Positive Psychology Approaches to Interventions for Cancer Dyads: A Scoping Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Definition of PPA and Scope of Review
2.2. Information Sources and Search Strategy
2.3. Eligibility Criteria
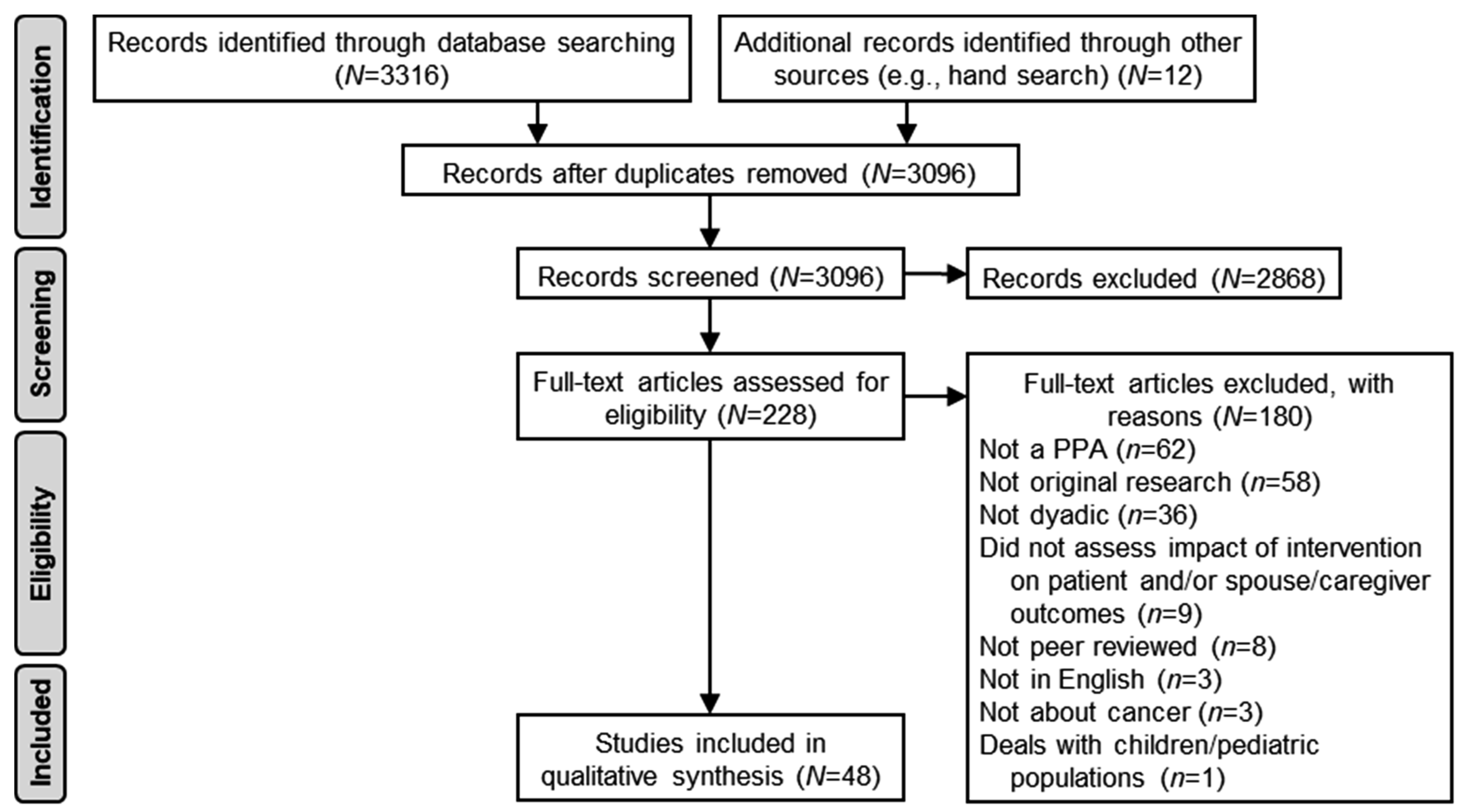
2.4. Study Selection Process
3. Results
3.1. Positive Psychology Approaches: Intervention Content
3.2. Outcomes Assessed
4. Discussion
4.1. Limitations and Future Directions
4.2. Clinical Implications
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Islami, F.; Ward, E.M.; Sung, H.; Cronin, K.A.; Tangka, F.K.L.; Sherman, R.L.; Zhao, J.; Anderson, R.N.; Henley, S.J.; Yabroff, K.R.; et al. Annual Report to the Nation on the Status of Cancer, Part 1: National Cancer Statistics. J. Natl. Cancer Inst. 2021, 113, 1648–1669. [Google Scholar] [CrossRef]
- Ellis, K.R.; Janevic, M.R.; Kershaw, T.; Caldwell, C.H.; Janz, N.K.; Northouse, L. Engagement in health-promoting behaviors and patient–caregiver interdependence in dyads facing advanced cancer: An exploratory study. J. Behav. Med. 2017, 40, 506–519. [Google Scholar] [CrossRef] [PubMed]
- Kelley, D.E.; Kent, E.E.; Litzelman, K.; Mollica, M.A.; Rowland, J.H. Dyadic associations between perceived social support and cancer patient and caregiver health: An actor-partner interdependence modeling approach. Psycho-Oncology 2019, 28, 1453–1460. [Google Scholar] [CrossRef] [PubMed]
- Teo, I.; Krishnan, A.; Lee, G.L. Psychosocial interventions for advanced cancer patients: A systematic review. Psycho-Oncology 2019, 28, 1394–1407. [Google Scholar] [CrossRef]
- Ahn, S.; Romo, R.; Campbell, C.L. A systematic review of interventions for family caregivers who care for patients with advanced cancer at home. Patient Educ. Couns. 2020, 103, 1518–1530. [Google Scholar] [CrossRef]
- Kershaw, T.; Ellis, K.R.; Yoon, H.; Schafenacker, A.; Katapodi, M.; Northouse, L. The Interdependence of Advanced Cancer Patients’ and Their Family Caregivers’ Mental Health, Physical Health, and Self-Efficacy over Time. Ann. Behav. Med. 2015, 49, 901–911. [Google Scholar] [CrossRef] [PubMed]
- Badr, H.; Bakhshaie, J.; Chhabria, K. Dyadic Interventions for Cancer Survivors and Caregivers: State of the Science and New Directions. Semin. Oncol. Nurs. 2019, 35, 337–341. [Google Scholar] [CrossRef] [PubMed]
- Hu, Y.; Liu, T.; Li, F. Association between dyadic interventions and outcomes in cancer patients: A meta-analysis. Support. Care Cancer 2019, 27, 745–761. [Google Scholar] [CrossRef] [PubMed]
- American Psychological Association. APA Dictionary of Psychology; American Psychological Association: Worcester, MA, USA, 2020. [Google Scholar]
- Seligman, M.E.P.; Steen, T.A.; Park, N.; Peterson, C. Positive Psychology Progress: Empirical Validation of Interventions. Am. Psychol. 2005, 60, 410–421. [Google Scholar] [CrossRef]
- Sin, N.L.; Lyubomirsky, S. Enhancing well-being and alleviating depressive symptoms with positive psychology interventions: A practice-friendly meta-analysis. J. Clin. Psychol. 2009, 65, 467–487. [Google Scholar] [CrossRef] [PubMed]
- Seligman, M.E. Flourish: The New Positive Psychology and the Search for Well-Being; Free Press: New York, NY, USA, 2011. [Google Scholar]
- Seligman, M. PERMA and the building blocks of well-being. J. Posit. Psychol. 2017, 13, 333–335. [Google Scholar] [CrossRef]
- Bolier, L.; Haverman, M.; Westerhof, G.J.; Riper, H.; Smit, F.; Bohlmeijer, E. Positive psychology interventions: A meta-analysis of randomized controlled studies. BMC Public Health 2013, 13, 119. [Google Scholar] [CrossRef] [PubMed]
- Terrill, A.L.; Reblin, M.; MacKenzie, J.J.; Cardell, B.; Einerson, J.; Berg, C.A.; Majersik, J.J.; Richards, L. Development of a novel positive psychology-based intervention for couples post-stroke. Rehabil. Psychol. 2018, 63, 43–54. [Google Scholar] [CrossRef]
- Alschuler, K.N.; Arewasikporn, A.; Nelson, I.K.; Molton, I.R.; Ehde, D.M. Promoting resilience in individuals aging with multiple sclerosis: Results from a pilot randomized controlled trial. Rehabil. Psychol. 2018, 63, 338–348. [Google Scholar] [CrossRef] [PubMed]
- Cohn, M.A.; Pietrucha, M.E.; Saslow, L.R.; Hult, J.R.; Moskowitz, J.T. An online positive affect skills intervention reduces depression in adults with type 2 diabetes. J. Posit. Psychol. 2014, 9, 523–534. [Google Scholar] [CrossRef]
- Müller, R.; Gertz, K.J.; Molton, I.R.; Terrill, A.L.; Bombardier, C.H.; Ehde, D.M.; Jensen, M.P. Effects of a Tailored Positive Psychology Intervention on Well-Being and Pain in Individuals With Chronic Pain and a Physical Disability: A Feasibility Trial. Clin. J. Pain 2016, 32, 32–44. [Google Scholar] [CrossRef] [PubMed]
- Cohn, M.A.; Fredrickson, B.L. In search of durable positive psychology interventions: Predictors and consequences of long-term positive behavior change. J. Posit. Psychol. 2010, 5, 355–366. [Google Scholar] [CrossRef] [PubMed]
- van der Spek, N.; Vos, J.; van Uden-Kraan, C.F.; Breitbart, W.; Cuijpers, P.; Holtmaat, K.; Witte, B.I.; Tollenaar, R.A.E.M.; Verdonck-de Leeuw, I.M. Efficacy of meaning-centered group psychotherapy for cancer survivors: A randomized controlled trial. Psychol Med. 2017, 47, 1990–2001. [Google Scholar] [CrossRef] [PubMed]
- Otto, A.K.; Szczesny, E.C.; Soriano, E.C.; Laurenceau, J.-P.; Siegel, S.D. Effects of a randomized gratitude intervention on death-related fear of recurrence in breast cancer survivors. Health Psychol. 2016, 35, 1320–1328. [Google Scholar] [CrossRef]
- Casellas-Grau, A.; Font, A.; Vives, J. Positive psychology interventions in breast cancer. A systematic review. Psycho-Oncology 2013, 23, 9–19. [Google Scholar] [CrossRef]
- Jacobs, J.M.; Shaffer, K.M.; Nipp, R.D.; Fishbein, J.; MacDonald, J.; El-Jawahri, A.; Pirl, W.; Jackson, V.A.; Park, E.R.; Temel, J.S.; et al. Distress is Interdependent in Patients and Caregivers with Newly Diagnosed Incurable Cancers. Ann. Behav. Med. 2017, 51, 519–531. [Google Scholar] [CrossRef] [PubMed]
- Hou, W.K.; Liang, L.; Lau, K.M.; Hall, M. Savouring and psychological well-being in family dyads coping with cancer: An actor–partner interdependence model. Eur. J. Cancer Care 2019, 28, e13047. [Google Scholar] [CrossRef] [PubMed]
- Alex, L.P.; Joseph, S.; Harrington, S.; Wood, A.M. Positive psychology: Past, present, and (possible) future. J. Posit. Psychol. 2006, 1, 3–16. [Google Scholar] [CrossRef]
- Rashid, T.; Seligman, M.P. Positive Psychotherapy: Clinician Manual; Oxford University Press: Oxford, UK, 2018. [Google Scholar]
- Allen, J.G.; Romate, J.; Rajkumar, E. Mindfulness-based positive psychology interventions: A systematic review. BMC Psychol. 2021, 9, 116. [Google Scholar] [CrossRef] [PubMed]
- Peters, M.D.J.; Godfrey, C.M.; Khalil, H.; McInerney, P.; Parker, D.; Soares, C.B. Guidance for conducting systematic scoping reviews. Int. J. Evid. Based Healthc. 2015, 13, 141–146. [Google Scholar] [CrossRef]
- Harden, J.; Falahee, M.; Bickes, J.; Schafenacker, A.; Walker, J.; Mood, D.; Northouse, L. Factors associated with prostate cancer patients’ and their spouses’ satisfaction with a family-based intervention. Cancer Nurs. 2009, 32, 482–492. [Google Scholar] [CrossRef]
- Lapid, M.I.; Atherton, P.J.; Kung, S.; Sloan, J.A.; Shahi, V.; Clark, M.M.; Rummans, T.A. Cancer caregiver quality of life: Need for targeted intervention. Psycho-Oncology 2016, 25, 1400–1407. [Google Scholar] [CrossRef]
- Martinez, K.A.; Friese, C.; Kershaw, T.; Given, C.W.; Fendrick, A.M.; Northouse, L. Effect of a Nurse-Led Psychoeducational Intervention on Healthcare Service Utilization Among Adults With Advanced Cancer. Oncol. Nurs. Forum 2015, 42, E310–E318. [Google Scholar] [CrossRef][Green Version]
- McMillan, S.C.; Small, B.J. Using the COPE intervention for family caregivers to improve symptoms of hospice homecare patients: A clinical trial. Oncol. Nurs. Forum 2007, 34, 313–321. [Google Scholar] [CrossRef][Green Version]
- Piderman, K.M.; Johnson, M.E.; Frost, M.H.; Atherton, P.J.; Satele, D.V.; Clark, M.M.; Lapid, M.I.; Sloan, J.A.; Rummans, T.A. Spiritual quality of life in advanced cancer patients receiving radiation therapy. Psycho-Oncology 2014, 23, 216–221. [Google Scholar] [CrossRef]
- Winger, J.G.; Rand, K.L.; Hanna, N.; Jalal, S.I.; Einhorn, L.H.; Birdas, T.J.; Ceppa, D.P.; Kesler, K.A.; Champion, V.L.; Mosher, C.E. Coping Skills Practice and Symptom Change: A Secondary Analysis of a Pilot Telephone Symptom Management Intervention for Lung Cancer Patients and Their Family Caregivers. J. Pain Symptom Manag. 2018, 55, 1341–1349.e1344. [Google Scholar] [CrossRef] [PubMed]
- Titler, M.G.; Shuman, C.; Dockham, B.; Harris, M.; Northouse, L. Acceptability of a Dyadic Psychoeducational Intervention for Patients and Caregivers. Oncol. Nurs. Forum 2020, 47, 342–351. [Google Scholar] [CrossRef] [PubMed]
- Cottingham, A.H.; Beck-Coon, K.; Bernat, J.K.; Helft, P.R.; Schmidt, K.; Shields, C.G.; Torke, A.M.; Johns, S.A. Addressing personal barriers to advance care planning: Qualitative investigation of a mindfulness-based intervention for adults with cancer and their family caregivers. Palliat. Support. Care 2019, 17, 276–285. [Google Scholar] [CrossRef] [PubMed]
- Lau, B.H.P.; Chow, A.Y.M.; Ng, T.K.; Fung, Y.L.; Lam, T.C.; So, T.H.; Chan, J.S.M.; Chan, C.H.Y.; Zhou, J.; Tam, M.Y.J.; et al. Comparing the efficacy of integrative body-mind-spirit intervention with cognitive behavioral therapy in patient-caregiver parallel groups for lung cancer patients using a randomized controlled trial. J. Psychosoc. Oncol. 2020, 38, 389–405. [Google Scholar] [CrossRef]
- Xiu, D.; Fung, Y.L.; Lau, B.H.; Wong, D.F.K.; Chan, C.H.Y.; Ho, R.T.H.; So, T.H.; Lam, T.C.; Lee, V.H.; Lee, A.W.M.; et al. Comparing dyadic cognitive behavioral therapy (CBT) with dyadic integrative body-mind-spirit intervention (I-BMS) for Chinese family caregivers of lung cancer patients: A randomized controlled trial. Support. Care Cancer 2020, 28, 1523–1533. [Google Scholar] [CrossRef]
- Li, Q.; Xu, Y.; Zhou, H.; Loke, A.Y. A couple-based complex intervention for Chinese spousal caregivers and their partners with advanced cancer: An intervention study. Psycho-Oncology 2015, 24, 1423–1431. [Google Scholar] [CrossRef]
- Mosher, C.E.; Secinti, E.; Hirsh, A.T.; Hanna, N.; Einhorn, L.H.; Jalal, S.I.; Durm, G.; Champion, V.L.; Johns, S.A. Acceptance and commitment therapy for symptom interference in advanced lung cancer and caregiver distress: A pilot randomized trial. J. Pain Symptom Manag. 2019, 58, 632–644. [Google Scholar] [CrossRef]
- Milbury, K.; Weathers, S.-P.; Durrani, S.; Li, Y.; Whisenant, M.; Li, J.; Lim, B.; Weinberg, J.S.; Kesler, S.R.; Cohen, L. Online couple-based meditation intervention for patients with primary or metastatic brain tumors and their partners: Results of a pilot randomized controlled trial. J. Pain Symptom Manag. 2020, 59, 1260–1267. [Google Scholar] [CrossRef]
- Saita, E.; Acquati, C.; Molgora, S. Promoting Patient and Caregiver Engagement to Care in Cancer. Front. Psychol. 2016, 7, 1660. [Google Scholar] [CrossRef]
- Collins, A.L.; Love, A.W.; Bloch, S.; Street, A.F.; Duchesne, G.M.; Dunai, J.; Couper, J.W. Cognitive existential couple therapy for newly diagnosed prostate cancer patients and their partners: A descriptive pilot study. Psycho-Oncology 2013, 22, 465–469. [Google Scholar] [CrossRef]
- Couper, J.; Collins, A.; Bloch, S.; Street, A.; Duchesne, G.; Jones, T.; Olver, J.; Love, A. Cognitive existential couple therapy (CECT) in men and partners facing localised prostate cancer: A randomised controlled trial. BJU Int. 2015, 115, 35–45. [Google Scholar] [CrossRef]
- McMillan, S.C.; Small, B.J.; Weitzner, M.; Schonwetter, R.; Tittle, M.; Moody, L.; Haley, W.E. Impact of coping skills intervention with family caregivers of hospice patients with cancer: A randomized clinical trial. Cancer 2006, 106, 214–222. [Google Scholar] [CrossRef]
- Meyers, F.J.; Carducci, M.; Loscalzo, M.J.; Linder, J.; Greasby, T.; Beckett, L.A. Effects of a problem-solving intervention (COPE) on quality of life for patients with advanced cancer on clinical trials and their caregivers: Simultaneous care educational intervention (SCEI): Linking palliation and clinical trials. J. Palliat. Med. 2011, 14, 465–473. [Google Scholar] [CrossRef] [PubMed]
- Gremore, T.M.; Brockstein, B.; Porter, L.S.; Brenner, S.; Benfield, T.; Baucom, D.H.; Sher, T.G.; Atkins, D. Couple-based communication intervention for head and neck cancer: A randomized pilot trial. Support. Care Cancer 2021, 29, 3267–3275. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.; Chen, J.; Wang, Y.; Xu, W.; Xie, M.; Wu, Y.; Hu, R. Effects of family participatory dignity therapy on the psychological well-being and family function of patients with haematologic malignancies and their family caregivers: A randomised controlled trial. Int. J. Nurs. Stud. 2021, 118, 103922. [Google Scholar] [CrossRef]
- Milbury, K.; Mallaiah, S.; Mahajan, A.; Armstrong, T.; Weathers, S.P.; Moss, K.E.; Goktepe, N.; Spelman, A.; Cohen, L. Yoga Program for High-Grade Glioma Patients Undergoing Radiotherapy and Their Family Caregivers. Integr. Cancer Ther. 2018, 17, 332–336. [Google Scholar] [CrossRef]
- Milbury, K.; Li, J.; Weathers, S.P.; Mallaiah, S.; Armstrong, T.; Li, Y.; Bruera, E.; Cohen, L. Pilot randomized, controlled trial of a dyadic yoga program for glioma patients undergoing radiotherapy and their family caregivers. Neurooncol. Pract. 2019, 6, 311–320. [Google Scholar] [CrossRef] [PubMed]
- Milbury, K.; Liao, Z.; Shannon, V.; Mallaiah, S.; Nagarathna, R.; Li, Y.; Yang, C.; Carmack, C.; Bruera, E.; Cohen, L. Dyadic yoga program for patients undergoing thoracic radiotherapy and their family caregivers: Results of a pilot randomized controlled trial. Psycho-Oncology 2019, 28, 615–621. [Google Scholar] [CrossRef] [PubMed]
- Manne, S.L.; Siegel, S.D.; Heckman, C.J.; Kashy, D.A. A randomized clinical trial of a supportive versus a skill-based couple-focused group intervention for breast cancer patients. J. Consult. Clin. Psychol. 2016, 84, 668–681. [Google Scholar] [CrossRef] [PubMed]
- Northouse, L.L.; Walker, J.; Schafenacker, A.; Mood, D.; Mellon, S.; Galvin, E.; Harden, J.; Freeman-Gibb, L. A family-based program of care for women with recurrent breast cancer and their family members. Oncol. Nurs. Forum 2002, 29, 1411–1419. [Google Scholar] [CrossRef]
- Northouse, L.; Kershaw, T.; Mood, D.; Schafenacker, A. Effects of a family intervention on the quality of life of women with recurrent breast cancer and their family caregivers. Psycho-Oncol. J. Psychol. Soc. Behav. Dimens. Cancer 2005, 14, 478–491. [Google Scholar] [CrossRef]
- Northouse, L.L.; Mood, D.W.; Schafenacker, A.; Montie, J.E.; Sandler, H.M.; Forman, J.D.; Hussain, M.; Pienta, K.J.; Smith, D.C.; Kershaw, T. Randomized clinical trial of a family intervention for prostate cancer patients and their spouses. Cancer 2007, 110, 2809–2818. [Google Scholar] [CrossRef] [PubMed]
- Northouse, L.L.; Mood, D.W.; Schafenacker, A.; Kalemkerian, G.; Zalupski, M.; LoRusso, P.; Hayes, D.F.; Hussain, M.; Ruckdeschel, J.; Fendrick, A.M. Randomized clinical trial of a brief and extensive dyadic intervention for advanced cancer patients and their family caregivers. Psycho-Oncology 2013, 22, 555–563. [Google Scholar] [CrossRef] [PubMed]
- Northouse, L.; Schafenacker, A.; Barr, K.L.; Katapodi, M.; Yoon, H.; Brittain, K.; Song, L.; Ronis, D.L.; An, L. A tailored Web-based psychoeducational intervention for cancer patients and their family caregivers. Cancer Nurs. 2014, 37, 321–330. [Google Scholar] [CrossRef]
- Dockham, B.; Schafenacker, A.; Yoon, H.; Ronis, D.L.; Kershaw, T.; Titler, M.; Northouse, L. Implementation of a psychoeducational program for cancer survivors and family caregivers at a cancer support community affiliate: A pilot effectiveness study. Cancer Nurs. 2016, 39, 169–180. [Google Scholar] [CrossRef] [PubMed]
- Titler, M.G.; Visovatti, M.A.; Shuman, C.; Ellis, K.R.; Banerjee, T.; Dockham, B.; Yakusheva, O.; Northouse, L. Effectiveness of implementing a dyadic psychoeducational intervention for cancer patients and family caregivers. Support. Care Cancer 2017, 25, 3395–3406. [Google Scholar] [CrossRef] [PubMed]
- Chen, H.L.; Annie Kao, T.S.; Reuille, K.M.; Northouse, L. FOCUS Program: Treating Patients With Cancer and Family Caregivers as a Unit of Care. Clin. J. Oncol. Nurs. 2021, 25, E17–E25. [Google Scholar] [CrossRef] [PubMed]
- Birnie, K.; Garland, S.N.; Carlson, L.E. Psychological benefits for cancer patients and their partners participating in mindfulness-based stress reduction (MBSR). Psycho-Oncology 2010, 19, 1004–1009. [Google Scholar] [CrossRef]
- Lengacher, C.A.; Kip, K.E.; Barta, M.; Post-White, J.; Jacobsen, P.B.; Groer, M.; Lehman, B.; Moscoso, M.S.; Kadel, R.; Le, N.; et al. A pilot study evaluating the effect of mindfulness-based stress reduction on psychological status, physical status, salivary cortisol, and interleukin-6 among advanced-stage cancer patients and their caregivers. J. Holist. Nurs. 2012, 30, 170–185. [Google Scholar] [CrossRef]
- Johns, S.A.; Beck-Coon, K.; Stutz, P.V.; Talib, T.L.; Chinh, K.; Cottingham, A.H.; Schmidt, K.; Shields, C.; Stout, M.E.; Stump, T.E.; et al. Mindfulness Training Supports Quality of Life and Advance Care Planning in Adults With Metastatic Cancer and Their Caregivers: Results of a Pilot Study. Am. J. Hosp. Palliat. Care 2020, 37, 88–99. [Google Scholar] [CrossRef] [PubMed]
- Chien, C.H.; Chung, H.J.; Liu, K.L.; Pang, S.T.; Wu, C.T.; Chang, Y.H.; Huang, X.Y.; Chang, Y.H.; Lin, T.P.; Lin, W.Y.; et al. Effectiveness of a couple-based psychosocial intervention on patients with prostate cancer and their partners: A quasi-experimental study. J. Adv. Nurs. 2020, 76, 2572–2585. [Google Scholar] [CrossRef] [PubMed]
- Song, L.; Rini, C.; Deal, A.M.; Nielsen, M.E.; Chang, H.; Kinneer, P.; Teal, R.; Johnson, D.C.; Dunn, M.W.; Mark, B.; et al. Improving Couples’ Quality of Life Through a Web-Based Prostate Cancer Education Intervention. Oncol. Nurs. Forum 2015, 42, 183–192. [Google Scholar] [CrossRef] [PubMed]
- Kayser, K.; Feldman, B.N.; Borstelmann, N.A.; Daniels, A.A. Effects of a randomized couple-based intervention on quality of life of breast cancer patients and their partners. Soc. Work Res. 2010, 34, 20–32. [Google Scholar] [CrossRef]
- Bevans, M.; Castro, K.; Prince, P.; Shelburne, N.; Prachenko, O.; Loscalzo, M.; Soeken, K.; Zabora, J. An individualized dyadic problem-solving education intervention for patients and family caregivers during allogeneic HSCT: A feasibility study. Cancer Nurs. 2010, 33, E24. [Google Scholar] [CrossRef] [PubMed]
- Baucom, D.H.; Porter, L.S.; Kirby, J.S.; Gremore, T.M.; Wiesenthal, N.; Aldridge, W.; Fredman, S.J.; Stanton, S.E.; Scott, J.L.; Halford, K.W. A couple-based intervention for female breast cancer. Psycho-Oncol. J. Psychol. Soc. Behav. Dimens. Cancer 2009, 18, 276–283. [Google Scholar] [CrossRef] [PubMed]
- Robertson, J.; McNamee, P.; Molloy, G.; Hubbard, G.; McNeill, A.; Bollina, P.; Kelly, D.; Forbat, L. Couple-Based Psychosexual Support Following Prostate Cancer Surgery: Results of a Feasibility Pilot Randomized Control Trial. J. Sex. Med. 2016, 13, 1233–1242. [Google Scholar] [CrossRef] [PubMed]
- Heinrichs, N.; Zimmermann, T.; Huber, B.; Herschbach, P.; Russell, D.W.; Baucom, D.H. Cancer distress reduction with a couple-based skills training: A randomized controlled trial. Ann. Behav. Med. 2012, 43, 239–252. [Google Scholar] [CrossRef]
- Mosher, C.E.; Winger, J.G.; Hanna, N.; Jalal, S.I.; Einhorn, L.H.; Birdas, T.J.; Ceppa, D.P.; Kesler, K.A.; Schmitt, J.; Kashy, D.A.; et al. Randomized Pilot Trial of a Telephone Symptom Management Intervention for Symptomatic Lung Cancer Patients and Their Family Caregivers. J. Pain Symptom Manag. 2016, 52, 469–482. [Google Scholar] [CrossRef] [PubMed]
- Milbury, K.; Chaoul, A.; Engle, R.; Liao, Z.; Yang, C.; Carmack, C.; Shannon, V.; Spelman, A.; Wangyal, T.; Cohen, L. Couple-based Tibetan yoga program for lung cancer patients and their caregivers. Psycho-Oncology 2015, 24, 117. [Google Scholar] [CrossRef]
- Shields, C.G.; Rousseau, S.J. A pilot study of an intervention for breast cancer survivors and their spouses. Fam. Process. 2004, 43, 95–107. [Google Scholar] [CrossRef]
- Wagner, C.D.; Johns, S.; Brown, L.F.; Hanna, N.; Bigatti, S.M. Acceptability and feasibility of a meaning-based intervention for patients with advanced cancer and their spouses: A pilot study. Am. J. Hosp. Palliat. Med. 2016, 33, 546–554. [Google Scholar] [CrossRef]
- Mosher, C.E.; Secinti, E.; Johns, S.; O’Neil, B.H.; Helft, P.R.; Shahda, S.; Jalal, S.I.; Champion, V.L. Examining the effect of peer helping in a coping skills intervention: A randomized controlled trial for advanced gastrointestinal cancer patients and their family caregivers. Qual. Life Res. 2018, 27, 515–528. [Google Scholar] [CrossRef] [PubMed]
- Clark, M.M.; Rummans, T.A.; Atherton, P.J.; Cheville, A.L.; Johnson, M.E.; Frost, M.H.; Miller, J.J.; Sloan, J.A.; Graszer, K.M.; Haas, J.G.; et al. Randomized controlled trial of maintaining quality of life during radiotherapy for advanced cancer. Cancer 2013, 119, 880–887. [Google Scholar] [CrossRef] [PubMed]
- Shennan, C.; Payne, S.; Fenlon, D. What is the evidence for the use of mindfulness-based interventions in cancer care? A review. Psycho-Oncology 2011, 20, 681–697. [Google Scholar] [CrossRef]
- Wood, A.W.; Gonzalez, J.; Barden, S.M. Mindful Caring: Using Mindfulness-Based Cognitive Therapy With Caregivers of Cancer Survivors. J. Psychosoc. Oncol. 2015, 33, 66–84. [Google Scholar] [CrossRef] [PubMed]
- Prip, A.; Møller, K.A.; Nielsen, D.L.; Jarden, M.; Olsen, M.-H.; Danielsen, A.K. The Patient-Healthcare Professional Relationship and Communication in the Oncology Outpatient Setting: A Systematic Review. Cancer Nurs. 2018, 41, E11–E22. [Google Scholar] [CrossRef]
- Corn, B.W.; Feldman, D.B.; Wexler, I. The science of hope. Lancet Oncol. 2020, 21, e452–e459. [Google Scholar] [CrossRef]
- Park, C.L. Meaning and meaning making in cancer survivorship. In The Human Quest for Meaning: Theories, Research, and Applications, 2nd ed.; Personality and Clinical Psychology Series; Routledge/Taylor & Francis Group: New York, NY, USA, 2012; pp. 521–538. [Google Scholar]
- Applebaum, A.J.; Breitbart, W. Care for the cancer caregiver: A systematic review. Palliat. Support. Care 2013, 11, 231–252. [Google Scholar] [CrossRef] [PubMed]
- Matzka, M.; Köck-Hódi, S.; Jahn, P.; Mayer, H. Relationship among symptom clusters, quality of life, and treatment-specific optimism in patients with cancer. Support. Care Cancer 2018, 26, 2685–2693. [Google Scholar] [CrossRef] [PubMed]
- Craig, H.; Freak-Poli, R.; Phyo, A.Z.Z.; Ryan, J.; Gasevic, D. The association of optimism and pessimism and all-cause mortality: A systematic review. Personal. Individ. Differ. 2021, 177, 110788. [Google Scholar] [CrossRef]
- Hobbs, G.S.; Landrum, M.B.; Arora, N.K.; Ganz, P.A.; van Ryn, M.; Weeks, J.C.; Mack, J.W.; Keating, N.L. The role of families in decisions regarding cancer treatments. Cancer 2015, 121, 1079–1087. [Google Scholar] [CrossRef] [PubMed]
- Tulsky, J.A.; Steinhauser, K.E.; LeBlanc, T.W.; Bloom, N.; Lyna, P.R.; Riley, J.; Pollak, K.I. Triadic agreement about advanced cancer treatment decisions: Perceptions among patients, families, and oncologists. Patient Educ. Couns. 2021, 105, 982–986. [Google Scholar] [CrossRef]
- Kadambi, S.; Soto-Perez-de-Celis, E.; Garg, T.; Loh, K.P.; Krok-Schoen, J.L.; Battisti, N.M.L.; Moffat, G.T.; Gil-Jr, L.A.; Mohile, S.; Hsu, T. Social support for older adults with cancer: Young International Society of Geriatric Oncology review paper. J. Geriatr. Oncol. 2020, 11, 217–224. [Google Scholar] [CrossRef]
- del-Pino-Casado, R.; Frías-Osuna, A.; Palomino-Moral, P.A.; Ruzafa-Martínez, M.; Ramos-Morcillo, A.J. Social support and subjective burden in caregivers of adults and older adults: A meta-analysis. PLoS ONE 2018, 13, e0189874. [Google Scholar] [CrossRef] [PubMed]
- Seligman, M.E.P.; Csikszentmihalyi, M. Positive psychology: An introduction. Am. Psychol. 2000, 55, 5–14. [Google Scholar] [CrossRef] [PubMed]
- Proyer, R.; Gander, F.; Wellenzohn, S.; Ruch, W. Positive psychology interventions in people aged 50–79 years: Long-term effects of placebo-controlled online interventions on well-being and depression. Aging Ment. Health 2014, 18, 997–1005. [Google Scholar] [CrossRef]
- Mitchell, J.; Vella-Brodrick, D.; Klein, B. Positive Psychology and the Internet: A Mental Health Opportunity. E-J. Appl. Psychol. 2010, 6, 30–41. [Google Scholar] [CrossRef]
| Intervention Name | Citation | Study Type | N Dyads in Final Sample | Sample Description a [Location] | Primary Outcome(s) | Summary of Results | |
|---|---|---|---|---|---|---|---|
| 4Cs program (Caring for Couples Coping with Cancer) | Li et al. (2015) [39] | Single-arm trial | 92 | Cancer PTs & SPs [Hong Kong] | Self-efficacy | CBI-B | Significant improvements were seen in couples’ self-efficacy, communication, dyadic coping, physical health subscale (PCS) of MOS-SF-12, anxiety, and benefit finding; SPs had higher self-efficacy, PCS score, and anxiety than PTs |
| Communication | CRCP | ||||||
| Dyadic coping | DCI | ||||||
| QOL | MOS-SF-12 | ||||||
| Anxiety & depression | HADS | ||||||
| Benefit-finding | BFS | ||||||
| Relationship satisfaction | DAS | ||||||
| ACT (Acceptance and Commitment Therapy) | Mosher et al. (2019) [40] | RCT: ACT vs. education/ support control condition | 50 | PTs with advanced lung cancer (III-IV NSCLC or extensive stage small cell lung cancer) diagnosed ≥3 weeks prior & distressed CGs (T-score ≥55 on PROMIS anxiety or depression measure, or DT score ≥3) (72% SPs) [USA] | Global symptom interference | MDASI (Global Symptom Interference subscale) | ACT did not reduce PT symptom interference or PT or CG distress |
| Fatigue interference | FSI (Fatigue Interference subscale) | ||||||
| Pain interference | PROMIS-SFv1.0-Pain Interference 4a | ||||||
| Task avoidance due to dyspnea | Single PROMIS item | ||||||
| Anxiety | PROMIS-SFv1.0-Anxiety 4a | ||||||
| Depression | PROMIS-SFv1.0-Depression 4a | ||||||
| Psychological distress | Single-item DT | ||||||
| CBM (Couple-Based Meditation) | Milbury et al. (2020) [41] | RCT: CBM vs. usual care | 35 | Brain cancer PTs & SPs [USA] | Feasibility & acceptability | Consent rates, attrition, attendance, homework completion, satisfaction | CBM was feasible, acceptable, and possibly efficacious; both PTs & SPs rated CBM as beneficial, but significant group differences (CBM vs. usual care) were only found for PTs |
| Cancer-specific symptoms | MDASI-BT | ||||||
| Depression | CES-D | ||||||
| Mindfulness | MAAS | ||||||
| Intimacy | PAIRI | ||||||
| CDGI (Cancer Dyads Group Intervention) | Saita et al. (2016) [42] | RCT: CDGI vs. usual care | 50 | Cancer PTs within 3 months of diagnosis & SPs, family members, or friends (75% SPs) [Italy] | Cancer-specific coping strategies | Mini-MAC | CDGI dyads reported increased Fighting Spirit & Avoidance and decreased Fatalism & Anxious Preoccupation coping styles, while control dyads reported increased Hopelessness/Helplessness & decreased Fatalism |
| Intimacy | IOS | ||||||
| CECT (Cognitive Existential Couple Therapy) | Collins et al. (2013) [43] | Single-arm pilot feasibility & acceptability trial | 12 | PTs with recently-diagnosed early-stage prostate cancer & SPs [Australia] | Feasibility | Participant retention | CECT was both feasible & acceptable to dyads |
| Acceptability | Semi-structured interview | ||||||
| Couper et al. (2015) [44] | RCT: CECT vs. usual care | 62 | PTs with localized prostate cancer (T1–T3, N0, M0) diagnosed in past 12 months & SPs [Australia] | Relationship function | FRI | Compared to usual care, those in the CECT group showed improved coping for PTs, decreased cancer-related distress for SPs, & improved relationship function for both PTs & SPs | |
| COPE | McMillan et al. (2006) [45] | RCT: COPE + usual hospice care vs. usual hospice care vs. usual hospice care + three supportive visits | 329 | Advanced cancer PTs in hospice & family CGs (% SPs not reported) [USA] | QOL | CQOL-C | COPE improved CG overall quality of life & decreased burden related to PT symptoms and CG tasks; COPE did not affect CG mastery |
| Physical symptoms | MSAS | ||||||
| Caregiving mastery | Author-designed scale | ||||||
| Caregiving burden | CDS | ||||||
| McMillan & Small (2007) [32] | Secondary analysis of data from McMillan et al. (2006) [45] | 329 | See McMillan et al. (2006) [45] | Pain | NRS | COPE did not affect PT QOL or intensity of pain, dyspnea, or constipation, but it did significantly improve PT symptom distress | |
| Dyspnea | DIS | ||||||
| Constipation | CAS | ||||||
| Symptom distress | MSAS | ||||||
| QOL | HQLI | ||||||
| Meyers et al. (2011) [46] | RCT: COPE vs. usual care | 476 | Advanced cancer PTs with relapsed, refractory, or recurrent solid tumors or lymphoma on phase 1–3 clinical trials & CGs (70% SPs) [USA] | QOL | COHQOL | No group differences in PT quality of life; CGs in COPE had a smaller decline in quality of life compared to controls | |
| Social problem solving | SPSI-R | ||||||
| CSC (Couple-Based Supportive Communi-cation intervention) | Gremore et al. (2021) [47] | Pilot RCT: CSC vs. usual care | 20 | PTs with non-metastatic head & neck cancer receiving active treatment & SPs [USA] | Acceptability | CSQ | 98% of sessions were completed, with high levels of satisfaction with the intervention; PTs and SPs in CSC had improvements in individual and relationship functioning, relative to those in usual care |
| Relationship satisfaction | DAS; MSIS | ||||||
| Post-traumatic stress | IES-R | ||||||
| Depression | CES-D | ||||||
| Anxiety | PROMIS-Anxiety | ||||||
| QOL | FACT-HN (PTs); CQOL-C (CGs) | ||||||
| Fatigue | BFI | ||||||
| Pain | BPI | ||||||
| Dignity Therapy | Wang et al. (2021) [48] | RCT | 68 | PTs with hematologic neoplasms & CGs (47.2% SPs) [China] | Hope | HHI | PTs in intervention had higher hope, spiritual well-being, and family cohesion and adaptability vs. control group; CGs in intervention had lower anxiety, depression, and higher family adaptability vs. control group |
| Spiritual well-being | FACIT-SP | ||||||
| Anxiety | SAS | ||||||
| Depression | SDS | ||||||
| Family adaptability and cohesion | FACES-II | ||||||
| DYP (Dyadic Yoga Program) | Milbury, et al. (2018) [49] | Single-arm pilot study | 5 | High-grade glioma PTs receiving ≥4 weeks radiation & family CGs (60% SPs) [USA] | Feasibility | Consent rates; session attendance; questionnaire completion; attrition; participant evaluations | Intervention was feasible and all participants perceived the program as useful and beneficial; no statistically-significant improvements for PTs or CGs, but clinically-significant improvements seen in cancer-related symptoms, sleep disturbance, depression symptoms, and mental QOL for PTs, and in mental QOL for FCGs; however, a marginally-significant increase in depression symptoms was seen in CGs |
| Cancer-related symptoms | MDASI | ||||||
| Depression | CES-D | ||||||
| Fatigue | BFI | ||||||
| Sleep disturbance | PSQI | ||||||
| QOL | MOS-SF-36 | ||||||
| Millbury, Li, et al. (2019) [50] | Pilot RCT | 20 | PTs with grade I-IV glioma to be treated with ≥20 fractions of radiotherapy & family CGs (55% SPs) [USA] | Feasibility | Consent rates, class attendance, completion of questionnaires, attrition | Found to be acceptable and well-received by participants. Supported clinically significant decrease in overall cancer-related symptom severity, specifically affective, treatment-related, mood and GI-related symptom severity. A large effect was found in reduction of caregiver depressive symptoms. Clinically significant improvements in patient/caregiver QOL. | |
| Cancer-related symptoms | MDAST-BT | ||||||
| Depressive symptoms | CES-D | ||||||
| Fatigue | BFI | ||||||
| QOL | SF-36 | ||||||
| Millbury, Liao, et al. (2019) [51] | Pilot RCT | 26 | Patients with stage I-IIIB non-small cell lung or esophageal cancer undergoing at least 5 weeks of thoracic radiotherapy & family CGs (81% SPs) [USA] | Feasibility | Consent rates, class attendance, completion of questionnaires, attrition | Intervention was feasible via a priori criteria, with 80% of dyads attending all yoga sessions. Observed clinically significant improvement in patient social function, role performance, and mental health. Caregiver treatment response less pronounced. | |
| Patient physical function | 6MWT | ||||||
| Depressive symptoms | CES-D | ||||||
| QOL | SF-36 | ||||||
| ECG (Enhanced Couple-Focused Group Intervention) | Manne et al. (2016) [52] | RCT: ECG vs. couples’ support group (SG) | 302 | Female PTs with early-stage breast cancer who received surgery in the past 12 months & SPs [USA] | Psychological well-being | MHI (Anxiety, Depression, & Well-Being subscales) | No significant differences between ECG & SG groups; dyads in both groups had improved psychological well-being & cancer distress |
| Cancer-specific distress | IES | ||||||
| Relationship satisfaction | DAS | ||||||
| FOCUS | Northouse et al. (2002) [53] | RCT: FOCUS + usual care vs. usual care | 117 | Female PTs with recurrence or progression of breast cancer in the past month & family members (64% SPs) [USA] | Acceptability | Author-designed scale | Both FOCUS & usual care participants had high satisfaction with their care, but FOCUS PTs and CGs were more satisfied in areas of their lives that were addressed by the intervention, & FOCUS PTs felt that their nurses were more understanding |
| Northouse et al. (2005) [54] | RCT: FOCUS + usual care vs. usual care | 134 | PTs with recurrence or progression of breast cancer in past month & family CGs (62% SPs) [USA] | Illness appraisals | AIS | PTs in FOCUS had less hopelessness at 3 months (no change among CGs); PTs & CGs in FOCUS had less negative appraisals of the illness & caregiving respectively | |
| Caregiving appraisals | ACS | ||||||
| Uncertainty | MUIS | ||||||
| Hopelessness | BHS | ||||||
| Coping strategies | Brief COPE | ||||||
| Northouse et al. (2007) [55] | RCT: FOCUS vs. usual care | 235 | Prostate cancer PTs & SPs [USA] | QOL | MOS-SF-12; FACT-G | FOCUS PTs had less uncertainty and improved communication compared to controls; FOCUS SPs had improved quality of life, self-efficacy, communication, and caregiving appraisals compared to controls | |
| Prostate cancer-specific QOL | FACT-P; EPIC; EPIC-S | ||||||
| Caregiving appraisals | ACS | ||||||
| Uncertainty | MUIS | ||||||
| Hopelessness | BHS | ||||||
| Coping strategies | Brief COPE | ||||||
| Cancer-related self-efficacy | LCSES | ||||||
| Communication about cancer | LMISS | ||||||
| Emotional distress | OSQ | ||||||
| Harden et al. (2009) [29] | Secondary analysis of data from Northouse et al. (2007) [55] | 86 | See Northouse et al. (2007) [55] | Acceptability | Author-designed scale | PTs & SPs were very satisfied with FOCUS; PTs who were better-functioning before FOCUS (e.g., better quality of life, better coping) & SPs who reported more positive changes post-FOCUS were more satisfied | |
| Northouse et al. (2013) [56] | RCT: brief FOCUS vs. extensive FOCUS vs. usual care | 302 | PTs with advanced lung, colorectal, breast, or prostate cancer within 6 months of new diagnosis, progression, or change of treatment & family CGs (74% SPs) [USA] | Illness appraisals | AIS | PTs & CGs in both FOCUS groups had more positive outcomes compared to usual care; extensive FOCUS improved dyad self-efficacy, brief FOCUS improved dyad health behaviors, and both improved dyad coping & social QOL | |
| Caregiving appraisals | ACS | ||||||
| Hopelessness | BHS | ||||||
| Uncertainty | MUIS-B | ||||||
| Coping strategies | Brief COPE | ||||||
| Health behaviors | Author-designed scale | ||||||
| Social support | SSQ | ||||||
| Communication about cancer | LMISS | ||||||
| Cancer-related self-efficacy | LCSES | ||||||
| QOL | FACT-G | ||||||
| Northouse et al. (2014) [57] | Single-arm feasibility study | 38 | PTs with lung, colorectal, breast, or prostate cancer diagnosed 2–12 months prior & family CGs (68.4% SPs) [USA] | Mood disturbance | POMS-SF | Dyads had improvements in mood disturbance & QOL | |
| QOL | FACT-G | ||||||
| Martinez et al. (2015) [31] | Secondary analysis of data from Northouse et al. (2013) [56] | 484 patients | See Northouse et al. (2013) [56] | Health care utilization | Emergency department visits, inpatient hospitalizations (abstracted from PT medical records) | No differences in health care utilization across study groups | |
| Dockham et al. (2016) [58] | Single-arm pilot effectiveness study | 34 | Cancer survivors & family CGs (91% SPs) [USA] | QOL | FACT-G | PTs & CGs had increases in physical, emotional, functional, and overall QOL | |
| Titler et al. (2017) [59] | Single-arm trial | 36 | Cancer PTs in treatment or completed treatment within past 18 months & family CGs (% SPs not reported) [USA] | Emotional distress | CSSDS | Significant improvements were observed in overall QOL, emotional and functional well-being, and emotional distress | |
| QOL | FACT-G | ||||||
| Chen et al. (2021) [60] | Single-arm pilot study | 29 | Cancer PTs recruited from an infusion center (any site, stage, time since diagnosis; life expectancy 6+ months) & family CGs (63.33% SPs) [USA] | Coping | Brief COPE | From pre- to post-intervention, PTs and CGs showed improved self-efficacy, CGs showed improved QOL, and PTs showed decreased use of substances for coping | |
| QOL | FACT-G (PTs); CQOL-C (CGs) | ||||||
| Self-efficacy | LCSES | ||||||
| Acceptability | Author-designed scale | ||||||
| Titler et al. (2020) [35] | Secondary analysis of Titler et al. (2017) [59] | 36 | See Titler et al. (2017) [59] | Satisfaction | Author-designed scale | Participants reported that the program did not duplicate services, that it helped them cope with cancer, & that they would recommend the program to others; the most beneficial aspects of the program were the group format and dyadic approach | |
| I-BMS (Integrative Body-Mind-Spirit intervention) | Lau et al. (2020) [37] | RCT: I-BMS vs. CBT (same data as Xiu et al. (2020) [38] report on PT outcomes) | 157 | Lung cancer PTs age ≥21 & CGs (68.15% SPs) [Hong Kong] | QOL | FACT-G; EORTC QLQ-30; HWS | CBT led to greater reduction in emotional vulnerability vs. I-BMS; I-BMS resulted in greater increase in overall QOL and spiritual self-care, and more reduction in depression vs. CBT; PTs in both groups had improvement in physical, emotional, & spiritual QOL |
| Sleep disturbance | ISI | ||||||
| Death anxiety | Death Anxiety Scale | ||||||
| Anxiety & depression | HADS; Dysfunctional Attitudes Scale | ||||||
| Xiu et al. (2020) [38] | RCT: I-BMS vs. CBT (same data as Lau et al. (2020) [37] report on CG outcomes) | 157 | See Lau et al. (2020) [37] | Anxiety & depression | HADS | CGs in both I-BMS and CBT had improved QOL immediately following intervention and at follow-up; insomnia improved for both groups at T1 but deteriorated at follow-up; both groups had reduced anxiety and perceived stress at follow-up | |
| Perceived stress | PSS | ||||||
| Sleep disturbance | ISI | ||||||
| Caregiving burden | CRA | ||||||
| QOL | CQOL-C | ||||||
| MBSR (Mindfulness-Based Stress Reduction) | Birnie et al. (2010) [61] | Single-arm trial | 21 | Cancer PTs (any site, stage, time since diagnosis) & SPs [Canada] | Mood disturbance | POMS | PTs & SPs had decreases in mood disturbance and in muscle tension, neurological/GI, & upper respiratory subscales of the C-SOSI, and increases in mindfulness |
| Stress | C-SOSI | ||||||
| Mindfulness | MAAS | ||||||
| MBSR-C (MBSR for Cancer) | Lengacher et al. (2012) [62] | Single-arm pilot study | 26 | PTs with stage 3–4 breast, colon, lung, or prostate cancer, who had completed surgery and were receiving radiation and/or chemotherapy & family CGs (% SPs not reported) [USA] | Perceived stress | PSS | From baseline to post-intervention, PT perceived stress and anxiety improved; CGs had decreased cortisol & IL-6 from pre- to post-session at some weeks |
| Depression | CES-D | ||||||
| Anxiety | STAI | ||||||
| Physical & psychological symptoms | MSAS | ||||||
| QOL | MOS-SF-36 | ||||||
| Stress markers | Salivary cortisol & interleukin-6 (IL-6) | ||||||
| MODEL Care (Mindfully Optimized Delivery of End-of-Life Care) | Cottingham et al. (2019) [36] | Secondary analysis of Johns et al. (2020) [63] | 12 | See Johns et al. (2020) [63] | Lived experience | Qualitative interviews | PTs & CGs reported the intervention (1) enhanced adaptive coping practices, (2) lowered emotional reactivity, (3) strengthened their relationship with each other, & (4) improved their communication, including communication about cancer |
| Johns et al. (2020) [63] | Single-arm pilot study | 13 | PTs treated for stage 3B-4 solid malignancies with prognosis of <12 months (but not in hospice) & family CGs (69.2% SPs) [USA] | Feasibility & acceptability | Accrual; attendance; retention; satisfaction & perceived helpfulness | PT engagement in advanced care planning more than doubled; PT distress decreased; CG QOL and family communication improved; PTs and CGs both had reduced sleep disturbance and avoidant coping | |
| Advanced care planning engagement | Completion of advanced care plan; goals of care discussions with oncologist & with family | ||||||
| Family communication | ODCNF | ||||||
| QOL | MQOL (PTs); CQOL-C (CGs) | ||||||
| Avoidant coping | Mini-MAC; Brief COPE | ||||||
| Distress | PHQ-8; GAD-7 | ||||||
| Sleep disturbance | PSQI | ||||||
| Fatigue interference | FSI | ||||||
| PIP/MPI (Couple-Based Psychosocial Information Package and Multimedia Psychosocial Intervention) | Chien et al. (2020) [64] | RCT: PIP vs. MPI vs. control | 103 | Newly-diagnosed prostate cancer PTs & SPs [Taiwan] | Disease appraisals | CAHS | SPs in MPI & PIP groups had improved positive & negative affect and mental HRQOL compared to control group. PTs were satisfied with MPI. |
| Prostate cancer-specific anxiety | MAX-PC | ||||||
| Positive & negative affect | PANAS | ||||||
| Relationship satisfaction | DAS (Dyadic Satisfaction subscale) | ||||||
| HRQOL | MOS-SF-12 | ||||||
| Satisfaction | Author-designed scale | ||||||
| PERC (Prostate Cancer Education and Resources for Couples) | Song et al. (2015) [65] | Single-arm pilot feasibility & acceptability study | 22 | Localized prostate cancer PTs who completed primary treatment & SPs [USA] | QOL | FACT-G | Dyads had high website use, were satisfied with the intervention, and found it helpful; PTs had improvement in physical, social, and overall QOL |
| Prostate cancer-specific QOL | EPIC | ||||||
| Communication about cancer | MISS | ||||||
| Feasibility & acceptability | Recruitment & retention rates; participant website activity; semi-structured interviews | ||||||
| Partners in Coping Program (PICP) | Kayser et al. (2010) [66] | RCT: PICP vs. hospital standard social work services (SSWS) | 47 | Non-metastatic primary breast cancer PTs within 3 months of diagnosis and currently receiving treatment & SPs [USA] | Breast cancer-specific QOL | FACT-B | No differences in QOL for PTs and SPs in the PICP group vs. the SSWS group |
| QOL | QL-SP | ||||||
| Illness intrusiveness | IIRS | ||||||
| Prepared Family Caregiver Problem-Solving Intervention (PSE) | Bevans et al. (2010) [67] | Single-arm pilot feasibility study | 8 | Allogeneic hematopoietic stem cell transplant PTs & family CGs (100% SPs) [USA] | Feasibility | Interventionist notes (participant attendance, session length, reasons for variation) | PSE was feasible, with high attendance & high dyad satisfaction |
| Acceptability | Semi-structured interview (issues affecting ability to participate, satisfaction, application of the problem-solving strategy) | ||||||
| Relationship Enhancement (RE) | Baucom et al. (2009) [68] | Pilot RCT: RE vs. usual care | 14 | Female PTs with stage I-II breast cancer & male SPs [USA] | Psychological distress | BSI-18 | Compared to usual care, PTs & SPs in RE had improved psychological function & relationship function and PTs had fewer physical symptoms, both immediately post-intervention & one year later |
| Post-traumatic growth | PGI | ||||||
| Functional QOL | FACT-B (Functional Well-Being subscale) | ||||||
| Self image | SIS | ||||||
| Relationship function | QMI | ||||||
| Sexual function | DISF-SR | ||||||
| Fatigue | BFI | ||||||
| Pain | BPI | ||||||
| Physical symptoms | RSC | ||||||
| RIPSToP (RelatIonal Psychosexual Treatment for Couples with Prostate Cancer) | Robertson et al. (2016) [69] | RCT: RIPSToP vs. usual care | 43 | Prostate cancer PTs & SPs [United Kingdom] | Feasibility & acceptability | Recruitment & retention rates; interventionist self-reported fidelity | RE was feasible and acceptable; PTs in RIPSToP had significant improvement in sexual bother compared to those in usual care |
| Sexual function | EPIC (Sexual Bother subscale) | ||||||
| Side by Side | Heinrichs et al. (2012) [70] | RCT: Side by Side vs. Couples Control Program (cancer education control group) | 72 | Female PTs with stages I-III breast or gynecological cancer ≤4 weeks from diagnosis & male SPs [Germany] | Relationship function | QMI | In Side by Side, PTs had lower fear of progression, and PTs & SPs had decreased avoidance, increased posttraumatic growth, improved communication quality, & more dyadic coping compared to controls |
| Communication quality | PFB (Communication subscale) | ||||||
| Dyadic coping | DCI | ||||||
| Cancer-specific distress | QSC-R23 | ||||||
| Fear of progression | FPQ | ||||||
| Cancer-related avoidance | DII-R (Avoidance-Defense subscale) | ||||||
| Post-traumatic growth | PGI | ||||||
| TSM (Telephone-Based Symptom Management) | Mosher et al. (2016) [71] | RCT: TSM vs. education control condition | 106 | Lung cancer PTs & family CGs (63% SPs) [USA] | Depression | PHQ-9 (8 item version used) | Compared to education, PTs & CGs in TSM did not have improved depressive symptoms or anxiety, and PTs did not have improved fatigue or breathlessness; TSM also did not improve PT or CG self-efficacy in managing symptoms, nor perceived social constraints from the CG |
| Anxiety | GAD-7 | ||||||
| Pain | BPI-SF | ||||||
| Fatigue | FSI | ||||||
| Physical symptoms | MSAS (4 items only) | ||||||
| Winger et al. (2018) [34] | Secondary analysis of data from Mosher et al. (2016) [71] | 51 | Subset of PTs from Mosher et al. (2016) [71] Lung cancer PTs ≥3 weeks after diagnosis & family CGs (62.75% SPs) [USA] | Pain | BPI-SF | Assertive communication (taught in TSM) was associated with less PT pain interference & psychological distress; guided imagery (taught in TSM) was associated with less CG psychological distress; however, other coping skills taught in TSM were associated with increases in some PT symptoms (e.g., pain & fatigue interference) | |
| Fatigue interference | FSI | ||||||
| Dyspnea | MSAS (single breathless-ness item) | ||||||
| Depression | PHQ-8 | ||||||
| Anxiety | GAD-7 | ||||||
| TYC (Couple-Based Tibetan Yoga) | Milbury et al. (2015) [72] | Single-arm pilot study | 10 | PTs with stages I-IIIB NSCLC receiving ≥5 weeks radiation & family CGs (90% SPs) [USA] | Feasibility | Consent rates; session attendance; participant evaluations; questionnaire completion; attrition | Intervention was feasible and most participants perceived the program as useful and beneficial; spiritual QOL improved over time for PTs, and fatigue and anxiety improved over time for CGs |
| Psychological distress | CES-D; BSI-18 (Anxiety subscale) | ||||||
| Sleep disturbance | PSQI | ||||||
| Fatigue | BFI | ||||||
| Health-related QOL | MOS-SF-36 | ||||||
| Spiritual QOL | FACT-Sp | ||||||
| Meaning-making | FMCS | ||||||
| (Unnamed) | Shields et al. (2004) [73] | Non-randomized, controlled trial: 2-session intervention vs. 1-session intervention vs. control | 48 | Breast cancer PTs & male SPs [USA] | Feasibility & acceptability | Recruitment & retention rates | Intervention was generally feasible & acceptable; 2-session format produced most positive change in psychological well-being and cancer-specific distress |
| Psychological well-being | MOS-SF-12 (Mental Health subscale) | ||||||
| Cancer-specific distress | IES | ||||||
| Relationship function | RDAS | ||||||
| (Unnamed) | Wagner et al. (2016) [74] | Single-arm pilot study | 12 | PTs with incurable stage IIB-IV lung or breast cancer & SPs [USA] | Feasibility & acceptability | Recruitment & retention rates | Generally feasible & acceptable; SPs in the intervention had reduced depression and anxiety |
| Anxiety & depression | HADS | ||||||
| (Unnamed) | Mosher et al. (2018) [75] | RCT: peer helping + coping skills vs. coping skills | 50 | PTs with stage IV GI cancer diagnosed ≥8 weeks prior & family CGs (76% SPs) [USA] | Feasibility | Recruitment, retention, & session completion rates | Intervention was feasible & acceptable; those in the coping skills (control) group had more improvement in meaning in life/peace compared to the peer helping + coping skills intervention |
| Acceptability | Purpose-designed scale | ||||||
| Spiritual QOL | FACIT-Sp (Meaning/ Peace subscale) | ||||||
| (Unnamed) | Clark et al. (2013) [76] | RCT: intervention vs. usual care | 117 | Advanced cancer PTs diagnosed in the past 12 months who were scheduled for radiation therapy & CGs (79% SPs) [USA] | QOL | FACT-G | Intervention PTs had higher overall QOL compared to usual care |
| Piderman et al. (2014) [33] | Secondary analysis of data from Clark et al. (2013) [76] | 117 | See Clark et al. (2013) [76] | QOL | FACT-G; LASA | Intervention PTs had improved spiritual & overall QOL compared to usual care | |
| Spiritual QOL | FACIT-Sp | ||||||
| Lapid et al. (2016) [30] | Secondary analysis of data from Clark et al. (2013) [76] | 116 | See Clark et al. (2013) [76] | QOL | CQOL-C; LASA | CGs in the intervention (vs. usual care) had improved QOL in several specific domains (including spiritual well-being, mood, vigor/fatigue, and adaptation to cancer), but there were no group differences for overall QOL | |
| Intervention | Citation(s) | Relevant Pillars of Positive Psychology | Intervention Description | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| PE | E | PR | MM | A | Details of Intervention Delivery | Intervention Components | Additional Information | ||||
| M | OH | OG | |||||||||
| 4Cs | Li et al. (2015) [39] | 🗸 | 🗸 | 🗸 | Six weekly in-person group-based sessions; delivered by a researcher/therapist |
| N/A | ||||
| ACT | Mosher et al. (2019) [40] | 🗸 | 🗸 | Six weekly 50-min phone sessions (dyads attended sessions 1 & 4–6 together; sessions 2–3 delivered to PTs & CGs separately); delivered by master’s level SW |
| The intervention targets processes of the ACT model of behavior change, including mindfulness, perspective taking, cognitive defusion, acceptance, values clarification, and committed action (pp. 634–635). | |||||
| CBM | Milbury et al. (2020) [41] | 🗸 | 🗸 | 🗸 | Four weekly 60-min sessions delivered via FaceTime; delivered by a master’s-level licensed psychological counselor intern |
| Informed by the positive psychology literature and integrates both intrapersonal (i.e., meditations) and interpersonal (i.e., emotional sharing) components | ||||
| CDGI | Saita et al. (2016) [42] | 🗸 | 🗸 | 🗸 | Eight in-person group-based sessions which met every 2–3 weeks for “a couple of hours;” delivered by 2 psychosocial oncology practitioners |
| CDGI is a supportive group-based intervention for cancer patient and caregiver dyads theoretically inspired by the Bio-psychosocial Model, the Symbolic Relational Model, and the Psycho-Educational Approach (p. 3). | ||||
| CECT | Collins et al. (2013) [43]; Couper et al. (2015) [44] | 🗸 | Six weekly 60–90 min in-person sessions + 2 follow-up sessions at 10 weeks & 9 months; delivered by mental health professionals supervised by a clinical psychologist and two psychiatrists | CECT aims to address key existential and functional themes including the following (Collins, p. 466):
| CECT combines supportive, existential and cognitive therapy approaches in a structured way to assist couples to develop a positive attitude, use adaptive coping strategies, and maintain a sense of meaning and authenticity in their lives together (Couper et al., 2015, p. 36) [44]. | ||||||
| COPE | McMillan et al. (2006) [45]; McMillan & Small (2007) [32]; Meyers et al. (2011) [46] | 🗸 | Three in-person sessions delivered over 1 month; delivered by trained health educators |
| COPE addresses problems known to affect patients with cancer including physical symptoms (pain or nausea), psychological symptoms (anxiety or depression), or issues related to resources or relationships, including communicating with one’s health care team or getting support or services from family, friends, and community organizations. | ||||||
| CSC | Gremore et al. (2021) [47] | 🗸 | Four 75-min in-person sessions with couples while PT received chemotherapy; delivered by clinical psychologist |
| Based on social-cognitive processing theory and the intimacy model | ||||||
| Dignity Therapy | Wang et al. (2021) [48] | 🗸 | 🗸 | 🗸 | Five to six sessions, including an introductory session, two to three 45–60 min interview sessions, a photo collection and interview transcript editing session, and a session to share a final e-product with the dyad; delivered-by a nurse or physician trained in dignity therapy |
| Based on Confucianism | ||||
| DYP | Milbury, et al. (2018) [49]; Milbury, Li, et al. (2019) [50]; Milbury, Liao, et al. (2019) [51] | 🗸 | 12 sessions delivered over course of patient’s radiotherapy, 2–3x per week, 60 min per session; delivered by two certified instructors (International Association of Yoga Therapists) |
| With traditional Indian yoga practice in mind, the underlying philosophy of this dyadic intervention was based on principles of interdependence: reciprocal support, teamwork, and equity, which were interwoven in all aspects of the program (p. 333). | ||||||
| ECG | Manne et al. (2016) [52] | 🗸 | Eight weekly 90-min in-person group-based sessions; delivered by two therapists (SWs or psychologists) per group |
| N/A | ||||||
| FOCUS | Northouse et al. (2002, 2005, 2007, 2013, 2014) [53,54,55,56,57]; Harden et al. (2009) [29]; Martinez et al. (2015) [31]; Dockham et al. (2016) [58]; Titler et al. (2017) [59]; Chen et al. (2021) [60]; Titler et al. (2020) [35] | 🗸 | 🗸 | Three monthly 90-min home visits (initial phase) + two monthly 30-min phone sessions (booster phase) after the home visit phase; delivered by master’s-level nurse. Brief version and web-based sessions also exist. |
| N/A | |||||
| I-BMS | Lau et al. (2020) [37]; Xiu et al. (2020) [38] | 🗸 | 🗸 | Eight weekly 3-h group sessions + 2 follow-up group sessions; first seven sessions, PTs & CGs attended parallel group sessions in different rooms; delivered by two to three facilitators (SW or psychologist); |
| Based on “Daoist philosophy, traditional Chinese medicine (TCM) and Western psychotherapy models…[enables] participants to appreciate the interconnectedness of their bodies, emotions, and spirituality (i.e., sense of peace, meaning), thereby building holistic capacity for transformative changes beyond the reduction of symptoms…I-BMS facilitates well-being through appreciating the interdependence among one’s body, mind and spirit, and building resources for personal growth…” (Lau et al., 2020, p. 391) [37] | |||||
| MBSR | Birnie et al. (2010) [61] | 🗸 | Eight weekly 90-min sessions + one 3- or 6-h weekend silent retreat |
| N/A | ||||||
| MBSR-C | Lengacher et al. (2012) [62] | 🗸 | 6-week intervention consisting of three in-person classes (weeks 1, 3, & 6), listening to audiotaped sessions at home on CDs, and at-home practice exercises; delivered by licensed clinical psychologist |
| MBSR specifically adapted for cancer context | ||||||
| MODEL Care | Cottingham et al. (2019) [36]; Johns et al. (2020) [63] | 🗸 | 🗸 | 🗸 | 🗸 | Six weekly 2-h in-person group sessions + home practice; delivered by facilitator trained in mindfulness practices |
| Draws on MBSR and mindful speaking/listening practices | |||
| PIP/MPI | Chien et al. (2020) [64] | 🗸 | PIP: Information manuals & 6 weeks of telephone counseling; MPI: Weekly psychosocial information film, psychosocial information manual & professional support for 6 weeks. Both delivered by trained nurses. |
| Based on transactional model of stress and coping | ||||||
| PERC | Song et al. (2015) [65] | 🗸 | Two mandatory + five optional web-based sessions over up to 8 weeks (dyads could complete together or separately); self-guided |
| “PERC takes a supportive educational approach to helping couples work together to mitigate the impact of patients’ symptoms after treatment for prostate cancer…The mandatory modules provided information about how couples can work as a team (e.g., communication) and various survivorship issues (e.g., distress, relaxation, communication with healthcare team). The optional modules focused on the management of prostate cancer-specific and general symptoms” (p. 184). | ||||||
| PICP | Kayser et al. (2010) [66] | 🗸 | Nine 60-min in-person sessions, once every 2 weeks; delivered by a SW |
| PICP developed using a cognitive-behavioral framework. Sessions (left) organized to go from “less personal and emotional issues to more intimate and emotion-focused issues” (p. 24). | ||||||
| PSE | Bevans et al. (2010) [67] | 🗸 | Four in-person sessions (median = 45 min) over course of PT’s hematopoietic stem cell transplant (pre-transplant to 4 weeks post-discharge); delivered by clinicians “with advanced degrees” (e.g., SW, nurse specialist) |
| Seeks “to empower dyads to cope with cancer and cancer treatments using two major processes from the social problem-solving literature: Problem orientation and problem-solving skills. An optimistic approach to managing the problem and permission to be creative was reinforced throughout the session” (p. 4). [USA] | ||||||
| RE | Baucom et al. (2009) [68] | 🗸 | 🗸 | Six 75-min in-person sessions, once every 2 weeks; delivered by psychology doctoral students |
| N/A | |||||
| RIPSToP | Robertson et al. (2016) [69] | 🗸 | Six 50-min in-person sessions, once every 2–3 weeks; delivered by registered therapy practitioners |
| Included “assistance with emotional disclosure, psychoeducation, relational and sexual needs, and dyadic adjustment and coping” (p. 1234). | ||||||
| Side by Side | Heinrichs et al. (2012) [70] | 🗸 | Four 120-min home visits, once every 2 weeks; delivered by therapists |
| Origins in CanCOPE, a couple-based coping intervention. “Significant emphasis on sharing thoughts and feelings and couple’s communication in cancer-related areas” (p. 243). “Within the framework of a cognitive-behavioral theory of conceptualizing relationship difficulties as well as building on couples’ strengths, we based our approach and hypotheses on an adaptation model of couples functioning” (p. 240). | ||||||
| TSM | Mosher et al. (2016) [71]; Winger et al. (2018) [34] | 🗸 | 🗸 | Four weekly 45-min phone sessions; delivered by a SW |
| “The primary goal of the intervention was to teach patients and caregivers various evidence-based cognitive-behavioral and emotion-focused strategies for managing anxiety and depressive symptoms, pain, fatigue, and breathlessness.” (Mosher et al., 2016, p. 471) [71]. | |||||
| TYC | Milbury et al. (2015) [72] | 🗸 | 10–15 45–60 min in-person sessions (2–3 weekly sessions over 5–6 weeks, delivered alongside radiation treatments); interventionists not described |
| Starting with session 1, instructors convey that the practice targets the needs of both dyad members with a focus on their interconnectedness. Starting with session 5, the dyad is given time for expressing emotional attachment, closeness, and compassion (e.g., holding hands, gazing into each other’s eyes, verbal sharing of love and affection) (pp. 2–3). | ||||||
| Unnamed | Shields et al. (2004) [73] | 🗸 | Two-session intervention: two 4-h in-person group-based sessions; interventionists not described one-session intervention: one 4-h in-person group-based session; interventionists not described |
| “Our workshop builds on established family oriented interventions for medical illness, techniques developed for marital therapy, and cognitive therapy techniques adapted for use with couples” (p. 100). | ||||||
| Unnamed | Wagner et al. (2016) [74] | 🗸 | 🗸 | Four 60-min in-person sessions; delivered by psychologist |
| “Grounded in existential psychotherapy and designed to increase meaning in life and sense of transcendence, determine wishes and hopes, and help patients and their partners communicate more openly about death and dying” (p. 548). | |||||
| Unnamed | Mosher et al. (2018) [75] | 🗸 | 🗸 | Five weekly 50 to 60-min phone sessions; delivered by psychology doctoral students supervised by psychologists |
| N/A | |||||
| Unnamed | Clark et al. (2013) [76]; Piderman et al. (2014) [33]; Lapid et al. (2016) [30] | 🗸 | 🗸 | 🗸 | Six 90-min in-person sessions, three times per week (CGs attended two per week) + 10 phone sessions, once every 2 weeks; in-person sessions delivered by a psychologist supported by other staff (e.g., APN, chaplain, SW), phone sessions, led by a psychologist or physical therapist |
| “The structured, multidisciplinary intervention focused on specific strategies to address all five QOL domains. The content was developed by a multidisciplinary treatment and designed to impact physical, mental, social, emotional, and spiritual QOL” (Clark et al., 2013, p. 4) [76]. | ||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Otto, A.K.; Ketcher, D.; Reblin, M.; Terrill, A.L. Positive Psychology Approaches to Interventions for Cancer Dyads: A Scoping Review. Int. J. Environ. Res. Public Health 2022, 19, 13561. https://doi.org/10.3390/ijerph192013561
Otto AK, Ketcher D, Reblin M, Terrill AL. Positive Psychology Approaches to Interventions for Cancer Dyads: A Scoping Review. International Journal of Environmental Research and Public Health. 2022; 19(20):13561. https://doi.org/10.3390/ijerph192013561
Chicago/Turabian StyleOtto, Amy K., Dana Ketcher, Maija Reblin, and Alexandra L. Terrill. 2022. "Positive Psychology Approaches to Interventions for Cancer Dyads: A Scoping Review" International Journal of Environmental Research and Public Health 19, no. 20: 13561. https://doi.org/10.3390/ijerph192013561
APA StyleOtto, A. K., Ketcher, D., Reblin, M., & Terrill, A. L. (2022). Positive Psychology Approaches to Interventions for Cancer Dyads: A Scoping Review. International Journal of Environmental Research and Public Health, 19(20), 13561. https://doi.org/10.3390/ijerph192013561






