The Dental Aesthetic Index and Dental Health Component of the Index of Orthodontic Treatment Need as Tools in Epidemiological Studies
Abstract
:1. Introduction
2. Experimental Section
2.1. Sample
2.2. Reproducibility, Validity and Time Evaluations
2.3. Statistical Analysis
3. Results and Discussion
3.1. Results
3.2. Discussion
4. Conclusions
Acknowledgments
- Conflict of InterestThe authors declare no conflict of interest.
References
- Brook, PH; Shaw, WC. The development of an index of orthodontic treatment priority. Eur. J. Orthod 1989, 11, 309–320. [Google Scholar]
- Cons, NC; Jenny, J; Kohout, FJ; Songpaisan, Y; Jotikastira, D. Utility of the dental aesthetic index in industrialized and developing countries. J. Public Health Dent 1989, 49, 163–166. [Google Scholar]
- Richmond, S; Shaw, WC; O’brien, K; Buchanan, IB; Stephens, CD; Andrews, M; Roberts, CT. The relationship between the index of orthodontic treatment need and the consensus opinion of a panel of 74 dentists. Br. Dent. J 1995, 178, 370–374. [Google Scholar]
- Jenny, J; Cons, NC. Comparing and contrasting two orthodontic indices, the index of orthodontic treatment need and the dental aesthetic index. Am. J. Orthod. Dentofac. Orthop 1996, 110, 410–416. [Google Scholar]
- Freire, MC; Reis, SC; Gonçalves, MM; Balbo, PL; Leles, CR. Oral health in 12 year-old students from public and private schools in the city of Goiânia. Rev. Panam. Salud. Public 2010, 28, 86–91. [Google Scholar]
- Manzanera, D; Montiel-Company, JM; Almerich-Silla, JM; Gandía, JL. Orthodontic treatment need in Spanish schoolchildren: An epidemiological study using the Index of Orthodontic Treatment Need. Eur. J. Orthod 2009, 31, 180–183. [Google Scholar]
- Shivakumar, KM; Chandu, GN; Subba Reddy, VV; Shafiulla, MD. Prevalence of malocclusion and orthodontic treatment needs among middle and high school children of Davangere city, India by Dental Aesthetic Index. J. Indian Soc. Pedod. Prev. Dent 2009, 27, 211–218. [Google Scholar]
- Nelson, S; Armogan, V; Abel, Y; Broadbent, BH; Hans, M. Disparity in orthodontic utilization and treatment need among high school students. Public Health Dent 2004, 64, 26–30. [Google Scholar]
- Jenny, J; Cons, NC. Establishing malocclusion severity levels on the dental aesthetic index (DAI) scale. Aust. Dent. J 1996, 41, 43–46. [Google Scholar]
- Richmond, S; Shaw, WC; O’brien, KD; Buchanan, IB; Jones, R; Stephens, S; Roberts, CT; Andrew, M. The development of the PAR index (peer assessment rating): Reliability and validity. Eur. J. Orthod 1992, 14, 125–139. [Google Scholar]
- Buchanan, IB; Downing, A; Stirrups, DR. A comparison of the index of orthodontic treatment need applied clinically and to diagnostic records. Br. J. Orthod 1994, 21, 185–188. [Google Scholar]
- Freer, E; Freer, TF. Variations in treatment need using four screening methods. Aust. Orthod. J 1999, 15, 214–218. [Google Scholar]
- Batarrita, JA. Entre el consenso y la evidencia científica. Gac. Sanit 2005, 19, 65–70. [Google Scholar]
- Ovsenik, M; Primozic, J. Evaluation of 3 occlusal indexes: Eismann index, Eismann-Farcnik index, and index of orthodontic treatment need. Am. J. Orthod. Dentofac. Orthop 2007, 131, 496–503. [Google Scholar]
- Sim, J; Wright, CC. The Kappa statistic in reliability studies: Use, interpretation and sample size requirements. Phys. Ther 2005, 85, 257–268. [Google Scholar]
- Cunha, ACPP; Miguel, JA; Lima, KC. DAI and IOTN index assessment in the prognosis of malocclusions and requirement of orthodontic treatment. Dental Press J. Orthod 2003, 8, 51–58. [Google Scholar]
- Beglin, FM; Firestone, AR; Vig, KWL; Beck, FM; Kuthy, RA; Wade, D. A comparison of the reliability and validity of 3 occlusal indices of orthodontic treatment need. Am. J. Orthod. Dentofac. Orthop 2001, 120, 240–246. [Google Scholar]
- Lima, RB; Paiva, ACP; Farias, ACR; Lima, KC. An analysis of reproducibility of DAI and IOTN indices in a Brazilian scene. Cien. Saude Colet 2010, 15, 785–792. [Google Scholar]
- Arruda, AO. Occlusal indices as judged by subjective opinions. Am. J. Orthod. Dentofac. Orthop 2008, 134, 671–675. [Google Scholar]
- Firestone, AR; Beck, FM; Beglin, FM; Vig, KWL. Evaluation of the peer assessment rating (PAR) index as an index of orthodontic treatment need. Am. J. Orthod. Dentofac. Orthop 2002, 122, 463–469. [Google Scholar]
- Younis, JW; Vig, KWL; Rinchuse, DJ; Weyant, RJ. A validation study of three indexes of orthodontic treatment need in the United States. Community Dent. Oral. Epidemiol 1997, 25, 358–362. [Google Scholar]
- Soumes, M; Bassigny, F; Zenati, N; Riordan, PJ; Boy-Lefevre, ML. Orthodontic Treatment need in French schoolchildren: An epidemiological study using the Index of Orthodontic Treatment Need. Eur. J. Orthod 2006, 28, 605–609. [Google Scholar]
- Marques, LS; Pordeus, IA; Ramos-Jorge, ML; Filogônio, CA; Filogônio, CB; Pereira, LJ; Paiva, SM. Factors associated with the desire for orthodontic treatment among Brazilian adolescents and their parents. BMC Oral Health 2009, 18, 9–34. [Google Scholar]
- Spalj, S; Slaj, M; Varga, S; Strujic, M; Slaj, M. Perception of orthodontic treatment need in children and adolescents. Eur. J. Orthod 2010, 32, 387–394. [Google Scholar]
| DAI | Frequency (n = 131) |
| No need or little need | 11% |
| Elective treatment | 28% |
| Highly desirable treatment | 22% |
| Essential treatment | 39% |
| IOTN | |
| No need | 9% |
| Moderate need | 19% |
| In need of severe treatment | 72% |
| DHC | |||
|---|---|---|---|
| DAI | Need | No need | Total |
| Need | 83% | 5% | 88% |
| No need | 8% | 4% | 12% |
| Total | 91% | 9% | 100% |
| Average time (SD) | Median time | Range (Minimum-Maximum) | P value * | |
|---|---|---|---|---|
| DAI | 118.9 (±37.7) | 116.0 | 46.0–215.0 | <0.001 |
| DHC-IOTN | 59.5 (±41.9) | 47.0 | 3.0–200.0 |
| DAI | DHC | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| GOLD STANDARD | Cutoff points | 25 | 31 | 2 | 3 | ||||
| Need | No need | Need | No need | Need | No need | Need | No need | ||
| Need | 47% | 5% | 31% | 21% | 52% | 0% | 44% | 8% | |
| No need | 41% | 7% | 24% | 24% | 39% | 9% | 27% | 21% | |
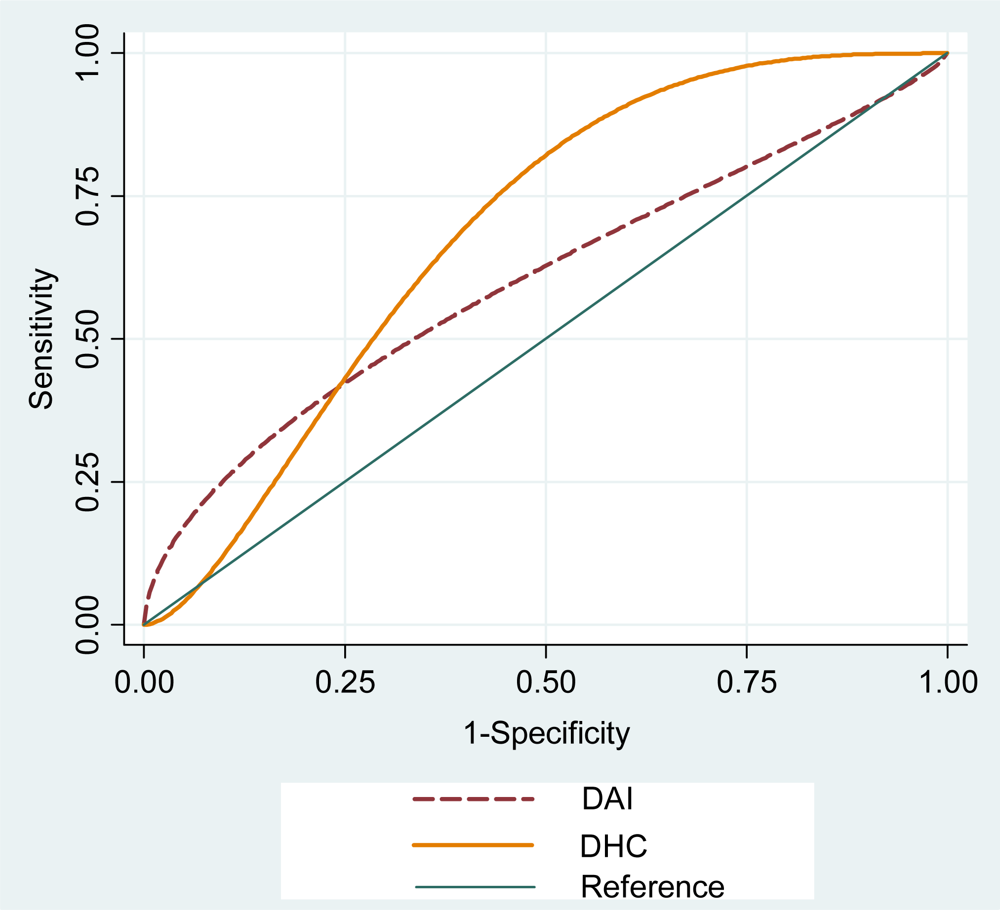
| DAI (CI95%) | DHC (CI95%) | |||
|---|---|---|---|---|
| Cutoff points | 25 | 31 | 2 | 3 |
| Sensitivity | 91 (81–96) | 56 (44–68) | 100 (93–100) | 85 (74–92) |
| Specificity | 14 (7–26) | 53 (40–67) | 19 (10–31) | 43 (31–56) |
| PPV* | 28 (24–32) | 57 (45–69) | 31 (27–34) | 62 (54–70) |
| NPV** | 82 (51–95) | 53 (40–65) | 100 (81–100) | 73 (52–87) |
| Accuracy*** | 61 (51–70)**** | 67 (58–77) ***** | ||
© 2011 by the authors; licensee MDPI, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Cardoso, C.F.; Drummond, A.F.; Lages, E.M.B.; Pretti, H.; Ferreira, E.F.; Abreu, M.H.N.G. The Dental Aesthetic Index and Dental Health Component of the Index of Orthodontic Treatment Need as Tools in Epidemiological Studies. Int. J. Environ. Res. Public Health 2011, 8, 3277-3286. https://doi.org/10.3390/ijerph8083277
Cardoso CF, Drummond AF, Lages EMB, Pretti H, Ferreira EF, Abreu MHNG. The Dental Aesthetic Index and Dental Health Component of the Index of Orthodontic Treatment Need as Tools in Epidemiological Studies. International Journal of Environmental Research and Public Health. 2011; 8(8):3277-3286. https://doi.org/10.3390/ijerph8083277
Chicago/Turabian StyleCardoso, Chrystiane F., Alexandre F. Drummond, Elisabeth M.B. Lages, Henrique Pretti, Efigênia F. Ferreira, and Mauro Henrique N.G. Abreu. 2011. "The Dental Aesthetic Index and Dental Health Component of the Index of Orthodontic Treatment Need as Tools in Epidemiological Studies" International Journal of Environmental Research and Public Health 8, no. 8: 3277-3286. https://doi.org/10.3390/ijerph8083277




