Parental Confidence in Relation to Antipyretic Use, Warning Signs, Symptoms and Well-Being in Fever Management—Results from an App-Based Registry
Abstract
1. Introduction
2. Methods
2.1. Study Design
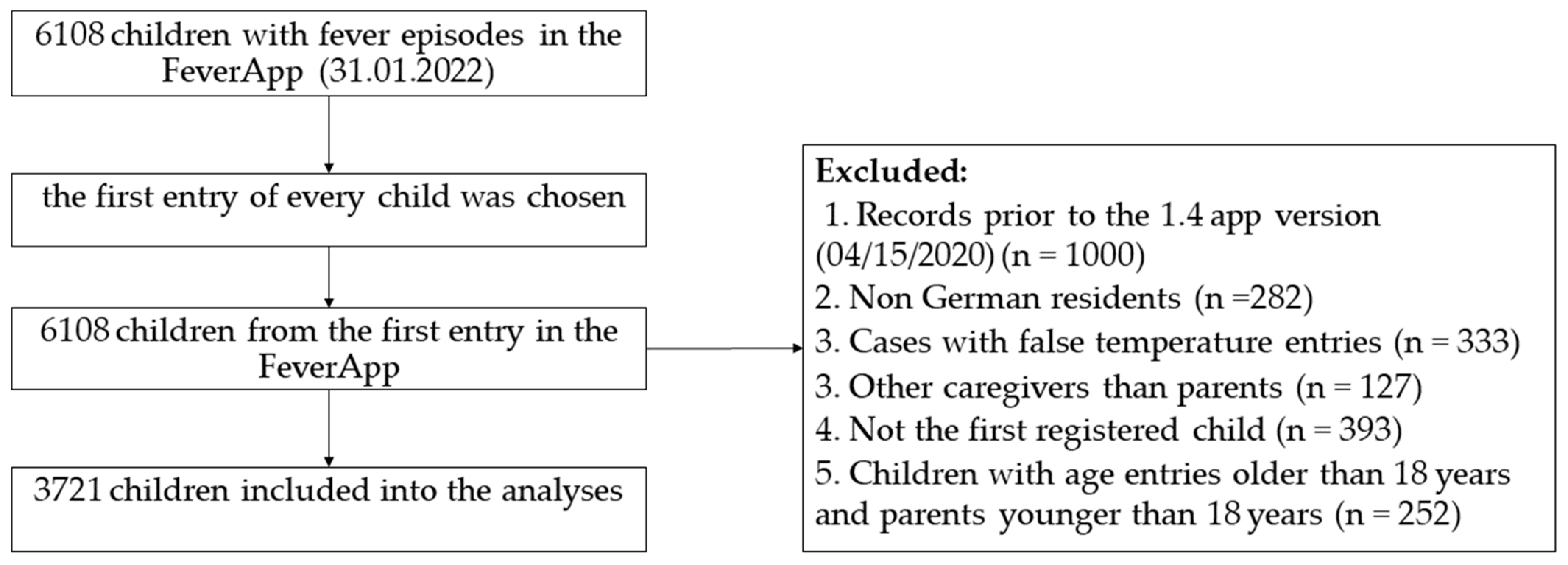
2.2. Sample Definition
2.3. Variable Selection
2.4. Variable Description
2.5. Statistical Analysis
3. Results
3.1. Descriptive Statistics
3.2. Logistic Regression with the Dependent Variable Parental Confidence
3.2.1. Bivariate Associations of Parental Confidence and Fever-Relevant Parameters
3.2.2. Multivariate Associations of Parental Confidence and Fever Relevant Parameters
3.3. Logistic Regression with the Dependent Variable Antipyretic Use
3.3.1. Bivariate Associations of Antipyretics Use and Fever Relevant Parameters
3.3.2. Multivariate Associations of Antipyretics Use and Fever-Relevant Parameters
4. Discussion
4.1. Aim of the Study and Discussion of Descriptive Analyses Results
4.2. Discussion of Bivariate and Multivariate Logistic Analyses Results
4.3. Strengths and Limitations of the Study
4.4. Implications for Future Research
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Jenetzky, E.; Schwarz, S.; Fingerhut, I.; Hamideh Kerdar, S.; Gwiasda, M.; Rathjens, L.; Kulikova, O.; Martin, D. Das FieberApp Register. Gesundheitswesen 2021, 83 (Suppl. S1), 4–11. [Google Scholar] [CrossRef]
- Martin, D.; Wachtmeister, J.; Ludwigs, K.; Jenetzky, E. The FeverApp registry—Ecological momentary assessment (EMA) of fever management in families regarding conformity to up-to-date recommendations. BMC Med. Inform. Decis. Mak. 2020, 20, 249. [Google Scholar] [CrossRef] [PubMed]
- Schmitt, B.D. Fever Phobia: Misconceptions of Parents about Fevers. Am. J. Dis. Child. 1980, 134, 176–181. [Google Scholar] [CrossRef] [PubMed]
- Kramer, M.S.; Naimark, L.; Leduc, D.G. Parental Fever Phobia and Its Correlates. Pediatrics 1985, 75, 1110–1113. [Google Scholar] [CrossRef] [PubMed]
- Blumenthal, I. What parents think of fever. Fam. Pract. 1998, 15, 513–518. [Google Scholar] [CrossRef]
- Crocetti, M.; Moghbeli, N.; Serwint, J. Fever Phobia Revisited: Have Parental Misconceptions about Fever Changed in 20 Years? Pediatrics 2001, 107, 1241–1246. [Google Scholar] [CrossRef]
- Karwowska, A.; Nijssen-Jordan, C.; Johnson, D.; Davies, H.D. Parental and health care provider understanding of childhood fever: A Canadian perspective. CJEM 2002, 4, 394–400. [Google Scholar] [CrossRef]
- Betz, M.G.; Grunfeld, A.F. ‘Fever Phobia’ in the Emergency Department: A Survey of Children’s Caregivers. Eur. J. Emerg. Med. 2009, 13, 129–133. [Google Scholar] [CrossRef]
- Gunduz, S.; Usak, E.; Koksal, T.; Canbal, M. Why Fever Phobia Is Still Common? Iran Red Crescent. Med. J. 2016, 18, e23827. [Google Scholar] [CrossRef]
- MacMahon, D.; Brabyn, C.; Dalziel, S.R.; McKinlay, C.J.; Tan, E. Fever phobia in caregivers presenting to New Zealand emergency deparments. Emerg. Med. Australas. 2021, 33, 1074–1081. [Google Scholar] [CrossRef]
- Langer, T.; Pfeifer, M.; Soenmez, A.; Tarhan, B.; Jeschke, E.; Ostermann, T. Fearful or Functional—A Cross-Sectional Survey of the Concepts of Childhood Fever among German and Turkish Mothers in Germany. BMC Pediatr. 2011, 11, 41. [Google Scholar] [CrossRef] [PubMed]
- Hamideh Kerdar, S.; Himbert, C.; Martin, D.; Jenetzky, E. Cross-Sectional Study of Parental Knowledge, Behaviour and Anxiety in Management of Paediatric Fever among German Parents. BMJ Open 2021, 11, e054742. [Google Scholar] [CrossRef] [PubMed]
- Purssell, E.; Collin, J. Fever Phobia: The Impact of Time and Mortality—A Systematic Review and Meta-Analysis. Int. J. Nurs. Stud. 2016, 56, 81–89. [Google Scholar] [CrossRef] [PubMed]
- Deutsche Gesellschaft für Kinder- und Jugendmedizin. “DGKJ_Fieber_18MeinKindhatFieber”. Available online: https://www.dgkj.de/eltern/dgkj-elterninformationen/elterninfo-fieber/ (accessed on 14 September 2022).
- El-Radhi, A.S.M. Fever management: Evidence vs current practice. World J. Clin. Pediatr. 2012, 1, 29–33. [Google Scholar] [CrossRef] [PubMed]
- Adeboye, A.; Rafeek, A.Y.; Olusimbo, K.I. Fever: A Literature Review of Perceptions, Perspectives and Practices. J. Tradit. Med. Clin. Naturopat. 2017, 6, 249. [Google Scholar] [CrossRef]
- Azab, S.M.; Hirshon, J.M.; Hayes, B.D.; El-Setouhy, M.; Smith, G.S.; Sakr, M.L.; Tawfik, H.; Klein-Schwartz, W. Epidemiology of acute poisoning in children presenting to the poisoning treatment center at Ain Shams university in Cairo, Egypt, 2009–2013. Clin. Toxicol. 2016, 54, 20–26. [Google Scholar] [CrossRef]
- Charkaluk, M.L.; Kalach, N.; El Kohen, R.; Kremp, O. Familial use of ibuprofen in febrile children: A prospective study in the emergency room of an hospital in Lille. Arch. Pediatr. 2005, 12, 1209–1214. [Google Scholar] [CrossRef]
- Rathjens, L.; Martin, D.; Hamideh Kerdar, S.; Gwiasda, M.; Schwarz, S.; Jenetzky, E. Data Completeness and Concordance in the FeverApp Registry: Comparative Study. JMIR Pediatr. Parent. 2022; accepted. [Google Scholar] [CrossRef]
- Ruud, N.; Oostenbrink, R.; Dons, E.; Bouwhuis, C.; Moll, H. Parental Fever Attitude and Management: Influence of Parental Ethnicity and Child’s Age. Pediatr. Emerg. Care 2010, 26, 339–342. [Google Scholar] [CrossRef]
- Walsh, A.; Edwards, H. Management of Childhood Fever by Parents: Literature Review. J. Adv. Nurs. 2006, 54, 217–227. [Google Scholar] [CrossRef]
- Field, A. Discovering Statistics Using SPSS, 4th ed.; Sage: London, UK, 2013; pp. 760–814. ISBN 978-1-4462-4917-8. [Google Scholar]
- Box, G.E.P.; Tidwell, P.W. Transformation of the Independent Variables. Technometrics 1962, 4, 531–550. [Google Scholar] [CrossRef]
- Destatis, Statistisches Bundesamt. Bevölkerung im Alter von 15 Jahren und mehr nach Allgemeinen und Beruflichen Bildungsabschlüssen nach Jahren. Available online: https://www.destatis.de/DE/Themen/Gesellschaft-Umwelt/Bildung-Forschung-Kultur/Bildungsstand/Tabellen/bildungsabschluss.html (accessed on 14 September 2022).
- Destatis, Statistisches Bundesamt. Bevölkerung und Erwerbstätigkeit Bevölkerung mit Migrationshintergrund—Ergebnisse des Mikrozensus 2019. Available online: https://www.bpb.de/medien/276613/destatis_Fachserie%201%20Reihe%202.2.pdf (accessed on 14 September 2022).
- Muijs, D. Doing Quantitative Research in Education with SPSS, 2nd ed.; Sage: London, UK, 2010; pp. 124–138. ISBN 978-1-84920-323-4. [Google Scholar]
- Jenetzky, E.; Kulikova, O.; Martin, D. Survey on Parental Fever Reduction with Antipyretics in Children. In Proceedings of the 65th Annual Meeting of the German Association for Medical Informatics, Biometry and Epidemiology (GMDS), Meeting of the Central European Network (CEN: German Region, Austro-Swiss Region and Polish Region) of the International Biometric Society (IBS), Berlin, Germany, 6–9 September 2020. [Google Scholar] [CrossRef]
- Cinar, N.D.; Altun, I.; Altınkaynak, S.; Walsh, A. Turkish Parents’ Management of Childhood Fever: A Cross-Sectional Survey Using the PFMS-TR. Aust. Emerg. Nurs. J. 2014, 17, 3–10. [Google Scholar] [CrossRef] [PubMed]
- Zyoud, S.H.; Al-Jabi, S.W.; Sweileh, W.M.; Nabulsi, M.M.; Tubaila, M.F.; Awang, R.; Sawalha, A.F. Beliefs and practices regarding childhood fever among parents: A cross-sectional study from Palestine. BMC Pediatr. 2013, 13, 66. [Google Scholar] [CrossRef]
- Niehues, T. The Febrile Child: Diagnosis and Treatment. Dtsch. Arztebl. Int. 2013, 110, 764–774. [Google Scholar] [CrossRef] [PubMed]
- Gwiasda, M.; Schwarz, S.; Büssing, A.; Jenetzky, E.; Krafft, H.; Hamideh Kerdar, S.; Rathjens, L.; Boehm, K.; Martin, D. Changing Knowledge and Attitudes about Childhood Fever: Testing a Video Instruction before Its Application in a Health App. GMS J. Med. Educ. 2022, 39, Doc25. [Google Scholar] [CrossRef]
- Taveras, E.M.; Durousseau, S.; Flores, G. Parents’ Beliefs and Practices Regarding Childhood Fever: A Study of a Multiethnic and Socioeconomically Diverse Sample of Parents. Pediatr. Emerg. Care 2004, 20, 579–587. [Google Scholar] [CrossRef]
- Schwarz, S.; Martin, D.; Büssing, A.; Kulikova, O.; Krafft, H.; Gwiasda, M.; Hamideh Kerdar, S.; Fingerhut, I.; Jenetzky, E. Sociodemographic Characteristics and Interests of FeverApp Users. Int. J. Environ. Res. Public Health 2021, 18, 3121. [Google Scholar] [CrossRef]

| Parents | n | Missings | |
|---|---|---|---|
| Age in years 1 (M, SD) | 33.96 (4.94) | 3721 | 0 |
| School degree 1 (%, n) | |||
| General qualification for university entrance | 51.1 (1903) | 3648 | 73 |
| Advanced technical college entrance qualification | 21.0 (783) | ||
| Intermediate school-leaving certificate | 20.7 (771) | ||
| Lower secondary school-leaving certificate | 4.6 (173) | ||
| none | 0.5 (18) | ||
| Migration background 1 (%, n) | 8.9 (330) | 3721 | 0 |
| Confidence in children’s fever management 2 (%, n) | 3530 | 191 | |
| very low–moderate | 39.8 (1481) | ||
| high–very high | 58.0 (2049) | ||
| Children | |||
| Female 1 (%, n) | 47.5 (1767) | 3721 | 0 |
| Age in months 1 (M, SD) | 20.92 (22.97) | 3721 | 0 |
| Fever episode in the last 12 months 1 (%, n) | 3355 | 366 | |
| Yes | 58.6 (1967) | ||
| No | 41.4 (1388) | ||
| Temperature 2 (%, n) | 3721 | 0 | |
| under 38.5 °C | 44.5 (1656) | ||
| 38.5 °C and over | 55.5 (2065) | ||
| Well-Being 2 (%, n) | 3343 | 378 | |
| very low–moderate | 82.3 (2751) | ||
| high–very high | 17.7 (592) | ||
| Warning signs 2 (%, n) | 18.9 (644) | 3405 | 316 |
| Rash 2 (%, n) | 4.8 (165) | 3465 | 256 |
| Diarrhea 2 (%, n) | 14.2 (508) | 3574 | 147 |
| Dehydration 2 (%, n) | 15.2 (527) | 3461 | 260 |
| Symptoms 2 (%, n) | 84.4 (2966) | 3514 | 207 |
| Pain 2 (%, n) | 44.6 (1050) | 2352 | 1369 |
| Pain imputed 2 (%, n) | 28.2 (1050) | 3721 | 0 |
| Antipyretics dose 2 (%, n) | 2513 | 1208 | |
| No | 85.3 (2144) | ||
| Yes | 14.7 (369) |
| Parental Confidence | |||||
|---|---|---|---|---|---|
| Low | High | n | OR [95% CI] | p-Value | |
| Parents | |||||
| Age in years (M, SD) | 33.76 (4.848) | 34.11 (5.023) | 3530 | 1.014 [1.001–1.028] | 0.041 |
| Higher school degree (%, n) | 53.4 (774) | 51.1 (1029) | 3463 | 0.913 [0.798–1.046] | 0.189 |
| Migration background (%, n) | 9.5 (140) | 8.3 (171) | 3530 | 0.872 [0.690–1.102] | 0.252 |
| Children | |||||
| Female (%, n) | 51.5 (763) | 44.2 (906) | 3530 | 0.746 [0.652–0.853] | <0.001 |
| Age 12 months and over (%, n) | 46.4 (687) | 58.2 (1192) | 3530 | 1.608 [1.405–1.839] | <0.001 |
| At least one fever episode in the last 12 months (%, n) | 52.3 (699) | 63.5 (1175) | 3187 | 1.589 [1.377–1.833] | <0.001 |
| Fever (%, n) | 60.9 (902) | 52.1 (1068) | 3530 | 0.699 [0.610–0.800] | <0.001 |
| High well-being (%, n) | 13.3 (181) | 20.6 (384) | 3226 | 1.693 [1.396–2.052] | <0.001 |
| Warning signs (%, n) | 26.3 (360) | 13.9 (274) | 3340 | 0.453 [0.380–0.539] | <0.001 |
| Rash (%, n) | 5.1 (72) | 4.5 (89) | 3384 | 0.875 [0.636–1.203] | 0.412 |
| Diarrhea/Vomiting (%, n) | 16.1 (234) | 13.1 (265) | 3485 | 0.783 [0.648–0.948] | 0.012 |
| Dehydration (%, n) | 19.8 (275) | 12.3 (244) | 3373 | 0.567 [0.470–0.685] | <0.001 |
| Symptoms (%, n) | 87.3 (1252) | 82.7 (1662) | 3444 | 0.694 [0.572–0.843] | <0.001 |
| Pain imputed (%, n) | 28.9 (428) | 28.7 (589) | 3530 | 0.993 [0.856–1.150] | 0.921 |
| Independent Variables | OR | 95% CI | p-Value |
|---|---|---|---|
| Constant | 2.389 | <0.001 | |
| Parents | |||
| Age in years | 0.992 | [0.976–1.009] | 0.382 |
| Children | |||
| Female | 0.770 | [0.655–0.906] | 0.002 |
| Age in Months 12 or older | 1.498 | [1.244–1.803] | <0.001 |
| At least one fever episode in the last 12 Months | 1.522 | [1.271–1.822] | <0.001 |
| Fever | 0.673 | [0.566–0.800] | <0.001 |
| High well-being | 1.252 | [0.993–1.580] | 0.058 |
| Warning signs | 0.494 | [0.401–0.608] | <0.001 |
| Diarrhea/Vomiting | 1.055 | [0.837–1.330] | 0.649 |
| Dehydration | 0.646 | [0.515–0.811] | <0.001 |
| Symptoms | 0.814 | [0.640–1.035] | 0.093 |
| Use of Antipyretics | |||||
|---|---|---|---|---|---|
| No | Yes | n | OR [95% CI] | p-Value | |
| Parents | |||||
| Age in years (M, SD) | 33.88 (4.928) | 33.91 (4.555) | 2513 | 1.001 [0.979–1.024] | 0.923 |
| Higher school degree (%, n) | 54.6 (1154) | 51.3 (184) | 2474 | 0.876 [0.700–1.095] | 0.245 |
| Migration background (%, n) | 8.0 (172) | 8.7 (32) | 2513 | 1.089 [0.734–1.615] | 0.673 |
| High confidence (%, n) | 61.4 (1291) | 54.4 (196) | 2464 | 0.753 [0.601–0.943] | 0.013 |
| Children | |||||
| Female (%, n) | 47.8 (1024) | 50.1 (185) | 2513 | 1.100 [0.882–1.372] | 0.399 |
| Age 12 months and over (%, n) | 47.5 (1019) | 60.4 (223) | 2513 | 1.686 [1.346–2.112] | <0.001 |
| At least one fever episode in the last 12 months (%, n) | 52.4 (1002) | 68.1 (233) | 2256 | 1.946 [1.524–2.484] | <0.001 |
| Fever (%, n) | 46.4 (995) | 75.1 (277) | 2513 | 3.477 [2.706–4.467] | <0.001 |
| High well-being (%, n) | 22.5 (441) | 6.4 (21) | 2289 | 0.234 [0.148–0.369] | <0.001 |
| Warning signs (%, n) | 14.4 (295) | 24.0 (81) | 2383 | 1.878 [1.421–2.482] | <0.001 |
| Rash | 4.7 (96) | 5.1 (18) | 2400 | 1.100 [0.656–1.843] | 0.719 |
| Diarrhea/Vomiting | 12.0 (254) | 14.5 (52) | 2474 | 1.241 [0.900–1.712] | 0.189 |
| Dehydration | 13.6 (278) | 19.3 (67) | 2392 | 1.521 [1.132–2.043] | 0.005 |
| Symptoms (%, n) | 80.8 (1685) | 90.2 (323) | 2443 | 2.191 [1.520–3.157] | <0.001 |
| Pain imputed (%, n) | 24.1 (517) | 34.4 (127) | 2513 | 1.652 [1.304–2.092] | <0.001 |
| Independent Variables | OR | 95% CI | p-Value |
|---|---|---|---|
| Constant | 0.063 | <0.001 | |
| Parents | |||
| High confidence | 0.726 | [0.550–0960] | 0.024 |
| Children | |||
| Age in Months 12 or older | 1.015 | [0.752–1.371] | 0.920 |
| At least one fever episode in the last 12 Months | 1.775 | [1.300–2.425] | <0.001 |
| Fever | 2.576 | [1.897–3.500] | <0.001 |
| High well-being | 0.373 | [0.220–0.632] | <0.001 |
| Warning signs | 1.501 | [1.078–2.090] | 0.016 |
| Dehydration | 0.880 | [0.606–1.278] | 0.502 |
| Symptoms | 1.308 | [0.835–2.048] | 0.241 |
| Pain imputed | 1.235 | [0.922–1.654] | 0.157 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Möhler, R.; Jenetzky, E.; Schwarz, S.; Gwiasda, M.; Rathjens, L.; Szoke, H.; Martin, D. Parental Confidence in Relation to Antipyretic Use, Warning Signs, Symptoms and Well-Being in Fever Management—Results from an App-Based Registry. Int. J. Environ. Res. Public Health 2022, 19, 14502. https://doi.org/10.3390/ijerph192114502
Möhler R, Jenetzky E, Schwarz S, Gwiasda M, Rathjens L, Szoke H, Martin D. Parental Confidence in Relation to Antipyretic Use, Warning Signs, Symptoms and Well-Being in Fever Management—Results from an App-Based Registry. International Journal of Environmental Research and Public Health. 2022; 19(21):14502. https://doi.org/10.3390/ijerph192114502
Chicago/Turabian StyleMöhler, Ricarda, Ekkehart Jenetzky, Silke Schwarz, Moritz Gwiasda, Larisa Rathjens, Henrik Szoke, and David Martin. 2022. "Parental Confidence in Relation to Antipyretic Use, Warning Signs, Symptoms and Well-Being in Fever Management—Results from an App-Based Registry" International Journal of Environmental Research and Public Health 19, no. 21: 14502. https://doi.org/10.3390/ijerph192114502
APA StyleMöhler, R., Jenetzky, E., Schwarz, S., Gwiasda, M., Rathjens, L., Szoke, H., & Martin, D. (2022). Parental Confidence in Relation to Antipyretic Use, Warning Signs, Symptoms and Well-Being in Fever Management—Results from an App-Based Registry. International Journal of Environmental Research and Public Health, 19(21), 14502. https://doi.org/10.3390/ijerph192114502







