Prepulse Inhibition in Cocaine Addiction and Dual Pathologies
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- European Monitoring Centre for Drugs and Drug Addiction and Europol. In EU Drug Markets Report 2019; Publications Office of the European Union: Luxembourg, 2019.
- Araos, P.; Vergara-Moragues, E.; Pedraz, M.; Pavón, F.J.; Campos Cloute, R.; Calado, M.; Ruiz, J.J.; García-Marchena, N.; Gornemann, I.; Torrens, M.; et al. Psychopathological comorbidity in cocaine users in outpatient treatment. Adicciones 2014, 26, 15–26. [Google Scholar] [CrossRef] [PubMed]
- Arias, F.; Szerman, N.; Vega, P.; Mesias, B.; Basurte, I.; Morant, C.; Ochoa, E.; Poyo, F.; Babin, F. Cocaine abuse or dependency and other pyschiatric disorders. Madrid study on dual pathology. Rev. Psiquiatr. Salud Ment. 2013, 6, 121–128. [Google Scholar] [CrossRef] [PubMed]
- Lévesque, A.; Roy, É.; Jutras-Aswad, D.; Zang, G.; Artenie, A.A.; Bruneau, J. Examining the link between psychological distress, mental health disorders and sharing behaviors among cocaine users. Addict. Behav. 2016, 62, 54–59. [Google Scholar] [CrossRef]
- Barnaby, L.; Gibson, R.C. Factors affecting completion of a 28-day inpatient substance abuse treatment programme at the University Hospital of the West Indies. West. Indian Med. J. 2008, 57, 364–368. [Google Scholar]
- Kim, J.H.; Lawrence, A.J. Drugs currently in Phase II clinical trials for cocaine addiction. Expert Opin. Investig. Drugs 2014, 23, 1105–1122. [Google Scholar] [CrossRef]
- Ligabue, K.P.; Schuch, J.B.; Scherer, J.N.; Ornell, F.; Roglio, V.S.; Assunção, V.; Rebelatto, F.P.; Hildalgo, M.P.; Pechansky, F.; Kessler, F.; et al. Increased cortisol levels are associated with low treatment retention in crack cocaine users. Addict. Behav. 2020, 103, 106260. [Google Scholar] [CrossRef]
- Arenas, M.C.; Daza-Losada, M.; Vidal-Infer, A.; Aguilar, M.A.; Miñarro, J.; Rodríguez-Arias, M. Capacity of novelty-induced locomotor activity and the hole-board test to predict sensitivity to the conditioned rewarding effects of cocaine. Physiol. Behav. 2014, 133, 152–160. [Google Scholar] [CrossRef] [PubMed]
- Arenas, M.C.; Navarro-Francés, C.I.; Montagud-Romero, S.; Miñarro, J.; Manzanedo, C. Baseline prepulse inhibition of the startle reflex predicts the sensitivity to the conditioned rewarding effects of cocaine in male and female mice. Psychopharmacology 2018, 235, 2651–2663. [Google Scholar] [CrossRef] [PubMed]
- Mateos-García, A.; Roger-Sánchez, C.; Rodriguez-Arias, M.; Miñarro, J.; Aguilar, M.A.; Manzanedo, C.; Arenas, M.C. Higher sensitivity to the conditioned rewarding effects of cocaine and MDMA in High-Novelty-Seekers mice exposed to a cocaine binge during adolescence. Psychopharmacology 2015, 232, 101–113. [Google Scholar] [CrossRef] [PubMed]
- Vidal-Infer, A.; Arenas, M.C.; Daza-Losada, M.; Aguilar, M.A.; Miñarro, J.; Rodríguez-Arias, M. High novelty-seeking predicts greater sensitivity to the conditioned rewarding effects of cocaine. Pharmacol. Biochem. Behav. 2012, 102, 124–132. [Google Scholar] [CrossRef]
- Braff, D.L.; Geyer, M.A.; Swerdlow, N.R. Human studies of prepulse inhibition of startle: Normal subjects, patient groups, and pharmacological studies. Psychopharmacology 2001, 156, 234–258. [Google Scholar] [CrossRef] [PubMed]
- Swerdlow, N.R.; Weber, M.; Qu, Y.; Light, G.A.; Braff, D.L. Realistic expectations of prepulse inhibition in translational models for schizophrenia research. Psychopharmacology 2008, 199, 331–388. [Google Scholar] [CrossRef]
- Graham, F.K. The more or less startling effects of weak prestimulation. Psychophysiology 1975, 12, 238–248. [Google Scholar] [CrossRef] [PubMed]
- Graham, F.K.; Murray, G.M. Discordant effects of weak prestimulation on magnitude and latency of the reflex blink. Physiol. Psychol. 1977, 5, 108–114. [Google Scholar] [CrossRef]
- Schell, A.M.; Wynn, J.K.; Dawson, M.E.; Sinaii, N.; Niebala, C.B. Automatic and controlled attentional processes in startle eyeblink modification: Effects of habituation of the prepulse. Psychophysiology 2000, 37, 409–417. [Google Scholar] [CrossRef]
- Francis, D.D.; Szegda, K.; Campbell, G.; Martin, W.D.; Insel, T.R. Epigenetic sources of behavioral differences in mice. Nat. Neurosci. 2003, 6, 445–446. [Google Scholar] [CrossRef]
- Greenwood, T.A.; Light, G.A.; Swerdlow, N.R.; Calkins, M.E.; Green, M.F.; Gur, R.E.; Gur, R.C.; Lazzeroni, L.C.; Nuechterlein, K.H.; Olincy, A.; et al. Gating deficit heritability and correlation with increased clinical severity in schizophrenia patients with positive family history. Am. J. Psychiatry 2016, 173, 385–391. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Quednow, B.B.; Ejebe, K.; Wagner, M.; Giakoumaki, S.G.; Bitsios, P.; Kumari, V.; Roussos, P. Meta-analysis on the association between genetic polymorphisms and prepulse inhibition of the acoustic startle response. Schizophr. Res. 2018, 198, 52–59. [Google Scholar] [CrossRef]
- Swerdlow, N.R.; Bhakta, S.G.; Rana, B.K.; Kei, J.; Chou, H.H.; Talledo, J.A. Sensorimotor gating in healthy adults tested over a 15 year period. Biol. Psychol. 2017, 123, 177–186. [Google Scholar] [CrossRef] [PubMed]
- Arenas, M.C.; Caballero-Reinaldo, C.; Navarro-Francés, C.I.; Manzanedo, C. Efecto de la cocaína sobre la inhibición por prepulso de la respuesta de sobresalto. Rev. Neurol. 2017, 65, 507–519. [Google Scholar] [CrossRef]
- Braff, D.L. Prepulse inhibition of the startle reflex: A window on the brain in schizophrenia. Curr. Top. Behav. Neurosci. 2010, 4, 349–371. [Google Scholar] [CrossRef]
- Haß, K.; Bak, N.; Szycik, G.R.; Glenthøj, B.Y.; Oranje, B. Deficient prepulse inhibition of the startle reflex in schizophrenia using a cross-modal paradigm. Biol. Psychol. 2017, 128, 112–116. [Google Scholar] [CrossRef]
- Siegel, S.J.; Talpos, J.C.; Geyer, M.A. Animal models and measures of perceptual processing in schizophrenia. Neurosci. Biobehav. Rev. 2013, 37, 2092–2098. [Google Scholar] [CrossRef]
- Swerdlow, N.R.; Light, G.A.; Sprock, J.; Calkins, M.E.; Green, M.F.; Greenwood, T.A.; Gur, R.E.; Gur, R.C.; Lazzeroni, L.C.; Nuechterlein, K.H.; et al. Deficient prepulse inhibition in schizophrenia detected by the multi-site COGS. Schizophr. Res. 2014, 152, 503–512. [Google Scholar] [CrossRef] [PubMed]
- Swerdlow, N.R.; Light, G.A.; Thomas, M.L.; Sprock, J.; Calkins, M.E.; Green, M.F.; Greenwood, T.A.; Gur, R.E.; Gur, R.C.; Lazzeroni, L.C.; et al. Deficient prepulse inhibition in schizophrenia in a multi-site cohort: Internal replication and extension. Schizophr. Res. 2018, 198, 6–15. [Google Scholar] [CrossRef] [PubMed]
- Kumari, V.; Das, M.; Hodgins, S.; Zachariah, E.; Barkataki, I.; Howlett, M.; Sharma, T. Association between violent behaviour and impaired prepulse inhibition of the startle response in antisocial personality disorder and schizophrenia. Behav. Brain Res. 2005, 158, 159–166. [Google Scholar] [CrossRef] [PubMed]
- Sedgwick, O.; Young, S.; Greer, B.; Arnold, J.; Parsons, A.; Puzzo, I.; Terracciano, M.; Das, M.; Kumari, V. Sensorimotor gating characteristics of violent men with comorbid psychosis and dissocial personality disorder: Relationship with antisocial traits and psychosocial deprivation. Schizophr. Res. 2018, 198, 21–27. [Google Scholar] [CrossRef]
- Loomans, M.M.; Tulen, J.H.M.; Van Marle, H.J.C. The startle paradigm in a forensic psychiatric setting: Elucidating psychopathy. Crim. Behav. Ment Heal. 2015, 25, 42–53. [Google Scholar] [CrossRef]
- Fuertes-Saiz, A.; Benito, A.; Mateu, C.; Carratalá, S.; Almodóvar, I.; Baquero, A.; Haro, G. Sensorimotor Gating in Cocaine-Related Disorder with Comorbid Schizophrenia or Antisocial Personality Disorder. J. Dual. Diagn. 2019, 1–11. [Google Scholar] [CrossRef]
- Swerdlow, N.R.; Caine, S.B.; Braff, D.L.; Geyer, M.A. The neural substrates of sensorimotor gating of the startle reflex: A review of recent findings and their implications. J. Psychopharmacol. 1992, 6, 176–190. [Google Scholar] [CrossRef]
- Swerdlow, N.R.; Geyer, M.A.; Braff, D.L. Neural circuit regulation of prepulse inhibition of startle in the rat: Current knowledge and future challenges. Psychopharmacology 2001, 156, 194–215. [Google Scholar] [CrossRef]
- Swerdlow, N.R.; Light, G.A. Animal Models of Deficient Sensorimotor Gating in Schizophrenia: Are They Still Relevant? Curr. Top. Behav. Neurosci. 2016, 28, 305–325. [Google Scholar] [CrossRef] [PubMed]
- Swerdlow, N.R.; Geyer, M.A. Using an animal model of deficient sensorimotor gating to study the pathophysiology and new treatments of schizophrenia. Schizophr. Bull. 1998, 24, 285–301. [Google Scholar] [CrossRef]
- Zhang, J.; Forkstam, C.; Engel, J.A.; Svensson, L. Role of dopamine in prepulse inhibition of acoustic startle. Psychopharmacology 2000, 149, 181–188. [Google Scholar] [CrossRef] [PubMed]
- Doherty, J.M.; Masten, V.L.; Powell, S.B.; Ralph, R.J.; Klamer, D.; Low, M.J.; Geyer, M.A. Contributions of dopamine D1, D2, and D3 receptor subtypes to the disruptive effects of cocaine on prepulse inhibition in mice. Neuropsychopharmacology 2008, 33, 2648–2656. [Google Scholar] [CrossRef] [PubMed]
- Mestre-Pintó, J.I.; Domingo-Salvany, A.; Martín-Santos, R.; Torrens, M. Dual diagnosis screening interview to identify psychiatric comorbidity in substance users: Development and validation of a brief instrument. Eur. Addict. Res. 2013, 20, 41–48. [Google Scholar] [CrossRef]
- Torrens, M.; Serrano, D.; Astals, M.; Pérez-Domínguez, G.; Martín-Santos, R. Diagnosing comorbid psychiatric disorders in substance abusers: Validity of the Spanish versions of the psychiatric research interview for substance and mental disorders and the structured clinical interview for DSM-IV. Am. J. Psychiatry 2004, 161, 1231–1237. [Google Scholar] [CrossRef] [PubMed]
- Sheehan, D.V.; Lecrubier, Y.; Sheehan, K.H.; Amorim, P.; Janavs, J.; Weiller, E.; Hergueta, T.; Baker, R.; Dunbar, G.C. The Mini-International Neuropsychiatric Interview (M.I.N.I.): The development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J. Clin. Psychiatry 1998, 59, 22–33. [Google Scholar]
- Levenson, M.R.; Kiehl, K.A.; Fitzpatrick, C.M. Assessing Psychopathic Attributes in a Noninstitutionalized Population. J. Pers. Soc. Psychol. 1995, 68, 151–158. [Google Scholar] [CrossRef]
- Cutler, B.; Hare, R.D. Hare Psychopathy Checklist–Revised (PCL–R). In Encyclopedia of Psychology and Law, 2nd ed.; SAGE Publications: Thousand Oaks, CA, USA, 2013. [Google Scholar] [CrossRef]
- Torrubia, R.; Ávila, C.; Moltó, J.; Caseras, X. The Sensitivity to Punishment and Sensitivity to Reward Questionnaire (SPSRQ) as a measure of Gray’s anxiety and impulsivity dimensions. Pers. Individ. Dif. 2001, 31, 837–862. [Google Scholar] [CrossRef]
- Patton, J.H.; Stanford, M.S.; Barratt, E.S. Factor structure of the barratt impulsiveness scale. J. Clin. Psychol. 1995, 51, 768–774. [Google Scholar] [CrossRef]
- Powell, S.B.; Young, J.W.; Ong, J.C.; Caron, M.G.; Geyer, M.A. Atypical antipsychotics clozapine and quetiapine attenuate prepulse inhibition deficits in dopamine transporter knockout mice. Behav. Pharmacol. 2008, 19, 562–565. [Google Scholar] [CrossRef] [PubMed]
- Swerdlow, N.R.; Talledo, J.; Sutherland, A.N.; Nagy, D.; Shoemaker, J.M. Antipsychotic effects on prepulse inhibition in normal “low gating” humans and rats. Neuropsychopharmacol 2006, 31, 2011–2021. [Google Scholar] [CrossRef] [PubMed]
- Fargotstein, M.; Hasenkamp, W.; Gross, R.; Cuthbert, B.; Green, A.; Swails, L.; Lewison, B.; Boshoven, W.; Keyes, M.; Duncan, E. The effect of antipsychotic medications on acoustic startle latency in schizophrenia. Schizophr. Res. 2018, 198, 28–35. [Google Scholar] [CrossRef]
- Kumari, V.; Antonova, E.; Geyer, M.A.; Ffytche, D.; Williams, S.C.; Sharma, T. A fMRI investigation of startle gating deficits in schizophrenia patients treated with typical or atypical antipsychotics. Int. J. Neuropsychopharmacol. 2007, 10, 463–477. [Google Scholar] [CrossRef]
- Cutler, A.J.; Goldstein, J.M.; Tumas, J.A. Dosing and switching strategies for quetiapine fumarate. Clin. Ther. 2002, 24, 209–222. [Google Scholar] [CrossRef]
- Leumann, L.; Feldon, J.; Vollenweider, F.X.; Ludewig, K. Effects of typical and atypical antipsychotics on prepulse inhibition and latent inhibition in chronic schizophrenia. Biol. Psychiatry 2002, 52, 729–739. [Google Scholar] [CrossRef]
- Greenwood, T.A.; Shutes-david, A.; Tsuang, D.W. Endophenotypes in Schizophrenia: Digging Deeper to Identify Genetic Mechanisms. J. Psychiatry Brain Sci. 2019, 4, 1–26. [Google Scholar] [CrossRef]
- Kohl, S.; Heekeren, K.; Klosterkötter, J.; Kuhn, J. Prepulse inhibition in psychiatric disorders-Apart from schizophrenia. J. Psychiatr. Res. 2013, 47, 445–452. [Google Scholar] [CrossRef]
- Gómez-Nieto, R.; Hormigo, S.; López, D.E. Prepulse Inhibition of the Auditory Startle Reflex Assessment as a Hallmark of Brainstem Sensorimotor Gating Mechanisms. Brain Sci. 2020, 10, 639. [Google Scholar] [CrossRef]
- Mansbach, R.S.; Geyer, M.A.; Braff, D.L. Dopaminergic stimulation disrupts sensorimotor gating in the rat. Psychopharmacology 1998, 94, 507–514. [Google Scholar] [CrossRef] [PubMed]
- Roussos, P.; Giakoumaki, S.G.; Bitsios, P. The Dopamine D3 Receptor Ser9Gly Polymorphism Modulates Prepulse Inhibition of the Acoustic Startle Reflex. Biol. Psychiatry 2008, 64, 235–240. [Google Scholar] [CrossRef]
- Swerdlow, N.R.; Braff, D.L.; Geyer, M.A.; Koob, G.F. Central dopamine hyperactivity in rats mimics abnormal acoustic startle response in schizophrenics. Biol. Psychiatry 1986, 21, 23–33. [Google Scholar] [CrossRef]
- Vinkers, C.H.; Risbrough, V.B.; Geyer, M.A.; Caldwell, S.; Low, M.J.; Hauger, R.L. Role of dopamine D1 and D2 receptors in CRF-induced disruption of sensorimotor gating. Pharmacol. Biochem. Behav. 2007, 86, 550–558. [Google Scholar] [CrossRef] [PubMed]
- Egerton, A.; Chaddock, C.A.; Winton-Brown, T.T.; Bloomfield, M.A.P.; Bhattacharyya, S.; Allen, P.; McGuire, P.K.; Howes, O.D. Presynaptic striatal dopamine dysfunction in people at ultra-high risk for psychosis: Findings in a second cohort. Biol. Psychiatry 2013, 74, 106–112. [Google Scholar] [CrossRef]
- Howes, O.D.; Kambeitz, J.; Kim, E.; Stahl, D.; Slifstein, M.; Abi-Dargham, A.; Kapur, S. The nature of dopamine dysfunction in schizophrenia and what this means for treatment: Meta-analysisof imaging studies. Arch. Gen. Psychiatry 2012, 69, 776–786. [Google Scholar] [CrossRef]
- Van der Elst, M.C.J.; Ellenbroek, B.A.; Cools, A.R. Cocaine strongly reduces prepulse inhibition in apomorphine-susceptible rats, but not in apomorphine-unsusceptible rats: Regulation by dopamine D2 receptors. Behav. Brain Res. 2006, 175, 392–398. [Google Scholar] [CrossRef]
- Arenas, M.C.; Blanco-gandía, M.C.; Miñarro, J.; Manzanedo, C. Prepulse Inhibition of the Startle Reflex as a Predictor of Vulnerability to Develop Locomotor Sensitization to Cocaine. Front. Behav. Neurosci. 2020, 13, 1–11. [Google Scholar] [CrossRef]
- Koob, G.F.; Volkow, N.D. Neurocircuitry of addiction. Neuropsychopharmacology 2010, 35, 217–238. [Google Scholar] [CrossRef]
- Volkow, N.D.; Wang, G.J.; Fowler, J.S.; Tomasi, D.; Telang, F. Addiction: Beyond dopamine reward circuitry. Proc. Natl. Acad. Sci. USA 2011, 108, 15037–15042. [Google Scholar] [CrossRef] [PubMed]
- Comín, M.; Redondo, S.; Daigre, C.; Grau-López, L.; Casas, M.; Roncero, C. Clinical differences between cocaine-dependent patients with and without antisocial personality disorder. Psychiatry Res. 2016, 246, 587–592. [Google Scholar] [CrossRef]
- Dumais, A.; Côté, G.; Lesage, A. Clinical and sociodemographic profiles of male inmates with severe mental illness: A comparison with voluntarily and involuntarily hospitalized patients. Can. J. Psychiatry 2010, 55, 172–179. [Google Scholar] [CrossRef] [PubMed]
- Rozya, P.; Sawicka, M.; Żochowska, A.; Bronowski, P. Strengths in patients with schizophrenia and healthy people—similarities and differences. Psychiatr. Pol. 2019, 53, 93–104. [Google Scholar] [CrossRef] [PubMed]
- Grace, A.A.; Gomes, F.V. The Circuitry of Dopamine System Regulation and its Disruption in Schizophrenia: Insights into Treatment and Prevention. Schizophr. Bull. 2019, 45, 148–157. [Google Scholar] [CrossRef] [PubMed]
- Hantsoo, L.; Golden, C.; Kornfield, S.; Grillon, C.; Epperson, C.N. Startling Differences: Using the Acoustic Startle Response to Study Sex Differences and Neurosteroids in Affective Disorders. Curr. Psychiatry 2018, 20, 40. [Google Scholar] [CrossRef] [PubMed]
- Wojciechowski, T.W. Heterogeneity in the Development of Drug Use Versatility: Risk Factors for Polydrug Use throughout the Life-Course. Subst. Use Misuse 2019, 54, 758–768. [Google Scholar] [CrossRef] [PubMed]
| Variables | Total | Control | CRD | CRD+SCZ | CRD+APD | χ2 (Sig.) |
|---|---|---|---|---|---|---|
| Marital status | ||||||
| Single | 44 (59.5%) | 8 (34.5%) | 6 (42.9%) | 18 (85.7%) | 12 (75%) | 37.672 (0.000) * |
| Married | 18 (24.3%) | 14 (60.9%) | 2 (14.3%) | 1 (4.8%) | 1 (6.3%) | |
| Separated | 2 (2.7%) | 0 | 2 (14.3%) | 0 | 0 | |
| Divorced | 10 (13.5%) | 1 (4.3%) | 4 (28.6%) | 2 (9.5%) | 3 (18.8%) | |
| Current living arrangement | ||||||
| Alone | 19 (25.7%) | 5 (21.7%) | 5 (35.7%) | 5 (23.8%) | 4 (25%) | 42.290 (0.001) * |
| Only with children | 1 (1.4%) | 0 | 0 | 0 | 1 (6.3%) | |
| With parents | 19 (25.7%) | 1 (4.3%) | 3 (21.4%) | 10 (47.6%) | 5 (31.3%) | |
| As a couple without children | 5 (6.8%) | 2 (8.7%) | 2 (14.3%) | 0 | 1 (6.3%) | |
| As a couple with children | 19 (25.7%) | 14 (60.9%) | 3 (21.4%) | 1 (4.8%) | 1 (6.3%) | |
| With friends | 6 (8.1%) | 1 (4.3%) | 0 | 4 (19%) | 1 (6.3%) | |
| Other arrangement | 5 (6.8%) | 0 | 1 (7.1%) | 1 (4.8%) | 3 (18.8%) | |
| Number of children | ||||||
| 0 | 38 (55.1%) | 9 (40.9%) | 5 (35.7%) | 17 (89.5%) | 7 (50%) | 16.578 (0.56) |
| 1 | 14 (20.3%) | 4 (18.2%) | 5 (35.7%) | 1 (5.3%) | 4 (28.6%) | |
| 2 | 14 (20.3%) | 7 (31.8%) | 3 (21.4%) | 1 (5.3%) | 3 (21.4%) | |
| 3 | 3 (4.3%) | 2 (9.1%) | 1 (7.1%) | 0 | 0 | |
| Education | ||||||
| Incomplete primary education | 23 (31.1%) | 1 (4.3%) | 2 (14.3%) | 11 (52.4%) | 9 (56.3%) | 48.038 (0.000) * |
| Incomplete vocational training | 10 (13.5%) | 3 (13%) | 5 (35.7%) | 1 (4.8%) | 1 (6.3%) | |
| Non-compulsory secondary education | 21 (28.4%) | 4 (17.4%) | 5 (35.7%) | 6 (28.6%) | 6 (37.5%) | |
| Incomplete university bachelor’s degree | 7 (9.5%) | 3 (13%) | 1 (7.1%) | 3 (14.3%) | 0 | |
| University bachelor’s degree | 5 (6.8%) | 4 (17.4%) | 1 (7.1%) | 0 | 0 | |
| Advanced university graduate or doctorate degree | 8 (10.8%) | 8 (34.8%) | 0 | 0 | 0 | |
| Employment status | ||||||
| Other arrangement | 1 (1.4%) | 0 | 0 | 1 (4.8%) | 0 | 81.262 (0.000) * |
| Student or studying for public servant exams | 3 (4.1%) | 3 (13%) | 0 | 0 | 0 | |
| Permanent disability or pensioner | 23 (31.1%) | 0 | 2 (14.3%) | 15 (71.4%) | 6 (37.5%) | |
| Unemployed, having previously worked | 18 (24.3%) | 0 | 5 (35.7%) | 5 (23.8%) | 8 (50%) | |
| Unemployed, not having previously worked | 2 (2.7%) | 0 | 1 (7.1%) | 0 | 1 (6.3%) | |
| Unpaid employment in a family business | 1 (1.4%) | 0 | 1 (7.1%) | 0 | 0 | |
| On a temporary contract or temporary employment relationship | 6 (8.1%) | 3 (13%) | 3 (21.4%) | 0 | 0 | |
| In a permanent employment relationship or contract, or self-employed | 20 (27%) | 17 (73.9%) | 2 (14.3%) | 0 | 1 (6.3%) |
| Variables | CRD | CRD+SCZ | CRD+APD | F/χ2 (Sig.) |
|---|---|---|---|---|
| Cocaine | ||||
| Addiction % (n) | 100 (14) | 100 (21) | 100 (16) | - |
| Addiction severity | 7.14 (1.83) | 7.67 (2.72) | 7.75 (1.77) | 0.32 (0.724) |
| Age at onset of use | 23.71 (6.62) | 18.81 (4.03) | 18.88 (6.13) | 3.97 (0.025) * |
| Age at onset of addiction | 27.64 (7.92) | 20.24 (4.13) | 20.44 (7.33) | 6.64 (0.003) ** |
| Weekly use | 4–6 days | Less than a day | Daily | 13.98 (0.058) |
| Route of use | Intranasal | Intranasal | Smoked/Injected | 11.08 (0.022) * |
| Nicotine Addiction % (n) | 92.3 (12) | 100 (20) | 93.3 (14) | 1.50 (0.470) |
| Alcohol Addiction % (n) | 50 (7) | 66.7 (14) | 56.3 (9) | 1.02 (0.671) |
| Cannabis Addiction % (n) | 57.1 (8) | 76.2 (16) | 75 (12) | 1.68 (0.462) |
| Amphetamine Addiction % (n) | 7.1 (1) | 9.5 (2) | 25 (4) | 2.54 (0.346) |
| Heroin Addiction % (n) | 42.9 (6) | 19 (4) | 87.5 (14) | 17.21 (<0.001) ** |
| Other opiates Addiction % (n) | 0 | 0 | 12.5 (2) | 4.55 (0.166) |
| Sedatives Addiction % (n) | 14.3 (2) | 14.3 (3) | 62.5 (10) | 12.29 (0.002) ** |
| Antipsychotics | ||||
| Treatment % (n) | 25 (3) | 100 (19) | 12.5 (2) | 50.48 (<0.001) ** |
| Mean daily dose 1 | 0.45 (0.39) | 90.09 (52.09) | 0.11 (0.08) | 6.88 (0.006) ** |
| Quetiapine | ||||
| Treatment % (n) | 33.3 (4) | 73.7 (14) | 16.7 (2) | 10.77 (0.004) ** |
| Mean daily dose | 381.25 (251.14) | 514.28 (292.48) | 100 (70.71) | 2.09 (0.154) |
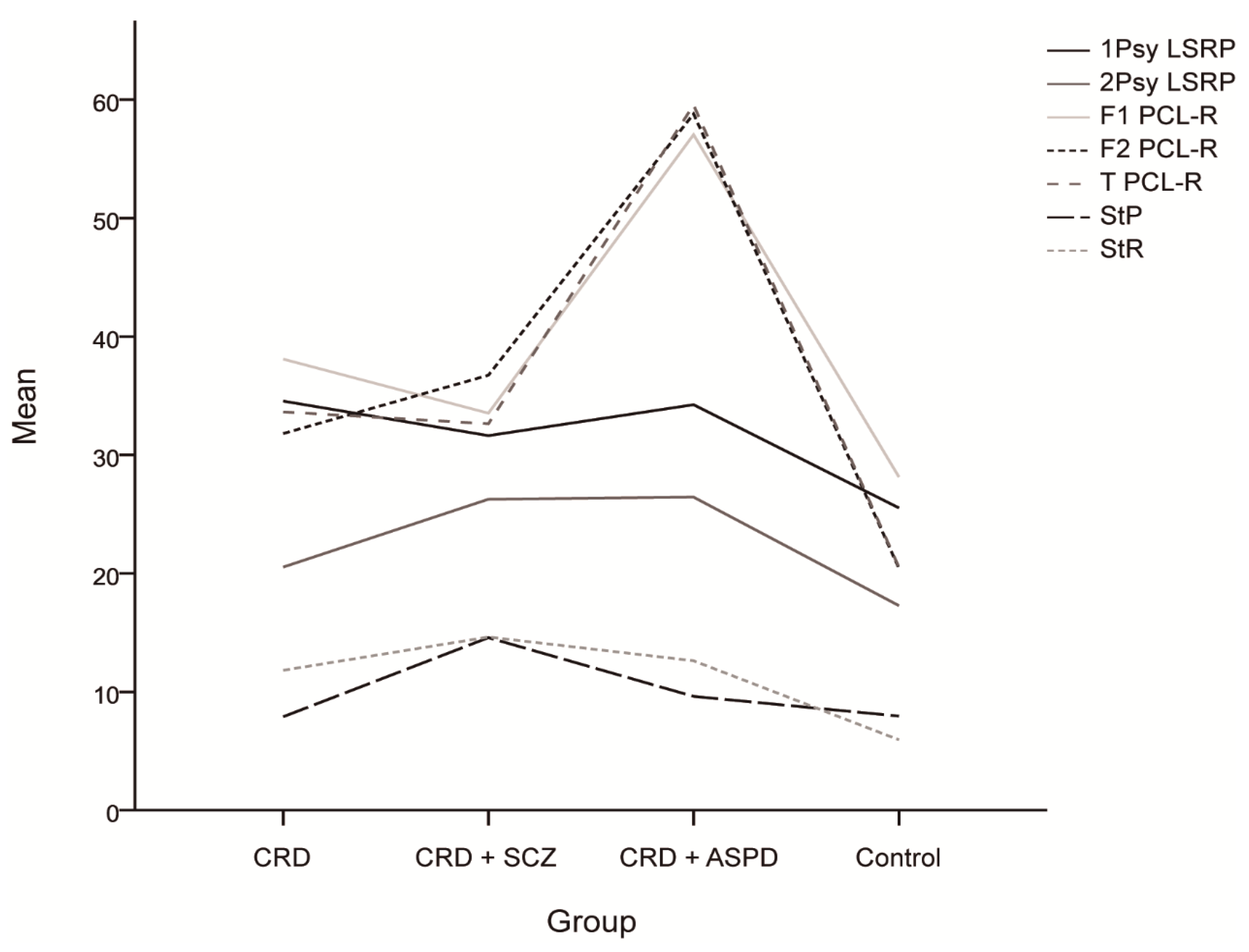
| Instrument | Variable | Group (n) | Mean (SD) | F (df; Sig.) |
|---|---|---|---|---|
| LSRP | Primary psychopathy | Control (23) | 25.39 (5.255) | 9.842 (3, 68; p = 0.000) * |
| CRD (13) | 34.77 (7.981) | |||
| CRD+SCZ (21) | 31.95 (5.527) | |||
| CRD+APD (16) | 34.25 (6.202) | |||
| Secondary psychopathy | Control (23) | 17.26 (3.063) | 15.474 (3, 68; p = 0.000) * | |
| CRD (13) | 21.23 (7.585) | |||
| CRD+SCZ (21) | 26.29 (5.100) | |||
| CRD+APD (16) | 26.44 (4.953) | |||
| PCL-R | Interpersonal/affective factor | Control (21) | 28.14 (2.762) | 103.019 (3, 63; p = 0.000) * |
| CRD (11) | 38.09 (7.217) | |||
| CRD+SCZ (19) | 33.53 (3.533) | |||
| CRD+APD (16) | 57.06 (7.750) | |||
| Social deviation factor | Control (21) | 20.43 (1.076) | 230.574 (3, 63; p = 0.000) * | |
| CRD (11) | 31.82 (4.238) | |||
| CRD+SCZ (19) | 36.74 (4.175) | |||
| CRD+APD (16) | 58.81 (4.175) | |||
| Total score | Control (21) | 20.52 (1.250) | 230.495 (3, 63; p = 0.000) * | |
| CRD (11) | 33.64 (4.178) | |||
| CRD+SCZ (19) | 32.63 (4.284) | |||
| CRD+APD (16) | 59.56 (5.573) | |||
| SPSRQ | Sensitivity to punishment | Control (23) | 8.26 (5.986) | 6.369 (3, 68; p = 0.001) * |
| CRD (13) | 8.00 (4.583) | |||
| CRD+SCZ (21) | 14.57 (5.363) | |||
| CRD+APD (16) | 9.63 (5.084) | |||
| Sensitivity to reward | Control (23) | 5.83 (3.950) | 15.509 (3, 68; p = 0.000) * | |
| CRD (13) | 10.92 (5.634 | |||
| CRD+SCZ (21) | 14.48 (4.214) | |||
| CRD+APD (16) | 12.63 (4.193) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gil-Miravet, I.; Fuertes-Saiz, A.; Benito, A.; Almodóvar, I.; Ochoa, E.; Haro, G. Prepulse Inhibition in Cocaine Addiction and Dual Pathologies. Brain Sci. 2021, 11, 269. https://doi.org/10.3390/brainsci11020269
Gil-Miravet I, Fuertes-Saiz A, Benito A, Almodóvar I, Ochoa E, Haro G. Prepulse Inhibition in Cocaine Addiction and Dual Pathologies. Brain Sciences. 2021; 11(2):269. https://doi.org/10.3390/brainsci11020269
Chicago/Turabian StyleGil-Miravet, Isis, Alejandro Fuertes-Saiz, Ana Benito, Isabel Almodóvar, Enrique Ochoa, and Gonzalo Haro. 2021. "Prepulse Inhibition in Cocaine Addiction and Dual Pathologies" Brain Sciences 11, no. 2: 269. https://doi.org/10.3390/brainsci11020269
APA StyleGil-Miravet, I., Fuertes-Saiz, A., Benito, A., Almodóvar, I., Ochoa, E., & Haro, G. (2021). Prepulse Inhibition in Cocaine Addiction and Dual Pathologies. Brain Sciences, 11(2), 269. https://doi.org/10.3390/brainsci11020269







