Abstract
Metabolic syndrome (MetS) is chronic inflammatory epidemic state contributing to total and cardiovascular mortality. The current study planned to assess and screen risk factors for MetS and its components. A cross-sectional study conducted to assess age, gender, social status, employment, education, family history, physical activity, dietary habits, alcohol, sleep, body mass index and stress as determinants of MetS. The results were analyzed by Chi Square test with statistical significance of p value <0.05. The frequency of MetS was 17.38% as per modified National Cholesterol Education Program–Adult Treatment Panel III criteria. Females (57.38%), age >50 years (86.90%; p < 0.05), middle socioeconomic status (70.50%), illiteracy (39.35%), and unemployment (81.97%; p < 0.05) were found contributing though to different extents. Subjects with a sedentary lifestyle (72.14%), positive family history (42.63%), omnivore diet (47.55%), stress (78.69%; p < 0.05), insomnia (29.51%) and increased BMI (83.62%; p < 0.001) had shown predisposition to MetS. However, the protective role of alcohol (38.28%), an active lifestyle (36.21%), vegetarian diet (62.07%) and adequate sleep (73.11%) was observed. A significant hypertension (98.37%; p < 0.001), dyslipidemia (77.05%; p < 0.001), dysglycemia (75.41%; p < 0.001) and obesity (59.02%; p < 0.001) was reported in MetS. Common concerns of female gender, increasing age and BMI, sedentary lifestyle, stress and positive family history should be considered for early identification and appropriate intervention to fight the growing MetS epidemic.
1. Introduction
The Metabolic Syndrome (MetS) is a modern day epidemic which predicts total and cardiovascular diseases (CVD) mortality [1]; the incidence and progression of carotid atherosclerosis [2]; and sudden death independent of other cardiovascular risks [3]. Subjects with MetS have three-fold risk of a heart attack or stroke, two-fold risk of CVD or dying from such events, and five-fold greater risk of developing type 2 diabetes mellitus in both sexes when compared to people without it [4].
MetS represents as a constellation of interconnected physiological, biochemical, clinical and metabolic risk factors including hypertension, dyslipidemia, central obesity, glucose intolerance, pro-inflammatory and pro-thrombotic states, which reflects an underlying insulin resistance [5]. Various bodies such as the World Health Organization (WHO) [6], the European Group for the study of Insulin Resistance (EGIR) [7], the National Cholesterol Education Program–Adult Treatment Panel III (NCEP–ATP III) [8], and the International Diabetes Federation (IDF) [9] share common ground to define MetS by acknowledging the disorders of glucose metabolism, hypertension, dyslipidemia and obesity. These underlying mechanisms are exacerbated by the complex interplay between age, genetic conditioning, and an inappropriate lifestyle comprising sedentary lifestyle and surplus availability of energy dense salt enriched food [10].
MetS is a chronic low grade inflammatory state starting from adipose tissue and further recruits immune cells which consequently releases inflammatory cytokines (TNF-α, IL-6, adiponectin, etc.) and results in an insulin-resistant state. When the secretary capacity of the pancreas is overwhelmed by battling an insulin resistance state, diabetes develops [11]. Furthermore, an increased secretion of prothrombin activator inhibitor-1 contributes to a pro-coagulant state; and along with endothelial dysfunction leads to increased risk of atherothrombosis, hypertension and CVD [12]. Estrogen production by an enlarged stromal mass predisposes the subject to the development of breast cancer [13]. Moreover, several drugs, e.g., corticosteroids, antidepressants, antipsychotics, antihistamines can produce weight gain and predispose to MetS features: obesity and glucose intolerance [14]. Hence, the constellation of these multiple underlying mechanisms results in MetS.
The prevalence of MetS varies depending on the definition applied, the ethnicity, and the age of the study population. The age-adjusted prevalence among adults population was estimated to be 24%–25% in the United States, was approximately 23% in European countries and estimated to be 20%–25% among South Asians [15]. The prevalence in Asia has increased rapidly in the recent years due to rapid socioeconomic transitions to increasing affluence, urbanization, mechanization, auto-mobilization, and urban migration [15]. However, the ethnic, cultural, environmental or economic differences contribute to varied prevalence across Asian countries [16].
Furthermore, some non-obese individuals are insulin resistant and have metabolic abnormalities. Examples are seen in individuals with two diabetic parents or one parent and a first- or second-degree relative and/or individuals of South Asian ethnicity [17]. This might be contributed to an abnormal fat distribution especially upper-body (or abdominal) obesity which correlates more strongly the MetS than do lower-body obesity [18].
MetS have multiple systemic involvement with nonalcoholic fatty liver disease (NAFLD), polycystic ovarian syndrome, sleep and breathing disorders, Alzheimer’s disease, cancers such as breast, prostate, and pancreas, focal segmental glomerulosclerosis, acanthosis nigricans, cataract and glaucoma [19]. However, early interventions may prevent these costly and deadly diseases primarily through lifestyle modifications. Hence, the current study is designed to assess and screen the risk factors of MetS by NCEP ATP III guidelines [8] because it uses measurements and laboratory results that are readily facilitating its clinical and epidemiological application in terms of time, cost and application procedures at a primary care settings.
2. Experimental Section
2.1. Design Overview
This cross-sectional study was undertaken among the Ex-Servicemen settled in the Sultanpur Lodhi, District Kapurthala, Punjab (India). Ex-Servicemen Contributory Health Scheme (ECHS) Polyclinic is a primary care center which provides free at-the-point-of-access medical and follow up services to their registered patients. Data was collected on all the retired and registered veterans residing in the region of Sultanpur Lodhi, hence the sample size is equal to the veterans population size. The selection criteria was the subjects who had been retired from their defense services; their family members comprising spouse, parents and children; and had visited the polyclinic from August 2013 to November 2013. Thus, individuals >20 years old were recruited irrespective of disease status for the MetS screening with the inclusion of diabetics, hypertensives and dyslipidemic patients and the exclusion of pregnant females. However, the prevalence of these disorders was ascertained based on the physician’s self-report diagnosis and/or use of prescription medications along with therapeutics in the medical records. Institutional ethical committee approval was obtained prior to the start of study and informed written consent was taken from all the recruited subjects in an interview process. The Chi Square test (χ2) was used for statistical analysis with p value <0.05 as a statistically significant.
2.2. Definition of MetS
The prevalence of MetS was assessed by the modified NCEP-ATP III guidelines [8]; wherein presence of any three following traits in the same individual would meet the criteria:
- (1)
- Abdominal obesity: Waist circumference (WC) ≥102 cm (>40 in) in men or ≥88 cm (>35 in) in women;
- (2)
- Serum Triglycerides (TGs): ≥150 mg/dL (≥1.7 mmol/L);
- (3)
- High Density Lipoprotein-Cholesterol (HDL-C): <40 mg/dL (<1.03 mmol/L) in men or <50 mg/dL (<1.29 mmol/L) in women;
- (4)
- Fasting blood glucose (FBG) level: ≥100 mg/dL (≥5.6 mmol/L);
- (5)
- Blood pressure (BP): ≥130/85 mmHg.
However, the current study used a correspondence of a WC of 102 cm to body mass index (BMI) of ≥29.40 kg/m2 defined in a linear regression analysis which is similar to BMI cut-offs used in previous modified NCEP definitions [20].
2.3. Survey Questionnaires
It enlists the socio-demographic variables, risk factors and the components of MetS. Socio-demographic variables include age, gender, education, socio-economic status (SES) and employment status. Education level was classified into four categories: no/little formal, primary, secondary and graduation. SES was defined into lower, middle and upper on the basis of retired ranks of ex-servicemen including their household income and assets. The recommendations by the American College of Sports Medicine and the American Heart Association for doing 30 min of moderate-intensity physical activity on ≥5 days of the week or 20 min of vigorous-intensity physical activity on ≥3 days of the week were considered [21]. The family history was defined as positive if a first-degree male relative (e.g., father, brother) and female relative have cardiovascular diseases before the age of 55 or 65 years respectively [22]. Sleep adequacy was evaluated on the basis of sleep duration (7 to 8 h), difficulty in initiating and maintaining sleep. Job strain, social constraints, financial un-stability and emotional distress in the form of anxiety and/or depression were included under “stress” which significantly affects the daily life activities. Heavy alcohol consumption was defined by a self-reported >5 drinks on a single occasion, or a daily drinking of >1 drink per day [23].
2.4. Clinical and Biochemical Measurements
Height was determined using a wall mounted, non-extendable measuring tape with subjects standing in an erect barefoot position, arms by side, and feet together. Weight measurements were taken with each subject standing at the center of the weighing scale in light clothing without shoes and socks. BMI was calculated as weight per square meter (kg/m2) and divided into normal weight (≤24.99 kg/m2), overweight (≥25.00 kg/m2) and obesity (≥29.44 kg/m2) [8,20]. BP was measured in the right arm with the subject seated and rested for 5 min using a standard mercury sphygmomanometer and suitable calibrated cuff. A blood sample was obtained from all individuals after 8–10 h of fasting to measure FBG with Erba glucose kit (GOD-POD method, end point); TGs using Erba triglyceride Des kit (GPO-Trinder method, end point) and HDL-C by cholesterol kit (Phosphotungstic acid method, end point) [8]. All the parameters were measured in a fully automated analyzer, Accurex. The clinical laboratory meets the standards of National Accreditation Board for Testing and Calibration Laboratories, India which is based on ISO/IEC standard 17025.
3. Results
All the subjects (N = 351) were divided into two cohorts: subjects with (N = 61) and without MetS (N = 290). The frequency of MetS was 17.38% in the present study as per the modified NCEP ATP III criteria. Table 1 reflects 13.12%, 47.55% and 39.35% of patients with MetS belonged to 36–50 years, 51–65 years and >65 years of age; and patients who didn’t meet the MetS criteria had 24.83%, 37.25% and 33.45% for the same age groups, respectively. This shows a statistically significant (p < 0.05) age related higher frequency of MetS among subjects >50 years old (86.90%) (Figure 1).
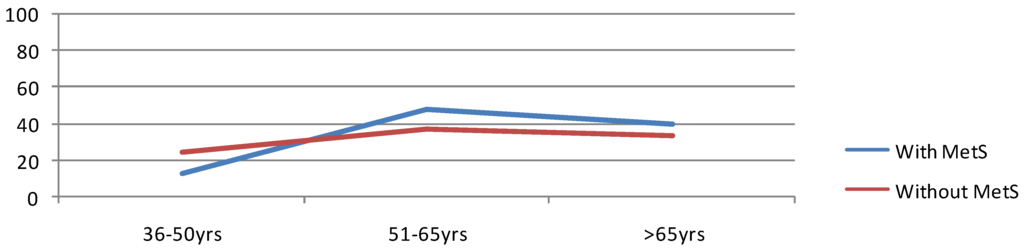
Figure 1.
Age group specific prevalence of Metabolic syndrome (MetS).
Figure 1.
Age group specific prevalence of Metabolic syndrome (MetS).
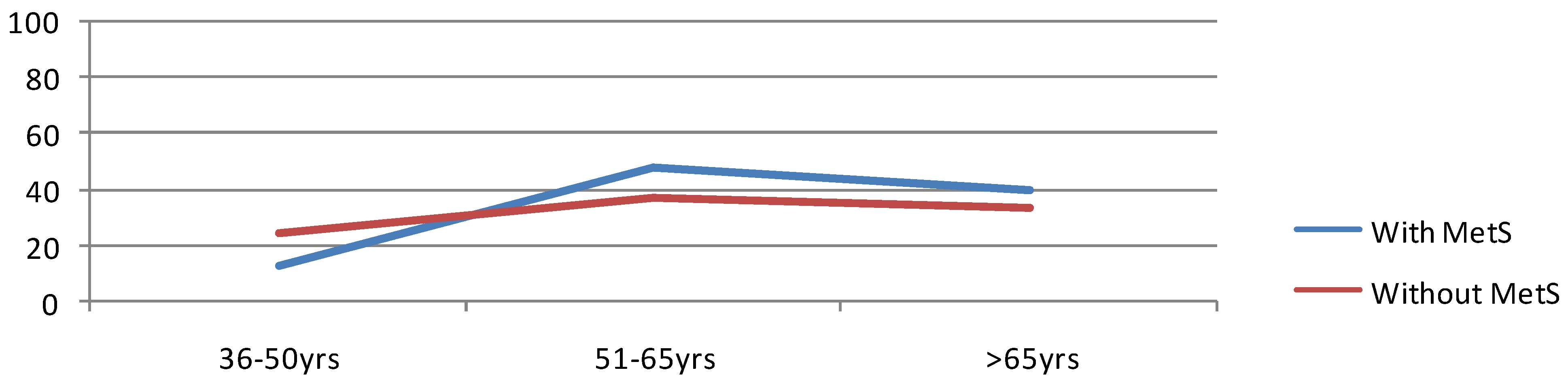

Table 1.
Comparison of socio-demographic variables in all the study subjects *.
| Category | Frequency, N (%) | Metabolic syndrome | χ2 value | |
|---|---|---|---|---|
| Yes (61) | No (290) | |||
| Age (years) | ||||
| 20–35 | 13 (3.71) | 00 (0.00) | 13 (4.49) | 5.42 (<0.05) |
| 36–50 | 80 (22.80) | 08 (13.12) | 72 (24.83) | |
| 51–65 | 137 (39.04) | 29 (47.55) | 108 (37.25) | |
| >65 | 121 (34.48) | 24 (39.35) | 97 (33.45) | |
| Gender | ||||
| Males | 174 (49.58) | 26 (42.63) | 148 (51.04) | 1.43 |
| Females | 177 (50.43) | 35 (57.38) | 142 (48.97) | |
| Education | ||||
| No/Little | 108 (30.77) | 24 (39.35) | 84 (40.20) | 3.73 |
| Primary | 106 (30.20) | 18 (29.51) | 88 (30.35) | |
| Secondary | 121 (34.48) | 18 (29.51) | 103 (35.52) | |
| Graduation | 16 (4.56) | 01 (1.64) | 15 (5.18) | |
| Socio economic status | ||||
| Middle | 223 (63.54) | 43 (70.50) | 180 (62.07) | 1.56 |
| Upper | 128 (36.47) | 18 (29.51) | 110 (37.94) | |
| Occupation | ||||
| Unemployed | 250 (71.23) | 50 (81.97) | 200 (68.97) | 4.18 (<0.05) |
| Employed | 101 (28.78) | 11 (18.04) | 90 (31.04) | |
* Parentheses represent frequency of the variables.
Among both genders, females (57.38%) had been more frequently diagnosed with MetS than men (42.63%); however, no statistically significant relation was reported. 39.35%, 29.51%, 29.51% and 1.64% of patients with MetS had no/little, primary, secondary and graduation level education; and subjects without MetS had 48.03%, 27.12%, 21.47% and 3.39% for the same education categories, respectively. It shows an inverse association between level of education and MetS. Taking SES into consideration, middle social class subjects (70.50%) had a higher frequency of MetS than upper class subjects (29.51%). Similarly, subjects who were unemployed (81.97%) had a statistically significant (p < 0.05) higher frequency of MetS than employed groups (18.04%).
Table 2 depicts a statistically significant (p < 0.001) higher frequency of MetS among obese (59.02%) and overweight subjects (24.60%) than normal weight subjects (16.40%). A positive family history (42.63%) had predisposed the subjects to MetS than their counterparts (31.38%). Similarly, sedentary lifestyle (72.14%) had contributed to a higher frequency of MetS than active lifestyle (27.87%). Subjects who prefer omnivorous meals had been more frequently diagnosed with the syndrome (47.55%) than without it (37.94%). Contrarily, vegetarian dietary habits play a protective role against MetS (62.07%) as compared to their counterparts (52.46%).

Table 2.
Comparison of the risk factors in the subjects with and without Metabolic syndrome *.
| Category | Frequency, N (%) | Metabolic syndrome | χ2 value | |
|---|---|---|---|---|
| Yes (61) | No (290) | |||
| Body Mass Index | ||||
| Normal | 57 (16.24) | 16.40 (10) | 16.21 (47) | 53.91 (<0.001) |
| Overweight | 107 (30.49) | 15 (24.60) | 92 (31.73) | |
| Obese | 187 (53.28) | 36 (59.02) | 15 (52.07) | |
| Family history | ||||
| Positive | 117 (33.34) | 26 (42.63) | 91 (31.38) | 2.89 |
| Negative | 234 (66.67) | 35 (57.38) | 199 (68.63) | |
| Physical activity | ||||
| Adequate | 122 (34.76) | 17 (27.87) | 105 (36.21) | 1.57 |
| In adequate | 229 (65.25) | 44 (72.14) | 185 (63.80) | |
| Dietary habits | ||||
| Vegetarians | 212 (60.40) | 32 (52.46) | 180 (62.07) | 1.96 |
| Omnivores | 139 (39.61) | 29 (47.55) | 110 (37.94) | |
| Stress levels | ||||
| Significant | 159 (35.33) | 48 (78.69) | 111 (38.28) | 6.36 (<0.05) |
| Insignificant | 192 (64.68) | 13 (21.14) | 179 (61.73) | |
| Sleep | ||||
| Adequate | 255 (72.65) | 43 (70.50) | 212 (73.11) | 0.19 |
| Inadequate | 96 (27.36) | 18 (29.51) | 78 (26.90) | |
| Alcohol | ||||
| Yes | 128 (36.47) | 17 (27.86) | 111 (38.28) | 2.36 |
| No | 223 (63.54) | 44 (72.14) | 179 (61.73) | |
| Smoking | ||||
| Current | 12 (3.42) | 12 (19.68) | 00 (0.00) | 0.54 |
| Ex/Never | 339 (96.59) | 49 (80.33) | 290 (100.00) | |
* Parentheses represent frequency of the variables.
Statistically significant stress (p < 0.05) levels were found to be more related to MetS (78.69%) than insignificant stress (21.14%). Moreover, sleep inadequacy had shown higher association levels with MetS (29.51%) than their counterparts (26.90%). On the other hand, subjects with alcohol consumption had a lower frequency of MetS (38.28%) as compared to the other group (27.86%). However, the low smoking frequency (3.42%) in the study subjects restrains us from giving an analysis of its relation with MetS. Figure 2 shows the graphical prevalence of cardiovascular risk factors in a decreasing order among subjects with the MetS.

Figure 2.
Graphical presentation of the risk factors in metabolic syndrome.
Figure 2.
Graphical presentation of the risk factors in metabolic syndrome.

Table 3 reflects a statistically significant (p < 0.001) higher frequency of hypertension (98.37%), dyslipidemia (77.05%), hyperglycemia (75.41%) and obesity (59.02%) among the subjects with MetS than those without it (hypertension: 37.94%, dyslipidemia: 17.59%, hyperglycemia: 13.45% and obesity: 16.21%).

Table 3.
Comparison of all the components of Metabolic Syndrome in the study subjects *.
| Category | Frequency, N (%) | Metabolic syndrome | χ2 value | ||
|---|---|---|---|---|---|
| Yes (61) | No (290) | ||||
| Hypertension | |||||
| Normal | 48.44 (170) | 1.64 (01) | 62.07 (180) | 73.69 (<0.001) | |
| Diseased | 98.37(60) | 37.94 (110) | |||
| Dyslipidemia | |||||
| Normal | 27.93 (98) | 22.96 (14) | 82.42 (239) | 88.51 (<0.001) | |
| Diseased | 47 (77.05) | 51 (17.59) | |||
| Dysglycemia | |||||
| Normal | 85 (24.22) | 15 (24.60) | 251 (86.56) | 105.36 (<0.001) | |
| Diseased | 46 (75.41) | 39 (13.45) | |||
| Obesity | |||||
| Normal | 83 (23.65) | 25 (40.99) | 243 (83.80) | 51.16 (<0.001) | |
| Diseased | 36 (59.02) | 47 (16.21) | |||
* Parentheses represent frequency of the variables.
4. Discussion
The current study was designed to assess and screen the patients with the MetS in order to begin efforts to adequately implement the treatments to reduce the risk of subsequent diseases. The modified NCEP ATP III guidelines had estimated the frequency of 17.38% in the present study which corroborate with the prevalence rate of Deepa et al. (18.30%) [24] and Sawant et al. (19.52%) [25]. Conversely, Hu et al. [26] and Can et al. [27] have found an increased rate of MetS by ATP III in Finland (39.10%) and Turkey (38%), respectively. However, Chennai Urban Population Study (CUPS) has reported 11.20% prevalence of the MetS defined by EGIR [28]. Moreover, The Bruneck Study found the prevalence of 34.10% and 17.80% among the same subjects with the WHO and the ATP III MetS criteria respectively [29]. These discrepancies might be attributable to differences in the syndrome definitions and its components; and the characteristics of the population studied [30].
A statistically significant (p < 0.05) increase in the frequency of MetS (86.90%) after the age of 50 years was observed (Table 1) in concordance with Kanjlal et al. [31], who reported maximum prevalence in the age group of 50–59 years; and Reddy et al. [32] noticed among the age group >60 years old in Indian population. An overall increasing trend with advancing age might be contributed to an evolution of insulin resistance, hormonal alterations, and increase in visceral adipose tissue with age [33].
A higher trend of MetS in females (57.38%) than males (42.63%) in the present study was found to be supported by Magnat et al. [34]. Conversely, Sawant et al. [25] reports the prevalence of MetS in males doubles that of females. Women transition from the pre-menopause to post-menopause state with substantial metabolic changes and estrogen deficiency might lead them to an increased predisposition to MetS.
An inverse relation of both household income and education with MetS in the present study was found in consistence Riediger et al. [35]. Contrarily, Magnat et al. [34] has found MetS to be more prevalent among upper social class subjects than lower classes. Moreover, a statistically significant (p < 0.05) higher prevalence of MetS was found among unemployed (81.97%) than employed groups (18.04%) in the current study. Similarly, Demiral et al. [36] has depicted the prevalence of MetS significantly higher among homemakers than working population. Contrarily, Chandola et al. [37] has found a positive dose-response association between exposure to work related stress and the MetS.
A statistically significant (p < 0.001) association of MetS with an increase in BMI (83.62%) in the present study (Table 2) has been found to be consistent with other studies [25,34]. Higher categories of BMI were significantly associated with MetS and its each component, including abdominal obesity, high TG, low HDL-C, high BP and high FBG in both sexes [38]. However, MetS was reported among 16.40% of subjects with normal BMI in the current study which is in concordance to Corral et al. [39]. It has been suggested that metabolically obese normal weight persons have an abnormal body mass distribution with an elevated fat mass of >30% that might predisposes them to the MetS [39].
A positive family history (42.63%) has shown predisposition to MetS than a negative family history in the current study, which was found supported by Lee et al. [40]. Dallongeville et al. [41] has further suggested that MetS is a contributor to the familial aggregation of premature CVD independently of other classical cardiovascular risk factors. Furthermore, a higher frequency of MetS among sedentary subjects in the present study was found supported by Baceviciene et al. [42]. Similarly, Edwardson et al. [43] has observed that greater time spent sedentary increases the MetS odds with no differences for subgroups of sex, sedentary behavior measure, MetS definition, study quality or country income.
MetS was reported more frequently among subjects who prefer omnivores (47.55%) than vegetarian meals. Rizzo et al. [44] has further shown TGs, glucose, BP, WC, and BMI were significantly lower in vegetarians than non-vegetarians after adjusting for age, sex, ethnicity, smoking, alcohol intake, physical activity, and dietary energy intake. A vegetarian diet, being rich in vegetables and fruits, and typically including a low glycemic index foods such as beans, legumes, and nuts, which reduces oxidative stress, chronic inflammation, and thus MetS and its components. Conversely, Shang et al. [45] has suggested that vegan diets did not decrease the risk of MetS compared with pesco-vegetarian, lacto-vegetarian and non-vegetarian diets.
A statistically significant (p < 0.05) stress predisposition of the study subjects to MetS (78.69%) was found in consistence with Pyykkonon et al. [46]. Similarly, stressful life events were found to be associated with insulin resistance, obesity, and TGs, and regarded as poor metabolic health indicators [46]. Conversely, alcohol consumption had shown a protective role in the prevalence of MetS in the current study. Similarly, Freiberg et al. [47] has observed a favorable influence of mild to moderate alcohol consumption on lipids, WC and fasting insulin levels with a lower MetS prevalence. Contrarily, Baik and Shin [48] have noticed heavy drinking association with an increased MetS risk by influencing its components.
Sleep inadequacy had further contributed to the diagnosis of MetS in the present study (29.51%). Chronic sleep insufficiency or deprivation not only leads to frequent mental and physical distress; but further contributes to the aging process and increases the risk for diabetes and obesity [49]. Similarly, Coughlin et al. [50] has shown obstructive sleep apnea is independently associated with an increase in the cardiovascular risk factors that comprises the MetS and its overall prevalence.
A statistically significant (p < 0.001) highest prevalence of hypertension (98.37%) followed by dyslipidemia (77.05%), dysglycemia (75.41%) and obesity (59.02%) was observed in the current study. Similarly, Sidorenkov et al. [51] found hypertension as the most frequent element in both sexes, followed by dyslipidemia, central obesity and hyperglycemia by using NCEP ATP III guidelines. Furthermore, Rodríguez et al. [52] has noticed an independent association of age, gender, moderately-intense physical activity, elevated fasting plasma glucose level, dyslipidemia, hypertension, treatment with oral hypoglycaemic agents, and the presence of endocrine disorders with MetS which has been found consistent to the present study.
Hence, a healthy lifestyle should be adopted, the beginning in childhood and adolescence in the view of the malignant nature of cardiovascular risk factors, which start at an early age in Asian Indians. Continuing surveillance efforts would provide an opportunity to develop evidence-based cost-effective CVD prevention, detection, and management strategies. Lifestyle changes in the form of regular physical activity, lifetime abstinence or cessation of tobacco, reduced intake of trans- and saturated fatty acids, moderation of alcohol, and increased consumption of fruits and vegetables would delay the onset of advanced forms of MetS and subsequent high-risk status.
The use of cross sectional data could not help to examine the causal pathways. The sample was not randomly selected and cannot exclude a healthy volunteer bias related to voluntary participation in the study, which could tend to underestimate the actual prevalence of MetS in the study population. However, this study being the first one in this region of India contributes to map the prevalence of MetS worldwide, particularly with regards to the Asian region.
5. Conclusions
Female gender, advancing age, illiteracy, unemployment, positive family history, obesity and a sedentary lifestyle were found to contribute to Metabolic Syndrome. Therefore, early identification of the metabolic abnormalities and taking appropriate intervention by instituting holistic, multidisciplinary, and multi-sectorial preventive measures at an individual, community, and societal level would help to promote healthy dietary habits and physically active lifestyles that may fight against the growing epidemic of Metabolic Syndrome.
Acknowledgments
I would acknowledge all the patients who gave their consent to be a part of this study. I am thankful to the entire staff of polyclinic for their consistent support and Manjit Kaur for her assistance in the statistical analysis.
Conflicts of Interest
The author declares no conflict of interest.
References
- Nilsson, P.M.; Engstrom, G.; Hedblad, B. The metabolic syndrome and incidence of cardiovascular disease in non-diabetic subjects—A population-based study comparing three different definitions. Diabet. Med. 2007, 24, 464–472. [Google Scholar] [CrossRef]
- Bonora, E.; Kiechl, S.; Willeit, J.; Oberhollenzer, F.; Egger, G.; Bonadonna, R.C.; Muggeo, M. Carotid atherosclerosis and coronary heart disease in the metabolic syndrome. Prospective data from the Bruneck Study. Diabetes Care 2003, 26, 1251–1257. [Google Scholar] [CrossRef]
- Empana, J.P.; Duciemetiere, P.; Balkau, B.; Jouven, X. Contribution of the metabolic syndrome to sudden death risk in asymptomatic men: the Paris Prospective Study I. Eur. Heart J. 2007, 28, 1149–1154. [Google Scholar] [CrossRef]
- Stern, M.P.; Williams, K.; González-Villalpando, C.; Hunt, K.J.; Haffner, S.M. Does the metabolic-syndrome improve identification of individuals at risk of type 2 diabetes and/or cardiovascular disease? Diabetes Care 2004, 27, 2676–2681. [Google Scholar] [CrossRef]
- Alberti, K.G.; Eckel, R.H.; Grundy, S.M.; Zimmet, P.Z.; Cleeman, J.I.; Donato, K.A.; Fruchart, J.C.; James, W.P.; Loria, C.M.; Smith, S.C., Jr.; et al. Hnizing the metabolic syndrome: a joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation 2009, 120, 1640–1645. [Google Scholar] [CrossRef]
- Alberti, K.G.; Zimmet, P.Z. Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet. Med. 1998, 15, 539–553. [Google Scholar] [CrossRef]
- Balkau, B.; Charles, M.A. Comment on the provisional report from the WHO consultation: European Group for the Study of Insulin Resistance (EGIR). Diabet. Med. 1999, 16, 442–443. [Google Scholar] [CrossRef]
- Grundy, S.M.; Cleeman, J.I.; Daniels, S.R.; Donato, K.A.; Eckel, R.H.; Franklin, B.A.; Gordon, D.J.; Krauss, R.M.; Savage, P.J.; Smith, S.C., Jr.; et al. Diagnosis and management of the metabolic syndrome: An American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement. Circulation 2005, 112, 2735–2752. [Google Scholar] [CrossRef]
- Alberti, K.G.; Zimmet, P.; Shaw, J. The metabolic syndrome—A new worldwide definition. Lancet 2005, 366, 1059–1062. [Google Scholar] [CrossRef]
- Zimmet, P. Globalization, coca-colonization and the chronic disease epidemic: can the doomsday scenario be averted? J. Intern. Med. 2000, 247, 301–310. [Google Scholar] [CrossRef]
- Petersen, K.F.; Shulman, G.I. Etiology of insulin resistance. Am. J. Med. 2006, 119, S10–S16. [Google Scholar] [CrossRef]
- Kohler, H.P.; Grant, P.J. Plasminogen-activator inhibitor type 1 and coronary artery disease. N. Engl. J. Med. 2000, 342, 1792–1801. [Google Scholar] [CrossRef]
- Schapira, D.V.; Clark, R.A.; Wolff, P.A.; Jarrett, A.R.; Kumar, N.B.; Aziz, N.M. Visceral obesity and breast cancer risk. Cancer 1994, 74, 632–639. [Google Scholar] [CrossRef]
- Grundy, S.M.; Hansen, B.; Smith, S.C.; Cleeman, J.I.; Kahn, R.A.; and for Conference Participants. Clinical Management of Metabolic Syndrome: Report of the American Heart Association/National Heart, Lung, and Blood Institute/American Diabetes Association Conference on scientific issues related to management. Circulation 2004, 109, 551–556. [Google Scholar] [CrossRef]
- Eapen, D.; Kalra, G.L.; Merchant, N.; Arora, A.; Khan, B.V. Metabolic syndrome and cardiovascular disease in South Asians. Vasc. Health Risk Manag. 2009, 5, 731–743. [Google Scholar]
- Lao, X.Q.; Zhang, Y.H.; Sang Wong, M.C.; Xu, Y.J.; Xu, H.F.; Nie, S.P.; Ma, W.J.; Thomas, G.N.; Sun Yu, I.T. The prevalence of metabolic syndrome and cardiovascular risk factors in adults in southern China. BMC Public Health 2012, 12, 64. [Google Scholar] [CrossRef]
- Perseghin, G.; Ghosh, S.; Gerow, K.; Shulman, G.I. Metabolic defects in lean non diabetic offspring of NIDDM parents: a cross-sectional study. Diabetes 1997, 46, 1001–1009. [Google Scholar] [CrossRef]
- Jensen, M.D.; Haymond, M.W.; Rizza, R.A.; Cryer, P.E.; Miles, J.M. Influence of body fat distribution on free fatty acid metabolism in obesity. J. Clin. Invest. 1989, 83, 1168–1173. [Google Scholar] [CrossRef]
- Kaur, J. A comprehensive review on metabolic syndrome. Cardiol. Res. Pract. 2014, 2014, 943162:1–943162:21. [Google Scholar]
- Sattar, N.; Gaw, A.; Scherbakova, O.; Ford, I.; O’Reilly, D.S.; Haffner, S.M.; Isles, C.; Macfarlane, P.W.; Packard, C.J.; Cobbe, S.M.; et al. Metabolic syndrome with and without C-reactive protein as a predictor of coronary heart disease and diabetes in the West of Scotland coronary prevention study. Circulation 2003, 108, 414–419. [Google Scholar] [CrossRef]
- Haskell, W.L.; Lee, I.M.; Pate, R.R.; Powell, K.E.; Blair, S.N.; Franklin, B.A.; Macera, C.A.; Heath, G.W.; Thompson, P.D.; Bauman, A. Physical activity and public health: updated recommendation for adults from the American College of Sports Medicine and the American Heart Association. Med. Sci. Sports Exerc. 2007, 39, 1423–1434. [Google Scholar] [CrossRef]
- Chobanian, A.V.; Bakris, G.L.; Black, H.R.; Cushman, W.C.; Green, L.A.; Izzo, J.L., Jr.; Jones, D.W.; Materson, B.J.; Oparil, S.; Wright, J.T., Jr.; et al. Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure; National Heart, Lung, and Blood Institute; National High Blood Pressure Education Program Coordinating Committee: Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension 2003, 42, 1206–1252. [Google Scholar] [CrossRef]
- Amparo, P.; Farr, S.L.; Dietz, P.M. Chronic disease risk factors among American Indian/Alaska Native women of reproductive age. Prev. Chronic Dis. 2011, 8, A118. [Google Scholar]
- Deepa, M.; Farooq, S.; Datta, M.; Deepa, R.; Mohan, V. Prevalence of metabolic syndrome using WHO, ATPIII and IDF definitions in Asian Indians: The Chennai Urban Rural Epidemiology Study (CURES-34). Diabetes 2007, 23, 127–134. [Google Scholar]
- Sawant, A.; Mankeshwar, R.; Shah, S.; Raghavan, R.; Dhongde, G.; Raje, H.; D’souza, S.; Subramanium, A.; Dhairyawan, P.; Todur, S.; et al. Prevalence of Metabolic Syndrome in urban India. Cholesterol 2011, 7, 920983:1–920983:7. [Google Scholar]
- Hu, G.; Lindström, J.; Jousilahti, P.; Peltonen, M.; Sjöberg, L.; Kaaja, R.; Sundvall, J.; Tuomilehto, J. The increasing prevalence of metabolic syndrome among Finnish men and women over a decade. J. Clin. Endocrinol. Metab. 2008, 93, 832–836. [Google Scholar]
- Can, A.S.; Bersot, T.P. Analysis of agreement among definitions of metabolic Syndrome in nondiabetic Turkish adults: A methodological study. BMC Public Health 2007, 7, 353. [Google Scholar] [CrossRef]
- Mohan, V.; Shanthirani, S.; Deepa, R.; Premalatha, G.; Sastry, N.G.; Saroja, R. Intra-urban differences in the prevalence of the metabolic syndrome in southern India—the Chennai Urban Population Study (CUPS No. 4). Diabetic Med. 2001, 18, 280–287. [Google Scholar] [CrossRef]
- Bonora, E.; Kiechl, S.; Willeit, J.; Oberhollenzer, F.; Egger, G.; Bonadonna, R.C.; Muggeo, M. The metabolic syndrome in subjects aged 40–79 from the Bruneck study. Epidemiology and cardiovascular risk. Diabetes 2001, 50, A203. [Google Scholar]
- Rantala, A.O.; Kauma, H.; Lilja, M.; Savolainen, M.J.; Reunanen, A.; Kesäniemi, Y.A. Prevalence of the metabolic syndrome in drug-treated hypertensive patients and control subjects. J. Intern. Med. 1999, 245, 163–174. [Google Scholar] [CrossRef]
- Kanjilal, S.; Shanker, J.; Rao, V.S.; Khadrinarasimhaih, N.; Mukherjee, M.; Iyengar, S.S.; Kakkar, V.V. Prevalence and component analysis of metabolic syndrome: An Indian atherosclerosis research study perspective. Vasc. Health Risk Manag. 2008, 4, 189–197. [Google Scholar] [CrossRef]
- Reddy, K.S.; Prabhkaran, D.; Chaturvedi, V.; Jeemon, P.; Thankappan, K.R.; Ramakrishnan, L.; Mohan, B.V.M.; Pandav, C.S.; Ahmed, F.U.; Josh, P.P.; et al. Methods for establishing a surveillance system for cardiovascular diseases in Indian industrial populations. Bull. WHO 2004, 84, 461–469. [Google Scholar]
- Boden, G.; Chen, X.; DeSantis, R.A.; Kendrick, Z. Effects of age and body fat on insulin resistance in healthy men. Diabetes Care 1993, 16, 728–733. [Google Scholar]
- Mangat, C.; Goel, N.K.; Walia, D.K.; Agarwal, N.; Sharma, M.K.; Kaur, J.; Singh, R.; Singh, G. Metabolic Syndrome: A challenging health Issue in highly urbanized Union Territory of north India. Diabetol. Metab. Syndr. 2010, 2, 19. [Google Scholar]
- Riediger, N.D.; Clara, I. Prevalence of metabolic syndrome in the Canadian adult population. CMAJ 2011, 183, E1127–E1134. [Google Scholar] [CrossRef]
- Demiral, Y.; Arik, H.; Toğrul, B.U. The association between employment status and metabolic syndrome in women: modifying effect of education. Women Health 2012, 52, 755–770. [Google Scholar] [CrossRef]
- Chandola, T.; Brunner, E.; Marmot, M. Chronic stress at work and the metabolic syndrome: prospective Study. BMJ 2006. [Google Scholar] [CrossRef]
- Hwang, L.C.; Bai, C.H.; Chen, C.J. Prevalence of obesity and metabolic syndrome in Taiwan. J. Formos. Med. Assoc. 2006, 105, 626–635. [Google Scholar] [CrossRef]
- Corral, A.R.; Somers, V.K.; Sierra-Johnson, J.; Korenfeld, Y.; Boarin, S.; Korinek, J.; Jensen, M.D.; Parati, G.; Lopez-Jimenez, F. Normal weight obesity: A risk factor for cardiometabolic dysregulation and cardiovascular mortality. Eur. Heart J. 2010, 31, 737–746. [Google Scholar] [CrossRef]
- Lee, W.Y.; Jung, C.H.; Park, J.S.; Rhee, E.J.; Kim, S.W. Effects of smoking, alcohol, exercise, education, and family history on the metabolic syndrome as defined by the ATP III. Diabetes Res. Clin. Pract. 2005, 67, 70–77. [Google Scholar]
- Dallongeville, J.; Grupposo, M.C.; Cottel, D.; Ferrières, J.; Arveiler, D.; Bingham, A.; Ruidavets, J.B.; Haas, B.; Ducimetière, P.; Amouyel, P. Association between the metabolic syndrome and parental history of premature cardiovascular disease. Eur. Heart J. 2006, 27, 722–728. [Google Scholar] [CrossRef]
- Baceviciene, M.; Luksiene, D.I.; Cesnaitiene, V.J.; Raubaite, S.; Peasey, A.; Tamosiunas, A. Dose-response association between physical activity and metabolic syndrome. Cent. Eur. J. Med. 2013, 8, 273–282. [Google Scholar] [CrossRef]
- Edwardson, C.L.; Gorely, T.; Davies, M.J.; Gray, L.J.; Khunti, K.; Wilmot, E.G.; Yates, T.; Biddle, S.J.H. Association of sedentary behavior with metabolic syndrome: A meta-analysis. PLoS One 2012, 7, e34916. [Google Scholar]
- Rizzo, N.S.; Sabate, J.; Jaceldo-Siegl, K.; Fraser, G.E. Vegetarian dietary patterns are associated with a lower risk of metabolic syndrome- The Adventist Health Study 2. Diabetes Care 2011, 34, 1225–1227. [Google Scholar] [CrossRef]
- Shang, P.; Shu, Z.; Wang, Y.; Li, N.; Du, S.; Sun, F.; Xia, Y.; Zhan, S. Veganism does not reduce the risk of the metabolic syndrome in a Taiwanese cohort. Asia Pac. J. Clin. Nutr. 2011, 20, 404–410. [Google Scholar]
- Pyykkonen, A.J.; Raikkonen, K.; Tuomi, T.; Eriksson, J.G.; Groop, L.; Isomaa, B.O. Stressful life events and the metabolic syndrome. The Prevalence, Prediction and Prevention of Diabetes (PPP)-Botnia Study. Diabetes Care 2010, 33, 378–384. [Google Scholar] [CrossRef]
- Freiberg, M.S.; Cabral, H.J.; Heeren, T.C.; Vasan, R.S.; Ellison, R.C. Alcohol consumption and the prevalence of the Metabolic Syndrome in the U.S. A cross-sectional analysis of data from the Third National Health and Nutrition Examination Survey. Diabetes Care 2004, 27, 2954–2959. [Google Scholar] [CrossRef]
- Baik, I.; Shin, C. Prospective study of alcohol consumption and metabolic Syndrome. Am. J. Clin. Nutr. 2008, 87, 1455–1463. [Google Scholar]
- Lam, J.C.M.; Ip, M.S.M. Sleep & the metabolic syndrome. Indian J. Med. Res. 2010, 131, 206–216. [Google Scholar]
- Coughlin, S.R.; Mawdsley, L.; Mugarza, J.A.; Calverley, P.M.A.; Wilding, J.P.H. Obstructive sleep apnoea is independently associated with an increased prevalence of metabolic syndrome. Eur. Heart J. 2004, 25, 735–741. [Google Scholar] [CrossRef]
- Sidorenkov, O.; Nilssen, O.; Brenn, T.; Martiushov, S.; Arkhipovsky, V.L.; Grjibovski, A.M. Prevalence of the metabolic syndrome and its components in northwest Russia: The Arkhangelsk study. BMC Public Health 2010, 10, 23. [Google Scholar] [CrossRef]
- Rodríguez, A.; Delgado-Cohen, H.; Reviriego, J.; Serrano-Ríos, M. Risk factors associated with metabolic syndrome in type 2 diabetes mellitus patients according to World Health Organization, Third Report National Cholesterol Education Program, and International Diabetes Federation definitions. Diabetes, Metab. Syndrome Obes. Targets Ther. 2011, 4, 1–4. [Google Scholar]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
