Diabetes, Iron-Deficiency Anemia, and Endocrine, Nutritional, and Metabolic Disorders in Children: A Socio-Epidemiological Study in Urban Kazakhstan
Abstract
1. Introduction
2. Materials and Methods
Data Analysis
3. Results
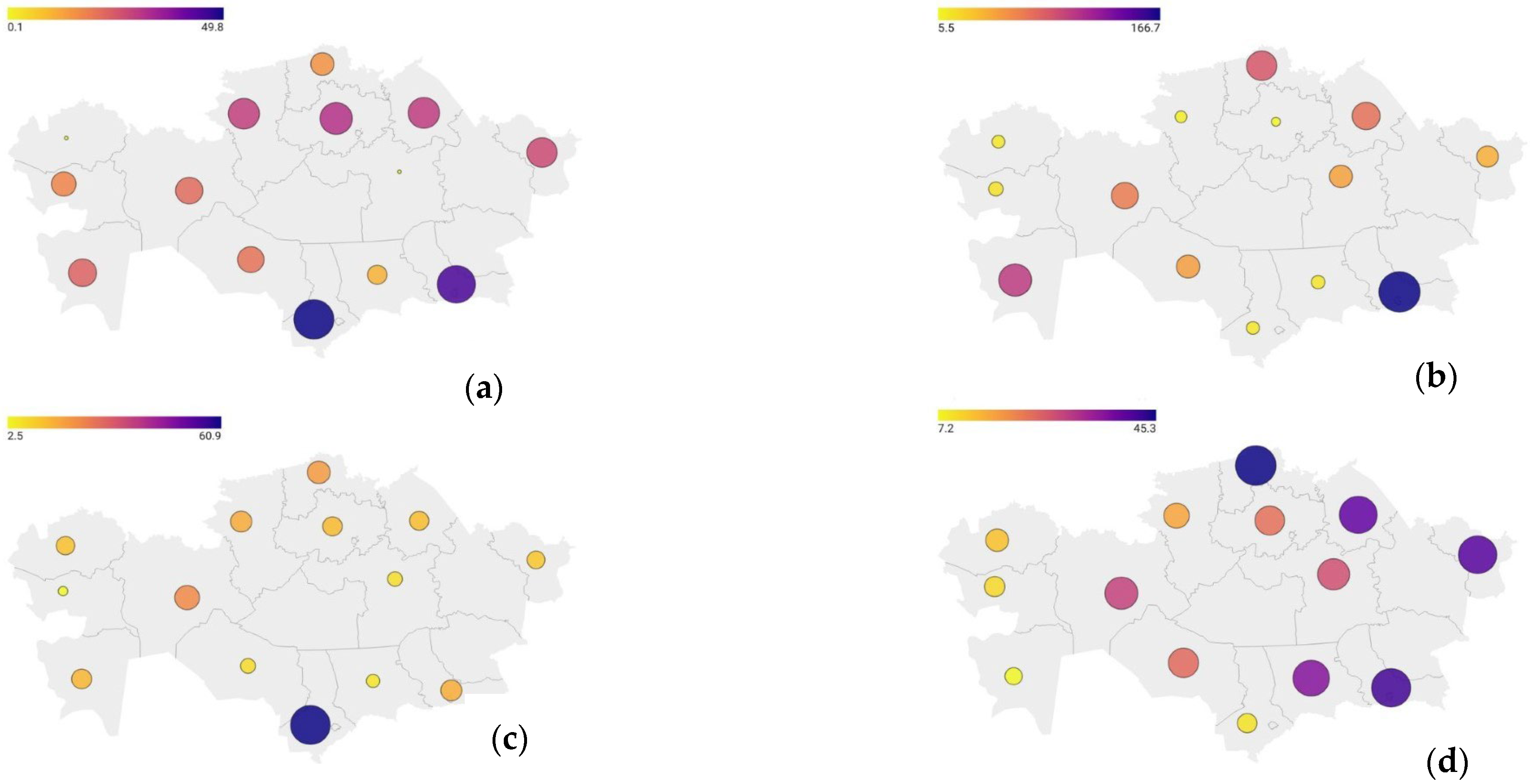
3.1. Trends in DM, IDA, ENMD Incidence of Children in Urban Areas of Kazakhstan
3.2. Descriptive Statistics of Variables
3.3. Factors Affecting to the Incidences of IDA, DM, and ENMD Among Children Aged 0–14 and Adolescents Aged 15–17
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization (WHO). World Health Statistics 2020: Monitoring Health for the SDGs, Sustainable Development Goals; WHO: Geneva, Switzerland, 2020; Available online: https://creativecommons.org/licenses/by-nc-sa/3.0/igo (accessed on 19 June 2025).
- Aksenova, E.I.; Korotkova, Y.O.; Gorbatov, C.Y.; Kamynina, N.N. Monitoring of Risk Factors for Noncommunicable Diseases in the Adult Population: International Experience; NIIOZMM: Moscow, Russia, 2022; p. 70. (In Russian) [Google Scholar]
- Mukhazhanova, B.S.; Tulegenova, R.A.; Seyduanova, L.B. Approaches to Improving the Effectiveness of the Quality of Medical Services. Med. Ecol. 2025, 1, 153–163. (In Russian) [Google Scholar] [CrossRef]
- Nagaeva, T.A.; Basareva, N.I.; Ponomareva, D.A. Basics of Health Formation in Children and Adolescents: Lecture Course; Publishing House of Siberian State Medical University: Tomsk, Russia, 2020; p. 196. Available online: https://elar.ssmu.ru/bitstream/20.500.12701/3235/1/tut_ssmu-2020-19.pdf (accessed on 19 June 2025).
- UNICEF Innocenti—Global Office of Research and Foresight. Innocenti Report Card 19: Child Well-Being in an Unpredictable World; UNICEF: Florence, Italy, 2025; Available online: https://www.unicef.org/innocenti/reports/child-well-being-unpredictable-world (accessed on 19 June 2025).
- Biswas, T.; Townsend, N.; Huda, M.M.; Maravilla, J.; Begum, T.; Pervin, S.; Ghosh, A.; Mahumud, R.A.; Islam, S.; Anwar, N.; et al. Prevalence of Multiple Non-Communicable Diseases Risk Factors among Adolescents in 140 Countries: A Population-Based Study. EClinicalMedicine 2022, 53, 101591. [Google Scholar] [CrossRef] [PubMed]
- Dau, L.; Barros, P.; Cilliers, E.J.; Hemsley, B.; Martin, M.; Lakhanpaul, M.; Smith, M. Urban Density and Child Health and Wellbeing: A Scoping Review of the Literature. Health Place 2025, 91, 103393. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Global Strategy for Women’s, Children’s and Adolescents’ Health (2016–2030): Early Childhood Development. Report by the Director-General; WHO: Geneva, Switzerland, 2018; Available online: https://iris.who.int/bitstream/handle/10665/276426/A71_19Rev1-ru.pdf?sequence=1&isAllowed=y (accessed on 19 June 2025).
- World Health Organization (WHO). Adolescent and Young Adult Health: Risks and Solutions. Available online: https://www.who.int/news-room/fact-sheets/detail/adolescents-health-risks-and-solutions (accessed on 19 June 2025).
- UNICEF Office of Research—Innocenti. Innocenti Report Card 19: Child Well-Being in an Unpredictable World; UNICEF: Florence, Italy, 2025. [Google Scholar]
- World Health Organization (WHO). Noncommunicable Diseases; WHO: Geneva, Switzerland, 2024. [Google Scholar]
- Critsina, O.P.; Trankovskaya, L.V.; Semaniv, E.V.; Lisetskaya, E.A. Factors Forming the Health of Modern Children and Adolescents. Pac. Med. J. 2020, 3, 19–24. (In Russian) [Google Scholar] [CrossRef]
- Martsev, A.A. Comprehensive Analysis of Disease Incidence and Children’s Health Risk Assessment at the Regional Level. Zdorov’e Naseleniya I Sreda Obitaniya 2023, 31, 46–53. (In Russian) [Google Scholar] [CrossRef]
- Polunina, N.V.; Buslaeva, G.N.; Golukhov, G.N.; Polunin, V.S.; Kostenko, E.V.; Ashanina, N.M.; Bespalyuk, G.N.; Tyazhelnikov, A.A.; Shindryaeva, N.N.; Pavlova, S.V.; et al. (Eds.) Population Health: Methods for Its Study and Evaluation; Pirogov Russian National Research Medical University: Moscow, Russia, 2020; Available online: https://rsmu.ru/fileadmin/templates/DOC/Faculties/PF/Oziz_dept/MP_Zdorove_naselenija.pdf (accessed on 19 June 2025).
- Aubakirova, Z.S.; Alekseenko, A.N.; Stolyarova, E.O.; Krasnobaeva, N.L.; Omirzak, T.E. Demographic Security of Kazakhstan: Potential, Risks and Prospects; Media Alliance: Ust-Kamenogorsk, Kazakhstan, 2022; p. 515. Available online: https://www.ektu.kz/files/Altaytanu/pub/Mono/2022_02/Демoграфическая_безoпаснoсть_книга_25.01.2023.pdf (accessed on 19 June 2025).
- Ng, K.; Adayeva, A.; Abdrakhmanova, S.; Whiting, S.; Williams, J.; Slazhnyova, T.; Kaussova, G. Patterns and Trajectories of Inequality in Physical Activity from Childhood to Adolescence in Kazakhstan. Prev. Med. Rep. 2024, 42, 102729. [Google Scholar] [CrossRef]
- Xiao, Y.; Mann, J.J.; Chow, J.C.C.; Brown, T.T.; Snowden, L.R.; Yip, P.S.F.; Tsai, A.C.; Hou, Y.; Pathak, J.; Wang, F.; et al. Patterns of Social Determinants of Health and Child Mental Health, Cognition, and Physical Health in a U.S. Cohort. JAMA Pediatr. 2023, 177, 1294–1305. [Google Scholar] [CrossRef]
- Mbogori, T.; Kimmel, K.; Zhang, M.; Kandiah, J.; Wang, Y. Nutrition Transition and Double Burden of Malnutrition in Africa: A Case Study of Four Selected Countries with Different Social Economic Development. AIMS Public Health 2020, 7, 425–439. [Google Scholar] [CrossRef]
- Oladeji, O.E.; Aja-Nwachuku, A.G.; Ekeoha, C.E.; Zainab, O.; Chukwu, B.D.; Okoye, C.U. Double Burden of Malnutrition: A Narrative Review of Its Drivers and Mitigation Strategies in Urban Settings. EAS Journal of Nutrition and Food Sciences 2025, 7, 5. [Google Scholar] [CrossRef]
- Rachmi, C.N.; Li, M.; Baur, L.A. Overweight and Obesity in Indonesia: A Systematic Review of the Literature. Asia Pac. J. Clin. Nutr. 2021, 30, 177–190. [Google Scholar] [CrossRef]
- Nel, J.H.; Steyn, N.P. The Nutrition Transition and the Double Burden of Malnutrition in Sub-Saharan African Countries: How Do These Countries Compare with the Recommended LANCET COMMISSION Global Diet? Int. J. Environ. Res. Public Health 2022, 19, 16791. [Google Scholar] [CrossRef]
- Popkin, B.M.; Reardon, T. Obesity and the Food System Transformation in Latin America. Obes. Rev. 2018, 19, 1028–1064. [Google Scholar] [CrossRef]
- Committee on the Rights of the Child. Report on the Situation of Children in the Republic of Kazakhstan in 2022; Committee on the Rights of the Child: Astana, Kazakhstan, 2023; p. 186. Available online: https://www.gov.kz/uploads/2023/11/1/b8ee69921eeadb84f1e65a983f8689a3_original.4360246.pdf (accessed on 19 June 2025).
- Committee on Statistics of the Ministry of National Economy of the Republic of Kazakhstan. Children of Kazakhstan: Statistical Yearbook; Committee on Statistics: Astana, Kazakhstan, 2023; p. 126. Available online: https://stat.gov.kz/upload/iblock/816/u1yx5oz6pa89ejra0j64jzjou0gwmn75/%D0%A1-18-%D0%93-2018-2022%20(%D1%80%D1%83%D1%81).pdf (accessed on 19 June 2025).
- Tretyakova, S.N.; Tursun, A.O.; Khabieva, T.N.; Davydenko, M.V.; Kurtyukova, M. Trends in Primary Morbidity in the Republic of Kazakhstan. Actual Probl. Theor. Clin. Med. 2020, 2, 37–41. (In Russian) [Google Scholar]
- Ministry of Health of the Republic of Kazakhstan. Instruction on Coding of Morbidity and Mortality According to the International Statistical Classification of Diseases and Related Health Problems, 10th Revision (ICD-10). Order No. 258/2020 of 11 December 2020; Registered on 15 December 2020. Available online: https://adilet.zan.kz/rus/docs/V2000021769 (accessed on 21 June 2025).
- Doku, D.T.; Neupane, S. Double Burden of Malnutrition: Increasing Overweight and Obesity and Stalled Underweight Trends among Ghanaian Women. Int. J. Environ. Res. Public Health 2021, 18, 7000. [Google Scholar] [CrossRef] [PubMed]
- Khajieva, G.; Omir, A. Problems of Socio-Economic Development of Kazakhstan’s Regions in the Context of Adaptation to the Sustainable Development. Econ. Strategy Pract. 2020, 15, 175–186. (In Russian) [Google Scholar] [CrossRef]
- Jia, M.; Zhen, L.; Xiao, Y. Changing Food Consumption and Nutrition Intake in Kazakhstan. Nutrients 2022, 14, 326. [Google Scholar] [CrossRef]
- Spankulova, L.; Chulanova, Z.; Konyrbay, A. Evaluating Healthcare Accessibility in Kazakhstan: Urban and Rural Perspectives. Eurasian J. Econ. Bus. Stud. 2024, 68, 5–19. [Google Scholar] [CrossRef]
- Ministry of Health of the Republic of Kazakhstan. Health of the Population of the Republic of Kazakhstan and the Activities of Health Care Organizations for 2013–2023; Ministry of Health of the Republic of Kazakhstan: Astana, Kazakhstan, 2023. [Google Scholar]
- Bureau of National Statistics of the Agency for Strategic Planning and Reforms of the Republic of Kazakhstan. Available online: https://stat.gov.kz/en (accessed on 19 June 2025).
- Ministry of Health of the Republic of Kazakhstan. On Amendments to the Order of the Minister of Health of the Republic of Kazakhstan Dated March 6, 2013, No. 128 On Approval of Forms Intended for the Collection of Administrative Data from Healthcare Entities. Registered in the Ministry of Justice of the Republic of Kazakhstan. Available online: https://adilet.zan.kz/rus/docs/V1700014953 (accessed on 7 August 2025).
- Ministry of Health of the Republic of Kazakhstan. On Approval of the Methodology for the Formation (Calculation) of Indicators in the Field of Healthcare. Order of the Minister of Health of the Republic of Kazakhstan dated November 30, 2020, No. ҚР DSM-212/2020. Registered with the Ministry of Justice of the Republic of Kazakhstan on November 30, 2020, No. 21698. Available online: https://adilet.zan.kz/rus/docs/V2000021698 (accessed on 7 August 2025).
- Bureau of National Statistics. Agency for Strategic Planning and Reforms of the Republic of Kazakhstan. Statistics for Children Portal. Available online: https://bala.stat.gov.kz (accessed on 7 August 2025).
- Remy, L.L.; Clay, T.; Oliva, G. Do We Have a Linear Trend? A Beginner’s Approach to Analysis of Trends in Community Health Indicators; University of California: San Francisco, CA, USA, 2005; Available online: http://www.ucsf.edu/fhop (accessed on 19 June 2025).
- Safiri, S.; Kolahi, A.A.; Noori, M.; Nejadghaderi, S.A.; Karamzad, N.; Bragazzi, N.L.; Sullman, M.J.M.; Abdollahi, M.; Collins, G.S.; Kaufman, J.S.; et al. Burden of Anemia and Its Underlying Causes in 204 Countries and Territories, 1990–2019: Results from the Global Burden of Disease Study 2019. J. Hematol. Oncol. 2021, 14, 185. [Google Scholar] [CrossRef]
- Sharif, N.; Neyazi, A.; Khatib, M.N.; Baldaniya, L.; Ballal, S.; Kavita, V.; Maharana, L.; Arya, R.; Bushi, G.; Shabil, M.; et al. Anemia in Asian Children: Trends in the Prevalence, Etiology and Analysis of Geographic Inequalities. World J. Pediatr. 2025, 21, 396–405. [Google Scholar] [CrossRef]
- Behera, D.K.; Rahut, D.B.; Tripathy, S.; Negi, S. Burden and Causes of Anemia in Vietnam: Insights from the Global Burden of Disease Data. BMC Public Health 2024, 24, 3026. [Google Scholar] [CrossRef]
- Oktarina, C.; Dilantika, C.; Sitorus, N.L.; Basrowi, R.W. Relationship Between Iron Deficiency Anemia and Stunting in Pediatric Populations in Developing Countries: A Systematic Review and Meta-Analysis. Children 2024, 11, 1268. [Google Scholar] [CrossRef]
- Mantadakis, E.; Chatzimichael, E.; Zikidou, P. Iron Deficiency Anemia in Children Residing in High and Low-Income Countries: Risk Factors, Prevention, Diagnosis and Therapy. Mediterr. J. Hematol. Infect. Dis. 2020, 12, e2020041. [Google Scholar] [CrossRef] [PubMed]
- Flora, R.; Zulkarnain, M.; Fajar, N.A.; Jasmine, A.B.; Yuliana, I.; Tanjung, R.; Sulaiman, S.; Putra, S.A.; Martini, S.; Aguscik, A. Factors Associated with Iron Deficiency in Elementary School Children. Open Access Maced. J. Med. Sci. 2022, 10, 97–100. [Google Scholar] [CrossRef]
- Zhang, K.; Kan, C.; Han, F.; Zhang, J.; Ding, C.; Guo, Z.; Huang, N.; Zhang, Y.; Hou, N.; Sun, X. Global, Regional, and National Epidemiology of Diabetes in Children from 1990 to 2019. JAMA Pediatr. 2023, 177, 837–846. [Google Scholar] [CrossRef] [PubMed]
- Cioana, M.; Deng, J.; Nadarajah, A.; Hou, M.; Qiu, Y.; Chen, S.S.J.; Rivas, A.; Toor, P.P.; Banfield, L.; Thabane, L.; et al. Global Prevalence of Diabetic Retinopathy in Pediatric Type 2 Diabetes: A Systematic Review and Meta-Analysis. JAMA Netw. Open 2023, 6, e231887. [Google Scholar] [CrossRef]
- Kushwaha, S.; Srivastava, R.; Bhadada, S.K.; Khanna, P. Prevalence of Pre-Diabetes and Diabetes among School-Age Children and Adolescents of India: A Brief Report. Diabetes Res. Clin. Pract. 2023, 202, 110738. [Google Scholar] [CrossRef]
- Hong, Y.H.; Chung, I.H.; Han, K.; Chung, S.; Taskforce Team of the Obesity Fact Sheet of the Korean Society for the Study of Obesity. Prevalence of Type 2 Diabetes Mellitus among Korean Children, Adolescents, and Adults Younger than 30 Years: Changes from 2002 to 2016. Diabetes Metab. J. 2022, 46, 297–306. [Google Scholar] [CrossRef]
- Lawrence, J.M.; Divers, J.; Isom, S.; Saydah, S.; Imperatore, G.; Pihoker, C.; Marcovina, S.M.; Mayer-Davis, E.J.; Hamman, R.F.; Dolan, L.; et al. Trends in Prevalence of Type 1 and Type 2 Diabetes in Children and Adolescents in the US, 2001–2017. JAMA 2021, 326, 717–727. [Google Scholar] [CrossRef]
- Stahl-Pehe, A.; Kamrath, C.; Prinz, N.; Kapellen, T.; Menzel, U.; Kordonouri, O.; Schwab, K.O.; Bechtold-Dalla Pozza, S.; Rosenbauer, J.; Holl, R.W. Prevalence of Type 1 and Type 2 Diabetes in Children and Adolescents in Germany from 2002 to 2020: A Study Based on Electronic Health Record Data from the DPV Registry. J. Diabetes 2022, 14, 840–850. [Google Scholar] [CrossRef]
- Bendor, C.D.; Bardugo, A.; Pinhas-Hamiel, O.; Afek, A.; Twig, G. Cardiovascular Morbidity, Diabetes and Cancer Risk among Children and Adolescents with Severe Obesity. Cardiovasc. Diabetol. 2020, 19, 79. [Google Scholar] [CrossRef]
- AlKuwari, M.; Soliman, A.; Elsiddig, S.; Alaaraj, N.; Hamed, N.; Alyafei, F.; AlHumaidi, N. Impact of iron deficiency anemia on growth and endocrine functions: Reversibility with treatment. Endocr. Abstr. 2025, 110, EP1060. [Google Scholar] [CrossRef]
- Khatiwada, S.; Gelal, B.; Baral, N.; Lamsal, M. Association between iron status and thyroid function in Nepalese children. Thyroid Res. 2016, 9, 2. [Google Scholar] [CrossRef] [PubMed]
- Huang, X.; Mao, M.; Guo, T.; Wu, Y.; Xu, Q.; Dai, J.; Huang, Y. Iron Status, Thyroid Dysfunction, and Iron Deficiency Anemia: A Two-Sample Mendelian Randomization Study. Ann. Nutr. Metab. 2024, 80, 295–306. [Google Scholar] [CrossRef] [PubMed]
- Calcaterra, V.; Cena, H.; Bolpagni, F.; Taranto, S.; Vincenti, A.; Madini, N.; Diotti, M.; Quatrale, A.; Zuccotti, G. The Interplay Between Iron Metabolism and Insulin Resistance: A Key Factor in Optimizing Obesity Management in Children and Adolescents. Nutrients 2025, 17, 1211. [Google Scholar] [CrossRef]
- Nurmadieva, G.T.; Zhetpisbaev, B.A. Influence of the Ecosystem on Human Health in the Industrial Developed Regions of Kazakhstan: A Literature Review. Sci. Healthc. 2018, 20, 86–107. (In Russian) [Google Scholar]
- Unerbaeva, R.; Kupeshova, S.; Kusmoldayeva, Z.; Тaszharganov, S. Differentiation of Regions of the Republic of Kazakhstan by Living Standard. KazUEFIT Herald 2024, 3, 94–102. (In Russian) [Google Scholar]
- Pigarova, E.A.; Vorotnikova, S.Y. Human Resources Problems of the Endocrinological Service and Strategies for Their Solution. Probl. Endocrinol. 2021, 67, 8–10. (In Russian) [Google Scholar] [CrossRef]
- Harrison, W.N.; Mittal, V.S.; O’Toole, J.K.; Quinonez, R.A.; Mink, R.; Leyenaar, J.K. Child Health Needs and the Pediatric Hospital Medicine Workforce: 2020–2040. Pediatrics 2024, 153 (Suppl. 2), e2023063678M. [Google Scholar] [CrossRef]
| Region | IDA | DM | ENMD | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Annual Average Change | CI (Lower; Upper) | p-Value | Annual Average Change | CI (Lower; Upper) | p-Value | Annual Average Change | CI (Lower; Upper) | p-Value | |
| Kazakhstan | −285.52 | −360.73; −210.31 | <0.001 | 0.84 | 0.77; 1.60 | <0.05 | −75.68 | −96.00; −55.37 | <0.001 |
| Akmola | −122.47 | −209.17; −35.77 | <0.05 | −0.06 | −1.72 | 0.94 | −21.41 | −34.01; −8.80 | <0.01 |
| Aktobe | −324.92 | −418.31; −231.53 | <0.001 | 0.33 | −1.24; 1.89 | 0.64 | −129.33 | −159.26; −99.41 | <0.001 |
| Almaty | −97.72 | −499.48; 304.04 | 0.59 | 1.09 | −0.56; 2.74 | 0.17 | −41.97 | −115.73; 31.79 | 0.23 |
| Atyrau | −22.57 | −106.04; 60.89 | 0.56 | 0.79 | 0.39; 1.19 | <0.01 | −19.40 | −33.19; −5.61 | <0.05 |
| West Kazakhstan | −28.75 | −79.44; 21.95 | 0.23 | 0.71 | −0.29; 1.71 | 0.14 | −20.17 | −32.39; −7.94 | <0.01 |
| Zhambyl | −357.01 | −472.67; −241.35 | <0.001 | 2.21 | 0.99; 3.42 | <0.01 | −49.02 | −84.55; −13.49 | <0.05 |
| Karaganda | −192.48 | −221.33; −163.62 | <0.001 | 1.41 | −0.50; 3.32 | 0.01 | 15.48 | −19.28; 50.23 | 0.34 |
| Kostanay | −105.25 | −141.13; −69.36 | <0.001 | 0.59 | −0.43; 1.61 | 0.22 | −56.82 | −101.13; −12.52 | <0.05 |
| Kyzylorda | −462.8 | −581.97; −343.55 | <0.001 | 2.38 | 1.49; 3.27 | <0.001 | −65.90 | −148.09; 16.29 | 0.10 |
| Mangistau | −307.8 | −495.98; −119.56 | <0.01 | −0.10 | −0.93; 0.73 | 0.79 | −15.55 | −179.66; 148.56 | 0.83 |
| South Kazakhstan | −591.3 | −1007.96; −174.56 | <0.05 | −2.13 | −5.41; 1.15 | 0.18 | −165.24 | −234.82; −95.66 | <0.001 |
| Pavlodar | −249.90 | −317.0; −182.78 | <0.01 | 2.25 | 0.97; 3.53 | <0.01 | −132.05 | −181.57; −82.52 | <0.001 |
| North Kazakhstan | −173.59 | −197.5; −149.59 | <0.001 | 1.37 | −0.64; 5.37 | 0.11 | −85.11 | −130.08; −40.14 | <0.01 |
| East Kazakhstan | −173.59 | −197.5; −149.59 | <0.001 | 1.68 | −0.10; 3.47 | 0.06 | −54.10 | −86.05; −22.15 | <0.01 |
| Astana | −148.08 | −208.43; −87.72 | <0.001 | 1.96 | 0.22; 3.69 | <0.05 | −22.34 | −201.81; 157.13 | 0.79 |
| Almaty city | −69.69 | −128.69; −10.67 | <0.05 | 0.19 | −0.14; 0.51 | 0.23 | −274.13 | −378.49; −169.78 | <0.001 |
| Region | IDA | DM | ENMD | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Annual Average Change | CI (Lower; Upper) | p-Value | Annual Average Change | CI (Lower; Upper) | p-Value | Annual Average Change | CI (Lower; Upper) | p-Value | |
| Kazakhstan | −305.39 | −336.96; −273.82 | <0.001 | 1.67 | 0.26; 3.07 | <0.05 | −153.92 | −192.11; −115.73 | <0.001 |
| Akmola | −200.46 | −315.68; −85.23 | <0.01 | −1.03 | −3.42; 1.36 | 0.35 | −138.43 | −218.21; −58.66 | <0.01 |
| Aktobe | −748.51 | −908.32; −588.70 | <0.01 | 2.35 | −1.43; 6.13 | 0.19 | −619.9 | −751.98; −487.77 | <0.001 |
| Almaty | −214.78 | −423.48; −6.09 | <0.05 | 5.91 | −2.02; 13.83 | 0.13 | −349.6 | −691.98; −7.29 | <0.05 |
| Atyrau | −118.13 | −300.32; 64.06 | 0.18 | 0.71 | −0.99; 2.41 | 0.37 | 10.06 | −47.42; 67.53 | 0.70 |
| West Kazakhstan | 22.75 | −10.61; 56.11 | 0.16 | 0.43 | −1.16; 2.04 | 0.55 | 24.33 | 8.22; 40.44 | <0.01 |
| Zhambyl | −243.16 | −335.94; −150.39 | <0.001 | 1.39 | −0.44; 3.23 | 0.12 | −7.33 | −149.11; 134.46 | 0.91 |
| Karaganda | −98.34 | −120.29; −76.39 | <0.001 | 2.37 | −1.41; 6.14 | 0.19 | 55.76 | 23.69; 87.83 | <0.01 |
| Kostanay | −373.85 | −532.2; −215.41 | <0.001 | −0.28 | −4.14; 3.59 | 0.88 | −83.71 | −134.88; −32.55 | <0.01 |
| Kyzylorda | −264.68 | −474.59; −54.78 | <0.05 | 5.72 | 1.04; 10.39 | <0.05 | −287.7 | −558.93; −16.55 | <0.05 |
| Mangistau | −801.52 | −972.23; −630.79 | <0.001 | 3.31 | −2.17; 8.79 | 0.21 | −80.82 | −211.43; 49.79 | 0.19 |
| South Kazakhstan | −548.20 | −964.99; −131.42 | <0.05 | −1.86 | −4.71; 0.99 | 0.17 | −123.1 | −207.96; −38.32 | <0.01 |
| Pavlodar | −148.93 | −224.88; −72.99 | <0.01 | 2.75 | −1.42; 6.92 | 0.17 | −420.2 | −527.48; −313.02 | <0.001 |
| North Kazakhstan | −102.98 | −142.16; −63.80 | <0.001 | 9.64 | 2.41; 16.86 | 0.012 | −57.19 | −142.23; 27.85 | 0.16 |
| East Kazakhstan | −249.73 | −304.28; −195.18 | <0.001 | −0.63 | −4.47; 3.20 | 0.71 | −158.47 | −311.10; −5.85 | <0.05 |
| Astana | −258.1 | −547.96; 3.18 | 0.07 | 2.29 | −0.73; 5.33 | 0.12 | −88.44 | −289.54; 112.68 | 0.35 |
| Almaty city | −381.56 | −539.02; −224.09 | <0.001 | −0.68 | −1.96; 0.60 | 0.26 | −297.35 | −502.05; −92.66 | <0.01 |
| Variables | Mean | Minimum | Maximum | Std. Deviation |
|---|---|---|---|---|
| incidence of IDA in children 0–14 years of age in urban areas (per 100,000 population) | 2396.8744 | 253.00 | 7421.10 | 1704.34813 |
| incidence of IDA in adolescents 15–17 years old in urban areas (per 100,000 population) | 2526.1010 | 111.40 | 9957.60 | 1972.51857 |
| incidence of endocrine system diseases, nutritional and metabolic disorders in children 0–14 years of age in urban areas (per 100,000 population) | 1047.8030 | 112.70 | 3911.20 | 738.54446 |
| incidence of ENMD in adolescents 15–17 years of age in urban areas (per 100,000 population) | 2196.8884 | 163.30 | 8234.90 | 1447.70057 |
| incidence of DM in children 0–14 years of age in urban areas (per 100,000 population) | 16.5477 | 2.50 | 60.90 | 9.46182 |
| incidence of DM in adolescents 15–17 years old in urban areas (per 100,000 population) | 23.6471 | 0.00 | 166.70 | 22.54657 |
| Variables | Mean | Minimum | Maximum | Std. Deviation |
|---|---|---|---|---|
| The average share of the urban population with incomes below the subsistence minimum, % | 2.46 | 1.20 | 4.10 | 1.25 |
| Gini coefficient quantifies income inequality on a scale from 0 (perfect equality) to 1 (maximum inequality) | 0.24 | 0.16 | 0.32 | 0.04 |
| The average household monetary expenditures per capita, in thousands KZT | 55.20 | 22.63 | 12.14 | 20.70 |
| Household income used for consumption by region, thousand KZT | 57.16 | 24.13 | 12.14 | 20.63 |
| The average per capita food expenditures, in thousands KZT | 13.18 | 3.44 | 33.38 | 6.41 |
| The number of specialized therapists | 16.20 | 6.10 | 30.60 | 5.13 |
| The average number of general practitioners per 10,000 urban population | 5.80 | 1.80 | 10.90 | 1.64 |
| The average number of endocrinologists | 0.60 | 0.20 | 1.40 | 0.22 |
| The average number of pediatricians | 3.84 | 2.10 | 8.10 | 1.06 |
| Number of organizations with children’s outpatient departments and offices per 1000 population | 107.29 | 7.00 | 1337.00 | 220.08 |
| The availability of pediatricians (including neonatologists) for the 0–14 age group per 1000 children | 0.82 | 0.19 | 2.65 | 0.41 |
| The average availability of pediatric hospital beds of all profiles for the 0–14 age group per 1000 children | 3.99 | 1.91 | 8.01 | 1.16 |
| Predictor | B | Std. Error | Sig. | 95.0% Confidence Interval for B | R2 | |
|---|---|---|---|---|---|---|
| Lower Bound | Upper Bound | |||||
| Incidence of IDA in children 0–14 years of age in urban areas (per 100,000 population) | ||||||
| The average per capita food expenditures, in thousands KZT | −203.452 | 22.250 | 0.000 | −253.785 | −153.120 | 0.903 |
| Incidence of IDA in adolescents 15–17 years of age in urban areas (per 100,000 population) | ||||||
| The average per capita food expenditures, in thousands KZT | −215.967 | 10.450 | 0.000 | −239.608 | −192.327 | 0.979 |
| Incidence of endocrine system diseases, nutritional and metabolic disorders in children 0–14 years of age in urban areas (per 100,000 population) | ||||||
| The average number of pediatricians | 890.987 | 70.120 | 0.000 | 732.364 | 1049.609 | 0.947 |
| Incidence of endocrine system diseases, nutritional and metabolic disorders in adolescents 15–17 years of age in urban areas (per 100,000 population) | ||||||
| The number of specialized therapists | 603.730 | 64.459 | 0.000 | 455.088 | 752.372 | 0.950 |
| The average number of general practitioners per 10,000 urban population | 801.574 | 319.884 | 0.037 | 63.920 | 1539.228 | |
| Incidence of DM in children 0–14 years of age in urban areas (per 100,000 population) | ||||||
| The average household monetary expenditures per capita, in thousands KZT | 0.489 | 0.092 | 0.001 | 0.000 | 0.001 | 0.844 |
| The average number of general practitioners per 10,000 urban population | 5.259 | 1.504 | 0.008 | 1.791 | 8.727 | |
| Incidence of DM in adolescents 15–17 years of age in urban areas (per 100,000 population) | ||||||
| Household income used for consumption by region, thousand KZT | 0.379 | 0.038 | 0.000 | 0.289 | 0.469 | 0.960 |
| The average availability of pediatric hospital beds of all profiles for the 0–14 age group per 1000 children | 19.314 | 2.677 | 0.000 | 12.985 | 25.644 | |
| The average number of endocrinologists | 56.508 | 14.876 | 0.007 | 21.332 | 91.683 | |
| Tolerance > 10; VIF < 4 | ||||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rogova, S.; Plotnikova, O.; Kalishev, M.; Nukeshtayeva, K.; Bolatova, Z.; Galayeva, A. Diabetes, Iron-Deficiency Anemia, and Endocrine, Nutritional, and Metabolic Disorders in Children: A Socio-Epidemiological Study in Urban Kazakhstan. Int. J. Environ. Res. Public Health 2025, 22, 1346. https://doi.org/10.3390/ijerph22091346
Rogova S, Plotnikova O, Kalishev M, Nukeshtayeva K, Bolatova Z, Galayeva A. Diabetes, Iron-Deficiency Anemia, and Endocrine, Nutritional, and Metabolic Disorders in Children: A Socio-Epidemiological Study in Urban Kazakhstan. International Journal of Environmental Research and Public Health. 2025; 22(9):1346. https://doi.org/10.3390/ijerph22091346
Chicago/Turabian StyleRogova, Svetlana, Olga Plotnikova, Marat Kalishev, Karina Nukeshtayeva, Zhanerke Bolatova, and Aza Galayeva. 2025. "Diabetes, Iron-Deficiency Anemia, and Endocrine, Nutritional, and Metabolic Disorders in Children: A Socio-Epidemiological Study in Urban Kazakhstan" International Journal of Environmental Research and Public Health 22, no. 9: 1346. https://doi.org/10.3390/ijerph22091346
APA StyleRogova, S., Plotnikova, O., Kalishev, M., Nukeshtayeva, K., Bolatova, Z., & Galayeva, A. (2025). Diabetes, Iron-Deficiency Anemia, and Endocrine, Nutritional, and Metabolic Disorders in Children: A Socio-Epidemiological Study in Urban Kazakhstan. International Journal of Environmental Research and Public Health, 22(9), 1346. https://doi.org/10.3390/ijerph22091346









