Validation of the Portuguese Version of the Fertility Adjustment Scale
Abstract
:1. Introduction
2. Materials and Methods
3. Results
3.1. Sample Characteristics
3.2. Descriptive Statistics of FAS
3.3. Confirmatory Factor Analysis
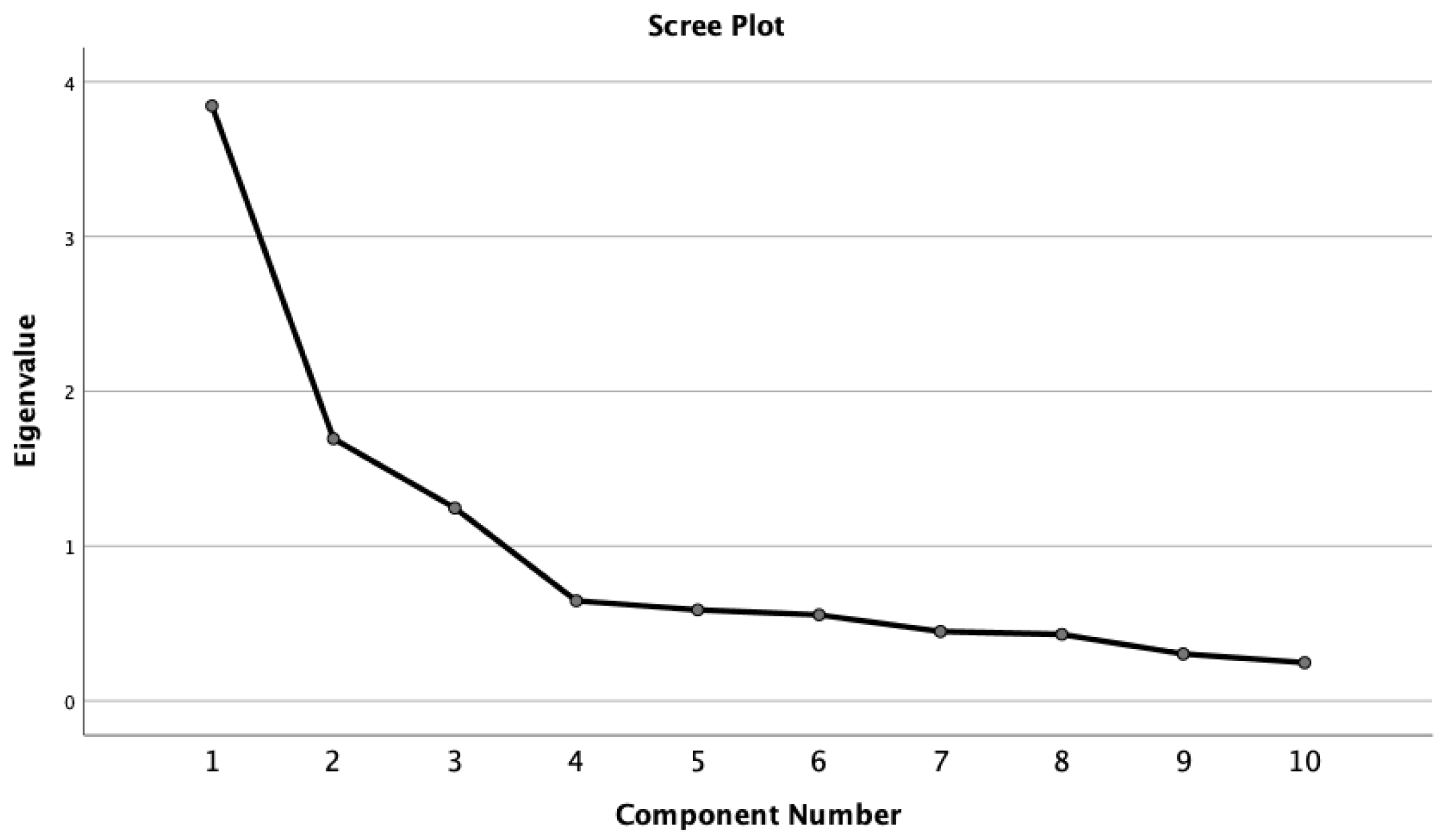
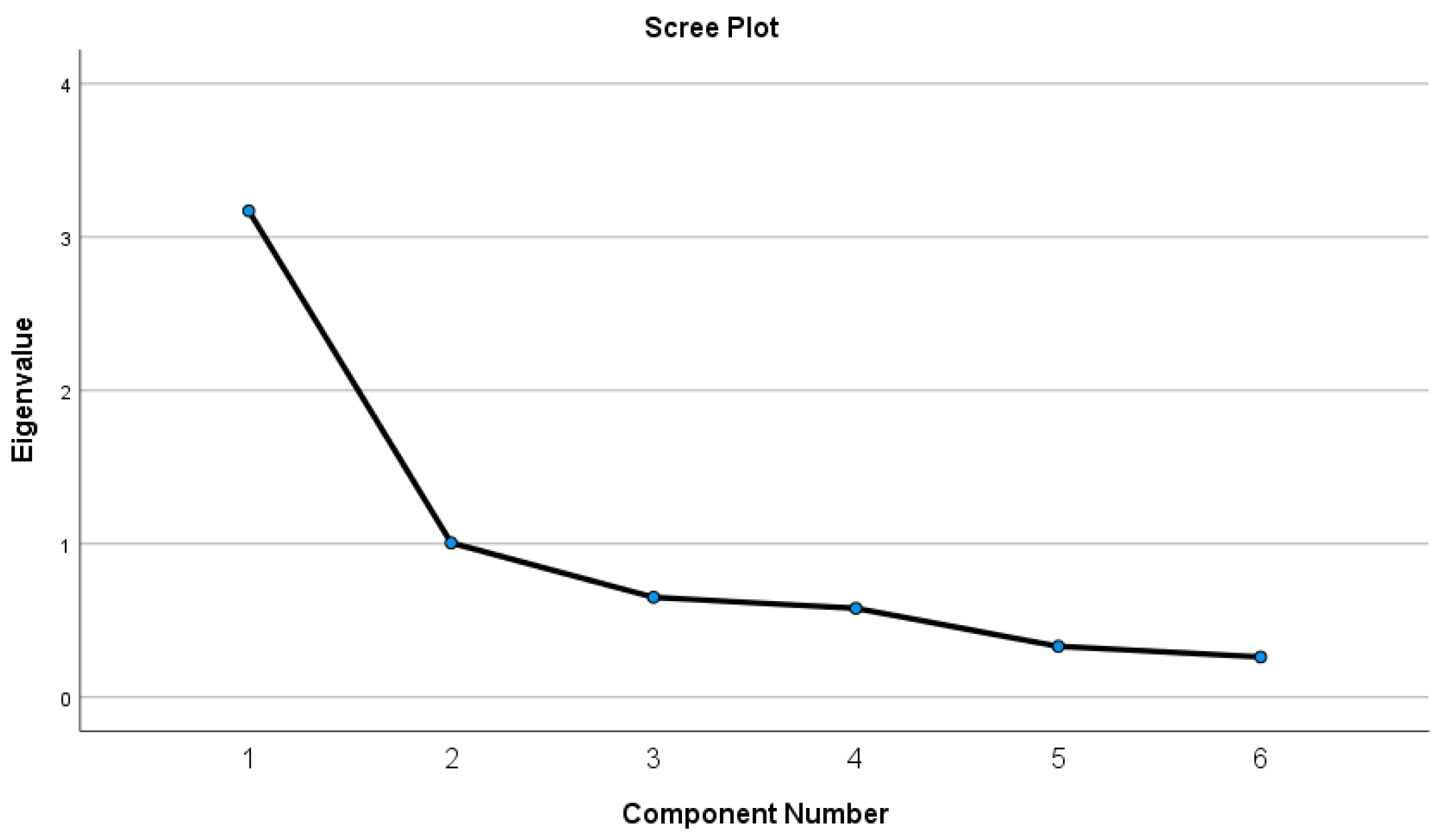
3.4. Exploratory Factor Analysis
3.5. Reliability and Validity
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Zegers-Hochschild, F.; Adamson, G.D.; Dyer, S.; Racowsky, C.; de Mouzon, J.; Sokol, R.; Rienzi, L.; Sunde, A.; Schmidt, L.; Cooke, I.D.; et al. The International Glossary on Infertility and Fertility Care, 2017. Fertil. Steril. 2017, 108, 393–406. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Romeiro, J.; Caldeira, S. The Human Responses and Nursing Diagnoses of Those Living With Infertility: A Qualitative Systematic Review. Int. J. Nurs. Knowl. 2018, 30, 173–189. [Google Scholar] [CrossRef] [PubMed]
- Greil, A.L.; Slauson-Blevins, K.; McQuillan, J. The Experience of Infertility: A Review of Recent Literature. Sociol. Health Illn. 2010, 32, 140–162. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Agostini, F.; Monti, F.; Andrei, F.; Paterlini, M.; Palomba, S.; La Sala, G.B. Assisted Reproductive Technology Treatments and Quality of Life: A Longitudinal Study among Subfertile Women and Men. J. Assist. Reprod. Genet. 2017, 34, 1307–1315. [Google Scholar] [CrossRef] [PubMed]
- Cabral, H.; Bucher-Maluschke, J. Development of Resilience Contribution in the Infertility Context: Review. Psicol. Saúde E. Doenças 2016, 17, 503–514. [Google Scholar] [CrossRef]
- Peters, K.; Jackson, D.; Rudge, T. Surviving the Adversity of Childlessness: Fostering Resilience in Couples. Contemp. Nurse 2011, 40, 130–140. [Google Scholar] [CrossRef] [PubMed]
- Glover, L.; Hunter, M.; Richards, J.M.; Katz, M.; Abel, P.D. Development of the Fertility Adjustment Scale. Fertil. Steril. 1999, 72, 623–628. [Google Scholar] [CrossRef]
- Chochovski, J.; Moss, S.A.; Charman, D.P. Recovery after Unsuccessful in Vitro Fertilization: The Complex Role of Resilience and Marital Relationships. J. Psychosom Obs. Gynaecol. 2013, 34, 122–128. [Google Scholar] [CrossRef]
- Gameiro, S.; van den Belt-Dusebout, A.W.; Smeenk, J.M.J.; Braat, D.D.M.; van Leeuwen, F.E.; Verhaak, C.M. Women’s Adjustment Trajectories during IVF and Impact on Mental Health 11–17 Years Later. Hum. Reprod. 2016, 31, 1788–1798. [Google Scholar] [CrossRef] [Green Version]
- Iordăchescu, D.A.; Paica, C.I.; Boca, A.E.; Gică, C.; Panaitescu, A.M.; Peltecu, G.; Veduță, A.; Gică, N. Anxiety, Difficulties, and Coping of Infertile Women. Healthcare 2021, 9, 466. [Google Scholar] [CrossRef]
- Gameiro, S.; Boivin, J.; Peronace, L.; Verhaak, C.M. Why Do Patients Discontinue Fertility Treatment? A Systematic Review of Reasons and Predictors of Discontinuation in Fertility Treatment. Hum. Reprod. Update 2012, 18, 652–669. [Google Scholar] [CrossRef] [PubMed]
- Boivin, J.; Gameiro, S. Evolution of Psychology and Counseling in Infertility. Fertil. Steril. 2015, 104, 251–259. [Google Scholar] [CrossRef] [PubMed]
- Gameiro, S.; Verhaak, C.M.; Kremer, J.A.; Boivin, J. Why We Should Talk about Compliance with Assisted Reproductive Technologies (ART): A Systematic Review and Meta-Analysis of ART Compliance Rates. Hum. Reprod. Update 2013, 19, 124–135. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zurlo, M.C.; Cattaneo Della Volta, M.F.; Vallone, F. Predictors of Quality of Life and Psychological Health in Infertile Couples: The Moderating Role of Duration of Infertility. Qual. Life Res. 2018, 27, 945–954. [Google Scholar] [CrossRef] [PubMed]
- Tiyuri, A.; Vagharseyyedin, S.A.; Torshizi, M.; Bahramian, N.; Hajihosseini, M. The Persian Version of Fertility Adjustment Scale: Psychometric Properties. Int. J. Fertil. Steril. 2018, 12, 130–135. [Google Scholar] [CrossRef] [PubMed]
- Torabi, M.; Kazemi, A.; Abdishahshahani, M. Psychometric Properties of Revised Version of the Fertility Adjustment Scale in Infertile Couples Undergoing Assisted Reproductive Technology. Eur. J. Obstet. Gynecol. Reprod. Biol. 2019, 243, 16–20. [Google Scholar] [CrossRef] [PubMed]
- Lopes, V.; Leal, I. Avaliação em Sexualidade e Parentalidade—Escala de Ajustamento à Fertilidade (EAF); Isabel Leal e João Maroco; LivPsic: Porto, Portugal, 2010; ISBN 978-989-8148-32-2. [Google Scholar]
- Lopes, V.M.S. Personalidade e Ajustamento Emocional na Infertilidade. Master’s Thesis, Instituto Superior de Psicologia Aplicada, Lisboa, Portugal, 2008. [Google Scholar]
- IBM. SPSS Version 26.0. Available online: https://www.ibm.com/us-en/ (accessed on 9 August 2020).
- Pestana, M.H.; Gageiro, J.N. Análise de Dados Para Ciências Sociais: A Complementariedade do SPSS; Sílabo: Lisboa, Portugal, 2003; ISBN 978-972-618-297-9. [Google Scholar]
- Nunnally, J.C.; Bernstein, I.H. The Assessment of Reliability. In Psychometric Theory; McGraw-Hill: New York, NY, USA, 1994; Volume 3, pp. 248–292. ISBN 978-0-07-047849-7. [Google Scholar]
- Hair, J.F.; Black, W.C.; Babin, B.J.; Anderson, R.E. Multivariate Data Analysis; Prentice Hall: Ithaca, NY, USA, 2010; ISBN 978-0-13-813263-7. [Google Scholar]
- Tabachnick, B.G.; Fidell, L.S. Using Multivariate Statistics, 5th ed.; Allyn & Bacon/Pearson Education: Boston, MA, USA, 2007; ISBN 978-0-205-45938-4. [Google Scholar]
- Awang, Z. The second order Confirmatory Factor Analysis. In A Handbook on SEM; MPWS Universiti Sultan Zainal Abidin: Penang, Malaysa, 2012; pp. 163–181. [Google Scholar]
- Hooper, D.; Coughlan, J.; Mullen, M. Structural Equation Modelling: Guidelines for Determining Model Fit. Electron. J. Bus. Res. Methods 2008, 6, 53–60. [Google Scholar] [CrossRef]
- Hu, L.; Bentler, P.M. Fit Indices in Covariance Structure Modeling: Sensitivity to Underparameterized Model Misspecification. Psychol. Methods 1998, 3, 424–453. [Google Scholar] [CrossRef]
- Hayton, J.C.; Allen, D.G.; Scarpello, V. Factor Retention Decisions in Exploratory Factor Analysis: A Tutorial on Parallel Analysis. Organ. Res. Methods 2004, 7, 191–205. [Google Scholar] [CrossRef]
- de Carvalho Ng Deep, C.A.F.; Pereira, I. Adaptação Da “The Resilience Scale” Para a População Adulta Portuguesa. Psicol. USP 2012, 23, 417–433. [Google Scholar] [CrossRef] [Green Version]
- Gomez, R.; Fisher, J.W. Domains of Spiritual Well-Being and Development and Validation of the Spiritual Well-Being Questionnaire. Personal. Individ. Differ. 2003, 35, 1975–1991. [Google Scholar] [CrossRef] [Green Version]
- Yong, A.G.; Pearce, S. A Beginners Guide to Factor Analysis: Focusing on Exploratory Factor Analysis. Tutor. Quant. Methods Psychol. 2013, 9, 79–94. [Google Scholar] [CrossRef]
- Nagórska, M.; Bartosiewicz, A.; Obrzut, B.; Darmochwał-Kolarz, D. Gender Differences in the Experience of Infertility Concerning Polish Couples: Preliminary Research. Int. J. Environ. Res. Public Health 2019, 16, 2337. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Moura-Ramos, M.; Gameiro, S.; Canavarro, M.C.; Soares, I.; Almeida-Santos, T. Does Infertility History Affect the Emotional Adjustment of Couples Undergoing Assisted Reproduction? The Mediating Role of the Importance of Parenthood. Br. J. Health Psychol. 2016, 21, 302–317. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Verhaak, C.M.; Smeenk, J.M.J.; Evers, A.W.M.; Kremer, J.A.; Kraaimaat, F.W.; Braat, D.D.M. Women’s Emotional Adjustment to IVF: A Systematic Review of 25 Years of Research. Hum. Reprod. Update 2007, 13, 27–36. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sathian, B.; Asim, M.; Banerjee, I.; Pizarro, A.B.; Roy, B.; van Teijlingen, E.R.; do Nascimento, I.J.B.; Alhamad, H.K. Impact of COVID-19 on Clinical Trials and Clinical Research: A Systematic Review. Nepal. J. Epidemiol. 2020, 10, 878–887. [Google Scholar] [CrossRef] [PubMed]
- Alviggi, C.; Esteves, S.C.; Orvieto, R.; Conforti, A.; La Marca, A.; Fischer, R.; Andersen, C.Y.; Bühler, K.; Sunkara, S.K.; Polyzos, N.P.; et al. COVID-19 and Assisted Reproductive Technology Services: Repercussions for Patients and Proposal for Individualized Clinical Management. Reprod. Biol. Endocrinol. 2020, 18, 45. [Google Scholar] [CrossRef] [PubMed]
| Variable | FAS | |||
|---|---|---|---|---|
| Response Mean (SD) | p | Total Mean (SD) | ||
| Social—Demographic | ||||
| Gender | 0.080 a | |||
| Female | 3.94 (0.71) | 39.49 (7.10) | ||
| Male | 3.90 (0.00) | 39.00 (0.00) | ||
| Age | 0.902 b | |||
| ≤34 | 4.05 (0.71) | 40.53 (7.13) | ||
| 35–40 | 4.01 (0.62) | 40.17 (6.26) | ||
| 41–51 | 3.30 (0.66) | 33.09 (6.65) | ||
| ≥52 | 3.00 (0.00) | 30.00 (0.00) | ||
| Marital Status | 0.768 b | |||
| Married | 4.00 (0.71) | 40.06 (7.11) | ||
| Together | 3.89 (0.56) | 38.97 (7.21) | ||
| Divorced/Separated | 3.73 (0.45) | 36.33 (5.68) | ||
| Single | 3.73 (0.45) | 37.33 (4.50) | ||
| Current relationship (years) | 0.890 b | |||
| ≤3 | 3.98 (0.62) | 39.88 (6.26) | ||
| 4–6 | 4.04 (0.65) | 40.44 (6.50) | ||
| 7–9 | 4.05 (0.75) | 40.53 (7.57) | ||
| ≥10 | 3.75 (0.73) | 37.58 (7.37) | ||
| Education level | 0.956 b | |||
| Middle school | 3.90 (0.00) | 39.00 (0.00) | ||
| High school | 3.98 (0.67) | 39.80 (6.74) | ||
| Professional course | 4.15 (0.79) | 41.55 (7.90) | ||
| Bachelor/Graduation | 3.92 (0.72) | 39.25 (7.23) | ||
| Master’s | 3.95 (0.65) | 39.52 (6.50) | ||
| Ph.D. | 3.40 (0.96) | 34.00 (9.64) | ||
| Employment status | 0.353 b | |||
| Employed | 3.96 (0.70) | 39.61 (7.03) | ||
| Unemployed | 3.96 (0.60) | 39.63 (6.02) | ||
| Student | 3.25 (1.34) | 32.50 (13.43) | ||
| Occupation | 0.574 b | |||
| Representatives of the legislative branch of executive bodies, officers, directors, and executive managers | 3.74 (0.83) | 37.40 (8.38) | ||
| Experts from intellectual and scientific activities | 4.09 (0.67) | 40.94 (6.79) | ||
| Intermediate-level technicians and professions | 4.07 (0.33) | 40.75 (3.30) | ||
| Administrative staff | 3.86 (0.61) | 38.64 (6.18) | ||
| Personal service, security, and safety workers and salespeople | 3.92 (0.80) | 39.22 (8.02) | ||
| Skilled workers in industry, construction, and craftsmen | 2.90 (0.00) | 29.00 (0.00) | ||
| Plant and machine operators | 4.90 (0.00) | 49.00 (0.00) | ||
| Spirituality—Religion | ||||
| Spiritual person | 0.490 a | |||
| No | 4.01 (0.64) | 40.16 (6.40) | ||
| Yes | 3.92 (0.72) | 39.26 (7.24) | ||
| Spiritual importance | 0.745 b | |||
| Not important | 4.03 (0.59) | 40.36 (5.98) | ||
| Little importance | 3.83 (0.72) | 38.39 (7.22) | ||
| Important | 3.94 (0.70) | 39.47 (7.05) | ||
| Very important | 4.17 (0.84) | 41.71 (8.45) | ||
| Spiritual change with diagnosis | 0.501 b | |||
| No change | 4.03 (0.70) | 40.34 (7.07) | ||
| Less important | 3.72 (0.82) | 37.29 (8.29) | ||
| More important | 3.92 (0.62) | 39.25 (6.21) | ||
| Spiritual change with treatment | 0.360 b | |||
| No change | 3.94 (0.75) | 39.49 (7.57) | ||
| Less important | 3.80 (0.80) | 38.00 (8.00) | ||
| More important | 4.00 (0.57) | 40.08 (5.77) | ||
| Religious person | 0.181 a | |||
| No | 3.78 (0.59) | 37.82 (5.92) | ||
| Yes | 4.02 (0.74) | 40.28 (7.41) | ||
| Religion importance | 0.745 b | |||
| Not important | 4.03 (0.59) | 40.36 (5.98) | ||
| Little importance | 3.83 (0.72) | 38.39 (7.22) | ||
| Important | 3.94 (0.70) | 39.47 (7.05) | ||
| Very important | 4.17 (0.84) | 41.71 (8.45) | ||
| Religion changes with diagnosis | 0.372 b | |||
| No change | 4.04 (0.71) | 40.42 (7.12) | ||
| Less important | 3.82 (0.75) | 38.28 (7.56) | ||
| More important | 3.90 (0.62) | 39.00 (6.27) | ||
| Religion changes with treatment | 0.066 b | |||
| No change | 3.98 (0.79) | 39.85 (7.91) | ||
| Less important | 3.90 (0.75) | 39.08 (7.59) | ||
| More important | 3.92 (0.52) | 39.21 (5.20) | ||
| Clinical—Infertility | ||||
| Type | 0.979 a | |||
| Primary | 3.99 (0.68) | 39.95 (6.84) | ||
| Secondary | 3.64 (0.77) | 36.42 (7.71) | ||
| Nature | 0.179 b | |||
| Never been pregnant | 4.02 (7.59) | 40.22 (7.59) | ||
| Natural pregnancy without live birth | 3.76 (0.57) | 37.66 (5.78)) | ||
| Natural pregnancy, had child, not able to have another child | 3.83 (0.70) | 38.33 (7.01) | ||
| Pregnancy with treatment, did not have a child | 4.17 (0.36) | 41.78 (3.62) | ||
| Pregnancy with treatment, had child, not able to have another child | 3.30 (0.84) | 33.00 (8.48) | ||
| Cause | 0.038 b | |||
| Female | 3.75 (0.83) | 37.52 (8.30) | ||
| Male | 4.11 (0.42) | 41.13 (4.20) | ||
| Mixed | 4.13 (0.71) | 41.38 (7.11) | ||
| Unknown | 3.98 (0.58) | 39.83 (5.82) | ||
| Waiting diagnosis | 4.17 (0.38) | 41.77 (3.86) | ||
| Diagnosis (years) | 0.052 b | |||
| ≤3 | 3.94 (0.62) | 39.40 (6.22) | ||
| 4–6 | 3.98 (0.78) | 39.80 (8.93) | ||
| 7–9 | 3.97 (0.89) | 39.70 (8.93) | ||
| ≥10 | 3.97 (1.01) | 39.71 (10.14) | ||
| Consultation (years) | 0.031 b | |||
| ≤3 | 3.95 (0.62) | 39.55 (6.24) | ||
| 4–6 | 3.85 (0.87) | 38.57 (8.73) | ||
| 7–9 | 4.21 (0.76) | 42.10 (7.68) | ||
| ≥10 | 3.66 (1.20) | 36.60 (12.03) | ||
| Treatments | ||||
| Previous treatments | 0.948 a | |||
| No | 4.01 (0.71) | 40.12 (7.11) | ||
| Yes | 3.89 (0.69) | 38.94 (6.98) | ||
| Time in current treatment (months) | ||||
| ≤3 | 3.66 (0.23) | 36.66 (2.30) | ||
| 4–6 | 3.87 (0.51) | 38.75 (5.12) | ||
| 7–12 | 3.79 (0.71) | 37.93 (7.19) | ||
| 13–24 | 4.19 (0.73) | 41.92 (7.33) | ||
| 24–36 | 3.76 (0.55) | 37.60 (5.50) | ||
| ≥37 | 3.84 (0.78) | 38.43 (7.89) | ||
| Current treatment | 0.228 b | |||
| Previous tests | 3.93 (0.82) | 39.30 (8.26) | ||
| Waiting to start | 4.04 (0.61) | 40.48 (6.13) | ||
| In cycle | 3.97 (0.61) | 39.78 (6.18) | ||
| OI | 3.90 (0.00) | 0.839 b | 39.00 (0.00) | |
| IUI | 4.10 (0.42) | 41.00 (4.24) | ||
| IVF | 3.81 (0.70) | 38.10 (7.06) | ||
| ICSI | 4.22 (0.65) | 42.25 (6.50) | ||
| Other | 4.25 (0.49) | 42.50 (4.94) | ||
| Tests after cycle | 3.62 (0.84) | 39.48 (7.03) | ||
| Item | Mean | 95% CI | SD | Skewness | Std. Error | Kurtosis | Std. Error | Cronbach Alpha (without Item) |
|---|---|---|---|---|---|---|---|---|
| 1. | 4.50 | 4.19–4.82 | 1.61 | −0.913 | 0.237 | −0.299 | 0.469 | (0.400) |
| 2. | 3.35 | 3.00–3.70 | 1.76 | −0.015 | 0.237 | −1.336 | 0.469 | (0.440) |
| 3. | 4.61 | 4.27–4.94 | 1.66 | −1.038 | 0.237 | −0.180 | 0.469 | (0.403) |
| 4. | 3.62 | 3.32–3.94 | 1.62 | −0.266 | 0.237 | −1.065 | 0.469 | (0.517) |
| 5. | 3.94 | 3.62–4.26 | 1.60 | −0.329 | 0.237 | −0.962 | 0.469 | (0.400) |
| 6. | 4.33 | 3.99–4.65 | 1.69 | −0.685 | 0.237 | −0.746 | 0.469 | (0.429) |
| 7. | 3.42 | 3.10–3.75 | 1.61 | −0.028 | 0.237 | −1.135 | 0.469 | (0.558) |
| 8. | 4.33 | 4.03–4.58 | 1.42 | −0.701 | 0.237 | −0.256 | 0.469 | (0.521) |
| 9. | 3.86 | 3.54–4.22 | 1.73 | −0.329 | 0.237 | −1.198 | 0.469 | (0.480) |
| 10. | 3.54 | 3.22–3.86 | 1.65 | −0.030 | 0.237 | −1.113 | 0.469 | (0.569) |
| Total | 39.48 | 38.20–40.91 | 7.03 | −0.275 | 0.237 | 0.183 | 0.469 | 0.505 |
| Models | χ | df | χ/df | p | RMSEA (90%CI) | CFI | TLI | NFI |
|---|---|---|---|---|---|---|---|---|
| 10-item 3-factor [17,18] | 84.608 | 32 | 2.644 | 0.000 | 0.126 (0.094–0.159) | 0.844 | 0.780 | 0.778 |
| 6-item 2-factor | 28.402 | 8 | 3.550 | 0.000 | 0.157 (0.097–0.222) | 0.906 | 0.824 | 0.878 |
| 6-item 1-factor | 40.594 | 9 | 4.510 | 0.000 | 0.185 (0.129–0.244) | 0.855 | 0.758 | 0.826 |
| Components Extraction Based on K1 Criterion and Percentage (%) of Variance | ||||||
|---|---|---|---|---|---|---|
| Component | Three-Factor (10 Items) | Two-Factor (6 Items) | ||||
| Total | % Variance | Cumulative % | Total | % Variance | Cumulative % | |
| 1 | 3.844 | 38.444 | 38.444 | 3.170 | 52.840 | 52.840 |
| 2 | 1.694 | 16.939 | 55.383 | 1.006 | 16.762 | 69.602 |
| 3 | 1.246 | 12.460 | 67.843 | |||
| Varimax Rotation Factor Loading | |||||
|---|---|---|---|---|---|
| Three-Factor (10 Items) | Two-Factor (6 Items) | ||||
| Components | 1 | 2 | 3 | 1 | 2 |
| 1 | 0.84 | 0.80 | |||
| 2 | 0.81 | 0.83 | |||
| 3 | 0.78 | 0.77 | |||
| 4 | 0.74 | ||||
| 5 | 0.75 | 0.82 | |||
| 6 | 0.57 | 0.66 | |||
| 7 | 0.75 | ||||
| 8 | 0.64 | ||||
| 9 | 0.68 | 0.81 | |||
| 10 | 0.74 | ||||
| Communalities | |||
|---|---|---|---|
| Variables | 10-Item | 6-Item 2-Factor | |
| Initial | Extraction | Extraction | |
| 1. | 1.000 | 0.73 | 0.68 |
| 2. | 1.000 | 0.68 | 0.71 |
| 3. | 1.000 | 0.74 | 0.73 |
| 4. | 1.000 | 0.61 | |
| 5. | 1.000 | 0.69 | 0.74 |
| 6. | 1.000 | 0.64 | 0.63 |
| 7. | 1.000 | 0.63 | |
| 8. | 1.000 | 0.80 | |
| 9. | 1.000 | 0.60 | 0.67 |
| 10. | 1.000 | 0.63 | |
| Factor | Skewness | Kurtosis | ||||
|---|---|---|---|---|---|---|
| Total Mean | SD | Statistic | SD | Statistic | Std. Error | |
| 1 | 3.64 | 1.45 | −0.196 | 0.237 | −0.861 | 0.469 |
| 2 | 4.32 | 1.35 | −0.812 | 0.237 | −0.067 | 0.469 |
| Discriminant Validity of the Reconfigured FAS Factors | ||||||
|---|---|---|---|---|---|---|
| FAS Total | FAS—Factor 1 Centrality of Parenting | FAS—Factor 2 Suspended Life | ||||
| r | p | r | p | r | p | |
| SWBQp variables | −0.128 | 0.197 | −0.022 | 0.823 | −0.278 ** | 0.004 |
| Personal | −0.248 * | 0.011 | −0.121 | 0.220 | −0.397 ** | 0.000 |
| Communal | −0.027 | 0.785 | 0.059 | 0.554 | −0.177 | 0.072 |
| Environmental | −0.170 | 0.084 | −0.123 | 0.214 | 0.198 * | 0.044 |
| Transcendental | 0.002 | 0.982 | 0.095 | 0.339 | −0.170 | 0.084 |
| RS variables | −0.239 * | 0.015 | −0.057 | 0.568 | −0.336 ** | 0.000 |
| Perseverance | −0.139 | 0.159 | −0.134 | 0.176 | −0.243 * | 0.013 |
| Meaning of life | −0.229 * | 0.020 | −0.163 | 0.099 | −0.324 ** | 0.001 |
| Serenity | −0.265 ** | 0.006 | −0.184 | 0.061 | −0.362 ** | 0.000 |
| Self-reliance and self-confidence | −0.252 ** | 0.010 | −0.141 | 0.153 | −0.290 ** | 0.003 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Romeiro, J.; Nogueira, P.; Caldeira, S. Validation of the Portuguese Version of the Fertility Adjustment Scale. Healthcare 2022, 10, 563. https://doi.org/10.3390/healthcare10030563
Romeiro J, Nogueira P, Caldeira S. Validation of the Portuguese Version of the Fertility Adjustment Scale. Healthcare. 2022; 10(3):563. https://doi.org/10.3390/healthcare10030563
Chicago/Turabian StyleRomeiro, Joana, Paulo Nogueira, and Sílvia Caldeira. 2022. "Validation of the Portuguese Version of the Fertility Adjustment Scale" Healthcare 10, no. 3: 563. https://doi.org/10.3390/healthcare10030563
APA StyleRomeiro, J., Nogueira, P., & Caldeira, S. (2022). Validation of the Portuguese Version of the Fertility Adjustment Scale. Healthcare, 10(3), 563. https://doi.org/10.3390/healthcare10030563








