Utilizing Structural Equation Modeling–Artificial Neural Network Hybrid Approach in Determining Factors Affecting Perceived Usability of Mobile Mental Health Application in the Philippines
Abstract
:1. Introduction
2. Literature Review and Conceptual Framework
2.1. Technology Acceptance Model

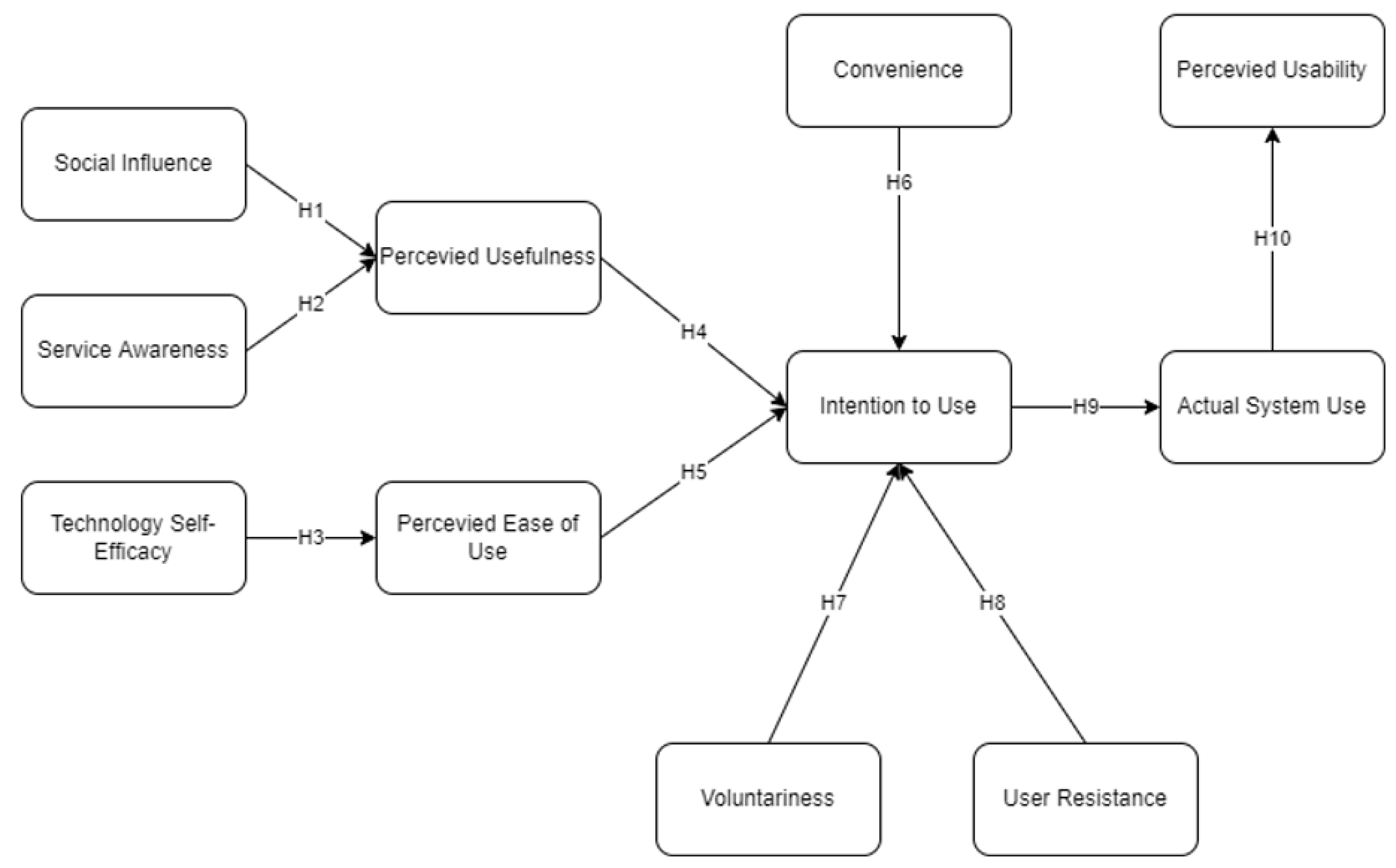
2.2. Conceptual Framework
3. Methodology
3.1. Participants
3.2. Questionnaire
3.3. Structural Equation Modeling
3.4. Artificial Neural Network
4. Results
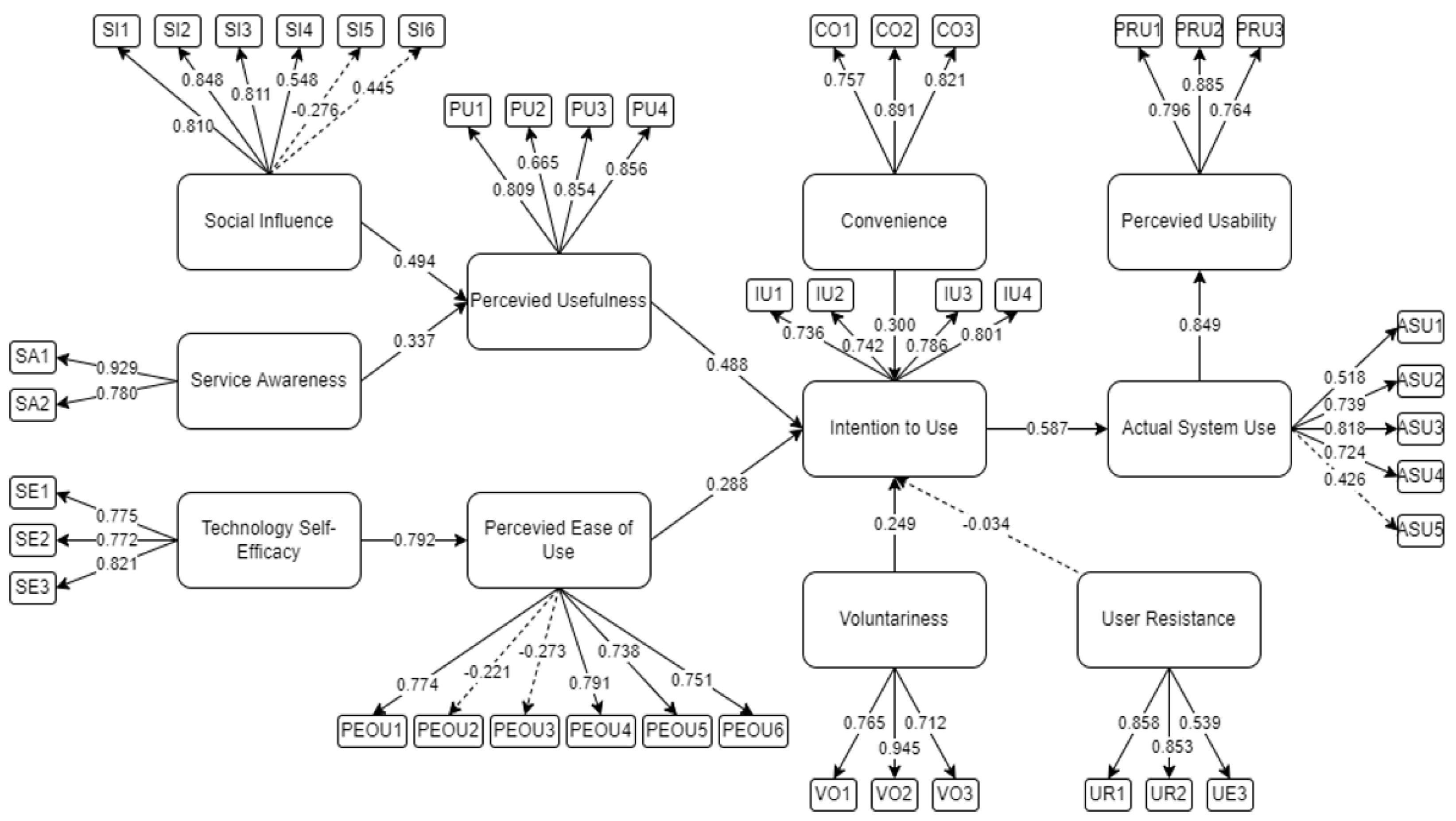
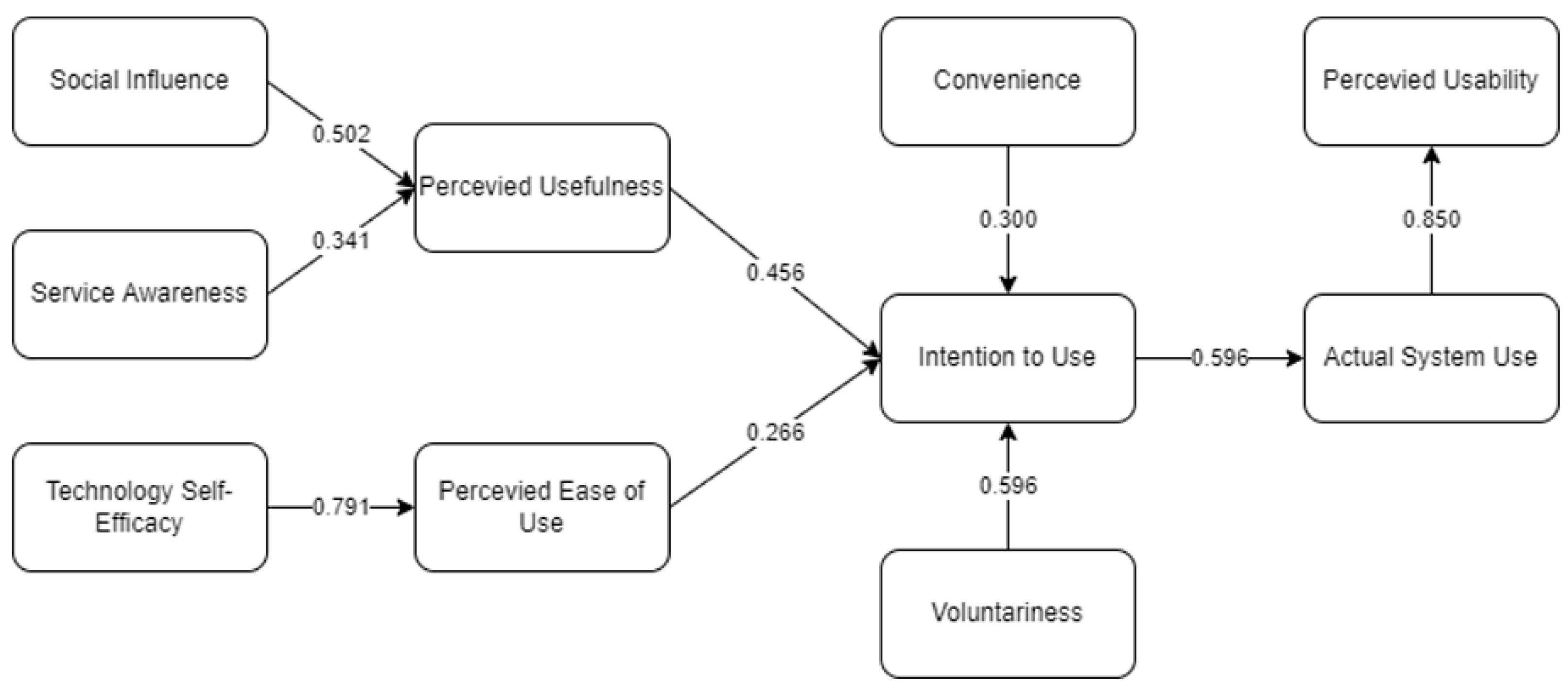
4.1. Structural Equation Modeling Results
4.2. Artificial Neural Network Results
5. Discussion
5.1. Theoretical and Practical Contribution
5.2. Limitations and Future Research
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Maravilla, N.M.A.T.; Tan, M.J.T. Philippine Mental Health Act: Just an act? A call to look into the bi-directionality of mental health and economy. Front. Psychol. 2021, 12, 706483. [Google Scholar] [CrossRef] [PubMed]
- Estrada, C.A.; Usami, M.; Satake, N.; Gregorio, E.; Leynes, C.; Balderrama, N.; Fernandez de Leon, J.; Concepcion, R.A.; Tuazon Timbalopez, C.; Tsujii, N. Current situation and challenges for mental health focused on treatment and care in Japan and the Philippines-highlights of the training program by the National Center for Global Health and Medicine. BMC Proc. 2020, 14, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Martinez, A.B.; Co, M.; Lau, J.; Brown, J.S. Filipino help-seeking for mental health problems and associated barriers and facilitators: A systematic review. Soc. Psychiatry Psychiatr. Epidemiol. 2020, 55, 1397–1413. [Google Scholar] [CrossRef] [PubMed]
- WHO. Global Health Estimates 2016: Deaths by Cause, Age, Sex, by Country and by Region, 2000–2016. Available online: https://www.who.int/data/gho/data/themes/mortality-and-global-health-estimates (accessed on 12 March 2022).
- WHO. Global Health Observatory Data Repository: Human Resources Data by Country; WHO: Geneva, Switzerland, 2019.
- Department of Health. Your Mind Matters: DOH Calls for Unified Response to Mental Health. Available online: https://doh.gov.ph/press-release/YOUR-MIND-MATTERS-DOH-CALLS-FOR-UNIFIED-RESPONSE-TO-MENTAL-HEALTH (accessed on 23 March 2022).
- Kamal, S.A.; Shafiq, M.; Kakria, P. Investigating acceptance of telemedicine services through an extended technology acceptance model (TAM). Technol. Soc. 2020, 60, 101212. [Google Scholar] [CrossRef]
- WHO; Department of Health. WHO-AIMS Report on Mental Health System in The Philippines. Available online: https://www.who.int/docs/default-source/mental-health/special-initiative/who-special-initiative-country-report---philippines---2020.pdf?sfvrsn=4b4ec2ee_8 (accessed on 23 March 2022).
- Lally, J.; Tully, J.; Samaniego, R. Mental health services in the Philippines. BJPsych Int. 2019, 16, 62–64. [Google Scholar] [CrossRef] [PubMed]
- Conde, B. Philippines mental health country profile. Int. Rev. Psychiatry 2004, 16, 159–166. [Google Scholar] [CrossRef]
- Isaac, M.; Ahmed, H.U.; Chaturvedi, S.K.; Hopwood, M.J.; Javeed, A.; Kanba, S.; Mufti, A.A.; Maramis, A.; Samaniego, R.M.; Udomratn, P. Postgraduate training in psychiatry in Asia. Curr. Opin. Psychiatry 2018, 31, 396–402. [Google Scholar] [CrossRef]
- Tuliao, A.P.; Velasquez, P.A. Revisiting the General Help Seeking Questionnaire: Adaptation, Exploratory Factor Analysis, and Further Validation in a Filipino College Student Sample. Philipp. J. Psychol. 2014, 47, 1–17. [Google Scholar]
- URC. USAID Renewhealth-Expanding Access to Community-Based Drug Rehabilitation in the Philippines. Available online: https://www.urc-chs.com/projects/renewhealth/ (accessed on 23 March 2022).
- URC. Mental Health on the Move in the Philippines–Meet the Lusog-Isip App. Available online: https://www.urc-chs.com/news/mental-health-on-the-move-in-the-philippines-meet-the-lusog-isip-app/ (accessed on 23 March 2022).
- Tubaishat, A. Perceived usefulness and perceived ease of use of electronic health records among nurses: Application of technology acceptance model. Inform. Health Soc. Care 2018, 43, 379–389. [Google Scholar] [CrossRef]
- Tsai, J.-M.; Cheng, M.-J.; Tsai, H.-H.; Hung, S.-W.; Chen, Y.-L. Acceptance and resistance of telehealth: The perspective of dual-factor concepts in technology adoption. Int. J. Inf. Manag. 2019, 49, 34–44. [Google Scholar] [CrossRef]
- Sohn, K.; Kwon, O. Technology acceptance theories and factors influencing artificial Intelligence-based intelligent products. Telemat. Inform. 2020, 47, 101324. [Google Scholar] [CrossRef]
- Talukder, M.S.; Sorwar, G.; Bao, Y.; Ahmed, J.U.; Palash, M.A.S. Predicting antecedents of wearable healthcare technology acceptance by elderly: A combined SEM-Neural Network approach. Technol. Forecast. Soc. Chang. 2020, 150, 119793. [Google Scholar] [CrossRef]
- Tao, D.; Wang, T.; Wang, T.; Zhang, T.; Zhang, X.; Qu, X. A systematic review and meta-analysis of user acceptance of consumer-oriented health information technologies. Comput. Hum. Behav. 2020, 104, 106147. [Google Scholar] [CrossRef]
- Davis, F.D.; Bagozzi, R.P.; Warshaw, P.R. User acceptance of computer technology: A comparison of two theoretical models. Manag. Sci. 1989, 35, 982–1003. [Google Scholar] [CrossRef] [Green Version]
- Min, S.; So, K.K.F.; Jeong, M. Consumer adoption of the Uber mobile application: Insights from diffusion of innovation theory and technology acceptance model. J. Travel Tour. Mark. 2019, 36, 770–783. [Google Scholar] [CrossRef]
- Campbell, S.W.; Russo, T.C. The cocial construction of mobile telephony: An application of the social influence model to perceptions and uses of mobile phones within personal communication networks. Commun. Monogr. 2003, 70, 317–334. [Google Scholar] [CrossRef]
- Walrave, M.; Waeterloos, C.; Ponnet, K. Ready or not for contact tracing? Investigating the adoption intention of COVID-19 contact-tracing technology using an extended unified theory of acceptance and use of technology model. Cyberpsychol. Behav. Soc. Netw. 2021, 24, 377–383. [Google Scholar] [CrossRef] [PubMed]
- Safi, S.; Thiessen, T.; Schmailzl, K.J. Acceptance and resistance of new digital technologies in medicine: Qualitative study. JMIR Res. Protoc. 2018, 7, e11072. [Google Scholar] [CrossRef]
- Ong, A.K.S.; Prasetyo, Y.T.; Pinugu, J.N.J.; Chuenyindee, T.; Chin, J.; Nadlifatin, R. Determining factors influencing students’ future intentions to enroll in chemistry-related courses: Integrating self-determination theory and theory of planned behavior. Int. J. Sci. Educ. 2022, 1–23. [Google Scholar] [CrossRef]
- Meuter, M.L.; Ostrom, A.L.; Bitner, M.J.; Roundtree, R. The influence of technology anxiety on consumer use and experiences with self-service technologies. J. Bus. Res. 2003, 56, 899–906. [Google Scholar] [CrossRef]
- Lee, J.; Kim, J.; Choi, J.Y. The adoption of virtual reality devices: The technology acceptance model integrating enjoyment, social interaction, and strength of the social ties. Telemat. Inform. 2019, 39, 37–48. [Google Scholar] [CrossRef]
- Sun, H.; Zhang, P. The role of moderating factors in user technology acceptance. Int. J. Hum.-Comput. Stud. 2006, 64, 53–78. [Google Scholar] [CrossRef] [Green Version]
- Shin, D. How does immersion work in augmented reality games? A user-centric view of immersion and engagement. Inf. Commun. Soc. 2019, 22, 1212–1229. [Google Scholar] [CrossRef]
- Okumus, B.; Ali, F.; Bilgihan, A.; Ozturk, A.B. Psychological factors influencing customers’ acceptance of smartphone diet apps when ordering food at restaurants. Int. J. Hosp. Manag. 2018, 72, 67–77. [Google Scholar] [CrossRef]
- Lu, J.; Liu, C.; Wei, J. How important are enjoyment and mobility for mobile applications? J. Comput. Inf. Syst. 2017, 57, 1–12. [Google Scholar] [CrossRef]
- Tamilmani, K.; Rana, N.P.; Wamba, S.F.; Dwivedi, R. The extended Unified Theory of Acceptance and Use of Technology (UTAUT2): A systematic literature review and theory evaluation. Int. J. Inf. Manag. 2021, 57, 102269. [Google Scholar] [CrossRef]
- Wu, J.; Du, H. Toward a better understanding of behavioral intention and system usage constructs. Eur. J. Inf. Syst. 2012, 21, 680–698. [Google Scholar] [CrossRef]
- Tam, C.; Santos, D.; Oliveira, T. Exploring the influential factors of continuance intention to use mobile Apps: Extending the expectation confirmation model. Inf. Syst. Front. 2020, 22, 243–257. [Google Scholar] [CrossRef]
- Dehghani, M. Exploring the motivational factors on continuous usage intention of smartwatches among actual users. Behav. Inf. Technol. 2018, 37, 145–158. [Google Scholar] [CrossRef]
- Huang, C.-Y.; Yang, M.-C. Empirical investigation of factors influencing consumer intention to use an artificial intelligence-powered mobile application for weight loss and health management. Telemed. E-Health 2020, 26, 1240–1251. [Google Scholar] [CrossRef]
- Pee, L.G.; Jiang, J.; Klein, G. Signaling effect of website usability on repurchase intention. Int. J. Inf. Manag. 2018, 39, 228–241. [Google Scholar] [CrossRef]
- Gelderblom, H.; Matthee, M.; Hattingh, M.; Weilbach, L. High school learners’ continuance intention to use electronic textbooks: A usability study. Educ. Inf. Technol. 2019, 24, 1753–1776. [Google Scholar] [CrossRef]
- Venkatesh, V.; Thong, J.Y.; Xu, X. Consumer acceptance and use of information technology: Extending the unified theory of acceptance and use of technology. MIS Q. 2012, 157–178. [Google Scholar] [CrossRef] [Green Version]
- Alam, M.Z.; Hoque, M.R.; Hu, W.; Barua, Z. Factors influencing the adoption of mHealth services in a developing country: A patient-centric study. Int. J. Inf. Manag. 2020, 50, 128–143. [Google Scholar] [CrossRef]
- Sonderegger, A.; Sauer, J. The influence of design aesthetics in usability testing: Effects on user performance and perceived usability. Appl. Ergon. 2010, 41, 403–410. [Google Scholar] [CrossRef] [Green Version]
- Prasetyo, Y.T.; Ong, A.K.S.; Concepcion, G.K.F.; Navata, F.M.B.; Robles, R.A.V.; Tomagos, I.J.T.; Young, M.N.; Diaz, J.F.T.; Nadlifatin, R.; Redi, A.A.N.P. Determining factors Affecting acceptance of e-learning platforms during the COVID-19 pandemic: Integrating Extended technology Acceptance model and DeLone & Mclean is success model. Sustainability 2021, 13, 8365. [Google Scholar]
- Duarte, P.; Pinho, J.C. A mixed methods UTAUT2-based approach to assess mobile health adoption. J. Bus. Res. 2019, 102, 140–150. [Google Scholar] [CrossRef]
- Fan, Y.; Chen, J.; Shirkey, G.; John, R.; Wu, S.R.; Park, H.; Shao, C. Applications of structural equation modeling (SEM) in ecological studies: An updated review. Ecol. Processes 2016, 5, 19. [Google Scholar] [CrossRef] [Green Version]
- Al-Mashraie, M.; Chung, S.H.; Jeon, H.W. Customer switching behavior analysis in the telecommunication industry via push-pull-mooring framework: A machine learning approach. Comput. Ind. Eng. 2020, 144, 106476. [Google Scholar] [CrossRef]
- Bae, J.; Kim, G.; Lee, S.J. Real-time prediction of nuclear power plant parameter trends following operator actions. Expert Syst. Appl. 2021, 186, 115848. [Google Scholar] [CrossRef]
- Pradhan, B.; Lee, S. Landslide susceptibility assessment and factor effect analysis: Backpropagation artificial neural networks and their comparison with frequency ratio and bivariate logistic regression modelling. Environ. Model. Softw. 2010, 25, 747–759. [Google Scholar] [CrossRef]
- Satwik, P.; Sundram, M. An integrated approach for weather forecasting and disaster prediction using deep learning architecture based on memory Augmented Neural Network’s (MANN’s). Mater. Today Proc. 2021. [Google Scholar] [CrossRef]
- Gefen, D.; Karahanna, E.; Straub, D.W. Trust and TAM in online shopping: An integrated model. MIS Q. 2003, 27, 51–90. [Google Scholar] [CrossRef]
- Steiger, J.H. Understanding the limitations of global fit assessment in structural equation modeling. Personal. Individ. Differ. 2007, 42, 893–898. [Google Scholar] [CrossRef]
- Gefen, D.; Straub, D.; Boudreau, M.-C. Structural equation modeling and regression: Guidelines for research practice. Commun. Assoc. Inf. Syst. 2000, 4, 7. [Google Scholar] [CrossRef] [Green Version]
- Woody, E. An SEM perspective on evaluating mediation: What every clinical researcher needs to know. J. Exp. Psychopathol. 2011, 2, 210–251. [Google Scholar] [CrossRef]
- Sharma, S.K.; Al-Badi, A.; Rana, N.P.; Al-Azizi, L. Mobile applications in government services (mG-App) from user’s perspectives: A predictive modelling approach. Gov. Inf. Q. 2018, 35, 557–568. [Google Scholar] [CrossRef] [Green Version]
- Lallmahomed, M.Z.; Lallmahomed, N.; Lallmahomed, G.M. Factors influencing the adoption of e-Government services in Mauritius. Telemat. Inform. 2017, 34, 57–72. [Google Scholar] [CrossRef]
- Alalwan, A.A.; Dwivedi, Y.K.; Rana, N.P. Factors influencing adoption of mobile banking by Jordanian bank customers: Extending UTAUT2 with trust. Int. J. Inf. Manag. 2017, 37, 99–110. [Google Scholar] [CrossRef]
- Wu, P.; Zhang, R.; Zhu, X.; Liu, M. Factors Influencing Continued Usage Behavior on Mobile Health Applications. Healthcare 2022, 10, 208. [Google Scholar] [CrossRef]
- Nikolopoulou, K.; Gialamas, V.; Lavidas, K. Habit, hedonic motivation, performance expectancy and technological pedagogical knowledge affect teachers’ intention to use mobile internet. Comput. Educ. Open 2021, 2, 100041. [Google Scholar] [CrossRef]
- Venkatesh, V. Adoption and use of AI tools: A research agenda grounded in UTAUT. Ann. Oper. Res. 2021, 308, 641–652. [Google Scholar] [CrossRef]
- Palau-Saumell, R.; Forgas-Coll, S.; Sánchez-García, J.; Robres, E. User acceptance of mobile apps for restaurants: An expanded and extended UTAUT-2. Sustainability 2019, 11, 1210. [Google Scholar] [CrossRef] [Green Version]
- Ong, A.K.S.; Prasetyo, Y.T.; Salazar, J.M.L.D.; Erfe, J.J.C.; Abella, A.A.; Young, M.N.; Chuenyindee, T.; Nadlifatin, R.; Redi, A.A.N.P. Investigating the acceptance of the reopening bataan nuclear power plant: Integrating protection motivation theory and extended theory of planned behavior. Nucl. Eng. Technol. 2021, 54, 1115–1125. [Google Scholar] [CrossRef]
- Thakur, R. The role of self-efficacy and customer satisfaction in driving loyalty to the mobile shopping application. Int. J. Retail. Distrib. Manag. 2018, 46, 283–303. [Google Scholar] [CrossRef]
- Ahmad, S.Z.; Khalid, K. The adoption of M-government services from the user’s perspectives: Empirical evidence from the United Arab Emirates. Int. J. Inf. Manag. 2017, 37, 367–379. [Google Scholar] [CrossRef]
- Chuenyindee, T.; Ong, A.K.; Prasetyo, Y.T.; Persada, S.F.; Nadlifatin, R.; Sittiwatethanasiri, T. Factors affecting the perceived usability of the COVID-19 contact-tracing application “Thai chana” during the early COVID-19 omicron period. Int. J. Environ. Res. Public Health 2022, 19, 4383. [Google Scholar] [CrossRef]
- Ong, A.K.; Prasetyo, Y.T.; Velasco, K.E.; Abad, E.D.; Buencille, A.L.; Estorninos, E.M.; Cahigas, M.M.; Chuenyindee, T.; Persada, S.F.; Nadlifatin, R.; et al. Utilization of random forest classifier and artificial neural network for predicting the acceptance of reopening decommissioned nuclear power plant. Ann. Nucl. Energy 2022, 175, 109188. [Google Scholar] [CrossRef]
- Ong, A.K.; Chuenyindee, T.; Prasetyo, Y.T.; Nadlifatin, R.; Persada, S.F.; Gumasing, M.J.; German, J.D.; Robas, K.P.; Young, M.N.; Sittiwatethanasiri, T. Utilization of random forest and deep learning neural network for predicting factors affecting perceived usability of a COVID-19 contact tracing mobile application in Thailand “Thaichana”. Int. J. Environ. Res. Public Health 2022, 19, 6111. [Google Scholar] [CrossRef]

| Variable | Frequency | Percent (%) |
|---|---|---|
| Sex | ||
| Female | 128 | 51.00 |
| Male | 123 | 49.00 |
| Age | ||
| 18 years old and younger | 4 | 1.59 |
| 18–25 | 219 | 87.25 |
| 26–32 | 24 | 9.56 |
| 33–39 | 3 | 1.20 |
| 40–47 | 1 | 0.40 |
| 48 years old and older | 0 | 0.00 |
| Occupation | ||
| Student | 133 | 52.99 |
| Working | 118 | 47.01 |
| Educational Attainment | ||
| Primary | 3 | 1.20 |
| Secondary | 57 | 22.71 |
| Bachelor’s degree | 173 | 68.92 |
| Master’s degree | 11 | 4.38 |
| Doctorate degree | 7 | 2.79 |
| Access to Internet | ||
| Yes | 241 | 96.02 |
| No | 10 | 3.98 |
| Use of Online Treatment in the past | ||
| Yes | 61 | 24.30 |
| No | 190 | 75.70 |
| Construct | Items | Measurement Items | References |
|---|---|---|---|
| Social Influence | SI1 | Your friends and family think that mobile mental health applications are a useful thing. | Venkatesh et al. [39] |
| SI2 | Your friends and family think that mobile mental health applications would be useful for you. | Venkatesh et al. [39] | |
| SI3 | Your friends and family would also use mobile mental health applications. | Venkatesh et al. [39] | |
| SI4 | You often discuss the advantages of mobile treatment with your friends/family. | ||
| SI5 | Your friends and family would be surprised if you use a mobile mental health application. | ||
| SI6 | Your family and friends suggested that you use mobile mental health application. | Venkatesh et al. [39] | |
| Service Awareness | SA1 | You are aware of the existence of mobile mental health awareness. | Talukder et al. [18] |
| SA2 | You are aware of different available mobile metal health application. | Talukder et al. [18] | |
| Self-efficacy | SE1 | I feel confident finding information and advice in a mobile mental health application. | Meuter et al. [26] |
| SE2 | I have the necessary skills for using a mobile mental health application successfully. | Meuter et al. [26] | |
| SE3 | I feel confident using the mobile mental health application regularly. | ||
| Perceived Usefulness | PU1 | I find mobile mental health to be useful to improve my life in general. | Venkatesh et al. [39] |
| PU2 | Using a mobile mental health application would improve my life quickly. | Venkatesh et al. [39] | |
| PU3 | I would find mobile mental health applications useful. | Venkatesh et al. [39] | |
| PU4 | I think that mobile mental health applications provide very useful services. | Venkatesh et al. [39] | |
| Perceived Ease of Use | PEOU1 | I find it easy to get the benefits from a mobile mental health application. | Venkatesh et al. [39] |
| PEOU2 | Using a mobile mental health application will be complicated. | Venkatesh et al. [39] | |
| PEOU3 | Using a mobile mental health application will take a lot of effort. | Venkatesh et al. [39] | |
| PEOU4 | I find mobile mental health applications are easy to use. | Venkatesh et al. [39] | |
| PEOU5 | Learning to operate a mobile mental health application would be/is ease for me. | Venkatesh et al. [39] | |
| PEOU6 | The interface of the mental health mobile application is user-friendly and fool-proof. | Venkatesh et al. [39] | |
| Convenience | CO1 | I find using the mobile mental health application convenient. | Shin [29] |
| CO2 | I can use the mobile mental health anywhere and anytime. | Shin [29] | |
| CO3 | I can use the mobile mental health whenever needed in an undesirable situation. | Shin [29] | |
| Voluntariness | VO1 | I use mobile mental health application at my own will. | Tamilmani et al. [32] |
| VO2 | I was not forced by anyone to use the mobile mental health application. | Tamilmani et al. [32] | |
| VO3 | I was introduced to use the mobile mental health application. | Tamilmani et al. [32] | |
| User Resistance | UR1 | I wouldn’t want the mobile mental health application to alter my traditional way of using health care services. | Tsai et al. [16] |
| UR2 | I wouldn’t want the mobile mental health application to interfere or change the way I interact with doctors. | Tsai et al. [16] | |
| UR3 | Mobile mental health application can never replace the traditional therapy consultation. | Tsai et al. [16] | |
| Intention to Use | IU1 | Assuming that I was given the chance to access mental health mobile application, I intend to use its services. | Venkatesh et al. [39] |
| IU2 | Whenever I would need remote medical care from professionals, I would gladly use mobile mental health application services. | Venkatesh et al. [39] | |
| IU3 | I intend to check the availability of a suited mobile mental health application. | Venkatesh et al. [39] | |
| IU4 | I intend to use a mobile mental health application. | ||
| Actual System Use | ASU1 | I use mobile mental health applications daily. | Alam et al. [40] |
| ASU2 | I find mobile mental health applications useful when coping to different situation. | ||
| ASU3 | Mobile health applications activities help lighten my mood and my state of mind. | Alam et al. [40] | |
| ASU4 | Mobile health application motivates me in my daily life. | Alam et al. [40] | |
| ASU5 | I encounter no problem when using the application. | ||
| Perceived Usability | PRU1 | Mobile mental health is useful during undesirable situations (e.g., racing negative thoughts, down mood). | Sonderegger and Sauer [41] |
| PRU2 | Mobile mental health applications help me cope. | Sonderegger and Sauer [41] | |
| PRU3 | Mobile mental health applications are useful whenever there is no one I can talk to. | Sonderegger and Sauer [41] |
| Variable | Item | Mean | StD | Factor Loading | |
|---|---|---|---|---|---|
| Initial | Final | ||||
| Social Influence | SI1 | 3.5538 | 0.82468 | 0.810 | 0.822 |
| SI2 | 3.5219 | 0.85470 | 0.848 | 0.876 | |
| SI3 | 3.3825 | 0.92365 | 0.811 | 0.784 | |
| SI4 | 2.7888 | 0.94193 | 0.548 | 0.507 | |
| SI5 | 3.0996 | 1.03249 | −0.276 | - | |
| SI6 | 2.7769 | 0.91980 | 0.445 | - | |
| Service Awareness | SA1 | 3.6096 | 1.13796 | 0.929 | 0.915 |
| SA2 | 3.2550 | 1.18942 | 0.780 | 0.792 | |
| Technology Self-Efficacy | SE1 | 3.4980 | 0.86891 | 0.775 | 0.778 |
| SE2 | 3.6853 | 0.87667 | 0.772 | 0.770 | |
| SE3 | 3.2829 | 0.84123 | 0.821 | 0.821 | |
| Perceived Usefulness | PU1 | 3.5976 | 0.78066 | 0.809 | 0.810 |
| PU2 | 3.2629 | 0.85941 | 0.665 | 0.665 | |
| PU3 | 3.7610 | 0.76330 | 0.854 | 0.853 | |
| PU4 | 3.8127 | 0.75947 | 0.856 | 0.856 | |
| Perceived Ease of Use | PEOU1 | 3.5458 | 0.71617 | 0.774 | 0.785 |
| PEOU2 | 2.6494 | 0.84652 | −0.221 | - | |
| PEOU3 | 2.6574 | 0.94770 | −0.273 | - | |
| PEOU4 | 3.5618 | 0.68642 | 0.791 | 0.785 | |
| PEOU5 | 3.7012 | 0.74455 | 0.738 | 0.727 | |
| PEOU6 | 3.4382 | 0.70368 | 0.751 | 0.762 | |
| Convenience | CO1 | 3.6693 | 0.71987 | 0.757 | 0.756 |
| CO2 | 3.7490 | 0.77250 | 0.891 | 0.891 | |
| CO3 | 3.7251 | 0.80008 | 0.821 | 0.821 | |
| Voluntariness | VO1 | 3.7490 | 0.82750 | 0.765 | 0.766 |
| VO2 | 3.8645 | 0.81828 | 0.945 | 0.944 | |
| VO3 | 1.9880 | 0.92296 | 0.712 | 0.713 | |
| User Resistance | UR1 | 3.1912 | 0.88277 | 0.858 | - |
| UR2 | 3.3984 | 0.87215 | 0.853 | - | |
| UR3 | 3.5458 | 0.89045 | 0.539 | - | |
| Intention to Use | IU1 | 4.0040 | 0.71273 | 0.736 | 0.737 |
| IU2 | 3.9124 | 0.79516 | 0.742 | 0.742 | |
| IU3 | 3.8406 | 0.78390 | 0.786 | 0.785 | |
| IU4 | 3.6813 | 0.82098 | 0.801 | 0.800 | |
| Actual System Use | ASU1 | 2.4263 | 0.87495 | 0.518 | 0.550 |
| ASU2 | 3.4582 | 0.79577 | 0.739 | 0.742 | |
| ASU3 | 3.3825 | 0.76755 | 0.818 | 0.807 | |
| ASU4 | 3.1992 | 0.78496 | 0.724 | 0.723 | |
| ASU5 | 3.2829 | 0.71251 | 0.426 | - | |
| Perceived Usability | PRU1 | 3.7331 | 0.80278 | 0.796 | 0.795 |
| PRU2 | 3.5339 | 0.75488 | 0.885 | 0.883 | |
| PRU3 | 3.6972 | 0.78737 | 0.764 | 0.765 | |
| Goodness-of-Fit Measures of SEM | Parameter Estimates | Minimum Cut-Off |
|---|---|---|
| Incremental Fit Index (IFI) | 0.888 | >0.80 |
| Tucker–Lewis Index (TLI) | 0.868 | >0.80 |
| Comparative Fit Index (CFI) | 0.886 | >0.80 |
| Goodness-of-Fit Index (GFI) | 0.876 | >0.80 |
| Adjusted Goodness-of-Fit Index (AGFI) | 0.828 | >0.80 |
| Root Mean Square Error (RMSEA) | 0.068 | <0.07 |
| No | Variable | Direct Effect | p-Value | Indirect Effect | p-Value | Total Effect | p-Value |
|---|---|---|---|---|---|---|---|
| 1 | SE → PEOU | 0.791 | 0.012 | - | - | 0.791 | 0.012 |
| 2 | IU → ASU | 0.596 | 0.032 | - | - | 0.596 | 0.032 |
| 3 | SI → PU | 0.502 | 0.020 | - | - | 0.502 | 0.020 |
| 4 | PU → IU | 0.456 | 0.010 | - | - | 0.456 | 0.010 |
| 5 | SA → PU | 0.341 | 0.003 | - | - | 0.341 | 0.003 |
| 6 | CO → IU | 0.300 | 0.009 | - | - | 0.300 | 0.009 |
| 7 | PEOU → IU | 0.266 | 0.036 | - | - | 0.266 | 0.036 |
| 8 | VO → IU | 0.596 | 0.011 | - | - | 0.596 | 0.011 |
| 9 | ASU → PRU | 0.850 | 0.008 | - | - | 0.850 | 0.008 |
| 10 | SE → IU | - | - | 0.210 | 0.026 | 0.210 | 0.026 |
| 11 | SA → IU | - | - | 0.155 | 0.003 | 0.155 | 0.003 |
| 12 | SI → IU | - | - | 0.229 | 0.009 | 0.229 | 0.009 |
| 13 | CO → ASU | - | - | 0.179 | 0.009 | 0.179 | 0.009 |
| 14 | VO → ASU | - | - | 0.152 | 0.012 | −0.152 | 0.012 |
| 15 | SE → ASU | - | - | 0.125 | 0.030 | 0.125 | 0.030 |
| 16 | SA → ASU | - | - | 0.093 | 0.005 | 0.093 | 0.005 |
| 17 | SI → ASU | - | - | 0.137 | 0.016 | 0.137 | 0.016 |
| 18 | PEOU → ASU | - | - | 0.158 | 0.036 | 0.158 | 0.036 |
| 19 | PU → ASU | - | - | 0.272 | 0.018 | 0.272 | 0.018 |
| 20 | CO → PRU | - | - | 0.152 | 0.008 | 0.152 | 0.008 |
| 21 | VO → PRU | - | - | 0.129 | 0.010 | −0.129 | 0.010 |
| 22 | SE → PRU | - | - | 0.106 | 0.028 | 0.106 | 0.028 |
| 23 | SA → PRU | - | - | 0.079 | 0.002 | 0.079 | 0.002 |
| 24 | SI → PRU | - | - | 0.116 | 0.016 | 0.116 | 0.016 |
| 25 | PEOU → PRU | - | - | 0.135 | 0.032 | 0.135 | 0.032 |
| 26 | PU → PRU | - | - | 0.231 | 0.012 | 0.231 | 0.012 |
| 27 | IU → PRU | - | - | 0.507 | 0.016 | 0.507 | 0.016 |
| Factor | Normalized Importance |
|---|---|
| Social Influence | 55.2% |
| Service Awareness | 58.4% |
| Technology Self-Efficacy | 56.0% |
| Perceived Usefulness | 50.7% |
| Perceived Ease of Use | 65.3% |
| Convenience | 78.1% |
| Voluntariness | 100% |
| Intention to Use | 54.4% |
| Actual System Use | 45.7% |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yuduang, N.; Ong, A.K.S.; Vista, N.B.; Prasetyo, Y.T.; Nadlifatin, R.; Persada, S.F.; Gumasing, M.J.J.; German, J.D.; Robas, K.P.E.; Chuenyindee, T.; et al. Utilizing Structural Equation Modeling–Artificial Neural Network Hybrid Approach in Determining Factors Affecting Perceived Usability of Mobile Mental Health Application in the Philippines. Int. J. Environ. Res. Public Health 2022, 19, 6732. https://doi.org/10.3390/ijerph19116732
Yuduang N, Ong AKS, Vista NB, Prasetyo YT, Nadlifatin R, Persada SF, Gumasing MJJ, German JD, Robas KPE, Chuenyindee T, et al. Utilizing Structural Equation Modeling–Artificial Neural Network Hybrid Approach in Determining Factors Affecting Perceived Usability of Mobile Mental Health Application in the Philippines. International Journal of Environmental Research and Public Health. 2022; 19(11):6732. https://doi.org/10.3390/ijerph19116732
Chicago/Turabian StyleYuduang, Nattakit, Ardvin Kester S. Ong, Nicole B. Vista, Yogi Tri Prasetyo, Reny Nadlifatin, Satria Fadil Persada, Ma. Janice J. Gumasing, Josephine D. German, Kirstien Paola E. Robas, Thanatorn Chuenyindee, and et al. 2022. "Utilizing Structural Equation Modeling–Artificial Neural Network Hybrid Approach in Determining Factors Affecting Perceived Usability of Mobile Mental Health Application in the Philippines" International Journal of Environmental Research and Public Health 19, no. 11: 6732. https://doi.org/10.3390/ijerph19116732
APA StyleYuduang, N., Ong, A. K. S., Vista, N. B., Prasetyo, Y. T., Nadlifatin, R., Persada, S. F., Gumasing, M. J. J., German, J. D., Robas, K. P. E., Chuenyindee, T., & Buaphiban, T. (2022). Utilizing Structural Equation Modeling–Artificial Neural Network Hybrid Approach in Determining Factors Affecting Perceived Usability of Mobile Mental Health Application in the Philippines. International Journal of Environmental Research and Public Health, 19(11), 6732. https://doi.org/10.3390/ijerph19116732









