Sasang Constitution Type Combined with General Obesity May Act as a Risk Factor for Prediabetes Mellitus
Abstract
1. Introduction
2. Materials and Methods
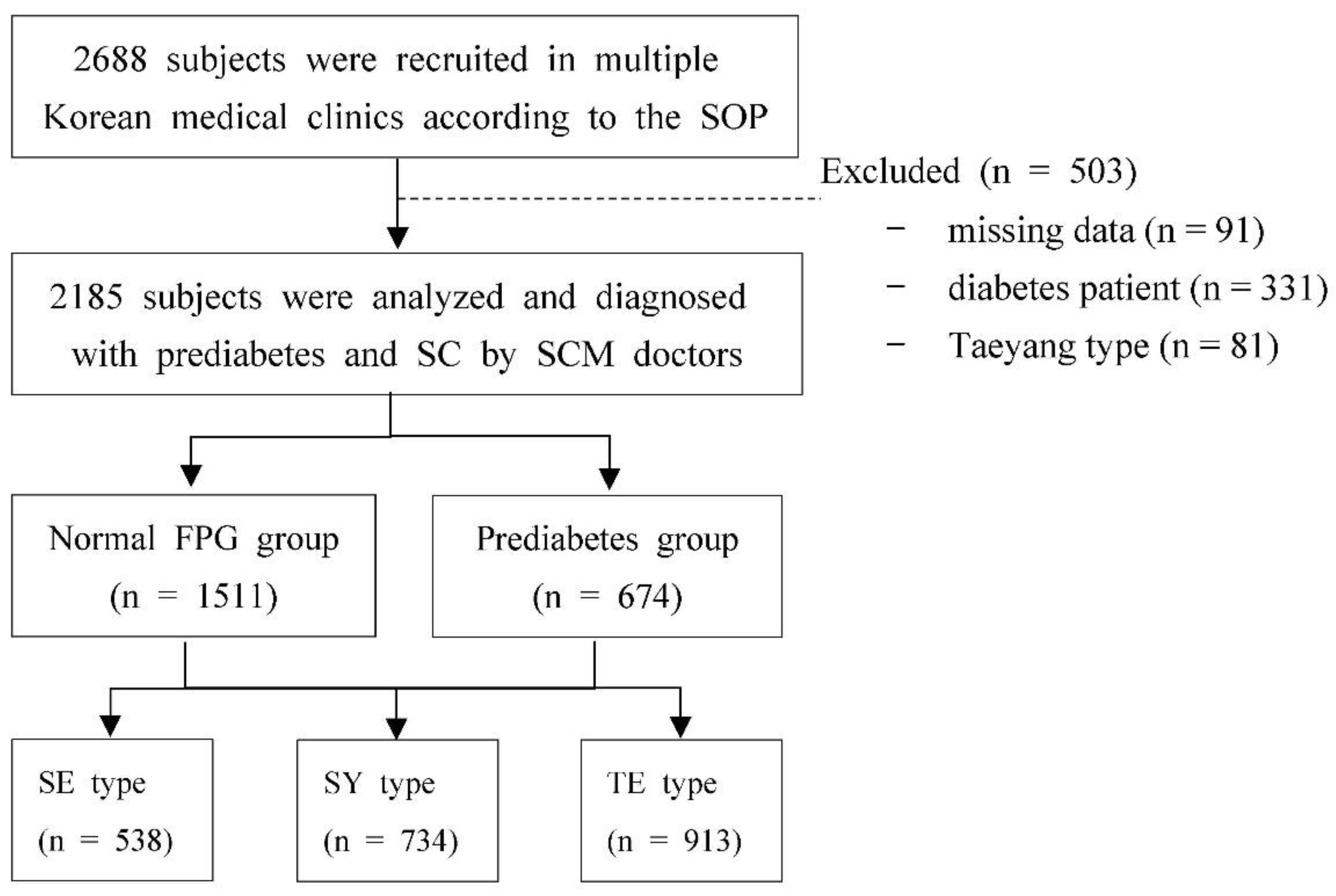
2.1. Data Source and Subjects
2.2. Diagnostic Criteria
2.2.1. Introduction to the Sasang Constitution
2.2.2. Diagnosis of SC
2.2.3. Pre-DM
2.2.4. General Obesity
2.3. Statistical Analysis
3. Results
3.1. Differences in General Characteristics
3.2. FPG Values According to Sasang Constitution and Obesity Status
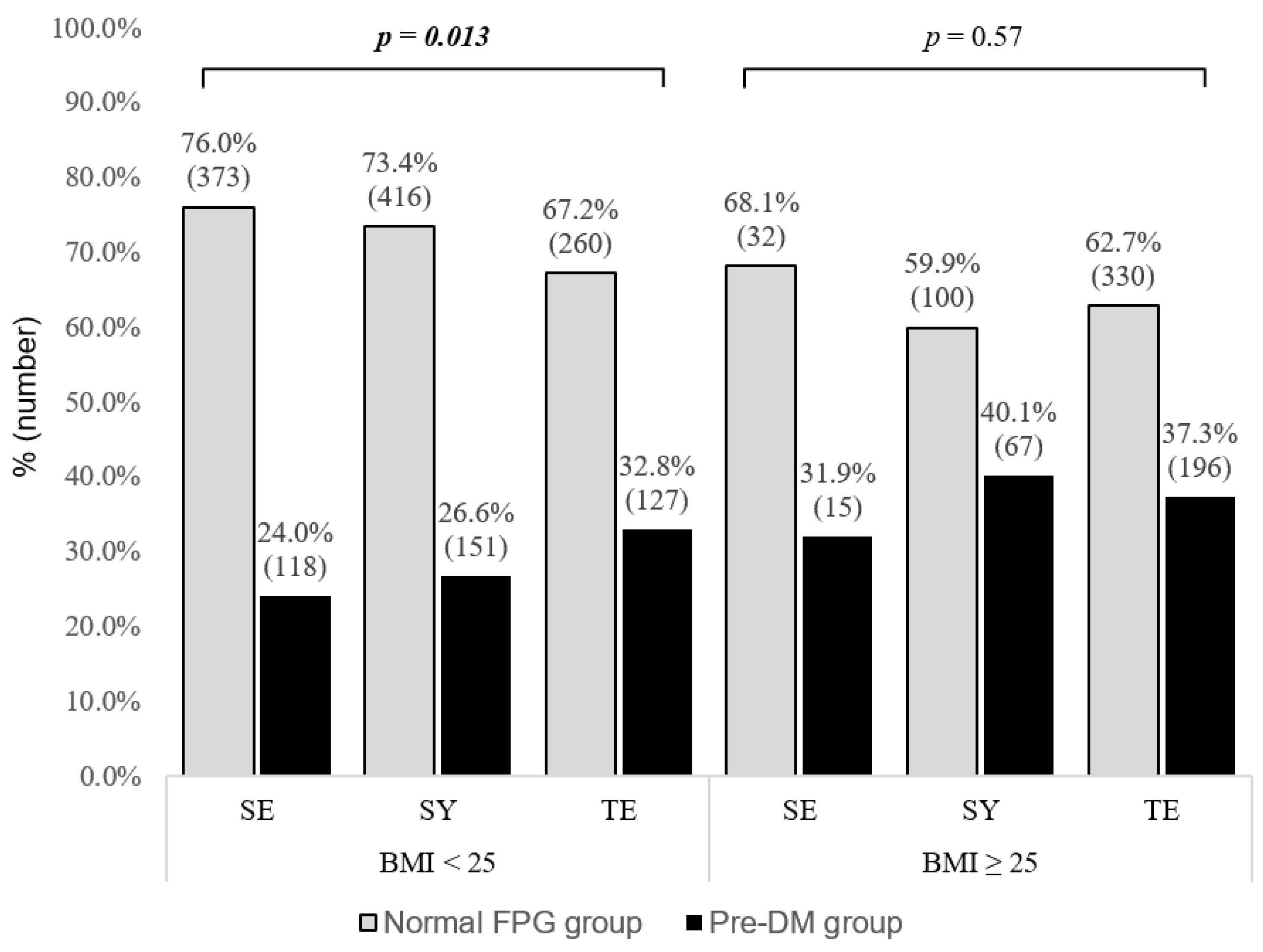
3.3. Proportion of Normal and Prediabetic Individuals by SC Type in Stratified BMI Groups
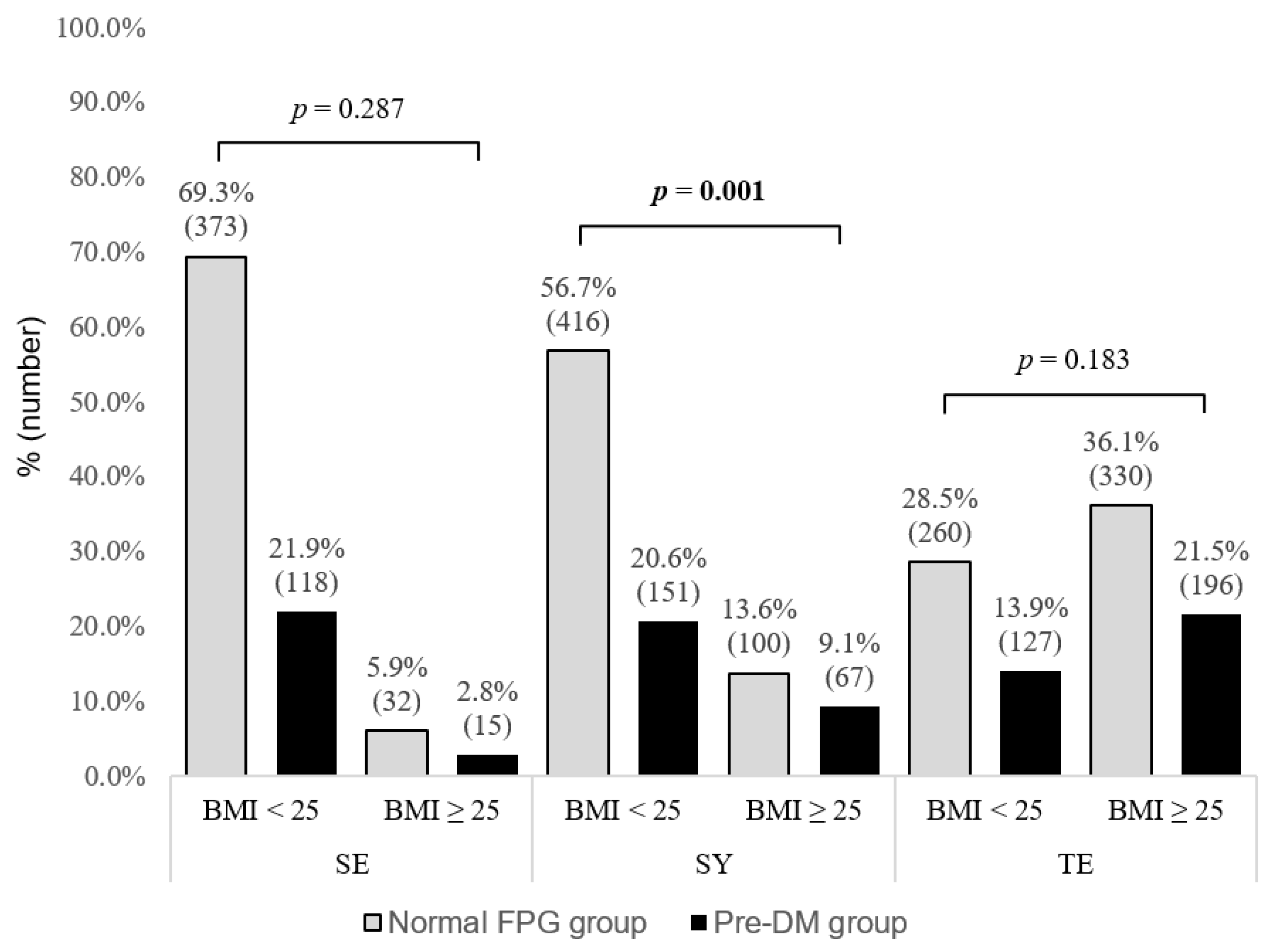
3.4. Proportion of Normal and Prediabetic Individuals Stratified by BMI in Each SC Type Group
3.5. Adjusted ORs of the Obese Group for Pre-DM Compared with the Normal BMI Group among Individuals with SE, SY and TE Types
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Hostalek, U. Global epidemiology of prediabetes—Present and future perspectives. Clin. Diabetes Endocrinol. 2019, 5, 5. [Google Scholar] [CrossRef] [PubMed]
- American Diabetes Association. Classification and diagnosis of diabetes. Diabetes Care 2017, 40 (Suppl. 1), S11–S24. [Google Scholar] [CrossRef] [PubMed]
- Brannick, B.; Wynn, A.; Dagogo-Jack, S. Prediabetes as a toxic environment for the initiation of microvascular and macrovascular complications. Exp. Biol. Med. 2016, 241, 1323–1331. [Google Scholar] [CrossRef] [PubMed]
- Abraham, T.M.; Fox, C.S. Implications of Rising Prediabetes Prevalence. Diabetes Care 2013, 36, 2139–2141. [Google Scholar] [CrossRef]
- Cai, L.; Li, X.; Cui, W.; You, D.; Golden, A.R. Trends in diabetes and pre-diabetes prevalence and diabetes awareness, treatment and control across socioeconomic gradients in rural southwest China. J. Public Health 2018, 40, 375–380. [Google Scholar] [CrossRef]
- Cullmann, M.; Hilding, A.; Östenson, C.G. Alcohol consumption and risk of pre-diabetes and type 2 diabetes development in a Swedish population. Diabet. Med. 2012, 29, 441–452. [Google Scholar] [CrossRef]
- Eriksson, A.K.; Ekbom, A.; Granath, F.; Hilding, A.; Efendic, S.; Östenson, C.G. Psychological distress and risk of pre-diabetes and Type 2 diabetes in a prospective study of Swedish middle-aged men and women. Diabet. Med. 2008, 25, 834–842. [Google Scholar] [CrossRef]
- American Diabetes Association. Economic costs of diabetes in the US in 2002. Diabetes Care 2003, 26, 917–932. [Google Scholar] [CrossRef]
- American Diabetes Association. Screening for type 2 diabetes. Diabetes Care 2004, 27 (Suppl. 1), S11–S14. [Google Scholar] [CrossRef]
- American Diabetes Association. Standards of Medical Care in Diabetes-2008. Diabetes Care 2008, 31, S12–S54. [Google Scholar] [CrossRef]
- Haffner, S.M. Epidemiology of type 2 diabetes: Risk factors. Diabetes Care 1998, 21, C3–C6. [Google Scholar] [CrossRef] [PubMed]
- Kopelman, P.G. Obesity as a medical problem. Nature 2000, 404, 635–643. [Google Scholar] [CrossRef] [PubMed]
- Boles, A.; Kandimalla, R.; Reddy, P.H. Dynamics of diabetes and obesity: Epidemiological perspective. Biochim. Biophys. Acta. 2017, 1863, 1026–1036. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.M. Longevity and Life Preservation in Oriental Medicine (東醫壽世保元); Kyung Hee University Press: Seoul, Republic of Korea, 1996. [Google Scholar]
- Kim, J.Y.; Pham, D.D. Sasang constitutional medicine as a holistic tailored medicine. Evid.-Based Complement. Altern. Med. 2009, 6 (Suppl. 1), 11–19. [Google Scholar] [CrossRef] [PubMed]
- Shim, E.B.; Lee, S.; Kim, J.Y.; Earm, Y.E. Physiome and sasang constitutional medicine. J. Physiol. Sci. 2008, 58, 433–440. [Google Scholar] [CrossRef] [PubMed]
- Lee, T.; Lee, S.; Choe, B.; Song, I. A study on the prevalences of chronic diseases according to Sasang constitution at a health examination center. J. Sasang Constitut. Med. 2005, 17, 32–45. (In Korean) [Google Scholar]
- Lee, J.; Lee, J.; Lee, E.; Yoo, J.; Kim, Y.; Koh, B. The sasang constitutional types can act as a risk factor for hypertension. Clin. Exp. Hypertens. 2011, 33, 525–532. [Google Scholar] [CrossRef]
- Lee, T.G.; Koh, B.; Lee, S. Sasang constitution as a risk factor for diabetes mellitus: A cross-sectional study. Evid.-Based Complement. Altern. Med. 2009, 6, 99–103. [Google Scholar] [CrossRef]
- Choi, K.; Lee, J.; Yoo, J.; Lee, E.; Koh, B.; Lee, J. Sasang constitutional types can act as a risk factor for insulin resistance. Diabetes Res. Clin. Pract. 2011, 91, e57–e60. [Google Scholar] [CrossRef]
- Song, K.H.; Yu, S.G.; Kim, J.Y. Prevalence of metabolic syndrome according to Sasang constitutional medicine in Korean subjects. Evid.-Based Complement. Altern. Med. 2012, 2012, 646794. [Google Scholar] [CrossRef]
- Jin, H.J.; Baek, Y.; Kim, H.S.; Ryu, J.; Lee, S. Constitutional multicenter bank linked to Sasang constitutional phenotypic data. BMC Complement. Altern. Med. 2015, 15, 46. [Google Scholar] [CrossRef] [PubMed]
- American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care 2014, 37 (Suppl. 1), S81–S90. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.W.; Jang, E.S.; Lee, J.; Kim, J.Y. Current researches on the methods of diagnosing sasang constitution: An overview. Evid.-Based Complement. Altern. Med. 2009, 6 (Suppl. S1), 43–49. [Google Scholar] [CrossRef] [PubMed]
- Baek, Y.H.; Kim, H.S.; Lee, S.W.; Jang, E.S. The Concordance and Validity Assessment of Diagnosis for the Expert in Sasang Constitution. J. Sasang Constit. Med. 2014, 26, 295–303. (In Korean) [Google Scholar] [CrossRef]
- Lee, S.Y.; Park, H.S.; Kim, D.J.; Han, J.H.; Kim, S.M.; Cho, G.J.; Kim, D.Y.; Kwon, H.S.; Kim, S.R.; Lee, C.B. Appropriate waist circumference cutoff points for central obesity in Korean adults. Diabetes Res. Clin. Pract. 2007, 75, 72–80. [Google Scholar] [CrossRef]
- Baek, Y.; Park, K.; Lee, S.; Jang, E. The prevalence of general and abdominal obesity according to sasang constitution in Korea. BMC Complement. Altern. Med. 2014, 14, 298. [Google Scholar] [CrossRef]
- Grundy, S.M. Pre-diabetes, metabolic syndrome, and cardiovascular risk. J. Am. Coll. Cardiol. 2012, 59, 635–643. [Google Scholar] [CrossRef]
- Kim, M.J.; Yoo, J.S.; Koh, S.B.; Park, J.K. Prevalence of Hypertension and Risk Factor according to Sasang Constitution. J. Sasang Constitut. Med. 2009, 21, 150–164. (In Korean) [Google Scholar]
- Cho, N.H.; Kim, J.Y.; Kim, S.S.; Lee, S.K.; Shin, C. Predicting type 2 diabetes using S asang constitutional medicine. J. Diabetes Investig. 2014, 5, 525–532. [Google Scholar] [CrossRef]
- Oguoma, V.M.; Nwose, E.U.; Ulasi, I.I.; Akintunde, A.A.; Chukwukelu, E.E.; Bwititi, P.T.; Richards, R.S.; Skinner, T.C. Cardiovascular disease risk factors in a Nigerian population with impaired fasting blood glucose level and diabetes mellitus. BMC Public Health 2017, 17, 36. [Google Scholar] [CrossRef]
- Ling, C.; Rönn, T. Epigenetics in human obesity and type 2 diabetes. Cell Metab. 2019, 29, 1028–1044. [Google Scholar] [CrossRef] [PubMed]
| Normal FPG Group (n = 1511) | Pre-DM Group (n = 674) | Total (n = 2185) | p Value | |
|---|---|---|---|---|
| Sex (N, %) | ||||
| Male | 483 (62.5) | 290 (37.5) | 773 (100) | <0.001 |
| Female | 1028 (72.8) | 384 (27.2) | 1412 (100) | |
| Age (years) | 54.9 ± 9.9 | 57.9 ± 10.2 | 55.8 ± 10.1 | <0.001 |
| SC type (N, %) | ||||
| SE | 405 (75.3) | 133 (24.7) | 538 (100) | <0.001 |
| SY | 516 (70.3) | 218 (29.7) | 734 (100) | |
| TE | 590 (64.6) | 323 (35.4) | 913 (100) | |
| BMI (kg/m2) | 23.7 ± 3.1 | 24.3 ± 3.1 | 23.9 ± 3.1 | <0.001 |
| BMI < 25 | 1049 (72.6) | 396 (27.4) | 1445 (100) | <0.001 |
| BMI ≥ 25 | 462 (62.4) | 278 (37.6) | 740 (100) | |
| FPG (mg/dL) | 87.8 ± 7.9 | 108.0 ± 6.8 | 94 ± 12.0 | <0.001 |
| Systolic BP (mmHg) | 120.3 ± 15.2 | 124.8 ± 15.8 | 121.7 ± 15.5 | <0.001 |
| Diastolic BP (mmHg) | 77.6 ± 10.8 | 80 ± 11.6 | 78.4 ± 11.1 | <0.001 |
| TGs (mg/dL) | 128.6 ± 77.8 | 147.9 ± 95.2 | 134.5 ± 84 | <0.001 |
| HDL-C (mg/dL) | 47.5 ± 12.4 | 44.8 ± 11.7 | 46.6 ± 12.3 | <0.001 |
| Normal FPG Group | Pre-DM Group | Total | p Value a | |
|---|---|---|---|---|
| SC type | ||||
| SE | 87.6 ± 7.8 | 107.2 ± 6.7 | 92.4 ± 11.3 | <0.001 |
| SY | 87.2 ± 7.9 | 108.3 ± 6.7 | 93.4 ± 12.3 | <0.001 |
| TE | 88.5 ± 7.8 | 108.1 ± 6.9 | 95.4 ± 12.0 | <0.001 |
| p value b | 0.014 (SE < TE) | 0.36 | <0.001 (SE, SY < TE) | |
| BMI | ||||
| BMI < 25 | 87.4 ± 7.8 | 108.0 ± 6.8 | 93.0 ± 11.9 | <0.001 |
| BMI ≥ 25 | 88.8 ± 8.0 | 108.0 ± 6.8 | 96.0 ± 12.0 | <0.001 |
| p value b | 0.002 | 0.96 | <0.001 |
| SE | SY | TE | |||
|---|---|---|---|---|---|
| ORs (95% CIs) | p Value | ORs (95% CIs) | p Value | ||
| BMI < 25 a | |||||
| Crude | Reference | 1.147 (0.869–1.516) | 0.333 | 1.544 (1.148–2.077) | 0.004 |
| Model 1 | Reference | 1.122 (0.845–1.489) | 0.427 | 1.427 (1.054–1.932) | 0.021 |
| Model 2 | Reference | 1.095 (0.822–1.457) | 0.536 | 1.354 (0.995–1.844) | 0.054 |
| BMI ≥ 25 a | |||||
| Crude | Reference | 1.429 (0.719–2.841) | 0.308 | 1.267 (0.669–2.399) | 0.467 |
| Model 1 | Reference | 1.355 (0.676–2.716) | 0.392 | 1.205 (0.632–2.299) | 0.571 |
| Model 2 | Reference | 1.355 (0.671–2.734) | 0.397 | 1.158 (0.604–2.221) | 0.659 |
| Total b | |||||
| Crude | Reference | 1.286 (1.0–1.655) | 0.05 | 1.667 (1.314–2.115) | <0.001 |
| Model 1 | Reference | 1.187 (0.916–1.54) | 0.195 | 1.353 (1.031–1.776) | 0.029 |
| Model 2 | Reference | 1.161 (0.894–1.509) | 0.263 | 1.281 (0.973–1.686) | 0.077 |
| ORs (95% CIs) for Pre-DM | p Value | |
|---|---|---|
| SE | ||
| BMI < 25 | Reference | |
| Crude | 1.482 (0.776–2.831) | 0.234 |
| Model 1 | 1.303 (0.673–2.523) | 0.432 |
| Model 2 | 1.096 (0.553–2.17) | 0.793 |
| SY | ||
| BMI < 25 | Reference | |
| Crude | 1.846 (1.286–2.649) | 0.001 |
| Model 1 | 1.734 (1.2–2.507) | 0.003 |
| Model 2 | 1.604 (1.093–2.354) | 0.016 |
| TE | ||
| BMI < 25 | Reference | |
| Crude | 1.216 (0.923–1.603) | 0.165 |
| Model 1 | 1.201 (0.907–1.589) | 0.201 |
| Model 2 | 1.042 (0.777–1.397) | 0.785 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Baek, Y.; Lee, S.; Jeong, K.; Jang, E. Sasang Constitution Type Combined with General Obesity May Act as a Risk Factor for Prediabetes Mellitus. Healthcare 2022, 10, 2286. https://doi.org/10.3390/healthcare10112286
Baek Y, Lee S, Jeong K, Jang E. Sasang Constitution Type Combined with General Obesity May Act as a Risk Factor for Prediabetes Mellitus. Healthcare. 2022; 10(11):2286. https://doi.org/10.3390/healthcare10112286
Chicago/Turabian StyleBaek, Younghwa, Siwoo Lee, Kyoungsik Jeong, and Eunsu Jang. 2022. "Sasang Constitution Type Combined with General Obesity May Act as a Risk Factor for Prediabetes Mellitus" Healthcare 10, no. 11: 2286. https://doi.org/10.3390/healthcare10112286
APA StyleBaek, Y., Lee, S., Jeong, K., & Jang, E. (2022). Sasang Constitution Type Combined with General Obesity May Act as a Risk Factor for Prediabetes Mellitus. Healthcare, 10(11), 2286. https://doi.org/10.3390/healthcare10112286






