Design and Preclinical Evaluation of Nicotine–Stearic Acid Conjugate-Loaded Solid Lipid Nanoparticles for Transdermal Delivery: A Technical Note
Abstract
1. Introduction
2. Materials and Methods
2.1. Materials
2.2. Methods
2.2.1. Preparation of SLNs
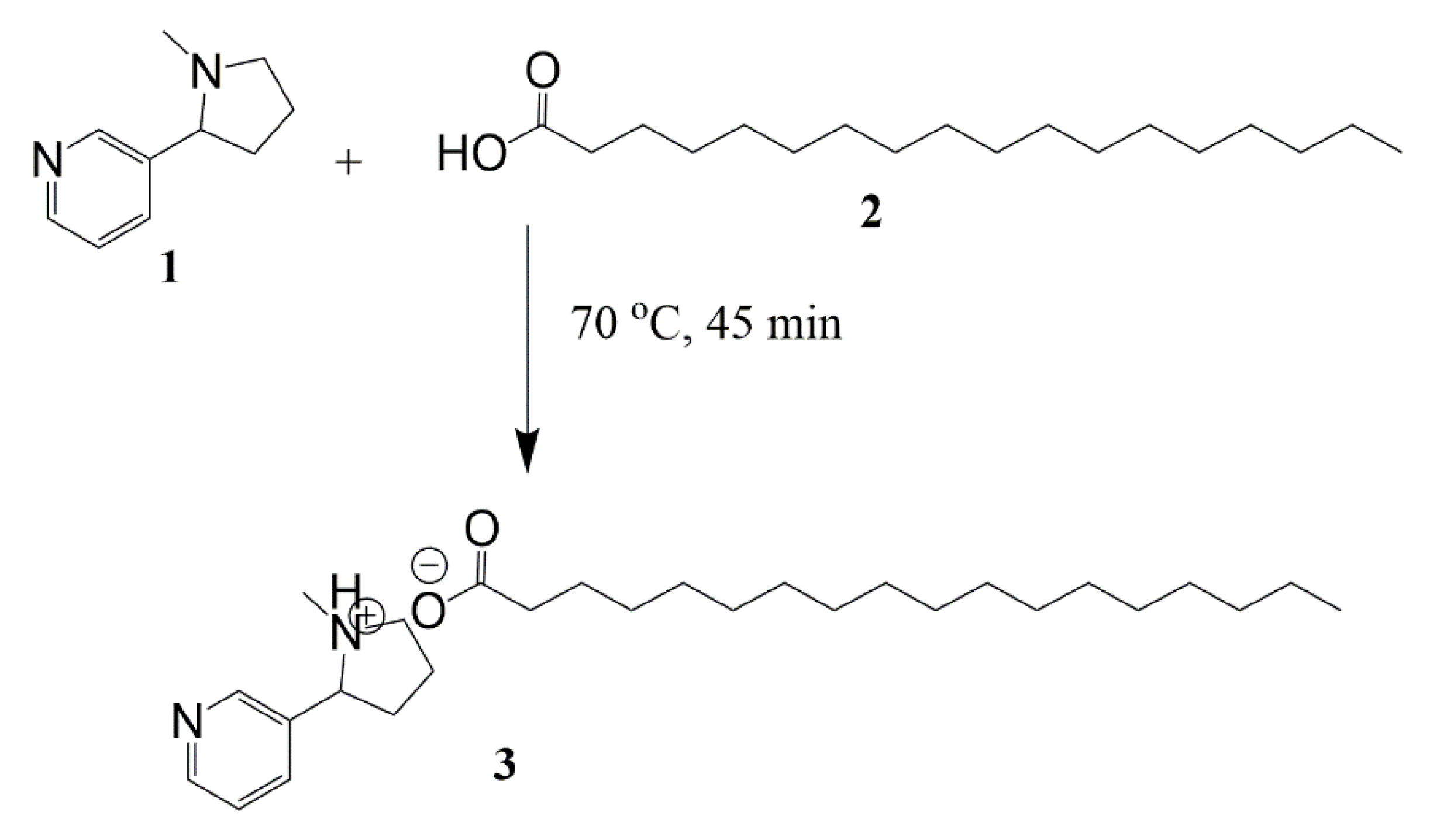
2.2.2. Preparation of Nicotine–Stearic Acid (NSA) Conjugate
2.2.3. Particle Size and ZP Analysis by DLS
2.2.4. Percentage Entrapment Efficiency (%EE) and Loading Capacity (%LC)
2.2.5. Scanning Transmission Electron Microscopy
2.2.6. Differential Scanning Calorimetry (DSC)
2.2.7. X-ray Diffraction (XRD)
2.2.8. Physical Stability Studies
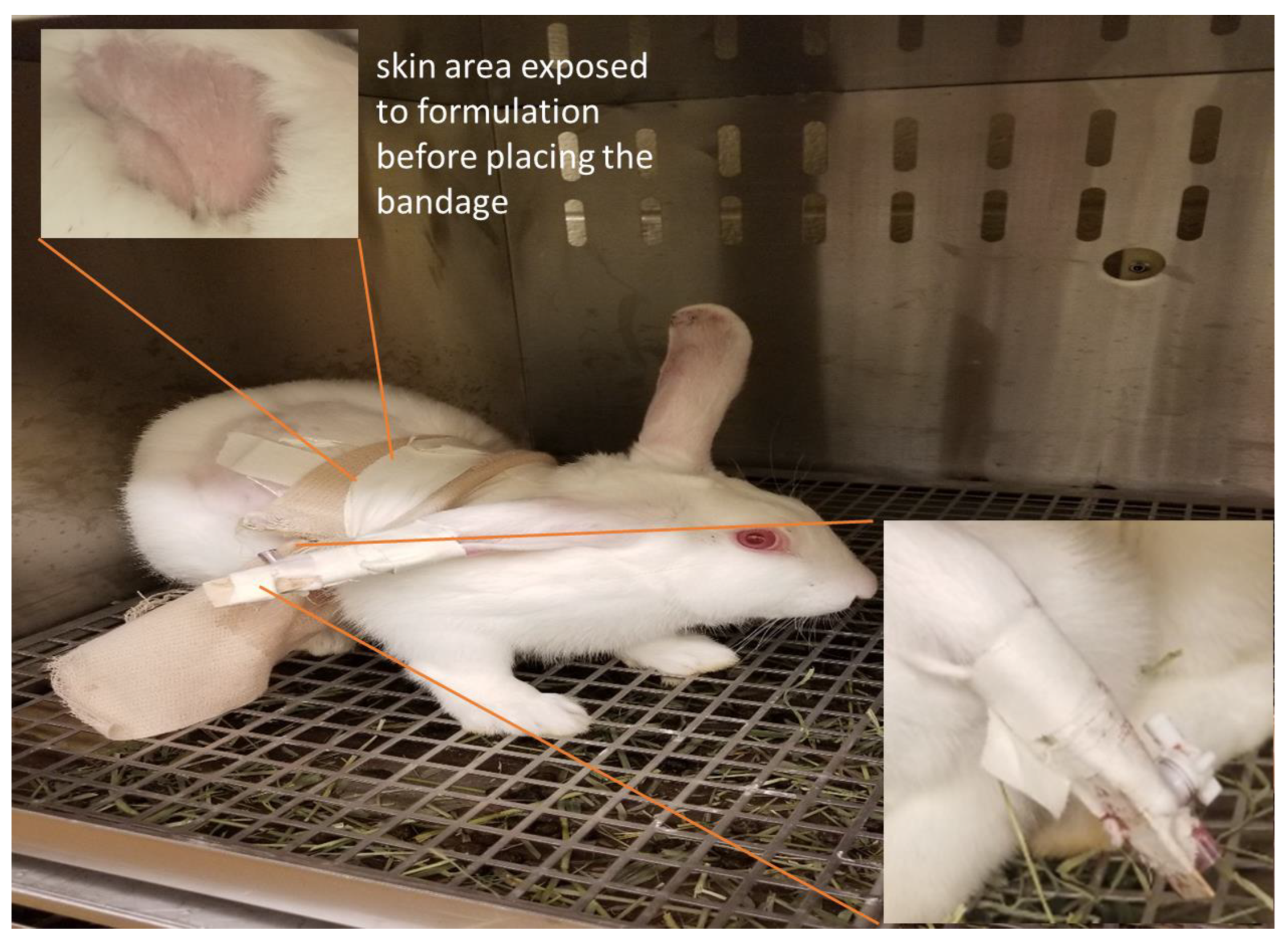
2.2.9. Testing of Nicotine Formulations in Rabbits
2.2.10. Statistical Analysis
3. Results
3.1. Optimization of SLN Formulation
3.1.1. Effect of Poloxamer 188 Concentration
3.1.2. Effect of Nicotine Loading
3.1.3. Preparation of NSA Conjugate and Loading into SLNs
3.2. Surface Morphology of SLNs
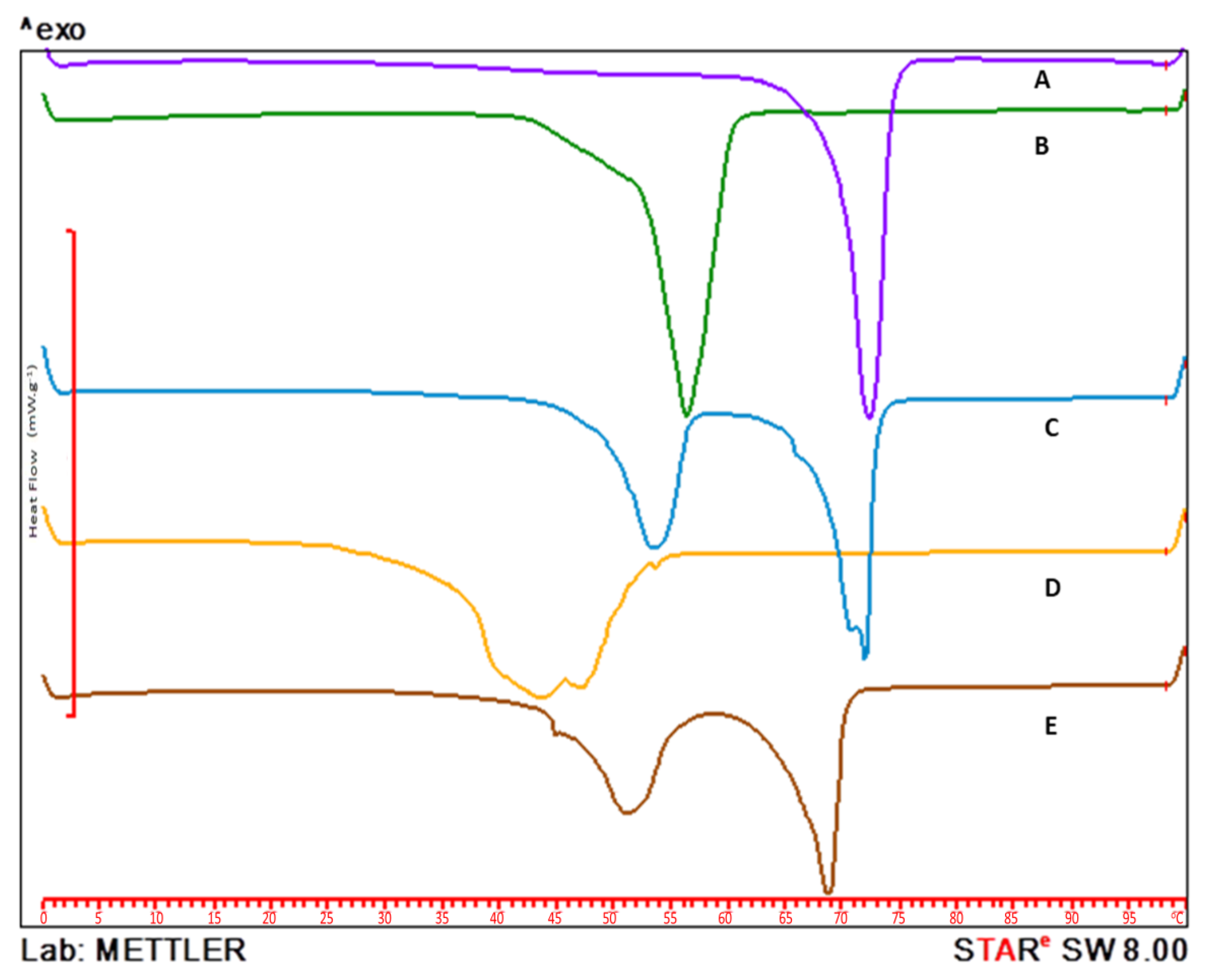
3.3. Differential Scanning Calorimetry (DSC)
3.4. X-ray Diffraction
3.5. Short Term Physical Stability
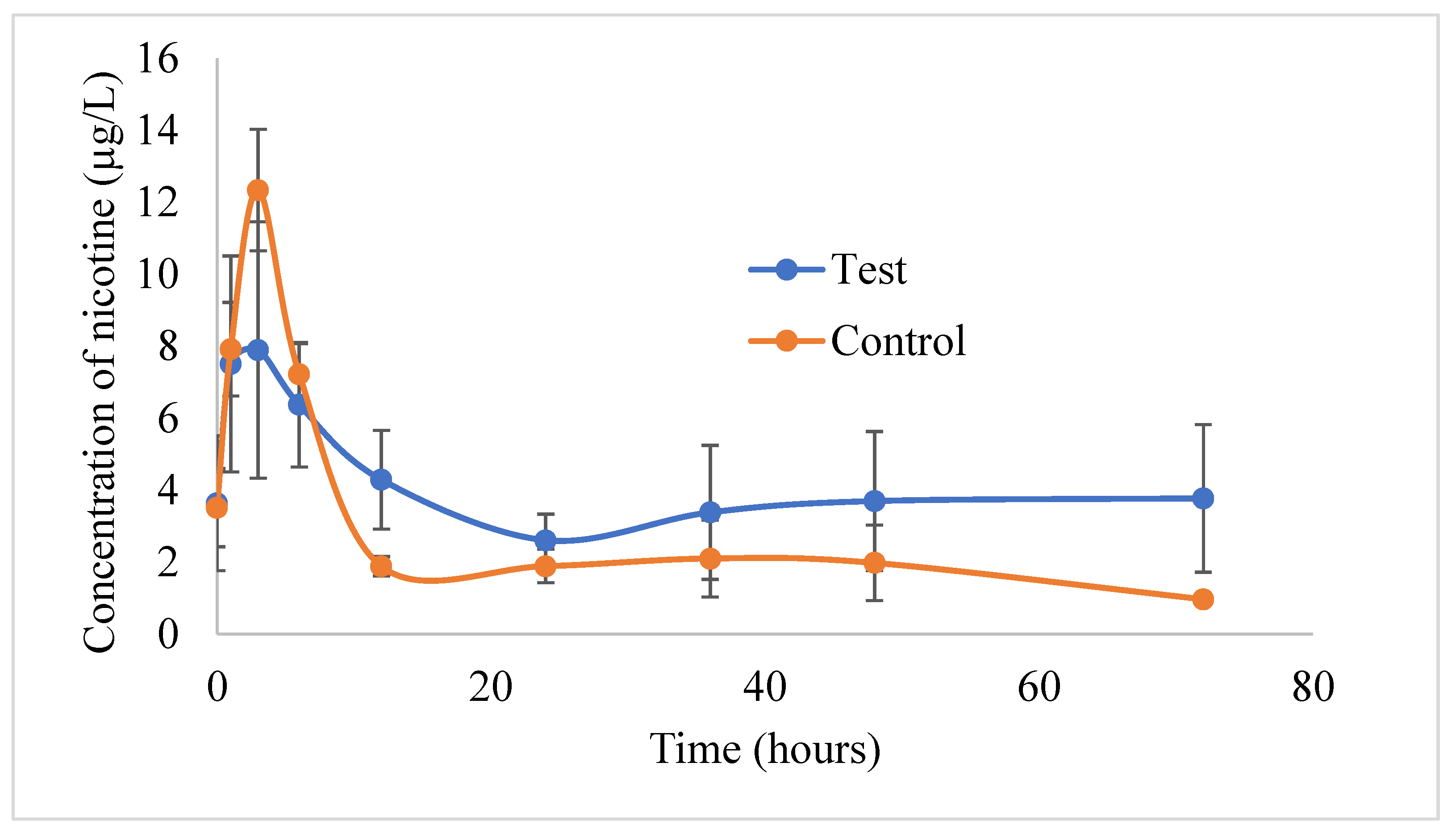
3.6. Analysis of Rabbit Plasma Samples
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Rasmussen, S.; Horkan, K.H.; Kotler, M. Pharmacokinetic evaluation of two nicotine patches in smokers. Clin. Pharmacol. Drug Dev. 2018, 7, 506–512. [Google Scholar] [CrossRef]
- Jain, D.; Chaudhary, P.; Varshney, N.; Bin Razzak, K.S.; Verma, D.; Khan Zahra, T.R.; Janmeda, P.; Sharifi-Rad, J.; Daştan, S.D.; Mahmud, S.; et al. Tobacco smoking and liver cancer risk: Potential avenues for carcinogenesis. J. Oncol. 2021, 2021, 5905357. [Google Scholar] [CrossRef]
- Gulati, G.K.; Berger, L.R.; Hinds, B.J. A preclinical evaluation of a programmable CNT membrane device for transdermal nicotine delivery in hairless guinea pigs. J. Control. Release 2018, 293, 135–143. [Google Scholar] [CrossRef]
- Lardi, C.; Vogt, S.; Pollak, S.; Thierauf, A. Complex suicide with homemade nicotine patches. Forensic Sci. Int. 2014, 236, e14–e18. [Google Scholar] [CrossRef]
- Glover, L.M.; Ma, J.Z.; Kesh, A.; Tompkins, L.K.; Hart, J.L.; Mattingly, D.T.; Walker, K.; Robertson, R.M.; Payne, T.; Sims, M. The social patterning of electronic nicotine delivery system use among US adults. Prev. Med. 2018, 116, 27–31. [Google Scholar] [CrossRef]
- Riggs, N.R.; Pentz, M.A. Inhibitory control and the onset of combustible cigarette, e-cigarette, and hookah use in early adolescence: The moderating role of socioeconomic status. Child Neuropsychol. 2016, 22, 679–691. [Google Scholar] [CrossRef]
- Dai, H. Tobacco Product Use Among Lesbian, Gay, and Bisexual Adolescents. Pediatrics 2017, 139, e20163276. [Google Scholar] [CrossRef]
- Harrell, M.B.; Mantey, D.S.; Chen, B.; Kelder, S.H.; Barrington-Trimis, J. Impact of the e-cigarette era on cigarette smoking among youth in the United States: A population-level study. Prev. Med. 2022, 164, 107265. [Google Scholar] [CrossRef]
- Juluri, A.; Modepalli, N.; Jo, S.; Repka, M.A.; Nanjappa Shivakumar, H.; Narasimha Murthy, S. Minimally Invasive Transdermal Delivery of Iron–Dextran. J. Pharm. Sci. 2013, 102, 987–993. [Google Scholar] [CrossRef]
- Schlam, T.R.; Cook, J.W.; Baker, T.B.; Hayes-Birchler, T.; Bolt, D.M.; Smith, S.S.; Fiore, M.C.; Piper, M.E. Can we increase smokers’ adherence to nicotine replacement therapy and does this help them quit? Psychopharmacology 2018, 235, 2065–2075. [Google Scholar] [CrossRef]
- Wadgave, U.; Nagesh, L. Nicotine Replacement Therapy: An Overview. Int. J. Health Sci. (Qassim) 2016, 10, 425–435. [Google Scholar] [CrossRef]
- Shiffman, S.; Brockwell, S.E.; Pillitteri, J.L.; Gitchell, J.G. Use of smoking-cessation treatments in the United States. Am. J. Prev. Med. 2008, 34, 102–111. [Google Scholar] [CrossRef]
- Hughes, J.R.; Solomon, L.J.; Peasley-Miklus, C.E.; Callas, P.W.; Fingar, J.R. Effectiveness of continuing nicotine replacement after a lapse: A randomized trial. Addict. Behav. 2018, 76, 68–81. [Google Scholar] [CrossRef]
- Herman, A.I.; Sofuoglu, M. Interventions For Addiction: Chapter 35. Medications to Treat Addictions: Nicotine Replacement; Elsevier Inc.: Amsterdam, The Netherlands, 2013. [Google Scholar]
- Li, Q.; Wan, X.; Liu, C.; Fang, L. Investigating the role of ion-pair strategy in regulating nicotine release from patch: Mechanistic insights based on intermolecular interaction and mobility of pressure sensitive adhesive. Eur. J. Pharm. Sci. 2018, 119, 102–111. [Google Scholar] [CrossRef]
- Ma, P.; Kendzor, D.E.; Poonawalla, I.B.; Balis, D.S.; Businelle, M.S. Daily nicotine patch wear time predicts smoking abstinence in socioeconomically disadvantaged adults: An analysis of ecological momentary assessment data. Drug Alcohol Depend. 2016, 169, 64–67. [Google Scholar] [CrossRef]
- Juluri, A.; Peddikotla, P.; Repka, M.A.; Murthy, S.N. Transdermal iontophoretic delivery of propofol: A general anaesthetic in the form of its phosphate salt. J. Pharm. Sci. 2013, 102, 500–507. [Google Scholar] [CrossRef]
- Ahluwalia, J.S.; McNagny, S.E.; Clark, W.S. Smoking cessation among inner-city African Americans using the nicotine transdermal patch. J. Gen. Intern. Med. 1998, 13, 1–8. [Google Scholar] [CrossRef]
- Cummings, K.M.; Hyland, A.; Ockene, J.K.; Hymowitz, N.; Manley, M. Use of the nicotine skin patch by smokers in 20 communities in the United States, 1992–1993. Tob. Control 1997, 6, S63. [Google Scholar] [CrossRef]
- Mills, E.J.; Wu, P.; Lockhart, I.; Wilson, K.; Ebbert, J.O. Adverse events associated with nicotine replacement therapy (NRT) for smoking cessation. A systematic review and meta-analysis of one hundred and twenty studies involving 177,390 individuals. Tob Induc. Dis. 2010, 8, 8. [Google Scholar] [CrossRef]
- Hollands, G.J.; Naughton, F.; Farley, A.; Lindson, N.; Aveyard, P. Interventions to increase adherence to medications for tobacco dependence. Cochrane Database Syst. Rev. 2019. [Google Scholar] [CrossRef]
- Balmford, J.; Borland, R.; Hammond, D.; Cummings, K.M. Adherence to and reasons for premature discontinuation from stop-smoking medications: Data from the ITC Four-Country Survey. Nicotine Tob. Res. 2011, 13, 94–102. [Google Scholar] [CrossRef]
- Shadel, W.G.; Galvan, F.H.; Tucker, J.S. Developing a nicotine patch adherence intervention for HIV-positive Latino smokers. Addict. Behav. 2016, 59, 52–57. [Google Scholar] [CrossRef]
- Sengar, V.; Jyoti, K.; Jain, U.K.; Katare, O.P.; Chandra, R.; Madan, J. Lipid nanoparticles for topical and transdermal delivery of pharmaceuticals and cosmeceuticals: A glorious victory. In Lipid Nanocarriers for Drug Targeting; Elsevier: Amsterdam, The Netherlands, 2018; pp. 413–436. [Google Scholar]
- Cannon, J.B. Lipids in transdermal and topical drug delivery. Am. Pharm. Rev. 2014, 17, 7. [Google Scholar]
- Jenning, V.; Gysler, A.; Schäfer-Korting, M.; Gohla, S.H. Vitamin A loaded solid lipid nanoparticles for topical use: Occlusive properties and drug targeting to the upper skin. Eur. J. Pharm. Biopharm. 2000, 49, 211–218. [Google Scholar] [CrossRef] [PubMed]
- Bhaskar, K.; Anbu, J.; Ravichandiran, V.; Venkateswarlu, V.; Rao, Y.M. Lipid nanoparticles for transdermal delivery of flurbiprofen: Formulation, in vitro, ex vivo and in vivo studies. Lipids Health Dis. 2009, 8, 6. [Google Scholar] [CrossRef] [PubMed]
- Ding, Y.; Nielsen, K.A.; Nielsen, B.P.; Bøje, N.W.; Müller, R.H.; Pyo, S.M. Lipid-drug-conjugate (LDC) solid lipid nanoparticles (SLN) for the delivery of nicotine to the oral cavity–optimization of nicotine loading efficiency. Eur. J. Pharm. Biopharm. 2018, 128, 10–17. [Google Scholar] [CrossRef]
- Nakmode, D.; Bhavana, V.; Thakor, P.; Madan, J.; Singh, P.K.; Singh, S.B.; Rosenholm, J.M.; Bansal, K.K.; Mehra, N.K. Fundamental Aspects of Lipid-Based Excipients in Lipid-Based Product Development. Pharmaceutics 2022, 14, 831. [Google Scholar] [CrossRef]
- Bolla, P.K.; Kalhapure, R.S.; Rodriguez, V.A.; Ramos, D.V.; Dahl, A.; Renukuntla, J. Preparation of solid lipid nanoparticles of furosemide-silver complex and evaluation of antibacterial activity. J. Drug Deliv. Sci. Technol. 2019, 49, 6–13. [Google Scholar] [CrossRef]
- Kalhapure, R.S.; Akamanchi, K.G. A novel biocompatible bicephalous dianionic surfactant from oleic acid for solid lipid nanoparticles. Colloids Surf B Biointerfaces 2013, 105, 215–222. [Google Scholar] [CrossRef]
- Kalhapure, R.S.; Bolla, P.K.; Boddu, S.H.; Renukuntla, J. Evaluation of Oleic Acid and Polyethylene Glycol Monomethyl Ether Conjugate (PEGylated Oleic Acid) as a Solubility Enhancer of Furosemide. Processes 2019, 7, 520. [Google Scholar] [CrossRef]
- Manca, M.L.; Castangia, I.; Matricardi, P.; Lampis, S.; Fernàndez-Busquets, X.; Fadda, A.M.; Manconi, M. Molecular arrangements and interconnected bilayer formation induced by alcohol or polyalcohol in phospholipid vesicles. Colloids Surf. B Biointerfaces 2014, 117, 360–367. [Google Scholar] [CrossRef]
- Godage, N.H.; Cudjoe, E.; Neupane, R.; Boddu, S.H.S.; Bolla, P.K.; Renukuntla, J.; Gionfriddo, E. Biocompatible SPME fibers for direct monitoring of nicotine and its metabolites at ultra trace concentration in rabbit plasma following the application of smoking cessation formulations. J. Chromatogr. A 2020, 1626, 461333. [Google Scholar] [CrossRef]
- Patere, S.N.; Desai, N.S.; Jain, A.S.; Kadam, P.P.; Thatte, U.M.; Gogtay, N.; Kapadia, C.J.; Farah, N.; Nagarsenker, M.S. Compritol®888 ATO a lipid excipient for sustained release of highly water soluble active: Formulation, scale-up and IVIVC study. Curr. Drug Deliv. 2013, 10, 548–556. [Google Scholar] [CrossRef]
- Shah, M.; Chuttani, K.; Mishra, A.K.; Pathak, K. Oral solid compritol 888 ATO nanosuspension of simvastatin: Optimization and biodistribution studies. Drug. Dev. Ind. Pharm. 2011, 37, 526–537. [Google Scholar] [CrossRef]
- Seo, J.W.; Kim, K.J.; Kim, S.H.; Hwang, K.M.; Seok, S.H.; Park, E.S. Effect of Process Parameters on Formation and Aggregation of Nanoparticles Prepared with a Shirasu Porous Glass Membrane. Chem. Pharm. Bull (Tokyo) 2015, 63, 792–798. [Google Scholar] [CrossRef]
- Park, K.M.; Lee, M.K.; Hwang, K.J.; Kim, C.K. Phospholipid-based microemulsions of flurbiprofen by the spontaneous emulsification process. Int. J. Pharm. 1999, 183, 145–154. [Google Scholar] [CrossRef]
- Rodriguez, V.A.; Bolla, P.K.; Kalhapure, R.S.; Boddu, S.H.S.; Neupane, R.; Franco, J.; Renukuntla, J. Preparation and Characterization of Furosemide-Silver Complex Loaded Chitosan Nanoparticles. Processes 2019, 7, 206. [Google Scholar] [CrossRef]
- Kalhapure, R.S.; Bolla, P.; Dominguez, D.C.; Dahal, A.; Boddu, S.H.; Renukuntla, J. FSE–Ag complex NS: Preparation and evaluation of antibacterial activity. IET Nanobiotechnol. 2018, 12, 836–840. [Google Scholar] [CrossRef]
- Rowe, R.C.; Sheskey, P.J.; Quinn, M.E. Hanbook of Pharmaceutical Excipients, 6th ed.; Pharmaceutical Press: London, UK, 2009. [Google Scholar]
- George, T.P. 31—Nicotine and Tobacco. In Goldman’s Cecil Medicine, 24th ed.; Goldman, L., Schafer, A.I., Eds.; W.B. Saunders: Philadelphia, PA, USA, 2012; pp. 142–146. [Google Scholar] [CrossRef]


| Poloxamer 188 (% w/w) | Size (nm) | PDI |
|---|---|---|
| 0.5 | 301.4 ± 70.94 | 0.306 ± 0.081 |
| 1 | 195.7 ± 26.77 | 0.338 ± 0.093 |
| 1.5 | 138.7 ± 9.923 | 0.291 ± 0.069 |
| 2 | 115.1 ± 0.873 | 0.246 ± 0.008 |
| Nicotine (% w/w) | Size (nm) | PDI | ZP (mV) | Entrapment Efficiency |
|---|---|---|---|---|
| 0.1 | 114.4 ± 2.33 | 0.213 ± 0.012 | −48.2 ± 3.49 | 4.59 ± 18.81 |
| 0.2 | 136.0 ± 23.47 | 0.271 ± 0.061 | −46.1 ± 7.56 | 11.51 ± 1.93 |
| 0.25 | 108.3 ± 2.77 | 0.201 ± 0.010 | −29.6 ± 6.95 | 15.66 ± 15.38 |
| 0.5 | 112.3 ± 1.54 | 0.197 ± 0.008 | −46.6 ± 4.89 | 11.15 ± 2.59 |
| 1.0 | 119.3 ± 2.70 | 0.151 ± 0.008 | −52.4 ± 4.54 | 16.47 ± 5.64 |
| Ingredient | Quantity |
|---|---|
| Nicotine−stearic acid conjugate (equivalent to 50 mg of nicotine) | 156 mg |
| Compritol 888 ATO | 500 mg |
| Poloxamer 188 | 300 mg |
| Milli-Q water (quantity sufficient) | 20 mL |
| Storage Condition | ||||||
|---|---|---|---|---|---|---|
| 4 °C | RT | 4 °C | RT | 4 °C | RT | |
| Time (Days) | Particle Size (nm) | PDI | ZP (mV) | |||
| 0 | 113.5 ± 00.91 | 113.5 ± 0.91 | 0.211 ± 0.01 | 0.211 ± 0.01 | −48.1 ± 5.75 | −48.1 ± 5.75 |
| 30 | 128.3 ± 10.40 | 116.0 ± 3.36 | 0.291 ± 0.04 | 0.230 ± 0.011 | −43.1 ± 4.12 | −51.3 ± 6.72 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Renukuntla, J.; Peterson-Sockwell, S.; Clark, B.A.; Godage, N.H.; Gionfriddo, E.; Bolla, P.K.; Boddu, S.H.S. Design and Preclinical Evaluation of Nicotine–Stearic Acid Conjugate-Loaded Solid Lipid Nanoparticles for Transdermal Delivery: A Technical Note. Pharmaceutics 2023, 15, 1043. https://doi.org/10.3390/pharmaceutics15041043
Renukuntla J, Peterson-Sockwell S, Clark BA, Godage NH, Gionfriddo E, Bolla PK, Boddu SHS. Design and Preclinical Evaluation of Nicotine–Stearic Acid Conjugate-Loaded Solid Lipid Nanoparticles for Transdermal Delivery: A Technical Note. Pharmaceutics. 2023; 15(4):1043. https://doi.org/10.3390/pharmaceutics15041043
Chicago/Turabian StyleRenukuntla, Jwala, Samuel Peterson-Sockwell, Bradley A. Clark, Nipunika H. Godage, Emanuela Gionfriddo, Pradeep Kumar Bolla, and Sai H. S. Boddu. 2023. "Design and Preclinical Evaluation of Nicotine–Stearic Acid Conjugate-Loaded Solid Lipid Nanoparticles for Transdermal Delivery: A Technical Note" Pharmaceutics 15, no. 4: 1043. https://doi.org/10.3390/pharmaceutics15041043
APA StyleRenukuntla, J., Peterson-Sockwell, S., Clark, B. A., Godage, N. H., Gionfriddo, E., Bolla, P. K., & Boddu, S. H. S. (2023). Design and Preclinical Evaluation of Nicotine–Stearic Acid Conjugate-Loaded Solid Lipid Nanoparticles for Transdermal Delivery: A Technical Note. Pharmaceutics, 15(4), 1043. https://doi.org/10.3390/pharmaceutics15041043













