Sleep Quality and Aging: A Systematic Review on Healthy Older People, Mild Cognitive Impairment and Alzheimer’s Disease
Abstract
1. Introduction
2. Materials and Methods
2.1. Research Strategies
2.2. Eligibility Criteria
2.3. Data Collection
2.4. Quality Assessment
3. Results
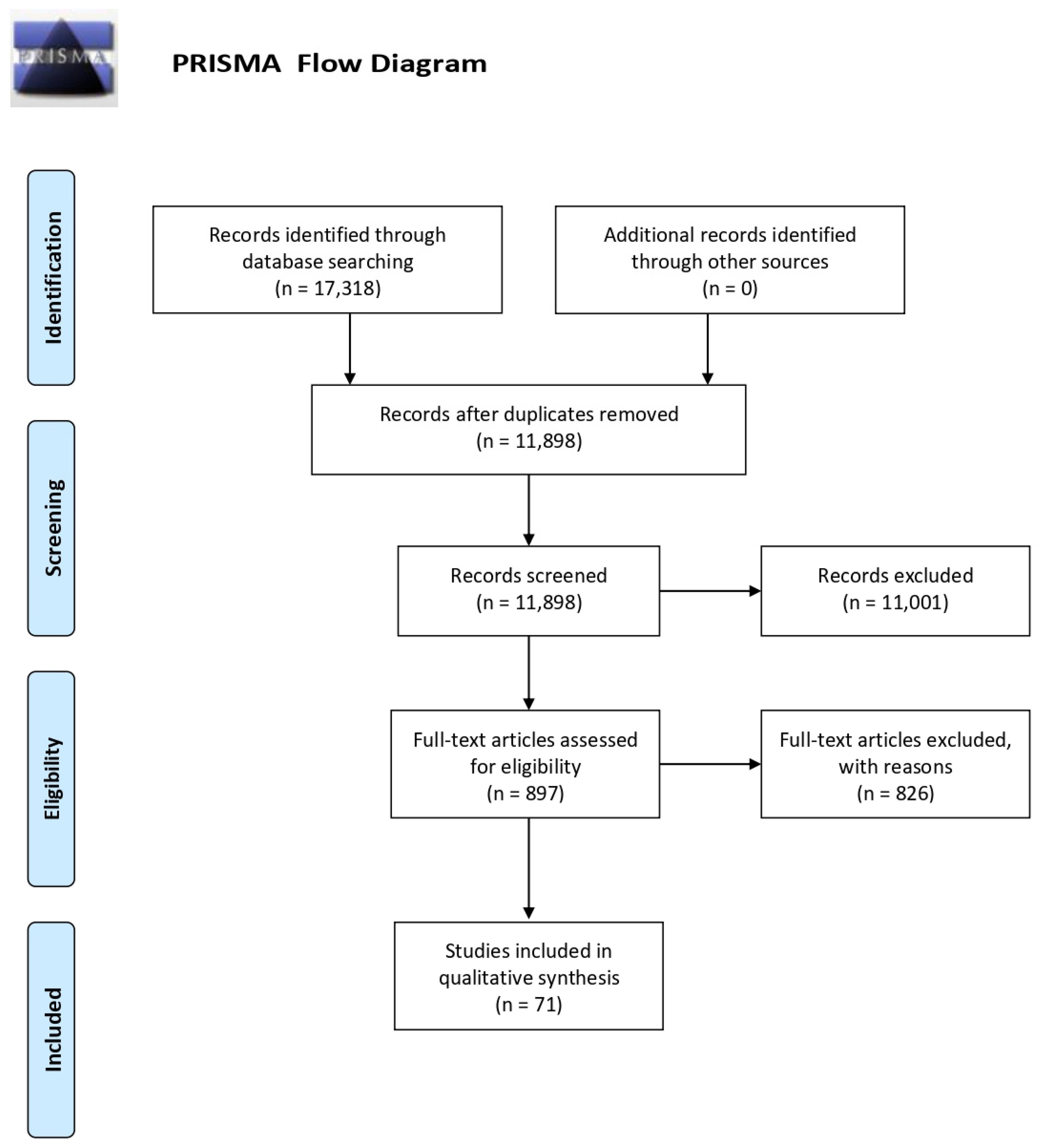
3.1. Studies Selection
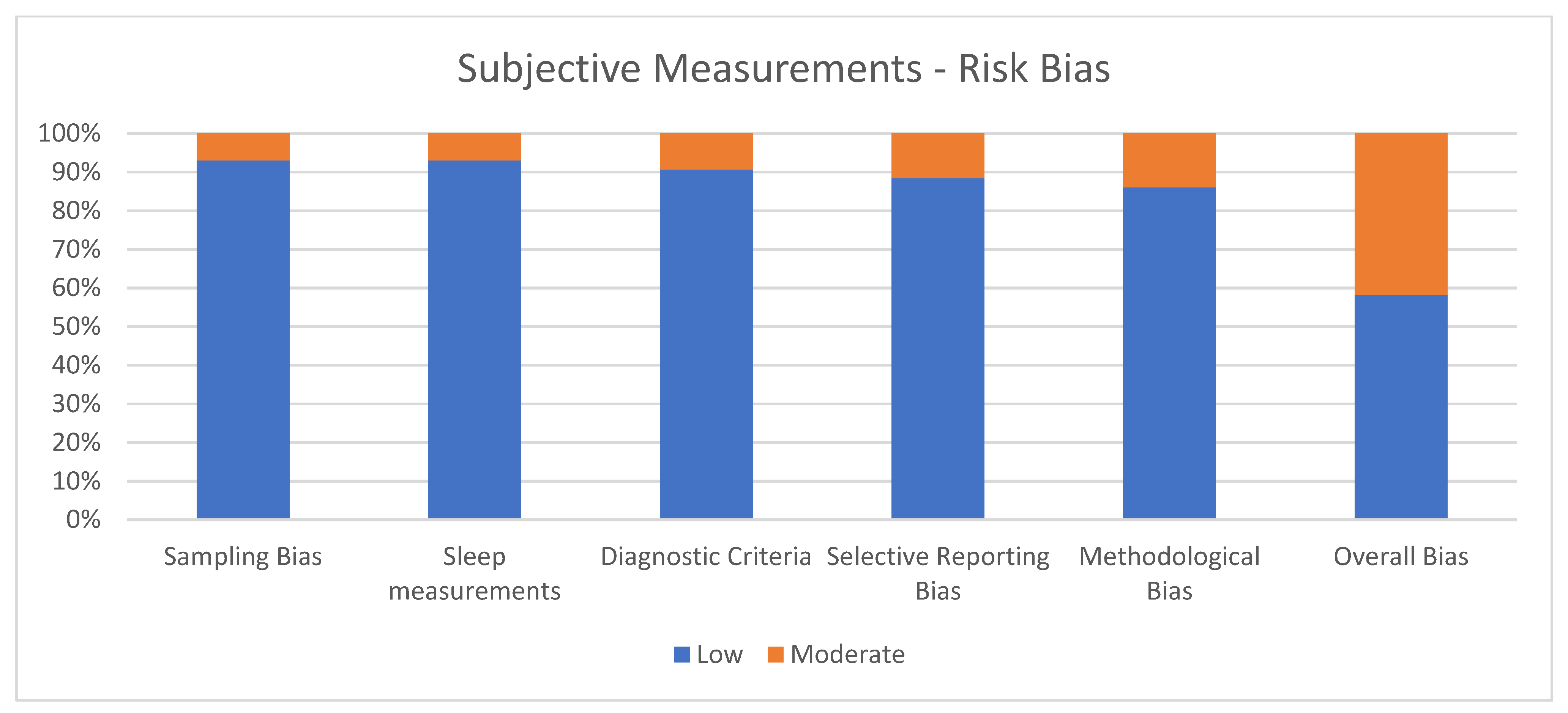
3.2. Quality Assessment of Subjective Measurements
3.3. Quality Assessment of Objective Measurements
3.4. Sleep in Healthy Older People
3.4.1. Subjective Measurements (N = 14)
Pittsburgh Sleep Quality Index—PSQI Results (N = 11)
Neuropsychiatric Inventory—NPI Results (N = 2)
Other Subjective Sleep Measurement Results (N = 4)
3.4.2. Objective Measurements (N = 7)
Polysomnographic Results (N = 3)
Actigraphy Results (N = 4)
3.5. Sleep in Pathological Older People
3.5.1. Diagnostic Criteria
3.5.2. Subjective Measurements (N = 27)
Pittsburgh Sleep Quality Index—PSQI Results (N = 11)
Neuropsychiatric Inventory—NPI Results (N = 13)
Other Subjective Measurements Results (N = 9)
3.5.3. Objective Measurements (N = 31)
Polysomnography Results (N = 23)
Actigraphy Results (N = 8)
3.6. Diurnal Sleepiness (N = 10)
3.6.1. Healthy Older People (N = 2)
3.6.2. Pathological Older People (N = 8)
4. Discussion
Limitation
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Guarino, A.; Favieri, F.; Boncompagni, I.; Agostini, F.; Casagrande, M. Executive functions in Alzheimer disease: A systematic review. Front. Aging Neurosci. 2019, 10, 437. [Google Scholar] [CrossRef] [PubMed]
- Guarino, A.; Forte, G.; Giovannoli, J.; Casagrande, M. Executive Functions in the elderly with mild cognitive impairment: A systematic review on motor and cognitive inhibition, conflict control and cognitive flexibility. Aging Ment. Health 2020, 24, 1028–1045. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Dementia. Available online: https://www.who.int/news-room/fact-sheets/detail/dementia (accessed on 1 September 2021).
- Ashraf, G.M.; Chibber, S.; Mohammad; Zaidi, S.K.; Tabrez, S.; Ahmad, A.; Shakil, S.; Mushtaq, G.; Baeesa, S.S.; Kamal, M.A. Recent Updates on the Association Between Alzheimer’s Disease and Vascular Dementia. Med. Chem. 2016, 12, 226–237. [Google Scholar] [CrossRef] [PubMed]
- Petersen, R.C. Mild Cognitive Impairment. Minneap. Minn. 2016, 22, 404–418. [Google Scholar] [CrossRef] [PubMed]
- Winblad, B.; Palmer, K.; Kivipelto, M.; Jelic, V.; Fratiglioni, L.; Wahlund, L.O.; Nordberg, A.; Bäckman, L.; Albert, M.; Almkvist, O.; et al. Mild cognitive impairment–beyond controversies, towards a consensus: Report of the International Working Group on Mild Cognitive Impairment. J. Intern. Med. 2004, 256, 240–246. [Google Scholar] [CrossRef] [PubMed]
- Cooke, J.R.; Ancoli-Israel, S. Normal and abnormal sleep in the elderly. Handb. Clin. Neurol. 2011, 98, 653–665. [Google Scholar]
- Dijk, D.J.; Duffy, J.F.; Czeisler, C.A. Contribution of circadian physiology and sleep homeostasis to age-related changes in human sleep. Chronobiol. Int. 2000, 17, 285–311. [Google Scholar] [CrossRef]
- Espiritu, J.R.D. Aging-Related Sleep Changes. Clin. Geriatr. Med. 2008, 24, 1–14. [Google Scholar] [CrossRef]
- Gadie, A.; Shafto, M.; Leng, Y.; Kievit, R.A. How are age-related differences in sleep quality associated with health outcomes? An epidemiological investigation in a UK cohort of 2406 adults. BMJ Open 2017, 7, e014920. [Google Scholar] [CrossRef]
- Mander, B.A.; Winer, J.R.; Walker, M.P. Sleep and human aging. Neuron 2017, 94, 19–36. [Google Scholar] [CrossRef]
- Monk, T.H. Aging human circadian rhythms: Conventional wisdom may not always be right. J. Biol. Rhythm. 2005, 20, 366–374. [Google Scholar] [CrossRef] [PubMed]
- Da Silva, R. Executive functions in Alzheimer disease: A systematic review. Sleep Sci. 2015, 8, 36–41. [Google Scholar] [CrossRef] [PubMed]
- Fortier-Brochu, É.; Beaulieu-Bonneau, S.; Ivers, H.; Morin, C.M. Insomnia and daytime cognitive performance: A meta-analysis. Sleep Med. Rev. 2012, 16, 83–94. [Google Scholar] [CrossRef] [PubMed]
- Martella, D.; Marotta, A.; Fuentes, L.J.; Casagrande, M. Inhibition of Return, but not Facilitation, Disappears under Vigilance Decrease due to Sleep Deprivation. Exp. Psychol. 2014, 61, 99–109. [Google Scholar] [CrossRef] [PubMed]
- Martella, D.; Casagrande, M.; Lupianez, J. Alerting, Orienting and Executive Control: The effects of sleep deprivation on the attentional networks. Exp. Brain Res. 2011, 210, 81–89. [Google Scholar] [CrossRef]
- Maccari, L.; Martella, D.; Marotta, A.; Sebastiani, M.; Banaj, N.; Fuentes, L.J.; Casagrande, M. Effects of sleep loss on emotion recognition: A dissociation between face and word stimuli. Exp. Brain Res. 2014, 232, 3147–3157. [Google Scholar] [CrossRef]
- Casagrande, M.; Forte, G.; Tambelli, R.; Favieri, F. The Coronavirus Pandemic: A possible Model of the Direct and Indirect Impact of the Pandemic on Sleep Quality in Italians. Nat. Sci. Sleep 2021, 13, 191–199. [Google Scholar] [CrossRef]
- Gothe, N.P.; Ehlers, D.K.; Salerno, E.A.; Fanning, J.; Kramer, A.F.; McAuley, E. Physical activity, sleep and quality of life in older adults: Influence of physical, mental and social well-being. Behav. Sleep Med. 2020, 18, 797–808. [Google Scholar] [CrossRef]
- Mecca, A.P.; Michalak, H.R.; McDonald, J.W.; Kemp, E.C.; Pugh, E.A.; Becker, M.L.; Alzheimer’s Disease Neuroimaging Initiative (ADNI). Sleep disturbance and the risk of cognitive decline or clinical conversion in the ADNI cohort. Dement. Geriatr. Cogn. Disord. 2018, 45, 232–242. [Google Scholar] [CrossRef]
- Kyle, S.D.; Sexton, C.E.; Feige, B.; Luik, A.I.; Lane, J.; Saxena, K.; Spiegelhalder, K. Sleep and cognitive performance: Cross-sectional associations in the UK Biobank. Sleep 2017, 38, 85–91. [Google Scholar] [CrossRef]
- Prince, T.M.; Abel, T. The impact of sleep loss on hippocampal function. Learn. Mem. 2013, 20, 558–569. [Google Scholar] [CrossRef]
- Xie, L.; Kang, H.; Xu, Q.; Chen, M.J.; Liao, Y.; Thiyagarajan, M.; O’Donnell, J.; Christensen, D.J.; Nicholson, C.; Iliff, J.J.; et al. Sleep Drives Metabolite Clearance from the adult brain. Science 2013, 342, 373–377. [Google Scholar] [CrossRef] [PubMed]
- Zimmerman, M.E.; Bigal, M.E.; Katz, M.J.; Brickman, A.M.; Lipton, R.B. Sleep onset/maintenance difficulties and cognitive function in nondemented older adults: The role of cognitive reserve. J. Int. Neuropsychol. Soc. 2012, 18, 461. [Google Scholar] [CrossRef]
- Casagrande, M.; Favieri, F.; Tambelli, R.; Forte, G. The enemy who sealed the world: Effects quarantine due to the COVID-19 on sleep quality, anxiety, and psychological distress in the Italian population. Sleep 2020, 75, 12–20. [Google Scholar] [CrossRef] [PubMed]
- Moran, M.; Lynch, C.A.; Walsh, C.; Coen, R.; Coakley, D.; Lawlor, B.A. Sleep disturbance in mild to moderate Alzheimer’s disease. Sleep 2005, 6, 347–352. [Google Scholar] [CrossRef] [PubMed]
- Nowak, L.; Davis, J.E. A Qualitative Examination of the Phenomenon of Sundowning. J. Nurs. Scholarsh 2007, 39, 256–258. [Google Scholar] [CrossRef] [PubMed]
- Kang, D.W.; Lee, C.U.; Lim, H.K. Role of Sleep Disturbance in the Trajectory of Alzheimer’s Disease. Clin. Psychopharmacol. Neurosci. 2017, 15, 89–99. [Google Scholar] [CrossRef]
- Beaulieu-Bonneau, S.; Hudon, C. Sleep disturbances in older adults with mild cognitive impairment. Int. Psychogeriatr. 2009, 21, 654–666. [Google Scholar] [CrossRef]
- Diem, S.J.; Blackwell, T.L.; Stone, K.L.; Yaffe, K.; Tranah, G.; Cauley, J.A.; Ensrud, K.E. Measures of sleep–wake patterns and risk of mild cognitive impairment or dementia in older women. Am J. Geriatr. 2016, 24, 248–258. [Google Scholar] [CrossRef]
- Dlugaj, M.; Weinreich, G.; Weimar, C.; Stang, A.; Dragano, N.; Wessendorf, T.E. Heinz Nixdorf Recall Study Investigative Group; Sleep-disordered breathing, sleep quality, and mild cognitive impairment in the general population. J. Alzheimer’s Dis. 2014, 41, 479–497. [Google Scholar] [CrossRef]
- Guarnieri, B.; Adorni, F.; Musicco, M.; Appollonio, I.; Bonanni, E.; Caffarra, P.; Caltagirone, C.; Cerroni, G.; Concari, L.; Cosentino, F.I.I.; et al. Prevalence of Sleep Disturbances in Mild Cognitive Impairment and Dementing Disorders: A Multicenter Italian Clinical Cross-Sectional Study on 431 Patients. Dement. Geriatr. Cogn. Disord. 2012, 33, 50–58. [Google Scholar] [CrossRef] [PubMed]
- Ju, Y.E.S.; McLeland, J.S.; Toedebusch, C.D.; Xiong, C.; Fagan, A.M.; Duntley, S.P.; Holtzman, D.M. Sleep quality and preclinical Alzheimer disease. JAMA Neurol. 2013, 70, 587–593. [Google Scholar] [CrossRef] [PubMed]
- Ju, Y.E.S.; Lucey, B.P.; Holtzman, D.M. Sleep and Alzheimer disease pathology—A bidirectional relationship. Nat. Rev. Neurol. 2014, 10, 115–119. [Google Scholar] [CrossRef] [PubMed]
- Lim, A.S.; Kowgier, M.; Buchman, A.S.; Bennett, D.A. Sleep fragmentation and the risk of incident Alzheimer’s disease and cognitive decline in older persons. Sleep 2013, 36, 1027–1032. [Google Scholar] [CrossRef]
- Sterniczuk, R.; Theou, O.; Rusak, B.; Rockwood, K. Sleep disturbance is associated with incident dementia and mortality. Curr. Alzheimer Res. 2013, 10, 767–775. [Google Scholar] [CrossRef]
- Liberati, A.; Douglas, G.A.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.A.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. J. Clin. Epidemiol. 2009, 62, 1–34. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. The PRISMA Group Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef]
- Higgins, J.P.; Altman, D.G.; Gøtzsche, P.C.; Jüni, P.; Moher, D.; Oxman, A.D.; Savović, J.; Schulz, K.F.; Weeks, L.; Sterne, J.A. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. Br. Med. J. 2011, 343, d5928. [Google Scholar] [CrossRef]
- Schmidt, C.; Peigneux, P.; Cajochen, C.; Collette, F. Adapting test timing to the sleep-wake schedule: Effects on diurnal neurobehavioral performance changes in young evening and older morning chronotypes. Chronobiol. Int. 2012, 29, 482–490. [Google Scholar] [CrossRef]
- Jirong, Y.; Changquan, H.; Hongmei, W.; Hongmei, D.; Bi-Rong, D. Association of sleep quality and dementia among long-lived Chinese older adults. Age 2013, 35, 1423–1432. [Google Scholar] [CrossRef]
- Buysse, D.J.; Reynolds, C.F., III; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The Pittsburgh Sleep Quality Index: A new Instrument for Psychiatric Practice and Research. J. Psychiatr. Res. 1989, 28, 193–213. [Google Scholar] [CrossRef]
- Bernstein, J.P.K.; De Vito, A.; Weitzner, D.S.; MacAulay, R.; Calamia, R.; Keller, J.N. Examining Relationships between Multiple Self-Reported Sleep Measures and Gait Domains in Cognitively Healthy Older Adults. J. Gerontol. 2019, 66, 47–54. [Google Scholar] [CrossRef] [PubMed]
- Brown, B.M.; Rainey-Smith, S.R.; Villemagne, V.L.; Weinborn, M.; Bucks, R.S.; Sohrabi, H.R.; Martins, R.N. The relationship between sleep quality and brain amyloid burden. J. Sleep Res. 2016, 39, 1063–1068. [Google Scholar] [CrossRef] [PubMed]
- Curcio, G.; Tempesta, D.; Scarlata, S.; Marzano, C.; Moroni, F.; Rossini, P.M.; De Gennaro, L. Validity of the Italian version of the Pittsburgh Sleep Quality Index (PSQI). Neurol. Sci. 2013, 34, 511–519. [Google Scholar] [CrossRef] [PubMed]
- De Gennaro, L.; Gorgoni, M.; Reda, F.; Lauri, G.; Truglia, I.; Cordone, S.; Rossini, P.M. The Fall of Sleep K-Complex in Alzheimer Disease. Sci. Rep. 2017, 7, 39688. [Google Scholar] [CrossRef]
- Fjell, A.; Idland, A.V.; Sala-Llonch, R.; Watne, L.O.; Borza, T.; Brækhus, A.; Walhovd, K.B. Neuroinflammation and tau interact with amyloid in predicting sleep problems in aging independently of atrophy. Cereb. Cortex 2018, 28, 2775–2785. [Google Scholar] [CrossRef]
- Landry, G.J.; Best, J.R.; Liu-Ambrose, T. Measuring sleep quality in older adults: A comparison using subjective and objective methods. Front. Aging Neurosci. 2015, 7, 166. [Google Scholar] [CrossRef]
- Mary, A.; Bourguignon, M.; Wens, V.L.; Op de Beeck, M.; Leproult, R.; De Tiège, X.; Peigneux, P. Aging reduces experience-induced sensorimotor plasticity A magnetoencephalographic study. Neuroimage Clin. 2015, 104, 59–68. [Google Scholar] [CrossRef] [PubMed]
- Rainey-Smith, S.R.; Mazzucchelli, G.N.; Villemagne, V.L.; Brown, B.M.; Porter, T.; Weinborn, M.; Laws, S.M. Genetic variation in Aquaporin-4 moderates the relationship between sleep and brain Aβ-amyloid burden. Trans. Psychiatry 2018, 8, 47. [Google Scholar] [CrossRef]
- Sani, T.P.; Bond, R.L.; Marshall, C.R.; Hardy, C.J.D.; Russell, L.L.; Moore, K.M.; Warren, J.D. Sleep symptoms in syndromes of frontotemporal dementia and Alzheimer’s disease: A proof-of-principle behavioural study. eNeurologicalSci 2019, 17, 100212. [Google Scholar] [CrossRef]
- Squelard, G.P.; Missotten, P.A.; Paquay, L.; De Lepeleire, J.; Buntinx, F.J.V.M.; Fontaine, O.; Ylieff, M.J.D. Neuropsychiatric Inventory data in a Belgian sample of elderly persons with and without dementia. Clin. Interv. Aging 2012, 7, 424–430. [Google Scholar] [CrossRef] [PubMed]
- Tatsch, M.F.; Bottino, C.M.D.; Azevedo, D.J.; Hototian, S.R.; Moscoso, M.A.; Folquitto, J.C.; Louza, M.R. Neuropsychiatric symptoms in Alzheimer disease and cognitively impaired, nondemented elderly from a community-based sample in Brazil: Prevalence and relationship with dementia severity. Am. J. Geriatr. Psychiatry 2006, 14, 438–445. [Google Scholar] [CrossRef] [PubMed]
- Bliwise, D.L.; Tinklenberg, J.R.; Yesavage, J.A. Timing of sleep and wakefulness in Alzheimer’s disease patients residing at home. Biol. Psychiatry 1992, 31, 1163–1165. [Google Scholar] [CrossRef]
- Wilckens, K.A.; Woo, S.G.; Erickson, K.I.; Wheeler, M.E. Sleep continuity and total sleep time are associated with task-switching and preparation in young and older adults. J. Sleep Res. 2014, 23, 508–516. [Google Scholar] [CrossRef] [PubMed]
- Kume, Y.; Kodama, A.; Sato, K.; Kurosawa, S.; Ishikawa, T.; Ishikawa, S. Sleep/awake status throughout the night and circadian motor activity patterns in older nursing-home residents with or without dementia, and older community-dwelling people without dementia. Int. Psychogeriatr. 2016, 28, 2001–2008. [Google Scholar] [CrossRef] [PubMed]
- Prinz, P.N.; Vitaliano, P.P.; Vitiello, M.V.; Bokan, J.; Raskind, M.; Peskind, E.; Gerber, C. Sleep, EEG and mental function changes in senile dementia of the Alzheimer’s type. Neurobiol. Aging 1982, 3, 361–370. [Google Scholar] [CrossRef]
- Reynolds, C.F.; Kupfer, D.J.; Taska, L.S.; Hoch, C.C. Slow wave sleep in elderly depressed, demented, and healthy subjects. J. Sleep Res. 1985, 8, 155–159. [Google Scholar] [CrossRef][Green Version]
- Wilckens, K.A.; Tudorascu, D.L.; Snitz, B.E.; Prince, J.C.; Aizenstein, H.J.; Lopez, O.L.; Cohen, A.D. Sleep moderates the relationship between amyloid beta and memory recall. Neurobiol. Aging 2018, 71, 142–148. [Google Scholar] [CrossRef]
- Paavilainen, P.; Korhonen, I.B.; Lötjönen, J.; Cluitmans, L.O.; Jylhä, M.; Särelä, A.; Partinen, M. Circadian activity rhythm in demented and non-demented nursing-home residents measured by telemetric actigraphy. J. Sleep Res. 2005, 14, 61–68. [Google Scholar] [CrossRef]
- Dykierek, P.; Stadtmüller, G.; Schramm, P.; Bahro, M.; van Calker, D.; Braus, D.F.; Riemann, D. The value of REM sleep parameters in differentiating Alzheimer’s disease from old-age depression and normal aging. J. Psychiatr. Res. 1998, 32, 1–9. [Google Scholar] [CrossRef]
- Fernández-Martínez, M.; Castro, J.; Molano, A.; Zarranz, J.J.; Rodrigo, R.M.; Ortega, R. Prevalence of neuropsychiatric symptoms in Alzheimer’s disease and vascular dementia. Curr. Alzheimer Res. 2008, 5, 61–69. [Google Scholar] [CrossRef] [PubMed]
- Gorgoni, M.; Lauri, L.; Truglia, I.; Cordone, S.; Sarasso, S.; Scarpelli, S.; De Gennaro, L. Parietal Fast Sleep Spindle Density Decrease in Alzheimer’s Disease and Amnesic Mild Cognitive Impairment. J. Neural Transpl. Plast. 2016, 2016, 8376108. [Google Scholar] [CrossRef] [PubMed]
- Matsuoka, T.; Imai, A.; Fujimoto, H.; Kato, Y.; Shibata, K.; Nakamura, K.; Narumoto, J. Neural Correlates of Sleep Disturbance in Alzheimer’s Disease: Role of the Precuneus in Sleep Disturbance. J. Alzheimer’s Dis. 2018, 63, 957–964. [Google Scholar] [CrossRef]
- Pocnet, C.; Antonietti, J.P.; Donati, A.; Popp, J.; von Gunten, A. Behavioral and psychological symptoms and cognitive decline in patients with amnestic MCI and mild AD: A two-year follow-up study. Int. Psychogeriatr. 2015, 27, 79–1389. [Google Scholar] [CrossRef]
- Scaricamazza, E.; Colonna, I.; Sancesario, G.M.; Assogna, F.; Orfei, M.D.; Franchini, F.; Liguori, C. Neuropsychiatric symptoms differently affect mild cognitive impairment and Alzheimer’s disease patients: A retrospective observational study. Neurol Sci 2019, 40, 1377–1382. [Google Scholar] [CrossRef] [PubMed]
- Shin, H.Y.; Han, H.J.; Shin, D.J.; Park, H.M.; Lee, Y.B.; Park, K.H. Sleep Problems Associated with Behavioral and Psychological Symptoms as Well as Cognitive Functions in Alzheimer’s Disease. Clin. Neurol. Neurosurg. 2014, 10, 203–209. [Google Scholar] [CrossRef] [PubMed]
- Tadokoro, K.; Ohta, Y.; Hishikawa, N.; Nomura, E.; Wakutani, Y.B.; Takao, Y.; Abe, K. Discrepancy of subjective and objective sleep problems in Alzheimer’s disease and mild cognitive impairment detected by a home-based sleep analysis. J. Clin. Neurosci. 2020, 74, 76–80. [Google Scholar] [CrossRef] [PubMed]
- Yatawara, C.; Hiu, S.; Tan, L.; Kandiah, N. Neuropsychiatric symptoms in South-East Asian patients with mild cognitive impairment and dementia: Prevalence, subtypes, and risk factors. Int. J. Geriatr. Psychiatry 2017, 33, 122–130. [Google Scholar] [CrossRef]
- Zhou, G.; Liu, S.; Yu, X.; Zhao, X.; Ma, L.; Shan, P. High prevalence of sleep disorders and behavioral and psychological symptoms of dementia in late-onset Alzheimer disease: A study in Eastern China. Am. J. Med. 2019, 98, e18405. [Google Scholar] [CrossRef]
- Hoch, C.C.; Reynolds, C.F., III; Houck, P.R. Sleep patterns in Alzheimer, depressed, and healthy elderly. West. J. Nurs. Res. 1998, 10, 239–256. [Google Scholar] [CrossRef]
- Hot, P.; Rauchs, G.; Bertran, F.; Denise, P.; Desgranges, B.; Clochon, P.; Eustache, F. Changes in sleep theta rhythm are related to episodic memory impairment in early Alzheimer’s disease. Biol. Psychol. 2011, 87, 334–339. [Google Scholar] [CrossRef] [PubMed]
- Kundermann, B.; Thum, A.; Rocamora, R.; Haag, A.; Krieg, J.C.; Hemmeter, U. Comparison of polysomnographic variables and their relationship to cognitive impairment in patients with Alzheimer’s disease and frontotemporal dementia. J. Psychiatr. Res. 2011, 45, 1585–1592. [Google Scholar] [CrossRef] [PubMed]
- Liguori, C.; Chiaravalloti, A.; Nuccetelli, M.; Izzi, F. Hypothalamic dysfunction is related to sleep impairment and CSF biomarkers in Alzheimer’s disease. J. Neurol. 2017, 264, 2215–2223. [Google Scholar] [CrossRef] [PubMed]
- Liguori, C.; Mercuri, M.B.; Nuccetelli, M.; Izzi, F.; Bernardini, S.; Placidi, F. Cerebrospinal Fluid Orexin Levels and Nocturnal Sleep Disruption in Alzheimer’s Disease Patients Showing Neuropsychiatric Symptoms. J. Neurol. 2018, 66, 993–999. [Google Scholar] [CrossRef]
- Loewenstein, R.J.; Weingartner, H.; Gillin, J.C.; Kaye, W.; Ebert, W.; Mendelson, W.B. Disturbances of sleep and cognitive functioning in patients with dementia. Neurobiol. Aging 1982, 3, 371–377. [Google Scholar] [CrossRef]
- Montplaisir, J.; Petit, D.; Lorrain, D.; Gauthier, S. Sleep in Alzheimer’s disease: Further considerations on the role of brainstem and forebrain cholinergic populations in sleep-wake mechanisms. J. Sleep Res. 1995, 18, 145–148. [Google Scholar] [CrossRef]
- Prinz, P.N.; Peskind, E.R.; Vitaliano, P.P.; Raskind, M.A.; Eisdorfer, C.; Zemcuznikov, N.; Gerber, C.J. Changes in the sleep and waking EEGs of nondemented and demented elderly subjects. J. Am. Geriatr. Soc. 1982, 30, 86–93. [Google Scholar] [CrossRef]
- Rauchs, G.; Schabus, M.; Parapatics, S.; Bertran, F.; Clochon, P.; Anderer, P. Is there a link between sleep changes and memory in Alzheimer’s disease? NeuroReport: For Rapid. Neurosci. Res. Commun. 2008, 19, 1159–1162. [Google Scholar]
- Reynolds, C.F.; Kupfer, D.J.; Taska, L.S.; Hoch, C.C.; Spiker, D.G.; Sewitch, D.E.; Morycz, R. EEG sleep in elderly depressed, demented, and healthy subjects. Biol. Psychiatry 1985, 20, 431–442. [Google Scholar] [CrossRef]
- Tsuno, N.; Shigeta, M.; Hyoki, K.; Faber, P.L.; Lehman, D. Fluctuations of Source of EEG Activity during Transation. Neuropsychobiology 2004, 50, 267–272. [Google Scholar] [CrossRef]
- Khou, C.S.; Rendzia, B.; Watts, A. Evaluation of waist-worn actigraphy monitors for the assessment of sleep in older adults with and without Alzheimer’s disease. J. Rehabil. Assist. Technol. Eng. 2018, 5, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.H.; Friedland, R.; Whitehouse, P.I.; Woo, J.I. Twenty-Four-Hour Rhythms of Sleep-Wake Cycle and Temperature in Alzheimer’s Disease. J. Neuropsychiatry Clin. 2004, 16, 192–198. [Google Scholar] [CrossRef] [PubMed]
- Liguori, C.; Spanetta, M.; Izzi, F.; Franchini, F.; Nuccetelli, M.; Sancesario, G.M.; Di Santo, S.; Bernardini, S.; Mercuri, N.B.; Placidi, F. Sleep-wake cycle in Alzheimer’s disease is associated with tau pathology and orexin dysregulation. J. Alzheimer’s Dis. 2020, 74, 501–508. [Google Scholar] [CrossRef]
- Liguori, C.; Placidi, F.; Izzi, F.; Spanetta, M.; Mercuri, N.B.; Di Pucchio, A. Sleep dysregulation, memory impairment, and CSF biomarkers during different levels of neurocognitive functioning in Alzheimer’s disease course. Alzheimer’s Res. Ther. 2020, 12, 1–13. [Google Scholar]
- Liguori, C.; Romigi, A.; Nuccetelli, M.; Zannino, S.; Sancesario, G.; Martorana, A.; Placidi, F. Orexinergic System Dysregulation, Sleep Impairment, and Cognitive Decline in Alzheimer Disease. JAMA Neurol. 2014, 71, 1498–1505. [Google Scholar] [CrossRef]
- Fernández-Martínez, M.; Molano, A.; Castro, J.; Zarranz, J.J. Prevalence of neuropsychiatric symptoms in mild cognitive impairment and Alzheimer’s disease, and its relationship with cognitive impairment. Curr. Alzheimer Res. 2010, 7, 517–526. [Google Scholar] [CrossRef] [PubMed]
- Hita-Yañez, E.; Atienza, M.; Cantero, J.L.; Hita-Yanez, E.; Atienza, M.; Cantero, J.L. Polysomnographic and subjective sleep markers of mild cognitive impairment. J. Sleep Res. 2013, 36, 1327–1334. [Google Scholar] [CrossRef]
- Lee, K.S.; Cho, H.S.; Hong, C.H.; Kim, D.G.; Oh, B.H. Differences in neuropsychiatric symptoms according to mild cognitive impairment subtypes in the community. Dement. Geriatr. Cogn. Disord. 2008, 26, 212–217. [Google Scholar] [CrossRef]
- Muangpaisan, W.; Intalapaporn, S.; Assantachai, P. Neuropsychiatric symptoms in the community-based patients with mild cognitive impairment and the influence of demographic factors. Int. J. Geriatr. Psychiatry 2008, 23, 699–703. [Google Scholar] [CrossRef]
- Ng, K.P.; Pascoal, T.A.; Mathotaarachchi, S.; Chung, C.O.; Benedet, A.L.; Shin, M.; Initi, A.D.N. Neuropsychiatric symptoms predict hypometabolism in preclinical Alzheimer disease. Neurology 2017, 88, 1814–1821. [Google Scholar] [CrossRef]
- Palmer, K.; Mitolo, M.; Burgio, F.; Meneghello, F.; Venneri, A. Sleep Disturbance in Mild Cognitive Impairment and Association with Cognitive Functioning. A Case-Control Study. Front. Aging Neurosci. 2018, 10, 360. [Google Scholar] [CrossRef] [PubMed]
- Peters, K.R.; Rockwood, K.; Black, S.E.; Hogan, D.B.; Gauthier, S.G.; Loy-English, I.; Feldman, H.H. Neuropsychiatry symptom clusters and functional disability in cognitively-impaired-not-demented individuals. Am J. Geriatr. 2008, 16, 136–144. [Google Scholar] [CrossRef] [PubMed]
- Reijs, B.L.R.; Vos, S.J.B.; Soininen, H.; Lotjonen, J.; Koikkalainen, J.; Pikkarainen, M.; Visser, P.J. Association between Later Life Lifestyle Factors and Alzheimer’s Disease Biomarkers in Non-Demented Individuals: A Longitudinal Descriptive Cohort Study. J. Alzheimer’s Dis. 2017, 60, 1387–1395. [Google Scholar] [CrossRef] [PubMed]
- Rozzini, L.; Chilovi, B.V.; Peli, M.; Conti, M.; Rozzini, R.; Trabucchi, M.; Padovani, A. Anxiety symptoms in mild cognitive impairment. Int. J. Geriatr. Psychiatry 2009, 24, 300–305. [Google Scholar] [CrossRef]
- Sanchez-Espinosa, M.P.; Atienza, M.; Cantero, J.L. Sleep deficits in mild cognitive impairment are related to increased levels of plasma amyloid-beta and cortical thinning. Neuroimage Clin. 2014, 98, 395–404. [Google Scholar] [CrossRef]
- Sun, Q.; Lou, L.; Ren, H.; Wei, C.; Xing, M.; Cheng, Y.; Zhang, N. Semantic clustering and sleep in patients with amnestic mild cognitive impairment or with vascular cognitive impairment-no dementia. Int. Psychogeriatr. 2016, 28, 1493–1502. [Google Scholar] [CrossRef] [PubMed]
- Tuna, F.; Üstündağ, A.; Başak, C.H.; Tuna, H. Rapid Geriatric Assessment, Physical Activity, and Sleep Quality in Adults Aged more than 65 Years: A Preliminary Study. J. Nutr. Health Aging 2019, 23, 617–622. [Google Scholar] [CrossRef]
- Yu, J.; Mahendran, R.; Rawtaer, I.; Kua, E.H.; Feng, L. Poor sleep quality is observed in mild cognitive impairment and is largely unrelated to depression and anxiety. Aging Ment. Health 2017, 21, 823–828. [Google Scholar] [CrossRef]
- Carnicelli, L.; Maestri, M.; Di Coscio, E.; Tognoni, G.; Fabbrini, M.; Schirru, A.; Bonanni, E. A longitudinal study of polysomnographic variables in patients with mild cognitive impairment converting to Alzheimer’s disease. J. Sleep Res. 2019, 28, e12821. [Google Scholar] [CrossRef]
- Wams, E.J.; Wilcock, G.K.; Foster, R.G.; Wulff, K. Sleep-Wake Patterns and Cognition of Older Adults with Amnestic Mild Cognitive Impairment (aMCI): A Comparison with Cognitively Healthy Adults and Moderate Alzheimer’s Disease Patients. Curr. Alzheimer Res. 2017, 14, 1030–1041. [Google Scholar] [CrossRef]
- Westerberg, C.E.; Lundgren, E.M.; Florczak, S.M.; Mesulam, M.M.; Weintraub, S.; Zee, P.C.; Paller, K.A. Sleep Influences the Severity of Memory Disruption in Amnestic Mild Cognitive Impairment Results from Sleep Self-assessment and Continuous Activity Monitoring. Alzheimer Dis. Assoc. Disord. 2010, 24, 325–333. [Google Scholar] [CrossRef] [PubMed]
- Westerberg, C.E.; Mander, B.A.; Florczak, S.M.; Weintraub, S.; Mesulam, M.M.; Zee, P.C.; Paller, K.A. Concurrent Impairments in Sleep and Memory in Amnestic Mild Cognitive Impairment. J. Int. Neuropsychol. Soc. 2012, 18, 490–500. [Google Scholar] [CrossRef] [PubMed]
- Hita-Yañez, E.; Atienza, M.; Cantero, J.L.; Hita-Yanez, E.; Atienza, M.; Cantero, J.L. Sleep patterns in elders with mild cognitive impairment: The role of memory decline and ApoE ε4 genotype. Curr. Alzheimer Res. 2012, 9, 290–297. [Google Scholar] [CrossRef]
- Maestri, M.; Carnicelli, L.; Tognoni, G.; Di Coscio, E.; Giorgi, F.S.; Volpi, L.; Bonanni, E. Non-rapid eye movement sleep instability in mild cognitive impairment: A pilot study. Sleep 2015, 16, 1139–1145. [Google Scholar] [CrossRef] [PubMed]
- Naismith, S.L.; Hickie, I.B.; Terpening, Z.; Rajaratnam, S.M.W.; Hodges, J.R.; Bolitho, S.; Lewis, S.J.G. Circadian Misalignment and Sleep Disruption in Mild Cognitive Impairment. J. Alzheimer’s Dis. 2014, 38, 857–866. [Google Scholar] [CrossRef] [PubMed]
- Xie, L.Q.; Yang, B.X.; Liao, Y.H.; Gao, G.X.; Jiang, N.; Zhou, J.; Richmond, C.J. Sleep Disturbance in Older Adults with or without Mild Cognitive Impairment and Its Associated Factors Residing in Rural Area, China. Int. J. Geriatr. Psychiatry 2020, 33, 122–130. [Google Scholar] [CrossRef]
- Alfini, A.; Albert, M.; Faria, A.V.; Soldan, A.; Pettigrew, C.; Wanigatunga, S.; Zipunnikov, V.; Spira, A.P. Associations of actigraphic sleep and circadian rest/activity rhythms with cognition in the early phase of Alzheimer’s disease. Sleep Adv. 2021, 2, zpab007. [Google Scholar] [CrossRef]
- Wang, L.; Li, J.; Wang, Z.; Du, Y.; Sun, T.; Na, L.; Niu, Y. Social capital and cognitive decline: Does sleep duration mediate the association? PLoS ONE 2021, 16, e0252208. [Google Scholar] [CrossRef]
- Liu, S.; Pan, J.; Lei, Q.; He, L.; Zhong, B.; Meng, Y.; Li, Z. Spontaneous K-Complexes may be biomarkers of the progression of amnestic mild cognitive impairment. Sleep Med. 2020, 67, 99–109. [Google Scholar] [CrossRef]
- McKhann, G.; Drachman, D.; Folstein, M.; Katzman, R.; Price, D.; Stadlan, E.M. Clinical diagnosis of Alzheimer’s disease: Report of the NINCDS-ADRDA Work Group* under the auspices of Department of Health and Human Services Task Force on Alzheimer’s Disease. Neurology 1984, 34, 939. [Google Scholar] [CrossRef]
- Jack, C.R., Jr.; Bennett, D.A.; Blennow, K.; Carrillo, M.C.; Dunn, B.; Haeberlein, S.B.; Holtzman, D.M.; Jagust, W.; Jessen, F.; Karlawish, J.; et al. NIA-AA research framework: Toward a biological definition of Alzheimer’s disease. Alzheimer’s Dement. 2018, 14, 535–562. [Google Scholar] [CrossRef] [PubMed]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 3rd ed.; American Psychiatric Publishing Inc.: Washington, DC, USA, 1980. [Google Scholar]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 4th ed.; American Psychiatric Publishing Inc.: Washington, DC, USA, 1994. [Google Scholar]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Publishing Inc.: Washington, DC, USA, 2013. [Google Scholar]
- Petersen, R.C.; Smith, G.E.; Waring, S.C.; Ivnik, R.J.; Tangalos, E.G.; Kokmen, E. Mild cognitive impairment: Clinical characterization and outcome. Arch. Neurol. 1999, 56, 303–308. [Google Scholar] [CrossRef] [PubMed]
- Petersen, R.C.; Smith, G.E.; Waring, S.C.; Ivnik, R.J.; Kokmen, E.; Tangelos, E.G. Aging, memory, and Mild Cognitive Impairment. Int. Psychogeriatr. 1997, 9, 65–69. [Google Scholar] [CrossRef]
- Petersen, R.C. Mild Cognitive Impairment. N. Engl. J. Med. 2011, 364, 2227–2234. [Google Scholar] [CrossRef]
- Petersen, R.C.; Aisen, P.; Boeve, B.F.; Geda, Y.E.; Ivnik, R.J.; Knopman, D.S.; Mielke, M.; Pankratz, V.S.; Roberts, R.; Rocca, W.A.; et al. Mild cognitive impairment due to Alzheimer disease in the community. Ann. Neurol. 2013, 74, 199–208. [Google Scholar] [CrossRef]
- Albert, M.S.; DeKosky, S.T.; Dickson, D.; Dubois, B.; Feldman, H.H.; Fox, N.C.; Gamst, A.; Holtzman, D.M.; Jagust, W.J.; Petersen, R.C.; et al. The diagnosis of mild cognitive impairment due to Alzheimer’s disease: Recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimer’s Dement. 2011, 7, 270–279. [Google Scholar] [CrossRef]
- Cockrell, J.R.; Folstein, M.F.; Copeland, J.R.M.; Abou-Saleh, M.T.; Blazer, D.G. Principles and Practice of Geriatric Psychiatry; John Wiley & Sons: New York, NY, USA, 2002; pp. 147–158. [Google Scholar]
- Portet, F.; Ousset, P.J.; Visser, P.J.; Frisoni, G.B.; Nobili, F.; Scheltens, P.; Vellas, B.; Touchon, J.; MCI Working Group of the European Consortium on Alzheimer’s Disease (EADC). Mild cognitive impairment (MCI) in medical practice: A critical review of the concept and new diagnostic procedure. Report of the MCI Working Group of the European Consortium on Alzheimer’s Disease. J. Neurol. Neurosurg. Psychiatry 2006, 77, 714–718. [Google Scholar] [CrossRef] [PubMed]
- Artero, S.; Petersen, R.; Touchon, J.; Ritchie, K. Revised criteria for mild cognitive impairment: Validation within a longitudinal population study. Dement. Geriatr. Cogn. Disord. 2006, 22, 465–470. [Google Scholar] [CrossRef]
- Johar, I.; Mollenhauer, B.; Aarsland, D. Cerebrospinal fluid biomarkers of cognitive decline in Parkinson’s disease. Int. Rev. Neurobiol. 2017, 132, 275–294. [Google Scholar]
- Morris, J.C. Clinical dementia rating: A reliable and valid diagnostic and staging measure for dementia of the Alzheimer type. Int. Psychogeriatr. 1997, 9, 173–176. [Google Scholar] [CrossRef]
- Vitiello, V.M. Sleep Disorders and aging: Understanding the causes. J. Gerontol. A Biol. Sci. Med. 1997, 52, M189–M191. [Google Scholar] [CrossRef] [PubMed]
- Ward, A.M.; McLaren, D.G.; Schultz, A.P.; Chhatwal, J.; Boot, B.P.; Hedden, T.; Sperling, R.A. Daytime sleepiness is associated with decreased default mode network connectivity in both young and cognitively intact elderly subjects. J. Sleep Res. 2013, 36, 1609–1615. [Google Scholar] [CrossRef] [PubMed]
- Bombois, S.; Derambure, P.; Pasquier, F.; Monaca, C. Sleep Disorders in Aging and Dementia. J. Nutr. Health Aging 2010, 14, 212–217. [Google Scholar] [CrossRef] [PubMed]
- Frohnhofen, H.Y.; Schlitzer, J.; Netzer, N. Sleep in older adults and in subject with dementia. Z Gerontol. Geriat. 2017, 50, 603–608. [Google Scholar] [CrossRef]
- Lim, A.S.; Yu, L.; Kowgier, M.; Schneider, J.A.; Buchman, A.S.; Bennett, D.A. Modification of the relationship of the apolipoprotein E ε4 allele to the risk of Alzheimer disease and neurofibrillary tangle density by sleep. JAMA Neurol. 2017, 70, 1544–1551. [Google Scholar] [CrossRef]
- Lucey, B.P.; McCullough, A.; Landsness, E.C.; Toedebusch, C.D.; McLeland, J.S.; Zaza, A.M.; Holtzman, D.M. Reduced non–rapid eye movement sleep is associated with tau pathology in early Alzheimer’s disease. Sci. Trans. Med. 2019, 11, 474. [Google Scholar] [CrossRef]
- Shokri-Kojori, E.; Wang, G.J.; Wiers, C.E.; Demiral, S.B.; Gou, M.; Kim, S.W.; Volkow, N.D. β-Amyloid accumulation in the human brain after one night of sleep deprivation. Proc. Sci. 2018, 115, 4483–4488. [Google Scholar] [CrossRef]
- Vaou, O.E.; Lin, S.H.; Branson, C.; Auerbach, S. Sleep and dementia. Curr. Sleep Med. Rep. 2008, 4, 134–142. [Google Scholar] [CrossRef]
- Hu, M.; Zhang, P.; Li, C.; Tan, Y.; Li, G.; Xu, D.; Chen, L. Sleep disturbance in mild cognitive impairment: A systematic review of objective measures. Neurol. Sci. 2017, 38, 1363–1371. [Google Scholar] [CrossRef]
- D’Rozario, A.L.; Chapman, J.L.; Phillips, C.L.; Palmer, J.R.; Hoyos, C.M.; Mowszowski, L.; Duffy, S.L.; Marshall, N.S.; Benca, R.; Naismith, S.L. Objective measurement of sleep in mild cognitive impairment: A systematic review and meta-analysis. Sleep Med. Rev. 2020, 52, 101308. [Google Scholar] [CrossRef]
- Carskadon, M.A.; Van den Hoed, J.; Dement, W.C. Sleep and daytime sleepiness in the elderly. J. Ger. Psychiat. 1980, 13, 135–151. [Google Scholar]
- Ohayon, M.M.; Vecchierini, M.F. Daytime sleepiness and cognitive impairment in the elderly population. Arch. Intern. Medic. 2002, 162, 201–208. [Google Scholar] [CrossRef] [PubMed]
- Sforza, E.; Pichot, V.; Saint Martin, M.; Barthélémy, J.C.; Roche, F. Prevalence and determinants of subjective sleepiness in healthy elderly with unrecognized obstructive sleep apnea. Sleep Med. 2015, 16, 981–986. [Google Scholar] [CrossRef] [PubMed]
- Alperin, N.; Wiltshire, J.; Lee, S.H.; Ramos, A.R.; Hernandez-Cardenache, R.; Rundek, T.; Curiel Cid, R.; Loewenstein, D. Effect of sleep quality on amnestic mild cognitive impairment vulnerable brain regions in cognitively normal elderly individuals. Sleep 2019, 42, zsy254. [Google Scholar] [CrossRef] [PubMed]
- Jack, C.R., Jr.; Wiste, H.J.; Vemuri, P.; Weigand, S.D.; Senjem, M.L.; Zeng, G.; Bernstein, M.A.; Gunter, J.L.; Pankratz, V.S.; Aisen, P.S.; et al. Brain beta-amyloid measures and magnetic resonance imaging atrophy both predict time-to-progression from mild cognitive impairment to Alzheimer’s disease. Brain 2010, 133, 3336–3348. [Google Scholar] [CrossRef]
- Marotta, A.; Martella, D.; Maccari, L.; Sebastiani, M.; Casagrande, M. Poor vigilance affects attentional orienting triggered by central uninformative gaze and arrow cues. Cogn. Proc. 2014, 15, 503–513. [Google Scholar] [CrossRef]
- Casagrande, M.; Martella, D.; Di Pace, E.; Pirri, F.; Guadalupi, F. Orienting and alerting: Effects of 24 h of prolonged wakefulness. Exp. Brain Res. 2006, 171, 184–193. [Google Scholar] [CrossRef]

| Database | N° |
|---|---|
| PsychINFO | 2192 |
| PsycArticles | 15 |
| Medline | 4633 |
| PubMed | 10,478 |
| Authors | Group | N° | Age (SD) | (%F) | MMSE (SD) | Measurements | Results |
|---|---|---|---|---|---|---|---|
| Bernstein et al. [43] | HS | 423 | 69.9 (7.6) | 64.4 | 29.5 | PSQI ISI | PSQI 11.2% poor sleep quality. ISI 7.8% mild or severe insomnia. |
| Bliwise et al. [54] | HS | 30 | 73.8 | 66.7 | ≥28 | Sleep Diary | No difference between males and females. |
| Brown et al. [44] | HS | 184 | 75.5 (6.1) | 58.7 | 28.9 (1.3) | PSQI | 41% poor sleep quality. |
| Curcio et al. [45] | HS | 10 | 68.6 (7.0) | 50 | 26.7 (1.3) | PSQI | PSQI TOT: 3.9 (0.9) |
| De Gennaro et al. [46] | HS | 20 | 70.3 | 60 | 28.75 | PSQI | PSQI TOT: 6.0 (0.7) |
| Fjell et al. [47] | HS | 91 | 72 | 51.6 | 29 | PSQI | PSQI TOT: 6.3 (3.8) |
| Jirong et al. [41] | HS | 251 | 93.7 (3.4) | 49.8 | - | PSQI | 37% poor sleep quality. |
| Landry et al. [48] | HS | 78 | 71.6 (6.6) | 67 | 28.8 (1.2) | PSQI Sleep Diary | PSQI 64% poor sleep quality. Sleep Diary SL: 22.6 (16.2) Awakenings: 2.1 (1) Sleep windows (min): 461.7 (50.2) SD (min): 398 (61.7) |
| Mary et al. [49] | HS | 14 | 69.1 (1.5) | 57.1 | Mattis: 141.4 (1.9) | PSQI St. Mary’s Hospital Sleep Questionnaire | PSQI SD (hr): 7.39 (1.0) SL (min): 12.5 (16.3) SMHSQ SD (hr): 7.1 (1.1) SL (min): 12.4 (12.3) |
| Rainey-Smith et al. [50] | HS | 462 | 75 (6) | 58.1 | 28.9 (1.3) | PSQI | 49.1% poor sleep quality |
| Sani et al. [51] | HS | 25 | 67.3 (7.5) | 60 | 29.5 (0.7) | PSQI | 28% sleep disturbances. 12% excessive diurnal sleepiness. 20% disruptive sleep events. |
| Schmidt et al. [40] | HS | 14 | 67.2 (4.0) | 57.1 | Mattis: 139.4 (3.8) | PSQI | PSQI TOT: 3.9 (2.0) |
| Squelard et al. [52] | HS | 46 | 79.3 (7.9) | 76.1 | 24.7 (6.0) | NPI | 6.5% sleep disturbances. |
| Tatsch et al. [53] | HS | 78 | 72.3 (8.2) | 67.9 | 25.2 (3.6) | NPI | 3.8% sleep disturbances. |
| Authors | Group | N° | Age (SD) | (%F) | MMSE (SD) | Measurements | Results |
|---|---|---|---|---|---|---|---|
| Curcio et al. [45] | HS | 10 | 68.6 (7.0) | 50 | 26.7 (1.3) | PSG | L NREM1(min): 18.0 (4.4) L NREM2(min): 21.1 (16.4) L SWS (min): 81.9 (6.5) L REM (min): 146.7 (32.1) NREM1 (%): 12.6 (2.3) NREM2 (%): 69.9 (2.0) SWS (%): 0.4 (0.2) REM (%): 17.0 (1.6) Awakenings (n): 25.0 (2.5) TST (min): 347.5 (22.3) TBT (min): 532.9 (171.7) SE (%): 70.8 (6.4) |
| Prinz et al. [57] | HS | 22 | 69.0 (6.4) | 50 | 29.6 | PSG | TIB: 456.3 (37.7) NREM 3–4 (%TIB): 8.9 (5.2) REM (%TIB): 16.8 (4.1) W (%TIB): 21 (7.2) Awakenings (n°): 13.6 (4.7) LREM: 65 (24.7) |
| Reynolds III et al. [58] | HS | 25 | 69.0 (5.0) | 68 | 29.2 (0.9) | PSG | SL (min): 22.2 (16.9) W (min): 47.4 (32.8) TSA (min): 368.7 (44.5) Arousal (n): 6.8 (2.7) SE (%): 84.1 (8.3) Sleep maintenance (%): 88.6 (7.3) NREM1(%): 9.7 (8.2) NREM2(%): 64.9 (8.3) Stage N (%): 2.6 (6.2) NREM3–4(%): 2.5 (3.9) REM (%): 20.2 (4.9) LREM: 57.6 (16.9) REM time (min): 75.0 (21.2) |
| Authors | Group | N° | Age (SD) | (%F) | MMSE (SD) | Measurements | Results |
|---|---|---|---|---|---|---|---|
| Kume et al. [56] | HS | 17 | 82.2 (4.2) | 76.4 | CDR: 0 | Actigraphy | TST (min): 380.2 (43.7) SL: 13.1 (13.5) SE (%): 83.7 (4.1) Awakening time (min): 57.5 (20.7) |
| Landry et al. [48] | HS | 78 | 71.6 (6.6) | 67 | 28.8 (1.2) | Actigraphy | 19.5% poor sleep quality. |
| Paavilainen et al. [60] | HS | 19 | 81.5 (9.0) | - | 26.2 (2.9) | Actigraphy | TIB (h): 9.0 (1.2) |
| Wilckens et al. 2018 [59] | HS | 45 | 62.8 (6.0) | 71.1 | 28.8 (1.0) | Actigraphy | TST (min): 362.4 (63.1) WASO (min): 63.4 (42.5) |
| Authors | Group | N° | Age (SD) | (%F) | MMSE (SD) | Diagnostic Criteria | Measurements | Results |
|---|---|---|---|---|---|---|---|---|
| Fernández-Martínez et al. [62] | AD | 37 | 74.4 (6.7) | 64.9 | 18.4 (2.8) | NINCDS–ADRDA | NPI | 35.1% sleep disturbances. |
| Fernández-Martínez et al. [87] | MCI HS | 91 50 | 74.2 (5.3) 74.5 (7.0) | 45.1 66.0 | 26.4 (1.8) 28.6 (1.1) | Petersen | NPI | MCI: 23.1% sleep disturbances. HS: 14% sleep disturbances. |
| Gorgoni et al. [63] | AD aMCI HS | 15 15 15 | 70.8 71.1 70.8 | 66.7 60.0 33.3 | 16.1 26.1 29.1 | DSM IV Petersen | PSQI | No difference has been found. |
| Hita-Yañez et al. [88] | HS MCI | 25 25 | 67.1 (5.3) 70.5 (6.8) | 52 28 | 28.1 (1.3) 26.7 (2.4) | DSM V Petersen CDR ≤ 0.5 | Interview | MCI: higher WASO. SL and awakenings. MCI: lower sleep quality and SD. |
| Lee et al. [89] | aMCI naMCI | 217 165 | 72.8 (6.9) 71.5 (5.8) | 62.2 69.9 | 20.8 (4.5) 22.1 (3.8) | Petersen | NPI | aMCI: 18.8% sleep disturbances. naMCI: 18% sleep disturbances. No difference between aMCI and naMCI has been found. |
| Matsuoka et al. [64] | AD | 63 | 79 (6.9) | 69.8 | 20.1 (4.2) | NINCDS–ADRDA | NPI | 30.2% sleep disturbances. |
| Muangpaisan et al. [90] | MCI HS | 77 30 | 66.3 (7.9) 63.7 (7.3) | 35 25 | 26.5 (1.0) 28.1 (1.8) | Petersen | NPI | MCI: 45.5% sleep disturbances. HS: 23.3% sleep disturbances. No difference between HS and MCI has been found. |
| Naismith et al. [106] | HS MCI | 26 26 | 65.9 (9.8) 70.1 (9.9) | 53.8 34.6 | 29.2 (1.1) 27.5 (2.1) | Petersen | PSQI | No difference between HS and MCI has been found. |
| Ng et al. [91] | HS Pre-AD | 22 33 | 75.2 (7.2) 76.9 (6.2) | 36.3 60.6 | 29.0 (1.5) 28.9 (0.9) | MMSE < 24 | NPI | Pre-AD: higher sleep disturbances. |
| Palmer et al. [92] | MCI HS | 69 72 | 75.7 (7.7) 71.8 (7.7) | 60.9 58.3 | 25.6 (2.9) 28.6 (1.4) | Petersen | SCADS | MCI: 21.7% poor sleep quality. HS: 15.3% poor sleep quality. |
| Peters et al. [93] | MCI | 193 | 67 (11.4) | 53 | 26.3 | DSM-IV-TR | NPI | 39.9% sleep disturbance. |
| Pocnet et al. [65] | HS MCI AD | 64 46 54 | 66 73 79 | 54.7 65.2 72.2 | T1,2 = 29/29 T1,2 = 28/28 T1,2 = 24/23 | Winblad NINCDS–ADRDA | NPI | Follow-up (2 years) MCI: increased sleep disturbances. |
| Reijs et al. [94] | MCI | 353 | 70.6 (6.9) | 59.0 | 26.2 (2.9) | NINCDS–ADRDA | NPI | 22% sleep disturbances. |
| Rozzini et al. [95] | MCI | 13 | 71.8 (7.4) | 55 | 27.6 (1.9) | Artero | NPI | NPI: 0.5 (1.2) |
| Scaricamazza et al. [66] | MCI AD | 20 45 | 69.7 (6.2) 66.4 (9.2) | 60 64.4 | 26.8 (1.6) 22.4 (1.2) | Petersen NINCDS–ADRDA | NPI | AD: higher sleep disturbances. |
| Shin et al. [67] | AD | 63 | 74.8 (6.1) | 73 | 16.7 (4.4) | NINCDS–ADRDA | PSQI | PSQI TOT: 5.4 (3.9) SE (%): 87.2 (11.7) TIB (min): 510 (93.5) |
| Sun et al. [97] | aMCI HS | 50 38 | 68.8 (5.9) 68.7 (5.5) | 66.0 63.1 | 26.6 (1.3) 28.5 (1.1) | Petersen | PSQI ISI | PSQI aMCI: higher poor sleep quality. ISI aMCI: higher severe insomnia. |
| Tadokoro et al. [68] | HS MCI AD | 22 20 21 | 74.0 (7.8) 77.6 (6.5) 75.5 (6.2) | 59.1 50.0 61.9 | 29.0 (1.1) 26.9 (2.3) 20.7 (6.6) | DSM 5 | PSQI | AD: higher poor sleep quality than MCI and HS. |
| Tuna et al. [98] | MCI | 56 | 69.7 (4.0) | 58.9 | 7 | RCS < 8 | PSQI | 53.6% poor sleep quality. |
| Wams et al. [101] | HS aMCI | 18 8 | 73.8 (4.6) 77.1 (4.0) | 46.1 50 | MMSE ≥ 27 26 < MMSE < 20 | NINCDS–ADRDA | PSQI JSQ | No difference between HS and aMCI has been found. |
| Westerberg et al. [102] | aMCI HS | 10 10 | 71.1 72.5 | 80 70 | 27.8 29.3 | Petersen | PSQI Karolinska Sleep Diary | No difference between HS and aMCI has been found. |
| Westerberg et al. [103] | HS aMCI | 16 8 | 72.7 (5.1) 75.6 (7.2) | - - | 28.4 (0.4) 27.3 (0.6) | Petersen | PSQI | No difference between HS and aMCI has been found. |
| Xie et al. [107] | MCI HS | 479 734 | 60–80+ 60–80+ | 61.4 49.3 | - - | Portet Johar | AIS | MCI: higher SL, TST, WASO, early awakenings and sleep disturbances. |
| Yatawara et al. [69] | MCI AD | 38 158 | 64.4 (9.1) 69.6 (9.6) | 47.3 46.8 | 27.3 (1.7) 21.1 (4.7) | Petersen NIA-AA | NPI | AD: 40% sleep disturbances. MCI: 31% sleep disturbances. |
| Yu et al. [99] | HS MCI | 48 48 | 68.1 (5.6) 67.9 (4.9) | 66.7 83.3 | MoCA: 26.2 (3.5) 24.2 (3.6) | Petersen | PSQI | MCI: higher poor sleep quality. |
| Zhou et al. [70] | AD HS | 84 92 | 66.5 (7.0) 69.0 (8.2) | 66.7 56.5 | 18.1 (3.2) 28.7 (1.8) | NINCDS–ADRDA | PSQI NPI | PSQI AD: higher poor sleep quality. NPI AD: higher sleep disturbances. |
| Wang et al. [109] | HS MCI | 804 151 | 66.6 (5.1) 68.7 (5.8) | 49 76.4 | - - 23.6 (5.4) | MMSE < 17 Cui | Interview | MCI: Higher SD than HS. |
| Authors | Group | N° | Age (SD) | (%F) | MMSE (SD) | Diagnostic Criteria | Measurements | Results |
|---|---|---|---|---|---|---|---|---|
| Carnicelli et al. [100] | MCI HS | 19 11 | 69.8 (15.5) 69.2 (12.6) | 47.3 45.5 | 25.3 (1.2) 29.3 (0.6) | Petersen | PSG | MCI: lower %REM. |
| De Gennaro et al. [46] | HS AD | 20 20 | 70.3 72.0 | 60 65 | 28.75 16.4 | DSM IV NINCDS–ADRDA | PSG | AD: higher LREM1, LREM2. AD: lower %SWS. |
| Dykierek et al. [61] | AD HS | 35 42 | 62.1 (8.9) 64.4 (7.5) | 54.4 47.6 | 19.5 (5.2) 29.2 (1.0) | NINCDS–ADRDA | PSG | AD: lower SPT and REM density. |
| Gorgoni et al. [63] | AD aMCI HS | 15 15 15 | 70.8 71.1 70.8 | 66.7 60.0 33.3 | 16.1 26.1 29.1 | DSM IV NIA–AA Petersen | PSG | AD: lower %SWS than HS. No difference between MCI vs. HS and AD vs. MCI has been found. |
| Hita-Yañez et al. [104] | HS MCI | 25 25 | 67.1 (5.3) 70.5 (6.8) | 52 28 | 28.1 (1.3) 26.7 (2.4) | Petersen | PSG | MCI: higher AI SWS. MCI: lower %REM. |
| Hoch et al. [71] | AD HS | 20 23 | 71.6 (4.9) 68.9 (3.8) | 65 65.2 | 17.3 (5.7) 29.2 (0.9) | DSM III NINCDS–ADRDA | PSG | AD: higher SL, %NREM, and total recording time. AD: lower SE and %NREM2. |
| Hot et al. [72] | AD HS | 14 14 | 76.7 (3.8) 76.7 (4.1) | 50 57.1 | 24.8 (2.4) 29.4 (1.0) | NINCDS–ADRDA | PSG | AD: lower %SE. |
| Kundermann et al. [73] | AD | 15 | 71.1 (ES: 1.8) | 40 | MMST: 21.7 (ES: 1.1) | NINCDS–ADRDA | PSG | SPT: 402.5 min (ES: 15.2) TST: 292.8 min (ES: 21.6) WASO:136.2 min (ES: 20.1) LREM: 124.1 min (ES: 19.4) SE: 59.5% (ES: 4.6) NREM 1: 8.6% (ES: 1.0) NREM 2: 30.6% (ES: 2.6) SWS: 13.1% (ES: 2.5) REM: 8.0% (ES: 1.2) |
| Liguori et al. [86] | AD HS | 48 29 | 70.5 (7.6) 70.4 (9.9) | 47.9 48.3 | 19.4 (5.3) 28.7 (1.1) | NINCDS–ADRDA | PSG | AD: higher LREM, WASO. and %NREM1. AD: lower %SE, %NREM3, %REM. |
| Liguori et al. [74] | AD HS | 18 18 | 71.6 (3.9) 74.4 (2.8) | 55.6 61.1 | 22.6 (1.3) 28.9 (2.1) | NINCDS–ADRDA | PSG | AD: higher SL, LREM, WASO, and NREM1. AD: lower TST, %SE, NREM3, and REM. |
| Liguori et al. [75] | AD | 20 | 70.75 (8.1) | 55 | 21.9 (5.2) | Biomarkers Diagnostic Criteria | PSG | TST (min): 368.7 (70.6) SE (%): 74.7 (13.7) LREM: 204.8(147.8) WASO: 130.8 (88.9) NREM1: 31.9 (10.2) NREM2: 49.4 (12.2) NREM3: 12.1 (8.2) REM: 6.5 (4.1) |
| Loewenstein et al. [76] | HS AD | 8 9 | 61.9 60.3 | 37.5 33.3 | - | DSM III | PSG | AD: lower delta waves. |
| Maestri et al. [105] | HS MCI AD | 11 11 11 | 72.7 (5.9) 68.5 (7.0) 69.2 (12.6) | 63.6 63.6 45.5 | 29.3 (1.0) 24.9 (1.2) 21.2 (0.8) | NINCDS–ADRDA | PSG | AD: higher NREM1 and NREM2 than HS. AD: higher NREM1 than MCI. AD: lower TST, NREM3, and REM than HS. MCI: lower REM than HS. |
| Montplaisir et al. [77] | HS AD | 10 10 | 58.3 60.6 | - - | 29.3 (5.3) 20.6 (1.0) | NINCDS–ADRDA | PSG | AD: higher EEG Slowing Index. AD: lower K-complex, sleep spindles and REM. |
| Naismith et al. [106] | HS MCI | 26 26 | 65.9 (9.8) 70.1 (9.9) | 53.8 34.6 | 29.2 (1.1) 27.5 (2.1) | Petersen | PSG | MCI: lower LREM and WASO. |
| Prinz et al. [78] | HS AD | 11 10 | 72.2 (10.6) 73.3 (11.4) | 0 - | - 3.3 (6.5) | MMSE > 20 | PSG | AD: higher wakefulness. AD: lower NREM3, NREM4, and REM |
| Rauchs et al. [79] | AD HS | 14 14 | 76.9 (4.1) 75.1 (4.6) | 64.3 64.3 | 24.9 (2.0) 29.4 (0.9) | NINCDS–ADRDA MMSE < 21 | PSG | AD: lower sleep spindles activity. |
| Reynolds III et al. [80] | HS AD | 24 22 | 69.5 (4.5) 70.9 (8.1) | 66.7 68.1 | - 16.5 (5.0) | DSM III | PSG | AD: lower TSA. |
| Sanchez-Espinosa et al. [96] | HS aMCI | 21 21 | 67 (5.5) 69.8 (6.5) | 47.6 28.6 | 28.3 (1.3) 26.7 (2.5) | Petersen | PSG | aMCI: higher AI SWS. aMCI: lower %REM. |
| Tsuno et al. [81] | AD | 12 | 75.6 (10.7) | 83.3 | 14.4 (5.7) | NINCDS–ADRDA | PSG | SL (min): 14.6 (5.9) |
| Westerberg et al. [103] | HS aMCI | 16 8 | 72.7 (5.1) 75.6 (7.2) | - - | 28.4 (0.4) 27.3 (0.6) | Petersen | PSG | aMCI: lower SWS. |
| Liguori et al. [84] | MCI mAD msAD HS | 59 56 48 41 | 67.4 (8.4) 69.9 (7.3) 71.7 (7.2) 67.2 (8.6) | 52.6 62.5 60.4 52 | 28.9 (1.5) 24.5 (1.9) 15.4 (3.2) 29.2 (0.9) | NIA–AA Albert | PSG | msAD: lower TST, %SE NREM3%, REM% than mAD, MCI, and HS. msAD: higher NREM1% than MCI and HS. msAD: higher TIB than HS, MCI, and mAD. mAD: higher TST, NREM3%, REM% than msAD but lower than MCI and HS. mAD: higher TIB than msAD. mAD: higher WASO, LREM and NREM1% than HS. mAD: higher SE% than msAD but lower than HS. MCI: higher TST, NREM3% than mAD and msAD. MCI: higher SE% than msAD but lower than HS. MCI: higher REM% than msAD and mAD but lower than HS. MCI: higher LREM and WASO than HS. MCI: higher NREM1% than HS but lower than mAD and msAD. MCI: lower TIB than msAD. HS: higher TST and NREM3% than mAD and msAD. HS: higher SE%, REM% and lower WASO, NREM%1 than MCI, mAD and msAD. HS: lower LREM than MCI and mAD. |
| Liu et al. [110] | HS sMCI pMCI | 22 25 20 | 70.6 (6.0) 71.6 (5.2) 70.8 (4.3) | 63.6 52 45 | 28.4 (1.7) 26.7 (2.0) 26.9 (1.6) | Petersen | PSG | HS: higher TST and SE% than sMCI and pMCI. HS: lower LREM than sMCI and pMCI. |
| Authors | Group | N° | Age (SD) | (%F) | MMSE (SD) | Diagnostic Criteria | Measurement | Results |
|---|---|---|---|---|---|---|---|---|
| Alfini et al. [108] | HS MCI | 153 26 | 71.8 (8.3) 77.3 (7.9) | 67.3 50 | - - | Albert | Actigraphy | MCI: lower SE% than HC. |
| Khou et al. [82] | HS AD | 51 35 | 73.4 (6.5) 73.7 (7.8) | 69 31 | - - | NINCDS−ADRDA | Actigraphy | AD: higher TST and TIB. |
| Lee et al. [83] | AD HS | 7 11 | 77.0 (4.3) 74.2 (5.2) | 57.1 63.6 | 1 < CDR < 2 CDR: 0 | NINCDS−ADRDA | Actigraphy | No difference between HS and AD has been found. |
| Liguori et al. [85] | HS AD | 10 18 | 61.8(11.2) 71.0 (5.9) | 40 55.5 | - - | NIA–AA | Actigraphy | AD: lower SE% and higher SL. |
| Tadokoro et al. [68] | HS MCI AD | 22 20 21 | 74.0 (7.8) 77.6 (6.5) 75.5 (6.2) | 59.1 50.0 61.9 | 29.0 (1.1) 26.9 (2.3) 20.7 (6.6) | DSM 5 | Actigraphy | AD: higher NREM than MCI and HS. AD: lower REM than MCI and HS. MCI: lower REM than HS. |
| Wams et al. [101] | HS aMCI | 18 8 | 73.8 (4.6) 77.1 (4.0) | 46.1 50 | MMSE ≥ 27 26 < MMSE < 20 | NINCDS−ADRDA | Actigraphy | No difference between HS and aMCI has been found. |
| Westerberg et al. [102] | aMCI HS | 10 10 | 71.1 72.5 | 80 70 | 27.8 29.3 | Petersen | Actigraphy | aMCI: higher variability. aMCI: start sleep later. |
| Wilckens et al. [59] | HS MCI | 28 13 | 82.1 (7.2) 86.7 (10.2) | 71.4 30.8 | 28.4 (1.4) 26.8 (2.0) | Albert | Actigraphy | No difference between HS and MCI has been found. |
| Authors | Group | N° | Age (SD) | (%F) | MMSE (SD) | Measurements | Results |
|---|---|---|---|---|---|---|---|
| Bernstein et al. [43] | HS | 423 | 69.9 (7.6) | 64.4 | 29.5 | ESS | 18% excessive diurnal sleepiness. |
| Ward et al. [127] | HS | 84 | 73.2 (5.7) | 48.8 | 29 (0.9) | ESS | ESS: 5.9 (3.7) |
| Authors | Group | N° | Age (SD) | (%F) | MMSE (SD) | Diagnostic Criteria | Measurements | Results |
|---|---|---|---|---|---|---|---|---|
| Hita-Yañez et al. [88] | HS MCI | 25 25 | 67.1 (5.3) 70.5 (6.8) | 52 28 | 28.1 (1.3) 26.7 (2.4) | DSM 5 Petersen CDR ≤ 0.5 | ESS | No difference between HS and MCI has been found. |
| Naismith et al. [106] | HS MCI | 26 26 | 65.9 (9.8) 70.1 (9.9) | 53.8 34.6 | 29.2 (1.1) 27.5 (2.1) | Petersen | ESS | MCI: higher diurnal sleepiness. |
| Sanchez-Espinosa et al. [96] | HS aMCI | 21 21 | 67 (5.5) 69.8 (6.5) | 47.6 28.6 | 28.3 (1.3) 26.7 (2.5) | Petersen | ESS | No difference between HS and aMCI has been found. |
| Sun et al. [97] | aMCI HS | 50 38 | 68.8 (5.9) 68.7 (5.5) | 66.0 63.1 | 26.6 (1.3) 28.5 (1.1) | Petersen | ESS | aMCI: higher diurnal sleepiness. |
| Tadokoro et al. [68] | HS MCI AD | 22 20 21 | 74.0 (7.8) 77.6 (6.5) 75.5 (6.2) | 59.1 50.0 61.9 | 29.0 (1.1) 26.9 (2.3) 20.7 (6.6) | DSM 5 | ESS | No difference has been found. |
| Westerberg et al. [102] | aMCI HS | 10 10 | 71.1 72.5 | 80 70 | 27.8 29.3 | Petersen | ESS | No difference between HS and aMCI has been found. |
| Westerberg et al. [103] | HS aMCI | 16 8 | 72.7 (5.1) 75.6 (7.2) | - - | 28.4 (0.4) 27.3 (0.6) | Petersen | ESS | No difference between HS and aMCI has been found. |
| Zhou et al. [70] | AD HS | 84 92 | 66.5 (7.0) 69.0 (8.2) | 66.7 56.5 | 18.1 (3.2) 28.7 (1.8) | NINCDS–ADRDA | ESS | AD: higher diurnal sleepiness. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Casagrande, M.; Forte, G.; Favieri, F.; Corbo, I. Sleep Quality and Aging: A Systematic Review on Healthy Older People, Mild Cognitive Impairment and Alzheimer’s Disease. Int. J. Environ. Res. Public Health 2022, 19, 8457. https://doi.org/10.3390/ijerph19148457
Casagrande M, Forte G, Favieri F, Corbo I. Sleep Quality and Aging: A Systematic Review on Healthy Older People, Mild Cognitive Impairment and Alzheimer’s Disease. International Journal of Environmental Research and Public Health. 2022; 19(14):8457. https://doi.org/10.3390/ijerph19148457
Chicago/Turabian StyleCasagrande, Maria, Giuseppe Forte, Francesca Favieri, and Ilaria Corbo. 2022. "Sleep Quality and Aging: A Systematic Review on Healthy Older People, Mild Cognitive Impairment and Alzheimer’s Disease" International Journal of Environmental Research and Public Health 19, no. 14: 8457. https://doi.org/10.3390/ijerph19148457
APA StyleCasagrande, M., Forte, G., Favieri, F., & Corbo, I. (2022). Sleep Quality and Aging: A Systematic Review on Healthy Older People, Mild Cognitive Impairment and Alzheimer’s Disease. International Journal of Environmental Research and Public Health, 19(14), 8457. https://doi.org/10.3390/ijerph19148457






