Post-COVID Syndrome in Adults—An Overview
Abstract
1. Introduction
2. Defining Post-COVID Syndrome
3. Prevalence of Post-COVID Syndrome
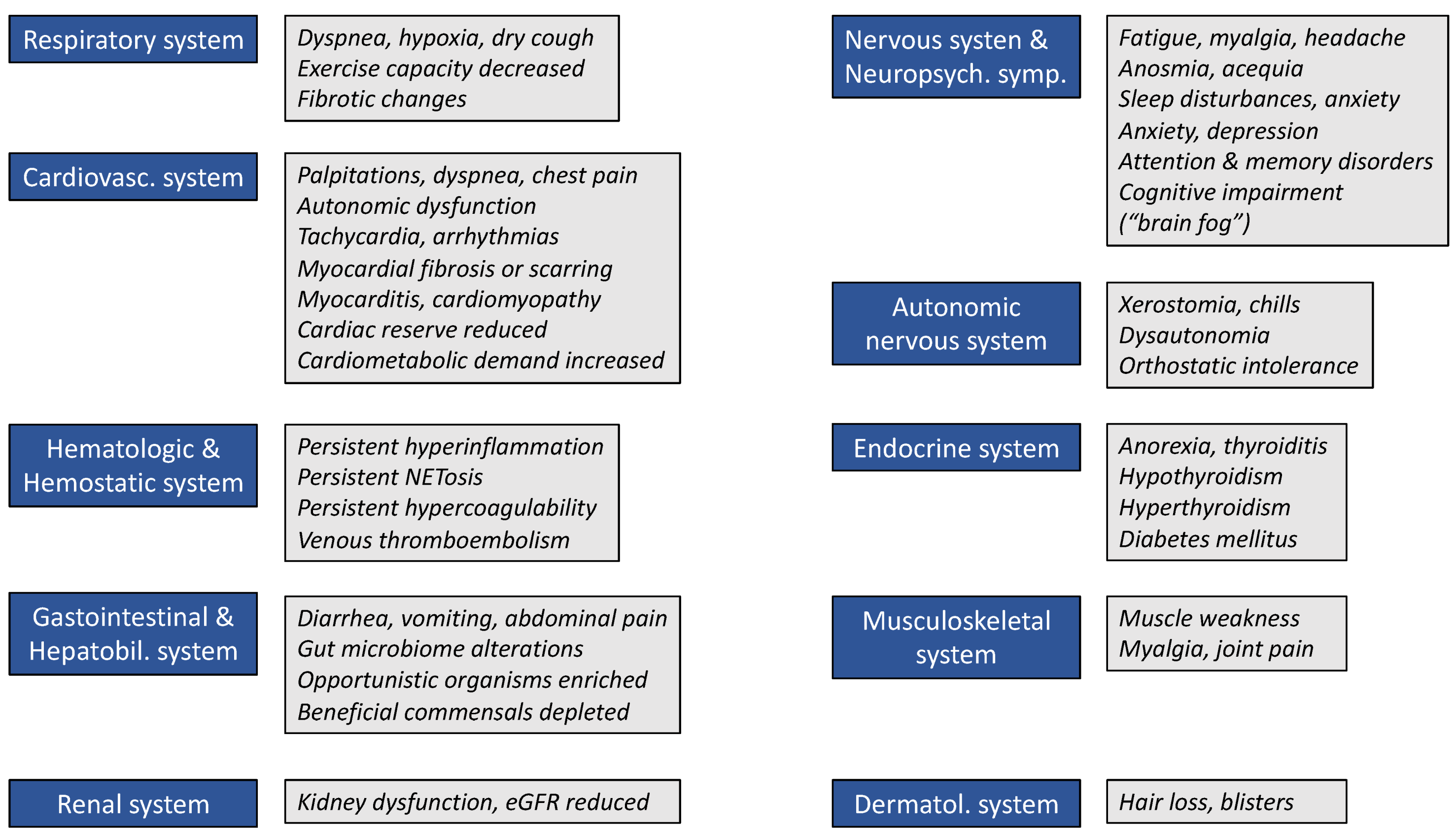
4. Symptoms and Sequelae of Post-COVID Syndrome
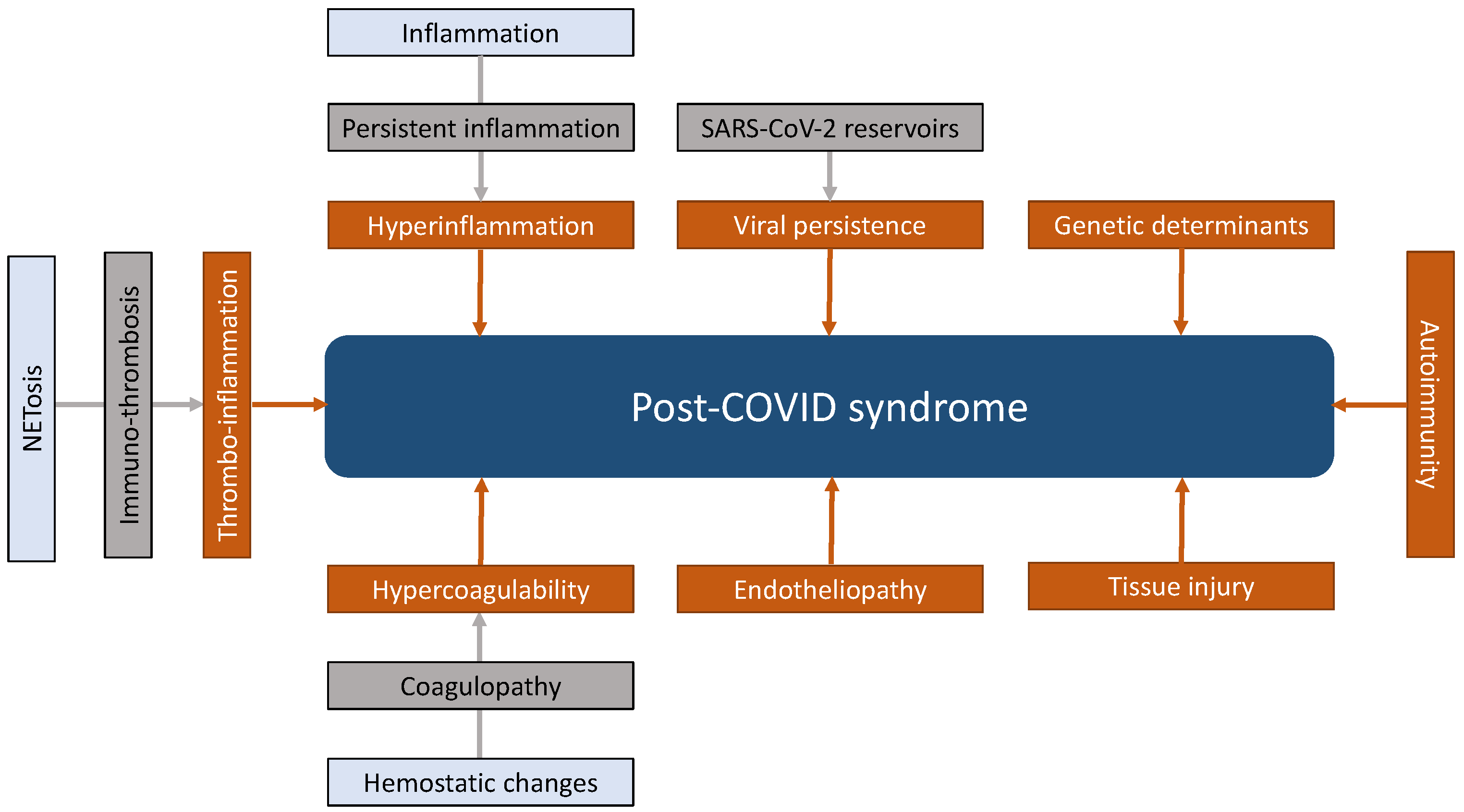
5. Pathogenesis of Post-COVID Syndrome
5.1. Predominant Pathomechanisms of Acute COVID-19
5.2. Pathomechanisms Contributing to Post-COVID Syndrome
5.2.1. Viral Persistence and Abnormalities in Adaptive Immunity Including Autoimmunity
5.2.2. NETosis: A Structural and Functional Link in COVID-19 between Innate Immunity, Inflammation, Endothelial Dysfunction, Hemostasis, and Thrombosis
5.2.3. Hemostatic Abnormalities in COVID-19 and Post-COVID Syndrome
5.2.3.1. Prevalence of Thrombotic Complications
5.2.3.2. COVID-19-Associated Coagulopathy—A Hypercoagulable Condition
5.2.3.3. Platelet Dysfunction in COVID-19
5.2.4. Post-COVID Syndrome and Autoimmunity
5.2.4.1. Epidemiology
5.2.4.2. COVID-19—A Trigger or Cause for Autoimmune Diseases
5.2.4.3. Autoimmunity—A Hallmark of Post-COVID Syndrome
6. COVID-19 and Post-COVID Syndrome in Immunocompromised Hosts
7. Risk Determinants Associated with Post-COVID Syndrome
8. Impact of Vaccination on the Prevention and Treatment of Post-COVID Syndrome
8.1. Breakthrough SARS-CoV-2 Infection in Vaccinated People
8.2. Impact of Vaccination on Post-COVID Symptoms
9. Genetic Basis of the Susceptibility to and Severity of COVID-19
10. Psychosocial Impact of COVID-19 and Post-COVID Syndrome
11. Conclusions, Future Directions, and Perspectives
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Rao, S.; Lee, G.M.; Razzaghi, H.; Lorman, V.; Mejias, A.; Pajor, N.M.; Thacker, D.; Webb, R.; Dickinson, K.; Bailey, L.C.; et al. Clinical features and burden of postacute sequelae of SARS-CoV-2 infection in children and adolescents. JAMA Pediatr. 2022, 176, 1000–1009. [Google Scholar] [CrossRef]
- Lopez-Leon, S.; Wegman-Ostrosky, T.; del Valle, N.C.A.; Perelman, C.; Sepulveda, R.; Rebolledo, P.A.; Cuapio, A.; Villapol, S. Long-COVID in children and adolescents: A systematic review and meta-analyses. Sci. Rep. 2022, 12, 9950. [Google Scholar] [CrossRef]
- Quinn, K.L.; Katz, G.M.; Bobos, P.; Sander, B.; McNaughton, C.D.; Cheung, A.M.; Herridge, M.S.; Atzema, C.L.; Born, K.B.; Chan, C.; et al. Understanding the post COVID-19 condition (long COVID) in adults and the expected burden for Ontario. In Science Briefs, Ontario COVID-19 Advisory Table; 2022; Volume 3, pp. 1–32. Available online: https://covid19-sciencetable.ca/sciencebrief/understanding-the-post-covid-19-condition-long-covid-in-adults-and-the-expected-burden-for-ontario/ (accessed on 31 January 2023).
- World Health Organization. A Clinical Case Definition of Post COVID-19 Condition by a Delphi Consensus, 6 October 2021. Available online: https://www.who.int/publications-detail-redirect/WHO-2019-nCoV-Post_COVID-19_condition-Clinical_case_definition-2021.1 (accessed on 6 October 2021).
- National Institue for Health Care and Excellence. COVID-19 Rapid Guideline: Managing the Long-Term Effects of COVID-19. NICE. Available online: https://www.nice.org.uk/guidance/ng188 (accessed on 18 December 2020).
- Centers for Disease Control and Prevention. Evaluating and Caring for Patients with Post-COVID Conditions: Interim Guidance. Available online: https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-care/post-covid-background.html (accessed on 11 February 2020).
- Centers for Disease Control and Prevention. Post-COVID Conditions. Available online: https://www.cdc.gov/coronavirus/2019-ncov/long-term-effects/index.html (accessed on 11 July 2022).
- Robert Koch Institute. What is Long COVID? RKI Portal on Long COVID. Available online: https.//www.rki.de (accessed on 11 November 2022).
- Public Health Agency of Canada. Post-COVID-19 Condition. Available online: https://www.canada.ca/en/public-health/services/diseases/2019-novel-coronavirus-infection/symptoms/post-covid-19-condition.html (accessed on 20 August 2021).
- Chen, C.; Haupert, S.R.; Zimmermann, L.; Shi, X.; Fritsche, L.G.; Mukherjee, B. Global prevalence of post-coronavirus disease 2019 (COVID-19) condition or long COVID: A meta-analysis and systematic review. J. Infect. Dis. 2022, 226, 1593–1607. [Google Scholar] [CrossRef] [PubMed]
- Nasserie, T.; Hittle, M.; Goodman, S.N. Assessment of the Frequency and Variety of Persistent Symptoms Among Patients With COVID-19: A Systematic Review. JAMA Netw. Open. 2021, 4, e2111417. [Google Scholar] [CrossRef] [PubMed]
- Alkodaymi, M.S.; Omrani, O.A.; Fawzy, N.A.; Shaar, B.A.; Almamlouk, R.; Riaz, M.; Obeidat, M.; Obeidat, Y.; Gerberi, D.; Taha, R.M.; et al. Prevalence of post-acute COVID-19 syndrome symptoms at different follow-up periods: A systematic review and meta-analysis. Clin. Microbiol. Infect. 2022, 28, 657–666. [Google Scholar] [CrossRef] [PubMed]
- Office for National Statistics (in the UK). Self-Reported Long COVID after Infection with the Omicron Variant in the UK. Available online: https://www.ons.gov.uk/peoplepopulationandcommunity/healthandsocialcare/conditionsanddiseases/bulletins/selfreportedlongcovidafterinfectionwiththeomicronvariant/18july2022 (accessed on 18 July 2022).
- Carmona-Torre, F.; Mínguez-Olaondo, A.; López-Bravo, A.; Tijero, B.; Grozeva, V.; Walcker, M.; Azkune-Galparsoro, H.; de Munain, A.L.; Alcaide, A.B. Dysautonomia in COVID-19 patients: A narrative review on clinical course, diagnostic and therapeutic strategies. Front. Neurol. 2022, 13, 886609. [Google Scholar] [CrossRef]
- Huseynov, A.; Akin, I.; Duerschmied, D.; Scharf, R.E. Cardiac arrhythmias in post-COVID syndrome: Prevalence, pathology, diagnosis, and treatment. Viruses 2023, 15, 389. [Google Scholar] [CrossRef]
- Xie, Y.; Al-Aly, Z. Risks and burdens of incident diabetes in long COVID: A cohort study. Lancet Diabetes Endocrinol. 2022, 10, 311–321. [Google Scholar] [CrossRef]
- Rojas, M.; Rodríguez, Y.; Acosta-Ampudia, Y.; Monsalve, D.M.; Zhu, C.; Li, Q.-Z.; Ramírez-Santana, C.; Anaya, J.-M. Autoimmunity is a hallmark of post-COVID syndrome. J. Transl. Med. 2022, 20, 129. [Google Scholar] [CrossRef]
- Xie, Y.; Xu, E.; Bowe, B.; Al-Aly, Z. Long-term cardiovascular outcomes of COVID-19. Nat. Med. 2022, 28, 583–590. [Google Scholar] [CrossRef]
- Katsoularis, I.; Fonseca-Rodríguez, O.; Farrington, P.; Jerndal, H.; Lundevaller, E.H.; Sund, M.; Lindmark, K.; Connolly, A.-M.F. Risks of deep vein thrombosis, pulmonary embolism, and bleeding after COVID-19: Nationwide self-controlled cases series and matched cohort study. Br. Med. J. 2022, 377, e069590. [Google Scholar] [CrossRef] [PubMed]
- Wang, S.; Quan, L.; Chavarro, J.E.; Slopen, N.; Kubzansky, L.D.; Koenen, K.C.; Kang, J.H.; Weisskopf, M.G.; Branch-Elliman, W.; Roberts, A.L. Associations of depression, anxiety, worry, perceived stress, and loneliness prior to infection with risk of post-COVID-19 conditions. JAMA Psychiatry 2022, 79, 1081–1091. [Google Scholar] [CrossRef] [PubMed]
- Xie, Y.; Xu, E.; Al-Aly, Z. Risks of mental health outcomes in people with COVID-19: Cohort study. Br. Med. J. 2022, 376, e068993. [Google Scholar] [CrossRef]
- Mehandru, S.; Merad, M. Pathological sequelae of long-haul COVID. Nat. Immunol. 2022, 23, 194–202. [Google Scholar] [CrossRef]
- Nalbandian, A.; Sehgal, K.; Gupta, A.; Madhavan, M.V.; McGroder, C.; Stevens, J.S.; Cook, J.R.; Nordvig, A.S.; Shalev, D.; Sehrawat, T.S.; et al. Post-acute COVID-19 syndrome. Nat. Med. 2021, 27, 601–615. [Google Scholar] [CrossRef]
- Maltezou, H.C.; Pavli, A.; Tsakris, A. Post-COVID syndrome: An insight on its pathogenesis. Vaccines 2021, 9, 497. [Google Scholar] [CrossRef]
- Batiha, G.E.; Al-Kuraishy, H.M.; Al-Gareeb, A.I.; Welson, N.N. Pathophysiology of post-COVID syndromes. Virol. J. 2022, 19, 158. [Google Scholar] [CrossRef]
- Castanares-Zapatero, D.; Chalon, P.; Kohn, L.; Dauvrin, M.; Detollenaere, J.; de Noordhout, C.M.; Jong, C.P.-D.; Cleemput, I.; Heede, K.V.D. Pathophysiology and mechanism of long COVID: A comprehensive review. Ann. Med. 2022, 54, 1473–1487. [Google Scholar] [CrossRef]
- Rossetti, C.L.; Cazarin, J.; Hecht, F.; de Lima Beltrão, F.E.; Ferreira AC, F.; Fortunato, R.S.; Ramos, H.E.; de Carvalho, D.P. COVID-19 and thyroid function: What do we know so far? Front. Endocrinol. 2022, 13, 1041676. [Google Scholar] [CrossRef] [PubMed]
- Anaya, J.M.; Herran, M.; Beltran, S.; Rojas, M. Is post-COVID syndrome an autoimmune disease? Exp. Rev. Clin. Immunol. 2022, 18, 653–666. [Google Scholar] [CrossRef] [PubMed]
- Ma, M.J.; Qiu, S.F.; Cui, X.M.; Ni, M.; Liu, H.J.; Ye, R.Z.; Yao, L.; Liu, H.B.; Cao, W.C.; Song, H.B. Persistent SARS-CoV-2 infection in asymptomatic young adults. Signal Transduct. Target Ther. 2022, 7, 77. [Google Scholar] [CrossRef]
- Stein, S.R.; Ramelli, S.C.; Grazioli, A.; Chung, J.Y.; Singh, M.; Yinda, C.K.; Winkler, C.W.; Sun, J.; Dickey, J.M.; Ylaya, K.; et al. SARS-CoV-2 infection and persistence in the human body and brain at autopsy. Nature 2022, 612, 758–763. [Google Scholar] [CrossRef] [PubMed]
- Buonsenso, D.; Piazza, M.; Boner, A.L.; Bellanti, J.A. Long COVID: A proposed hypothesis-driven model of viral persistence for the pathophysiology of the syndrome. Allergy Asthma Proc. 2022, 43, 187–193. [Google Scholar] [CrossRef] [PubMed]
- Krishna, B.A.; Lim, E.Y.; Mactavous, L.; Lyons, P.A.; Doffinger, R.; Bradley, J.R.; Smith, K.G.C.; Sinclair, J.; Matheson, N.J.; Lehner, P.J.; et al. Evidence of previous SARS-CoV-2 infection in seronegative patients with long COVID. EBioMedicine 2022, 81, 104129. [Google Scholar] [CrossRef]
- Stark, K.; Massberg, S. Interplay between inflammation and thrombosis in cardiovascular pathology. Nat. Rev. Cardiol. 2021, 18, 666–682. [Google Scholar] [CrossRef] [PubMed]
- Wagner, D.D.; Heger, L.A. Thromboinflammation: From Atherosclerosis to COVID-19. Arterioscl. Thromb. Vasc. Biol. 2022, 42, 1103–1112. [Google Scholar] [CrossRef] [PubMed]
- Fuchs, T.A.; Brill, A.; Duerschmied, D.; Schatzberg, D.; Monestier, M.; Myers, D.D., Jr.; Wrobleski, S.K.; Wakefield, T.W.; Hartwig, J.H.; Wagner, D.D. Extracellular DNA traps promote thrombosis. Proc. Natl. Acad. Sci. USA. 2010, 107, 15880–15885. [Google Scholar] [CrossRef]
- Martinod, K.; Wagner, D.D. Thrombosis: Tangled up in NETs. Blood 2014, 123, 2768–2776. [Google Scholar] [CrossRef]
- Brinkmann, V.; Reichard, U.; Goosmann, C.; Fauler, B.; Uhlemann, Y.; Weiss, D.S.; Weinrauch, Y.; Zychlinsky, A. Neutrophil extracellular traps kill bacteria. Science 2004, 303, 1532–1535. [Google Scholar] [CrossRef]
- Aymonnier, K.; Ng, J.; Fredenburgh, L.E.; Zambrano-Vera, K.; Münzer, P.; Gutch, S.; Fukui, S.; Desjardins, M.; Subramaniam, M.; Baron, R.M.; et al. Inflammasome activation in neutrophils of patients with severe COVID-19. Blood Adv. 2022, 6, 2001–2013. [Google Scholar] [CrossRef]
- Zuo, Y.; Yalavarthi, S.; Shi, H.; Gockman, K.; Zuo, M.; Madison, J.A.; Blair, C.N.; Weber, A.; Barnes, B.J.; Egeblad, M.; et al. Neutrophil extracellular traps in COVID-19. J. Clin. Investig. 2020, 5, e138999. [Google Scholar] [CrossRef] [PubMed]
- Münzer, P.; Negro, R.; Fukui, S.; di Meglio, L.; Aymonnier, K.; Chu, L.; Cherpokova, D.; Gutch, S.; Sorvillo, N.; Shi, L.; et al. NLRP3 Inflammasome assembly in neutrophils is supported by PAD4 and promotes NETosis under sterile conditions. Front. Immunol. 2021, 12, 683803. [Google Scholar] [CrossRef] [PubMed]
- Escher, R.; Breakey, N.; Lammle, B. Severe COVID-19 infection associated with endothelial activation. Thromb. Res. 2020, 190, 62. [Google Scholar] [CrossRef]
- Varga, Z.; Flammer, A.J.; Steiger, P.; Haberecker, M.; Andermatt, R.; Zinkernagel, A.S.; Mehra, M.R.; Schuepbach, R.A.; Ruschitzka, F.; Moch, H. Endothelial cell infection and endotheliitis in COVID-19. Lancet 2020, 395, 1417–1418. [Google Scholar] [CrossRef]
- Ladikou, E.E.; Sivaloganathan, H.; Milne, K.M.; Arter, W.E.; Ramasamy, R.; Saad, R.; Stoneham, S.M.; Philips, B.; Eziefula, A.C.; Chevassut, T. Von Willebrand factor (vWF): Marker of endothelial damage and thrombotic risk in COVID-19? Clin. Med. 2020, 20, e178–e182. [Google Scholar] [CrossRef]
- Middeldorp, S.; Coppens, M.; van Haaps, T.F.; Foppen, M.; Vlaar, A.P.; Müller, M.C.; Bouman, C.C.; Beenen, L.F.; Kootte, R.S.; Heijmans, J.; et al. Incidence of venous thromboembolism in hospitalized patients with COVID-19. J. Thromb. Haemost. 2020, 18, 1995–2002. [Google Scholar] [CrossRef] [PubMed]
- Di Minno, A.; Ambrosino, P.; Calcaterra, I.; Di Minno, M.N.D. COVID-19 and venous thromboembolism: A meta-analysis of literature studies. Sem. Thromb. Hemost. 2020, 46, 763–771. [Google Scholar] [CrossRef]
- Leentjens, J.; van Haaps, T.F.; Wessels, P.F.; Schutgens, R.E.G.; Middeldorp, S. COVID-19-associated coagulopathy and antithrombotic agents-lessons after 1 year. Lancet Haematol. 2021, 8, e524–e533. [Google Scholar] [CrossRef] [PubMed]
- Jiménez, D.; García-Sanchez, A.; Rali, P.; Muriel, A.; Bikdeli, B.; Ruiz-Artacho, P.; Le Mao, R.; Rodríguez, C.; Hunt, B.J.; Monreal, M. Incidence of VTE and bleeding among hospitalized patients with coronavirus disease 2019: A systematic review and meta-analysis. Chest 2021, 159, 1182–1196. [Google Scholar] [CrossRef] [PubMed]
- Tan, B.K.; Mainbourg, S.; Friggeri, A.; Bertoletti, L.; Douplat, M.; Dargaud, Y.; Grange, C.; Lobbes, H.; Provencher, S.; Lega, J.-C. Arterial and venous thromboembolism in COVID-19: A study-level meta-analysis. Thorax 2021, 76, 970–979. [Google Scholar] [CrossRef]
- Xie, J.; Prats-Uribe, A.; Feng, Q.; Wang, Y.; Gill, D.; Paredes, R.; Prieto-Alhambra, D. Clinical and genetic risk factors for acute incident venous thromboembolism in ambulatory patients with COVID-19. JAMA Intern. Med. 2022, 182, 1063–1070. [Google Scholar] [CrossRef] [PubMed]
- Zuin, M.; Engelen, M.M.; Barco, S.; Spyropoulos, A.C.; Vanassche, T.; Hunt, B.J.; Vandenbriele, C.; Verhamme, P.; Kucher, N.; Rashidi, F.; et al. Incidence of venous thromboembolic events in COVID-19 patients after hospital discharge: A systematic review and meta-analysis. Thromb. Res. 2022, 209, 94–98. [Google Scholar] [CrossRef] [PubMed]
- Conway, E.M.; Mackman, N.; Warren, R.Q.; Wolberg, A.S.; Mosnier, L.O.; Campbell, R.A.; Gralinski, L.E.; Rondina, M.T.; van de Veerdonk, F.L.; Hoffmeister, K.M.; et al. Understanding COVID-19-associated coagulopathy. Nat. Rev. Immunol. 2022, 22, 639–649. [Google Scholar] [CrossRef] [PubMed]
- Burn, E.; Duarte-Salles, T.; Fernandez-Bertolin, S.; Reyes, C.; Kostka, K.; Delmestri, A.; Rijnbeek, P.; Verhamme, K.; Prieto-Alhambra, D. Venous or arterial thrombosis and deaths among COVID-19 cases: A European network cohort study. Lancet Infect. Dis. 2022, 22, 1142–1152. [Google Scholar] [CrossRef]
- Whiteley, W.; Wood, A. Risk of arterial and venous thromboses after COVID-19. Lancet Infect. Dis. 2022, 22, 1093–1094. [Google Scholar] [CrossRef]
- Langer, F.; Kluge, S.; Klamroth, R.; Oldenburg, J. Coagulopathy in COVID-19 and its implication for safe and efficacious thromboprophylaxis. Hamostaseologie 2020, 40, 264–269. [Google Scholar] [CrossRef]
- Connors, J.M.; Levy, J.H. COVID-19 and its implications for thrombosis and anticoagulation. Blood 2020, 135, 2033–2040. [Google Scholar] [CrossRef]
- Rieder, M.; Baldus, N.; Stallmann, D.; Jeserich, M.; Goller, I.; Wirth, L.; Pollmeier, L.; Hofmann, M.; Bode, C.; Busch, H.-J.; et al. Early SARS-CoV-2 infection: Platelet-neutrophil complexes and platelet function. Res. Pract. Thromb. Haemost. 2022, 100025. [Google Scholar] [CrossRef]
- Martyanov, A.A.; Boldova, A.E.; Stepanyan, M.G.; An, O.I.; Gur’Ev, A.S.; Kassina, D.V.; Volkov, A.Y.; Balatskiy, A.V.; Butylin, A.A.; Karamzin, S.S.; et al. Longitudinal multiparametric characterization of platelet dysfunction in COVID-19: Effects of disease severity, anticoagulation therapy and inflammatory status. Thromb. Res. 2022, 211, 27–37. [Google Scholar] [CrossRef]
- Anaya, J.-M.; Monsalve, D.M.; Rojas, M.; Rodríguez, Y.; Montoya-García, N.; Mancera-Navarro, L.M.; Villadiego-Santana, A.M.; Rodríguez-Leguizamón, G.; Acosta-Ampudia, Y.; Ramírez-Santana, C. Latent rheumatic, thyroid and phospholipid autoimmunity in hospitalized patients with COVID-19. J. Transl. Autoimmun. 2021, 4, 100091. [Google Scholar] [CrossRef]
- Bastard, P.; Gervais, A.; Le Voyer, T.; Rosain, J.; Philippot, Q.; Manry, J.; Michailidis, E.; Hoffmann, H.-H.; Eto, S.; Garcia-Prat, M.; et al. Autoantibodies neutralizing type I IFNs are present in ~4% of uninfected individuals over 70 years old and account for ~20% of COVID-19 deaths. Sci. Immunol. 2021, 6. [Google Scholar] [CrossRef] [PubMed]
- Wang, E.Y.; Mao, T.; Klein, J.; Dai, Y.; Huck, J.D.; Jaycox, J.R.; Liu, F.; Zhou, T.; Israelow, B.; Wong, P.; et al. Diverse functional autoantibodies in patients with COVID-19. Nature 2021, 595, 283–288. [Google Scholar] [CrossRef] [PubMed]
- Chang, R.; Yen-Ting Chen, T.; Wang, S.I.; Hung, Y.M.; Chen, H.Y.; Wei, C.J. Risk of autoimmune diseases in patients with COVID-19: A retrospective cohort study. EClinicalMedicine 2023, 56, 101783. [Google Scholar] [CrossRef] [PubMed]
- Kim, B.; Kaistha, S.D.; Rouse, B.T. Viruses and autoimmunity. Autoimmunity 2006, 39, 71–77. [Google Scholar] [CrossRef] [PubMed]
- Getts, D.R.; Chastain, E.M.; Terry, R.L.; Miller, S.D. Virus infection, antiviral immunity, and autoimmunity. Immunol. Rev. 2013, 255, 197–209. [Google Scholar] [CrossRef]
- Fujinami, R.S.; von Herrath, M.G.; Christen, U.; Whitton, J.L. Molecular mimicry, bystander activation, or viral persistence: Infections and autoimmune disease. Clin. Microbiol. Rev. 2006, 19, 80–94. [Google Scholar] [CrossRef]
- Acha-Orbea, H. Bacterial and viral superantigens: Roles in autoimmunity? Ann. Rheum. Dis. 1993, 52 (Suppl. S1), S6–S16. [Google Scholar] [CrossRef]
- Canas, C.A. The triggering of post-COVID-19 autoimmunity phenomena could be associated with both transient immunosuppression and an inappropriate form of immune reconstitution in susceptible individuals. Med. Hypotheses 2020, 145, 110345. [Google Scholar] [CrossRef]
- Anaya, J.-M.; Rojas, M.; Salinas, M.L.; Rodríguez, Y.; Roa, G.; Lozano, M.; Rodríguez-Jiménez, M.; Montoya, N.; Zapata, E.; Monsalve, D.M.; et al. Post-COVID syndrome. A case series and comprehensive review. Autoimmun. Rev. 2021, 20, 102947. [Google Scholar] [CrossRef]
- Acosta-Ampudia, Y.; Monsalve, D.M.; Rojas, M.; Rodríguez, Y.; Zapata, E.; Ramírez-Santana, C.; Anaya, J.-M. Persistent autoimmune activation and proinflammatory state in post-coronavirus disease 2019 syndrome. J. Infect. Dis. 2022, 225, 2155–2162. [Google Scholar] [CrossRef]
- Tang, K.T.; Hsu, B.C.; Chen, D.Y. Autoimmune and rheumatic manifestations associated with COVID-19 in adults: An updated systematic review. Front. Immunol. 2021, 12, 645013. [Google Scholar] [CrossRef]
- Jakharia, N.; Subramanian, A.K.; Shapiro, A.E. COVID-19 in the immunocompromised host, including people with human immunodeficiency virus. Infect. Dis. Clin. N. Am. 2022, 36, 397–421. [Google Scholar] [CrossRef]
- Corey, L.; Beyrer, C.; Cohen, M.S.; Michael, N.L.; Bedford, T.; Rolland, M. SARS-CoV-2 variants in patients with immunosuppression. N. Engl. J. Med. 2021, 385, 562–566. [Google Scholar] [CrossRef]
- Jing, Y.; Luo, L.; Chen, Y.; Westerberg, L.S.; Zhou, P.; Xu, Z.; Herrada, A.A.; Park, C.-S.; Kubo, M.; Mei, H.; et al. SARS-CoV-2 infection causes immunodeficiency in recovered patients by downregulating CD19 expression in B cells via enhancing B-cell metabolism. Signal Transduct. Target Ther. 2021, 6, 345. [Google Scholar] [CrossRef]
- Kuczborska, K.; Buda, P.; Ksiazyk, J. Long-COVID in immunocompromised children. Eur. J. Pediatr. 2022, 181, 3501–3509. [Google Scholar] [CrossRef]
- Iqbal, F.M.; Lam, K.; Sounderajah, V.; Clarke, J.M.; Ashrafian, H.; Darzi, A. Characteristics and predictors of acute and chronic post-COVID syndrome: A systematic review and meta-analysis. EClinicalMedicine 2021, 36, 100899. [Google Scholar] [CrossRef]
- Klein, J.; Wood, J.; Jaycox, J.; Lu, P.; Dhodapkar, R.M.; Gehlhausen, J.R.; Tabachnikova, A.; Tabacof, L.; Malik, A.A.; Kamath, K.; et al. Distinguishing features of Long COVID identified through immune profiling. medRxiv 2022. [Google Scholar] [CrossRef]
- Subramanian, A.; Nirantharakumar, K.; Hughes, S.; Myles, P.; Williams, T.; Gokhale, K.M.; Taverner, T.; Chandan, J.S.; Brown, K.; Simms-Williams, N.; et al. Symptoms and risk factors for long COVID in non-hospitalized adults. Nat. Med. 2022, 28, 1706–1714. [Google Scholar] [CrossRef] [PubMed]
- Zheng, C.; Shao, W.; Chen, X.; Zhang, B.; Wang, G.; Zhang, W. Real-world effectiveness of COVID-19 vaccines: A literature review and meta-analysis. Int. J. Infect. Dis. 2022, 114, 252–260. [Google Scholar] [CrossRef] [PubMed]
- Nixon, D.F.; Ndhlovu, L.C. Vaccine breakthrough infections with SARS-CoV-2 variants. N. Engl. J. Med. 2021, 385, e7. [Google Scholar] [PubMed]
- Juthani, P.V.; Gupta, A.; A Borges, K.; Price, C.C.; I Lee, A.; Won, C.H.; Chun, H.J. Hospitalisation among vaccine breakthrough COVID-19 infections. Lancet Infect. Dis. 2021, 21, 1485–1486. [Google Scholar] [CrossRef] [PubMed]
- Notarte, K.I.; Catahay, J.A.; Velasco, J.V.; Pastrana, A.; Ver, A.T.; Pangilinan, F.C.; Peligro, P.J.; Casimiro, M.; Guerrero, J.J.; Gellaco, M.M.L.; et al. Impact of COVID-19 vaccination on the risk of developing long-COVID and on existing long-COVID symptoms: A systematic review. EClinicalMedicine 2022, 53, 101624. [Google Scholar] [CrossRef]
- Antonelli, M.; Penfold, R.S.; Merino, J. Risk factors and disease profile of post-vaccination SARS-CoV-2 infection in UK users of the COVID Symptom Study app: A prospective, community-based, nested, case-control study. Lancet Infect. Dis. 2022, 22, 43–55. [Google Scholar] [CrossRef] [PubMed]
- Al-Aly, Z.; Bowe, B.; Xie, Y. Long COVID after breakthrough SARS-CoV-2 infection. Nat. Med. 2022, 28, 1461–1467. [Google Scholar] [CrossRef]
- Ayoubkhani, D.; Bermingham, C.; Pouwels, K.B.; Glickman, M.; Nafilyan, V.; Zaccardi, F.; Khunti, K.; A Alwan, N.; Walker, A.S. Trajectory of long covid symptoms after COVID-19 vaccination: Community based cohort study. Br. Med. J. 2022, 377, e069676. [Google Scholar] [CrossRef] [PubMed]
- Tran, V.T.; Perrodeau, E.; Saldanha, J.; Pane, I.; Ravaud, P. Efficacy of COVID-19 vaccination on the symptoms of patients with long-COVID: A target trial emulation using data from the ComPaRe e-cohort in France. SSRN 2021. [Google Scholar] [CrossRef]
- Tsuchida, T.; Hirose, M.; Inoue, Y.; Kunishima, H.; Otsubo, T.; Matsuda, T. Relationship between changes in symptoms and antibody titers after a single vaccination in patients with Long COVID. J. Med. Virol. 2022, 94, 3416–3420. [Google Scholar] [CrossRef]
- Chapman, S.J.; Hill, A.V. Human genetic susceptibility to infectious disease. Nat. Rev. Genet. 2012, 13, 175–188. [Google Scholar] [CrossRef]
- Casanova, J.L.; Su, H.C.; Effort, C.H.G. A global effort to define the human genetics of protective immunity to SARS-CoV-2 infection. Cell 2020, 181, 1194–1199. [Google Scholar] [CrossRef]
- The Severe COVID-19 GWAS Group. Genomwide association study of severe COVID-19 with respiratory failure. N. Engl. J. Med. 2020, 383, 1522–1534. [Google Scholar] [CrossRef]
- Pairo-Castineira, E.; Clohisey, S.; Klaric, L.; Bretherick, A.D.; Rawlik, K.; Pasko, D.; Walker, S.; Parkinson, N.; Fourman, M.H.; Russell, C.D.; et al. Genetic mechanisms of critical illness in COVID-19. Nature 2021, 591, 92–98. [Google Scholar] [CrossRef] [PubMed]
- Niemi, M.E.K.; Karjalainen, J.; Liao, R.G.; Neale, B.M.; Daly, M. COVID-19 Host Genetics Initiative. Mapping the human genetic architecture of COVID-19. Nature 2021, 600, 472–477. [Google Scholar]
- Asgari, S.; Pousaz, L.A. Human genetic variants identified that affect COVID susceptibility and severity. Nature 2021, 600, 390–391. [Google Scholar] [CrossRef] [PubMed]
- Andreakos, E.; Abel, L.; Vinh, D.C.; Kaja, E.; Drolet, B.A.; Zhang, Q.; O’Farrelly, C.; Novelli, G.; Rodríguez-Gallego, C.; Haerynck, F.; et al. Author Correction: A global effort to dissect the human genetic basis of resistance to SARS-CoV-2 infection. Nat. Immunol. 2022, 23, 341. [Google Scholar] [CrossRef] [PubMed]
- Rosa, H.; Hollstein, B. Unverfügbarkeit als soziale Erfahrung. Ein soziologischer Deutungsversuch der Corona-Krise angewendet auf die Wirtschaftsethik. In Sonderband Zschr f. Wirtschafts- u. Unternehmensethik (ZfWU)/J Business, Economics & Ethics; Brink, A., Hollstein, B., Hübscher, M.C., Neuhäuser, C., Eds.; Nomos Verlags Ges.: Baden-Baden, German, 2020; Volume 21, pp. 21–34. ISBN 978-3-8487-6847-9. [Google Scholar]
- Scharf, R.E. How the COVID-19 pandemic impacts lives of life scientists. Hamostaseologie 2021, 41, 9–13. [Google Scholar] [CrossRef]
- Dubey, S.; Biswas, P.; Ghosh, R.; Chatterjee, S.; Dubey, M.J.; Chatterjee, S.; Lahiri, D.; Lavie, C.J. Psychosocial impact of COVID-19. Diabetes Metab. Syndr. 2020, 14, 779–788. [Google Scholar] [CrossRef]
- Grasso, M.; Klicperová-Baker, M.; Koos, S.; Kosyakova, Y.; Petrillo, A.; Vlase, I. The impact of the coronavirus crisis on European societies. What have we learnt and where do we go from here. Introduction to the COVID volume. Eur. Soc. 2021, 23 (Suppl. S1), S2–S32. [Google Scholar] [CrossRef]
| Origin | Term | Definition |
|---|---|---|
| World Health Organization (WHO) [4] | Post COVID-19 condition | Symptoms occurring at least three months after probable or confirmed SARS-CoV-2 infection. Symptoms must last for at least two months and cannot be explained by an alternative diagnosis. Symptoms may be new onset following recovery from acute SARS-CoV-2 infection or persist from the initial illness. Symptoms may fluctuate or relapse. |
| National Institute for Clinical Excellence (NICE) [5] | Long COVID (includes ongoing symptomatic COVID-19 and post-COVID syndrome) | Symptoms of COVID-19 experienced for 12 or more weeks after initial recovery. Persistence of COVID-19 signs and symptoms that continue to develop after acute COVID-19 and can include both ongoing symptomatic COVID-19 and post-COVID syndrome. Ongoing symptomatic COVID-19 Signs and symptoms which persist from 4 to 12 weeks after acute COVID-19. Post COVID-19 syndrome Signs and symptoms that develop during or after an infection consistent with COVID-19, continue for more than 12 weeks and are not explained by an alternate diagnosis. |
| Centers for Disease Control and Prevention (CDC) [6,7] | Post COVID-19 condition | The United States (US) Centers for Disease Control and Prevention uses the term ‘post-COVID conditions’ as an umbrella term for the wide range of health consequences that are present ≥4 weeks after infection with SARS-CoV-2. This includes both general complications of prolonged acute illness and new, returning, or ongoing health problems as post-acute sequelae of SARS-CoV-2 infection (PASC). |
| Robert Koch Institute (RKI) [8] | Long COVID-19 vs. post-COVID-19 condition or post-COVID syndrome | Long COVID * Longer-term health impairments following a SARS-CoV-2 infection that are present beyond the acute phase of the sickness of 4 weeks. The symptoms either begin during the acute phase of the disease and persist for a longer period of time, appear or reoccur in the course of weeks and months after the infection. Post-COVID condition or post-COVID syndrome Symptoms are either still present at least 12 weeks and longer after the acute infection or appear anew after this period and cannot be explained otherwise. |
| Government of Canada [9] | Post COVID-19 condition | Symptoms of COVID-19 experienced for 12 or more weeks after initial recovery. |
| Author (Year) | Pooled Prevalence | ||
|---|---|---|---|
| VTE (95% CI) | DVT (95% CI) | PE (95% CI) | |
| Di Minno et al., [45] (2021) | 31.3 (24.3–39.2) | 19.8 (10.5–34.0) | 18.9 (14.4–24.3) |
| Leentjens et al., [46] (2021) | 14.1 (11.6–16.9) | n.d. | n.d. |
| Jiménez et al., [47] (2021) | 17.0 (13.4–20.9) | 12.1 (8.4–16.4) | 7.8 (2.6–15.3) |
| Tan et al., [48] (2021) | 14.7 (12.1–17.6) | 11.2 (8.4–14.3) | 7.8 (6.2 9.4) |
| Autoimmune Disease | Adjusted Hazard Ratio (aHR) | 95% Confidence Interval (CI) |
|---|---|---|
| Rheumatoid arthritis | 2.98 | 2.78–3.20 |
| Ankylosing spondylitis | 3.21 | 2.50–4.13 |
| Systemic lupus erythematosus | 2.99 | 2.68–3.34 |
| Dermatopolymyositis | 1.96 | 1.47–2.61 |
| Systemic sclerosis | 2.58 | 2.02–3.28 |
| Sjögren’s syndrome | 2.62 | 2.29–3.00 |
| Mixed connective tissue disease | 3.14 | 2.26–4.36 |
| Behçet’s disease | 2.32 | 1.38–3.89 |
| Polymyalgia rheumatica | 2.90 | 2.36–3.57 |
| Vasculitis | 1.96 | 1.74–2.20 |
| Psoriasis | 2.91 | 2.67–3.17 |
| Inflammatory bowel disease | 1.78 | 1.72–1.84 |
| Celiac disease | 2.68 | 2.51–2.85 |
| Diabetes mellitus type 1 | 2.68 | 2.51–2.85 |
| Mortality | 1.20 | 1.16–1.24 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Scharf, R.E.; Anaya, J.-M. Post-COVID Syndrome in Adults—An Overview. Viruses 2023, 15, 675. https://doi.org/10.3390/v15030675
Scharf RE, Anaya J-M. Post-COVID Syndrome in Adults—An Overview. Viruses. 2023; 15(3):675. https://doi.org/10.3390/v15030675
Chicago/Turabian StyleScharf, Rüdiger E., and Juan-Manuel Anaya. 2023. "Post-COVID Syndrome in Adults—An Overview" Viruses 15, no. 3: 675. https://doi.org/10.3390/v15030675
APA StyleScharf, R. E., & Anaya, J.-M. (2023). Post-COVID Syndrome in Adults—An Overview. Viruses, 15(3), 675. https://doi.org/10.3390/v15030675







