Time-Driven Activity-Based Costing for Capturing the Complexity of Healthcare Processes: The Case of Deep Vein Thrombosis and Leg Ulcers
Abstract
1. Introduction
2. Materials and Methods
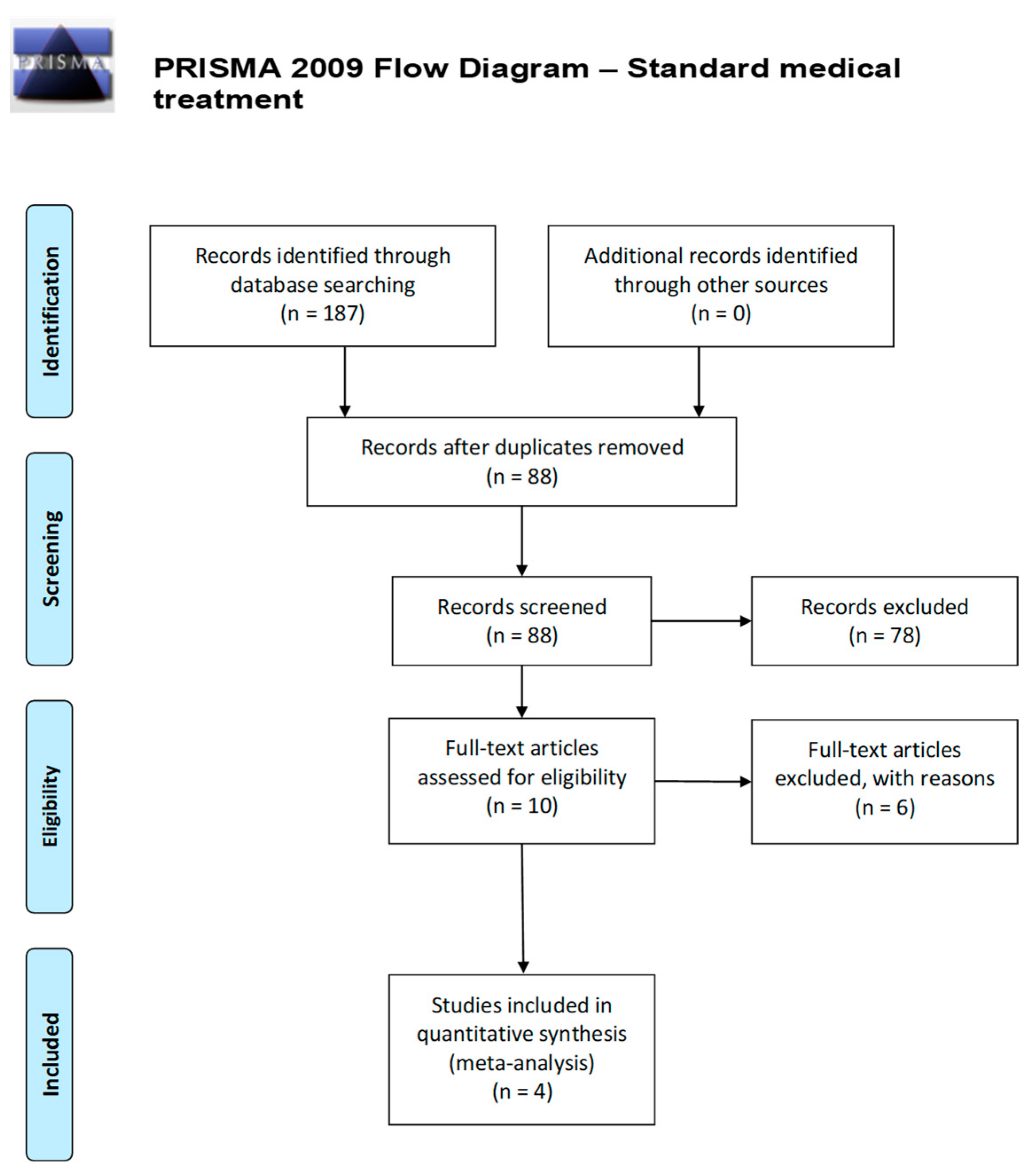
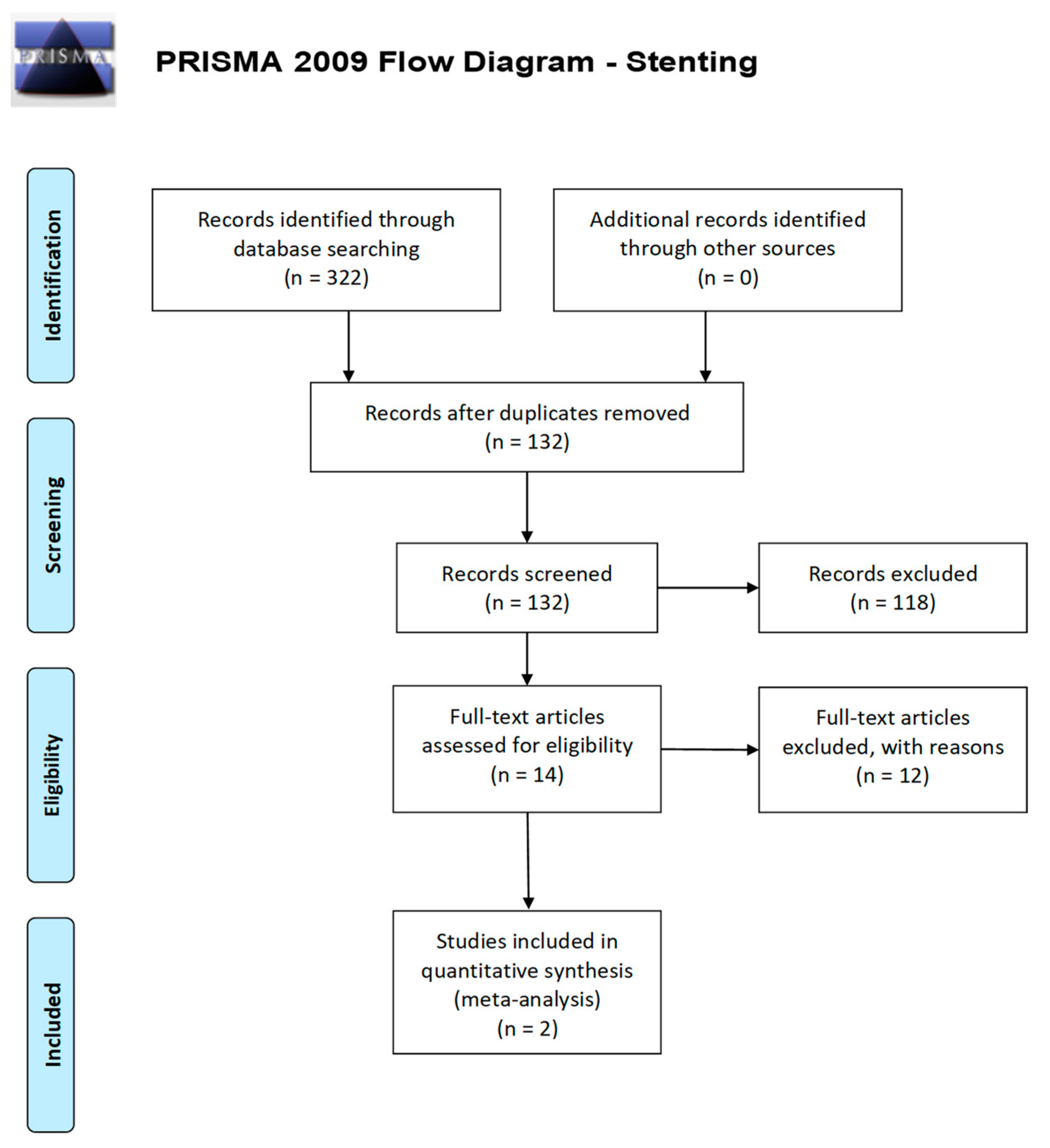
2.1. Literature Review
2.2. Clinical Data Synthesis
2.3. TDABC
- Process mapping and recording time data: three rounds of data gathering were performed. Firstly, we conducted an online interview due to mobility restrictions during the COVID-19 pandemic to identify the main phases and activities that characterize surgical procedures. The interview was conducted on 3 June 2021 and included a vascular surgeon and her staff. In particular, the vascular surgeon interviewed was the head of the Hesperia surgical team, with over 20 years of experience. Her staff consisted of a second vascular surgeon, the nursing coordinator, and two administrative assistants. During the interview, we asked them to describe all activities involving staff and patient flows from patient admission to its discharge. For each activity, we therefore asked to indicate the execution time, the kind of personnel involved, goods and services consumed, spaces and technologies used. A draft of a process map was developed, which specified resources (personnel and clinical) required in each step of the care cycle. Additionally, it included an estimation of the time of each resource used. Secondly, we conducted a face-to-face interview with the vascular surgeon. This step was critical to validate the process map and time estimation and to gather possible missing data. This second interview was conducted on 12 July 2021 at Hesperia Hospital. Thirdly, we conducted an in-depth observation of the processes mapped by following a patient during her hospitalization, from admission to discharge. This allowed us to compare data gathered through interviews with the actual care activities, solving possible misalignment in activities, sequence, and timing. This third step was implemented between 10 and 11 November 2021 at Hesperia Hospital.
- Costs data gathering and utilization: Once the processes and resources were mapped, the cost data collection phase was initiated. We defined a template and the personnel of the administrative office at Hesperia Hospital supported us in identifying and isolating the cost of personnel, goods and services, spaces and technology. The capacity cost rate for each resource and process step was calculated as the euro per minute capacity cost rate for all the clinical resources absorbed by the process steps. For healthcare personnel, costs were computed by multiplying the minutes spent in each phase by the wage per minute for each role (details about the capacity costs for the different roles and timings applied are reported in Supplementary Table S3). Finally, the cost of caring for the patient in the total care cycle was estimated.
2.4. Cost-Effectiveness Model
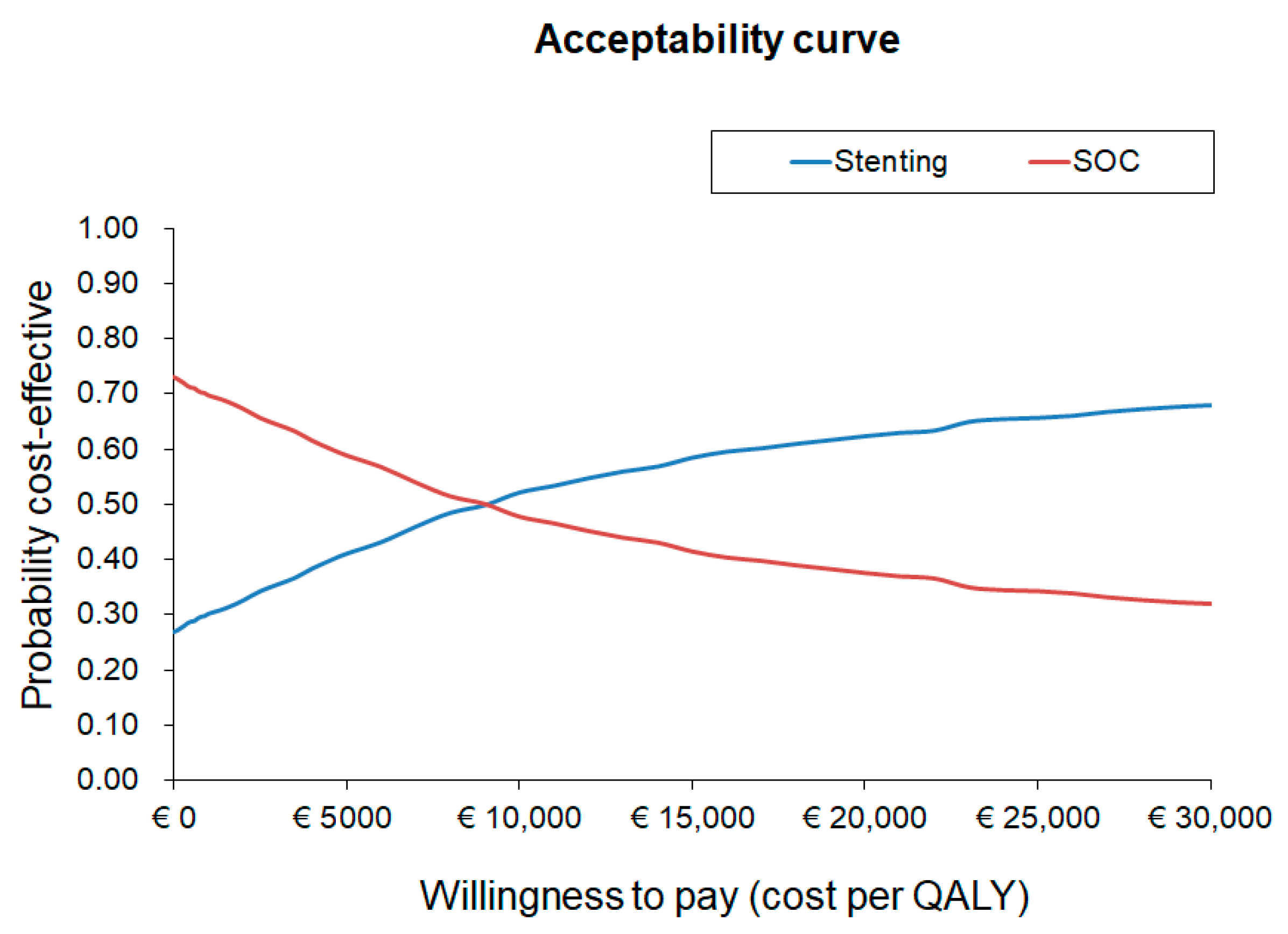
2.5. Cost-Effectiveness Analysis
3. Results
Cost-Effectiveness Analysis
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
Appendix B
| Item | Guidance for Reporting | Reported in Section | |
|---|---|---|---|
| TITLE | |||
| Title | 1 | Identify the study as an economic evaluation and specify the interventions being compared. | Title page |
| ABSTRACT | |||
| Abstract | 2 | Provide a structured summary that highlights context, key methods, results and alternative analyses. | Title page |
| INTRODUCTION | |||
| Background and objectives | 3 | Give the context for the study, the study question and its practical relevance for decision making in policy or practice. | Introduction |
| METHODS | |||
| Health economic analysis plan | 4 | Indicate whether a health economic analysis plan was developed and where available. | Materials and Methods |
| Study population | 5 | Describe characteristics of the study population (such as age range, demographics, socioeconomic, or clinical characteristics). | Cost-effectiveness model |
| Setting and location | 6 | Provide relevant contextual information that may influence findings. | Cost-effectiveness model |
| Comparators | 7 | Describe the interventions or strategies being compared and why chosen. | Introduction, Cost-effectiveness model |
| Perspective | 8 | State the perspective(s) adopted by the study and why chosen. | Materials and Methods |
| Time horizon | 9 | State the time horizon for the study and why appropriate. | Cost-effectiveness model |
| Discount rate | 10 | Report the discount rate(s) and reason chosen. | Cost-effectiveness model |
| Selection of outcomes | 11 | Describe what outcomes were used as the measure(s) of benefit(s) and harm(s). | Cost-effectiveness model |
| Measurement of outcomes | 12 | Describe how outcomes used to capture benefit(s) and harm(s) were measured. | Cost-effectiveness analysis |
| Valuation of outcomes | 13 | Describe the population and methods used to measure and value outcomes. | Materials and Methods |
| Measurement and valuation of resources and costs | 14 | Describe how costs were valued. | TDABC |
| Currency, price date, and conversion | 15 | Report the dates of the estimated resource quantities and unit costs, plus the currency and year of conversion. | TDABC |
| Rationale and description of model | 16 | If modelling is used, describe in detail and why used. Report if the model is publicly available and where it can be accessed. | Cost-effectiveness model |
| Analytics and assumptions | 17 | Describe any methods for analysing or statistically transforming data, any extrapolation methods, and approaches for validating any model used. | Clinical data synthesis |
| Characterizing heterogeneity | 18 | Describe any methods used for estimating how the results of the study vary for sub-groups. | Not reported |
| Characterizing distributional effects | 19 | Describe how impacts are distributed across different individuals or adjustments made to reflect priority populations. | Not reported |
| Characterizing uncertainty | 20 | Describe methods to characterize any sources of uncertainty in the analysis. | Cost-effectiveness analysis |
| Approach to engagement with patients and others affected by the study | 21 | Describe any approaches to engage patients or service recipients, the general public, communities, or stakeholders (e.g., clinicians or payers) in the design of the study. | TDABC |
| RESULTS | |||
| Study parameters | 22 | Report all analytic inputs (e.g., values, ranges, references) including uncertainty or distributional assumptions. | Materials and Methods, Supplementary Tables S1–S4 |
| Summary of main results | 23 | Report the mean values for the main categories of costs and outcomes of interest and summarise them in the most appropriate overall measure. | Results |
| Effect of uncertainty | 24 | Describe how uncertainty about analytic judgments, inputs, or projections affect findings. Report the effect of choice of discount rate and time horizon, if applicable. | Results |
| Effect of engagement with patients and others affected by the study | 25 | Report on any difference patient/service recipient, general public, community, or stakeholder involvement made to the approach or findings of the study | Results |
| DISCUSSION | |||
| Study findings, limitations, generalizability, and current knowledge | 26 | Report key findings, limitations, ethical or equity considerations not captured, and how these could impact patients, policy, or practice. | Discussion |
| OTHER RELEVANT INFORMATION | |||
| Source of funding | 27 | Describe how the study was funded and any role of the funder in the identification, design, conduct, and reporting of the analysis | Funding |
| Conflicts of interest | 28 | Report authors conflicts of interest according to journal or International Committee of Medical Journal Editors requirements. | Conflicts of Interest |
References
- Porter, M.E.; Lee, T.H. The strategy that will fix health care. Harv. Bus. Rev. 2013, 91, 24. [Google Scholar]
- Porter, M.E.; Teisberg, E.O. Redefining Health Care: Creating Value-Based Competition on Results; Harvard Business Press: Boston, MA, USA, 2006; ISBN 978-1-59139-778-6. [Google Scholar]
- Kaplan, R.S.; Porter, M.E. How to Solve the Cost Crisis in Health Care. Harv. Bus. Rev. 2011, 89, 46–52, 54, 56–61 passim. [Google Scholar]
- Keel, G.; Savage, C.; Rafiq, M.; Mazzocato, P. Time-Driven Activity-Based Costing in Health Care: A Systematic Review of the Literature. Health Policy Amst. Neth. 2017, 121, 755–763. [Google Scholar] [CrossRef] [PubMed]
- Grey, J.E.; Harding, K.G.; Enoch, S. Venous and Arterial Leg Ulcers. BMJ 2006, 332, 347–350. [Google Scholar] [CrossRef] [PubMed]
- Kolluri, R. Management of Venous Ulcers. Tech. Vasc. Interv. Radiol. 2014, 17, 132–138. [Google Scholar] [CrossRef] [PubMed]
- Partsch, H. 7—Compression therapy in venous leg ulcers. In Venous Ulcers; Bergan, J.J., Shortell, C.K., Eds.; Academic Press: San Diego, CA, USA, 2007; pp. 77–90. ISBN 978-0-12-373565-2. [Google Scholar]
- Salute, M. Della Nomenclatore Protesica. Available online: https://www.salute.gov.it/portale/temi/p2_6.jsp?id=1312&area=programmazioneSanitariaLea&menu=lea (accessed on 7 April 2023).
- Murphy, E.H. Surveying the 2019 Venous Stent Landscape. Endovasc Today 2019, 18, 53–64. [Google Scholar]
- Schwein, A.; Georg, Y.; Lejay, A.; Nicolini, P.; Hartung, O.; Contassot, D.; Thaveau, F.; Heim, F.; Chakfe, N. Endovascular Treatment for Venous Diseases: Where Are the Venous Stents? Methodist DeBakey Cardiovasc. J. 2018, 14, 208. [Google Scholar] [CrossRef] [PubMed]
- Breen, K. Role of Venous Stenting for Venous Thromboembolism. Hematol. Am. Soc. Hematol. Educ. Program 2020, 2020, 606–611. [Google Scholar] [CrossRef] [PubMed]
- Dake, M.D.; O’Sullivan, G.; Shammas, N.W.; Lichtenberg, M.; Mwipatayi, B.P.; Settlage, R.A.; VERNACULAR Trial Investigators. Three-Year Results from the Venovo Venous Stent Study for the Treatment of Iliac and Femoral Vein Obstruction. Cardiovasc. Intervent. Radiol. 2021, 44, 1918–1929. [Google Scholar] [CrossRef]
- O’Sullivan, G.J.; Karunanithy, N.; Binkert, C.A.; Ortega, M.R.; Lichtenberg, M.; McCann-Brown, J.A. One Year Outcomes of the VIVO-EU Study of Treatment of Symptomatic Iliofemoral Outflow Obstruction with the Zilver Vena Venous Self-Expanding Stent. Cardiovasc. Intervent. Radiol. 2021, 44, 1930–1936. [Google Scholar] [CrossRef] [PubMed]
- Murphy, E.; Gibson, K.; Sapoval, M.; Dexter, D.J.; Kolluri, R.; Razavi, M.; Black, S. Pivotal Study Evaluating the Safety and Effectiveness of the Abre Venous Self-Expanding Stent System in Patients With Symptomatic Iliofemoral Venous Outflow Obstruction. Circ. Cardiovasc. Interv. 2022, 15, e010960. [Google Scholar] [CrossRef] [PubMed]
- Hofmann, L.R.; Gagne, P.; Brown, J.A.; Saunders, A.; Comerota, A.; VIVO Study Investigators. Twelve-Month End Point Results from the Evaluation of the Zilver Vena Venous Stent in the Treatment of Symptomatic Iliofemoral Venous Outflow Obstruction (VIVO Clinical Study). J. Vasc. Surg. Venous Lymphat. Disord. 2023, 11, 532–541.e4. [Google Scholar] [CrossRef] [PubMed]
- Salute, M. Della Principali Caratteristiche Diagnosis Related Groups (DRG). Available online: https://www.salute.gov.it/portale/temi/p2_6.jsp?lingua=italiano&id=1349&area=ricoveriOspedalieri&menu=sistema (accessed on 7 April 2023).
- Rognoni, C.; Lugli, M.; Maleti, O.; Tarricone, R. Clinical Guidelines versus Current Clinical Practice for the Management of Deep Vein Thrombosis. J. Vasc. Surg. Venous Lymphat. Disord. 2021, 9, 1334–1344.e1. [Google Scholar] [CrossRef] [PubMed]
- Washington University School of Medicine. Chronic Venous Thrombosis: Relief with Adjunctive Catheter-Directed Therapy—The C-TRACT Trial; National Library of Medicine: Bethesda, MD, USA, 2022. Available online: https://clinicaltrials.gov/ct2/show/NCT03250247 (accessed on 14 March 2023).
- Berger, M.L.; Sox, H.; Willke, R.J.; Brixner, D.L.; Eichler, H.-G.; Goettsch, W.; Madigan, D.; Makady, A.; Schneeweiss, S.; Tarricone, R.; et al. Good Practices for Real-World Data Studies of Treatment and/or Comparative Effectiveness: Recommendations from the Joint ISPOR-ISPE Special Task Force on Real-World Evidence in Health Care Decision Making. Pharmacoepidemiol. Drug Saf. 2017, 26, 1033–1039. [Google Scholar] [CrossRef]
- Pongiglione, B.; Torbica, A.; Blommestein, H.; de Groot, S.; Ciani, O.; Walker, S.; Dams, F.; Blankart, R.; Mollenkamp, M.; Kovács, S.; et al. Do Existing Real-World Data Sources Generate Suitable Evidence for the HTA of Medical Devices in Europe? Mapping and Critical Appraisal. Int. J. Technol. Assess. Health Care 2021, 37, e62. [Google Scholar] [CrossRef]
- Tarricone, R.; Boscolo, P.R.; Armeni, P. What Type of Clinical Evidence Is Needed to Assess Medical Devices? Eur. Respir. Rev. Off. J. Eur. Respir. Soc. 2016, 25, 259–265. [Google Scholar] [CrossRef]
- Tangney, E.; O’Donnell, T.; Iafrati, M. Cost and Benefit Analysis of Stenting Versus Compression Therapy for Patients With Chronic Total Venous Occlusion. J. Vasc. Surg. Venous Lymphat. Disord. 2016, 4, 137. [Google Scholar] [CrossRef]
- Rognoni, C.; Lugli, M.; Maleti, O.; Tarricone, R. Venous Stenting for Patients with Outflow Obstruction and Leg Ulcers: Cost-Effectiveness and Budget Impact Analyses. J. Comp. Eff. Res. 2020, 9, 705–720. [Google Scholar] [CrossRef]
- Introduction to Meta-Analysis | Wiley Online Books. Available online: https://onlinelibrary.wiley.com/doi/book/10.1002/9780470743386 (accessed on 7 April 2023).
- Husereau, D.; Drummond, M.; Petrou, S.; Carswell, C.; Moher, D.; Greenberg, D.; Augustovski, F.; Briggs, A.H.; Mauskopf, J.; Loder, E.; et al. Consolidated Health Economic Evaluation Reporting Standards (CHEERS)—Explanation and Elaboration: A Report of the ISPOR Health Economic Evaluation Publication Guidelines Good Reporting Practices Task Force. Value Health J. Int. Soc. Pharmacoecon. Outcomes Res. 2013, 16, 231–250. [Google Scholar] [CrossRef]
- Husereau, D.; Drummond, M.; Augustovski, F.; de Bekker-Grob, E.; Briggs, A.H.; Carswell, C.; Caulley, L.; Chaiyakunapruk, N.; Greenberg, D.; Loder, E.; et al. Consolidated Health Economic Evaluation Reporting Standards (CHEERS) 2022 Explanation and Elaboration: A Report of the ISPOR CHEERS II Good Practices Task Force. Value Health J. Int. Soc. Pharmacoecon. Outcomes Res. 2022, 25, 10–31. [Google Scholar] [CrossRef]
- PE Guidelines around the World: Italy. Available online: https://tools.ispor.org/PEguidelines/countrydet.asp?c=13&t=4 (accessed on 7 April 2023).
- Kaplan, R.S.; Blackstone, R.P.; Haas, D.A.; Thaker, N.G.; Frank, S.J. Measuring and Communicating Health Care Value with Charts. Harv. Bus. Rev. website 2015. Available online: https://hbr.org/2015/10/measuring-and-communicating-health-care-value-with-charts (accessed on 14 March 2023).
- Thaker, N.G.; Ali, T.N.; Porter, M.E.; Feeley, T.W.; Kaplan, R.S.; Frank, S.J. Communicating Value in Health Care Using Radar Charts: A Case Study of Prostate Cancer. J. Oncol. Pract. 2016, 12, 813–820. [Google Scholar] [CrossRef]
- Ashrani, A.A.; Heit, J.A. Incidence and cost burden of post-thrombotic syndrome. J Thromb. Thrombolysis 2009, 28, 465–476. [Google Scholar] [CrossRef]
- Kolluri, R.; Lugli, M.; Villalba, L.; Varcoe, R.; Maleti, O.; Gallardo, F.; Black, S.; Forgues, F.; Lichtenberg, M.; Hinahara, J.; et al. An Estimate of the Economic Burden of Venous Leg Ulcers Associated with Deep Venous Disease. Vasc. Med. Lond. Engl. 2022, 27, 63–72. [Google Scholar] [CrossRef] [PubMed]
- Niñerola, A.; Hernández-Lara, A.-B.; Sánchez-Rebull, M.-V. Improving Healthcare Performance through Activity-Based Costing and Time-Driven Activity-Based Costing. Int. J. Health Plann. Manag. 2021, 36, 2079–2093. [Google Scholar] [CrossRef] [PubMed]
- Tarricone, R.; Amatucci, F.; Armeni, P.; Banks, H.; Borsoi, L.; Callea, G.; Ciani, O.; Costa, F.; Federici, C.; Torbica, A.; et al. Establishing a National HTA Program for Medical Devices in Italy: Overhauling a Fragmented System to Ensure Value and Equal Access to New Medical Technologies. Health Policy 2021, 125, 602–608. [Google Scholar] [CrossRef] [PubMed]
- Amsler, F.; Willenberg, T.; Blättler, W. In Search of Optimal Compression Therapy for Venous Leg Ulcers: A Meta-Analysis of Studies Comparing Diverse [Corrected] Bandages with Specifically Designed Stockings. J. Vasc. Surg. 2009, 50, 668–674. [Google Scholar] [CrossRef] [PubMed]
- Raju, S.; Owen, S.; Neglen, P. The Clinical Impact of Iliac Venous Stents in the Management of Chronic Venous Insufficiency. J. Vasc. Surg. 2002, 35, 8–15. [Google Scholar] [CrossRef] [PubMed]
- Hartung, O.; Otero, A.; Boufi, M.; De Caridi, G.; Barthelemy, P.; Juhan, C.; Alimi, Y.S. Mid-Term Results of Endovascular Treatment for Symptomatic Chronic Nonmalignant Iliocaval Venous Occlusive Disease. J. Vasc. Surg. 2005, 42, 1138–1144; discussion 1144. [Google Scholar] [CrossRef]
- Tarricone, R.; Torbica, A.; Drummond, M. Challenges in the Assessment of Medical Devices: The MedtecHTA Project. Health Econ. 2017, 26, 5–12. [Google Scholar] [CrossRef]
- Tarricone, R.; Callea, G.; Ogorevc, M.; Prevolnik Rupel, V. Improving the Methods for the Economic Evaluation of Medical Devices. Health Econ. 2017, 26 (Suppl. S1), 70–92. [Google Scholar] [CrossRef] [PubMed]
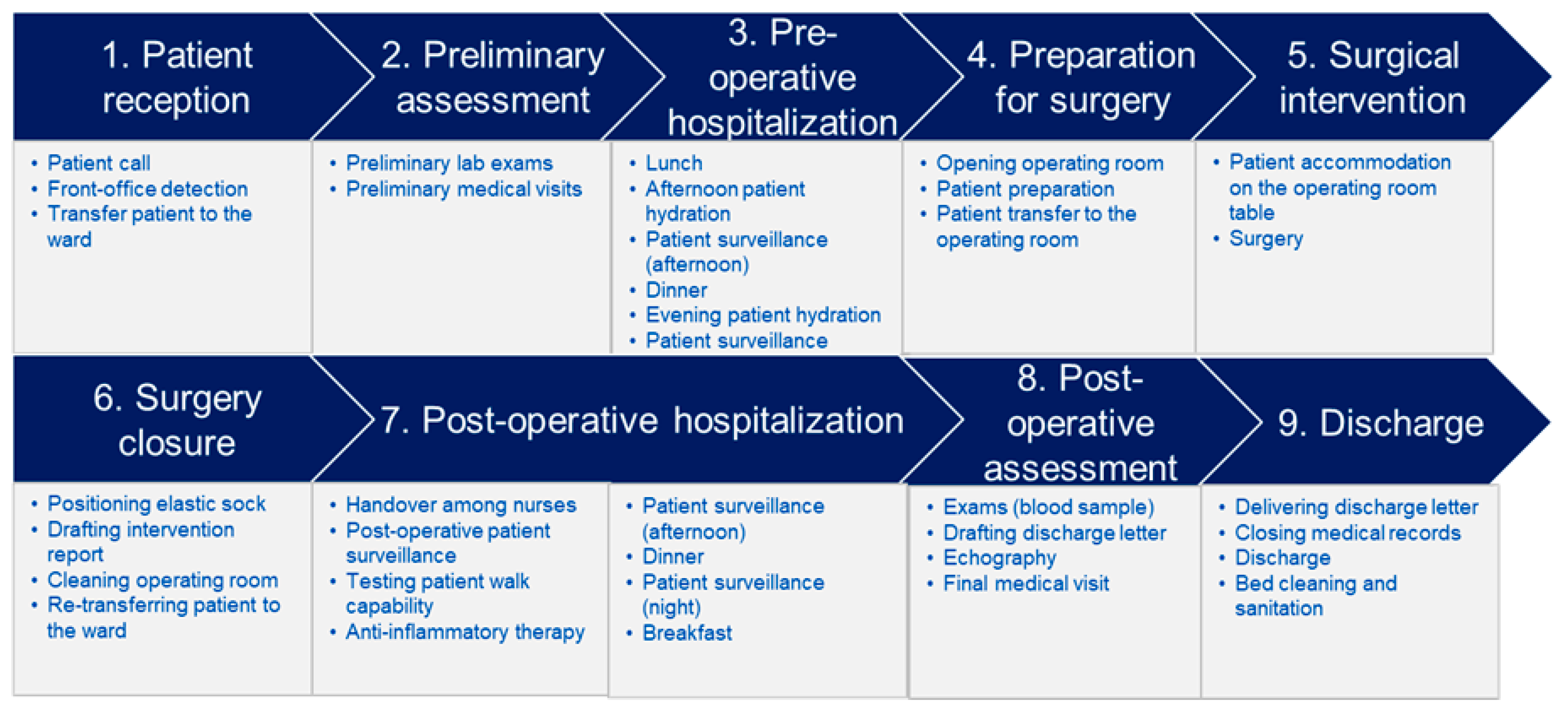

| Macro-Phase | Timing (in Minutes) | Timing (%) | Personnel Costs (EUR) | Good, Services, Tech and Infrastructural Costs (EUR) | Total Costs (EUR) | Total Costs (%) |
|---|---|---|---|---|---|---|
| 1 Patient reception | 21 | 1% | 13.42 | 0.67 | 14.09 | 0% |
| 2 Preliminary assessment | 127 | 4% | 185.82 | 239.56 | 425.38 | 8% |
| 3 Pre-operative hospitalization | 1161 | 39% | 106.07 | 37.16 | 143.22 | 3% |
| 4 Preparation for surgery | 87 | 3% | 70.07 | 10.48 | 80.56 | 2% |
| 5 Surgical intervention | 145 | 5% | 479.67 | 3519.51 | 3999.18 | 79% |
| 6 Surgery closure | 80 | 3% | 92.31 | 10.85 | 103.16 | 2% |
| 7 Post-operative hospitalization | 1255 | 42% | 144.66 | 40.16 | 184.82 | 4% |
| 8 Post-operative assessment | 35 | 1% | 50.87 | 1.12 | 51.99 | 1% |
| 9 Discharge | 72 | 2% | 77.27 | 2.30 | 79.58 | 2% |
| Total | 2983 | 100% | 1220.17 | 3861.82 | 5081.99 | 100% |
| Phase | Timing (in Minutes) | Personnel Costs (EUR) | Good, Services, Tech and Infrastructural Costs (EUR) | Cost Borne by the Patient (EUR) | Total Costs (EUR) |
|---|---|---|---|---|---|
| First visit | |||||
| Patient reception | 2 | 0.73 | 0.02 | - | 0.75 |
| Acquisition of informed consent | 3 | 1.10 | 0.03 | - | 1.13 |
| Dermatological visit | 65 | 51.16 | 58.59 | - | 109.75 |
| Communication to patient and caregiver | 20 | 32.32 | 0.11 | - | 32.43 |
| Definition of treatment program * | 15 | 24.24 | 67.38 | - | 91.62 |
| Delivery of treatment program * | 15 | 8.10 | 0.08 | - | 8.18 |
| Total | 120 | 117.65 | 126.21 | - | 243.86 |
| Subsequent visits and treatments (each month) | |||||
| Patient reception | 2 | 0.73 | 0.02 | - | 0.75 |
| Visit | 20 | 32.32 | 0.32 | - | 32.64 |
| Cleansing, curettage and swab | 20 | 21.56 | 3.11 | - | 24.67 |
| Wound debridement **** | 20 | 32.32 | 8.95 | - | 41.27 |
| Medication ** | 5 | 2.70 | 3.36 | - | 6.06 |
| Treatment and bandages | 107 | 57.66 | 241.43 | 38.72 | 337.80 |
| Booking next visit | 3 | 1.62 | 0.02 | - | 1.64 |
| Total | 176.8 | 148.91 | 257.21 | 38.72 | 444.83 |
| Final phase (in case of ulcer healing) | |||||
| Last medical visit | 20 | 32.32 | 0.11 | - | 32.43 |
| Instruction on braces use | 10 | 5.40 | 0.05 | - | 5.45 |
| Closing therapy *** | 25.00 | 185.50 | 210.50 | ||
| Control visits | 40 | 64.64 | 0.43 | - | 65.07 |
| Total | 70 | 102.36 | 25.59 | 185.50 | 313.45 |
| Parameter | Lower Limit | Base Case | Upper Limit | Lower ICUR Limit (EUR) | Upper ICUR Limit (EUR) | Variation (EUR) |
|---|---|---|---|---|---|---|
| Stenting % ulcers healed | 0.65 | 0.81 | 0.97 | 62,363.85 | Dominant | CEA result change |
| SOC % ulcers healed | 0.49 | 0.61 | 0.73 | 1436.29 | 33,566.77 | 32,130.48 |
| Utility healed ulcer | 0.80 | 1.00 | 1.00 | 36,040.67 | 10,270.18 | 25,770.49 |
| Utility active ulcer | 0.58 | 0.73 | 0.88 | 7007.05 | 19,221.46 | 12,214.41 |
| Cost Stenting | 4187.20 | 5234.00 | 6280.80 | 4489.06 | 16,051.30 | 11,562.24 |
| Cost FUP—active ulcer (monthly) | 324.89 | 406.11 | 487.33 | 13,754.31 | 6786.05 | 6968.26 |
| SOC mean healing time (months) | 2.40 | 3.00 | 3.60 | 11,016.75 | 9549.95 | 1466.80 |
| Utility recurred ulcer | 0.51 | 0.64 | 0.77 | 9787.21 | 10,803.29 | 1016.08 |
| Cost first visit—active ulcer | 195.09 | 243.86 | 292.63 | 10,540.74 | 9999.62 | 541.12 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rognoni, C.; Furnari, A.; Lugli, M.; Maleti, O.; Greco, A.; Tarricone, R. Time-Driven Activity-Based Costing for Capturing the Complexity of Healthcare Processes: The Case of Deep Vein Thrombosis and Leg Ulcers. Int. J. Environ. Res. Public Health 2023, 20, 5817. https://doi.org/10.3390/ijerph20105817
Rognoni C, Furnari A, Lugli M, Maleti O, Greco A, Tarricone R. Time-Driven Activity-Based Costing for Capturing the Complexity of Healthcare Processes: The Case of Deep Vein Thrombosis and Leg Ulcers. International Journal of Environmental Research and Public Health. 2023; 20(10):5817. https://doi.org/10.3390/ijerph20105817
Chicago/Turabian StyleRognoni, Carla, Alessandro Furnari, Marzia Lugli, Oscar Maleti, Alessandro Greco, and Rosanna Tarricone. 2023. "Time-Driven Activity-Based Costing for Capturing the Complexity of Healthcare Processes: The Case of Deep Vein Thrombosis and Leg Ulcers" International Journal of Environmental Research and Public Health 20, no. 10: 5817. https://doi.org/10.3390/ijerph20105817
APA StyleRognoni, C., Furnari, A., Lugli, M., Maleti, O., Greco, A., & Tarricone, R. (2023). Time-Driven Activity-Based Costing for Capturing the Complexity of Healthcare Processes: The Case of Deep Vein Thrombosis and Leg Ulcers. International Journal of Environmental Research and Public Health, 20(10), 5817. https://doi.org/10.3390/ijerph20105817






