Knowledge, Attitudes, and Practices of Artisanal and Small-Scale Miners regarding Tuberculosis, Human Immunodeficiency Virus, and Silicosis in Zimbabwe
Abstract
1. Introduction
2. Methods
2.1. Study Design
2.2. General Setting
2.3. Specific Setting
2.4. Screening for TB/HIV and Silicosis
2.5. Mobilization of ASMs for WBS
2.6. Study Population
2.7. Sampling Procedure
2.8. Data Variables, Sources of Data, and Data Collection
2.9. Data Analysis
2.10. Ethical Approval
3. Results
4. Knowledge, Attitudes, and Practices Regarding HIV, TB, and Silicosis among ASMs
4.1. Knowledge about HIV, TB, and Silicosis
4.2. Attitudes and Practices among ASMs regarding HIV, TB, and Silicosis
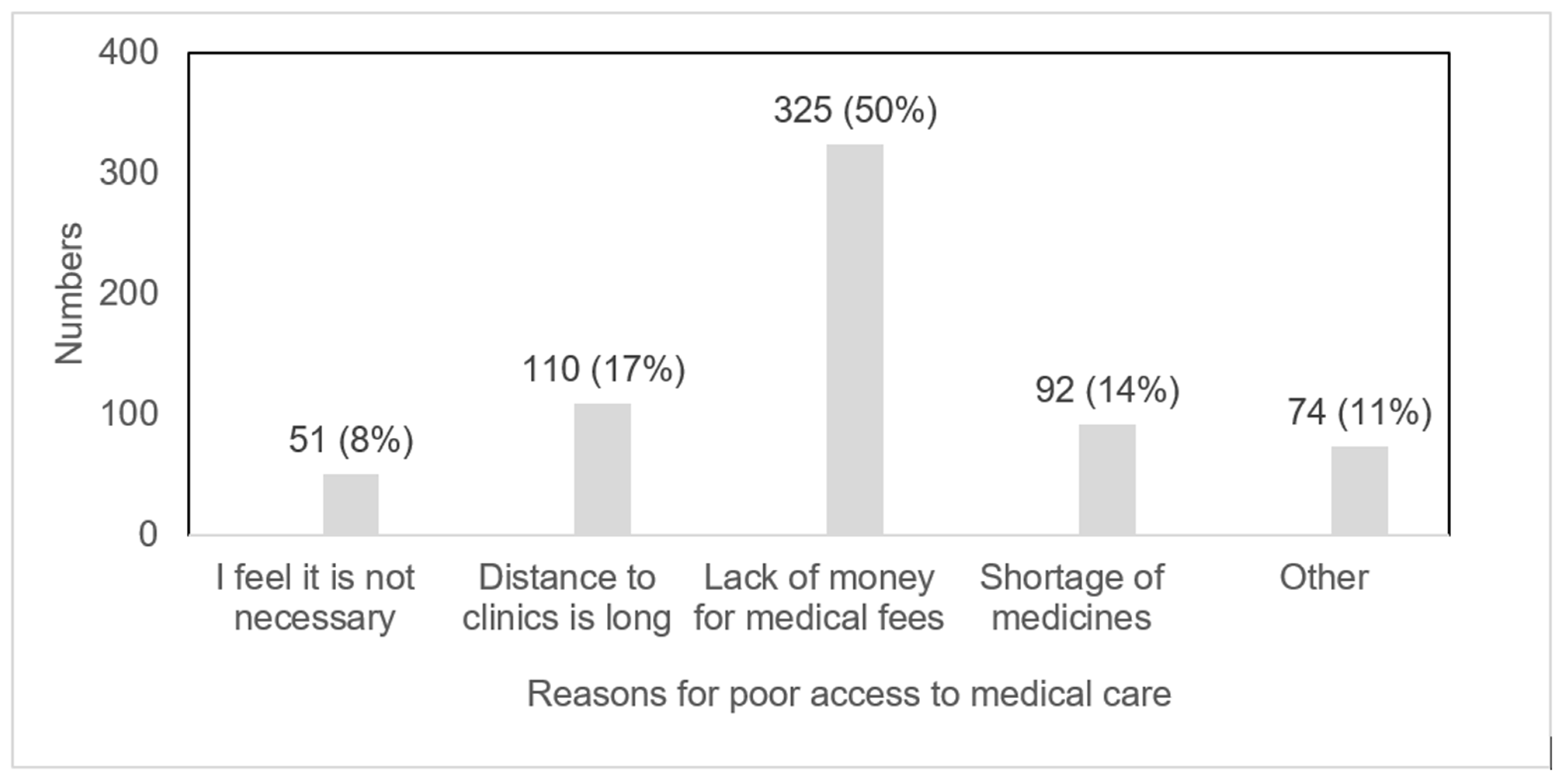
4.3. Key Challenges in Accessing Medical Care
4.4. Possibilities of Reducing TB, HIV, and Silicosis among ASMs
5. Discussion
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Fritz, M.; McQuilken, J.; Collins, N.; Weldegiorgis, F. Global Trends in Artisanal and Small-Scale Mining (ASM): A Review of Key Numbers and Issues; International Institute for Sustainable Development: Winnipeg, MB, Canada, 2018. [Google Scholar]
- EPRM Case study Intel; The European Partnership for Responsible Minerals: The Hague, The Netherlands, 2023.
- Hilson, G.; McQuilken, J.; Perks, R. State of the Artisanal and Small-Scale Mining Sector Acknowledgments and Key Contributors; DELVE: Boston, MA, USA, 2019; pp. 1–98. [Google Scholar]
- Maendelo Diamonds. Maendeleo Diamond Standards TM. 2023, pp. 1–6. Available online: https://www.resolve.ngo/maendeleo_diamond_standards.htm (accessed on 1 October 2023).
- Ledwaba, P.; Nhlengetwa, K. When policy is not enough: Prospects and challenges of artisanal and small-scale mining in South Africa. J. Sustain. Dev. Law Policy 2016, 7, 25. [Google Scholar] [CrossRef]
- Weldegiorgis, F.; Lawson, L.; Verbrugge, H. Women in Artisanal and Small-Scale Mining: Challenges and Opportunities for Greater Participation; IISD: Winnipeg, MB, Canada, 2018. [Google Scholar]
- Hilson, G.; McQuilken, J. Four decades of support for artisanal and small-scale mining in sub-Saharan Africa: A critical review. Extr. Ind. Soc. 2014, 1, 104–118. [Google Scholar] [CrossRef]
- African Minerals Development Centre. Zimbabwe Artisanal and Small Scale Mining Profile. 2023. Available online: https://knowledge.uneca.org/asm/zimbabwe (accessed on 2 November 2023).
- PACT. A Golden Opportunity: A Scoping Study of Artisanal and Small Scale Gold Mining in Zimbabwe. Twenty-First Century Schools; PACT Institute: Washington, DC, USA, 2015; pp. 73–89. [Google Scholar]
- Sibanda, M.B.; Mathe, B. Alternative Livelihoods: Small Scale Mining in Hope Fountain, Umguza Rural District, Zimbabwe. Int. J. Multidiscip. Res. Growth Eval. 2021, 2, 205–213. [Google Scholar]
- USAID. Artisanal and Small-scale Mining_LandLinks. 2021. Available online: https://www.land-links.org/issue/artisanal-and-small-scale-mining/ (accessed on 20 October 2023).
- Landrigan, P.; Bose-O’Reilly, S.; Elbel, J.; Nordberg, G.; Lucchini, R.; Bartrem, C.; Grandjean, P.; Mergler, D.; Moyo, D.; Nemery, B.; et al. Reducing disease and death from Artisanal and Small-Scale Mining (ASM)-the urgent need for responsible mining in the context of growing global demand for minerals and metals for climate change mitigation. Environ. Health 2022, 21, 78. [Google Scholar] [CrossRef]
- Richard, M.; Moher, P.; Telmer, K. Health in Artisanal and Small-Scale; Artisanal Gold Council: Victoria, BC, Canada, 2015. [Google Scholar]
- Matamala Pizarro, J.; Aguayo Fuenzalida, F. Mental health in mine workers: A literature review. Ind. Health 2021, 59, 343–370. [Google Scholar] [CrossRef]
- GoContractor. Why Mental Health Matters in Mining_Online Training. 2017. Available online: https://gocontractor.com/blog/mental-health-matters-mining/ (accessed on 20 October 2023).
- Han, B.; Yan, B.; Zhang, J.; Zhao, N.; Sun, J.; Li, C.; Lei, X.; Liu, H.; Chen, J. The influence of the social support on symptoms of anxiety and depression among patients with silicosis. Sci. World J. 2014, 2014, 724804. [Google Scholar] [CrossRef][Green Version]
- Balmes, J.R.; Ladou, J.; Harrison, R.J. Current occupational and environmental medicine. In Proceedings of the 20th USENIX Security Symposium, San Francisco, CA, USA, 8–12 August 2011; pp. 395–410. [Google Scholar]
- PEPFAR. Zimbabwe Population-Based HIV Impact Assessment Zimphia 2020 Key Findings. 2020. Available online: https://zw.usembassy.gov/national-hiv-survey-zimphia-2020-results-indicate-zimbabwe-is-on-track-to-achieve-hiv-epidemic-control-by-2030/ (accessed on 20 August 2023).
- Moyo, D.; Ncube, R.; Kavenga, F.; Chikwava, L.; Mapuranga, T.; Chiboyiwa, N.; Chimunhu, C.; Mudzingwa, F.; Muzvidziwa, O.; Ncube, P.; et al. The Triple Burden of Tuberculosis, Human Immunodeficiency Virus and Silicosis among Artisanal and Small-Scale Miners in Zimbabwe. Int. J. Environ. Res. Public Health 2022, 19, 13822. [Google Scholar] [CrossRef]
- Knight, D.; Ehrlich, R.; Fielding, K.; Jeffery, H.; Grant, A.; Churchyard, G. Trends in silicosis prevalence and the healthy worker effect among gold miners in South Africa: A prevalence study with follow up of employment status Environmental health. BMC Public Health 2015, 15, 1258. [Google Scholar] [CrossRef] [PubMed]
- Ehrlich, R.; Akugizibwe, P.; Siegfried, N.; Rees, D. The association between silica exposure, silicosis and tuberculosis: A systematic review and meta-analysis. BMC Public Health 2021, 21, 953. [Google Scholar] [CrossRef]
- Nyavaya, K. Zimbabwe’s Rugged Artisanal and Small-Scale Mining Sector. 2022. Available online: https://apo.org.au/node/316751 (accessed on 24 October 2023).
- The Union Zimbabwe Trust. Kunda-Nqob’i TB; The Union of Zimbabwe Trust: Harare, Zimbabwe, 2022. [Google Scholar]
- Sibanda, M. (4) Holding a Mirror for Artisanal and Small-Scale Mining Taxation Challenges in Zimbabwe_LinkedIn. 2021. Available online: https://www.linkedin.com/pulse/holding-mirror-artisanal-small-scale-mining-taxation-zimbabwe/ (accessed on 25 August 2023).
- Katova, L. 2022 Population and Housing Census. Preliminary Report. 2022. Available online: https://zimbabwe.opendataforafrica.org/anjlptc/2022-population-housing-census-preliminary (accessed on 15 October 2023).
- Food and Agriculture Organization of the United Nations. Fertilizer Use by Crop in Zimbabwe; Food and Agriculture Organization of the United Nations: Rome, Italy, 2006; Available online: https://www.fao.org/3/a0395e/a0395e06.htm (accessed on 27 August 2023).
- Mwandiringana, E.; Ye, J. Mining what is not mine: Artisanal gold mining in Gwanda, Zimbabwe. Extr. Ind. Soc. 2023, 13, 101217. [Google Scholar] [CrossRef]
- Tunatazama-Community Monitors. Gwanda_Small Scale Mining a Blessing and A Curse-Tunatazama-Community Monitors. Available online: https://communitymonitors.net/2018/06/7105/ (accessed on 15 August 2023).
- The Chronicle Breaking News. Gwanda Residents Irked by Hookers Working from Home. 2021. Available online: https://www.chronicle.co.zw/gwanda-residents-irked-by-hookers-working-from-home/ (accessed on 15 August 2023).
- Moyo, D.; Zishiri, C.; Ncube, R.; Madziva, G.; Sandy, C.; Mhene, R.; Siziba, N.; Kavenga, F.; Moyo, F.; Muzvidziwa, O.; et al. Tuberculosis and Silicosis Burden in Artisanal and Small-Scale Gold Miners in a Large Occupational Health Outreach Programme in Zimbabwe. Environ. Res. Public Health 2021, 18, 11031. [Google Scholar] [CrossRef]
- Ahadzi, D.F. Awareness of adverse health effects of silica dust exposure among stone quarry workers in Ghana. Preprints 2021, 0171119931. [Google Scholar]
- Dixit, R.; Kuldeep, R.; Goyal, M.; Agarwal, D.; Jalutharia, J. Sociodemographic profile, work practices, and disease awareness among stone mine workers having silicosis from Central Rajasthan. Lung India Off. Organ Indian Chest Soc. 2023, 40, 117–122. [Google Scholar] [CrossRef] [PubMed]
- Gottesfeld, P.; Andrew, D.; Dalhoff, J. Silica Exposures in Artisanal Small-Scale Gold Mining in Tanzania and Implications for Tuberculosis Prevention. J. Occup. Environ. Hyg. 2015, 12, 647–653. [Google Scholar] [CrossRef] [PubMed]
- Mabe, F.N. Small-scale mining policies in Ghana: Miners’ knowledge, attitudes and practices. Resour. Policy 2023, 85, 103924. [Google Scholar] [CrossRef]
- Ralph, O.; Gilles, N.; Fon, N.; Luma, H.; Greg, N. Impact of artisanal gold mining on human health and the environment in the Batouri Gold District, East Cameroon. Acad. J. Interdiscip. Stud. 2018, 7, 25–44. [Google Scholar] [CrossRef]
- Guidelines for HIV Prevention, Testing and Treatment of HIV in Zimbabwe. The AIDS and TB Directorate, Ministry of Health and Child Care, Zimbabwe, AUGUST 2022. Available online: https://www.prepwatch.org/wp-content/uploads/2023/08/Guidelines-for-HIV-Prevention-Testing-and-Treatment-of-HIV-in-Zimbabwe-August-2022.pdf (accessed on 20 August 2023).
- Zimbabwe National Tuberculosis and Leprosy Management Programs, 5th ed. May 2023. Available online: https://uzt.org.zw/wp-content/uploads/2023/11/Zimbabwe-National-TB-guidelines.pdf (accessed on 20 August 2023).
- Podewils, L.J.; Long, E.F.; Fuller, T.J.; Mwakazanga, D.; Kapungu, K.; Tembo, M.; Mwanza, S.; Curran, K.G.; Smith, J.P.; Tobias, J.L.; et al. Zambia Assessment of Tuberculosis (TB) and HIV in the Mines (ZATHIM): Implications for programs and policies. BMC Public Health 2022, 22, 791. [Google Scholar] [CrossRef]
- Nguyen, V.; Thu, H.N.T.; Le Thi, H.; Ngoc, A.N.; Van, D.K.; Thi, Q.P.; Nhu, N.T.; Thanh, T.N.; Quoc, D.N.; Mai, H.P.T.; et al. Knowledge, Attitude, and Practices (KAP) on Silicosis Among High-Risk Worker Population in Five Provinces in Vietnam. In Proceedings of the International Conference on Innovations for Sustainable and Responsible Mining, Hanoi, Vietnam, 15–17 October 2020; Springer: Berlin/Heidelberg, Germany, 2021; Volume 109, pp. 469–484. [Google Scholar]
- Nandi, S.; Burnase, N.; Barapatre, A.; Gulhane, P.; Dhatrak, S. Assessment of Silicosis Awareness among Stone Mine Workers of Rajasthan State. Indian J. Occup. Environ. Med. 2018, 22, 97–100. [Google Scholar]
- Girdler-Brown, B.V.; White, N.W.; Ehrlich, R.I.; Churchyard, G.J. The burden of silicosis, pulmonary tuberculosis and COPD among former Basotho goldminers. Am. J. Ind. Med. 2008, 51, 640–647. [Google Scholar] [CrossRef]
- Souza, T.P.; Watte, G.; Gusso, A.M.; Souza, R.; da Moreira, J.S.; Knorst, M.M. Silicosis prevalence and risk factors in semi-precious stone mining in Brazil. Am. J. Ind. Med. 2017, 60, 529–536. [Google Scholar] [CrossRef]
- Siabi, E.K.; Donkor, P.; Mensah, S.K.; Dzane, R.K.; Kurantin, N.; Frimpong, K.; Siabi, S.E.; Vuu, C.; van Etten, E. Assessing the knowledge and practices of occupational safety and health in the artisanal and small-scale gold mining sector of Ghana: A case of obuasi. Heliyon 2022, 8, e11464. [Google Scholar] [CrossRef] [PubMed]
- Khaji, R.A.; Kabwebwe, V.M.; Mringo, A.G.; Nkwabi, T.F.; Bigio, J.; Mergenthaler, C.; Aguilera, V.N.; Pande, T.; Rahman, M.T.; Haraka, F. Factors affecting motivation among key populations to engage with tuberculosis screening and testing services in northwest tanzania: A mixed-methods analysis. Int. J. Environ. Res. Public Health 2021, 18, 9654. [Google Scholar] [CrossRef] [PubMed]
- Knowledge, Attitudes and Practises (KAP) on TB, HIV and Silicosis Among Key Populations Aged 15 and 59 years in Southern Africa. Select Research. Available online: https://www.timssa.co.za/Documents/Studies/KAP%20Study%20-%20Select%20Research.pdf (accessed on 20 October 2023).
- McMichael, A.J. Standardized mortality ratios and the “healthy worker effect”: Scratching beneath the surface. J. Occup. Med. 1976, 18, 165–168. [Google Scholar] [CrossRef] [PubMed]
| Characteristic | Number ((%) §) | |
|---|---|---|
| Sex | Male | 602 (92) |
| Female | 43 (7) | |
| Not recorded | 7 (1) | |
| Age category in years | <20 | 34 (5) |
| 20–24 | 102 (16) | |
| 25–34 | 236 (36) | |
| 35–44 | 167 (26) | |
| ≥45 | 101 (15) | |
| Not recorded | 12 (2) | |
| Level of education | None | 37 (6) |
| Primary | 104 (16) | |
| Secondary | 454 (70) | |
| Tertiary | 45 (7) | |
| Not recorded | 12 (1) | |
| District of operation | Gwanda | 362 (56) |
| Chirumhanzu | 236 (36) | |
| Gweru | 54 (8) | |
| Years as a miner (n = 609) | <5 | 262 (43) |
| 5–9.9 | 169 (28) | |
| ≥10 | 178 (29) |
| Characteristic | No (%) ⁑ | Yes (%) ⁑ | I Don’t Know (%) ⁑ |
|---|---|---|---|
| TB can be cured (n = 633) | 18 (3) | 504 (80) | 111 (17) |
| Dust generated during mining can cause TB | 30 (5) | 571 (88) | 50 (8) |
| HIV increase chances of contracting TB | 73 (11) | 340 (52) | 236 (36) |
| ASM have higher risk of getting TB compared to general population | 40 (6) | 564 (87) | 48 (7) |
| Silica dust causes permanent and incurable lung disease (n = 650) | 81 (13) | 382 (59) | 187 (29) |
| Silicosis can be transmitted from one person to the other (n = 648) | 192 (30) | 224 (35) | 232 (36) |
| The risk of getting TB is low in ASMs | 332 (51) | 226 (35) | 89 (14) |
| Use of a piece of cloth to cover one’s mouth and nose is a good way to prevent dust inhalation. | 189 (29) | 434 (67) | 28 (4) |
| Drinking milk or juice clears dust in the lungs and prevents TB. | 135 (21) | 434 (67) | 82 (13) |
| Characteristic | No (%) ⁑ | Yes (%) ⁑ | I Don’t Know (%) |
|---|---|---|---|
| It is crucial for ASMs to have yearly tests for TB, HIV, OLDs | 6 (1) | 625 (96) | 21 (3) |
| It is necessary to buy special respirators to prevent dust inhalation | 29 (4) | 595 (91) | 28 (4) |
| Wearing a respirator, not a piece of cloth during mining, is good. | 28 (4) | 574 (88) | 48 (8) |
| It is important for ASMs to always have access to condoms. | 50 (8) | 584 (90) | 16 (2) |
| It is possible to reduce HIV, TB, and silicosis in mining. | 68 (11) | 475 (73) | 106 (16) |
| It is important to always seek medical treatment when one is not feeling well. | 15 (2) | 620 (97) | 7 (1) |
| I would participate if TB, HIV, and silicosis screening services were brought to mining sites. | 14 (2) | 620 (97) | 6 (1) |
| Characteristic | Number (%) § | |
|---|---|---|
| Method for preventing dust inhalation (n = 646) | Nothing | 117 (18) |
| A piece of cloth | 447 (69) | |
| Special respirators | 82 (13) | |
| Frequency of use of cloth or respirator (n = 532) | Rarely | 53 (10) |
| Sometimes | 231 (43) | |
| Most of the times | 89 (17) | |
| Every time | 159 (30) | |
| Use water to suppress dust (n = 645) | Never | 322 (50) |
| Sometimes | 186 (29) | |
| Most of the times | 53 (8) | |
| Every time | 84 (13) | |
| Condom use during sex outside home (n = 628) | Never | 85 (14) |
| Sometimes | 141 (23) | |
| Most of the times | 97 (15) | |
| Every time | 305 (49) | |
| I seek medical care whenever I am sick (n = 649) | Yes | 480 (74) |
| No | 169 (26) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Moyo, D.; Kavenga, F.; Ncube, R.T.; Macheri, F.P.; Mando, T.C.; Moyo, F.; Muzvidziwa, O.; Ncube, M.; Masvingo, H.; Chigaraza, B.; et al. Knowledge, Attitudes, and Practices of Artisanal and Small-Scale Miners regarding Tuberculosis, Human Immunodeficiency Virus, and Silicosis in Zimbabwe. Int. J. Environ. Res. Public Health 2023, 20, 7116. https://doi.org/10.3390/ijerph20237116
Moyo D, Kavenga F, Ncube RT, Macheri FP, Mando TC, Moyo F, Muzvidziwa O, Ncube M, Masvingo H, Chigaraza B, et al. Knowledge, Attitudes, and Practices of Artisanal and Small-Scale Miners regarding Tuberculosis, Human Immunodeficiency Virus, and Silicosis in Zimbabwe. International Journal of Environmental Research and Public Health. 2023; 20(23):7116. https://doi.org/10.3390/ijerph20237116
Chicago/Turabian StyleMoyo, Dingani, Fungai Kavenga, Ronald Thulani Ncube, Farai Peter Macheri, Tariro Christwish Mando, Florence Moyo, Orippa Muzvidziwa, Mpokiseng Ncube, Hellen Masvingo, Blessings Chigaraza, and et al. 2023. "Knowledge, Attitudes, and Practices of Artisanal and Small-Scale Miners regarding Tuberculosis, Human Immunodeficiency Virus, and Silicosis in Zimbabwe" International Journal of Environmental Research and Public Health 20, no. 23: 7116. https://doi.org/10.3390/ijerph20237116
APA StyleMoyo, D., Kavenga, F., Ncube, R. T., Macheri, F. P., Mando, T. C., Moyo, F., Muzvidziwa, O., Ncube, M., Masvingo, H., Chigaraza, B., Nyambo, A., Mangwanya, A., Mwale, R. N., Mazadza, T., Magidi, T., Benny, G., Ndudzo, C., Kandido, V. V., Mutungamiri, K., & Timire, C. (2023). Knowledge, Attitudes, and Practices of Artisanal and Small-Scale Miners regarding Tuberculosis, Human Immunodeficiency Virus, and Silicosis in Zimbabwe. International Journal of Environmental Research and Public Health, 20(23), 7116. https://doi.org/10.3390/ijerph20237116






