Comparative Performance of Four Established Neonatal Disease Scoring Systems in Predicting In-Hospital Mortality and the Potential Role of Thromboelastometry
Abstract
:1. Introduction
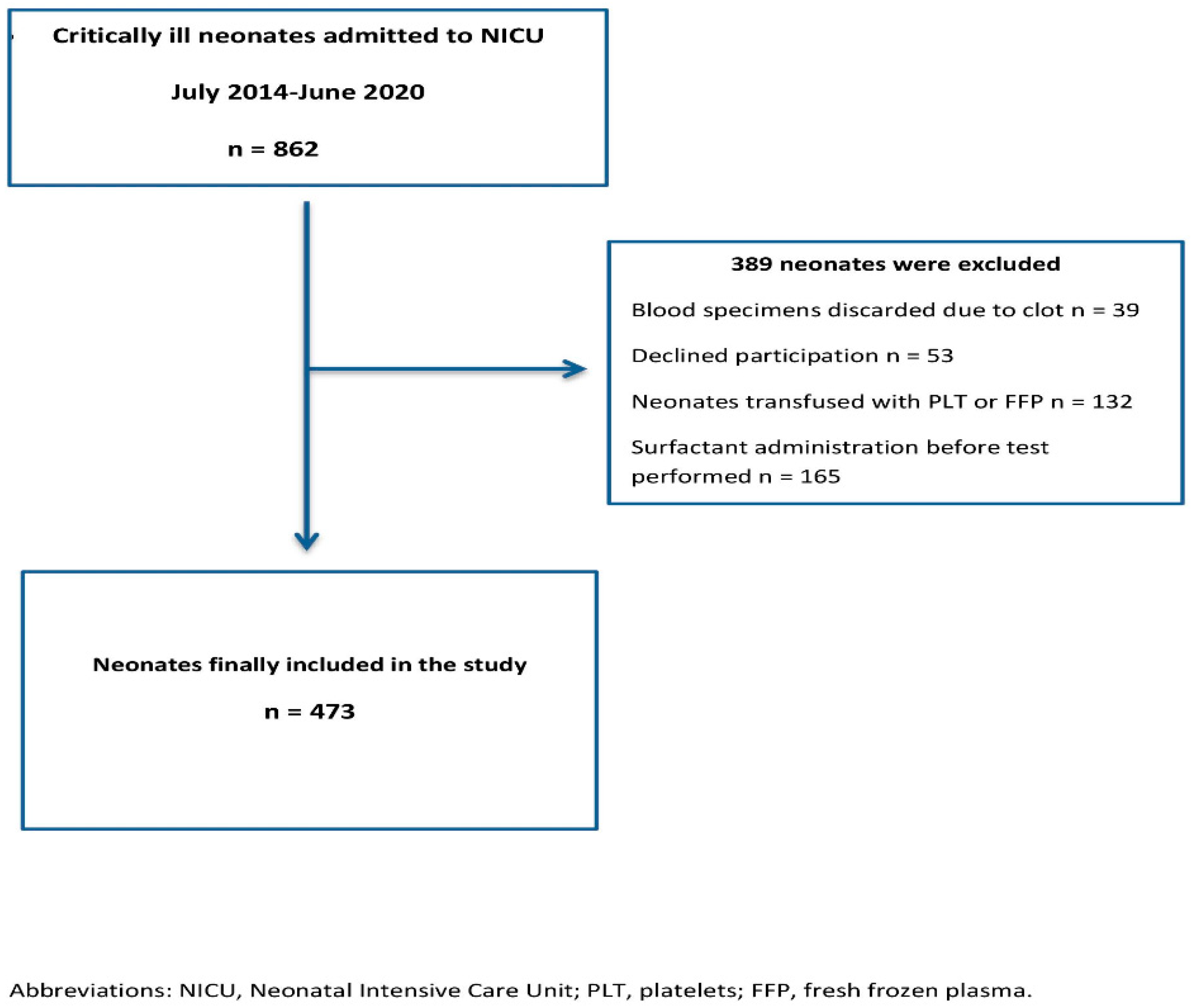
2. Materials and Methods
Statistical Analysis
3. Results
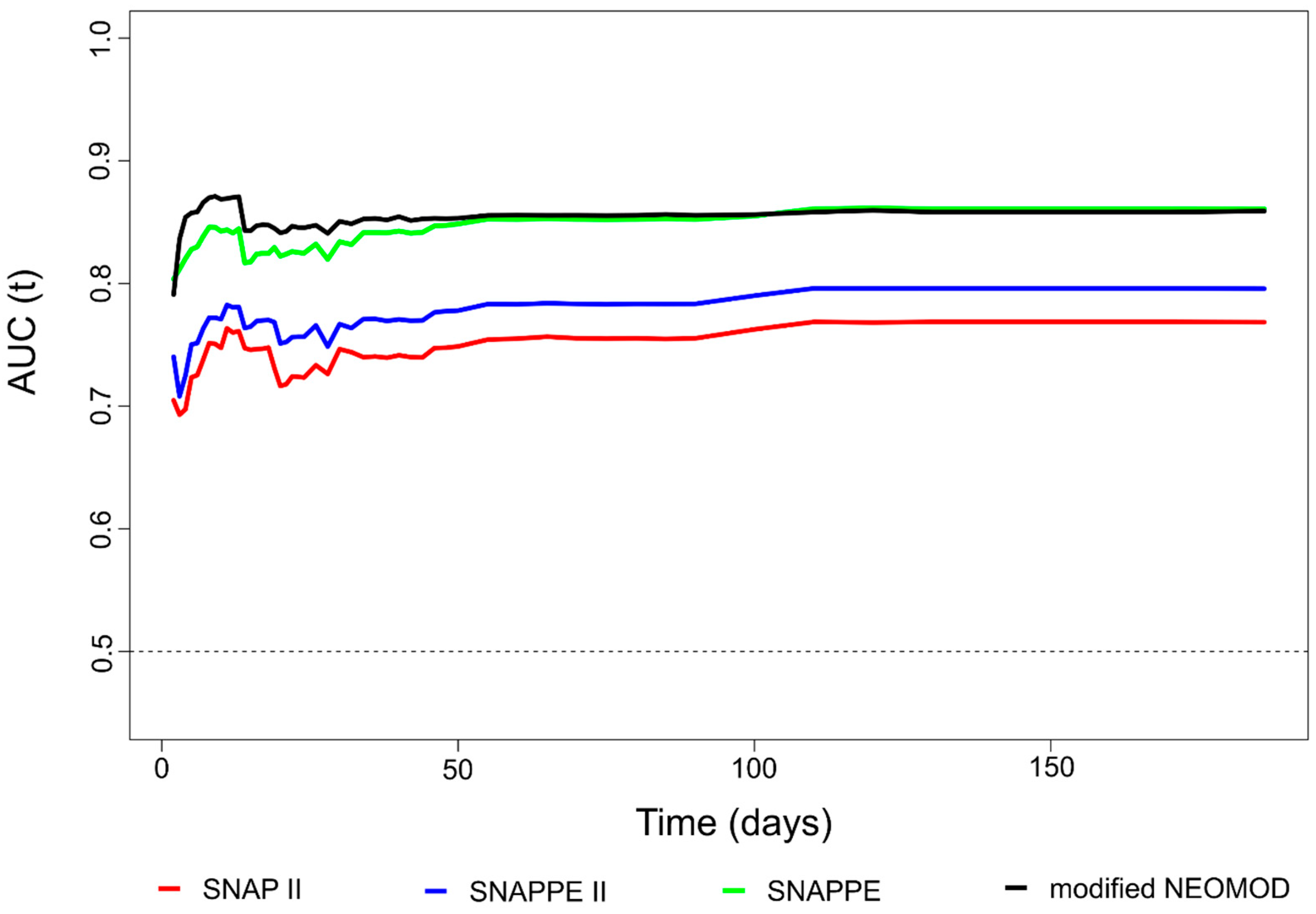
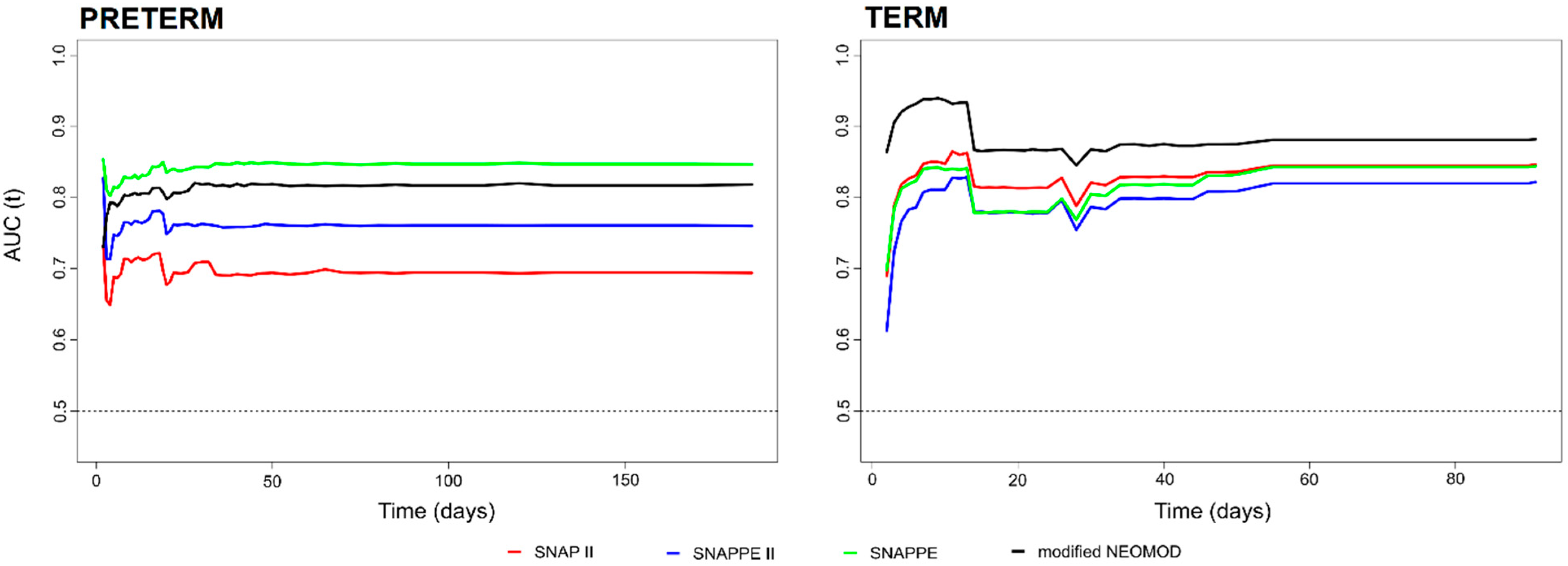
3.1. Performance over Time of SNAP II, SNAPPE II, SNAPPE and Modified NEOMOD Score
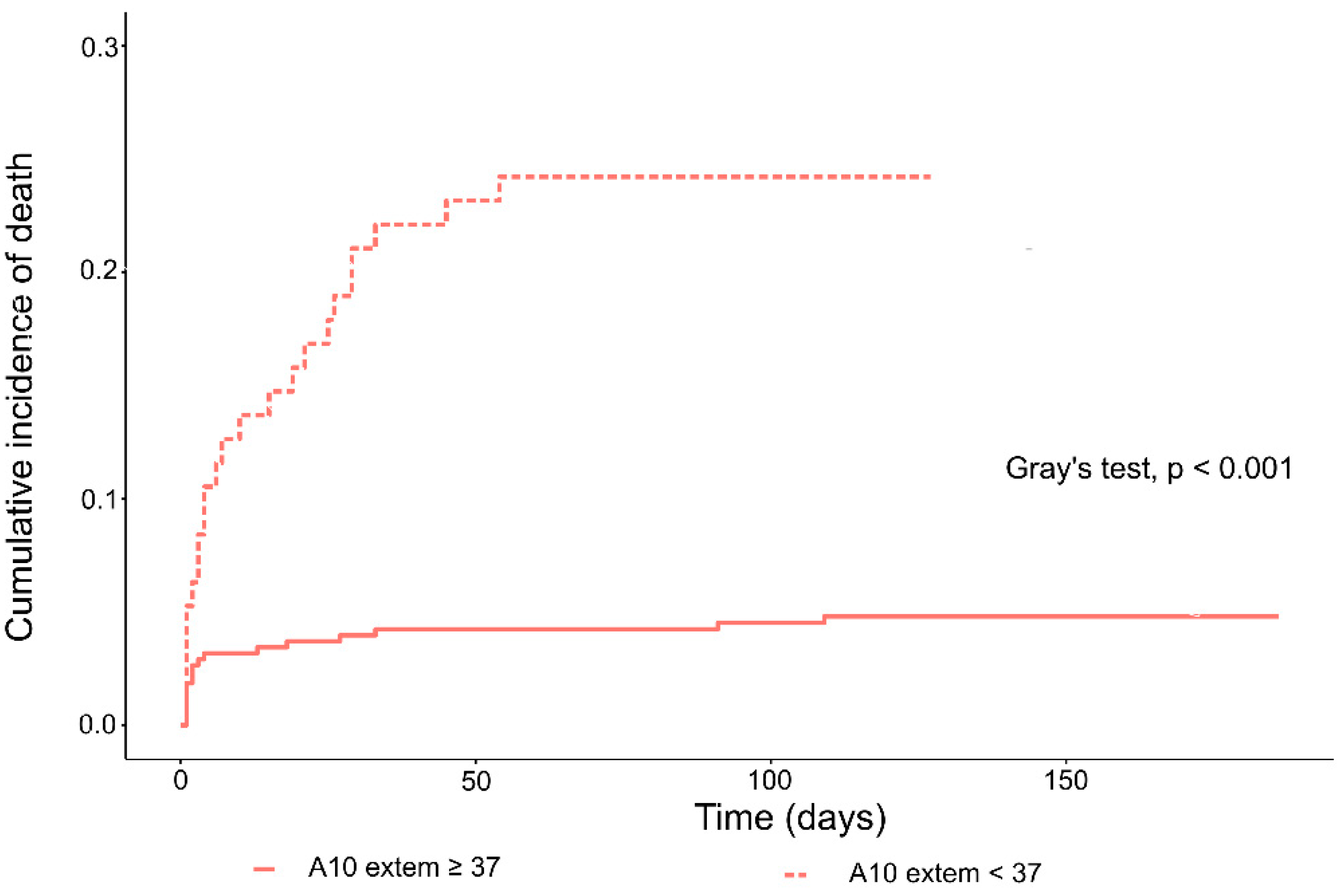
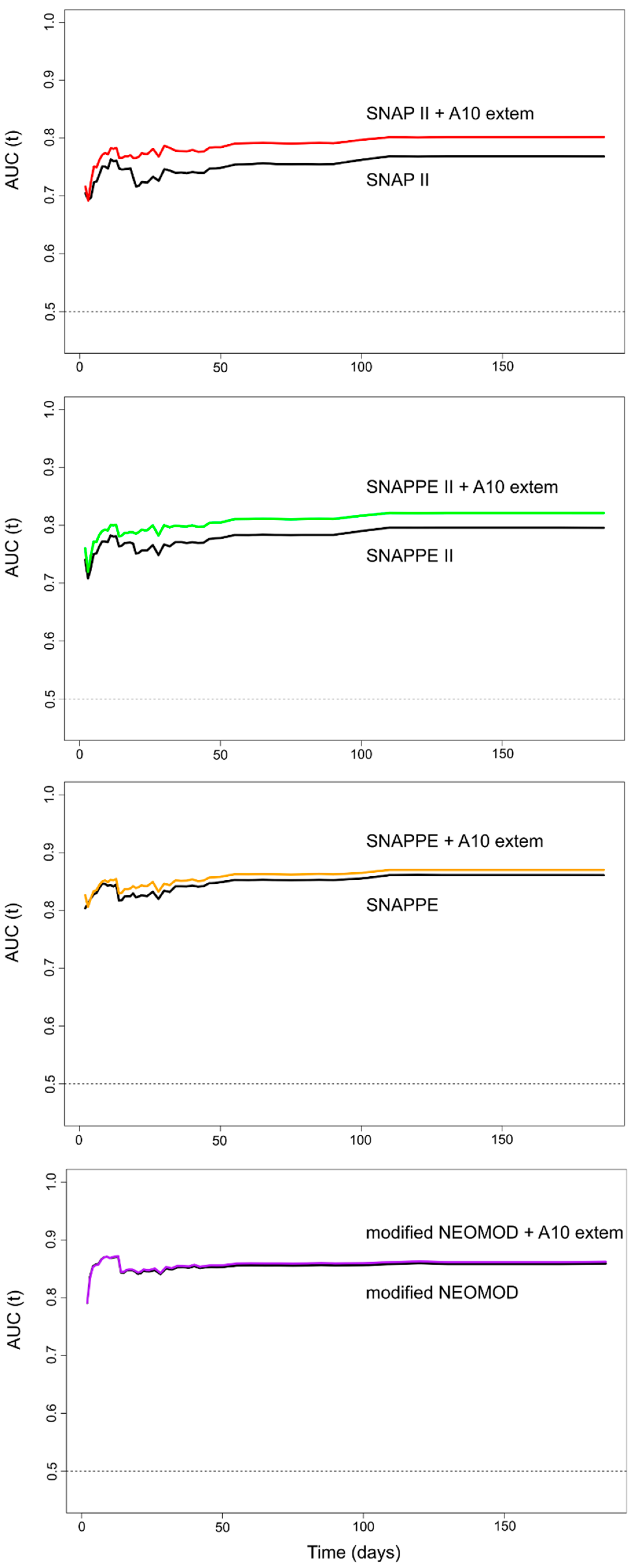
3.2. Multivariable Models including the A10 EXTEM Parameter
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Dorling, J.S.; Field, D.J.; Manktelow, B. Neonatal disease severity scoring systems. Arch. Dis. Child. Fetal Neonatal Ed. 2005, 90, F11–F16. [Google Scholar] [CrossRef] [PubMed]
- Pollack, M.M.; Koch, M.A.; Bartel, D.A.; Rapoport, I.; Dhanireddy, R.; El-Mohandes, A.A.; Harkavy, K.; Subramanian, K.N. A comparison of neonatal mortality risk prediction models in very low birth weight infants. Pediatrics 2000, 105, 1051–1057. [Google Scholar] [CrossRef] [PubMed]
- Janota, J.; Stranák, Z.; Statecná, B.; Dohnalová, A.; Sípek, A.; Simák, J. Characterization of multiple organ dysfunction syndrome in very low birthweight infants: A new sequential scoring system. Shock 2001, 15, 348–352. [Google Scholar] [CrossRef]
- Wood, N.S.; Marlow, N.; Costeloe, K.; Gibson, A.T.; Wilkinson, A.R. Neurologic and developmental disability after extremely preterm birth. EPICure Study Group. N. Engl. J. Med. 2000, 343, 378–384. [Google Scholar] [CrossRef] [PubMed]
- Levi, M.; van der Poll, T. Inflammation and coagulation. Crit. Care Med. 2010, 38, S26–S34. [Google Scholar] [CrossRef] [PubMed]
- van der Poll, T.; Büller, H.R.; ten Cate, H.; Wortel, C.H.; Bauer, K.A.; van Deventer, S.J.; Hack, C.E.; Sauerwein, H.P.; Rosenberg, R.D.; ten Cate, J.W. Activation of coagulation after administration of tumor necrosis factor to normal subjects. N. Engl. J. Med. 1990, 322, 1622–1627. [Google Scholar] [CrossRef] [PubMed]
- Levi, M.; van der Poll, T. Two-way interactions between inflammation and coagulation. Trends Cardiovasc. Med. 2005, 15, 254–259. [Google Scholar] [CrossRef] [PubMed]
- Mallett, S.V.; Cox, D.J. Thrombelastography. Br. J. Anaesth. 1992, 69, 307–313. [Google Scholar] [CrossRef]
- Sokou, R.; Tsantes, A.G.; Konstantinidi, A.; Ioakeimidis, G.; Lampridou, M.; Parastatidou, S.; Theodoraki, M.; Piovani, D.; Iliodromiti, Z.; Boutsikou, T.; et al. Rotational thromboelastometry in neonates admitted to a Neonatal Intensive Care Unit. A large cross-sectional study. Semin. Thromb. Hemost. 2021, 47, 875–884. [Google Scholar] [CrossRef]
- Sokou, R.; Giallouros, G.; Konstantinidi, A.; Pantavou, K.; Nikolopoulos, G.; Bonovas, S.; Lytras, T.; Kyriakou, E.; Lambadaridis, I.; Gounaris, A.; et al. Thromboelastometry for diagnosis of neonatal sepsis-associated coagulopathy: An observational study. Eur. J. Pediatrics 2018, 177, 355–362. [Google Scholar] [CrossRef]
- Konstantinidi, A.; Sokou, R.; Tsantes, A.G.; Parastatidou, S.; Bonovas, S.; Kouskouni, E.; Gounaris, A.K.; Tsantes, A.E.; Iacovidou, N. Thromboelastometry Variables in Neonates with Perinatal Hypoxia. Semin. Thromb. Hemost. 2020, 46, 428–434. [Google Scholar] [CrossRef]
- Cetinkaya, M.; Köksal, N.; Özkan, H. A new scoring system for evaluation of multiple organ dysfunction syndrome in premature infants. Am. J. Crit. Care 2012, 21, 328–337. [Google Scholar] [CrossRef] [PubMed]
- Richardson, D.K.; Corcoran, J.D.; Escobar, G.J.; Lee, S.K. SNAP-II and SNAPPE-II: Simplified newborn illness severity and mortality risk scores. J. Pediatrics 2001, 138, 92–100. [Google Scholar] [CrossRef] [PubMed]
- Richardson, D.K.; Phibbs, C.S.; Gray, J.E.; McCormick, M.C.; Workman-Daniels, K.; Goldmann, D.A. Birth weight and illness severity: Independent predictors of neonatal mortality. Pediatrics 1993, 91, 969–975. [Google Scholar] [CrossRef]
- Janota, J.; Simak, J.; Stranak, Z.; Matthews, T.; Clarke, T.; Corcoran, D. Critically ill newborns with multiple organ dysfunction: Assessment by NEOMOD score in a tertiary NICU. Ir. J. Med. Sci. 2008, 177, 11–17. [Google Scholar] [CrossRef] [PubMed]
- Tarnow-Mordi, W.; Ogston, S.; Wilkinson, A.R.; Reid, E.; Gregory, J.; Saeed, M.; Wilkie, R. Predicting death from initial disease severity in very low birthweight infants: A method for comparing the performance of neonatal units. BMJ 1990, 300, 1611–1614. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Network, The International Neonatal. The CRIB (clinical risk index for babies) score: A tool for assessing initial neonatal risk and comparing performance of neonatal intensive care units. Lancet 1993, 342, 193–198. [Google Scholar] [CrossRef]
- Pollack, M.M.; Ruttimann, U.E.; Getson, P.R. Pediatric risk of mortality (PRISM) score. Crit. Care Med. 1988, 16, 1110–1116. [Google Scholar] [CrossRef]
- Knaus, W.A.; Wagner, D.P.; Draper, E.A.; Zimmerman, J.E.; Bergner, M.; Bastos, P.G.; Sirio, C.A.; Murphy, D.J.; Lotring, T.; Damiano, A.; et al. The APACHE III prognostic system. Risk prediction of hospital mortality for critically ill hospitalized adults. Chest 1991, 100, 1619–1636. [Google Scholar] [CrossRef] [Green Version]
- Le Gall, J.R.; Lemeshow, S.; Saulnier, F. A new Simplified Acute Physiology Score (SAPS II) based on a European/North American multicenter study. JAMA 1993, 270, 2957–2963. [Google Scholar] [CrossRef]
- Wolkewitz, M.; Cooper, B.S.; Bonten, M.J.; Barnett, A.G.; Schumacher, M. Interpreting and comparing risks in the presence of competing events. BMJ 2014, 349, g5060. [Google Scholar] [CrossRef] [Green Version]
- Fine, J.P.; Gray, R.J. A Proportional Hazards Model for the Subdistribution of a Competing Risk. J. Am. Stat. Assoc. 1999, 94, 496–509. [Google Scholar] [CrossRef]
- Kamarudin, A.N.; Cox, T.; Kolamunnage-Dona, R. Time-dependent ROC curve analysis in medical research: Current methods and applications. BMC Med. Res. Methodol. 2017, 17, 53. [Google Scholar] [CrossRef] [Green Version]
- Gray, R.J. A Class of K-Sample Tests for Comparing the Cumulative Incidence of a Competing Risk. Ann. Stat. 1988, 16, 1141–1154. [Google Scholar] [CrossRef]
- Richardson, D.K.; Gray, J.E.; McCormick, M.C.; Workman, K.; Goldmann, D.A. Score for Neonatal Acute Physiology: A physiologic severity index for neonatal intensive care. Pediatrics 1993, 91, 617–623. [Google Scholar]
- Morse, S.; Groer, M.; Shelton, M.M.; Maguire, D.; Ashmeade, T. A Systematic Review: The Utility of the Revised Version of the Score for Neonatal Acute Physiology among Critically Ill Neonates. J. Perinat. Neonatal Nurs. 2015, 29, 315–344-E2. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lim, L.; Rozycki, H.J. Postnatal SNAP-II scores in neonatal intensive care unit patients: Relationship to sepsis, necrotizing enterocolitis, and death. J. Matern. -Fetal Neonatal Med. 2008, 21, 415–419. [Google Scholar] [CrossRef] [PubMed]
- Griffin, M.P.; Moorman, J.R. Toward the early diagnosis of neonatal sepsis and sepsis-like illness using novel heart rate analysis. Pediatrics 2001, 107, 97–104. [Google Scholar] [CrossRef]
- Sundaram, V.; Dutta, S.; Ahluwalia, J.; Narang, A. Score for neonatal acute physiology II predicts mortality and persistent organ dysfunction in neonates with severe septicemia. Indian Pediatrics 2009, 46, 775–780. [Google Scholar]
- Costeloe, K.; Hennessy, E.; Gibson, A.T.; Marlow, N.; Wilkinson, A.R. The EPICure study: Outcomes to discharge from hospital for infants born at the threshold of viability. Pediatrics 2000, 106, 659–671. [Google Scholar] [CrossRef] [Green Version]
- Santhakumaran, S.; Statnikov, Y.; Gray, D.; Battersby, C.; Ashby, D.; Modi, N. Survival of very preterm infants admitted to neonatal care in England 2008–2014: Time trends and regional variation. Arch. Dis. Child. Fetal Neonatal Ed. 2018, 103, F208–F215. [Google Scholar] [CrossRef]
- Lee, S.M.; Lee, M.H.; Chang, Y.S. The Clinical Risk Index for Babies II for Prediction of Time-Dependent Mortality and Short-Term Morbidities in Very Low Birth Weight Infants. Neonatology 2019, 116, 244–251. [Google Scholar] [CrossRef] [PubMed]
- Parry, G.; Tucker, J.; Tarnow-Mordi, W. CRIB II: An update of the clinical risk index for babies score. Lancet 2003, 361, 1789–1791. [Google Scholar] [CrossRef]
- Veldman, A.; Fischer, D.; Nold, M.; Wong, F. Disseminated Intravascular Coagulation in Term and Preterm Neonates. Semin. Thromb. Hemost. 2010, 36, 419–428. [Google Scholar] [CrossRef] [PubMed]
- Adamzik, M.; Langemeier, T.; Frey, U.H.; Görlinger, K.; Saner, F.; Eggebrecht, H.; Peters, J.; Hartmann, M. Comparison of thrombelastometry with simplified acute physiology score II and sequential organ failure assessment scores for the prediction of 30-day survival: A cohort study. Shock 2011, 35, 339–342. [Google Scholar] [CrossRef]
- Ostrowski, S.R.; Windeløv, N.A.; Ibsen, M.; Haase, N.; Perner, A.; Johansson, P.I. Consecutive thrombelastography clot strength profiles in patients with severe sepsis and their association with 28-day mortality: A prospective study. J. Crit. Care 2013, 28, 317.e1–317.e11. [Google Scholar] [CrossRef] [PubMed]
- Semeraro, N.; Ammollo, C.T.; Semeraro, F.; Colucci, M. Sepsis-associated disseminated intravascular coagulation and thromboembolic disease. Mediterr. J. Hematol. Infect. Dis. 2010, 2, e2010024. [Google Scholar] [CrossRef]

| Mean ± SD; Median (IQR) or n (%) | |
|---|---|
| Gender (males) | 300 (63.4%) |
| Gestational age (weeks) | 35.2 ± 4.37; 37 (32–39) |
| Birth weight (g) | 2434 ± 983; 2580 (1480–3240) |
| Cesarean section | 320 (67.7%) |
| 5 min APGAR score | 8.13 ± 1.54; 8 (8–9) |
| Temperature (°C) | 36.9 ± 0.53; 37.0 (36.7–37.1) |
| Mean blood pressure (mmHg) | 53.1 ± 9.1; 53.0 (47.0–58.0) |
| Blood Ph | 7.38 ± 0.08; 7.39 (7.35–7.43) |
| SNAP II | 3.87 ± 7.53; 0 (0–5) |
| SNAPPE II | 7.86 ± 12.2; 5 (0–12) |
| SNAPPE | 7.62 ± 10.4; 4 (1–10) |
| NEOMOD score | 5.09 ± 2.99; 4 (3–7) |
| Suspected sepsis | 176 (37.2%) |
| Sepsis | 136 (28.8%) |
| Respiratory distress syndrome | 243 (51.4%) |
| Intraventricular hemorrhage | 147 (31.1%) |
| Intrauterine growth retardation | 57 (12.1%) |
| Perinatal hypoxia | 144 (30.4%) |
| Acute renal failure | 70 (14.8%) |
| Disseminated intravascular coagulopathy | 77 (16.3%) |
| Periventricular leuokomalacia | 69 (14.6%) |
| Seizures | 32 (6.8%) |
| Necrotizing enterocolitis | 18 (3.8%) |
| WBC (×103, cells/µL) | 14.5 ± 8.07; 12.9 (9.47–17.9) |
| Neutrophils (%) | 58.3 ± 17.5; 60.5 (47.0–72.0) |
| Platelets (×103, cells/µL) | 216 ± 136; 221 (100–295) |
| Albumin (g/dL) | 2.56 ± 0.43; 2.50 (2.30–2.80) |
| Hematocrit (%) | 41.1 ± 7.08; 40.9 (36.3–45.9) |
| C-reactive protein (mg/L) | 33.1 ± 45.2; 13.6 (3.40–47.2) |
| SGOT (IU/L) | 120 ± 397; 56.0 (34.0–92.0) |
| SGPT (IU/L) | 47.7 ± 125; 19.0 (12.0–35.0) |
| Total bilirubin (mg/dL) | 7.57 ± 6.63; 6.05 (3.95–9.45) |
| Direct bilirubin (mg/dL) | 1.39 ± 4.39; 0.30 (0.20–0.50) |
| Blood urea nitrogen (mg/dL) | 40.4 ± 35.2; 30.0 (20.0–50.0) |
| Creatinine (mg/dL) | 0.66 ± 0.39; 0.60 (0.40–0.80) |
| Extem ROTEMS parameters: | |
| CT | 76.4 ± 294; 52.0 (45.0–63.0) |
| A10 | 49.3 ± 15.3; 52.0 (41.0–60.0) |
| A20 | 54.6 ± 14.8; 58.0 (47.0–65.0) |
| A30 | 55.6 ± 14.5; 58.0 (48.0–65.0) |
| CFT | 189 ± 521; 88.0 (62.0–140) |
| MCF (mm) | 56.7 ± 15.0; 59.0 (49.0–67.0) |
| ALPHA-angle | 71.5 ± 12.3; 75.0 (68.0–80.0) |
| LI60 (%) | 94.5 ± 7.46; 95.0 (93.0–99.0) |
| ML (%) | 10.1 ± 12.0; 8.00 (3.00–13.00) |
| Time (Days) a | SNAP II | SNAPPE II | SNAPPE | Modified NEOMOD |
|---|---|---|---|---|
| 5 | 0.724 (0.617–0.830) | 0.750 (0.638–0.863) | 0.828 (0.741–0.915) b,c | 0.858 (0.779–0.936) b,c |
| 15 | 0.746 (0.644–0.847) | 0.765 (0.659–0.871) | 0.818 (0.725–0.910) | 0.843 (0.757–0.929) b |
| 30 | 0.746 (0.656–0.837) | 0.767 (0.675–0.859) | 0.834 (0.756–0.912) b,c | 0.851 (0.780–0.921) b,c |
| 60 | 0.755 (0.668–0.842) | 0.783 (0.697–0.869) | 0.852 (0.780–0.925) b,c | 0.856 (0.792–0.920) b,c |
| 90 | 0.755 (0.668–0.842) | 0.783 (0.697–0.870) | 0.852 (0.780–0.925) b,c | 0.856 (0.791–0.920) b,c |
| 120 | 0.768 (0.685–0.852) | 0.796 (0.713–0.879) | 0.862 (0.793–0.930) b,c | 0.860 (0.798–0.921) b |
| Time (Days) a | SNAP II | SNAPPE II | SNAPPE | Modified NEOMOD |
|---|---|---|---|---|
| Preterm neonates (n = 224) | ||||
| 5 | 0.688 (0.548–0.828) | 0.747 (0.595–0.900) | 0.815 (0.714–0.916) | 0.792 (0.664–0.921) |
| 15 | 0.715 (0.580–0.850) | 0.770 (0.625–0.915) | 0.834 (0.737–0.930) b | 0.806 (0.683–0.928) |
| 30 | 0.709 (0.591–0.828) | 0.763 (0.641–0.885) | 0.843 (0.763–0.924) b | 0.819 (0.720–0.917) |
| 60 | 0.694 (0.574–0.814) | 0.760 (0.641–0.879) | 0.847 (0.768–0.925) b | 0.818 (0.723–0.912) |
| 90 | 0.695 (0.575–0.815) | 0.761 (0.642–0.880) | 0.847 (0.769–0.926) b | 0.817 (0.722–0.912) |
| 120 | 0.693 (0.574–0.813) | 0.761 (0.643–0.879) | 0.849 (0.771–0.927) b | 0.820 (0.725–0.916) |
| Term neonates d (n = 249) | ||||
| 5 | 0.827 (0.676–0.978) | 0.783 (0.612–0.954) | 0.819 (0.644–0.994) | 0.928 (0.855–0.999) b,c |
| 15 | 0.814 (0.666–0.962) | 0.780 (0.617–0.944) | 0.779 (0.602–0.956) | 0.865 (0.728–0.999) |
| 30 | 0.821 (0.688–0.954) | 0.787 (0.641–0.933) | 0.805 (0.657–0.952) | 0.868 (0.757–0.979) |
| 60 | 0.845 (0.731–0.959) | 0.820 (0.693–0.947) | 0.843 (0.714–0.972) | 0.881 (0.787–0.975) |
| 90 | 0.845 (0.731–0.959) | 0.820 (0.693–0.947) | 0.843 (0.714–0.972) | 0.881 (0.787–0.975) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sokou, R.; Tritzali, M.; Piovani, D.; Konstantinidi, A.; Tsantes, A.G.; Ioakeimidis, G.; Lampridou, M.; Parastatidou, S.; Iacovidou, N.; Kokoris, S.; et al. Comparative Performance of Four Established Neonatal Disease Scoring Systems in Predicting In-Hospital Mortality and the Potential Role of Thromboelastometry. Diagnostics 2021, 11, 1955. https://doi.org/10.3390/diagnostics11111955
Sokou R, Tritzali M, Piovani D, Konstantinidi A, Tsantes AG, Ioakeimidis G, Lampridou M, Parastatidou S, Iacovidou N, Kokoris S, et al. Comparative Performance of Four Established Neonatal Disease Scoring Systems in Predicting In-Hospital Mortality and the Potential Role of Thromboelastometry. Diagnostics. 2021; 11(11):1955. https://doi.org/10.3390/diagnostics11111955
Chicago/Turabian StyleSokou, Rozeta, Maroula Tritzali, Daniele Piovani, Aikaterini Konstantinidi, Andreas G. Tsantes, Georgios Ioakeimidis, Maria Lampridou, Stavroula Parastatidou, Nicoletta Iacovidou, Styliani Kokoris, and et al. 2021. "Comparative Performance of Four Established Neonatal Disease Scoring Systems in Predicting In-Hospital Mortality and the Potential Role of Thromboelastometry" Diagnostics 11, no. 11: 1955. https://doi.org/10.3390/diagnostics11111955
APA StyleSokou, R., Tritzali, M., Piovani, D., Konstantinidi, A., Tsantes, A. G., Ioakeimidis, G., Lampridou, M., Parastatidou, S., Iacovidou, N., Kokoris, S., Nikolopoulos, G. K., Kopterides, P., Bonovas, S., & Tsantes, A. E. (2021). Comparative Performance of Four Established Neonatal Disease Scoring Systems in Predicting In-Hospital Mortality and the Potential Role of Thromboelastometry. Diagnostics, 11(11), 1955. https://doi.org/10.3390/diagnostics11111955











