Direct Effect of Local Cryotherapy on Muscle Stimulation, Pain and Strength in Male Office Workers with Lateral Epicondylitis, Non-Randomized Clinical Trial Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
- -
- Age from 25 to 40 years;
- -
- Pain around the lateral epicondyle during the extension of wrist and fingers against resistance and/or pain with resisted supination, pain with passive stretch to the wrist extensor or supinator muscles, and tenderness over the lateral epicondyle;
- -
- Symptoms lasting for at least 3 months;
- -
- Unilateral epicondylitis.
2.2. Experimental Design and Protocol
- Preparation for research
- -
- Detailed presentation of examination procedures by the researcher;
- -
- Skin preparation for sEMG measurement;
- -
- Making sure that procedures were understood and performing 1 PFG and sEMG test run;
- After 10 min of rest, the subject assessed pain in the lateral epicondylar region on a 10-point VAS scale (visual analogue scale) felt during the resisted extension of the wrist in the upper limb diagnosed with LE;
- Immediately after VAS, PFG was assessed;
- Immediately after PFG, the extensor carpi radialis activity was assessed (EMG) during the rest position, and maximal voluntary contraction (MVC), and 60 s of fatigue isometric contraction were measured;
- After 10 min of rest, a local cryotherapy treatment with liquid nitrogen vapours in the area of the lateral epicondyle and forearm was performed;
- Immediately after the end of LC, the measurement procedures were repeated in the indicated sequence (points 2–5).
2.3. Pain Assessment
2.4. Pain-Free Grip (PFG)
2.5. Surface Electromyography
2.6. Local Cryotherapy
2.7. Statistical Analysis
3. Results
3.1. Effect of Local Cryotherapy on Resting and MVC Signal Amplitude, PFG and VAS
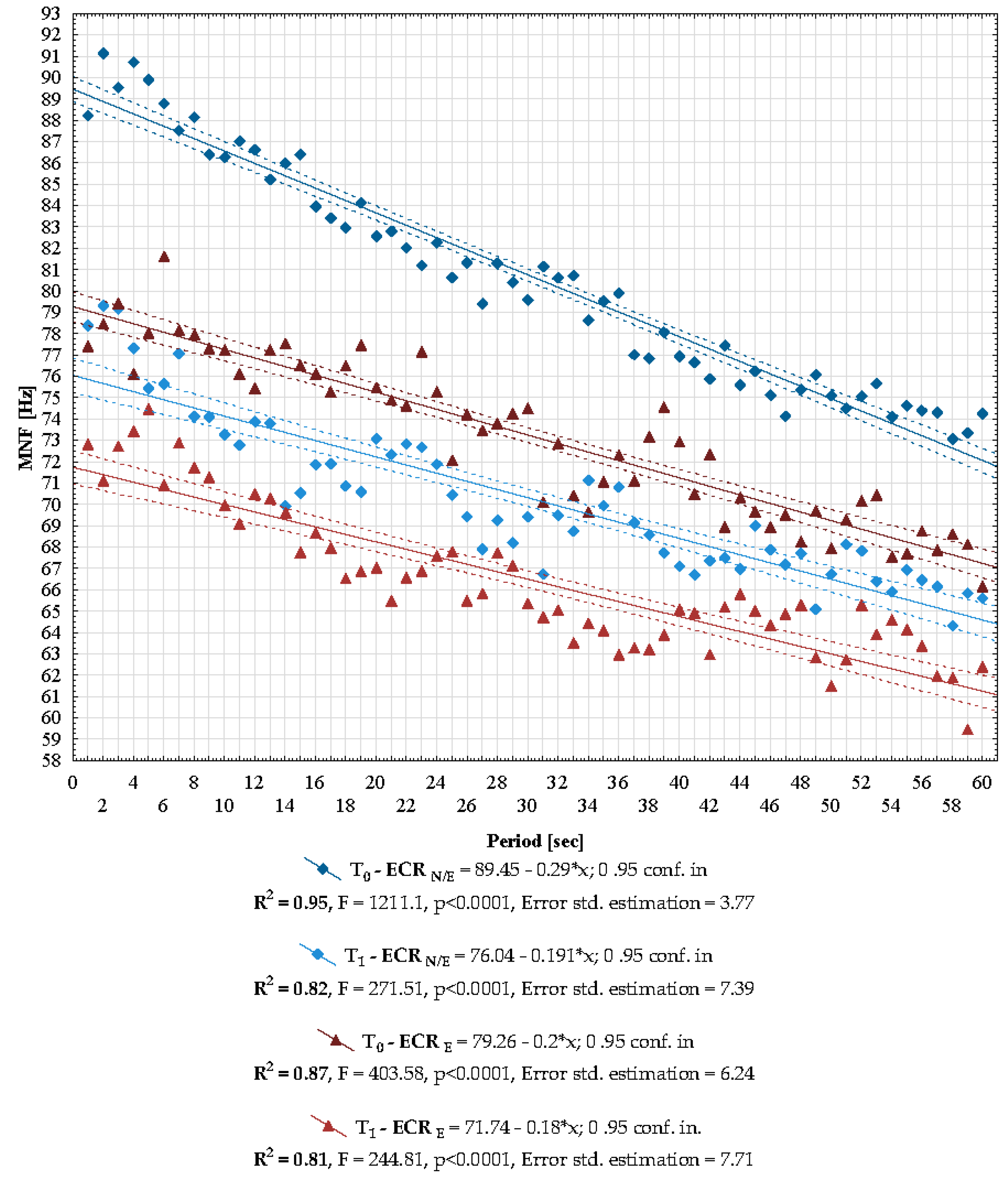
3.2. Effect of Local Cryotherapy on Electromyographic Indices of Fatigue
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Viswas, R.; Ramachandran, R.; Korde Anantkumar, P. Comparison of Effectiveness of Supervised Exercise Program and Cyriax Physiotherapy in Patients with Tennis Elbow (Lateral Epicondylitis): A Randomized Clinical Trial. Sci. World J. 2012, 2012, 939645. [Google Scholar] [CrossRef] [PubMed]
- Ahmad, Z.; Siddiqui, N.; Malik, S.S.; Abdus-Samee, M.; Tytherleigh-Strong, G.; Rushton, N. Lateral epicondylitis. Bone Jt. J. 2013, 95-B, 1158–1164. [Google Scholar] [CrossRef] [PubMed]
- Ma, K.L.; Wang, H.Q. Management of Lateral Epicondylitis: A Narrative Literature Review. Pain Res. Manag. 2020, 2020, 6965381. [Google Scholar] [CrossRef] [PubMed]
- Smith, P.N.; Ling, R.S.M.; Taylor, R. Tendinosis of the elbow (tennis elbow). Clinical features and findings of histological, immunohistochemical, and electron microscopy studies. J. Bone Jt. Surg. Am. 1999, 81, 259–278. [Google Scholar] [CrossRef]
- Bass, E. Tendinopathy: Why the Difference Between Tendinitis and Tendinosis Matters. Int. J. Ther. Massage Bodyw. 2012, 5, 14. [Google Scholar] [CrossRef]
- Patterson-Kane, J.C.; Becker, D.L.; Rich, T. The Pathogenesis of Tendon Microdamage in Athletes: The Horse as a Natural Model for Basic Cellular Research. J. Comp. Pathol. 2012, 147, 227–247. [Google Scholar] [CrossRef]
- Ljung, B.O.; Alfredson, H.; Forsgren, S. Neurokinin 1-receptors and sensory neuropeptides in tendon insertions at the medial and lateral epicondyles of the humerus Studies on tennis elbow and medial epicondylalgia. J. Orthop. Res. 2004, 22, 321–327. [Google Scholar] [CrossRef]
- Han, S.H.; An, H.J.; Song, J.Y.; Shin, D.E.; Kwon, Y.D.; Shim, J.S.; Lee, S.C. Effects of corticosteroid on the expressions of neuropeptide and cytokine mRNA and on tenocyte viability in lateral epicondylitis. J. Inflamm. 2012, 9, 40. [Google Scholar] [CrossRef]
- Uchio, Y.; Ochi, M.; Ryoke, K.; Sakai, Y.; Ito, Y.; Kuwata, S. Expression of neuropeptides and cytokines at the extensor carpi radialis brevis muscle origin. J. Shoulder Elb. Surg. 2002, 11, 570–575. [Google Scholar] [CrossRef]
- Zwerus, E.L.; Somford, M.P.; Maissan, F.; Heisen, J.; Eygendaal, D.; Van Den Bekerom, M.P. Physical examination of the elbow, what is the evidence? A systematic literature review. Br. J. Sports Med. 2018, 52, 1253–1260. [Google Scholar] [CrossRef]
- Lenoir, H.; Mares, O.; Carlier, Y. Management of lateral epicondylitis. Orthop. Traumatol. Surg. Res. 2019, 105, S241–S246. [Google Scholar] [CrossRef] [PubMed]
- Shiri, R.; Viikari-Juntura, E.; Varonen, H.; Heliövaara, M. Prevalence and Determinants of Lateral and Medial Epicondylitis: A Population Study. Am. J. Epidemiol. 2006, 164, 1065–1074. [Google Scholar] [CrossRef] [PubMed]
- Vicenzino, B.; Wright, A. Lateral epicondylalgia I: Epidemiology, pathophysiology, aetiology and natural history. Phys. Ther. Rev. 2013, 1, 23–34. [Google Scholar] [CrossRef]
- Weber, C.; Thai, V.; Neuheuser, K.; Groover, K.; Christ, O. Efficacy of physical therapy for the treatment of lateral epicondylitis: A meta-analysis. BMC Musculoskelet Disord. 2015, 16, 223. [Google Scholar] [CrossRef] [PubMed]
- Yan, C.; Xiong, Y.; Chen, L.; Endo, Y.; Hu, L.; Liu, M.; Liu, J.; Xue, H.; Abududilibaier, A.; Mi, B.; et al. A comparative study of the efficacy of ultrasonics and extracorporeal shock wave in the treatment of tennis elbow: A meta-analysis of randomized controlled trials. J. Orthop. Surg. Res. 2019, 14, 248. [Google Scholar] [CrossRef]
- Kim, Y.J.; Wood, S.M.; Yoon, A.P.; Howard, J.C.; Yang, L.Y.; Chung, K.C. Efficacy of Nonoperative Treatments for Lateral Epicondylitis: A Systematic Review and Meta-Analysis. Plast. Reconstr. Surg. 2021, 147, 112–125. [Google Scholar] [CrossRef]
- Özmen, T.; Koparal, S.S.; Karataş, Ö.; Eser, F.; Özkurt, B.; Gafuroğlu, Ü. Comparison of the clinical and sonographic effects of ultrasound therapy, extracorporeal shock wave therapy, and Kinesio taping in lateral epicondylitis. Turk. J. Med. Sci. 2021, 51, 76–83. [Google Scholar] [CrossRef]
- Manias, P.; Stasinopoulos, D. A controlled clinical pilot trial to study the effectiveness of ice as a supplement to the exercise programme for the management of lateral elbow tendinopathy. Br. J. Sports Med. 2006, 40, 81–85. [Google Scholar] [CrossRef]
- Muhsen, A.; Moss, P.; Gibson, W.; Walker, B.; Angela Jacques, M.B.; Schug, S.; Wright, A. The Association Between Conditioned Pain Modulation and Manipulation-induced Analgesia in People With Lateral Epicondylalgia. Clin. J. Pain 2019, 35, 435–442. [Google Scholar] [CrossRef]
- Yarrobino, T.E.; Kalbfleisch, J.H.; Ferslew, K.E.; Panus, P.C. Lidocaine iontophoresis mediates analgesia in lateral epicondylalgia treatment. Physiother. Res. Int. 2006, 11, 152–160. [Google Scholar] [CrossRef]
- Cholewka, A.; Stanek, A.; Wójcik, M.; Sieroń-Stołtny, K.; Drzazga, Z. Does local cryotherapy improve thermal diagnosis similar to whole-body cryotherapy in spinal diseases? J. Therm. Anal. Calorim. 2017, 127, 1155–1162. [Google Scholar] [CrossRef]
- Loro, W.A.; Thelen, M.D.; Rosenthal, M.D.; Stoneman, P.D.; Ross, M.D. The effects of cryotherapy on quadriceps electromyographic activity and isometric strength in patient in the early phases following knee surgery. J. Orthop. Surg. 2019, 27, 2309499019831454. [Google Scholar] [CrossRef] [PubMed]
- Kennet, J.; Hardaker, N.; Hobbs, S.; Selfe, J. Cooling efficiency of 4 common cryotherapeutic agents. J. Athl. Train. 2007, 42, 343–348. [Google Scholar] [PubMed]
- Costello, J.T.; Donnelly, A.E.; Karki, A.; Selfe, J. Effects of whole body cryotherapy and cold water immersion on knee skin temperature. Int. J. Sports Med. 2014, 35, 35–40. [Google Scholar] [CrossRef] [PubMed]
- Mourot, L.; Cluzeau, C.; Regnard, J. Hyperbaric Gaseous Cryotherapy: Effects on Skin Temperature and Systemic Vasoconstriction. Arch. Phys. Med. Rehabil. 2007, 88, 1339–1343. [Google Scholar] [CrossRef]
- Hermann, J. Kryotherapie. Z. Rheumatol. 2009, 68, 539–542. [Google Scholar] [CrossRef]
- Stanek, A.; Wielkoszyński, T.; Bartuś, S.; Cholewka, A. Whole-Body Cryostimulation Improves Inflammatory Endothelium Parameters and Decreases Oxidative Stress in Healthy Subjects. Antioxidants 2020, 9, 1308. [Google Scholar] [CrossRef]
- Allan, R.; Malone, J.; Alexander, J.; Vorajee, S.; Ihsan, M.; Gregson, W.; Kwiecien, S.; Mawhinney, C. Cold for centuries: A brief history of cryotherapies to improve health, injury and post-exercise recovery. Eur. J. Appl. Physiol. 2022, 122, 1153–1162. [Google Scholar] [CrossRef]
- Stanek, A.; Kasperczyk, S.; Birkner, E. Influence of Cryogenic Temperatures on Inflammatory Markers in Patients with Ankylosing Spondylitis. Pol. J. Environ. Stud. 2010, 19, 167–175. [Google Scholar]
- Delimar, V.; Vukorepa, M. Local cryotherapy, comparison of cold air and ice massage on pain and handgrip strength in patients with rheumatoid arthritis. Psychiatr. Danub. 2021, 33, 757–761. [Google Scholar]
- Ksiezopolska-Pietrzak, K. Cryotherapy in osteoporosis. Pol. Merkur. Lek. 1998, 5, 222–224. [Google Scholar]
- Lubkowska, A. Cryotherapy: Physiological Considerations and Applications to Physical Therapy. In Physical Therapy Perspectives in the 21st Century-Challenges and Possibilities; Bettany-Saltikov, J., Paz-Lourido, B., Eds.; Intech Open: London, UK, 2012; Available online: https://www.intechopen.com/chapters/35000 (accessed on 25 March 2022). [CrossRef]
- Yilmaz, N.; Kiyak, E. The effects of local cold application on fibromyalgia pain. Int. J. Rheum. Dis. 2017, 20, 929–934. [Google Scholar] [CrossRef] [PubMed]
- Rivenburgh, D.W. Physical modalities in the treatment of tendon injuries. Clin. Sports Med. 1992, 11, 645–659. [Google Scholar] [CrossRef]
- Gonzales, B.R.; Hagin, V.; Guillot, R.; Placet, V.; Monnier-Benoit, P.; Groslambert, A. Self-paced cycling performance and recovery under a hot and highly humid environment after cooling. J. Sports Med. Phys. Fit. 2014, 54, 43–52. [Google Scholar]
- Ückert, S.; Joch, W. Effects of warm-up and precooling on endurance performance in the heat. Br. J. Sports Med. 2007, 41, 380–384. [Google Scholar] [CrossRef]
- Ranalli, G.F.; Demartini, J.K.; Casa, D.J.; Mcdermott, B.P.; Armstrong, L.E.; Maresh, C.M. Effect of body cooling on subsequent aerobic and anaerobic exercise performance: A systematic review. J. Strength Cond. Res. 2010, 24, 3488–3496. [Google Scholar] [CrossRef]
- Richer, N.; Marchand, A.A.; Descarreaux, M. Management of Chronic Lateral Epicondylitis With Manual Therapy and Local Cryostimulation: A Pilot Study. J. Chiropr. Med. 2017, 16, 279–288. [Google Scholar] [CrossRef]
- Vigotsky, A.D.; Halperin, I.; Lehman, G.J.; Trajano, G.S.; Vieira, T.M. Interpreting signal amplitudes in surface electromyography studies in sport and rehabilitation sciences. Front. Physiol. 2018, 8, 985. [Google Scholar] [CrossRef]
- Merletti, R.; Farina, D. Surface Electromyography: Physiology, Engineering, and Applications; Merletti, R., Farina, D., Eds.; John Wiley & Sons, Inc.: Hoboken, NJ, USA, 2016; ISBN 9781119082934. [Google Scholar]
- Georgakis, A.; Stergioulas, L.K.; Giakas, G. Fatigue analysis of the surface EMG signal in isometric constant force contractions using the averaged instantaneous frequency. IEEE Trans. Biomed. Eng. 2003, 50, 262–265. [Google Scholar] [CrossRef]
- Rampichini, S.; Vieira, T.M.; Castiglioni, P.; Merati, G. Complexity Analysis of Surface Electromyography for Assessing the Myoelectric Manifestation of Muscle Fatigue: A Review. Entropy (Basel) 2020, 22, 529. [Google Scholar] [CrossRef]
- Cifrek, M.; Medved, V.; Tonković, S.; Ostojić, S. Surface EMG based muscle fatigue evaluation in biomechanics. Clin. Biomech. (Bristol, Avon) 2009, 24, 327–340. [Google Scholar] [CrossRef] [PubMed]
- Beretta-Piccoli, M.; Cescon, C.; Barbero, M.; Villiger, M.; Clijsen, R.; Kool, J.; Kesselring, J.; Bansi, J. Upper and lower limb performance fatigability in people with multiple sclerosis investigated through surface electromyography: A pilot study. Physiol. Meas. 2020, 41, 025002. [Google Scholar] [CrossRef] [PubMed]
- González-Izal, M.; Malanda, A.; Gorostiaga, E.; Izquierdo, M. Electromyographic models to assess muscle fatigue. J. Electromyogr. Kinesiol. 2012, 22, 501–512. [Google Scholar] [CrossRef] [PubMed]
- Mugnosso, M.; Zenzeri, J.; Hughes, C.M.L.; Marini, F. Coupling Robot-Aided Assessment and Surface Electromyography (sEMG) to Evaluate the Effect of Muscle Fatigue on Wrist Position Sense in the Flexion-Extension Plane. Front. Hum. Neurosci. 2019, 13, 396. [Google Scholar] [CrossRef]
- Hohenauer, E.; Cescon, C.; Deliens, T.; Clarys, P.; Clijsen, R. The effect of local skin cooling before a sustained, submaximal isometric contraction on fatigue and isometric quadriceps femoris performance: A randomized controlled trial. J. Therm. Biol. 2017, 65, 88–94. [Google Scholar] [CrossRef]
- Rojas, M.; Mañanas, M.A.; Müller, B.; Chaler, J. Activation of forearm muscles for wrist extension in patients affected by lateral epicondylitis. Annu. Int. Conf. IEEE Eng. Med. Biol. Soc. 2007, 2007, 4858–4861. [Google Scholar] [CrossRef]
- Lund, J.P.; Donga, R.; Widmer, C.G.; Stohler, C.S. The pain-adaptation model: A discussion of the relationship between chronic musculoskeletal pain and motor activity. Can. J. Physiol. Pharmacol. 1991, 69, 683–694. [Google Scholar] [CrossRef]
- Blanchette, M.-A.; Normand, M.C. Impairment assessment of lateral epicondylitis through electromyography and dynamometry. J. Can. Chiropr. Assoc. 2011, 55, 96. [Google Scholar]
- Wakabayashi, H.; Wijayanto, T.; Tochihara, Y. Neuromuscular function during knee extension exercise after cold water immersion. J. Physiol. Anthropol. 2017, 36, 28. [Google Scholar] [CrossRef]
- Mallette, M.M.; Green, L.A.; Gabriel, D.A.; Cheung, S.S. The effects of local forearm muscle cooling on motor unit properties. Eur. J. Appl. Physiol. 2018, 118, 401–410. [Google Scholar] [CrossRef]
- Krause, K.H.; Magyarosy, I.; Gall, H.; Ernst, E.; Pongratz, D.; Schoeps, P. Effects of heat and cold application on turns and amplitude in surface EMG. Electromyogr. Clin. Neurophysiol. 2001, 41, 67–70. [Google Scholar] [PubMed]
- Petrofsky, J.; Laymon, M. Muscle Temperature and EMG Amplitude and Frequency During Isometric Exercise. Aviat. Space Environ. Med. 2005, 76, 1024–1030. [Google Scholar] [PubMed]
- Tassignon, B.; Serrien, B.; de Pauw, K.; Baeyens, J.P.; Meeusen, R. Continuous knee cooling affects functional hop performance–A randomized controlled trial. J. Sport. Sci. Med. 2018, 17, 322–329. [Google Scholar]
- Anaya-Terroba, L.; Arroyo-Morales, M.; Fernández-de-las-Peñas, C.; Díaz-Rodríguez, L.; Cleland, J.A. Effects of ice massage on pressure pain thresholds and electromyography activity postexercise: A randomized controlled crossover study. J. Manip. Physiol. Ther. 2010, 33, 212–219. [Google Scholar] [CrossRef]
- Agostinucci, J.; McLinden, J.; Cherry, E. The effect of cryotherapy and exercise on lateral epicondylitis: A controlled randomised study. Int. J. Ther. Rehabil. 2012, 19, 641–650. [Google Scholar] [CrossRef]
- Heller, G.Z.; Manuguerra, M.; Chow, R. How to analyze the Visual Analogue Scale: Myths, truths and clinical relevance. Scand. J. Pain 2016, 13, 67–75. [Google Scholar] [CrossRef]
- Smidt, N.; Van der Windt, D.A.; Assendelft, W.J.; Mourits, A.J.; Devill, W.L.; De Winter, A.F.; Bouter, L.M. Interobserver reproducibility of the assessment of severity of complaints, grip strength, and pressure pain threshold in patients with lateral epicondylitis. Arch. Phys. Med. Rehabil. 2002, 83, 1145–1150. [Google Scholar] [CrossRef]
- Beretta-Piccoli, M.; Cescon, C.; Barbero, M.; D’Antona, G. Reliability of surface electromyography in estimating muscle fiber conduction velocity: A systematic review. J. Electromyogr. Kinesiol. 2019, 48, 53–68. [Google Scholar] [CrossRef]
- McManus, L.; De Vito, G.; Lowery, M.M. Analysis and Biophysics of Surface EMG for Physiotherapists and Kinesiologists: Toward a Common Language With Rehabilitation Engineers. Front. Neurol. 2020, 11, 576729. [Google Scholar] [CrossRef]
- Hermens, H.J.; Freriks, B.; Disselhorst-Klug, C.; Rau, G. Development of recommendations for SEMG sensors and sensor placement procedures. J. Electromyogr. Kinesiol. 2000, 10, 361–374. [Google Scholar] [CrossRef]
- Merletti, R.; Muceli, S. Tutorial. Surface EMG detection in space and time: Best practices. J. Electromyogr. Kinesiol. 2019, 49, 102363. [Google Scholar] [CrossRef] [PubMed]
- De Luca, C.J. The use of surface electromyography in biomechanics. J. Appl. Biomech. 1997, 13, 135–163. [Google Scholar] [CrossRef]
- Yu, S.Y.; Chen, S.; Yan, H.D.; Fan, C.Y. Effect of cryotherapy after elbow arthrolysis: A prospective, single-blinded, randomized controlled study. Arch. Phys. Med. Rehabil. 2015, 96, 1–6. [Google Scholar] [CrossRef]
- Pouedras, M.; Blancheton, A.; Agneray, H.; Crenn, V.; Bellemère, P. Effect of cryotherapy on pain and analgesic consumption after wrist or thumb surgery. Hand Surg. Rehabil. 2021, 40, 190–193. [Google Scholar] [CrossRef]
- Pawik, M.; Kowalska, J.; Rymaszewska, J. The effectiveness of whole-body cryotherapy and physical exercises on the psychological well-being of patients with multiple sclerosis: A comparative analysis. Adv. Clin. Exp. Med. 2019, 28, 1477–1483. [Google Scholar] [CrossRef] [PubMed]
- Kunkle, B.F.; Kothandaraman, V.; Goodloe, J.B.; Curry, E.J.; Friedman, R.J.; Li, X.; Eichinger, J.K. Orthopaedic Application of Cryotherapy: A Comprehensive Review of the History, Basic Science, Methods, and Clinical Effectiveness. JBJS Rev. 2021, 9, e20.00016. [Google Scholar] [CrossRef]
- Vulpiani, M.C.; Nusca, S.M.; Vetrano, M.; Ovidi, S.; Baldini, R.; Piermattei, C.; Ferretti, A.; Saraceni, V.M. Extracorporeal shock wave therapy vs cryoultrasound therapy in the treatment of chronic lateral epicondylitis. One year follow up study. Muscles Ligaments Tendons J. 2015, 5, 167. [Google Scholar] [CrossRef]
- Day, J.M.; Lucado, A.M.; Uhl, T.L. A comprehensive rehabilitation program for treating lateral elbow tendinopathy. Int. J. Sports Phys. Ther. 2019, 14, 818. [Google Scholar] [CrossRef]
- Huber, J.; Lisiński, P.; Polowczyk, A. Reinvestigation of the dysfunction in neck and shoulder girdle muscles as the reason of cervicogenic headache among office workers. Disabil. Rehabil. 2013, 35, 793–802. [Google Scholar] [CrossRef]
- Huber, J.; Kulczyk, A.; Lisinski, P.; Lipiec, J. The use of surface electromyography for diagnosis of muscle dysfunction with pain symptoms. Trends Sport Sci. 2013, 20, 135–139. [Google Scholar]
- Huber, J.; Torlińska, T.; Skoracka, J.; Witkowska, A.; Szukała, A.; Bryl, A.; Sprawności, Z.D.; Ruchowych, J.; Mięśniu, W.; Człowieka, Z.; et al. Daily fluctuation of healthy human muscle motor units activity in electromyographic examinations. Now. Lek. 2007, 76, 390–397. [Google Scholar]
- Colloca, C.J.; Keller, T.S. Electromyographic reflex responses to mechanical force, manually assisted spinal manipulative therapy. Spine 2001, 26, 1117–1124. [Google Scholar] [CrossRef] [PubMed]
- Staudenmann, D.; Roeleveld, K.; Stegeman, D.F.; van Dieen, J.H. Methodological aspects of SEMG recordings for force estimation--a tutorial and review. J. Electromyogr. Kinesiol. 2010, 20, 375–387. [Google Scholar] [CrossRef] [PubMed]
- Sanya, A.O.; Bello, A.O. Effects of cold application on isometric strength and endurance of quadriceps femoris muscle. Afr. J. Med. Med. Sci. 1999, 28, 195–198. [Google Scholar] [PubMed]
- Barnes, W.S.; Larson, M.R. Effects of localized hyper- and hypothermia on maximal isometric grip strength. Am. J. Phys. Med. 1985, 64, 305–314. [Google Scholar]
- Winkel, J.; Jørgensen, K. Significance of skin temperature changes in surface electromyography. Eur. J. Appl. Physiol. Occup. Physiol. 1991, 63, 345–348. [Google Scholar] [CrossRef]
- Bell, D.G. The influence of air temperature on the EMG/force relationship of the quadriceps. Eur. J. Appl. Physiol. Occup. Physiol. 1993, 67, 256–260. [Google Scholar] [CrossRef]
- Akehi, K.; Long, B.C.; Warren, A.J.; Goad, C.L. Ankle joint angle and lower leg musculotendinous unit responses to cryotherapy. J. Strength Cond. Res. 2016, 30, 2482–2492. [Google Scholar] [CrossRef]
- Petrofsky, J.S.; Lind, A.R. The influence of temperature on the amplitude and frequency components of the EMG during brief and sustained isometric contractions. Eur. J. Appl. Physiol. Occup. Physiol. 1980, 44, 189–200. [Google Scholar] [CrossRef]
- Drinkwater, E.J.; Behm, D.G. Effects of 22 degrees C muscle temperature on voluntary and evoked muscle properties during and after high-intensity exercise. Appl. Physiol. Nutr. Metab. 2007, 32, 1043–1051. [Google Scholar] [CrossRef]
- Garcia, L.M.; Soares, A.B.; Simieli, C.; Boratino, A.V.P.; de Jesus Guirro, R.R. On the effect of thermal agents in the response of the brachial biceps at different contraction levels. J. Electromyogr. Kinesiol. 2014, 24, 881–887. [Google Scholar] [CrossRef]
- Halder, A.; Gao, C.; Miller, M. Effects of Cooling on Ankle Muscle Strength, Electromyography, and Gait Ground Reaction Forces. J. Sport. Med. (Hindawi Publ. Corp.) 2014, 2014, 520124. [Google Scholar] [CrossRef] [PubMed]
- Bailey, D.M.; Erith, S.J.; Griffin, P.J.; Dowson, A.; Brewer, D.S.; Gant, N.; Williams, C. Influence of cold-water immersion on indices of muscle damage following prolonged intermittent shuttle running. J. Sports Sci. 2007, 25, 1163–1170. [Google Scholar] [CrossRef] [PubMed]
- Guilhem, G.; Hug, F.; Couturier, A.; Regnault, S.; Bournat, L.; Filliard, J.R.; Dorel, S. Effects of air-pulsed cryotherapy on neuromuscular recovery subsequent to exercise-induced muscle damage. Am. J. Sports Med. 2013, 41, 1942–1951. [Google Scholar] [CrossRef] [PubMed]
- Bigland-Ritchie, B.; Woods, J.J. Changes in muscle contractile properties and neural control during human muscular fatigue. Muscle Nerve 1984, 7, 691–699. [Google Scholar] [CrossRef] [PubMed]
- Cè, E.; Rampichini, S.; Agnello, L.; Limonta, E.; Veicsteinas, A.; Esposito, F. Combined effects of fatigue and temperature manipulation on skeletal muscle electrical and mechanical characteristics during isometric contraction. J. Electromyogr. Kinesiol. 2012, 22, 348–355. [Google Scholar] [CrossRef]
- Wakabayashi, H.; Oksa, J.; Tipton, M.J. Exercise performance in acute and chronic cold exposure. J. Phys. Fit. Sport. Med. 2015, 4, 177–185. [Google Scholar] [CrossRef]
- Racinais, S.; Oksa, J. Temperature and neuromuscular function. Scand. J. Med. Sci. Sports 2010, 20 (Suppl. 3), 1–18. [Google Scholar] [CrossRef]
- Radecka, A.; Pluta, W.; Lubkowska, A. Assessment of the Dynamics of Temperature Changes in the Knee Joint Area in Response to Selected Cooling Agents in Thermographic Tests. Int. J. Environ. Res. Public Health 2021, 18, 5326. [Google Scholar] [CrossRef]
- Severijns, D.; Zijdewind, I.; Dalgas, U.; Lamers, I.; Lismont, C.; Feys, P. The Assessment of Motor Fatigability in Persons With Multiple Sclerosis: A Systematic Review. Neurorehabil. Neural Repair 2017, 31, 413–431. [Google Scholar] [CrossRef]
- Pointon, M.; Duffield, R.; Cannon, J.; Marino, F.E. Cold application for neuromuscular recovery following intense lower-body exercise. Eur. J. Appl. Physiol. 2011, 111, 2977–2986. [Google Scholar] [CrossRef] [PubMed]
- Mucke, R.; Heuer, D. Behaviour of EMG-parameters and conduction velocity in contractions with different muscle temperatures. Biomed. Biochim. Acta 1989, 48, S459–S464. [Google Scholar] [PubMed]
- De Jong, R.H.; Hershey, W.N.; Wagman, I.H. Nerve conduction velocity during hypothermia in man. Anesthesiology 1966, 27, 805–810. [Google Scholar] [CrossRef] [PubMed]
- Bigland-Ritchie, B.; Donovan, E.F.; Roussos, C.S. Conduction velocity and EMG power spectrum changes in fatigue of sustained maximal efforts. J. Appl. Physiol. 1981, 51, 1300–1305. [Google Scholar] [CrossRef] [PubMed]
- Richards, J.; Gechev, A.; Alexander, J.; Macedo, L.; May, K.A.; Lindley, S.B. The Effect of Local Cooling at the Elbow on Nerve Conduction Velocity and Motor Unit Behaviour: An Exploration of a Novel Neurological Assessment. Sensors 2021, 21, 6703. [Google Scholar] [CrossRef]


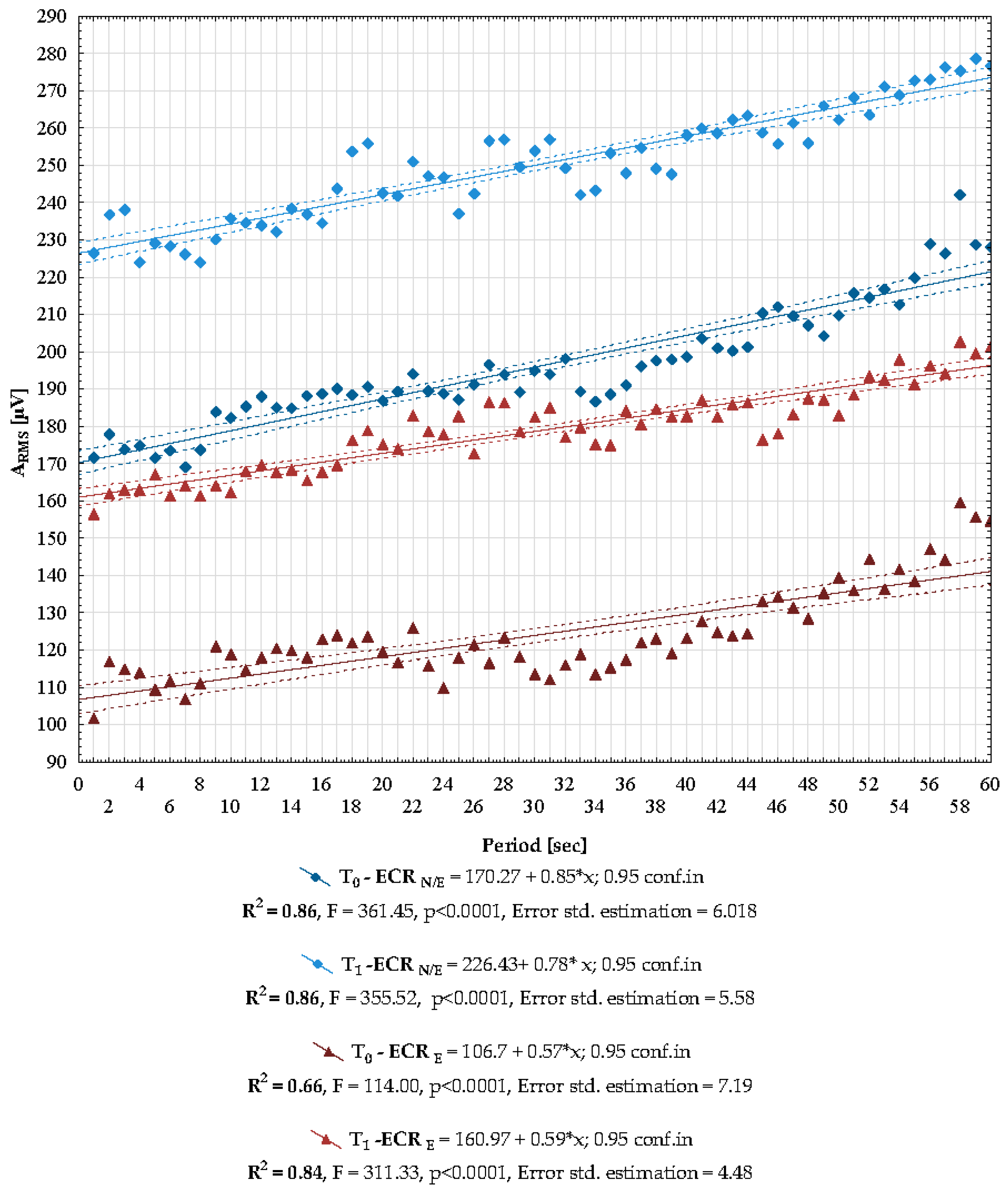
| Median (Min.–Max.) | T0 [µV] | T1 | Wilcoxon Test |
|---|---|---|---|
| ECR N/LE | 192.62 (169.07–242.17) | 250.33 (223.99–278.63) | Z = 6.735 p < 0.0001 |
| ECR E | 121.21 (101.73–159.56) | 179.27 (156.42–202.77) | Z = 6.165 p < 0.0001 |
| U Manna-Whitneya Test | Z = −9.261 p < 0.0001 | Z = −9.441 p < 0.0001 |
| Median (Min.–Max.) | T0 | T1 | Wilcoxon Test | |
|---|---|---|---|---|
| ECR N/E | 80.51818 (73.07–91.13) | 69.41932857 (64.32–79.31) | Z = 6.736 | p < 0.0001 |
| ECR E | 73.32914 (66.17–81.62) | 65.4 (59.47–74.46) | Z = 6.738 | p < 0.0001 |
| Mann–Whitney U Test | Z = 6.836 p < 0.0001 | Z = 5.393 p < 0.0001 | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Radecka, A.; Lubkowska, A. Direct Effect of Local Cryotherapy on Muscle Stimulation, Pain and Strength in Male Office Workers with Lateral Epicondylitis, Non-Randomized Clinical Trial Study. Healthcare 2022, 10, 879. https://doi.org/10.3390/healthcare10050879
Radecka A, Lubkowska A. Direct Effect of Local Cryotherapy on Muscle Stimulation, Pain and Strength in Male Office Workers with Lateral Epicondylitis, Non-Randomized Clinical Trial Study. Healthcare. 2022; 10(5):879. https://doi.org/10.3390/healthcare10050879
Chicago/Turabian StyleRadecka, Aleksandra, and Anna Lubkowska. 2022. "Direct Effect of Local Cryotherapy on Muscle Stimulation, Pain and Strength in Male Office Workers with Lateral Epicondylitis, Non-Randomized Clinical Trial Study" Healthcare 10, no. 5: 879. https://doi.org/10.3390/healthcare10050879
APA StyleRadecka, A., & Lubkowska, A. (2022). Direct Effect of Local Cryotherapy on Muscle Stimulation, Pain and Strength in Male Office Workers with Lateral Epicondylitis, Non-Randomized Clinical Trial Study. Healthcare, 10(5), 879. https://doi.org/10.3390/healthcare10050879







