Abstract
Global turbulence and uncertainty force civil servants and executors to optimise public finance distribution. The COVID-19 pandemic aligned with the necessity of assessing the efficiency of healthcare financing due to its capability in overcoming the negative consequences. The paper analyses the peculiarities of healthcare financing in 34 European countries and points out trends and changes in its structure and dynamics. It also realises cluster analysis to reveal models of healthcare financing and their specific features. Panel data regression analysis was used to assess the efficiency of healthcare financing within each cluster by clarifying the relationship between healthcare expenditures and public health outcome—life expectancy. The distributed lag model was also used to test for time lags between financial inflows in healthcare and its outcome. Empirical results highlight key tips for optimising healthcare financing and creating the benchmark model.
1. Introduction
Over the past several decades, there has been an increase in healthcare expenditures in most of the world’s countries (Sen 2005) due to several factors. First, the state of public health and the volume of financial resources necessary for its maintenance depends on economic factors. Thus, the increase in economic well-being in developed countries contributed to the increase in quality of life, improvement of living conditions, and expansion of access to better medical care, which collectively had a positive effect on life expectancy (McKeown 1976; Letunovska et al. 2022). Positive economic dynamics in the poorest countries contributed to improving sanitary conditions and partially eliminating food security problems. These changes, in turn, made it possible to level certain risks of exacerbation of chronic diseases, improved the general state of health of the population, and increased life expectancy (Fogel 1997; Dollar and Kraay 2002; Frimpong and Adu 2014; Sanjeev and Verhoeven 2001).
In addition, achieving a high level of well-being allowed business entities to shift their focus from obtaining exclusively economic benefits and generating surplus profits to implementing social initiatives. In particular, at the end of the 1990s and the beginning of the 2000s, corporate social responsibility gained more and more popularity, which has not lost its relevance even today. Building a model of socially responsible business is based on the need to take into account and balance the interests of all stakeholders (Kakabadse et al. 2005; Dacko-Pikiewicz 2019), including business owners and shareholders, as well as counterparties, customers, employees, and society as a whole. The personnel perspective of implementing corporate social responsibility aims to provide decent working conditions and a high-quality social package for employees. Thus, the high-quality and socially oriented policy of human resources management, which became possible due to high rates of economic growth, contributed to the improvement of employee health due to the creation of a favourable social and psychological climate in the team, the arrangement of workplaces taking into account the requirements of ergonomics, a qualitative and comprehensive social package, and the ability to satisfy not only basic needs but also the needs of a higher level according to Maslow’s pyramid at the expense of a decent salary (Davidson 2015; Rajiani and Kot 2020; Szczepańska-Woszczyna and Gatnar 2022).
The ecological perspective of adapting the socially responsible business model involves the implementation of environmental initiatives aimed at reducing the negative anthropogenic impact on the environment, preserving the eco-system, and actively implementing eco-innovations (Senaratne et al. 2021). Thus, on the one hand, the intensification of production processes to ensure economic growth triggered significant deterioration of the environment and the growth of environmental risks and threats, as well as their globalisation. However, achieving a certain level of well-being made it possible to form a financial reserve to expand the possibilities of implementing a wide range of environmental projects. In modern conditions, balancing economic interests and environmental risks is one of the most challenging tasks, which provokes heated discussions. There is no simple solution to the given dilemma since the complete levelling of the negative impact of production processes on the environment is quite likely to level the positive dynamics of GDP growth, which, in turn, eliminates all the positive effects of intensive economic growth described above. However, ignoring environmental threats is also a harmful strategy. That is why the most realistic development option is accepting an acceptable level of adverse environmental impacts and permanent work on developing and implementing eco-innovations. The dialectical connection of ecological and economic determinants is reflected accordingly in the public health system’s functioning: economic benefits ensure better living conditions and medical care, and the negative ecological effect of economic activity leads to the deterioration of population health indicators. These effects crystallised especially clearly in the context of the unfolding of the COVID-19 pandemic and overcoming its consequences (Smiianov et al. 2020; Letunovska et al. 2024).
The development of technologies, innovations, and digitalisation of business processes is a crucial determinant of socio-economic development (Infante-Moro and Gallardo-Pérez 2020; Wróblewski and Lis 2021; Infante-Moro and Gallardo-Pérez 2022; Baltgailis and Simakhova 2022; Kwilinski 2023; Kwilinski et al. 2020, 2024a, 2024b, 2024c; Abad-Segura et al. 2024; Melnychenko 2021). The development of digital technologies not only became an impetus for the deepening of scientific research and the cultivation of innovations, which contributed to the acceleration of economic growth, but also made it possible to ensure the transition to a qualitatively new stage of the development of the public health system. In particular, the implementation of innovative technologies in the medical sphere allowed: (1) to create qualitatively new equipment that provides better diagnosis and implementation of medical invasions; (2) to update disease treatment protocols to ensure their higher efficiency; (3) to create new medical drugs with better effectiveness and fewer side effects; (4) to invent alternative approaches and means of treatment (Mitchell and Kan 2019; Kadar and Reicher 2020; Aliyeva 2022; Kwilinski 2023; Wei et al. 2023).
Thus, from all of the above, it can be concluded that the high rates of economic growth, scientific and technological progress, and the social transformations caused by it have made it possible to improve the population’s health and life expectancy over the past 30 years. However, many researchers emphasise the negative impacts of economic growth on the public health system. Thus, the wide offer of various food products, their widespread advertising in combination with the existence of financial opportunities for their purchase has greatly actualised the problems of obesity and increased the risks of chronic diseases for which excess weight is the primary risk factor (diabetes, cardiovascular diseases) (Dong et al. 2022; Veckalne et al. 2023). Against the background of the aggravation of this problem in highly developed countries, scientists also find evidence of the opposite processes in low- and middle-income countries, namely: the growth of economic well-being in these countries allows individuals to choose higher quality foods, consuming more healthy food (vegetables and fruits) (Frank et al. 2019). Another problem of the 21st century is the decrease in the level of physical activity of the population, which is primarily caused by the development of digital technologies (television, the Internet, social media) and the opportunity to be fully realised in the digital environment (Wei et al. 2023). Among the negative manifestations of the intensification of economic growth for the public health system, scientists also note the increase in cancer cases (Teoh et al. 2020). A paradoxical negative result of the growth of economic well-being is an increase in the expenditure burden on the social security system, the public health system, and insurance medicine because, in the conditions of improving the quality of life and increasing the life expectancy of the population, the share of the elderly population also increases significantly (Chen et al. 2022).
All the above-described regularities convincingly testify to a connection (not always positive) between the level of economic development and the resulting parameters of public health (in particular, the population’s life expectancy). However, the question arises as to whether the growth of healthcare expenditures in most countries during the last few decades results from corresponding positive economic dynamics and the consequence of the processes mentioned above or whether such growth is still due to objective needs. Considering the above, the main task of this research is to determine the efficiency of healthcare financing in 34 European countries. In particular, several econometric procedures will identify temporal, geographical, and causal patterns in the “healthcare financing → life expectancy” chain. All this in the complex will answer the question: “Does every unit of investment in the public health system ensure a parity increase in the population’s life expectancy?”. After all, the central hypothesis of the research is that the spending of financial resources on healthcare is inefficient and achieving similar results in the increase of life expectancy would be possible with lower expenses. Under such a scenario, the increase in spending on healthcare is not an objective need but a particular “tradition” due to the country’s ability to permanently increase funding in this area due to a permanent increase in economic well-being (Szczepańska-Woszczyna et al. 2024). Recent research papers demonstrate somewhat controversial results on the issue, as there are scientists who both support and reject the hypothesis. Moreover, research on the assessment of healthcare financing due to improvement of health outcomes dominantly focuses on low-income African or Asian countries. At the same time, there is a lack of research on high- and middle-income European countries. Additionally, some research focuses on clarifying changes in healthcare financing and healthcare efficiency patterns due to the consequences of global financial crisis but still lacks publications that cover the pandemic period. Finally, most recent research on efficiency of healthcare financing considers the period from 2000 to 2014, 2019, or 2019, while it is necessary to regularly update such empirical research to reveal new tendencies (especially after a coronavirus pandemic). All these drawbacks of recent research bring to the necessity of further developments and support the urgency of this research.
Considering the above-mentioned research gaps, the aim of the paper is to assess the efficiency of healthcare financing in 34 European countries during 2000–2022 and point out key policy implications for its improvement. Due to the research objectives, the structure of the paper is as follows: (1) modelling the efficiency of healthcare financing using stochastic frontier analysis; (2) identifying the model of healthcare financing considering values of different healthcare expenditures in 2000–2022 and grouping of countries in clusters due to similarity of the revealed patterns; (3) modelling the relationships between health expenditure and life expectancy within each cluster using panel data regression model and distributional-lag modelling; (4) generalization and interpretation of all modelling results to develop recommendations on improvement of efficiency of healthcare financing for each cluster of countries.
2. Materials and Methods
The research task was implemented using a combination of various methods, analytical and econometric procedures.
2.1. Research Variables
The basic assumption of this study is that the efficiency of healthcare financing implies an increase in return from each unit of financial resources spent on healthcare measures (considering private individuals, state authorities, and foreign donors), which is realised in increasing life expectancy. Despite several other effective initial parameters, the indicator of population life expectancy was chosen as the key performance indicator of the efficiency of the public health system. The logic of such a choice is consistent with numerous scientific studies (Liu and Zhong 2022; Jetter et al. 2019; Cole 2019; Shahbaz et al. 2019; Cetin and Bahce 2016; Frimpong and Adu 2014). Thus, the outcome variable within this study is Life expectancy at birth, total (years) (Life).
Instead, the set of factor variables (input variables) is represented by the following indicators:
- –
- Capital health expenditure to GDP ratio, % (Cap);
- –
- Domestic general government health expenditure to current health expenditure ratio, % (Dom_gov);
- –
- Domestic private health expenditure to current health expenditure ratio, % (Dom_prv);
- –
- External health expenditure to current health expenditure ratio, % (Ext);
- –
- Out-of-pocket expenditure to current health expenditure ratio, % (OoP).
2.2. Data Sources
In terms of the indicators mentioned above, an array of statistical data was formed for 34 European countries (Albania, Austria, Belgium, Bosnia and Herzegovina, Bulgaria, Croatia, Czech Republic, Denmark, Estonia, Finland, France, Germany, Greece, Hungary, Iceland, Ireland, Italy, Latvia, Lithuania, Moldova, Netherlands, North Macedonia, Norway, Poland, Portugal, Romania, Serbia, Slovak Republic, Slovenia, Spain, Sweden, Switzerland, Ukraine, United Kingdom) for 2000–2022. Public data from the collection “Health Nutrition and Population Statistics” of the World Bank group (World Bank 2024) was taken as the basis for forming the data sample.
2.3. Stages of Investigation
Carrying out the research task involves the following:
- (1)
- determining the efficiency of healthcare financing using stochastic frontier analysis;
- (2)
- clustering of countries considering options of healthcare financing; qualitative analysis of clusters and identifying specific features for each model of healthcare financing, characteristic of each of the clusters;
- (3)
- substantiating additional determinants of the efficiency of healthcare financing through the formalisation of temporal and causal patterns in the chain “healthcare financing → life expectancy” based on distributional-lag modelling; generalisation and qualitative interpretation of the modelling results, formation of recommendations for each cluster/model of healthcare financing regarding ways to improve its efficiency.
- Determining the efficiency of healthcare financing in scientific research is traditionally carried out using two tools—Data Envelopment Analysis (DEA) (Charnes et al. 1978; Afonso and Aubyn 2011; Karagiannis 2015; Tigga and Mishra 2015; Kaya Samut and Cafrı 2016; Stefko et al. 2018; Ahmed et al. 2019; Chitnis and Mishra 2019; Kohl et al. 2019; Hamzah et al. 2021; Arhin et al. 2023a) and Stochastic Frontier Analysis (Newhouse 1994; Skinner 1994; Kumbhakar and Lovell 2000; Hollingsworth 2003; Greene 2004; Luis Orea and Kumbhakar 2004; Rosko and Mutter 2008; Hamidi and Akinci 2016; Izón and Pardini 2017; Bashir et al. 2022; Arhin et al. 2023b; Bala et al. 2023; Kang et al. 2023; Sülkü et al. 2023). The difference between these approaches is that DEA determines the frontier based on the level of indicators achieved. In contrast, Stochastic Frontier Analysis calculates the frontier considering the most successful combination of input and output factors. In contrast, the inefficiency parameter determines the deviation of the actual level of the indicator from the potentially possible maximum. Thus, in the first case, there will necessarily be a country with 100% efficiency among the calculated values of technical efficiency. In contrast, in the second case, as a rule, none of the countries will have absolute efficiency. In previous studies, the authors calculated the efficiency of healthcare financing using DEA for the same sample of 34 European countries. In particular, according to the results of this analysis, the technical efficiency of healthcare financing is in the range of [0.92; 1.00], while for 15 out of 34 countries, the indicator is the maximum. Thus, the DEA approach did not allow for the identification of absolute flagships since the variation between the levels of efficiency of healthcare financing in the studied European countries is insignificant. That is why, as part of this study, the level of efficiency of healthcare financing will be evaluated using Stochastic Frontier Analysis, that is, based on the assumption that no country currently functions on the frontier but, on the contrary, has the potential for growth due to the elimination of those prerequisites that create inefficiency. The efficiency of healthcare financing will be determined using the command “xtfrontier” in the Stata 14.2/SE software product.
- Clustering of countries according to the criterion of financing the healthcare system will be carried out based on the factor (input) variables specified above, using the command “xtregcluster” in Stata 14.2/SE software product. The methodology of this approach was developed (Sarafidis and Weber 2015), and the specifics of the application are described in detail in the work (Christodoulou and Sarafidis 2017). The above command allows the grouping of objects into clusters, for each of which the slope coefficient is homogeneous. The two-way structure of the error components explains the within-cluster heterogeneity. Furthermore, the slope coefficients vary across groups. The number of clusters is considered unknown and determined from the data based on minimising an information criterion for a rigorously consistent model (Christodoulou and Sarafidis 2017). A qualitative analysis of the efficiency of healthcare financing within each cluster will allow for formalising the specific features. These specific features determine the healthcare system’s financial support models
- Identifying the additional determinants of the efficiency of healthcare financing through the formalisation of temporal and causal patterns in the chain “healthcare financing → life expectancy”. The distributed-lag modelling in Stata 14.2/SE software product is used. It is tested for causal relationships between input and output variables with a 0–3-year lag.
The generalisation and qualitative interpretation of all modelling results aim to identify specific patterns of the healthcare financing models and formalise certain steps that will increase their efficiency.
3. Results
3.1. Determining the Efficiency of Financing the Healthcare System
Before determining the efficiency of healthcare financing, the general parameters, which are this study’s input and output variables, are analysed (Table 1).

Table 1.
Averaged values of input and output determinants of the performance of public health systems in 34 European countries.
Thus, it can be noted that longer life expectancy is characteristic of countries with higher well-being, economic development, and social security. In particular, the highest life expectancy is in Switzerland (82.19 years). At the same time, Iceland, Italy, Spain, Sweden, France, and Norway, for which the average life expectancy is about 81 years, are also included in the group of leading countries. Another 7 highly developed countries have a typical life expectancy of about 80 years, and another 4—about 79 years. Conversely, below-average life expectancy is typical for countries with comparatively lower rates of economic growth, most of which are countries of the former socialist bloc. Thus, Albania and the Czech Republic form a transitive group of countries whose life expectancy slightly deviates from the average for the entire sample (77.66 years). On the other hand, 14 out of 34 countries are characterised by a life expectancy lower than the sample average. Moreover, the lowest life expectancy is in Ukraine (69.85 years) and Moldova (68.97 years), which is more than 3 years less than the previous country (Latvia, life expectancy—73.09 years), even though the width of the step changes in the level of the indicator between other countries in the rating, as a rule, do not exceed 1 year.
Analysing the general distribution patterns of input performance indicators of the healthcare system (different groups of healthcare expenditures), it can be noted that the Netherlands (1.99%) and Austria (0.67%) have the most considerable specific weight of capital expenditures for healthcare in GDP. At the same time, many countries from the upper part of the rating are characterised by a minimum level of the indicator approaching 0. In contrast, for countries from the lower part of the rating, on the contrary, the moderate size of the indicator is in the range of about 0.2–0.4% of GDP (only Latvia and Moldova are characterised by a higher volume of capital expenditures in the amount of 0.49% of GDP and 0.54% of GDP, respectively). The analysis of the structure of current expenditures on healthcare does not allow, at first glance, to determine the optimal ratio between these types of expenditures, which will ensure a proper and proportional increase in the population’s life expectancy. Thus, both among the countries located at the top of the table (with a higher life expectancy) and among the countries from the bottom of the table, various options from the following combinations are characteristic—the preponderance of government current healthcare expenditures over private, the preponderance of private current healthcare expenditure over government, and the approximately equal ratio between government and private current healthcare expenditure. At the same time, according to the data presented in the table, it is possible to formulate an assumption that the need to attract external donors to finance the current needs of ensuring the functioning of the healthcare system is due to the lack of internal financial opportunities for its financing, which is more characteristic of the group of countries in the lower part of the table. It is also worth noting that for the same group of countries, a comparatively higher share of out-of-pocket expenditures in current healthcare expenditures is more characteristic. Thus, for the countries of the “green” group, on average, this type of expenditure on healthcare is 18.5% of the volume of current expenditures, while in the countries of the “yellow” and “red” groups it is more than 31%. Thus, it seems logical to assume that in countries with higher efficiency of the healthcare system (higher life expectancy), the need to finance medical services with out-of-pocket expenditures is almost twice as low as in countries where the life expectancy is below the average of a sample of countries.
Considering the healthcare system’s input and output performance indicators, we determine the performance indicator using the “xtfrontier” command in Stata 14.2/SE software product—technical efficiency indicators varying in the range [0.56; 0.72]. The lowest indicator was recorded in Moldova in 2000 and the highest in Italy in 2022. Figure 1 shows the average values of indicators of the technical efficiency of healthcare financing across the 34 countries of the sample.
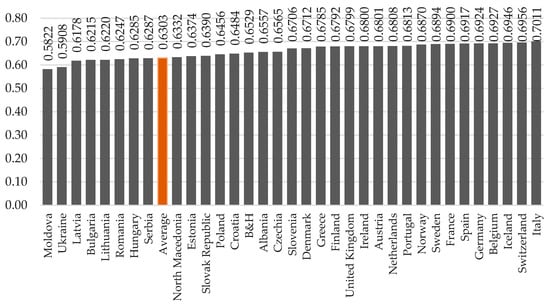
Figure 1.
Technical efficiency of healthcare financing (average value for 2000–2022) in 34 European countries. Source: Authors’ calculations in Stata 14.2/SE software (Stata Software 2024) based on World Bank data (World Bank 2024).
According to the data presented in Figure 1, it can be noted that in the studied countries, the level of technical efficiency of healthcare financing is relatively high and is concentrated in the third quartile. The spread of variation of the indicator between countries is insignificant; only the gap between Moldova, Ukraine and the rest of the sample countries is more significant at about 2–3%, while the deviation between the indicator levels in consecutive other countries does not exceed 1%. The general distribution patterns of the indicator of the technical efficiency of healthcare financing are quite closely correlated with the distribution of the initial parameter—the population’s life expectancy, i.e., the higher efficiency is found in states with a higher level of socio-economic development and well-being.
3.2. Clustering of Countries according to the Criterion of Financing the Healthcare System
The clustering of countries was implemented using “xtregcluster” in the Stata 14.2/SE software product. Clustering is based only on indicators of healthcare financing (input variables). It is worth noting that since the approach applicable to panel data was used, belonging to a specific cluster does not change depending on the variation of the time factor but is identical for each specific country throughout the entire observation period. According to the clustering results, it was determined that the grouping of countries in three clusters is optimal. The first cluster included Albania, the Czech Republic, Denmark, Finland, Iceland, Ireland, Latvia, North Macedonia, Poland, Sweden, and Great Britain. The second cluster included Austria, Belgium, Bosnia and Herzegovina, Bulgaria, Croatia, Estonia, France, Germany, Greece, Hungary, Italy, Lithuania, Moldova, Norway, Portugal, Romania, Serbia, Slovakia, Slovenia, Spain, Switzerland, and Ukraine. The third cluster included only one country—the Netherlands. Summarising averaged characteristics for each of the clusters are given in Table 2.

Table 2.
Averaged values of healthcare financing proxies for clusters of countries.
The generalisation of the clustering results made it possible to identify the following specific features of the healthcare financing models, which are characteristic of the countries included in the corresponding cluster:
- –
- The model of financial support of the healthcare system of the countries in the first cluster is characterised by a moderate amount of capital expenditures for healthcare, external healthcare expenditures, and current out-of-pocket expenditures, while the ratio of public funding of the healthcare system to private funding is approximately 73% vs. 27%; all this makes it possible to ensure relatively high efficiency of healthcare financing within 66.4%;
- –
- The model of healthcare financing of the countries in the second cluster is characterised by the minimum level of capital expenditures on healthcare but the maximum level of external healthcare expenditures and current out-of-pocket expenditures, while the ratio of public financing of the healthcare system to private funding is very similar to model 3 at 68% vs. 32%; the efficiency of healthcare financing is the lowest among the three clusters—65.6% on average;
- –
- The model of healthcare financing of the countries in the third cluster is characterised by the maximum level of capital expenditures on healthcare but the minimum level of external healthcare expenditures and current out-of-pocket expenditures, while the ratio of public financing of the healthcare system to private financing is 67% vs. 33%; the efficiency of healthcare financing is the highest and is 68.1% on average.
Thus, model 3 can be characterised as a model with the highest level of autonomy and efficiency of financial provision of the healthcare system, which can be considered a benchmark. Model 1 is optimal and characterised by a moderate level of financial indicators. Model 2 is the least effective, and it is characterised by transferring the financial burden to individuals—consumers of medical services due to the highest value of the out-of-pocket expenditures.
3.3. Formalisation of Temporal and Causal Patterns in the Chain “Healthcare Financing → Life Expectancy”
Using distributed-lag modelling in Stata 14.2/SE software product, the results of determining the causal relationships in the chain “healthcare financing → life expectancy” were obtained for each cluster of countries identified at the previous stage of the research. A lag of up to 3 years was tested (longer lags are ineffective due to the size of the sample observation period). The simulation results regarding clusters are presented in Table 3, Table 4 and Table 5.

Table 3.
Distributed-lag modelling results on the impact of healthcare financing on life expectancy for 11 countries of cluster 1 for 2000–2022.

Table 4.
Distributed-lag modelling results on the impact of healthcare financing on life expectancy for 22 countries of cluster 2 for 2000–2022.

Table 5.
Distributed-lag modelling results on the impact of healthcare financing on life expectancy for 1 country (the Netherlands) of cluster 3 for 2000–2022.
The following patterns are characteristic of the group of countries of the first cluster:
- –
- A positive, considerable, and statistically significant impact of the growth of capital healthcare expenditures on both without a lag and with a lag of 1–3 years (the most qualitative relationship from an econometric point of view is in the model with a lag of 3 years: an increase in capital healthcare expenditures in GDP by 1% causes an increase in the life expectancy of the population in the countries of the first cluster by 2.5 years);
- –
- The statistical significance of the positive impact of the increase in the specific weight of domestic government and private healthcare expenditures in current expenditures on life expectancy is manifested only with a lag of 3 years;
- –
- The growth of external healthcare expenditures harms the life expectancy of the population, and this relationship is statistically significant without time lags;
- –
- An increase in the specific weight of out-of-pocket expenditures in the structure of current healthcare expenditures hurts the population’s life expectancy. At the same time, the best statistical quality of the relationship is realised with a lag of 2 years when the influence of the indicator is the highest.
The following patterns are characteristic of the group of countries of the second cluster:
- –
- The positive effect of the growth of capital healthcare expenditures on the increase in life expectancy was confirmed without a lag and with a lag of 1 year. However, the most statistically significant result is precisely without a lag, in which a 1% increase in the specific weight of capital expenditures in GDP leads to an increase in life expectancy in the countries of the second cluster by 2.07 years;
- –
- An interesting fact is that the growth of the specific weight of public, private and external healthcare expenditures in current expenditures without a time lag is characterised by a statistically significant negative impact on life expectancy in the countries of the second cluster; however, their growth with a lag of 3 years is accompanied by a significant growth in life expectancy. An increase in the specific weight of out-of-pocket expenditures in the structure of current healthcare expenditures negatively affected life expectancy of the population at all time intervals (the most statistically significant result is without a time lag, while with an increase in the lag, the quality and strength of the relationships worsen).
The following patterns are characteristic of the group of countries of the third cluster:
- –
- The positive effect of the increase in capital healthcare expenditures on the increase in life expectancy is statistically significant at all time intervals; however, this relationship is most qualitative in the model without a time lag, i.e., a 1% increase in the specific weight of capital expenditures in GDP is accompanied by an increase in life expectancy of 1.6 years almost instantaneously;
- –
- Instead, the growth of the specific weight of public, private and external healthcare expenditures in current expenditures acts as a destructive determinant of changes in life expectancy; this effect is most strongly realised without a lag and with a lag of 1 year;
- –
- An increase in the specific weight of out-of-pocket expenditures in current expenditures by 1% leads to a reduction in life expectancy without a time lag of 0.21 years.
4. Discussion
The generalisation of scientific studies related to identifying the factors of growth of healthcare expenditures proved the existence of a relationship between the rates of economic development and the growth of healthcare expenses (Alipouri Sakha et al. 2024; Atilgan et al. 2024; Das 2024; Beylik et al. 2022; Rokicki et al. 2021; Gallardo-Albarran 2018; Vargas Bustamante and Shimoga 2018; Ye and Zhang 2018; Wang 2015). At the same time, there is an assumption that in high-, upper-middle-, and middle-income countries, the increase in healthcare expenditures is not a necessity but a “tradition” or “habit”, which is possible due to the existence of a reserve of financial resources. Even though sustainable economic development allows investing more financial resources in improvement of social protection and promoting public health, there is no irrefutable evidence that a greater volume of financial resources equals better health outcomes. Some researchers even consider that a decrease of public financing of healthcare allows maintaining stable health outcomes (Rechel 2019; Balkhi et al. 2021). Basically, scientists (Brikci et al. 2024; Gaylong et al. 2023) argued that up to 40% of budget financial resources might be used inefficiently because of funding delays. Researchers also strongly support the idea that government effectiveness, control of corruption, and good governance are necessary preconditions for more effective public funds distribution and utilization (Nakatani et al. 2024; Domapielle et al. 2022; Xu and Lin 2022; Nakatani et al. 2022; Ivanková et al. 2020; Zeng et al. 2020; Saltman 2018; Kulkarni 2016).
Efficiency of healthcare financing also depends on the initial state of healthcare system. Specifically, there is evidence that investment in healthcare infrastructure promotes system resilience to shocks like COVID-19 pandemic and contributes to better performance of health outcomes (Antohi et al. 2022; Lupu and Tiganasu 2022; Novignon and Tabiri 2022; Waitzberg et al. 2021; Legido-Quigley et al. 2020; Choonara and Eyles 2016). In turn, Hadad et al. (2013) and Raghupathi and Raghupathi (2020) pointed out that healthcare system efficiency depends not only on institutional capacity of financial support but also on transformation of the population’s behaviour to a healthier and more responsible lifestyle.
Formalisation of temporal and causal patterns in the chain “healthcare financing → life expectancy” for each cluster of countries using distributed-lag modelling (lag up to 3 years) made it possible to obtain interesting results. Thus, for the countries of cluster 1, the growth of capital healthcare expenditures is essential, as it provides the most significant contribution to the population’s life expectancy growth. Novignon and Tabiri (2022) also pointed out that investment in healthcare infrastructure development is crucially important for promoting health outcomes.
At the same time, an increase in the specific weight of public and private current expenditures on healthcare will also have a positive effect on the performance indicator in the medium term (lag of 3 years). Similarly, Onofrei et al. (2021) obtained evidence of positive, long-run relationships between public health expenditures and life expectancy for developing EU counties. Li and Yuan (2019) also pointed out that an increase in domestic government health expenditure positively affects health outcomes, especially in rural areas in low-income regions. Obrizan and Wehby (2018) evaluated relationships between healthcare expenditures and life expectancy in 175 countries and revealed that an increase in health spending more strongly contributes to an increase in life expectancy in countries with comparably low life expectancy. Bein et al. (2017) also obtained similar results: considering healthcare expenditures and life expectancy data for 2000–2014, they revealed with panel data regression technique that “there is a strong, positive association between total healthcare expenditures and total life expectancy”. Rahman et al. (2018) realised research on data for 15 countries in 1995–2014 and concluded that both an increase in public and private healthcare expenditures matter for improvement of health outcomes, but private healthcare expenditures have a stronger impact. Fujii (2018) also came to the same conclusions as Rahman et al. (2018). Specifically, it was found that private healthcare expenditure is more effective in promoting health outcomes than public healthcare expenditures but only for countries with ineffective government. For countries with effective government, both types of healthcare expenditures are almost equally effective in improving health outcomes. In contrast, Sango-Coke and Bein (2018) declared that an increase in the public healthcare sector is more vital for improving life expectancy in West African countries. This conclusion is also fair for the Pakistan case: an increase in public health expenditure provokes improvement in life expectancy both in the short and long run (Ullah et al. 2021). Zeng and Niu (2023) also realised research based on data for West African countries during 1995–2019 and revealed that total healthcare expenditure positively affected healthy life expectancy in the long run, while out-of-pocket health expenditures had a negative effect. Moreover, they revealed that public and private healthcare expenditure have a positive influence on health outcomes in the short run. Interestingly, Gallet and Doucouliagos (2017) and Bokhari et al. (2007) argued that healthcare spending has a better relationship with mortality rate instead of life expectancy.
In turn, Grigoli and Kapsoli (2018) argued that government spending on health issues is quite low in emerging and developing countries (80 countries, observation period 2001–2010) and its increase does not necessarily associate with an increase in life expectancy; scientists argued that only effective allocation of budget resources might contribute to better health outcomes. Herrera and Pang (2005) realised research in which they investigated the relationship between public health expenditures and health outcomes for 140 developing countries in 1996–2002. Scientists found that “countries with higher ratios of public to private financing of the service provision score lower efficiency”, while in our research this conclusion is unfair.
Moreover, an increase in out-of-pocket expenditures, on the contrary, has a negative medium-term effect. Sarker et al. (2021) also argued that an increase in out-of-pocket expenditures might significantly damage resilience of the healthcare system, especially in low-income countries where households might spend up to 35% of their income on healthcare. Behera and Dash (2018, 2019) point out that a decrease in out-of-pocket health expenditures is within core priorities in low-income and middle-income countries across the Asia-Pacific region. Grigorakis et al. (2018) based on the research of 26 EU and OECD countries during 1995–2013, concluded that these countries should realize measures for decreasing out-of-pocket health expenditures. Cacace (2021) also came to a similar conclusion for the group of Central and Eastern European Countries.
The countries of the first cluster are also recommended to reduce their dependence on external financial resources for healthcare. In contrast, Li and Yuan (2019) declare that an increase in external healthcare expenditures positively influences health outcomes.
For the countries of cluster 2, which is characterised by the lowest level of capital expenditures on healthcare, the increase of this group of expenditures in GDP provides the most significant contribution to the population’s life expectancy growth (without a lag). An increase in the share of public, private, and external healthcare expenditures in the structure of current expenditures has a negative immediate effect on the population’s life expectancy. However, this effect becomes almost three times stronger and changes its sign to “+” with a lag of 3 years. On the other hand, the negative effect of the increase in out-of-pocket expenditures on life expectancy persists at all time intervals. For the country of cluster 3, the positive return is achieved exclusively due to the growth of capital expenditures on healthcare. Shimul et al. (2023) also declared that developing countries (as in cluster 1) are more sensitive to changes in volumes of healthcare expenditures than developed countries (as in cluster 3). However, Khan and Husnain (2019), in contrast, proved that elasticity of healthcare expenditures is less than unity in developing Asian countries in the short run, while in the long run these relationships become more relative and impactful.
5. Conclusions
In terms of understanding retrospective and current trends of health financing frameworks and efficiency of healthcare financing due to improvement of health outputs, most scientists agree that socio-economic conditions do influence the volume of health financing.
The analysis of input (healthcare financing indicators) and output (population’s life expectancy) performance indicators of the healthcare system in 34 European countries during 2000–2022 showed that the average life expectancy of these countries is about 78 years. At the same time, the longest life expectancy is in Switzerland, Iceland, Italy, Spain, Sweden, France, and Norway, and the lowest (with a significant difference from the nearest country) in Ukraine and Moldova. According to these data, a certain peculiarity is observed: life expectancy is higher in more developed countries, which correlates with numerous scientific studies developed in the literature review. Based on the analysis results, it was also preliminarily established that a relatively lower level of capital healthcare expenditures is inherent in highly developed countries than in developing countries. However, there are certain exceptions to this statement. In particular, countries with a high level of socio-economic development—the Netherlands and Austria—have the most significant weight of capital healthcare expenditures in GDP, while in the group of developing countries, there are also leaders in this indicator—Latvia and Moldova. According to the results of a comparative analysis of the values of the healthcare performance parameters averaged over 23 years in 34 European countries, it is impossible to determine a model of the relationship between the types of current healthcare expenditures (domestic government and domestic private healthcare expenditures) that would ensure the most significant increase in life expectancy. At the same time, it can be assumed that the predominance of external current expenditures and out-of-pocket expenditures in current healthcare expenditures is a more valid trend for the group of countries with life expectancy below the sample average (middle-income countries).
Determining the efficiency of healthcare financing revealed a relatively high level of technical efficiency in these countries, which varies in the range [0.56; 0.72]. At the same time, Italy has the maximum healthcare financing efficiency value: the 23-year-averaged efficiency is 0.7011, while the most considerable absolute value of the indicator for the sample is 0.7178 (Italy, 2022). The model of healthcare financial provision in Moldova is the least efficient: the 23-year-averaged efficiency level is 0.5822, while the minimum absolute value of the indicator is 0.5604 (Moldova, 2000). Generally, it can be noted that the ranking of the studied countries according to the indicator of the efficiency of healthcare financing almost coincides with the order of their ranking according to the criterion of life expectancy. In turn, Medeiros and Schwierz (2015), while estimating healthcare financial efficiency in EU countries, obtained similar results. Specifically, the authors concluded that Belgium, Cyprus, Spain, France, Italy, Sweden and the Netherlands have the highest performance indicator, while the Czech Republic, Lithuania and Slovakia have the lowest ones. In contrast, Kujawska (2021) considered that Cyprus, Greece and Luxembourg are the most effective in healthcare financing (based on DEA analysis for 30 European countries for 2000–2014). Despite the discrepancy in the list of benchmark countries, there are matches in the list of countries with the lowest efficiency (Lithuania, Estonia, Hungary, Latvia, Slovakia, Austria) except for Austria, which is considered rather efficient within our research.
Based on the input parameters of healthcare financing, 34 studied European countries were grouped into 3 clusters. The first cluster (11 countries) is characterised by an average level of capital healthcare expenditures, external and out-of-pocket expenditures, and the ratio between public and private financing of the current needs of the healthcare system is approximately 73% to 27%. The second cluster (22 countries) is characterised by a low level of capital healthcare expenditures but a high level of external and out-of-pocket expenditures. The ratio of current public to current private spending on healthcare averages 68% to 32%. It is worth noting that the average levels of the efficiency of healthcare financing in the countries of the first and second clusters are practically identical (0.6639 vs. 0.6562). The highest efficiency is in the third cluster, which includes only one country—the Netherlands (technical efficiency 0.6808). This cluster is characterised by the most significant amount of capital healthcare expenditures and the lowest amount of external and out-of-pocket healthcare expenditures. In contrast, the ratio of current public and current private healthcare expenditures is almost identical to the countries of the second cluster—67% to 33%.
Summarising the results of the conducted research, it is possible to partially confirm the assumption that spending financial resources on healthcare is inefficient and achieving similar results would be possible with lower expenses, which is most clearly confirmed for the flagship cluster 3. At the same time, it is worth noting that in the less developed countries of the sample (clusters 1 and 2), the growth of current expenditures (except for out-of-pocket expenditures) makes it possible to achieve a positive effect on life expectancy in the medium term. Thus, a general recommendation can be formulated as follows: to ensure the increase in life expectancy in high-income countries, it is advisable to redistribute current and capital expenditures in favour of the latter, while in middle-income countries, the priority is to increase the weight of capital expenditures, however, without reducing public current and private current healthcare expenditures but by reducing the weight of out-of-pocket expenditures.
Author Contributions
Conceptualization, A.K. and A.V.; methodology, A.K. and A.V.; software, A.K. and A.V.; validation, A.K. and A.V.; formal analysis, A.K. and A.V.; investigation, A.K. and A.V.; resources, A.K. and A.V.; data curation, A.K. and A.V.; writing—original draft preparation, A.K. and A.V.; writing—review and editing, A.K. and A.V.; visualisation, A.K. and A.V.; supervision, A.K. and A.V.; project administration, A.K. and A.V.; funding acquisition, A.K. and A.V. All authors have read and agreed to the published version of the manuscript.
Funding
This research was funded by the Ministry of Education and Science of Ukraine, grant number 0122U000778 (“Socio-economic recovery after COVID-19: modelling the implications for macroeconomic stability, national security and local community resilience”) and grant number 0122U000781 (“The impact of COVID-19 on the transformation of the system of medical and social security of population: economic, financial-budgetary, institutional-political determinants”).
Informed Consent Statement
Not applicable.
Data Availability Statement
Data are available from the authors upon request.
Acknowledgments
The authors express their gratitude to the reviewers and the editorial team for their time, valuable feedback, and professionalism during the review and processing of the manuscript. Their insights and suggestions have made a significant contribution to the improvement of our work.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- Abad-Segura, Emilio, Alfonso Infante-Moro, Mariana-Daniela González-Zamar, and Eloy López-Meneses. 2024. Influential factors for a secure perception of accounting management with blockchain technology. Journal of Open Innovation: Technology, Market, and Complexity 10: 100264. [Google Scholar] [CrossRef]
- Afonso, António, and Miguel St. Aubyn. 2011. Assessing health efficiency across countries with a two-step and bootstrap analysis. Applied Economics Letters 18: 1427–30. [Google Scholar] [CrossRef]
- Ahmed, Sayem, Md Zahid Hasan, Mary MacLennan, Farzana Dorin, Mohammad Wahid Ahmed, Md Mehedi Hasan, Shaikh Mehdi Hasan, Mohammad Touhidul Islam, and Jahangir A. M. Khan. 2019. Measuring the efficiency of health systems in Asia: A data envelopment analysis. BMJ Open 9: e022155. [Google Scholar] [CrossRef]
- Alipouri Sakha, Minoo, Mohammad Bazyar, and Arash Rashidian. 2024. Classification and focus comparison of health financing frameworks: A scoping review. The International Journal of Health Planning and Management 39: 1146–71. [Google Scholar] [CrossRef]
- Aliyeva, Zamina. 2022. Innovation in healthcare management: Drug decriminalisation for reducing the health damage from crime. Marketing and Management of Innovations 1: 37–57. [Google Scholar] [CrossRef]
- Antohi, Valentin Marian, Romeo Victor Ionescu, Monica Laura Zlat, Cristian Mirica, and Nicoleta Cristache. 2022. Approaches to Health Efficiency across the European Space through the Lens of the Health Budget Effort. International Journal of Environmental Research and Public Health 19: 3063. [Google Scholar] [CrossRef]
- Arhin, Kwadwo, Oteng-Abayie, Eric Fosu, and Jacob Novignon. 2023a. Assessing the efficiency of health systems in achieving the universal health coverage goal: Evidence from Sub-Saharan Africa. Health Economics Review 13: 25. [Google Scholar] [CrossRef] [PubMed]
- Arhin, Kwadwo, Oteng-Abayie, Eric Fosu, and Jacob Novignon. 2023b. Effects of healthcare financing policy tools on health system efficiency: Evidence from sub-Saharan Africa. Heliyon 9: e20573. [Google Scholar] [CrossRef] [PubMed]
- Atilgan, Emre, H. Murat Ertuğrul, Onur Baycan, and Hakan Ulucan. 2024. Health-led growth hypothesis and health financing systems: An econometric synthesis for OECD countries. Frontiers in Public Health 12: 1437304. [Google Scholar] [CrossRef]
- Bala, Muhammad Muazu, Shailender Singh, and Dhruba Kumar Gautam. 2023. Stochastic frontier approach to efficiency analysis of health facilities in providing services for non-communicable diseases in eight LMICs. International Health 15: 512–25. [Google Scholar] [CrossRef]
- Balkhi, Bander, Dhfer Alshayban, and Nawaf M. Alotaibi. 2021. Impact of Healthcare Expenditures on Healthcare Outcomes in the Middle East and North Africa (MENA) Region: A Cross-Country Comparison, 1995–2015. Frontiers in Public Health 8: 624962. [Google Scholar] [CrossRef]
- Baltgailis, Jurijs, and Anastasiia Simakhova. 2022. The Technological Innovations of Fintech Companies to Ensure the Stability of the Financial System in Pandemic Times. Marketing and Management of Innovations 2: 55–65. [Google Scholar] [CrossRef]
- Bashir, Saima, Grasic Muhammad Nasir, Katja Grasic, Marc Moulin, and Shehzad Ali. 2022. Association between efficiency and quality of care of public healthcare facilities: Evidence from Pakistan. The International Journal of Health Planning and Management 37: 2240–55. [Google Scholar] [CrossRef] [PubMed]
- Behera, Deepak Kumar, and Umakant Dash. 2018. Healthcare financing in South-East Asia: Does fiscal capacity matter? International Journal of Healthcare Management 13 Suppl. S1: 375–84. [Google Scholar] [CrossRef]
- Behera, Deepak Kumar, and Umakant Dash. 2019. Impact of macro-fiscal determinants on health financing: Empirical evidence from low-and middle-income countries. Global Health Research and Policy 4: 1–13. [Google Scholar] [CrossRef]
- Bein, Murad A., Dogan Unlucan, Globalahan Olowu, and Wagdi Kalifa. 2017. Healthcare spending and health outcomes: Evidence from selected East African countries. African Health Sciences 17: 247–54. [Google Scholar] [CrossRef] [PubMed]
- Beylik, Umut, Umit Cirakli, Murat Cetin, Eyyup Ecevit, and Osman Senol. 2022. The relationship between health expenditure indicators and economic growth in OECD countries: A Driscoll-Kraay approach. Frontiers in Public Health 10: 1050550. [Google Scholar] [CrossRef]
- Bokhari, Farasat A. S., Yunwei Gai, and Pablo Gottret. 2007. Government health expenditures and health outcomes. Health Economics 16: 257–73. [Google Scholar] [CrossRef] [PubMed]
- Brikci, Nouria, Rotimi Alao, Hong Wang, Darius Erlangga, and Kara Hanson. 2024. Improving the efficiency in spending for health: A systematic review of evidence. SSM—Health Systems 2: 100008. [Google Scholar] [CrossRef]
- Cacace, Mirella. 2021. Case study C: Transforming healthcare financing in Central and Eastern European countries. In Handbook on Social Protection Systems. Cheltenham: Elgar, pp. 78–82. [Google Scholar] [CrossRef]
- Cetin, Volkan Recai, and Serdal Bahce. 2016. Measuring the efficiency of health systems of OECD countries by data envelopment analysis. Applied Economics 48: 3497–507. [Google Scholar] [CrossRef]
- Charnes, Abraham, William W. Cooper, and E. L. Rhodes. 1978. Measuring the efficiency of decision making units. European Journal of Operational Research 2: 429–44. [Google Scholar] [CrossRef]
- Chen, Qiuxing, Qiaozhu Chi, Yang Chen, Oleksii Lyulyov, and Tetyana Pimonenko. 2022. Does population aging impact China’s economic growth? International Journal of Environmental Research and Public Health 19: 12171. [Google Scholar] [CrossRef] [PubMed]
- Chitnis, Asmita, and Dharmesh K. Mishra. 2019. Performance Efficiency of Indian Private Hospitals Using Data Envelopment Analysis and Super-efficiency DEA. Journal of Health Management 21: 279–93. [Google Scholar] [CrossRef]
- Choonara, Shakira, and John Eyles. 2016. Out of control: Profit-seeking behaviour, unnecessary medical procedures and rising costs of private medical care in South Africa. BMJ Glob Health 1: e000013. [Google Scholar] [CrossRef]
- Christodoulou, Demetris, and Vasilis Sarafidis. 2017. Regression clustering for panel-data models with fixed effects. The Stata Journal 17: 314–329. [Google Scholar] [CrossRef]
- Cole, Wade M. 2019. Wealth and health revisited: Economic growth and well-being in developing countries, 1970 to 2015. Social Science Research 77: 45–67. [Google Scholar] [CrossRef]
- Dacko-Pikiewicz, Zdzislawa. 2019. Building a family business brand in the context of the concept of stakeholder-oriented value. Forum Scientiae Oeconomia 7: 37–51. [Google Scholar] [CrossRef]
- Das, Tiken. 2024. Impact of Health and Non-health Inputs on Health Outcomes: A Comparative Study of South Asia, Southeast Asia, BRICS and ASEAN Regions. Arthaniti: Journal of Economic Theory and Practice 23: 09767479241256168. [Google Scholar] [CrossRef]
- Davidson, Alan. 2015. Social Determinants of Health: A Comparative Approach. Oxford: Oxford University Press. 296p. [Google Scholar]
- Dollar, David, and Aart Kraay. 2002. Growth Is Good for the Poor. Journal of Economic Growth 7: 195–225. [Google Scholar] [CrossRef]
- Domapielle, Maximillian Kolbe, Joshua Sumankuuro, and Frederick Der Bebelleh. 2022. Revisiting the debate on health financing in Low and Middle-income countries: An integrative review of selected models. The International Journal of Health Planning and Management 37: 3061–74. [Google Scholar] [CrossRef]
- Dong, Zhiwei, Liping Wu, Yang Chen, Oleksii Lyulyov, and Tetyana Pimonenko. 2022. Intergenerational transmission of obesity: Role of education and income. International Journal of Environmental Research and Public Health 19: 15931. [Google Scholar] [CrossRef]
- Fogel, Robert William. 1997. New findings on secular trends in nutrition and mortality: Some implications for population theory. Handbook of Population and Family Economics 1A: 433–81. [Google Scholar] [CrossRef]
- Frank, Sarah M., Jacqui Webster, Briar McKenzie, Pascal Geldsetzer, Jennifer Manne-Goehler, Glennis Andall-Brereton, Corine Houehanou, Dismand Houinato, Mongal Singh Gurung, Brice Wilfried Bicaba, and et al. 2019. Consumption of fruits and vegetables among individuals 15 years and older in 28 low- and middle-income countries. Journal of Nutrition 149: 1252–59. [Google Scholar] [CrossRef] [PubMed]
- Frimpong, Prince Boakye, and George Adu. 2014. Population health and economic growth in Sub-Saharan Africa: A panel cointegration analysis. Journal of African Business 15: 36–48. [Google Scholar] [CrossRef]
- Fujii, Tomoki. 2018. Sources of health financing and health outcomes: A panel data analysis. Health Economics 27: 1996–2015. [Google Scholar] [CrossRef] [PubMed]
- Gallardo-Albarran, Daniel. 2018. Health and economic development since 1900. Economics & Human Biology 31: 228–37. [Google Scholar] [CrossRef]
- Gallet, Craig A., and Hristos Doucouliagos. 2017. The impact of healthcare spending on health outcomes: A meta-regression analysis. Social Science & Medicine 179: 9–17. [Google Scholar] [CrossRef]
- Gaylong, Ruchi, Vijay Kumar Tiwari, and T. P. Sherin Raj. 2023. Planning and financing of RMNCH+ A under National Health Mission: A case study of the Gurugram District of Haryana State. The International Journal of Health Planning and Management 38: 951–66. [Google Scholar] [CrossRef]
- Greene, William. 2004. Distinguishing between heterogeneity and inefficiency: Stochastic frontier analysis of the World Health Organization’s panel data on national health care systems. Health Economics 13: 959–80. [Google Scholar] [CrossRef]
- Grigoli, Francesco, and Javier Kapsoli. 2018. Waste not, want not: The efficiency of health expenditure in emerging and developing economies. Review of Development Economics 22: 384–403. [Google Scholar] [CrossRef]
- Grigorakis, Nikolaos, Christos Floros, Haritini Tsangari, and Evangelos Tsoukatos. 2018. Macroeconomic and financing determinants of out of pocket payments in health care: Evidence from selected OECD countries. Journal of Policy Modeling 40: 1290–312. [Google Scholar] [CrossRef]
- Hadad, Sharon, Yossi Hadad, and Tzahit Simon-Tuval. 2013. Determinants of healthcare system’s efficiency in OECD countries. The European Journal of Health Economics 14: 253–65. [Google Scholar] [CrossRef] [PubMed]
- Hamidi, Samer, and Fevzi Akinci. 2016. Measuring Efficiency of Health Systems of the Middle East and North Africa (MENA) Region Using Stochastic Frontier Analysis. Applied Health Economics and Health Policy 14: 337–47. [Google Scholar] [CrossRef]
- Hamzah, Nurhafiza Md, Ming-Miin Yu, and Kok Fong See. 2021. Assessing the efficiency of Malaysia health system in COVID-19 prevention and treatment response. Health Care Management Science 24: 273–85. [Google Scholar] [CrossRef]
- Herrera, Santiago, and Gaobo Pang. 2005. Efficiency of Public Spending in Developing Countries: An Efficiency Frontier Approach. In Policy Research Working Paper. Washington, DC: The World Bank, vol. 3645. [Google Scholar] [CrossRef]
- Hollingsworth, Bruce. 2003. Non-parametric and parametric applications measuring efficiency in health care. Health care Management Science 6: 203–18. [Google Scholar] [CrossRef]
- Infante-Moro, Juan C. Infante-Moro Alfonso, and Julia Gallardo-Pérez. 2020. Motivational factors that justify the implementation of the Internet of things as a security system in the hotel sector. Revista de Pensamiento Estrategico y Seguridad CISDE 5: 81–91. [Google Scholar]
- Infante-Moro, Juan C. Infante-Moro Alfonso, and Julia Gallardo-Pérez. 2022. Key factors to raise cybersecurity awareness among employees. Revista de Pensamiento Estrategico y Seguridad CISDE 7: 69–79. [Google Scholar]
- Ivanková, V. Viera, Martin Rigelský, Kotulič Rastislav, and Jaroslav Gonos. 2020. The governance of efficient healthcare financing system in OECD countries. Polish Journal of Management Studies 21: 179–94. [Google Scholar] [CrossRef]
- Izón, Germán M., and Chelsea A. Pardini. 2017. Cost inefficiency under financial strain: A stochastic frontier analysis of hospitals in Washington State through the Great Recession. Health Care Management Science 20: 232–45. [Google Scholar] [CrossRef]
- Jetter, Michael, Sabine Laudage, and David Stadelmann. 2019. The intimate link between income levels and life expectancy: Global evidence from 213 years. Social Science Quarterly 100: 1387–403. [Google Scholar] [CrossRef]
- Kadar, Beata, and Regina Zsuzsanna Reicher. 2020. Innovations in health care management: The effect of the pandemic on the labour market change. Marketing and Management of Innovations 4: 120–30. [Google Scholar] [CrossRef]
- Kakabadse, Nada K., Cécile Rozuel, and Linda Lee-Davies. 2005. Corporate social responsibility and stakeholder approach: A conceptual review. International Journal of Business Governance and Ethics 1: 277–302. [Google Scholar] [CrossRef]
- Kang, Jing, Rong Peng, Jung Feng, Junyuan Wei, Zhen Li, Fen Huang, Fu Yu, Xiaorong Su, Yujun Chen, Xianjing Qin, and et al. 2023. Health systems efficiency in China and ASEAN, 2015–2020: A DEA-Tobit and SFA analysis application. BMJ Open 13: e075030. [Google Scholar] [CrossRef] [PubMed]
- Karagiannis, Roxani. 2015. A system-of-equations two-stage DEA approach for explaining capacity utilization and technical efficiency. Annals of Operations Research 227: 25–43. [Google Scholar] [CrossRef]
- Kaya Samut, Pınar, and Reyhan Cafrı. 2016. Analysis of the Efficiency Determinants of Health Systems in OECD Countries by DEA and Panel Tobit. Social Indicators Research 129: 113–32. [Google Scholar] [CrossRef]
- Khan, Muhammad Arshad, and Muhammad Iftikhar Ul Husnain. 2019. Is health care a luxury or necessity good? Evidence from Asian countries. International Journal of Health Economics and Management 19: 213–33. [Google Scholar] [CrossRef]
- Kohl, Sebastian, Fügener Jan Schoenfelder, and Jens O. Brunner Andreas. 2019. The use of Data Envelopment Analysis (DEA) in healthcare with a focus on hospitals. Health Care Management Science 22: 245–86. [Google Scholar] [CrossRef]
- Kujawska, Justyna. 2021. Efficiency of healthcare systems in European countries—The DEA network approach. Quantitative Methods in Economics XIX: 60–70. [Google Scholar] [CrossRef]
- Kulkarni, Lalitagauri. 2016. Health inputs, health outcomes and public health expenditure: Evidence from the BRICS countries. International Journal of Applied Economics 31: 72–84. [Google Scholar]
- Kumbhakar, Subal C., and C. A. Knox Lovell. 2000. Stochastic Frontier Analysis. Cambridge: Cambridge University Press. [Google Scholar]
- Kwilinski, Aleksy. 2023. The Relationship between Sustainable Development and Digital Transformation: Bibliometric Analysis. Virtual Economics 6: 56–69. [Google Scholar] [CrossRef]
- Kwilinski, Aleksy, Katarzyna Szczepańska-Woszczyna, Oleksii Lyulyov, and Tetyana Pimonenko. 2024a. Government Effectiveness and Immigrant Outflows: Their Role in Advancing Greenfield Investment Globally and Regionally. Polish Journal of Management Studies 29: 365–79. [Google Scholar] [CrossRef]
- Kwilinski, Aleksy, Katarzyna Szczepańska-Woszczyna, Oleksii Lyulyov, and Tetyana Pimonenko. 2024b. Digital Public Services: Catalysts for Healthcare Efficiency. Journal of Open Innovation: Technology, Market, and Complexity 10: 100319. [Google Scholar] [CrossRef]
- Kwilinski, Aleksy, Oleksandr Vyshnevskyi, and Henryk Dzwigol. 2020. Digitalization of the EU Economies and People at Risk of Poverty or Social Exclusion. Journal of Risk and Financial Management 13: 142. [Google Scholar] [CrossRef]
- Kwilinski, Aleksy, Peter Merritt, and Lukasz Wroblewski. 2024c. Advancing Sustainable Development Goals through Digital Culture: A Global Research Overview. Cultural Management: Science and Education 8: 61–80. [Google Scholar] [CrossRef]
- Legido-Quigley, Helena, Asgari Nima, Teo Yik Ying, Leung Gabriel, Oshitani Hitoshi, Fukuda Keiji, Cook Alex, Yang Hsu Li, Shibuya Kenji, and David Heymann. 2020. Are high-performing health systems resilient against the COVID-19 epidemic? Lancet 395: 848–50. [Google Scholar] [CrossRef]
- Letunovska, Nataliia, Oleksii Lyulov, and Tetyana Pimonenko. 2024. COVID-19’s impact on the competitiveness of the national health social systems: A comparative analysis of the pre-vaccination and vaccination periods. AIP Conference Proceedings 3033: 020008. [Google Scholar]
- Letunovska, Nataliia, Rafis Abazov, and Yang Chen. 2022. Framing a Regional Spatial Development Perspective: The Relation between Health and Regional Performance. Virtual Economics 5: 87–99. [Google Scholar] [CrossRef]
- Li, Jiannan, and Bocong Yuan. 2019. Understanding the effectiveness of government health expenditure in improving health equity: Preliminary evidence from global health expenditure and child mortality rate. The International Journal of Health Planning and Management 34: e1968–79. [Google Scholar] [CrossRef] [PubMed]
- Liu, Hui, and Kaiyang Zhong. 2022. Relationship between health spending, life expectancy and renewable energy in China: A new evidence from the VECM approach. Frontiers in Public Health 10: 993546. [Google Scholar] [CrossRef] [PubMed]
- Lupu, Dan, and Ramona Tiganasu. 2022. COVID-19 and the efficiency of health systems in Europe. Health Economics Review 12: 14. [Google Scholar] [CrossRef]
- McKeown, Thomas. 1976. The Modern Rise of Population. Cambridge: Academic Press. 168p. [Google Scholar]
- Medeiros, João, and Christoph Schwierz. 2015. Efficiency Estimates of Health Care Systems in the EU. Europen Economy. Economic Papers 549. Available online: https://ec.europa.eu/economy_finance/publications/economic_paper/2015/pdf/ecp549_en.pdf (accessed on 1 February 2024).
- Melnychenko, Oleksandr. 2021. The Energy of Finance in Refining of Medical Surge Capacity. Energies 14: 210. [Google Scholar] [CrossRef]
- Mitchell, Marc, and Lena Kan. 2019. Digital Technology and the Future of Health Systems. Health Systems & Reform 5: 113–20. [Google Scholar] [CrossRef]
- Nakatani, Ryota, Qianqian Zhang, and Isaura Garcia Valdes. 2022. Fiscal Decentralization Improves Social Outcomes When Countries Have Good Governance. In IMF Working Papers. Washington, DC: IMF. [Google Scholar] [CrossRef]
- Nakatani, Ryota, Qianqian Zhang, and Isaura Garcia Valdes. 2024. Expenditure Decentralization and Health Outcomes: The Importance of Governance. The Journal of Federalism 54: 59–87. [Google Scholar] [CrossRef]
- Newhouse, Joseph P. 1994. Frontier estimation: How useful a tool for health economics? Journal of Health Economics 13: 317–22. [Google Scholar] [CrossRef] [PubMed]
- Novignon, Jacob, and Kwasi Gyabaa Tabiri. 2022. Leveraging COVID-19 pandemic response for improved health system financing: Lessons from Ghana. The International Journal of Health Planning and Management 37: 2211–23. [Google Scholar] [CrossRef]
- Obrizan, Maksym, and George L. Wehby. 2018. Health Expenditures and Global Inequalities in Longevity. World Development 101: 28–36. [Google Scholar] [CrossRef]
- Onofrei, Mihaela, Anca-Florentina Vatamanu, Georgeta Vintilă, and Elena Cigu. 2021. Government Health Expenditure and Public Health Outcomes: A Comparative Study among EU Developing Countries. International Journal of Environmental Research and Public Health 18: 10725. [Google Scholar] [CrossRef]
- Orea, Luis, and Subal C. Kumbhakar. 2004. Efficiency measurement using a latent class stochastic frontier model. Empirical Economics 29: 169–18. [Google Scholar] [CrossRef]
- Raghupathi, Viju, and Wullianallur Raghupathi. 2020. The influence of education on health: An empirical assessment of OECD countries for the period 1995–2015. Archives of Public Health 78: 20. [Google Scholar] [CrossRef]
- Rahman, Mohammad Mafizur, Rasheda Khanam, and Maisha Rahman. 2018. Health care expenditure and health outcome nexus: New evidence from the SAARC-ASEAN region. Globalization and Health 14: 113. [Google Scholar] [CrossRef]
- Rajiani, Ismi, and Sebastian Kot. 2020. Javanese Indonesia: Human Resource Management Issues in a Uniquely Collectivist Culture. Cultural Management: Science and Education 4: 9–21. [Google Scholar] [CrossRef]
- Rechel, Bernd. 2019. Funding for public health in Europe in decline? Health Policy 123: 21–26. [Google Scholar] [CrossRef] [PubMed]
- Rokicki, Tomasz, Aleksandra Perkowska, and Marcin Ratajczak. 2021. Differentiation in Healthcare Financing in EU Countries. Sustainability 13: 251. [Google Scholar] [CrossRef]
- Rosko, Michael D., and Ryan L. Mutter. 2008. Stochastic frontier analysis of hospital inefficiency: A review of empirical issues and an assessment of robustness. Medical Care Research and Review: MCRR 65: 131–66. [Google Scholar] [CrossRef]
- Saltman, Richard B. 2018. The impact of slow economic growth on health sector reform: A cross-national perspective. Health Economics, Policy, and Law 13: 382–405. [Google Scholar] [CrossRef] [PubMed]
- Sango-Coke, Elizabeth Yinka, and Murad A. Bein. 2018. The Impact of Healthcare spending on Life Expectancy: Evidence from Selected West African Countries. African Journal of Reproductive Health 22: 64–71. [Google Scholar]
- Sanjeev, Gupta, and Marijn Verhoeven. 2001. The efficiency of government expenditure: Experiences from Africa. Journal of Policy Modelling 23: 433–467. [Google Scholar] [CrossRef]
- Sarafidis, Vasilis, and Neville Weber. 2015. A partially heterogeneous framework for analysing panel data. Oxford Bulletin of Economics and Statistics 77: 274–96. [Google Scholar] [CrossRef]
- Sarker, Abdur Razzaque, Marufa Sultana, Khorshed Alam, Nausad Ali, Nurnabi Sheikh, Raisul Akram, and Alec Morton. 2021. Households’ out-of-pocket expenditure for healthcare in Bangladesh: A health financing incidence analysis. The International Journal of Health Planning and Management 36: 2106–117. [Google Scholar] [CrossRef]
- Sen, Anindya. 2005. Is Health Care a Luxury? New Evidence from OECD Data. International Journal of Health Care Finance and Economics 5: 147–64. [Google Scholar] [CrossRef]
- Senaratne, Malshini, Andrew Zimbroff, and Jared T. Stevens. 2021. An instrument to assess Blue Economy entrepreneurship eco-systems: A case study from the Seychelles. Journal of the Indian Ocean Region 17: 205–23. [Google Scholar] [CrossRef]
- Shahbaz, Muhammad, Muhammad Shafiullah, and Mantu K. Mahalik. 2019. The dynamics of financial development, globalisation, economic growth and life expectancy in sub-Saharan Africa. Australian Economic Papers 58: 444–79. [Google Scholar] [CrossRef]
- Shimul, Shafiun Nahin, Muhammad Ihsan Kabir, and Fariha Kadir. 2023. Resiliency of healthcare expenditure to income shock: Evidence from dynamic heterogeneous panels. Frontiers in Public Health 11: 1085338. [Google Scholar] [CrossRef] [PubMed]
- Skinner, Jonathan. 1994. What do stochastic frontier cost functions tell us about inefficiency? Journal of Health Economics 13: 323–28. [Google Scholar] [CrossRef]
- Smiianov, Vladyslav, Oleksii Lyulyov, Tetyana Pimonenko, Tetyana Andrushchenko, Serhii Sova, and Natalia Grechkovskaya. 2020. The impact of the pandemic lockdown on air pollution, health and economic growth: System dynamics analysis. Wiadomości Lekarskie LXXIII: 2332–8. [Google Scholar] [CrossRef]
- Stata Software. 2024. Available online: https://www.stata.com/ (accessed on 1 February 2024).
- Stefko, Robert, Beata Gavurova, and Kristina Kocisova. 2018. Healthcare efficiency assessment using DEA analysis in the Slovak Republic. Health Economics Review 8: 6. [Google Scholar] [CrossRef]
- Sülkü, Seher Nur, Alper Mortaş, and Aziz Küçük. 2023. Measuring efficiency of public hospitals under the impact of COVID-19: The case of Türkiye. Cost Effectiveness and Resource Allocation 21: 70. [Google Scholar] [CrossRef]
- Szczepańska-Woszczyna, Katarzyna, and Sylwia Gatnar. 2022. Key Competences of Research and Development Project Managers in High Technology Sector. Forum Scientiae Oeconomia 10: 107–30. [Google Scholar] [CrossRef]
- Szczepańska-Woszczyna, Katarzyna, Vysochyna Alina, and Aleksy Kwilinski. 2024. Public Health Efficiency and Country Competitiveness: Empirical Study in Pre-Pandemic and Pandemic Periods. Forum Scientiae Oeconomia 12: 151–66. [Google Scholar] [CrossRef]
- Teoh, Jeremy Yuen-Chun, Junjie Huang, Wendy Yuet-Kiu Ko, Veeleah Lok, Peter Choi, Chi-Fai Ng, Shomik Sengupta, Hugh Mostafid, Ashish M. Kamat, Peter C. Black, and et al. 2020. Global trends of bladder cancer incidence and mortality, and their associations with tobacco use and gross domestic product per capita. European Urology 78: 893–906. [Google Scholar] [CrossRef]
- Tigga, Nutan Shashi, and Udaya S. Mishra. 2015. On measuring technical efficiency of the health system in India: An application of data envelopment analysis. Journal of Health Management 17: 285–98. [Google Scholar] [CrossRef]
- Ullah, Irfan, Assad Ullah, Sher Ali, Petra Poulova, Ahsan Akbar, Muhammad Haroon Shah, Alam Rehman, Muhammad Zeeshan, and Fakhr E. Alam Afridi. 2021. Public Health Expenditures and Health Outcomes in Pakistan: Evidence from Quantile Autoregressive Distributed Lag Model. Risk Management and Healthcare Policy 14: 3893–909. [Google Scholar] [CrossRef]
- Vargas Bustamante, Arturo, and Sandhya V. Shimoga. 2018. Comparing the Income Elasticity of Health Spending in Middle-Income and High-Income Countries: The Role of Financial Protection. International Journal of Health Policy and Management 7: 255–63. [Google Scholar] [CrossRef] [PubMed]
- Veckalne, Regina, Martins Kapustins, and Tatjana Tambovceva. 2023. Smart Cities, Green Diets: How the Lucy Veg App Supports Valencia’s Vegan Community and Contributes to SDGs. Virtual Economics 6: 7–22. [Google Scholar] [CrossRef] [PubMed]
- Waitzberg, Ruth, Wilm Quentin, Erin Webb, and Sherry Glied. 2021. The Structure and Financing of Health Care Systems Affected How Providers Coped With COVID-19. The Milbank Quarterly 99: 542–64. [Google Scholar] [CrossRef]
- Wang, Fuhmei. 2015. More Health Expenditure, Better Economic Performance? Empirical Evidence From OECD Countries. Inquiry: A Journal of Medical Care Organization, Provision and Financing 52: 0046958015602666. [Google Scholar] [CrossRef]
- Wei, Xiaolong, Tao Wang, Yang Chen, Oleksii Lyulyov, and Tetyana Pimonenko. 2023. The Effects of Population Aging on Sports Industry Development: The Mediating Effect of Technological Innovation. International Journal of Environmental Research and Public Health 20: 2085. [Google Scholar] [CrossRef] [PubMed]
- World Bank. 2024. Data Bank. Health Nutrition and Population Statistics. Available online: http://databank.worldbank.org/data/home.aspx (accessed on 1 February 2024).
- Wróblewski, Łukasz, and Marcin Lis. 2021. Marketing Mix of Cultural Institutions on the Cross-Border Market of a City Divided by a Border—An Analysis and Evaluation. Polish Journal of Management Studies 23: 555–72. [Google Scholar] [CrossRef]
- Xu, Wangzi, and Jia Lin. 2022. Fiscal Decentralization, Public Health Expenditure and Public Health–Evidence From China. Frontiers in Public Health 10: 773728. [Google Scholar] [CrossRef]
- Ye, Liping, and Xinping Zhang. 2018. Nonlinear Granger Causality between Health Care Expenditure and Economic Growth in the OECD and Major Developing Countries. International Journal of Environmental Research and Public Health 15: 1953. [Google Scholar] [CrossRef]
- Zeng, Meng, and Lu Niu. 2023. Spatiotemporal patterns of healthy life expectancy and the effects of health financing in West African countries, 1995–2019: A Spatial Panel Modelling Study. Journal of Global Health 13: 04123. [Google Scholar] [CrossRef] [PubMed]
- Zeng, Wu, Yao Yao, Hélène Barroy, Jonathan Cylus, and Guohong Li. 2020. Improving fiscal space for health from the perspective of efficiency in low- and middle-income countries: What is the evidence? Journal of Global Health 10: 020421. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).

