Burnout in International Medical Students: Characterization of Professionalism and Loneliness as Predictive Factors of Burnout
Abstract
1. Introduction
1.1. Background
1.2. Study Purpose
2. Material and Methods
2.1. Participants
2.2. Main Measures
2.3. Procedures
2.4. Data Analysis
3. Results
4. Discussion
4.1. Positive Correlation between Burnout and the Measures of Loneliness and Medical Professionalism
4.2. Characterization of Predictors for Global Burnout
4.3. Characterization of Predictors for Each Domain of Burnout
4.4. Limitiations of the Study
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Ball, S.; Bax, A. Self-care in Medical Education. Acad. Med. 2002, 77, 911–917. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, R.E.; Matthews, J.R.; Grandy, T.G.; Lupo, J.V. The question of stress among first-year medical students. Acad. Med. 1983, 58, 367–372. [Google Scholar] [CrossRef] [PubMed]
- Bianchi, R.; Schonfeld, I.S.; Laurent, E. Burnout-depression overlap: A review. Clin. Psychol. Rev. 2015, 36, 28–41. [Google Scholar] [CrossRef] [PubMed]
- Bridgeman, P.J.; Bridgeman, M.B.; Barone, J. Burnout syndrome among healthcare professionals. Am. J. Health. Syst. Pharm. 2018, 75, 147–152. [Google Scholar] [CrossRef]
- Garcia, C.d.L.; Abreu, L.C.D.; Ramos, J.L.S.; Castro, C.F.D.D.; Smiderle, F.R.N.; Santos, J.A.D.; Bezerra, I.M.P. Influence of Burnout on Patient Safety: Systematic Review and Meta-Analysis. Medicina 2019, 55, 553. [Google Scholar] [CrossRef]
- Hall, L.H.; Johnson, J.; Watt, I.; Tsipa, A.; O’Connor, D.B. Healthcare Staff Wellbeing, Burnout, and Patient Safety: A Systematic Review. PLoS ONE 2016, 11, e0159015. [Google Scholar] [CrossRef]
- Shanafelt, T.D.; Balch, C.M.; Bechamps, G.; Russell, T.; Dyrbye, L.; Satele, D.; Collicott, P.; Novotny, P.J.; Sloan, J.; Freischlag, J. Burnout and Medical Errors Among American Surgeons. Ann. Surg. 2010, 251, 995–1000. [Google Scholar] [CrossRef]
- Fahrenkopf, A.M.; Sectish, T.C.; Barger, L.K.; Sharek, P.J.; Lewin, D.; Chiang, V.W.; Edwards, S.; Wiedermann, B.L.; Landrigan, C.P. Rates of medication errors among depressed and burnt out residents: Prospective cohort study. BMJ 2008, 336, 488–491. [Google Scholar] [CrossRef]
- Dyrbye, L.N.; Varkey, P.; Boone, S.L.; Satele, D.V.; Sloan, J.A.; Shanafelt, T.D. Physician Satisfaction and Burnout at Different Career Stages. Mayo Clin. Proc. 2013, 88, 1358–1367. [Google Scholar] [CrossRef]
- Ratanawongsa, N.; Roter, D.; Beach, M.C.; Laird, S.L.; Larson, S.M.; Carson, K.A.; Cooper, L.A. Physician Burnout and Patient-Physician Communication During Primary Care Encounters. J. Gen. Intern. Med. 2008, 23, 1581. [Google Scholar] [CrossRef]
- West, C.P.; Huschka, M.M.; Novotny, P.J.; Sloan, J.A.; Kolars, J.C.; Habermann, T.M.; Shanafelt, T.D. Association of Perceived Medical Errors With Resident Distress and Empathy. JAMA 2006, 296, 1071. [Google Scholar] [CrossRef]
- West, C.P. Association of Resident Fatigue and Distress With Perceived Medical Errors. JAMA 2009, 302, 1294. [Google Scholar] [CrossRef]
- Cheng, J.; Zhao, Y.Y.; Wang, J.; Sun, Y.H. Academic burnout and depression of Chinese medical students in the pre-clinical years: The buffering hypothesis of resilience and social support. Psychol. Health Med. 2020, 25, 1094–1105. [Google Scholar] [CrossRef]
- Pagnin, D.; De Queiroz, V.; De Oliveira Filho, M.A.; Gonzalez, N.V.A.; Salgado, A.E.T.; Cordeiro e Oliveira, B.; Lodi, C.S.; Melo, R.M.D.S. Burnout and career choice motivation in medical students. Med. Teach. 2013, 35, 388–394. [Google Scholar] [CrossRef]
- Schaufeli, W.B.; Martínez, I.M.; Pinto, A.M.; Salanova, M.; Bakker, A.B. Burnout and Engagement in University Students. J. Cross. Cult. Psychol. 2002, 33, 464–481. [Google Scholar] [CrossRef]
- Salmela-Aro, K.; Savolainen, H.; Holopainen, L. Depressive Symptoms and School Burnout During Adolescence: Evidence from Two Cross-lagged Longitudinal Studies. J. Youth Adolesc. 2009, 38, 1316–1327. [Google Scholar] [CrossRef]
- IsHak, W.; Nikravesh, R.; Lederer, S.; Perry, R.; Ogunyemi, D.; Bernstein, C. Burnout in medical students: A systematic review. Clin. Teach. 2013, 10, 242–245. [Google Scholar] [CrossRef]
- Chunming, W.M.; Harrison, R.; MacIntyre, R.; Travaglia, J.; Balasooriya, C. Burnout in medical students: A systematic review of experiences in Chinese medical schools. BMC Med. Educ. 2017, 17, 217. [Google Scholar] [CrossRef]
- Brazeau, C.M.L.R.L.R.; Schroeder, R.; Rovi, S.; Boyd, L. Relationships between medical student burnout, empathy, and professionalism climate. Acad. Med. 2010, 85, S33–S36. [Google Scholar] [CrossRef]
- Dyrbye, L.N.; Massie, F.S.; Eacker, A.; Harper, W.; Power, D.; Durning, S.J.; Thomas, M.R.; Moutier, C.; Satele, D.; Sloan, J.; et al. Relationship between Burnout and Professional Conduct and Attitudes Among US Medical Students. JAMA 2010, 304, 1173. [Google Scholar] [CrossRef]
- Paro, H.B.M.S.; Silveira, P.S.P.; Perotta, B.; Gannam, S.; Enns, S.C.; Giaxa, R.R.B.; Bonito, R.F.; Martins, M.A.M.A.; Tempski, P.Z. Empathy among Medical Students: Is There a Relation with Quality of Life and Burnout? PLoS ONE 2014, 9, e94133. [Google Scholar] [CrossRef] [PubMed]
- Dahlin, M.; Joneborg, N.; Runeson, B. Performance-based self-esteem and burnout in a cross-sectional study of medical students. Med. Teach. 2007, 29, 43–48. [Google Scholar] [CrossRef] [PubMed]
- Howe, A.; Smajdor, A.; Stöckl, A. Towards an understanding of resilience and its relevance to medical training. Med. Educ. 2012, 46, 349–356. [Google Scholar] [CrossRef] [PubMed]
- Dyrbye, L.N.; Thomas, M.R.; Huntington, J.L.; Lawson, K.L.; Novotny, P.J.; Sloan, J.A.; Shanafelt, T.D. Personal Life Events and Medical Student Burnout: A Multicenter Study. Acad. Med. 2006, 81, 374–384. [Google Scholar] [CrossRef] [PubMed]
- Maslach, C.; Jackson, S.E.; Leiter, M.P. Maslach Burnout Inventory. In Evaluating Stress: A book of Resources; Zalaquett, C.P., Wood, R.J., Eds.; Scarecrow Press, Inc.: Lanhan, MD, USA, 1997; pp. 191–218. ISBN 978-0-8108-3231-2. [Google Scholar]
- Hojat, M.; Mangione, S.; Nasca, T.J.; Cohen, M.J.M.; Gonnella, J.S.; Erdmann, J.B.; Veloski, J.; Magee, M. The Jefferson Scale of Physician Empathy: Development and Preliminary Psychometric Data. Educ. Psychol. Meas. 2001, 61, 349–365. [Google Scholar] [CrossRef]
- Hojat, M.; Fields, S.K.; Veloski, J.J.; Griffiths, M.; Cohen, M.J.M.; Plumb, J.D. Psychometric Properties of an Attitude Scale Measuring Physician-Nurse Collaboration. Eval. Health Prof. 1999, 22, 208–220. [Google Scholar] [CrossRef] [PubMed]
- Wetzel, A.P.; Mazmanian, P.E.; Hojat, M.; Kreutzer, K.O.; Carrico, R.J.; Carr, C.; Veloski, J.; Rafiq, A. Measuring Medical Students’ Orientation Toward Lifelong Learning: A Psychometric Evaluation. Acad. Med. 2010, 85, S41–S44. [Google Scholar] [CrossRef]
- DiTommaso, E.; Brannen, C.; Best, L.A. Measurement and Validity Characteristics of the Short Version of the Social and Emotional Loneliness Scale for Adults. Educ. Psychol. Meas. 2004, 64, 99–119. [Google Scholar] [CrossRef]
- DiTommaso, E.; Spinner, B. Social and emotional loneliness: A re-examination of weiss’ typology of loneliness. Pers. Individ. Dif. 1997, 22, 417–427. [Google Scholar] [CrossRef]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; Lawrence Erlbaum Associates Publishers: New York, NY, USA, 1988. [Google Scholar]
- Gross, J. Nortest: Tests for Normality. Available online: https://cran.r-project.org/web/packages/nortest/index.html (accessed on 22 January 2021).
- Stanley, D. Apatables: Create American Psychological Association (APA) Style Tables. Available online: https://cran.r-project.org/web/packages/apaTables/index.html (accessed on 20 January 2022).
- Kassambara, A. Rstatix: Pipe-Friendly Framework for Basic Statistical Tests. Available online: https://cran.r-project.org/web/packages/rstatix/index.html (accessed on 20 January 2022).
- Bliese, P. Multilevel: Multilevel Functions. Available online: https://cran.r-project.org/web/packages/multilevel/index.html (accessed on 20 January 2022).
- Flynn, T.C. What makes internship so bad—and so good. Pharos Alpha Omega Alpha Honor. Med. Soc. 1986, 49, 7–8. [Google Scholar]
- Butterfield, P.S. The Stress of Residency. Arch. Intern. Med. 1988, 148, 1428. [Google Scholar] [CrossRef]
- Gil-Calderón, J.; Alonso-Molero, J.; Dierssen-Sotos, T.; Gómez-Acebo, I.; Llorca, J. Burnout syndrome in Spanish medical students. BMC Med. Educ. 2021, 21, 231. [Google Scholar] [CrossRef]
- Santen, S.A.; Holt, D.B.; Kemp, J.D.; Hemphill, R.R. Burnout in medical students: Examining the prevalence and associated factors. South. Med. J. 2010, 103, 758–763. [Google Scholar] [CrossRef]
- Mian, A.; Kim, D.; Chen, D.; Ward, W.L. Medical Student and Resident Burnout: A Review of Causes, Effects, and Prevention. J. Fam. Med. Dis. Prev. 2018, 4, 1–8. [Google Scholar] [CrossRef]
- Marilaf Caro, M.; San-Martín, M.; Delgado-Bolton, R.; Vivanco, L. Empathy, loneliness, burnout, and life satisfaction in Chilean nurses of palliative care and homecare services | Empatía, soledad, desgaste y satisfacción personal en Enfermeras de cuidados paliativos y atención domiciliaria de Chile. Enfermería Clínica 2017, 27, 379–386. [Google Scholar] [CrossRef]
- Soler-Gonzalez, J.; San-Martín, M.; Delgado-Bolton, R.; Vivanco, L. Human connections and their roles in the occupational well-being of healthcare professionals: A study on loneliness and empathy. Front. Psychol. 2017, 8, 1475. [Google Scholar] [CrossRef]
- Lopes, A.R.; Nihei, O.K. Burnout among nursing students: Predictors and association with empathy and self-efficacy. Rev. Bras. Enferm. 2020, 73, e2018028. [Google Scholar] [CrossRef]
- Dyrbye, L.N.; Thomas, M.R.; Harper, W.; Massie, F.S.; Power, D.V.; Eacker, A.; Szydlo, D.W.; Novotny, P.J.; Sloan, J.A.; Shanafelt, T.D. The learning environment and medical student burnout: A multicentre study. Med. Educ. 2009, 43, 274–282. [Google Scholar] [CrossRef]
- Berduzco-Torres, N.; Medina, P.; Choquenaira-Callañaupa, B.; San-Martín, M.; Delgado Bolton, R.C.R.C.; Vivanco, L. Family Loneliness: Its Effects in the Development of Empathy, Teamwork and Lifelong Learning Abilities in Medical Students. Front. Psychol. 2020, 11, 2046. [Google Scholar] [CrossRef]
- Usán Supervía, P.; Salavera Bordás, C. Burnout, Goal Orientation and Academic Performance in Adolescent Students. Int. J. Environ. Res. Public Health 2020, 17, 6507. [Google Scholar] [CrossRef]
- Kachel, T.; Huber, A.; Strecker, C.; Höge, T.; Höfer, S. Development of Cynicism in Medical Students: Exploring the Role of Signature Character Strengths and Well-Being. Front. Psychol. 2020, 11, 328. [Google Scholar] [CrossRef] [PubMed]
- Haidet, P.; Stein, H.F. The role of the student-teacher relationship in the formation of physicians: The hidden curriculum as process. J. Gen. Intern. Med. 2006, 21, 16–20. [Google Scholar] [CrossRef] [PubMed]
- San-Martín, M.; Delgado-Bolton, R.; Vivanco, L. Role of a semiotics-based curriculum in empathy enhancement: A longitudinal study in three dominican medical schools. Front. Psychol. 2017, 8, 2018. [Google Scholar] [CrossRef] [PubMed]
- Fernández-Rodríguez, L.J.; Bardales-Zuta, V.H.; San-Martín, M.; Delgado Bolton, R.C.; Vivanco, L. Empathy Enhancement Based on a Semiotics Training Program: A Longitudinal Study in Peruvian Medical Students. Front. Psychol. 2020, 11, 2980. [Google Scholar] [CrossRef]
- Tuirán-Gutiérrez, G.J.; San-Martín, M.; Delgado-Bolton, R.; Bartolomé, B.; Vivanco, L. Improvement of Inter-Professional Collaborative Work Abilities in Mexican Medical and Nursing Students: A Longitudinal Study. Front. Psychol. 2019, 10, 5. [Google Scholar] [CrossRef]
- Shadid, A.; Shadid, A.M.; Shadid, A.; Almutairi, F.E.; Almotairi, K.E.; Aldarwish, T.; Alzamil, O.; Alkholaiwi, F.; Khan, S.-U.-D. Stress, Burnout, and Associated Risk Factors in Medical Students. Cureus 2020, 12, e6633. [Google Scholar] [CrossRef]
- Humphris, G.; Blinkhorn, A.; Freeman, R.; Gorter, R.; Hoad-Reddick, G.; Murtomaa, H.; O’Sullivan, R.; Splieth, C. Psychological stress in undergraduate dental students: Baseline results from seven European dental schools. Eur. J. Dent. Educ. 2002, 6, 22–29. [Google Scholar] [CrossRef]
- Hojat, M.; Veloski, J.J.; Gonnella, J.S. Measurement and correlates of physicians’ lifelong learning. Acad. Med. 2009, 84, 1066–1074. [Google Scholar] [CrossRef]
- López-Morales, H.; Rivera-Diaz, E.; Ore-Zuñiga, A.; Vera-Portilla, A.; San-Martín, M.; Delgado Bolton, R.C.; Vivanco, L. Positive Impact of Professionalism on the Perception of Global Well-Being: A Study in Healthcare Professionals Starting Their First Working Experience in Peruvian Rural Areas. Front. Public Health 2020, 8, 575774. [Google Scholar] [CrossRef]
- Alcorta-Garza, A.; San-Martín, M.; Delgado-Bolton, R.; Soler-González, J.; Roig, H.; Vivanco, L. Cross-Validation of the Spanish HP-Version of the Jefferson Scale of Empathy Confirmed with Some Cross-Cultural Differences. Front. Psychol. 2016, 7, 1002. [Google Scholar] [CrossRef][Green Version]
| Scales | n | PR | AR | M (SD) | Mdn | Reliability |
|---|---|---|---|---|---|---|
| MBI-GS | 171 | 0–96 | 4–80 | 37 (15) | 36 | 0.83 |
| Exhaustion | 179 | 0–30 | 0–30 | 18 (7) | 18 | 0.84 |
| Cynicism | 175 | 0–30 | 0–29 | 9 (7) | 8 | 0.75 |
| Professional Efficacy | 173 | 0–36 | 0–36 | 26 (6) | 27 | 0.77 |
| SELSA-S | 178 | 15–105 | 15–86 | 37 (14) | 37 | 0.82 |
| Family domain | 186 | 5–35 | 5–33 | 8 (5) | 6 | 0.84 |
| Romantic domain | 179 | 5–35 | 5–27 | 18 (10) | 21 | 0.89 |
| Social domain | 187 | 5–35 | 5–29 | 11 (5) | 9 | 0.84 |
| JSE-S | 182 | 20–140 | 65–138 | 105 (14) | 106 | 0.82 |
| JSAPNC | 181 | 15–60 | 29–59 | 47 (6) | 47 | 0.81 |
| JeffSPLL-MS | 176 | 14–56 | 24–53 | 42 (6) | 42 | 0.76 |
| MBI-GS | ||||
|---|---|---|---|---|
| Global Score | Exhaustion | Cynicism | Professional Efficacy | |
| Medical professionalism | ||||
| Empathy | −0.27 *** | −0.10 | −0.28 *** | +0.17 * |
| Teamwork | −0.10 | −0.01 | −0.20 ** | −0.05 |
| Lifelong learning | −0.36 *** | −0.16 * | −0.24 ** | +0.39 *** |
| Loneliness | ||||
| Global score | +0.14 | +0.07 | +0.08 | −0.12 |
| Family loneliness | +0.31 *** | +0.20 ** | +0.20 ** | −0.23 ** |
| Romantic loneliness | −0.04 | −0.02 | −0.08 | −0.02 |
| Social loneliness | +0.28 *** | +0.22 ** | +0.19 * | −0.16 * |
| Academic achievement | ||||
| Global course score | −0.06 | −0.10 | −0.13 | −0.03 |
| Course of studies | −0.06 | −0.13 | +0.003 | −0.06 |
| Age | −0.07 | −0.09 | −0.07 | +0.01 |
| Predictors | β | SE | t | p | VIF |
|---|---|---|---|---|---|
| Global burnout | |||||
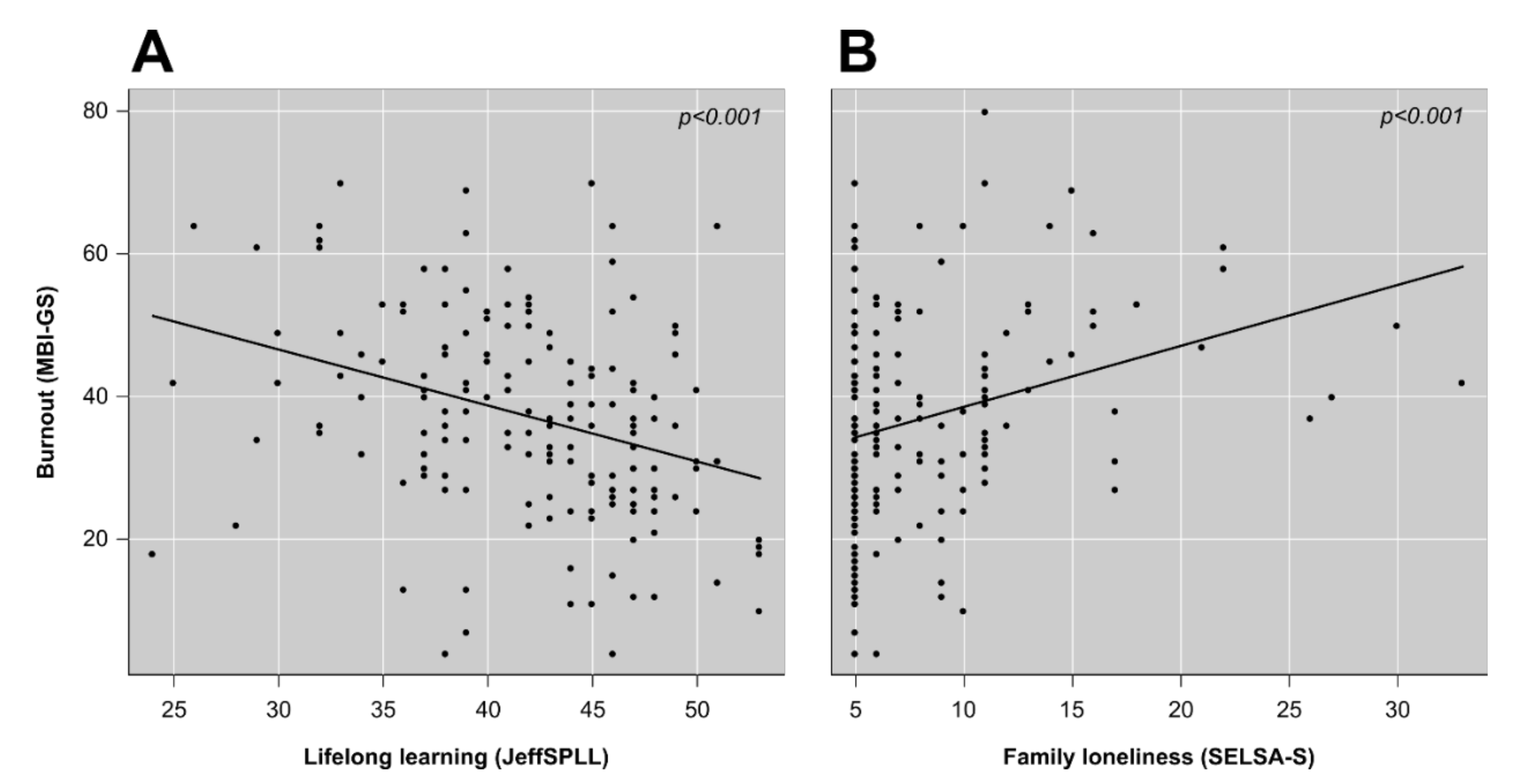
| Lifelong learning | −0.74 | 0.17 | −4.43 | <0.001 | 1.00 |
| Family loneliness | +0.77 | 0.20 | +3.87 | <0.001 | 1.00 |
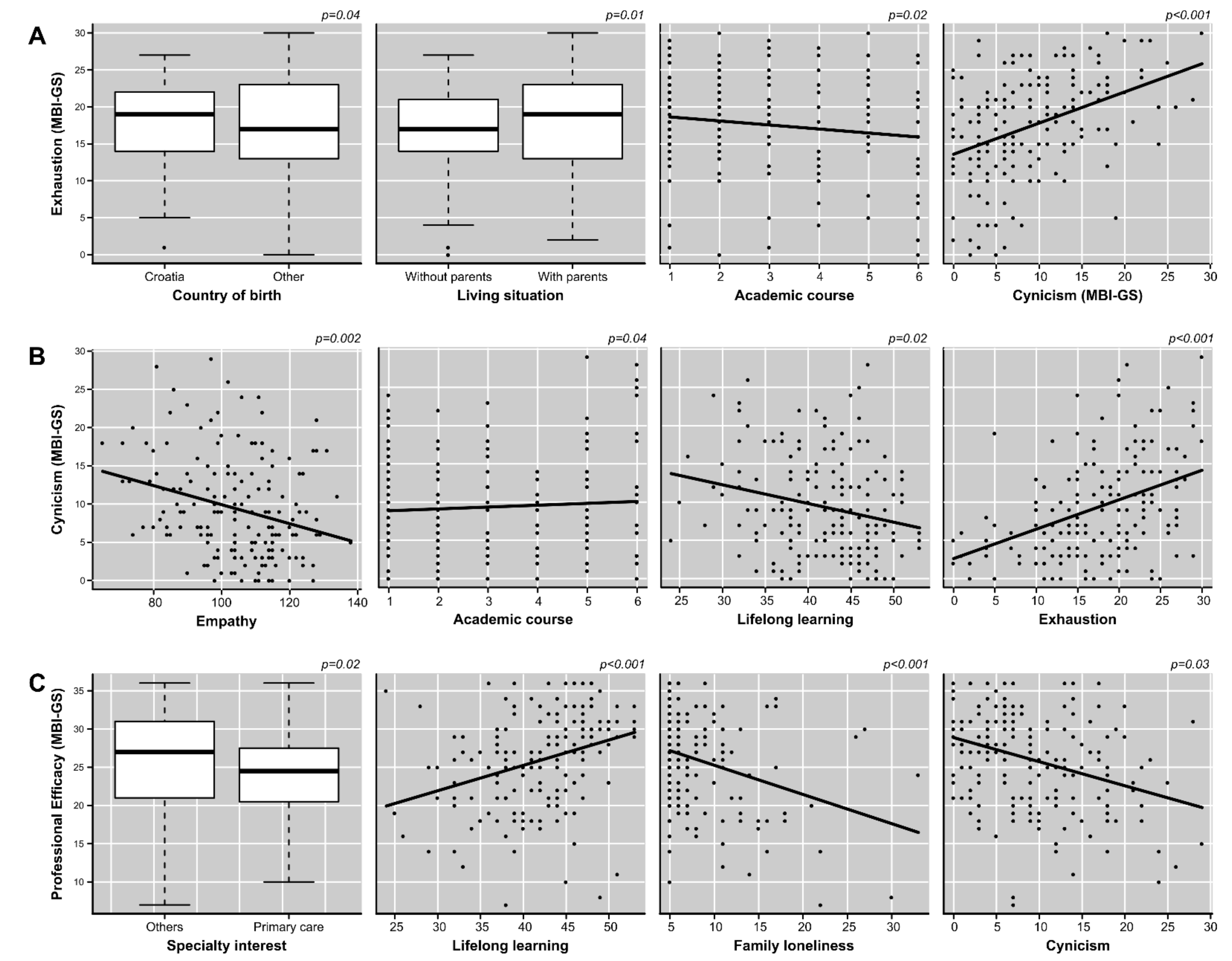
| Exhaustion domain | |||||
| Cynicism | +0.41 | 0.07 | +5.49 | <0.001 | 1.01 |
| Country of birth (different than Croatia) | −2.72 | 1.37 | −1.99 | 0.04 | 1.41 |
| Living with parents (yes) | +2.92 | 1.18 | +2.48 | 0.01 | 1.35 |
| Academic year | −0.66 | 0.29 | −2.27 | 0.02 | 1.08 |
| Cynicism domain | |||||
| Exhaustion | +0.34 | 0.07 | +5.22 | <0.001 | 1.04 |
| Empathy | −0.10 | 0.03 | −3.16 | 0.002 | 1.02 |
| Lifelong learning | −0.17 | 0.07 | −2.36 | 0.02 | 1.05 |
| Academic year | +0.51 | 0.26 | +1.98 | 0.04 | 1.03 |
| Professional efficacy | |||||
| Lifelong learning | +0.28 | 0.07 | +3.74 | <0.001 | 1.06 |
| Family loneliness | −0.35 | 0.09 | −3.89 | <0.001 | 1.08 |
| Speciality (Primary care) | −3.35 | 1.38 | −2.43 | 0.02 | 1.03 |
| Cynicism | −0.16 | 0.07 | −2.22 | 0.03 | 1.11 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gradiski, I.P.; Borovecki, A.; Ćurković, M.; San-Martín, M.; Delgado Bolton, R.C.; Vivanco, L. Burnout in International Medical Students: Characterization of Professionalism and Loneliness as Predictive Factors of Burnout. Int. J. Environ. Res. Public Health 2022, 19, 1385. https://doi.org/10.3390/ijerph19031385
Gradiski IP, Borovecki A, Ćurković M, San-Martín M, Delgado Bolton RC, Vivanco L. Burnout in International Medical Students: Characterization of Professionalism and Loneliness as Predictive Factors of Burnout. International Journal of Environmental Research and Public Health. 2022; 19(3):1385. https://doi.org/10.3390/ijerph19031385
Chicago/Turabian StyleGradiski, Ivan P., Ana Borovecki, Marko Ćurković, Montserrat San-Martín, Roberto C. Delgado Bolton, and Luis Vivanco. 2022. "Burnout in International Medical Students: Characterization of Professionalism and Loneliness as Predictive Factors of Burnout" International Journal of Environmental Research and Public Health 19, no. 3: 1385. https://doi.org/10.3390/ijerph19031385
APA StyleGradiski, I. P., Borovecki, A., Ćurković, M., San-Martín, M., Delgado Bolton, R. C., & Vivanco, L. (2022). Burnout in International Medical Students: Characterization of Professionalism and Loneliness as Predictive Factors of Burnout. International Journal of Environmental Research and Public Health, 19(3), 1385. https://doi.org/10.3390/ijerph19031385







