Development of a Novel Lipid-Based Nanosystem Functionalized with WGA for Enhanced Intracellular Drug Delivery
Abstract
1. Introduction
2. Materials and Methods
2.1. Development and Characterization of the Lipid Nanocarriers
2.2. Nanocarriers Surface Functionalization
2.3. Evaluation of the Presence and Activity of Lectins WGA on the Surface of the Nanocarriers
2.3.1. Hemagglutinating Activity (HA)
2.3.2. Enzyme-Linked Immunosorbent Assay
2.4. Determination of Drug Content and Release Profile
2.5. In Vitro Studies: Internalization Assay, Cell Health, and Lipid Content
2.5.1. Cell Culture
2.5.2. Internalization Assays
2.5.3. High Content Analysis (HCA)
Cell Health
Lipid Content
2.6. Statistical Analysis
3. Results
3.1. Design of Lipid Nanocarriers: Development and Characterization
Particle Size, Polydispersion Index (PDI), and Zeta Potential of the Nanocarrieres Produced by High-Pressure Homogenization
3.2. Evaluation of the Presence and Activity of Lectins on the Surface of the Nanocarriers
3.2.1. Determination of Hemagglutination Activity
3.2.2. Enzyme-Linked Immunosorbent Assay (ELISA)
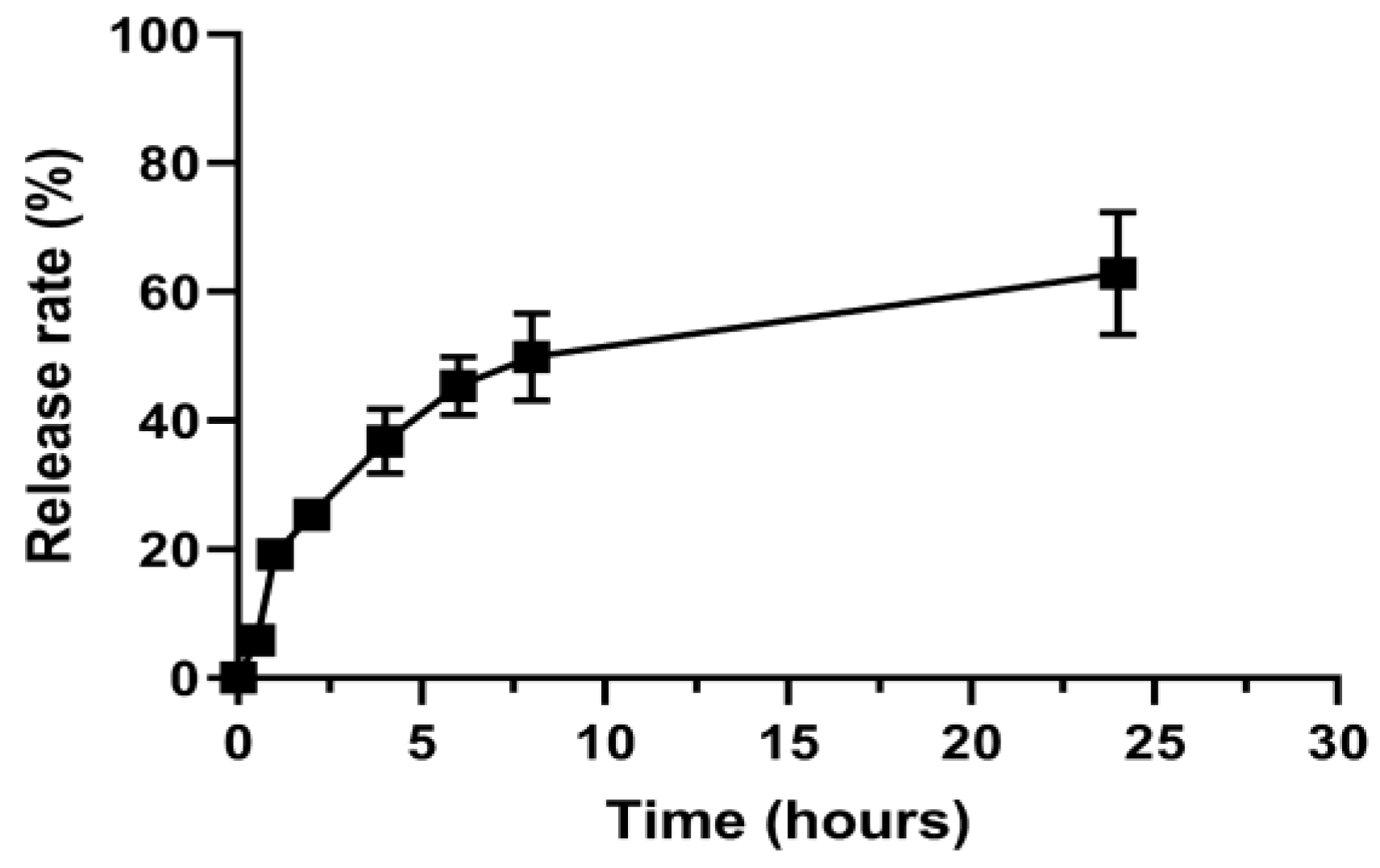
3.3. Drug Content and Release Profile
3.4. Flow Cytometry
3.5. Internalization of the Particles Functionalized with WGA Lectin
3.6. High Content Analysis (HCA)
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Dhiman, N.; Awasthi, R.; Sharma, B.; Kharkwal, H.; Kulkarni, G.T. Lipid nanoparticles as carriers for bioactive delivery. Front. Chem. 2021, 9, 580118. [Google Scholar] [CrossRef]
- Puri, A.; Loomis, K.; Smith, B.; Lee, J.-H.; Yavlovich, A.; Heldman, E.; Blumenthal, R. Lipid-based nanoparticles as pharmaceutical drug carriers: From concepts to clinic. Crit. Rev. Ther. Drug Carr. Syst. 2009, 26, 523–580. [Google Scholar] [CrossRef]
- Naseri, N.; Valizadeh, H.; Zakeri-Milani, P. Solid lipid nanoparticles and nanostructured lipid carriers: Structure preparation and application. Adv. Pharm. Bull. 2015, 5, 305–313. [Google Scholar] [CrossRef]
- Mo, Y.; Lim, L.-Y. Mechanistic study of the uptake of wheat germ agglutinin-conjugated PLGA nanoparticles by A549 cells. J. Pharm. Sci. 2004, 93, 20–28. [Google Scholar] [CrossRef]
- Berg, J.M.; Tymoczko, J.L.; Stryer, L. Lectins are specific carbohydrate-binding proteins. Section 4.1, The purification of proteins is an essential first step in understanding their function 2002. In Biochemistry, 5th ed.; W. H. Freeman and Company: New York, NY, USA, 2002. [Google Scholar]
- Reisch, A.; Klymchenko, A.S. Fluorescent polymer nanoparticles based on dyes: Seeking brighter tools for bioimaging. Small 2016, 12, 1968–1992. [Google Scholar] [CrossRef]
- Shen, Y.; Chen, J.; Liu, Q.; Feng, C.; Gao, X.; Wang, L.; Zhang, Q.; Jiang, X. Effect of wheat germ agglutinin density on cellular uptake and toxicity of wheat germ agglutinin conjugated PEG-PLA nanoparticles in Calu-3 cells. Int. J. Pharm. 2011, 413, 184–193. [Google Scholar] [CrossRef]
- Gabor, F.; Bogner, E.; Weissenboeck, A.; Wirth, M. The lectin-cell interaction and its implications to intestinal lectin-mediated drug delivery. Adv. Drug Deliv. Rev. 2004, 56, 459–480. [Google Scholar] [CrossRef]
- De Castro, C.E.; Ribeiro, C.A.S.; da Silva, M.C.C.; Gonçalves Dal-Bó, A.; Giacomelli, F.C. Sweetness reduces cytotoxicity and enables faster cellular uptake of Sub-30 Nm amphiphilic nanoparticles. Langmuir 2019, 35, 8060–8067. [Google Scholar] [CrossRef]
- Dal Bó, A.G.; Soldi, V.; Giacomelli, F.C.; Jean, B.; Pignot-Paintrand, I.; Borsali, R.; Fort, S. Self-assembled carbohydrate-based micelles for lectin targeting. Soft Matter 2011, 7, 3453. [Google Scholar] [CrossRef]
- Dal Bó, A.G.; Soldi, V.; Giacomelli, F.C.; Travelet, C.; Borsali, R.; Fort, S. Synthesis, micellization and lectin binding of new glycosurfactants. Carbohydr. Res. 2014, 397, 31–36. [Google Scholar] [CrossRef]
- Sharma, A.; Sharma, S.; Khuller, G.K. Lectin-functionalized poly (lactide-co-glycolide) nanoparticles as oral/aerosolized antitubercular drug carriers for treatment of tuberculosis. J. Antimicrob. Chemother. 2004, 54, 761–766. [Google Scholar] [CrossRef] [PubMed]
- Pandey, R.; Khuller, G.K. Nanotechnology based drug delivery system(s) for the management of tuberculosis. Indian J. Exp. Biol 2006, 44, 357–366. [Google Scholar] [PubMed]
- Hadrich, G.; Boschero, R.A.; Appel, A.S.; Falkembach, M.; Monteiro, M.; Da Silva, P.E.A.; Dailey, L.A.; Dora, C.L. Tuberculosis treatment facilitated by lipid nanocarriers: Can inhalation improve the regimen? Assay Drug Dev. Technol. 2020, 18, 298–307. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.-Y.; Koller, R.; Wirth, M.; Gabor, F. Lectin-coated PLGA microparticles: Thermoresponsive release and in vitro evidence for enhanced cell interaction. Int. J. Pharm. 2012, 436, 738–743. [Google Scholar] [CrossRef]
- Meng, Y.; Hou, X.; Lei, J.; Chen, M.; Cong, S.; Zhang, Y.; Ding, W.; Li, G.; Li, X. Multi-functional liposomes enhancing target and antibacterial immunity for antimicrobial and anti-biofilm against methicillin-resistant Staphylococcus aureus. Pharm. Res. 2016, 33, 769–775. [Google Scholar] [CrossRef]
- Liu, Y.; Liu, J.; Liang, J.; Zhang, M.; Li, Z.; Wang, Z.; Dang, B.; Feng, N. Mucosal Transfer of wheat germ agglutinin modified lipid–polymer hybrid nanoparticles for oral delivery of oridonin. Nanomed. Nanotechnol. Biol. Med. 2017, 13, 2219–2229. [Google Scholar] [CrossRef]
- Pooja, D.; Tunki, L.; Kulhari, H.; Reddy, B.B.; Sistla, R. Characterization, biorecognitive activity and stability of WGA grafted lipid nanostructures for the controlled delivery of rifampicin. Chem. Phys. Lipids 2015, 193, 11–17. [Google Scholar] [CrossRef]
- Moulari, B.; Béduneau, A.; Pellequer, Y.; Lamprecht, A. Lectin-decorated nanoparticles enhance binding to the inflamed tissue in experimental colitis. J. Control. Release 2014, 188, 9–17. [Google Scholar] [CrossRef]
- Hädrich, G.; Dora, C.L.; Vaz, G.R.; Boschero, R.; Appel, A.S.; Ramos, C.; Halicki, P.C.B.; Bidone, J.; Teixeira, H.F.; Muccillo-Baisch, A.L.; et al. Development of lipid nanocarriers for tuberculosis treatment: Evaluation of suitable excipients and nanocarriers. Curr. Drug Deliv. 2021, 18, 770–778. [Google Scholar] [CrossRef]
- Imbuluzqueta, E.; Gamazo, C.; Ariza, J.; Blanco-Prieto, M.J. Drug delivery systems for potential treatment of intracellular bacterial infections. Front. Biosci. 2010, 15, 397–417. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, G.; Chen, C.; Portnoy, D.A. Strategies used by bacteria to grow in macrophages. In Myeloid Cells in Health and Disease: A Synthesis; American Society for Microbiology: Washington, DC, USA, 2017; Volume 4, pp. 701–725. [Google Scholar] [CrossRef]
- Dal Bó, A.G.; Soldi, V.; Giacomelli, F.C.; Travelet, C.; Jean, B.; Pignot-Paintrand, I.; Borsali, R.; Fort, S. Self-assembly of amphiphilic glycoconjugates into lectin-adhesive nanoparticles. Langmuir 2012, 28, 1418–1426. [Google Scholar] [CrossRef] [PubMed]
- Güll, I.; Wirth, M.; Gabor, F. Development of a sensitive and reliable ELISA for quantification of wheat germ agglutinin. J. Immunol. Methods 2007, 318, 20–29. [Google Scholar] [CrossRef] [PubMed]
- Dora, C.L.; Silva LF, C.; Tagliari, M.P.; Segatto Silva, M.A.; Lemos Senna, E. Formulation study of quercetin-loaded lipid-based nanocarriers obtained by hot solvent diffusion method. Lat. Am. J. Pharm. 2011, 30, 289–296. [Google Scholar]
- Hädrich, G.; Monteiro, S.O.; Rodrigues, M.R.; de Lima, V.R.; Putaux, J.L.; Bidone, J.; Teixeira, H.F.; Muccillo-Baisch, A.L.; Dora, C.L. Lipid-based nanocarrier for quercetin delivery: System characterization and molecular interactions studies. Drug Dev. Ind. Pharm. 2016, 42, 1165–1173. [Google Scholar] [CrossRef] [PubMed]
- Hädrich, G.; Vaz, G.R.; Maidana, M.; Kratz, J.M.; Loch-Neckel, G.; Favarin, D.C.; Rogerio, A.D.P.; Da Silva, F.M.R.; Muccillo-Baisch, A.L.; Dora, C.L. Anti-inflammatory effect and toxicology analysis of oral delivery quercetin nanosized emulsion in rats. Pharm. Res. 2016, 33, 983–993. [Google Scholar] [CrossRef]
- Hoffman, E.; Kumar, A.; Kanabar, V.; Arno, M.; Preux, L.; Millar, V.; Page, C.; Collins, H.; Mudway, I.; Dailey, L.A.; et al. In vitro multiparameter assay development strategy toward differentiating macrophage responses to inhaled medicines. Mol. Pharm. 2015, 12, 2675–2687. [Google Scholar] [CrossRef]
- Hoffman, E.; Patel, A.; Ball, D.; Klapwijk, J.; Millar, V.; Kumar, A.; Martin, A.; Mahendran, R.; Dailey, L.A.; Forbes, B.; et al. Morphometric characterization of rat and human alveolar macrophage cell models and their response to amiodarone using high content image analysis. Pharm. Res. 2017, 34, 2466–2476. [Google Scholar] [CrossRef]
- Hatakeyama, T.; Karino, R.; Terai, Y.; Kimura, M.; Unno, H.; Goda, S. An assay for carbohydrate-binding activity of lectins using polyamidoamine dendrimer conjugated with carbohydrates. Biosci. Biotechnol. Biochem. 2012, 76, 1999–2001. [Google Scholar] [CrossRef]
- Gioria, S.; Caputo, F.; Urbán, P.; Maguire, C.M.; Bremer-Hoffmann, S.; Prina-Mello, A.; Calzolai, L.; Mehn, D. Are existing standard methods suitable for the evaluation of nanomedicines: Some case studies. Nanomedicine 2018, 13, 539–554. [Google Scholar] [CrossRef]
- Patel, A.; Hoffman, E.; Ball, D.; Klapwijk, J.; Steven, R.T.; Dexter, A.; Bunch, J.; Baker, D.; Murnane, D.; Hutter, V.; et al. Comparison of oral, intranasal and aerosol administration of amiodarone in rats as a model of pulmonary phospholipidosis. Pharmaceutics 2019, 11, 345. [Google Scholar] [CrossRef]
- Monteiro, L.M.; Löbenberg, R.; Cotrim, P.C.; Barros De Araujo, G.L.; Bou-Chacra, N. Buparvaquone nanostructured lipid carrier: Development of an affordable delivery system for the treatment of leishmaniases. Biomed. Res. Int. 2017, 2017, 9781603. [Google Scholar] [CrossRef] [PubMed]
- Plattner, V.E.; Wagner, M.; Ratzinger, G.; Gabor, F.; Wirth, M. Targeted drug delivery: Binding and uptake of plant lectins using human 5637 bladder cancer cells. Eur. J. Pharm. Biopharm. 2008, 70, 572–576. [Google Scholar] [CrossRef] [PubMed]
- Neutsch, L.; Eggenreich, B.; Herwig, E.; Marchetti-Deschmann, M.; Allmaier, G.; Gabor, F.; Wirth, M. Lectin bioconjugates trigger urothelial cytoinvasion—A glycotargeted approach for improved intravesical drug delivery. Eur. J. Pharm. Biopharm. 2012, 82, 367–375. [Google Scholar] [CrossRef]
- Apfelthaler, C.; Anzengruber, M.; Gabor, F.; Wirth, M. Poly-(l)-glutamic acid drug delivery system for the intravesical therapy of bladder cancer using WGA as targeting moiety. Eur. J. Pharm. Biopharm. 2017, 115, 131–139. [Google Scholar] [CrossRef]
- Yi, S.M.; Harson, R.E.; Zabner, J.; Welsh, M.J. Lectin binding and endocytosis at the apical surface of human airway epithelia. Gene Ther. 2001, 8, 1826–1832. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Zhao, Y.; Liu, J.; Zhang, M.; Yu, M.; Feng, N. Wheat germ agglutinin modification of lipid–polymer hybrid nanoparticles: Enhanced cellular uptake and bioadhesion. RSC Adv. 2016, 6, 36125–36135. [Google Scholar] [CrossRef]
- Liu, Y.; Wang, P.; Sun, C.; Feng, N.; Zhou, W.; Yang, Y.; Tan, R.; Chen, Z.; Wu, S.; Zhao, J. Wheat germ agglutinin-grafted lipid nanoparticles: Preparation and in vitro evaluation of the association with Caco-2 monolayers. Int. J. Pharm. 2010, 397, 155–163. [Google Scholar] [CrossRef] [PubMed]
- Auth, J.; Fröba, M.; Große, M.; Rauch, P.; Ruetalo, N.; Schindler, M.; Morokutti-kurz, M.; Graf, P.; Dolischka, A.; Prieschl-grassauer, E.; et al. Lectin from Triticum vulgaris (WGA) inhibits infection with SARS-CoV-2 and its variants of concern alpha and beta. Int. J. Mol. Sci. 2021, 22, 10205. [Google Scholar] [CrossRef]



| Excipients | Amount for 10 mL (mg) | % of Each Compound in Relation to Total Solids |
|---|---|---|
| Egg lecithin E80 | 100.0 mg | 18.1 |
| Trimyristine | 280.0 mg | 50.8 |
| Castor oil | 120.0 mg | 21.7 |
| PEG-660 stearate | 25.0 mg | 4.55 |
| C18PEG900GlcNAc | 25.0 mg | 4.55 |
| Nanocarrier | Size (nm) | PDI | Zeta Potential (mV) |
|---|---|---|---|
| NLC 1 | 159.8 ± 3.42 | 0.144 ± 0.01 | −23.8 ± 1.11 |
| NLC-Glc Nac | 157.3 ± 1.63 | 0.111 ± 0.01 | −28.5 ± 0.08 |
| NLC-WGA | 157.6 ± 1.10 | 0.095 ± 0.01 | −19.0 ± 0.96 |
| NLC-QU | 121.9 ± 0.05 | 0.170 ± 0.022 | −13.5 ± 0.702 |
| Zero-Order | First Order | Higuchi | |
|---|---|---|---|
| Equation | Y = 2.2919x + 17.64 | Y = −0.0166x + 1.9147 | Y = 13.779x + 4.3262 |
| Correlation coefficient (r2) | 0.6828 | 0.8029 | 0.9144 |
| Constant release (k) | 2.2919 | 0.0382 | 13.779 |
| Treatment | Cell Volume—FSC (×106) | Cellular Complexity (×106) | Viable Cells (%) | Cellular Internalization of the NR |
|---|---|---|---|---|
| NR | 1.62 ± 0.06 b | 2.22 ± 0.37 b | 92.9 ± 1.8 b | 3468 ± 591 c |
| NLC-NR | 2.10 ± 0.13 a | 2.73 ± 0.15 a | 81.6 ± 3.9 a | 16021 ± 5805 bc |
| NLC-NR-C18PEG900GlcNAc | 2.04 ± 0.11 ab | 2.67 ± 0.14 a | 84.3 ± 3.4 a | 31260 ± 8647 ab |
| NLC-NR-WGA | 2.10 ± 0.15 a | 2.92 ± 0.12 a | 82.7 ± 4.5 a | 50628 ± 14459 a |
| No. | Parameter | No. | Parameter | ||
|---|---|---|---|---|---|
| 1 | Abnormal nuclear area | <74 µm2 or >194 µm2 | 6 | Elevated vacuole number per cell | >1 with >0.9 µm2 |
| 2 | Elevated mitochondrial activity | FI > 8914 a.u. | 7 | Elevated vacuole area per cell | >4 µm2 |
| 3 | Reduced mitochondrial activity | FI < 3098 a.u. | 8 | Elevated phospholipid content | FI > 91 a.u. |
| 4 | Elevated membrane permeability | FI > 7397 a.u. | 9 | Elevated neutral lipid content | FI > 6986 a.u. |
| 5 | Elevated cellular area | > 642 µm2 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hädrich, G.; Vaz, G.R.; Bidone, J.; Yurgel, V.C.; Teixeira, H.F.; Gonçalves Dal Bó, A.; da Silva Pinto, L.; Hort, M.A.; Ramos, D.F.; Junior, A.S.V.; et al. Development of a Novel Lipid-Based Nanosystem Functionalized with WGA for Enhanced Intracellular Drug Delivery. Pharmaceutics 2022, 14, 2022. https://doi.org/10.3390/pharmaceutics14102022
Hädrich G, Vaz GR, Bidone J, Yurgel VC, Teixeira HF, Gonçalves Dal Bó A, da Silva Pinto L, Hort MA, Ramos DF, Junior ASV, et al. Development of a Novel Lipid-Based Nanosystem Functionalized with WGA for Enhanced Intracellular Drug Delivery. Pharmaceutics. 2022; 14(10):2022. https://doi.org/10.3390/pharmaceutics14102022
Chicago/Turabian StyleHädrich, Gabriela, Gustavo Richter Vaz, Juliana Bidone, Virginia Campello Yurgel, Helder Ferreira Teixeira, Alexandre Gonçalves Dal Bó, Luciano da Silva Pinto, Mariana Appel Hort, Daniela Fernandes Ramos, Antonio Sergio Varela Junior, and et al. 2022. "Development of a Novel Lipid-Based Nanosystem Functionalized with WGA for Enhanced Intracellular Drug Delivery" Pharmaceutics 14, no. 10: 2022. https://doi.org/10.3390/pharmaceutics14102022
APA StyleHädrich, G., Vaz, G. R., Bidone, J., Yurgel, V. C., Teixeira, H. F., Gonçalves Dal Bó, A., da Silva Pinto, L., Hort, M. A., Ramos, D. F., Junior, A. S. V., Almeida da Silva, P. E., & Dora, C. L. (2022). Development of a Novel Lipid-Based Nanosystem Functionalized with WGA for Enhanced Intracellular Drug Delivery. Pharmaceutics, 14(10), 2022. https://doi.org/10.3390/pharmaceutics14102022







