A Systematic Review and Bayesian Network Meta-Analysis Investigating the Effectiveness of Psychological Short-Term Interventions in Inpatient Palliative Care Settings
Abstract
:1. Background
2. Methods
2.1. Eligibility Criteria
- (1)
- Participants: PIP of 18 years and older; at least 50% of the study population must be inpatients.
- (2)
- Intervention: psychological short-term interventions (e.g., mindfulness-based interventions, LRI, CBT, and related approaches) administered within eight weeks from baseline to follow-up assessment; number of sessions may range from one to twelve.
- (3)
- Comparison groups: control groups, e.g., standard care, no treatment, waitlist control, active attention control.
- (4)
- Outcomes: anxiety, depression, and distress.
- (5)
- Study designs: randomised controlled trial (RCT), clinical controlled trial, or waitlist-controlled trial.
- (1)
- Studies of complementary therapies such as physical (e.g., yoga, physiotherapy), music, art, or aromatherapy as well as group, partner, or caregiver-delivered therapies.
- (2)
- Interventions delivered online and solely by telephone.
- (3)
- Studies written in a language other than English or German.
- (4)
- Grey literature, conference proceedings, abstracts, posters, editorials, protocols, unavailable full texts, or studies that report only qualitative results.
- (5)
- Studies with insufficient information on outcome data or inclusion criteria (studies comparing only two equal interventions with no additional control condition were excluded).
2.2. Search Strategy
2.3. Study Selection
2.4. Analysis Method
3. Results
3.1. Result of the Literature Search
3.2. Data Collection Process
3.3. Outcome Measures
3.3.1. Depression
3.3.2. Anxiety
3.3.3. Distress
3.4. Risk of Bias Assesment
4. Study Characteristics
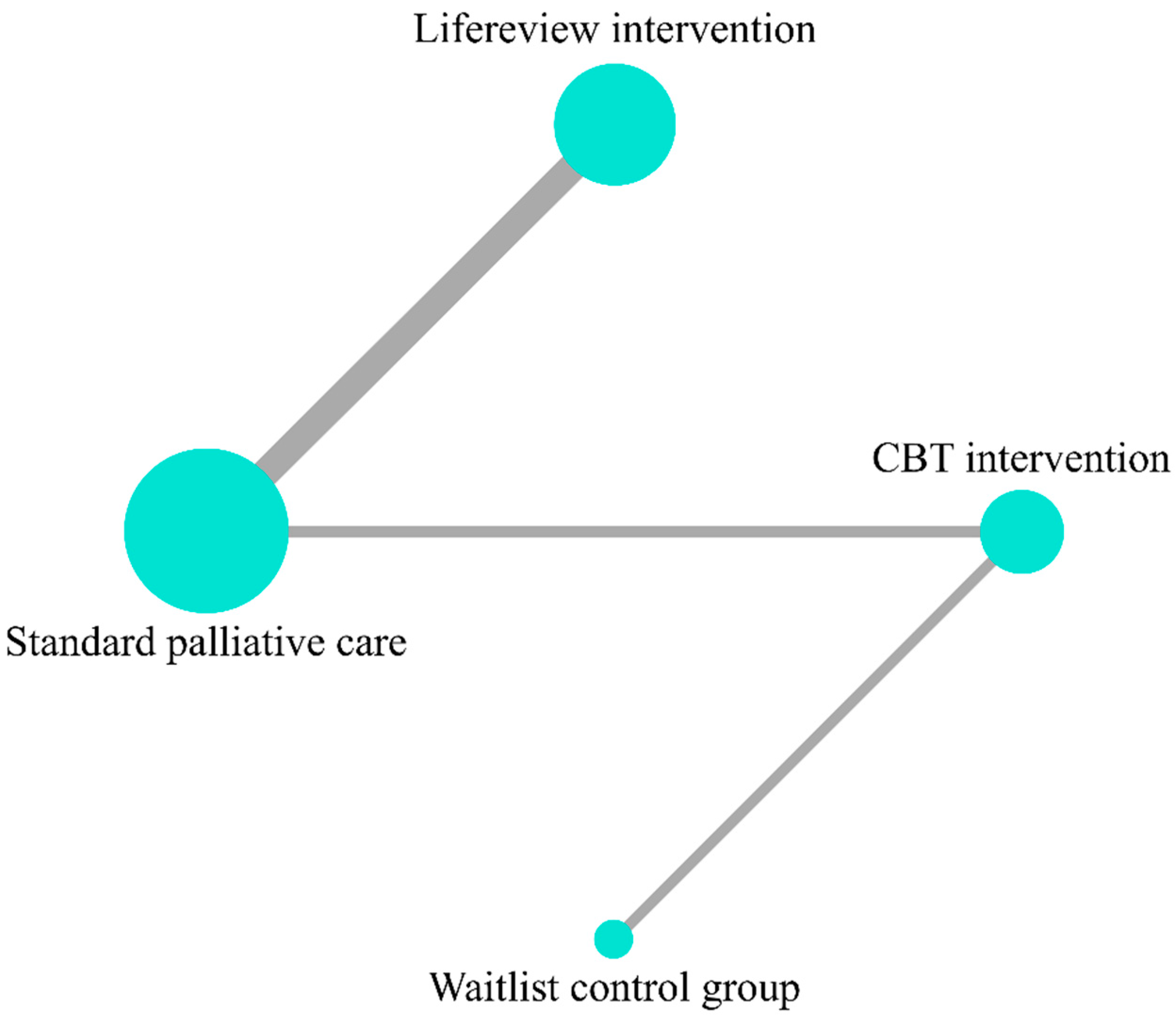
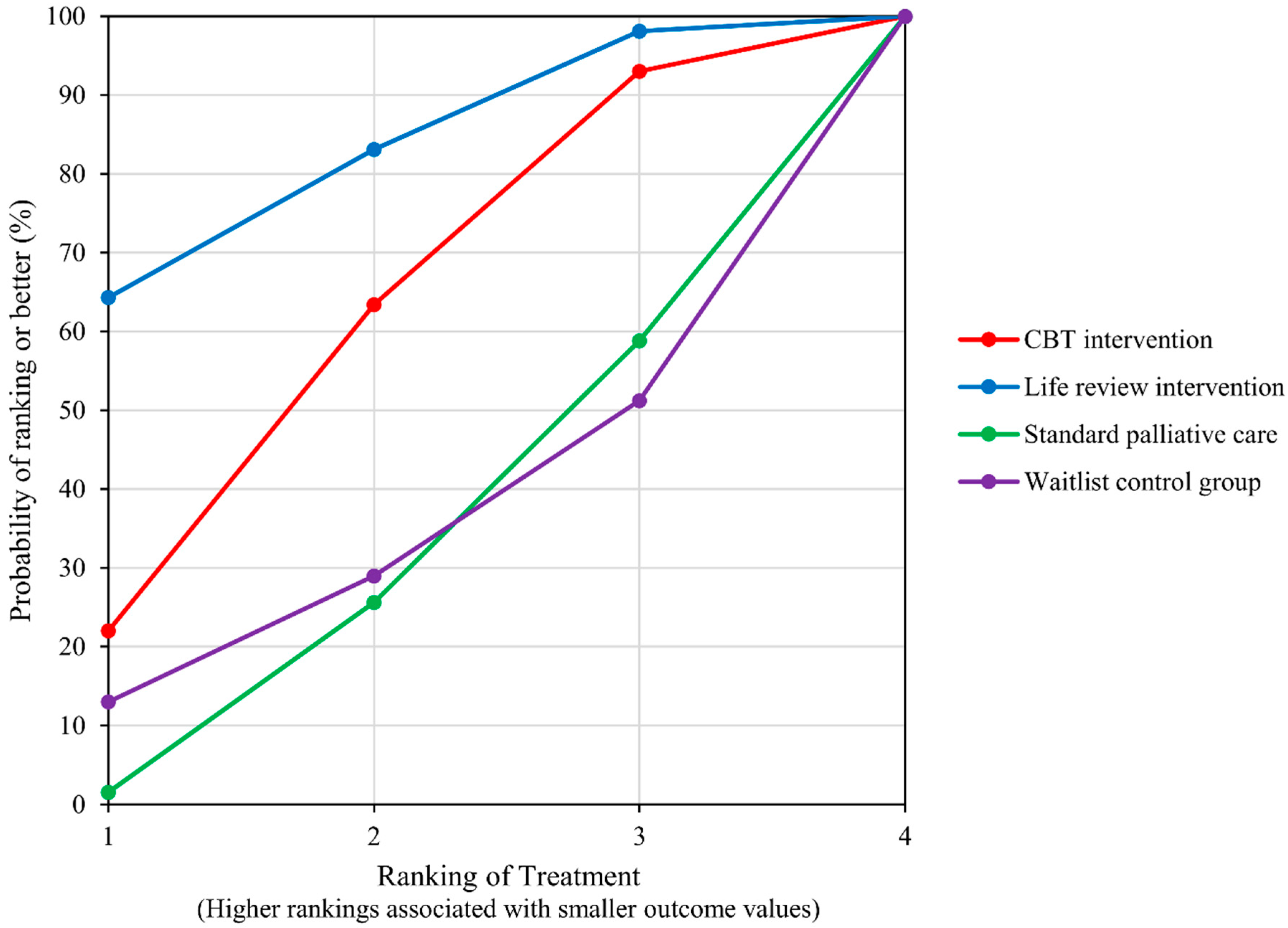
4.1. Anxiety and Depression (as Measured by the HADS Total)
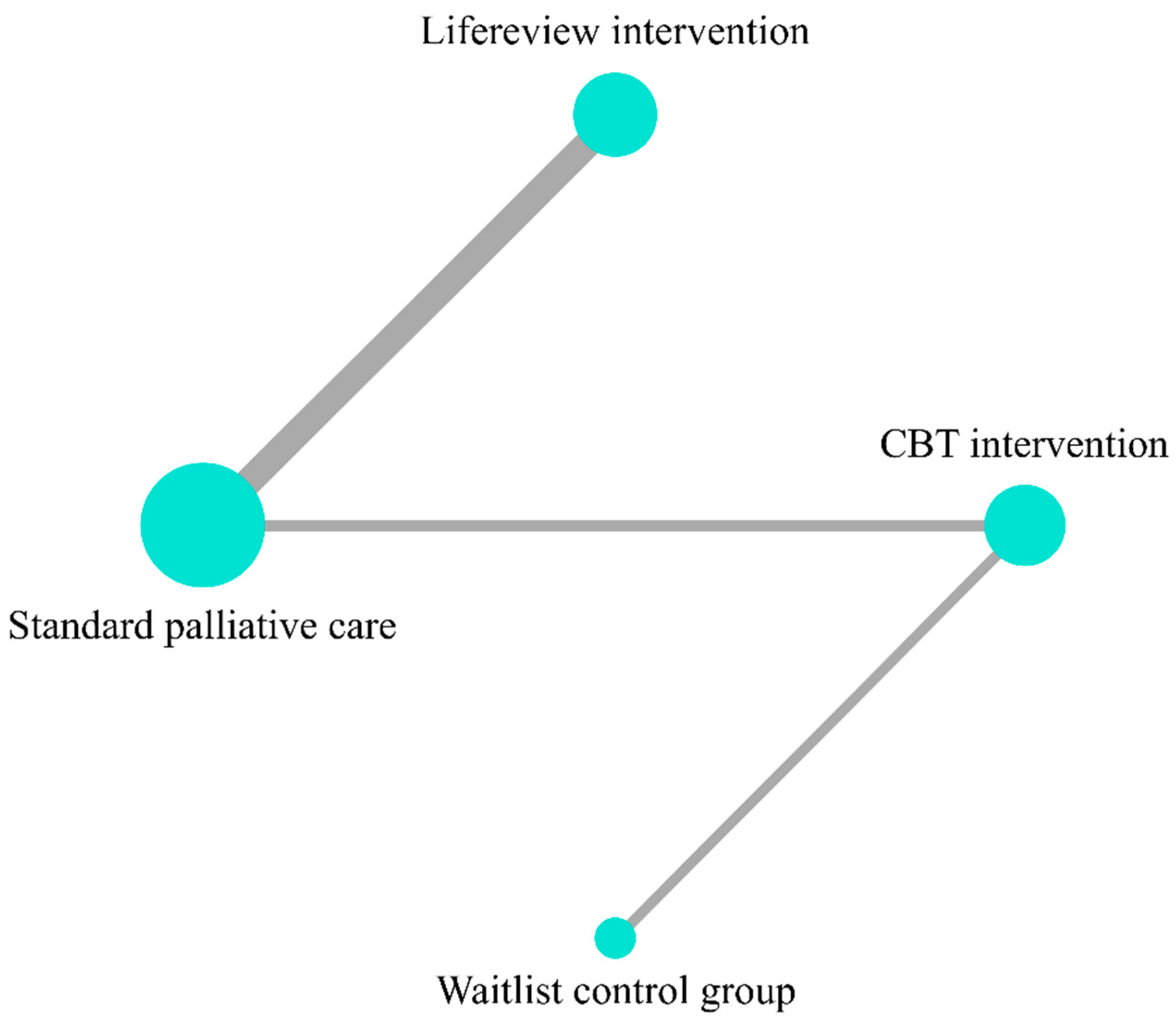
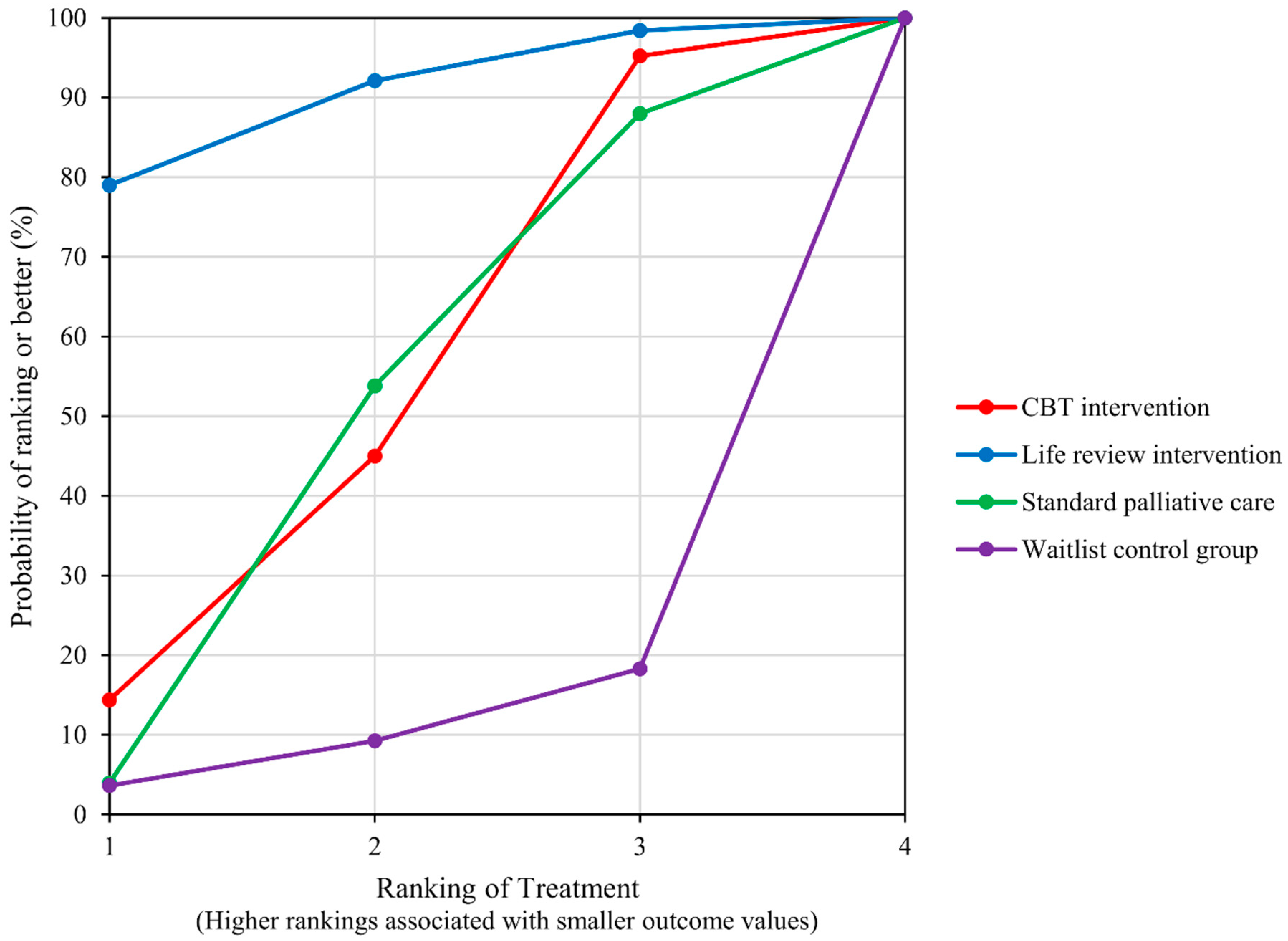
4.2. Depression
4.3. Anxiety
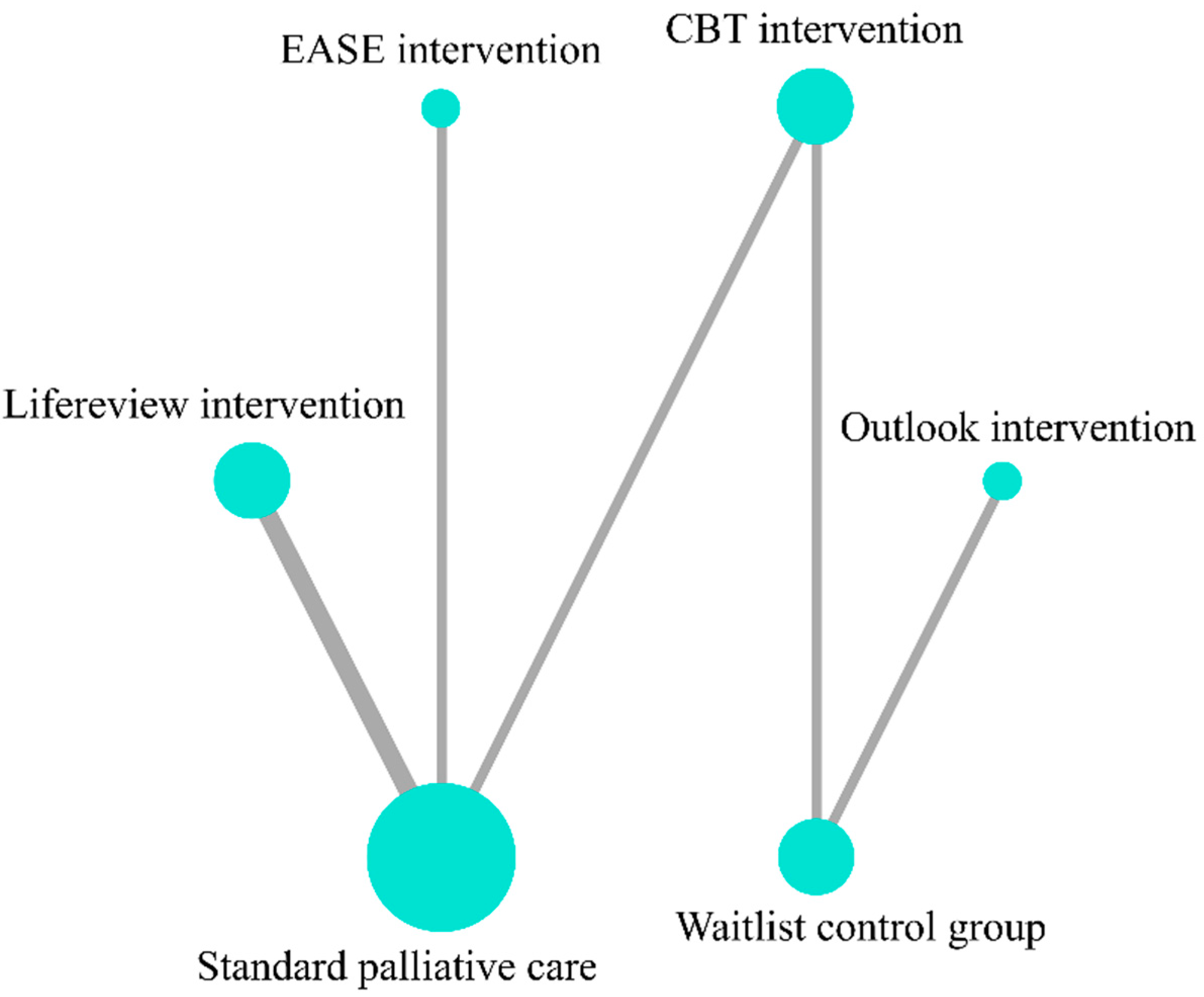
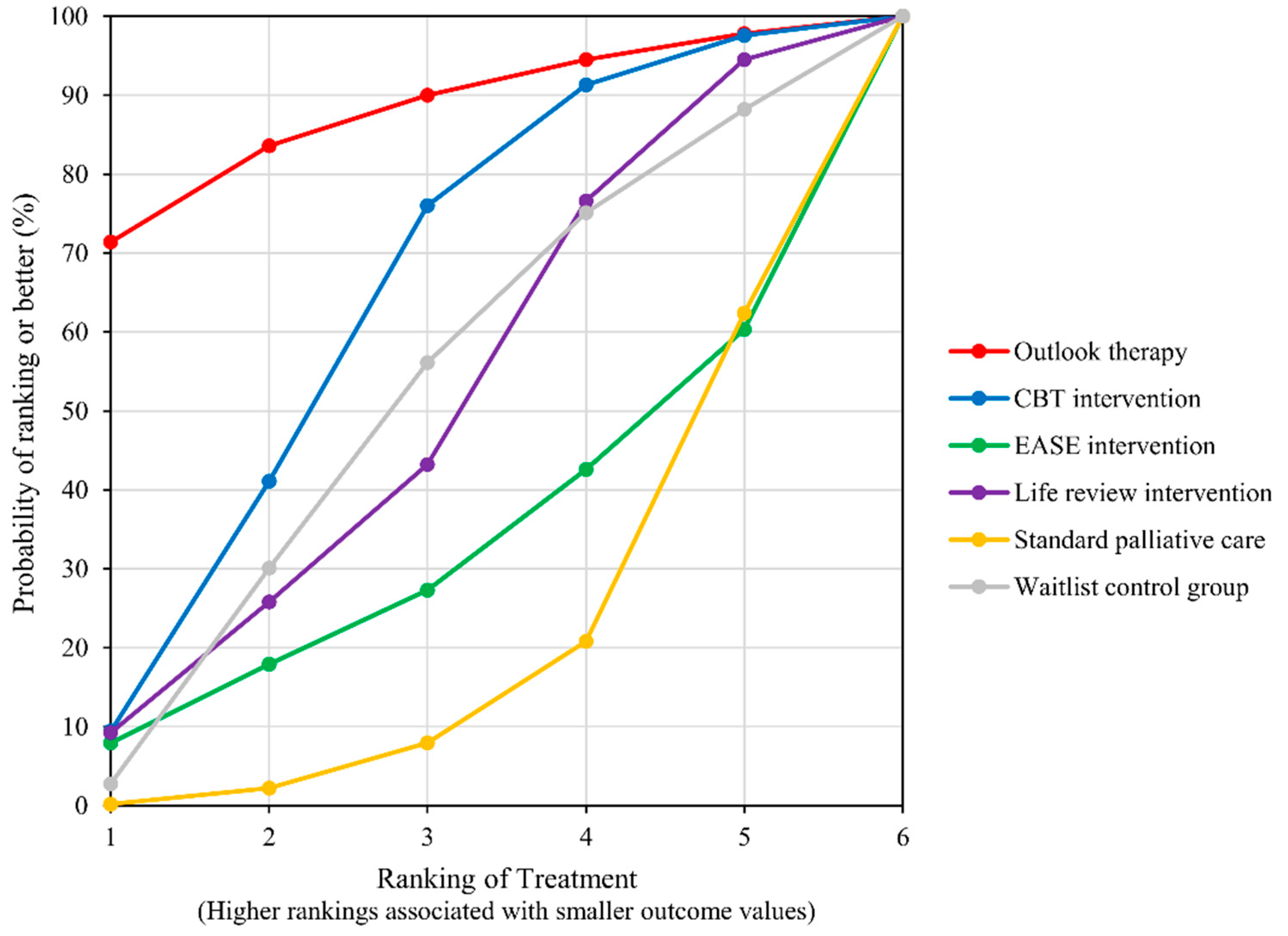
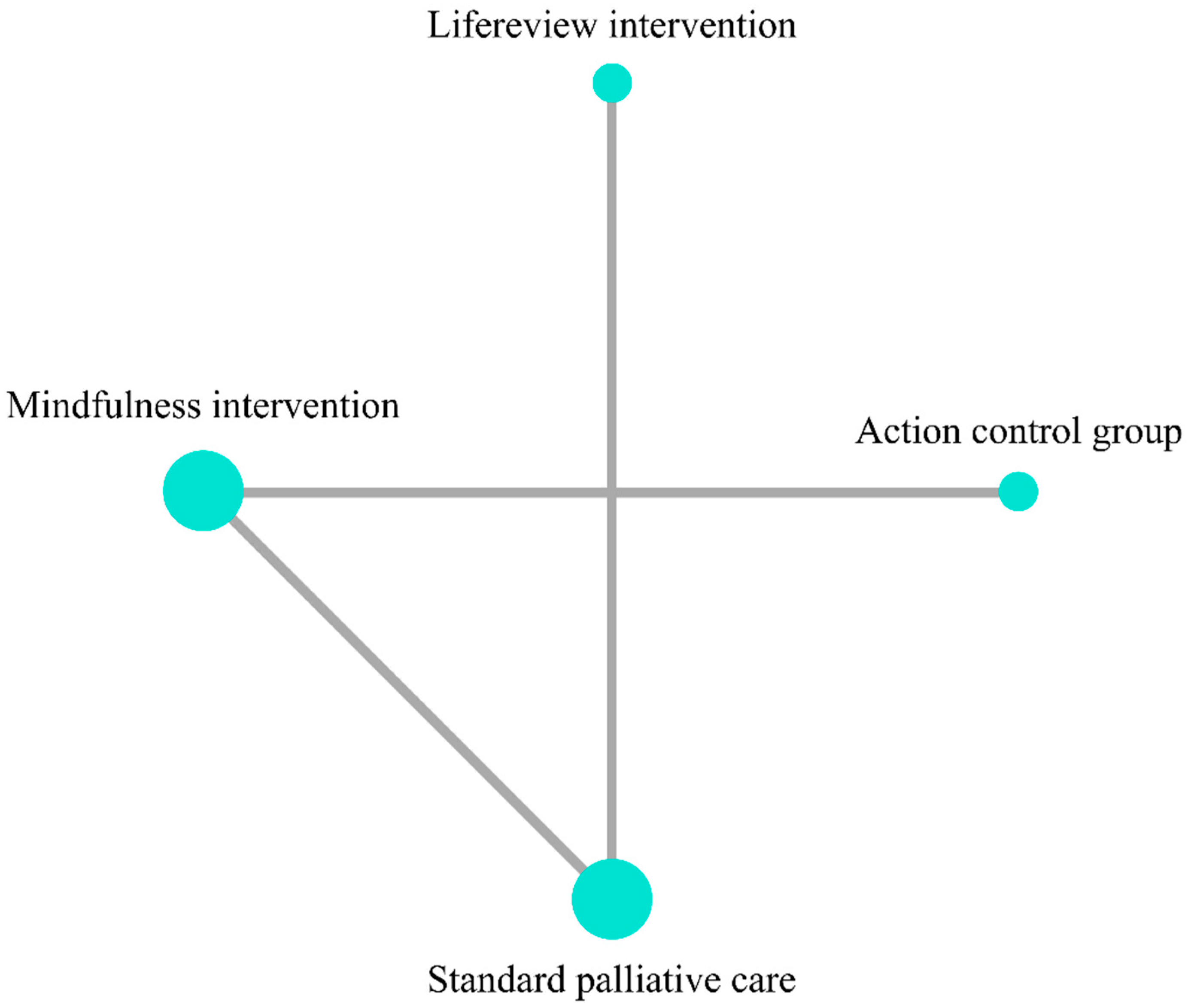
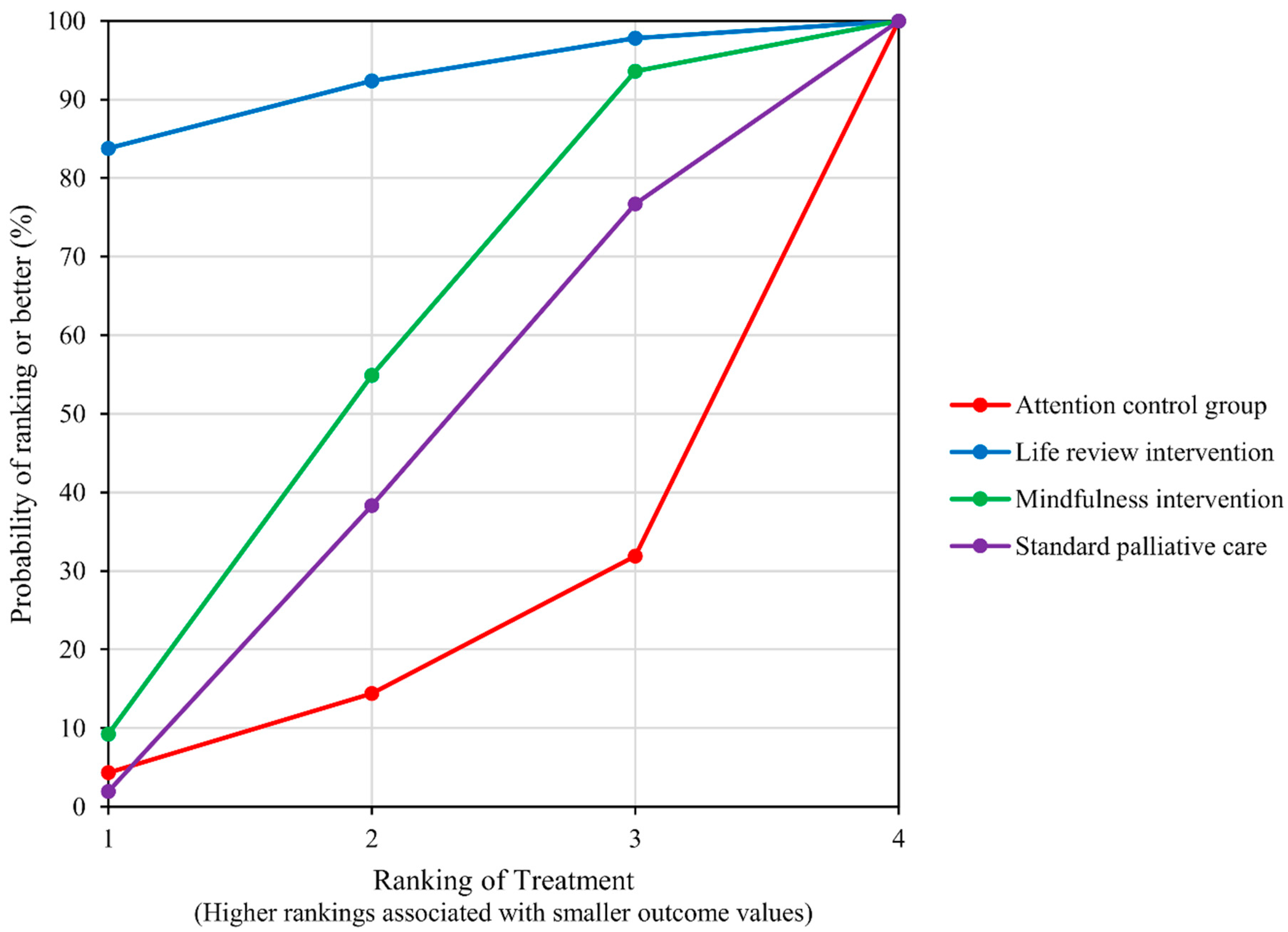
4.4. Distress
5. Discussion
6. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
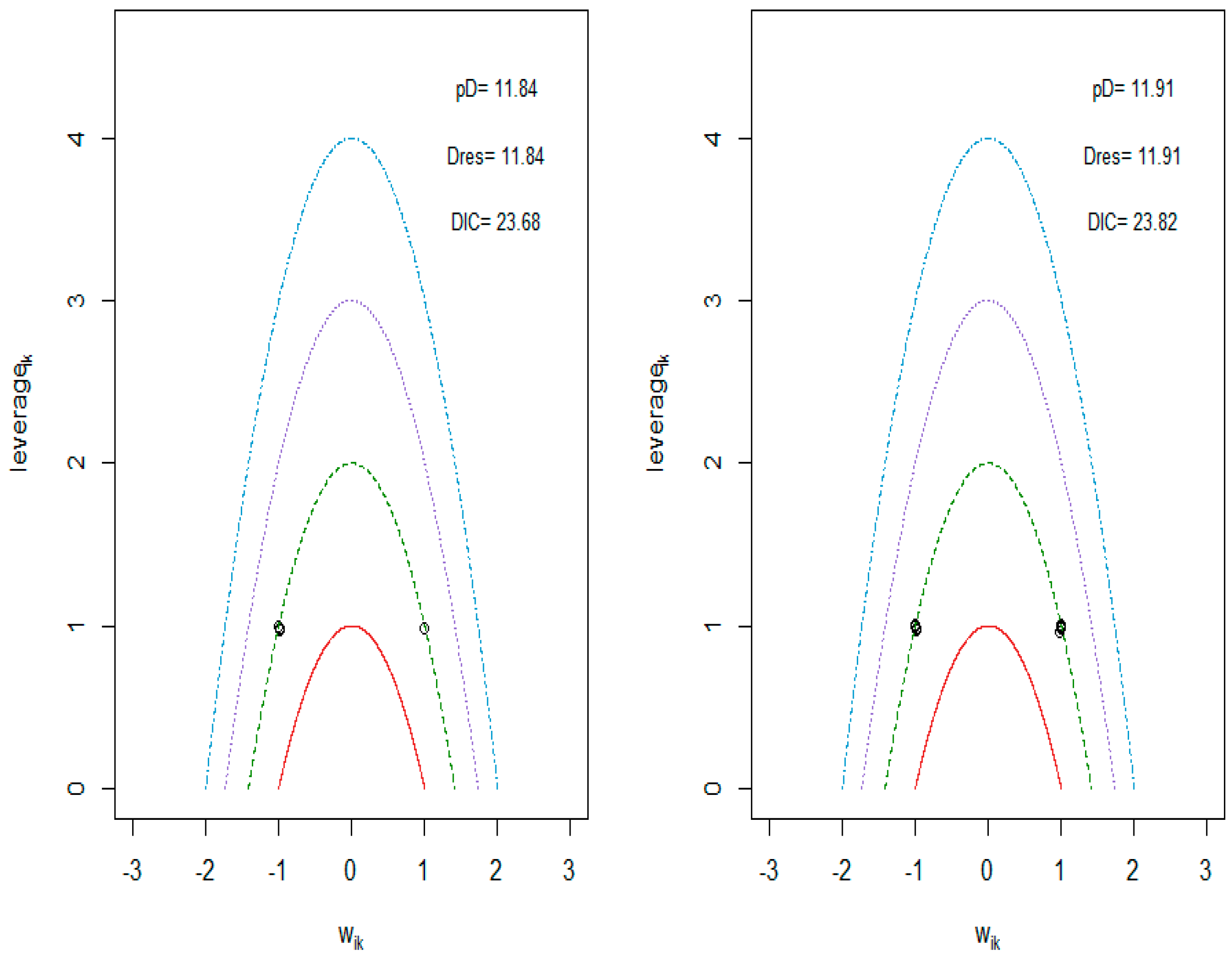
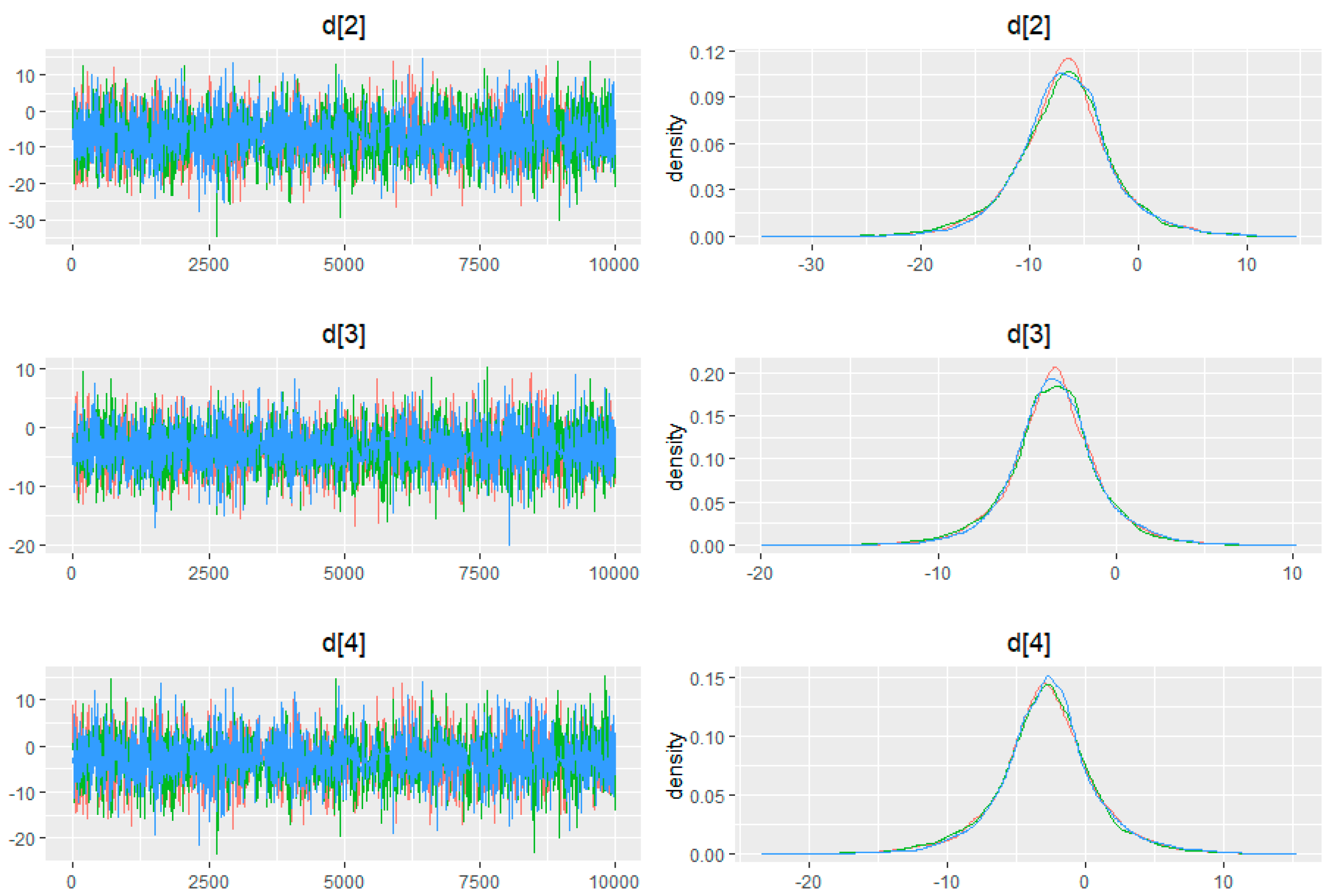
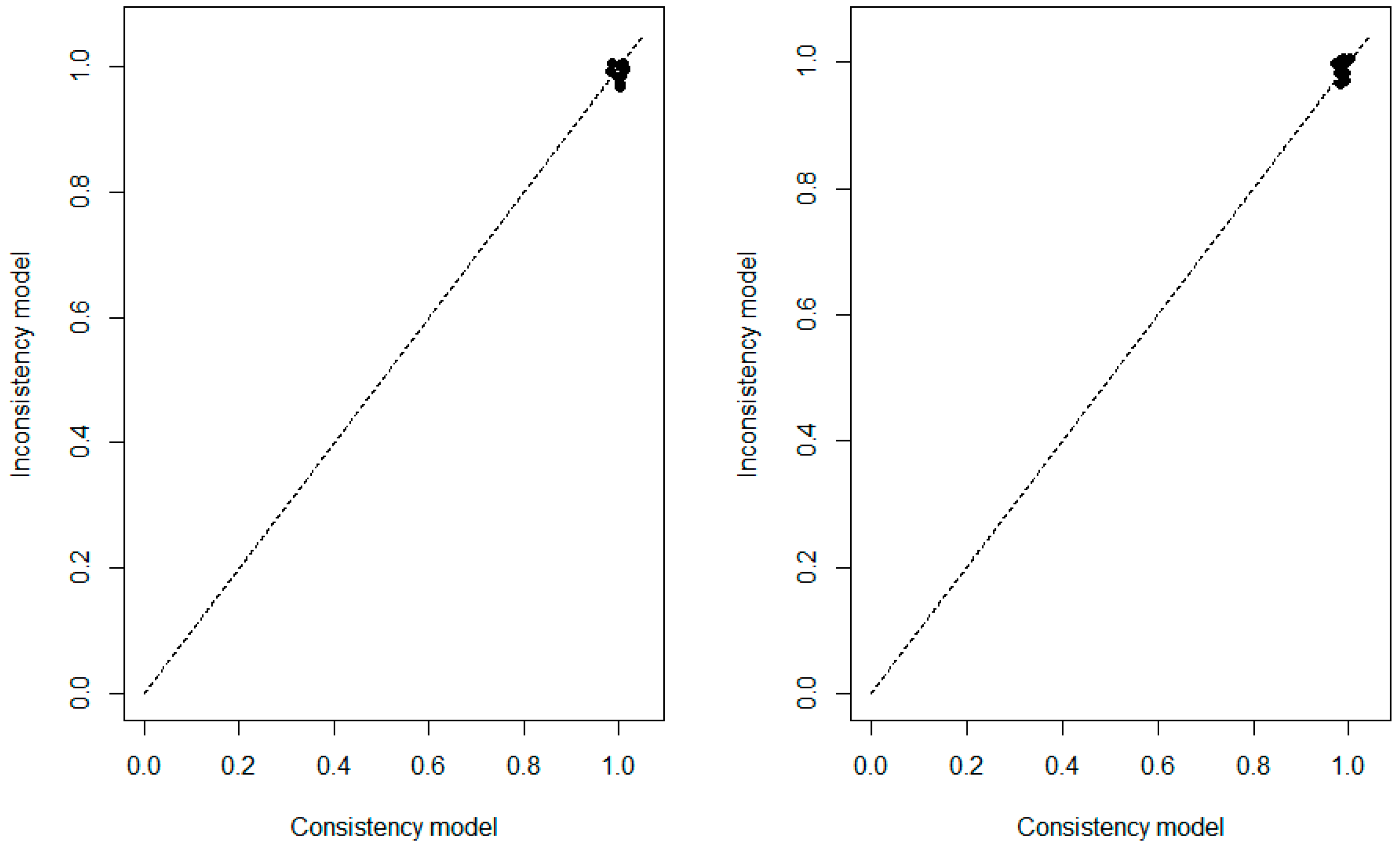
References
- Kelly, B.; McClement, S.; Chochinov, H.M. Measurement of psychological distress in palliative care. Palliat. Med. 2006, 20, 779–789. [Google Scholar] [CrossRef] [PubMed]
- Sewtz, C.; Muscheites, W.; Grosse-Thie, C.; Kriesen, U.; Leithaeuser, M.; Glaeser, D.; Hansen, P.; Kundt, G.; Fuellen, G.; Junghanss, C. Longitudinal observation of anxiety and depression among palliative care cancer patients. Ann. Palliat. Med. 2021, 10, 3836–3846. [Google Scholar] [CrossRef] [PubMed]
- Mundle, R.; Afenya, E.; Agarwal, N. The effectiveness of psychological intervention for depression, anxiety, and distress in prostate cancer: A systematic review of literature. Prostate Cancer Prostatic Dis. 2021, 24, 674–687. [Google Scholar] [CrossRef] [PubMed]
- Warth, M.; Kessler, J.; Koehler, F.; Aguilar-Raab, C.; Bardenheuer, H.J.; Ditzen, B. Brief psychosocial interventions improve quality of life of patients receiving palliative care: A systematic review and meta-analysis. Palliat. Med. 2019, 33, 332–345. [Google Scholar] [CrossRef]
- Hazlett-Stevens, H.; Craske, M.G. Brief Cognitive-Behavioral Therapy: Definition and Scientific Foundations. Handb. Brief Cogn. Behav. Ther. 2002, 1–20. [Google Scholar] [CrossRef]
- Stern, T.A.; Rosenbaum, J.F.; Fava, M.; Biederman, J.; Rauch, S.L. Massachusetts General Hospital Comprehensive Clinical Psychiatry; Elsevier Health Sciences: Cambridge, MA, USA, 2008. [Google Scholar]
- Beck, A.T. Cognitive Therapy of Depression; Guilford Press: New York, NY, USA, 1979. [Google Scholar]
- Xiao, J.; Chow, S.K.-H.; Liu, Y.; Chan, C.W. Effects of dignity therapy on dignity, psychological well-being, and quality of life among palliative care cancer patients: A systematic review and meta-analysis. Psycho-Oncology 2019, 28, 1791–1802. [Google Scholar] [CrossRef]
- von Blanckenburg, P.; Leppin, N. Psychological interventions in palliative care. Curr. Opin. Psychiatry 2018, 31, 389–395. [Google Scholar] [CrossRef]
- Kissane, D.W.; Levin, T.; Hales, S.; Lo, C.; Rodin, G. Psychotherapy for Depression in Cancer and Palliative Care. In Depression and Cancer; Wiley: Chichester, UK, 2010; pp. 177–206. [Google Scholar]
- Hofmann, S.G.; Asnaani, A.; Vonk, I.J.J.; Sawyer, A.T.; Fang, A. The Efficacy of Cognitive Behavioral Therapy: A Review of Meta-analyses. Cogn. Ther. Res. 2012, 36, 427–440. [Google Scholar] [CrossRef] [Green Version]
- Thoma, N.; Pilecki, B.; McKay, D. Contemporary Cognitive Behavior Therapy: A Review of Theory, History, and Evidence. Psychodyn. Psychiatry 2015, 43, 423–461. [Google Scholar] [CrossRef]
- Kabat-Zinn, J.; Lipworth, L.; Burney, R. The clinical use of mindfulness meditation for the self-regulation of chronic pain. J. Behav. Med. 1985, 8, 163–190. [Google Scholar] [CrossRef]
- Baer, R.A. Mindfulness training as a clinical intervention: A conceptual and empirical review. Clin. Psychol. Sci. Pract. 2003, 10, 125–143. [Google Scholar] [CrossRef]
- Martínez, M.; Arantzamendi, M.; Belar, A.; Carrasco, J.M.; Carvajal, A.; Rullán, M.; Centeno, C. ‘Dignity therapy’, a promising intervention in palliative care: A comprehensive systematic literature review. Palliat. Med. 2016, 31, 492–509. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Steinhauser, K.E.; Alexander, S.C.; Byock, I.R.; George, L.K.; Olsen, M.K.; Tulsky, J.A. Do Preparation and Life Completion Discussions Improve Functioning and Quality of Life in Seriously Ill Patients? Pilot Randomized Control Trial. J. Palliat. Med. 2008, 11, 1234–1240. [Google Scholar] [CrossRef] [PubMed]
- Catalá-López, F.; Tobías, A.; Cameron, C.; Moher, D.; Hutton, B. Network meta-analysis for comparing treatment effects of multiple interventions: An introduction. Rheumatol. Int. 2014, 34, 1489–1496. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Altman, D.G.; Liberati, A.; Tetzlaff, J. PRISMA statement. Epidemiology 2011, 22, 128. [Google Scholar] [CrossRef] [Green Version]
- Amir-Behghadami, M.; Janati, A. Population, Intervention, Comparison, Outcomes and Study (PICOS) design as a framework to formulate eligibility criteria in systematic reviews. Emerg. Med. J. 2020, 37, 387. [Google Scholar] [CrossRef]
- Béliveau, A.; Boyne, D.J.; Slater, J.; Brenner, D.; Arora, P. BUGSnet: An R package to facilitate the conduct and reporting of Bayesian network Meta-analyses. BMC Med. Res. Methodol. 2019, 19, 196. [Google Scholar] [CrossRef] [Green Version]
- Bhattacharya, R.; Lin, L.; Patrangenaru, V. Markov Chain Monte Carlo (MCMC) Simulation and Bayes Theory. In Mathematical Statistics and Large Sample Theory; Springer: Berlin/Heidelberg, Germany, 2016; pp. 325–332. [Google Scholar]
- Ando, M.; Morita, T.; Akechi, T.; Okamoto, T. Efficacy of Short-Term Life-Review Interviews on the Spiritual Well-Being of Ter-minally Ill Cancer Patients. J. Pain Symptom Manag. 2010, 39, 993–1002. [Google Scholar] [CrossRef]
- Do Carmo, T.M.; Paiva, B.S.R.; de Oliveira, C.Z.; Nascimento, M.S.A.; Paiva, C.E. The feasibility and benefit of a brief psychosocial intervention in addition to early palliative care in patients with advanced cancer to reduce depressive symptoms: A pilot randomized controlled clinical trial. BMC Cancer 2017, 17, 564. [Google Scholar] [CrossRef]
- Juliao, M.; Oliveira, F.; Nunes, B.; Vaz Carneiro, A.; Barbosa, A. Efficacy of dignity therapy on depression and anxiety in Portu-guese terminally ill patients: A phase II randomized controlled trial. J. Palliat. Med. 2014, 17, 688–695. [Google Scholar] [CrossRef]
- Kwan, C.W.; Chan, C.W.; Choi, K.C. The effectiveness of a nurse-led short term life review intervention in enhancing the spiritual and psychological well-being of people receiving palliative care: A mixed method study. Int. J. Nurs. Stud. 2019, 91, 134–143. [Google Scholar] [CrossRef] [PubMed]
- Savard, J.; Simard, S.; Giguère, I.; Ivers, H.; Morin, C.M.; Maunsell, E.; Gagnon, P.; Robert, J.; Marceau, D. Randomized clinical trial on cognitive therapy for de-pression in women with metastatic breast cancer: Psychological and immunological effects. Palliat. Supportive Care 2006, 4, 219–237. [Google Scholar] [CrossRef] [PubMed]
- Ng, C.G.; Lai, K.T.; Tan, S.B.; Sulaiman, A.H.; Zainal, N.Z. The Effect of 5 Minutes of Mindful Breathing to the Perception of Distress and Physiological Responses in Palliative Care Cancer Patients: A Randomized Controlled Study. J. Palliat. Med. 2016, 19, 917–924. [Google Scholar] [CrossRef] [PubMed]
- Warth, M.; Koehler, F.; Aguilar-Raab, C.; Bardenheuer, H.J.; Ditzen, B.; Kessler, J. Stress-reducing effects of a brief mindfulness intervention in palliative care: Results from a randomised, crossover study. Eur. J. Cancer Care 2020, 29, e13249. [Google Scholar] [CrossRef] [PubMed]
- Zigmond, A.S.; Snaith, R.P. The hospital anxiety and depression scale. Acta Psychiatr. Scand. 1983, 67, 361–370. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Beck, A.T.; Ward, C.; Mendelson, M.; Mock, J.; Erbaugh, J. An inventory for measuring depression. Arch. Gen. Psychiatry 1961, 4, 561–571. [Google Scholar] [CrossRef] [Green Version]
- Radloff, L.S. The CES-D scale: A self-report depression scale for research in the general population. Appl. Psychol. Meas. 1977, 1, 385–401. [Google Scholar] [CrossRef]
- Rodin, G.; Malfitano, C.; Rydall, A.; Schimmer, A.; Marmar, C.M.; Mah, K.; Lo, C.; Nissim, R.; Zimmermann, C. Emotion And Symptom-focused Engagement (EASE): A randomized phase II trial of an integrated psychological and palliative care intervention for patients with acute leukemia. Support. Care Cancer 2019, 28, 163–176. [Google Scholar] [CrossRef]
- Beck, A.T.; Steer, R.A.; Brown, G.K. Beck Depression Inventory (BDI-II); Pearson: San Antonio, TX, USA, 1996; Volume 10. [Google Scholar]
- McNair, D.M.; Lorr, M.; Droppleman, L.F. EdITS Manual for the Profile of Mood States (POMS); Educational and Industrial Testing Service: San Diego, CA, USA, 1992. [Google Scholar]
- Higgins, J.P.T.; Altman, D.G.; Gøtzsche, P.C.; Jüni, P.; Moher, D.; Oxman, A.D.; Savović, J.; Schulz, K.F.; Weeks, L.; Sterne, J.A.; et al. The Cochrane Col-laboration’s tool for assessing risk of bias in randomised trials. BMJ 2011, 343, d5928. [Google Scholar] [CrossRef] [Green Version]
- Munder, T.; Barth, J. Cochrane’s risk of bias tool in the context of psychotherapy outcome research. Psychother. Res. 2017, 28, 347–355. [Google Scholar] [CrossRef]
- Weru, J.; Gatehi, M.; Musibi, A. Randomized control trial of advanced cancer patients at a private hospital in Kenya and the impact of dignity therapy on quality of life. BMC Palliat. Care 2020, 19, 114. [Google Scholar] [CrossRef] [PubMed]
- Keall, R.M.; Clayton, J.M.; Butow, P.N. Therapeutic life review in palliative care: A systematic review of quantitative evaluations. J. Pain Symptom Manag. 2015, 49, 747–761. [Google Scholar] [CrossRef] [PubMed]
- Hall, S.; Chochinov, H.; Harding, R.; Murray, S.; Richardson, A.; Higginson, I.J. A Phase II randomised controlled trial assessing the feasibility, acceptability and potential effectiveness of Dignity Therapy for older people in care homes: Study protocol. BMC Geriatr. 2009, 9, 9. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wang, C.W.; Chow, A.Y.; Chan, C.L. The effects of life review interventions on spiritual well-being, psychological distress, and quality of life in patients with terminal or advanced cancer: A systematic review and meta-analysis of randomized controlled trials. Palliat. Med. 2017, 31, 883–894. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fulton, J.J.; Newins, A.R.; Porter, L.S.; Ramos, K. Psychotherapy targeting depression and anxiety for use in palliative care: A meta-analysis. J. Palliat. Med. 2018, 21, 1024–1037. [Google Scholar] [CrossRef] [Green Version]
- Cillessen, L.; Johannsen, M.; Speckens, A.E.; Zachariae, R. Mindfulness-based interventions for psychological and physical health outcomes in cancer patients and survivors: A systematic review and meta-analysis of randomized controlled trials. Psycho-Oncology 2019, 28, 2257–2269. [Google Scholar] [CrossRef] [Green Version]
- Trueman, I.; Parker, J. Exploring community nurses’ perceptions of life review in palliative care. J. Clin. Nurs. 2006, 15, 197–207. [Google Scholar] [CrossRef] [Green Version]
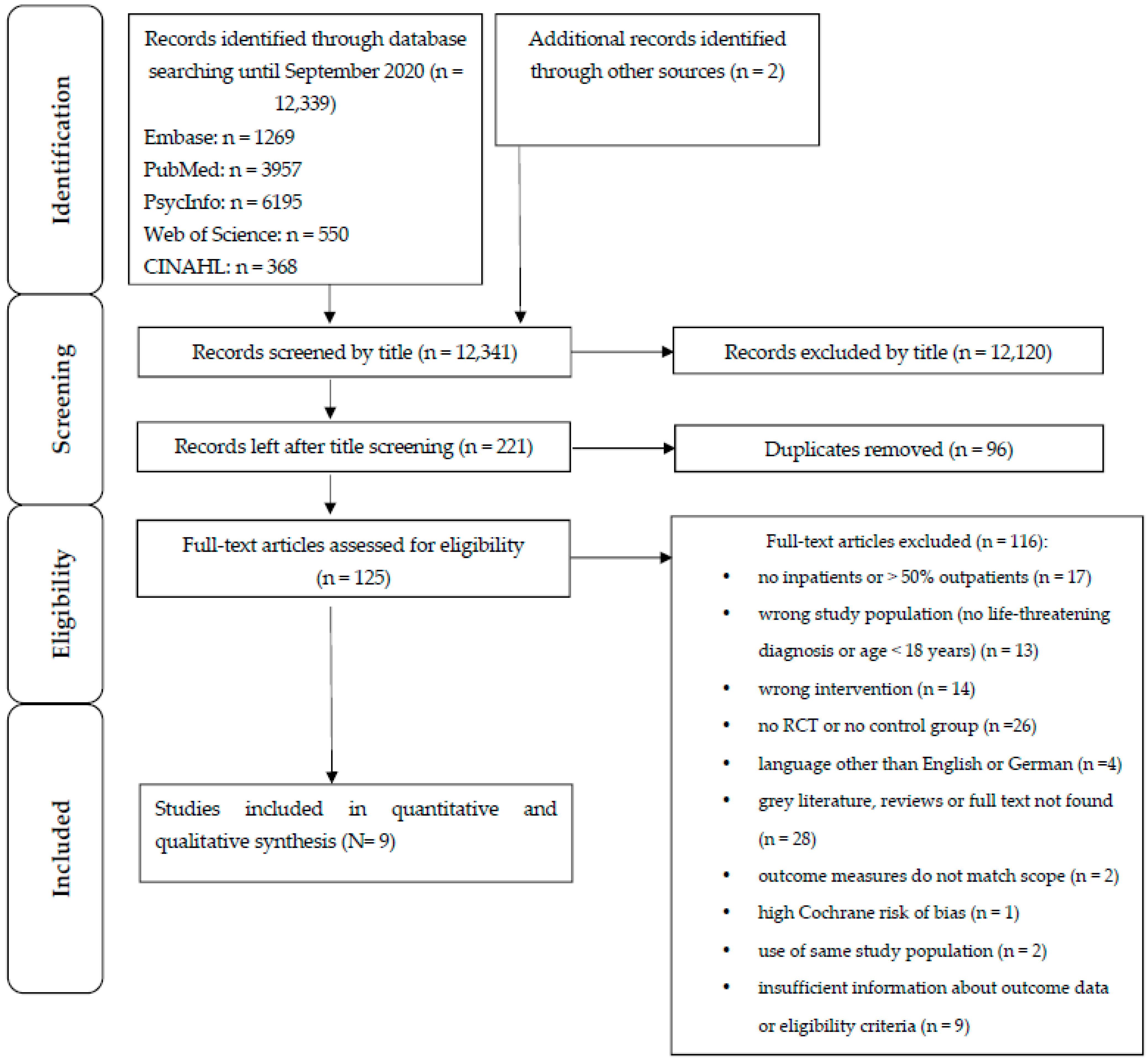
| Study | RAND | ALLO | BLPP | BLOA | INCDAT | SELREP | OTBI |
|---|---|---|---|---|---|---|---|
| Steinhauser et al., 2008 [16] | ? | ? | HIGH | LOW | LOW | LOW | LOW |
| Ando et al., 2010 [22] | LOW | LOW | HIGH | LOW | ? | LOW | LOW |
| Do Carmo et al., 2017 [23] | LOW | LOW | HIGH | LOW | ? | LOW | LOW |
| Juliao et al., 2014 [24] | LOW | LOW | HIGH | LOW | ? | LOW | LOW |
| Kwan et al., 2019 [25] | LOW | LOW | LOW | LOW | ? | LOW | HIGH |
| Savard et al., 2006 [26] | LOW | LOW | HIGH | LOW | HIGH | LOW | LOW |
| NG et al., 2016 [27] | ? | ? | HIGH | ? | ? | LOW | LOW |
| Warth et al., 2020 [28] | LOW | LOW | HIGH | HIGH | LOW | LOW | LOW |
| Rodin et al., 2019 [32] | LOW | LOW | HIGH | ? | LOW | LOW | LOW |
| Study | Design | Country of First Author | Intervention | Control Group | Sample Size at Baseline | Gender (m/f) | Outcomes | Study Characteristics: -Length to Follow up (FU) after Baseline Assessment; -Number of Sessions; -Duration of Sessions. |
|---|---|---|---|---|---|---|---|---|
| Juliao et al., 2014 [22] | RCT | Portugal | LRI | Standard PC | N = 80 | 37 m (46.25%), 43 f (53.75%) | HADS total HADS Depression HADS Anxiety | -FU on day 4 -Two intervention sessions between day 1 and day 4 -Each session lasting for 30–60 min |
| Ando et al., 2010 [20] | RCT | Japan | LRI | Standard PC | N = 68 | 32 m (47.01%), 36 f (52.94%) | HADS total Distress thermometer | -FU after 1 week -Two sessions within one week -Each session lasting for 30–60 min |
| Kwan et al., 2019 [23] | RCT | Hong Kong | LRI | Standard PC | N = 109 | 62 m (56.9%), 47 f (43,1%) | HADS total HADS Depression HADS Anxiety | -FU after 8 days -Two sessions within 8 days -Each session lasting for 45 min |
| Do Carmo et al., 2017 [21] | RCT | Brazil | CBT intervention | Standard PC | N = 63 | 22 m (34.92%), 41 f (65.08%) | HADS total HADS Depression HADS Anxiety | -FU on day 45 (after 6.5 weeks intervention)-Up to 5 to 7 sessions in a week for 6.5 weeks -Each session lasting 45 to 90 min |
| Savard et al., 2006 [24] | RCT | Canada | CBT intervention | Waitlist control group | N = 37 | 100% f | HADS total HADS Depression BDI HADS Anxiety | -FU after 8 weeks -8 weekly sessions across 8 weeks -Each session lasting 60 to90 min |
| Steinhauser et al., 2008 [16] | RCT | USA | Outlook intervention | Attention control group | N = 42 | 19 f (46%), 23 m (54%) | Depression CESD Anxiety POMS | -FU after 3 weeks -1 weekly session for 3 weeks (3 sessions in total) -Each session lasting 45 to 60 min |
| Rodin et al., 2019 [30] | RCT | Canada | Emotion and Symptom-focused Engagement intervention (EASE) | Standard PC | N = 42 | 26 m (61.90%), 16 f (38.10%) | BDI-II | -FU after 4 weeks -8 to 12 sessions for 4 weeks -Each session lasting 30 to 60 min |
| Warth et al., 2020 [26] | Randomized crossover trial | Germany | Mindfulness intervention | Standard PC | N = 42 | 13 m (31%), 29 f (69%) | Distress VAS | -FU after 20 min of the intervention on the same day -1 session -Session lasting 20 min |
| Ng et al., 2016 [25] | RCT | Malaysia | Mindfulness intervention | Attention control group | N = 60 | 29 m (48.30%), 31 f (51.70%) | One-item numeric distress scale | -FU took place 5 min after the end of intervention -1 session -Session lasting 5 min |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Schweighoffer, R.; Schumacher, A.M.; Blaese, R.; Walter, S.; Eckstein, S. A Systematic Review and Bayesian Network Meta-Analysis Investigating the Effectiveness of Psychological Short-Term Interventions in Inpatient Palliative Care Settings. Int. J. Environ. Res. Public Health 2022, 19, 7711. https://doi.org/10.3390/ijerph19137711
Schweighoffer R, Schumacher AM, Blaese R, Walter S, Eckstein S. A Systematic Review and Bayesian Network Meta-Analysis Investigating the Effectiveness of Psychological Short-Term Interventions in Inpatient Palliative Care Settings. International Journal of Environmental Research and Public Health. 2022; 19(13):7711. https://doi.org/10.3390/ijerph19137711
Chicago/Turabian StyleSchweighoffer, Reka, Andrea M. Schumacher, Richard Blaese, Silke Walter, and Sandra Eckstein. 2022. "A Systematic Review and Bayesian Network Meta-Analysis Investigating the Effectiveness of Psychological Short-Term Interventions in Inpatient Palliative Care Settings" International Journal of Environmental Research and Public Health 19, no. 13: 7711. https://doi.org/10.3390/ijerph19137711
APA StyleSchweighoffer, R., Schumacher, A. M., Blaese, R., Walter, S., & Eckstein, S. (2022). A Systematic Review and Bayesian Network Meta-Analysis Investigating the Effectiveness of Psychological Short-Term Interventions in Inpatient Palliative Care Settings. International Journal of Environmental Research and Public Health, 19(13), 7711. https://doi.org/10.3390/ijerph19137711





