Abstract
The original SARS-CoV-2 lineages have been replaced by successive variants of concern (VOCs) over time. The aim of this study was to perform an assessment of the placental infection by SARS-CoV-2 according to the predominant variant at the moment of COVID-19 diagnosis. This was a prospective study of SARS-CoV-2-positive pregnant women between March 2020 and March 2022. The population was divided into pregnancies affected by COVID-19 disease during 2020 (Pre-VOC group) and pregnancies affected after December 2020 by SARS-CoV-2 variants of concern (VOC group). The presence of virus was assessed by RT-PCR, and the viral variant was determined by whole genome sequencing. A total of 104 placentas were examined, among which 54 cases belonged to the Pre-VOC group and 50 cases belonged to the VOC group. Sixteen positive placental RT-PCR tests for SARS-CoV-2 were reported. The NGS analysis confirmed the SARS-CoV-2 lineage in placenta tissue. All samples corresponded to the Pre-VOC group, whereas no placental presence of SARS-CoV-2 was detected in the VOC group (16, 29.6% vs. 0, 0.0% p = 0.000). Preterm birth (9, 16.7% vs. 2, 4%; p = 0.036) and hypertensive disorders of pregnancy (14, 25.9% vs. 3, 6%; p = 0.003) were more frequent in the Pre-VOC group than in the VOC group. Finally, the VOC group was composed of 23 unvaccinated and 27 vaccinated pregnant women; no differences were observed in the sub-analysis focused on vaccination status. In summary, SARS-CoV-2-positive placentas were observed only in pregnancies infected by SARS-CoV-2 wildtype. Thus, placental SARS-CoV-2 presence could be influenced by SARS-CoV-2 variants, infection timing, or vaccination status. According to our data, the current risk of SARS-CoV-2 placental infection after maternal COVID disease during pregnancy should be updated.
1. Introduction
Since the coronavirus disease (COVID-19) outbreak caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the virus has been constantly changing [1,2,3]. The initial period of the pandemic up to December 2020, when SARS-CoV-2 wildtype was the predominant variant, has been referred to as pre-variants of concern (Pre-VOC) era. Then, the original SARS-CoV-2 lineages have been replaced by successive variants of concern (VOCs) (Alpha, Beta, Gamma, Delta, Omicron) over time [4]. These variants exhibit higher transmissibility and cause COVID-19 disease of lower severity (with associated lower mortality rates) compared to SARS-CoV-2 wildtype [5,6].
Apart from this evolution, since May 2021, the COVID-19 vaccines have become available for pregnant women, and their effectiveness has been demonstrated in the pregnant population [7,8,9].
The pregnancy complications associated with SARS-CoV-2 infection have become an issue of concern. Reports have shown an increase in maternal and neonatal morbidity and mortality in pregnant women with COVID-19 diagnosis during the first months of the pandemic [10,11]. On the other hand, the literature is undecided about the relationship between VOCs, vaccination and maternal outcomes [7,12,13,14].
In the context of maternal disease severity or vertical transmission to the fetus or newborn, several studies have studied the presence of SARS-CoV-2 virus in placenta. Whereas some studies have detected SARS-CoV-2 in 95–100% of analyzed placentas [15,16], others have only detected around 6–20% [17,18,19] and some cannot detect SARS-CoV-2 at all in placentas [20,21]. This variability can be explained, because different studies describe pregnant women with different grades of COVID-19 severity, and different methodologies have been used for viral RNA detection. In addition, variability might depend on the viral linage and on the vaccination status of women suffering COVID-19 disease. Although the SARS-CoV-2 lineages have changed in the course of the pandemic, the relationship between the predominant variant causing COVID-19 disease and either placental infection or the lineage actually infecting the placenta has hardly been reported on.
The aim of this study was to analyze the frequency of placental infection by SARS-CoV-2 in SARS-CoV-2-positive women during pregnancy. We analyzed samples of SARS-CoV-2-positive women during 2020, when the Pre-VOC predominated, and samples collected during waves of VOC (Supplemental Figure S1).
2. Materials and Methods
We performed a prospective study in a Spanish tertiary care hospital (Hospital Clínico Lozano Blesa, Zaragoza, Spain) between March 2020 and March 2022. The inclusion criteria were SARS-CoV-2 infection during the pregnancy and placenta tissue available for analysis. The study was divided into two periods according to the date of their positive RT-PCR test and the periods of dominance of the SARS-CoV-2 variants. The Pre-VOC group was defined as women who tested positive for SARS-CoV-2 during 2020 (when the wildtype strain was predominant). The VOC group was defined as women who tested positive during 2021 and 2022 (era of all the other variants).
SARS-CoV-2 infection was diagnosed based on the positive RT-PCR test for SARS-CoV-2 from nasopharyngeal swabs. RT-PCR test kits from different companies were used: Viasure (CerTest Biotec, Zaragoza, Aragón, Spain), M2000 SARS-CoV-2 Assay (Abbott RealTime SARS-CoV-2 Assay, Abbott Molecular, Abbott Park, Green Oaks, IL, USA), TaqPath COVID-19 (Thermo Fisher Scientific, Waltham, MA, USA) and Alinity SARS-CoV-2 (Abbott Alinity, Abbott Molecular, Abbott Park, Green Oaks, IL, USA). As suggested by the manufacturer for nasopharyngeal specimens, cycle threshold (CT) values below 37 were taken as positive. Symptoms of COVID-19 have been divided into 3 types [22]: asymptomatic infection refers no clinical symptoms or signs; mild infection refers to symptoms such as fever, cough, headache, anosmia and asthenia; and severe infection refers dyspnea and hypoxemia accompanied by chest imaging compatible with pneumonia and respiratory infection. To determine the percentage of predominant variants of SARS-CoV-2 circulating in our patient recruitment area during sample collection, data were downloaded from the official local and national public sequence database [23] (Supplementary Figure S2).
The collection of placental tissue samples, posterior treatment and storage in RNAtmLater, and subsequent purification of RNA and SARS-CoV-2 RT-PCR analysis was carried out as described in a previous study [24]. The RNA from placentas with a positive in SARS-CoV-2 RT-PCR was analyzed by NGS to identify SARS-CoV-2 lineage, using a modified version of the COVID-19 ARTIC v4 Illumina library construction and sequencing protocol v4. Details on sequencing procedures and subsequent data analysis are provided in the Appendix A. Typical coverage of the SARS-CoV-2 genome obtained by whole genome sequencing is shown in Supplementary Figure S3.
Small for gestational age (SGA) was defined as birthweight below the 10th centile according to local standards [25]. Hypertensive disorders of pregnancy (HDPs) were divided into 4 categories, which were defined according to the criteria proposed by International Society for the Study of Hypertension in Pregnancy (ISSHP) [26]: preeclampsia (PE), chronic hypertension, chronic hypertension with superimposed PE and gestational hypertension.
Clinical characteristics, laboratory results, and maternal and neonatal outcomes were collected from medical records. All patients provided written informed consent. The study was approved by the Research Ethics Committee of the Community of Aragon (C.I. PI21/155 and COL21/000), and all patients provided written informed consent.
Statistical analysis was performed using SPSS 22.0. Categorical variables were presented as frequencies or percentages. Continuous variables were presented using mean ± standard deviation (SD), median, or range. For continuous variables, Shapiro–Wilk tests of normality were used to evaluate the distributions. Data were analyzed using Student’s t test or Mann–Whitney U test for continuous variables and the Pearson χ2 test for the categorical ones. Statistical significance was considered p < 0.05.
3. Results
Fifty-four women in the Pre-VOC group and fifty women in the VOC group were included. Demographic and clinical data, as well as a description of SARS-CoV-2, are shown in Table 1. The study group was comparable regarding maternal age, maternal weight, Caucasian ethnicity and primiparous. There were no significant differences for gestation age at birth, birth weight, SGA, umbilical arteria pH < 7.1, induced labor and caesarean. Nevertheless, preterm birth and HDP were more frequent in the Pre-VOC group than in the VOC group (p = 0.036, and p = 0.003, respectively).

Table 1.
Demographic and obstetrical data and SARS-CoV-2 infection characteristics.
Description of SARS-CoV-2 infection is presented in Table 1. No significant differences between trimester of SARS-CoV-2 maternal infection among cohorts were found (p = 0.083). Maternal diagnosis of COVID-19 was most frequent during the third trimester, 67 mothers (64.4%), whereas 33 women (31.7%) were in the second trimester and only four women (3.8%) were in the first trimester. However, we found significant differences according to the timing of maternal SARS-CoV-2 infection (p = 0.001) and the interval average from diagnosis of SARS-CoV-2 to delivery (Pre-VOC: 75.0 ± 54.2 days vs. VOC group: 50.3 ± 57.8, p = 0.027). Although no significant differences were found in the overall severity of SARS-CoV-2 symptoms between the groups (p = 0.184), the vast majority of patients with severe symptoms, four of five, were found in the Pre-VOC group.
We analyzed placental tissue from 104 patients by RT-PCR. Sixteen placentas were positive to SARS-CoV-2, and all were included in the Pre-VOC group. To confirm the presence and lineage of SARS-CoV-2 in the 16 positive placental samples identified, we performed whole viral genome sequencing by NGS. The assigned lineage in analyzed samples by whole genome sequencing corresponded to the predominant variant in our recruitment area at the time of infection of our study subjects. These results are shown in Table 2.

Table 2.
Description of sixteen positive placental SARS-CoV-2 cases. Assignment of SARS-CoV-2 lineage in each sample positive for placental SARS-CoV-2 based on the results of whole genome sequencing (see Supplementary Methods for details).
Additionally, we examined the vaccination status of study subjects. In the Pre-VOC group period, vaccination was still not available. In the VOC group, 27 women were vaccinated, whereas 23 women were unvaccinated (Figure 1). About vaccinated women, they were given viral vector (ChAdOx1-S (AstraZeneca)) or mRNA vaccines (mRNA-1273 (Moderna) or BNT162b2 (Pfizer-BioNTech)). Six women had only a single dose, whereas 20 women were completely vaccinated, and one had a booster vaccination. The average time between the last dose received and the COVID-19-positive result was 129.2 ± 85.1 days (Supplementary Table S1). Ten women had received the first dose before pregnancy, five women received the first dose during the first trimester, nine received the first dose during the second trimester and three received the first dose during the third trimester. Finally, we performed a sub-analysis to compare the Pre-VOC group with either the unvaccinated or the vaccinated VOC group (Table 3). Despite that in our sample we did not find differences among the overall maternal COVID-19 symptoms (p = 0.218), none of the cases or no severe cases occurred in the vaccinated VOC group.
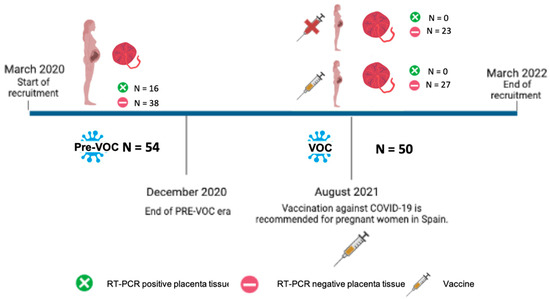
Figure 1.
Analysis of association of SARS-CoV-2 placental infection with variant of concern era and vaccination. Pre-VOC group N = 54. VOC group = 50, including 23 unvaccinated women and 27 vaccinated women. Overall, 16 placentas were positive to SARS-CoV-2. All were included in the Pre-VOC group, no women were included in the VOC group.

Table 3.
Results of sub-analysis focused on vaccination status.
4. Discussion
Our findings suggest that the frequency of SARS-CoV-2-positive placental tests may differ based on SARS-CoV-2 variants. We found a significantly higher frequency of positive placental RT-PCR SARS-CoV-2 in the placentas from women infected with SARS-CoV-2 wildtype compared with women infected with variants of concern of SARS-CoV-2, even adjusting for the vaccination status of the mother.
There are very few studies published describing the relation between SARS-CoV-2 variants of concern and placental health. Shanes et al. [27] detailed that maternal vascular malperfusion is a feature of SARS-CoV-2 infection during pregnancy and proposed that the lesion frequency changed with the predominant circulating variant. These findings are consistent with our results, given that positive placental SARS-CoV-2 could vary depending on the SARS-CoV-2 variants.
In fact, only a very limited number of studies combine data about the relationship between SARS-CoV-2 variants and positive placental SARS-CoV-2 tests. Wierz et al. [28], reporting on an isolated case, detected the presence of the Alpha variant in placental tissue using MALDI-TOF technology. Argueta et al. [29] described a cohort of placental samples from mothers positive for SARS-CoV-2 at delivery, where forty-two percent had detectable RNA, and underscored two placentas from mothers infected with the Alpha variant. A single case of SARS-CoV-2 variant Delta in a placenta after two successive COVID-19 episodes in unvaccinated woman in the same pregnancy has also been reported [30]. These isolated cases carried SARS-CoV-2 variants of concern in placenta tissue in contrast to our cohort, in which we only detected the SARS-CoV-2 wildtype. This observation could be explained by the frequency of SARS-CoV-2 infection early during pregnancy, vaccination status or herd immunity. Independent of these variables, in our limited analyses, no placental infection of SARS-CoV-2 was detected starting in 2021 (Table 1). Altogether, very few cases of placental presence of SARS-CoV-2 VOC have been described, suggesting it is rare. However, whether the frequency of placental infection, replication and/or symptoms in placenta are different between Pre-VOC on the one hand, and VOC and posterior variants on the other, remains to be established. Altered angiogenesis and enhanced vascular alterations are associated with both COVID-19 and PE [31]. We hypothesize that the resulting increased permeability of the blood vessels may allow more infiltrations of SARS-CoV-2 infected cells into the placenta and subsequent placental infection. A recent study provides evidence that disease severity is reduced in pregnant women infected by newer variants such as the omicron strain compared to women infected with wildtype SARS-CoV-2 at the beginning of the pandemic [32]. Our data suggest that the presence of placental SARS-CoV-2 is less frequent in mothers infected with VOC compared to SARS-CoV-2 wildtype. Therefore, if placental infection was a function of disease severity, the reduced frequency we observe after 2020 could be explained by the more limited vascular damage associated with less severe disease.
Pregnant women and their fetuses represent a high-risk population during infectious disease outbreaks [33]. For several viral diseases, severity is dependent on the trimester of infection. In the case of Rubella [34], the risk of fetal infection is highest in the first trimester especially prior to 10 weeks of gestation. On the other hand, severe disease was more prevalent among women in the third trimester of pregnancy during an influenza pandemic (H1N1). Moreover, from implantation and trophoblast invasion during early pregnancy onwards, successful pregnancy requires an environment that is tolerant toward maternal/fetal immunological differences [35]. In light of these combined observations, we analyzed the frequency of placental SARS-CoV-2 as a function of the trimester of infection. We included women infected by SARS-CoV-2 during all stages or trimesters of pregnancy in contrast to many studies that focus on women with a positive SARS-CoV-2 diagnosis at labor on hospital admission [36,37]. The vast majority of SARS-CoV-2-positive placentas (12 out of 16) were delivered by women who were diagnosed with COVID-19 disease more than 10 days before delivery (Table 2). Indeed, the seven cases that correspond to women who were diagnosed with COVID-19 before the third trimester all belong to the Pre-VOC group. While we cannot exclude the possibility that these mothers were re-infected later during pregnancy, an equally plausible explication resides in persistent infection. This timeframe would define these cases as post-COVID-19 syndrome, according to most actual definitions [38]. Glynn et al. [39] studied placental pathology, differentiating between acute or nonacute SARS-CoV-2 based on infection <14 or ≥14 days from delivery admission. This study provides evidence that histologic lesions in the placenta may differ based on the timing of SARS-CoV-2 infection during pregnancy. Furthermore, a significantly lower placental weight was reported in the non-acute cohort, suggesting long-term sequelae in response to SARS-CoV-2 infection. As SARS-CoV-2 infection may be persistent after infection during early pregnancy, and distinct placental lesions may develop during this time, further research is called for to mechanistically understand the effects on both placental and fetal health and to evaluate potential effects on newborns.
Whereas it was not the primary outcome of this study, we showed worse maternal and perinatal outcome in the Pre-VOC group compared to the VOC group. In fact, the association with preeclampsia that was reported early in the pandemic [24,40] is confirmed by our data (Pre-VOC group 14/54 HDP cases vs. VOC group 3/50 HDP cases, p = 0.003). Several studies correlate a worse perinatal outcome such as preterm birth, small for gestational age or ICU admission with hypertensive disorder of pregnancy [41,42]. Consistent with these reports, we observed higher rates of preterm birth in the Pre-VOC group than in the VOC group (9, 16.7% vs. 2, 4%; p = 0.036). Our results support reported findings suggesting that successive waves of SARS-CoV-2 variants of concern are associated with decreased severity in pregnant women [31,43,44], while other studies show that the VOC cases of severe COVID-19 disease during pregnancy are limited to women that are unvaccinated [9,45,46,47]. We also addressed the potential influence of vaccination on the presence of SARS-CoV-2 in the placenta. We did not detect SARS-CoV-2 in placenta tissue from 27 vaccinated women. Our data do not show significant differences between vaccination status and COVID-19 complications. This was probably due to the small sample size as well as because the vast majority of vaccinated women contracted the virus when Omicron was the most dominant strain. All vaccinated women in our study received vaccines not adapted to BA.4 and BA.5 Omicron variants. However, several studies published support the vaccine effectiveness in the pregnant population, showing a reduced risk for severe symptoms and complications in vaccinated women [9,48,49].
We assume that the sample size of this study is insufficient to provide evidence about the clinical outcomes associated with SARS-CoV-2 variants of concern, but it was not the main objective of this study. We consider that the prospective sampling of 106 placentas during the course of the pandemic provides enough consistency to evaluate the risk of placental infection over time as a function of different variants and clinical scenarios. Moreover, to collect the placentas of all SARS-CoV-2-positive pregnancies during the period of study, we needed to know at delivery time which women had passed COVID-19 during pregnancy and to have research staff available for sample collection and preservation. These requirements were very difficult to meet at certain times of the pandemic, and a much more limited number of samples was collected. This may have caused selection bias. It is important to note that the detection of the viral genome in the placental tissue does not necessarily mean that active infectious particles have been detected. However, the genome-wide coverage that we obtain in most positive samples (see Supplementary Figure S3) would suggest that replication occurs and active infection may take place. Moreover, we now confirm that the lineage infecting the placenta corresponds to the predominant lineage at the moment of SARS-CoV-2 infection and not to rare variants with tropism for placenta.
In summary, SARS-CoV-2-positive placentas were observed only in pregnancies infected by the SARS-CoV-2 wildtype. The frequency of placental SARS-CoV-2 may be determined by the SARS-CoV-2 variant, infection timing, or vaccination status of the mother. According to our data, the current risk of SARS-CoV-2 placental infection after maternal COVID disease during pregnancy should be updated.
Supplementary Materials
The following supporting information can be downloaded at: https://www.mdpi.com/article/10.3390/v15091918/s1, Figure S1: Description of the SARS-CoV-2 pandemic in Aragón (Spain) and the placental samples collected in the timeframes indicated; Figure S2: SARS-CoV-2 variants and The ongoing evolution of variants of concern and interest of SARS-CoV-2 in Aragón, Spain; Figure S3: Representation of coverage of the SARS-CoV-2 genome obtained by whole genome sequencing. Three representative images are shown Table S1: Temporal trends in COVID-19 vaccine in our 27 vaccinated women.
Author Contributions
A.M.-M., M.F., J.S. and D.O. were responsible for the design of the study and the writing of the manuscript. M.F., M.P., P.C., S.R.-M., C.P., J.S. and D.O. were responsible for the analysis and interpretation of the data. P.C. and S.R.-M. contributed to the writing of the manuscript. M.F., M.P., M.S., A.M.-M., J.S., A.C.-S., M.O.C. and M.S. were responsible for the laboratory analysis. P.C., S.R.-M., C.P. and D.O. were responsible for the collection of clinical data of the patients. All authors have read and agreed to the published version of the manuscript.
Funding
The work described in this manuscript has been financed by grants from the Government of Aragon (LMP228_21 (2022–2023)) and co-financed by FEDER (“Una manera de hacer Europa, Construyendo Europa desde Aragón”/European Social Funds): 277B05_17D. The funding bodies played no role in the design of the study, in the collection, analysis, and interpretation of data, in writing the manuscript, and in the decision to submit the article for publication. A. Medel-Martinez, P. Calvo, M. Fabre, C. Paules, D. Oros, and S. Ruiz-Martinez were supported by a research grant from the Instituto de Salud Carlos III (FI21/00224, CM20/00078, CM22/00045, JR19/00006, INT20/00033, and CM18/00202).
Institutional Review Board Statement
The study was approved by the Research Ethics Committee of the Community of Aragon 268 (C.I. PI21/155 and COL21/000).
Informed Consent Statement
Written informed consent has been obtained from the patient(s) to publish this paper.
Data Availability Statement
All data are presented in this study. Original data are available upon request from the corresponding author.
Acknowledgments
We acknowledge the use of the Sequencing and Functional Genomics Core Facility (Servicio Científico Técnico de Secuenciación y Genómica Funcional) of the Instituto Aragonés de Ciencias de la Salud (IACS) and Universidad de Zaragoza, Spain. We are grateful to all patients who provided clinical samples at the Biochemistry Department and Obstetrics Department, Hospital Clínico Universitario Lozano Blesa Zaragoza, Spain.
Conflicts of Interest
The authors declare no conflict of interest.
Appendix A
- Whole genome sequencing
RNA was analyzed using a modified version of the COVID-19 ARTIC v4 Illumina library construction and sequencing protocol v4. Briefly, cDNA was synthesized by incubating SuperScript IV reverse transcriptase (Thermo Fisher Scientific, Waltham, MA, USA) with random hexamers and deoxynucleotide triphosphates. The reaction mixture was firstly incubated at 65 °C for 5 min and then at 42 °C for 50 min and at 70 °C for 10 min. Once the cDNA had been synthesized, amplicons were generated with ARTIC v3 two primer pools that covered the whole SARS-CoV-2 genome (Integrated DNA Technologies, Coralville, Iowa, USA). PCR conditions were 98 °C for 30 s, followed by 35 cycles of amplification for 98 °C for 15 s and 63 °C for 5 min, with a final 65 °C extension for 5 min. Amplicons from both pool reactions were mixed and purified with AMPure XP beads (Beckman Coulter, Brea, California, USA) and eluted in 10 Mm Tris-HCl (pH 8.0). Libraries were generated using the Illumina DNA Prep library preparation kit that uses transposomes with adapter sequences to bind fragmented DNA and introduces Illumina index adaptors by the amplification of tagmented DNA (Illumina, Spain Ref #20018705, San Diego, California, USA). Libraries were finally purified and quantified with the Qubit™ dsDNA HS Assay Kit (Thermo Fisher Scientific, Waltham, MA, USA) on a Qubit 4 Fluorometer reader (Thermo Fisher Scientific, Waltham, MA, USA). Libraries were sequenced on a MiSeq instrument (Illumina, San Diego, CA, USA using 150 bp paired-end read). Analysis was performed using DRAGEN COVID Lineage application V3.5.6 (Ilumina, San Diego, CA, USA) and results were downloaded from the BaseSpace Platform. Consensus sequences were assigned to lineages by Pangolin v.2.0.4. According to the settings of the BaseSpace Platform, lineage assignment required a coverage ≥10× over 50% using standard settings. For all except samples 5, 11 and 16, sufficient reads and coverage were obtained to assign the variant present. The variant present in placentas samples was assigned as the pango lineage B.1.177 (six samples), whereas other samples could be only identified as parent lineage B.1. due to limited coverage (seven samples) (Table 2).
References
- Rambaut, A.; Loman, N.; Pybus, O.; Barclay, W.; Barrett, J.; Carabelli, A.; Connor, T.; Peacock, T.; Robertson, D.L.; Volz, E.; et al. Preliminary genomic characterisation of an emergent SARS-CoV-2 lineage in the UK defined by a novel set of spike mutations. Virological 2020. Available online: https://virological.org/t/preliminary-genomic-characterisation-of-an-emergent-sars-cov-2-lineagein-the-uk-defined-by-a-novel-set-of-spike-mutations/563 (accessed on 10 August 2023).
- European Centre for Disease Prevention and Control. Threat Assessment Brief: Emergence of SARS-CoV-2 B.1.617 Variants in India and Situation in the EU/EEA. 11 May 2021. Available online: https://www.ecdc.europa.eu/en/publications-data/threat-assessment-emergence-sars-cov-2-b1617-variants (accessed on 10 August 2023).
- Cao, Y.; Wang, J.; Jian, F.; Xiao, T.; Song, W.; Yisimayi, A.; Huang, W.; Li, Q.; Wang, P.; An, R.; et al. Omicron escapes the majority of existing SARS-CoV-2 neutralizing antibodies. Nature 2022, 602, 657–663. [Google Scholar] [CrossRef]
- World Health Organization (WHO). WHO Tracking SARS-CoV-2 Variants. Available online: https://www.who.int/activities/tracking-SARS-CoV-2-variants (accessed on 10 August 2023).
- Mediavilla, J.R.; Lozy, T.; Lee, A.; Kim, J.; Kan, V.W.; Titova, E.; Amin, A.; Zody, M.C.; Corvelo, A.; Oschwald, D.M.; et al. Molecular and Clinical Epidemiology of SARS-CoV-2 Infection among Vaccinated and Unvaccinated Individuals in a Large Healthcare Organization from New Jersey. Viruses 2023, 15, 1699. [Google Scholar] [CrossRef]
- Esper, F.P.; Adhikari, T.M.; Tu, Z.J.; Cheng, Y.-W.; El-Haddad, K.; Farkas, D.H.; Bosler, D.; Rhoads, D.; Procop, G.W.; Ko, J.S.; et al. Alpha to Omicron: Disease Severity and Clinical Outcomes of Major SARS-CoV-2 Variants. J. Infect. Dis. 2023, 227, 344–352. [Google Scholar] [CrossRef]
- Fiolet, T.; Kherabi, Y.; MacDonald, C.J.; Ghosn, J.; Peiffer-Smadja, N. Comparing COVID-19 vaccines for their characteristics, efficacy and effectiveness against SARS-CoV-2 and variants of concern: A narrative review. Clin. Microbiol. Infect. 2022, 28, 202–221. [Google Scholar] [CrossRef]
- Male, V. SARS-CoV-2 infection and COVID-19 vaccination in pregnancy. Nat. Rev. Immunol. 2022, 22, 277–282. [Google Scholar] [CrossRef]
- Villar, J.; Soto Conti, C.P.; Gunier, R.B.; Ariff, S.; Craik, R.; Cavoretto, P.I.; Rauch, S.; Gandino, S.; Nieto, R.; Winsey, A.; et al. Pregnancy outcomes and vaccine effectiveness during the period of omicron as the variant of concern, INTERCOVID-2022: A multinational, observational study. Lancet 2023, 11, 447–457. [Google Scholar] [CrossRef]
- Villar, J.; Ariff, S.; Gunier, R.B.; Thiruvengadam, R.; Rauch, S.; Kholin, A.; Roggero, P.; Prefumo, F.; do Vale, M.S.; Cardona-Perez, J.A.; et al. Maternal and Neonatal Morbidity and Mortality Among Pregnant Women With and Without COVID-19 Infection: The INTERCOVID Multinational Cohort Study. JAMA Pediatr. 2021, 175, 817–826, Correction in JAMA Pediatr. 2022, 176, 104. [Google Scholar] [CrossRef]
- Savasi, V.M.; Parisi, F.; Patanè, L.; Ferrazzi, E.; Frigerio, L.; Pellegrino, A.; Spinillo, A.; Tateo, S.; Ottoboni, M.; Veronese, P.; et al. Clinical findings and disease severity in hospitalized pregnant women with coronavirus disease 2019 (COVID-19). Obstet. Gynecol. 2020, 136, 252–258. [Google Scholar] [CrossRef]
- Seasely, A.R.; Blanchard, C.T.; Arora, N.; Battarbee, A.N.; Casey, B.M.; Dionne-Odom, J.; Leal, S.M., Jr.; Moates, D.B.; Sinkey, R.G.; Szychowski, J.M.; et al. Maternal and Perinatal Outcomes Associated With the Omicron Variant of Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) Infection. Obstet. Gynecol. 2022, 140, 262–265. [Google Scholar] [CrossRef]
- Vousden, N.; Ramakrishnan, R.; Bunch, K.; Morris, E.; Simpson, N.A.B.; Gale, C.; O’Brien, P.; Quigley, M.; Brocklehurst, P.; Kurinczuk, J.J.; et al. Severity of maternal infection and perinatal outcomes during periods of SARS-CoV-2 wildtype, alpha, and delta variant dominance in the UK: Prospective cohort study. BMJ Med. 2022, 1, e000053. [Google Scholar] [CrossRef] [PubMed]
- Mihajlovic, S.; Nikolic, D.; Santric-Milicevic, M.; Milicic, B.; Rovcanin, M.; Acimovic, A.; Lackovic, M. Four Waves of the COVID-19 Pandemic: Comparison of Clinical and Pregnancy Outcomes. Viruses 2022, 14, 2648. [Google Scholar] [CrossRef] [PubMed]
- Taglauer, E.; Benarroch, Y.; Rop, K.; Barnett, E.; Sabharwal, V.; Yarrington, C.; Wachman, E.M. Consistent localization of SARS-CoV-2 spike glycoprotein and ACE2 over TMPRSS2 predominance in placental villi of 15 COVID-19 positive maternal-fetal dyads. Placenta 2020, 100, 69–74. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, D.A.; Baldewijns, M.; Benachi, A.; Bugatti, M.; Collins, R.R.J.; De Luca, D.; Facchetti, F.; Linn, R.L.; Marcelis, L.; Morotti, D.; et al. Chronic Histiocytic Intervillositis With Trophoblast Necrosis Is a Risk Factor Associated with Placental Infection from Coronavirus Disease 2019 (COVID-19) and Intrauterine Maternal-Fetal Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) Transmission in Live-Born and Stillborn Infants. Arch. Pathol. Lab. Med. 2021, 145, 517–528. [Google Scholar] [PubMed]
- Kotlyar, A.M.; Grechukhina, O.; Chen, A.; Popkhadze, S.; Grimshaw, A.; Tal, O.; Taylor, H.S.; Tal, R. Vertical transmission of coronavirus disease 2019: A systematic review and meta-analysis. Am. J. Obstet. Gynecol. 2021, 224, 35–53.e3. [Google Scholar] [CrossRef]
- Fenizia, C.; Biasin, M.; Cetin, I.; Vergani, P.; Mileto, D.; Spinillo, A.; Gismondo, M.R.; Perotti, F.; Callegari, C.; Mancon, A.; et al. Analysis of SARS-CoV-2 vertical transmission during pregnancy. Nat. Commun. 2020, 11, 5128. [Google Scholar] [CrossRef]
- Dubucs, C.; Groussolles, M.; Ousselin, J.; Sartor, A.; Van Acker, N.; Vayssière, C.; Pasquier, C.; Reyre, J.; Batlle, L.; Stèphanie Favarel Clinical Research Associate; et al. Severe placental lesions due to maternal SARS-CoV-2 infection associated to intrauterine fetal death. Hum. Pathol. 2022, 121, 46–55. [Google Scholar] [CrossRef]
- Celik, E.; Vatansever, C.; Ozcan, G.; Kapucuoglu, N.; Alatas, C.; Besli, Y.; Palaoglu, E.; Gursoy, T.; Manici, M.; Turgal, M.; et al. Placental deficiency during maternal SARS-CoV-2 infection. Placenta 2022, 117, 47–56. [Google Scholar] [CrossRef]
- Garcia-Flores, V.; Romero, R.; Xu, Y.; Theis, K.R.; Arenas-Hernandez, M.; Miller, D.; Peyvandipour, A.; Galaz, J.; Levenson, D.; Bhatti, G.; et al. Maternal-fetal immune responses in pregnant women infected with SARS-CoV-2. Nat. Commun. 2022, 13, 320. [Google Scholar] [CrossRef]
- Gao, Z.; Xu, Y.; Sun, C.; Wang, X.; Guo, Y.; Qiu, S.; Ma, K. A systematic review of asymptomatic infections with COVID-19. J. Microbiol. Immunol. Infect. 2021, 54, 12–16. [Google Scholar] [CrossRef]
- Evolución Diaria COVID-19 en Aragón. Datos Completes. Available online: https://www.aragon.es/coronavirus/situacion-actual/evolucion-diaria-datos-completos (accessed on 10 August 2023).
- Fabre, M.; Calvo, P.; Ruiz-Martinez, S.; Peran, M.; Oros, D.; Medel-Martinez, A.; Strunk, M.; Benito Ruesca, R.; Schoorlemmer, J.; Paules, C. Frequent Placental SARS-CoV-2 in Patients with COVID-19-Associated Hypertensive Disorders of Pregnancy. Fetal Diagn. Ther. 2021, 48, 801–811. [Google Scholar] [CrossRef] [PubMed]
- Figueras, F.; Meler, E.; Iraola, A.; Eixarch, E.; Coll, O.; Figueras, J.; Francis, A.; Gratacos, E.; Gardosi, J. Customized birthweight standards for a Spanish population. Eur. J. Obstet. Gynecol. Reprod. Biol. 2008, 136, 20–24. [Google Scholar] [CrossRef] [PubMed]
- Magee, L.A.; Brown, M.A.; Hall, D.R.; Gupte, S.; Hennessy, A.; Karumanchi, S.A.; Kenny, L.C.; McCarthy, F.; Myers, J.; Poon, L.C.; et al. The 2021 International Society for the Study of Hypertension in Pregnancy classification, diagnosis & management recommendations for international practice. Pregnancy Hypertens. 2022, 27, 148–169. [Google Scholar] [CrossRef] [PubMed]
- Shanes, E.D.; Miller, E.S.; Otero, S.; Ebbott, R.; Aggarwal, R.; Willnow, A.S.; Ozer, E.A.; Mithal, L.B.; Goldstein, J.A. Placental Pathology After SARS-CoV-2 Infection in the Pre-Variant of Concern, Alpha/Gamma, Delta, or Omicron Eras. Int. J. Surg. Pathol. 2022, 31, 387–397. [Google Scholar] [CrossRef] [PubMed]
- Wierz, M.; Sauerbrei, B.; Wandernoth, P.; Kriegsmann, M.; Casadonte, R.; Kriegsmann, K.; Kriegsmann, J. Detection of Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) including Variant Analysis by Mass Spectrometry in Placental Tissue. Viruses 2022, 14, 604. [Google Scholar] [CrossRef]
- Argueta, L.B.; Lacko, L.A.; Bram, Y.; Tada, T.; Carrau, L.; Rendeiro, A.F.; Zhang, T.; Uhl, S.; Lubor, B.C.; Chandar, V.; et al. Inflammatory responses in the placenta upon SARS-CoV-2 infection late in pregnancy. iScience 2022, 25, 104223. [Google Scholar] [CrossRef]
- Dubucs, C.; Groussolles, M.; Brazet, E.; Courtade-Saïdi, M.; Van Acker, N.; Ousselin, J.; Pasquier, C.; Aziza, J. Fetal death and placental lesions after two COVID-19 episodes in single pregnancy in unvaccinated woman. Ultrasound Obstet. Gynecol. 2022, 60, 814–816. [Google Scholar] [CrossRef]
- Heeralall, C.; Ibrahim, U.H.; Lazarus, L.; Gathiram, P.; Mackraj, I. The effects of COVID-19 on placental morphology. Placenta 2023, 138, 88–96. [Google Scholar] [CrossRef]
- Serra, F.E.; Rosa Junior, E.R.; de Rossi, P.; Francisco, R.P.V.; Rodrigues, A.S. COVID-19: Impact of Original, Gamma, Delta, and Omicron Variants of SARS-CoV-2 in Vaccinated and Unvaccinated Pregnant and Postpartum Women. Vaccines 2022, 10, 2172. [Google Scholar] [CrossRef]
- Kourtis, A.P.; Read, J.S.; Jamieson, D.J. Pregnancy and infection. N. Engl. J. Med. 2014, 370, 2211–2218. [Google Scholar] [CrossRef]
- Silasi, M.; Cardenas, I.; Kwon, J.Y.; Racicot, K.; Aldo, P.; Mor, G. Viral infections during pregnancy. Am. J. Reprod. Immunol. 2015, 73, 199–213. [Google Scholar] [CrossRef]
- Mor, G.; Aldo, P.; Alvero, A.B. The unique immunological and microbial aspects of pregnancy. Nat. Rev. Immunol. 2017, 17, 469–482. [Google Scholar] [CrossRef] [PubMed]
- Cribiù, F.M.; Erra, R.; Pugni, L.; Rubio-Perez, C.; Alonso, L.; Simonetti, S.; Croci, G.A.; Serna, G.; Ronchi, A.; Pietrasanta, C.; et al. Severe SARS-CoV-2 placenta infection can impact neonatal outcome in the absence of vertical transmission. J. Clin. Investig. 2021, 131, e145427. [Google Scholar] [CrossRef]
- Smithgall, M.C.; Liu-Jarin, X.; Hamele-Bena, D.; Cimic, A.; Mourad, M.; Debelenko, L.; Chen, X. Third-trimester placentas of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2)-positive women: Histomorphology, including viral immunohistochemistry and in-situ hybridization. Histopathology 2020, 77, 994–999. [Google Scholar] [CrossRef] [PubMed]
- Salamanna, F.; Veronesi, F.; Martini, L.; Landini, M.P.; Fini, M. Post-COVID-19 Syndrome: The Persistent Symptoms at the Post-viral Stage of the Disease. A Systematic Review of the Current Data. Front. Med. 2021, 8, 653516. [Google Scholar] [CrossRef] [PubMed]
- Glynn, S.M.; Yang, Y.J.; Thomas, C.; Friedlander, R.L.; Cagino, K.A.; Matthews, K.C.; Riley, L.E.; Baergen, R.N.; Prabhu, M. SARS-CoV-2 and Placental Pathology: Malperfusion Patterns Are Dependent on Timing of Infection During Pregnancy. Am. J. Surg. Pathol. 2022, 46, 51–57. [Google Scholar] [CrossRef] [PubMed]
- Papageorghiou, A.T.; Deruelle, P.; Gunier, R.B.; Rauch, S.; García-May, P.K.; Mhatre, M.; Usman, M.A.; Abd-Elsalam, S.; Etuk, S.; Simmons, L.E.; et al. Preeclampsia and COVID-19: Results from the INTERCOVID prospective longitudinal study. Am. J. Obstet. Gynecol. 2021, 225, 289.e1–289.e17. [Google Scholar] [CrossRef]
- Duley, L. The global impact of pre-eclampsia and eclampsia. Semin. Perinatol. 2009, 33, 130–137. [Google Scholar] [CrossRef]
- Cunningham, F.G.; Leveno, K.J.; Dashe, J.S.; Bloom, S.L.; Spong, C.T.; Casey, B.M. Williams obstetrics. In Hypertensive Disorders, 24th ed.; Leveno, K.J., Bloom, S.L., Dashe, J.S., Hoffman, B.L., Eds.; McGraw Hill: New York, NY, USA, 2014; Chapter 40; pp. 728–779. [Google Scholar]
- Stock, S.J.; Moore, E.; Calvert, C.; Carruthers, J.; Denny, C.; Donaghy, J.; Hillman, S.; Hopcroft, L.E.M.; Hopkins, L.; Goulding, A.; et al. Pregnancy outcomes after SARS-CoV-2 infection in periods dominated by delta and omicron variants in Scotland: A population-based cohort study. Lancet Respir. Med. 2022, 10, 1129–1136. [Google Scholar] [CrossRef]
- Menni, C.; Valdes, A.M.; Polidori, L.; Antonelli, M.; Penamakuri, S.; Nogal, A.; Louca, P.; May, A.; Figueiredo, J.C.; Hu, C.; et al. Symptom prevalence, duration, and risk of hospital admission in individuals infected with SARS-CoV-2 during periods of omicron and delta variant dominance: A prospective observational study from the ZOE COVID Study. Lancet 2022, 399, 1618–1624. [Google Scholar] [CrossRef]
- Shoji, K.; Tsuzuki, S.; Akiyama, T.; Matsunaga, N.; Asai, Y.; Suzuki, S.; Iwamoto, N.; Funaki, T.; Yamada, M.; Ozawa, N.; et al. Comparison of clinical characteristics of COVID-19 in pregnant women between the Delta and Omicron variants of concern predominant periods. J. Infect. Chemother. 2023, 29, 33–38. [Google Scholar] [CrossRef] [PubMed]
- Adhikari, E.H.; SoRelle, J.A.; McIntire, D.D.; Spong, C.Y. Increasing severity of COVID-19 in pregnancy with Delta (B.1.617.2) variant surge. Am. J. Obstet. Gynecol. 2022, 226, 149–151. [Google Scholar] [CrossRef] [PubMed]
- Konstantinidou, A.E.; Angelidou, S.; Havaki, S.; Paparizou, K.; Spanakis, N.; Chatzakis, C.; Sotiriadis, A.; Theodora, M.; Donoudis, C.; Daponte, A.; et al. Stillbirth due to SARS-CoV-2 placentitis without evidence of intrauterine transmission to fetus: Association with maternal risk factors. Ultrasound Obstet. Gynecol. 2022, 59, 813–822. [Google Scholar] [CrossRef]
- Kontovazainitis, C.G.; Katsaras, G.N.; Gialamprinou, D.; Mitsiakos, G. COVID-19 vaccination and pregnancy: A systematic review of maternal and neonatal outcomes. J. Perinat. Med. 2023, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Blakeway, H.; Prasad, S.; Kalafat, E.; Heath, P.T.; Ladhani, S.N.; Le Doare, K.; Magee, L.A.; O’Brien, P.; Rezvani, A.; von Dadelszen, P.; et al. COVID-19 vaccination during pregnancy: Coverage and safety. Am. J. Obstet. Gynecol. 2022, 226, 236.e1–236.e14. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).