The Relationship between Wellbeing, Self-Determination, and Resettlement Stress for Asylum-Seeking Mothers Attending an Ecosocial Community-Based Intervention: A Mixed-Methods Study
Abstract
:1. Introduction
1.1. Aims
1.2. Self-Efficacy and Basic Psychological Needs Theory
1.2.1. Self-Efficacy
1.2.2. Basic Psychological Needs Theory
1.3. Adaptive Stress
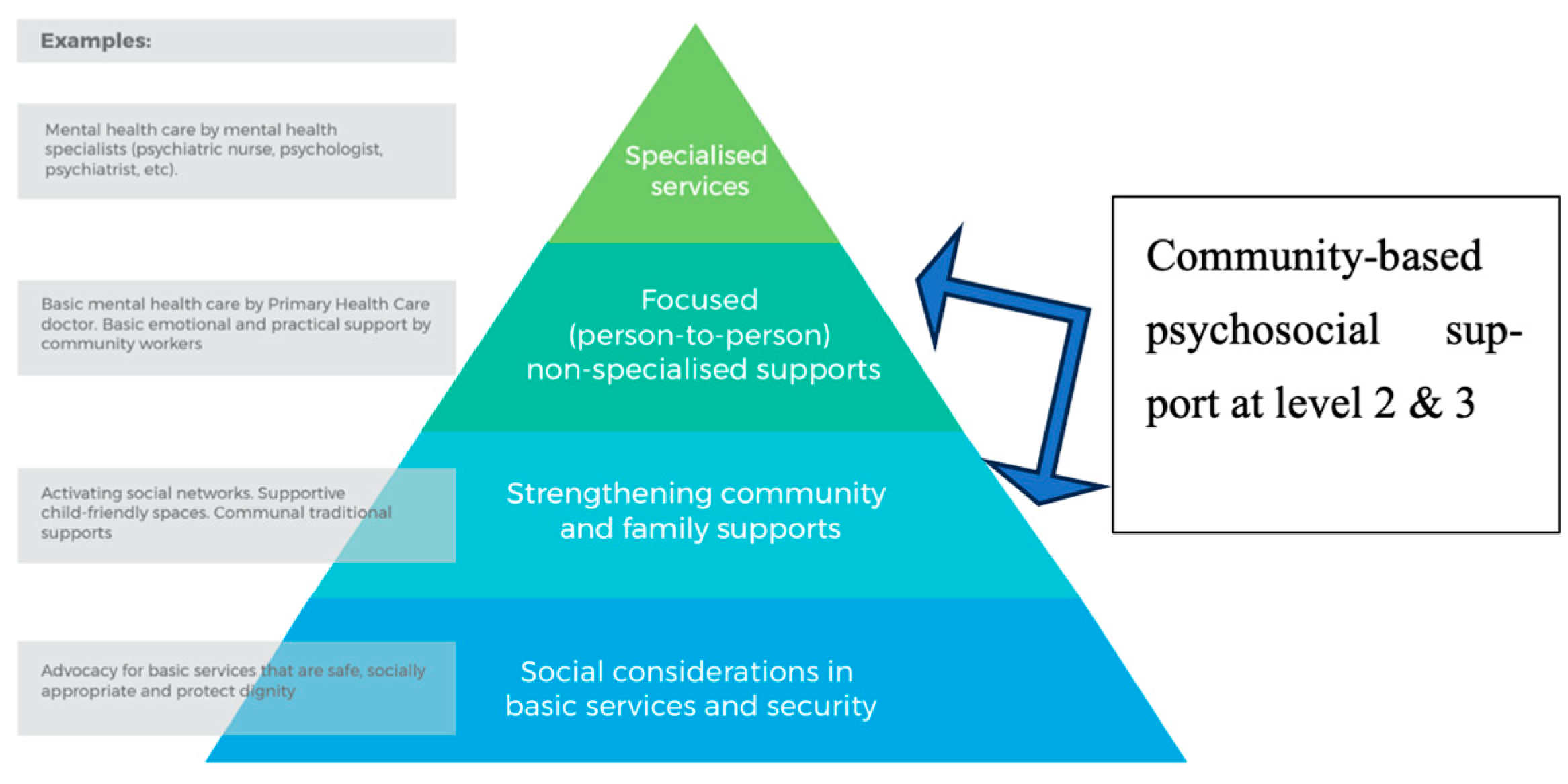
1.4. Community-Based Psychosocial Support
1.5. Research Objectives
2. Methods
2.1. Study Design and Sample
2.2. Measurements
2.3. Data Analysis
3. Results
3.1. Quantitative Results
3.2. Qualitative Results
3.3. Community and Relatedness
3.3.1. Bonding with Other Asylum Seekers
When I speak up, she says I feel what you feel. [….] It’s necessary for people like us who don’t know anybody […] to meet people who are in the same situation as you.
3.3.2. Connection with Service Providers
People I didn’t know approached me, it’s wonderful to feel that wow, I have people around me. I’m not alone. People who are going to make it easier for me to fit in, I’m not just another commodity, just another object. One more workforce. I am a person who is considered.
3.4. Competence and Empowerment
Wrong information made [claimants think] there is no door open for me […] in this country [… and] they got depressed [that] way. […. So having access to] information gives me the strength that I’m not alone, there is a supporter.
[This activity] allowed me to shed the weight that I’ve been carrying since [my country of origin] [because] it forced me in a conscious way to let [my pre-migration experience] stay in the past, and to then be equipped to start my life here in Canada with a clear idea of where I want to go.
3.5. Enhanced Wellbeing
You find a person who comes to dance in front of you with full of energy. You’ll ask yourself: Can I dance too? And that’s when you realize that yes, there are moments in life where you can tolerate. […] You don’t just have to cry. You can let go.
[The workshop] takes my mind off the current reality a little bit, I forget about the woman [crying] on the floor and I think about something else […] This is the only place where I smile.
You are tied in a house, no activities, […] you don’t do anything. So when I [was] at home the next day [after the workshop], I put some music, I try moving my body. […] I feel relief. I feel happy [and] I check my blood pressure, it was normal. So like, I see it is my stress. Whenever I’m working since that day, like if I want to clean up my apartment or trying to settle some things, I just put on the music.
4. Discussion
4.1. Need Satisfaction as Predictor of Wellbeing
4.2. Frequent Program Attendance May Enhance Wellbeing
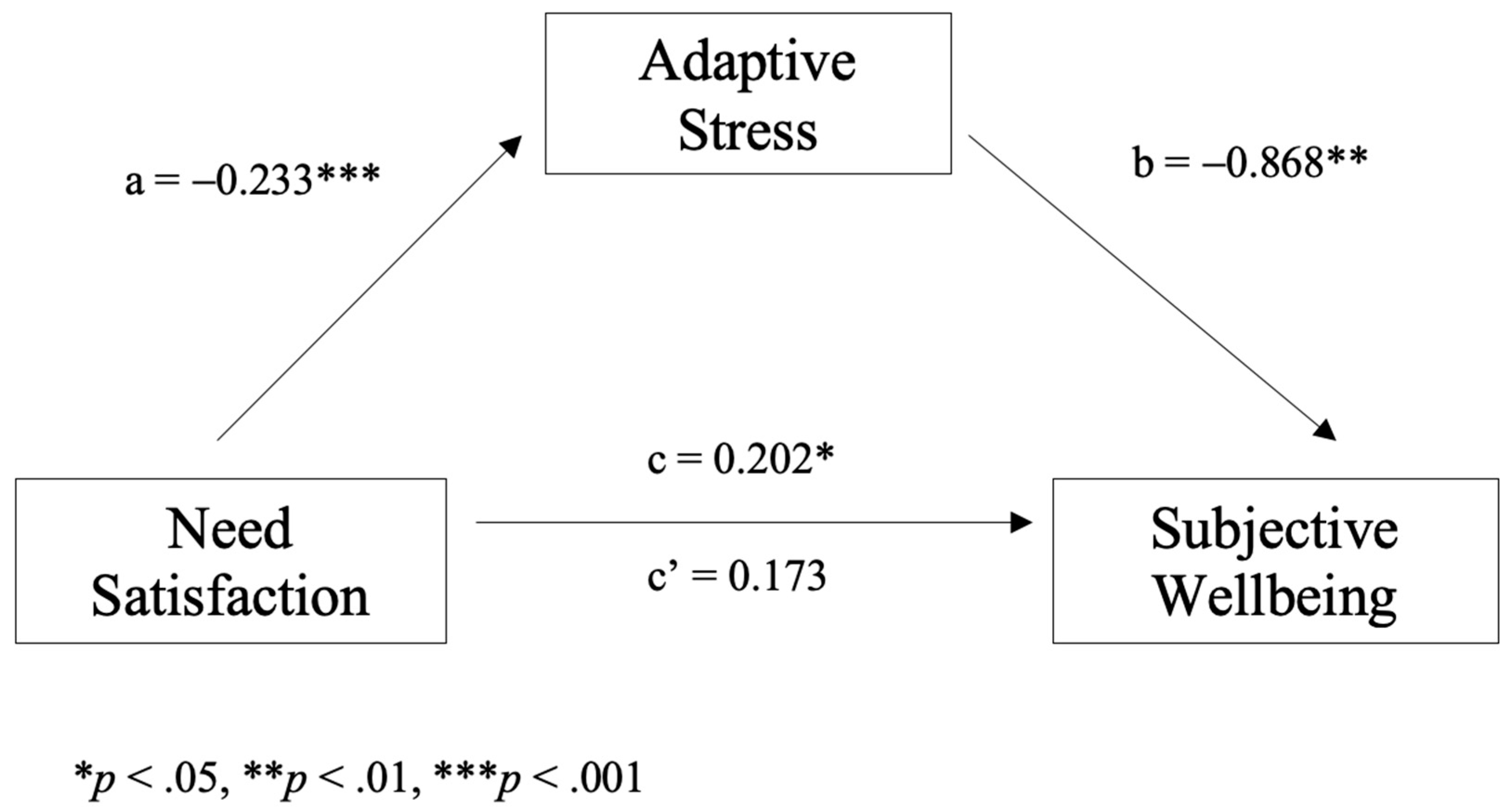
4.3. Mediating Effect of Adaptive Stress
4.4. Qualitative Findings
4.5. Limitations
4.6. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Newnham, E.A.; Pearman, A.; Olinga-Shannon, S.; Nickerson, A. The mental health effects of visa insecurity for refugees and people seeking asylum: A latent class analysis. Int. J. Public Health 2019, 64, 763–772. [Google Scholar] [CrossRef] [PubMed]
- Steel, Z.; Momartin, S.; Silove, D.; Coello, M.; Aroche, J.; Tay, K.W. Two year psychosocial and mental health outcomes for refugees subjected to restrictive or supportive immigration policies. Soc. Sci. Med. 2011, 72, 1149–1156. [Google Scholar] [CrossRef]
- Merry, L.; Pelaez, S.; Edwards, N.C. Refugees, asylum-seekers and undocumented migrants and the experience of parenthood: A synthesis of the qualitative literature. Glob. Health 2017, 13, 75. [Google Scholar] [CrossRef] [PubMed]
- Zivot, C.; Dewey, C.; Heasley, C.; Srinivasan, S.; Little, M. Exploring the State of Gender-Centered Health Research in the Context of Refugee Resettlement in Canada: A Scoping Review. Int. J. Environ. Res. Public Health 2020, 17, 7511. [Google Scholar] [CrossRef] [PubMed]
- Shaw, S.A.; Funk, M. A Systematic Review of Social Service Programs Serving Refugees. Res. Soc. Work. Pract. 2019, 29, 847–862. [Google Scholar] [CrossRef]
- Bandura, A. Human agency in social cognitive theory. Am. Psychol. 1989, 44, 1175. [Google Scholar] [CrossRef]
- Ryan, R.M.; Deci, E.L. Self-Determination Theory: Basic Psychological Needs in Motivation, Development, and Wellness; Guilford Publications: New York, NY, USA, 2017. [Google Scholar]
- Vansteenkiste, M.; Ryan, R.M. On psychological growth and vulnerability: Basic psychological need satisfaction and need frustration as a unifying principle. J. Psychother. Integr. 2013, 23, 263. [Google Scholar] [CrossRef]
- Benight, C.C.; Bandura, A. Social cognitive theory of posttraumatic recovery: The role of perceived self-efficacy. Behav. Res. Ther. 2004, 42, 1129–1148. [Google Scholar] [CrossRef]
- Luszczynska, A.; Gutiérrez-Doña, B.; Schwarzer, R. General self-efficacy in various domains of human functioning: Evidence from five countries. Int. J. Psychol. 2005, 40, 80–89. [Google Scholar] [CrossRef]
- Schwarzer, R.; Jerusalem, M. Generalized self-efficacy scale. In Measures in Health Psychology: A User’s Portfolio. Causal and Control Beliefs; Weinman, J., Wright, S., Johnston, M., Eds.; NFER-Nelson: Slough, UK, 1995; Volume 35, p. 37. [Google Scholar]
- Sulaiman-Hill, C.M.R.; Thompson, S.C. Learning to Fit in: An Exploratory Study of General Perceived Self Efficacy in Selected Refugee Groups. J. Immigr. Minor. Health 2013, 15, 125–131. [Google Scholar] [CrossRef]
- Tip, L.K.; Brown, R.; Morrice, L.; Collyer, M.; Easterbrook, M.J. Believing is achieving: A longitudinal study of self-efficacy and positive affect in resettled refugees. J. Ethn. Migr. Stud. 2020, 46, 3174–3190. [Google Scholar] [CrossRef]
- Pak, Ş.; Yurtbakan, T.; Acarturk, C. Social Support and Resilience among Syrian Refugees: The Mediating Role of Self-Efficacy. J. Aggress. Maltreatment Trauma 2022, 32, 382–398. [Google Scholar] [CrossRef]
- Yang, M.M. A Study of Self-Efficacy in a Group of Hmong Refugees. Master’s Thesis, Smith College, Northampton, MA, USA, 2014. [Google Scholar]
- Alharbi, B.H.M. Psychological Security And Self-Efficacy Among Syrian Refugee Students Inside And Outside The Camps. J. Int. Educ. Res. 2017, 13, 59–68. [Google Scholar] [CrossRef]
- Deci, E.L.; Ryan, R.M. The “What” and “Why” of Goal Pursuits: Human Needs and the Self-Determination of Behavior. Psychol. Inq. 2000, 11, 227–268. [Google Scholar] [CrossRef]
- Richey, M.; Brooks, J.; Ravishankar, M. Building self-determination of disadvantaged groups: Insights from an entrepreneurship focused program for refugees. Int. J. Entrep. Behav. Res. 2022. ahead of print. [Google Scholar] [CrossRef]
- Turan, N.; İpekçi, B.; Yılmaz, M.Y. Self-Determination and Psychological Adaptation in Forcibly Displaced People. N. Engl. J. Public Policy 2019, 31, 11. [Google Scholar]
- Lera, M.-J.; Abualkibash, S. Basic Psychological Needs Satisfaction: A Way to Enhance Resilience in Traumatic Situations. Int. J. Environ. Res. Public Health 2022, 19, 6649. [Google Scholar] [CrossRef] [PubMed]
- Yeung, N.C.Y.; Lu, Q.; Wong, C.C.Y.; Huynh, H.C. The roles of needs satisfaction, cognitive appraisals, and coping strategies in promoting posttraumatic growth: A stress and coping perspective. Psychol. Trauma Theory Res. Pract. Policy 2016, 8, 284. [Google Scholar] [CrossRef] [PubMed]
- Weinstein, N.; Khabbaz, F.; Legate, N. Enhancing need satisfaction to reduce psychological distress in Syrian refugees. J. Consult. Clin. Psychol. 2016, 84, 645–650. [Google Scholar] [CrossRef] [PubMed]
- Alkire, S. Subjective Quantitative Studies of Human Agency. Soc. Indic. Res. 2005, 74, 217–260. [Google Scholar] [CrossRef]
- Silove, D. The ADAPT model: A conceptual framework for mental health and psychosocial programming in post conflict settings. Intervention 2013, 11, 237–248. [Google Scholar] [CrossRef]
- Chase, L.E.; Rousseau, C. Ethnographic case study of a community day center for asylum seekers as early stage mental health intervention. Am. J. Orthopsychiatry 2018, 88, 48–58. [Google Scholar] [CrossRef] [PubMed]
- Tay, A.K.; Rees, S.; Tam, N.; Kareth, M.; Silove, D. Developing a measure of adaptive stress arising from the psychosocial disruptions experienced by refugees based on a sample of displaced persons from West Papua. Int. J. Methods Psychiatr. Res. 2019, 28, e1770. [Google Scholar] [CrossRef] [PubMed]
- van Heemstra, H.E.; Scholte, W.F.; Nickerson, A.; Boelen, P.A. Can circumstances be softened? Self-efficacy, post-migratory stressors, and mental health among refugees. Int. J. Environ. Res. Public Health 2021, 18, 1440. [Google Scholar] [CrossRef]
- Cogo, A.; Inman, S.; McCormack, P.; Rogers, M. Stories from lockdown: The impact of the Covid19 pandemic on the well-being of clients at Southwark Day Centre for Asylum Seekers (SDCAS). 2021. Available online: https://openresearch.lsbu.ac.uk/item/8wwv0 (accessed on 17 January 2022).
- Sanchez, J. Thriving Together: A Scoping Review of Interventions to Improve Refugee Social Capital and Health in Wellesley Junior Fellowship Report. 2016. Available online: https://www.wellesleyinstitute.com/wp-content/uploads/2016/10/Thriving-Together.pdf (accessed on 20 April 2023).
- Spring, H.C.; Howlett, F.K.; Connor, C.; Alderson, A.; Antcliff, J.; Dutton, K.; Gray, O.; Hirst, E.; Jabeen, Z.; Jamil, M.; et al. The value and meaning of a community drop-in service for asylum seekers and refugees. Int. J. Migr. Health Soc. Care 2019, 15, 31–45. [Google Scholar] [CrossRef]
- Yalim, A.C.; Kim, I. Mental health and psychosocial needs of Syrian refugees: A literature review and future directions. Adv. Soc. Work 2018, 18, 833–852. [Google Scholar] [CrossRef]
- Slewa-Younan, S.; Blignault, I.; Renzaho, A.M.; Doherty, M. Community-Based Mental Health and Wellbeing Support for Refugees. 2018. Available online: https://www.saxinstitute.org.au/wp-content/uploads/Community-based-mental-health-and-wellbeing-support-for-refugees_FINAL.pdf (accessed on 20 April 2023).
- World Health Organization (WHO). Mental Health Promotion and Mental Health Care in Refugees and Migrants: Technical Guidance. 2018. Available online: https://www.euro.who.int/en/publications/abstracts/mental-health-promotion-and-mental-health-care-in-refugees-and-migrants-2018 (accessed on 18 January 2023).
- Inter-Agency Standing Committee. Mental Health and Psychosocial Support in Humanitarian Emergencies: What Should Protection Programme Managers Know? Inter-Agency Standing Committee: Geneva, Switzerland, 2010; Available online: https://interagencystandingcommittee.org/system/files/legacy_files/MHPSS%20Protection%20Actors.pdf (accessed on 18 October 2023).
- Krieger, N. Methods for the Scientific Study of Discrimination and Health: An Ecosocial Approach. Am. J. Public Health 2012, 102, 936–944. [Google Scholar] [CrossRef]
- Ahmed, A.; Stewart, D.E.; Teng, L.; Wahoush, O.; Gagnon, A.J. Experiences of immigrant new mothers with symptoms of depression. Arch. Womens Ment. Health 2008, 11, 295–303. [Google Scholar] [CrossRef]
- Khanlou, N.; Haque, N.; Skinner, A.; Mantini, A.; Kurtz Landy, C. Scoping review on maternal health among immigrant and refugee women in Canada: Prenatal, intrapartum, and postnatal care. J. Pregnancy 2017, 8783294. [Google Scholar] [CrossRef]
- Reynolds, B.; White, J. Seeking asylum and motherhood: Health and wellbeing needs. Community Pract. 2010, 83, 20–23. [Google Scholar]
- Rezazadeh, M.S.; Hoover, M.L. Women’s experiences of immigration to Canada: A review of the literature. Can. Psychol. Can. 2018, 59, 76–88. [Google Scholar] [CrossRef]
- Gagnon, A.J.; Carnevale, F.; Mehta, P.; Rousseau, H.; Stewart, D.E. Developing population interventions with migrant women for maternal-child health: A focused ethnography. BMC Public Health 2013, 13, 471. [Google Scholar] [CrossRef] [PubMed]
- Gewalt, S.C.; Berger, S.; Ziegler, S.; Szecsenyi, J.; Bozorgmehr, K. Psychosocial health of asylum seeking women living in state-provided accommodation in Germany during pregnancy and early motherhood: A case study exploring the role of social determinants of health. PLoS ONE 2018, 13, e0208007. [Google Scholar] [CrossRef]
- Hawkins, M.M.; Schmitt, M.E.; Adebayo, C.T.; Weitzel, J.; Olukotun, O.; Christensen, A.M.; Ruiz, A.M.; Gilman, K.; Quigley, K.; Dressel, A.; et al. Promoting the health of refugee women: A scoping literature review incorporating the social ecological model. Int. J. Equity Health 2021, 20, 45. [Google Scholar] [CrossRef]
- Russo, A.; Lewis, B.; Joyce, A.; Crockett, B.; Luchters, S. A qualitative exploration of the emotional wellbeing and support needs of new mothers from Afghanistan living in Melbourne, Australia. BMC Pregnancy Childbirth 2015, 15, 197. [Google Scholar] [CrossRef]
- Green, C.A.; Duan, N.; Gibbons, R.D.; Hoagwood, K.E.; Palinkas, L.A.; Wisdom, J.P. Approaches to Mixed Methods Dissemination and Implementation Research: Methods, Strengths, Caveats, and Opportunities. Adm. Policy Ment. Health Ment. Health Serv. Res. 2015, 42, 508–523. [Google Scholar] [CrossRef]
- Diener, E.; Emmons, R.A.; Larsen, R.J.; Griffin, S. The satisfaction with life scale. J. Personal. Assess. 1985, 49, 71–75. [Google Scholar] [CrossRef] [PubMed]
- Emmons, R.A.; Diener, E. Personality Correlates of Subjective Well-Being. Pers. Soc. Psychol. Bull. 1985, 11, 89–97. [Google Scholar] [CrossRef]
- Luhmann, M.; Krasko, J.; Terwiel, S. Subjective well-being as a dynamic construct. In The Handbook of Personality Dynamics and Processes; Elsevier: Amsterdam, The Netherlands, 2021; pp. 1231–1249. [Google Scholar]
- Sheldon, K.M.; Elliot, A.J.; Kim, Y.; Kasser, T. Whats satisfying about satisfying events? Comparing ten candidate psychological needs. J. Personal. Soc. Psychol. 2001, 80, 325–339. [Google Scholar] [CrossRef] [PubMed]
- Holding, A.; Fortin, J.-A.; Carpentier, J.; Hope, N.; Koestner, R. Letting Go of Gold: Examining the Role of Autonomy in Elite Athletes’ Disengagement from Their Athletic Careers and Well-Being in Retirement. J. Clin. Sport Psychol. 2018, 14, 88–108. [Google Scholar] [CrossRef]
- Braun, V.; Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef]
- Stewart, M.; Anderson, J.; Beiser, M.; Mwakarimba, E.; Neufeld, A.; Simich, L.; Spitzer, D. Multicultural Meanings of Social Support among Immigrants and Refugees. Int. Migr. 2008, 46, 123–159. [Google Scholar] [CrossRef]
- Aubé, T.; Pisanu, S.; Merry, L. La Maison Bleue: Strengthening resilience among migrant mothers living in Montreal, Canada. PLoS ONE 2019, 14, e0220107. [Google Scholar] [CrossRef] [PubMed]
- Stewart, M.; Simich, L.; Shizha, E.; Makumbe, K.; Makwarimba, E. Supporting African refugees in Canada: Insights from a support intervention. Health Soc. Care Community 2012, 20, 516–527. [Google Scholar] [CrossRef] [PubMed]
- Nannestad, P.; Svendsen, G.L.H.; Svendsen, G.T. Bridge Over Troubled Water? Migration and Social Capital. J. Ethn. Migr. Stud. 2008, 34, 607–631. [Google Scholar] [CrossRef]
- Beiser, M.; Hou, F. Predictors of positive mental health among refugees: Results from Canada’s General Social Survey. Transcult. Psychiatry 2017, 54, 675–695. [Google Scholar] [CrossRef]
- Cargo, M.; Mercer, S.L. The Value and Challenges of Participatory Research: Strengthening Its Practice. Annu. Rev. Public Health 2008, 29, 325–350. [Google Scholar] [CrossRef]
- Mitschke, D.B.; Praetorius, R.T.; Kelly, D.R.; Small, E.; Kim, Y.K. Listening to refugees: How traditional mental health interventions may miss the mark. Int. Soc. Work 2017, 60, 588–600. [Google Scholar] [CrossRef]
- Cleveland, J.; Hanley, J.; Cardona, M.S.; Turcotte-Plamondon, M.; Wolofsky, T.; Leloup, X.; Merry, L.; Rose, D. Ŀe Parcours D’installation des Demandeurs D’asile au Québec; Institut Universitaire SHERPA: Montrea, QC, Canada, 2021; Available online: https://sherpa-recherche.com/realisations/publications/parcours-dinstallation-des-demandeurs-dasile-au-quebec/ (accessed on 3 June 2023).
- Wu, Y.M.; Alzaghoul, A.F.; King, L.I.; Kuftedjian, R.; Kronick, R. Adaptation under strain: An ethnographic process evaluation of community-based psychosocial support services for refugee claimants during the height of the COVID-19 pandemic in Montreal, Canada. Front. Public Health 2023, 11, 1698. [Google Scholar] [CrossRef]
- Creswell, J.W. A Concise Introduction to Mixed Methods Research; SAGE Publications: New York, NY, USA, 2014. [Google Scholar]
- Sulaiman-Hill, C.M.; Thompson, S.C. Sampling challenges in a study examining refugee resettlement. BMC Int. Health Hum. Rights 2011, 11, 2. [Google Scholar] [CrossRef]
| Name | Items | Likert Scale | Cronbach’s Alpha |
|---|---|---|---|
| Satisfaction With Life Scale (shortened) |
| 7-point Likert scale: (1) “not at all true” to (7) “very true” | 0.75 |
| Mood Report |
| 7-point Likert scale: (1) “not at all” to (7) “extremely” | 0.88 |
| Basic Psychological Need Satisfaction Scale (shortened) |
| 4-point Likert scale: (1) “not at all” to (4) “extremely” | 0.87 |
| General Self-Efficacy Scale (shortened) |
| 4-point Likert scale: (1) “not at all true” to (4) “exactly true” | 0.63 |
| Adaptive Stress Index: Role and Identity; Existential Meaning. |
| 4-point Likert scale: (1) “not at all” to (4) “extremely” | 0.81 |
| Sociodemographic Variable | n | % or M (SD) |
|---|---|---|
| Age | 40 | 35.4 (7.2) |
| Highest level of education | ||
| Primary school | 0 | 0 |
| Secondary school | 14 | 35.0% |
| University and above | 25 | 62.5% |
| Civil status 1—Single 2—Married | 2 34 | 5.0% 59.6% |
| 3—Separated | 1 | 2.5% |
| 4—Divorced | 1 | 2.5% |
| 5—Widowed | 0 | 0% |
| 6—Prefer not to answer | 1 | 2.5% |
| No. of children Length of stay (months) Program attendance | 40 38 39 | 2.4 (1.0) 4.6 (8.6) 4 |
| Predictor | B | SE B | ß | t | p | VIF | ΔR2 | Adj R2 |
|---|---|---|---|---|---|---|---|---|
| Model 1 | 0.087 | |||||||
| Constant | 4.031 | 0.302 | 13.360 | <0.001 | ||||
| Length of stay | −0.068 | 0.030 | −0.507 | −2.250 | 0.031 | 2.060 | ||
| Program attendance | 0.313 | 0.150 | −0.471 | 2.091 | 0.044 | 2.060 | ||
| Model 2 | 0.095 | 0.182 | ||||||
| Constant | 2.050 | 0.924 | 2.218 | 0.033 | ||||
| Length of stay | −0.054 | 0.029 | −0.402 | −1.838 | 0.075 | 2.159 | ||
| Program attendance | 0.284 | 0.142 | 0.427 | 1.994 | 0.054 | 2.077 | ||
| Self-efficacy | 0.629 | 0.279 | 0.344 | 2.253 | 0.031 | 1.057 | ||
| Model 3 | 0.128 | 0.310 | ||||||
| Constant | 0.888 | 0.952 | 0.934 | 0.357 | ||||
| Length of stay | −0.063 | 0.027 | −0.473 | −2.337 | 0.026 | 2.197 | ||
| Program attendance | 0.340 | 0.132 | 0.512 | 2.570 | 0.015 | 2.130 | ||
| Self-efficacy | 0.317 | 0.218 | 0.173 | 1.125 | 0.269 | 1.273 | ||
| Need satisfaction | 0.378 | 0.140 | 0.408 | 2.700 | 0.011 | 1.223 |
| Predictor | B | SE B | ß | t | p | VIF | ΔR2 | Adj R2 |
|---|---|---|---|---|---|---|---|---|
| Model 1 | 0.048 | |||||||
| Constant | 2.122 | 0.151 | 14.014 | <0.001 | ||||
| Length of stay | 0.017 | 0.015 | 0.271 | 1.154 | 0.256 | 2.079 | ||
| Program attendance | −0.143 | 0.074 | −0.451 | −1.922 | 0.063 | 2.079 | ||
| Model 2 | −0.01 | 0.038 | ||||||
| Constant | 2.499 | 0.490 | 5.103 | <0.001 | ||||
| Length of stay | 0.015 | 0.015 | 0.231 | 0.959 | 0.345 | 2.170 | ||
| Program attendance | −0.138 | 0.075 | −0.437 | −1.848 | 0.074 | 2.091 | ||
| Self-efficacy | −0.119 | 0.147 | −0.136 | −0.810 | 0.424 | 1.056 | ||
| Model 3 | 0.26 | 0.298 | ||||||
| Constant | 3.268 | 0.469 | 6.974 | <0.001 | ||||
| Length of stay | 0.021 | 0.013 | 0.331 | 1.596 | 0.120 | 2.209 | ||
| Program attendance | −0.176 | 0.065 | −0.557 | −2.722 | 0.010 | 2.146 | ||
| Self-efficacy | 0.084 | 0.137 | 0.096 | 0.611 | 0.546 | 1.264 | ||
| Need satisfaction | −0.247 | 0.068 | −0.561 | −3.639 | <0.001 | 1.220 |
| Participant Code | Region of Origin | Length of Resettlement (Months) | Marital Status | Number of Children | Education Level | Language |
|---|---|---|---|---|---|---|
| Gloria | Central Africa | 7 | Married | 2 | Professional | French |
| Cassandra | Caribbean | 16 | Married * | 1 | Professional | French |
| Aisha | East Africa | 36 | Single | 2 | Highschool | English |
| Fatima | East Africa | 4 | Single | 1 | Professional | English |
| Mary | West Africa | 27 | Single | 2 | Professional | English |
| Tenneh | West Africa | 2 | Single | 2 | Highschool | English |
| Rosine | Central Africa | 5 | Married * | 2 | Professional | French |
| Adriana | South America | 5 | Married | 3 | Professional | Spanish |
| Selma | West Africa | 3 | Married | 2 | Professional | English |
| Daniela | South America | 1.5 | Married | 2 | Professional | Spanish |
| Divine | Central Africa | 2 | Married | 3 | Highschool | French |
| Fernanda | Central America | 4 | Married | 3 | Professional | Spanish |
| Rosa | South America | 3 | Married | 2 | Professional | Spanish |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wu, Y.M.; Kreitewolf, J.; Kronick, R. The Relationship between Wellbeing, Self-Determination, and Resettlement Stress for Asylum-Seeking Mothers Attending an Ecosocial Community-Based Intervention: A Mixed-Methods Study. Int. J. Environ. Res. Public Health 2023, 20, 7076. https://doi.org/10.3390/ijerph20227076
Wu YM, Kreitewolf J, Kronick R. The Relationship between Wellbeing, Self-Determination, and Resettlement Stress for Asylum-Seeking Mothers Attending an Ecosocial Community-Based Intervention: A Mixed-Methods Study. International Journal of Environmental Research and Public Health. 2023; 20(22):7076. https://doi.org/10.3390/ijerph20227076
Chicago/Turabian StyleWu, Yufei Mandy, Jens Kreitewolf, and Rachel Kronick. 2023. "The Relationship between Wellbeing, Self-Determination, and Resettlement Stress for Asylum-Seeking Mothers Attending an Ecosocial Community-Based Intervention: A Mixed-Methods Study" International Journal of Environmental Research and Public Health 20, no. 22: 7076. https://doi.org/10.3390/ijerph20227076
APA StyleWu, Y. M., Kreitewolf, J., & Kronick, R. (2023). The Relationship between Wellbeing, Self-Determination, and Resettlement Stress for Asylum-Seeking Mothers Attending an Ecosocial Community-Based Intervention: A Mixed-Methods Study. International Journal of Environmental Research and Public Health, 20(22), 7076. https://doi.org/10.3390/ijerph20227076






