Synthesis of Two Methotrexate Prodrugs for Optimizing Drug Loading into Liposomes
Abstract
1. Introduction
2. Results and Discussion
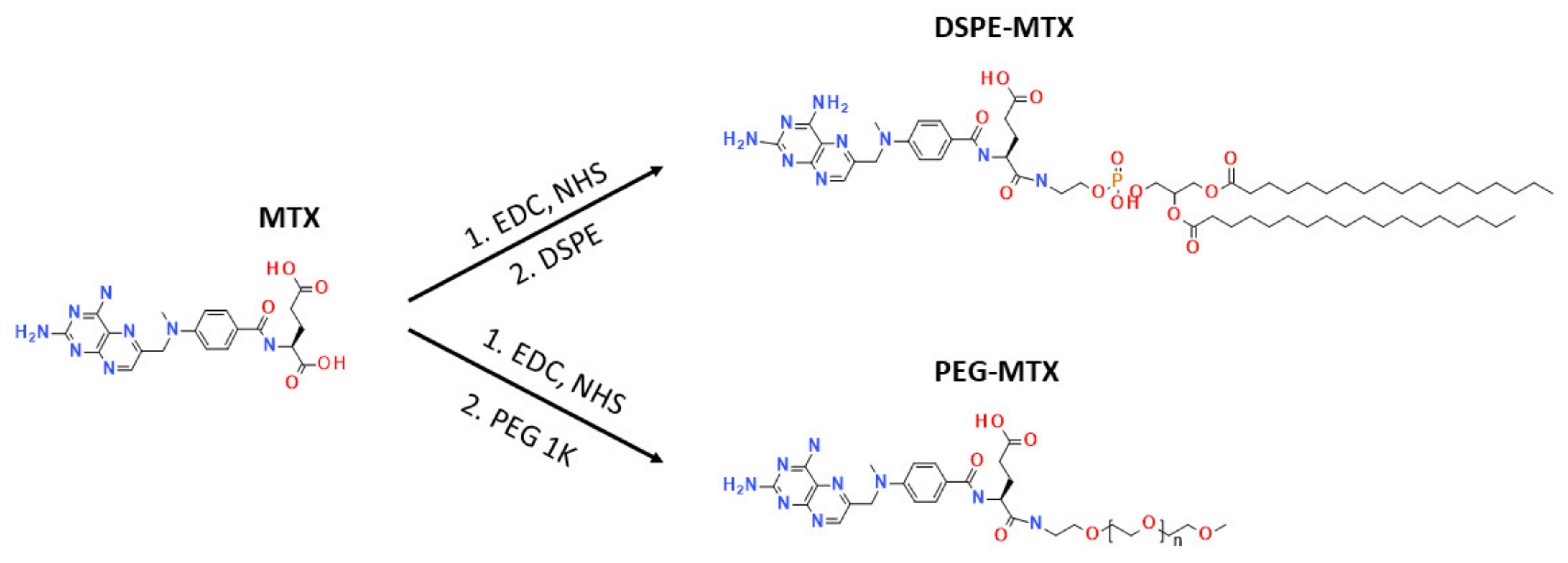
2.1. MTX Prodrug Synthesis and Characterizations
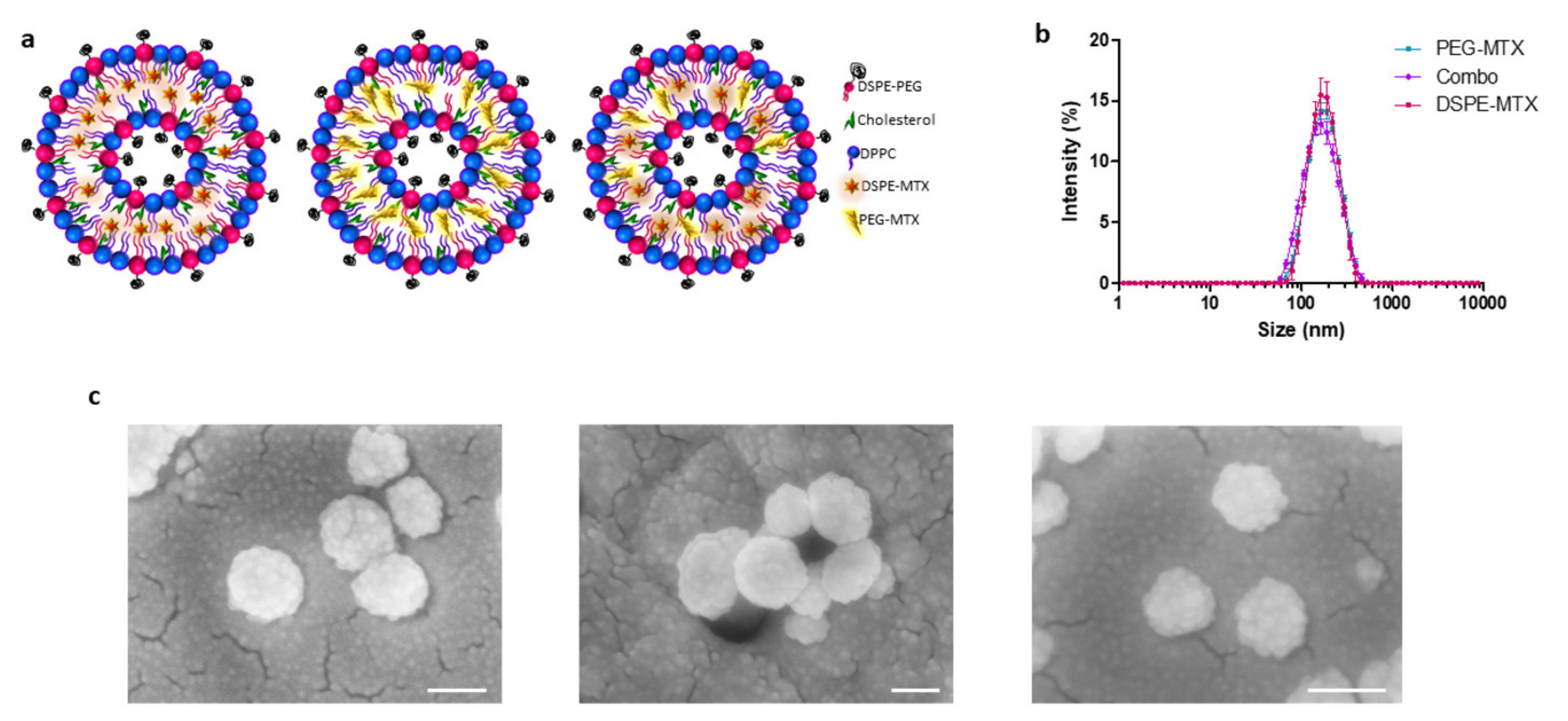
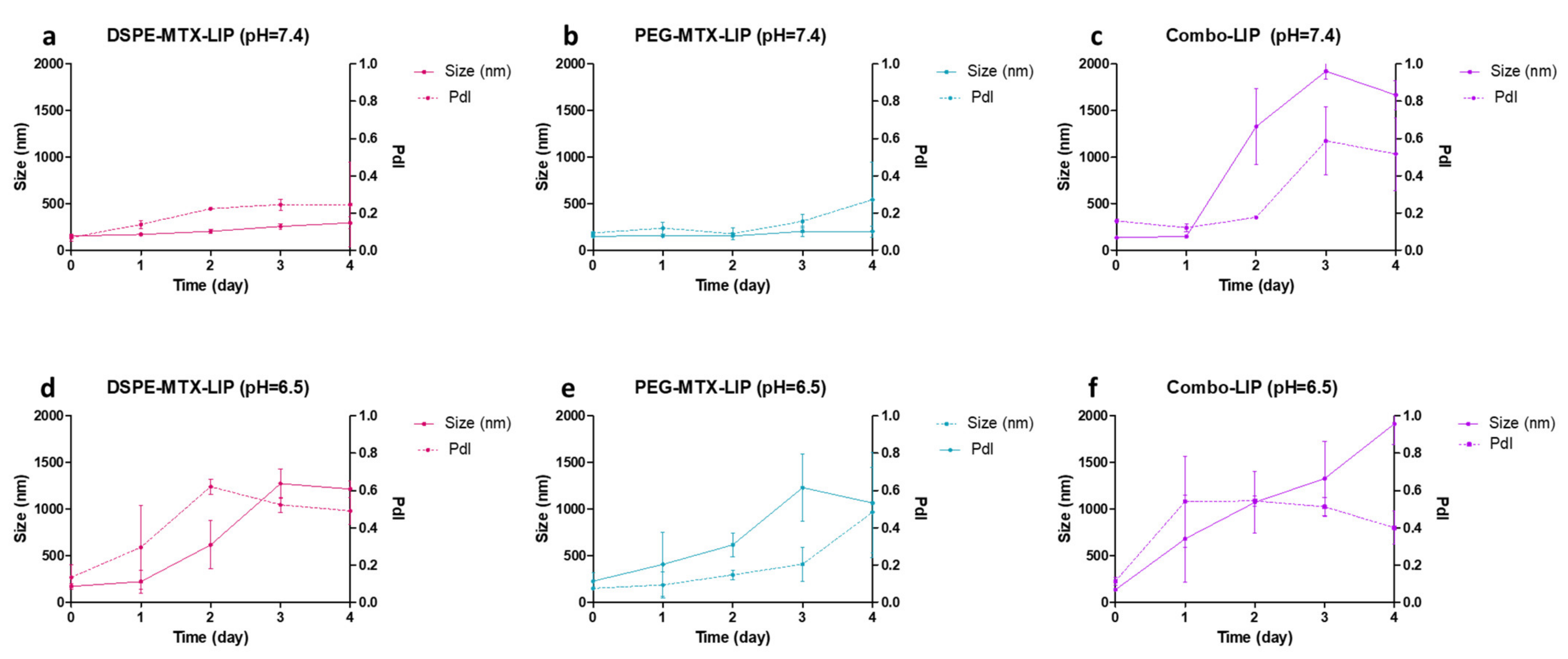
2.2. MTX Liposome Assembly and Characterization
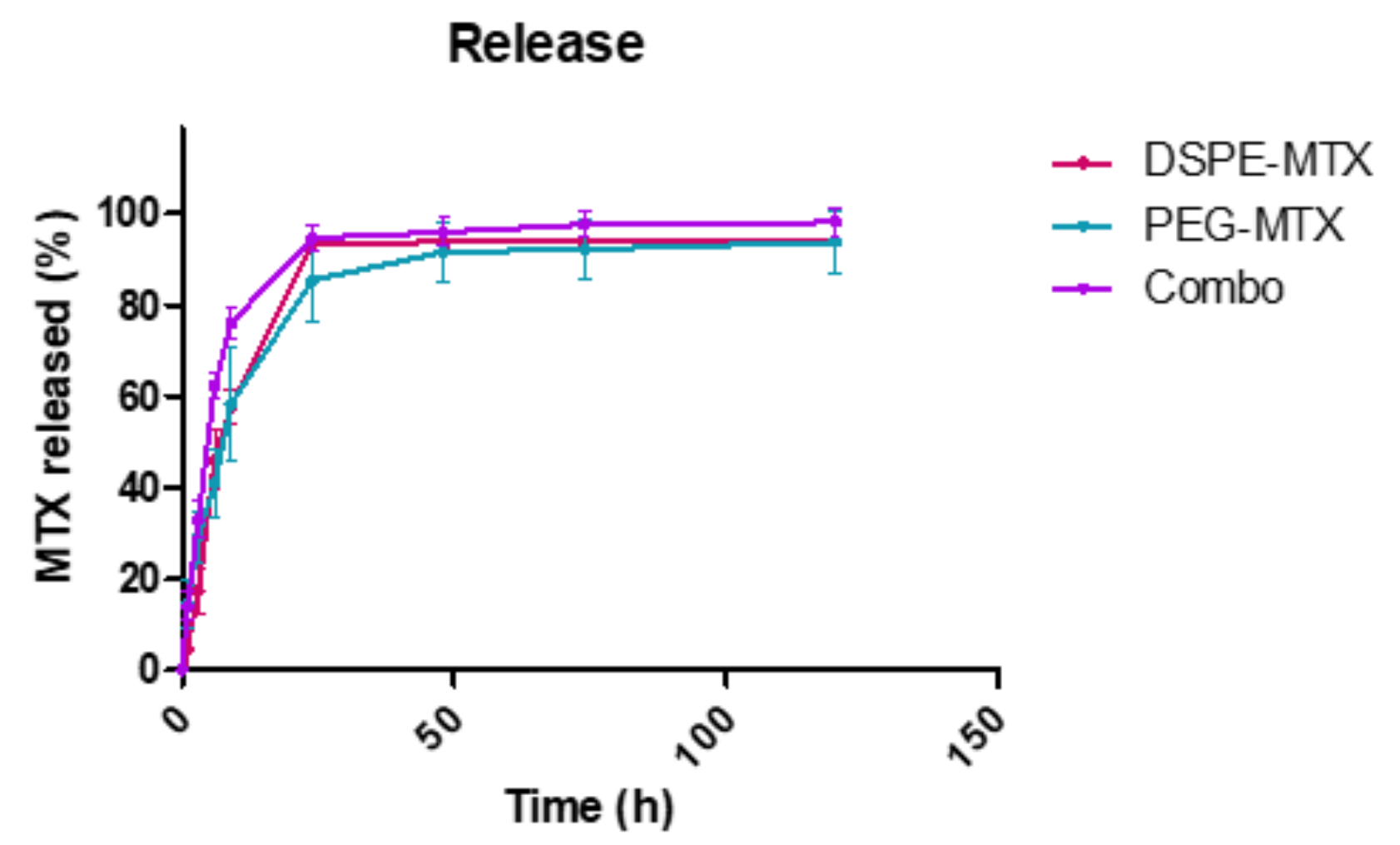
2.3. MTX-Liposome Release Profiles
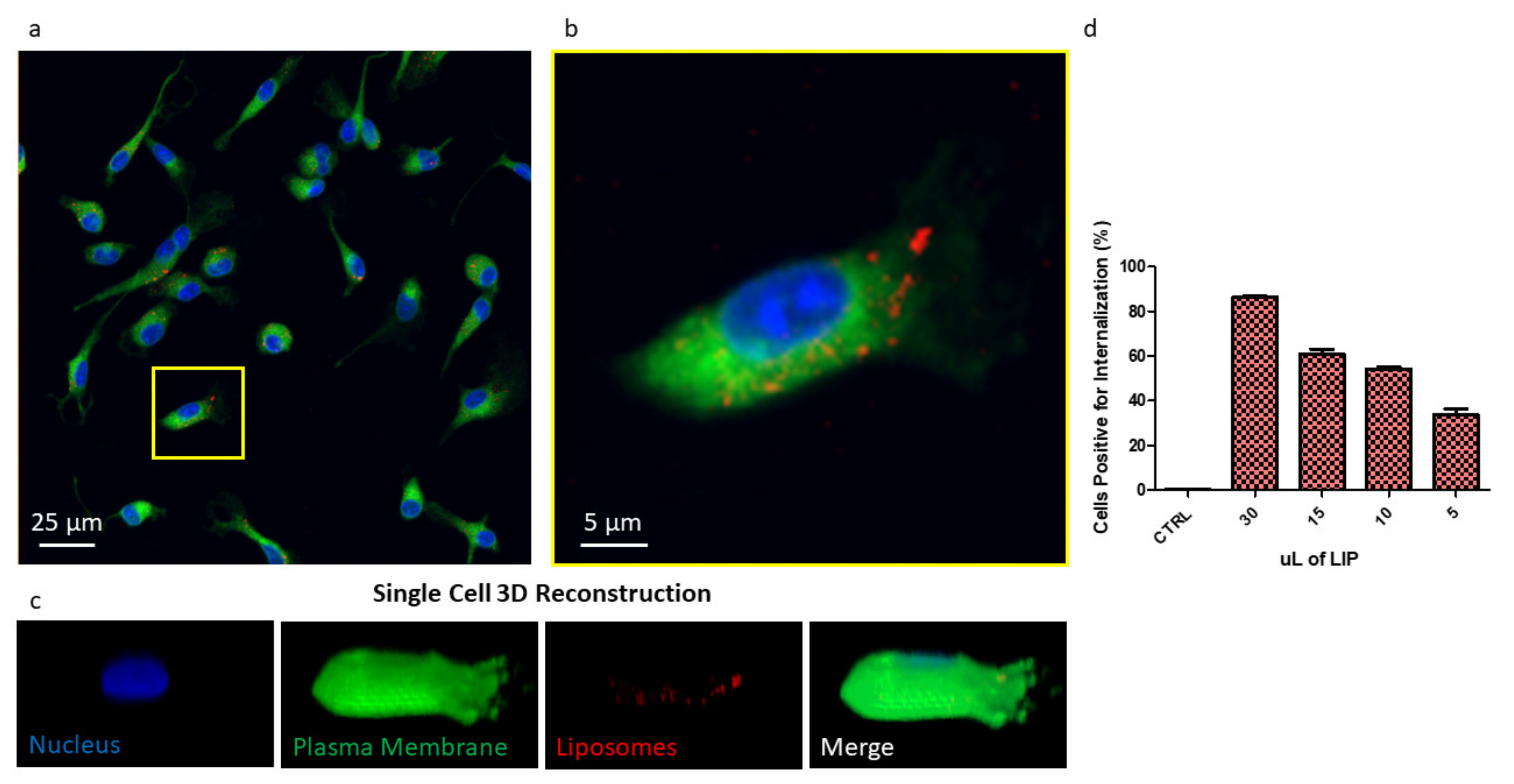
2.4. Liposome Uptake
2.5. Cell Cytotoxicity Analyses
3. Conclusions
4. Materials and Methods
4.1. Materials
4.2. Synthesis of DSPE-MTX
4.3. Synthesis of PEG-MTX
4.4. Synthesis of DSPE-Cy5
4.5. Determination of Log P
4.6. Synthesis of MTX Liposomes (MTX-LIP) and Cy5 Liposomes (Cy5-LIP)
4.7. Liposome Morphological Characterization
4.8. Particles Size, Surface Charge and Stability Characterizations
4.9. Drug Loading and Release Analysis
4.10. Cy5 Loading and Release Analysis
4.11. Bone Marrow Derived Macrophages Harvesting
4.12. Confocal Fluorescent Microscopy Imaging
4.13. Cell Internalization Studies
4.14. Toxicity Analysis
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Purcell, W.T.; Ettinger, D.S. Novel antifolate drugs. Curr. Oncol. Rep. 2003, 5, 114–125. [Google Scholar] [CrossRef]
- Abolmaali, S.S.; Tamaddon, A.M.; Dinarvand, R. A review of therapeutic challenges and achievements of methotrexate delivery systems for treatment of cancer and rheumatoid arthritis. Cancer Chemother. Pharmacol. 2013, 71, 1115–1130. [Google Scholar] [CrossRef]
- Kasim, N.A.; Whitehouse, M.; Ramachandran, C.; Bermejo, M.; Lennernäs, H.; Hussain, A.S.; Junginger, H.E.; Stavchansky, S.A.; Midha, K.K.; Shah, V.P.; et al. Molecular Properties of WHO Essential Drugs and Provisional Biopharmaceutical Classification. Mol. Pharm. 2004, 1, 85–96. [Google Scholar] [CrossRef] [PubMed]
- Bedoui, Y.; Guillot, X.; Sélambarom, J.; Guiraud, P.; Giry, C.; Jaffar-Bandjee, M.C.; Ralandison, S.; Gasque, P. Methotrexate an Old Drug with New Tricks. Int. J. Mol. Sci. 2019, 20, 5023. [Google Scholar] [CrossRef]
- Genestier, L.; Paillot, R.; Quemeneur, L.; Izeradjene, K.; Revillard, J.-P. Mechanisms of action of methotrexate. Immunopharmacology 2000, 47, 247–257. [Google Scholar] [CrossRef]
- Oh, J.-M.; Park, M.; Kim, S.-T.; Jung, J.-Y.; Kang, Y.-G.; Choy, J.-H. Efficient delivery of anticancer drug MTX through MTX-LDH nanohybrid system. J. Phys. Chem. Solids 2006, 67, 1024–1027. [Google Scholar] [CrossRef]
- Bailey, L.B.; Gregory, J.F. Folate Metabolism and Requirements. J. Nutr. 1999, 129, 779–782. [Google Scholar] [CrossRef] [PubMed]
- Chan, E.S.L.; Cronstein, B.N. Mechanisms of action of methotrexate. Bull. Hosp. Jt. Dis. 2013, 71, 5. [Google Scholar]
- Van Roon, E.N.; van de Laar, M.A. Methotrexate bioavailability. Clin. Exp. Rheumatol. 2010, 28 (Suppl. 61), S27–S32. [Google Scholar]
- Lin, J.; Liu, G.; Fan, Z.; Su, G.; Li, Y.; Song, L.; Zhu, X.; Hou, Z. Self-assembly of multifunctional integrated nanoparticles loaded with a methotrexate–phospholipid complex: Combining simplicity and efficacy in both targeting and anticancer effects. RSC Adv. 2016, 6, 86717–86727. [Google Scholar] [CrossRef]
- Chan, E.S.; Cronstein, B.N. Methotrexate—How does it really work? Nat. Rev. Rheumatol. 2010, 6, 175–178. [Google Scholar] [CrossRef]
- Iqbal, M.P. Accumulation of methotrexate in human tissues following high-dose methotrexate therapy. J. Pak. Med. Assoc. 1998, 48, 341–343. [Google Scholar] [PubMed]
- Conway, R.; Carey, J.J. Risk of liver disease in methotrexate treated patients. World J. Hepatol. 2017, 9, 1092–1100. [Google Scholar] [CrossRef]
- Prey, S.; Paul, C. Effect of folic or folinic acid supplementation on methotrexate-associated safety and efficacy in inflammatory disease: A systematic review. Br. J. Dermatol. 2009, 160, 622–628. [Google Scholar] [CrossRef]
- Romão, V.C.; Lima, A.; Bernardes, M.; Canhão, H.; Fonseca, J.E. Three decades of low-dose methotrexate in rheumatoid arthritis: Can we predict toxicity? Immunol. Res. 2014, 60, 289–310. [Google Scholar] [CrossRef]
- Schnabel, A.; Gross, W.L. Low-dose methotrexate in rheumatic diseases—Efficacy, side effects, and risk factors for side effects. Semin. Arthritis Rheum. 1994, 23, 310–327. [Google Scholar] [CrossRef]
- Karasulu, H.Y.; Karabulut, B.; Goker, E.; Güneri, T.; Gabor, F. Controlled Release of Methotrexate from W/O Microemulsion and Its In Vitro Antitumor Activity. Drug Deliv. 2007, 14, 225–233. [Google Scholar] [CrossRef] [PubMed]
- Li, M.-H.; Choi, S.K.; Thomas, T.P.; Desai, A.; Lee, K.-H.; Kotlyar, A.; Holl, M.M.B.; Baker, J.R. Dendrimer-based multivalent methotrexates as dual acting nanoconjugates for cancer cell targeting. Eur. J. Med. Chem. 2012, 47, 560–572. [Google Scholar] [CrossRef]
- Nogueira, D.R.; Tavano, L.; Mitjans, M.; Perez, L.; Infante, M.R.; Vinardell, P. In vitro antitumor activity of methotrexate via pH-sensitive chitosan nanoparticles. Biomaterials 2013, 34, 2758–2772. [Google Scholar] [CrossRef] [PubMed]
- Sartori, T.; Murakami, F.S.; Cruz, A.P.; De Campos, A.M. Development and validation of a fast RP-HPLC method for determination of methotrexate entrapment efficiency in polymeric nanocapsules. J. Chromatogr. Sci. 2008, 46, 505–509. [Google Scholar] [CrossRef]
- Zhang, Y.; Jin, T.; Zhuo, R.-X. Methotrexate-loaded biodegradable polymeric micelles: Preparation, physicochemical properties and in vitro drug release. Colloids Surf. B Biointerfaces 2005, 44, 104–109. [Google Scholar] [CrossRef] [PubMed]
- Curcio, M.; Mauro, L.; Naimo, G.D.; Amantea, D.; Cirillo, G.; Tavano, L.; Casaburi, I.; Nicoletta, F.P. Facile synthesis of pH-responsive polymersomes based on lipidized PEG for intracellular co-delivery of curcumin and methotrexate. Colloids Surf. B Biointerfaces 2018, 167, 568–576. [Google Scholar] [CrossRef]
- Guimarães, D.; Noro, J.; Loureiro, A.; Lager, F.; Renault, G.; Cavaco-Paulo, A.; Nogueira, E. Increased Encapsulation Efficiency of Methotrexate in Liposomes for Rheumatoid Arthritis Therapy. Biomedicines 2020, 8, 630. [Google Scholar] [CrossRef]
- Celia, C.; Cristiano, M.C.; Froiio, F.; Di Francesco, M.; D’Avanzo, N.; Di Marzio, L.; Fresta, M. Nanoliposomes as Multidrug Carrier of Gemcitabine/Paclitaxel for the Effective Treatment of Metastatic Breast Cancer Disease: A Comparison with Gemzar and Taxol. Adv. Ther. 2021, 4, 2000121. [Google Scholar] [CrossRef]
- Popa, M.; Uglea, C.V. Polymeric Nanomedicines; Bentham Science Publishers: Sharjah, United Arab Emirates, 2013. [Google Scholar]
- Sercombe, L.; Veerati, T.; Moheimani, F.; Wu, S.Y.; Sood, A.K.; Hua, S. Advances and Challenges of Liposome Assisted Drug Delivery. Front. Pharmacol. 2015, 6, 286. [Google Scholar] [CrossRef] [PubMed]
- Lamichhane, N.; Udayakumar, T.; D’Souza, W.D.; Simone, C.B.; Raghavan, S.R.; Polf, J.; Mahmood, J. Liposomes: Clinical applications and potential for image-guided drug delivery. Molecules 2018, 23, 288. [Google Scholar] [CrossRef]
- Tetko, I.V.; Tanchuk, V.Y.; Kasheva, T.N.; Villa, A.E.P. Estimation of Aqueous Solubility of Chemical Compounds Using E-State Indices. J. Chem. Inf. Comput. Sci. 2001, 41, 1488–1493. [Google Scholar] [CrossRef]
- Tetko, I.V.; Tanchuk, V.Y.; Villa, A.E. Prediction of n-octanol/water partition coefficients from PHYSPROP database using artificial neural networks and E-state indices. J. Chem. Inf. Comput. Sci. 2001, 41, 1407–1421. [Google Scholar] [CrossRef] [PubMed]
- ACDLabs. Partition Coefficient Calculation with ACD/LogP. 2021. Available online: https://www.acdlabs.com/products/percepta/predictors/logp/index.php (accessed on 5 January 2021).
- Di Francesco, V.; Gurgone, V.; Palomba, R.; Marques Ferreira, M.F.M.; Catelani, T.; Cervadoro, A.; Maffia, P.; Decuzzi, P. Modulating lipoprotein transcellular transport and atherosclerotic plaque formation in apoe-/-mice via nanoformulated lipid-methotrexate conjugates. ACS Appl. Mater. Interfaces 2020, 12, 34. [Google Scholar] [CrossRef] [PubMed]
- De Rose, R.F.; Cristiano, M.C.; Celano, M.; Maggisano, V.; Vero, A.; Lombardo, G.E.; Di Francesco, M.; Paolino, D.; Russo, D.; Cosco, D. PDE5 Inhibitors-Loaded Nanovesicles: Physico-Chemical Properties and In Vitro Antiproliferative Activity. Nanomater. 2016, 6, 92. [Google Scholar] [CrossRef]
- Dos Santos, A.M.; Carvalho, F.C.; Teixeira, D.A.; Azevedo, D.L.; de Barros, V.M.; Dalfon Gremiao, M.P. Computational and experimental approaches for development of methotrexate nanosuspensions by bottom-up nanoprecipitation. Int. J. Pharm. 2017, 524, 330–338. [Google Scholar] [CrossRef] [PubMed]
- Palanikumar, L.; Al-Hosani, S.; Kalmouni, M.; Nguyen, V.P.; Ali, L.; Pasricha, R.; Barrerra, F.; Magzoub, M. pH-responsive high stability polymeric nanoparticles for targeted delivery of anticancer therapeutics. Commun. Biol. 2020, 3, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Aigner, T.; Söder, S. Histopathological examination of joint degeneration: Typing, grading and staging of osteoarthritis. Der Pathologe 2006, 27, 431–438. [Google Scholar] [CrossRef]
- Rajamäki, K.; Nordström, T.; Nurmi, K.; Åkerman, K.E.O.; Kovanen, P.T.; Öörni, K.; Eklund, K.K. Extracellular Acidosis Is a Novel Danger Signal Alerting Innate Immunity via the NLRP3 Inflammasome. J. Biol. Chem. 2013, 288, 13410–13419. [Google Scholar] [CrossRef] [PubMed]
- Di Francesco, M.; Celia, C.; Cristiano, M.C.; D’Avanzo, N.; Ruozi, B.; Mircioiu, C.; Cosco, D.; Di Marzio, L.; Fresta, M. Doxorubicin Hydrochloride-Loaded Nonionic Surfactant Vesicles to Treat Metastatic and Non-Metastatic Breast Cancer. ACS Omega 2021, 6, 2973–2989. [Google Scholar] [CrossRef] [PubMed]
- Mircioiu, C.; Voicu, V.; Anuta, V.; Tudose, A.; Celia, C.; Paolino, D.; Fresta, M.; Sandulovici, R.; Mircioiu, I. Mathematical Modeling of Release Kinetics from Supramolecular Drug Delivery Systems. Pharmaceutics 2019, 11, 140. [Google Scholar] [CrossRef]
- Rigter, P.; Peppas, N. A simple equation for description of solute relase I. Fickian and non-fickian release from non-swellable devices in the form of slabs, spherer, cylinders or discs. J. Control. Release 1987, 5, 23–36. [Google Scholar]
- Mohan, A.; Narayanan, S.; Sethuraman, S.; Krishnan, U.M. Novel Resveratrol and 5-Fluorouracil Coencapsulated in PEGylated Nanoliposomes Improve Chemotherapeutic Efficacy of Combination against Head and Neck Squamous Cell Carcinoma. BioMed Res. Int. 2014, 2014, 424239. [Google Scholar] [CrossRef]
- Er, Y.; Barnes, T.J.; Fornasiero, D.; Prestidge, C.A. The encapsulation and release of guanosine from PEGylated liposomes. J. Liposome Res. 2009, 19, 29–36. [Google Scholar] [CrossRef] [PubMed]
- Jain, A.; Jain, S.K. In vitro release kinetics model fitting of liposomes: An insight. Chem. Phys. Lipids 2016, 201, 28–40. [Google Scholar] [CrossRef]
- Prakash, J.D.; Duggirala, R.L.; Ariya, R.; Kumari, T. Formulation and In vitro Characterization of Ketoconazole Liposomal Gel for Transdermal Delivery. Res. J. Pharm. Technol. 2017, 10, 205. [Google Scholar] [CrossRef]
- Tiwari, G.; Tiwari, G.; Wal, P.; Wal, A. Development and Optimization of Liposomes Containing 5 Fluorouracil and Tretinoin for Skin Warts: 32 Experimental Design. FABAD J. Pharm. Sci. 2019, 44, 17–26. [Google Scholar]
- Zhao, L.; Wei, Y.; Guo, J.; Zheng, X.; Wu, J.; Zhou, Y.; Yu, Y.; Zhang, L.; Ye, Y. Preparation, pharmacokinetics and biodistribution of baicalin-loaded liposomes. Int. J. Nanomed. 2014, 9, 3623–3630. [Google Scholar] [CrossRef]
- Zhang, T.; Li, Y.; Song, Y.; Chen, X.; Li, J.; Peng, Q.; He, J.; Fei, X. Curcumin- and Cyclopamine-Loaded Liposomes to Enhance Therapeutic Efficacy Against Hepatic Fibrosis. Drug Des. Dev. Ther. 2020, 14, 5667–5678. [Google Scholar] [CrossRef]
- Jeong, C.; Noh, I.; Rejinold, N.S.; Kim, J.; Jon, S.; Kim, Y.-C. Self-Assembled Supramolecular Bilayer Nanoparticles Composed of Near-Infrared Dye as a Theranostic Nanoplatform To Encapsulate Hydrophilic Drugs Effectively. ACS Biomater. Sci. Eng. 2019, 6, 474–484. [Google Scholar] [CrossRef]
- Cadinoiu, A.N.; Rata, D.M.; Atanase, L.I.; Daraba, O.M.; Gherghel, D.; Vochita, G.; Popa, M. Aptamer-Functionalized Liposomes as a Potential Treatment for Basal Cell Carcinoma. Polymers 2019, 11, 1515. [Google Scholar] [CrossRef]
- Ferreira, M.; Rizzuti, I.F.; Palange, A.L.; Barbato, M.G. Optimizing the Pharmacological Properties of Discoidal Polymeric Nanoconstructs Against Triple Negative Breast Cancer Cells. Front. Bioeng. Biotechnol. 2020, 8, 5. [Google Scholar] [CrossRef] [PubMed]
- Palomba, R.; Palange, A.L.; Rizzuti, I.F.; Ferreira, M.; Cervadoro, A.; Barbato, M.G.; Canale, C.; Decuzzi, P. Modulating Phagocytic Cell Sequestration by Tailoring Nanoconstruct Softness. ACS Nano 2018, 12, 1433–1444. [Google Scholar] [CrossRef]
- Taraballi, F.; Corradetti, B.; Minardi, S.; Powel, S.; Cabrera, F.; Van Eps, J.L.; Weiner, B.K.; Tasciotti, E. Biomimetic collagenous scaffold to tune inflammation by targeting macrophages. J. Tissue Eng. 2016, 7, 2041731415624667. [Google Scholar] [CrossRef]

| Compound | Formula Weight | Exact Mass | Molecular Formula | Yield (%) | Log P | ||
|---|---|---|---|---|---|---|---|
| Biovia | VCClab | ACD Chemsketh | |||||
| MTX | 4454.44 | 454.439 | C20H22N8O5 | - | 0.11 | −0.91 | 0.023 ± 0.83 |
| DSPE-MTX | 1184.49 | 1183.73 | C61H102N9O12P | 81.1 | 13.84 | 7.53 | 16.63 ± 1.03 |
| PEG-MTX | 1480.69 | 1479.80 | C67H117N9O27 | 78.3 | −0.67 | 0.42 | −0.43 ± 0.93 |
| Liposomes | Size (nm) | Pdl | Z Pot (mV) | %EE |
|---|---|---|---|---|
| DSPE-MTX | 159 ± 3 | 0.14 ± 0.02 | −38 ± 0.26 | 79.9 ± 5.6 |
| PEG-MTX | 166 ± 0.6 | 0.18 ± 0.02 | −41 ± 0.4 | 82 ± 7.5 |
| Combo | 148 ± 1 | 0.17 ± 0.01 | −41 ± 3 | 80.2 ± 1.8 |
| Empty | 157.8 ± 2 | 0.17 ± 0.01 | −41.84 ± 1.2 | - |
| Prodrug | Zero-Order | First-Order | Higuchi | Korsmeyer-Peppas | Weibull | K | n | a | b |
|---|---|---|---|---|---|---|---|---|---|
| DSPE-MTX | 0.9796 | 0.9824 | 0.9004 | 0.9830 | 0.8905 | 6.80 | 0.9931 | 0.0527 | 1.3510 |
| PEG-MTX | 0.9648 | 0.9847 | 0.9821 | 0.9931 | 0.9672 | 13.85 | 0.64 | 0.1353 | 0.8829 |
| DSPE-MTX_ PEG-MTX | 0.9865 | 0.9942 | 0.9638 | 0.9966 | 0.9943 | 13.9 | 0.7506 | 0.1350 | 1.108 |
| Sample | IC50 72 h |
|---|---|
| MTX (μM) | 24.1 ± 0.14 |
| DSPE-MTX (μM) | 0.9 ± 0.1 |
| DSPE-MTX- LIP (μM) | 0.7 ± 0.12 |
| PEG-MTX (μM) | 2.5 ± 0.08 |
| PEG-MTX-LIP (μM) | 1.6 ± 0.1 |
| Combo (μM) | 0.6 ± 0.1 |
| Combo- LIP (μM) | 0.9 ± 0.1 |
| Empty LIP (μM) | - |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Di Francesco, V.; Di Francesco, M.; Decuzzi, P.; Palomba, R.; Ferreira, M. Synthesis of Two Methotrexate Prodrugs for Optimizing Drug Loading into Liposomes. Pharmaceutics 2021, 13, 332. https://doi.org/10.3390/pharmaceutics13030332
Di Francesco V, Di Francesco M, Decuzzi P, Palomba R, Ferreira M. Synthesis of Two Methotrexate Prodrugs for Optimizing Drug Loading into Liposomes. Pharmaceutics. 2021; 13(3):332. https://doi.org/10.3390/pharmaceutics13030332
Chicago/Turabian StyleDi Francesco, Valentina, Martina Di Francesco, Paolo Decuzzi, Roberto Palomba, and Miguel Ferreira. 2021. "Synthesis of Two Methotrexate Prodrugs for Optimizing Drug Loading into Liposomes" Pharmaceutics 13, no. 3: 332. https://doi.org/10.3390/pharmaceutics13030332
APA StyleDi Francesco, V., Di Francesco, M., Decuzzi, P., Palomba, R., & Ferreira, M. (2021). Synthesis of Two Methotrexate Prodrugs for Optimizing Drug Loading into Liposomes. Pharmaceutics, 13(3), 332. https://doi.org/10.3390/pharmaceutics13030332








