] [PubMed]
- Kang, Y.; Xu, S. Comprehensive overview of COVID-19 based on current evidence. Dermatol. Ther. 2020, 33, e13525. [Google Scholar] [CrossRef] [PubMed]
- Li, Q.; Guan, X.; Wu, P.; Wang, X.; Zhou, L.; Tong, Y.; Ren, R.; Leung, K.S.M.; Lau, E.H.Y.; Wong, J.Y.; et al. Early transmission dynamics in Wuhan, China, of novel coronavirus-infected pneumonia. N. Engl. J. Med. 2020, 382, 1199–1207. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.C.; Chen, C.S.; Chan, Y.J. The outbreak of COVID-19: An overview. J. Chin. Med. Assoc. 2020, 83, 217–220. [Google Scholar] [CrossRef]
- Zeng, J.H.; Liu, Y.X.; Yuan, J.; Wang, F.X.; Wu, W.B.; Li, J.X.; Wang, L.F.; Gao, H.; Wang, Y.; Dong, C.F.; et al. First case of COVID-19 complicated with fulminant myocarditis: A case report and insights. Infection 2020, 48, 773–777. [Google Scholar] [CrossRef]
- Alhogbani, T. Acute myocarditis associated with novel Middle east respiratory syndrome coronavirus. Ann. Saudi Med. 2016, 36, 78–80. [Google Scholar] [CrossRef]
- Chen, T.; Wu, D.; Chen, H.; Yan, W.; Yang, D.; Chen, G.; Ma, K.; Xu, D.; Yu, H.; Wang, H.; et al. Clinical characteristics of 113 deceased patients with coronavirus disease 2019: Retrospective study. BMJ 2020, 368, m1091. [Google Scholar] [CrossRef]
- Zhou, F.; Yu, T.; Du, R.; Fan, G.; Liu, Y.; Liu, Z.; Xiang, J.; Wang, Y.; Song, B.; Gu, X.; et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study. Lancet 2020, 395, 1054–1062. [Google Scholar] [CrossRef]
- Driggin, E.; Madhavan, M.V.; Bikdeli, B.; Chuich, T.; Laracy, J.; Biondi-Zoccai, G.; Brown, T.S.; Der Nigoghossian, C.; Zidar, D.A.; Haythe, J.; et al. Cardiovascular considerations for patients, health care workers, and health systems during the COVID-19 pandemic. J. Am. Coll. Cardiol. 2020, 75, 2352–2371. [Google Scholar] [CrossRef]
- Sedaghat, Z.; Karimi, N. Guillain Barre syndrome associated with COVID-19 infection: A case report. J. Clin. Neurosci. 2020, 76, 233–235. [Google Scholar] [CrossRef] [PubMed]
- Paybast, S.; Gorji, R.; Mavandadi, S. Guillain-Barré Syndrome as a neurological complication of novel COVID-19 infection: A case report and review of the literature. Neurologist 2020, 25, 101–103. [Google Scholar] [CrossRef] [PubMed]
- Diez-Porras, L.; Vergés, E.; Gil, F.; Vidal, M.J.; Massons, J.; Arboix, A. Guillain-Barré-Strohl syndrome and COVID-19: Case report and literature review. Neuromuscul. Disord. 2020, 30, 859–861. [Google Scholar] [CrossRef] [PubMed]
- Rana, S.; Lima, A.A.; Chandra, R.; Valeriano, J.; Desai, T.; Freiberg, W.; Small, G. Novel coronavirus (COVID-19)-Associated Guillain-Barré syndrome: Case Report. J. Clin. Neuromuscul. Dis. 2020, 21, 240–242. [Google Scholar] [CrossRef]
- Zito, A.; Alfonsi, E.; Franciotta, D.; Todisco, M.; Gastaldi, M.; Cotta Ramusino, M.; Ceroni, M.; Costa, A. COVID-19 and Guillain-Barré syndrome: A case report and review of literature. Front. Neurol. 2020, 11, 909. [Google Scholar] [CrossRef]
- Ottaviani, D.; Boso, F.; Tranquillini, E.; Gapeni, I.; Pedrotti, G.; Cozzio, S.; Guarrera, G.M.; Giometto, B. Early Guillain-Barré syndrome in coronavirus disease 2019 (COVID-19): A case report from an Italian COVID-hospital. Neurol. Sci. 2020, 41, 1351–1354. [Google Scholar] [CrossRef]
- Ye, M.; Ren, Y.; Lv, T. Encephalitis as a clinical manifestation of COVID-19. Brain Behav. Immun. 2020, 88, 945–946. [Google Scholar] [CrossRef]
- Filatov, A.; Sharma, P.; Hindi, F.; Espinosa, P.S. Neurological complications of coronavirus disease (COVID-19): Encephalopathy. Cureus 2020, 12, e7352. [Google Scholar] [CrossRef]
- Bridwell, R.; Long, B.; Gottlieb, M. Neurologic complications of COVID-19. Am. J. Emerg. Med. 2020, 38, e3–e1549. [Google Scholar] [CrossRef]
- Ucpinar, B.A.; Sahin, C.; Yanc, U. Spontaneous pneumothorax and subcutaneous emphysema in COVID-19 patient: Case report. J. Infect. Public Health 2020, 13, 887–889. [Google Scholar] [CrossRef]
- Al-Shokri, S.D.; Ahmed, A.O.E.; Saleh, A.O.; AbouKamar, M.; Ahmed, K.; Mohamed, M.F.H. Case report: COVID-19-related pneumothorax-case series highlighting a significant complication. Am. J. Trop. Med. Hyg. 2020, 103, 1166–1169. [Google Scholar] [CrossRef] [PubMed]
- Alhakeem, A.; Khan, M.M.; Al Soub, H.; Yousaf, Z. Case report: COVID-19-Associated bilateral spontaneous pneumothorax-a literature review. Am. J. Trop. Med. Hyg. 2020, 103, 1162–1165. [Google Scholar] [CrossRef] [PubMed]
- Hazariwala, V.; Hadid, H.; Kirsch, D.; Big, C. Spontaneous pneumomediastinum, pneumopericardium, pneumothorax and subcutaneous emphysema in patients with COVID-19 pneumonia, a case report. J. Cardiothorac. Surg. 2020, 15, 301. [Google Scholar] [CrossRef] [PubMed]
- Shan, S.; Guangming, L.; Wei, L.; Xuedong, Y. Spontaneous pneumomediastinum, pneumothorax and subcutaneous emphysema in COVID-19: Case report and literature review. Rev. Inst. Med. Trop. Sao Paulo 2020, 62, e76. [Google Scholar] [CrossRef]
- Volpi, S.; Ali, J.M.; Suleman, A.; Ahmed, R.N. Pneumomediastinum in COVID-19 patients: A case series of a rare complication. Eur. J. Cardiothorac. Surg. 2020, 58, 646–647. [Google Scholar] [CrossRef] [PubMed]
- Quincho-Lopez, A.; Quincho-Lopez, D.L.; Hurtado-Medina, F.D. Case report: Pneumothorax and pneumomediastinum as uncommon complications of COVID-19 pneumonia-literature review. Am. J. Trop. Med. Hyg. 2020, 103, 1170–1176. [Google Scholar] [CrossRef]
- Garg, D.; Muthu, V.; Sehgal, I.S.; Ramachandran, R.; Kaur, H.; Bhalla, A.; Puri, G.D.; Chakrabarti, A.; Agarwal, R. Coronavirus disease (COVID-19) associated mucormycosis (CAM): Case report and systematic review of literature. Mycopathologia 2021, 186, 289–298. [Google Scholar] [CrossRef]
- Akel, T.; Qaqa, F.; Abuarqoub, A.; Shamoon, F. Pulmonary embolism: A complication of COVID 19 infection. Thromb. Res. 2020, 193, 79–82. [Google Scholar] [CrossRef]
- Gasparotto, M.; Framba, V.; Piovella, C.; Doria, A.; Iaccarino, L. Post-COVID-19 arthritis: A case report and literature review. Clin. Rheumatol. 2021, 40, 3357–3362. [Google Scholar] [CrossRef]
- Melquist, S.; Estepp, K.; Aleksandrovich, Y.; Lee, A.; Beiseker, A.; Hamedani, F.S.; Bassett, J. COVID-19 presenting as fulminant hepatic failure: A case report. Medicine 2020, 99, e22818. [Google Scholar] [CrossRef]
- Chacko, M.; Job, A.; Caston, F.; George, P.; Yacoub, A.; Cáceda, R. COVID-19-Induced psychosis and suicidal behavior: Case report. SN Compr. Clin. Med. 2020, 2, 2391–2395. [Google Scholar] [CrossRef] [PubMed]
- Huarcaya-Victoria, J.; Herrera, D.; Castillo, C. Psychosis in a patient with anxiety related to COVID-19: A case report. Psychiatry Res. 2020, 289, 113052. [Google Scholar] [CrossRef] [PubMed]
- Chandra, P.S.; Shiva, L.; Nagendrappa, S.; Ganjekar, S.; Thippeswamy, H. COVID 19 related Psychosis as an interface of fears, socio-cultural issues and vulnerability—Case report of two women from India. Psychiatry Res. 2020, 290, 113136. [Google Scholar] [CrossRef] [PubMed]
- Valdés-Florido, M.J.; López-Díaz, Á.; Palermo-Zeballos, F.J.; Martínez-Molina, I.; Martín-Gil, V.E.; Crespo-Facorro, B.; Ruiz-Veguilla, M. Reactive psychoses in the context of the COVID-19 pandemic: Clinical perspectives from a case series. Rev. Psiquiatr. Salud Ment. 2020, 13, 90–94. [Google Scholar] [CrossRef]
- Paul, T.; Joy, A.R.; Alsoub, H.A.R.S.; Parambil, J.V. Case Report: Ischemic colitis in severe COVID-19 pneumonia: An unforeseen gastrointestinal complication. Am. J. Trop. Med. Hyg. 2021, 104, 63–65. [Google Scholar] [CrossRef] [PubMed]
- Schultz, K.; Wolf, J.M. Digital ischemia in COVID-19 patients: Case report. J. Hand Surg. Am. 2020, 45, 518–522. [Google Scholar] [CrossRef] [PubMed]
- Mehta, P.; Bunker, C.B.; Ciurtin, C.; Porter, J.C.; Chambers, R.C.; Papdopoulou, C.; Garthwaite, H.; Hillman, T.; Heightman, M.; Howell, K.J.; et al. Chilblain-like acral lesions in long COVID-19: Management and implications for understanding microangiopathy. Lancet Infect. Dis. 2021, 21, 912. [Google Scholar] [CrossRef]
- Ciotti, M.; Ciccozzi, M.; Terrinoni, A.; Jiang, W.C.; Wang, C.B.; Bernardini, S. The COVID-19 pandemic. Crit. Rev. Clin. Lab. Sci. 2020, 57, 365–388. [Google Scholar] [CrossRef]
- Zimmermann, P.; Pittet, L.F.; Curtis, N. How common is long COVID in children and adolescents? Pediatr. Infect. Dis. J. 2021, 40, e482–e487. [Google Scholar] [CrossRef]
- Zimmermann, P.; Pittet, L.F.; Curtis, N. Long COVID in children and adolescents. BMJ 2022, 376, o143. [Google Scholar] [CrossRef]
- Siebach, M.K.; Piedimonte, G.; Ley, S.H. COVID-19 in childhood: Transmission, clinical presentation, complications and risk factors. Pediatr. Pulmonol. 2021, 56, 1342–1356. [Google Scholar] [CrossRef] [PubMed]
- Leung, E.C.; Chow, V.C.; Lee, M.K.; Lai, R.W. Deep throat saliva as an alternative diagnostic specimen type for the detection of SARS-CoV-2. J. Med. Virol. 2021, 93, 533–536. [Google Scholar] [CrossRef] [PubMed]
- Whittaker, E.; Bamford, A.; Kenny, J.; Kaforou, M.; Jones, C.E.; Shah, P.; Ramnarayan, P.; Fraisse, A.; Miller, O.; Davies, P.; et al. PIMS-TS study group and EUCLIDS and PERFORM consortia. clinical characteristics of 58 children with a pediatric inflammatory multisystem syndrome temporally associated with SARS-CoV-2. JAMA 2020, 324, 259–269. [Google Scholar] [CrossRef] [PubMed]
- Verdoni, L.; Mazza, A.; Gervasoni, A.; Martelli, L.; Ruggeri, M.; Ciuffreda, M.; Bonanomi, E.; D’Antiga, L. An outbreak of severe Kawasaki-like disease at the Italian epicentre of the SARS-CoV-2 epidemic: An observational cohort study. Lancet 2020, 395, 1771–1778. [Google Scholar] [CrossRef]
- Swann, O.V.; Holden, K.A.; Turtle, L.; Pollock, L.; Fairfield, C.J.; Drake, T.M.; Seth, S.; Egan, C.; Hardwick, H.E.; Halpin, S.; et al. ISARIC4C investigators. Clinical characteristics of children and young people admitted to hospital with COVID-19 in United Kingdom: Prospective multicentre observational cohort study. BMJ 2020, 370, m3249. [Google Scholar] [CrossRef]
- Zhang, F.; Xiong, Y.; Wei, Y.; Hu, Y.; Wang, F.; Li, G.; Liu, K.; Du, R.; Wang, C.Y.; Zhu, W. Obesity predisposes to the risk of higher mortality in young COVID-19 patients. J. Med. Virol. 2020, 92, 2536–2542. [Google Scholar] [CrossRef]
- Leon-Abarca, J.A. Obesity and immunodeficiencies are the main pre-existing conditions associated with mild to moderate COVID-19 in children. Pediatr. Obes. 2020, 15, e12713. [Google Scholar] [CrossRef]
- Khan, S.; Dickerman, J.D. Hereditary thrombophilia. Thromb. J. 2006, 4, 15. [Google Scholar] [CrossRef][Green Version]
- Aydin, S.; Ugur, K.; Yalcin, H.; Sahin, İ.; Akkoc, R.F.; Yakar, B.; Yucel, D.; Aydin, S. Overview of COVID-19’s relationship with thrombophilia proteins. Turk. J. Biochem. 2021, 46, 609–622. [Google Scholar] [CrossRef]
- Ten Kate, M.K.; Van der Meer, J. Protein S deficiency: A clinical perspective. Haemophilia 2008, 14, 1222–1228. [Google Scholar] [CrossRef]
- Juhl, D.; Kuta, P.; Shneyder, M.; Wünsche, F.; Nowak-Göttl, U. Two novel variants in the protein S Gene PROS1 are associated with protein S deficiency and thrombophilia. Acta Haematol. 2021, 144, 222–226. [Google Scholar] [CrossRef] [PubMed]
- Brouwer, J.L.; Lijfering, W.M.; Ten Kate, M.K.; Kluin-Nelemans, H.C.; Veeger, N.J.; Van der Meer, J. High long-term absolute risk of recurrent venous thromboembolism in patients with hereditary deficiencies of protein S, protein C or antithrombin. Thromb. Haemostasis. 2009, 101, 93–99. [Google Scholar] [CrossRef]
- Verhovsek, M.; Moffat, K.A.; Hayward, C.P. Laboratory testing for fibrinogen abnormalities. Am. J. Hematol. 2008, 83, 928–931. [Google Scholar] [CrossRef] [PubMed]
- Haverkate, F.; Samama, M. Familial dysfibrinogenemia and thrombophilia. Report on a study of the SSC Subcommittee on Fibrinogen. Thromb. Haemost. 1995, 73, 151–161. [Google Scholar] [PubMed]
- Filip, A.; Badulescu, O.V.; Sirbu, P.D.; Cojocaru, E.; Filip, N.; Puha, G.; Trandafir, L.; Iancu, C.; Trandafirescu, M.F.; Alexa, O. Serum homocysteine and reactive species levels in fragility fractures of the pelvis. Revista de Chimie 2019, 70, 3216–3219. [Google Scholar] [CrossRef]
- Filip, C.; Albu, E.; Lupascu, D.; Filip, N. The influence of a new rutin derivative in an experimental model of induced hyperhomocysteinemia in rats. Farmacia 2017, 65, 596–599. [Google Scholar]
- Albu, E.; Filip, C.; Zamosteanu, N.; Jaba, I.M.; Linic, I.S.; Sosa, I. Hyperhomocysteinemia is an indicator of oxidant stress. Med. Hypotheses 2012, 78, 554–555. [Google Scholar] [CrossRef]
- Filip, C.; Albu, E.; Zamosteanu, N.; Silion, M.; Jerca, L.; Gheroghita, N.; Mungiu, C. Hyperhomocysteinemia’s effect on antioxidant capacity in rats. Open Med. 2010, 5, 620–626. [Google Scholar] [CrossRef]
- Albu, E.; Lupascu, D.; Filip, C.; Jaba, I.M.; Zamosteanu, N. The influence of a new rutin derivative on homocysteine, cholesterol and total antioxidative status in experimental diabetes in rat. Farmacia 2013, 61, 1167–1177. [Google Scholar]
- Filip, N.; Iancu, C.E. Introductory Chapter: General Aspects Regarding Homocysteine. In Non-Proteinogenic Amino Acids; IntechOpen: London, UK, 2018. [Google Scholar]
- Filip, C.; Socolov, D.G.; Albu, E.; Filip, C.; Serban, R.; Popa, R.F. Serological parameters and vascular investigation for a better assessment in dvt during pregnancy—A systematic review. Medicina 2021, 57, 160. [Google Scholar] [CrossRef]
- Trandafir, L.M.; Russu, G.; Moscalu, M.; Miron, I.; Lupu, V.V.; Leon Constantin, M.M.; Cojocaru, E.; Lupu, A.; Frasinariu, O.E. Waist circumference a clinical criterion for prediction of cardio-vascular complications in children and adolescences with overweight and obesity. Medicine 2020, 99, e20923. [Google Scholar] [CrossRef] [PubMed]
- Buca, B.R.; Tartau, L.M.; Rezus, C.; Filip, C.; Pinzariu, A.C.; Rezus, E.; Popa, G.E.; Panainte, A.; Lupusoru, C.E.; Bogdan, M.; et al. The effects of two nitric oxide donors in acute inflammation in rats. Rev. Chim. 2018, 69, 2899–2903. [Google Scholar] [CrossRef]
- Moroşan, E.; Mihailovici, M.S.; Giuşcă, S.E.; Cojocaru, E.; Avădănei, E.R.; Căruntu, I.D.; Teleman, S. Hepatic steatosis background in chronic hepatitis B and C—Significance of similarities and differences. Rom. J. Morphol. Embryol. 2014, 55, 1041–1047. [Google Scholar] [PubMed]
- Ridker, P.M.; Hennekens, C.H.; Selhub, J.; Miletich, J.P.; Malinow, M.R.; Stampfer, M.J. Interrelation of hyperhomocyst(e)inemia, factor V Leiden, and risk of future venous thromboembolism. Circulation 1997, 95, 1777–1782. [Google Scholar] [CrossRef] [PubMed]
- Varga, E.A.; Moll, S. Cardiology patient pages. Prothrombin 20210 mutation (factor II mutation). Circulation 2004, 20, e15-18. [Google Scholar] [CrossRef]
- Emmerich, J.; Rosendaal, F.R.; Cattaneo, M.; Margaglione, M.; De Stefano, V.; Cumming, T.; Arruda, V.; Hillarp, A.; Reny, J.L. Combined effect of factor V Leiden and prothrombin 20210A on the risk of venous thromboembolism-pooled analysis of 8 case-control studies including 2310 cases and 3204 controls. Study group for pooled-analysis in venous thromboembolism. Thromb. Haemost. 2001, 86, 809–816, Erratum in: Thromb. Haemost. 2001, 86, 1598. [Google Scholar]
- De Stefano, V.; Chiusolo, P.; Paciaroni, K.; Leone, G. Epidemiology of factor V Leiden: Clinical implications. Semin. Thromb. Hemost. 1998, 24, 367–379. [Google Scholar] [CrossRef]
- Gazzaruso, C.; Paolozzi, E.; Valenti, C.; Brocchetta, M.; Naldani, D.; Grignani, C.; Salvucci, F.; Marino, F.; Coppola, A.; Gallotti, P. Association between antithrombin and mortality in patients with COVID-19. A possible link with obesity. Nutr. Metab. Cardiovasc. Dis. 2020, 30, 1914–1919. [Google Scholar] [CrossRef]
- Kujovich, J.L. Factor V Leiden Thrombophilia. In GeneReviews; University of Washington: Seattle, WA, USA, 1993. [Google Scholar]
- Gardner, A.J.; Kirkin, D.J.; Rodriguez-Villar, S.; Leoz Abellanas, G.; Tee, A.; Valentin, A. Antithrombin III deficiency-induced coagulopathy in the context of COVID-19: A case series. Br. J. Haematol. 2021, 194, 1007–1009. [Google Scholar] [CrossRef]
- Dinarvand, P.; Moser, K.A. Protein C deficiency. Arch. Pathol. Lab. Med. 2019, 143, 1281–1285. [Google Scholar] [CrossRef]
- Lu, H.; Chen, M.; Tang, S.; Yu, W. Association of coagulation disturbances with severity of COVID-19: A longitudinal study. Hematology 2021, 26, 656–662. [Google Scholar] [CrossRef] [PubMed]
- Hardy, M.; Michaux, I.; Lessire, S.; Douxfils, J.; Dogné, J.M.; Bareille, M.; Horlait, G.; Bulpa, P.; Chapelle, C.; Laporte, S.; et al. Prothrombotic disturbances of hemostasis of patients with severe COVID-19: A prospective longitudinal observational study. Thromb. Res. 2021, 197, 20–23. [Google Scholar] [CrossRef] [PubMed]
- Ferrari, E.; Sartre, B.; Squara, F.; Contenti, J.; Occelli, C.; Lemoel, F.; Levraut, J.; Doyen, D.; Dellamonica, J.; Mondain, V.; et al. High prevalence of acquired thrombophilia without prognosis value in patients with coronavirus disease 2019. J. Am. Heart Assoc. 2020, 9, e017773. [Google Scholar] [CrossRef] [PubMed]
- De la Morena-Barrio, M.E.; Bravo-Pérez, C.; De la Morena-Barrio, B.; Orlando, C.; Cifuentes, R.; Padilla, J.; Miñano, A.; Herrero, S.; Marcellini, S.; Revilla, N.; et al. A pilot study on the impact of congenital thrombophilia in COVID-19. Eur. J. Clin. Investig. 2021, 51, e13546. [Google Scholar] [CrossRef]
- Burlacu, A.; Artene, B.; Crisan-Dabija, R.; Popa, I.V.; Covic, A. Is thrombophilic genetic profile responsible for an acute ischemic stroke in a COVID-19 male patient? Clin. Appl. Thromb. Hemost. 2020, 26, 1076029620967107. [Google Scholar] [CrossRef]
- Bussani, R.; Schneider, E.; Zentilin, L.; Collesi, C.; Ali, H.; Braga, L.; Volpe, M.C.; Colliva, A.; Zanconati, F.; Berlot, G.; et al. Persistence of viral RNA, pneumocyte syncytia and thrombosis are hallmarks of advanced COVID-19 pathology. EBio Med. 2020, 61, 103104. [Google Scholar] [CrossRef]
- Yuriditsky, E.; Horowitz, J.M.; Merchan, C.; Ahuja, T.; Brosnahan, S.B.; McVoy, L.; Berger, J.S. Thromboelastography profiles of critically Ill patients with coronavirus disease 2019. Crit. Care Med. 2020, 48, 1319–1326. [Google Scholar] [CrossRef]
- Brosnahan, S.B.; Smilowitz, N.R.; Amoroso, N.E.; Barfield, M.; Berger, J.S.; Goldenberg, R.; Ishida, K.; Talmor, N.; Torres, J.; Yaghi, S.; et al. Thrombosis at hospital presentation in patients with and without coronavirus disease 2019. J. Vasc. Surg. Venous Lymphat. Disord. 2021, 9, 845–852. [Google Scholar] [CrossRef]
- Abdullaev, A.; Fevraleva, I.; Odilov, A.; Volkov, A.; Babichenko, I.; Sudarikov, A. Thrombotic events and the profile of hereditary thrombophilia factors in COVID-19 patients. HemaSphere 2021, 5, 641. [Google Scholar]
- Zhang, Y.; Guo, R.; Kim, S.H.; Shah, H.; Zhang, S.; Liang, J.H.; Fang, Y.; Gentili, M.; Leary, C.N.O.; Elledge, S.J.; et al. SARS-CoV-2 hijacks folate and one-carbon metabolism for viral replication. Nat. Commun. 2021, 12, 1676. [Google Scholar] [CrossRef]
- Karst, M.; Hollenhorst, J.; Achenbach, J. Life-threatening course in coronavirus disease 2019 (COVID-19): Is there a link to methylenetetrahydrofolic acid reductase (MTHFR) polymorphism and hyperhomocysteinemia? Med. Hypotheses 2020, 144, 110234. [Google Scholar] [CrossRef] [PubMed]
- Cappadona, C.; Paraboschi, E.M.; Ziliotto, N.; Bottaro, S.; Rimoldi, V.; Gerussi, A.; Azimonti, A.; Brenna, D.; Brunati, A.; Cameroni, C.; et al. MEDTEC Students against Coronavirus: Investigating the role of hemostatic genes in the predisposition to COVID-19 Severity. J. Pers. Med. 2021, 11, 1166. [Google Scholar] [CrossRef] [PubMed]
- Ponti, G.; Roli, L.; Oliva, G.; Manfredini, M.; Trenti, T.; Kaleci, S.; Iannella, R.; Balzano, B.; Coppola, A.; Fiorentino, G.; et al. Homocysteine (Hcy) assessment to predict outcomes of hospitalized COVID-19 patients: A multicenter study on 313 COVID-19 patients. Clin. Chem. Lab. Med. 2021, 59, e354–e357. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Cao, W.; Jiang, W.; Xiao, M.; Li, Y.; Tang, N.; Liu, Z.; Yan, X.; Zhao, Y.; Li, T.; et al. Profile of natural anticoagulant, coagulant factor and anti-phospholipid antibody in critically ill COVID-19 patients. J. Thromb. Thrombolysis 2020, 50, 580–586. [Google Scholar] [CrossRef]
- Nogueira, R.G.; Abdalkader, M.; Qureshi, M.M.; Frankel, M.R.; Mansour, O.Y.; Yamagami, H.; Qiu, Z.; Farhoudi, M.; Siegler, J.E.; Yaghi, S.; et al. Global impact of COVID-19 on stroke care. Int J. Stroke 2021, 16, 573–584. [Google Scholar] [CrossRef]
- Topcuoglu, M.A.; Pektezel, M.Y.; Oge, D.D.; Bulut Yüksel, N.D.; Ayvacioglu, C.; Demirel, E.; Balci, S.; Arat, A.; Akinci, S.B.; Arsava, E.M. Stroke mechanism in COVID-19 infection: A prospective case-control study. J. Stroke Cerebrovasc. Dis. 2021, 30, 105919. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).