History of Brain Injury Alters Cerebral Haemodynamic Oscillations with Cardiac Influence
Abstract
1. Introduction
2. Materials and Methods
Statistical Analysis
3. Results
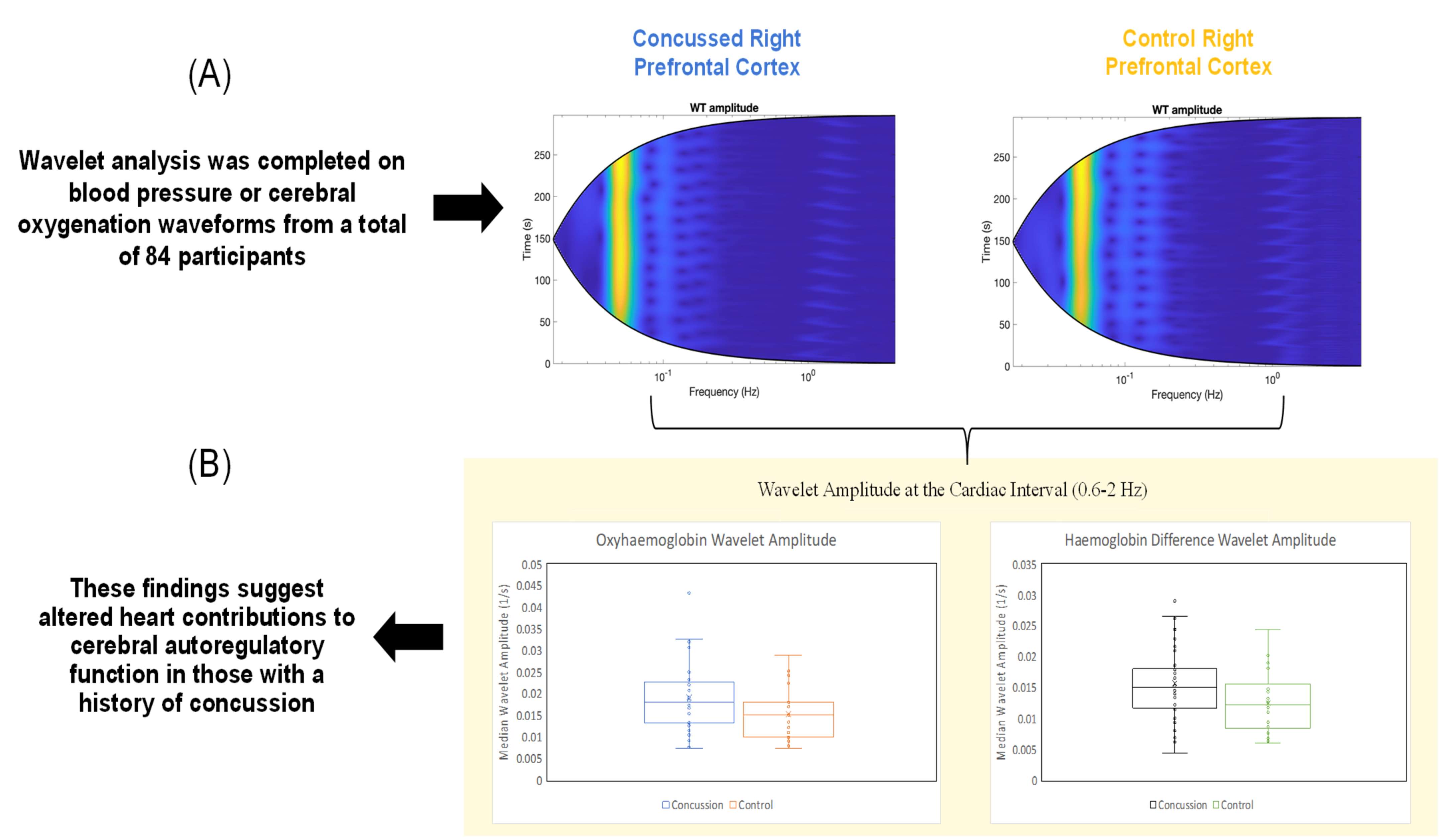
3.1. Pre-Frontal Cortex Oxygenation (NIRS Parameters)
3.2. Blood Pressure (BP)
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Bailey, D.M.; Jones, D.W.; Sinnott, A.; Brugniaux, J.V.; New, K.J.; Hodson, D.; Marley, C.J.; Smirl, J.D.; Ogoh, S.; Ainslie, P.N. Impaired cerebral haemodynamic function associated with chronic traumatic brain injury in professional boxers. Clin. Sci. 2013, 124, 177–189. [Google Scholar] [CrossRef] [PubMed]
- Bishop, S.; Dech, R.; Baker, T.; Butz, M.; Aravinthan, K.; Neary, J.P. Parasympathetic baroreflexes and heart rate variability during acute stage of sport concussion recovery. Brain Inj. 2017, 31, 247–259. [Google Scholar] [CrossRef] [PubMed]
- Bishop, S.A.; Dech, R.T.; Guzik, P.; Neary, J.P. Heart rate variability and implication for sport concussion. Clin. Physiol. Funct. Imaging 2018, 38, 733–742. [Google Scholar] [CrossRef] [PubMed]
- Bishop, S.A.; Neary, J.P. Assessing prefrontal cortex oxygenation after sport concussion with near-infrared spectroscopy. Clin. Physiol. Funct. Imaging 2018, 38, 573–585. [Google Scholar] [CrossRef]
- Ellingson, C.J.; Singh, J.; Ellingson, C.A.; Sirant, L.W.; Krätzig, G.P.; Dorsch, K.D.; Piskorski, J.; Neary, J.P. Alterations in Baroreflex Sensitivity and Blood Pressure Variability Following Sport-Related Concussion. Life 2022, 12, 1400. [Google Scholar] [CrossRef]
- Ellis, M.J.; Cordingley, D.; Vis, S.; Reimer, K.; Leiter, J.; Russell, K. Vestibulo-ocular dysfunction in pediatric sports-related concussion. J. Neurosurg. Pediatr. 2015, 16, 248–255. [Google Scholar] [CrossRef]
- Leddy, J.; Baker, J.G.; Haider, M.N.; Hinds, A.; Willer, B. A physiological approach to prolonged recovery from sport-related concussion. J. Athl. Train. 2017, 52, 299–308. [Google Scholar] [CrossRef]
- Leddy, J.J.; Baker, J.G.; Merchant, A.; Picano, J.; Gaile, D.; Matuszak, J.; Willer, B. Brain or strain? Symptoms alone do not distinguish physiologic concussion from cervical/vestibular injury. Clin. J. Sport Med. 2015, 25, 237–242. [Google Scholar] [CrossRef]
- Leddy, J.J.; Haider, M.N.; Hinds, A.L.; Darling, S.; Willer, B.S. A Preliminary Study of the Effect of Early Aerobic Exercise Treatment for Sport-Related Concussion in Males. Clin. J. Sport Med. 2019, 29, 353–360. [Google Scholar] [CrossRef]
- Len, T.K.; Neary, J.P.; Asmundson, G.; Goodman, D.G.; Bjornson, B.; Bhambhani, Y.N. Cerebrovascular reactivity impairment after sport-induced concussion. Med. Sci. Sport. Exerc. 2011, 43, 2241–2248. [Google Scholar] [CrossRef]
- Mutch, W.A.C.; Ellis, M.J.; Ryner, L.N.; McDonald, P.J.; Morissette, M.P.; Pries, P.; Essig, M.; Mikulis, D.J.; Duffin, J.; Fisher, J.A. Patient-specific alterations in CO2 cerebrovascular responsiveness in acute and sub-acute sports-related concussion. Front. Neurol. 2018, 9, 23. [Google Scholar] [CrossRef] [PubMed]
- Tiberini, P.; D’Antona, G.; Cicchella, A. Brain Oxygenation in Post-concussion Combat Sport Athletes. Front. Sport. Act. Living 2021, 3, 725096. [Google Scholar] [CrossRef]
- Willer, B.S.; Haider, M.N.; Bezherano, I.; Wilber, C.G.; Mannix, R.; Kozlowski, K.; Leddy, J.J. Comparison of Rest to Aerobic Exercise and Placebo-like Treatment of Acute Sport-Related Concussion in Male and Female Adolescents. Arch. Phys. Med. Rehabil. 2019, 100, 2267–2275. [Google Scholar] [CrossRef]
- Len, T.; Neary, J. Cerebrovascular pathophysiology following mild traumatic brain injury. Clin. Physiol. Funct. Imaging 2011, 31, 85–93. [Google Scholar] [CrossRef] [PubMed]
- Len, T.K.; Neary, J.P.; Asmundson, G.J.; Candow, D.G.; Goodman, D.G.; Bjornson, B.; Bhambhani, Y.N. Serial monitoring of CO2 reactivity following sport concussion using hypocapnia and hypercapnia. Brain Inj. 2013, 27, 346–353. [Google Scholar] [CrossRef]
- Hocke, L.M.; Duszynski, C.C.; Debert, C.T.; Dleikan, D.; Dunn, J.F. Reduced functional connectivity in adults with persistent post-concussion symptoms: A functional near-infrared spectroscopy study. J. Neurotrauma 2018, 35, 1224–1232. [Google Scholar] [CrossRef] [PubMed]
- Fountaine, M.F.L.; Hohn, A.N.; Testa, A.J.; Weir, J.P. Attenuation of Spontaneous Baroreceptor Sensitivity after Concussion. Med. Sci. Sport. Exerc. 2019, 51, 792–797. [Google Scholar] [CrossRef]
- Balestrini, C.S.; Moir, M.E.; Abbott, K.C.; Klassen, S.A.; Fischer, L.K.; Fraser, D.D.; Shoemaker, J.K. Autonomic Dysregulation in Adolescent Concussion Is Sex- and Posture-Dependent. Clin. J. Sport. Med. 2021, 31, 257–265. [Google Scholar] [CrossRef]
- Gall, B.; Parkhouse, W.; Goodman, D. Exercise following a sport induced concussion. Br. J. Sport. Med. 2004, 38, 773–777. [Google Scholar] [CrossRef]
- Conder, R.L.; Conder, A.A. Heart rate variability interventions for concussion and rehabilitation. Front. Psychol. 2014, 5, 890. [Google Scholar] [CrossRef]
- Purkayastha, S.; Williams, B.; Murphy, M.; Lyng, S.; Sabo, T.; Bell, K.R. Reduced heart rate variability and lower cerebral blood flow associated with poor cognition during recovery following concussion. Auton. Neurosci. 2019, 220, 102548. [Google Scholar] [CrossRef] [PubMed]
- Labrecque, L.; Rahimaly, K.; Imhoff, S.; Paquette, M.; Le Blanc, O.; Malenfant, S.; Drapeau, A.; Smirl, J.D.; Bailey, D.M.; Brassard, P. Dynamic cerebral autoregulation is attenuated in young fit women. Physiol. Rep. 2019, 7, e13984. [Google Scholar] [CrossRef] [PubMed]
- Sirant, L.W.; Singh, J.; Martin, S.; Gaul, C.A.; Stuart-Hill, L.; Candow, D.G.; Mang, C.; Neary, J.P. Long-term effects of multiple concussions on prefrontal cortex oxygenation during repeated squat-stands in retired contact sport athletes. Brain Inj. 2022, 36, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Wright, A.D.; Smirl, J.D.; Bryk, K.; Fraser, S.; Jakovac, M.; Van Donkelaar, P. Sport-related concussion alters indices of dynamic cerebral autoregulation. Front. Neurol. 2018, 9, 196. [Google Scholar] [CrossRef] [PubMed]
- Singh, J.; Ellingson, C.J.; Ellingson, C.A.; Scott, P.; Neary, J.P. Cardiac cycle timing and contractility following acute sport-related concussion. Res. Sport. Med. 2022, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Champagne, A.A.; Coverdale, N.S.; Ross, A.; Chen, Y.; Murray, C.I.; Dubowitz, D.; Cook, D.J. Multi-modal normalization of resting-state using local physiology reduces changes in functional connectivity patterns observed in mTBI patients. NeuroImage Clin. 2020, 26, 102204. [Google Scholar] [CrossRef] [PubMed]
- McCuddy, W.T.; Espana, L.Y.; Nelson, L.D.; Birn, R.M.; Mayer, A.R.; Meier, T.B. Association of acute depressive symptoms and functional connectivity of emotional processing regions following sport-related concussion. Neuroimage Clin. 2018, 19, 434–442. [Google Scholar] [CrossRef]
- Niu, X.; Bai, L.; Sun, Y.; Wang, S.; Cao, J.; Sun, C.; Wang, Z.; Xu, H.; Gan, S.; Fan, G.; et al. Disruption of periaqueductal grey-default mode network functional connectivity predicts persistent post-traumatic headache in mild traumatic brain injury. J. Neurol. Neurosurg. Psychiatry 2019, 90, 326–332. [Google Scholar] [CrossRef]
- Walton, S.R.; Kerr, Z.Y.; Mannix, R.; Brett, B.L.; Chandran, A.; DeFreese, J.D.; McCrea, M.A.; Guskiewicz, K.M.; Meehan, W.P.; Echemendia, R.J. Subjective concerns regarding the effects of sport-related concussion on long-term brain health among former NFL players: An NFL-LONG study. Sport. Med. 2022, 52, 1189–1203. [Google Scholar] [CrossRef]
- Liu, H.; Chen, F.; Hartmann, V.; Khalid, S.G.; Hughes, S.; Zheng, D. Comparison of different modulations of photoplethysmography in extracting respiratory rate: From a physiological perspective. Physiol. Meas. 2020, 41, 094001. [Google Scholar] [CrossRef]
- Sharma, A.; Hind, K.; Hume, P.; Singh, J.; Neary, J.P. Neurovascular coupling by functional near infra-red spectroscopy and sport-related concussion in retired rugby players: The UK rugby health project. Front. Hum. Neurosci. 2020, 14, 42. [Google Scholar] [CrossRef] [PubMed]
- Highton, D.; Ghosh, A.; Tachtsidis, I.; Panovska-Griffiths, J.; Elwell, C.E.; Smith, M. Monitoring cerebral autoregulation after brain injury: Multimodal assessment of cerebral slow-wave oscillations using near-infrared spectroscopy. Anesth. Analg. 2015, 121, 198. [Google Scholar] [CrossRef] [PubMed]
- Mol, A.; Meskers, C.G.; Sanders, M.L.; Müller, M.; Maier, A.B.; van Wezel, R.J.; Claassen, J.A.; Elting, J.W.J. Cerebral autoregulation assessed by near-infrared spectroscopy: Validation using transcranial Doppler in patients with controlled hypertension, cognitive impairment and controls. Eur. J. Appl. Physiol. 2021, 121, 2165–2176. [Google Scholar] [CrossRef] [PubMed]
- Steiner, L.A.; Pfister, D.; Strebel, S.P.; Radolovich, D.; Smielewski, P.; Czosnyka, M. Near-infrared spectroscopy can monitor dynamic cerebral autoregulation in adults. Neurocritical. Care. 2009, 10, 122–128. [Google Scholar] [CrossRef] [PubMed]
- Thewissen, L.; Caicedo, A.; Lemmers, P.; Van Bel, F.; Van Huffel, S.; Naulaers, G. Measuring near-infrared spectroscopy derived cerebral autoregulation in neonates: From research tool toward bedside multimodal monitoring. Front. Pediatr. 2018, 6, 117. [Google Scholar] [CrossRef]
- Stefanovska, A.; Bracic, M.; Kvernmo, H.D. Wavelet analysis of oscillations in the peripheral blood circulation measured by laser Doppler technique. IEEE Trans. Biomed. Eng. 1999, 46, 1230–1239. [Google Scholar] [CrossRef]
- Li, Z.; Zhang, M.; Xin, Q.; Luo, S.; Cui, R.; Zhou, W.; Lu, L. Age-related changes in spontaneous oscillations assessed by wavelet transform of cerebral oxygenation and arterial blood pressure signals. J. Cereb. Blood Flow Metab. 2013, 33, 692–699. [Google Scholar] [CrossRef]
- Gruszecka, A.; Waskow, M.; Malkiewicz, M.A.; Neary, J.P.; Singh, J.; Teckchandani, T.; Kratzig, G.P.; Wszedybyl-Winklewska, M.; Frydrychowski, A.F.; Rumiński, J. Mild poikilocapnic hypoxia increases very low frequency haemoglobin oxygenation oscillations in prefrontal cortex. Biol. Res. 2021, 54, 39. [Google Scholar] [CrossRef]
- Gruszecki, M.; Lancaster, G.; Stefanovska, A.; Neary, J.P.; Dech, R.T.; Guminski, W.; Frydrychowski, A.F.; Kot, J.; Winklewski, P.J. Human subarachnoid space width oscillations in the resting state. Sci. Rep. 2018, 8, 3057. [Google Scholar] [CrossRef]
- McCrory, P.; Meeuwisse, W.; Dvořák, J.; Aubry, M.; Bailes, J.; Broglio, S.; Cantu, R.C.; Cassidy, D.; Echemendia, R.J.; Castellani, R.J.; et al. Consensus statement on concussion in sport-the 5(th) international conference on concussion in sport held in Berlin, October 2016. Br. J. Sport. Med. 2017, 51, 838–847. [Google Scholar] [CrossRef]
- Ellingson, C.J.; Singh, J.; Ellingson, C.A.; Dech, R.; Piskorski, J.; Neary, J.P. The influence of external stressors on physiological testing: Implication for return-to-play protocols. Curr. Res. Physiol. 2022, 5, 240–245. [Google Scholar] [CrossRef] [PubMed]
- Smirl, J.D.; Hoffman, K.; Tzeng, Y.C.; Hansen, A.; Ainslie, P.N. Methodological comparison of active- and passive-driven oscillations in blood pressure; implications for the assessment of cerebral pressure-flow relationships. J. Appl. Physiol. 2015, 119, 487–501. [Google Scholar] [CrossRef] [PubMed]
- Neary, J.P.; Singh, J.; Bishop, S.A.; Dech, R.T.; Butz, M.J.A.; Len, T.K. An Evidence-Based Objective Study Protocol for Evaluating Cardiovascular and Cerebrovascular Indices Following Concussion: The Neary Protocol. Methods Protoc. 2019, 2, 23. [Google Scholar] [CrossRef] [PubMed]
- Gruszecka, A.; Gruszecki, M.; Neary, J.P.; Singh, J.; Teckchandani, T.; Waskow, M.; Wszedybyl-Winklewska, M.; Guminski, W.; Frydrychowski, A.F.; Rumiński, J. Comparison of near infrared spectroscopy (NIRS) and near-infrared transillumination-backscattering sounding (NIR-T/BSS) methods. Sci. Rep. 2020, 10, 18668. [Google Scholar] [CrossRef]
- Bu, L.; Li, J.; Li, F.; Liu, H.; Li, Z. Wavelet coherence analysis of cerebral oxygenation signals measured by near-infrared spectroscopy in sailors: An exploratory, experimental study. BMJ Open 2016, 6, e013357. [Google Scholar] [CrossRef]
- Tan, Q.; Zhang, M.; Wang, Y.; Zhang, M.; Wang, Y.; Xin, Q.; Wang, B.; Li, Z. Frequency-specific functional connectivity revealed by wavelet-based coherence analysis in elderly subjects with cerebral infarction using NIRS method. Med. Phys. 2015, 42, 5391–5403. [Google Scholar] [CrossRef]
- Bu, L.; Wang, D.; Huo, C.; Xu, G.; Li, Z.; Li, J. Effects of poor sleep quality on brain functional connectivity revealed by wavelet-based coherence analysis using NIRS methods in elderly subjects. Neurosci. Lett. 2018, 668, 108–114. [Google Scholar] [CrossRef]
- Smith, M. Shedding light on the adult brain: A review of the clinical applications of near-infrared spectroscopy. Philos. Trans. A Math. Phys. Eng. Sci. 2011, 369, 4452–4469. [Google Scholar] [CrossRef]
- Liu, H.; Allen, J.; Khalid, S.G.; Chen, F.; Zheng, D. Filtering-induced time shifts in photoplethysmography pulse features measured at different body sites: The importance of filter definition and standardization. Physiol. Meas. 2021, 42, 074001. [Google Scholar] [CrossRef]
- Razali, N.M.; Wah, Y.B. Power comparisons of shapiro-wilk, kolmogorov-smirnov, lilliefors and anderson-darling tests. J. Stat. Model. Anal. 2011, 2, 21–33. [Google Scholar]
- Neary, J.P.; Singh, J.; Christiansen, J.P.; Teckchandani, T.A.; Potter, K.L. Causal Link between Ventricular Ectopy and Concussion. Case Rep. Med. 2020, 7154120. [Google Scholar] [CrossRef] [PubMed]
| Right-Side Pre-Frontal Cortex | Left-Side Pre-Frontal Cortex | |||||||
|---|---|---|---|---|---|---|---|---|
| Interval | HbO2 (1/s) | tHb (1/s) | HbDiff (1/s) | HbO2 (1/s) | tHb (1/s) | HbDiff (1/s) | BP (1/s) | |
| Injured | 0.052–0.145 | 0.0976 (0.0308) | 0.1016 (0.0294) | 0.0959 (0.0385) | 0.0939 (0.0290) | 0.1002 (0.0372) | 0.0975 (0.0265) | 0.0613 (0.0150) |
| 0.145–0.6 | 0.0255 (0.0096) | 0.0297 (0.0110) | 0.0203 (0.0091) | 0.0257 (0.0111) | 0.0309 (0.0110) | 0.0189 (0.0089) | 0.0429 (0.0128) | |
| 0.6–2.0 | 0.0180 (0.009) * | 0.0200 (0.0098) | 0.0150 (0.006) ** | 0.0159 (0.0081) | 0.0178 (0.0117) | 0.0140 (0.0063) | 0.1050 (0.0320) | |
| Control | 0.052–0.145 | 0.0889 (0.0343) | 0.0999 (0.0363) | 0.0936 (0.0267) | 0.0874 (0.0259) | 0.0892 (0.0357) | 0.0853 (0.0167) | 0.0571 (0.0137) |
| 0.145–0.6 | 0.0291 (0.0170) | 0.0363 (0.0206) | 0.0198 (0.0146) | 0.0229 (0.0207) | 0.0295 (0.0253) | 0.0170 (0.0150) | 0.0423 (0.0174) | |
| 0.6–2.0 | 0.0150 (0.008) * | 0.0179 (0.0105) | 0.0120 (0.006) ** | 0.0150 (0.0087) | 0.0181 (0.0089) | 0.0140 (0.0113) | 0.1014 (0.0574) | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Neary, J.P.; Singh, J.; Sirant, L.W.; Gaul, C.A.; Martin, S.; Stuart-Hill, L.; Candow, D.G.; Mang, C.S.; Kratzig, G.P. History of Brain Injury Alters Cerebral Haemodynamic Oscillations with Cardiac Influence. Brain Sci. 2022, 12, 1443. https://doi.org/10.3390/brainsci12111443
Neary JP, Singh J, Sirant LW, Gaul CA, Martin S, Stuart-Hill L, Candow DG, Mang CS, Kratzig GP. History of Brain Injury Alters Cerebral Haemodynamic Oscillations with Cardiac Influence. Brain Sciences. 2022; 12(11):1443. https://doi.org/10.3390/brainsci12111443
Chicago/Turabian StyleNeary, J. Patrick, Jyotpal Singh, Luke W. Sirant, Catherine A. Gaul, Steve Martin, Lynneth Stuart-Hill, Darren G. Candow, Cameron S. Mang, and Gregory P. Kratzig. 2022. "History of Brain Injury Alters Cerebral Haemodynamic Oscillations with Cardiac Influence" Brain Sciences 12, no. 11: 1443. https://doi.org/10.3390/brainsci12111443
APA StyleNeary, J. P., Singh, J., Sirant, L. W., Gaul, C. A., Martin, S., Stuart-Hill, L., Candow, D. G., Mang, C. S., & Kratzig, G. P. (2022). History of Brain Injury Alters Cerebral Haemodynamic Oscillations with Cardiac Influence. Brain Sciences, 12(11), 1443. https://doi.org/10.3390/brainsci12111443