Diabetes and Cardiovascular Diseases Risk Assessment in Community Pharmacies: An Implementation Study
Abstract
1. Introduction
2. Materials and Methods
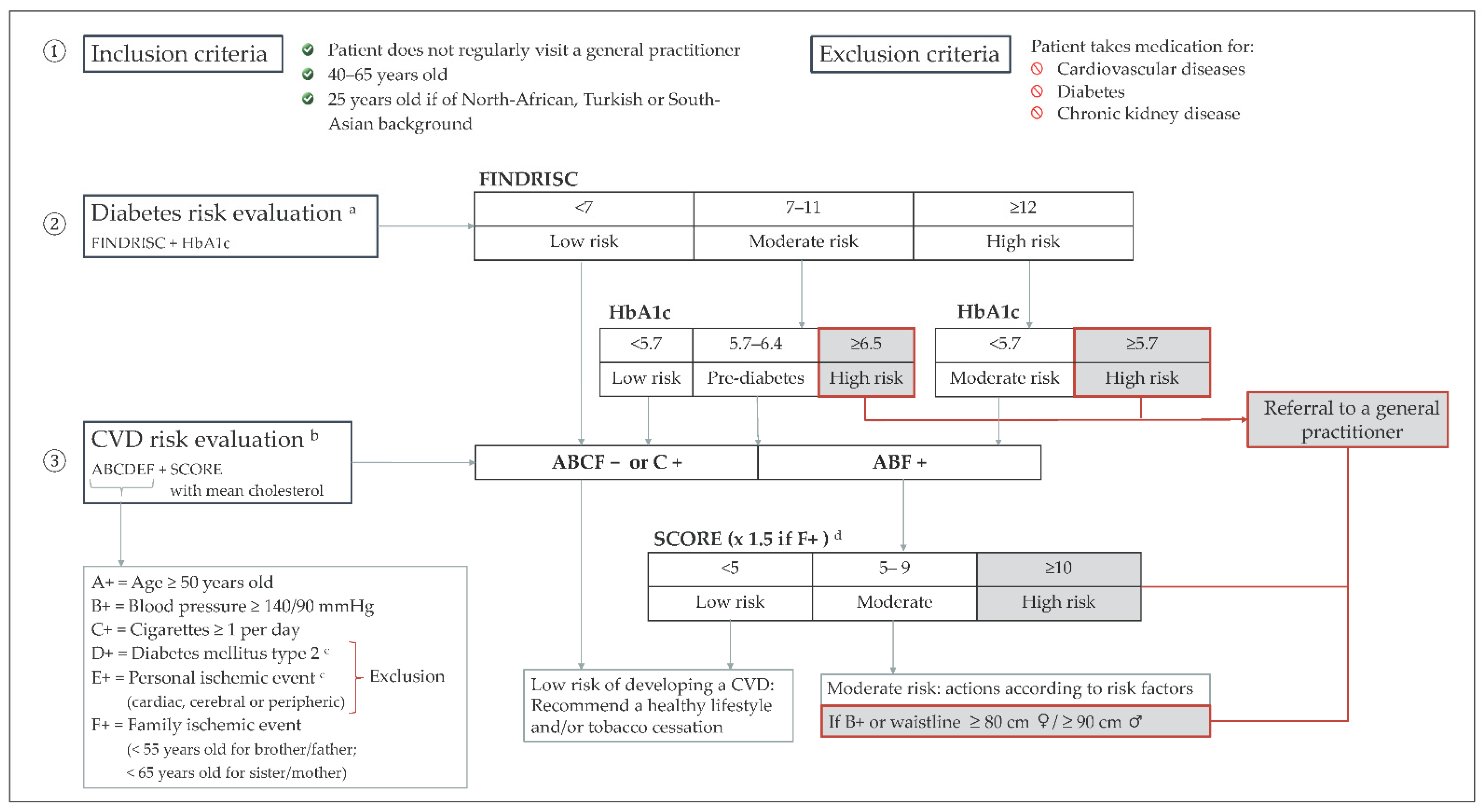
2.1. Description of the Screening Service
2.2. The Organisation of the Screening Service
2.3. Study Design
2.4. Participants
2.5. Data Collection
2.6. Data Analysis
2.7. Ethics Approval
3. Results
3.1. Reach
3.1.1. Description of the Patient Characteristics
3.1.2. Proportions of Risk Profiles
3.1.3. Reasons for Participating in or Rejecting the Risk Assessment
3.1.4. Barriers and Facilitators to Service Proposal and Patient Participation
3.2. Effectiveness
3.2.1. Outcome of Medical Follow-Up of Patients Identified as High-Risk
3.2.2. Patient Perception of and Attitude during the Risk Assessment
3.3. Adoption
Pharmacists’ Reasons for Adopting or Rejecting the Service
3.4. Implementation
3.4.1. Internal Organisation and Adaptation to Implement the Project
3.4.2. Time Needed to Provide the Service
3.4.3. Facilitators and Barriers for Optimal Implementation
3.4.4. Adherence to the Protocol
3.5. Maintenance Outlook
3.5.1. Pharmacist Satisfaction and Service Acceptability to Patients
3.5.2. Sustainability Factors
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Dimension | Outcomes | Themes | Illustrative Quotes |
|---|---|---|---|
| Reach | Reasons for participation in the risk assessment | Perceived utility—prevention and increased awareness | “It is better to act in prevention rather than in cure” (PA16) “It motivates people to be more careful” (PA1) “I think it isn’t a bad idea because there are people who have diabetes problems and are not aware of it” (PA2) “When you go to the doctor in general it’s because you’re ill, this time you got personal advice and it was free” (PA17) |
| Avoidance of a medical consultation | “Even if I visit a lot of doctors because of my job, I don’t necessarily go to the doctor very often personally” (PA6) “Usually, you have to make an appointment to go to the doctor, take a blood test and then wait for the result. Whereas here, it’s direct. After a few questions and after taking the blood pressure, you have the results” (PA15) “I don’t have a GP... So for me, it was easier to go there to see if I have something” (PA18) | ||
| Concerns about one’s own health | “I was curious to know some information about my health because, actually, I haven’t been to the doctor in years” (PA18) “My dad takes glucophage medicine, he’s on the limit of diabetes… And I have a super sweet tooth!” (PA19) “After a blood test, I was warned by my doctor that I’m at risk of being pre-diabetic” (FA11) | ||
| Trust and loyalty to their pharmacist | “You trust your pharmacist. In general, you have your pharmacist. You don’t go to 25 different pharmacies” (PA20) “I believe that patients know their pharmacist better than their doctor because they go to the pharmacist more frequently and often ask very personal questions” (PA6) | ||
| Facilitators, according to patients | Free-of-charge service to maintain high accessibility to the target population | “I think if it’s free people will do it. If you need to pay for it, even if it’s only €5, I’m not sure they’ll do it. I don’t think you’ll get the target population you want at that point. I think you’ll reach the people who are already health-conscious” (PA19) | |
| The convenience of the community pharmacies | “Especially now because of the health crisis too, it is easier to go to the pharmacist, rather than to the GP” (PA13) “I think that people perhaps go more easily to the pharmacist than to the GP. You go to the doctor when you’re ill but at the pharmacist, you can go just because you need some aspirin or something” (PA19) “I think it’s useful in terms of accessibility for everyone. Everybody goes to the pharmacy more easily to get something” (PA12) | ||
| Effectiveness | Patients’ attitude during the screening | Fear of the finger prick | “I was at ease except that I’m a person who’s fearful, just to get pricked” (PA15) |
| Increased reassurance if glycated haemoglobin measured | “I think honestly, I think I would have been even more reassured if I had done the test” (PA20) | ||
| Clear, reassuring communication of the results by the pharmacists | “He was benevolent, that’s all, in terms of the explanation” (PA6) “It’s reassuring to have explanations at every step and to have explanations that are in our language and not just in medical language, sometimes we’re a bit confused!” (PA12) “Delicate, respectful... especially in prevention, especially not alarmist” (PA16) | ||
| Receiving a printout of the results to help information recollection | “For me it was enough to tell me about it orally” (PA17) “It’s true that I kind of left empty-handed. As I didn’t have anything in my hands, it made the test seem less useful”. “I remembered what he told me. But I think that for patients who are perhaps less used to medical vocabulary, I think it is important that they can read it again at their ease” (PA22) | ||
| Patients’ perception of the risk assessment | Increased awareness of one’s own health | “I was under a lot of stress with some complicated years and I let my blood pressure go too far. I didn’t pay attention to it any more, and I became aware of it thanks to the screening. I was living like that, without realising it” (PA9) “I thought it was really very useful: there were some things that I didn’t necessarily expect” (PA16) | |
| Implementation of lifestyle changes | “She gave me some advice on nutritherapy. There are a lot of habits that I’m changing. I was already eating quite well, but there are lots of things I have improved since then” (PA19) | ||
| Outlook for maintenance | Patient acceptability | Satisfaction with the service | “It’s a good initiative for a lot of people and it’s very easy to do” (PA11) “I find it very professional, and I would say it exceeded my expectations” (PA17) |
| Personalised counselling | “The only thing maybe is to give people more explanation... We got explanation, but maybe not with enough depth” (PA1) | ||
| Factors for sustainability | Increased awareness of the service through communication | “I think it would be good to increase the communication. I didn’t see the poster elsewhere, only in the pharmacy. I wouldn’t have been aware” (PA7) “It lacks media coverage because most people don’t know about it” (PA11) “It needs to be known, so a different approach to communication would be interesting” (PA17) | |
| Communication with the family physician | “I think that the family doctor should be aware of what we do. I think it’s normal for the medical professions to pass on information to each other” (PA20) |
Appendix B
| Dimension | Outcomes | Themes | Illustrative Quotes |
|---|---|---|---|
| Reach | Service proposal and reach to the target population | Use of visual materials (folders, posters) to raise patient’s curiosity | “We always put folders in every time we sold a drug and it worked. There were a few people who came back and asked how it works and if they could doit” (FA7) “Half of the cases were people who came to us to ask based on the posters and what they saw on the screens” (FA8) “We had our screens behind us showing slides with diabetes on them and so on. And we recruited all our patients this way” (FA13) “I think that the poster on the window and the little folders that I had put on the counter, next to the card machine, attracted the most attention” (FA6) |
| Use of the FINDRISC questionnaire | “If they didn’t have time, we gave them the FINDRISC questionnaire. We said, ‘Here, fill it in at home. And if you see you have a high score, then we can go further in the screening’” (FA14) “We gave them the questionnaire that they could take home. They could fill it in and come back later” (FA12) | ||
| Proposal to the patients as an opportunity (free-of-charge and in collaboration with universities) | “We presented it in an attractive way: ‘Oh, you have the chance to do a measurement normally done in the lab that youwould haveto pay for. Here it’s free’” (FA14) “It was really something that motivated people as well, to say, ‘It’s free. It’s anonymous. And it’s a plus that we offer you here at the pharmacy. If you want to do it, you’ll have extra information about your health that you usually don’t have in a check-up’” (FA12) “The fact that we say it’s in partnership with universities helped a lot. We are taken seriously straight away” (FA7) | ||
| Active approach to increase uptake | “We kind of forgot about it(the project), so we targeted very quickly and in fact,it worked well as soon as we started” (FA4) “We had our own little challenge to do and in the end, when you get in the mood, as soon as you start offering it to everyone, you get plenty” (FA14) | ||
| Barriers to proposing the service | Fear of stigmatising and of patients’ reactions | “We also had to deal with patients we knew a little less... I found that the most difficult part because we’re not the kind of people who are going to force people. We sometimes felt a bit uncomfortable proposing this to them” (FA13) “We know very well that it is towards those people (obese or overweight) we should go, but we are always afraid of stigmatising. You’re never in people’s heads, so you never know how they might react” (FA8) “It’s certain that there are people to whom I could have or perhaps should have proposed it, but I didn’t know how to approach the problem... Especially with people of foreign origin, you feel them to be more suspicious more quickly” (FA6) | |
| Lack of time | “The other problem is time; sometimes we had no time, or we had to do something else” (FA7) “It’s more a problem of timing. In the middle of winter when people are waiting outside (sanitary crisis restrictions), we have to be as quick as possible” (FA11) | ||
| Language barrier | “For language reasons, especially... It’s difficult to explain something like thatif the person in front of you doesn’t speak your language” (FA7) “If I didn’t mention it, it’s because I had people in front of me who didn’t speak French or Dutch well” (FA10) | ||
| Barriers to reaching patients | Inclusion criteria too strict | “We were a little frustrated because there were a lot of requests from people over 65 who didn’t necessarily have a doctor and it would have been really interesting to be able to test them” (FA14) “To be less limited, for example in terms of origin or age. Someone who is young and not at risk; it is still sending a good message, particularly in families where there is diabetes” (PA11) | |
| Reasons for refusal to participate, according to the pharmacists | Lack of time | “It’s all about timing. There are some people who said: ‘I will come back,’ but they don’t always come back” (FA3) “I don’t think there was a refusal on the principle of the test. It’s more refusal because ‘I don’t have a moment to come back’ or ‘I can’t do it now’” (FA11) | |
| Patients feared the results of the risk assessment | “Some refused because they knew very well that they would be in the red. Probably or not. But they were afraid toknowthe truth” (FA5) “One literally said she was afraid of the outcome” (FA7) | ||
| Effectiveness | Patient’s attitude during the screening | Patients were afraid to perform the fingerpick, assisted by the pharmacist | “People were really afraid of needles, in general” (FA14) “I always asked them, ‘Do you want to do the prick yourself or do you want me to do it?’ And they’d all say, ‘You can do it,’ and I did it every time” (FA13) |
| Adoption | Reasons for adopting the project | Opportunity to offer a new service to the patients | “PeopleI had invited to participate (in another pilot project) were happy and thought it was nice that I was proposing it. So it was to offer my services to the pharmacy customers” (FA6) “For me, it’s important that our profession evolves and diversifies. And so offering things like that to patients is a plus for the profession of pharmacist” (FA12) |
| Opportunity to show the added-value of the pharmacist | “If the pharmacist does this in the future, everywhere, we will be valued, we will no longer be considered as pure salesmen as some people see it” (FA4) “It was also important to reposition the role of the pharmacist with the population” (FA9) “It was to prove that the pharmacist can bring many things to the patients apart from dispensing advice or medicines” (FA12) | ||
| Prevention services are part of the future of the community pharmacy | “I think it’s really the future of the pharmacist tohave a rolein prevention” (FA5) “It’s really the future of pharmacy and we’re going to have to do consultations and coaching” (FA14) “For me, one of the paths we need to take is to move towards prevention and play an active role in this area” (FA13) Because I’m convinced that as a pharmacist, we have a role to play in, in screening for diabetes and many other things as well (FA11) | ||
| Reasons for rejecting the project | Inappropriate timing due to the COVID-19 sanitary crisis | “With COVID, we were reluctant to take people behind of the counter. At the beginning,around November-December,the virus was circulating significantly” (Dropout 1) | |
| Lack of time/staff | “It’s purely a lack of time. At the moment, we are understaffed so it was a bit difficult for us to carry out the project” (Dropout 2) | ||
| Implementation | Internal organisations and adaptation to implement the project | Lack of training of the staff can limit service delivery | “We did one(training session)again with my whole team, too, so that they could be familiar with handling the device. (FA14) “I explained it to the team, but there was no one who really wanted to get into it. They didn’t feel comfortable enough” (FA10) “We have some pharmacists working one or two days a week, so it’s almost not necessary. It was a good solution not to train everybody and to have only one or two in the pharmacy who knew how to do it” (FA13) |
| Performing the service on the spot, if possible, is more efficient than scheduling an appointment | “Webookedappointments for the first twoorthree. But after that it was really…as soon as we saw the patient, we offered to do it immediately if possible. I find that works best” (FA7) “We didn’t work very much by appointment because we quickly noticed that people didn’t always show up” (FA8) “At the beginning, we did the appointment thing. Later, we were very used to it, we didn’t have to prepare at all in fact. We knew how to do it at the time” (FA13) “That’s what we should be able to do, to do the screening on the spot, but for practical reasons it wasn’t always possible” (FA11) | ||
| Optimisation over time | “We’d arrive in the morning, I’d switch on the machine so I knew that if anyone turned up, we’d be able to do it straight away. There was no waiting time” (FA9) “We even did it in pairs, there was a certain rotation. While one asked the questions and measured the blood pressure or whatever, the other encoded the data and so it was quicker for the patient too” (FA16) “At a certain point, once we’d done it, it was more structured, even us in terms of our speech in relation to the person in front of us” (FA4) “You get used to the protocol and everything. We also optimise our time” (FA12) | ||
| Time needed to provide the service | Time varied between pharmacists and depending on the patient | “We rarely spend more than 10 min, 15 min with the patient. After that, it becomes complicated to keep him longer” (FA8) “It wasn’t too long for the patient, nor for us. We were able to fit it in easily during the working day” (FA16) “It really varies from one patient to another. Some we finished in fifteen minutes. Some are still there after 30 or 40 min” (FA7) | |
| Facilitators of and barriers to optimal implementation | Confidential area to perform the service | “I’vededicateda small space where I can do that, where I’m really in privateandpeople are not disturbed by other peoplethat come and go” (FA10) “If I was to develop this in the long term, I would need more space in the pharmacy that I could dedicate to that” (FA11) “When you ask someone to measure their waist size and there are several people around, it’s perhaps a bit embarrassing. You need to have a confidential room to set this up” (FA14) | |
| Need for a sufficient taskforce | “It’s easier in a team with several people. I can’t imagine a single pharmacist taking time like that for patients” (FA14) “As I was doing it on my own, if I had people in, I had to make the patient wait” (FA3) “There had to be at least two of us so that one of us could take care of the test from start to finish” (FA11) | ||
| Adherence to the protocol | Inclusion of patients over 65 years old | “We didn’t always respect the age limit. But the age, come on, it’s a shame” (FA7) “We didn’t realise straight away that there was an age limit. So I think we had two or three times at the beginning, until an email reminded us that it wasn’t over 65. Afterwards, we respected it but it was a bit frustrating” (FA14) “We screened people over 65. We felt that as long as people wanted to do it, and were not under the supervision of a doctor, we didn’t feel comfortable refusing” (FA13) | |
| Outlook for maintenance | Pharmacists’ experience with the service | Improved patient-pharmacist relationship | “It was a way of getting to know them and their story even better” (FA13) “I felt that the patients perhaps appreciated the explanation, communication and interaction with them even more than the measurement of glycated haemoglobin” (FA1) “I find it creates a different bond” (FA8) |
| Increased dialogue for patient awareness | “Sometimes we would talk about other diseases or other problems. It wasn’t only diabetes.Sometimes it was also a way of talking about other things or aboutlifestyle” (FA7) “For those who were a bit on the edge, we took the opportunity to have a small nutritional consultation and give advice. This led to other health discussions” (FA14) “We also came across patients who needed to talk and that was sometimes the triggering factor” (FA13) “We would continue to do it, even without the POCT because it raises awareness” (FA14) | ||
| Personal satisfaction with the service | “It really made us feel valued in ourprofession” (FA7) “I’m delighted; frankly, I think it has a huge beneficial impact” (FA3) | ||
| Factors for sustainability | Increased interprofessional collaboration, through GP-CP practice groups | “Weshould dothis in consultation with medical practices that agree with us and with whom we exchange information” (FA10) “Perhaps we need to attack this from another angle, which is that of medical-pharmaceutical consultation” (FA2) | |
| Data sharing with GPs | “A communication channel that would enable to transfer indirectly but immediately the results to the doctor, in agreement with the patient” (FA2) | ||
| Financial compensation for service performed and medical devices | “The price of the machine. I imagine that it must not be cheap, so is it feasible to buy it as a small independent owner?” (FA13) “All work deserves a salary. You also have to think in terms of the savings that would be generated in the sense that diabetes that is discovered earlier, generates less costs in terms of social security later on, and so it’s the ‘balance’ that would justify the fee” (FA8) “I believe the consumables would cost more than the device actually. There should be a fixed fee for each patient with which we take the time to explain things, to take the measurements” (FA13) | ||
| Periodical offer of the service, in parallel with prevention campaigns | “Maybe have a rotation with several pharmacies and each one does its own diabetes month. So if wefind eligiblepeople, we can say: ‘in two months, we will have the machine, we can already make an appointment’” (FA14) “It would be logical to do this every year for example” (FA1) | ||
| Extra formal training needed | “If we have to take over and start doing this systematically then we need to have much more effective training… it should be in the student curriculum, if at some point we manage to systematise it” (FA6) | ||
| Increased awareness of the service through media coverage or the community | “First of all is communication, people being aware that we do screening in pharmacies” (FA11) “Local magazines, local websites, but also local radio stations” (FA1) “I think it would help if the PCSWs or the local authorities advertised the project” (FA10) | ||
| Free-of-charge service for the patient to maintain high accessibility | “The financial barrier: it has to be free, at least in my neighbourhood” (FA11) “Here it didn’t pose any problems because it was free, but it’s obvious that if you have to start charging... I don’t know if the take-up would have been as good” (FA6) | ||
| Patient perception of the pharmacist’s role | “The only barrier is again communication. The Belgian population does not yetperceivethat the pharmacist has a role in this and is capable of doing so. I think that mentalities must clearly change” (FA3) “It has to become part of people’s mentality to come and get tested” (FA6) |
References
- World Health Organization. Noncommunicable Diseases Country Profiles 2018; World Health Organization: Geneva, Switzerland, 2018. [Google Scholar]
- Chatterjee, R.; Narayan, K.M.; Lipscomb, J.; Phillips, L.S. Screening adults for pre-diabetes and diabetes may be cost-saving. Diabetes Care 2010, 33, 1484–1490. [Google Scholar] [CrossRef] [PubMed]
- Thomas, C.; Brennan, A.; Goka, E.; Squires, H.Y.; Brenner, G.; Bagguley, D.; Buckley Woods, H.; Gillett, M.; Leaviss, J.; Clowes, M.; et al. What are the cost-savings and health benefits of improving detection and management for six high cardiovascular risk conditions in England? An economic evaluation. BMJ Open 2020, 10, e037486. [Google Scholar] [CrossRef] [PubMed]
- Tsuyuki, R.T.; Beahm, N.P.; Okada, H.; Al Hamarneh, Y.N. Pharmacists as accessible primary health care providers: Review of the evidence. Can. Pharm. J. 2018, 151, 4–5. [Google Scholar] [CrossRef] [PubMed]
- Agomo, C.O. The role of community pharmacists in public health: A scoping review of the literature. J. Pharm. Health Serv. Res. 2012, 3, 25–33. [Google Scholar] [CrossRef]
- Anderson, C.; Zhan, K.; Boyd, M.; Mann, C. The role of pharmacists in general practice: A realist review. Res. Soc. Adm. Pharm. 2019, 15, 338–345. [Google Scholar] [CrossRef] [PubMed]
- Ayorinde, A.A.; Porteous, T.; Sharma, P. Screening for major diseases in community pharmacies: A systematic review. Int. J. Pharm. Pract. 2013, 21, 349–361. [Google Scholar] [CrossRef]
- Willis, A.; Rivers, P.; Gray, L.J.; Davies, M.; Khunti, K. The effectiveness of screening for diabetes and cardiovascular disease risk factors in a community pharmacy setting. PLoS ONE 2014, 9, e91157. [Google Scholar] [CrossRef]
- San-Juan-Rodriguez, A.; Newman, T.V.; Hernandez, I.; Swart, E.C.S.; Klein-Fedyshin, M.; Shrank, W.H.; Parekh, N. Impact of community pharmacist-provided preventive services on clinical, utilization, and economic outcomes: An umbrella review. Prev. Med. 2018, 115, 145–155. [Google Scholar] [CrossRef]
- Costa, R.; de Valk, H.A.G. Socio-spatial Disparities in Brussels and its Hinterland. In Urban Socio-Economic Segregation and Income Inequality: A Global Perspective; van Ham, M., Tammaru, T., Ubarevičienė, R., Janssen, H., Eds.; Springer International Publishing: Cham, Switzerland, 2021; pp. 271–291. [Google Scholar]
- Cès, S.; Baeten, R. Inequalities in Access to Healthcare in Belgium; European Social Observatory: Brussels, Belgium, 2020; 184p. [Google Scholar]
- Missinne, S.; Luyten, S. Les Médecins Généralistes en Région Bruxelloise: Qui Sont-Ils, où Pratiquent-Ils et où se Situent les Potentielles Pénuries? Observatoire de la Santé et du Social de Bruxelles: Brussels, Belgium, 2018. [Google Scholar]
- Geers Janice, S.A.; Leen, H.; Marleen, D.; Dominique, V. Abstracts of the Third National Poct Symposium, Antwerp, Belgium, March 17th, 2017. Acta Clin. Belg. 2017, 72, 1–14. [Google Scholar] [CrossRef]
- Projet Chronilux. Available online: https://www.chronilux.be/depistage-diabete-2022/ (accessed on 30 May 2022).
- Moullin, J.C.; Sabater-Hernández, D.; Benrimoj, S.I. Model for the evaluation of implementation programs and professional pharmacy services. Res. Soc. Adm. Pharm. 2016, 12, 515–522. [Google Scholar] [CrossRef]
- Raine, R.; Fitzpatrick, R.; Barratt, H.; Bevan, G.; Black, N.; Boaden, R.; Bower, P.; Campbell, M.; Denis, J.-L.; Devers, K. Challenges, solutions and future directions in the evaluation of service innovations in health care and public health. Health Serv. Deliv. Res. 2016, 4, 121–132. [Google Scholar] [CrossRef] [PubMed]
- Victora, C.G.; Habicht, J.-P.; Bryce, J. Evidence-based public health: Moving beyond randomized trials. Am. J. Public Health 2004, 94, 400–405. [Google Scholar] [CrossRef] [PubMed]
- Moullin, J.C.; Sabater-Hernandez, D.; Benrimoj, S.I. Qualitative study on the implementation of professional pharmacy services in Australian community pharmacies using framework analysis. BMC Health Serv. Res. 2016, 16, 439. [Google Scholar] [CrossRef] [PubMed]
- Curran, G.M.; Shoemaker, S.J. Advancing pharmacy practice through implementation science. Res. Soc. Adm. Pharm. 2017, 13, 889–891. [Google Scholar] [CrossRef]
- Lindstrom, J.; Tuomilehto, J. The diabetes risk score: A practical tool to predict type 2 diabetes risk. Diabetes Care 2003, 26, 725–731. [Google Scholar] [CrossRef]
- Boland, B.; De Muylder, R.; Goderis, G.; Degryse, J.; Gueuning, Y.; Paulus, D.; Jeanjean, M. Cardiovascular prevention in general practice: Development and validation of an algorithm. Acta Cardiol. 2004, 59, 598–605. [Google Scholar] [CrossRef]
- De Bacquer, D.; De Backer, G. Predictive ability of the SCORE Belgium risk chart for cardiovascular mortality. Int. J. Cardiol. 2010, 143, 385–390. [Google Scholar] [CrossRef]
- Boland, B.; Christiaens, T.; Goderis, G.; Govaerts, F.; Philips, H.; Smeets, F.; Van de Vyver, N.; Van Duppen, D. Globaal cardiovasculair risicobeheer. Huisarts Nu 2007, 36, 339–371. [Google Scholar]
- Ujcic-Voortman, J.K.; Schram, M.T.; Jacobs-van der Bruggen, M.A.; Verhoeff, A.P.; Baan, C.A. Diabetes prevalence and risk factors among ethnic minorities. Eur. J. Public Health 2009, 19, 511–515. [Google Scholar] [CrossRef]
- Vandenheede, H.; Deboosere, P. Type 2 diabetes in Belgians of Turkish and Moroccan origin. Arch. Public Health 2009, 67, 62–87. [Google Scholar] [CrossRef][Green Version]
- Bastiaens, H.; Benhalima, K.; Cloetens, H.; Feyen, L.; Nobels, F.; Koeck, P.; Sunaert, P.; van Crombrugge, P.; van Pottelbergh, I.; van Leeuwen, E.; et al. Diabète Sucré de Type 2—Recommandations de Bonne Pratique; Domus Medica: Brussels, Belgium. Available online: https://www.trajetdesoins.be/fr/Bibliotheque/pdf/RBP_Diabete2_FR.pdf (accessed on 30 May 2022).
- Vandersmissen, G.J.M.; Godderis, L. Evaluation of the Finnish Diabetes Risk Score (FINDRISC) for diabetes screening in occupational health care. Int. J. Occup. Med. Environ. Health 2015, 28, 587–591. [Google Scholar] [CrossRef] [PubMed]
- Glasgow, R.E.; Vogt, T.M.; Boles, S.M. Evaluating the public health impact of health promotion interventions: The RE-AIM framework. Am. J. Public Health 1999, 89, 1322–1327. [Google Scholar] [CrossRef] [PubMed]
- D’Lima, D.; Soukup, T.; Hull, L. Evaluating the Application of the RE-AIM Planning and Evaluation Framework: An Updated Systematic Review and Exploration of Pragmatic Application. Front. Public Health 2021, 9, 755738. [Google Scholar] [CrossRef] [PubMed]
- Krska, J.; Morecroft, C.W. Views of the general public on the role of pharmacy in public health. J. Pharm. Health Serv. Res. 2010, 1, 33–38. [Google Scholar]
- Melton, B.L.; Lai, Z. Review of community pharmacy services: What is being performed, and where are the opportunities for improvement? Integr. Pharm. Res. Pract. 2017, 6, 79–89. [Google Scholar] [CrossRef]
- Katangwe, T.; Family, H.; Sokhi, J.; Al-Jabr, H.; Kirkdale, C.L.; Twigg, M.J. The community pharmacy setting for diabetes prevention: Views and perceptions of stakeholders. PLoS ONE 2019, 14, e0219686. [Google Scholar] [CrossRef] [PubMed]
- Alzubaidi, H.; Namara, K.M.; Saidawi, W.; Hasan, S.; Krass, I. Pharmacists’ experiences and views on providing screening services: An international comparison. Res. Soc. Adm. Pharm. 2020, 16, 1558–1568. [Google Scholar] [CrossRef]
- Siu, A.H.Y.; Krass, I.; Mitchell, B.; McNamara, K. Implementation of diabetes screening in community pharmacy—Factors influencing successful implementation. Res. Soc. Adm. Pharm. 2021, 17, 1606–1613. [Google Scholar] [CrossRef]
- Mc Namara, K.P.; Krass, I.; Peterson, G.M.; Alzubaidi, H.; Grenfell, R.; Freedman, B.; Dunbar, J.A. Implementing screening interventions in community pharmacy to promote interprofessional coordination of primary care—A mixed methods evaluation. Res. Soc. Adm. Pharm. 2020, 16, 160–167. [Google Scholar] [CrossRef]
- Corscadden, L.; Levesque, J.F.; Lewis, V.; Strumpf, E.; Breton, M.; Russell, G. Factors associated with multiple barriers to access to primary care: An international analysis. Int. J. Equity Health 2018, 17, 28. [Google Scholar] [CrossRef]
- Eades, C.E.; Ferguson, J.S.; O’Carroll, R.E. Public health in community pharmacy: A systematic review of pharmacist and consumer views. BMC Public Health 2011, 11, 582. [Google Scholar] [CrossRef] [PubMed]
- Kaae, S.; Traulsen, J.M.; Norgaard, L.S. Customer interest in and experience with various types of pharmacy counselling—A qualitative study. Health Expect 2014, 17, 852–862. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Wright, D.; Little, R.; Turner, D.; Thornley, T. Diabetes Screening Through Community Pharmacies in England: A Cost-Effectiveness Study. Pharmacy 2019, 7, 30. [Google Scholar] [CrossRef] [PubMed]
- Alzubaidi, H.T.; Chandir, S.; Hasan, S.; McNamara, K.; Cox, R.; Krass, I. Diabetes and cardiovascular disease risk screening model in community pharmacies in a developing primary healthcare system: A feasibility study. BMJ Open 2019, 9, e031246. [Google Scholar] [CrossRef]
- Nhim, K.; Khan, T.; Gruss, S.; Wozniak, G.; Kirley, K.; Schumacher, P.; Albright, A. Facilitators to referrals to CDC’s National Diabetes Prevention Program in primary care practices and pharmacies: DocStyles 2016–2017. Prev. Med. 2021, 149, 106614. [Google Scholar] [CrossRef]
- Bollen, A.; Harrison, R.; Aslani, P.; van Haastregt, J.C.M. Factors influencing interprofessional collaboration between community pharmacists and general practitioners-A systematic review. Health Soc. Care Community 2019, 27, e189–e212. [Google Scholar] [CrossRef]
- Almansour, H.A.; Aloudah, N.M.; Alhawassi, T.M.; Chaar, B.; Krass, I.; Saini, B. Physicians’ views on cardiovascular disease risk prevention services by pharmacists and potential for collaboration. Explor. Res. Clin. Soc. Pharm. 2021, 4, 100077. [Google Scholar] [CrossRef]
- Van Hoof, V.; Barglazan, D.; Blairon, L.; Braekevelt, B.; Debois, R.; De Vos, N.V.J.; Gruson, D.; Jonckheere, J.; Lanckmans, K.; Moens, M.; et al. Organisation and quality monitoring for point-of-care testing (POCT) in Belgium: Proposal for an expansion of the legal framework for POCT into primary health care. Acta Clin. Belg. 2022, 77, 329–336. [Google Scholar] [CrossRef]
| Dimension and Definition | Quantitative Data | Qualitative Data |
|---|---|---|
| Reach (The absolute number, proportion, and representativeness of individuals willing to participate in a given intervention) |
|
|
| Effectiveness (The impact of an intervention on important outcomes, including potential negative effects, quality of life, and economic outcomes) |
|
|
| Adoption (The absolute number, proportion, and representativeness of: (a) settings; and (b) intervention agents (people who deliver the programme) who are willing to initiate a programme) |
|
|
| Implementation (The interventions agents’ fidelity to the various elements of an intervention’s protocol) |
|
|
| Likelihood of maintenance a (The extent to which: (a) a behaviour is sustained or more after intervention; and (b) a programme becomes institutionalised or part of the routine organisational practices). | / |
|
| Diabetes Risk Profile | |||||||
|---|---|---|---|---|---|---|---|
| Low | Moderate | High | Undetermined | ||||
| FINDRISC a | n (%) | HbA1C | n (%) | n (%) | n (%) | n (%) | n (%) |
| <7 | 47 (12.5%) | / | / | 47 (12.5%) | |||
| 7–11 | 128 (34.0%) | <5.7 | 98 (26.1%) | 98 (26.1%) | |||
| 5.7–6.4 | 26 (6.9%) | 26 (6.9%) | |||||
| ≥6.5 | 2 (0.5%) | 2 (0.5%) | |||||
| No data | 2 (0.5%) | 2 (0.5%) | |||||
| ≥12 | 201 (53.5%) | <5.7 | 126 (33.5%) | 126 (33.5%) | |||
| ≥5.7 | 72 (19.1%) | 72 (19.1%) | |||||
| No data | 3 (0.8%) | 3 (0.8%) | |||||
| 376 (100%) | 376 (100%) | 145 (38.6%) | 152 (40.4%) | 74 (19.7%) | 5 (1.3%) | ||
| Cardiovascular Risk Profile | ||||||
|---|---|---|---|---|---|---|
| Low | Moderate | High | Undetermined | |||
| n (%) | n (%) | n (%) | n (%) | n (%) | ||
| ABCF− or C+ a | ABCF− | 67 (26.3%) | 67 (26.3%) | |||
| ABF+ b | Score < 5 | 152 (59.6%) | 152 (59.6%) | |||
| Score 5–9 | 24 (9.4%) | 24 (9.4%) | ||||
| Score ≥ 10 | 6 (2.4%) | 6 (2.35%) | ||||
| Missing score | 6 (2.4%) | 6 (2.4%) | ||||
| 255 (100%) | 219 (85.9%) | 24 (9.4%) | 6 (2.4%) | 6 (2.4%) | ||
| 51 | Patients with High Level of Risk for Diabetes or Cardiovascular Diseases | |
|---|---|---|
| 18 | Did not consent to be contacted by the research team | |
| 33 | Possible inclusions | |
| 13 lost to Follow-up | 3 | No contact details |
| 2 | Wrong contact details | |
| 8 | Unsuccessful contact attempts | |
| 20 | Inclusions | |
| 2 | Not aware that there was a high risk | |
| 3 | Had not (yet) gone to a general practitioner, but aware that there was a high risk | |
| 3 | Went to a general practitioner for another reason; high risk not discussed as not considered a priority | |
| 6 | Already in medical follow-up for cardiovascular disease/risk of diabetes | |
| 5 | Went to a general practitioner/specialist, with a negative outcome on diagnosis | |
| 1 | Diagnosis | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rondeaux, S.; Braeckman, T.; Beckwé, M.; Biset, N.; Maesschalck, J.; Duquet, N.; De Wulf, I.; Devroey, D.; De Vriese, C. Diabetes and Cardiovascular Diseases Risk Assessment in Community Pharmacies: An Implementation Study. Int. J. Environ. Res. Public Health 2022, 19, 8699. https://doi.org/10.3390/ijerph19148699
Rondeaux S, Braeckman T, Beckwé M, Biset N, Maesschalck J, Duquet N, De Wulf I, Devroey D, De Vriese C. Diabetes and Cardiovascular Diseases Risk Assessment in Community Pharmacies: An Implementation Study. International Journal of Environmental Research and Public Health. 2022; 19(14):8699. https://doi.org/10.3390/ijerph19148699
Chicago/Turabian StyleRondeaux, Sarah, Tessa Braeckman, Mieke Beckwé, Natacha Biset, Joris Maesschalck, Nathalie Duquet, Isabelle De Wulf, Dirk Devroey, and Carine De Vriese. 2022. "Diabetes and Cardiovascular Diseases Risk Assessment in Community Pharmacies: An Implementation Study" International Journal of Environmental Research and Public Health 19, no. 14: 8699. https://doi.org/10.3390/ijerph19148699
APA StyleRondeaux, S., Braeckman, T., Beckwé, M., Biset, N., Maesschalck, J., Duquet, N., De Wulf, I., Devroey, D., & De Vriese, C. (2022). Diabetes and Cardiovascular Diseases Risk Assessment in Community Pharmacies: An Implementation Study. International Journal of Environmental Research and Public Health, 19(14), 8699. https://doi.org/10.3390/ijerph19148699






